ORIGINAL ARTICLE. The JAK2 V617F tyrosine kinase mutation in blood donors with upper-limit haematocrit levels
|
|
|
- Lydia Holt
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE The JAK2 V617F tyrosine kinase mutation in blood donors with upper-limit haematocrit levels Giuseppe Tagariello, Rosanna Di Gaetano, Roberto Sartori, Daniela Zanotto, Donata Belvini, Paolo Radossi, Renzo Risato, Giovanni Roveroni, Roberta Salviato, Cristina Tassinari, Nunzio Toffano Servizio Trasfusionale, Centro Regionale per le Malattie del Sangue ed Emofilia, Ospedale di Castelfranco Veneto e Montebelluna, Azienda ULSS 8 Regione Veneto, Italy Background. It is not rare to observe in blood donors a level of haematocrit (Hct) above or close to the highest normal limit. In the case of blood donors the diagnosis and clinical evaluation of this alteration may be complicated by regular blood donations that can mask an underlying disease such as polycythaemia vera. Recently a single acquired mutation in the Janus kinase 2 gene (JAK2) on chromosome 9 was identified and it was found that the incidence of this mutation was high in patients with polycythaemia vera. Material and Methods. From the January 1, 2006 to December 31, 2006 all consecutive donors with a Hct above 50% if males (n=84) and 46% if females (n=19) underwent JAK2 mutation analysis. Seventy-nine donors (59 males and 20 females) whose Hct was normal at their last blood donation were randomly selected and used as controls. Results. Among the group of blood donors with a high Hct, we identified one donor who was positive for the JAK2 mutation. This man had a Hct of 50.6% at his last donation, while his average Hct in the preceding year was 51.7%. The prevalence of the JAK2 mutation could be estimated to be 1%, 0.6% or 0.02% in the three different populations considered: donors with a Hct level above the upper limit of normal, all tested donors or the entire donor cohort attending our transfusion service, respectively. Conclusions. The present study suggests that apparently healthy subjects with repeatedly high levels of Hct may have the acquired mutation in JAK2. Laboratory screening tests for JAK2 may be offered to blood donors at transfusion services with expertise in molecular genetics. Keywords: JAK2 mutations, haematocrit, polycythaemia vera, myeloproliferative disorder, blood donors. Introduction Blood donors have their haematocrit (Hct) and haemoglobin (Hb) values tested regularly to exclude anaemia, which is the most frequent cause for not being accepted as a donor 1. However, it is not uncommon to observe a Hb or Hct value above or close to the upper limit of normal and in some studies such values have been investigated to exclude or confirm the presence of secondary causes of erythrocytosis as well as a primary myeloproliferative disorder (MPD) such as polycythaemia vera (PV) 2. Among the cohort of blood donors, the diagnosis and clinical evaluation of high Hct and Hb values may be complicated by numerous, regular blood donations that can mask an underlying disease because of the steady decrement of blood mass caused by the donations. MPD is the name given to a family of diseases in which blood cells are overproduced; based on the prevalent single lineage, different types of disorders SIMTI Servizi Srl 111
2 Tagariello G et al. can be distinguished, including idiopathic myelofibrosis, essential thrombocythaemia and PV 3,4. Polycythaemia vera is characterized by an increased production of red blood cells and it is the most common chronic MPD with a reported annual incidence of about 2 per 100,000 persons. The male to female ratio is 1.2, the average age at diagnosis is approximately 60 years and the most frequent causes of death are thrombosis and haematological malignancies 5-8. It is currently diagnosed according to the PV Study Group (PVSG) criteria, which are based on the findings of a physical examination plus laboratory examination of blood and bone marrow cells 3,4. The cause of PV was unknown until 2005 when four independent research groups identified a single acquired mutation in the Janus kinase 2 gene (JAK2) on chromosome 9 and it was found that the incidence of this mutation was high in patients with PV The JAK2 protein functions as an intermediate between membrane receptors and signalling molecules. The point mutation in exon 12 of JAK2, leading to a valineto-phenylalanine substitution (V617F) due to replacement of G by T in nucleotide sequences (1848G>T), causes constitutive activation of the tyrosine kinase that is believed to confer erythropoietin hypersensitivity and erythropoietin-independent survival to the myeloid stem cell 13. In recent studies the JAK2 mutation has been found in 65-97% of patients with PV, but also in other MPD such as hypereosinophilic syndrome, chronic neutrophilic leukaemia, chronic idiopathic myelofibrosis and essential thrombocythaemia 14,15. On the basis of these recent findings, a new diagnostic algorithm for PV has been suggested in which the first step in the diagnosis of an erythrocytosis is to determine whether JAK2 V617F is present in the granulocytes In keeping with the important aim of preventive medicine offered by transfusion services to blood donors, all consecutive donors at our centre with a Hct value >50% for males and >46% for females were screened for this mutation. Concurrently, blood samples from a group of donors with normal Hct values were collected to act as controls. The objective was not only to estimate the incidence of this mutation in blood donors with Hct values above or near the upper limit of normal, but also to evaluate whether or not blood banks might be able to contribute to screening for undiagnosed patients with PV. Materials and methods Study population In our transfusion centre nearly 6,000 donors are provide a total number of approximately 12,000 donations per year, including whole blood, plasma, platelets and multi-component products (plasma-platelets, erythrocytes-plasma, etc.). Prior to each donation all data, including red blood cell, white blood cell and platelet counts, haematocrit and haemoglobin concentration, are routinely recorded in a database. Between January 1, 2006 and December 31, 2006 there were 11,240 donations from 5,636 regular blood donors (total donation index 1.99 per year). From these, 84 males and 19 females were identified as having a high Hct, defined as above 50% for men and above 46% for women. In this cohort, during a 1,846-year donation period, the average number of donations per male was 22.1 and per female Seventy-nine donors (59 male and 20 female) whose Hct had been normal at their last blood donation were randomly selected and used as controls (Table I). JAK2 mutation screening All analyses were carried out in our laboratory which is specialised in molecular medicine, mainly as a national referral centre for haemophilia genetics. In order to identify the V617F (1848G>T) mutation within JAK2 we used the amplification refractory mutation system (ARMS) which, under ideal polymerase chain reaction (PCR) conditions, is an extremely efficient detection method for the single base change 20. Peripheral blood was collected into Vacutainer tubes containing EDTA and DNA was extracted as previously reported 18.. The presence of the V617F (1848G>T) mutation was identified by PCR, using four primers: forward outer (FO), 5' TCC TCA GAA CGT TGA TGG CAG 3', reverse outer (RO), 5' ATT GCT TTC CTT TTT CAC AAG AT 3', forward wild-type-specific (Fwt), 5' CAT TTG GTT TTA AAT TAT GGA GTA TAT G 3' and reverse mutant specific (Rmt) 5' GTT TTA CTT ACT CTC GTC TCC ACA AAA 3'. The FO and RO primers flank the JAK2 exon 12 and amplify a 453 bp product control in all cases. The Fwt and RO primers amplify a 229 bp wildtype-specific band (1848G) while FO and Rmt amplify a 279 bp mutant-specific band (1848T). The PCR were performed using AmpliTaq Gold PCR Master Mix 2X 250U/5mL (Appleare), 1.5 mm 112
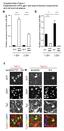
3 JAK 2 mutation in blood donors Table I - General characteristics of subjects with high haematocrit and normal values Males Females Hct (N=84) Normal Hct (N=59) P* Hct (N=19) Normal Hct (N=209) P* mean ± SD mean ± SD mean ± SD mean ± SD Hct (%) ± ± 1.87 < ± ± 1.77 < Hb (g/dl) ± ± 0.6 < ± ± 0.72 < WBC (x10 9 /L) ± ± < ± ± NS PLTs (x10 9 /L) 236 ± ± 52.0 NS 244 ± ± 49.6 NS Donations (n.) 22.1 ± ± 12.4 NS ± ± 11.1 NS Age (yrs) 44.5 ± ± 8.60 NS 43.8 ± ± 11.8 NS Years since first donation 11.1 ± ± 6.8 NS 8.20 ± ± 7.6 NS Legend- Ht: haematocrit; Hb: haemoglobin; PLTs: platelet count; WBC: white blood cell count; SD: standard deviation; NS: not significant *T test for independent samples and homogeneous variance MgCl 2, 150 ng of blood donor's DNA and 1 µm and 0.5 µm of the outer primers (FO and RO) and the mutant/wild-type-specific inner primers (Fwt and Rmt), respectively. The amplification conditions consisted of a starting denaturation step of one cycle at 94 C for 5 min followed by 35 cycles of denaturation (95 C, 30 sec), annealing (60 C, 30 sec) and extension (72 C for 60 sec). These cycles were followed by a final extension step of one cycle at 72 C for 5 min. Products were resolved on 6% acrylamide gel and examined after staining with ethidium bromide (Figure 1). Results The mean haematological values in the two different populations over the entire donation life period are reported in table I. There were statistically significant differences between the two groups for Hct and Hb in both males and females (t-test for independent samples and homogeneous variance), as expected, but also for white blood cell count in the subgroup of males but not in the females (Table I). The mean Hct value of the last donations from the 103 donors with high Hct levels was 51.02% for males and 46.9% for females, while the mean value of the control cohort with a normal Hct at their last donation was 42% and 39% for males and females, respectively (data not shown). Among the 84 men with a high Hct we identified one positive for the JAK2 mutation. He had a Hct of 50.6% during the last donation while his average Hct in the last year was 51.7%. As the patient's Hb concentration was above 18.5 g/dl he met both the Figure 1 - Pattern of the JAK2 1848G>T mutation detection in polyacrylamide gel. Lane M, 100 bp ladder; lane 1, negative control; lane 2, normal genotype sample; lane 3, heterozygous blood donor; lane 4, positive heterozygous control. FO and RO primers generate a control 453 bp band in all cases. Fwt and RO primers generate a 229 bp wild-type G-specific product and FO and Rmt primers generate a 279 bp mutant T-specific product. major criteria of the new WHO proposal for the diagnosis of PV 16. The entire donation history of this patient is shown in figure 2. These results account for a total prevalence of the JAK2 mutation of 1% in the blood donor population with elevated Hct (1 out of 103). None of the 79 blood donors (male and female) with a normal Hct in their last donation had the JAK2 mutation. 113
4 Tagariello G et al Ht (%) Ht WBCs PLTs WBCs (x 10-3 L -1 ) PLTs (x 10-3 L -1 ) 0 0 May-96 Feb-98 Dec-99 May-01 Dec-01 Jul-02 Apr-03 Nov-03 Jul-04 Mar-05 Nov-05 Mar-06 donations Figure 2 - Haematocrit (Ht), white blood cell count (WBCs) and platelet count (PLTs) in the JAK2-positive 43-year old male blood donor over the 10-year period he had donated blood. All three lines show an increasing trend, in accordance with the natural history of PV Discussion The recent proposal of a new diagnostic flow procedure for the diagnosis of PV prompted us to perform a study on blood donors with high Hct levels to ascertain whether any of them had an underlying disease. For this purpose we looked for the JAK2 mutation in a cohort of 182 donors, a proportion of whom had what we defined as a high Hct (>50% for males, >46% for females) at their last donation. In this subgroup with high Hct, we found one male with the JAK2 mutation and after further haematological investigation PV was diagnosed according to the criteria of the PVSG. The estimated prevalence of PV is considered to be 1-5 cases/million per year although from a large study performed in Vicenza 21 the prevalence in an unselected population seems much higher (around 300/million annually). This is also confirmed by another Italian study which reported 8 cases of MPD among a population of 90,000 blood donors 22. On the other hand, in a pre-selected blood donor cohort of 81 consecutive donors with Hct levels >49%, Zanella et al. reported a 3.7% prevalence of PV, diagnosed according to the PVSG criteria 2. Our results seem to be in keeping with those of the few studies evaluating the supposed 'normal' population of blood donors 2,22 or general population 21. In these studies the prevalence of MPD is around 1-3% which is similar to the prevalence that we found, but very different from that in a hospitalised population. None of our blood donors had a history of present or past thrombosis, but this is very probably due to the presence of low vascular risk and presumably related to the young age of this cohort. An interesting question is whether the prolonged myeloid 'stimulus' from phlebotomies can induce inhibition of the feed-back control of cells committed to becoming red cells; it could also be suspected that blood donations may trigger the onset of a preexisting, latent, primary MPD. However, among the family of haematological malignancies, only PV has been reported to be more frequent in blood donors than in the general population and this might be due 114
5 JAK 2 mutation in blood donors to early detection because of frequent blood tests carried out in such subjects 22,23. In a hospital setting, in which blood samples were randomly collected, surprisingly 37 out of a total of 3,935 were found to be positive for the JAK2 mutation. However, only one of these samples had blood results indicative of possible PV but several had non-haematological diseases. On average, samples with the mutation had normal red cell counts but significantly higher white blood cell and platelet counts, although most were within the normal range. These data suggest that the JAK2 V617F mutation is much more common than MPD and its occurrence might be a prelude to whole blood cell abnormalities and other diseases, but it cannot by itself be used to diagnose MPD 24. Passamonti et al. reported that they did not find the mutation in any of 75 healthy individuals investigated 25. The present study suggests that subjects with repeatedly high Hct levels may have the acquired mutation in JAK2. This finding should be confirmed in a larger donor population. The follow-up of the negative donors could, however, also be useful in the light of the possible identification of an acquired mutation, which would provide additional information for understanding the natural course of the development of PV. This could be of particular importance if supersensitive assays able to detect small amounts of JAK2 V617F in healthy individuals were used, in a situation analogous to that of BCR/ABL 26. Finally, the overall objectivity and accessibility of JAK2 mutation screening using peripheral blood enables a practical, modern approach to studying patients suspected of having PV that does not require red cell mass measurements and reduces the number of bone marrow examinations 27,28. The possibility of bypassing a bone marrow examination if peripheral blood mutation screening reveals the presence of JAK2 V617F could be argued. However, such a policy is currently considered premature and would lead to the loss of useful baseline information from bone marrow histology and cytogenetic analysis. Nevertheless, the remarkably close association between PV and JAK2 V617F has further undermined the already limited value of red cell mass measurements and specialised biological assays for the diagnosis of PV such as erythroid colony formation, megakaryocyte thrombopoietin receptor expression and platelet-rich plasma serotonin level. This news is to be welcomed because each of these assays entails a certain level of expertise that is not widely available clinically. Obviously, for routine clinical practice the feasibility of such a process depends on the availability of laboratory screening tests for JAK2 V617F which may be offered also at a transfusion service with particular expertise in molecular genetics. Acknowledgements This study was supported in part by Avis Castellana, Borsa di studio Giorgio Lago and Associazione progresso ematologico, Castelfranco Veneto (TV), Italy. We thank Mrs. Gabrielle Clarke for editing this manuscript. References 1) Davey RJ. The blood centre as a community health resource. Vox Sang 2006; 91: ) Zanella A, Silvani C, Banfi P, et al. Screening and evaluation of blood donors with upper-limit hematocrit levels. Transfusion 1987; 27: ) Thiele J, Kvasnicka HM. A critical reappraisal of the WHO classification of the chronic myeloproliferative disorders. Leuk Lymphoma 2006; 47: ) Thiele J, Kvasnicka HM. Chronic myeloproliferative disorders with thrombocythemia: a comparative study of two classification systems (PVSG, WHO) on 839 patients. Ann Hematol 2003; 82: ) Finazzi G. A prospective analysis of thrombotic events in the European collaboration study on low-dose aspirin in polycythemia (ECLAP). Pathol Biol 2004; 52: ) Marchioli R, Finazzi G, Landolfi R, et al. Vascular and neoplastic risk in a large cohort of patients with polycythemia vera. J Clin Oncol 2005; 23: ) Stuart BJ, Viera AJ. Polycythemia vera. Am Fam Physician 2004; 69: ) Tefferi A, Spivak JL. Polycythemia vera: scientific advances and current practice. Semin Hematol 2005; 42: ) Baxter RJ, Scott LM, Campbell PJ, et al., Cancer Genome Project. Acquired mutation of the tyrosine kinase JAK2 in human myeloproliferative disorders. Lancet 2005; 365: ) James C, Ugo V, Le Couedic SP, et al. A unique clonal JAK2 mutation leading to constitutive signalling causes polycythemia vera. Nature 2005; 434: ) Kralovics R, Passamonti F, Buser AS, et al. A gain-offunction mutation of JAK2 in myeloproliferative disorders. N Engl J Med 2005; 352: ) Levine RL, Wadleigh M, Cools J, et al. Activating mutation in the tyrosine kinase JAK2 in polycythemia vera, essential thrombocythemia, and myeloid 115
6 Tagariello G et al. metaplasia with myelofibrosis. Cancer Cell 2005; 7: ) Zhao ZJ, Vainchenker W, Krantz SB, et al. Role of tyrosine kinases and phosphatases in polycythemia vera. Semin Hematol 2005; 42: ) Tefferi A, Gilliland DG. The JAK2V617F tyrosine kinase mutation in myeloproliferative disorders: status report and immediate implications for disease classification and diagnosis. Mayo Clin Proc 2005; 80: ) Tefferi A. Classification, diagnosis and management of myeloproliferative disorders in the JAK2V617F era. Hematology Am Soc Hematol Educ Program 2006; 34: ) Tefferi A, Thiele J, Orazi A, et al. Proposals and rationale for revision of the World Health Organization diagnostic criteria for polycythemia vera, essential thrombocythemia, and primary myelofibrosis: recommendations from an ad hoc international expert panel. Blood ;110: ) Chang CC. BCR/ABL-negative chronic myeloproliferative disorders: JAK2 mutation and beyond. Arch Path Lab Med 2006; ) James C, Delhommeau F, Marzac C, et al. Detection of JAK2 V617F as a first intention diagnostic test for erythrocytosis. Leukemia 2006; 20: ) Michiels JJ, De Raeve H, Berneman Z, et al. The 2001 World Health Organization and updated European clinical and pathological criteria for the diagnosis, classification, and staging of the Philadelphia chromosome-negative chronic myeloproliferative disorders. Semin Thromb Hemost 2006; 32: ) Jones AV, Kreil S, Zoi K, et al. Widespread occurrence of the JAK2 V617F mutation in chronic myeloproliferative disorders. Blood 2005; 106: ) Ruggeri M, Tosetto A, Frezzato M, Rodeghiero F The rate of progression to polycythemia vera or essential thrombocythemia in patients with erythrocytosis or thrombocytosis. Ann Intern Med 2003; 139: ) Randi ML, Rossi C, Barbone E, et al. Myeloproliferative disease in patients with a history of multiple blood donations: a report of 8 cases. Haematologica 1994; 79: ) Merk K, Mattsson A, Holm G, et al. The incidence of cancer among blood donors. Int J Epidemiol 1990; 19: ) Xu X, Zhang Q, Luo J, et al. JAK2(V617F): Prevalence in a large Chinese hospital population. Blood 2007; 109: ) Passamonti F, Rumi E, Pietra D, et al. JAK2 (V617F) mutation in healthy individuals. Br J Haematol 2007;136: ) Bose S, Deininger M, Gora-Tybor J, et al. The presence of typical and atypical BCR-ABL fusion genes in leukocytes of normal individuals: biologic significance and implications for the assessment of minimal residual disease. Blood 1998; 92: ) Tefferi A. The rise and fall of red cell mass measurement in polycythemia vera Curr Hematol Rep 2005; 4: ) Vardiman JW, Harris NL, Brunning RD. The World Health Organization (WHO) classification of the myeloid neoplasms. Blood 2002; 100: Reveived: 4 September Revision accepted: 6 November 2008 Correspondence: Giuseppe Tagariello, MD Servizio Trasfusionale, Centro Regionale per le Malattie del Sangue ed Emofialia Ospedale di Castelfranco Veneto, Castelfranco Veneto (TV) - Italy giuseppe.tagariello@ulssasolo.ven.it 116
Polycythemia Vera and Essential Thombocythemia A Single Institution Experience
 INDIAN JOURNAL OF MEDICAL & PAEDIATRIC ONCOLOGY Vol. 29 No 4, 2008 7 Original Article-I Polycythemia Vera and Essential Thombocythemia A Single Institution Experience CECIL ROSS, NAVYA, VANAMALA AND KARUNA
INDIAN JOURNAL OF MEDICAL & PAEDIATRIC ONCOLOGY Vol. 29 No 4, 2008 7 Original Article-I Polycythemia Vera and Essential Thombocythemia A Single Institution Experience CECIL ROSS, NAVYA, VANAMALA AND KARUNA
Characterization of blood donors with high haemoglobin concentration
 STATE OF THE ART 2A-S05-02 ISBT Science Series (2013) 8, 114 118 ISBT Science Series 2013 International Society of Blood Transfusion Characterization of blood donors with high haemoglobin concentration
STATE OF THE ART 2A-S05-02 ISBT Science Series (2013) 8, 114 118 ISBT Science Series 2013 International Society of Blood Transfusion Characterization of blood donors with high haemoglobin concentration
Emerging diagnostic and risk stratification criteria
 PV STATE OF MIND Polycythemia vera: Emerging diagnostic and risk stratification criteria Rami S. Komrokji, MD Moffitt Cancer Center, Tampa, Florida Disclosure These slides were developed by Incyte Corporation
PV STATE OF MIND Polycythemia vera: Emerging diagnostic and risk stratification criteria Rami S. Komrokji, MD Moffitt Cancer Center, Tampa, Florida Disclosure These slides were developed by Incyte Corporation
A. ILEA 1* A. M. VLADAREANU 2 E. NICULESCU-MIZIL 3
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 1-2016 THE SIMULTANEOUS OCCURRENCE OF THE BCR-ABL TRANSLOCATION AND THE Jak2V617F MUTATION. DETECTION AND DYNAMICS
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 1-2016 THE SIMULTANEOUS OCCURRENCE OF THE BCR-ABL TRANSLOCATION AND THE Jak2V617F MUTATION. DETECTION AND DYNAMICS
ASSESSMENT OF JAK2V617F MUTATION FREQUENCY IN PATIENTS WITH POLYCYTHEMIA VERA CITY OF TABRIZ IN IRAN
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Asadi et al. SJIF Impact Factor 5.210 Volume 4, Issue 11, 369-380 Research Article ISSN 2278 4357 ASSESSMENT OF JAK2V617F MUTATION FREQUENCY IN PATIENTS
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Asadi et al. SJIF Impact Factor 5.210 Volume 4, Issue 11, 369-380 Research Article ISSN 2278 4357 ASSESSMENT OF JAK2V617F MUTATION FREQUENCY IN PATIENTS
Technical Bulletin No. 100
 CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 100 August 2, 2012 JAK2 AND MPL 515 MUTATIONAL ANALYSIS Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Technical Director, CPAL Jill A.
CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 100 August 2, 2012 JAK2 AND MPL 515 MUTATIONAL ANALYSIS Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Technical Director, CPAL Jill A.
Decreased expression of PIAS1 and PIAS3 in essential thrombocythemia patients
 Decreased expression of PIAS1 and PIAS3 in essential thrombocythemia patients H.-H. Hsiao 1,2, Y.-C. Liu 1,2, M.-Y. Yang 3, Y.-F. Tsai 2, T.-C. Liu 1,2, C.-S. Chang 1,2 and S.-F. Lin 1,2 1 Faculty of Medicine,
Decreased expression of PIAS1 and PIAS3 in essential thrombocythemia patients H.-H. Hsiao 1,2, Y.-C. Liu 1,2, M.-Y. Yang 3, Y.-F. Tsai 2, T.-C. Liu 1,2, C.-S. Chang 1,2 and S.-F. Lin 1,2 1 Faculty of Medicine,
The Internists Approach to Polycythemia and Implications of Uncontrolled Disease
 The Internists Approach to Polycythemia and Implications of Uncontrolled Disease Mary Jo K. Voelpel, DO, FACOI, MA, CS Associate Clinical Professor MSU-COM Disclosures NONE Overview 1. Objectives 2. Case
The Internists Approach to Polycythemia and Implications of Uncontrolled Disease Mary Jo K. Voelpel, DO, FACOI, MA, CS Associate Clinical Professor MSU-COM Disclosures NONE Overview 1. Objectives 2. Case
Evaluation of JAK2V617F mutation prevalence in myeloproliferative neoplasm by AS-RT-PCR
 Original Article Evaluation of JAK2V617F mutation prevalence in myeloproliferative neoplasm by AS-RT-CR Karimzadeh. 1 M.Sc, Ghaffari.SH 2 h.d, Chahardouli.B 2 M.Sc,Zaghal.A 1 M.Sc, Einollahi.N 1 h.d, Mousavi.SA
Original Article Evaluation of JAK2V617F mutation prevalence in myeloproliferative neoplasm by AS-RT-CR Karimzadeh. 1 M.Sc, Ghaffari.SH 2 h.d, Chahardouli.B 2 M.Sc,Zaghal.A 1 M.Sc, Einollahi.N 1 h.d, Mousavi.SA
WHO Update to Myeloproliferative Neoplasms
 WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: October 15, 2018 Related Policies: None JAK2, MPL and CALR Testing for Myeloproliferative Neoplasms Description Somatic (acquired) genetic variants in JAK2, MPL,
FEP Medical Policy Manual Effective Date: October 15, 2018 Related Policies: None JAK2, MPL and CALR Testing for Myeloproliferative Neoplasms Description Somatic (acquired) genetic variants in JAK2, MPL,
The treatment of polycythaemia vera: an update in the JAK2 era
 Intern Emerg Med (2007) 2:13 18 DOI 10.1007/s11739-007-0003-4 IM REVIEW G. Finazzi T. Barbui The treatment of polycythaemia vera: an update in the JAK2 era Received: 31 August 2006 / Accepted in original
Intern Emerg Med (2007) 2:13 18 DOI 10.1007/s11739-007-0003-4 IM REVIEW G. Finazzi T. Barbui The treatment of polycythaemia vera: an update in the JAK2 era Received: 31 August 2006 / Accepted in original
Hydroxyurea: the comparator in studies with new anti-jak2 inhibitors
 Hematology Meeting Reports 2009;3(3):108 114 SESSION VIII xg. Finazzi T. Barbui 1 x Divisione di Ematologia e 1 Fondazione per la Ricerca Ospedali Riuniti di Bergamo, Italy Hydroxyurea: the comparator
Hematology Meeting Reports 2009;3(3):108 114 SESSION VIII xg. Finazzi T. Barbui 1 x Divisione di Ematologia e 1 Fondazione per la Ricerca Ospedali Riuniti di Bergamo, Italy Hydroxyurea: the comparator
Myeloproliferative Disorders in the Elderly: Clinical Presentation and Role of Bone Marrow Examination
 Myeloproliferative Disorders in the Elderly: Clinical Presentation and Role of Bone Marrow Examination Arati V. Rao, M.D. Division of Medical Oncology and Geriatrics Duke University Medical Center Durham
Myeloproliferative Disorders in the Elderly: Clinical Presentation and Role of Bone Marrow Examination Arati V. Rao, M.D. Division of Medical Oncology and Geriatrics Duke University Medical Center Durham
Practice Patterns in the Diagnosis and Treatment of Polycythemia Vera in the Post JAK2 V617F Discovery Era
 1238 Original Research Practice Patterns in the Diagnosis and Treatment of Polycythemia Vera in the Post JAK2 V617F Discovery Era Elizabeth M. Kander, MD a ; Alison R. Moliterno, MD b ; Alfred Rademaker,
1238 Original Research Practice Patterns in the Diagnosis and Treatment of Polycythemia Vera in the Post JAK2 V617F Discovery Era Elizabeth M. Kander, MD a ; Alison R. Moliterno, MD b ; Alfred Rademaker,
Abstract. Hematopathology / Early Prepolycythemic Phase of PV
 Hematopathology / Early Prepolycythemic Phase of PV The Significance of Bone Marrow Biopsy and JAK2 V617F Mutation in the Differential Diagnosis Between the Early Prepolycythemic Phase of Polycythemia
Hematopathology / Early Prepolycythemic Phase of PV The Significance of Bone Marrow Biopsy and JAK2 V617F Mutation in the Differential Diagnosis Between the Early Prepolycythemic Phase of Polycythemia
Classification, Diagnosis and Management of Myeloproliferative Disorders in the JAK2V617F Era
 Classification, Diagnosis and Management of Myeloproliferative Disorders in the JAK2V617F Era Ayalew Tefferi JAK2V617F, a somatic gain-of-function mutation involving the JAK2 tyrosine kinase gene, occurs
Classification, Diagnosis and Management of Myeloproliferative Disorders in the JAK2V617F Era Ayalew Tefferi JAK2V617F, a somatic gain-of-function mutation involving the JAK2 tyrosine kinase gene, occurs
MPL W515L K mutation
 MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
74y old Female with chronic elevation of Platelet count. August 18, 2005 Faizi Ali, MD Hematopathology Fellow
 74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms
 Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms Sonam Prakash declares affiliation with Incyte Corporation: Advisor for Hematopathology Publications Steering Committee Sonam Prakash,
Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms Sonam Prakash declares affiliation with Incyte Corporation: Advisor for Hematopathology Publications Steering Committee Sonam Prakash,
JAK2 V617F and the evolving paradigm of polycythemia vera
 VOLUME 45 ㆍ NUMBER 2 ㆍ June 2010 THE KOREAN JOURNAL OF HEMATOLOGY REVIEW ARTICLE JAK2 V617F and the evolving paradigm of polycythemia vera Robert T. Means, Jr. Department of Internal Medicine and Markey
VOLUME 45 ㆍ NUMBER 2 ㆍ June 2010 THE KOREAN JOURNAL OF HEMATOLOGY REVIEW ARTICLE JAK2 V617F and the evolving paradigm of polycythemia vera Robert T. Means, Jr. Department of Internal Medicine and Markey
MYELOPROLIFERATIVE NEOPLASMS
 9 : 2 MYELOPROLIFERATIVE NEOPLASMS Introduction William Dameshek in 1951 introduced the term Myeloproliferative disorders (MPD). This included polycythemia vera (PV), essential thrombocythemia (ET), primary
9 : 2 MYELOPROLIFERATIVE NEOPLASMS Introduction William Dameshek in 1951 introduced the term Myeloproliferative disorders (MPD). This included polycythemia vera (PV), essential thrombocythemia (ET), primary
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms. Curtis A. Hanson, MD
 Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Polycythemia vera: Emerging diagnostic and risk stratification criteria
 This article, sponsed by Incyte Cpation, is based on a paid interview with Rami S. Komrokji, MD, of Moffitt Cancer Center, Tampa, Flida, conducted on May 4, 2015. Polycythemia vera: Emerging diagnostic
This article, sponsed by Incyte Cpation, is based on a paid interview with Rami S. Komrokji, MD, of Moffitt Cancer Center, Tampa, Flida, conducted on May 4, 2015. Polycythemia vera: Emerging diagnostic
CLINICAL CASE PRESENTATION
 European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
[COMPREHENSIVE GENETIC ASSAY PANEL ON
 2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
Focus on aggressive polycythemia vera
 Focus on aggressive polycythemia vera Jerry L. Spivak, MD Professor of Medicine and Oncology Director, the Johns Hopkins Center for the Chronic Myeloproliferative Disorders Johns Hopkins University School
Focus on aggressive polycythemia vera Jerry L. Spivak, MD Professor of Medicine and Oncology Director, the Johns Hopkins Center for the Chronic Myeloproliferative Disorders Johns Hopkins University School
Molecular Diagnostics for Myeloproliferative Neoplasms. Noah Brown, MD April 16, 2015
 Molecular Diagnostics for Myeloproliferative Neoplasms Noah Brown, MD April 16, 2015 Outline 1. Brief MPN Introduction 2. When/How Should Molecular Testing be Performed? 3. JAK2 V617F Mutation Testing
Molecular Diagnostics for Myeloproliferative Neoplasms Noah Brown, MD April 16, 2015 Outline 1. Brief MPN Introduction 2. When/How Should Molecular Testing be Performed? 3. JAK2 V617F Mutation Testing
IJHOSCR. Original Article. International Journal of Hematology- Oncology and Stem Cell Research
 IJHOSCR International Journal of Hematology- Oncology and Stem Cell Research Original Article JAK2V617F Allele Burden Measurement in Peripheral Blood of Iranian Patients with Myeloproliferative Neoplasms
IJHOSCR International Journal of Hematology- Oncology and Stem Cell Research Original Article JAK2V617F Allele Burden Measurement in Peripheral Blood of Iranian Patients with Myeloproliferative Neoplasms
Why do patients with polycythemia vera clot? Kinsey McCormick Hematology Fellows conference August 10, 2012
 Why do patients with polycythemia vera clot? Kinsey McCormick Hematology Fellows conference August 10, 2012 Outline Case presentation Overview of PV Disease course Mechanisms of thrombosis Case Presentation
Why do patients with polycythemia vera clot? Kinsey McCormick Hematology Fellows conference August 10, 2012 Outline Case presentation Overview of PV Disease course Mechanisms of thrombosis Case Presentation
The 2008 World Health Organization Classification System for Myeloproliferative Neoplasms
 Review Article The 2008 World Health Organization Classification System for Myeloproliferative Neoplasms Order Out of Chaos Ayalew Tefferi, MD 1 ; Juergen Thiele, MD 2 ; and James W. Vardiman, MD 3 The
Review Article The 2008 World Health Organization Classification System for Myeloproliferative Neoplasms Order Out of Chaos Ayalew Tefferi, MD 1 ; Juergen Thiele, MD 2 ; and James W. Vardiman, MD 3 The
Supplementary Document
 Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms
 Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
Polycthemia Vera (Rubra)
 Polycthemia Vera (Rubra) Polycthemia Vera (Rubra) Increased red cells Clonal Myeloid lineages also increased 2-13 cases per million Mean age: 60 years Sites of Involvement Bone marrow Peripheral blood
Polycthemia Vera (Rubra) Polycthemia Vera (Rubra) Increased red cells Clonal Myeloid lineages also increased 2-13 cases per million Mean age: 60 years Sites of Involvement Bone marrow Peripheral blood
TRANSLOCATION t(3;12)(q26;q21) IN JAK2 V617F POINT MUTATION NEGATIVE CHRONIC IDIOPATHIC MYELOFIBROSIS: A CASE REPORT
 17 (1), 2014 63-68 DOI: 10.2478/bjmg-2014-0026 CASE REPORT TRANSLOCATION t(3;12)(q26;q21) IN JAK2 V617F POINT MUTATION NEGATIVE CHRONIC IDIOPATHIC MYELOFIBROSIS: A CASE REPORT Mešanović S. 1,*, Šahović
17 (1), 2014 63-68 DOI: 10.2478/bjmg-2014-0026 CASE REPORT TRANSLOCATION t(3;12)(q26;q21) IN JAK2 V617F POINT MUTATION NEGATIVE CHRONIC IDIOPATHIC MYELOFIBROSIS: A CASE REPORT Mešanović S. 1,*, Šahović
CLINICAL POLICY DEPARTMENT: Medical Management DOCUMENT NAME: JakafiTM REFERENCE NUMBER: NH.PHAR.98
 PAGE: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
PAGE: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
JAK2 V617F analysis. Indication: monitoring of therapy
 JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
Characterization of MPL-mutated myeloid neoplasms: a review of 224 MPL+ cases
 Article Characterization of MPL-mutated myeloid neoplasms: a review of 224 MPL+ cases Keming Lin 1,*, Gang Xu 1, Jie-Gen Jiang 1, Mayuko Imai 1, Zhao Wu 1, Paris Petersen 1, Kim Janatpour 1, and Bashar
Article Characterization of MPL-mutated myeloid neoplasms: a review of 224 MPL+ cases Keming Lin 1,*, Gang Xu 1, Jie-Gen Jiang 1, Mayuko Imai 1, Zhao Wu 1, Paris Petersen 1, Kim Janatpour 1, and Bashar
Definition of subtypes of essential thrombocythaemia and relation to polycythaemia vera based on JAK2 V617F mutation status: a prospective study
 Definition of subtypes of essential thrombocythaemia and relation to polycythaemia vera based on JAK V617F mutation status: a prospective study *Peter J Campbell, *Linda M Scott, Georgina Buck, Keith Wheatley,
Definition of subtypes of essential thrombocythaemia and relation to polycythaemia vera based on JAK V617F mutation status: a prospective study *Peter J Campbell, *Linda M Scott, Georgina Buck, Keith Wheatley,
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
Brief Communication Diagnostic Hematology
 Brief Communication Diagnostic Hematology Ann Lab Med 2015;35:233-237 http://dx.doi.org/10.3343/alm.2015.35.2.233 ISSN 2234-3806 eissn 2234-3814 Incidence, Clinical Features, and Prognostic Impact of CALR
Brief Communication Diagnostic Hematology Ann Lab Med 2015;35:233-237 http://dx.doi.org/10.3343/alm.2015.35.2.233 ISSN 2234-3806 eissn 2234-3814 Incidence, Clinical Features, and Prognostic Impact of CALR
ORIGINAL ARTICLE. A Tefferi 1, TL Lasho 1, J Huang 1, C Finke 1, RA Mesa 1,CYLi 2,WWu 3, CA Hanson 2 and A Pardanani 1
 (28) 22, 756 76 & 28 Nature Publishing Group All rights reserved 887-6924/8 $3. www.nature.com/leu ORIGINAL ARTICLE, compared to either a higher allele burden or unmutated status, is associated with inferior
(28) 22, 756 76 & 28 Nature Publishing Group All rights reserved 887-6924/8 $3. www.nature.com/leu ORIGINAL ARTICLE, compared to either a higher allele burden or unmutated status, is associated with inferior
Predictive factors of thrombosis for patients with essential thrombocythaemia: A single center study*
 Original papers Predictive factors of thrombosis for patients with essential thrombocythaemia: A single center study* Iwona Prajs A F, Kazimierz Kuliczkowski F Department and Clinic of Hematology, Blood
Original papers Predictive factors of thrombosis for patients with essential thrombocythaemia: A single center study* Iwona Prajs A F, Kazimierz Kuliczkowski F Department and Clinic of Hematology, Blood
RESEARCH ARTICLE. Abstract. Introduction
 RESEARCH ARTICLE Characterization and Prognosis Significance of JAK2 (V617F), MPL, and CALR Mutations in Philadelphia-Negative Myeloproliferative Neoplasms Roongrudee Singdong 1, Teerapong Siriboonpiputtana
RESEARCH ARTICLE Characterization and Prognosis Significance of JAK2 (V617F), MPL, and CALR Mutations in Philadelphia-Negative Myeloproliferative Neoplasms Roongrudee Singdong 1, Teerapong Siriboonpiputtana
Department of Hematology, Sakarya University Training and Research Hospital, Sakarya, Turkey.
 Original Article Hematology Medical Journal of Islamic World Academy of Sciences doi: 10.5505/ias.2018.90093 2018;26(3): 59-64 Retrospective analysis of patients with chronic myeloproliferative neoplasms:
Original Article Hematology Medical Journal of Islamic World Academy of Sciences doi: 10.5505/ias.2018.90093 2018;26(3): 59-64 Retrospective analysis of patients with chronic myeloproliferative neoplasms:
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Managing ET in Tiziano Barbui MD
 Managing ET in 2019 Tiziano Barbui MD (tbarbui@asst-pg23.it) Hematology and Foundation for Clinical Research, Hospital Papa Giovanni XXIII Bergamo, Italy Managing ET in 2019 Establish diagnosis Risk Stratification
Managing ET in 2019 Tiziano Barbui MD (tbarbui@asst-pg23.it) Hematology and Foundation for Clinical Research, Hospital Papa Giovanni XXIII Bergamo, Italy Managing ET in 2019 Establish diagnosis Risk Stratification
Transplants for MPD and MDS
 Transplants for MPD and MDS The question is really who to transplant, with what and when. Focus on myelofibrosis Jeff Szer Royal Melbourne Hospital Myelodysplasia Little needs to be said Despite new therapies
Transplants for MPD and MDS The question is really who to transplant, with what and when. Focus on myelofibrosis Jeff Szer Royal Melbourne Hospital Myelodysplasia Little needs to be said Despite new therapies
MPN What's new in the morphological classification, grading of fibrosis and the impact of novel drugs
 MPN What's new in the morphological classification, grading of fibrosis and the impact of novel drugs Hans Michael Kvasnicka University of Frankfurt, Germany hans-michael.kvasnicka@kgu.de Disclosure of
MPN What's new in the morphological classification, grading of fibrosis and the impact of novel drugs Hans Michael Kvasnicka University of Frankfurt, Germany hans-michael.kvasnicka@kgu.de Disclosure of
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: October 15, 2017 Related Policies: None JAK2, MPL, and CALR Testing for Myeloproliferative Neoplasms Description Somatic (acquired) genetic variants in JAK2, MPL,
FEP Medical Policy Manual Effective Date: October 15, 2017 Related Policies: None JAK2, MPL, and CALR Testing for Myeloproliferative Neoplasms Description Somatic (acquired) genetic variants in JAK2, MPL,
Understanding how Jakafi (ruxolitinib) inhibits* overactive JAK pathway signaling
 Understanding how Jakafi (ruxolitinib) inhibits* overactive JAK pathway signaling * Jakafi, a kinase inhibitor, inhibits and (Janus-associated kinases 1 and 2), which mediate the signaling of cytokines
Understanding how Jakafi (ruxolitinib) inhibits* overactive JAK pathway signaling * Jakafi, a kinase inhibitor, inhibits and (Janus-associated kinases 1 and 2), which mediate the signaling of cytokines
Highest rates of thrombosis = age > 70, history of thrombosis, active disease (> 6 phlebotomies/yr) [2]
![Highest rates of thrombosis = age > 70, history of thrombosis, active disease (> 6 phlebotomies/yr) [2] Highest rates of thrombosis = age > 70, history of thrombosis, active disease (> 6 phlebotomies/yr) [2]](/thumbs/87/95709298.jpg) Polycythemia Vera Treatment Policy Prepared by Dr. Jeannie Callum Updated May 2003 Introduction PV is a chronic, clonal, myeloproliferative disorder, classically associated with an increase in red cell
Polycythemia Vera Treatment Policy Prepared by Dr. Jeannie Callum Updated May 2003 Introduction PV is a chronic, clonal, myeloproliferative disorder, classically associated with an increase in red cell
International Journal of Gerontology
 International Journal of Gerontology 7 (2013) 40e44 Contents lists available at SciVerse ScienceDirect International Journal of Gerontology journal homepage: www.ijge-online.com Original Article JAK2 V617F
International Journal of Gerontology 7 (2013) 40e44 Contents lists available at SciVerse ScienceDirect International Journal of Gerontology journal homepage: www.ijge-online.com Original Article JAK2 V617F
The Importance of Identification of M-BCR- ABL Oncogene and JAK2 V617F Mutation in Myeloproliferative Neoplasms
 Acta Medica Marisiensis 2014;60(2):44-48 DOI: 10.2478/amma-2014-0010 RESEARCH ARTICLE The Importance of Identification of M-BCR- ABL Oncogene and JAK2 V617F Mutation in Myeloproliferative Neoplasms Szántó
Acta Medica Marisiensis 2014;60(2):44-48 DOI: 10.2478/amma-2014-0010 RESEARCH ARTICLE The Importance of Identification of M-BCR- ABL Oncogene and JAK2 V617F Mutation in Myeloproliferative Neoplasms Szántó
Methylation status of SOCS1 and SOCS3 in BCR-ABL negative and. JAK2V617F negative chronic myeloproliferative disorders.
 Methylation status of SOCS1 and SOCS3 in BCR-ABL negative and JAK2V617F negative chronic myeloproliferative disorders. To the Editor BCR-ABL negative Chronic Myeloproliferative Disorders (s) are a heterogeneous
Methylation status of SOCS1 and SOCS3 in BCR-ABL negative and JAK2V617F negative chronic myeloproliferative disorders. To the Editor BCR-ABL negative Chronic Myeloproliferative Disorders (s) are a heterogeneous
Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards
 Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards incubated in 100 % ethanol overnight at 4 C and embedded in
Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards incubated in 100 % ethanol overnight at 4 C and embedded in
Supplementary Table 3. 3 UTR primer sequences. Primer sequences used to amplify and clone the 3 UTR of each indicated gene are listed.
 Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
c Tuj1(-) apoptotic live 1 DIV 2 DIV 1 DIV 2 DIV Tuj1(+) Tuj1/GFP/DAPI Tuj1 DAPI GFP
 Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Understanding Your Blood Work Results
 Understanding Your Blood Work Results Carlos Besses, MD, hd Hematology Department Hospital del Mar - IMIM, Barcelona Carlos Besses Disclosures Novartis Honorarium Speaker Shire Honorarium Speaker Galena
Understanding Your Blood Work Results Carlos Besses, MD, hd Hematology Department Hospital del Mar - IMIM, Barcelona Carlos Besses Disclosures Novartis Honorarium Speaker Shire Honorarium Speaker Galena
New WHO Classification of Myeloproliferative Neoplasms
 New WHO Classification of Myeloproliferative Neoplasms Hans Michael Kvasnicka Senckenberg Institute of Pathology, University of Frankfurt, Germany hans-michael.kvasnicka@kgu.de Principles and rationale
New WHO Classification of Myeloproliferative Neoplasms Hans Michael Kvasnicka Senckenberg Institute of Pathology, University of Frankfurt, Germany hans-michael.kvasnicka@kgu.de Principles and rationale
Published Ahead of Print on October 13, 2009 as /JCO J Clin Oncol by American Society of Clinical Oncology INTRODUCTION
 Published Ahead of Print on October 13, 9 as 1.1/JCO.9.23. The latest version is at http://jco.ascopubs.org/cgi/doi/1.1/jco.9.23. JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Pegylated Interferon
Published Ahead of Print on October 13, 9 as 1.1/JCO.9.23. The latest version is at http://jco.ascopubs.org/cgi/doi/1.1/jco.9.23. JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Pegylated Interferon
Disclosures. Myeloproliferative Neoplasms: A Case-Based Approach. Objectives. Myeloproliferative Neoplasms. Myeloproliferative Neoplasms
 Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
An elevated hematocrit or platelet count in an otherwise
 The Rate of Progression to Polycythemia Vera or Essential Thrombocythemia in Patients with Erythrocytosis or Thrombocytosis Marco Ruggeri, MD; Alberto Tosetto, MD; Maurizio Frezzato, MD; and Francesco
The Rate of Progression to Polycythemia Vera or Essential Thrombocythemia in Patients with Erythrocytosis or Thrombocytosis Marco Ruggeri, MD; Alberto Tosetto, MD; Maurizio Frezzato, MD; and Francesco
Chronic Idiopathic Myelofibrosis (CIMF)
 Chronic Idiopathic Myelofibrosis (CIMF) CIMF Synonyms Agnogenic myeloid metaplasia Myelosclerosis with myeloid metaplasia Chronic granulocytic-megakaryocytic myelosis CIMF Megakaryocytic proliferation
Chronic Idiopathic Myelofibrosis (CIMF) CIMF Synonyms Agnogenic myeloid metaplasia Myelosclerosis with myeloid metaplasia Chronic granulocytic-megakaryocytic myelosis CIMF Megakaryocytic proliferation
Prognostic models in PV and ET
 Prognostic models in PV and ET Francesco Passamonti Hematology, Varese, Italy Current risk stratification in PV and ET: statement from European LeukemiaNet consensus Age over 60 years Previuos thrombosis
Prognostic models in PV and ET Francesco Passamonti Hematology, Varese, Italy Current risk stratification in PV and ET: statement from European LeukemiaNet consensus Age over 60 years Previuos thrombosis
Masked polycythaemia vera: presenting features, response to treatment and. clinical outcomes. Running title: masked polycythaemia vera.
 Masked polycythaemia vera: presenting features, response to treatment and clinical outcomes Running title: masked polycythaemia vera Alberto Alvarez-Larrán 1, Anna Angona 1, Agueda Ancochea 1, Francesc
Masked polycythaemia vera: presenting features, response to treatment and clinical outcomes Running title: masked polycythaemia vera Alberto Alvarez-Larrán 1, Anna Angona 1, Agueda Ancochea 1, Francesc
School of Pathology and Laboratory Medicine: Current and New Research Interests
 School of Pathology and Laboratory Medicine: Current and New Research Interests W/Professor Wendy Erber Current Research Interests Viral immunology and immunogenetics Bone pathology and cell signalling
School of Pathology and Laboratory Medicine: Current and New Research Interests W/Professor Wendy Erber Current Research Interests Viral immunology and immunogenetics Bone pathology and cell signalling
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Case Workshop of Society for Hematopathology and European Association for Haematopathology
 Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
RESEARCH ARTICLE. Methylated Alteration of SHP1 Complements Mutation of JAK2 Tyrosine Kinase in Patients with Myeloproliferative Neoplasm
 RESEARCH ARTICLE Methylated Alteration of SHP1 Complements Mutation of JAK2 Tyrosine Kinase in Patients with Myeloproliferative Neoplasm Jun-Jun Yang 1&, Hui Chen 1&, Xiao-Qun Zheng 1, Hai-Ying Li 2, Jian-Bo
RESEARCH ARTICLE Methylated Alteration of SHP1 Complements Mutation of JAK2 Tyrosine Kinase in Patients with Myeloproliferative Neoplasm Jun-Jun Yang 1&, Hui Chen 1&, Xiao-Qun Zheng 1, Hai-Ying Li 2, Jian-Bo
Polycythemia Vera and other Myeloproliferative Neoplasms. A.Mousavi
 Polycythemia Vera and other Myeloproliferative Neoplasms A.Mousavi Chronic MPNs Multipotent hematopoietic progenitor cell is origin. Overproduction of one or more formed element of blood cells without
Polycythemia Vera and other Myeloproliferative Neoplasms A.Mousavi Chronic MPNs Multipotent hematopoietic progenitor cell is origin. Overproduction of one or more formed element of blood cells without
A Case Report of Chronic Myelogenous Leukemia With JAK2- and BCR/ABL-Positive Mutation
 A Case Report of Chronic Myelogenous Leukemia With JAK2- and BCR/ABL-Positive Mutation Mamatha Siricilla, MD; Kamyar Nader, MD; and Andres Ferber, MD Abstract Myeloproliferative neoplasms (MPNs) include
A Case Report of Chronic Myelogenous Leukemia With JAK2- and BCR/ABL-Positive Mutation Mamatha Siricilla, MD; Kamyar Nader, MD; and Andres Ferber, MD Abstract Myeloproliferative neoplasms (MPNs) include
Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas. James J. Stark, MD, FACP
 Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS
Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS
Supplemental Data. Shin et al. Plant Cell. (2012) /tpc YFP N
 MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
Welcome to Master Class for Oncologists. Session 3: 9:15 AM - 10:00 AM
 Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
JAK2 V617F Mutation in Patients With Catastrophic Intra-abdominal Thromboses
 Coagulation and Transfusion Medicine / JAK2 V617F IN ABDOMINAL THROMBOSIS JAK2 V617F Mutation in Patients With Catastrophic Intra-abdominal Thromboses Christine McMahon, MD, 1,2 Kareem Abu-Elmagd, MD,
Coagulation and Transfusion Medicine / JAK2 V617F IN ABDOMINAL THROMBOSIS JAK2 V617F Mutation in Patients With Catastrophic Intra-abdominal Thromboses Christine McMahon, MD, 1,2 Kareem Abu-Elmagd, MD,
Baseline clinical characteristics for the 81 CMML patients Routine diagnostic testing and statistical analyses... 3
 Next-Generation Sequencing Technology Reveals a Characteristic Pattern of Molecular Mutations in 72.8% of Chronic Myelomonocytic Leukemia (CMML) by Detecting Frequent Alterations in TET2, CBL, RAS, and
Next-Generation Sequencing Technology Reveals a Characteristic Pattern of Molecular Mutations in 72.8% of Chronic Myelomonocytic Leukemia (CMML) by Detecting Frequent Alterations in TET2, CBL, RAS, and
research paper Summary
 research paper An elevated venous haemoglobin concentration cannot be used as a surrogate marker for absolute erythrocytosis: a study of patients with polycythaemia vera and apparent polycythaemia Peter
research paper An elevated venous haemoglobin concentration cannot be used as a surrogate marker for absolute erythrocytosis: a study of patients with polycythaemia vera and apparent polycythaemia Peter
a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53
 1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
The prognostic relevance of serum lactate dehydrogenase and mild bone marrow reticulin fibrosis in essential thrombocythemia
 Received: 3 February 2017 Revised: 13 February 2017 Accepted: 14 February 2017 DOI: 10.1002/ajh.24689 RESEARCH ARTICLE The prognostic relevance of serum lactate dehydrogenase and mild bone marrow reticulin
Received: 3 February 2017 Revised: 13 February 2017 Accepted: 14 February 2017 DOI: 10.1002/ajh.24689 RESEARCH ARTICLE The prognostic relevance of serum lactate dehydrogenase and mild bone marrow reticulin
CASE REPORT. Abstract. Introduction
 CASE REPORT The Amelioration of Myelofibrosis with Thrombocytopenia by a JAK1/2 Inhibitor, Ruxolitinib, in a Post-polycythemia Vera Myelofibrosis Patient with a JAK2 Exon 12 Mutation Kazuhiko Ikeda 1,2,
CASE REPORT The Amelioration of Myelofibrosis with Thrombocytopenia by a JAK1/2 Inhibitor, Ruxolitinib, in a Post-polycythemia Vera Myelofibrosis Patient with a JAK2 Exon 12 Mutation Kazuhiko Ikeda 1,2,
Supplementary information. Supplementary figure 1. Flow chart of study design
 Supplementary information Supplementary figure 1. Flow chart of study design Supplementary Figure 2. Quantile-quantile plot of stage 1 results QQ plot of the observed -log10 P-values (y axis) versus the
Supplementary information Supplementary figure 1. Flow chart of study design Supplementary Figure 2. Quantile-quantile plot of stage 1 results QQ plot of the observed -log10 P-values (y axis) versus the
Related Policies None
 Medical Policy MP 2.04.60 BCBSA Ref. Policy: 2.04.60 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Medicine Related Policies None DISCLAIMER Our medical policies are designed for informational
Medical Policy MP 2.04.60 BCBSA Ref. Policy: 2.04.60 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Medicine Related Policies None DISCLAIMER Our medical policies are designed for informational
Myelofibrosis a Reference Guide for Journalists
 Myelofibrosis a Reference Guide for Journalists What Is Myelofibrosis? Myelofibrosis is an uncommon blood cancer characterized by bone marrow scarring (fibrosis), enlarged spleen (splenomegaly), potential
Myelofibrosis a Reference Guide for Journalists What Is Myelofibrosis? Myelofibrosis is an uncommon blood cancer characterized by bone marrow scarring (fibrosis), enlarged spleen (splenomegaly), potential
London Cancer. Myelofibrosis guidelines. August Review August Version v1.0. Page 1 of 12
 London Cancer Myelofibrosis guidelines August 2013 Review August 2013 Version v1.0 Page 1 of 12 CONTENTS 1. DIAGNOSIS... 3 1a. BCSH (2012)... 3 1b. WHO (2009) diagnostic criteria for PMF:... 4 2. MOLECULAR
London Cancer Myelofibrosis guidelines August 2013 Review August 2013 Version v1.0 Page 1 of 12 CONTENTS 1. DIAGNOSIS... 3 1a. BCSH (2012)... 3 1b. WHO (2009) diagnostic criteria for PMF:... 4 2. MOLECULAR
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Latest updates in Myeloproliferative Neoplasms. Elizabeth Hexner, MD, MSTR
 Latest updates in Myeloproliferative Neoplasms Elizabeth Hexner, MD, MSTR Disclosures Nothing to disclose Agenda/Goals Treatment goals in PV Indications for cytoreduction in patients polycythemia vera
Latest updates in Myeloproliferative Neoplasms Elizabeth Hexner, MD, MSTR Disclosures Nothing to disclose Agenda/Goals Treatment goals in PV Indications for cytoreduction in patients polycythemia vera
Mayo Clinic Treatment Strategy in Essential Thrombocythemia, Polycythemia Vera and Myelofibrosis 2013 Update
 Mayo Clinic Treatment Strategy in Essential Thrombocythemia, Polycythemia Vera and Myelofibrosis 2013 Update Ayalew Tefferi Mayo Clinic, Rochester, MN 0 20 40 60 80 100 Percent Survival in 337 Mayo Clinic
Mayo Clinic Treatment Strategy in Essential Thrombocythemia, Polycythemia Vera and Myelofibrosis 2013 Update Ayalew Tefferi Mayo Clinic, Rochester, MN 0 20 40 60 80 100 Percent Survival in 337 Mayo Clinic
Molecular aberrations in MPN. and use in the clinic. Timothy Devos MD PhD
 Molecular aberrations in MPN and use in the clinic Timothy Devos MD PhD MB&C2017 24-3-2017 Introduction 1951: William Dameshek MPD MPN = clonal, hematopoietic stem cell disorders, proliferation in BM of
Molecular aberrations in MPN and use in the clinic Timothy Devos MD PhD MB&C2017 24-3-2017 Introduction 1951: William Dameshek MPD MPN = clonal, hematopoietic stem cell disorders, proliferation in BM of
DEMOGRAPHIC FEATURES OF CHRONIC MYELOPROLIFERATIVE NEOPLASMS PRESENTING AT SHAIKH ZAYED MEDICAL COMPLEX, LAHORE
 ORIGINAL ARTICLE DEMOGRAPHIC FEATURES OF CHRONIC MYELOPROLIFERATIVE NEOPLASMS PRESENTING AT SHAIKH ZAYED MEDICAL COMPLEX, LAHORE AMMAR T. AND AZIZ M. Department of Hematology, Shaikh Zayed Hospital, Lahore
ORIGINAL ARTICLE DEMOGRAPHIC FEATURES OF CHRONIC MYELOPROLIFERATIVE NEOPLASMS PRESENTING AT SHAIKH ZAYED MEDICAL COMPLEX, LAHORE AMMAR T. AND AZIZ M. Department of Hematology, Shaikh Zayed Hospital, Lahore
International Journal of Scientific & Engineering Research, Volume 8, Issue 12, December-2017 ISSN
 ISSN 2229-5518 286 Overview of management strategies toward Thrombocythemia Mayada Amin Aljudaibi, Reem Ali Mohammed Alamoodi, Abrar Ali Mohammed Alamoodi, Samar Mohammed Hasan Al_Hashemi, Bashayer Sadagah
ISSN 2229-5518 286 Overview of management strategies toward Thrombocythemia Mayada Amin Aljudaibi, Reem Ali Mohammed Alamoodi, Abrar Ali Mohammed Alamoodi, Samar Mohammed Hasan Al_Hashemi, Bashayer Sadagah
Frequent reduction or absence of detection of the JAK2-mutated clone in JAK2V617F-positive patients within the first years of hydroxyurea therapy
 Frequent reduction or absence of detection of the JAK2-mutated clone in JAK2V617F-positive patients within the first years of hydroxyurea therapy François Girodon, 1,2 Céline Schaeffer, 1 Cédric Cleyrat,
Frequent reduction or absence of detection of the JAK2-mutated clone in JAK2V617F-positive patients within the first years of hydroxyurea therapy François Girodon, 1,2 Céline Schaeffer, 1 Cédric Cleyrat,
Rischio emorragico e trombotico nella TE e PV
 Convegno Interregionale SIE Delegazione Triveneto Approfondimento sulle sindromi mielodisplastiche e mieloproliferative Sessione: Sindromi Mieloproliferative Croniche Rischio emorragico e trombotico nella
Convegno Interregionale SIE Delegazione Triveneto Approfondimento sulle sindromi mielodisplastiche e mieloproliferative Sessione: Sindromi Mieloproliferative Croniche Rischio emorragico e trombotico nella
"Calreticulin Mutation Analysis in Iranian patients suffering from Essential thrombocythemia and Primary Myelofibrosis
 "Calreticulin Mutation Analysis in Iranian patients suffering from Essential thrombocythemia and Primary Myelofibrosis Dr Behzad Poopak, DCLS PhD. Associate professor of fhematology Islamic Azad University
"Calreticulin Mutation Analysis in Iranian patients suffering from Essential thrombocythemia and Primary Myelofibrosis Dr Behzad Poopak, DCLS PhD. Associate professor of fhematology Islamic Azad University
Supplementary Materials
 Supplementary Materials 1 Supplementary Table 1. List of primers used for quantitative PCR analysis. Gene name Gene symbol Accession IDs Sequence range Product Primer sequences size (bp) β-actin Actb gi
Supplementary Materials 1 Supplementary Table 1. List of primers used for quantitative PCR analysis. Gene name Gene symbol Accession IDs Sequence range Product Primer sequences size (bp) β-actin Actb gi
Disclosures for Ayalew Tefferi
 Disclosures for Ayalew Tefferi Principal investigator role Employee Consultant Major Stockholder Speakers Bureau Scientific Advisory Board Janssen, Geron, Celgene, Sanofi-Aventis, Gilead Sciences, Incyte
Disclosures for Ayalew Tefferi Principal investigator role Employee Consultant Major Stockholder Speakers Bureau Scientific Advisory Board Janssen, Geron, Celgene, Sanofi-Aventis, Gilead Sciences, Incyte
Calreticulin Exon 9 Mutations in Myeloproliferative Neoplasms
 Original Article Diagnostic Hematology Ann Lab Med 2015;35:22-27 http://dx.doi.org/10.3343/alm.2015.35.1.22 ISSN 2234-3806 eissn 2234-3814 Calreticulin Exon 9 Mutations in Myeloproliferative Neoplasms
Original Article Diagnostic Hematology Ann Lab Med 2015;35:22-27 http://dx.doi.org/10.3343/alm.2015.35.1.22 ISSN 2234-3806 eissn 2234-3814 Calreticulin Exon 9 Mutations in Myeloproliferative Neoplasms
