Mantle cell lymphoma
|
|
|
- Bernice Hawkins
- 5 years ago
- Views:
Transcription
1 Critical Reviews in Oncology/Hematology 82 (2012) Mantle cell lymphoma Sergio Cortelazzo a, Maurilio Ponzoni b,c, Andrés J.M. Ferreri c,d,, Martin Dreyling e a Hematology and Bone Marrow Transplantation Unit, Azienda Ospedaliera Bolzano, Italy b Pathology Unit, San Raffaele Scientific Institute, Milan, Italy c Unit of Lymphoid Malignancies, San Raffaele Scientific Institute, Milan, Italy d Medical Oncology Unit, San Raffaele Scientific Institute, Milan, Italy e Medizinische Klinik III der Universität München Grosshadern, München, Germany Accepted 4 May 2011 Contents 1. General information Definition Incidence Risk factors Pathology and biology Morphology Immunophenotype Genetic features Diagnosis Clinical presentations Staging Staging procedures Staging system Minimal residual disease Prognosis Natural history Prognostic factors Treatment Treatment of limited disease (stage I II) Treatment of advanced disease (stage III IV) Standard-dose chemotherapy High-dose chemotherapy supported by autologous stem cell transplant Rituximab-based immunotherapy Radioimmunotherapy Allogeneic transplantation Salvage therapy for patients who are not candidates to intensive treatments New agents and strategies for MCL Conflict of interest Reviewer References Biographies Corresponding author at: Unit of Lymphoid Malignancies, Medical Oncology Unit, Department of Oncology, San Raffaele Scientific Institute, Via Olgettina 60, Milan, Italy. Tel.: , fax: addresses: andres.ferreri@hsr.it, start@istitutotumori.mi.it (A.J.M. Ferreri) /$ see front matter 2011 Elsevier Ireland Ltd. All rights reserved. doi: /j.critrevonc
2 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) Abstract MCL is a well-characterized clinically aggressive lymphoma with a poor prognosis. Recent research findings have slightly improved the outcome of this neoplasm. The addition of rituximab to conventional chemotherapy has increased overall response rates, but it does not improve overall survival with respect to chemotherapy alone. The use of intensive frontline therapies including rituximab and consolidated by ASCT ameliorates response rate and prolongs progression-free survival, but any impact on survival remains to be proven. Furthermore, the optimal timing, cytoreductive regimen and conditioning regimen, and the clinical implications of achieving a disease remission even at molecular level remain to be elucidated. The development of targeted therapies as the consequence of better dissection of pathogenetic pathways in MCL might improve the outcome of conventional chemotherapy in most patients and spare the toxicity of intense therapy in a minority of MCL patients characterized by a relatively indolent disease. Patients not eligible for intensive regimens, such as hyperc-vad, may be considered for less demanding therapies, such as the combination of rituximab either with CHOP or with purine analogues, or bendamustine. Allogeneic SCT can be an effective option for relapsed disease in patients who are fit enough and have a compatible donor. Maintenance rituximab may be considered after response to immunochemotherapy for relapsed disease, although there are currently no data to recommend this approach as the first-line strategy. As the optimal approach to the management of MCL is still evolving, it is critical that these patients be enrolled in clinical trials to identify better treatment options Elsevier Ireland Ltd. All rights reserved. Keywords: B-cell lymphomas; Cyclin D1; bcl-1; Allogeneic transplantation 1. General information 1.1. Definition Mantle cell lymphoma (MCL) is currently defined as a unique type of B-cell lymphoma composed of monomorphic small to medium-sized lymphoid cells with irregular profile in their nuclei and a CCND1 translocation [1]. It has been postulated that MCL could arise from a peripheral B- cell of the inner mantle zone, mostly of naïve pre-germinal centre type. Interestingly enough, somatic hypermutations in immunoglobulin variable region heavy chain (IGHV) genes are detected in 15 40% of MCLs, indicating that some tumors originate in cells that may have experienced the mutational machinery of follicular germinal centre Incidence MCL accounts for 3 10% of all non-hodgkin s lymphomas (NHL) [1], with an incidence of about 0.4 per 100,000 person/years. In the US, the incidence rate has increased in the total population, particularly in the elderly. White males display substantial prevalence of MCL independently of any ethnic group [2 4]. A variation in geographical distribution has been observed for this lymphoma. In fact, a higher incidence of MCL has been reported in Switzerland and Northern Italy, with respect to the US, Canada, South Africa, England, Germany, and Hong Kong [5] Risk factors No risk factors have been clearly identified for MCL. For example, there are no convincing data concerning the role of chronic antigenic stimulation in the genesis of this lymphoma, although with rare exceptions [6,7], since there is not established evidence that viruses known to cause NHL in humans, such as Epstein-Barr virus, human T-cell leukemia/lymphoma virus, or others, could be involved in the pathogenesis of MCL. More recently, a case-control study has suggested an association between Borrelia burgdorferi infection and the risk of MCL development [8], although this association was suggested on the bases of serological tests and epidemiological data but not by the use of molecular methods. No correlation between MCL and inherited immunologic deficiency disease or other immunologic disorders has been reported. Several chemical substances, such as solvents, insecticides, pesticides and fertilizers, as well as dusts and particles, hair dyes, smoking and diet have been suggested as possible aetiological factors in NHL [9]. Pesticides [10], organophosphate insecticides [11] and phenoxy herbicides [12] have been suggested as causative agents in NHL in general in people whose work involves application of these substances [13,14]; accordingly, also MCL may occur in these workers. Occasional cases of MCL have been observed in families in which a first-degree relative was carrying this lymphoma or other NHLs. The tumor in these relatives appears at a younger age than in the parents, thus suggesting a genetic predisposition [15]. 2. Pathology and biology 2.1. Morphology MCL produces node enlargement that is macroscopically characterized by a homogeneous tan cut surface, with or without micronodular appearance. Three microscopic architectural patterns have been described in lymph nodes: enlarged mantle zone (26% of cases), nodular (13%) and diffuse (61%), which might represent different stages of tumor infiltration [16 18]. More recently, the so called in situ pattern has been added, which is characterized by only slightly enlarged mantle zones [19]. The most common pattern consists of a diffuse, monotonous subversion of lymph
3 80 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) node structure by a monomorphous population of small to medium-sized lymphoid cells with slightly to markedly irregular nuclei, usually resembling centrocytes. The other two patterns are defined by the presence of variably sized, vaguely circumscribed nodules. Tumor nodules surrounding usually atrophic reactive germinal centres characterize Mantle zone pattern. When these latter are lacking, the nodular pattern is present and it resembles a collection of primary follicles. The neoplastic population is frequently accompanied by scattered, characteristically pink, epithelioid histiocytes and hyalinized small vessels. MCL encompasses different cytological types [1], which should be recognized for a correct diagnosis. As previously mentioned, MCL is usually composed by cells slightly larger than normal lymphocytes, showing irregular or cleaved nuclei in the majority of cases with more dispersed chromatin, scant pale cytoplasm, and inconspicuous nucleoli. In Giemsa stained sections, the cytoplasm is pale blue to pale grey. Some exceptions to this general rule do exist. In some cases the nuclei are very regular and resemble small lymphocytes. The classical cytological appearance of MCL small cell variant is a monotonous proliferation of small/medium cells with irregular nuclei and inconspicuous nucleoli. This variant has been frequently recognized in patients with a leukemic and splenomegaly presentation without lymph nodes and has a more indolent clinical course [20]. In other situations, neoplastic lymphocytes closely resemble marginal zone lymphocytes, usually by virtue of their clear, relatively abundant cytoplasm. Less frequently, large nuclei with dispersed chromatin and a high proliferation fraction are observed [21]. These morphologically aggressive variants may resemble lymphoblasts (blastoid variant), occurring usually de novo and less frequently evolving from a pre-existing classical MCL [22], or are more pleomorphic. Pleomorphic MCL are composed of a more heterogeneous population of larger cells (Zoldan 1996) and their increased proliferation activity is usually lower than in blastoid cases [23,24]. The blastoid and pleomorphic variants are considered to be associated with a poorer prognosis. Some tumors may have discordant morphology with areas of pleomorphic cells intermingled with others with a classical morphology [25] (Table 1). In classic MCL, transformed large cells are not observed. Proliferation index evaluated by Ki-67 immunostaining appears a useful morphologic prognosticator [26]; proliferation activity may vary in different cases, but it is generally low, with a percentage of Ki-67 positive cells around 15 30%. In blastoid variant there is a high proliferative activity (Ki-67 positive cells > 40%) and sometimes a starry sky pattern similar to Burkitt s lymphoma [24,27]. In the spleen, MCL obliterates white pulp germinal centres and extends into the red pulp, conferring a macroscopic miliary aspect to the cut surface [28,29]. In cases with a leukemic phase, the splenic sinusoids are also involved. Cytologically, some cases may mimic splenic marginal zone lymphoma. In the bone marrow, MCL may grow with paratrabecular, nodular or interstitial distributions. It should be also noted Table 1 Cytological characterization of mantle cell lymphoma subtypes. Classical type - small to medium-sized indented nuclei with moderately dispersed chromatin. - scanty pale cytoplasm. - monotonous cell population. - occasional larger neoplastic cells infrequently interspersed. Small cell type - small round or slightly indented nuclei with dense nuclear chromatin. - mimicking lymphocytic lymphoma/b-cll with lack of prolymphocytes and paraimmunoblasts. Pleomorphic type - mixture of tumor cells with nuclei of different sizes (medium-large) and shapes mimicking large B cell lymphoma. - nuclear chromatin plumed or pale. - moderate amount of cytoplasm. Blastic type - monomorphic sheets of small to medium-sized blasts with fine dispersed chromatin mimicking lymphoblastic lymphoma/all. - narrow rim of cytoplasm. - frequent apoptotic bodies. Modified from Tiemann M that bone marrow involvement may consist also of prominent intrasinusoidal involvement [30]. Any portion of the gastrointestinal tract may be involved by MCL, usually under the form of many sessile or pedunculated polyps throughout the entire length of the small and large intestine in a pattern termed multiple intestinal lymphomatous polyposis [31 34]. Rarely, lymphoepithelial lesions (usually associated with MALT lymphoma) may occur. Since multiple intestinal polyposis may be a manifestation also of follicular lymphoma, a correct differential diagnosis is required Immunophenotype The cells of MCL express high levels of monotypic surface immunoglobulin, usually sigm+ or IgD+, more frequently with lambda than kappa restriction. They are usually CD5+, CD43+ and express the B-cell-associated-antigens (CD19, CD20, CD22, CD79a and CD79b). Neoplastic cells are usually negative for CD3, CD23, CD11c, CD10 and BCL6. Aberrant phenotypes have been described, sometimes in association with blastoid/pleomorphic variants; these variants include negativity for CD5 (12% of cases), and positivity for CD10 (8%), CD23 (21%) [35], bcl-6 (12%), and MUM1 (35%) [36]. CD21+ Mantle cells often show a strong alkaline phosphatase enzyme activity [37]. A disorganized meshwork of follicular dendritic cells, detectable by stains for CD21, CD23 or CD35, is prominent. Strong immunohistochemical expression of bcl-2 protein can be observed. The bcl-2 positive nature of mantle cells and the bcl-2 negativity of residual follicular centre cells may highlight mantle zone or nodular patterns. MCL characteristically display nuclear positivity for cyclin D1 (bcl-1), which is strongly associated with all variants of this lymphoma, including the small group of CD5-negative cases. Recently,
4 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) SOX11 expression has been demonstrated in many MCL [38] and, most importantly, in those rare cyclin D1-negative MCL [39] Genetic features Immunoglobulin heavy and light chain genes are rearranged in MCL. Variable region genes are unmutated in the majority of the cases, while in 20 30% of the cases IgG genes show somatic hypermutation. It has been hypothesized that MCL, even the cases with unmutated IgH genes, might derive not from pregerminal centre B-cells of the mantle zone as previously believed, but from marginal zone or peripheral blood memory B-cell which have undergone an extra-follicular T- independent antigen response [40]. The mutational status of the IGHV genes in MCL, in contrast to CLL, does not correlate with survival [41]; however, MCL with a leukemic, non-nodal clinical presentation have more frequently mutated IGHV genes and have a longer survival [20]. MCL shows a biased usage of VH genes, suggesting a process driven by common antigen selection; VH3-21, VH- 23 and VH34 are the most common involved families [42,43]. Cases with leukemic or extra-nodal MCL seem to have a better prognosis when compared with patients with nodal involvement and this difference is associated with a higher rate of mutated IGHV [20,44]. Leukemic cases have a biased usage of VH4-39. Cases bearing VH3-21 genes seem to have less genomic imbalances and a trend for a better survival [45]. The translocation t(11:14) juxtaposes the cyclin D1 gene (CCND1) at 11q13 to the immunoglobulin heavy chain (IgH) promotor locus at chromosome 14q32. This translocation may be implicated in the pathogenesis and development of lymphomas, and is detected by conventional cytogenetics in up to 65% of MCLs. However, using different fluorescent in situ hybridization (FISH) techniques, it can be found in virtually all cases of MCL [46]. Immunohistochemistry can still be false negative (although rarely), mainly due to the quality of the material. Polymerase chain reaction (PCR) is only positive in 20 30% due to the widely scattered breakpoint region on 11q13, but when it is positive, PCR is an excellent tool for molecular follow-up studies [47]. t(11:14) results in overexpression of cyclin D1, a member of the D-type G1 cyclin, which regulate the early phases of the cell-cycle [48] and that is not expressed in normal lymphocytes [49 54]. Cyclin D1, like other cyclins, forms complexes with cyclin-dependent kinases (CDK4 and CDK6) and leads to phosphorylation and inactivation of tumor suppressor gene retinoblastoma (RB1). RB1 plays a master role in the G1-S transition by sequestering and inactivating E2F transcription factors involved in the transactivation of essential genes required for S phase entry and DNA replication, including cyclin E [55]. The initial phosphorylation of RB1 by cyclin D1/CDK4-6 initiates the release of E2F transcription factors, promoting the accumulation of cyclin E/CDK2 complexes that will produce the irreversible inactivation of RB1 and the subsequent progression into S phase. The cyclin D1/CDK4-6 complex also binds the CDK inhibitor p27kip1, which both stabilizes the activity of cyclin D1/CDK4 and sequesters p27 preventing its inhibition the subsequent activation of other CDK complexes required for cell cycle progression [56]. Thus, cyclin D1 overexpression is directly related to the pathogenesis of MCL by overcoming the suppressor effect exerted by retinoblastoma protein in the G1/S transition. The pathogenetic role of cyclin D1 activation in human neoplasia is suggested by the ability of cyclin D1 overexpression to transform cells in vitro and contribute to B-cell lymphomagenesis in transgenic mice [57,58]. In addition to inappropriate and constant expression of cyclin D1, MCL show a high expression of p27, probably because the p27 is sequestered in complexes containing cyclin D1, thereby blocking its cell cycle inhibitory function [56]. More recently, gene expression profile analysis had identified rare MCL, which lacked cyclin D1 expression, but had a gene expression signature typical of MCL. These cases seem to have a clinical behavior and secondary genetic alteration profile similar to conventional MCL. Cyclin D1 negative MCL frequently express variant cyclin D2 (CCND2) or cyclin D3 (CCND3) with translocations such as of the CCND2 gene from chromosome 12p13 to the Ig kappa locus (IgG@) at 2p12 or a novel cryptic t(2;14)(p24;q32) targeting MYCN a new lymphoma oncogene associated with blastoid MCL [59,60] resulting in deregulation of similar intracellular pathways in CCND1-negative and -positive MCL [61 63]. These findings suggest that the deregulation of other cyclins may be an alternative mechanism to cyclin D1 overexpression in MCL tumorogenesis. In addition to cyclin D1 deregulation, non-random secondary chromosomal alterations are also required for MCL pathogenesis. Accordingly, MCL represents the lymphoma subtype with the highest number of cytogenetic alterations. Secondary chromosomal aberrations including gains in 3q26 (31 50%), 7p21 (16 34%) and 8q24 (16 36%:MYC) as well as losses of 1p 13-p31 (29 52%), 6q23-27 (23 38%), 9p21 (18 31%), 11q22-23 (21 59%), 13q11-q13 (22 55%), 13q14-q34 (43 51%) and 17p13pter (21 45%) has been reported. Trisomy 12 was found in 25% of cases [1]. Crucial target genes alterations have been reported. Deletions of the INK4a/ARF locus on 9p21, which encodes the tumor suppressor genes p14 and p16 that inhibit cell cycle progression like p27 (14 20%) have been associated with more aggressive (blastic) histology [27,59]. Mutations of p53 in 17p13 (10 25%) are associated with a more aggressive histology and a shorter survival [27,64,65]. Deletion of 11q22-23 containing the ataxia telangiectasia mutated (ATM) tumor suppressor gene or point mutations in the ATM gene are also seen in about 25 50% of MCL cases [59,65,66]. Upto50% of patients demonstrate activation of the Wnt signalling pathway, with the consequent incorporation of beta-catenin into a transcriptionally active complex in the nucleus and the activation of multiple target genes, including cyclin D1 and c-myc [67].
5 82 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) A multivariate analysis showed that the evaluation of 3q and 9q alterations and the quantitative measurement of tumor cell proliferation [59,68] allow the definition of prognostic subgroups [63]. In pleomorphic and blastoid variants, tetraploidy has been also observed [24]. The presence of t(8;14)(q24;q32) with MYC translocation occurs rarely and is associated with an aggressive clinical course. Oncogenic alterations have been found in several genes targeting cell cycle regulatory elements and the DNA damage response pathway. Highly proliferative and clinically aggressive MCL carry oncogenic alterations in the two major regulatory pathways, INK 4a/CDK4/RB1 and ARF/MDM2/p53, respectively, which are involved in cell cycle control and senescence [59,69 71]. Recently, it was reported that PI3 K/Akt pathway is constitutively activated in patients with blastoid variants and a small subset of typical MCL cases [72]. Akt promotes cell growth, cell survival, and tumorogenesis by phosphorylaying multiple proteins. Akt enhances cell survival by promoting activation of NFkb, a transcription factor that turns on antiapoptotic genes. Akt also increases protein translation, and hence cell growth, by promoting the phosphorylation of mammalian target of rapamycin (mtor) and p70s6 kinase and favors tumorogenesis by phosphorylating MDM-2, a negative regulator of the p53 tumor suppressor. Recent data suggest that AkT and mtor have different functional characteristics in MCL [73]. mtor forms the complexes mtorc1 (mtor-raptor) and mtorc2 (mtor-rictor), which have distinct substrates and mechanisms of activation [74]. The best-known substrates of TORC1 are ribosomal protein S6 and 4E-EBP1. Recent genetic studies in a murine model demonstrated that phosphorylation of 4E-BP1 is a key step in the oncogenic pathway downstream of AKT/mTOR, while phosphorylation of S6 was dispensable. Phosphorylation of 4E-BP1 leads to its dissociation from eif4 resulting in increased translation of key proteins including cyclin D1, c-myc and MCL- 1. The main substrate of mtorc2 is AKT. Rapamycin and its analogues (rapalogs) are allosteric inhibitors of the mtorc1 complex that block some but not all mtorc1 functions and have no effect on mtorc2 [75]. Inhibiting the PI3 K/Akt pathway with chemical inhibitors of either Akt or its upstream activator PI3 K it reduces the phosphorylation of involved proteins, in addition to reducing NF-kB activation in the MCL cells. These effects might correlate with increased apoptosis and decreased proliferation of the MCL cells. Actually, rapalogs do not induce apoptosis of MCL cells in vitro, but most studies report induction of Go/G1 arrest [76 78]. The mechanisms of cell cycle arrest have remained ill defined and effects on cyclin D1 and p27 differ between different studies. One explanation for this variability could be that GSK-3, which promotes nuclear export and proteasomal degradation of cyclin D1, is inactivated by phosphorylation through either AKT or mtor. Thus, mtor inhibitors will increase cyclin D1 proteolysis only when inactivation of GSK-3 is dependent on mtor but not AKT [79]. Regarding the alterations of the genes targeting the mechanisms involved in genome stability, inactivating mutations of ATM gene, at 11q22-23, as previously reported, have been detected in several patients with MCL [66]. ATM inactivation is associated with a high number of chromosomal alterations suggesting that its deregulation is important for the accumulation of chromosomal alterations [80]. 3. Diagnosis 3.1. Clinical presentations Usually, MCL occurs in adults with a median age ranging between 60 and 65 years, and a high male-to-female ratio [81,82]. At diagnosis, 80% of patients or more have a Karnofsky performance status >70 [82,82], 30% have systemic symptoms [84], and 70% or more have disseminated disease (stage III or IV disease) [25,81,83,84]. At presentation, there is involvement of lymph nodes (75%), spleen (massive splenomegaly in 45 60% of cases), liver (hepatomegaly in 35%) [84], Waldeyer s ring, bone marrow (>60%) [82], blood (13 77%) and extranodal sites, especially the gastrointestinal tract (GI). MCL can involve any region of the gastrointestinal tract, occasionally presenting as multiple intestinal poliposis. Less commonly, skin, lung, breast, soft tissue, salivary glands, and orbit are involved [23]. Generalized lymphadenopathies is the most frequent clinical finding, but isolated splenomegaly without lymphodenopathies has been occasionally observed [81,82]. These patients present with a leukemic form, usually with splenomegaly. Generally they have an indolent disease and long survival (5 12 years) and may be characterized by a negative staining for SOX11 [44]. An extranodal organ as the exclusive site of disease is observed in 25% of cases. More than two extranodal sites are contemporaneously involved at diagnosis in 30 50% of cases. CNS involvement at diagnosis is rare (<5%), but there is an actuarial 5-year risk of up to 26%, usually as a late event in the clinical evolution of the disease especially in patients with blastoid histology, high proliferative index, and high LDH serum levels [85,86]. Since this malignancy involves bone marrow in more than 60% of cases [87,88], peripheral blood abnormalities are frequent (20 55% of cases), and a leukemic phase resembling chronic lymphocytic leukemia is observed in one fourth of cases [89]. Atypical lymphoid cells may be observed in the peripheral blood in absence of lymphocytosis and they may be detected by flow cytometry in virtually all the patients [90,91]. A very aggressive leukemic form has been reported in a few patients with blastoid morphology, complex karyotypes, occasionally with 8q24 anomalies and a median survival of 3 months [92]. Anemia, high LDH and increased 2-microglobulin serum levels may be detected in half of patients. A monoclonal serum component, usually at low levels, has been reported in 10 30% of cases [81,93,94].
6 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) Less than 30% of patients present with GI symptoms such as bleeding or abdominal pain. However, the great majority of MCL patients show GI tract involvement at the time of diagnosis, not uncommonly in the form of minute lymphoid infiltrates. In fact, it has been reported that MCL was present histologically in the lower GI tract of 88% and in the upper GI tract of 43% of patients who underwent endoscopy. Notably, microscopic evidence of MCL was found in 84% of patients with normal visual findings by lower endoscopy and in 45% of patients with macroscopically normal findings by upper endoscopy. It is noteworthy that most of patients with GI MCL presented with advanced stage of disease due to the presence of bone marrow involvement so that the use of endoscopy resulted in changes in clinical management in only few patients (4%) [95]. Multiple lymphomatous polyposis is a rare form of intestinal involvement in MCL. This form arises with remarkable male predominance, presenting with weight loss, diarrhea, weakness, abdominal pain, rectal bleeding, and anemia. It is often associated with large tumor masses and regional lymphadenopathies [33,96]. On the other hand, cases with exclusive GI involvement tend to have a slightly more indolent course. 4. Staging 4.1. Staging procedures Complete staging work-up for MCL is the same as that used routinely for nodal NHL. It includes an accurate physical examination, complete haematological and biochemical exams, total-body computerized tomography, optional GI examination, and bone marrow aspirate and biopsy. The correlation between peripheral blood counts and marrow involvement is variable. A leukemic phase is observed in 20 25% of cases [89]. The most frequent intrathoracic abnormality is mediastinal or hilar adenopathy, which needs computerized tomography for an adequate evaluation. The presence of pulmonary masses or pleural effusions should be verified histologically. (18F)Fluorodeoxyglucose Positron Emission tomography (FDG-PET) scanning showed a high sensitivity for the detection of lymph node involvement and higher FDG-uptake was shown in patients with the more aggressive blastoid variant in comparison with common MCL [97]. However, sensitivity of extranodal involvement is lower and routine use of FDG-PET is not recommended before treatment for patients with incurable, routinely FDG-avid, aggressive histologies such as MCL, unless response rate is a major end point of the trial [98]. Similarly, FDG-PET cannot be recommended for routine post therapy assessment and relapse surveillance because CT-based designation systems had equivalent prognostic value [97,99]. Furthermore, the addition of rituximab to polychemotherapy resulted in reduced positive predictive value and sensitivity of mid and post therapy PET in patients with MCL. Therefore, positive PET imaging in residual masses of these patients requires histological confirmation before to change the therapeutic plan [100]. Upper endoscopy and colonscopy are indicated for patients with GI symptoms. As asymptomatic GI involvement is common, colonscopy with several biopsy samples of macroscopically evident lesions should also be performed in patients with limited clinical stage, to exclude advanced stages which may change clinical management [95]. Under certain circumstances, special staging procedures are required. For instance, CNS MRI and CSF cytologic examination is indicated in patients with neurological symptoms, or blastoid variant [85,86]. Although extremely rare, bone lesions should be confirmed by routine X-ray studies, CT scan and/mri and biopsied if possible. Ultrasonography and MRI are useful to investigate the involvement of breast, soft tissue, salivary glands, or orbits. Finally, PCR analysis of bcl-1 rearrangement and sequencing of IgH genes can be used to detect lymphomatous cells in peripheral blood, with a 44% of positive bcl-1 rearrangement, 44% of negative bcl-1 but positive immunoglobulin genes rearrangement and 12% of both negative procedures [101] Staging system The standard staging system used for MCL is the same as that proposed for Hodgkin s disease at the Ann Arbor Conference in 1971, and largely used for most NHL [102]. The Ann Arbor staging system reflects both the number of sites of involvement and the presence of disease above or below the diaphragm. This staging system considers four stage of disease: Stage I: involvement of a single lymph node region (I) or a single extranodal site (IE). Stage II: involvement of two or more lymph node regions on the same side of the diaphragm (II) or localized involvement of an extralymphatic site (IIE). Stage III: involvement of lymph nodes regions on both sides of the diaphragm (III) or localized involvement of an extralymphatic site (IIIE) or spleen (IIIs) or both (IIIEs). Stage IV: diffuse or disseminated involvement of one or more extralymphatic organs with or without associated lymph node involvement. Localized involvement of liver or bone marrow is also considered stage IV. Patients are divided in two subsets according to the presence (A) or absence (B) of systemic symptoms. Fever of no evident cause, night sweats and weight loss of more than 10% of body weight are considered systemic symptoms. Even though it is a frequent accompanying symptom, itch should not be considered as a systemic symptom. The presence of bulky mass, such as a lesion of 10 cm or more in the longest diameter is designated as X, while the extranodal involvement should be identified by a symbol (O: bone, L: lung, D: skin, etc.).
7 84 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) Minimal residual disease Molecular monitoring of minimal residual disease (MRD) in MCL provides an early endpoint to assess the curative potential of novel chemotherapy approaches and predicts relapse due to its sensitivity to detect tumor cells contained in the graft in autografting programs [ ]. MRD in MCL is currently detected by PCR, analyzing the rearrangement of bcl-1 (see Section 2.3). Since this rearrangement is detectable in 50% of patients with MCL, an alternative strategy of PCR amplification and sequencing of IgH genes is advisable. The rearrangement of variable, diverse and joining segments of IgH genes generates unique DNA sequences that are clone specific. These sequences are named complementarydetermining regions (CDR) and code for the antigen binding site [109]. Clone-specific primers and probes can be obtained from CDR sequences and used for the PCR detection of lymphoma cells. Comprehensively, the bcl-1/igh translocation and clonally rearranged IgH genes provided molecular markers for detection and follow-up of MRD by PCR amplification in >70 90% of cases [103]. The same methods can be used to detect lymphomatous cells in peripheral blood during staging (see item #4.1). However, because of limited patient numbers and lack of relevant patient populations achieving MRD negativity, a useful prognostic algorithm could not be established by qualitative PCR in MCL [ ]. Recently, a sensitive quantitative real-time PCR (RQ-PCR) using allelespecific primers in combination with consensus probes has been shown to be a useful tool for MRD monitoring clinical trials in MCL [113]. A quantitative IGH RQ-PCR assay based on the design of individual allele-specific forward primers matching the clonal VH-DH-JH region for MRD quantification allow to estimate tumor cell load over a wide dynamic range of 5 log levels up to a highly reproducible sensitivity level of Quantitative MRD assessment during treatment allowed evaluation of the effects of single treatment elements on tumor clearance in peripheral blood and bone marrow [114]. Furthermore, molecular monitoring of MRD by IGH RQ-PCR provides good kinetic evidence of the presence of active disease (M-rel). The presence of a documented M-rel without additional signs of disease activity has been treated delivering immunotherapy. This approach resulted in a progressive decrease in tumor burden, which was effectively monitored by IGH RQ-PCR. The majority of patients reverted to PCR negativity preventing the clinical relapse [115,116]. Therefore, the use of RQ-PCR may be an effective tool to control the clinical activity of therapy and tailor different treatments for patients with MCL. 5. Prognosis 5.1. Natural history The MCL is a disease generally associated with rapid progression, only temporary responses to chemotherapy, and a high recurrence rate resulting in a poor long-term prognosis with reported median overall survival (OS) of 3 4 years [82, ]. However, some patients succumb to their disease in less than 6 months, whereas others (8%) survive more than 10 years. The blastoid and pleomorphic variants appear more aggressive, with a median OS of 18 months [1,120]. Interestingly, recent studies identified a subset of patients with a leukemic and splenomegaly presentation without lymphnodes, who have an indolent lymphoid proliferation and longer survival (5 12 years) even without the need of any treatment, suggesting that the biological behavior of MCL may be more heterogeneous that initially thought [20,44]. It is noteworthy that median OS of patients with advanced non blastoid or pleomorphic MCL almost doubled during the past 30 years from 2.7 years up to 4.8 years in recent studies. The superior outcome may be a result of the improvement of treatment regimens including immunochemotherapy or high-dose chemotherapy supported by autologous stem cell transplantation (HDC-ASCT), advances in general supportive care and new diagnostic tools [121]. MCL is generally now treated earlier and more aggressively than in the past. Unfortunately, with the current treatments, including very aggressive approaches, MCL remains an incurable disease. Recently, it has been reported an institutional experience, which included a treatment policy of watching asymptomatic MCL patients without therapy until disease symptoms develop [122]. The authors identified approximately a third of patients who could be managed in this manner with a subset not requiring therapy for a year or more. They attributed these findings to inherently lower risk disease in this group, as these patients tended to be younger and had better performance status. Moreover, the asymptomatic group of patients had a significantly better survival rate than patients who were treated immediately. These data suggest that it could be reasonable to use a close observation strategy with deferred therapy in selected asymptomatic patients with newly diagnosed MCL [116]. Survival curves for patients with MCL do not show a plateau [123], with a median time to relapse of 24 months [124]. Relapse usually involves bone marrow, lymph nodes, and GI, having a preference for initial sites of disease. CNS involvement has been observed in 20% of patients after a median follow-up of 18 months [125], but brain relapses can also be observed after 4 5 years of follow-up [85,86,126]. Usually, CNS relapse is observed in patients with progressive leukemic disease and blastoid variant, and is associated with neurological symptoms and positive CSF cytology examination. In these patients, survival after relapse is <2 months [126]. Transformation of MCL to a large-cell lymphoma does not appear to occur. However, loss of a mantle zone growth pattern, increase in nuclear size, pleomorphism and chromatin dispersal, and increase in mitotic activity may be observed in some relapses fulfilling the criteria for a blastoid or pleomorphic MCL [1]. Blastoid transformation occurs in few cases; this event is related to leukocytosis, elevated LDH and high
8 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) Ki-67, and with a median survival time from transformation of 4 months [127], with a worse OS in patients older than 60 and with lymphoma with an increased proliferating index [25,26] Prognostic factors The evaluation of new therapeutic approaches for patients with MCL requires a correct risk stratification. Several variables like age >65 years, poor performance status, advanced disease, leukemic phase, splenomegaly, high LDH serum levels, bulky disease, hepatomegaly, number of nodal sites involved and anemia have been reported as indicators of worse survival [23,81,93,117,120, ]. All these variables correlated with survival but none of them was validated as a tool for the selection of therapy. The value of the IPI, largely and successfully used in other aggressive lymphomas, is debated [23,81,93,131,132]. The Follicular Lymphoma International Prognostic Index (FLIPI) [133] represents an improvement when compared with the IPI [128], but it is still not the ideal prognostic index for MCL [134]. Recently, a specific MCL prognostic index (MIPI, Mantle-cell lymphoma International Prognostic Index) for advanced stages, based on four independent prognostic factors (age, ECOG performance status, LDH and white blood cell counts) has shown the capability to clearly separate MCL patients treated with CHOP ± rituximab or MCP regimens into three prognostic subgroups [135] (Fig. 1). In one monocenter experience, MIPI did not show the same prognostic value in patients treated with a more intensive regimen (R-Hyper-CVAD/MTX-AraC; see later), whereas a number of multicenter trials have confirmed the validity of MIPI also after a more aggressive regimen [ ]. The blastoid and pleomorphic variants seem to be associated with worse outcome [1]. The proliferation index has been Fig. 1. MIPI: Mantle cell lymphoma Prognostic index. This figure was originally published in Ref. [135]. Fig. 2. Progrnostic role of cell Proliferation (Ki-67). This figure was originally published in Ref. [25]. recognized as the best predictor of survival in MCL patients [23,25] (Fig. 2). Ki67 stain may have a profound effect on therapeutic options in risk-adapted therapeutic strategies [26,135], but immunohistochemical techniques are semiquantitative in nature, and in a recent multicenter study, the inter-laboratory variation of the Ki-67 immunostaining was surprisingly high [139]. Recently, a standardized measure of Ki-67 determination has been proposed [140]. A signature based on the expression of 20 genes designed by gene expression profiling clearly discriminates subrgroups of patients with MCL with different median OS [59]. Other adverse prognostic parameters include complex karyotypes and specific chromosomal alterations, such as gains in 3q, 12q, Xq and losses in 9p, 9q and 17p [63, ], inactivation of TP53 [145], CDKN2A locus [146] and high levels of cyclin D1 or MDM2. However, they lose their predictive value in multivariate analysis suggesting that the proliferation activity may represent an integrator of different oncogenic events [59]. On the contrary, the quantitative gene expression of MYC, MDM2 and CCND1 maintain their prognostic value independently of the tumor proliferation [147]. Moreover, the inactivation of the two regulatory pathways INK4a/CDK4 and ARF/p53 was associated with a short survival independently of Ki-67 proliferation index [69]. It is noteworthy that the impact of the chromosome 3q and 9q alterations on survival is independent of the microarray proliferation signature, while their integration with the quantitative measurement of tumor cell proliferation may improve the definition of prognostic subgroups of the patients [59,68]. Recently, it was reported a quantitative gene expression-based (qrt-pcr) prognostic model that is applicable to fresh frozen as well as to paraffin-embedded tissue specimens. The survival predictor was composed of five genes: RAN, MYC, TNFRSF10B, POLE2, and SLC29A2. All genes are involved in the biologic process of proliferation and were included in the abovedescribed gene expression-based proliferation signature [59]. This model predicts survival of patients with MCL with widely disparate outcome and seems to be superior to the immunohistochemical marker Ki-67 [148]. The integration
9 86 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) of these molecular and genetic prognostic predictors may become an essential tool in the clinical, but it still needs proper validation. 6. Treatment 6.1. Treatment of limited disease (stage I II) The proportion of patients with stage I or II is rather low in MCL ranging from 5% to 25% in different series [135]. A standard treatment option for patients with stage I II MCL has not been established. Combined treatment with 3 4 cycles of primary systemic conventional-dose polychemotherapy followed by involved field radiotherapy is suitable for individual clinical use on a type R basis (Fig. 3). This strategy obtained long term remissions in 11 out of 16 patients treated in British Colombia, on a type 3 level of evidence [149]. Radiation therapy alone has been used for patients with limited disease in retrospective series [117,150,151], obtaining a complete remission (CR) in 64 80% of cases. Almost 34 70% of responders experienced relapse after 8 99 months from treatment, with 30% of patients alive at a median follow-up of 13 years Treatment of advanced disease (stage III IV) Some selected patients with MCL can be managed with wait and watch strategy, on a type 3 level of evidence (Fig. 3). These patients have more indolent tumors or low risk, who typically present with lymphocytosis, a few enlarged lymph nodes, splenomegaly, and a Ki-67 index < 10% [135,152]. Preliminary results from a single institution showed that one third of patients with asymp- Fig. 3. Clinical recommendations outside of clinical trials. This Figure was originally published in Blood Online Martin Dreyling, Wolfgang Hiddemann for The European MCL Network Current treatment standards and emerging strategies in mantle cell lymphoma Hematology, Jan 2009; 2009: tomatic MCL were observed for more than three months before initiating therapy. Treatment was postponed for more than one year in 14% of cases and more than five years in 3%. Notably, OS of this subgroup was similar to that of patients who are treated immediately at diagnosis [122]. Unfortunately, none of potential prognostic factors was able to predict which patients would progress slowly and reported data come from a retrospective analysis of a small group of cases. One recent small series suggested that especially SOX-11 negative cases display a more indolent course but these data have to be validated prospectively [44]. Thus, to conclude that a watch and wait policy could be indicated for patients with indolent MCL may be premature, and the general practice, on a type R basis, is to start therapy at diagnosis, while tailoring treatment to the patient s age and co-morbidity. Despite an improvement in survival during the last 30 years, the long-term outcome for most patients with MCL is still poor with a median OS of 4.8 years and a tendency to relapse early and to respond insufficiently to salvage treatment [121]. There is no evidence that current treatment programs are curative [153]. However, patients with advanced or symptomatic disease are treated with combination chemotherapy to decrease tumor bulk and alleviate symptoms. There is no widely accepted standard first-line therapy for newly diagnosed MCL. As MCL usually presents at an advanced stage, systemic treatment is the standard, and surgery is usually not employed, but may be of value in patients with MCL involving the GI tract presenting with bowel obstruction, on a type R basis. Similarly, patients with massive splenomegaly often benefit from splenectomy to relieve symptoms and improve blood counts [154,155]. Likewise, radiation therapy is usually reserved to localized disease, both alone or added to chemotherapy, ona type R basis [149,150] Standard-dose chemotherapy Anthracycline-based regimens are considered the cornerstone of upfront MCL therapy, despite conflicting evidence regarding the real benefits of the anthracycline component. However, CR rates (CRRs) with CHOP (cyclophosphamide, doxorubicin, vincristine and prednisone) regimen were consistently lower in MCL in comparison with other lymphomas, ranging between 13% and 51% in the reported series, on a type C basis [156]. Actually, randomized trials comparing anthracycline-based regimens with chemotherapy combinations without this drug showed controversial results, on a type 2 level of evidence [118,123,157], while, in a randomized trial, treatment with CHOP or MCP (mitoxantrone, chlorambucil and prednisone) showing no difference between the two regimens in terms of response rate (ORR: 87% vs. 73%; CRR: 15% vs. 20%), time to treatment failure (TTF) (21 months vs. 15 months) and OS (61 months vs. 48 months). CHOP produced more nonhematologic toxicities, while MCP was associated with a higher rate of myelosuppression [158].
10 S. Cortelazzo et al. / Critical Reviews in Oncology/Hematology 82 (2012) Fludarabine monotherapy has only moderate efficacy in patients with MCL [159]: In relatively small phase II studies, reported ORR were generally low (40 50%) with a CRR of 20 30% and remission periods tended to be short (4 8 months). In patients with relapsed or refractory MCL, the ORRs are even less favorable. It is therefore recommended to use fludarabine monotherapy only in the setting of pretreated MCL patients when other therapeutic options are not available (type R basis). Fludarabine-containing chemotherapy regimens that include anthracyclines or alkylating agents are effective in MCL, but it remains unclear whether or not this will lead to improved survival rates of MCL patients [159]. In a recently completed trial of the European MCL Network named MCL Elderly Trial, patients 60 years old and ineligible for ASCT were randomly allocated to receive 8 courses (once every 3 weeks) of R-CHOP or 6 courses (once every 4 weeks) of rituximab, fludarabine, cyclophosphamide (R- FC) chemotherapy. After a second randomization, patients in clinical remission received maintenance treatment with either interferon- (3 3 M IU; Pegylated Interferon 1 g/kg weekly) or rituximab (375 mg/m 2 ; at 2-monthly intervals). Maintenance treatment was given until clinical relapse. Definitive data are not still available but probably this trial will provide important therapeutic recommendations on the efficacy of fludarabine-based chemoimmunotherapy and maintenance treatment with type 1 or 2 evidence level. 2-Chlorodeoxyadenosine (2-CDA), as a single agent, has shown an 81% ORR (CRR 42%) with a median PFS of 13.6 months and 81% of patients remaining alive at 2 years [160]. When combined with mitoxantrone the ORR was 100% (CR 44%) with a median response duration of 24 months, and a 4-year OS of 80% [161] High-dose chemotherapy supported by autologous stem cell transplant Improvements in transplantation technology combined with the poor outcome achieved with conventional treatment have lead to the widespread use of HDC-ASCT in the management of MCL. Overall, this strategy is usually restricted to younger patients and may potentially be hampered by the risk of secondary myelodysplastic syndromes and acute leukemias. Early trials of HDC-ASCT in MCL showed disappointing results, but they were plagued by small numbers, retrospective designs, and short follow-up [162]. More recently, evidence has emerged that autologous transplantation may be of benefit in MCL if used earlier during the course of the disease, particularly in first CR, on a type 3 level of evidence [ ]). Notably, the addition of cytarabine as part of the initial treatment seems to be associated with high CRR and improved outcomes after HDC-ASCT [164,165]. Similarly, ORRs >90% have been obtained with an alternating regimen of hyper-cvad (fractionated cyclophosphamide, vincristine, adriamycin, and dexamethasone) with high-dose cytarabine and methotrexate in 45 patients <65 years of age with advanced stage MCL. Hyper-CVAD/A-M chemotherapy has been associated with significantly better ORR (92% vs. 56%), 3-year EFS (73% vs. 28%) and 3- year OS (73% vs. 56%) compared to a historic control group treated with CHOP-like regimen, on a type 3 level of evidence [168]. At a median follow-up of 49 months, the OS and DFS rate at 5 years were 77% and 43%, respectively, with significant variations among IPI risk groups [132]. A prospective trial performed by European MCL Network randomly assigned 122 patients <65 years of age with advanced stage MCL in CR or PR after CHOP-like induction therapy to consolidation with HDC-ASCT or maintenance therapy with interferon alpha (IFN) [169]. In this study, after median follow-up of 6.1 years, a HDC-ASCT has been related to a significantly better 3-year PFS (54% vs. 25%) and trend towards improved OS (median OS 7.5 years vs. 5.4 years), on a type 2 level of evidence [170]. As expected, toxicity was significantly higher in the HDC-ASCT study arm in comparison to IFN (treatment-related mortality: 5% vs. 0%), whereas long-term effects were more frequently encountered under IFN maintenance. Notably, patients who received transplants in CR had a 3-year PFS of 71% in comparison to only 19% in the IFN study group. Thus, patients consolidated in first CR by HDC-ASCT may have a better outcome than patients treated by HDC-ASCT later in the course of their disease. This is supported by studies demonstrating persistence of lymphoma cells in autografts, even after extensive antibody ex vivo purging [171]. In fact, in the pre-rituximab era, early ASCT extended the median remission duration by 1 2 years, but most patients eventually experienced relapse. The lack of an obvious plateau in PFS after such a dose-intensified consolidation indicates that late disease control is a major problem. Incorporation of current or future monoclonal antibody therapies as in vivo purging or antibody maintenance might improve the prognosis of these patients Rituximab-based immunotherapy Rituximab alone. MCL are uniformly CD20 positive, expressing high levels of this cell-surface protein [172]. However, in MCL the anti-cd20 antibody rituximab (R-) showed somehow less impressive results than in other B-cell indolent malignancies. Rituximab has been tested as a single agent for both untreated and relapsed MCL patients, with an ORR of 27 30% and 2% CRR [ ], with response lasting 6 12 months and no differences between chemotherapy-naïve and pretreated patients [173,175]. Notably, the addition of four doses at 8-week interval after the conventional induction with four weekly doses or the use of 500 mg/m 2 did not significantly improve outcome [173,174]. Comprehensively, rituximab monotherapy is not adequate for MCL and should instead be used in combination with chemotherapy [176]. Nevertheless, rituximab alone has shown efficacy in the treatment of isolated molecular relapses [115,116]. These observations may underlie the observed benefit of maintenance therapy with rituximab (see below).
Mantle Cell Lymphoma
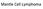 Mantle Cell Lymphoma Clinical Case A 56 year-old woman complains of pain and fullness in the left superior abdominal quadrant for the last 8 months. She has lost 25 kg, and lately has had night sweats.
Mantle Cell Lymphoma Clinical Case A 56 year-old woman complains of pain and fullness in the left superior abdominal quadrant for the last 8 months. She has lost 25 kg, and lately has had night sweats.
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
FOLLICULARITY in LYMPHOMA
 FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
Update: Non-Hodgkin s Lymphoma
 2008 Update: Non-Hodgkin s Lymphoma ICML 2008: Update on non-hodgkin s lymphoma Diffuse Large B-cell Lymphoma Improved outcome of elderly patients with poor-prognosis diffuse large B-cell lymphoma (DLBCL)
2008 Update: Non-Hodgkin s Lymphoma ICML 2008: Update on non-hodgkin s lymphoma Diffuse Large B-cell Lymphoma Improved outcome of elderly patients with poor-prognosis diffuse large B-cell lymphoma (DLBCL)
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Case 3. Ann T. Moriarty,MD
 Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Indolent Lymphomas: Current. Dr. Laurie Sehn
 Indolent Lymphomas: Current Dr. Laurie Sehn Why does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with current standard
Indolent Lymphomas: Current Dr. Laurie Sehn Why does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with current standard
Indolent Lymphomas. Dr. Melissa Toupin The Ottawa Hospital
 Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
LYMPHOMAS an overview of some subtypes of NHLs
 One of the confusing aspects of the lymphoid neoplasms concerns the use of the descriptive terms "leukemia" and "lymphoma." LYMPHOMAS an overview of some subtypes of NHLs Leukemia is used for lymphoid
One of the confusing aspects of the lymphoid neoplasms concerns the use of the descriptive terms "leukemia" and "lymphoma." LYMPHOMAS an overview of some subtypes of NHLs Leukemia is used for lymphoid
Pathology of the indolent B-cell lymphomas Elias Campo
 Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Diffuse Large B-Cell Lymphoma (DLBCL)
 Diffuse Large B-Cell Lymphoma (DLBCL) DLBCL/MCL Dr. Anthea Peters, MD, FRCPC University of Alberta/Cross Cancer Institute Disclosures Honoraria from Janssen, Abbvie, Roche, Lundbeck, Seattle Genetics Objectives
Diffuse Large B-Cell Lymphoma (DLBCL) DLBCL/MCL Dr. Anthea Peters, MD, FRCPC University of Alberta/Cross Cancer Institute Disclosures Honoraria from Janssen, Abbvie, Roche, Lundbeck, Seattle Genetics Objectives
Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma:
 1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
CLL: disease specific biology and current treatment. Dr. Nathalie Johnson
 CLL: disease specific biology and current treatment Dr. Nathalie Johnson Disclosures Consultant and Advisory boards Roche, Abbvie, Gilead, Jansson, Lundbeck,Merck Research funding Roche, Abbvie, Lundbeck
CLL: disease specific biology and current treatment Dr. Nathalie Johnson Disclosures Consultant and Advisory boards Roche, Abbvie, Gilead, Jansson, Lundbeck,Merck Research funding Roche, Abbvie, Lundbeck
Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo
 Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas NAIVE -B LYMPHOCYTE MEMORY CELL CLL MCL FL MZL Small cell size Low proliferation
Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas NAIVE -B LYMPHOCYTE MEMORY CELL CLL MCL FL MZL Small cell size Low proliferation
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Immunopathology of Lymphoma
 Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Prepared by: Dr.Mansour Al-Yazji
 C L L CLL Prepared by: Abd El-Hakeem Abd El-Rahman Abu Naser Ahmed Khamis Abu Warda Ahmed Mohammed Abu Ghaben Bassel Ziad Abu Warda Nedal Mostafa El-Nahhal Dr.Mansour Al-Yazji LEUKEMIA Leukemia is a form
C L L CLL Prepared by: Abd El-Hakeem Abd El-Rahman Abu Naser Ahmed Khamis Abu Warda Ahmed Mohammed Abu Ghaben Bassel Ziad Abu Warda Nedal Mostafa El-Nahhal Dr.Mansour Al-Yazji LEUKEMIA Leukemia is a form
HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD
 HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD OUTLINE High grade B-cell lymphoma with MYC and BCL2 and/or BCL6 rearrangements Patient presentation 2008/2016
HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD OUTLINE High grade B-cell lymphoma with MYC and BCL2 and/or BCL6 rearrangements Patient presentation 2008/2016
MANTLE CELL LYMPHOMA
 MANTLE CELL LYMPHOMA CLINICAL CASE PRESENTATION Martin Dreyling Medizinische Klinik III LMU München Munich, Germany esmo.org Multicenter Evaluation of MCL Annency Criteria fulfilled event free interval
MANTLE CELL LYMPHOMA CLINICAL CASE PRESENTATION Martin Dreyling Medizinische Klinik III LMU München Munich, Germany esmo.org Multicenter Evaluation of MCL Annency Criteria fulfilled event free interval
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU
 Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU Lecture outline Time 10:00 11:00 11:15 12:10 12:20 13:15 Content Introduction to lymphoma Review of lymphocyte biology
Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU Lecture outline Time 10:00 11:00 11:15 12:10 12:20 13:15 Content Introduction to lymphoma Review of lymphocyte biology
Indolent B-Cell Non-Hodgkin s Lymphomas
 Review Article [1] December 01, 1997 Myelodysplastic Syndromes [2] By John E. Seng, MD [3] and Bruce A. Peterson, MD [4] The indolent B-cell non-hodgkin s lymphomas are a diverse group of disorders that
Review Article [1] December 01, 1997 Myelodysplastic Syndromes [2] By John E. Seng, MD [3] and Bruce A. Peterson, MD [4] The indolent B-cell non-hodgkin s lymphomas are a diverse group of disorders that
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology. Songlin Zhang, MD, PhD LSUHSC-Shreveport
 From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
CLL & SLL: Current Management & Treatment. Dr. Isabelle Bence-Bruckler
 CLL & SLL: Current Management & Treatment Dr. Isabelle Bence-Bruckler Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of white blood cell B lymphocyte Lymphocytic Cancer
CLL & SLL: Current Management & Treatment Dr. Isabelle Bence-Bruckler Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of white blood cell B lymphocyte Lymphocytic Cancer
New Evidence reports on presentations given at EHA/ICML Bendamustine in the Treatment of Lymphoproliferative Disorders
 New Evidence reports on presentations given at EHA/ICML 2011 Bendamustine in the Treatment of Lymphoproliferative Disorders Report on EHA/ICML 2011 presentations Efficacy and safety of bendamustine plus
New Evidence reports on presentations given at EHA/ICML 2011 Bendamustine in the Treatment of Lymphoproliferative Disorders Report on EHA/ICML 2011 presentations Efficacy and safety of bendamustine plus
2012 by American Society of Hematology
 2012 by American Society of Hematology Common Types of HIV-Associated Lymphomas DLBCL includes primary CNS lymphoma (PCNSL) Burkitt Lymphoma HIV-positive patients have a 60-200 fold increased incidence
2012 by American Society of Hematology Common Types of HIV-Associated Lymphomas DLBCL includes primary CNS lymphoma (PCNSL) Burkitt Lymphoma HIV-positive patients have a 60-200 fold increased incidence
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Non-Hodgkin lymphoma
 Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
GENETIC MARKERS IN LYMPHOMA a practical overview. P. Heimann Dpt of Medical Genetics Erasme Hospital - Bordet Institute
 GENETIC MARKERS IN LYMPHOMA a practical overview P. Heimann Dpt of Medical Genetics Erasme Hospital - Bordet Institute B and T cell monoclonalities Rearrangement of immunoglobin and TCR genes may help
GENETIC MARKERS IN LYMPHOMA a practical overview P. Heimann Dpt of Medical Genetics Erasme Hospital - Bordet Institute B and T cell monoclonalities Rearrangement of immunoglobin and TCR genes may help
accumulation the blood, marrow, lymph nodes, and spleen.
 Chronic Lymphocytic Leukemia accumulation of mature-appearing appearing lymphocytes in the blood, marrow, lymph nodes, and spleen. CLL cells are: monoclonal l B lymphocytes that express CD19. CD5, and
Chronic Lymphocytic Leukemia accumulation of mature-appearing appearing lymphocytes in the blood, marrow, lymph nodes, and spleen. CLL cells are: monoclonal l B lymphocytes that express CD19. CD5, and
Solomon Graf, MD February 22, 2013
 Solomon Graf, MD February 22, 2013 Case Review of FL pathology, prognosis Grading of FL Grade 3 disease High proliferative index in grade 1/2 disease Pediatric FL Future of FL classification 57 yo man
Solomon Graf, MD February 22, 2013 Case Review of FL pathology, prognosis Grading of FL Grade 3 disease High proliferative index in grade 1/2 disease Pediatric FL Future of FL classification 57 yo man
Disclosures WOJCIECH JURCZAK
 Disclosures WOJCIECH JURCZAK ABBVIE (RESEARCH FUNDING), CELGENE (RESEARCH FUNDING); EISAI (RESEARCH FUNDING); GILEAD (RESEARCH FUNDING); JANSEN (RESEARCH FUNDING); MORPHOSYS (RESEARCH FUNDING), MUNDIPHARMA
Disclosures WOJCIECH JURCZAK ABBVIE (RESEARCH FUNDING), CELGENE (RESEARCH FUNDING); EISAI (RESEARCH FUNDING); GILEAD (RESEARCH FUNDING); JANSEN (RESEARCH FUNDING); MORPHOSYS (RESEARCH FUNDING), MUNDIPHARMA
Highlights of ICML 2015
 Highlights of ICML 2015 Jonathan W. Friedberg M.D. Director, James P. Wilmot Cancer Center Statistics, ICML 2015: a global meeting Almost 3700 participants. 90 countries represented. Attendees: USA 465
Highlights of ICML 2015 Jonathan W. Friedberg M.D. Director, James P. Wilmot Cancer Center Statistics, ICML 2015: a global meeting Almost 3700 participants. 90 countries represented. Attendees: USA 465
Brad S Kahl, MD. Tracks 1-21
 I N T E R V I E W Brad S Kahl, MD Dr Kahl is Associate Professor and Director of the Lymphoma Service at the University of Wisconsin School of Medicine and Public Health and Associate Director for Clinical
I N T E R V I E W Brad S Kahl, MD Dr Kahl is Associate Professor and Director of the Lymphoma Service at the University of Wisconsin School of Medicine and Public Health and Associate Director for Clinical
Update: New Treatment Modalities
 ASH 2008 Update: New Treatment Modalities ASH 2008: Update on new treatment modalities GA101 Improves tumour growth inhibition in mice and exhibits a promising safety profile in patients with CD20+ malignant
ASH 2008 Update: New Treatment Modalities ASH 2008: Update on new treatment modalities GA101 Improves tumour growth inhibition in mice and exhibits a promising safety profile in patients with CD20+ malignant
CLL & SLL: Current Management & Treatment. Dr. Peter Anglin
 CLL & SLL: Current Management & Treatment Dr. Peter Anglin Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of blood cell B lymphocyte Lymphocytic Cancer of white blood
CLL & SLL: Current Management & Treatment Dr. Peter Anglin Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of blood cell B lymphocyte Lymphocytic Cancer of white blood
Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL
 New Evidence reports on presentations given at ASH 2009 Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL From ASH 2009: Non-Hodgkin
New Evidence reports on presentations given at ASH 2009 Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL From ASH 2009: Non-Hodgkin
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent
 Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Aggressive Lymphomas - Current. Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre
 Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
B Cell Lymphoma: Aggressive
 B Cell Lymphoma: Aggressive UpToDate: Introduction: Risk Factors: Biology: Symptoms: Diagnosis: Ibrutinib approved for mantle cell lymphoma as 2nd line therapy. - Aggressive lymphomas are a group of malignant
B Cell Lymphoma: Aggressive UpToDate: Introduction: Risk Factors: Biology: Symptoms: Diagnosis: Ibrutinib approved for mantle cell lymphoma as 2nd line therapy. - Aggressive lymphomas are a group of malignant
MARIO PETRINI Ematologia PISA UO Ematologia - Pisa
 I LINFOMI NON HODGKIN A BASSO GRADO DI MALIGNITA PESCARA 2008 linfomi mantellari MARIO PETRINI Ematologia PISA Mantle Cell Lymphoma Typical (Classic) small to medium-sized Ly with scanty cytoplasm, irregular
I LINFOMI NON HODGKIN A BASSO GRADO DI MALIGNITA PESCARA 2008 linfomi mantellari MARIO PETRINI Ematologia PISA Mantle Cell Lymphoma Typical (Classic) small to medium-sized Ly with scanty cytoplasm, irregular
TRANSPARENCY COMMITTEE OPINION. 27 January 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 January 2010 TORISEL 25 mg/ml, concentrate for solution and diluent for solution for infusion Box containing 1
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 January 2010 TORISEL 25 mg/ml, concentrate for solution and diluent for solution for infusion Box containing 1
Defined lymphoma entities in the current WHO classification
 Defined lymphoma entities in the current WHO classification Luca Mazzucchelli Istituto cantonale di patologia, Locarno Bellinzona, January 29-31, 2016 Evolution of lymphoma classification Rappaport Lukes
Defined lymphoma entities in the current WHO classification Luca Mazzucchelli Istituto cantonale di patologia, Locarno Bellinzona, January 29-31, 2016 Evolution of lymphoma classification Rappaport Lukes
Patterns of Lymphoid Neoplasia in Peripheral Blood. Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure
 Patterns of Lymphoid Neoplasia in Peripheral Blood Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure Dr Baltrucki has received an honorarium for his participation as a faculty presenter in this
Patterns of Lymphoid Neoplasia in Peripheral Blood Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure Dr Baltrucki has received an honorarium for his participation as a faculty presenter in this
Marked improvement of overall survival in mantle cell lymphoma: a population based study from the Swedish Lymphoma Registry.
 Marked improvement of overall survival in mantle cell lymphoma: a population based study from the Swedish Lymphoma Registry. Abrahamsson, Anna; Dahle, Nina; Jerkeman, Mats Published in: Leukemia & lymphoma
Marked improvement of overall survival in mantle cell lymphoma: a population based study from the Swedish Lymphoma Registry. Abrahamsson, Anna; Dahle, Nina; Jerkeman, Mats Published in: Leukemia & lymphoma
The patient had a mild splenomegaly but no obvious lymph node enlargement. The consensus phenotype obtained from part one of the exercise was:
 Case History An 86 year old male was admitted to hospital with chest infection. Haematological examination subsequently revealed the following: Hb- 11.0 g/dl; WBC- 67.1 x 10^9/l; PLT- 99 x10^9/l; RBC-
Case History An 86 year old male was admitted to hospital with chest infection. Haematological examination subsequently revealed the following: Hb- 11.0 g/dl; WBC- 67.1 x 10^9/l; PLT- 99 x10^9/l; RBC-
Small B-cell (Histologically Low Grade) Lymphoma
 Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Bendamustine is Effective Therapy in Patients with Rituximab-Refractory, Indolent B-Cell Non-Hodgkin Lymphoma
 Bendamustine is Effective Therapy in Patients with Rituximab-Refractory, Indolent B-Cell Non-Hodgkin Lymphoma Kahl BS et al. Cancer 2010;116(1):106-14. Introduction > Bendamustine is a novel alkylating
Bendamustine is Effective Therapy in Patients with Rituximab-Refractory, Indolent B-Cell Non-Hodgkin Lymphoma Kahl BS et al. Cancer 2010;116(1):106-14. Introduction > Bendamustine is a novel alkylating
Change Summary - Form 2018 (R3) 1 of 12
 Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Lymphatic system component
 Introduction Lymphatic system component Statistics Overview Lymphoma Non Hodgkin s Lymphoma Non- Hodgkin's is a type of cancer that originates in the lymphatic system. It is estimated to be the sixth most
Introduction Lymphatic system component Statistics Overview Lymphoma Non Hodgkin s Lymphoma Non- Hodgkin's is a type of cancer that originates in the lymphatic system. It is estimated to be the sixth most
New Targets and Treatments for Follicular Lymphoma
 Winship Cancer Institute of Emory University New Targets and Treatments for Follicular Lymphoma Jonathon B. Cohen, MD, MS Assistant Professor Div of BMT, Emory University Intro/Outline Follicular lymphoma,
Winship Cancer Institute of Emory University New Targets and Treatments for Follicular Lymphoma Jonathon B. Cohen, MD, MS Assistant Professor Div of BMT, Emory University Intro/Outline Follicular lymphoma,
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Aggressive B-cell Lymphomas
 Neoplastic Hematopathology Update 2018 Aggressive B-cell Lymphomas Raju K. Pillai City of Hope National Medical Center I do not have any disclosures Disclosures Outline New entities and changes in WHO
Neoplastic Hematopathology Update 2018 Aggressive B-cell Lymphomas Raju K. Pillai City of Hope National Medical Center I do not have any disclosures Disclosures Outline New entities and changes in WHO
Aggressive NHL and Hodgkin Lymphoma. Dr. Carolyn Faught November 10, 2017
 Aggressive NHL and Hodgkin Lymphoma Dr. Carolyn Faught November 10, 2017 What does aggressive mean? Shorter duration of symptoms Generally need treatment at time of diagnosis Immediate, few days, few weeks
Aggressive NHL and Hodgkin Lymphoma Dr. Carolyn Faught November 10, 2017 What does aggressive mean? Shorter duration of symptoms Generally need treatment at time of diagnosis Immediate, few days, few weeks
12 th Annual Hematology & Breast Cancer Update Update in Lymphoma
 12 th Annual Hematology & Breast Cancer Update Update in Lymphoma Craig Okada, MD, PhD Assistant Professor, Hematology January 14, 2010 Governors Hotel, Portland Oregon Initial Treatment of Indolent Lymphoma
12 th Annual Hematology & Breast Cancer Update Update in Lymphoma Craig Okada, MD, PhD Assistant Professor, Hematology January 14, 2010 Governors Hotel, Portland Oregon Initial Treatment of Indolent Lymphoma
Bendamustine for relapsed follicular lymphoma refractory to rituximab
 LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine for relapsed follicular lymphoma refractory to rituximab Bendamustine for relapsed follicular lymphoma refractory to rituximab Contents Summary 1
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine for relapsed follicular lymphoma refractory to rituximab Bendamustine for relapsed follicular lymphoma refractory to rituximab Contents Summary 1
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
The development of clonality testing for lymphomas in the Bristol Genetics Laboratory. Dr Paula Waits Bristol Genetics Laboratory
 The development of clonality testing for lymphomas in the Bristol Genetics Laboratory Dr Paula Waits Bristol Genetics Laboratory Introduction The majority of lymphoid malignancies belong to the B cell
The development of clonality testing for lymphomas in the Bristol Genetics Laboratory Dr Paula Waits Bristol Genetics Laboratory Introduction The majority of lymphoid malignancies belong to the B cell
Clinical Commissioning Policy Proposition: Bendamustine with rituximab for relapsed indolent non-hodgkin s lymphoma (all ages)
 Clinical Commissioning Policy Proposition: Bendamustine with rituximab for relapsed indolent non-hodgkin s lymphoma (all ages) Reference: NHS England 1607 1 First published: TBC Prepared by NHS England
Clinical Commissioning Policy Proposition: Bendamustine with rituximab for relapsed indolent non-hodgkin s lymphoma (all ages) Reference: NHS England 1607 1 First published: TBC Prepared by NHS England
1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes on the next page
 COME HOME Non-Hodgkin pathway development worksheet, v6 September 2014 1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes
COME HOME Non-Hodgkin pathway development worksheet, v6 September 2014 1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes
Test Utilization: Chronic Lymphocytic Leukemia
 Test Utilization: Chronic Lymphocytic Leukemia Initial Evaluation Diagnostic Criteria Selection of Tests for Prognosis Response to Therapy Challenges Assessment for persistent disease Paul J. Kurtin, M.D.
Test Utilization: Chronic Lymphocytic Leukemia Initial Evaluation Diagnostic Criteria Selection of Tests for Prognosis Response to Therapy Challenges Assessment for persistent disease Paul J. Kurtin, M.D.
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA. April 16, 2008
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
Non-Hodgkin s Lymphoma
 Non-Hodgkin s Lympoma Non-Hodgkin s Lymphomas Janet H. Van Cleave MSN, ACNP-CS, CS, AOCN Acute Care Nurse Practitioner The Mount Sinai Medical Center of New York City Doctoral Student, Yale University
Non-Hodgkin s Lympoma Non-Hodgkin s Lymphomas Janet H. Van Cleave MSN, ACNP-CS, CS, AOCN Acute Care Nurse Practitioner The Mount Sinai Medical Center of New York City Doctoral Student, Yale University
Update in Lymphoma Imaging
 Update in Lymphoma Imaging Victorine V. Muse, MD Lymphoma Update in Lymphoma Imaging Victorine V Muse, MD Heterogeneous group of lymphoid neoplasms divided into two broad histological categories Hodgkin
Update in Lymphoma Imaging Victorine V. Muse, MD Lymphoma Update in Lymphoma Imaging Victorine V Muse, MD Heterogeneous group of lymphoid neoplasms divided into two broad histological categories Hodgkin
Blood Cancers. Blood Cells. Blood Cancers: Progress and Promise. Bone Marrow and Blood. Lymph Nodes and Spleen
 Blood Cancers: Progress and Promise Mike Barnett & Khaled Ramadan Division of Hematology Department of Medicine Providence Health Care & UBC Blood Cancers Significant health problem Arise from normal cells
Blood Cancers: Progress and Promise Mike Barnett & Khaled Ramadan Division of Hematology Department of Medicine Providence Health Care & UBC Blood Cancers Significant health problem Arise from normal cells
Update: Chronic Lymphocytic Leukemia
 ASH 2008 Update: Chronic Lymphocytic Leukemia Improving Patient Response to Treatment with the Addition of Rituximab to Fludarabine-Cyclophosphamide ASH 2008: Update on chronic lymphocytic leukemia CLL-8
ASH 2008 Update: Chronic Lymphocytic Leukemia Improving Patient Response to Treatment with the Addition of Rituximab to Fludarabine-Cyclophosphamide ASH 2008: Update on chronic lymphocytic leukemia CLL-8
DETERMINATION OF A LYMPHOID PROCESS
 Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
A CASE OF PRIMARY THYROID LYMPHOMA. Prof Dr.Dilek Gogas Yavuz Marmara University School of Medicine Endocrinology and Metabolism Istanbul, Turkey
 A CASE OF PRIMARY THYROID LYMPHOMA Prof Dr.Dilek Gogas Yavuz Marmara University School of Medicine Endocrinology and Metabolism Istanbul, Turkey 38 year old female She recognized a mass in her right neck
A CASE OF PRIMARY THYROID LYMPHOMA Prof Dr.Dilek Gogas Yavuz Marmara University School of Medicine Endocrinology and Metabolism Istanbul, Turkey 38 year old female She recognized a mass in her right neck
CLL Biology and Initial Management. Gordon D. Ginder, MD Director, Massey Cancer Center Lipman Chair in Oncology
 CLL Biology and Initial Management Gordon D. Ginder, MD Director, Massey Cancer Center Lipman Chair in Oncology CLL- Epidemiology Most common adult leukemia 25-30% in western world Incidence in US 4.5
CLL Biology and Initial Management Gordon D. Ginder, MD Director, Massey Cancer Center Lipman Chair in Oncology CLL- Epidemiology Most common adult leukemia 25-30% in western world Incidence in US 4.5
Aggressive B-cell Lymphoma 2013
 Aggressive B-cell Lymphoma 2013 Diffuse Large B-Cell Lymphoma Burkitt Lymphoblastic lymphoma Gray zone Intermediate DLBCL/HL Intermediate BL/DLBCL Diffuse Large B-cell lymphoma Common morphology: diffuse
Aggressive B-cell Lymphoma 2013 Diffuse Large B-Cell Lymphoma Burkitt Lymphoblastic lymphoma Gray zone Intermediate DLBCL/HL Intermediate BL/DLBCL Diffuse Large B-cell lymphoma Common morphology: diffuse
Addition of Rituximab to Fludarabine and Cyclophosphamide in Patients with CLL: A Randomized, Open-Label, Phase III Trial
 Addition of Rituximab to Fludarabine and Cyclophosphamide in Patients with CLL: A Randomized, Open-Label, Phase III Trial Hallek M et al. Lancet 2010;376:1164-74. Introduction > In patients with CLL, the
Addition of Rituximab to Fludarabine and Cyclophosphamide in Patients with CLL: A Randomized, Open-Label, Phase III Trial Hallek M et al. Lancet 2010;376:1164-74. Introduction > In patients with CLL, the
Patient Case Studies & Panel Discussion
 Patient Case Studies & Panel Discussion Panelists: Jeremy S. Abramson, MD, Massachusetts General Hospital Cancer Center; Ranjana H. Advani, MD, Stanford Cancer Institute; Andrew D. Zelenetz, MD, PhD, Memorial
Patient Case Studies & Panel Discussion Panelists: Jeremy S. Abramson, MD, Massachusetts General Hospital Cancer Center; Ranjana H. Advani, MD, Stanford Cancer Institute; Andrew D. Zelenetz, MD, PhD, Memorial
Pathology #07. Hussein Al-Sa di. Dr. Sohaib Al-Khatib. Mature B-Cell Neoplasm. 0 P a g e
 Pathology #07 Mature B-Cell Neoplasm Hussein Al-Sa di Dr. Sohaib Al-Khatib 0 P a g e Thursday 18/2/2016 Our lecture today (with the next 2 lectures) will be about lymphoid tumors This is a little bit long
Pathology #07 Mature B-Cell Neoplasm Hussein Al-Sa di Dr. Sohaib Al-Khatib 0 P a g e Thursday 18/2/2016 Our lecture today (with the next 2 lectures) will be about lymphoid tumors This is a little bit long
Dr. Gopichand Pendurti M.B.B.S. Mentor: Dr. Francisco J. Hernandez-Ilizaliturri MD
 ACTIVITY OF RITUXIMAB AND OFATUMUMAB AGAINST MANTLE CELL LYMPHOMA(MCL) IN VITRO IN MCL CELL LINES BY COMPLEMENT DEPENDENT CYTOTOXICITY (CDC)AND ANTIBODY-DEPENDENT CELL MEDIATED CYTOTOXICITY ASSAYS(ADCC)
ACTIVITY OF RITUXIMAB AND OFATUMUMAB AGAINST MANTLE CELL LYMPHOMA(MCL) IN VITRO IN MCL CELL LINES BY COMPLEMENT DEPENDENT CYTOTOXICITY (CDC)AND ANTIBODY-DEPENDENT CELL MEDIATED CYTOTOXICITY ASSAYS(ADCC)
Follicular Lymphoma: the WHO
 Follicular Lymphoma: the WHO and the WHERE? Yuri Fedoriw, MD Associate Professor of Pathology and Laboratory Medicine Director of Hematopathology University of North Carolina Chapel Hill, NC Disclosure
Follicular Lymphoma: the WHO and the WHERE? Yuri Fedoriw, MD Associate Professor of Pathology and Laboratory Medicine Director of Hematopathology University of North Carolina Chapel Hill, NC Disclosure
Burkitt lymphoma. Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8
 Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
The Lymphomas. An overview..
 The Lymphomas An overview.. Peter Anglin MD, FRCPC, MBA Stronach Regional Cancer Centre Newmarket, ON The lymphomas are an important part of the history of medicine 1666 Magpighi publishes first recorded
The Lymphomas An overview.. Peter Anglin MD, FRCPC, MBA Stronach Regional Cancer Centre Newmarket, ON The lymphomas are an important part of the history of medicine 1666 Magpighi publishes first recorded
NICE guideline Published: 20 July 2016 nice.org.uk/guidance/ng52
 Non-Hodgkin s lymphoma: diagnosis and management NICE guideline Published: 20 July 2016 nice.org.uk/guidance/ng52 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Non-Hodgkin s lymphoma: diagnosis and management NICE guideline Published: 20 July 2016 nice.org.uk/guidance/ng52 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
EQA SCHEME CIRCULATION 33 EDUCATIONAL SLIDES DR GRAEME SMITH MONKLANDS DGH
 EQA SCHEME CIRCULATION 33 EDUCATIONAL SLIDES DR GRAEME SMITH MONKLANDS DGH CASE E1 M: 68 yrs Left destructive sinonasal lesion.?lymphoma?adenocarcinoma CD20 CD10 BCL6 MIB1 Answers Diffuse large B cell
EQA SCHEME CIRCULATION 33 EDUCATIONAL SLIDES DR GRAEME SMITH MONKLANDS DGH CASE E1 M: 68 yrs Left destructive sinonasal lesion.?lymphoma?adenocarcinoma CD20 CD10 BCL6 MIB1 Answers Diffuse large B cell
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Parts 2 and 3
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Parts 2 and 3 NEOPLASTIC LYMPHOID DISEASES Introduction o The bone marrow is the source of all cells in the
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Parts 2 and 3 NEOPLASTIC LYMPHOID DISEASES Introduction o The bone marrow is the source of all cells in the
CCND1-IGH Fusion-Amplification and MYC Copy Number Gain in a Case of Pleomorphic Variant Mantle Cell Lymphoma
 AJCP /CASE REPORT CCND1-IGH Fusion-Amplification and MYC Copy Number Gain in a Case of Pleomorphic Variant Mantle Cell Lymphoma Yuan Miao, MD, 1,2 Pei Lin, MD, 1 Wei Wang, MD, 1 L. Jeffrey Medeiros, MD,
AJCP /CASE REPORT CCND1-IGH Fusion-Amplification and MYC Copy Number Gain in a Case of Pleomorphic Variant Mantle Cell Lymphoma Yuan Miao, MD, 1,2 Pei Lin, MD, 1 Wei Wang, MD, 1 L. Jeffrey Medeiros, MD,
Angioimmunoblastic T-cell lymphoma: nobody knows what to do...
 Angioimmunoblastic T-cell lymphoma: nobody knows what to do... Felicitas Hitz, Onkologie/Hämatologie St.Gallen SAMO Lucerne 17.9.2011 : Problems PTCL are rare diseases with even rarer subgroups Difficulte
Angioimmunoblastic T-cell lymphoma: nobody knows what to do... Felicitas Hitz, Onkologie/Hämatologie St.Gallen SAMO Lucerne 17.9.2011 : Problems PTCL are rare diseases with even rarer subgroups Difficulte
Aggressive B cell Lymphomas
 Aggressive B cell Lymphomas I have nothing to disclose. Disclosures Raju K. Pillai City of Hope National Medical Center Outline WHO 2016 Classification Large B cell Lymphomas New entities and changes in
Aggressive B cell Lymphomas I have nothing to disclose. Disclosures Raju K. Pillai City of Hope National Medical Center Outline WHO 2016 Classification Large B cell Lymphomas New entities and changes in
Aggressive B-Cell Lymphomas
 Aggressive B-cell Lymphomas Aggressive B-Cell Lymphomas Stephen Hamilton Dutoit Institute of Pathology Aarhus Kommunehospital B-lymphoblastic lymphoma Diffuse large cell lymphoma, NOS T-cell / histiocyte-rich;
Aggressive B-cell Lymphomas Aggressive B-Cell Lymphomas Stephen Hamilton Dutoit Institute of Pathology Aarhus Kommunehospital B-lymphoblastic lymphoma Diffuse large cell lymphoma, NOS T-cell / histiocyte-rich;
FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting?
 Indolent Lymphoma Workshop Bologna, Royal Hotel Carlton May 2017 FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting? Armando López-Guillermo Department of Hematology, Hospital
Indolent Lymphoma Workshop Bologna, Royal Hotel Carlton May 2017 FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting? Armando López-Guillermo Department of Hematology, Hospital
Eurekah Bioscience Collection
 in Malignant 5/31/06 12:09 PM in Malignant to Leukemia and Lymphoma Eurekah Bioscience Collection in Malignant Sarah E. enrickson Elena M. artmann German Ott Andreas Rosenwald* The practice of clinical
in Malignant 5/31/06 12:09 PM in Malignant to Leukemia and Lymphoma Eurekah Bioscience Collection in Malignant Sarah E. enrickson Elena M. artmann German Ott Andreas Rosenwald* The practice of clinical
Diagnosis of lymphoid neoplasms has been
 Iranian Journal of Pathology (2007)2 (1), 1-61 Review Article Mehdi Nassiri Dep. of Pathology, University of Miami Miller School of Medicine, Miami, USA Abstract Correct diagnosis and classification of
Iranian Journal of Pathology (2007)2 (1), 1-61 Review Article Mehdi Nassiri Dep. of Pathology, University of Miami Miller School of Medicine, Miami, USA Abstract Correct diagnosis and classification of
3/24/2017 DENDRITIC CELL NEOPLASMS: HISTOLOGY, IMMUNOHISTOCHEMISTRY, AND MOLECULAR GENETICS. Disclosure of Relevant Financial Relationships
 DENDRITIC CELL NEOPLASMS: HISTOLOGY, IMMUNOHISTOCHEMISTRY, AND MOLECULAR GENETICS Jason L. Hornick, M.D., Ph.D. Director of Surgical Pathology and Immunohistochemistry Brigham and Women s Hospital Professor
DENDRITIC CELL NEOPLASMS: HISTOLOGY, IMMUNOHISTOCHEMISTRY, AND MOLECULAR GENETICS Jason L. Hornick, M.D., Ph.D. Director of Surgical Pathology and Immunohistochemistry Brigham and Women s Hospital Professor
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL)
 Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Acute Lymphoblastic Leukaemia
 Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
Lymphoma Read with the experts
 Lymphoma Read with the experts Marc Seltzer, MD Associate Professor of Radiology Geisel School of Medicine at Dartmouth Director, PET-CT Course American College of Radiology Learning Objectives Recognize
Lymphoma Read with the experts Marc Seltzer, MD Associate Professor of Radiology Geisel School of Medicine at Dartmouth Director, PET-CT Course American College of Radiology Learning Objectives Recognize
Lugano classification: Role of PET-CT in lymphoma follow-up
 CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
Aggressive B-cell lymphomas and gene expression profiling towards individualized therapy?
 Aggressive B-cell lymphomas and gene expression profiling towards individualized therapy? Andreas Rosenwald Institute of Pathology, University of Würzburg, Germany Barcelona, June 18, 2010 NEW WHO CLASSIFICATION
Aggressive B-cell lymphomas and gene expression profiling towards individualized therapy? Andreas Rosenwald Institute of Pathology, University of Würzburg, Germany Barcelona, June 18, 2010 NEW WHO CLASSIFICATION
