Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric Epithelial Neoplasia Patients
|
|
|
- Roland McCormick
- 5 years ago
- Views:
Transcription
1 CLINICAL RESEARCH e-issn DOI: /MSM Received: Accepted: Published: Combination of Paris and Vienna Classifications may Optimize Follow-Up of Gastric Epithelial Neoplasia Patients Authors Contribution: Study Design A Data Collection B Statistical Analysis C Data Interpretation D Manuscript Preparation E Literature Search F Funds Collection G ABCEF 1 Wen Hu CEF 2 Xin-Bo Ai BCF 1 Yi-Miao Zhu BC 3 Tie-Mei Han DF 4 Bo Shen ADEG 5 Wen-Sheng Pan 1 Department of Gastroenterology, Second Affiliated Hospital Binjiang Campus, School of Medicine, Zhejiang University, Hangzhou, Zhejiang, P.R. China 2 Department of Gastroenterology, Zhuhai Hospital, Jinan University College of Medicine, Zhuhai, Guangdong, P.R. China 3 Department of Gastroenterology, Fourth Affiliated Hospital, School of Medicine, Zhejiang University, Yiwu, Zhejiang, P.R. China 4 Digestive Disease Institute, Cleveland Clinic, Cleveland, OH, U.S.A. 5 Department of Gastroenterology, Second Affiliated Hospital, School of Medicine, Zhejiang University, Hangzhou, Zhejiang, P.R. China Corresponding Author: Source of support: Wen-Sheng Pan, wspan223@163.com This research was supported by grants from the National Health Key Special Fund (No ), the Health Department Fund (No. 2007A093), the Traditional Chinese Medicine Bureau Fund (No. 2007ZA019), the Natural Science Fund of Zhejiang Province (No. Y and Y12H160121), the Zhejiang Province Education Department Fund (No. Y and Y ), the Zhejiang Province Health Department Fund (No ), the Key Project of Zhejiang Province (No. 2009C and 2013C ), and the National Natural Science Foundation of China (general project No ) Background: Material/Methods: Results: Conclusions: MeSH Keywords: Full-text PDF: The aim of this study was to evaluate the efficiency of the combination of Paris and Vienna classifications in a follow-up study of gastric epithelial neoplasia (GEN) patients. This study was conducted between January 2003 and September 2010, during which 170 biopsy-proven GEN patients were followed up by gastroenterologists and pathologists according to our follow-up regimen (modified Vienna classification). In total, 161 patients with low-grade neoplasia (LGN) and 9 patients with high-grade neoplasia (HGN) were randomly enrolled in our study. Eighteen patients with depressed appearance were observed, of which 9 patients had HGN and 9 patients had low-grade dysplasia (LGD). Three patients with type 0-IIa were observed with lowgrade adenoma (LGA), and type 0 I was observed in 2 patients with LGN. Endoscopic or surgical treatments were performed to avoid potential malignancy or bleeding. Two patients with ulcer lesions, 2 patients with non-depressed type 0 appearance, and 3 patients without visible lesions were shown to have higher-grade lesions during follow-up. The misdiagnosis rate of forceps biopsy 62.07% was determined by comparing preand post-resection diagnoses of 29 patients. The combination of the Paris and Vienna classifications for GEN may optimize the follow-up routines for patients with suspicious precancerous lesions and may significantly improve the detection of early gastric cancer (EGC) while helping gastroenterologists select the best therapy option. Endoscopy, Gastrointestinal Follow-Up Studies Pathology Stomach Neoplasms
2 Hu W. et al.: CLINICAL RESEARCH Background Gastric cancer is a malignancy associated with considerable morbidity and mortality worldwide. The prognosis of advanced gastric cancer is significantly worse compared with early gastric cancer (EGC) [1]; therefore, how to detect and treat EGC is an important issue around the world. Since the inflammation-atrophy-metaplasia-dysplasia-carcinoma sequence was raised as a human model of gastric carcinogenesis [2], dysplasia, which is the last step of the development process for precancerous lesions, has been the major topic of discussion between endoscopists and pathologists. Dysplasia was precisely defined by an international IBDdysplasia morphology study group as lesions showing unequivocal, non-invasive (confined within the basement membrane), neoplastic transformation of the epithelium excluding all reactive changes and was then applied extensively to the whole gastrointestinal tract [3]. Dysplasia mainly depends upon the recognition of morphological features such as cytological and architectural changes in routinely processed hematoxylin and eosin (H&E)-stained sections [4]. Because large discrepancies existed between Western and Japanese pathologists, a series of meetings were held in Padova and Vienna for developing common terminologies for gastrointestinal epithelial neoplasia (GEN) [5 8]. Recently, Korean pathologists have made an effort to achieve an improved diagnostic consensus for GEN [9]. The revised Vienna classification categorizes biopsy-proven dysplasias into 5 groups and gives recommendations for each group [6]. The cut-off for choosing between endoscopic resection or follow-up for low-grade neoplasia (LGN) was not clearly established, while the choice of management for higher or lower grades was generally accepted. In contrast to the pathological perspective of the Vienna classification of GEN, the Paris classification is an endoscopic/macroscopic standard for GEN [10]. In the outstanding clinical research performed by Japanese experts, the medical term type 0 was defined for the endoscopic gross appearance of any tumor resembling early carcinoma, including adenoma/dysplasia and advanced carcinoma [11]. Not all type 0 lesions are malignant; for example, a type 0 IIa lesion can be a juvenile or proliferative polyp, and a type 0 III lesion can be a benign ulcer [10]. The above indicates that diagnosis of a precancerous lesion cannot be accomplished by pathology or endoscopy alone. We presumed that combining the 2 procedures may be a more optimal method during our follow-up study. Material and Methods Patients Our prospective study was conducted in the Second Affiliated Hospital of Zhejiang University School of Medicine. Patients who had undergone gastroscopy and biopsy-proven GEN were included between January 2003 and September Exclusion criteria included patients with a past history of cancer, those who have been using NSAIDs medications, those who have previously undergone surgical or endoscopic treatments, and those with severe concomitant illnesses (e.g., cardiac, respiratory, hepatic, or renal insufficiency). A total of 410 consecutive patients were enrolled in our prospective study. A total of 170 patients with a follow-up of more than 12 months (at least 3 examinations, mean 28 months, range months) were finally documented. There were 101 male patients (mean age 56 years, range years) and 69 female patients (mean age 56 years, range years). Written informed consent was obtained from all of the above patients (see detailed flowchart in Figure 1). Endoscopic assessment The clinical study was carried out with conventional singlechannel endoscopes (Olympus GIF-XQ 240 and GIF-XQ 260; Olympus Optical Co., Ltd, Tokyo, Japan). The macroscopic description of GEN was classified into the following 3 types: type 0 (including type 0 I, IIa, IIb, and type 0 IIc, IIa+IIc), no visible lesions (including patients without specific lesions but with background lesions such as erosion, atrophy, and superficial gastritis), and the ulcer type (including type 0 III; before we knew the pathologic results, we used ulcer instead of type 0 III ). Type 0 lesions were divided into depressed and non-depressed categories. The stomach was divided into 5 sections: cardia, fundus, body, antrum, and pylorus. The cross-sectional circumference was divided into 4 equal sections: greater curvature, lesser curvature, anterior wall, and posterior wall [12]. The detailed information (e.g., size and place) should be added after the macroscopic description. Biopsies were taken from visible lesions ranging 2 5, and biopsies were randomly taken from 2 sites with less curvature in the gastric antrum if there were no visible lesions. Biopsies were taken from the same place during follow-up. Histological assessment and H. pylori testing To minimize intra-procedural variation, all forceps biopsies were evaluated by the same experienced pathologist. All biopsy 993
3 CLINICAL RESEARCH Hu W. et al.: 159 patients lost to follow-up 28 patients did not fit for analysis due to limited duration 410 individuals assessed for eligibility 357 patients received follow-up/treatment according to the follow-up regimen 139 patients followed up without resection 24 patients received resection then follow-up 53 patients excluded 11 patients had history of gastric surgery 23 patients had severe concomitant diseases (cardiac), pulmonary or renal insufficiency) 19 patients had history of cancer 7 patients received resection during follow-up Figure 1. Flow of study participants. 170 patients included for outcome analysis samples were fixed in 10% formalin and embedded in paraffin. Sections were cut into 4-µm thickness for H&E staining. Endoscopic mucosal resection (EMR), endoscopic submucosal dissection (ESD) or polypectomy specimens were washed in normal saline, fixed in 10% formalin, sectioned serially at 2-mm intervals, and entirely embedded in paraffin. Surgical specimens were fixed in 10% formalin, after recording lesion location, number, size and macroscopic type, and each lesion was removed, embedded in paraffin, and sectioned along the longitudinal axis for H&E staining. Lymph nodes around the stomach were processed in the same way, and the number of metastases was recorded. Helicobacter pylori infection was defined as positive if a breath test, an H. pylori culture, or a histological evaluation according to the updated Sydney system [13] was positive. Breath tests for H. pylori were performed 1 month later after withdrawal of PPIs, bismuth, and any antibiotics in case of a false-negative result. The biopsy specimens for H. pylori tests were taken from the lesser curvature of the antrum. Medical treatments Most patients mainly had problems such as abdominal distension, acid regurgitation, and dyspepsia. Proton pump inhibitors (PPIs) and mucosal-protective drugs were prescribed to patients to relieve their symptoms. If the H. pylori test was positive, patients received H. pylori eradication therapy for 2 weeks until a negative result was obtained. Endoscopic and surgical treatments Endoscopic resection included ESD or EMR, with patients under intravenous sedation. With the application of marking dots around the lesion and necessary hemostatic treatment such as endoscopic clipping or thermocoagulation, every lesion was completely removed with negative margins and no complications. EMR was performed with a snare and the Endocut mode (50 W) of an electrosurgical generator (PSD-60; Olympus), after a saline solution containing mg/ml epinephrine was injected into the submucosa beneath the lesion. ESD was performed with an insulated tip knife (Olympus). After a 10% glycerin solution that contained mg/ml epinephrine was injected into the submucosa, a circumferential incision of the mucosa was then made outside the marking dots. The whole tissue, including some submucosa connective tissue, was dissected en bloc from the muscle layer [14]. Patients with HGN, or LGA but suspicious for potential malignancy received surgical gastrectomy due to incomplete endoscopic resection. The endoscopist marked the lesion locations with forceps or methylene blue staining. Follow-up regimen According to the Vienna classification (Revised, 2002) [7], biopsy-proven LGA or dysplasia belongs to category 3 (low-grade GEN), and high-grade adenoma or dysplasia belongs to category 4 (high-grade GEN). Previous reports strongly suggested that high-grade adenoma/dysplasia (HGD, category 4 in the Vienna classification) is highly predictive of invasive carcinoma (category 5), which either coexists or appears thereafter. Therefore, complete endoscopic or surgical resection is strongly recommended for patients with HGD, regardless of the macroscopic type [2,6,7]. We focused on the patients who have biopsy-proved dysplasia during the enrollment process. Patients with Paris classification (which may indicate dysplasia in pathology) were paid special attention. We followed up this group of patients every half year. Patients were enrolled into our group as soon as dysplasia was found. Patients without dysplasia in 2-year follow-up were not traced thereafter. 994
4 Hu W. et al.: CLINICAL RESEARCH Table 1. Modified Vienna classification (our follow-up and management regimen). Category Diagnosis Clinical management 3 Low grade neoplasia Endoscopic resection or follow-up 3.1 Low grade adenoma Endoscopic resection 3.2 Low grade dysplasia No visible lesion group Non-depressed type 0 group Depressed type 0 group Ulcer lesions Follow up (resection if potential for bleeding) every year Closely follow-up Endoscopic resection Rebiopsies, closely follow-up 4 High grade neoplasia Endoscopic resection/surgery 4.1 High grade adenoma/dysplasia 4.2 Non-invasive carcinoma (carcinoma in situ) 4.3 Suspicious for invasive carcinoma 4.4 Intramucosal carcinoma 5 Submucosal invasion by carcinoma Surgical resection Gastric adenoma is a benign tumor of the glandular epithelium with varying degrees of cellular atypia and has papillary and/ or tubular structures [15]. Gastric adenomas tend to develop into invasive adenocarcinoma [13 16]. Tumor size and grading of dysplasia have been indicated as prognostic factors of gastric adenomas [17], and the definite malignant potential of adenomas is indicative for endoscopic resection even if the adenomas are low-grade. While the recommendations for follow-up or endoscopic resection for category 3 (LGA/LGD) listed by the Vienna classification (Revised, 2002) seem very reasonable for managing LGN, endoscopists and gastroenterologists are still confused about how to proceed. No consensus or guideline for the detailed management of biopsy-proven LGN has yet been reached. Based on the present follow-up, we subdivided patients of this group into several categories with different recommendations. For patients who had no visible lesions, follow-up alone was recommended. For type 0 lesions, endoscopic resection was recommended for depressed lesions, and close follow-up was suitable for non-depressed lesions. Ulcer lesions should be carefully examined. Biopsy-proven HGN surrounding an ulcer lesion demonstrate potential malignancy and should be removed immediately. While LGD is not very indicative, it could indicate gastric cancer or inflammatory changes. Therefore, close follow-up should be initiated, and re-biopsy should be performed until healing takes place or higher-level neoplasia is observed. This regimen is summarized in Table 1. Results Based on the biopsy-proven findings, 170 patients were identified with GEN 161 patients with LGN and 9 patients with HGN (Table 2). According to our follow-up and treatment regimen, 24 patients had risk factors for malignancy changes or the potential for bleeding. Twenty-three of these patients received endoscopic resections or surgery. One patient had biopsyproven LGA and type 0 IIa+IIc appearance, but ESD failed to remove the lesion; therefore, the patient chose the followup regimen (Table 3). In total, 146 patients with LGD were documented. Two patients with ulcer lesions had biopsy-proven LGD, but re-biopsy within 1 month suggested HGD, while intramucosal carcinoma and high-grade dysplasia were proven with gastrectomy. Another 9 patients with ulcer lesions healed in the absence of neoplasia. Two patients with type 0 IIa lesions and biopsy-proven LGD became LGA in 1 year and underwent endoscopic resection. Another 2 patients with type 0 IIa lesions disappeared endoscopically and pathologically during the follow-up. Three patients with LGD but no visible lesion progressed endoscopically or pathologically. One patient had a type IIc lesion in 1 year and received ESD, while the other 2 had biopsies of LGA and received EMR or ESD after 2- and 7-year follow-up, respectively. 995
5 CLINICAL RESEARCH Hu W. et al.: Table 2. Demographic data and clinicopathological characteristics from 170 consecutive patients with biopsy-diagnosed gastric epithelial neoplasia (No. of H.pylori positive in the brackets). Low grade neoplasia (n=161) High grade neoplasia (n=9) Total (n=170) Demographics Sex (men/women) 95/66 6/3 101/69 Age, mean ±SD (years) 56.2± ± ±10.8 Endoscopic feature,no.(%) No visible lesion group 132 (36) (36) Type 0 18 (6) 9 (2) 27 (8) Non-depressed type 0 9 (3) 0 12 (3) Depressed type 0 9 (3) 9 (2) 15 (5) Size of lesion, mean ±SD (mm) 1.30± ± ±0.53 Background lesion Atrophic gastritis 16 (5) 7 (1) 23 (6) Non-atrophic gastritis 2 (1) 2 (1) 4 (2) Location of lesion Fundus 0 1 (0) 1 (0) Body 4 (1) 2 (0) 6 (1) Antrum 14 (5) 6 (2) 20 (7) Surface color Normal mucosa 4 (0) 0 4 (0) Erythema 14 (6) 9 (2) 23 (8) Surface nodularity Smooth 9 (3) 9 (2) 18 (5) Nodular 9 (3) 0 9 (3) Ulcer 11 (7) 0 11 (7) Single 7 (5) / 7 (5) Multiple 4 (2) / 4 (2) Background lesion Atrophic gastritis 1 (0) / 1 (0) Non-atrophic gastritis 10 (7) / 10 (7) Location of lesion Fundus 1 (1) / 1 (1) Body 1 (1) / 1 (1) Antrum 9 (5) / 9 (5) Pathological feature, no. (%) Low grade dysplasia 157 (48) / 157 (48) Low grade adenoma 4 (1) / 4 (1) 996
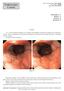
6 Hu W. et al.: CLINICAL RESEARCH Table patients received interventional treatments after initial evaluations. Patients need resection at enrollment Managements Outcomes 9 HGN 7 surgery,1 EMR and 1 ESD 1 advanced gastric carcinoma,6 early cancer, 1 HGD, 1 LGD 3 LGA with non-depressed type 0 appearance 2 EMR, 1 ESD 2 LGA, 1 HGA 1 LGA with depressed type 0 appearance ESD Failed, then chose follow-up 9 LGD with depressed type 0 appearance 1 surgery, 2 EMR and 6 ESD 1 hyperplastic polyp, 2 LGD, 3 HGD, 1 HGA, 2 early cancer 2 LGD with type 0-I lesion potential for bleeding 1 EMR, 1 polypectomy 1 hyperplastic polyp, 1 juvenile polyp with LGD HGN high grade neoplasia; EMR endoscopic mucosa resection; ESD endoscopic submucosal dissection; HGD high grade dysplasia; LGD low grade dysplasia; LGA low grade adenoma; HGA high grade adenoma. Ulcer (11) months 6 months Low grade dysplasia No dysplasia Low grade adenoma/high grade neoplasia/ depressed type 0 lesions Endoscopic/surgical resection 6 months 12 months 24 months 36 months Non-depressed type lesions (3) year 3 year 5 year 7 year 1 No visible lesions (132) Figure 2. Follow-up chart for low-grade neoplasia. The rest of the 128 non-type 0 patients did not progress endoscopically or pathologically. Eighty patients regressed spontaneously from the first follow-up examination; 31 of these patients regressed after a period of fluctuation between normal status and dysplasia and 18 of these patients persisted with LGD. The detailed follow-up processes are described in Figure 2. Figure 3 shows the endoscopic and histological follow-up record of a typical case with a major discrepancy between biopsy and final diagnosis. Efficiency of our follow-up and treatment regimen There were totally 4 patients who had type 0 lesions without dysplasia which were not traced after 2-year follow-up, and 4 997
7 CLINICAL RESEARCH Hu W. et al.: A C E B D F Figure 3. Follow-up process of one patient. (A) A 15-mm in size, superficial, and shallow depressed (type 0 IIa+IIc type in the Paris classification) lesion at the antrum (black arrows). (B) Histological morphology of low-grade dysplasia (white arrow) with the initial biopsy specimen, elongated gastric glands, and hyperplasia of fibrous tissue at the lamina propria (H&E, original magnification 100). (C) The lesion was removed by ESD. (D) Histological features of cancerous foci in the ESD specimen. Crowding glandular cells, with obvious structural and cellular atypia (white arrow) (H&E, original magnification 100). (E) The red ESD scar 1 month later (black arrows). (F) Histological findings suggested regenerative activity of glandular cells. (G) The white ESD scar 9 months later (black arrows). (H) Histological findings suggested elongated glandular cells with inflammatory cell infiltration and an absence of dysplasia. G H patients who had no dysplasia initially and were found to have dysplasia in follow-up were thus finally enrolled into our study. In total, there were 29 patients of gastric mucosal neoplasia who received endoscopic or surgical resections in our followup study, including 24 patients at enrollment (Table 3). The indications for interventional therapy were: HGN, LGA, depressed type 0 lesions with LGD, and other lesions with potential for bleeding. By comparing the biopsy and post-resection diagnoses, the misdiagnosis rate was 62.07% (18/29), and the under-diagnosis rate was 51.72% (15/29), with 38.9% (7/18) in the LGN group and 72.7% (8/11) in the HGN group, respectively (Table 4). Discussion Dysplasia was initially proposed by an international IBDdysplasia morphology study group as lesions showing unequivocal, non-invasive (confined within the basement membrane), neoplastic transformation of the epithelium excluding all reactive changes. However, the presence of dysplasia was confusing. Diagnosis of dysplasia mainly depends on the 998
8 Hu W. et al.: CLINICAL RESEARCH Table 4. Biopsy and post-resection diagnosis of 29 patients who received interventional treatment. No. Genda Age Macroscopic Biopsy-diag Vienna Management Final-diag Vienna 1 F 59 I LGD Category 3.2 EMR Hyperplastic polyp / 2 F 44 I LGD Category 3.2 Polypectomy Juvenile,LGD / 3 F 55 IIa LGA Category 3.1 EMR LGA Category F 55 IIa LGA Category 3.1 EMR LGA Category M 68 IIa LGA Category 3.1 ESD LGA Category M 45 IIa LGA Category 3.1 EMR LGA Category F 60 IIa LGA Category 3.1 EMR LGA Category M 78 IIa LGA Category 3.1 ESD LGA Category M 56 IIa LGA Category 3.1 EMR HGA Category M 49 IIa+IIc LGD Category 3.2 EMR Hyperplastic polyp / 11 M 59 IIa+IIc LGD Category 3.2 ESD LGD Category F 56 IIa+IIc LGD Category 3.2 ESD LGD Category M 34 IIa+IIc LGD Category 3.2 EMR HGA Category M 62 IIa+IIc LGD Category 3.2 ESD HGD Category F 56 IIc LGD Category 3.2 ESD HGD Category M 51 IIa+IIc LGD Category 3.2 SURGERY HGD Category F 64 IIa+IIc LGD Category 3.2 ESD Intramucosal ca Category M 71 IIa+IIc LGD Category 3.2 ESD Intramucosal ca Category M 55 IIa+IIc HGD Category 4.1 EMR LGD Category M 74 IIc HGD Category 4.1 SURGERY HGD Category F 72 IIa+IIc HGD Category 4.1 SURGERY Intramucosal ca Category F 45 IIc HGD Category 4.1 SURGERY Intramucosal ca Category M 54 IIa+IIc HGD Category 4.1 SURGERY Intramucosal ca Category F 70 IIc HGD Category 4.1 SURGERY Intramucosal ca Category M 56 IIc HGD Category 4.1 ESD Intramucosal ca Category M 69 IIa+IIc HGD Category 4.1 SURGERY Submucosal ca Category 5 27 M 56 IIa+IIc HGD Category 4.1 SURGERY Advan.Ca Type 2* 28 M 78 Ulcer HGD Category 4.1 SURGERY HGD Category M 68 Ulcer HGD Category 4.1 SURGERY Intramucosal ca Category 4.4 * Type 2 is ulcerative type of macroscopic classifications of advanced gastric cancer according to Japanese Gastric Cancer Association, means ulcerated tumors with raised margins surrounded by a thickened gastric wall with clear margins. F female; M male; EMR endoscopic mucosa resection; ESD endoscopic submucosal dissection; HGD high grade dysplasia; LGD low grade dysplasia; LGA low grade adenoma; HGA high grade adenoma; ca: carcinoma. 999
9 CLINICAL RESEARCH Hu W. et al.: recognition of morphological features such as cytological and architectural changes in routinely processed hematoxylin and eosin-stained sections, and our pathologists could not clearly differentiate these changes. Consequently, most endoscopists or gastroenterologists will be confused about dysplasia, and a definite diagnosis of a neoplastic lesion cannot be determined; thus, resection cannot be confidently recommended. Based on the consensus reached at the international pathological conferences held in Padova and Vienna, biopsy-proven HGN became a definite indication for resection, while LGD/LGN was still confusing. Previous studies showed that most cases of LGN disappeared due to over-diagnosing regenerative (i.e., inflammatory) lesions as neoplastic lesions [18]. In fact, we determined that most dysplasia specimens in pathological reports were randomly biopsied, and no visible lesions were observed in the endoscopic examination. There were 132/170 (77.6%) patients with LGN but no visible lesions; of the 132 cases, 111 (84.1%) regressed and 18 (13.6%) persisted, which agreed with previous studies. Depending on the recognition of outcomes in this group of neoplasia, we can presume that patients with neoplasia and no visible lesions may display reactive or regenerative inflammatory changes and can be reversed with or without medications. The Paris classification of superficial neoplastic lesions assisted us greatly in recognizing real neoplastic dysplasia. Since the macroscopic classification of early gastric carcinomas was established by Japanese experts, the prefix type 0 (e.g., 0 I, 0 IIa) has been widely used to distinguish early and superficial carcinomas from advanced carcinomas and is becoming the general practice in detecting endoscopic gross appearances of any tumor resembling early carcinoma, including adenoma/dysplasia and advanced carcinoma [11]. To extend the useful methodology of detecting precursor lesions endoscopically, Japanese experts convinced other participants to reach a consensus regarding the Paris endoscopic classification of superficial neoplastic lesions in Superficial neoplasia includes neoplastic lesions with no invasion in the lamina propria and carcinoma with invasion of the lamina propria and a depth of penetration limited to the mucosa (stomach and esophagus) or the submucosa (large bowel). Almost every superficial neoplasia has a superficial morphology, but not every lesion of superficial morphology suggests neoplasias (e.g., hyperplastic polyps in the GI tract have little or no potential for transformation into neoplastic lesions but always have a protruding morphology). It is reasonable that polypoid precursors play a minor role in the development of advanced gastric cancer, while depressed non-polypoid lesions (type 0 IIc) are the usual precursors [10]. Cho et al. [19] analyzed 236 LGD lesions treated with endoscopic resection and showed that depressed morphology, surface erythema, or a size of 1 cm or greater were risk factors for HGD/carcinoma; thus, endoscopic resection is recommended even with biopsy-proven LGD. Based on the above, we showed that the Paris classification is an efficient and accurate way to screen neoplastic and nonneoplastic lesions, and depressed appearance can be a specific indication for endoscopic or surgical resection. In our study, 4 patients who had type 0 lesions without dysplasia were not traced after 2-year follow-up, and 4 patients who had no dysplasia initially and found to have dysplasia thus were finally enrolled into our study. Eighteen patients with type 0 lesions and LGN were divided into 2 groups: 9 patients with non-depressed lesions and 9 with depressed lesions; clinical management revealed that 6/9 of the latter group were progressing to cancer (Table 3). Gastric adenomas are benign epithelial neoplastic tumors with a glandular organization that are characterized by localized proliferation of adenomatous epithelium with tubular and/or papillary structures [15]. Kamiya et al. reviewed 74 patients in the 1980s and observed gastric adenomas that underwent malignant changes with gradual transformation from moderate to severe dysplasia [16]. Kasuga et al. recently retrospectively reviewed 231 gastric adenomas by comparing forceps biopsy and post-resection diagnoses and recommended en bloc resection even when forceps biopsy indicated LGA [14]. In our study, we subdivided LGN into LGA and LGD groups to treat them. Seven patients with biopsy-proven LGA were resected quickly (except for 1 who failed in ESD), including 1 patient with high-grade adenoma and 6 with LGAs. Gastric ulcers have been frequently noted for their probability of malignancy. There are 2 hypotheses regarding malignant ulcers: first, long-time chronic ulcers lead to malignant changes, and second, the carcinoma itself presented with ulcer appearance [20]. There is no doubt that biopsy-proven HGN should be treated immediately, while in the case of biopsy-proven LGN, we can re-biopsy the lesion if suspicious for carcinoma or perform close follow-up within 1 month. In our study, 2 patients with LGN progressed to HGN within 1 month, which means that misdiagnosis took place the first time but the proper diagnosis was later discovered through close follow-up. There were 4 patients who developed multiple ulcers with LGN after the initial examinations, which may not indicate gastric cancer; however, close follow-up was required to exclude gastric lymphoma. From our follow-up chart of 146 patients, except for 129 nonvisible-lesion patients fluctuating between LGD and normal, 3 patients progressed to LGA or HGN ranging from 1 to 7 years, and 1 patient with non-depressed lesions progressed to LGA but finally had the lesions resected. Although the regression ratio was very high in the LGN group, a few did progress to HGN even after 6 years, which would be a possible sign of gastric cancer. We recommend using a follow-up strategy (we recommend at least once a year) for all cases of this group. 1000
10 Hu W. et al.: CLINICAL RESEARCH For patients who have visible lesions (e.g., non-depressed type 0 lesions) with LGN, we recommend that the first follow-up should be initiated in 3 6 months to reduce the possibility of misdiagnosing gastric adenomas. Special attention should be paid to ulcer lesions with LGN, as we mentioned above. The follow-up interval should be strictly controlled for 1 month until definite endoscopic mucosal healing occurs. In total, 29 patients received en bloc resection. All patients had 1 of the following indications: biopsy-proven HGN, biopsy-proven LGA, biopsy-proven LGD with depressed type 0 appearance, or potential for bleeding. By comparing the forceps biopsy and post-resection diagnoses, we determined that the misdiagnosis rate was 62.07% (18/29), and the under-diagnosis rate was 51.72% (15/29), with 38.9% (7/18) in the LGN group and 72.7% (8/11) in the HGN group. Endoscopic forceps biopsy (EFB) may cause errors in histological diagnosis and thus cause significant discrepancy between EFB and en bloc resection or surgical diagnosis [21]. Forceps biopsy errors are the leading cause of the high misdiagnosis rate, excluding variance among endoscopists and pathologists. In follow-up using the Paris classification and endoscopic techniques (EMR or ESD), with increasing attention to the probability of biopsy misdiagnosis, the problems seem to be solved to a certain extend; however, overtreatment can occur. The limitations of the present study include the following points. First, we enrolled 410 patients in the initial examination; however, due to poor patient compliance, only 170 patients could complete our follow-up. Second, medications for H. pylori eradication were prescribed in our follow-up group, and the efficiency of medications for reversing low-grade gastric neoplasia have not been well evaluated; thus, we could not exclude the possibility that medications influenced the regression of gastric neoplasia. We plan to continue our study by obtaining results from patients on a larger scale. Conclusions Diagnosis of GEN by endoscopy or pathology alone was shown be insufficiently accurate. Additionally, the combination of the Vienna and Paris classifications could be helpful for follow-up and timely treatment of suspicious precancerous lesions and for reducing the misdiagnosis rate of EGC, especially in countries where, unlike Japan, the early detection and treatment rates for gastric cancer are low and advanced equipment (such as narrow-band imaging, NBI, or magnifying endoscopy) or detection experience are lacking. Statement All the authors declare that they have no conflict of interest. Reference: 1. Wang ZQ, Cai Q, Jiang ZY et al: Prognostic role of MicroRNA-21 in gastric cancer: A meta-analysis. Med Sci Monit, 2015; 21: Correa P: A human model of gastric carcinogenesis. Cancer Res, 1988; 48: Riddell RH, Goldman H, Ransohoff DF et al: Dysplasia in inflammatory bowel disease: standardized classification with provisional clinical applications. Hum Pathol, 1983; 14: Geboes K, Sagaert X, Geboes KP: Dysplasia Intraepithelial Neoplasia and Neoplasia without Dysplasia in the Digestive Tract. European Gastroenterology & Hepatology Review, 2011; 7(1): Rugge M, Correa P, Dixon MF et al: Gastric dysplasia: the Padova international classification. Am J Surg Pathol, 2000; 24: Schlemper RJ, Riddell RH, Kato Y et al. The Vienna classification of gastrointestinal epithelial neoplasia. Gut, 2000; 47: Dixon MF: Gastrointestinal epithelial neoplasia: Vienna revisited. Gut, 2002; 51: Schlemper RJ, Kato Y, Stolte M: Review of histological classifications of gastrointestinal epithelial neoplasia: differences in diagnosis of early carcinomas between Japanese and Western pathologists. J Gastroenterol, 2001; 36: Kim JM, Cho MY, Sohn JH et al: Diagnosis of gastric epithelial neoplasia: Dilemma for Korean pathologists. World J of Gastroenterol, 2011; 17: Inoue H, Kashida H, Kudo S et al: The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach, and colon: November 30 to December 1, Gastrointest Endosc, 2003; 58: S Schlemper RJ, Hirata I, Dixon MF: The macroscopic classification of early neoplasia of the digestive tract. Endoscopy, 2002; 34: Dixon MF, Genta RM, Yardley JH, Correa P: Classification and grading of gastritis: the updated Sydney system. Am J Surg Pathol, 1996; 20: Association JGC: Japanese classification of gastric carcinoma: 3 rd English edition. Gastric Cancer, 2011; 14: Kasuga A, Yamamoto Y, Fujisaki J et al: Clinical characterization of gastric lesions initially diagnosed as low-grade adenomas on forceps biopsy. Dig Endosc, 2012; 24: Nakamura K, Sakaguchi H, Enjoji M: Depressed adenoma of the stomach. Cancer, 1988; 62: Kamiya T, Morishita T, Asakura H et al: Long-term follow-up study on gastric adenoma and its relation to gastric protruded carcinoma. Cancer, 1982; 50: Rocco A, Caruso R, Toracchio S et al: Gastric adenomas: relationship between clinicopathological findings, Helicobacter pylori infection, APC mutations and COX-2 expression. Ann Oncol, 2006; 17: vii Rugge M, Cassaro M, Di Mario F et al: The long term outcome of gastric non-invasive neoplasia. Gut, 2003; 52: Cho SJ, Choi I, Kim C et al: Risk of high-grade dysplasia or carcinoma in gastric biopsy-proven low-grade dysplasia: an analysis using the Vienna classification. Endoscopy, 2011; 43: Morson BC, Sobin LH, Grundmann E et al: Precancerous conditions and epithelial dysplasia in the stomach. J Clin Pathol, 1980; 33: Lee CK, Chung I-K, Lee S-H et al: Is endoscopic forceps biopsy enough for a definitive diagnosis of gastric epithelial neoplasia? J Gastroenterol Hepatol, 2010; 25:
Paris classification (2003) 삼성의료원내과이준행
 Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
Paris classification (2003) 삼성의료원내과이준행 JGCA classification - Japanese Gastric Cancer Association - Type 0 superficial polypoid, flat/depressed, or excavated tumors Type 1 polypoid carcinomas, usually attached
Prognostic analysis of gastric mucosal dysplasia after endoscopic resection: A single-center retrospective study
 JBUON 2019; 24(2): 679-685 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic analysis of gastric mucosal dysplasia after endoscopic resection:
JBUON 2019; 24(2): 679-685 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic analysis of gastric mucosal dysplasia after endoscopic resection:
Helicobacter pylori Improved Detection of Helicobacter pylori
 DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
DOI:http://dx.doi.org/10.7314/APJCP.2016.17.4.2099 RESEARCH ARTICLE Improved Detection of Helicobacter pylori Infection and Premalignant Gastric Mucosa Using Conventional White Light Source Gastroscopy
Gastric atrophy: use of OLGA staging system in practice
 Gastroenterology and Hepatology From Bed to Bench. 2016 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Gastric atrophy: use of OLGA staging system in practice Mahsa
Gastroenterology and Hepatology From Bed to Bench. 2016 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Gastric atrophy: use of OLGA staging system in practice Mahsa
Delayed Perforation Occurring after Endoscopic Submucosal Dissection for Early Gastric Cancer
 CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
Gastric Polyps. Bible class
 Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
How to treat early gastric cancer? Endoscopy
 How to treat early gastric cancer? Endoscopy Presented by Pierre H. Deprez Institution Cliniques universitaires Saint-Luc, Brussels Université catholique de Louvain 2 3 4 5 6 Background Diagnostic or therapeutic
How to treat early gastric cancer? Endoscopy Presented by Pierre H. Deprez Institution Cliniques universitaires Saint-Luc, Brussels Université catholique de Louvain 2 3 4 5 6 Background Diagnostic or therapeutic
Diagnosis and management of gastric dysplasia
 REVIEW Korean J Intern Med 2016;31:201-209 Diagnosis and management of gastric dysplasia Jae Kyu Sung Department of Internal Medicine, Chungnam National University School of Medicine, Daejeon, Korea Received
REVIEW Korean J Intern Med 2016;31:201-209 Diagnosis and management of gastric dysplasia Jae Kyu Sung Department of Internal Medicine, Chungnam National University School of Medicine, Daejeon, Korea Received
The white globe appearance (WGA): a novel marker for a correct diagnosis of early gastric cancer by magnifying. endoscopy with narrow-band imaging (M-
 E120 The white globe appearance (WGA): a novel marker for a correct diagnosis of early gastric cancer by magnifying endoscopy with narrow-band imaging (M-NBI) Authors Hisashi Doyama 1, Naohiro Yoshida
E120 The white globe appearance (WGA): a novel marker for a correct diagnosis of early gastric cancer by magnifying endoscopy with narrow-band imaging (M-NBI) Authors Hisashi Doyama 1, Naohiro Yoshida
Endoscopic Submucosal Dissection of an Inverted Early Gastric Cancer-Forming False Gastric Diverticulum
 CSE REPORT Clin Endosc 2016;49:86-90 http://dx.doi.org/10.5946/ce.2016.49.1.86 Print ISSN 2234-2400 / On-line ISSN 2234-2443 Open ccess Endoscopic Submucosal Dissection of an Inverted Early Gastric Cancer-Forming
CSE REPORT Clin Endosc 2016;49:86-90 http://dx.doi.org/10.5946/ce.2016.49.1.86 Print ISSN 2234-2400 / On-line ISSN 2234-2443 Open ccess Endoscopic Submucosal Dissection of an Inverted Early Gastric Cancer-Forming
Gastric Extremely Well-Diferentiated Intestinal-Type Adenocarcinoma: A Challenging Lesion to Achieve Complete Endoscopic Resection
 Gastric Extremely Well-Diferentiated Intestinal-Type Adenocarcinoma: A Challenging Lesion to Achieve Complete Endoscopic Resection The Harvard community has made this article openly available. Please share
Gastric Extremely Well-Diferentiated Intestinal-Type Adenocarcinoma: A Challenging Lesion to Achieve Complete Endoscopic Resection The Harvard community has made this article openly available. Please share
EMR, ESD and Beyond. Peter Draganov MD. Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida
 EMR, ESD and Beyond Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated by Endoscopy
EMR, ESD and Beyond Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated by Endoscopy
University Mainz. Early Gastric Cancer. Ralf Kiesslich. Johannes Gutenberg University Mainz, Germany. Early Gastric Cancer 15.6.
 Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
 Gut and Liver, Vol. 3, No. 4, December 2009, pp. 271-275 original article The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
Gut and Liver, Vol. 3, No. 4, December 2009, pp. 271-275 original article The Clinicopathological Features of Gastric Hyperplastic Polyps with Neoplastic Transformations: A Suggestion of Indication for
ESMO Preceptorship Gastrointestinal Tumours Valencia October 2017
 www.esmo.org ESMO Preceptorship Valencia 06-07 October 2017 Gastrointestinal Tumours I have no conflicts of interest to declare Fátima Carneiro Gastrointestinal tumours Multidisciplinary management, standards
www.esmo.org ESMO Preceptorship Valencia 06-07 October 2017 Gastrointestinal Tumours I have no conflicts of interest to declare Fátima Carneiro Gastrointestinal tumours Multidisciplinary management, standards
Current status of gastric ESD in Korea. Jun Haeng Lee. Department of Medicine Sungkyunkwanuniversity School of Medicie, Seoul, Korea
 Current status of gastric ESD in Korea Jun Haeng Lee. Department of Medicine Sungkyunkwanuniversity School of Medicie, Seoul, Korea Contents Brief history of gastric ESD in Korea ESD/EMR for gastric adenoma
Current status of gastric ESD in Korea Jun Haeng Lee. Department of Medicine Sungkyunkwanuniversity School of Medicie, Seoul, Korea Contents Brief history of gastric ESD in Korea ESD/EMR for gastric adenoma
Endoscopic Submucosal Dissection ESD
 Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract
 Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
Magnifying Endoscopy and Chromoendoscopy of the Upper Gastrointestinal Tract Alina M.Boeriu 1, Daniela E.Dobru 1, Simona Mocan 2 1) Department of Gastroenterology, University of Medicine and Pharmacy;
How to characterize dysplastic lesions in IBD?
 How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
The Paris classification of colonic lesions
 The Paris classification of colonic lesions Training to improve the interobserver agreement among international experts Sascha van Doorn, MD, PhD-student in CRC-reserach group of Evelien Dekker Introduction
The Paris classification of colonic lesions Training to improve the interobserver agreement among international experts Sascha van Doorn, MD, PhD-student in CRC-reserach group of Evelien Dekker Introduction
Clinicopathological Characteristics of Superficial Type
 Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 99-105 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 99-105 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
위암내시경진단 (2019) - 융기형위암을중심으로 성균관대학교의과대학내과이준행
 위암내시경진단 (2019) - 융기형위암을중심으로 성균관대학교의과대학내과이준행 위암내시경진단 (2019) 위암검진에대한짧지않은 comment 융기형암은융기되어있는가? 함몰형암은함몰되어있는가? Semi-pedunculated polyp Sentinel polyp or EGJ cancer? IIa + IIc 위암검진에대한짧지않은 comment 성균관대학교의과대학내과이준행
위암내시경진단 (2019) - 융기형위암을중심으로 성균관대학교의과대학내과이준행 위암내시경진단 (2019) 위암검진에대한짧지않은 comment 융기형암은융기되어있는가? 함몰형암은함몰되어있는가? Semi-pedunculated polyp Sentinel polyp or EGJ cancer? IIa + IIc 위암검진에대한짧지않은 comment 성균관대학교의과대학내과이준행
Departmental and institutional affiliation: Departments of Medicine, Samsung Medical
 Endoscopic Submucosal Dissection for Early Gastric Neoplasia Occurring in the Remnant Stomach after Distal Gastrectomy Short running title: ESD for tumors in the remnant stomach Authors: Ji Young Lee,
Endoscopic Submucosal Dissection for Early Gastric Neoplasia Occurring in the Remnant Stomach after Distal Gastrectomy Short running title: ESD for tumors in the remnant stomach Authors: Ji Young Lee,
Association of Helicobacter pylori infection with Atrophic gastritis in patients with Dyspepsia
 ADVANCES IN BIORESEARCH Adv. Biores., Vol 8 [3] May 2017: 137-141 2017 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
ADVANCES IN BIORESEARCH Adv. Biores., Vol 8 [3] May 2017: 137-141 2017 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
Large Colorectal Adenomas An Approach to Pathologic Evaluation
 Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
CASE REPORT. Introduction. Case Report. Kimitoshi Kubo 1, Noriko Kimura 2, Katsuhiro Mabe 1, Yusuke Nishimura 1 and Mototsugu Kato 1
 doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
IN THE DEVELOPMENT and progression of colorectal
 Digestive Endoscopy 2014; 26 (Suppl. 2): 73 77 doi: 10.1111/den.12276 Treatment strategy of diminutive colorectal polyp
Digestive Endoscopy 2014; 26 (Suppl. 2): 73 77 doi: 10.1111/den.12276 Treatment strategy of diminutive colorectal polyp
Advanced techniques for resection of large polyps. John G. Lee, MD February 2, 2018
 Advanced techniques for resection of large polyps John G. Lee, MD February 2, 2018 Background 1cm - large polyp on screening 2cm - large for polypectomy 3cm giant polyp 10-15% of polyps can t be removed
Advanced techniques for resection of large polyps John G. Lee, MD February 2, 2018 Background 1cm - large polyp on screening 2cm - large for polypectomy 3cm giant polyp 10-15% of polyps can t be removed
Citation Acta Medica Nagasakiensia. 1992, 37
 NAOSITE: Nagasaki University's Ac Title Author(s) Clinicopathological Study on Gastri Murata, Ikuo; Oda, Hidetoshi; Muta, Nakamuta, Kohji; Tsuruta, Hideo; Oh Makiyama, Kazuya; Hara, Kohei Citation Acta
NAOSITE: Nagasaki University's Ac Title Author(s) Clinicopathological Study on Gastri Murata, Ikuo; Oda, Hidetoshi; Muta, Nakamuta, Kohji; Tsuruta, Hideo; Oh Makiyama, Kazuya; Hara, Kohei Citation Acta
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
malignant polyp Daily Challenges in Digestive Endoscopy for Endoscopists and Endoscopy Nurses BSGIE Annual Meeting 18/09/2014 Mechelen
 Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions
 Showa Univ J Med Sci 29 3, 297 306, September 2017 Original Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions Shotaro HANAMURA, Kuniyo GOMI,
Showa Univ J Med Sci 29 3, 297 306, September 2017 Original Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions Shotaro HANAMURA, Kuniyo GOMI,
Surveying the Colon; Polyps and Advances in Polypectomy
 Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Principles of diagnosis, work-up and therapy The Gastroenterologist s role
 Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens
 ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
위 ESD 후내시경소견 성균관대학교의과대학내과이준행
 위 ESD 후내시경소견 성균관대학교의과대학내과이준행 문제의식 위궤양, 조기위암, 진행위암의내시경소견은배운다. 위암수술후소견은가끔배운다. 위암내시경시술후소견은배운적이없다. 관찰과조직검사에대한가이드라인이없다. ESD 후정상내시경소견 성균관대학교의과대학내과이준행 처음의뢰되었을때의사진 ESD M/D, 18mm, LP, RM (-), L/V (-) 추적내시경소견 2
위 ESD 후내시경소견 성균관대학교의과대학내과이준행 문제의식 위궤양, 조기위암, 진행위암의내시경소견은배운다. 위암수술후소견은가끔배운다. 위암내시경시술후소견은배운적이없다. 관찰과조직검사에대한가이드라인이없다. ESD 후정상내시경소견 성균관대학교의과대학내과이준행 처음의뢰되었을때의사진 ESD M/D, 18mm, LP, RM (-), L/V (-) 추적내시경소견 2
Correlation between Gastric Mucosal Morphologic Patterns and Histopathological Severity of
 Hindawi Publishing Corporation BioMed Research International Volume 2015, Article ID 808505, 7 pages http://dx.doi.org/10.1155/2015/808505 Research Article Correlation between Gastric Mucosal Morphologic
Hindawi Publishing Corporation BioMed Research International Volume 2015, Article ID 808505, 7 pages http://dx.doi.org/10.1155/2015/808505 Research Article Correlation between Gastric Mucosal Morphologic
Second-Look Endoscopy after Gastric Endoscopic Submucosal Dissection for Reducing Delayed Postoperative Bleeding
 Gut and Liver, Vol. 9, No. 1, January 2015, pp. 43-51 ORiginal Article Second-Look Endoscopy after Gastric Endoscopic Submucosal Dissection for Reducing Delayed Postoperative Bleeding Chan Hyuk Park, Jun
Gut and Liver, Vol. 9, No. 1, January 2015, pp. 43-51 ORiginal Article Second-Look Endoscopy after Gastric Endoscopic Submucosal Dissection for Reducing Delayed Postoperative Bleeding Chan Hyuk Park, Jun
Endoscopic Corner CASE 1. Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R
 170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
170 Endoscopic Corner Kimtrakool S Aniwan S Linlawan S Muangpaisarn P Sallapant S Rerknimitr R CASE 1 A 54-year-old woman underwent a colorectal cancer screening. Her fecal immunochemical test was positive.
Factors for Endoscopic Submucosal Dissection in Early Colorectal Neoplasms: A Single Center Clinical Experience in China
 ORIGINAL ARTICLE Clin Endosc 2015;48:405-410 http://dx.doi.org/10.5946/ce.2015.48.5.405 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Factors for Endoscopic Submucosal Dissection in Early Colorectal
ORIGINAL ARTICLE Clin Endosc 2015;48:405-410 http://dx.doi.org/10.5946/ce.2015.48.5.405 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Factors for Endoscopic Submucosal Dissection in Early Colorectal
Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong
 Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Endoscopic Corner CASE 1. Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R
 Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
Diagnostic accuracy of pit pattern and vascular pattern in colorectal lesions
 Diagnostic accuracy of pit pattern and vascular pattern in colorectal lesions Digestive Disease Center, Showa University Northern Yokohama Hospital Department of Pathology Yoshiki Wada, Shin-ei Kudo, Hiroshi
Diagnostic accuracy of pit pattern and vascular pattern in colorectal lesions Digestive Disease Center, Showa University Northern Yokohama Hospital Department of Pathology Yoshiki Wada, Shin-ei Kudo, Hiroshi
LARYNGEAL DYSPLASIA. Tomas Fernandez M; 3 rd year ENT resident, Son Espases University Hospital
 LARYNGEAL DYSPLASIA Tomas Fernandez M; 3 rd year ENT resident, Son Espases University Hospital INTRODUCTION Laryngeal cancer constitutes 1-2% of all malignancies diagnosed worldwide Survival is related
LARYNGEAL DYSPLASIA Tomas Fernandez M; 3 rd year ENT resident, Son Espases University Hospital INTRODUCTION Laryngeal cancer constitutes 1-2% of all malignancies diagnosed worldwide Survival is related
ESD for EGC with undifferentiated histology
 ESD for EGC with undifferentiated histology Jun Haeng Lee, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Biopsy: M/D adenocarcinoma ESD: SRC >>
ESD for EGC with undifferentiated histology Jun Haeng Lee, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Biopsy: M/D adenocarcinoma ESD: SRC >>
Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens
 The Korean Journal of Pathology 2006; 40: 32-8 Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens In Gu Do Youn Wha Kim Yong-Koo Park Department
The Korean Journal of Pathology 2006; 40: 32-8 Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens In Gu Do Youn Wha Kim Yong-Koo Park Department
Risk factors for lymph node metastasis in histologically poorly differentiated type early gastric cancer
 498 Original article Risk factors for lymph node metastasis in histologically poorly differentiated type early gastric cancer Authors C. Kunisaki 1, M. Takahashi 2, Y. Nagahori 3, T. Fukushima 3, H. Makino
498 Original article Risk factors for lymph node metastasis in histologically poorly differentiated type early gastric cancer Authors C. Kunisaki 1, M. Takahashi 2, Y. Nagahori 3, T. Fukushima 3, H. Makino
Management of pt1 polyps. Maria Pellise
 Management of pt1 polyps Maria Pellise Early colorectal cancer Malignant polyp Screening programmes SM Invasive adenocar cinoma Advances in diagnostic & therapeutic endoscopy pt1 polyps 0.75 5.6% of large-bowel
Management of pt1 polyps Maria Pellise Early colorectal cancer Malignant polyp Screening programmes SM Invasive adenocar cinoma Advances in diagnostic & therapeutic endoscopy pt1 polyps 0.75 5.6% of large-bowel
Endoscopic features suggesting gastric cancer in biopsy-proven gastric adenoma with high-grade neoplasia
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i34.12233 World J Gastroenterol 2014 September 14; 20(34): 12233-12240 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i34.12233 World J Gastroenterol 2014 September 14; 20(34): 12233-12240 ISSN 1007-9327
Endoscopic atrophic classification before and after H. pylori eradication is closely associated with histological atrophy and intestinal metaplasia
 E311 before and after H. pylori eradication is closely associated with histological atrophy and intestinal metaplasia Authors Institution Masaaki Kodama, Tadayoshi Okimoto, Ryo Ogawa, Kazuhiro Mizukami,
E311 before and after H. pylori eradication is closely associated with histological atrophy and intestinal metaplasia Authors Institution Masaaki Kodama, Tadayoshi Okimoto, Ryo Ogawa, Kazuhiro Mizukami,
Local recurrence after endoscopic resection of colorectal tumors
 Int J Colorectal Dis (2009) 24:225 230 DOI 10.1007/s00384-008-0596-8 ORIGINAL ARTICLE Local recurrence after endoscopic resection of colorectal tumors Kinichi Hotta & Takahiro Fujii & Yutaka Saito & Takahisa
Int J Colorectal Dis (2009) 24:225 230 DOI 10.1007/s00384-008-0596-8 ORIGINAL ARTICLE Local recurrence after endoscopic resection of colorectal tumors Kinichi Hotta & Takahiro Fujii & Yutaka Saito & Takahisa
Gastric Cancer Histopathology Reporting Proforma
 Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
Gastrointestinal Tract Cancer
 Gastrointestinal Tract Cancer Tumors of the Stomach Gastric adenocarcinoma Incidence and Epidemiology Incidence mortality rates USA High incidence: Japan, China, Chile, Ireland risk lower socioeconomic
Gastrointestinal Tract Cancer Tumors of the Stomach Gastric adenocarcinoma Incidence and Epidemiology Incidence mortality rates USA High incidence: Japan, China, Chile, Ireland risk lower socioeconomic
Introduction. Original articles. Nicolás Rocha, 1 Sandra Huertas, 2 Rosario Albis, 3 Diego Aponte, 4 Luis Carlos Sabbagh. 5
 Original articles Correlation of endoscopic and histological findings in diagnosis of gastrointestinal metaplasia in patients referred to the Clinica Colombia for upper endoscopies Nicolás Rocha, 1 Sandra
Original articles Correlation of endoscopic and histological findings in diagnosis of gastrointestinal metaplasia in patients referred to the Clinica Colombia for upper endoscopies Nicolás Rocha, 1 Sandra
Colonic Polyp. Najmeh Aletaha. MD
 Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Learning Objectives:
 Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Narrow Band Imaging for the Detection of Gastric Intestinal Metaplasia and Dysplasia During Surveillance Endoscopy
 Dig Dis Sci (2010) 55:3442 3448 DOI 10.1007/s10620-010-1189-2 ORIGINAL ARTICLE Narrow Band Imaging for the Detection of Gastric Intestinal Metaplasia and Dysplasia During Surveillance Endoscopy Lisette
Dig Dis Sci (2010) 55:3442 3448 DOI 10.1007/s10620-010-1189-2 ORIGINAL ARTICLE Narrow Band Imaging for the Detection of Gastric Intestinal Metaplasia and Dysplasia During Surveillance Endoscopy Lisette
Oesophagus and Stomach update dysplasia and early cancer
 Oesophagus and Stomach update dysplasia and early cancer Dr Tim Bracey STR teaching 13/4/16 Please check pathkids.com for previous talks One of the biggest units in the country (100 major resections per
Oesophagus and Stomach update dysplasia and early cancer Dr Tim Bracey STR teaching 13/4/16 Please check pathkids.com for previous talks One of the biggest units in the country (100 major resections per
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy
 Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
The surface mucous cells and the cardiac and pyloric glands secrete mucus which protects the stomach from self-digestion.
 PATHOLOGY OF THE STOMACH Stomach mucosa Gastric mucosa is covered by a layer of mucus. The mucosal glands comprise the cardiac glands, the fundic glands in the fundus and body of the stomach, and the pyloric
PATHOLOGY OF THE STOMACH Stomach mucosa Gastric mucosa is covered by a layer of mucus. The mucosal glands comprise the cardiac glands, the fundic glands in the fundus and body of the stomach, and the pyloric
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ
 Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endoscopic submucosal dissection of gastric lesions This procedure can be
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endoscopic submucosal dissection of gastric lesions This procedure can be
Expert panel observations
 Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
Chromoendoscopy or Narrow Band Imaging with Targeted biopsies Should be the Cancer Surveillance Endoscopy Procedure of Choice in Ulcerative Colitis
 Chromoendoscopy or Narrow Band Imaging with Targeted biopsies Should be the Cancer Surveillance Endoscopy Procedure of Choice in Ulcerative Colitis Bret A. Lashner, M.D. Professor of Medicine Director,
Chromoendoscopy or Narrow Band Imaging with Targeted biopsies Should be the Cancer Surveillance Endoscopy Procedure of Choice in Ulcerative Colitis Bret A. Lashner, M.D. Professor of Medicine Director,
Patient. Male 76 year old C.C: abdominal pain
 Patient Male 76 year old C.C: abdominal pain Bowel stool retention Suspected pulmonary TB at right upper lung Infiltration in right lower lung Pleural thickening at the Right chest Localized dilated small
Patient Male 76 year old C.C: abdominal pain Bowel stool retention Suspected pulmonary TB at right upper lung Infiltration in right lower lung Pleural thickening at the Right chest Localized dilated small
Analysis of microvascular density in early gastric carcinoma using magnifying endoscopy with narrow-band imaging
 E832 THIEME Analysis of microvascular density in early gastric using magnifying endoscopy with narrow-band imaging Authors Masashi Kawamura 1, Hiroshi Naganuma 2, Rie Shibuya 2, Tatsuya Kikuchi 1, Yoshitaka
E832 THIEME Analysis of microvascular density in early gastric using magnifying endoscopy with narrow-band imaging Authors Masashi Kawamura 1, Hiroshi Naganuma 2, Rie Shibuya 2, Tatsuya Kikuchi 1, Yoshitaka
Barrett s esophagus. Barrett s neoplasia treatment trends
 Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Introduction. Keywords Gastric cancer Endoscopic resection Helicobacter pylori Endoscopic gastrointestinal surgery
 Gastric Cancer (2018) 21:988 997 https://doi.org/10.1007/s10120-018-0819-9 ORIGINAL ARTICLE Diagnostic accuracy of demarcation using magnifying endoscopy with narrow band imaging for Helicobacter pylori
Gastric Cancer (2018) 21:988 997 https://doi.org/10.1007/s10120-018-0819-9 ORIGINAL ARTICLE Diagnostic accuracy of demarcation using magnifying endoscopy with narrow band imaging for Helicobacter pylori
Dysplasia 4/19/2017. How do I practice Chromoendoscopy for Surveillance of Colitis? SCENIC: Polypoid Dysplasia in UC. Background
 SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
Histopathogenesis of intestinal metaplasia: minute
 J Clin Pathol 1987;40:13-18 Histopathogenesis of intestinal metaplasia: minute lesions of intestinal metaplasia in ulcerated stomachs K MUKAWA, T NAKAMURA, G NAKANO, Y NAGAMACHI From the First Department
J Clin Pathol 1987;40:13-18 Histopathogenesis of intestinal metaplasia: minute lesions of intestinal metaplasia in ulcerated stomachs K MUKAWA, T NAKAMURA, G NAKANO, Y NAGAMACHI From the First Department
Gastroenterology Tutorial
 Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Long-Term Effects of Helicobacter pylori Eradication on Metachronous Gastric Cancer Development
 Gut and Liver, Vol. 12, No. 2, March 218, pp. 133-141 ORiginal Article Long-Term ffects of Helicobacter pylori radication on Metachronous Gastric Cancer Development Seung Jun Han 1, Sang Gyun Kim 1, Joo
Gut and Liver, Vol. 12, No. 2, March 218, pp. 133-141 ORiginal Article Long-Term ffects of Helicobacter pylori radication on Metachronous Gastric Cancer Development Seung Jun Han 1, Sang Gyun Kim 1, Joo
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions
 Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Earlyoesophagealcancer. dr. Nina Zidar Institute of Pathology Faculty ofmedicine University of Ljubljana Slovenia
 Earlyoesophagealcancer dr. Nina Zidar Institute of Pathology Faculty ofmedicine University of Ljubljana Slovenia Early carcinoma of oesophagus = tumor limited to mucosa or submucosa, not extending into
Earlyoesophagealcancer dr. Nina Zidar Institute of Pathology Faculty ofmedicine University of Ljubljana Slovenia Early carcinoma of oesophagus = tumor limited to mucosa or submucosa, not extending into
Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:506-511 Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program Su Youn Nam 1,2, Bum Joon Park 2,
ORIGINAL ARTICLE Korean J Intern Med 2018;33:506-511 Effect of Helicobacter pylori eradication on the regression of gastric polyps in National Cancer Screening Program Su Youn Nam 1,2, Bum Joon Park 2,
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Histopathology: gastritis and peptic ulceration
 Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Natural history of early gastric cancer: series of 21 cases
 Case rept Natural histy of early gastric : series of 21 cases Auths Hiroyoshi Iwagami 1, Ryu Ishihara 1,KentaroNakagawa 1, Masayasu Ohmi 1, Kenshi Matsuno 1, Shuntaro Inoue 1, Masamichi Arao 1,TaroIwatsubo
Case rept Natural histy of early gastric : series of 21 cases Auths Hiroyoshi Iwagami 1, Ryu Ishihara 1,KentaroNakagawa 1, Masayasu Ohmi 1, Kenshi Matsuno 1, Shuntaro Inoue 1, Masamichi Arao 1,TaroIwatsubo
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID
 ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
Mucinous Adenocarcinoma of the Stomach Clinicopathological
 THE KURUME MEDICAL JOURNAL Vo1. 43, p. 289-294, 1996 ORIGINAL ARTICLE Mucinous Adenocarcinoma of the Stomach Clinicopathological Studies KIKUO KOUFUJI, JINRYO TAKEDA, ATSUSHI TOYONAGA, ISSEI KODAMA, KEISHIRO
THE KURUME MEDICAL JOURNAL Vo1. 43, p. 289-294, 1996 ORIGINAL ARTICLE Mucinous Adenocarcinoma of the Stomach Clinicopathological Studies KIKUO KOUFUJI, JINRYO TAKEDA, ATSUSHI TOYONAGA, ISSEI KODAMA, KEISHIRO
We are IntechOpen, the first native scientific publisher of Open Access books. International authors and editors. Our authors are among the TOP 1%
 We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin
 The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin 24.06.15 Norman Barrett Smiles [A brief digression - Chair becoming
The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin 24.06.15 Norman Barrett Smiles [A brief digression - Chair becoming
Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 9: 1209-1214, 2015 Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions TATSUYA TOYOKAWA
EXPERIMENTAL AND THERAPEUTIC MEDICINE 9: 1209-1214, 2015 Risk factors for non-curative resection of early gastric neoplasms with endoscopic submucosal dissection: Analysis of 1,123 lesions TATSUYA TOYOKAWA
References. GI Biopsies. What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD
 What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD jcrawford1@nshs.edu Executive Director and Senior Vice President for Laboratory Services North
What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD jcrawford1@nshs.edu Executive Director and Senior Vice President for Laboratory Services North
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you)
 What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
Large polyps: EMR, ESD, TEM and segmental resection. Terry Phang 2017 SON fall update
 Large polyps: EMR, ESD, TEM and segmental resection Terry Phang 2017 SON fall update Key Points: Large polyps No RCT re: Recurrence, complications Piecemeal vs en bloc: EMR vs ESD Partial vs full-thickness:
Large polyps: EMR, ESD, TEM and segmental resection Terry Phang 2017 SON fall update Key Points: Large polyps No RCT re: Recurrence, complications Piecemeal vs en bloc: EMR vs ESD Partial vs full-thickness:
Early and long term outcomes of endoscopic submucosal dissection for early gastric cancer in a large patient series
 594 Early and long term outcomes of endoscopic submucosal dissection for early gastric cancer in a large patient series KEN OHNITA 1, HAJIME ISOMOTO 1, SABURO SHIKUWA 2, HIROYUKI YAJIMA 1, HITOMI MINAMI
594 Early and long term outcomes of endoscopic submucosal dissection for early gastric cancer in a large patient series KEN OHNITA 1, HAJIME ISOMOTO 1, SABURO SHIKUWA 2, HIROYUKI YAJIMA 1, HITOMI MINAMI
Disclosures. Gastric Intestinal Metaplasia and Early Gastric Cancer: Screening, Surveillance, and Endoscopic Therapy. ASGE Guidelines.
 Gastric Intestinal Metaplasia and Early Gastric Cancer: Screening, Surveillance, and Endoscopic Therapy Consultant for: Olympus Medtronic US Endoscopy Disclosures Joo Ha Hwang, MD, PhD Associate Professor
Gastric Intestinal Metaplasia and Early Gastric Cancer: Screening, Surveillance, and Endoscopic Therapy Consultant for: Olympus Medtronic US Endoscopy Disclosures Joo Ha Hwang, MD, PhD Associate Professor
Can magnifying endoscopy with narrow band imaging be useful for low grade adenomas in preoperative biopsy specimens?
 Gastric Cancer (2012) 15:170 178 DOI 10.1007/s10120-011-0093-6 ORIGINAL ARTICLE Can magnifying endoscopy with narrow band imaging be useful for low grade adenomas in preoperative biopsy specimens? Kazuhiro
Gastric Cancer (2012) 15:170 178 DOI 10.1007/s10120-011-0093-6 ORIGINAL ARTICLE Can magnifying endoscopy with narrow band imaging be useful for low grade adenomas in preoperative biopsy specimens? Kazuhiro
A218 : Esophagus cancer tissues. (formalin fixed)
 (formalin fixed) For research use only Specifications: No. of cases: 40 Tissue type: Esophagus cancer tissues No. of spots: 2 spots from each cancer case (80 spots) 4 non-neoplastic spots (4 spots) Total
(formalin fixed) For research use only Specifications: No. of cases: 40 Tissue type: Esophagus cancer tissues No. of spots: 2 spots from each cancer case (80 spots) 4 non-neoplastic spots (4 spots) Total
Hyperplastische Polyps Innocent bystanders?
 Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/48400
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/48400
Frozen Section Analysis of Esophageal Endoscopic Mucosal Resection Specimens in the Real-Time Management of Barrett s Esophagus
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:173 178 Frozen Section Analysis of Esophageal Endoscopic Mucosal Resection Specimens in the Real-Time Management of Barrett s Esophagus GANAPATHY A. PRASAD,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:173 178 Frozen Section Analysis of Esophageal Endoscopic Mucosal Resection Specimens in the Real-Time Management of Barrett s Esophagus GANAPATHY A. PRASAD,*
T. Shono, 1 K. Ishikawa, 1 Y. Ochiai, 1 M. Nakao, 1 O. Togawa, 1 M. Nishimura, 1 S. Arai, 1 K. Nonaka, 2 Y. Sasaki, 2 and H. Kita 1. 1.
 International Surgical Oncology Volume 2011, Article ID 948293, 6 pages doi:10.1155/2011/948293 Clinical Study Feasibility of Endoscopic Submucosal Dissection: A New Technique for En Bloc Resection of
International Surgical Oncology Volume 2011, Article ID 948293, 6 pages doi:10.1155/2011/948293 Clinical Study Feasibility of Endoscopic Submucosal Dissection: A New Technique for En Bloc Resection of
Definition of GERD American College of Gastroenterology
 Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
