Narrow-band imaging with magnifying endoscopy is accurate for detecting gastric intestinal metaplasia
|
|
|
- James Tucker
- 5 years ago
- Views:
Transcription
1 Online Submissions: doi: /wjg.v19.i World J Gastroenterol 2013 May 7; 19(17): ISSN (print) ISSN (online) 2013 Baishideng. All rights reserved. BRIEF ARTICLE Narrow-band imaging with magnifying endoscopy is accurate for detecting gastric intestinal metaplasia Edoardo Savarino, Marina Corbo, Pietro Dulbecco, Lorenzo Gemignani, Elisa Giambruno, Luca Mastracci, Federica Grillo, Vincenzo Savarino Edoardo Savarino, Gastroenterology Unit, Department of Surgical, Oncological and Gastroenterological Sciences, University of Padua, Padua, Italy Marina Corbo, Pietro Dulbecco, Lorenzo Gemignani, Elisa Giambruno, Vincenzo Savarino, Gastroenterology Unit, Department of Internal Medicine, University of Genoa, Genoa, Italy Luca Mastracci, Federica Grillo, Department of Anatomic Pathology, University of Genoa, Genoa, Italy Author contributions: Savarino E, Corbo M, Dulbecco P and Savarino V designed the research; Savarino E, Corbo M, Dulbecco P and Giambruno E collected data; Savarino E, Corbo M, Dulbecco P, Gemignani L, Mastracci L and Grillo F analysed data; and Savarino E, Corbo M, Gemignani L and Savarino V wrote the paper. Correspondence to: Edoardo Savarino, MD, PhD, Gastroenterology Unit, Department of Internal Medicine, University of Genoa, Viale Benedetto XV, Genova, Italy. edoardosavarino@gmail.it Telephone: Fax: Received: November 11, 2012 Revised: February 14, 2013 Accepted: March 6, 2013 Published online: May 7, 2013 Abstract AIM: To investigate the predictive value of narrowband imaging with magnifying endoscopy (NBI-ME) for identifying gastric intestinal metaplasia (GIM) in unselected patients. METHODS: We prospectively evaluated consecutive patients undergoing upper endoscopy for various indications, such as epigastric discomfort/pain, anaemia, gastro-oesophageal reflux disease, suspicion of peptic ulcer disease, or chronic liver diseases. Patients underwent NBI-ME, which was performed by three blinded, experienced endoscopists. In addition, five biopsies (2 antrum, 1 angulus, and 2 corpus) were taken and examined by two pathologists unaware of the endoscopic findings to determine the presence or absence of GIM. The correlation between light blue crest (LBC) appearance and histology was measured. Moreover, we quantified the degree of LBC appearance as less than 20% (+), 20%-80% (++) and more than 80% (+++) of an image field, and the semiquantitative evaluation of LBC appearance was correlated with IM percentage from the histological findings. RESULTS: We enrolled 100 (58 F/42 M) patients who were mainly referred for gastro-esophageal reflux disease/dyspepsia (46%), cancer screening/anaemia (34%), chronic liver disease (9%), and suspected celiac disease (6%); the remaining patients were referred for other indications. The prevalence of Helicobacter pylori (H. pylori ) infection detected from the biopsies was 31%, while 67% of the patients used proton pump inhibitors. LBCs were found in the antrum of 33 patients (33%); 20 of the cases were classified as LBC+, 9 as LBC++, and 4 as LBC+++. LBCs were found in the gastric body of 6 patients (6%), with 5 of them also having LBCs in the antrum. The correlation between the appearance of LBCs and histological GIM was good, with a sensitivity of 80% (95%CI: 67-92), a specificity of 96% (95%CI: 93-99), a positive predictive value of 84% (95%CI: 73-96), a negative predictive value of 95% (95%CI: 92-98), and an accuracy of 93% (95%CI: 90-97). The NBI-ME examination overlooked GIM in 8 cases, but the GIM was less than 5% in 7 of the cases. Moreover, in the 6 false positive cases, the histological examination showed the presence of reactive gastropathy (4 cases) or H. pylori active chronic gastritis (2 cases). The semiquantitative correlation between the rate of LBC appearance and the percentage of GIM was 79% (P < 0.01). CONCLUSION: NBI-ME achieved good sensitivity and specificity in recognising GIM in an unselected population. In routine clinical practice, this technique can reliably target gastric biopsies May 7, 2013 Volume 19 Issue 17
2 2013 Baishideng. All rights reserved. Key words: Narrow-band imaging; Magnification; Gastric intestinal metaplasia; Light blue crest; Gastric cancer; Endoscopy; Precancerous conditions; Gastric biopsy Core tip: Gastric cancer is one of the most common neoplastic diseases in the Western world and has a poor prognosis and inconsistent signs and symptoms in the early phases. Narrow-band imaging with magnifying endoscopy was shown to be a valid method for intestinal metaplasia (IM) detection, this technique can reliably target which patients should be biopsied to evaluate IM and those who do not need biopsies. Moreover, a semi-quantitative evaluation of light blue crest appearance was feasible as there was a good correlation with the histological assessment of IM percentage. Savarino E, Corbo M, Dulbecco P, Gemignani L, Giambruno E, Mastracci L, Grillo F, Savarino V. Narrow-band imaging with magnifying endoscopy is accurate for detecting gastric intestinal metaplasia. World J Gastroenterol 2013; 19(17): Available from: URL: v19/i17/2668.htm DOI: i INTRODUCTION Gastric cancer is the fourth most common cancer and the second leading cause of cancer-related death worldwide [1,2]. However, the mechanism of gastric carcinogenesis is unknown. The intestinal type tumour, according to the Lauren classification, is characterised by the presence of malignant cells forming glandular structures; in contrast to diffuse type carcinomas, these tumours are generally thought to be preceded by a sequence of precursor lesions. In this multistep model of gastric carcinogenesis, described several years ago by Correa et al [3], Helicobacter pylori (H. pylori) causes chronic inflammation of the gastric mucosa, which slowly progresses through the premalignant stages of atrophic gastritis, intestinal metaplasia and dysplasia, intramucosal carcinoma and invasive neoplasia [4]. Intestinal metaplasia (IM) is generally considered as the field cancerization in the gastric mucosa. At the cell level, intestinalized glands provide the cellular substrate that allows the gastric non-invasive neoplasia to develop. The reported progression rates of IM and dysplasia to cancer vary greatly from 0% to 10% per year for IM and from 0% to 73% per year for dysplasia [1]. The prevalence of this condition in Europe varies by country [5-9] ; for instance, a Swedish group reported an IM prevalence of 23% in the general population [10], while the prevalence has been estimated to be up to 25% in the Italian population, mainly occurring in the gastric antrum [7,11-13]. In Western countries, premalignant gastric lesions and early gastric cancer are generally diagnosed upon histologic examination of random biopsies, whereas in Asian countries, especially in Japan, the presence and extension of these lesions are frequently established during an endoscopy [14-16]. These remarkable differences are explained by different training and attitudes towards the inspection of the stomach in countries with a high gastric cancer incidence. The narrow-band imaging system (NBI) is based on the modification of optical filter spectral characteristics in the light source, which improves the visibility of mucosal structures. NBI may be combined with magnification endoscopy to obtain a clear visualisation of surface and vascular patterns [1,2]. Earlier studies using the NBI system with magnification endoscopy (NBI-ME) in the gastric mucosa showed that the appearance of a light blue crest (LBC) in the mucosa is a distinctive endoscopic finding that suggests an increased likelihood of detecting IM in the stomach. More precisely, blue-whitish patchy areas are often observed in NBI images of the antrum in patients with gastric IM. Uedo et al [16] tested NBI-ME on 34 patients with atrophic gastritis and found that the LBC appearance was frequently observed in gastric antrum as blue-white lines visible on the epithelial surface. These authors demonstrated that the appearance of LBCs correlated with histological evidence of IM, with a sensitivity of 89% (95%CI: 83-96), a specificity of 93% (95%CI: 88-97), a positive predictive value of 91% (95%CI: 85-96), a negative predictive value of 92% (95%CI: 87-97) and an accuracy of 91% (95%CI: 88-95). Despite these promising findings, the added value of NBI-ME in the stomach, and more precisely in detecting premalignant and malignant gastric lesions, requires confirmation from controlled longitudinal trials. Furthermore, a uniform and validated classification system is needed. Thus, the aim of our study was to define the value of NBI-ME for identifying gastric IM in an unselected population through the visualisation of LBC appearance. A secondary aim was to provide a semiquantitative evaluation of LBC appearance and to verify a correlation with the histological measurement of IM percentage. MATERIALS AND METHODS Subjects This prospective, blinded study included unselected consecutive patients presenting to the endoscopy unit of the University Hospital of Genoa, Italy. Patients underwent an upper endoscopy for various indications, such as epigastric discomfort/pain, anaemia, gastro-oesophageal reflux disease, suspicion of peptic ulcer disease, or chronic liver diseases. Exclusion criteria included a previous gastrectomy or partial gastric resection; treatment with antiplatelet medication, anticoagulant medication or nonsteroidal anti-inflammatory drugs; and the presence of haemorrhagic diseases. The study protocol was approved by the local Ethics Committee and was performed according to the Declaration of Helsinki. All patients pro May 7, 2013 Volume 19 Issue 17
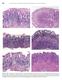
3 A B C D Figure 1 Normal mucosal aspects. A: Narrow-band-imaging with magnification endoscopy examination and the degree of light blue crest appearance; B: Light blue crest (LBC) +, less than 20%; C: LBC ++, 20%-80%; D: LBC +++, 80% or more. vided written informed consent before the start of the study. Study protocol All subjects who agreed to participate in our investigation underwent a thorough physical and clinical examination, a careful collection of their medical history (including current medications, tobacco use, and alcohol and coffee consumption) and an upper gastric intestinal (GI) endoscopy with the NBI-ME system to determine the presence or absence of gastric IM. Five biopsies (2 antrum, 1 angulus and 2 corpus) were collected from all patients according to the updated Sydney classification [17]. Endoscopic procedure The endoscopic examinations were performed by experienced endoscopists (Corbo M, Savarino E, and Dulbecco P) who were blinded to the conditions and medical histories of the patients. Before starting the study, each endoscopist underwent training to obtain good expertise in the detection of IM using NBI-ME. Each endoscopist performed > 300 NBI-ME gastroscopies in patients selected independently of a previous diagnosis of IM and compared their NBI-ME findings with those obtained after a histologic evaluation. At the end of this training, the overall ability to detect histologic IM using NBI-ME was very high (92%). The procedure was conducted with a magnifying endoscope (GIF-Q160Z; Olympus Medical Systems, Tokyo, Japan; 10.9 mm outer diameter insertion tube with a 2.8 mm channel diameter; optical magnification 115). A disposable attachment was fitted to the scope tip to maintain focal distance from the mucosa for magnifying observation (approximately 2 mm). A conscious sedation was performed at the request of the patient. Before the procedure, all patients ingested 66.6 mg of simethicone diluted in 40 ml of water (Istituto Biochimico Italiano Giovanni Lorenzini S.p.A., Aprilia, Italy). If poor visualisation persisted, the gastric mucosal surface was rinsed with an additional ml of the simethicone solution. After white light examination, the gastric antrum and body were examined by NBI for bluewhitish patchy areas and then by NBI-ME observation at the maximum magnification, as LBC was frequently observed in these areas. If no blue-whitish areas were observed, NBI-ME was conducted at the proximal and distal portions of the following areas: the anterior wall, the lesser curvature, the posterior wall, and the greater curvature, as previously described [16]. During NBI-ME observation, we assessed for the presence or absence of LBCs, defined as a fine, blue-white lines on the crests of the epithelial surface that are similar in appearance to the light reflected from a mirror. The patient was defined as LBC-negative if LBCs were not observed in any of the image fields and as LBC-positive if LBCs were observed in any of the image fields. Moreover, we quantified the degree of LBC appearance as less than 20% (+), 20%-80% (++) and more than 80% (+++) of an image field (Figure 1). In each examination, six pictures were taken and stored (one during NBI and two during NBI- ME observation, both in the antrum and in the corpus) May 7, 2013 Volume 19 Issue 17
4 Table 1 Demographic and clinical characteristics of unselected patients (n = 100) included in the study n (%) Demographic and clinical features Patients Age, yr (mean ± SD) 67 ± 12 Sex Male 42 (42) Female 58 (58) H. pylori infection Positive 31(31) Negative 69 (69) Smoking Non-smoker 68 (68) Current smoker 16 (16) Former smoker 16 (16) Alcohol consuming Non-drinker 75 (75) Current drinker 25 (25) Medication PPI users 67 (67) Light blue crests Present 33 (33) Absent 67 (67) Data are expressed as absolute numbers (percentages) or mean ± SD. H. pylori: Helicobacter pylori; PPI: Proton-pump inhibitors. A five biopsy set (2 antrum, 1 angulus, and 2 corpus) of LBC-positive areas was collected in all LBC-positive examinations; biopsy samples were taken from the non- LBC mucosa in the LBC-negative patients. Histological assessment All biopsy specimens were immersed in formalin and then embedded in paraffin. Sections cut from the paraffin blocks were stained with haematoxylin and eosin, Alcian blue PAS and Giemsa. The histological findings were evaluated by two expert pathologists who specialised in GI pathology; the pathologists were unaware of the medical history of the patients and of the endoscopic findings regarding LBC appearance. Inflammation, atrophy, metaplasia and dysplasia were classified according to the updated Sydney system [17] and the revised Vienna classification [18]. Intestinal metaplasia was also expressed as the percentage of metaplastic glands on the entire antral or oxyntic mucosa specimens. Moreover, each sample was evaluated for the presence of H. pylori. Statistical analysis Based on prior studies reporting a sensitivity of more than 80% and a specificity of more than 90%, we determined that a cohort of 100 patients was needed to detect an effect with a confidence interval of 95%, a sensitivity of 80% (interval width of 17%), and a specificity of 90% (interval width of 13%) (calculated with the Clopper- Pearson method using PASS 11; NCSS, LLC, Kaysville, Utah, United States; The sensitivity, specificity, positive and negative predictive values and accuracy were calculated and expressed as percentages and 95%CI. Pearson correlation analysis was used to compare the LBC grading with the percentage of histologically as- Table 2 Relationship between narrow-band-imaging with magnification endoscopy ranking and the percentage of gastric intestinal metaplasia detected by histological assessment Intestinal metaplasia LBC (n ) Total (n ) Negative % % %-45% %-80% % LBC: Light blue crest. sessed metaplasia. RESULTS The study included 100 consecutive patients (58 F/42 M, mean age 67 ± 12 years) who presented at our endoscopy unit between December 2010 and February The demographic and clinical characteristics of the patients are shown in Table 1. The patients were referred to our endoscopy unit mainly because of gastro-oesophageal reflux disease and/or dyspepsia symptoms (46%); 34% underwent the endoscopic procedure for cancer screening, anaemia, a positive faecal occult blood test or suspicion of a peptic ulcer; 9% for chronic liver disease; 6% for suspected celiac disease and the remaining patients for other indications. The prevalence of H. pylori infection on the biopsies was 31%; in addition, 67% of the patients used proton pump inhibitors, 16% were current smokers, and 25% of the patients were alcohol consumers. Endoscopic and histological findings During the upper NBI-ME procedure, we observed LBC appearance in the gastric antrum of 33 patients (33%); 20 of the LBCs were classified as LBC+, 9 as LBC++, and 4 as LBC+++. Moreover, we detected LBC appearance in the gastric body in only 6 patients (6%), and 5 of the patients also had LBC appearance in the antrum; of these, 3 cases were classified as LBC+, 2 as LBC++, and 1 as LBC+++. Intestinal metaplasia in the biopsy specimens (2 antrum, 1 angulus and 2 corpus) obtained during the endoscopy from both LBC-positive and -negative patients was classified as complete and incomplete based on special staining. Gastric IM was histologically detected in 35 (35%) patients, and 27 cases were LBC-positive. In five patients, histological IM was found in both the antrum and body, and this finding correlated with LBC appearance at both sites. A percentage of IM greater than 20% was observed in 13 (13%) of the cases. Accuracy of LBC presence for diagnosing gastric intestinal metaplasia For the diagnosis of IM, compared to histological assessment, the NBI-ME findings had an accuracy of 93% 2671 May 7, 2013 Volume 19 Issue 17
5 Flase negative n = 8 False positive n = 6 True negative n = 59 True positive n = 27 % Intestinal metaplasia LBC appearance ranking (degrees 1 to 4) Figure 2 Graphic representation of the correlation between the degree of light blue crest appearance during narrow-band imaging with magnifying endoscopy examination and the percentage of gastric intestinal metaplasia detected by histological examination. LBC: Light blue crest. (95%CI: 90-97), a sensitivity of 80% (95%CI: 67-92), a specificity of 96% (95%CI: 93-99), a positive predictive value of 84% (95%CI: 73-96), and a negative predictive value of 95% (95%CI: 92-98). Interestingly, in our study, the NBI-ME examination overlooked the presence of gastric IM in 8 cases (false negative cases), and 7 out of the 8 cases had an IM that was less than 5%. Moreover, in the 6 false positive cases, the histological examination showed the presence of reactive gastropathy (4 cases) or H. pylori active chronic gastritis (2 cases). The semiquantitative correlation between the grades of LBC appearance and the percentage of histological IM is shown in Table 2 and Figure 2; the correlation index was 79% (P < 0.01). DISCUSSION Intestinal metaplasia has been widely studied as the main mucosal background for the development of oesophageal and gastric adenocarcinomas. However, to date, no endoscopic patterns that clearly define IM or dysplasia in the stomach have been found. Kaminishi et al [19] evaluated the accuracy of endoscopic findings for diagnosing chronic gastritis and found that ash-coloured nodular changes were highly specific (98% ± 99%) but had a very poor sensitivity (6% ± 12%) for detecting histological IM; the authors concluded that conventional endoscopy is not really useful for diagnosing gastric IM. Later, Dinis-Ribeiro et al [20] observed that magnifying chromoendoscopy with methylene blue staining had good sensitivity (76%) and specificity (87%) for detecting gastric IM. Moreover, methylene blue chromoendoscopy has been found to be useful for assessing the extent of IM [21]. However, this latter technique is time consuming and has some limitations, including the need for preparation with mucolytic agents, dye spraying and vigorous irrigation of the mucosal surface; furthermore, a recent report suggests that methylene blue chromoendoscopy induced questionable oxidative DNA damage in a patient with Barrett s mucosa [22]. Therefore, collecting biopsies for subsequent histological evaluation remains the current gold standard for diagnosing IM. However, the fact that premalignant gastric lesions may occur multifocally represents a limitation of random biopsy sampling. Several new imaging techniques have been developed recently to improve the diagnostic yield of endoscopy. The NBI-ME system has the practical advantage of not requiring complex preparation procedures, the use of any staining technique or a long duration. The additional value of NBI-ME in the detection of gastric pre-malignant lesions is still unclear, especially in countries with a low gastric cancer incidence [7]. Recently, Capelle et al [23] compared the yield of NBI alone to that of white light endoscopy (WLE) in the surveillance of 43 patients with IM and dysplasia. The authors concluded that NBI alone considerably increased the detection of premalignant gastric lesions compared to routine WLE and appeared to be superior to WLE for the surveillance of patients with these advanced gastric lesions. However, a combination of NBI and magnification is likely to provide the best alternative to current endoscopic practice. Previous studies have already demonstrated a high correlation between the microvascular patterns found with NBI-ME and the diagnosis of gastric cancer [24,25]. Moreover, the combined optical technology of NBI with ME has been shown to identify with great accuracy the presence of gastric IM through the visualisation of LBC appearance on the epithelial surface [16]. However, the main limitations of the above-mentioned studies are that they were all conducted in patients with already known diagnoses of intestinal metaplasia/dysplasia/gastric cancer or in a population at a high risk for developing gastric cancer. Other limitations included the small sample sizes and the limited assessment of the gastric antrum and angulus with the exclusion of the gastric body. Therefore, no prospective data are available on the diagnostic utility and accuracy of NBI-ME for detecting IM in an unselected population presenting at an endos May 7, 2013 Volume 19 Issue 17
6 copy unit in routine clinical practice. Our study showed that NBI-ME allowed us to detect gastric IM areas with an accuracy of 93%, a sensitivity of 80%, a specificity of 96%, a positive predictive value of 84% and a negative predictive value of 95%. These results are similar to those recently published by Pimentel-Nunes et al [26], who found a sensitivity of 68% and a specificity of 87% using the same method and a simplified classification system for NBI in the diagnosis of gastric lesions. In our investigation, NBI-ME underestimated the presence of IM in 8 patients; for 7 of these patients, metaplasia was histologically estimated to be less than 5%. The fact that NBI-ME has its major limitation in identifying gastric IM lower than 5% when performed by experienced endoscopists represents a new finding about the diagnostic yield of this technique; at this stage, we can assume that this value constitutes the sensitivity limit of this technique. The false positive cases (6 patients) presented with a histological diagnosis of reactive gastropathy (4 cases) or H. pylori active chronic gastritis (2 cases). Both of these conditions may sometimes represent a confounding factor because they show endoscopic features similar to those of gastric IM. The prevalence of histologically observed IM in our cohort (35%) was slightly higher than the prevalence estimated in the general Western population (25%) [5-9] and in other studies on the Italian population (20%-30%) [5,8,11-13]. A possible explanation for our findings may be related to the higher mean age and prevalence of H. pylori infection in our patients, as it is well known that H. pylori infection, increased age and smoking (> 20 cigarettes/daily) are the main risk factors for the development of premalignant gastric lesions [27]. However, the prevalence of IM in the general population is reported to be highly variable. Additionally, the majority of data come from studies on patients with dyspeptic symptoms and/or suspected H. pylori infections, while information derived from unselected patients (i.e., consecutive patients enrolled independently of GI symptoms or clinical status) is limited. The semiquantitative evaluation of LBC appearance in our study and its correlation with the histological measurement of IM percentage shows that the agreement was high (79%). Previously, Uedo et al [16] also found a significant correlation between the diffuse positivity of LBC (+++) mucosa and the presence of histological markers of IM, such as immunohistochemical staining for CD10 and Alcian blue/high iron diamine. However, these authors did not assess the correlation between LBC appearance and the percentage of histologic IM. Therefore, to the best of our knowledge, our study is the first to show a good correlation between the degree of IM detected by NBI-ME and the severity of IM identified by histological measurement in a series of consecutive patients without specific indications to perform an upper GI endoscopy. In contrast to Uedo et al [16] who used NBI-ME and Capelle et al [23] who performed NBI alone, we opted to evaluate not only the antrum and the angulus of the stomach but also the body; including the body was recently emphasised in the ESGE guidelines [28], despite the significantly longer examination time. This measurement was included because our intention was to demonstrate the potential application of NBI-ME in a populationbased screening and surveillance setting, and we thought that gastric assessment of only one region of the stomach was not adequate and fully informative. However, IM is predominantly found in the antrum, which was confirmed in our study. Therefore, limiting the endoscopic evaluation to the antrum permits an accurate observation and a shorter duration of the examination. Moreover, it has been shown that three biopsies (two antral and one angular) appear to be the best compromise between acceptable accuracy and ease of use in the detection of IM by endoscopy [29]. Our study had some limitations. First, the study included only a single centre. Further research in larger multicentre prospective studies is necessary to evaluate whether NBI-ME yields adequate results in the detection and grading of gastric IM. Second, the endoscopic procedure of WLE and NBI-ME was performed by the same endoscopist; thus, detection of IM by NBI-ME could possibly be biased by the previous WLE observations. Third, as a learning curve must still be defined, regular training is mandatory to improve our findings. Indeed, despite our prolonged training, we obtained a value of sensitivity that was lower than the value obtained by Uedo et al [16]. This difference was likely the result of differences in training between Japanese and Western gastroenterologists. Due to the higher gastric cancer incidence, Japanese endoscopists are trained to scrutinise gastric mucosal areas that are compatible with atrophy and early cancer and spend more time on a thorough mucosal examination than in Western countries. In addition, uniform criteria for this technique must be adopted in large controlled trials in Western or Eastern countries. In conclusion, NBI-ME was shown to be a valid method for IM detection, except in those cases with IM lower than 5%, which may not be clinically relevant. In routine clinical practice, this technique can reliably target which patients should be biopsied to evaluate IM and those who do not need biopsies. Moreover, a semi-quantitative evaluation of LBC appearance was feasible as there was a good correlation with the histological assessment of IM percentage. COMMENTS Background Gastric cancer is one of the most common neoplastic diseases in the Western world and has a poor prognosis and inconsistent signs and symptoms in the early phases. Therefore, adequate screening and prevention are needed to improve the diagnostic process and to identify this condition and its risk factors earlier. Recently, upper gastric intestinal endoscopy has been enhanced with the addition of the narrow band imaging with magnification endoscopy (NBI-ME) technique, which was found to identify precancerous lesions, such as gastric intestinal metaplasia (GIM). Research frontiers Light blue crests (LBCs) are light-blue patches or lines visible on gastric mucosa by NBI endoscopy. Several studies have demonstrated that LBCs are a sign 2673 May 7, 2013 Volume 19 Issue 17
7 of underlying intestinal metaplasia, with a good correlation between endoscopic findings and histological assessments. Therefore, authors have assessed the predictive values of the NBI-ME technique to identify and estimate the extension of GIM to biopsies of the antrum, angulus and corpus in the stomach. Authors also studied the correlation between the appearance of LBCs and the histological detection of GIM in prospectively recruited consecutive unselected patients. Innovations and breakthroughs One hundred consecutive patients were studied. NBI-ME-aimed gastric bioptic samples were collected (2 in the antrum, 1 in the angulus, and 2 in the corpus) from each patient and compared with the presence or absence of LBCs as stated by skilled endoscopists; the biopsies were assessed according to the pathologists expertise in the upper digestive tract. They determined a correlation of 79% between the appearance of LBCs and histologically assessed GIM. Moreover, authors observed that the appearance of LBCs correlated with the histological evidence of intestinal metaplasia, with a sensitivity of 80%, a specificity of 96%, a positive predictive value of 84%, a negative predictive value of 95% and an overall accuracy of 93%. Their results are similar, if not superior, to those of previously published studies in selected populations. Applications NBI-ME is a good technique to identify areas suggestive of GIM in the stomach and can be used to take adequate biopsies from the stomach to provide the pathologist with a useful sample. This technique is easy to learn and provides an accuracy of greater than 90% for diagnosing GIM. Terminology NBI-ME is an endoscopic technique that uses narrow band imaging to produce superior image contrast combined with a magnification of the image up to 115; this technique enables a more accurate observation of the gastric epithelium. Gastric intestinal metaplasia is a condition characterised by the replacement of gastric epithelial cells with cells of intestinal morphology. GIM is a precancerous condition that can progress towards gastric cancer, especially the intestinal-type according to the Lauren classification. This progress varies from 0% to 10% according to different studies, with a prevalence of more than 20% in Western countries, and is considered to be the breaking point in the Correa sequence of carcinogenesis. Identifying this condition could halt or reverse the neoplastic progression. Peer review This research was performed by endoscopists who belong to single medical center in Italy. This article should be helpful for understanding the efficacy of NBI-magnifying endoscopy in detecting the presence of intestinal metaplasia of stomach. REFERENCES 1 de Vries AC, Haringsma J, Kuipers EJ. The detection, surveillance and treatment of premalignant gastric lesions related to Helicobacter pylori infection. Helicobacter 2007; 12: 1-15 [PMID: DOI: /j x] 2 Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics, CA Cancer J Clin 2005; 55: [PMID: DOI: /canjclin ] 3 Correa P. Human gastric carcinogenesis: a multistep and multifactorial process--first American Cancer Society Award Lecture on Cancer Epidemiology and Prevention. Cancer Res 1992; 52: [PMID: ] 4 Busuttil RA, Boussioutas A. Intestinal metaplasia: a premalignant lesion involved in gastric carcinogenesis. J Gastroenterol Hepatol 2009; 24: [PMID: DOI: /j x] 5 Inghelmann R, Grande E, Francisci S, Verdecchia A, Micheli A, Baili P, Capocaccia R, De Angelis R. Regional estimates of stomach cancer burden in Italy. Tumori 2007; 93: [PMID: ] 6 Peleteiro B, Bastos J, Barros H, Lunet N. Systematic review of the prevalence of gastric intestinal metaplasia and its arealevel association with smoking. Gac Sanit 2008; 22: ; discussion [PMID: ] 7 Craanen ME, Dekker W, Blok P, Ferwerda J, Tytgat GN. Intestinal metaplasia and Helicobacter pylori: an endoscopic bioptic study of the gastric antrum. Gut 1992; 33: [PMID: DOI: /gut ] 8 Zullo A, Hassan C, Romiti A, Giusto M, Guerriero C, Lorenzetti R, Campo SM, Tomao S. Follow-up of intestinal metaplasia in the stomach: When, how and why. World J Gastrointest Oncol 2012; 4: [PMID: DOI: /wjgo. v4.i3.30] 9 Tulassay Z, Stolte M, Engstrand L, Butruk E, Malfertheiner P, Dítê P, Tchernev K, Wong BC, Gottlow M, Eklund S, Wrangstadh M, Herszényi L, Nagy P. Twelve-month endoscopic and histological analysis following proton-pump inhibitorbased triple therapy in Helicobacter pylori-positive patients with gastric ulcers. Scand J Gastroenterol 2010; 45: [PMID: DOI: / ] 10 Petersson F, Borch K, Franzén LE. Prevalence of subtypes of intestinal metaplasia in the general population and in patients with autoimmune chronic atrophic gastritis. Scand J Gastroenterol 2002; 37: [PMID: DOI: / ] 11 Rugge M, Cassaro M, Leandro G, Baffa R, Avellini C, Bufo P, Stracca V, Battaglia G, Fabiano A, Guerini A, Di Mario F. Helicobacter pylori in promotion of gastric carcinogenesis. Dig Dis Sci 1996; 41: [PMID: DOI: / BF ] 12 Romano M, Cuomo A, Gravina AG, Miranda A, Iovene MR, Tiso A, Sica M, Rocco A, Salerno R, Marmo R, Federico A, Nardone G. Empirical levofloxacin-containing versus clarithromycin-containing sequential therapy for Helicobacter pylori eradication: a randomised trial. Gut 2010; 59: [PMID: DOI: /gut ] 13 Cassaro M, Rugge M, Gutierrez O, Leandro G, Graham DY, Genta RM. Topographic patterns of intestinal metaplasia and gastric cancer. Am J Gastroenterol 2000; 95: [PMID: DOI: /j x] 14 Sauerbruch T, Schreiber MA, Schüssler P, Permanetter W. Endoscopy in the diagnosis of gastritis. Diagnostic value of endoscopic criteria in relation to histological diagnosis. Endoscopy 1984; 16: [PMID: DOI: / s ] 15 Endoscopic Classification Review Group. Update on the paris classification of superficial neoplastic lesions in the digestive tract. Endoscopy 2005; 37: [PMID: DOI: /s ] 16 Uedo N, Ishihara R, Iishi H, Yamamoto S, Yamamoto S, Yamada T, Imanaka K, Takeuchi Y, Higashino K, Ishiguro S, Tatsuta M. A new method of diagnosing gastric intestinal metaplasia: narrow-band imaging with magnifying endoscopy. Endoscopy 2006; 38: [PMID: ] 17 Dixon MF, Genta RM, Yardley JH, Correa P. Classification and grading of gastritis. The updated Sydney System. International Workshop on the Histopathology of Gastritis, Houston Am J Surg Pathol 1996; 20: [PMID: DOI: / ] 18 Dixon MF. Gastrointestinal epithelial neoplasia: Vienna revisited. Gut 2002; 51: [PMID: DOI: / gut ] 19 Kaminishi M, Yamaguchi H, Nomura S, Oohara T, Sakai S, Fukutomi H, Nakahara A, Kashimura H, Oda M, Kitahora T, Ichikawa H, Yabana T, Yagawa Y, Sugiyama T, Itabashi M, Unakami M, Oguro Y, Sakita T. Endoscopic classification of chronic gastritis based on a pilot study by the Research Society for Gastritis. Dig Endosc 2002; 14: [DOI: / j x] 20 Dinis-Ribeiro M, da Costa-Pereira A, Lopes C, Lara-Santos L, Guilherme M, Moreira-Dias L, Lomba-Viana H, Ribeiro A, Santos C, Soares J, Mesquita N, Silva R, Lomba-Viana R. Magnification chromoendoscopy for the diagnosis of gastric intestinal metaplasia and dysplasia. Gastrointest Endosc 2003; 57: [PMID: DOI: /mge ] 21 Tatsuta M, Iishi H, Ichii M, Noguchi S, Okuda S, Taniguchi 2674 May 7, 2013 Volume 19 Issue 17
8 H. Chromoendoscopic observations on extension and development of fundal gastritis and intestinal metaplasia. Gastroenterology 1985; 88: [PMID: ] 22 Olliver JR, Wild CP, Sahay P, Dexter S, Hardie LJ. Chromoendoscopy with methylene blue and associated DNA damage in Barrett s oesophagus. Lancet 2003; 362: [PMID: DOI: /S (03) ] 23 Capelle LG, Haringsma J, de Vries AC, Steyerberg EW, Biermann K, van Dekken H, Kuipers EJ. Narrow band imaging for the detection of gastric intestinal metaplasia and dysplasia during surveillance endoscopy. Dig Dis Sci 2010; 55: [PMID: DOI: /s ] 24 Nakayoshi T, Tajiri H, Matsuda K, Kaise M, Ikegami M, Sasaki H. Magnifying endoscopy combined with narrow band imaging system for early gastric cancer: correlation of vascular pattern with histopathology (including video). Endoscopy 2004; 36: [PMID: DOI: / s ] 25 Kaise M, Kato M, Urashima M, Arai Y, Kaneyama H, Kanzazawa Y, Yonezawa J, Yoshida Y, Yoshimura N, Yamasaki T, Goda K, Imazu H, Arakawa H, Mochizuki K, Tajiri H. Magnifying endoscopy combined with narrow-band imaging for differential diagnosis of superficial depressed gastric lesions. Endoscopy 2009; 41: [PMID: DOI: / s ] 26 Pimentel-Nunes P, Dinis-Ribeiro M, Soares JB, Marcos-Pinto R, Santos C, Rolanda C, Bastos RP, Areia M, Afonso L, Bergman J, Sharma P, Gotoda T, Henrique R, Moreira-Dias L. A multicenter validation of an endoscopic classification with narrow band imaging for gastric precancerous and cancerous lesions. Endoscopy 2012; 44: [PMID: DOI: /s ] 27 de Vries AC, van Grieken NC, Looman CW, Casparie MK, de Vries E, Meijer GA, Kuipers EJ. Gastric cancer risk in patients with premalignant gastric lesions: a nationwide cohort study in the Netherlands. Gastroenterology 2008; 134: [PMID: DOI: /j.gastro ] 28 Dinis-Ribeiro M, Areia M, de Vries AC, Marcos-Pinto R, Monteiro-Soares M, O Connor A, Pereira C, Pimentel-Nunes P, Correia R, Ensari A, Dumonceau JM, Machado JC, Macedo G, Malfertheiner P, Matysiak-Budnik T, Megraud F, Miki K, O Morain C, Peek RM, Ponchon T, Ristimaki A, Rembacken B, Carneiro F, Kuipers EJ. Management of precancerous conditions and lesions in the stomach (MAPS): guideline from the European Society of Gastrointestinal Endoscopy (ESGE), European Helicobacter Study Group (EHSG), European Society of Pathology (ESP), and the Sociedade Portuguesa de Endoscopia Digestiva (SPED). Endoscopy 2012; 44: [PMID: DOI: /s ] 29 Mastracci L, Bruno S, Spaggiari P, Ceppa P, Fiocca R. The impact of biopsy number and site on the accuracy of intestinal metaplasia detection in the stomach A morphometric study based on virtual biopsies. Dig Liver Dis 2008; 40: [PMID: DOI: /j.dld ] P- Reviewer Tohda G S- Editor Gou SX L- Editor A E- Editor Zhang DN 2675 May 7, 2013 Volume 19 Issue 17
Identification of gastric atrophic changes: from histopathology to endoscopy
 Evidence in perspective 533 Identification of gastric atrophic changes: from histopathology to endoscopy Authors Mário Dinis-Ribeiro 1,2, Ernst J. Kuipers 3 Institutions Bibliography DOI http://dx.doi.org/
Evidence in perspective 533 Identification of gastric atrophic changes: from histopathology to endoscopy Authors Mário Dinis-Ribeiro 1,2, Ernst J. Kuipers 3 Institutions Bibliography DOI http://dx.doi.org/
Narrow Band Imaging for the Detection of Gastric Intestinal Metaplasia and Dysplasia During Surveillance Endoscopy
 Dig Dis Sci (2010) 55:3442 3448 DOI 10.1007/s10620-010-1189-2 ORIGINAL ARTICLE Narrow Band Imaging for the Detection of Gastric Intestinal Metaplasia and Dysplasia During Surveillance Endoscopy Lisette
Dig Dis Sci (2010) 55:3442 3448 DOI 10.1007/s10620-010-1189-2 ORIGINAL ARTICLE Narrow Band Imaging for the Detection of Gastric Intestinal Metaplasia and Dysplasia During Surveillance Endoscopy Lisette
Marginal turbid band and light blue crest, signs observed in magnifying narrow-band imaging endoscopy, are indicative of gastric intestinal metaplasia
 An et al. BMC Gastroenterology 2012, 12:169 RESEARCH ARTICLE Open Access Marginal turbid band and light blue crest, signs observed in magnifying narrow-band imaging endoscopy, are indicative of gastric
An et al. BMC Gastroenterology 2012, 12:169 RESEARCH ARTICLE Open Access Marginal turbid band and light blue crest, signs observed in magnifying narrow-band imaging endoscopy, are indicative of gastric
Helicobacter pylori Improved Detection of Helicobacter pylori
 DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
Introduction. Original articles. Nicolás Rocha, 1 Sandra Huertas, 2 Rosario Albis, 3 Diego Aponte, 4 Luis Carlos Sabbagh. 5
 Original articles Correlation of endoscopic and histological findings in diagnosis of gastrointestinal metaplasia in patients referred to the Clinica Colombia for upper endoscopies Nicolás Rocha, 1 Sandra
Original articles Correlation of endoscopic and histological findings in diagnosis of gastrointestinal metaplasia in patients referred to the Clinica Colombia for upper endoscopies Nicolás Rocha, 1 Sandra
Is there a role for screening gastric carcinoma or preneoplastic lesions?
 Is there a role for screening gastric carcinoma or preneoplastic lesions? Mário Dinis-Ribeiro, MD, PhD Instituto Português de Oncologia do Porto, Department of Gastroenterology Faculty of Medicine, University
Is there a role for screening gastric carcinoma or preneoplastic lesions? Mário Dinis-Ribeiro, MD, PhD Instituto Português de Oncologia do Porto, Department of Gastroenterology Faculty of Medicine, University
Gastric atrophy: use of OLGA staging system in practice
 Gastroenterology and Hepatology From Bed to Bench. 2016 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Gastric atrophy: use of OLGA staging system in practice Mahsa
Gastroenterology and Hepatology From Bed to Bench. 2016 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Gastric atrophy: use of OLGA staging system in practice Mahsa
A multicenter validation of an endoscopic classification with narrow band imaging for gastric precancerous and cancerous lesions
 236 A multicenter validation of an endoscopic classification with narrow band imaging for gastric precancerous and cancerous lesions Authors P. Pimentel-Nunes 1,2, *, M. Dinis-Ribeiro 1,3, *, J. B. Soares
236 A multicenter validation of an endoscopic classification with narrow band imaging for gastric precancerous and cancerous lesions Authors P. Pimentel-Nunes 1,2, *, M. Dinis-Ribeiro 1,3, *, J. B. Soares
Endoscopic atrophic classification before and after H. pylori eradication is closely associated with histological atrophy and intestinal metaplasia
 E311 before and after H. pylori eradication is closely associated with histological atrophy and intestinal metaplasia Authors Institution Masaaki Kodama, Tadayoshi Okimoto, Ryo Ogawa, Kazuhiro Mizukami,
E311 before and after H. pylori eradication is closely associated with histological atrophy and intestinal metaplasia Authors Institution Masaaki Kodama, Tadayoshi Okimoto, Ryo Ogawa, Kazuhiro Mizukami,
A Case and Control Study of the OLGA System s Impact on Detection of Chronic Atrophic Gastritis in Colombia
 Original articles A Case and Control Study of the OLGA System s Impact on Detection of Chronic Atrophic Gastritis in Colombia Diana Martínez, MD, 1 William Otero, MD, 2 Orlando Ricaurte, MD. 3 1 Pathologist
Original articles A Case and Control Study of the OLGA System s Impact on Detection of Chronic Atrophic Gastritis in Colombia Diana Martínez, MD, 1 William Otero, MD, 2 Orlando Ricaurte, MD. 3 1 Pathologist
Correlation between Gastric Mucosal Morphologic Patterns and Histopathological Severity of
 Hindawi Publishing Corporation BioMed Research International Volume 2015, Article ID 808505, 7 pages http://dx.doi.org/10.1155/2015/808505 Research Article Correlation between Gastric Mucosal Morphologic
Hindawi Publishing Corporation BioMed Research International Volume 2015, Article ID 808505, 7 pages http://dx.doi.org/10.1155/2015/808505 Research Article Correlation between Gastric Mucosal Morphologic
JMSCR Vol 05 Issue 07 Page July 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i7.148 Precancerous Risk Assessment of the Gastric
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i7.148 Precancerous Risk Assessment of the Gastric
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/48400
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/48400
Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions
 Showa Univ J Med Sci 29 3, 297 306, September 2017 Original Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions Shotaro HANAMURA, Kuniyo GOMI,
Showa Univ J Med Sci 29 3, 297 306, September 2017 Original Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions Shotaro HANAMURA, Kuniyo GOMI,
Disclosures. Gastric Intestinal Metaplasia and Early Gastric Cancer: Screening, Surveillance, and Endoscopic Therapy. ASGE Guidelines.
 Gastric Intestinal Metaplasia and Early Gastric Cancer: Screening, Surveillance, and Endoscopic Therapy Consultant for: Olympus Medtronic US Endoscopy Disclosures Joo Ha Hwang, MD, PhD Associate Professor
Gastric Intestinal Metaplasia and Early Gastric Cancer: Screening, Surveillance, and Endoscopic Therapy Consultant for: Olympus Medtronic US Endoscopy Disclosures Joo Ha Hwang, MD, PhD Associate Professor
Association of Helicobacter pylori infection with Atrophic gastritis in patients with Dyspepsia
 ADVANCES IN BIORESEARCH Adv. Biores., Vol 8 [3] May 2017: 137-141 2017 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
ADVANCES IN BIORESEARCH Adv. Biores., Vol 8 [3] May 2017: 137-141 2017 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract
 Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
Gastric cancer represents the fourth most common cancer
 GASTROENTEROLOGY 2008;134:945 952 Gastric Cancer Risk in Patients With Premalignant Gastric Lesions: A Nationwide Cohort Study in the Netherlands ANNEMARIE C. DE VRIES,* NICOLE C. T. VAN GRIEKEN, CASPAR
GASTROENTEROLOGY 2008;134:945 952 Gastric Cancer Risk in Patients With Premalignant Gastric Lesions: A Nationwide Cohort Study in the Netherlands ANNEMARIE C. DE VRIES,* NICOLE C. T. VAN GRIEKEN, CASPAR
White opaque substance visualized by magnifying narrow-band imaging is associated with intragastric acid conditions
 Original article White opaque substance visualized by magnifying narrow-band imaging is associated with intragastric acid conditions Authors Kazumi Togo 1,TetsuyaUeo 1,KenshiYao 2,KuratoWada 1, Hideho
Original article White opaque substance visualized by magnifying narrow-band imaging is associated with intragastric acid conditions Authors Kazumi Togo 1,TetsuyaUeo 1,KenshiYao 2,KuratoWada 1, Hideho
Investigation of mucosal pattern of gastric antrum using magnifying narrow-band imaging in patients with chronic atrophic fundic gastritis
 ORIGINAL ARTICLE Annals of Gastroenterology (017) 0, 0-08 Investigation of mucosal pattern of gastric antrum using magnifying narrow-band imaging in patients with chronic atrophic fundic gastritis Yasushi
ORIGINAL ARTICLE Annals of Gastroenterology (017) 0, 0-08 Investigation of mucosal pattern of gastric antrum using magnifying narrow-band imaging in patients with chronic atrophic fundic gastritis Yasushi
Guideline 1. INTRODUCTION!
 74 Management of precancerous conditions and lesions in the stomach (MAPS): guideline from the European Society of Gastrointestinal Endoscopy (ESGE), European Helicobacter Study Group (EHSG), European
74 Management of precancerous conditions and lesions in the stomach (MAPS): guideline from the European Society of Gastrointestinal Endoscopy (ESGE), European Helicobacter Study Group (EHSG), European
Is endoscopic nodular gastritis associated with premalignant lesions?
 ORIGINAL ARTICLE Is endoscopic nodular gastritis associated with premalignant lesions? R. Niknam 1#, A. Manafi 2, M. Maghbool 3, A. Kouhpayeh 4, L. Mahmoudi 5 * # 1 Gastroenterohepatology Research Center,
ORIGINAL ARTICLE Is endoscopic nodular gastritis associated with premalignant lesions? R. Niknam 1#, A. Manafi 2, M. Maghbool 3, A. Kouhpayeh 4, L. Mahmoudi 5 * # 1 Gastroenterohepatology Research Center,
Comparison of the Diagnostic Usefulness of Conventional Magnification and Near-focus Methods with Narrow-band Imaging for Gastric Epithelial Tumors
 ORIGINAL ARTICLE ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2015.15.1.39 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2015;15(1):39-43 Comparison of the Diagnostic Usefulness
ORIGINAL ARTICLE ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2015.15.1.39 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2015;15(1):39-43 Comparison of the Diagnostic Usefulness
Analysis of microvascular density in early gastric carcinoma using magnifying endoscopy with narrow-band imaging
 E832 THIEME Analysis of microvascular density in early gastric using magnifying endoscopy with narrow-band imaging Authors Masashi Kawamura 1, Hiroshi Naganuma 2, Rie Shibuya 2, Tatsuya Kikuchi 1, Yoshitaka
E832 THIEME Analysis of microvascular density in early gastric using magnifying endoscopy with narrow-band imaging Authors Masashi Kawamura 1, Hiroshi Naganuma 2, Rie Shibuya 2, Tatsuya Kikuchi 1, Yoshitaka
Staging of intestinal- and diffuse-type gastric cancers with the OLGA and OLGIM staging systems
 Alimentary Pharmacology and Therapeutics Staging of intestinal- and diffuse-type gastric cancers with the OLGA and OLGIM staging systems S.-J. Cho*, I. J. Choi*, M.-C. Kook*, B.-H. Nam, C. G. Kim*, J.
Alimentary Pharmacology and Therapeutics Staging of intestinal- and diffuse-type gastric cancers with the OLGA and OLGIM staging systems S.-J. Cho*, I. J. Choi*, M.-C. Kook*, B.-H. Nam, C. G. Kim*, J.
Supplementary material Online content viewable at: Guideline
 Management of epithelial precancerous conditions and lesions in the stomach (MAPS II): European Society of Gastrointestinal Endoscopy (ESGE), European Helicobacter and Microbiota Study Group (EHMSG), European
Management of epithelial precancerous conditions and lesions in the stomach (MAPS II): European Society of Gastrointestinal Endoscopy (ESGE), European Helicobacter and Microbiota Study Group (EHMSG), European
Histopathological study of gastric carcinoma with associated precursor lesions
 Original Research Article Histopathological study of gastric carcinoma with associated precursor lesions Manasa G C 1,*, Sunila 2, Manjunath GV 3 1 Assistant Professor, JJM Medical College, Tharalabalu
Original Research Article Histopathological study of gastric carcinoma with associated precursor lesions Manasa G C 1,*, Sunila 2, Manjunath GV 3 1 Assistant Professor, JJM Medical College, Tharalabalu
T he prognosis of gastric carcinoma depends on its stage at
 177 ORIGINAL ARTICLE A follow up model for patients with atrophic chronic gastritis and intestinal metaplasia M Dinis-Ribeiro, C Lopes, A da Costa-Pereira, M Guilherme, J Barbosa, H Lomba-Viana, R Silva,
177 ORIGINAL ARTICLE A follow up model for patients with atrophic chronic gastritis and intestinal metaplasia M Dinis-Ribeiro, C Lopes, A da Costa-Pereira, M Guilherme, J Barbosa, H Lomba-Viana, R Silva,
Ethnic Distribution of Atrophic Autoimmune Gastritis in the United States
 Ethnic Distribution of Atrophic Autoimmune Gastritis in the United States Robert M. Genta, Regan Allen, Massimo Rugge Miraca Life Sciences Research Institute, Miraca Life Sciences, Irving, Texas UTSW University
Ethnic Distribution of Atrophic Autoimmune Gastritis in the United States Robert M. Genta, Regan Allen, Massimo Rugge Miraca Life Sciences Research Institute, Miraca Life Sciences, Irving, Texas UTSW University
What Have We Accomplished in Endoscopic Image Analysis for Atrophic Gastritis?
 REVIEW ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2013.13.1.6 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2013;13(1):6-19 What Have We Accomplished in Endoscopic Image
REVIEW ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2013.13.1.6 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2013;13(1):6-19 What Have We Accomplished in Endoscopic Image
Green epithelium revealed by narrow-band imaging (NBI): a feature for practical assessment of extent of gastric cancer after H. pylori eradication
 Green epithelium revealed by narrow-band imaging (NBI): a feature for practical assessment of extent of gastric cancer after H. pylori eradication Authors Kazuyoshi Yagi 1, Itsuo Nagayama 1, Takahiro Hoshi
Green epithelium revealed by narrow-band imaging (NBI): a feature for practical assessment of extent of gastric cancer after H. pylori eradication Authors Kazuyoshi Yagi 1, Itsuo Nagayama 1, Takahiro Hoshi
University Mainz. Early Gastric Cancer. Ralf Kiesslich. Johannes Gutenberg University Mainz, Germany. Early Gastric Cancer 15.6.
 Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
Correlations Among Endoscopic, Histologic and Serologic Diagnoses for the Assessment of Atrophic Gastritis
 JOURNAL OF CANCER PREVENTION Vol. 19, No. 1, March, 2014 http://dx.doi.org/10.15430/jcp.2014.19.1.47 pissn 2288-3649 ㆍ eissn 2288-3657 Correlations Among Endoscopic, Histologic and Serologic Diagnoses
JOURNAL OF CANCER PREVENTION Vol. 19, No. 1, March, 2014 http://dx.doi.org/10.15430/jcp.2014.19.1.47 pissn 2288-3649 ㆍ eissn 2288-3657 Correlations Among Endoscopic, Histologic and Serologic Diagnoses
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Histopathological Characteristics of Atrophic Gastritis in Adult Population
 Journal of Pharmacy and Pharmacology 3 (2015) 133-138 doi: 10.17265/2328-2150/2015.03.004 D DAVID PUBLISHING Histopathological Characteristics of Atrophic Gastritis in Adult Population Marija Milićević,
Journal of Pharmacy and Pharmacology 3 (2015) 133-138 doi: 10.17265/2328-2150/2015.03.004 D DAVID PUBLISHING Histopathological Characteristics of Atrophic Gastritis in Adult Population Marija Milićević,
ORIGINAL ARTICLE Gastroenterology & Hepatology INTRODUCTION MATERIALS AND METHODS
 ORIGINAL ARTICLE Gastroenterology & Hepatology J Korean Med Sci 2013; 28: 744-749 Interobserver Variability and Accuracy of High-Definition Endoscopic Diagnosis for Gastric Intestinal Metaplasia among
ORIGINAL ARTICLE Gastroenterology & Hepatology J Korean Med Sci 2013; 28: 744-749 Interobserver Variability and Accuracy of High-Definition Endoscopic Diagnosis for Gastric Intestinal Metaplasia among
Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong
 Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Paris classification (2003) 삼성의료원내과이준행
 Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
Gastric Polyps. Bible class
 Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Prevalence of Multiple White and Flat Elevated Lesions in Individuals Undergoing a Medical Checkup
 doi: 10.2169/internalmedicine.9808-17 http://internmed.jp ORIGINAL ARTICLE Prevalence of Multiple White and Flat Elevated Lesions in Individuals Undergoing a Medical Checkup Kyoichi Adachi 1, Tomoko Mishiro
doi: 10.2169/internalmedicine.9808-17 http://internmed.jp ORIGINAL ARTICLE Prevalence of Multiple White and Flat Elevated Lesions in Individuals Undergoing a Medical Checkup Kyoichi Adachi 1, Tomoko Mishiro
Helicobacter pylori Eradication Therapy Success Regarding Different Treatment Period Based on Clarithromycin or Metronidazole Triple-Therapy Regimens
 Helicobacter ISSN 1523-5378 Filipec Blackwell Oxford, HEL 1083-4389 1523-5378 Journal XXX Original H. 2008 pylori Kanizaj compilation The UK Eradication Publishing Article Authors et al. Ltd 2008 Therapy
Helicobacter ISSN 1523-5378 Filipec Blackwell Oxford, HEL 1083-4389 1523-5378 Journal XXX Original H. 2008 pylori Kanizaj compilation The UK Eradication Publishing Article Authors et al. Ltd 2008 Therapy
Prognostic analysis of gastric mucosal dysplasia after endoscopic resection: A single-center retrospective study
 JBUON 2019; 24(2): 679-685 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic analysis of gastric mucosal dysplasia after endoscopic resection:
JBUON 2019; 24(2): 679-685 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic analysis of gastric mucosal dysplasia after endoscopic resection:
Update on the pathological classification of gastritis. Hala El-Zimaity, M.D. M.S. Epidemiology McMaster University Hamilton, Ontario Canada
 Update on the pathological classification of gastritis Hala El-Zimaity, M.D. M.S. Epidemiology McMaster University Hamilton, Ontario Canada CLASSIFICATION GASTRITIS GASTROPATHY 1. Acute 2. Chronic 3. Uncommon
Update on the pathological classification of gastritis Hala El-Zimaity, M.D. M.S. Epidemiology McMaster University Hamilton, Ontario Canada CLASSIFICATION GASTRITIS GASTROPATHY 1. Acute 2. Chronic 3. Uncommon
ESMO Preceptorship Gastrointestinal Tumours Valencia October 2017
 www.esmo.org ESMO Preceptorship Valencia 06-07 October 2017 Gastrointestinal Tumours I have no conflicts of interest to declare Fátima Carneiro Gastrointestinal tumours Multidisciplinary management, standards
www.esmo.org ESMO Preceptorship Valencia 06-07 October 2017 Gastrointestinal Tumours I have no conflicts of interest to declare Fátima Carneiro Gastrointestinal tumours Multidisciplinary management, standards
Diagnosis and management of gastric dysplasia
 REVIEW Korean J Intern Med 2016;31:201-209 Diagnosis and management of gastric dysplasia Jae Kyu Sung Department of Internal Medicine, Chungnam National University School of Medicine, Daejeon, Korea Received
REVIEW Korean J Intern Med 2016;31:201-209 Diagnosis and management of gastric dysplasia Jae Kyu Sung Department of Internal Medicine, Chungnam National University School of Medicine, Daejeon, Korea Received
Case Report Features of the Atrophic Corpus Mucosa in Three Cases of Autoimmune Gastritis Revealed by Magnifying Endoscopy
 Volume 2012, Article ID 368160, 4 pages doi:10.1155/2012/368160 Case Report Features of the Atrophic Corpus Mucosa in Three Cases of Autoimmune Gastritis Revealed by Magnifying Endoscopy Kazuyoshi Yagi,
Volume 2012, Article ID 368160, 4 pages doi:10.1155/2012/368160 Case Report Features of the Atrophic Corpus Mucosa in Three Cases of Autoimmune Gastritis Revealed by Magnifying Endoscopy Kazuyoshi Yagi,
594 Lewin, Weinstein, and Riddell s Gastrointestinal Pathology and Its Clinical Implications
 594 Lewin, Weinstein, and Riddell s Gastrointestinal Pathology and Its Clinical Implications Figure 13-20. Stages in the natural history of H. pylori. Biopsies from the antrum are on the left and the oxyntic
594 Lewin, Weinstein, and Riddell s Gastrointestinal Pathology and Its Clinical Implications Figure 13-20. Stages in the natural history of H. pylori. Biopsies from the antrum are on the left and the oxyntic
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
CASE REPORT. Introduction. Case Report. Kimitoshi Kubo 1, Noriko Kimura 2, Katsuhiro Mabe 1, Yusuke Nishimura 1 and Mototsugu Kato 1
 doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
The incidence of neoplasia in patients with autoimmune metaplastic atrophic gastritis: a renewed call for surveillance
 ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 The incidence of neoplasia in patients with autoimmune metaplastic atrophic gastritis: a renewed call for surveillance Nadim Mahmud a, Kristen
ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 The incidence of neoplasia in patients with autoimmune metaplastic atrophic gastritis: a renewed call for surveillance Nadim Mahmud a, Kristen
Original Article. Abstract
 Original Article Association of helicobacter pylori with carcinoma of stomach Muhammad Arif, Serajuddaula Syed Department of Pathology, Sindh Medical College, Karachi Abstract Objective: To note the association
Original Article Association of helicobacter pylori with carcinoma of stomach Muhammad Arif, Serajuddaula Syed Department of Pathology, Sindh Medical College, Karachi Abstract Objective: To note the association
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Table 2.9. Case control studies of helicobacter pylori infection and oesophageal adenocarcinoma
 Characteristics of Characteristics of controls Detection Chow et al (1998) 1993-1995 129 of newly diagnosed oesophageal/gastric cardia (OGC) adenocarcinoma. 224 population controls selected by random digit
Characteristics of Characteristics of controls Detection Chow et al (1998) 1993-1995 129 of newly diagnosed oesophageal/gastric cardia (OGC) adenocarcinoma. 224 population controls selected by random digit
THE PREVALENCE OF ATROPHIC GASTRITIS IN DYSPEPTIC PATIENTS AND ITS RISK FACTORS ABSTRACT
 THE PREVALENCE OF ATROPHIC GASTRITIS IN DYSPEPTIC PATIENTS AND ITS RISK FACTORS AZADBAKHT SALEH 1,2, MORADNIANI MOSAYEB 2, MIRBEIK-SABZEVARI ZOHRE 3*, AALIEHPOUR ASGHAR 4, AZADBAKHT SALEHEH 3 1 Hepatitis
THE PREVALENCE OF ATROPHIC GASTRITIS IN DYSPEPTIC PATIENTS AND ITS RISK FACTORS AZADBAKHT SALEH 1,2, MORADNIANI MOSAYEB 2, MIRBEIK-SABZEVARI ZOHRE 3*, AALIEHPOUR ASGHAR 4, AZADBAKHT SALEHEH 3 1 Hepatitis
Key quality measures in upper GI endoscopy. Report of the upper GI working group
 Key quality measures in upper GI endoscopy. Report of the upper GI working group Prof Dr. R. Bisschops University Hospitals Leuven KU Leuven Head of endoscopy raf.bisschops@uzleuven.be UPPER GI QM WORKING
Key quality measures in upper GI endoscopy. Report of the upper GI working group Prof Dr. R. Bisschops University Hospitals Leuven KU Leuven Head of endoscopy raf.bisschops@uzleuven.be UPPER GI QM WORKING
Case Report White opaque substance in superficial esophageal squamous cell carcinoma: report of a case
 Int J Clin Exp Pathol 2017;10(3):3565-3569 www.ijcep.com /ISSN:1936-2625/IJCEP0043182 Case Report White opaque substance in superficial esophageal squamous cell carcinoma: report of a case Honglei Wu 1,
Int J Clin Exp Pathol 2017;10(3):3565-3569 www.ijcep.com /ISSN:1936-2625/IJCEP0043182 Case Report White opaque substance in superficial esophageal squamous cell carcinoma: report of a case Honglei Wu 1,
Histopathology: gastritis and peptic ulceration
 Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 9: 1209-1214, 2015 Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions TATSUYA TOYOKAWA
EXPERIMENTAL AND THERAPEUTIC MEDICINE 9: 1209-1214, 2015 Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions TATSUYA TOYOKAWA
Comprehensive Investigation of Areae Gastricae Pattern in Gastric Corpus using
 1 Comprehensive Investigation of Areae Gastricae Pattern in Gastric Corpus using Magnifying Narrow Band Imaging Endoscopy in Patients with Chronic Atrophic Fundic Gastritis Running head: Magnifying NBI
1 Comprehensive Investigation of Areae Gastricae Pattern in Gastric Corpus using Magnifying Narrow Band Imaging Endoscopy in Patients with Chronic Atrophic Fundic Gastritis Running head: Magnifying NBI
Relative risk of dysplasia for patients with intestinal metaplasia in the distal oesophagus and in the gastric cardia
 Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Vital staining and Barrett s esophagus
 Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric Epithelial Neoplasia Patients
 CLINICAL RESEARCH e-issn 1643-3750 DOI: 10.12659/MSM.892697 Received: 2014.10.09 Accepted: 2014.12.03 Published: 2015.04.05 Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric
CLINICAL RESEARCH e-issn 1643-3750 DOI: 10.12659/MSM.892697 Received: 2014.10.09 Accepted: 2014.12.03 Published: 2015.04.05 Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric
Dysplasia 4/19/2017. How do I practice Chromoendoscopy for Surveillance of Colitis? SCENIC: Polypoid Dysplasia in UC. Background
 SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
In 1998, the American College of Gastroenterology issued ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
The white globe appearance (WGA): a novel marker for a correct diagnosis of early gastric cancer by magnifying. endoscopy with narrow-band imaging (M-
 E120 The white globe appearance (WGA): a novel marker for a correct diagnosis of early gastric cancer by magnifying endoscopy with narrow-band imaging (M-NBI) Authors Hisashi Doyama 1, Naohiro Yoshida
E120 The white globe appearance (WGA): a novel marker for a correct diagnosis of early gastric cancer by magnifying endoscopy with narrow-band imaging (M-NBI) Authors Hisashi Doyama 1, Naohiro Yoshida
Sonic hedgehog expression in gastric cancer and gastric adenoma
 ONCOLOGY REPORTS 17: 1051-1055, 2007 Sonic hedgehog expression in gastric cancer and gastric adenoma SUN-YOUNG LEE 1, HYE SEUNG HAN 2, KYUNG YUNG LEE 3, TAE SOOK HWANG 2, JEONG HWAN KIM 1, IN-KYUNG SUNG
ONCOLOGY REPORTS 17: 1051-1055, 2007 Sonic hedgehog expression in gastric cancer and gastric adenoma SUN-YOUNG LEE 1, HYE SEUNG HAN 2, KYUNG YUNG LEE 3, TAE SOOK HWANG 2, JEONG HWAN KIM 1, IN-KYUNG SUNG
Common Inflammatory Gastrointestinal Disorders: Endoscopic and Pathologic Correlations
 Common Inflammatory Gastrointestinal Disorders: Endoscopic and Pathologic Correlations Nicole C. Panarelli, M.D. Attending Pathologist Montefiore Medical Center Associate Professor of Pathology - Albert
Common Inflammatory Gastrointestinal Disorders: Endoscopic and Pathologic Correlations Nicole C. Panarelli, M.D. Attending Pathologist Montefiore Medical Center Associate Professor of Pathology - Albert
Technical and Endoscopic Factors in. in CDH1 Mutation Carriers
 Technical and Endoscopic Factors in Gastric Cancer Surveillance in CDH Mutation Carriers Carol A. Burke,3,5, Michael Cruise 2,5, Lisa LaGuardia 3,5, Margaret O Malley 3,5, Matthew Kalady 3,5, James Church
Technical and Endoscopic Factors in Gastric Cancer Surveillance in CDH Mutation Carriers Carol A. Burke,3,5, Michael Cruise 2,5, Lisa LaGuardia 3,5, Margaret O Malley 3,5, Matthew Kalady 3,5, James Church
The New England Journal of Medicine. Patients
 HELICOBACTER PYLORI INFECTION AND THE DEVELOPMENT OF GASTRIC CANCER NAOMI UEMURA, M.D., SHIRO OKAMOTO, M.D., SOICHIRO YAMAMOTO, M.D., NOBUTOSHI MATSUMURA, M.D., SHUJI YAMAGUCHI, M.D., MICHIO YAMAKIDO,
HELICOBACTER PYLORI INFECTION AND THE DEVELOPMENT OF GASTRIC CANCER NAOMI UEMURA, M.D., SHIRO OKAMOTO, M.D., SOICHIRO YAMAMOTO, M.D., NOBUTOSHI MATSUMURA, M.D., SHUJI YAMAGUCHI, M.D., MICHIO YAMAKIDO,
Histological features of nodular gastritis and its endoscopic classification
 Journal of Digestive Diseases 2011; 12; 436 442 doi: 10.1111/j.1751-2980.2011.00532.x Original article Histological features of nodular gastritis and its endoscopic classification Ryo NAKASHIMA,* Naoyoshi
Journal of Digestive Diseases 2011; 12; 436 442 doi: 10.1111/j.1751-2980.2011.00532.x Original article Histological features of nodular gastritis and its endoscopic classification Ryo NAKASHIMA,* Naoyoshi
Mucosal patterns of Helicobacter pylori-related gastritis without atrophy in the gastric corpus using standard endoscopy
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v16.i4.496 World J Gastroenterol 2010 January 28; 16(4): 496-500 ISSN 1007-9327 (print) 2010 Baishideng. All rights
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v16.i4.496 World J Gastroenterol 2010 January 28; 16(4): 496-500 ISSN 1007-9327 (print) 2010 Baishideng. All rights
The Association of CagA + Helicobacter pylori Infection and Gastric Carcinoma
 The Association of CagA + Helicobacter pylori Infection and Gastric Carcinoma PRESENTER: Dr. Md. Khalilur Rahman Student of M.D.(Internal Medicine) Sylhet MAG Osmani Medical College Gastric Cancer- ranked
The Association of CagA + Helicobacter pylori Infection and Gastric Carcinoma PRESENTER: Dr. Md. Khalilur Rahman Student of M.D.(Internal Medicine) Sylhet MAG Osmani Medical College Gastric Cancer- ranked
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
CLINICAL EFFECTIVENESS
 Re-audit of gastrointestinal tract specimens with respect to compliance with RCPath guidelines Dr Manisha Ram Dr Moina Kadri Background epidemiology and aetiology Over the past 20 years there has been
Re-audit of gastrointestinal tract specimens with respect to compliance with RCPath guidelines Dr Manisha Ram Dr Moina Kadri Background epidemiology and aetiology Over the past 20 years there has been
Correlation Between Endoscopic and Histological Findings in Different Gastroduodenal Lesion and its Association with Helicobacter Pylori
 ORIGINAL ARTICLE Correlation Between Endoscopic and Histological Findings in Different Gastroduodenal Lesion and its Association with Helicobacter Pylori *A. Sultana 1, SM Badruddoza 2, F Rahman 3 1 Dr.
ORIGINAL ARTICLE Correlation Between Endoscopic and Histological Findings in Different Gastroduodenal Lesion and its Association with Helicobacter Pylori *A. Sultana 1, SM Badruddoza 2, F Rahman 3 1 Dr.
Detection of Intestinal Metaplasia among Sudanese Patients with Chronic Gastritis by Using Combined Alcian Blue- PAS Technique
 International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Original Research Article Volume 3, Issue 6-2017 DOI: http://dx.doi.org/10.22192/ijcrms.2017.03.06.011
International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Original Research Article Volume 3, Issue 6-2017 DOI: http://dx.doi.org/10.22192/ijcrms.2017.03.06.011
H M T El-Zimaity, J Ramchatesingh, M Ali Saeed, D Y Graham
 J Clin Pathol 2001;54:679 683 679 Papers Gastrointestinal Mucosa Pathology Laboratory, VA Medical Center and Baylor College of Medicine, Houston, Texas 77030, USA H M T El-Zimaity J Ramchatesingh D Y Graham
J Clin Pathol 2001;54:679 683 679 Papers Gastrointestinal Mucosa Pathology Laboratory, VA Medical Center and Baylor College of Medicine, Houston, Texas 77030, USA H M T El-Zimaity J Ramchatesingh D Y Graham
Intestinal metaplasia at the gastro-oesophageal junction: Helicobacter pylori gastritis or gastro-oesophageal reflux disease?
 Gut 1998;43:17 21 17 Gastroenterology, Hepatology, and Infectious Diseases A Hackelsberger V Schultze G Manes J-E Dominguez-Muñoz P Malfertheiner Pathology, Otto-von-Guericke University, Magdeburg, Germany
Gut 1998;43:17 21 17 Gastroenterology, Hepatology, and Infectious Diseases A Hackelsberger V Schultze G Manes J-E Dominguez-Muñoz P Malfertheiner Pathology, Otto-von-Guericke University, Magdeburg, Germany
Correspondence should be addressed to Sehmus Olmez;
 Gastroenterology Research and Practice Volume 2015, Article ID 434039, 6 pages http://dx.doi.org/10.1155/2015/434039 Clinical Study The Prevalence of Gastric Intestinal Metaplasia and Distribution of Helicobacter
Gastroenterology Research and Practice Volume 2015, Article ID 434039, 6 pages http://dx.doi.org/10.1155/2015/434039 Clinical Study The Prevalence of Gastric Intestinal Metaplasia and Distribution of Helicobacter
Gastric mucosal status in patients with reflux esophagitis
 Gastric mucosal status in patients with reflux esophagitis Riyadh Mohamad Hasan 1, Batool Mutar Mahdi 2 1. Department of Surgery, Al-Kindy College of Medicine, University of Baghdad, Iraq 2. Department
Gastric mucosal status in patients with reflux esophagitis Riyadh Mohamad Hasan 1, Batool Mutar Mahdi 2 1. Department of Surgery, Al-Kindy College of Medicine, University of Baghdad, Iraq 2. Department
Risk Factors for Gastric Tumorigenesis in Underlying Gastric Mucosal Atrophy
 Gut and Liver, Vol. 11, No. 5, September 2017, pp. 612-619 ORiginal Article Risk Factors for Gastric Tumorigenesis in Underlying Gastric Mucosal Atrophy Ji Hyun Song 1, Sang Gyun Kim 2, Eun Hyo Jin 1,
Gut and Liver, Vol. 11, No. 5, September 2017, pp. 612-619 ORiginal Article Risk Factors for Gastric Tumorigenesis in Underlying Gastric Mucosal Atrophy Ji Hyun Song 1, Sang Gyun Kim 2, Eun Hyo Jin 1,
The gastroenterologist and chronic gastritis in daily clinical practice
 Review article The gastroenterologist and chronic gastritis in daily clinical practice William Otero Regino, MD. 1 1 Associate Professor of Medicine in the Gastroenterology Unit of the Universidad Nacional
Review article The gastroenterologist and chronic gastritis in daily clinical practice William Otero Regino, MD. 1 1 Associate Professor of Medicine in the Gastroenterology Unit of the Universidad Nacional
Endoscopic Corner CASE 1. Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R
 170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
Research Article Performance of Routine Helicobacter pylori Invasive Tests in Patients with Dyspepsia
 Gastroenterology Research and Practice Volume 2013, Article ID 184806, 5 pages http://dx.doi.org/10.1155/2013/184806 Research Article Performance of Routine Helicobacter pylori Invasive Tests in Patients
Gastroenterology Research and Practice Volume 2013, Article ID 184806, 5 pages http://dx.doi.org/10.1155/2013/184806 Research Article Performance of Routine Helicobacter pylori Invasive Tests in Patients
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy
 Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Maastricht Ⅴ /Florence
 2016 21 10 577 Maastricht Ⅴ /Florence 200001 2015 10 8 9 Maastricht V 1 / 2 3 4 / 5 Maastricht Ⅴ Interpretation of Management of Helicobacter pylori Infection the Maastricht Ⅴ / Florence Consensus Report
2016 21 10 577 Maastricht Ⅴ /Florence 200001 2015 10 8 9 Maastricht V 1 / 2 3 4 / 5 Maastricht Ⅴ Interpretation of Management of Helicobacter pylori Infection the Maastricht Ⅴ / Florence Consensus Report
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
The yield of UGIE: a study of a ten-year period in the Zaanstreek
 ORIGINAL ARTICLE The yield of UGIE: a study of a ten-year period in the Zaanstreek R.J.L.F. Loffeld *, A.B.M.M. van der Putten Department of Internal Medicine, De Heel Zaans Medical Centre, PO BOX 21,
ORIGINAL ARTICLE The yield of UGIE: a study of a ten-year period in the Zaanstreek R.J.L.F. Loffeld *, A.B.M.M. van der Putten Department of Internal Medicine, De Heel Zaans Medical Centre, PO BOX 21,
Learning Objectives:
 Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Comparative study of invasive methods for diagnosis of Helicobacter pylori in humans
 ISSN: 2319-7706 Volume 2 Number 7 (2013) pp. 63-68 http://www.ijcmas.com Original Research Article Comparative study of invasive methods for diagnosis of Helicobacter pylori in humans V.Subbukesavaraja
ISSN: 2319-7706 Volume 2 Number 7 (2013) pp. 63-68 http://www.ijcmas.com Original Research Article Comparative study of invasive methods for diagnosis of Helicobacter pylori in humans V.Subbukesavaraja
Novel endoscopic observation in Barrett s oesophagus using high resolution magnification endoscopy and narrow band imaging
 Alimentary Pharmacology & Therapeutics Novel endoscopic observation in Barrett s oesophagus using high resolution magnification endoscopy and narrow band imaging G. K. ANAGNOSTOPOULOS*, K. YAO*, P. KAYE,
Alimentary Pharmacology & Therapeutics Novel endoscopic observation in Barrett s oesophagus using high resolution magnification endoscopy and narrow band imaging G. K. ANAGNOSTOPOULOS*, K. YAO*, P. KAYE,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT.
 PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
The international health care burden of cancers of the gastrointestinal tract and liver
 The international health care burden of cancers of the gastrointestinal tract and liver William R. Brown 1*, Dennis J. Ahnen 2 1 Department of Medicine, University of Colorado School of Medicine, Denver,
The international health care burden of cancers of the gastrointestinal tract and liver William R. Brown 1*, Dennis J. Ahnen 2 1 Department of Medicine, University of Colorado School of Medicine, Denver,
Cholecystectomy and duodenogastric reflux: interacting effects over the gastric mucosa
 DOI 10.1186/s40064-016-3641-z RESEARCH Open Access Cholecystectomy and duodenogastric reflux: interacting effects over the gastric mucosa Erdinc Mercan 1, Ugur Duman 1, Deniz Tihan 1, Evren Dilektasli
DOI 10.1186/s40064-016-3641-z RESEARCH Open Access Cholecystectomy and duodenogastric reflux: interacting effects over the gastric mucosa Erdinc Mercan 1, Ugur Duman 1, Deniz Tihan 1, Evren Dilektasli
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
