Hematological malignancies :
|
|
|
- Georgiana Dennis
- 5 years ago
- Views:
Transcription
1 de DUVE INSTITUTE Hematological malignancies : Aims of the genetic characterization INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,14/02/2014 Professor Hélène Antoine-Poirel, MD, PhD Center for Human Genetics 1
2 Hematopoiesis
3 Normal hematopoiesis(2) : growth factors
4 Normal hematopoiesis(3) : transcription factors
5 Classification of hematological malignancies (WHO 2008) Clonal proliferation of a bone marrow hematopoietic precursor With block of differentiation = acute Without block of differentiation = chronic Myeloid lymphoid Quantitative abn Qualitative abn Acute Myeloblastic Leukemia Acute Lymphoblastic Leukemia Myeloproliferative neoplasm Myelodysplastic neoplasm
6 Classification of B-cell and T-cell lymphomas (WHO 2008) Anaplastic Large Cell lymphoma
7 Aims of the genetic characterization of cancers 1. Diagnosis Clonality and malignancy Classification (positive and differential diagnosis) 2. Prognosis 3. Minimal residual disease 4. Treatment Molecules targeting the genetic alteration Host polymorphisms triggering the drug response and/or toxicity Pharmacogenetics 5. Cancer genetic predisposition 6. Research 7
8 Clonality as a marker of malignancy All cells derive from the same ancestral cell where occurred the acquired initiating mutation Thrombocytosis, polycythemia, myelofibrosis : Myeloproliferative neoplasm or reactive proliferation? JAK2 V617F mutation = clonal myeloproliferative disorder polycythemia vera / Vaquez (95%) essential thrombocytosis (50-60%) myelofibrosis (50-60%) CalR (ex9) = clonal myeloproliferative disorder essential thrombocytosis (25%) myelofibrosis (35%) 8
9 Myeloproliferative neoplasms CalR CalR
10 Classification of Acute myeloid leukemia (AML) : FAB Classification (1976) Morphology (+ immunophenotype -1991) (AML minimally differentiated M0) AML without maturation M1 AML with maturation M2 Promyelocytic acute leukemia M3 Myelomonocytic leukemia M4 AML-M4 with abn eosinophils M4Eo Monoblastic/monocytic AL M5a/b Erythroid AL M6 Megacaryoblastic AL M7 10
11 Acute myeloid leukemia (AML) WHO classification (2008) Morphology + Immunophenotype + Genetics AML with recurrent genetic abnormalities AML with balanced translocations / inversions t(8;21)(q22;q22) RUNX1-RUNX1T1 inv/t(16;16)(p13;q22) CBFB-MYH11 abnormal eosinophils (M4Eo) t(15;17)(q22;q12) PML-RARa promyelocytic (M3) t(9;11)(p22;q23) MLLT3-MLL t(6;9)(p23;q34) DEK-NUP214 basophilia inv/t(3;3)(q21;q26.2) RPN1-EVI1 t(1;22)(p13;q13) RBM15-MKL1 megacaryoblastic (M7) AML with gene mutations Normal cytogenetics t(8;21), inv/t(16;16) FLT3-ITD, FLT3-TKD MLL-PTD NPM1 mutations (ex12) CEBPA mutations KIT mutations
12 Acute myeloid leukemia (AML) WHO classification (2008) AML with myelodysplasia-related changes following a myelodysplastic syndrome (MDS) or myeloproliferative disorder without prior MDS AML & myelodysplastic syndromes, therapy related Alkylants agents Ionizing radiation therapy Topoisomerase II inhibitors Others AML not otherwise specified AML with minimally differentiation AML without maturation AML with maturation Acute myelomonocytic leukemia Acute monoblastic & monocytic leukemia Acute erythroid leukemia Acute megacaryoblastic leukemia Acute basophilic leukemia Acute panmyelosis with myelofibrosis FAB M0 M1 M2 M4 M5a/b M6 M7 Myeloid sarcoma
13 Core Bing Factor : RUNX1/CBFα/AML1 & CBFβ GM-CSF, IL-3, M-CSF-R, TCRα, TCRß p21/waf1, MPO, NE, granzyme B, NP-3. AML-M2 : t(8;21)(q22;q22) AML-M4Eo : t/inv(16)(p13q22) Childhood preb ALL: t(12;21)(p13;q22)
14 Retinoic Acid Receptor - alpha RARα R A AA PML-RARα R R R R AA R AA A
15 MLL (11q23)
16 Molecular heterogeneity of AML with normal karyotype Roboz GJ ASH Education Book December 10, 2011 vol no
17 Cooperating mutations in leucemogenesis Class I mutations Proliferative and / or survival advantage FLT3-ITD FLT3-TKD KIT RAS PTPN11 JAK2 + AML Class II mutations block in hematopoietic differentiation and in resulting apoptosis PML-RARA == RUNX1-RUNX1T1 CBFB-MYH11 MLL fusions CEBPA NPM1? ASH 2005
18 Next Generation Sequencing : new recurring mutations 5 classes of genes involved in leukemogenesis == == == Murati A BMC Cancer 2012
19 Schematic representation of epigenetic regulation of a leukemogenic locus (LL) framed by histone H3 Murati A, et al, BMC Cancer 2012
20 Model of leukemogenesis: slot machine Murati A BMC Cancer 2012
21 Schematic representation of the current knowledge of genotype/phenotype relationships in MDS, MDS/MPN, and a related MPN like CNL SF3B1 & RARS SF3B1/JAK2 or SF3B1/MPL & RARS-T miscellanious? RCUD Various combinations RNA splicing (SRF2,U2F1) DNA methylation (TET2, DNMT3A) RCMD RAEB TET2/SRSF2 & CMML ASXL1 : poor CSF3R & CNL SETBP1 & acml Cazzola M, et al, Blood 2013
22 Acute lymphoblastic leukemia /lymphoma (ALL) FAB (1976) GEIL/EGIL (1994/95) WHO (2001/08) Morphology + Immunophenotype + Genetics ALL-L1 ALL-L2 ALL-L3 Pro-B-ALL Common ALL Pre-B-ALL Mature B-ALL Pro-T-ALL Pre-T-ALL Cortical T-ALL Medullary T-ALL ALL of B-cell precursors t(9;22)(q34;q11.2) 3-4% BCR-ABL t(v;11q23) 2-3% MLL Rgt t(12;21)(p13;q22) 16-29% ETV6-RUNX1 Hyperdiploidy > % Hypodiploidy 5% t(5;14)(q31;q32) IL3-IGH t(1;19)(q23;p13.3) 6% TCF3-PBX1 ALL of T-cell precursors 1p32 25% SIL-TAL1 del(9)(p21) 30% p16 t(10;v)(q24;v) 7-31% TLX1 t(5;14)(q35;q32) 13-20% TLX3 t(10;11)(p13;q14) 9-30% CALM-AF10 t(11;v)(q23;v) 8% MLL-v 9q34 6% NUP214-ABL inv(7)(p15q35) 5% TCRβ-HOXA
23 B-cell Lymphomas
24 B-cell Lymphomas t(14;18)(q32;q21) t(3;v)(q27;v) t(8;14)(q24;q32)
25 Diffuse Large B-Cell Lymphoma : Classification based on gene expression profiling Clinical heterogeneity of DLBCL Non reproducibility of morphology and immunohistochemistry Gene expression profiling : 2 main molecular subtypes of DLBCL : those derived from the lymph node germinal center (GCB) and others derived from an activated B-cell (ABC) (c) NFKB activation REL amplification BCL2 translocation Ash A. Alizadeh, Nature 2000
26 Relativity of the diagnostic value The specificity of genetic alterations is relative BCR-ABL : characteristics of CML (~100%) 25% of adult ALL (children : 2-4%) MYC : characteristics of Burkitt lymphomas (~95%) ~25% of childhood DLBCL (adults : 5-10%) BCL2 : characteristics of follicular lymphomas (~95%) ~20-30% of adult DLBCL (children : ~0%) Majoritary clone Primary genetic event? Sub-clone Secondary event?
27 Aims of the genetic characterization of cancers 1. Diagnosis Clonality and malignancy Classification (positive and differential diagnosis) 2. Prognosis 3. Minimal residual disease 4. Treatment Molecules targeting the genetic alteration Host polymorphisms triggering the drug response and/or toxicity Pharmacogenetics 5. Cancer genetic predisposition 6. Research 27
28 Childhood ALL : Impact of cytogenetics on survival (Moorman AV Blood 2007)
29 Adult ALL : Impact of cytogenetics on survival Cytogenetics : 1366 (90%) of 1522 patients Successful : 1003 cases (73%) Abnormal clone : 796 cases (79%) (Moorman AV Blood 2007)
30 Adult AML : Impact of cytogenetic entities recognized in 2008 WHO classification on survival Grimwade D et al. Blood 2010;116:
31 Adult AML : Impact of gene mutations on survival 3 prognostic groups using 4 marker combinations: low- risk, biallelic CEBPAm + and/or NPM1m + /DNMT3Am high-risk, DNMT3Am + and/or MLLm + and intermediate, all remaining cases Shen Y et al. Blood 2011;118:
32 Revised risk stratification of AML according to different models Risk profile Dohner H et al. (Blood 2010;115: )( ) Patel JP et al. (NEJM 2012;366: ) Grossmann V et al. (Blood 2012;120: ) Based on cytogenetic analysis mutation analyses of the NPM1, CEBPA, and FLT3 genes excluding cases of acute promyelocytic leukemia integrated cytogenetic and mutational analysis (MLL-PTD, FLT3-ITD, NPM1, CEBPA, TET2, ASXL1, DNMT3A, PHF6, IDH1, and IDH2) only molecular markers (PML-RARA, RUNX1-RUNX1T1, CBFB-MYH11, FLT3-ITD, MLL-PTD, mutations in NPM1, CEPBA, RUNX1, ASXL1, and TP53) Favorable t(8,21)(q22;q22); RUNX1-RUNX1T1 t/inv(16)(p13.1q22); CBFB-MYH11 NPM1 mut/flt3-itd- (*) CEBPA mut (*) Favorable cytogenetics NPM1 mut/flt3-itd-with IDH1 or IDH2 mutations Very favourable: PML-RARA CEBPA double-mut Favorable: RUNX1-RUNX1T1 CBFB-MYH11 NPM1 mut/flt3-itd- Intermediate Unfavorable Intermediate-I: NPM1 mut/flt3-itd + and normal karyotype NPM1 wt/flt3-itd + and normal karyotype NPM1 wt/flt3-itd- and normal karyotype Intermediate-II: t(9,11)(p22;q23); MLLT3-MLL Cytogenetic abnormalities not classified as favorable or adverse inv(3)(q21q26.2) or t(3,3)(q21;q26.2); RPN1-EVI1 t(6,9)(p23;q34); DEK-NUP214 t(v;11)(v;q23); MLL rearranged 5 or del(5q); -7; abnl(17p); complex karyotype CEBPA mut FLT3-ITD- and all these genes wildtype: ASXL1, MLL-PTD, PHF6, and TET2 FLT3-ITD+, trisomy 8-negative and all these genes wild-type: MLL-PTD, TET2, and DNMT3A Unfavorable cytogenetics FLT3-ITD+, CEBPA wt and any of these gene alterations: MLL-PTD, TET2, DNMT3A mutations or trisomy 8 CEBPA single-mut/flt3-itd + NPM1 mut/flt3-itd + Wild-type cases Unfavorable: MLL-PTD and/or RUNX1 and/or ASXL1 mut Very unfavourable: TP53 mut
33 Myelodysplastic syndromes (MDS): recurring chromosomal abnormalities & frequency at diagnosis Unbalanced MDS t-mds Balanced MDS t-mds +8 * 10% t(11;16)(q23;p13.3) 3% -7/del(7q) 10% 50% t(3;21)(q26.2;q22.1) 2% 5/del(5q) 10% 40% t(1.3)(p36.3;q21.2) 1% del(20q) * 5-8% t(2;11)(p21;q23) 1% -Y * 5% t/inv(3)t(q31q26.2) 1% i/t(17q) 3-5% t(6;9)(p23;q34) 1% -13/del(13q) 3% del(11q) 3% del/t(12p) 3% del(9p) 1-2% idic(x)(q13) 1-2% t-mds = therapy related-mds WHO 2008
34 Myelodysplastic syndromes (MDS): International Prognostic Score System IPSS (Greenberg, 1997) Score Prognostic variables % blast cells <5% 5-10% 11-19% 20-30% (AML) Cytopenias Hb<10mg/dL PN<1.8x109/L PQ<100x109/L Karyotype Good Intermediate Poor N -Y del(5q) del(20q) Other Complex ( 3 an) Chr7 abn
35 Myelodysplastic syndromes (MDS): Revised IPSS Score IPSS-R (Greenberg, 2012) Prognostic variable 0 0,5 1 1, % Bone marrow blast cells 2 >2-<5% 5-10% >10% Hb 10 8-<10 <8 PQ <100 <50 ANC 0,8 <0,8 Karyotype Very good Good Intermediary Poor Very poor -Y del(11q) +8-7 > 3 abn Normal +19 inv(3)/t(3q)/del(3q) del(5q) i(17q) 2 abn including- 7/del(7q) del(12p) Other simple abn complex = 3 an del(20q) Independant double clones 2 an including del(5q) del(7q-) 5 risk groups Very low Low IntermediaryHigh Very high Score 1,5 <1,5-3 <3-4,5 <4,5-6 >6
36 Multiple Myeloma Mayo Stratification of Myeloma and Risk-Adapted Therapy ( Dispenzieri A et al., Mayo Clin Proc ) High risk (~25% of patients) Al least one criteria : FISH 17p deletion FISH t(4;14) translocation FISH t(14;16) translocation Karyotype 13q deletion Karyotype hypodiploidy Plasma cell labelling index 3% Standard risk (~75% of patients) other FISH or karyotype abn, including : Hyperdiploidy FISH t(11;14) translocation FISH t(6;14) translocation
37 Aims of the genetic characterization of cancers 1. Diagnosis Clonality and malignancy Classification (positive and differential diagnosis) 2. Prognosis 3. Minimal residual disease 4. Treatment Molecules targeting the genetic alteration Host polymorphisms triggering the drug response and/or toxicity Pharmacogenetics 5. Cancer genetic predisposition 6. Research 37
38 Minimal residual disease After induction therapy of leukemias assessment of the complete remission at the different levels : clinical, morphological, immunological, cytogenetic, molecular (real-time PCR)
39 Childhood ALL Evaluation by Real-Time RT-PCR with oligonucleotide probes specific of the patient Immunoglobulin / TCR rearrangement Sensitivity : 10-4 Kaplan-Meier estimates of the Relapse-free Interval according to the - presence or absence and - level of Residual Disease in patients with a first Complete Remission of ALL at the end of induction therapy (Cave H et al. N Engl J Med 1998)
40 Chronic myeloid leukemia (CML) Cytogenetic & molecular response Cytogenetic response : Absent >95% Minimal 66-95% Minor 36-65% Partial 1-35% Complete 0% Assessment on at least 20 mitoses Major molecular response (MMR) : Decreased BCR-ABL transcript level 0.1% of average BCR-ABL transcript level in 30 untreated CML-CP European LeukemiaNet Recommendations (Baccarini, Blood 2013) : definition of the response to TKIs : optimal / warning / failure Based on cytogenetics, FISH and molecular analyses (BCR-ABL quantification & mutation analysis of the ABL TK domain)
41 Aims of the genetic characterization of cancers 1. Diagnosis Clonality and malignancy Classification (positive and differential diagnosis) 2. Prognosis 3. Minimal residual disease 4. Treatment Molecules targeting the genetic alteration Host polymorphisms triggering the drug response and/or toxicity Pharmacogenetics 5. Cancer genetic predisposition 6. Research 41
42 Promyelocytic acute leukemia (AML-M3/APL) faggot cells = bundles of Auer rods
43 Promyelocytic acute leukemia (AML-M3/APL) t(15;17)(q22;q21)
44 Promyelocytic acute leukemia (AML-M3/APL) FISH : fusion PML-RARA
45 Promyelocytic acute leukemia (AML-M3/APL) LMA M3 t(15;17)(q22;q21) = fusion between PML (15q22) and RARA, retinoic acid receptor alpha (17q21) Reduced sensitivity of the nuclear receptor to the ligand, retinoic acid All Trans Retinoic Acid ATRA (Vesanoid ) ( vitamin A)
46 Promyelocytic acute leukemia (AML-M3/APL) 1µM ATRA : differentiation induction with growth inhibition and apoptosis
47 RARα R A AA PML-RARα NPM-RARα NuMA-RARα R R R R AA ATRA sensitivity R R 45 mg/m 2 /jr A A AA AA R AA PLZF-RARα STAT5b-RARα R R R R R R R AA R A Poor ATRA sensitivity R R R R 45 mg/m 2 /jr R AA AA R
48 Chronic myeloid leukemia (CML) LMC t(9;22)(q34;q11) fusion between BCR (22q11) and ABL1 (9q34) Constitutively activated chimeric tyrosine kinase leukemia mouse Tyrosine kinase inhibitor (STI571 / Imatinib / Glivec )
49 Inhibitors of tyrosine kinase activity competitive antagonists of the ATP-binding site of bcr-abl Druker, B. J. Blood 2008;112:
50 Chronic myeloid leukemia (CML) : Glivec resistance LSI BCR/ABL (Vysis) LSI BCR/ABL (Vysis) 006C C BCR-ABL amplification ABL tyrosine kinase domain mutations and overexpression of drug-efflux proteins (ABCB1 and ABCG2) Development of new tyrosine kinase inhibitors (Dasatinib, Nilotinib, )
51 ABL KD Mutations Sensitivity of BCR/ABL Kinase Domain Mutations to TKIs (values are given as IC 50 Redaelli, S. et al. J Clin Oncol; 27:
52 Pharmacogenetics : Host polymorphisms trigger the drug response and/or toxicity Polymorphisms in susceptibility genes for environmental / genotoxic exposures Activation enzymes (phase I) = cytochromes Detoxification enzymes (Phase II) = Glutathion S-Transferase Nucleic acid synthesis : folat metabolism and Methotrexate 6-mercaptopurinethol metabolism : thiopurine methyltransferase (TPMT) deficit
53 Folate metabolism & Methotrexate enzymes subject to common genetic polymorphisms DHFR (dihydrofolate reductase), GGH (gamma glutamyl hydrolase), MTHFR (methylenetetra-hydrofolate reductase), FPGS (folylpoly-glutamate synthetase) Carroll, W. L. et al. Hematology 2003;2003:
54 Thiopurin metabolism : 6-mercaptopurine (Purinethol & ALL) Probability of complete remission vs thiopurine methyltransferase (TPMT) genotype in childhood ALL (SJCRH Total XII trial) Carroll, W. L. et al. Hematology 2003;2003:
55 Perspectives Exhaustive tumor sequencing (exome genome) Genetic «signature» of the tumor : specific & limited repertoire of synergistic «driver» mutations Relapse of acute leukemia : dynamic process with : New mutations Clonal selection : Persistance of a dominant clone and / or Selection & expansion of a minor clone Improved knowledge of the physiopathogeny Towards an integrated & dynamic classification? New therapeutic targets Combined targeted treatments = personalized therapeutic «strategies» (signalling pathways, epigenetic mutations)
56 Aims of the genetic characterization of cancers 1. Diagnosis Clonality and malignancy Classification (positive and differential diagnosis) 2. Prognosis 3. Minimal residual disease 4. Treatment Molecules targeting the genetic alteration Host polymorphisms triggering the drug response and/or toxicity Pharmacogenetics 5. Cancer genetic predisposition 6. Research 56
57 Predisposition to hematological malignancies Very rare familial disorders Bone marrow failures Fanconi anemia (FA complementation groups) Dyskeratosis congenita (TERC / TERT /DKC1) Diamond-Blackfan Anemia (RPS19) Shwachman-Diamond Syndrome (SBDS) Predisposition to AML / MDS CEBPA RUNX1 GATA2 Haematologica 2010 Low penetrance susceptibility Chronic Lymphocytic Leukemia Acute Lymphoblastic Leukemia
58 Thank you! de DUVE INSTITUTE 58
GENETICS OF HEMATOLOGICAL MALIGNANCIES
 de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
AML: WHO classification, biology and prognosis. Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen
 AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
Update on the WHO Classification of Acute Myeloid Leukemia. Kaaren K. Reichard, MD Mayo Clinic Rochester
 Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Molecular Markers in Acute Leukemia. Dr Muhd Zanapiah Zakaria Hospital Ampang
 Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities
 WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017
 Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota
 Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Treatments and Current Research in Leukemia. Richard A. Larson, MD University of Chicago
 Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
WHO Classification 7/2/2009
 Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party. The European Group for Blood and Marrow Transplantation
 36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
Combinations of morphology codes of haematological malignancies (HM) referring to the same tumour or to a potential transformation
 Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Krishna Reddy CH and Ashwin Dalal. Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad
 Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Disclosure: Objectives/Outline. Leukemia: Genealogy of Pathology Practice: Old Diseases New Expectations. Nothing to disclose.
 RC1 Leukemia: Genealogy of Pathology Practice: Old Diseases New Expectations RC2 Disclosure: Nothing to disclose Henry Moon Lecture: UCSF Annual Conference Kathryn Foucar, MD kfoucar@salud.unm.edu May
RC1 Leukemia: Genealogy of Pathology Practice: Old Diseases New Expectations RC2 Disclosure: Nothing to disclose Henry Moon Lecture: UCSF Annual Conference Kathryn Foucar, MD kfoucar@salud.unm.edu May
Objectives. Morphology and IHC. Flow and Cyto FISH. Testing for Heme Malignancies 3/20/2013
 Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia
 Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia Hartmut Döhner Medical Director, Department of Internal Medicine III Director, Comprehensive Cancer Center Ulm Ulm University,
Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia Hartmut Döhner Medical Director, Department of Internal Medicine III Director, Comprehensive Cancer Center Ulm Ulm University,
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD
 Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD What is it? clonal expansion of myeloid precursor cells with reduced capacity to differentiate as opposed to ALL/CLL, it is limited to the myeloid cell
Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD What is it? clonal expansion of myeloid precursor cells with reduced capacity to differentiate as opposed to ALL/CLL, it is limited to the myeloid cell
Recommended Timing for Transplant Consultation
 REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
2010 Hematopoietic and Lymphoid ICD-O Codes - Alphabetical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
2012 Hematopoietic and Lymphoid ICD-O Codes - Numerical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Diagnostic Molecular Pathology of Myeloid Neoplasms
 Diagnostic Molecular Pathology of Myeloid Neoplasms Beirut, Lebanon Tuesday November 29, 2011: Pre-congress workshop Adam Bagg University of Pennsylvania Philadelphia, USA Myeloid neoplasms Myeloproliferative
Diagnostic Molecular Pathology of Myeloid Neoplasms Beirut, Lebanon Tuesday November 29, 2011: Pre-congress workshop Adam Bagg University of Pennsylvania Philadelphia, USA Myeloid neoplasms Myeloproliferative
Molecular Hematopathology Leukemias I. January 14, 2005
 Molecular Hematopathology Leukemias I January 14, 2005 Chronic Myelogenous Leukemia Diagnosis requires presence of Philadelphia chromosome t(9;22)(q34;q11) translocation BCR-ABL is the result BCR on chr
Molecular Hematopathology Leukemias I January 14, 2005 Chronic Myelogenous Leukemia Diagnosis requires presence of Philadelphia chromosome t(9;22)(q34;q11) translocation BCR-ABL is the result BCR on chr
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
SUPPLEMENTARY INFORMATION
 Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Cytogenetics Update. Lynda J Campbell
 Cytogenetics Update Lynda J Campbell lynda.campbell@svhm.org.au Nowell and Hungerford, 1960 Ph Janet Rowley showed the Ph chromosome to be a balanced rearrangement: t(9;22) 9 22 Acute lymphoblastic leukaemia
Cytogenetics Update Lynda J Campbell lynda.campbell@svhm.org.au Nowell and Hungerford, 1960 Ph Janet Rowley showed the Ph chromosome to be a balanced rearrangement: t(9;22) 9 22 Acute lymphoblastic leukaemia
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Cost-Effective Strategies in the Workup of Hematologic Neoplasm. Karl S. Theil, Claudiu V. Cotta Cleveland Clinic
 Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms. Curtis A. Hanson, MD
 Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Myelodysplastic syndromes and the new WHO 2016 classification
 Myelodysplastic syndromes and the new WHO 2016 classification 32nd General Annual Meeting of the Belgian Hematology Society 10-11 February 2017 Gregor Verhoef, Departement of Hematology, University Hospital
Myelodysplastic syndromes and the new WHO 2016 classification 32nd General Annual Meeting of the Belgian Hematology Society 10-11 February 2017 Gregor Verhoef, Departement of Hematology, University Hospital
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Case 1. Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX
 Case 1 Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX Disclosure of Relevant Financial Relationships The USCAP requires that anyone in a position to influence or control the content of all CME
Case 1 Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX Disclosure of Relevant Financial Relationships The USCAP requires that anyone in a position to influence or control the content of all CME
The Revised 2016 WHO Classification of Acute Leukemias
 The Revised 2016 WHO Classification of Acute Leukemias Robert P Hasserjian, MD Associate Professor Massachusetts General Hospital and Harvard Medical School Acute leukemias Aggressive hematopoietic neoplasms
The Revised 2016 WHO Classification of Acute Leukemias Robert P Hasserjian, MD Associate Professor Massachusetts General Hospital and Harvard Medical School Acute leukemias Aggressive hematopoietic neoplasms
Acute Myeloid Leukemia with RUNX1 and Several Co-mutations
 Case SH2017-0281 Acute Myeloid Leukemia with RUNX1 and Several Co-mutations James Bauer, MD, PhD David Yang, MD Erik Ranheim, MD, PhD Catherine Leith, MB, Bchir Clinical History Chief Complaint: 72 year
Case SH2017-0281 Acute Myeloid Leukemia with RUNX1 and Several Co-mutations James Bauer, MD, PhD David Yang, MD Erik Ranheim, MD, PhD Catherine Leith, MB, Bchir Clinical History Chief Complaint: 72 year
The Past, Present, and Future of Acute Myeloid Leukemia
 The Past, Present, and Future of Acute Myeloid Leukemia Carter T. Davis, MD Hematology-Oncology Fellow Duke University Health System September 10, 2016 Overview Overview of Acute Myeloid Leukemia Review
The Past, Present, and Future of Acute Myeloid Leukemia Carter T. Davis, MD Hematology-Oncology Fellow Duke University Health System September 10, 2016 Overview Overview of Acute Myeloid Leukemia Review
Mixed Phenotype Acute Leukemias
 Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Kylie Lepic BSc, MD, FRCPC CAGPO Conference
 Acute Leukemia Kylie Lepic BSc, MD, FRCPC CAGPO Conference Oct 19, 2013 1 Disclosures No conflicts of interest 2 Objectives Case presentation Classification of leukemia Clinical manifestations Diagnosis
Acute Leukemia Kylie Lepic BSc, MD, FRCPC CAGPO Conference Oct 19, 2013 1 Disclosures No conflicts of interest 2 Objectives Case presentation Classification of leukemia Clinical manifestations Diagnosis
Cytogenetic and molecular abnormalities in AML. Dr Elizabeth Tegg Director of haematology Pathology West
 Cytogenetic and molecular abnormalities in AML Dr Elizabeth Tegg Director of haematology Pathology West Outline Classification of AML Types of genetic changes Next generation sequencing in HM Outline Classification
Cytogenetic and molecular abnormalities in AML Dr Elizabeth Tegg Director of haematology Pathology West Outline Classification of AML Types of genetic changes Next generation sequencing in HM Outline Classification
Enhancing Assessment of Myeloid Disorders in the Era of Precision Medicine
 Enhancing Assessment of Myeloid Disorders in the Era of Precision Medicine Michelle Afkhami, M.D. Medical Director, Clinical Molecular Diagnostic Laboratory City of Hope National Medical Center Objectives
Enhancing Assessment of Myeloid Disorders in the Era of Precision Medicine Michelle Afkhami, M.D. Medical Director, Clinical Molecular Diagnostic Laboratory City of Hope National Medical Center Objectives
Myelodysplastic syndromes
 Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Current Techniques in Molecular Biology Friedel Nollet, Ph.D.
 Current Techniques in Molecular Biology Friedel Nollet, Ph.D. Molecular Biology and Cytometry course May 16-17, 2013 Mol, SCK-CEN, Belgium Sanger DNA sequencing Kary Mullis received a Nobel Prize in chemistry
Current Techniques in Molecular Biology Friedel Nollet, Ph.D. Molecular Biology and Cytometry course May 16-17, 2013 Mol, SCK-CEN, Belgium Sanger DNA sequencing Kary Mullis received a Nobel Prize in chemistry
Acute leukemia and myelodysplastic syndromes
 11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities
 Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Molecular. Oncology & Pathology. Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine. Liquid Biopsy.
 Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression
 Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
TEST MENU TEST CPT CODES TAT. Chromosome Analysis Bone Marrow x 2, 88264, x 3, Days
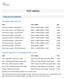 TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
Acute myeloid leukemia: prognosis and treatment. Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg
 Acute myeloid leukemia: prognosis and treatment Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg Patient Female, 39 years History: hypothyroidism Present:
Acute myeloid leukemia: prognosis and treatment Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg Patient Female, 39 years History: hypothyroidism Present:
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH )
 Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Out-Patient Billing CPT Codes
 Out-Patient Billing CPT Codes Updated Date: August 3, 08 Client Billed Molecular Tests HPV DNA Tissue Testing 8764 No Medicare Billed - Molecular Tests NeoARRAY NeoARRAY SNP/Cytogenetic No 89 NeoLAB NeoLAB
Out-Patient Billing CPT Codes Updated Date: August 3, 08 Client Billed Molecular Tests HPV DNA Tissue Testing 8764 No Medicare Billed - Molecular Tests NeoARRAY NeoARRAY SNP/Cytogenetic No 89 NeoLAB NeoLAB
THE LEUKEMIAS. ACUTE CHRONIC AML and ALL CLL and CML (any ages) (in the elderly)
 THE LEUKEMIAS Definition: malignant transformation of the pluripotent stem cell, successive expansion of the malignant clone from the bone marrow to the tissues THE LEUKEMIAS Characteristics: maturation
THE LEUKEMIAS Definition: malignant transformation of the pluripotent stem cell, successive expansion of the malignant clone from the bone marrow to the tissues THE LEUKEMIAS Characteristics: maturation
ADVANCES IN CHILDHOOD ACUTE LEUKEMIAS : GENERAL OVERVIEW
 ADVANCES IN CHILDHOOD ACUTE LEUKEMIAS : GENERAL OVERVIEW Danièle SOMMELET European Scientific Seminar Luxemburg, 3.11.2009 1 Definition of acute leukemias Malignant process coming from lymphoid (85 %)
ADVANCES IN CHILDHOOD ACUTE LEUKEMIAS : GENERAL OVERVIEW Danièle SOMMELET European Scientific Seminar Luxemburg, 3.11.2009 1 Definition of acute leukemias Malignant process coming from lymphoid (85 %)
Acute Leukemia Diagnosis
 Acute Leukemia Diagnosis Elizabeth A. Griffiths, MD Leukemia Service, Department of Medicine Roswell Park Cancer Institute SUNY-UB School of Medicine 3 841,390 843,820 Blood cancers are normal blood cells
Acute Leukemia Diagnosis Elizabeth A. Griffiths, MD Leukemia Service, Department of Medicine Roswell Park Cancer Institute SUNY-UB School of Medicine 3 841,390 843,820 Blood cancers are normal blood cells
Molecular Diagnostics of Myeloid and Lymphoid Neoplasms
 Molecular Diagnostics of Myeloid and Lymphoid Neoplasms Molecular Pathology: Principles in Clinical Practice - 2012 John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine
Molecular Diagnostics of Myeloid and Lymphoid Neoplasms Molecular Pathology: Principles in Clinical Practice - 2012 John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia
 Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
2 nd step do Bone Marrow Study If possible both the aspiration and
 Blood Malignancies-I Prof. Herman Hariman,SpPK a (KH). Ph.D.(U.K) Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. Clinpath, FK-USU First do the Full Blood Count Hb, WBCS, Platelets Morphology!! Such as blasts,
Blood Malignancies-I Prof. Herman Hariman,SpPK a (KH). Ph.D.(U.K) Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. Clinpath, FK-USU First do the Full Blood Count Hb, WBCS, Platelets Morphology!! Such as blasts,
Initial Diagnostic Workup of Acute Leukemia
 Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
Acute Leukemia. Sebastian Giebel. Geneva 03/04/
 Acute Leukemia (including ALL) Sebastian Giebel Geneva 03/04/2012 www.ebmt.org Acute leukemias: EBMT survey 2 AML: EBMT survey Gratwohl A, et al. Bone Marrow Transplant 2009 3 Acute leukemias: INCIDENCE
Acute Leukemia (including ALL) Sebastian Giebel Geneva 03/04/2012 www.ebmt.org Acute leukemias: EBMT survey 2 AML: EBMT survey Gratwohl A, et al. Bone Marrow Transplant 2009 3 Acute leukemias: INCIDENCE
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Acute Lymphoblastic and Myeloid Leukemia
 Acute Lymphoblastic and Myeloid Leukemia Pre- and Post-Disease Form Acute Lympoblastic Leukemia Mary Eapen MD, MS Acute Lymphoblastic Leukemia SEER Age-adjusted incidence rate 1.6 per 100,000 men and women
Acute Lymphoblastic and Myeloid Leukemia Pre- and Post-Disease Form Acute Lympoblastic Leukemia Mary Eapen MD, MS Acute Lymphoblastic Leukemia SEER Age-adjusted incidence rate 1.6 per 100,000 men and women
Dr. Anjali Kelkar (DNB Path, IFCAP)
 Acute Leukemias : Morphology and Beyond Dr. Anjali Kelkar (DNB Path, IFCAP) Consultant - Diagnostic Haematology NABL Assessor Senior Associate Professor, Incharge Haematology Labs Bharati Vidyapeeth Deemed
Acute Leukemias : Morphology and Beyond Dr. Anjali Kelkar (DNB Path, IFCAP) Consultant - Diagnostic Haematology NABL Assessor Senior Associate Professor, Incharge Haematology Labs Bharati Vidyapeeth Deemed
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow*
 Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow* Version: Protocol Posting Date: January 2018 This protocol is NOT required for accreditation
Protocol for the Examination of Specimens From Patients With Hematopoietic Neoplasms Involving the Bone Marrow* Version: Protocol Posting Date: January 2018 This protocol is NOT required for accreditation
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1
 Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
New drugs in Acute Leukemia. Cristina Papayannidis, MD, PhD University of Bologna
 New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation
 a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
Case #16: Diagnosis. T-Lymphoblastic lymphoma. But wait, there s more... A few weeks later the cytogenetics came back...
 Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Test Name Results Units Bio. Ref. Interval. Positive
 Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 4 MYELOID NEOPLASMS
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
Molecular Hematopathology
 Molecular Hematopathology Charles E. Hill, MD, PhD Emory University School of Medicine April 2013 The Association for Molecular Pathology Education. Innovation and Improved Patient Care. Advocacy. www.amp.org
Molecular Hematopathology Charles E. Hill, MD, PhD Emory University School of Medicine April 2013 The Association for Molecular Pathology Education. Innovation and Improved Patient Care. Advocacy. www.amp.org
Introduction: The Revised (4 th Edition) World Health Organization (WHO) Classification of Tumors of Hematopoietic and Lymphoid Tissues
 Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
Elisabeth Koller 3rd Medical Dept., Center for Hematology and Oncology, Hanusch Hospital, Vienna, Austria
 Elisabeth Koller 3rd Medical Dept., Center for Hematology and Oncology, Hanusch Hospital, Vienna, Austria Incidence Diagnosis Prognostic factors Treatment Induction therapy - HSCT Indications for HSCT
Elisabeth Koller 3rd Medical Dept., Center for Hematology and Oncology, Hanusch Hospital, Vienna, Austria Incidence Diagnosis Prognostic factors Treatment Induction therapy - HSCT Indications for HSCT
[COMPREHENSIVE GENETIC ASSAY PANEL ON
 2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
Molecular Advances in Hematopathology
 Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
School of Pathology and Laboratory Medicine: Current and New Research Interests
 School of Pathology and Laboratory Medicine: Current and New Research Interests W/Professor Wendy Erber Current Research Interests Viral immunology and immunogenetics Bone pathology and cell signalling
School of Pathology and Laboratory Medicine: Current and New Research Interests W/Professor Wendy Erber Current Research Interests Viral immunology and immunogenetics Bone pathology and cell signalling
Management of Myelodysplastic Syndromes
 Management of Myelodysplastic Syndromes Peter L. Greenberg, MD Stanford Cancer Institute Myelodysplastic Syndromes: Clinical & Molecular Advances for Disease Classification and Prognostication MDSs: A
Management of Myelodysplastic Syndromes Peter L. Greenberg, MD Stanford Cancer Institute Myelodysplastic Syndromes: Clinical & Molecular Advances for Disease Classification and Prognostication MDSs: A
Table 1: biological tests in SMD
 Table 1: biological tests in SMD Tests Mandatory Recommended Under validation Morphology Marrow aspirate Marrow biopsy 1 Iron staining Quantification of dysplasia WHO 2008 Classification Cytogenetics Conventional
Table 1: biological tests in SMD Tests Mandatory Recommended Under validation Morphology Marrow aspirate Marrow biopsy 1 Iron staining Quantification of dysplasia WHO 2008 Classification Cytogenetics Conventional
Acute myeloid leukemia: a comprehensive review and 2016 update
 OPEN Citation: (2016) 6, e441; doi:10.1038/bcj.2016.50 www.nature.com/bcj REVIEW Acute myeloid leukemia: a comprehensive review and 2016 update I De Kouchkovsky 1 and M Abdul-Hay 1,2 Acute myeloid leukemia
OPEN Citation: (2016) 6, e441; doi:10.1038/bcj.2016.50 www.nature.com/bcj REVIEW Acute myeloid leukemia: a comprehensive review and 2016 update I De Kouchkovsky 1 and M Abdul-Hay 1,2 Acute myeloid leukemia
Update on Myelodysplastic Syndromes and Myeloproliferative Neoplasms. Kaaren Reichard Mayo Clinic Rochester
 Update on Myelodysplastic Syndromes and Myeloproliferative Neoplasms Kaaren Reichard Mayo Clinic Rochester Reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Learning Objectives Present
Update on Myelodysplastic Syndromes and Myeloproliferative Neoplasms Kaaren Reichard Mayo Clinic Rochester Reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Learning Objectives Present
CHALLENGING CASES PRESENTATION
 CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
Fluorescence in-situ Hybridization (FISH) ETO(RUNX1T1)/AML1(RUNX1) or t(8;21)(q21.3;q22)
 PML/RARA t(15;17) Translocation Assay Result : nuc ish(pml 2)(RARA 2)[200] : 200/200(100%) interphase nuclei show normal 2O 2G signals for PML/RARA : is Negative for t(15;17)(q22;q21.1) 2 Orange 2 Green
PML/RARA t(15;17) Translocation Assay Result : nuc ish(pml 2)(RARA 2)[200] : 200/200(100%) interphase nuclei show normal 2O 2G signals for PML/RARA : is Negative for t(15;17)(q22;q21.1) 2 Orange 2 Green
Myelodysplastic syndromes: revised WHO classification and distinction from non-neoplastic conditions
 Myelodysplastic syndromes: revised WHO classification and distinction from non-neoplastic conditions Robert P Hasserjian, MD Associate Professor Massachusetts General Hospital and Harvard Medical School
Myelodysplastic syndromes: revised WHO classification and distinction from non-neoplastic conditions Robert P Hasserjian, MD Associate Professor Massachusetts General Hospital and Harvard Medical School
Oncology Cytogenetics Diagnostic Service - User Guide 2014
 Oncology Cytogenetics Diagnostic Service - User Guide 2014 Contact details Address: Cytogenetics Department 5 th Floor Tower Wing Guy s Hospital Great Maze Pond London SE1 9RT General enquiries 0207 188
Oncology Cytogenetics Diagnostic Service - User Guide 2014 Contact details Address: Cytogenetics Department 5 th Floor Tower Wing Guy s Hospital Great Maze Pond London SE1 9RT General enquiries 0207 188
Acute Myeloid Leukemia
 Acute Myeloid Leukemia Guido Marcucci, M.D. Director, Gehr Family Center for Leukemia Research Hematologic Malignancies and Stem Cell Transplantation Institute City of Hope Acute Myeloid Leukemia Gene
Acute Myeloid Leukemia Guido Marcucci, M.D. Director, Gehr Family Center for Leukemia Research Hematologic Malignancies and Stem Cell Transplantation Institute City of Hope Acute Myeloid Leukemia Gene
HSCT - Minimum Essential Data - A REGISTRATION - DAY 0
 HSCT - Minimum Essential Data - A REGISTRATION - DAY 0 Centre Identification EBMT Code (CIC): Contact person: Hospital: Email: Unit: Patient Data Date of this report: First transplant for this patient?:
HSCT - Minimum Essential Data - A REGISTRATION - DAY 0 Centre Identification EBMT Code (CIC): Contact person: Hospital: Email: Unit: Patient Data Date of this report: First transplant for this patient?:
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed
 MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual
 Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
MRD in CML (BCR-ABL1)
 MRD in CML (BCR-ABL1) Moleculaire Biologie en Cytometrie cursus Barbara Denys LAbo Hematologie UZ Gent 6 mei 2011 2008 Universitair Ziekenhuis Gent 1 Myeloproliferative Neoplasms o WHO classification 2008:
MRD in CML (BCR-ABL1) Moleculaire Biologie en Cytometrie cursus Barbara Denys LAbo Hematologie UZ Gent 6 mei 2011 2008 Universitair Ziekenhuis Gent 1 Myeloproliferative Neoplasms o WHO classification 2008:
