immunotherapy What you need to know about... LUNG CANCER TREATMENTS
|
|
|
- Iris Sullivan
- 5 years ago
- Views:
Transcription
1 LUNG CANCER TREATMENTS UPDATED MAY 2018 What you need to know about... immunotherapy Copyright 2018 LUNGevity Foundation All rights reserved. No part of this publication may be reproduced, distributed, or transmitted in any form or by any means without prior written permission.
2 foreword About LUNGevity LUNGevity is the largest national lung cancer-focused nonprofit, changing outcomes for people with lung cancer through research, education, and support. About the LUNGevity PATIENT EDUCATION SERIES LUNGevity has developed a comprehensive series of materials for patients/survivors and their caregivers, focused on understanding how lung cancer develops, how it can be diagnosed, and treatment options. Whether you have recently been diagnosed with lung cancer, someone you care about has been diagnosed, or you are concerned about your lung cancer risk, we have resources to help you. The medical experts and lung cancer survivors who provided their valuable expertise and experience in developing these materials all share the belief that well-informed patients make their own best advocates. In addition to this and other booklets in the LUNGevity patient education series, information and resources can be found on LUNGevity s website, under For Patients & Supporters and For Supporters & Advocates. This patient education booklet was produced through charitable donations from:
3 table of contents 01 Immune System...5 What is the immune system?... 5 How does the immune system work?... 7 What is the role of the immune system in cancer?... 8 Innate immune response... 8 Adaptive immune response... 9 How do cancer cells grow despite the innate and adaptive immune responses? Immunotherapy...12 What is immunotherapy?...12 Immune checkpoint inhibitors...13 Therapeutic cancer vaccines...21 Adoptive T cell transfer...26 Questions to ask your healthcare team about immunotherapy as a treatment option What clinical trial options are available?...31 Questions to ask your healthcare team if you are considering participating in an immunotherapy clinical trial...32 Resources to help you navigate your clinical trials search Glossary Notes... 42
4 introduction Immunotherapy is a type of biological therapy that harnesses and increases the natural ability of the patient s immune system to fight cancer. Instead of trying to stop or kill the person s cancer cells directly, as most cancer treatments do, immunotherapy trains the person s own natural immune system to recognize cancer cells and selectively target and kill them. This booklet will help you: Learn how the immune system works Understand how immunotherapy may boost the immune system to help fight lung cancer Find out what immunotherapy options are available now Understand whether immunotherapy might be a good treatment option for you YOU LL FIND A GLOSSARY TOWARD THE END OF THIS BOOKLET. Words included in the glossary appear blue the first time that they are used in the text. introduction LUNGEVITY FOUNDATION 4
5 01 immune system What is the immune system? The immune system is a network of cells, tissues, and organs that work together to protect the body from foreign invaders, such as bacteria or viruses. Key players in defending the body include a specific type of white blood cell (WBC) called lymphocytes. There are three major types of lymphocytes: Natural killer (NK) cells B cells T cells Lymphocytes grow and develop in the bone marrow, thymus, and spleen. They can also be found in clumps throughout the body, primarily as lymph nodes. Lymph nodes in the neck are called cervical lymph nodes, and those between the lungs in the middle of the chest are known as mediastinal lymph nodes. Clumps of 01 immune system LUNGEVITY FOUNDATION 5
6 lymphoid tissue are also found in the appendix, tonsils, and adenoids. Lymphocytes circulate through the body between the organs and nodes via lymphatic vessels and blood vessels. In this way, the immune system works in a coordinated way to monitor the body for germs and other abnormal cells. ORGANS OF THE IMMUNE SYSTEM Adenoids Lymph nodes Tonsils Thymus Spleen Appendix Bone marrow 01 immune system LUNGEVITY FOUNDATION 6
7 How does the immune system work? A key feature of the immune system is its ability to tell the difference between the body s own normal cells, or self, and cells and other substances that are foreign to the body, or non-self. Every cell in the body carries a set of distinctive proteins on its surface. These identifying surface proteins let the immune system know that they are cells that belong to the body. Healthy cells display normal proteins on their surface. The immune system has learned to ignore normal proteins. However, there are people with autoimmune disorders in which the immune system inappropriately tries to eliminate healthy cells. If the surface proteins are abnormal, such as when a virus infects cells, or when cells become cancerous, they can be recognized by the immune system. Proteins recognized by the immune system are called antigens. If a foreign substance such as a bacteria, virus, or tumor cell is recognized, the immune system kicks in to try to deal with it. It is the non-self antigens on the surface of these cells that the immune system identifies as abnormal. The immune system is great at recognizing bacteria and virus cells, because they look very different from healthy cells. On the other hand, tumor cells started as healthy cells and can look a lot like healthy cells. As a result, the body may have a harder time recognizing tumor cells as foreign. In other instances, the immune system may recognize a tumor antigen but may be unable to mount a response strong enough to destroy the tumor. As cancers grow, they can evolve ways to escape from attack by the immune system. For these reasons, many people with healthy immune systems still develop cancer and cancer still progresses. In many people with cancer, the cancer cells co-exist with immune cells capable of killing the cancer, but the cancer cells hold the immune cells back from working the way they should. 01 immune system LUNGEVITY FOUNDATION 7
8 What is the role of the immune system in cancer? The immune system has two responses that work together to detect and destroy cancer cells: Innate immune response Adaptive immune response Innate immune response Natural killer (NK) cells The innate immune response is the first line of defense. The innate immune system s normal function is to protect the body from initial invasion by bacteria and viruses, such as when bacteria invade broken skin or viruses land in the throat. The system includes natural killer (NK) cells, a type of lymphocyte that patrols the body and is on constant alert, looking for foreign invaders and abnormal cells. If cells from the innate immune system recognize a cancer cell as abnormal, they can attach to it and immediately release toxic chemicals that kill it. NK cells and other cells of the innate immune system do not need to recognize a specific abnormality on a cell to be able to do their job. NK CELL RELEASING TOXINS TO CANCER CELL NK cell Cancer cell NK cell releases toxins Cancer cell dies If bacteria, viruses, or cancer cells evade the innate response, then the adaptive immune response becomes active. 01 immune system LUNGEVITY FOUNDATION 8
9 Adaptive immune response The adaptive immune response recognizes specific abnormalities on cancer cells that make them different from the cells that are naturally found in the body. Though it is more effective than the innate immune response, the adaptive immune response takes longer to become activated. The cells of the adaptive immune response include the other two types of lymphocytes: B cells and T cells. B cells B cells are like the body s military intelligence system, seeking out their targets and sending defenses to lock onto them. They react to non-self antigens by making proteins called antibodies. Antibodies are proteins that can attach to foreign and abnormal cells and let the body know that they are dangerous. Antibodies can kill cancer cells in several ways, including binding natural killer cells to the cancer. B cells also create memory they start to make antibodies quickly when they recognize a past antigen. B CELL RELEASING ANTIBODY B cell NK cell Antibody Antigen Cancer cell B cell releases antibody Antibody binds to antigen on cancer cell NK cell binds to antibody on cancer cell 01 immune system LUNGEVITY FOUNDATION 9
10 T cells T cells are the major cells the body uses to recognize and destroy abnormal cells. Once a foreign antigen or abnormal cancer protein has been recognized by T cells, the T cells rapidly increase in number. An army of T cells can be formed; these T cells are specifically designed to attack and kill cells that have foreign antigens. The T cells are like soldiers, destroying the invaders. They are responsible for coordinating the entire immune response and destroying infected cells and cancer cells. T CELL ATTACKING CANCER CELL T cell Receptor Cancer cell Antigen T cell binds to cancer cell Cancer cell dies T cells also develop memory after an initial response to an antigen. This memory is meant to ensure that the attack on cancer cells can persist long-term, for months or longer. The memory also allows for future responses against the specific abnormal antigen on cancer cells, if and when the cancer comes back. 01 immune system LUNGEVITY FOUNDATION 10
11 How do cancer cells grow despite the innate and adaptive immune responses? If the immune system recognizes the lung tumor cells and can destroy them, why are lung tumors able to grow? Research has shown that tumors enable their own growth by turning off the immune response An immune response beyond what is normal or necessary can be toxic, so T cells have many normal methods to dampen themselves down and essentially turn themselves off. This may allow the growth and development of tumor cells despite the presence of T cells with the potential to kill cancer cells Scientists are working hard to understand exactly how this happens and how to best turn the T cells back on. 01 immune system LUNGEVITY FOUNDATION 11
12 02 immunotherapy Immunotherapy is a type of biological therapy. It aims to enhance the body s immune response and stop lung cancers from escaping from the immune system. Biological therapies use substances made from living organisms to treat disease. What is immunotherapy? Immunotherapy is a treatment that strengthens the natural ability of the patient s immune system to fight cancer. Instead of targeting the person s cancer cells directly, immunotherapy causes a person s natural immune system to selectively target and kill cancer cells. Immunotherapies do this in one of two ways: By enabling the immune system to mount or maintain a response By suppressing factors that prevent the immune response 02 immunotherapy LUNGEVITY FOUNDATION 12
13 There are many different types of immunotherapy. Three main types are currently being studied in people with non-small cell lung cancer (NSCLC): Immune checkpoint inhibitors Therapeutic cancer vaccines Adoptive T cell transfer Immune checkpoint inhibitors have made the most progress at this time, and the first U.S. Food and Drug Administration (FDA)-approved immunotherapy drugs for lung cancer belong to this group. Immunotherapy is also being studied in small cell lung cancer (SCLC). Immune checkpoint inhibitors Many lung cancers co-exist with T cells capable of killing the cancer cells. However, the immune system has many normal mechanisms for dampening itself down. The immune system has fail-safe mechanisms that are designed to suppress the immune response at appropriate times to minimize damage to healthy tissue. These mechanisms are called immune checkpoint pathways. They are essentially the brakes on the system that can prevent T cells from killing lung cancer cells. The challenge is that cancers are able to use these immune checkpoint pathways to lessen the immune response at the wrong times. This may allow cancer cells to thrive. How do immune checkpoint inhibitors work? Immune checkpoint inhibitors work by targeting and blocking the fail-safe mechanisms of the immune system. Their goal is to block the immune system from limiting itself, so that the original anti-cancer response works better. 02 immunotherapy LUNGEVITY FOUNDATION 13
14 What immune checkpoint inhibitors are currently available? There are currently four FDA-approved immune checkpoint inhibitors for treating patients with lung cancer. Three of them, nivolumab (Opdivo ), pembrolizumab (Keytruda ), and atezolizumab (Tecentriq ), treat patients whose NSCLC has already progressed to metastatic disease. One of them, durvalumab (Imfinzi ), treats patients at an earlier stage in order to reduce the risk of the lung cancer progressing. Durvalumab (Imfinzi ): Approved for patients with stage III NSCLC whose tumors are not able to be surgically removed and whose cancer has not progressed after treatment with concurrent platinum-based chemotherapy and radiation therapy (sometimes referred to as chemo-radiation or CRT). Nivolumab (Opdivo ): Approved for patients with metastatic NSCLC whose lung cancer has progressed on or after platinumbased chemotherapy. Patients with epidermal growth factor receptor (EGFR) or anaplastic lymphoma kinase (ALK) mutations should have disease progression on FDA-approved therapy for these mutations before receiving this drug. Note: Platinum-based chemotherapies include carboplatin and cisplatin. 02 immunotherapy LUNGEVITY FOUNDATION 14
15 Pembrolizumab (Keytruda ): Approved for patients with metastatic NSCLC in the following situations: As first-line treatment for patients whose tumors have a high (greater than or equal to 50%) Programmed Death Ligand 1 (PD-L1) expression Tumor Proportion Score (TPS), as determined by an FDA-approved test, with no EGFR or ALK mutation. Approximately 30% of patients with newly diagnosed metastatic NSCLC will have tumors with this high level of PD-L1 expression. (The TPS is the percentage of cancer cells that produce the PD-L1 proteins. The lung cancer tissue is stained with special dyes that mark PD-L1-positive tumor cells. A pathologist counts the number of cells that stain positive and determines the TPS.) For patients whose tumor expresses PD-L1 (TPS greater than or equal to 1%), as determined by an FDA-approved test, with disease progression on or after platinum-containing chemotherapy. Patients with EGFR or ALK mutations should have disease progression on FDA-approved therapy for these mutations before receiving this drug. As first-line treatment for patients with metastatic non-squamous NSCLC in combination with the chemotherapy drugs pemetrexed and carboplatin, irrespective of PD-L1 expression. Atezolizumab (Tecentriq ): Approved for patients with metastatic NSCLC whose lung cancer has progressed during or after being treated with platinum-containing chemotherapy. Patients with EGFR or ALK mutations should have disease progression on FDAapproved therapy for these mutations before receiving this drug. Patients with pre-existing autoimmune disorders should discuss them with their doctors. Those who go on an immune checkpoint inhibitor should be monitored very carefully for autoimmune side effects. 02 immunotherapy LUNGEVITY FOUNDATION 15
16 How are immune checkpoint inhibitors administered? FDA-approved immune checkpoint inhibitors are given intravenously. Infusion time and schedules vary, depending on the drug. Immune checkpoint inhibitors are given until disease progression or serious side effects occur. Durvalumab (Imfinzi ) is given intravenously over 60 minutes every 2 weeks for no more than 12 months Nivolumab (Opdivo ) is given intravenously over 30 minutes every 2 weeks or every 4 weeks Pembrolizumab (Keytruda ) is given intravenously over 30 minutes every 3 weeks Atezolizumab (Tecentriq ) is given intravenously over 60 minutes every 3 weeks How well do immune checkpoint inhibitors work? In clinical trials to date with NSCLC patients, approximately 20% have responded to immune checkpoint inhibitors. This includes patients who tested negative for Programmed Death 1/Programmed Death Ligand 1 (PD-1/PD-L1), as well as those who tested positive. The response may continue after treatment is stopped. Some of the responses to date have been long-term. There are many reasons to think that the results will improve as scientists learn how best to use these drugs. Scientists are looking for ways to increase the number of people who respond to this treatment. In clinical trials, they are combining treatments, boosting the immune system, and using other strategies. Note: Patients whose tumors have high levels of PD-L1 expression are more likely to respond to PD-1/PD-L1 therapies. However, even those with tumors that do not express PD-L1 may respond to these treatments. 02 immunotherapy LUNGEVITY FOUNDATION 16
17 How long does it take to see results from therapy with immune checkpoint inhibitors? Of the approximately 20% of patients in clinical trials with immune checkpoint inhibitors who have responded, most respond within the first couple of months. In a small subset of patients (1% 3%), the tumor on a CT scan may seem to get worse at first and then get better, or there may be new areas of tumor. Scientists have coined the term pseudoprogression to describe this situation. One theory of why this happens is that, as the lymphocytes come in to attack a tumor, the tumor gets larger, and then, as they kill cancer cells, the tumor gets smaller again. The current scientific thinking is that the tumors get larger because a large number of the patient s T cells move into the tumor to clean it up. Therefore, some tumors that look larger on scans are larger because the immune system is attacking the cancer, not because the cancer cells are growing. For the great majority of patients whose scans show worsening of disease after at least a couple of months on immunotherapy, the scans are accurately showing that the immunotherapy is not working. 02 immunotherapy LUNGEVITY FOUNDATION 17
18 In cases where the scan looks worse, the best course of action will likely be based on a number of factors: If the patient s scan looks worse, but he or she is feeling fine The doctor and patient may decide together to do another course of immunotherapy If the patient s scan looks worse and he or she is not feeling fine It may not make sense to continue with this type of therapy. In this case, the patient likely needs another kind of therapy to control the symptoms What are the side effects of immune checkpoint inhibitors? The most common side effects reported from immune checkpoint inhibitors as a group include: Nausea Fatigue Rash Musculoskeletal pain Cough Difficulty breathing Constipation Decreased appetite An immune checkpoint inhibitor side effect seen sometimes is pneumonitis, which is inflammation of the lung tissue that may lead to difficulty breathing if not treated early and correctly. 02 immunotherapy LUNGEVITY FOUNDATION 18
19 Pneumonitis and some of the other side effects seen with immune checkpoint inhibitors are related to turning on the immune system, which then may also attack some healthy cells and cause inflammation. Other examples of this include: Arthritis Colitis Hepatitis Inflammation of the endocrine glands, like the thyroid Nephritis and renal dysfunction Inflammation of the thyroid can cause either high or low thyroid hormone levels (hyperthyroidism or hypothyroidism, respectively). Inflammation of the liver can also occur, so liver function tests may be run periodically to check for that. Inflammation-related symptoms are usually easy to manage, but sometimes patients may need to take additional medications, including corticosteroids or thyroid hormone replacement. Note: It s important to let your doctor(s) know if you are experiencing any problems while on treatment, so they can sort out if the side effects are related to the treatment. It is especially important to be very clear with your doctor about the side effects that you are experiencing, because this may impact future treatment plans. Some patients experience side effects that are severe enough that they need to stop taking the immunotherapy treatment. In general, based on what has been seen with patients in clinical trials to date, these kinds of treatments are well tolerated by most patients. Because these drugs have only been studied in patients for a few years, we do not know for certain what the long-term side effects are in patients with profound responses, including remission of cancer. 02 immunotherapy LUNGEVITY FOUNDATION 19
20 However, doctors have some ideas about what they may be: One potential long-term side effect of immunotherapy may be that, if it affects the endocrine gland, a patient may need thyroid hormone supplementation for the rest of his or her life Some patients develop diabetes and need to be on medication Note: It s important to tell your doctor(s) if you were ever treated with immunotherapy, even a long time ago, because side effects can show up after long periods of time. RESOURCES FOR MANAGING TREATMENT SIDE EFFECTS: LUNGevity Survivor Resource Center survivor-resource-center Where do immune checkpoint inhibitors fit into the treatment plan for lung cancer? Durvalumab (Imfinzi ) is currently FDA-approved for patients with stage III NSCLC. The other three FDA-approved drugs in this class, nivolumab (Opdivo ), pembrolizumab (Keytruda ), and atezolizumab (Tecentriq ), are currently approved as second-line treatment or therapy for patients with metastatic NSCLC who have been or are being treated with platinum-based chemotherapy. In addition, pembrolizumab (Keytruda ) may be used for first-line treatment under certain circumstances. 02 immunotherapy LUNGEVITY FOUNDATION 20
21 Numerous immune checkpoint inhibitor drugs are being tested in clinical trials for lung cancer, including: IMMUNE CHECKPOINT INHIBITORS BEING TESTED Generic Name Brand Name Types of lung cancer being tested Ipilimumab Yervoy NSCLC, SCLC Durvalumab Imfinzi NSCLC, SCLC Avelumab Bavencio NSCLC Tremelimumab To be determined NSCLC PDR001 To be determined NSCLC REGN2810 To be determined NSCLC Immune checkpoint inhibitors are being used alone and in combination with other therapies in clinical trials, including: Chemotherapy Other checkpoint antibodies Targeted therapy Other immunotherapies Radiation therapy Therapies that block blood vessel formation Therapeutic cancer vaccines When most people think of a vaccine, they think of a traditional vaccine given to prevent an infectious disease, such as measles or polio. In addition to traditional vaccines, there are two types of cancer vaccines: A preventive cancer vaccine is given to prevent cancer from developing in healthy people. For example, the hepatitis B vaccine is given to children to protect against a hepatitis B viral infection, which can lead to liver cancer. 02 immunotherapy LUNGEVITY FOUNDATION 21
22 A therapeutic cancer vaccine, in contrast, is given to treat an existing cancer by causing a stronger and faster response from the immune system. Most commonly, this type of vaccine is used in patients in remission in an attempt to prevent likely relapse, or the cancer from returning. Where do therapeutic cancer vaccines fit in a lung cancer treatment plan? While there are yet no FDA-approved therapeutic cancer vaccines for lung cancer, therapeutic cancer vaccines are being studied in clinical trials for both SCLC and NSCLC. A number of different therapeutic vaccines are being studied: THERAPEUTIC CANCER VACCINES BEING STUDIED FOR LUNG CANCER Generic Name Brand Name Types of lung cancer being studied Tergenpumatucel-L HyperAcute NSCLC BI To be determined NSCLC CIMAvax-EGF To be determined NSCLC GV1001 To be determined NSCLC TG4010 To be determined NSCLC BEC2 To be determined NSCLC INGN To be determined SCLC 02 immunotherapy LUNGEVITY FOUNDATION 22
23 How do therapeutic cancer vaccines work? A therapeutic cancer vaccine is made from a patient s own tumor cells or from substances taken from the tumor cells. They are designed to work by activating the cells of the immune system to recognize and act against the specific antigen on the tumor cell. Because the immune system has special cells for memory, the hope is that the vaccines will also help keep the lung cancer from coming back. Note: There are several ways to receive therapeutic cancer vaccines. The figure below describes one method of receiving therapeutic cancer vaccines. THERAPEUTIC CANCER VACCINE Cancer cells are removed from patient Irradiation of cancer cells Cancer cell DNA Modified gene Enhanced immune response Patient receives modified cancer cells Genetic modification of cancer cells 02 immunotherapy LUNGEVITY FOUNDATION 23
24 How is a therapeutic cancer vaccine administered? Therapeutic cancer vaccines are given as an injection either: Right below the skin s top layer (intradermally) Beneath the skin (subcutaneously) Into the muscle (intramuscularly) TYPES OF INJECTIONS Skin Subcutaneous tissue Muscle Intradermal Subcutaneous Intramuscular Results of therapeutic cancer vaccine administration Several studies have suggested that therapeutic cancer vaccines may be most effective when given in combination with other forms of cancer therapy. In addition, they may even increase the effectiveness of the other treatments. There is also some evidence indicating that surgical removal of the tumor before administration of a cancer vaccine may make it easier for the immune system to develop an effective response. 02 immunotherapy LUNGEVITY FOUNDATION 24
25 What side effects of therapeutic cancer vaccines have been seen in clinical trials? The most common side effect of therapeutic cancer vaccines is inflammation at the site of the injection, including: Redness Pain Swelling Warming of the skin Itchiness Rash (occasional) Flu-like symptoms have also been reported after administration of a therapeutic cancer vaccine, including: Fever Muscle ache Chills Fatigue Weakness Headache Dizziness Occasional breathing difficulties Nausea or vomiting More serious health problems have been reported in a smaller number of people after receiving a therapeutic cancer vaccine, but these may not have been caused by the vaccine. Rarely, severe allergic reactions to specific vaccine ingredients have been seen following vaccination. 02 immunotherapy LUNGEVITY FOUNDATION 25
26 Adoptive T cell transfer Adoptive T cell transfer is being developed as a new approach to cancer treatment. The goal is to improve the ability of a person s own T cells to fight cancer. A sample of T cells is removed from the patient and then genetically changed in order to make the T cells more active against specific cancer cells. Scientists can change what is on the surface of the T cells. For example, they can add a receptor to the surface of the T cell that will target a specific antigen on a cancer cell. The receptors work like very specific Velcro that allows T cells to stick to cancer cells and kill the cells. The T cells are then returned to the patient, and the altered T cells quickly home in on their targets. ADOPTIVE T CELL TRANSFER T cells are removed from patient T cell DNA Modified gene Enhanced immune response Patient receives modified T cells Genetic modification of T cells 02 immunotherapy LUNGEVITY FOUNDATION 26
27 Where does adoptive T cell transfer fit into the treatment plan for lung cancer? Currently, there are no FDA-approved T cell transfer-based therapies for lung cancer. Adoptive T cell transfer is being studied in clinical trials. How does adoptive T cell transfer work? Typically, during an immune response, T cells multiply. After the initial response, most of the newly made T cells are eliminated. This keeps the total T cell number in the body at a normal level. The normal level of T cells is usually not high enough to sustain a response strong enough to effectively fight cancer. However, there is evidence that T cells have the ability to multiply in abundance when given to someone whose immune system has been weakened. Therefore, in an adoptive T cell transfer, patients are given chemotherapy prior to the adoptive T cell transfer in order to suppress their immune system. Once the chemotherapy is completed and the immune system is weakened, billions of modified T cells are then reintroduced into the patient. The goal of the T cell transfer is to enable the immune system to attack the tumors in a large number that is otherwise impossible and in a way that it is incapable of doing on its own. 02 immunotherapy LUNGEVITY FOUNDATION 27
28 How is adoptive T cell transfer administered? How are T cells removed from a patient? The three ways of performing adoptive T cell transfer include: Taking T cells from the bloodstream and putting special receptors, called chimeric antigen receptors (CARs), on them. CARs recognize specific proteins found on the surface of cancer cells. The CAR T cells then bind to the cancer cells that have those proteins and destroy them Collecting a sample from the tumor and multiplying the T cells in a laboratory Taking T cells from the bloodstream, through a procedure called leukapheresis, and genetically altering them to attack cancer cells that have specific antigens How are T cells returned to the patient? After the T cells are removed from a patient by any of these ways, the T cells are returned to the patient through an infusion. Results of clinical trials involving adoptive T cell transfer Clinical trials with very strong patient responses, including lasting responses, have led to FDA approval of two CAR T cell therapies: one for a type of lymphoma and the other for a type of leukemia. Whether T cell therapies will eventually prove to be effective in lung cancer is unknown. 02 immunotherapy LUNGEVITY FOUNDATION 28
29 What side effects have been seen in clinical trials involving adoptive T cell transfer? Among the most common side effects of adoptive T cell transfer is the serious cytokine-release syndrome. This is a rapid and large-scale release of cytokines into the bloodstream. Cytokines are chemical messengers that help the T cells carry out their duties. Too many cytokines can lead to dangerously high fevers and quick drops in blood pressure. In many patients, this side effect can be managed with standard supportive treatments, including steroids. Other serious side effects include neurotoxicity changes in the brain caused by the treatment that can result in a headache, seizures, confusion, infection, low blood cell counts, and a weakened immune system. 02 immunotherapy LUNGEVITY FOUNDATION 29
30 QUESTIONS TO ASK YOUR HEALTHCARE TEAM ABOUT IMMUNOTHERAPY AS A TREATMENT OPTION: Why do you recommend immunotherapy for me? Will immunotherapy be my only treatment or will it be combined with another treatment? Where do I go to get my immunotherapy? How will it be administered? How often will I get my treatment? How long will it last? How often do I need to be seen in-between treatments for a physical exam and/or lab work? What side effects can I expect? How will this treatment affect my daily life? Will I be able to work, exercise, and perform my usual activities? Are there any tests or procedures I will need to undergo during the treatment? When will you know whether or not the immunotherapy worked? What tests will I need after treatment is completed? Are there any long-term health issues I should expect from treatment with immunotherapy? How much will my treatment cost? 02 immunotherapy LUNGEVITY FOUNDATION 30
31 What clinical trial options are available? Clinical trials are ongoing in lung cancer patients to add to the understanding of these different types of immunotherapy. There have been clear advances in immunotherapy over the last decade, and these advances are based on information learned from patients who were enrolled in clinical trials. If you are considering whether to participate in a clinical trial, start by asking your doctor whether there is one for which you might qualify in your area. There are several other questions that you should consider asking your healthcare team about participating in a clinical trial. 02 immunotherapy LUNGEVITY FOUNDATION 31
32 QUESTIONS TO ASK YOUR HEALTHCARE TEAM IF YOU ARE CONSIDERING PARTICIPATING IN AN IMMUNOTHERAPY CLINICAL TRIAL: About your treatment history: What type(s) of treatment(s) for lung cancer have I had so far? What line of therapy am I looking for? If you have never been treated before, you are looking for a first-line clinical trial If you have had a prior chemotherapy for metastatic disease, you may be looking for a second-line clinical trial If you have had multiple lines of therapy, you want a clinical trial that allows for several previous treatments About immunotherapy clinical trials: What are the benefits and risks of participating in an immunotherapy clinical trial? How will I be monitored while participating in a clinical trial? What are my responsibilities during the clinical trial? Are there any costs associated with my participation in a clinical trial? Where can I learn more about clinical trials? Who can I talk to if I have questions during the clinical trial? What happens if I decide I do not want to participate in the clinical trial at some point? 02 immunotherapy LUNGEVITY FOUNDATION 32
33 In addition, below are several resources to help you find a clinical trial that may be a good match for you. RESOURCES TO HELP YOU NAVIGATE YOUR CLINICAL TRIALS SEARCH: LUNGevity Clinical Trial Finder: LUNGevity.org/index.html The LUNGevity Clinical Trial Finder helps you connect with lung cancer trials The screening process locates nearby clinical trials as well as provides information and links to centers performing these studies EmergingMed: networks/lungevity LUNGevity partners with this clinical trials matching service to help you with the decision of whether to participate in a clinical trial EmergingMed helps you identify lung cancer clinical trials for which you may be eligible Clinical trial navigators are available Monday through Friday from 9:00am to 5:00pm ET at U.S. National Institutes of Health: National Cancer Institute (NCI): Coalition of Cancer Cooperative Groups: 02 immunotherapy LUNGEVITY FOUNDATION 33
34 03 glossary Adaptive immune response Specific response of the immune system; creates T cells to respond to a specific antigen on a cancer cell Adenoids A mass of lymphatic tissue located where the nose blends into the throat Adoptive T cell therapy Therapy that involves removing some of a patient s own immune system cells often altering and increasing their ability to recognize and kill cancer cells growing billions of them in the laboratory, and infusing the cultured cells into the patient. The idea is to provide an invading force of immune cells that can attack tumors at a level that the immune system is not capable of doing on its own Anaplastic lymphoma kinase (ALK) A gene that the body normally produces but, when fused with another gene, produces an abnormal protein that leads to cancer cell growth Antibody A protein made by B cells in response to an antigen. Each antibody can bind to only one specific antigen. The purpose of this binding is to help destroy the antigen. Some antibodies destroy antigens directly. Others make it easier for white blood cells (WBCs) to destroy the antigen 03 glossary LUNGEVITY FOUNDATION 34
35 Antigen A protein on the surface of a cell that causes the body to make a specific immune response Arthritis A disease that causes inflammation and pain in the joints Autoimmune disorder A condition in which the body recognizes its own tissues as foreign and directs an immune response against them B cell A type of white blood cell (WBC) that circulates in the blood and lymph, seeking out foreign invaders. Upon meeting a non-self antigen, it makes proteins called antibodies, which detect and destroy the antigens. Also called B lymphocyte Bacteria A large group of single-cell microorganisms. Some cause infections and disease in animals and humans Biological therapy A type of treatment that uses substances made from living organisms to treat disease. These substances may occur naturally in the body or may be made in the laboratory. Some biological therapies stimulate or suppress the immune system to help the body fight cancer, infection, and other diseases. Other biological therapies attack specific cancer cells, which may help keep them from growing or kill them Bone marrow The soft, sponge-like tissue in the center of most bones. It produces white blood cells (WBCs), red blood cells, and platelets Cervical lymph nodes Lymph nodes found in the neck Chemotherapy Treatment with drugs that kill cancer cells Clinical trial A type of research study that tests how well new medical approaches work in people. These studies test new methods of screening, prevention, diagnosis, or treatment of a disease. Also called clinical research trial or study 03 glossary LUNGEVITY FOUNDATION 35
36 Colitis An illness that causes pain and swelling in the colon CT scan A procedure that uses a computer linked to an X-ray machine to make a series of detailed pictures of areas inside the body. The pictures are taken from different angles and are used to create 3-dimensional (3-D) views of tissues and organs. A dye may be injected into a vein or swallowed to help the tissues and organs show up more clearly. Also called computed tomography (CAT) scan Cytokine A type of protein that is made by certain immune and non-immune cells and has an effect on the immune system. Some cytokines stimulate the immune system, while others slow it down Disease progression Cancer that continues to grow or spread Endocrine gland A gland (for example, the thyroid or the pituitary) that produces an endocrine secretion Epidermal growth factor receptor (EGFR) The protein found on the surface of some cells and to which epidermal growth factor (a protein made by many cells in the body and by some types of tumors. It causes cells to grow and differentiate) binds, causing the cells to divide. It is found at abnormally high levels on the surface of many types of cancer cells, so these cells may divide excessively in the presence of epidermal growth factor First-line clinical trial A clinical trial for a patient who has never been treated before First-line treatment The first therapy given for a disease. It is often part of a standard set of treatments, such as surgery followed by chemotherapy and radiation. When used by itself, first-line treatment is the one accepted as the best treatment. If it doesn t cure the disease, or it causes severe side effects, other treatments may be added or used instead 03 glossary LUNGEVITY FOUNDATION 36
37 Foreign In medicine, this term describes something that comes from outside the body. A foreign substance in the body s tissues, such as a bacterium or virus, may be recognized by the immune system as not belonging to the body. This causes an immune response. Other foreign substances in the body, such as artificial joints, are designed to not cause an immune response Hepatitis Disease of the liver causing inflammation Immune checkpoint inhibitors Agents that target the pathways that tumor cells use to evade recognition and destruction by the immune system Immune response The activity of the immune system against foreign substances (antigens) Immune system A complex network of cells, tissues, organs, and the substances they make that help the body fight infections and other diseases. The immune system includes white blood cells (WBCs) and organs and tissues of the lymph system, such as the thymus, spleen, tonsils, lymph nodes, lymph vessels, and bone marrow Immunotherapy A type of cancer therapy that uses substances to stimulate or suppress the immune system to help the body fight cancer, infection, and other diseases. Some types of immunotherapy only target certain cells of the immune system. Others affect the immune system in a general way Infusion A method of putting fluids, including drugs, into the bloodstream. Also called intravenous infusion Innate immune response Immune response to a pathogen that involves the pre-existing defenses of the body; such a response is not specific to a pathogen Intradermal Within the skin. Also called intracutaneous 03 glossary LUNGEVITY FOUNDATION 37
38 Intramuscular Within a muscle Intravenous Into or within a vein. Intravenous, or IV, usually refers to a way of giving a drug or other substance through a needle or tube inserted into a vein Irradiate To treat with radiation Leukapheresis Removal of the blood to collect specific blood cells. The remaining blood is returned to the body Lymph node A rounded mass of lymphatic tissue that is surrounded by a capsule of connective tissue. Lymph nodes filter lymph (lymphatic fluid), and they store lymphocytes (white blood cells [WBCs]). They are located along lymphatic vessels Lymphatic vessels Thin-walled tubular structures that collect and filter lymph fluid before transporting it back to the blood circulation. Also called lymph vessels Lymphocyte A type of white blood cell (WBC) that is made in the bone marrow and is found in the blood and in lymph tissue. The main types of lymphocytes are B cells, T cells, and natural killer (NK) cells Mediastinal Of the area between the lungs. The organs in this area include the heart and its large blood vessels, the trachea, the esophagus, the thymus, and lymph nodes, but not the lungs Metastatic Spread of cancer from the primary site, or place where it started, to other places in the body Natural killer (NK) cell A type of white blood cell (WBC) that patrols the body and is on constant alert, seeking foreign invaders. Once NK cells recognize a cell as abnormal, they release granules (small particles) with enzymes that can kill tumor cells or cells infected with a virus 03 glossary LUNGEVITY FOUNDATION 38
39 Nephritis Acute or chronic inflammation of the kidney caused by infection, degenerative processes, or vascular disease Non-small cell lung cancer (NSCLC) A group of lung cancers that are named for the kinds of cells found in the cancer and how the cells look under a microscope. The three main types of NSCLC are squamous cell carcinoma, large cell carcinoma, and adenocarcinoma. NSCLC is the most common kind of lung cancer PD-1/PD-L1 See Programmed Death 1/Programmed Death Ligand 1 Pneumonitis Inflammation of the lungs that may be caused by disease, infection, radiation therapy or other therapies, allergy, or irritation of lung tissue by inhaled substance Programmed Death 1/Programmed Death Ligand 1 (PD-1/PD-L1) Part of the immune system mechanism that keeps T cells from functioning Protein A molecule, made up of amino acids, that is needed for the body to function properly. Proteins are the basis of body structures, such as skin and hair, and of other substances, such as enzymes, cytokines, and antibodies Pseudoprogression Growth in tumor size that is due to response to treatment and not to growth of cancer cells Radiation therapy The use of high-energy radiation from X-rays, gamma rays, neutrons, protons, and other sources to kill cancer cells and shrink tumors. Radiation may come from a machine outside the body (external-beam radiation therapy) or it may come from radioactive material placed in the body near cancer cells (internal radiation therapy, or brachytherapy). Also called irradiation and radiotherapy 03 glossary LUNGEVITY FOUNDATION 39
40 Relapse The return of a disease or the signs and symptoms of a disease after a period of improvement Renal dysfunction Reduced ability of the kidneys to filter blood and remove waste products and excess fluid from the body Second-line clinical trial Clinical trial for patients who have had a prior chemotherapy for metastatic disease Second-line treatment or therapy Treatment that is usually started after the first set of treatments doesn t work, has stopped working, or has side effects that are not tolerated Small cell lung cancer (SCLC) A fast-growing cancer that forms in tissues of the lung and can spread to other parts of the body. Named small for how the cancer cells look under a microscope Spleen An organ that is part of the lymphatic system. The spleen makes lymphocytes, filters the blood, stores blood cells, and destroys old blood cells. It is located on the left side of the abdomen near the stomach Stage The extent of a cancer in the body. Lung cancer stages range from Stage 0 (the lung cancer has neither invaded nearby tissue nor spread outside the lung) to Stage IV (the lung cancer may or may not have spread to the lymph nodes, but it has metastasized spread to another part of the body) Subcutaneous Beneath the skin T cell A type of white blood cell (WBC). T cells are part of the immune system and develop from stem cells in the bone marrow. They help protect the body from infection and may help fight cancer. Also called T lymphocyte 03 glossary LUNGEVITY FOUNDATION 40
41 Targeted therapy A type of treatment that uses drugs to attack specific types of cancer cells with less harm to normal cells. Some targeted therapies block the action of certain enzymes, proteins, or other molecules involved in the growth and spread of cancer cells Therapeutic cancer vaccine A type of treatment using a vaccine that is usually made from a patient s own tumor cells or from substances taken from tumor cells. A cancer vaccine may help the immune system kill cancer cells Thymus An organ that is part of the lymphatic system, in which T lymphocytes grow and multiply. The thymus is in the chest behind the breastbone Tumor An abnormal mass of tissue that results when cells divide more than they should or do not die when they should Virus A very simple microorganism that infects cells and may cause disease White blood cell (WBC) A type of blood cell that is made in the bone marrow and found in the blood and lymph tissue. WBCs are part of the body s immune system. They help the body fight infection and other diseases. Types of WBCs are granulocytes (neutrophils, eosinophils, and basophils), monocytes, and lymphocytes (natural killer [NK] cells, T cells, and B cells) 03 glossary LUNGEVITY FOUNDATION 41
42 04 notes 04 notes LUNGEVITY FOUNDATION 42
43 04 notes LUNGEVITY FOUNDATION 43
44 04 notes LUNGEVITY FOUNDATION 44
45 CHICAGO OFFICE 228 S. WABASH AVENUE, SUITE 700 CHICAGO, IL PH: F: BETHESDA OFFICE 6917 ARLINGTON ROAD, SUITE 352 BETHESDA, MD PH: F: May 2018 LUNGevity Foundation. All rights reserved.
IMMUNOTHERAPY FOR THE TREATMENT OF LUNG CANCER
 IMMUNOTHERAPY FOR THE TREATMENT OF LUNG CANCER A guide for patients and caregivers FREE TO BREATHE SUPPORT LINE (844) 835-4325 A FREE resource for lung cancer patients & caregivers About this brochure
IMMUNOTHERAPY FOR THE TREATMENT OF LUNG CANCER A guide for patients and caregivers FREE TO BREATHE SUPPORT LINE (844) 835-4325 A FREE resource for lung cancer patients & caregivers About this brochure
IMMUNOTHERAPY FOR LUNG CANCER
 IMMUNOTHERAPY FOR LUNG CANCER Patient and Caregiver Guide IMMUNOTHERAPY FOR LUNG CANCER Patient and Caregiver Guide TABLE OF CONTENTS Lung Cancer Basics... 2 Immunotherapy... 3 FDA Approved Immunotherapies...
IMMUNOTHERAPY FOR LUNG CANCER Patient and Caregiver Guide IMMUNOTHERAPY FOR LUNG CANCER Patient and Caregiver Guide TABLE OF CONTENTS Lung Cancer Basics... 2 Immunotherapy... 3 FDA Approved Immunotherapies...
IMMUNOTHERAPY FOR THE TREATMENT OF LUNG CANCER
 IMMUNOTHERAPY FOR THE TREATMENT OF LUNG CANCER A guide for patients and caregivers TM Content is consistent with the Oncology Nursing Society Standards and Guidelines. The ONS Seal of Approval does not
IMMUNOTHERAPY FOR THE TREATMENT OF LUNG CANCER A guide for patients and caregivers TM Content is consistent with the Oncology Nursing Society Standards and Guidelines. The ONS Seal of Approval does not
immunotherapy a guide for the patient
 immunotherapy FOR LUNG CANCER a guide for the patient TABLE OF CONTENTS lung cancer basics... 2 immunotherapy... 5 Checkpoint Inhibitors... 6-9 Monoclonal Antibodies... 9 Vaccines... 10 Adoptive T-Cell
immunotherapy FOR LUNG CANCER a guide for the patient TABLE OF CONTENTS lung cancer basics... 2 immunotherapy... 5 Checkpoint Inhibitors... 6-9 Monoclonal Antibodies... 9 Vaccines... 10 Adoptive T-Cell
What You Need to Know About Lung Cancer Immunotherapy
 What You Need to Know About Lung Cancer Immunotherapy Lung.org/immunotherapy What is immunotherapy? Immunotherapy for cancer, sometimes called immune-oncology, is a type of medicine that treats cancer
What You Need to Know About Lung Cancer Immunotherapy Lung.org/immunotherapy What is immunotherapy? Immunotherapy for cancer, sometimes called immune-oncology, is a type of medicine that treats cancer
Immunotherapy and Lung Cancer
 Immunotherapy and Lung Cancer This booklet explains how immunotherapy uses the body s own natural defenses to treat lung cancer. So far, immunotherapy is approved for non-small cell lung cancer (NSCLC)
Immunotherapy and Lung Cancer This booklet explains how immunotherapy uses the body s own natural defenses to treat lung cancer. So far, immunotherapy is approved for non-small cell lung cancer (NSCLC)
UNDERSTANDING SQUAMOUS CELL LUNG CANCER
 UNDERSTANDING SQUAMOUS CELL LUNG CANCER A guide for patients and caregivers FREE TO BREATHE SUPPORT LINE (844) 835-4325 A FREE resource for lung cancer patients & caregivers About this brochure This brochure
UNDERSTANDING SQUAMOUS CELL LUNG CANCER A guide for patients and caregivers FREE TO BREATHE SUPPORT LINE (844) 835-4325 A FREE resource for lung cancer patients & caregivers About this brochure This brochure
Preparing for Your Immune Checkpoint Inhibitor (CPI) Treatment
 Preparing for Your Immune Checkpoint Inhibitor (CPI) Treatment Overview What is the immune system? What are immune checkpoint inhibitors? What are the side effects to look out for? How are side effects
Preparing for Your Immune Checkpoint Inhibitor (CPI) Treatment Overview What is the immune system? What are immune checkpoint inhibitors? What are the side effects to look out for? How are side effects
YOUR GUIDE TO TECENTRIQ (atezolizumab) non-small cell lung cancer (NSCLC)
 YOUR GUIDE TO TECENTRIQ (atezolizumab) For previouslytreated advanced non-small cell lung cancer (NSCLC) ABOUT THIS BOOKLET This booklet is for people with advanced non-small cell lung cancer (NSCLC) who
YOUR GUIDE TO TECENTRIQ (atezolizumab) For previouslytreated advanced non-small cell lung cancer (NSCLC) ABOUT THIS BOOKLET This booklet is for people with advanced non-small cell lung cancer (NSCLC) who
Chapter 38- Immune System
 Chapter 38- Immune System First Line of Defense: Barriers Nonspecific defenses, such as the skin and mucous membranes, are barriers to potential pathogens. In addition to being a physical barrier to pathogens,
Chapter 38- Immune System First Line of Defense: Barriers Nonspecific defenses, such as the skin and mucous membranes, are barriers to potential pathogens. In addition to being a physical barrier to pathogens,
Biological Therapies for Cancer: Questions and Answers
 Biological Therapies for Cancer: Questions and Answers Key Points Biological therapies use the body s immune system to fight cancer or to lessen the side effects that may be caused by some cancer treatments
Biological Therapies for Cancer: Questions and Answers Key Points Biological therapies use the body s immune system to fight cancer or to lessen the side effects that may be caused by some cancer treatments
Immunotherapy Narrative Script:
 Immunotherapy Narrative Script: In order to understand immunotherapy, there are a few things we need to get straight in our heads first. The first thing we need to get a general understanding of is what
Immunotherapy Narrative Script: In order to understand immunotherapy, there are a few things we need to get straight in our heads first. The first thing we need to get a general understanding of is what
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHATIC AND IMMUNE SYSTEMS. Chapter 33
 LYMPHATIC AND IMMUNE SYSTEMS Chapter 33 THE LYMPHATIC SYSTEM The lymphatic system has three main functions Take up excess tissue fluid and return it to the bloodstream Receive fats called lipoproteins
LYMPHATIC AND IMMUNE SYSTEMS Chapter 33 THE LYMPHATIC SYSTEM The lymphatic system has three main functions Take up excess tissue fluid and return it to the bloodstream Receive fats called lipoproteins
What Is Small Cell Lung Cancer?
 About Small Cell Lung Cancer Overview If you have been diagnosed with small cell lung cancer or are worried about it, you likely have a lot of questions. Learning some basics is a good place to start.
About Small Cell Lung Cancer Overview If you have been diagnosed with small cell lung cancer or are worried about it, you likely have a lot of questions. Learning some basics is a good place to start.
Anemia: A condition in which the number of red blood cells is below normal.
 Veterinary Teaching Hospital Oncology Service Virginia-Maryland Regional College of Veterinary Medicine 245 Duck Pond Drive Blacksburg, VA 24061 Phone: 540-231-4621 Definitions This fact sheet is based
Veterinary Teaching Hospital Oncology Service Virginia-Maryland Regional College of Veterinary Medicine 245 Duck Pond Drive Blacksburg, VA 24061 Phone: 540-231-4621 Definitions This fact sheet is based
Chapter 24 The Immune System
 Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
biomarker testing What you need to know about... LUNG CANCER TREATMENTS
 LUNG CANCER TREATMENTS What you need to know about... biomarker testing Copyright 2018 LUNGevity Foundation All rights reserved. No part of this publication may be reproduced, distributed, or transmitted
LUNG CANCER TREATMENTS What you need to know about... biomarker testing Copyright 2018 LUNGevity Foundation All rights reserved. No part of this publication may be reproduced, distributed, or transmitted
Cancer , The Patient Education Institute, Inc. ocf80101 Last reviewed: 06/08/2016 1
 Cancer Introduction Cancer begins in your cells, which are the building blocks of your body. Extra cells can form a mass called a tumor. Some tumors aren t cancerous, while other ones are. Cells from cancerous
Cancer Introduction Cancer begins in your cells, which are the building blocks of your body. Extra cells can form a mass called a tumor. Some tumors aren t cancerous, while other ones are. Cells from cancerous
Guided Reading Activities
 Name Period Chapter 24: The Immune System Guided Reading Activities Big idea: Innate immunity Answer the following questions as you read modules 24.1 24.2: 1. Bacteria, viruses, and other microorganisms
Name Period Chapter 24: The Immune System Guided Reading Activities Big idea: Innate immunity Answer the following questions as you read modules 24.1 24.2: 1. Bacteria, viruses, and other microorganisms
Acute: Symptoms that start and worsen quickly but do not last over a long period of time.
 Cancer Glossary Acute: Symptoms that start and worsen quickly but do not last over a long period of time. Adjuvant therapy: Treatment given after the main treatment. It usually refers to chemotherapy,
Cancer Glossary Acute: Symptoms that start and worsen quickly but do not last over a long period of time. Adjuvant therapy: Treatment given after the main treatment. It usually refers to chemotherapy,
Esophageal Cancer. Source: National Cancer Institute
 Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 28 The Immune System Lesson 1: The Immune System Lesson Objectives Upon completion of this lesson,
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 28 The Immune System Lesson 1: The Immune System Lesson Objectives Upon completion of this lesson,
GAZYVA for Chronic Lymphocytic Leukemia (CLL)
 GAZYVA for Chronic Lymphocytic Leukemia (CLL) GAZYVA is a prescription medicine used with the chemotherapy drug, chlorambucil, to treat chronic lymphocytic leukemia (CLL) in adults who have not had previous
GAZYVA for Chronic Lymphocytic Leukemia (CLL) GAZYVA is a prescription medicine used with the chemotherapy drug, chlorambucil, to treat chronic lymphocytic leukemia (CLL) in adults who have not had previous
Oncology 101. Cancer Basics
 Oncology 101 Cancer Basics What Will You Learn? What is Cancer and How Does It Develop? Cancer Diagnosis and Staging Cancer Treatment What is Cancer? Cancer is a group of more than 100 different diseases
Oncology 101 Cancer Basics What Will You Learn? What is Cancer and How Does It Develop? Cancer Diagnosis and Staging Cancer Treatment What is Cancer? Cancer is a group of more than 100 different diseases
Immune System. Before You Read. Read to Learn
 Immune System 37 section 2 The Immune System Biology/Life Sciences 10.b Students know the role of antibodies in the body s response to infection. Also covers: Biology/Life Sciences 10.a, 10.e, 10.f Components
Immune System 37 section 2 The Immune System Biology/Life Sciences 10.b Students know the role of antibodies in the body s response to infection. Also covers: Biology/Life Sciences 10.a, 10.e, 10.f Components
Esophageal cancer. What is esophageal cancer? Esophageal cancer is a disease in which malignant (cancer) cells form in the tissues of the esophagus.
 Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Anatomy. Lymph: Tissue fluid that enters a lymphatic capillary (clear fluid that surrounds new piercings!)
 Lymphatic System Anatomy Lymphatic vessels: meet up in capillaries of of tissues to collect extra water, and have an end point of meeting up with lymphatic ducts that empty fluid into large veins in the
Lymphatic System Anatomy Lymphatic vessels: meet up in capillaries of of tissues to collect extra water, and have an end point of meeting up with lymphatic ducts that empty fluid into large veins in the
Immunity and Infection. Chapter 17
 Immunity and Infection Chapter 17 The Chain of Infection Transmitted through a chain of infection (six links) Pathogen: Disease causing microorganism Reservoir: Natural environment of the pathogen Portal
Immunity and Infection Chapter 17 The Chain of Infection Transmitted through a chain of infection (six links) Pathogen: Disease causing microorganism Reservoir: Natural environment of the pathogen Portal
Chapter 13 Lymphatic and Immune Systems
 The Chapter 13 Lymphatic and Immune Systems 1 The Lymphatic Vessels Lymphoid Organs Three functions contribute to homeostasis 1. Return excess tissue fluid to the bloodstream 2. Help defend the body against
The Chapter 13 Lymphatic and Immune Systems 1 The Lymphatic Vessels Lymphoid Organs Three functions contribute to homeostasis 1. Return excess tissue fluid to the bloodstream 2. Help defend the body against
Outline. Animals: Immunity. Defenses Against Disease. Key Concepts:
 Animals: Immunity Defenses Against Disease Outline 1. Key concepts 2. Physical barriers: Skin, Mucus and HCL in stomach 3. Non-specific 4. Specific responses Immune System a. Components of Immune system
Animals: Immunity Defenses Against Disease Outline 1. Key concepts 2. Physical barriers: Skin, Mucus and HCL in stomach 3. Non-specific 4. Specific responses Immune System a. Components of Immune system
Leukemia. There are different types of leukemia and several treatment options for each type.
 Leukemia Introduction Leukemia is the name of a group of cancers of the blood cells. Hundreds of thousands of people worldwide are diagnosed with leukemia each year. There are different types of leukemia
Leukemia Introduction Leukemia is the name of a group of cancers of the blood cells. Hundreds of thousands of people worldwide are diagnosed with leukemia each year. There are different types of leukemia
Giving appropriate patients another chance to fight OPDIVO
 For dmmr/msi-h Colorectal Cancer (CRC) All individuals depicted are models used for illustrative purposes only. Who is OPDIVO for? OPDIVO is a prescription medicine used to treat colorectal cancer (a type
For dmmr/msi-h Colorectal Cancer (CRC) All individuals depicted are models used for illustrative purposes only. Who is OPDIVO for? OPDIVO is a prescription medicine used to treat colorectal cancer (a type
Lymphoma is a cancer that develops in the white blood cells (lymphocytes) of the lymphatic system, which is part of the body's immune system.
 Scan for mobile link. Lymphoma Lymphoma is a cancer that develops in the white blood cells of the lymphatic system. Symptoms may include enlarged lymph nodes, unexplained weight loss, fatigue, night sweats
Scan for mobile link. Lymphoma Lymphoma is a cancer that develops in the white blood cells of the lymphatic system. Symptoms may include enlarged lymph nodes, unexplained weight loss, fatigue, night sweats
NON- HODGKIN LYMPHOMA
 NON- HODGKIN LYMPHOMA non - Hodgkin lymphoma This medical guide is designed for educational purposes to help patients understand. Please consult your doctor on specific questions and details about your
NON- HODGKIN LYMPHOMA non - Hodgkin lymphoma This medical guide is designed for educational purposes to help patients understand. Please consult your doctor on specific questions and details about your
UNIT 6: PHYSIOLOGY Chapter 31: Immune System and Disease
 CORNELL NOTES Directions: You must create a minimum of 5 questions in this column per page (average). Use these to study your notes and prepare for tests and quizzes. Notes will be stamped after each assigned
CORNELL NOTES Directions: You must create a minimum of 5 questions in this column per page (average). Use these to study your notes and prepare for tests and quizzes. Notes will be stamped after each assigned
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
GAZYVA: for follicular lymphoma that has not responded to or has returned after treatment
 GAZYVA: for follicular lymphoma that has not responded to or has returned after treatment GAZYVA is a prescription medicine used with the chemotherapy drug, bendamustine, followed by GAZYVA alone for follicular
GAZYVA: for follicular lymphoma that has not responded to or has returned after treatment GAZYVA is a prescription medicine used with the chemotherapy drug, bendamustine, followed by GAZYVA alone for follicular
offers the possibility of a longer life 1 BLINCYTO A guide for patients and caregivers
 In a study of 405 adults with Philadelphia chromosome negative relapsed or refractory B-cell precursor acute lymphoblastic leukemia, 271 were treated with BLINCYTO and 134 with chemotherapy. The adults
In a study of 405 adults with Philadelphia chromosome negative relapsed or refractory B-cell precursor acute lymphoblastic leukemia, 271 were treated with BLINCYTO and 134 with chemotherapy. The adults
The Lymphatic System
 The Lymphatic System The Lymphatic System The Lymphatic System Carries essential nutrients to the cells Collects cellular waste Plays an important role in the immune system of the body Lymph A fluid that
The Lymphatic System The Lymphatic System The Lymphatic System Carries essential nutrients to the cells Collects cellular waste Plays an important role in the immune system of the body Lymph A fluid that
General Information Key Points
 The content of this booklet was adapted from content originally published by the National Cancer Institute. Male Breast Cancer Treatment (PDQ ) Patient Version. Updated September 29,2017. https://www.cancer.gov/types/breast/patient/male-breast-treatment-pdq
The content of this booklet was adapted from content originally published by the National Cancer Institute. Male Breast Cancer Treatment (PDQ ) Patient Version. Updated September 29,2017. https://www.cancer.gov/types/breast/patient/male-breast-treatment-pdq
1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50%
 BIOL2030 Huaman A&P II -- Exam 3 -- XXXX -- Form A Name: 1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50% 2. Special lymphatic vessels called
BIOL2030 Huaman A&P II -- Exam 3 -- XXXX -- Form A Name: 1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50% 2. Special lymphatic vessels called
CANCER 1.7 M 609,000 26% 15.5 M 73% JUST THE FACTS. More Than 1,100 Cancer Treatments in Clinical Testing Offer Hope to Patients
 CANCER MEDICINES IN DEVELOPMENT 2018 REPORT JUST THE FACTS MORE THAN 1.7 M ESTIMATED NEW CASES OF CANCER IN 2018 IN THE UNITED STATES MORE THAN 609,000 U.S. CANCER DEATHS ARE EXPECTED IN 2018 SINCE PEAKING
CANCER MEDICINES IN DEVELOPMENT 2018 REPORT JUST THE FACTS MORE THAN 1.7 M ESTIMATED NEW CASES OF CANCER IN 2018 IN THE UNITED STATES MORE THAN 609,000 U.S. CANCER DEATHS ARE EXPECTED IN 2018 SINCE PEAKING
Lecture 10 Immune System
 Lecture 10 Immune System Lecture 10 1. Introduction 2. Nonspecific External Defenses 3. Innate Immune Response 4. Acquired Immune Response 5. Antibiotics and Vaccines 1 The not-so-common cold A cold is
Lecture 10 Immune System Lecture 10 1. Introduction 2. Nonspecific External Defenses 3. Innate Immune Response 4. Acquired Immune Response 5. Antibiotics and Vaccines 1 The not-so-common cold A cold is
Lesson 3: Immunizations
 K-W-L Graphic Organizer K (Know) What do you know about W (Want) What do you want to know about L (Learned) What did you learn about Glossary 1. antibodies: proteins created by the immune system to fight
K-W-L Graphic Organizer K (Know) What do you know about W (Want) What do you want to know about L (Learned) What did you learn about Glossary 1. antibodies: proteins created by the immune system to fight
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System Multiple-Choice Questions
 Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
BIT 120. Copy of Cancer/HIV Lecture
 BIT 120 Copy of Cancer/HIV Lecture Cancer DEFINITION Any abnormal growth of cells that has malignant potential i.e.. Leukemia Uncontrolled mitosis in WBC Genetic disease caused by an accumulation of mutations
BIT 120 Copy of Cancer/HIV Lecture Cancer DEFINITION Any abnormal growth of cells that has malignant potential i.e.. Leukemia Uncontrolled mitosis in WBC Genetic disease caused by an accumulation of mutations
Chapter 22: The Lymphatic System and Immunity
 Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Overview of the Lymphoid System
 Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
BLINCYTO can eliminate detectable traces of cancer 1
 For people* with B-cell precursor ALL who are MRD+, 1 BLINCYTO can eliminate detectable traces of cancer 1 In a study of 86 adults with MRD+ B-cell precursor ALL, BLINCYTO removed detectable traces of
For people* with B-cell precursor ALL who are MRD+, 1 BLINCYTO can eliminate detectable traces of cancer 1 In a study of 86 adults with MRD+ B-cell precursor ALL, BLINCYTO removed detectable traces of
Opdivo (nivolumab) An overview of Opdivo and why it is authorised in the EU. What is Opdivo and what is it used for?
 EMA/852560/2018 EMEA/H/C/003985 An overview of Opdivo and why it is authorised in the EU What is Opdivo and what is it used for? Opdivo is a cancer medicine used to treat the following: melanoma, a type
EMA/852560/2018 EMEA/H/C/003985 An overview of Opdivo and why it is authorised in the EU What is Opdivo and what is it used for? Opdivo is a cancer medicine used to treat the following: melanoma, a type
The immune system is made up of a complex and vital network of cells and organs that protect the body from infection.
 IMMUNE SYSTEM Viruses, bacteria and other germs are all around us. Most of the time, a healthy immune system keeps us well. The purpose of the immune system is to keep infectious micro-organisms, such
IMMUNE SYSTEM Viruses, bacteria and other germs are all around us. Most of the time, a healthy immune system keeps us well. The purpose of the immune system is to keep infectious micro-organisms, such
Chapter Pages Transmission
 Chapter 19.2 Pages 442-448 Transmission Immunity There are three lines of defense: 1 The skin and mucous membranes are a nonspecific barrier to infection. 2 Macrophages attack pathogens that enter the
Chapter 19.2 Pages 442-448 Transmission Immunity There are three lines of defense: 1 The skin and mucous membranes are a nonspecific barrier to infection. 2 Macrophages attack pathogens that enter the
4) What causes lymph to move? Skeletal muscle contraction; smooth muscle contraction, breathing (like blood moves through veins)
 NPHS Anatomy & Physiology UNIT 10 REVIEW GUIDE Lymphatic System 1) List the three functions of the lymphatic system. transports excess fluid to the bloodstream absorbs fats helps defend the body against
NPHS Anatomy & Physiology UNIT 10 REVIEW GUIDE Lymphatic System 1) List the three functions of the lymphatic system. transports excess fluid to the bloodstream absorbs fats helps defend the body against
Lymphatic System and Immunity
 Lymphatic System and Immunity Lymphatic System Immunity- ability to resist infection and disease through the activation of specific defenses These defenses can be found in the lymphatic system Lymphatic
Lymphatic System and Immunity Lymphatic System Immunity- ability to resist infection and disease through the activation of specific defenses These defenses can be found in the lymphatic system Lymphatic
Cancer of the oropharynx
 Cancer of the oropharynx Patient information What is cancer? The human body is made up of billions of cells. In healthy people, cells grow, divide and die. New cells constantly replace old ones in an orderly
Cancer of the oropharynx Patient information What is cancer? The human body is made up of billions of cells. In healthy people, cells grow, divide and die. New cells constantly replace old ones in an orderly
People who have received 1-3 prior treatments for their multiple myeloma may receive: Revlimid (lenalidomide)
 FINDTHE THE FIND STRENGTH STRENGTH WITHIN WITHIN TOHELP HELPFIGHT FIGHT TO MULTIPLEMYELOMA MYELOMA MULTIPLE Rick N. N. patient Rick patient What is? is a prescription medicine used with other medications
FINDTHE THE FIND STRENGTH STRENGTH WITHIN WITHIN TOHELP HELPFIGHT FIGHT TO MULTIPLEMYELOMA MYELOMA MULTIPLE Rick N. N. patient Rick patient What is? is a prescription medicine used with other medications
Randy J. EMPLICITI patient Ready to get started
 Randy J. EMPLICITI patient Ready to get started PICTURE YOUR IMMUNE SYSTEM AT WORK AGAINST MULTIPLE MYELOMA Randy J. EMPLICITI patient My body taking on multiple myeloma What is EMPLICITI? EMPLICITI is
Randy J. EMPLICITI patient Ready to get started PICTURE YOUR IMMUNE SYSTEM AT WORK AGAINST MULTIPLE MYELOMA Randy J. EMPLICITI patient My body taking on multiple myeloma What is EMPLICITI? EMPLICITI is
Get on with life, we ll see you. in 6 months. Living your life your way with MS
 Get on with life, we ll see you in 6 months. Living your life your way with MS If you re one of the 4000 New Zealanders affected by MS, ask your doctor or nurse if OCREVUS is right for you. Contents What
Get on with life, we ll see you in 6 months. Living your life your way with MS If you re one of the 4000 New Zealanders affected by MS, ask your doctor or nurse if OCREVUS is right for you. Contents What
OPTIONAL BIOLOGY 1 STUDY PACKET IMMUNE SYSTEM SC.912.L AA
 OPTIONAL BIOLOGY 1 STUDY PACKET IMMUNE SYSTEM SC.912.L.14.52 AA SC.912.L.14.52 AA Explain the basic functions of the human immune system, including specific and nonspecific immune response, vaccines and
OPTIONAL BIOLOGY 1 STUDY PACKET IMMUNE SYSTEM SC.912.L.14.52 AA SC.912.L.14.52 AA Explain the basic functions of the human immune system, including specific and nonspecific immune response, vaccines and
The Lymphatic System
 The Lymphatic System Combining Forms Aden/o Angi/o Hem/o Hist/o Immun/o Lymph/o Splen/o Thym/o Tox/o gland vessel (blood or lymph) blood tissue immune lymph spleen thymus gland poison Prefixes / Suffixes
The Lymphatic System Combining Forms Aden/o Angi/o Hem/o Hist/o Immun/o Lymph/o Splen/o Thym/o Tox/o gland vessel (blood or lymph) blood tissue immune lymph spleen thymus gland poison Prefixes / Suffixes
Cell-mediated response (what type of cell is activated and what gets destroyed?)
 The Immune System Reading Guide (Chapter 43) Name Per 1. The immune response in animals can be divided into innate immunity and adaptive immunity. As an overview, complete this figure indicating the divisions
The Immune System Reading Guide (Chapter 43) Name Per 1. The immune response in animals can be divided into innate immunity and adaptive immunity. As an overview, complete this figure indicating the divisions
The circulatory system brings many different materials to all the cells of the body and picks up waste from the same cells.
 CIRCULATION AND IMMUNITY The Circulatory System The circulatory system, otherwise known as the cardiovascular system, consists of the heart, blood vessels, and blood. This important system is a large network
CIRCULATION AND IMMUNITY The Circulatory System The circulatory system, otherwise known as the cardiovascular system, consists of the heart, blood vessels, and blood. This important system is a large network
Anatomy and Physiology 2
 Anatomy and Physiology 2 The Nervous System Nerves allows organisms to detect and respond to stimuli by transmitting electrical impulses cell to cell. Can send info at high speeds! Neurons are the smallest
Anatomy and Physiology 2 The Nervous System Nerves allows organisms to detect and respond to stimuli by transmitting electrical impulses cell to cell. Can send info at high speeds! Neurons are the smallest
Overview. Barriers help animals defend against many dangerous pathogens they encounter.
 Immunity Overview Barriers help animals defend against many dangerous pathogens they encounter. The immune system recognizes foreign bodies and responds with the production of immune cells and proteins.
Immunity Overview Barriers help animals defend against many dangerous pathogens they encounter. The immune system recognizes foreign bodies and responds with the production of immune cells and proteins.
For the Patient: USMAVFIPI
 For the Patient: USMAVFIPI Other Names: First-Line Treatment of Unresectable or Metastatic Melanoma Using Ipilimumab U = Undesignated (requires special request) SM = Skin and Melanoma AV = Advanced F =
For the Patient: USMAVFIPI Other Names: First-Line Treatment of Unresectable or Metastatic Melanoma Using Ipilimumab U = Undesignated (requires special request) SM = Skin and Melanoma AV = Advanced F =
Small Cell Lung Cancer
 Small Cell Lung Cancer Small cell lung cancer (SCLC) affects 15% of all lung cancer patients. SCLC is the most aggressive type of lung cancer. It may be treated with chemotherapy and radiation. SCLC has
Small Cell Lung Cancer Small cell lung cancer (SCLC) affects 15% of all lung cancer patients. SCLC is the most aggressive type of lung cancer. It may be treated with chemotherapy and radiation. SCLC has
Immunotherapy. A Cancer Treatment Option
 Immunotherapy A Cancer Treatment Option Introduction CureSearch for Children s Cancer has partnered with Dr. Jennifer Dean to share about immunotherapy, a revolutionary treatment that uses a patient s
Immunotherapy A Cancer Treatment Option Introduction CureSearch for Children s Cancer has partnered with Dr. Jennifer Dean to share about immunotherapy, a revolutionary treatment that uses a patient s
Discussing TECENTRIQ (atezolizumab) with your healthcare team Talking to Your Doctor
 Discussing TECENTRIQ (atezolizumab) with your healthcare team Talking to Your Doctor TECENTRIQ DISCUSSION SUPPORT What is TECENTRIQ? TECENTRIQ is a prescription medicine used to treat: A type of bladder
Discussing TECENTRIQ (atezolizumab) with your healthcare team Talking to Your Doctor TECENTRIQ DISCUSSION SUPPORT What is TECENTRIQ? TECENTRIQ is a prescription medicine used to treat: A type of bladder
LUNG CANCER TREATMENTS UPDATED MAY What you need to know about... targeted therapy
 LUNG CANCER TREATMENTS UPDATED MAY 2018 What you need to know about... targeted therapy foreword About LUNGevity LUNGevity is the largest national lung cancer-focused nonprofit, changing outcomes for people
LUNG CANCER TREATMENTS UPDATED MAY 2018 What you need to know about... targeted therapy foreword About LUNGevity LUNGevity is the largest national lung cancer-focused nonprofit, changing outcomes for people
Chapter 3 - The Immune System
 Chapter 3 - The Immune System What are germs? We all have heard that washing your hands helps stop the spread of germs What are germs exactly? Germs are disease-causing invaders or organisms, also called
Chapter 3 - The Immune System What are germs? We all have heard that washing your hands helps stop the spread of germs What are germs exactly? Germs are disease-causing invaders or organisms, also called
Chapter 40 Section 2 The Immune System
 Chapter 40 Section 2 The Immune System Science Standard 10a What is the role of the skin in providing nonspecific defenses against infection? What is the function of the immune system? The immune system
Chapter 40 Section 2 The Immune System Science Standard 10a What is the role of the skin in providing nonspecific defenses against infection? What is the function of the immune system? The immune system
Rick N. EMPLICITI patient Ready to get started
 Rick N. EMPLICITI patient Ready to get started PICTURE YOUR IMMUNE SYSTEM AT WORK AGAINST MULTIPLE MYELOMA Rick N. EMPLICITI patient My body taking on multiple myeloma What is EMPLICITI? EMPLICITI is a
Rick N. EMPLICITI patient Ready to get started PICTURE YOUR IMMUNE SYSTEM AT WORK AGAINST MULTIPLE MYELOMA Rick N. EMPLICITI patient My body taking on multiple myeloma What is EMPLICITI? EMPLICITI is a
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer starts in your cells. Cells are the building blocks of your tissues. Tissues make up the organs of your
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer starts in your cells. Cells are the building blocks of your tissues. Tissues make up the organs of your
For the Patient: USMAVPEM
 For the Patient: USMAVPEM Other Names: Treatment of Unresectable or Metastatic Melanoma Using Pembrolizumab U = Undesignated (requires special request) SM = Skin and Melanoma AV = Advanced PEM = Pembrolizumab
For the Patient: USMAVPEM Other Names: Treatment of Unresectable or Metastatic Melanoma Using Pembrolizumab U = Undesignated (requires special request) SM = Skin and Melanoma AV = Advanced PEM = Pembrolizumab
The Immune System and Disease
 Chapter 40 The Immune System and Disease Section 40 1 Infectious Disease (pages 1029 1033) This section describes the causes of disease and explains how infectious diseases are transmitted Introduction
Chapter 40 The Immune System and Disease Section 40 1 Infectious Disease (pages 1029 1033) This section describes the causes of disease and explains how infectious diseases are transmitted Introduction
Discussing TECENTRIQ (atezolizumab) with your healthcare team
 Discussing TECENTRIQ (atezolizumab) with your healthcare team What is TECENTRIQ? TECENTRIQ is a prescription medicine used to treat: a type of lung cancer called non-small cell lung cancer (NSCLC). TECENTRIQ
Discussing TECENTRIQ (atezolizumab) with your healthcare team What is TECENTRIQ? TECENTRIQ is a prescription medicine used to treat: a type of lung cancer called non-small cell lung cancer (NSCLC). TECENTRIQ
Immune System AP SBI4UP
 Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
more intense treatments are needed to get rid of the infection.
 What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
was proven to help people live longer1 BLINCYTO A guide for patients and caregivers
 In a clinical trial for people with a certain kind of ALL whose cancer has returned or didn t respond to treatment 1 BLINCYTO was proven to help people live longer1 In a study of 405 adults with ALL, 271
In a clinical trial for people with a certain kind of ALL whose cancer has returned or didn t respond to treatment 1 BLINCYTO was proven to help people live longer1 In a study of 405 adults with ALL, 271
Defense mechanism against pathogens
 Defense mechanism against pathogens Immune System What is immune system? Cells and organs within an animal s body that contribute to immune defenses against pathogens ( ) Bacteria -Major entry points ;open
Defense mechanism against pathogens Immune System What is immune system? Cells and organs within an animal s body that contribute to immune defenses against pathogens ( ) Bacteria -Major entry points ;open
Lecture 10 Immune System
 Lecture 10 Immune System Lecture 10 1. Introduction 2. Nonspecific External Defenses 3. Innate Immune Response 4. Acquired Immune Response 5. Antibiotics and Vaccines 1 The not-so-common cold A cold is
Lecture 10 Immune System Lecture 10 1. Introduction 2. Nonspecific External Defenses 3. Innate Immune Response 4. Acquired Immune Response 5. Antibiotics and Vaccines 1 The not-so-common cold A cold is
Return tissue fluid to the bloodstream (fluid balance) Immunity. Transport fats from the digestive tract to the bloodstream
 Lymphatic System L Y M P H A T I C C O M P O N E N T S What is a Lymphatic System? The lymphatic system is a complex system of fluid drainage and transport, immune response, and disease resistance. Fluid
Lymphatic System L Y M P H A T I C C O M P O N E N T S What is a Lymphatic System? The lymphatic system is a complex system of fluid drainage and transport, immune response, and disease resistance. Fluid
Acquired Immunity Cells are initially and require before they can work Responds to individual microbes
 1 of 10 THE IMMUNE SYSTEM CHAPTER 43; PAGES 898 921 WHY DO WE NEED AN IMMUNE SYSTEM? It s a dirty, dirty world out there and we are vastly outnumbered Bacteria and parasites are everywhere The body has
1 of 10 THE IMMUNE SYSTEM CHAPTER 43; PAGES 898 921 WHY DO WE NEED AN IMMUNE SYSTEM? It s a dirty, dirty world out there and we are vastly outnumbered Bacteria and parasites are everywhere The body has
Labor Dr. Gansauge Sedanstraße, Ulm
 Labor Dr. Gansauge Sedanstraße, Ulm 3 3 LANEX-DC Immunotherapy with dendritic cells The ability to fight cancer using one s own immune system has been a great dream of medical scientists for centuries.
Labor Dr. Gansauge Sedanstraße, Ulm 3 3 LANEX-DC Immunotherapy with dendritic cells The ability to fight cancer using one s own immune system has been a great dream of medical scientists for centuries.
1. Specificity: specific activity for each type of pathogens. Immunity is directed against a particular pathogen or foreign substance.
 L13: Acquired or adaptive (specific) immunity The resistance, which absent at the time of first exposure to a pathogen, but develops after being exposed to the pathogen is called acquired immunity. It
L13: Acquired or adaptive (specific) immunity The resistance, which absent at the time of first exposure to a pathogen, but develops after being exposed to the pathogen is called acquired immunity. It
Copyright Glencoe/McGraw-Hill, a division of the McGraw-Hill Companies, Inc. Name Date Class Circulation 33 Chapter 19 Circulation Section 1 The
 Copyright Glencoe/McGraw-Hill, a division of the McGraw-Hill Companies, Inc. Name Date Class Circulation 33 Chapter 19 Circulation Section 1 The Circulatory System A. Your system includes the blood, heart,
Copyright Glencoe/McGraw-Hill, a division of the McGraw-Hill Companies, Inc. Name Date Class Circulation 33 Chapter 19 Circulation Section 1 The Circulatory System A. Your system includes the blood, heart,
Cancer: Questions and Answers
 Cancer: Questions and Answers Key Points The survival rate for many types of cancer has improved in recent years; however, cancer is still the second leading cause of death in the United States (see paragraph
Cancer: Questions and Answers Key Points The survival rate for many types of cancer has improved in recent years; however, cancer is still the second leading cause of death in the United States (see paragraph
OBJECTIVES. The Amazing Immune System
 The Amazing Immune System Graphic source: (l) Jeanne Kelly, NIAID; (r) Wikimedia Commons OBJECTIVES Describe at least three components of the immune system Describe the role in our immune response of at
The Amazing Immune System Graphic source: (l) Jeanne Kelly, NIAID; (r) Wikimedia Commons OBJECTIVES Describe at least three components of the immune system Describe the role in our immune response of at
Infectious Diseases through Viruses. Obj. 3.c. & 3.g.
 Infectious Diseases through Viruses Obj. 3.c. & 3.g. Diseases Caused By Cells A disease is a condition that stops the body from functioning normally. Non-infectious diseases are not spread from person
Infectious Diseases through Viruses Obj. 3.c. & 3.g. Diseases Caused By Cells A disease is a condition that stops the body from functioning normally. Non-infectious diseases are not spread from person
The Immune System: The Mind Body Connection. Presented by Margaret Kemeny, Ph.D. Department of Psychiatry, University of California, San Francisco
 The Immune System: The Mind Body Connection Presented by Margaret Kemeny, Ph.D. Department of Psychiatry, University of California, San Francisco Psychoneuroimmunology Investigation of the bidirectional
The Immune System: The Mind Body Connection Presented by Margaret Kemeny, Ph.D. Department of Psychiatry, University of California, San Francisco Psychoneuroimmunology Investigation of the bidirectional
Chapter 17. The Lymphatic System and Immunity. Copyright 2010, John Wiley & Sons, Inc.
 Chapter 17 The Lymphatic System and Immunity Immunity Innate Immunity Fast, non-specific and no memory Barriers, ph extremes, Phagocytes & NK cells, fever, inflammation, complement, interferon Adaptive
Chapter 17 The Lymphatic System and Immunity Immunity Innate Immunity Fast, non-specific and no memory Barriers, ph extremes, Phagocytes & NK cells, fever, inflammation, complement, interferon Adaptive
Immune Checkpoint Inhibitors: A Guide for Cancer Patients
 Patient & Family Guide 2018 Immune Checkpoint Inhibitors: A Guide for Cancer Patients www.nscancercare.ca Immune Checkpoint Inhibitors: A Guide for Cancer Patients Table of Contents What Does My Immune
Patient & Family Guide 2018 Immune Checkpoint Inhibitors: A Guide for Cancer Patients www.nscancercare.ca Immune Checkpoint Inhibitors: A Guide for Cancer Patients Table of Contents What Does My Immune
Lifeblood Lab Activity
 History of Blood: It is the universal symbol of horror, of death, yet it is the one thing that keeps you living. It is the blood that is coursing through your veins. But, what do you really know about
History of Blood: It is the universal symbol of horror, of death, yet it is the one thing that keeps you living. It is the blood that is coursing through your veins. But, what do you really know about
phagocytic leukocyte Fighting the Enemy Within Immune System lymphocytes attacking cancer cell lymph system
 Fighting the Enemy Within phagocytic leukocyte Immune System lymphocytes attacking cancer cell lymph system AP Biology 2006-2007 Avenues of attack Points of entry digestive system respiratory system urinary
Fighting the Enemy Within phagocytic leukocyte Immune System lymphocytes attacking cancer cell lymph system AP Biology 2006-2007 Avenues of attack Points of entry digestive system respiratory system urinary
Bone Marrow Transplantation
 Bone Marrow Transplantation Introduction Bone marrow is the spongy tissue inside all of your bones, including your hip and thigh bones. The bone marrow is like a factory that makes different types of blood
Bone Marrow Transplantation Introduction Bone marrow is the spongy tissue inside all of your bones, including your hip and thigh bones. The bone marrow is like a factory that makes different types of blood
ANATOMY & PHYSIOLOGY II
 ANATOMY & PHYSIOLOGY II THE BODY SYSTEMS Anatomy & Physiology II The Body Systems Michelle Cochrane 2014 All rights reserved. This material is subject to copyright and may not be reprinted or reproduced
ANATOMY & PHYSIOLOGY II THE BODY SYSTEMS Anatomy & Physiology II The Body Systems Michelle Cochrane 2014 All rights reserved. This material is subject to copyright and may not be reprinted or reproduced
OPTIONAL GRADE 8 STUDY PACKET IMMUNE SYSTEM SC.6.L.14.5 AA
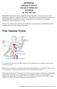 OPTIONAL GRADE 8 STUDY PACKET IMMUNE SYSTEM SC.6.L.14.5 AA SC.6.L.14.5 AA Identify and investigate the general functions of the major systems of the human body (digestive, respiratory, circulatory, reproductive,
OPTIONAL GRADE 8 STUDY PACKET IMMUNE SYSTEM SC.6.L.14.5 AA SC.6.L.14.5 AA Identify and investigate the general functions of the major systems of the human body (digestive, respiratory, circulatory, reproductive,
Keytruda. Keytruda (pembrolizumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.50 Subject: Keytruda Page: 1 of 6 Last Review Date: September 15, 2017 Keytruda Description Keytruda
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.50 Subject: Keytruda Page: 1 of 6 Last Review Date: September 15, 2017 Keytruda Description Keytruda
