Manthena V. Varma, PhD 1 and Ayman F. El-Kattan, PhD 2
|
|
|
- Georgina Harris
- 5 years ago
- Views:
Transcription
1 Supplement Article Transporter-Enzyme Interplay: Deconvoluting Effects of Hepatic Transporters and Enzymes on Drug Disposition Using Static and Dynamic Mechanistic Models The Journal of Clinical Pharmacology (2016), 56(S7) S99 S109 C 2016, The American College of Clinical Pharmacology DOI: /jcph.695 Manthena V. Varma, PhD 1 and Ayman F. El-Kattan, PhD 2 Abstract A large body of evidence suggests hepatic uptake transporters, organic anion-transporting polypeptides (OATPs), are of high clinical relevance in determining the pharmacokinetics of substrate drugs, based on which recent regulatory guidances to industry recommend appropriate assessment of investigational drugs for the potential drug interactions. We recently proposed an extended clearance classification system (ECCS) framework in which the systemic clearance of class 1B and 3B drugs is likely determined by hepatic uptake.the ECCS framework therefore predicts the possibility of drug-drug interactions (DDIs) involving OATPs and the effects of genetic variants of SLCO1B1 early in the discovery and facilitates decision making in the candidate selection and progression. Although OATP-mediated uptake is often the rate-determining process in the hepatic clearance of substrate drugs,metabolic and/or biliary components also contribute to the overall hepatic disposition and,more importantly,to liver exposure.clinical evidence suggests that alteration in biliary efflux transport or metabolic enzymes associated with genetic polymorphism leads to change in the pharmacodynamic response of statins, for which the pharmacological target resides in the liver. Perpetrator drugs may show inhibitory and/or induction effects on transporters and enzymes simultaneously. It is therefore important to adopt models that frame these multiple processes in a mechanistic sense for quantitative DDI predictions and to deconvolute the effects of individual processes on the plasma and hepatic exposure. In vitro data-informed mechanistic static and physiologically based pharmacokinetic models are proven useful in rationalizing and predicting transporter-mediated DDIs and the complex DDIs involving transporter-enzyme interplay. Keywords cytochrome P-450, drug transporters, drug-drug interactions, extended clearance classification system, organic anion-transporting polypeptides, physiologically based pharmacokinetic model, transporter-enzyme interplay Clearance is one of the most critical determinants of drug exposure in the systemic circulation and consequently at the pharmacological target compartment and, as a result, dictates the therapeutic dose. 1,2 A considerable amount of attention is made in the early drug discovery in identifying the predominant clearance mechanism, which is the cornerstone for (1) adoption of a reliable mechanism-based approach for clearance and consequently for dose predictions and (2) early assessment of the clinical risks associated with drugdrug interactions (DDIs) and genetic variants of drug transporters and/or metabolizing enzymes. 3,4 Drug clearance is often complex and entails more than one contributing process. In the liver, active and/or passive drug transport across the sinusoidal membrane governs the drug availability for subsequent biotransformation by the drug-metabolizing enzymes or efflux across canalicular membrane into bile. 5 In a mathematical sense, the hepatic intrinsic clearance (CL int,h )isa function of transporter-enzyme interplay (equation 1) involving several processes such as hepatic intrinsic active uptake clearance (PS active ), passive transport clearance (PS passive ), active basolateral efflux clearance (PS efflux ), and intrinsic biliary secretory (CL bile )and metabolic clearance (CL met ). 6 9 CL int,h = ( PS active + PS passive ) (CL met + CL bile ) ( PSpassive + PS efflux + CL met + CL bile ) (1) Under a limiting condition where PS passive + PS efflux is smaller than CL met + CL bile, hepatic intrinsic clearance is determined primarily by the hepatic uptake (PS active + PS passive ). On the other hand, when 1 Pharmacokinetics, Dynamics and Metabolism, Worldwide Research and Development, Pfizer Inc, Groton, CT, USA 2 Pharmacokinetics, Dynamics and Metabolism, Worldwide Research and Development, Pfizer Inc, Cambridge, MA, USA Submitted for publication 9 November 2015; accepted 14 December Corresponding Author: Manthena V. Varma, MS, PhD, Pharmacokinetics, Dynamics and Metabolism, Pfizer Global Research & Development, Groton, CT manthena.v.varma@pfizer.com
2 S100 The Journal of Clinical Pharmacology / Vol 56 No S7 (2016) PS passive + PS efflux is appreciable in relation to CL met +CL bile, all the individual processes (equation 1) are required to estimate the overall hepatic clearance. Therefore, it should be emphasized that irrespective of their passive permeability (high or low), uptake transport clearance determines the hepatic clearance of uptake transporter substrates, partially or completely. Drug transporters in the liver include members of the solute carrier family (SLCs), which primarily mediate influx or bidirectional transport of substrate drugs, and the members of the ATP-binding cassette family (ABCs), which functionally efflux drugs out of the hepatocytes into blood or bile compartments Biotransformation of drugs to metabolites occurs primarily by phase I and phase II metabolism, with the liver possessing a high abundance of the enzymes. Clinical evidence thus far suggests that the liver-specific SLC transporters, organic anion-transporting polypeptide (OATP)1B1 and OATP1B3 play a prominent role in the hepatic disposition and thus pharmacokinetics of several drugs, including statins, sartans, and certain glinides Due to the clinical relevance of safety and possibly of efficacy, recent EMA and USFDA regulatory guidances recommend appropriate assessment of investigational drugs for potential drug interactions involving OATP1B1 and OATP1B3 (as victims and/or perpetrators). 10,12,15 18 Practices are emerging or evolving in the drug discovery and development settings to assess OATP substrate and inhibition activity for new molecular entities (NMEs) in order to facilitate prediction/evaluation of pharmacokinetics and DDI liability. Although hepatic uptake could be the ratedetermining process in the systemic clearance of several OATP transporter substrates, enzymatic metabolism and/or biliary efflux may also contribute to the systemic clearance and elimination from the body. For instance, atorvastatin is largely metabolized by the CYP3A4, and repaglinide and cerivastatin are metabolized by CYP2C8 and CYP3A4. The transporter-enzyme interplay may determine the disposition of such dual substrates, and these multiple processes should be simultaneously considered using mechanistic models for the pharmacokinetic and DDI predictions. It is therefore important to adopt extended clearance concepts (equation 1) that frame these multiple processes in a mechanistic sense for clearance predictions and in deconvoluting the individual components of clearance (transporter-enzyme interplay) and thus build confidence in the absorption, distribution, metabolism, and elimination (ADME) attributes of NMEs. In this review theoretical concepts behind transporter-enzyme interplay in the hepatic disposition of drugs are reviewed, and the utility of integrated mechanistic models for predicting clinical pharmacokinetics and DDIs from in vitro data is presented. Further, the state of the mechanistic understanding of the role of transporters and enzymes in regulating the intracellular free target organ (liver) exposure is discussed. Extended Clearance Classification System: Predicting the Role of Hepatic Transporters in Systemic Clearance A broad range of extensive studies using preclinical species and in vitro human reagents are usually required to define the predominant clearance mechanism, which often limits the efficiency in the drug discovery settings. For instance, definitive uptake studies using primary suspension or cultured hepatocyte systems are needed to determine if hepatic uptake is a predominant clearance pathway. To provide early prediction, we recently proposed an extended clearance classification system (ECCS) a framework that can be applied for the prediction of the predominant ratedetermining clearance mechanism based on simple compound physicochemical and in vitro properties, ionization, molecular weight, and permeability (Figure 1). 5 The major mechanisms that determine the systemic clearance of drug molecules include hepatic metabolism, transporter-mediated hepatic uptake, and renal clearance. According to ECCS, compounds are classified as class 1A high-permeability, lowmolecular-weight (MW 400 Da) acids/zwitterions, for which metabolism is likely the primary systemic clearance mechanism; class 1B high-permeability, high-mw (>400 Da) acids/zwitterions, for which transporter-mediated hepatic uptake is the primary systemic clearance mechanism; class 2 highpermeability bases/neutrals, for which metabolism is the primary clearance mechanism; class 3A lowpermeability, low-mw ( 400 Da) acids/zwitterions subjected to renal clearance; class 3B lowpermeability, high-mw (>400 Da) acids/zwitterions with transporter-mediated hepatic uptake clearance; and class 4 low-permeability bases/neutrals with renal clearance likely the predominant clearance mechanism. Validation of this framework with more than 300 drugs for which the predominant clearance mechanism was identified using clinical data yielded a predictive success of >90%. 5 In general, systemic clearance of class 1B and 3B compounds (acids and zwitterions with MW > 400 Da) is primarily determined by the hepatic uptake mediated by OATP transporters. However, once cleared from the blood compartment to the liver compartment, class 1B compounds are metabolized and excreted in bile and/or urine as phase I and/or phase II metabolites, whereas class 3B OATP substrates are eliminated
3 Varma and El-Kattan S101 MW 400 MW >400 Class 1 Metabolism Class 2 High Permeable Class 1A Metabolism Class 1B Hepatic uptake MW 400 MW >400 Class 3 Class 4 Renal Clearance Low Permeable Class 3A Renal clearance Class 3B Hepatic uptake (or) Renal Acids/Zwitterions Bases/Neutrals Figure 1. Extended clearance classification system (ECCS) for predicting the clearance mechanism (rate-determining process). 5 Hepatic uptake mediated by OATPs is likely the rate-determining step in the clearance of class 1B and 3B compounds. unchanged in the bile. Various clinical DDIs, such as those with class 1B and 3B drugs (eg, statins) and singledose rifampicin or cyclosporine have been attributed to the inhibition of hepatic transport mediated by OATP1B1 and possibly other isoforms, OATP1B3 and OATP2B Polymorphisms in SLCO1B1 (encoding OATP1B1) have been demonstrated to have altered transporter activity leading to significant changes in systemic exposure for class 1B and 3B compounds. For all the other ECCS classes, hepatic transporters are less likely to contribute to the systemic clearance. Overall, the ECCS framework is effective in predicting the potential role of hepatic transporters (class 1B and 3B) and the scope of transporter-enzyme interplay in the systemic clearance and elimination of new molecular entities. This approach facilitates proactive prioritization of preclinical ADME characterization to enable medicinal chemistry design efforts toward clearance optimization. Additionally, ECCS can enable prioritization of DDI and pharmacogenetic studies during drug development. Transporter-Mediated Disposition: Pharmacokinetics Predictions Transport kinetic parameters needed for the mechanistic prediction of the hepatic clearance (equation 1) are often derived using primary or cultured hepatocytes Previous studies have demonstrated that in vitro metabolic clearance alone underpredicts in vivo clearance of several OATP substrate drugs; however, the in vitro in vivo correlation is improved when one considers hepatic uptake clearance For instance, Watanabe et al showed that the in vitro uptake clearance obtained using human hepatocytes was similar to in vivo hepatic clearance for several statins, suggesting that hepatic uptake is the ratedetermining process for the clearance of these drugs. 26 Similar conclusions were also reported by others. 28,30 Camenish and Umehara used suspended hepatocytes, liver microsomes, and sandwich-cultured hepatocytes to estimate the intrinsic sinusoidal uptake and efflux, metabolism, and biliary secretory clearances and showed a good in vitro in vivo extrapolation of human clearance for 13 selected compounds. 27 On the other hand, mechanistic approaches were proposed wherein the in vitro transport data have been integrated either into semimechanistic or whole-body PBPK models to simulate in vivo pharmacokinetics for OATP substrates in rats and humans A majority of these studies suggested a systematic underprediction of in vivo uptake clearance and therefore proposed the need for empirical scaling factors (SFs) for the uptake and efflux transport to accurately recapitulate
4 S102 The Journal of Clinical Pharmacology / Vol 56 No S7 (2016) human pharmacokinetics. 29,30,32 34 In some sense, the approach of empirical correction is similar to that proposed earlier for recovering in vivo hepatic clearance determined by metabolism (typical ECCS class 1A and 2 drugs), using in vitro metabolic stability assays based on human liver microsomes and hepatocytes. 35 To increase the confidence in the prospective application of SFs obtained by fitting observed human pharmacokinetics, Jones et al estimated SFs for 7 compounds individually and proposed to use the geometric mean value of these SFs for the novel compounds. 29 Further, to manage the parameter identifiability concern, which possibly occurred due to fitting individual plasma profiles, Li et al applied a nonnumerical global optimization method (ie, brute-force grid search method) that simultaneously leverages data for 7 compounds in searching for a unique set of SFs. 36 The globally fitted SFs have an overall better fitting on the pharmacokinetics of 7 compounds, compared with the geometric mean of individually fitted SFs, and further allowed construction of confidence intervals for globally optimized SFs as well as prediction intervals for the predicted plasma concentration-time courses. 36 However, because the fraction of each transporter s contribution to the total active uptake may be different for each compound, the underlying assumption that all transporters share a similar scaling factor may add to the uncertainty in applying the refined model for projecting pharmacokinetics of NMEs. In order to estimate transporter-specific scaling factors, the fractional contribution that each transporter made to the total active uptake needs to be better understood. 37 Alternatively, identifying selective substrates with clinical pharmacokinetic data could facilitate determination of transporter-specific SFs. Nevertheless, this PBPK platform was successfully applied to evaluate the tissue exposure and pharmacogenetic effects on the plasma pharmacokinetics of OATPs substrates. 38,39 It should be noted that the empirical SFs are influenced by the implementation of in vitro methodologies to estimate transporter kinetics, and thus, the derived SFs could vary from laboratory to laboratory. A potential reason for the need for SFs is differing transporter abundances between in vitro and in vivo systems, which may be accounted for by using the concept of relative expression factor (REF, ie, ratio between in vivo and in vitro protein expression). 37 After accounting for the experimentally determined abundance differences in their HEK-based transfected cells and the human hepatocytes or liver samples, Bosgra et al showed a reasonable prediction of the rosuvastatin plasma concentration-time profile using a PBPK model. 40 Although the REF methodology was shown to recover rosuvastatin pharmacokinetics, only minimal differences in the protein expression noted between the in vitro systems (eg, hepatocytes) and liver tissue (based on the LC-MS based quantitative proteomics of OATPs) imply that REFs cannot completely explain the in vitro in vivo disconnect in the hepatic uptake for OATP substrate drugs. The middleout PBPK models built and refined using in vitro and clinical pharmacokinetic data of a set of OATP substrates have proven useful for pharmacokinetic predictions in drug discovery and in assessing DDIs, and additional studies are warranted in this space to build further confidence in the prospective predictions. Transporter-Enzyme Interplay: Quantitative Predictions of DDIs As discussed, the overall hepatic intrinsic clearance involving transporter-enzyme interplay is defined by the extended clearance concept (equation 1). Therefore, the magnitude of change in the clearance of the victim drug when dosed with a perpetrator or a combination of perpetrator drugs can be mechanistically described by an extended net effect model. 44 In the presence of a perpetrator, the expected net effect of reversible inhibition of uptake or biliary efflux and reversible inhibition, time-dependent inhibition, and induction of CYPs on the intrinsic hepatic clearance can be estimated by equation 2: ( ) CL PS active int,h = + PS passive R OATP ( CL CYP + CL ) bile R CYP.TDI CYP.IND CYP. ( PS passive + R efflux CL CYP R CYP.TDI CYP.IND CYP + CL bile R efflux where R OATP and R efflux are the competitive inhibition terms against OATP-mediated uptake and ABC-mediated biliary efflux, respectively. R CYP is the competitive inhibition term, TDI CYP is the timedependent inhibition term, and IND CYP is the induction term against enzyme-based metabolism. 30,45,46 Figure 2 illustrates the influence of transport and metabolism components on the magnitude of DDIs of victim drug (AUC ratio). It should be emphasized that an OATP substrate drug with high active and low metabolic/biliary intrinsic clearance with reference to passive uptake will show higher DDIs. However, a substrate drug with a low active and high metabolic and biliary components will show lower change in plasma exposure, even when the coadministered perpetrator drug is a potent inhibitor of both active and metabolic/biliary processes (eg, R-value of 10) (Figure 2). Although comprehensive experimental data ) (2)
5 Varma and El-Kattan S103 When, R OATP = 1+I/KI OATP = 10 R CYP = 1+I/KI CYP = 10 At a fixed passive (as a function of activeto-passive ratio and metabolic-to-passive ratio) Low active uptake and high metabolism Low/No DDI risk Low active uptake and low metabolism DDI risk on inhibition of metabolism High active uptake and high metabolism DDI risk on inhibition of active uptake High active uptake and low metabolism High DDI risk Figure 2. Surface plot of the effect of 90% inhibition of both active uptake and metabolic/biliary clearance of victim drugs that are substrates to hepatic uptake transporter (eg, OATP1B1: atorvastatin and pravastatin) and enzyme (eg, CYP3A4: atorvastatin) or biliary efflux pump (eg, MRP2: pravastatin). Gray surface represents R-value (= 10, assuming 90% inhibition of uptake or biliary/metabolic clearance), and light gray surface represents R-value product (= 100,assuming 90% inhibition of both uptake and biliary/metabolic clearance).the magnitude of AUC change depends on the intrinsic victim characteristics along with the perpetrator interaction potential, as described by equation 2. Predicted AUC ratios were based on extended-clearance term assuming liver as the only clearing organ. PS passive was kept constant at 10 ml/(min kg). Based on the mechanistic predictions (extended neteffect model), it should be noted that the DDI is highest for victim drugs with CL met+bile < PS passive and PS active > PS passive (depicted as hypothetical drug 4). on the individual intrinsic clearances are required for applying the extended net effect model, they integrate the mechanistic aspects of transporter-enzyme interplay and are expected to produce quantitative predictions. When the perpetrator drug does not inhibit or induce metabolic or biliary pathways of the victim drug, the change in its hepatic clearance can be simplified to equation 3. CL int,h CL int,h ( PSactive + PS passive ) = ( );where, PS active + PS passive R OATP ( R OATP = 1 + [I ) u,max,in] Ki OATP (3) In addition to this, if PS active >> PS passive,the change in hepatic clearance, which signifies the AUC ratio, will be further simplified to R OATP (also referred as R-value). Here, I u,max,in is the relevant inhibitor unbound concentration at the inlet to the liver or portal vein concentration (equation 3), and K i is the unbound inhibition constant determined in vitro. 10,16,22,47,48 Generally, static models have the advantage of being simple and more transparent and can be valuable in quantitative predictions of DDI scenarios in drug discovery and development. The applicability of the extended net effect model in the prediction of complex DDIs associated with multiple enzyme- and transportermediated processes was presented earlier. 30,44,49 Hepatic transport kinetics and enzymatic (CYPs) stability data of the victim drug obtained from in vitro systems such as sandwich culture human hepatocytes (SCHH) or suspension hepatocytes and human liver microsomes can be used as inputs along with a validated scaling factor for active uptake for prospective predictions of transporter-mediated and complex DDI situations. 30,44,49 PBPK modeling approaches have emerged for a wide array of applications in the drug industry, mainly due to the significant advantages this platform provides compared to more traditional mathematical approaches Indeed, PBPK models provide a mechanistic framework to assess DDI risk during all stages of drug discovery and development. However, there is a level of uncertainty around the human pharmacokinetics and efficacious drug concentration in man prior to first-in-human (FIH) studies Furthermore, in complex situations such as when transporter-enzyme interplay is involved in drug disposition and DDIs, models need to be calibrated with both in vitro parameters ( bottom-up ) and observed in vivo PK or clinical DDI results ( top-down ). 51,52,56 59 Therefore, mechanistic static models are of utility at this stage. Applications of PBPK models for DDIs are generally fully realized once human plasma concentration-time profile data become available to verify or refine the bottomup models, which could be utilized to inform decisions on the inclusion and exclusion of concomitant medications during phase 2 studies and beyond. The application and utility of PBPK models for DDIs involving hepatic transporters and transporterenzyme interplay are now well documented in the literature. 34,49,56,58,60,61 Furthermore, PBPK models can
6 S104 The Journal of Clinical Pharmacology / Vol 56 No S7 (2016) Figure 3. A proposed strategy for model-based predictions of transporter and complex DDIs associated with transporter-enzyme interplay. (a) Different cutoff may be considered for the significance of R-value based on the therapeutic index of the victim drug. (b) Cutoff values for CYP interactions are given as suggested in the US FDA draft guidelines. 16 (c) For complete mathematical expressions of the extended net-effect model refer to Varma et al. 30 employ system parameters (eg, human demographics and genetics, tissue volumes and blood flows, enzyme and transporter expression levels) and drugdependent parameters (eg, tissue partition coefficients, metabolism, or transport rates), which allow prediction of outcomes across population extremes or disease variability beyond the prediction for an average individual. A strategy for model-based predictions of transporter and complex DDIs associated with transporterenzyme interplay has been put forward to facilitate decision making and address specific questions in various stages of NME progression (Figure 3). For evaluating DDI risk, an early assessment of hepatic transporter- or enzyme-mediated DDIs can be achieved with static basic models (R-value) incorporating in vitro and in vivo pharmacokinetic parameters of the perpetrator drug alone. The R-value generally provides an oversimplification of the transporter-mediated DDI risk, assuming that hepatic active transport (uptake and biliary efflux) is responsible individually for 100% of systemic clearance of the victim drug (equation 3). 10,16 A more conservative estimate (R-value product) with theoretical maximum inhibition of hepatic clearance (inhibition of both uptake and metabolism or biliary efflux simultaneously) was also suggested to minimize false-negative predictions. 10,22 Because of its conservative nature, a positive indication of DDI using these basic models would require further assessment using a static extended net effect model or dynamic PBPK models for quantitative prediction. Herein, the predictions are based on transporter-enzyme interplay and are for a given victim-perpetrator combination. In assessing the victim DDI liability of ECCS class 3B NMEs, reversible inhibition of hepatic uptake and/or biliary transporters should be considered simultaneously if the basic models show positive signal against individual mechanisms. Similarly, for ECCS class 1B NMEs, reversible inhibition of uptake transporters and/or enzyme inhibition and induction should be assessed simultaneously.
7 Varma and El-Kattan S105 It should be emphasized that situations arise where interactions at uptake and metabolism or biliary levels are small individually, but, when integrated together using mechanistic models, could be significantly higher (Figure 2). Therefore, basic model (eg, R-value) predictions are not necessarily conservative estimates of DDI risk and could result in false-negative predictions when multiple mechanisms are involved. Overall, when hepatic transporters are involved in the disposition of NMEs, mechanistic models integrating transporterenzyme interplay should be implemented (Figure 3). Transporter-Enzyme Interplay: Clinical Relevance of Unbound Concentration in Liver For several substrate drugs (eg, statins), free liver concentrations/exposures are key determinants of efficacy due to localization of pharmacological targets in the hepatocytes PK/PD relationships are typically established assuming plasma concentration and the intracellular concentration at target site are in equilibrium and identical, and therefore, a change in systemic pharmacokinetics is believed to translate to an equivalent effect on the target-site concentrations. However, substrates of hepatic active transport (eg, OATPs) are highly concentrated in the liver, and inhibition of hepatic uptake or metabolism and efflux will have differential effects on plasma and liver concentrations. 7,66 Free liver-to-plasma ratio, also referred as Kp uu,canbe described mathematically as in equation 4: Kp uu = PS uptake + PS passive PS passive + PS efflux + CL met+bile (4) However, the exposure of substrate drug in the liver (area under liver concentration-time profile, AUC h )is a function of metabolic and/or biliary intrinsic clearances, dose, and unbound faction in liver (f h ), when liver is the only eliminating organ (equation 5). 7 AUC h f h = Dose CL met+bile (5) Based on these equations, it can be indicated that the change in active uptake clearance due to drug interactions or polymorphic variants (1) does not alter the overall hepatic exposure (AUC h ), particularly when the nonhepatic clearance is negligible, and (2) possibly alters free hepatic concentration of substrate at a given time, ie, altered liver concentration-time profile shape and Kp uu. On the other hand, altered hepatic metabolic or biliary intrinsic clearance shows relatively less effect on the systemic exposure, whereas it significantly influences the hepatic exposure (Table 1). Although the direct clinical evidence on the potential changes in hepatic exposure is limited, conclusions may be drawn based on PBPK modeling and/or clinical pharmacodynamic readouts. When PBPK model-based sensitivity analyses have been used to assess the influence of transport and metabolic/biliary intrinsic clearances on the systemic and hepatic exposure, lack of change in AUC h was suggested with altered active uptake clearance for several OATP substrates, including pravastatin, 33 repaglinide, 58 rosuvastatin, 67 and glyburide. 60 Rose et al applied PBPK/PD model to assess the impact of genotype-dependent uptake by OATP1B1 on the pharmacodynamic response of rosuvastatin and indicated that reduced OATP1B1 activity translated to relatively large increases in plasma rosuvastatin concentration and a small change in liver exposure, as a result explaining the lack of significant impact on pharmacodynamic response in the clinical studies. 67 However, if the renal clearance is significant, the AUC h is relatively more affected, and plasma AUC is less affected, by the changes in hepatic uptake clearance. 7 This is exemplified by metformin, which is cleared mainly renally, although it is taken up by OCT1 into liver, where it manifests pharmacodynamic responses. 68,69 Polymorphism in SLC22A1 (gene encoding OCT1) showed minimal change in plasma exposure of metformin; however, the pharmacodynamic response (blood glucose and hemoglobin A1c change) is potentiated The SEARCH genome-wide association study found a significant association between c.521t>c single-nucleotide polymorphism in the SLCO1B1 gene and simvastatin-induced myopathy in individuals taking higher simvastatin doses linking higher systemic exposure of simvastatin acid in genetic variants to higher incidence of toxicity. 73 Interestingly, all the pharmacogenomic studies of statins showed lack of impact on the pharmacodynamic responses, although the plasma exposure is significantly increased in the population carrying a reduced-activity mutant of SLCO1B1 (Table 1). However, genetic variants of metabolizing enzymes (CYP3A) and biliary efflux transporters (ABCB1 and ABCG2) resulted in significant change in the pharmacodynamic effects of several statins. These clinical findings may suggest that the pharmacological response of statins (HMG-CoA reductase inhibition) is mainly associated with liver exposure (AUC h ) rather than the liver concentrationtime profile or Kp uu. Interestingly, simulations suggested minimal change in the concentration-time profiles in the liver along with minimal change in AUC h for pravastatin and rosuvastatin. 33,67 The possibility of increased systemic and thus hepatic exposure of statins due to reduced intestinal efflux and gut metabolism can not be ruled out. 9,74 Further understanding in these areas is warranted, which may be facilitated by the PBPK models integrated with pharmacodynamic
8 S106 The Journal of Clinical Pharmacology / Vol 56 No S7 (2016) Table 1. Differential Effects of Genotypic Variation in the Uptake Transporter (SLCO1B1) and Biliary Efflux Transporters or Metabolizing Enzymes on the Pharmacokinetics and Liver-Specific Pharmacodynamics of Statins Statin Gene Genotype Reference a Genotype Variant Change in Plasma AUC (%) Significant Change in Pharmacodynamic Effect(s) Genetic Variants of Hepatic Uptake Transporter (OATP1B1) Atorvastatin SLCO1B1 521TT 521TC No TT 521CC No 76 *1A/*1A *15/*15 - No 76 Pravastatin SLCO1B1 521TT 521TC No TT 521CC No 80 *1A/*1A *15/* No 80 Rosuvastatin SLCO1B1 521TT 521TC, 521CC - No TT 521CC No 83 *1A/*1A *15/* AA 388GG No 83 Simvastatin acid SLCO1B1 521TT 521CC No 76 *1A/*1A *15/*15 - No 76 Genetic Variants of Hepatic Efflux Transporters (BCRP and P-gp) and Metabolizing Enzymes Atorvastatin ABCG2 421CC 421AA CC 421CA No 86 ABCB1 3435CC 3435TT - Yes 87 CYP3A4 *1/*1 *1G/*1G 36,88 Yes AA 392GG - Yes 90 Pravastatin ABCG2 421CC 421AA No change CC 421CA No change 91 - Rosuvastatin ABCG2 421CC 421AA 217, ,92 Yes 83,93 ABCB1 2677GA, 2677GG, 2677TT GT Simvastatin acid ABCG2 421CC 421CA, 421AA No change 91 No 81 a Genotype reference: CYP3A4*1/*1, CYP3A5*3/*3, SLCO1B1 521TT; and variant genotype: CYP3A4*1G/*1G, CYP3A5*3/*3, SLCO1B1 521TT. models. More importantly, clinical risk-to-benefit assessment must be weighed in the dose adjustments during comedication. For instance, dose adjustments based on plasma exposure during comedication may avoid systemic adverse events (such as myopathy and rhabdomyolysis with statins), but they also reduce overall hepatic exposure (AUC h ) and could lead to lack of clinical efficacy due to reduced target-site exposure. Conclusion Drug disposition via liver involves several processes including influx transport into hepatocytes, basolateral efflux into blood circulation, hepatocytic metabolism, and canalicular efflux into bile. One or multiples of these processes determine the systemic clearance of a drug, as defined by the extended clearance concept. The understanding of transporter-enzyme interplay is thus important in defining the rate-determining step in the overall hepatic clearance and ultimately in assessing the variability in systemic pharmacokinetics and local tissue concentration associated with DDIs and pharmacogenomics. ECCS provides an early indication of the rate-determining step to the systemic clearance and can greatly facilitate clearance optimization and DDI predictions. Further, through the use of in vitro tools and translational models it is possible to quantitatively predict and rationalize the clinical DDI studies for drug candidates in development. Additionally, mechanistic models verified with early clinical data can be helpful in assessing DDIs associated with polymorphic clearance pathways or in understanding drug disposition and DDIs in disease states or in special populations. Conflict of Interest The authors have no conflicts of interest to declare. References 1. Obach RS, Baxter JG, Liston TE, et al. The prediction of human pharmacokinetic parameters from preclinical and in vitro metabolism data. J Pharmacol Exp Ther. 1997;283(1): van de Waterbeemd H, Gifford E. ADMET in silico modelling: towards prediction paradise? Nat Rev Drug Discov. 2003;2(3): Wienkers LC, Heath TG. Predicting in vivo drug interactions from in vitro drug discovery data. Nat Rev Drug Discov. 2005;4(10): Bjornsson TD, Callaghan JT, Einolf HJ, et al. The conduct of in vitro and in vivo drug-drug interaction studies: a Pharmaceutical Research and Manufacturers of America (PhRMA) perspective. Drug Metab Dispos. 2003;31(7): Varma MV, Steyn SJ, Allerton C, El-Kattan AF. Predicting clearance mechanism in drug discovery: extended clearance classification system (ECCS). Pharm Res. 2015;32(12):
9 Varma and El-Kattan S Li R, Barton HA, Varma MV. Prediction of pharmacokinetics and drug-drug interactions when hepatic transporters are involved. Clin Pharmacokinet. 2014;53(8): Shitara Y, Maeda K, Ikejiri K, Yoshida K, Horie T, Sugiyama Y. Clinical significance of organic anion transporting polypeptides (OATPs) in drug disposition: their roles in hepatic clearance and intestinal absorption. Biopharm Drug Dispos. 2013;34(1): Sirianni GL, Pang KS. Organ clearance concepts: new perspectives on old principles. J Pharmacokinet Biopharm. 1997;25(4): Yoshida K, Maeda K, Sugiyama Y. Hepatic and intestinal drug transporters: prediction of pharmacokinetic effects caused by drug-drug interactions and genetic polymorphisms. Annu Rev Pharmacol Toxicol. 2013;53: Giacomini KM, Huang SM, Tweedie DJ, et al. Membrane transporters in drug development. Nat Rev Drug Discov. 2010;9(3): Shitara Y, Horie T, Sugiyama Y. Transporters as a determinant of drug clearance and tissue distribution. Eur J Pharm Sci. 2006;27(5): Niemi M, Pasanen MK, Neuvonen PJ. Organic anion transporting polypeptide 1B1: a genetically polymorphic transporter of major importance for hepatic drug uptake. Pharmacol Rev. 2011;63(1): Treiber A, Schneiter R, Häusler S, Stieger B. Bosentan is a substrate of human OATP1B1 and OATP1B3: inhibition of hepatic uptake as the common mechanism of its interactions with cyclosporin A, rifampicin, and sildenafil. Drug Metab Dispos. 2007;35(8): Yamashiro W, Maeda K, Hirouchi M, Adachi Y, Hu Z, Sugiyama Y. Involvement of transporters in the hepatic uptake and biliary excretion of valsartan, a selective antagonist of the angiotensin II AT1-receptor, in humans. Drug Metab Dispos. 2006;34(7): EMA. Guideline on the Investigation of Drug Interactions. Committee for Human Medicinal Products (CHMP). London, UK; USFDA. Drug Interaction Studies Study Design, Data Analysis, Implications for Dosing, and Labeling Recommendations. Center for Drug Evaluation and Research (CDER). Silver Spring, MD; Barton HA, Lai Y, Goosen TC, et al. Model-based approaches to predict drug-drug interactions associated with hepatic uptake transporters: preclinical, clinical and beyond. Expert Opin Drug Metab Toxicol. 2013;9(4): Shitara Y, Sugiyama Y. Pharmacokinetic and pharmacodynamic alterations of 3-hydroxy-3-methylglutaryl coenzyme A (HMG-CoA) reductase inhibitors: drug-drug interactions and interindividual differences in transporter and metabolic enzyme functions. Pharmacol Ther. 2006;112(1): Lau YY, Huang Y, Frassetto L, Benet LZ. Effect of OATP1B transporter inhibition on the pharmacokinetics of atorvastatin in healthy volunteers. Clin Pharmacol Ther. 2007;81(2): Regazzi MB, Iacona I, Campana C, et al. Altered disposition of pravastatin following concomitant drug therapy with cyclosporin A in transplant recipients. Transplant Proc. 1993;25(4): Schneck DW, Birmingham BK, Zalikowski JA, et al. The effect of gemfibrozil on the pharmacokinetics of rosuvastatin. Clin Pharmacol Ther. 2004;75(5): Yoshida K, Maeda K, Sugiyama Y. Transporter-mediated drug-drug interactions involving OATP substrates: predictions based on in vitro inhibition studies. Clin Pharmacol Ther. 2012;91(6): Bi Y-a, Kazolias D, Duignan DB. Use of cryopreserved human hepatocytes in sandwich culture to measure hepatobiliary transport. Drug Metab Dispos. 2006;34(9): Brouwer KL, Keppler D, Hoffmaster KA, et al. In vitro methods to support transporter evaluation in drug discovery and development. Clin Pharmacol Ther. 2013;94(1): Zamek-Gliszczynski MJ, Lee CA, Poirier A, et al. ITC recommendations for transporter kinetic parameter estimation and translational modeling of transport-mediated PK and DDIs in humans. Clin Pharmacol Ther. 2013;94(1): Watanabe T, Kusuhara H, Maeda K, et al. Investigation of the rate-determining process in the hepatic elimination of HMG- CoA reductase inhibitors in rats and humans. Drug Metab Dispos. 2010;38(2): Camenisch G, Umehara K. Predicting human hepatic clearance from in vitro drug metabolism and transport data: a scientific and pharmaceutical perspective for assessing drug-drug interactions. Biopharm Drug Dispos. 2012;33(4): Menochet K, Kenworthy KE, Houston JB, Galetin A. Use of mechanistic modeling to assess interindividual variability and interspecies differences in active uptake in human and rat hepatocytes. Drug Metab Dispos. 2012;40(9): Jones HM, Barton HA, Lai Y, et al. Mechanistic pharmacokinetic modeling for the prediction of transporter-mediated disposition in humans from sandwich culture human hepatocyte data. Drug Metab Dispos. 2012;40(5): Varma MV, Bi Y-a, Kimoto E, Lin J. Quantitative prediction of transporter- and enzyme-mediated clinical drug-drug interactions of organic anion-transporting polypeptide 1B1 substrates using a mechanistic net-effect model. J Pharmacol Exp Ther. 2014;351(1): Paine SW, Parker AJ, Gardiner P, Webborn PJ, Riley RJ. Prediction of the pharmacokinetics of atorvastatin, cerivastatin, and indomethacin using kinetic models applied to isolated rat hepatocytes. Drug Metab Dispos. 2008;36(7): Poirier A, Cascais AC, Funk C, Lave T. Prediction of pharmacokinetic profile of valsartan in human based on in vitro uptake transport data. J Pharmacokinet Pharmacodyn. 2009;36(6): Watanabe T, Kusuhara H, Maeda K, Shitara Y, Sugiyama Y. Physiologically based pharmacokinetic modeling to predict transporter-mediated clearance and distribution of pravastatin in humans. J Pharmacol Exp Ther. 2009;328(2): Varma MV, Lai Y, Feng B, Litchfield J, Goosen TC, Bergman A. Physiologically based modeling of pravastatin transportermediated hepatobiliary disposition and drug-drug interactions. Pharm Res. 2012;29(10): Ito K, Houston JB. Prediction of human drug clearance from in vitro and preclinical data using physiologically based and empirical approaches. Pharm Res. 2005;22(1): Li R, Barton HA, Yates PD, et al. A middle-out approach to human pharmacokinetic predictions for OATP substrates using physiologically-based pharmacokinetic modeling. J Pharmacokinet Pharmacodyn. 2014;41(3): Hirano M, Maeda K, Shitara Y, Sugiyama Y. Contribution of OATP2 (OATP1B1) and OATP8 (OATP1B3) to the hepatic uptake of pitavastatin in humans. J Pharmacol Exp Ther. 2004;311(1): Li R, Barton HA, Maurer TS. Toward prospective prediction of pharmacokinetics in OATP1B1 genetic variant populations. CPT Pharmacometr Syst Pharmacol. 2014;3:e151.
10 S108 The Journal of Clinical Pharmacology / Vol 56 No S7 (2016) 39. Li R, Ghosh A, Maurer TS, Kimoto E, Barton HA. Physiologically based pharmacokinetic prediction of telmisartan in human. Drug Metab Dispos. 2014;42(10): Bosgra S, Steeg EV, Vlaming ML, et al. Predicting carriermediated hepatic disposition of rosuvastatin in man by scaling from individual transfected cell-lines in vitro using absolute transporter protein quantification and PBPK modeling. Eur J Pharm Sci. 2014;65: Badee J, Achour B, Rostami-Hodjegan A, Galetin A. Metaanalysis of expression of hepatic organic anion-transporting polypeptide (OATP) transporters in cellular systems relative to human liver tissue. Drug Metab Dispos. 2015;43(4): Kimoto E, Yoshida K, Balogh LM, et al. Characterization of organic anion transporting polypeptide (OATP) expression and its functional contribution to the uptake of substrates in human hepatocytes. Mol Pharmacol. 2012;9(12): Prasad B, Evers R, Gupta A, et al. Interindividual variability in hepatic organic anion-transporting polypeptides and P- glycoprotein (ABCB1) protein expression: quantification by liquid chromatography tandem mass spectroscopy and influence of genotype, age, and sex. Drug Metab Dispos. 2014;42(1): Varma MV, Lin J, Bi YA, et al. Quantitative prediction of repaglinide-rifampicin complex drug interactions using dynamic and static mechanistic models: delineating differential CYP3A4 induction and OATP1B1 inhibition potential of rifampicin. Drug Metab Dispos. 2013;41(5): Fahmi OA, Hurst S, Plowchalk D, et al. Comparison of different algorithms for predicting clinical drug-drug interactions, based on the use of CYP3A4 in vitro data: predictions of compounds as precipitants of interaction. Drug Metab Dispos. 2009;37(8): Fahmi OA, Maurer TS, Kish M, Cardenas E, Boldt S, Nettleton D. A combined model for predicting CYP3A4 clinical net drug-drug interaction based on CYP3A4 inhibition, inactivation, and induction determined in vitro. Drug Metab Dispos. 2008;36(8): Karlgren M, Ahlin G, Bergstrom CA, Svensson R, Palm J, Artursson P. In vitro and in silico strategies to identify OATP1B1 inhibitors and predict clinical drug-drug interactions. Pharm Res. 2012;29(2): Karlgren M, Vildhede A, Norinder U, et al. Classification of inhibitors of hepatic organic anion transporting polypeptides (OATPs): influence of protein expression on drug-drug interactions. J Med Chem. 2012;55(10): Varma MV, Lin J, Bi YA, Kimoto E, Rodrigues AD. Quantitative rationalization of gemfibrozil drug interactions: consideration of transporters-enzyme interplay and the role of circulating metabolite gemfibrozil 1-O-beta-glucuronide. Drug Metab Dispos. 2015;43(7): Jones HM, Chen Y, Gibson C, et al. Physiologically based pharmacokinetic modeling in drug discovery and development: a pharmaceutical industry perspective. Clin Pharmacol Ther. 2015;97(3): Huang SM, Rowland M. The role of physiologically based pharmacokinetic modeling in regulatory review. Clin Pharmacol Ther. 2012;91(3): Rostami-Hodjegan A. Physiologically based pharmacokinetics joined with in vitro-in vivo extrapolation of ADME: a marriage under the arch of systems pharmacology. Clin Pharmacol Ther. 2012;92(1): Sinha VK, Snoeys J, Osselaer NV, Peer AV, Mackie C, Heald D. From preclinical to human prediction of oral absorption and drug-drug interaction potential using physiologically based pharmacokinetic (PBPK) modeling approach in an industrial setting: a workflow by using case example. Biopharm Drug Dispos. 2012;33(2): Chen Y, Jin JY, Mukadam S, Malhi V, Kenny JR. Application of IVIVE and PBPK modeling in prospective prediction of clinical pharmacokinetics: strategy and approach during the drug discovery phase with four case studies. Biopharm Drug Dispos. 2012;33(2): Zhao P, Rowland M, Huang SM. Best practice in the use of physiologically based pharmacokinetic modeling and simulation to address clinical pharmacology regulatory questions. Clin Pharmacol Ther. 2012;92(1): Gertz M, Cartwright CM, Hobbs MJ, et al. Cyclosporine inhibition of hepatic and intestinal CYP3A4, uptake and efflux transporters: application of PBPK modeling in the assessment of drug-drug interaction potential. Pharm Res. 2013;30(3): Varma MV, Lai Y, Feng B, Litchfield J, Goosen TC, Bergman A. Physiologically based modeling of pravastatin transportermediated hepatobiliary disposition and drug-drug interactions. Pharm Res Varma MV, Lai Y, Kimoto E, Goosen TC, El-Kattan AF, Kumar V. Mechanistic modeling to predict the transporter- and enzyme-mediated drug-drug interactions of repaglinide. Pharm Res. 2013;30(4): Varma MV, Lai Y, Feng B, Litchfield J, Goosen TC, Bergman A. Response to the comment on the article Physiologically Based Modeling of Pravastatin Transporter-Mediated Hepatobiliary Disposition and Drug-Drug Interactions. Pharm Res. 2013;30(6): Varma MV, Scialis RJ, Lin J, et al. Mechanism-based pharmacokinetic modeling to evaluate transporter-enzyme interplay in drug interactions and pharmacogenetics of glyburide. AAPS J. 2014;16(4): Jamei M, Bajot F, Neuhoff S, et al. A mechanistic framework for in vitro-in vivo extrapolation of liver membrane transporters: prediction of drug-drug interaction between rosuvastatin and cyclosporine. Clin Pharmacokinet. 2014;53(1): Moller DE. New drug targets for type 2 diabetes and the metabolic syndrome. Nature. 2001;414(6865): Corsini A, Maggi FM, Catapano AL. Pharmacology of competitive inhibitors of HMG-CoA reductase. Pharmacol Res. 1995;31(1): Pfefferkorn JA, Guzman-Perez A, Litchfield J, et al. Discovery of (S)-6-(3-cyclopentyl-2-(4-(trifluoromethyl)-1 H-imidazol- 1-yl) propanamido) nicotinic acid as a hepatoselective glucokinase activator clinical candidate for treating type 2 diabetes mellitus. J Med Chem. 2012;55(3): Oballa RM, Belair L, Black WC, et al. Development of a livertargeted stearoyl-coa desaturase (SCD) inhibitor (MK-8245) to establish a therapeutic window for the treatment of diabetes and dyslipidemia. J Med Chem. 2011;54(14): Chu X, Korzekwa K, Elsby R, et al. Intracellular drug concentrations and transporters: measurement, modeling, and implications for the liver. Clin Pharmacol Ther. 2013;94(1): Rose RH, Neuhoff S, Abduljalil K, Chetty M, Rostami- Hodjegan A, Jamei M. Application of a physiologically based pharmacokinetic model to predict OATP1B1-related variability in pharmacodynamics of rosuvastatin. CPT: Pharmacometrics Syst Pharmacol. 2014;3:e Graham GG, Punt J, Arora M, et al. Clinical pharmacokinetics of metformin. Clin Pharmacokinet. 2011;50(2): Tzvetkov MV, Vormfelde SV, Balen D, et al. The effects of genetic polymorphisms in the organic cation transporters OCT1, OCT2, and OCT3 on the renal clearance of metformin. Clin Pharmacol Ther. 2009;86(3):
11 Varma and El-Kattan S Christensen MM, Hojlund K, Hother-Nielsen O, et al. Steadystate pharmacokinetics of metformin is independent of the OCT1 genotype in healthy volunteers. Eur J Clin Pharmacol. 2015;71(6): Shu Y, Brown C, Castro RA, et al. Effect of genetic variation in the organic cation transporter 1, OCT1, on metformin pharmacokinetics. Clin Pharmacol Ther. 2008;83(2): Christensen MM, Brasch-Andersen C, Green H, et al. The pharmacogenetics of metformin and its impact on plasma metformin steady-state levels and glycosylated hemoglobin A1c. Pharmacogenet Genomics. 2011;21(12): Group SC, Link E, Parish S, et al. SLCO1B1 variants and statin-induced myopathy-a genomewide study. NEnglJMed. 2008;359(8): Niemi M. Transporter pharmacogenetics and statin toxicity. Clin Pharmacol Ther. 2010;87(1): Pasanen MK, Fredrikson H, Neuvonen PJ, Niemi M. Different effects of SLCO1B1 polymorphism on the pharmacokinetics of atorvastatin and rosuvastatin. Clin Pharmacol Ther. 2007;82(6): Fu Q, Li YP, Gao Y, et al. Lack of association between SLCO1B1 polymorphism and the lipid-lowering effects of atorvastatin and simvastatin in Chinese individuals. Eur J Clin Pharmacol. 2013;69(6): Niemi M, Schaeffeler E, Lang T, et al. High plasma pravastatin concentrations are associated with single nucleotide polymorphisms and haplotypes of organic anion transporting polypeptide-c (OATP-C, SLCO1B1). Pharmacogenetics. 2004;14(7): Ho RH, Choi L, Lee W, et al. Effect of drug transporter genotypes on pravastatin disposition in Europeanand African-American participants. Pharmacogenet Genomics. 2007;17(8): Niemi M, Pasanen MK, Neuvonen PJ. SLCO1B1 polymorphism and sex affect the pharmacokinetics of pravastatin but not fluvastatin. Clin Pharmacol Ther. 2006;80(4): Martin NG, Li KW, Murray H, Putt W, Packard CJ, Humphries SE. The effects of a single nucleotide polymorphism in SLCO1B1 on the pharmacodynamics of pravastatin. Br J Clin Pharmacol. 2012;73(2): Bailey KM, Romaine SP, Jackson BM, et al. Hepatic metabolism and transporter gene variants enhance response to rosuvastatin in patients with acute myocardial infarction: the GEOSTAT-1 Study. Circ Cardiovasc Genet. 2010;3(3): Lee E, Ryan S, Birmingham B, et al. Rosuvastatin pharmacokinetics and pharmacogenetics in white and Asian subjects residing in the same environment. Clin Pharmacol Ther. 2005;78(4): Lee HK, Hu M, Lui S, Ho CS, Wong CK, Tomlinson B. Effects of polymorphisms in ABCG2, SLCO1B1, SLC10A1 and CYP2C9/19 on plasma concentrations of rosuvastatin and lipid response in Chinese patients. Pharmacogenomics. 2013;14(11): Pasanen MK, Neuvonen M, Neuvonen PJ, Niemi M. SLCO1B1 polymorphism markedly affects the pharmacokinetics of simvastatin acid. Pharmacogenet Genomics. 2006;16(12): Keskitalo JE, Zolk O, Fromm MF, Kurkinen KJ, Neuvonen PJ, Niemi M. ABCG2 polymorphism markedly affects the pharmacokinetics of atorvastatin and rosuvastatin. Clin Pharmacol Ther. 2009;86(2): Ferrari M, Guasti L, Maresca A, et al. Association between statin-induced creatine kinase elevation and genetic polymorphisms in SLCO1B1, ABCB1 and ABCG2. Eur J Clin Pharmacol. 2014;70(5): Shabana MF, Mishriki AA, Issac MS, Bakhoum SW. Do MDR1 and SLCO1B1 polymorphisms influence the therapeutic response to atorvastatin? A study on a cohort of Egyptian patients with hypercholesterolemia. Mol Diagnosis Ther. 2013;17(5): He BX, Shi L, Qiu J, Zeng XH, Zhao SJ. The effect of CYP3A4*1G allele on the pharmacokinetics of atorvastatin in Chinese Han patients with coronary heart disease. J Clin Pharmacol. 2014;54(4): Gao Y, Zhang LR, Fu Q. CYP3A4*1G polymorphism is associated with lipid-lowering efficacy of atorvastatin but not of simvastatin. Eur J Clin Pharmacol. 2008;64(9): Kajinami K, Brousseau ME, Ordovas JM, Schaefer EJ. CYP3A4 genotypes and plasma lipoprotein levels before and after treatment with atorvastatin in primary hypercholesterolemia. Am J Cardiol. 2004;93(1): Keskitalo JE, Pasanen MK, Neuvonen PJ, Niemi M. Different effects of the ABCG2 c.421c>a SNP on the pharmacokinetics of fluvastatin, pravastatin and simvastatin. Pharmacogenomics. 2009;10(10): Birmingham BK, Bujac SR, Elsby R, et al. Impact of ABCG2 and SLCO1B1 polymorphisms on pharmacokinetics of rosuvastatin, atorvastatin and simvastatin acid in Caucasian and Asian subjects: a class effect? Eur J Clin Pharmacol. 2015;71(3): Tomlinson B, Hu M, Lee VW, et al. ABCG2 polymorphism is associated with the low-density lipoprotein cholesterol response to rosuvastatin. Clin Pharmacol Ther. 2010;87(5): Zhou Q, Ruan ZR, Yuan H, Xu DH, Zeng S. ABCB1 gene polymorphisms, ABCB1 haplotypes and ABCG2 c.421c>a are determinants of inter-subject variability in rosuvastatin pharmacokinetics. Pharmazie. 2013;68(2):
Investigating Transporter-Mediated Drug-Drug Interactions Using a Physiologically Based Pharmacokinetic Model of Rosuvastatin
 Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 228 238; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12168 ORIGINAL ARTICLE Investigating Transporter-Mediated Drug-Drug Interactions Using
Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 228 238; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12168 ORIGINAL ARTICLE Investigating Transporter-Mediated Drug-Drug Interactions Using
Application of a Physiologically Based Pharmacokinetic Model to Predict OATP1B1-Related Variability in Pharmacodynamics of Rosuvastatin
 Original Article Citation: CPT Pharmacometrics Syst. Pharmacol. (), e; doi:./psp.. ASCPT All rights reserved -/ Application of a Physiologically Based Pharmacokinetic Model to Predict OATPB-Related Variability
Original Article Citation: CPT Pharmacometrics Syst. Pharmacol. (), e; doi:./psp.. ASCPT All rights reserved -/ Application of a Physiologically Based Pharmacokinetic Model to Predict OATPB-Related Variability
The Future of In Vitro Systems for the Assessment of Induction and Suppression of Enzymes and Transporters
 The Future of In Vitro Systems for the Assessment of Induction and Suppression of Enzymes and Transporters AAPS, San Diego November 6 th, 2014 Andrew Parkinson, XPD Consulting Lisa Almond, Simcyp-Certara
The Future of In Vitro Systems for the Assessment of Induction and Suppression of Enzymes and Transporters AAPS, San Diego November 6 th, 2014 Andrew Parkinson, XPD Consulting Lisa Almond, Simcyp-Certara
When does the rate-determining step in the hepatic clearance of a drug switch from
 When does the rate-determining step in the hepatic clearance of a drug switch from sinusoidal uptake to all hepatobiliary clearances? Implications for predicting drug-drug interactions Gabriela I. Patilea-Vrana
When does the rate-determining step in the hepatic clearance of a drug switch from sinusoidal uptake to all hepatobiliary clearances? Implications for predicting drug-drug interactions Gabriela I. Patilea-Vrana
Assessing the role of hepatic uptake in drug clearance - Pharmacokinetic and experimental considerations
 Assessing the role of hepatic uptake in drug clearance - Pharmacokinetic and experimental considerations Peter Webborn ISSX Short course Toronto 2013 1 Defining the why, when and how of Transporter studies
Assessing the role of hepatic uptake in drug clearance - Pharmacokinetic and experimental considerations Peter Webborn ISSX Short course Toronto 2013 1 Defining the why, when and how of Transporter studies
Drug disposition classification systems: A comparative review of BDDCS, ECCS and ECCCS
 Novartis Drug disposition classification systems: A comparative review of BDDCS, ECCS and ECCCS Birk Poller, Gian Camenisch - Novartis SOLVO - Meet The Experts Transporter Conference April 26, 2018 Drug
Novartis Drug disposition classification systems: A comparative review of BDDCS, ECCS and ECCCS Birk Poller, Gian Camenisch - Novartis SOLVO - Meet The Experts Transporter Conference April 26, 2018 Drug
MODELING MECHANISM BASED INACTIVATION USING PBPK JAN WAHLSTROM DIRECTOR, PRECLINICAL
 MODELING MECHANISM BASED INACTIVATION USING PBPK JAN WAHLSTROM DIRECTOR, PRECLINICAL ABSTRACT Quantitative prediction of the magnitude of drug-drug interactions (DDI) is critical to underwriting patient
MODELING MECHANISM BASED INACTIVATION USING PBPK JAN WAHLSTROM DIRECTOR, PRECLINICAL ABSTRACT Quantitative prediction of the magnitude of drug-drug interactions (DDI) is critical to underwriting patient
Comparison Between the US FDA, Japan PMDA and EMA In Vitro DDI Guidance: Are we Close to Harmonization?
 Comparison Between the US FDA, Japan PMDA and EMA In Vitro DDI Guidance: Are we Close to Harmonization? Brian Ogilvie, Ph.D. VP Scientific Consulting XenoTech, LLC bogilvie@xenotechllc.com 14 Jun, 2018
Comparison Between the US FDA, Japan PMDA and EMA In Vitro DDI Guidance: Are we Close to Harmonization? Brian Ogilvie, Ph.D. VP Scientific Consulting XenoTech, LLC bogilvie@xenotechllc.com 14 Jun, 2018
Building innovative drug discovery alliances. Hepatic uptake and drug disposition o in vitro and in silico approaches
 Building innovative drug discovery alliances Hepatic uptake and drug disposition o in vitro and in silico approaches Dr Beth Williamson Evotec AG, 2017 Outline Importance of predicting clearance In vitro
Building innovative drug discovery alliances Hepatic uptake and drug disposition o in vitro and in silico approaches Dr Beth Williamson Evotec AG, 2017 Outline Importance of predicting clearance In vitro
Strategy on Drug Transporter Investigation Why, How, Which & When. Jasminder Sahi
 Strategy on Drug Transporter Investigation Why, How, Which & When Jasminder Sahi Intestine Drug Absorption PEPT1 OATPs MCTs AE2 Epithelial Cell MCTs MRP3 Liver Excretion via Liver Kidney MRPs OATPs N PT1
Strategy on Drug Transporter Investigation Why, How, Which & When Jasminder Sahi Intestine Drug Absorption PEPT1 OATPs MCTs AE2 Epithelial Cell MCTs MRP3 Liver Excretion via Liver Kidney MRPs OATPs N PT1
The extended clearance model and its use for the interpretation of hepatobiliary elimination data
 ADMET & DMPK 3(1) (2015) 1-14; doi: 10.5599/admet.3.1.144 Open Access : ISSN : 1848-7718 Review http://www.pub.iapchem.org/ojs/index.php/admet/index The extended clearance model and its use for the interpretation
ADMET & DMPK 3(1) (2015) 1-14; doi: 10.5599/admet.3.1.144 Open Access : ISSN : 1848-7718 Review http://www.pub.iapchem.org/ojs/index.php/admet/index The extended clearance model and its use for the interpretation
Exploiting BDDCS and the Role of Transporters
 Exploiting BDDCS and the Role of Transporters (Therapeutic benefit of scientific knowledge of biological transporters, understanding the clinical relevant effects of active transport on oral drug absorption)
Exploiting BDDCS and the Role of Transporters (Therapeutic benefit of scientific knowledge of biological transporters, understanding the clinical relevant effects of active transport on oral drug absorption)
Pharmacokinetic Determinants of Statin-Induced Myopathy
 Pharmacokinetic Determinants of Statin-Induced Myopathy Rommel G. Tirona, B.Sc.Phm., Ph.D. Departments of Physiology & Pharmacology and Medicine The University of Western Ontario, London, Ontario, Canada
Pharmacokinetic Determinants of Statin-Induced Myopathy Rommel G. Tirona, B.Sc.Phm., Ph.D. Departments of Physiology & Pharmacology and Medicine The University of Western Ontario, London, Ontario, Canada
Under prediction of hepatic clearance from in vitro studies: prospects for resolution. J Brian Houston
 DDI, Seattle, June 2018 Under prediction of hepatic clearance from in vitro studies: prospects for resolution J Brian Houston Centre for Applied Pharmacokinetic Research (CAPkR) Scaling up in vitro parameters
DDI, Seattle, June 2018 Under prediction of hepatic clearance from in vitro studies: prospects for resolution J Brian Houston Centre for Applied Pharmacokinetic Research (CAPkR) Scaling up in vitro parameters
DRUG METABOLISM AND PHARMACOKINETICS (DMPK) Lena Gustavsson, H. Lundbeck A/S, November 2015
 DRUG METABOLISM AND PHARMACOKINETICS (DMPK), H. Lundbeck A/S, LEGU@lundbeck.com November 2015 DMPK in Drug Discovery and Development Agenda Introduction Optimizing pharmacokinetic properties Absorption
DRUG METABOLISM AND PHARMACOKINETICS (DMPK), H. Lundbeck A/S, LEGU@lundbeck.com November 2015 DMPK in Drug Discovery and Development Agenda Introduction Optimizing pharmacokinetic properties Absorption
T Eley, Y-H Han, S-P Huang, B He, W Li, W Bedford, M Stonier, D Gardiner, K Sims, P Balimane, D Rodrigues, RJ Bertz
 IN VIVO AND IN VITRO ASSESSMENT OF ASUNAPREVIR (ASV; BMS-650032) AS AN INHIBITOR AND SUBSTRATE OF ORGANIC ANION TRANSPORT POLYPEPTIDE (OATP) TRANSPORTERS IN HEALTHY VOLUNTEERS T Eley, Y-H Han, S-P Huang,
IN VIVO AND IN VITRO ASSESSMENT OF ASUNAPREVIR (ASV; BMS-650032) AS AN INHIBITOR AND SUBSTRATE OF ORGANIC ANION TRANSPORT POLYPEPTIDE (OATP) TRANSPORTERS IN HEALTHY VOLUNTEERS T Eley, Y-H Han, S-P Huang,
Itraconazole and Clarithromycin as Ketoconazole Alternatives for Clinical CYP3A Inhibition Studies to Quantify Victim DDI Potential
 Itraconazole and Clarithromycin as Ketoconazole Alternatives for Clinical CYP3A Inhibition Studies to Quantify Victim DDI Potential Alice Ban Ke, Ph.D. Consultant & Scientific Advisor Simcyp Limited Alice.Ke@certara.com
Itraconazole and Clarithromycin as Ketoconazole Alternatives for Clinical CYP3A Inhibition Studies to Quantify Victim DDI Potential Alice Ban Ke, Ph.D. Consultant & Scientific Advisor Simcyp Limited Alice.Ke@certara.com
Biopharmaceutics Drug Disposition Classification System (BDDCS) --- Its Impact and Application
 Biopharmaceutics Drug Disposition Classification System (BDDCS) --- Its Impact and Application Leslie Z. Benet, Ph.D. Professor of Bioengineering and Therapeutic Sciences Schools of Pharmacy and Medicine
Biopharmaceutics Drug Disposition Classification System (BDDCS) --- Its Impact and Application Leslie Z. Benet, Ph.D. Professor of Bioengineering and Therapeutic Sciences Schools of Pharmacy and Medicine
Evaluation of Drug-Drug Interactions FDA Perspective
 Evaluation of Drug-Drug Interactions FDA Perspective Kellie Schoolar Reynolds, Pharm.D. Deputy Director Division of Clinical Pharmacology IV Office of Clinical Pharmacology Office of Translational Sciences
Evaluation of Drug-Drug Interactions FDA Perspective Kellie Schoolar Reynolds, Pharm.D. Deputy Director Division of Clinical Pharmacology IV Office of Clinical Pharmacology Office of Translational Sciences
Drug Metabolism and Disposition
 Investigation of the Impact of Substrate Selection on In Vitro Organic Anion Transporting Polypeptide 1B1 Inhibition Profiles for the Prediction of Drug-drug Interactions Saki Izumi, Yoshitane Nozaki,
Investigation of the Impact of Substrate Selection on In Vitro Organic Anion Transporting Polypeptide 1B1 Inhibition Profiles for the Prediction of Drug-drug Interactions Saki Izumi, Yoshitane Nozaki,
Biopharmaceutics Drug Disposition Classification System (BDDCS) and Its Application in Drug Discovery and Development
 Biopharmaceutics Drug Disposition Classification System (BDDCS) and Its Application in Drug Discovery and Development Leslie Z. Benet, Ph.D. Professor of Bioengineering and Therapeutic Sciences University
Biopharmaceutics Drug Disposition Classification System (BDDCS) and Its Application in Drug Discovery and Development Leslie Z. Benet, Ph.D. Professor of Bioengineering and Therapeutic Sciences University
Mechanistic Modeling of Pitavastatin Disposition in Sandwich-Cultured Human Hepatocytes: A Proteomics-Informed Bottom-Up Approach s
 Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2016/02/03/dmd.115.066746.dc1 1521-009X/44/4/505 516$25.00 http://dx.doi.org/10.1124/dmd.115.066746 DRUG
Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2016/02/03/dmd.115.066746.dc1 1521-009X/44/4/505 516$25.00 http://dx.doi.org/10.1124/dmd.115.066746 DRUG
The Application of Physiologically Based Pharmacokinetic Modeling to Predict the Role of Drug Transporters: Scientific and Regulatory Perspectives
 Supplement Article The Application of Physiologically Based Pharmacokinetic Modeling to Predict the Role of Drug Transporters: Scientific and Regulatory Perspectives The Journal of Clinical Pharmacology
Supplement Article The Application of Physiologically Based Pharmacokinetic Modeling to Predict the Role of Drug Transporters: Scientific and Regulatory Perspectives The Journal of Clinical Pharmacology
Complexities of Hepatic Drug Transport: How Do We Sort It All Out?
 Complexities of Hepatic Drug Transport: How Do We Sort It All Out? Keith A. Hoffmaster Pfizer Research Technology Center Cambridge, MA NEDMDG 2005 Summer Symposium 06.08.2005 The Challenge Intestinal uptake
Complexities of Hepatic Drug Transport: How Do We Sort It All Out? Keith A. Hoffmaster Pfizer Research Technology Center Cambridge, MA NEDMDG 2005 Summer Symposium 06.08.2005 The Challenge Intestinal uptake
Kinetic characterization of rat hepatic uptake of 16 actively transported drugs. Yoshiyuki Yabe, Aleksandra Galetin and J Brian Houston
 DMD Fast Forward. Published on July 5, 2011 as doi:10.1124/dmd.111.040477 Kinetic characterization of rat hepatic uptake of 16 actively transported drugs Yoshiyuki Yabe, Aleksandra Galetin and J Brian
DMD Fast Forward. Published on July 5, 2011 as doi:10.1124/dmd.111.040477 Kinetic characterization of rat hepatic uptake of 16 actively transported drugs Yoshiyuki Yabe, Aleksandra Galetin and J Brian
In vitro substrate-dependent inhibition of OATP1B1 and its impact on DDI prediction
 SSX 3 rd Annual Conference (Oct 11, 2018) In vitro substrate-dependent inhibition of OATP1B1 and its impact on DDI prediction Yoshitane Nozaki, PhD DMPK Tsukuba Organic Anion Transporting Polypeptide (OATP)
SSX 3 rd Annual Conference (Oct 11, 2018) In vitro substrate-dependent inhibition of OATP1B1 and its impact on DDI prediction Yoshitane Nozaki, PhD DMPK Tsukuba Organic Anion Transporting Polypeptide (OATP)
Clinical Implications of Pharmacogenetic Variation on the Effects of Statins
 REVIEW ARTICLE Drug Saf 2011; 34 (1): 1-19 0114-5916/11/0001-0001/$49.95/0 ª 2011 Adis Data Information BV. All rights reserved. Clinical Implications of Pharmacogenetic Variation on the Effects of Statins
REVIEW ARTICLE Drug Saf 2011; 34 (1): 1-19 0114-5916/11/0001-0001/$49.95/0 ª 2011 Adis Data Information BV. All rights reserved. Clinical Implications of Pharmacogenetic Variation on the Effects of Statins
EVALUATION OF DRUG-DRUG INTERACTION POTENTIAL BETWEEN SACUBITRIL/VALSARTAN (LCZ696) AND STATINS USING A PHYSIOLOGICALLY- BASED PHARMACOKINETIC MODEL
 Drug metabolism and Pharmacokinetics/PK Sciences EVALUATIN F DRUG-DRUG INTERACTIN PTENTIAL BETWEEN SACUBITRIL/VALSARTAN (LCZ696) AND STATINS USING A PHYSILGICALLY- BASED PHARMACKINETIC MDEL Imad Hanna,
Drug metabolism and Pharmacokinetics/PK Sciences EVALUATIN F DRUG-DRUG INTERACTIN PTENTIAL BETWEEN SACUBITRIL/VALSARTAN (LCZ696) AND STATINS USING A PHYSILGICALLY- BASED PHARMACKINETIC MDEL Imad Hanna,
Transporters DDI-2018
 Transporters DDI-2018 Mark S. Warren, Ph.D. June 16, 2018 Senior Director of Assay Services DDI-2018: 21 st Conference on DDIs FDA guidance documents: A 21 year history 1997 2006 2012 2017 Each year, large
Transporters DDI-2018 Mark S. Warren, Ph.D. June 16, 2018 Senior Director of Assay Services DDI-2018: 21 st Conference on DDIs FDA guidance documents: A 21 year history 1997 2006 2012 2017 Each year, large
DMPK. APRIL 27 TH 2017 Jan Neelissen Scientific Adviser Science & Technology
 DMPK APRIL 27 TH 2017 Jan Neelissen Scientific Adviser Science & Technology What I learned is a good DMPK profile have acceptable water solubility for development be completely absorbed, preferably via
DMPK APRIL 27 TH 2017 Jan Neelissen Scientific Adviser Science & Technology What I learned is a good DMPK profile have acceptable water solubility for development be completely absorbed, preferably via
Pharmacokinetic Modeling & Simulation in Discovery and non-clinical Development
 Pharmacokinetic Modeling & Simulation in Discovery and non-clinical Development Where do we stand? Disclaimer I am not a bioinformatician, mathematician or biomedical engineer. I am a simple minded pharmacist,
Pharmacokinetic Modeling & Simulation in Discovery and non-clinical Development Where do we stand? Disclaimer I am not a bioinformatician, mathematician or biomedical engineer. I am a simple minded pharmacist,
RISK FACTORS AND DRUG TO STATIN-INDUCED MYOPATHY
 RISK FACTORS AND DRUG INTERACTION PREDISPOSING TO STATIN-INDUCED MYOPATHY Assist. Prof. Dr. Verawan Uchaipichat Clinical Pharmacy Department Khon Kaen University Advanced Pharmacotherapy 2012 Updated d
RISK FACTORS AND DRUG INTERACTION PREDISPOSING TO STATIN-INDUCED MYOPATHY Assist. Prof. Dr. Verawan Uchaipichat Clinical Pharmacy Department Khon Kaen University Advanced Pharmacotherapy 2012 Updated d
Welcome to the webinar... We will begin shortly
 Welcome to the webinar... We will begin shortly Evaluation of Ketoconazole and Its Alternative Clinical CYP3A4/5 Inhibitors as Inhibitors of Drug Transporters: The In Vitro Effects of Ketoconazole, Ritonavir,
Welcome to the webinar... We will begin shortly Evaluation of Ketoconazole and Its Alternative Clinical CYP3A4/5 Inhibitors as Inhibitors of Drug Transporters: The In Vitro Effects of Ketoconazole, Ritonavir,
FDA s Clinical Drug Interaction Studies Guidance (2017 Draft Guidance)
 FDA s Clinical Drug Interaction Studies Guidance (2017 Draft Guidance) Kellie S. Reynolds, Pharm.D. Deputy Director, Division of Clinical Pharmacology IV Office of Clinical Pharmacology (OCP) Office of
FDA s Clinical Drug Interaction Studies Guidance (2017 Draft Guidance) Kellie S. Reynolds, Pharm.D. Deputy Director, Division of Clinical Pharmacology IV Office of Clinical Pharmacology (OCP) Office of
Current Approaches and Applications of Phenotyping Methods for Drug Metabolizing Enzymes and Transporters
 Current Approaches and Applications of Phenotyping Methods for Drug Metabolizing Enzymes and Transporters Uwe Fuhr, University Hospital Cologne 1 Definition Phenotyping is quantifying the in vivo activity
Current Approaches and Applications of Phenotyping Methods for Drug Metabolizing Enzymes and Transporters Uwe Fuhr, University Hospital Cologne 1 Definition Phenotyping is quantifying the in vivo activity
Different Effects of SLCO1B1 Polymorphism on the Pharmacokinetics of Atorvastatin and Rosuvastatin
 nature publishing group Different Effects of SLCO1B1 Polymorphism on the Pharmacokinetics of Atorvastatin and Rosuvastatin MK Pasanen 1, H Fredrikson 1, PJ Neuvonen 1 and M Niemi 1 Thirty-two healthy volunteers
nature publishing group Different Effects of SLCO1B1 Polymorphism on the Pharmacokinetics of Atorvastatin and Rosuvastatin MK Pasanen 1, H Fredrikson 1, PJ Neuvonen 1 and M Niemi 1 Thirty-two healthy volunteers
Pursuing the holy grail of predicting and verifying tissue drug concentrations: A proteomics and PET imaging approach
 Pursuing the holy grail of predicting and verifying tissue drug concentrations: A proteomics and PET imaging approach Jashvant (Jash) Unadkat Milo Gibaldi Endowed Professor Dept. of Pharmaceutics School
Pursuing the holy grail of predicting and verifying tissue drug concentrations: A proteomics and PET imaging approach Jashvant (Jash) Unadkat Milo Gibaldi Endowed Professor Dept. of Pharmaceutics School
Prediction of in vivo hepatic clearance and DDI of OATP substrates: Comparison of different in vitro approaches. Yuichi Sugiyama
 Prediction of in vivo hepatic clearance and DDI of OATP substrates: Comparison of different in vitro approaches. Yuichi Sugiyama Sugiyama Laboratory, RIKEN Innovation Center, RIKEN, Research Cluster for
Prediction of in vivo hepatic clearance and DDI of OATP substrates: Comparison of different in vitro approaches. Yuichi Sugiyama Sugiyama Laboratory, RIKEN Innovation Center, RIKEN, Research Cluster for
SLCO1B1 Pharmacogenetic Competency
 SLCO1B1 Pharmacogenetic Competency Updated on 6/2015 Pre-test Question # 1 Which of the following is not currently a recognized SLCO1B1 phenotype? a) Low function b) Normal function c) Intermediate function
SLCO1B1 Pharmacogenetic Competency Updated on 6/2015 Pre-test Question # 1 Which of the following is not currently a recognized SLCO1B1 phenotype? a) Low function b) Normal function c) Intermediate function
Transporter-mediated disposition, clinical pharmacokinetics and cholestatic potential of glyburide and its primary active metabolites
 Transporter-mediated disposition, clinical pharmacokinetics and cholestatic potential of glyburide and its primary active metabolites Rui Li, Yi-an Bi, Anna Vildhede, Renato J. Scialis, Sumathy Mathialagan,
Transporter-mediated disposition, clinical pharmacokinetics and cholestatic potential of glyburide and its primary active metabolites Rui Li, Yi-an Bi, Anna Vildhede, Renato J. Scialis, Sumathy Mathialagan,
RSC, February Interplay between enzymes and. clearance and intracellular concentration of drugs. Centre for Applied Pharmacokinetic Research
 RSC, February 2014 Interplay between enzymes and transporters in defining hepatic drug clearance and intracellular concentration of drugs J Brian Houston Centre for Applied Pharmacokinetic Research (CAPkR)
RSC, February 2014 Interplay between enzymes and transporters in defining hepatic drug clearance and intracellular concentration of drugs J Brian Houston Centre for Applied Pharmacokinetic Research (CAPkR)
Withdrawal of Cerivastatin Revealed a Flaw of Post-marketing Surveillance System in the United States
 Bull. Natl. Inst. Health Sci., 123 Notes # Withdrawal of Cerivastatin Revealed a Flaw of Post-marketing Surveillance System in the United States Journal of American Medical Association (JAMA) Statin HMG
Bull. Natl. Inst. Health Sci., 123 Notes # Withdrawal of Cerivastatin Revealed a Flaw of Post-marketing Surveillance System in the United States Journal of American Medical Association (JAMA) Statin HMG
Viera Lukacova Director, Simulation Sciences
 Use of In Silico Mechanistic Models to Support Interspecies Extrapolation of Oral Bioavailability and Formulation Optimization: Model Example Using GastroPlus Viera Lukacova Director, Simulation Sciences
Use of In Silico Mechanistic Models to Support Interspecies Extrapolation of Oral Bioavailability and Formulation Optimization: Model Example Using GastroPlus Viera Lukacova Director, Simulation Sciences
1 Introduction: The Why and How of Drug Bioavailability Research
 j1 1 Introduction: The Why and How of Drug Bioavailability Research Han van de Waterbeemd and Bernard Testa Abbreviations ADME EMEA FDA NCE PD P-gp PK R&D Absorption, distribution, metabolism, and excretion
j1 1 Introduction: The Why and How of Drug Bioavailability Research Han van de Waterbeemd and Bernard Testa Abbreviations ADME EMEA FDA NCE PD P-gp PK R&D Absorption, distribution, metabolism, and excretion
Pharmacogenetics and Pharmacokinetics
 Chapter 2 Pharmacogenetics and Pharmacokinetics Mauro Saivezzo/ShutterStock, Inc. L earning O bjectives Upon completion of this chapter, the student will be able to: 1. Recognize the influence of genetic
Chapter 2 Pharmacogenetics and Pharmacokinetics Mauro Saivezzo/ShutterStock, Inc. L earning O bjectives Upon completion of this chapter, the student will be able to: 1. Recognize the influence of genetic
DRUG-DRUG INTERACTIONS OF GLECAPREVIR AND PIBRENTASVIR WITH PRAVASTATIN, ROSUVASTATIN, OR DABIGATRAN ETEXILATE
 DRUG-DRUG INTERACTIONS OF GLECAPREVIR AND PIBRENTASVIR WITH PRAVASTATIN, ROSUVASTATIN, OR DABIGATRAN ETEXILATE Matthew P. Kosloski, Weihan Zhao, Hong Li, Stanley Subhead Wang, Calibri Joaquin 14pt, Valdes,
DRUG-DRUG INTERACTIONS OF GLECAPREVIR AND PIBRENTASVIR WITH PRAVASTATIN, ROSUVASTATIN, OR DABIGATRAN ETEXILATE Matthew P. Kosloski, Weihan Zhao, Hong Li, Stanley Subhead Wang, Calibri Joaquin 14pt, Valdes,
Strategies for Developing and Validating PBPK Models for Extrapolation to Unstudied Population
 Strategies for Developing and Validating PBPK Models for Extrapolation to Unstudied Population Nina Isoherranen Department of Pharmaceutics University of Washington Processes driving drug disposition are
Strategies for Developing and Validating PBPK Models for Extrapolation to Unstudied Population Nina Isoherranen Department of Pharmaceutics University of Washington Processes driving drug disposition are
polymorphism on repaglinide pharmacokinetics persists over a wide dose range
 British Journal of Clinical Pharmacology DOI:./j.365-5.8.387.x The effect of SLCOB polymorphism on repaglinide pharmacokinetics persists over a wide dose range Annikka Kalliokoski, Mikko Neuvonen, Pertti
British Journal of Clinical Pharmacology DOI:./j.365-5.8.387.x The effect of SLCOB polymorphism on repaglinide pharmacokinetics persists over a wide dose range Annikka Kalliokoski, Mikko Neuvonen, Pertti
Evaluation of Proposed In Vivo Probe Substrates and Inhibitors for Phenotyping Transporter Activity in Humans
 Supplement Article Evaluation of Proposed In Vivo Probe Substrates and Inhibitors for Phenotyping Transporter Activity in Humans The Journal of Clinical Pharmacology (2016), 56(S7) S82 S98 C 2016, The
Supplement Article Evaluation of Proposed In Vivo Probe Substrates and Inhibitors for Phenotyping Transporter Activity in Humans The Journal of Clinical Pharmacology (2016), 56(S7) S82 S98 C 2016, The
Prediction of THC Plasma and Brain Concentrations following. Marijuana Administration: Approach and Challenges
 Prediction of THC Plasma and Brain Concentrations following Marijuana Administration: Approach and Challenges Contents: 1. Background and Significance 1.1. Introduction 1.2. THC - the primary chemical
Prediction of THC Plasma and Brain Concentrations following Marijuana Administration: Approach and Challenges Contents: 1. Background and Significance 1.1. Introduction 1.2. THC - the primary chemical
Leslie Z. Benet, PhD. Professor of Bioengineering and Therapeutic Sciences Schools of Pharmacy and Medicine University of California San Francisco
 Biopharmaceutics Drug Disposition Classification System (BDDCS) and Drug Interactions Leslie Z. Benet, PhD Professor of Bioengineering and Therapeutic Sciences Schools of Pharmacy and Medicine University
Biopharmaceutics Drug Disposition Classification System (BDDCS) and Drug Interactions Leslie Z. Benet, PhD Professor of Bioengineering and Therapeutic Sciences Schools of Pharmacy and Medicine University
Predicting Human Clearance of OATP substrates using Cynomolgus monkey: In vitroin
 Title Page Predicting Human Clearance of OATP substrates using Cynomolgus monkey: In vitroin vivo scaling of hepatic uptake clearance Tom De Bruyn, Ayşe Ufuk, Carina Cantrill, Rachel E Kosa, Yi-an Bi,
Title Page Predicting Human Clearance of OATP substrates using Cynomolgus monkey: In vitroin vivo scaling of hepatic uptake clearance Tom De Bruyn, Ayşe Ufuk, Carina Cantrill, Rachel E Kosa, Yi-an Bi,
Caveat: Validation and Limitations of Phenotyping Methods for Drug Metabolizing Enzymes and Transporters
 Caveat: Validation and Limitations of Phenotyping Methods for Drug Metabolizing Enzymes and Transporters Uwe Fuhr, University Hospital Cologne 1 How to Safeguard that Metrics Reflect E/T Activity? in healthy
Caveat: Validation and Limitations of Phenotyping Methods for Drug Metabolizing Enzymes and Transporters Uwe Fuhr, University Hospital Cologne 1 How to Safeguard that Metrics Reflect E/T Activity? in healthy
PBPK Modeling of Coproporphyrin I as an Endogenous Biomarker for Drug Interactions Involving Inhibition of Hepatic OATP1B1 and OATP1B3
 Citation: CPT Pharmacometrics Syst. Pharmacol. (208) XX, 9; doi:0.002/psp4.2348 ARTICLE PBPK Modeling of Coproporphyrin I as an Endogenous Biomarker for Drug Interactions Involving Inhibition of Hepatic
Citation: CPT Pharmacometrics Syst. Pharmacol. (208) XX, 9; doi:0.002/psp4.2348 ARTICLE PBPK Modeling of Coproporphyrin I as an Endogenous Biomarker for Drug Interactions Involving Inhibition of Hepatic
Univ.-Doz. Prof. Dr. W. Renner
 Pharmacogenetics of statin-inducedinduced myopathies Wilfried Renner Medical University Graz Clinical Institute of Medical and Chemical Laboratory Diagnostics It started with a fungus 1973: Isolation of
Pharmacogenetics of statin-inducedinduced myopathies Wilfried Renner Medical University Graz Clinical Institute of Medical and Chemical Laboratory Diagnostics It started with a fungus 1973: Isolation of
Evaluation and Quantitative Prediction of Renal Transporter-Mediated Drug-Drug Interactions. Bo Feng, Ph.D. DDI 2017 June 19-21, 2017
 Evaluation and Quantitative Prediction of Renal Transporter-Mediated Drug-Drug Interactions Bo Feng, Ph.D. DDI 2017 June 19-21, 2017 Outline Background of renal transporters. Clinically observed transporter-mediated
Evaluation and Quantitative Prediction of Renal Transporter-Mediated Drug-Drug Interactions Bo Feng, Ph.D. DDI 2017 June 19-21, 2017 Outline Background of renal transporters. Clinically observed transporter-mediated
Variability Due to Genetic Differences
 1 Variability Due to Genetic Differences Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland 2 Objectives Understand how between individual variation may contribute to :» drug
1 Variability Due to Genetic Differences Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland 2 Objectives Understand how between individual variation may contribute to :» drug
PBPK modeling of renal impairment what is missing?
 PBPK modeling of renal impairment what is missing? Aleksandra Galetin Centre for Applied Pharmacokinetic Research, University of Manchester, UK Outline of the presentation Physiological changes in renal
PBPK modeling of renal impairment what is missing? Aleksandra Galetin Centre for Applied Pharmacokinetic Research, University of Manchester, UK Outline of the presentation Physiological changes in renal
In vitro and in silico Predictions of Hepatic Transporter-Mediated Drug Clearance and Drug-Drug Interactions in vivo
 Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Pharmacy 193 In vitro and in silico Predictions of Hepatic Transporter-Mediated Drug Clearance and Drug-Drug Interactions in
Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Pharmacy 193 In vitro and in silico Predictions of Hepatic Transporter-Mediated Drug Clearance and Drug-Drug Interactions in
A study on pharmacokinetics of bosentan with systems modeling, Part 1: translating systemic plasma concentration to liver exposure in healthy subjects
 A study on pharmacokinetics of bosentan with systems modeling, Part 1: translating systemic plasma concentration to liver exposure in healthy subjects Rui Li, Mark Niosi, Nathaniel Johnson, David A. Tess,
A study on pharmacokinetics of bosentan with systems modeling, Part 1: translating systemic plasma concentration to liver exposure in healthy subjects Rui Li, Mark Niosi, Nathaniel Johnson, David A. Tess,
Current and Emerging Transporter Regulatory Themes in Drug Development: Relevance to Understanding PK/PD, DDIs, and Toxicity
 Current and Emerging Transporter Regulatory Themes in Drug Development: Relevance to Understanding PK/PD, DDIs, and Toxicity Maciej Zamek-Gliszczynski, Ph.D. 1940 s Probenecid & anion secretion 1950 s
Current and Emerging Transporter Regulatory Themes in Drug Development: Relevance to Understanding PK/PD, DDIs, and Toxicity Maciej Zamek-Gliszczynski, Ph.D. 1940 s Probenecid & anion secretion 1950 s
WHY... 8/21/2013 LEARNING OUTCOMES PHARMACOKINETICS I. A Absorption. D Distribution DEFINITION ADME AND THERAPEUIC ACTION
 PHARMACOKINETICS I Absorption & Distribution LEARNING OUTCOMES By the end of the lecture students will be able to.. Dr Ruwan Parakramawansha MBBS, MD, MRCP(UK),MRCPE, DMT(UK) (2013/08/21) Define pharmacokinetics,
PHARMACOKINETICS I Absorption & Distribution LEARNING OUTCOMES By the end of the lecture students will be able to.. Dr Ruwan Parakramawansha MBBS, MD, MRCP(UK),MRCPE, DMT(UK) (2013/08/21) Define pharmacokinetics,
Genetics and Genomics: Influence on Individualization of Medication Regimes
 Genetics and Genomics: Influence on Individualization of Medication Regimes Joseph S Bertino Jr., Pharm.D., FCCP Schenectady, NY USA Goals and Objectives To discuss pharmacogenetics and pharmacogenomics
Genetics and Genomics: Influence on Individualization of Medication Regimes Joseph S Bertino Jr., Pharm.D., FCCP Schenectady, NY USA Goals and Objectives To discuss pharmacogenetics and pharmacogenomics
Effects of Uptake and Efflux Transporter Inhibition on Erythromycin Breath Test Results
 nature publishing group Effects of Uptake and Efflux Transporter Inhibition on Erythromycin Breath Test Results LA Frassetto 1, S Poon 2, C Tsourounis 2, C Valera 2 and LZ Benet 3 The erythromycin breath
nature publishing group Effects of Uptake and Efflux Transporter Inhibition on Erythromycin Breath Test Results LA Frassetto 1, S Poon 2, C Tsourounis 2, C Valera 2 and LZ Benet 3 The erythromycin breath
The importance of pharmacogenetics in the treatment of epilepsy
 The importance of pharmacogenetics in the treatment of epilepsy Öner Süzer and Esat Eşkazan İstanbul University, Cerrahpaşa Faculty of Medicine, Department of Pharmacology and Clinical Pharmacology Introduction
The importance of pharmacogenetics in the treatment of epilepsy Öner Süzer and Esat Eşkazan İstanbul University, Cerrahpaşa Faculty of Medicine, Department of Pharmacology and Clinical Pharmacology Introduction
Mechanistic Pharmacokinetic Modeling for the Prediction of Transporter-Mediated Disposition in Humans from Sandwich Culture Human Hepatocyte Data S
 Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl////dmd..99.dc -9X//-7 7$. DRUG METABOLISM AND DISPOSITION Vol., No. Copyright by The American Society for
Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl////dmd..99.dc -9X//-7 7$. DRUG METABOLISM AND DISPOSITION Vol., No. Copyright by The American Society for
Drug-Disease Modeling Applied to Drug Development and Regulatory Decision Making in the Type 2 Diabetes Mellitus Arena
 Drug-Disease Modeling Applied to Drug Development and Regulatory Decision Making in the Type 2 Diabetes Mellitus Arena Tokyo, Japan, December 8, 2015 Stephan Schmidt, Ph.D. Assistant Professor Center for
Drug-Disease Modeling Applied to Drug Development and Regulatory Decision Making in the Type 2 Diabetes Mellitus Arena Tokyo, Japan, December 8, 2015 Stephan Schmidt, Ph.D. Assistant Professor Center for
Supporting information
 Supporting information Intracellular drug bioavailability: a new predictor of system dependent drug disposition Mateus, André 1* ; Treyer, Andrea 1* ; Wegler, Christine 1,2 ; Karlgren, Maria 1 ; Matsson,
Supporting information Intracellular drug bioavailability: a new predictor of system dependent drug disposition Mateus, André 1* ; Treyer, Andrea 1* ; Wegler, Christine 1,2 ; Karlgren, Maria 1 ; Matsson,
Section 5.2: Pharmacokinetic properties
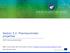 Section 5.2: Pharmacokinetic properties SmPC training presentation Note: for full information refer to the European Commission s Guideline on summary of product characteristics (SmPC) SmPC Advisory Group
Section 5.2: Pharmacokinetic properties SmPC training presentation Note: for full information refer to the European Commission s Guideline on summary of product characteristics (SmPC) SmPC Advisory Group
Clinical Pharmacology of DAA s for HCV: What s New and What s in the Pipeline
 Clinical Pharmacology of DAA s for HCV: What s New and What s in the Pipeline Anita Mathias, PhD Clinical Pharmacology, Gilead Sciences 14 th Int. Workshop on Clinical Pharmacology of HIV Therapy April
Clinical Pharmacology of DAA s for HCV: What s New and What s in the Pipeline Anita Mathias, PhD Clinical Pharmacology, Gilead Sciences 14 th Int. Workshop on Clinical Pharmacology of HIV Therapy April
Simultaneous Assessment of Uptake and Metabolism in Rat Hepatocytes: A. Comprehensive Mechanistic Model
 JPET Fast This Forward. article has not Published been copyedited on and December formatted. The 21, final 2011 version as may DOI:10.1124/jpet.111.187112 differ from this version. Simultaneous Assessment
JPET Fast This Forward. article has not Published been copyedited on and December formatted. The 21, final 2011 version as may DOI:10.1124/jpet.111.187112 differ from this version. Simultaneous Assessment
Culture Hepatocytes in Human Plasma to Count the free Concentration of Drug in Evaluation of Drug-drug Interaction. Chuang Lu
 Culture Hepatocytes in Human Plasma to Count the free Concentration of Drug in Evaluation of Drug-drug nteraction Chuang Lu Millennium, The Takeda Oncology Company Cambridge, MA, USA DD 205, Seattle, 6/29/205
Culture Hepatocytes in Human Plasma to Count the free Concentration of Drug in Evaluation of Drug-drug nteraction Chuang Lu Millennium, The Takeda Oncology Company Cambridge, MA, USA DD 205, Seattle, 6/29/205
Pharmacologic Considerations when using DAAs in Cirrhosis
 Pharmacologic Considerations when using DAAs in Cirrhosis Jennifer J. Kiser, PharmD Assistant Professor University of Colorado Denver 1 st International Workshop on the Optimal Use of DAAs in Liver Transplant
Pharmacologic Considerations when using DAAs in Cirrhosis Jennifer J. Kiser, PharmD Assistant Professor University of Colorado Denver 1 st International Workshop on the Optimal Use of DAAs in Liver Transplant
Cryo Characterization Report (CCR)
 Human Cryopreserved Hepatocytes Lot number: HUM4061B Date: October 19, 2014 Cryo Characterization Report (CCR) Lot Overview Qualification Catalog Number Quantity Cryopreserved human hepatocytes, Qualyst
Human Cryopreserved Hepatocytes Lot number: HUM4061B Date: October 19, 2014 Cryo Characterization Report (CCR) Lot Overview Qualification Catalog Number Quantity Cryopreserved human hepatocytes, Qualyst
Investigation of the Rate-Determining Process in the Hepatic Elimination of HMG-CoA Reductase Inhibitors in Rats and Humans
 9-9556//382-25 222$2. DRUG METABOLISM AND DISPOSITION Vol. 38, No. 2 Copyright 2 by The American Society for Pharmacology and Experimental Therapeutics 3254/3548264 DMD 38:25 222, 2 Printed in U.S.A. Investigation
9-9556//382-25 222$2. DRUG METABOLISM AND DISPOSITION Vol. 38, No. 2 Copyright 2 by The American Society for Pharmacology and Experimental Therapeutics 3254/3548264 DMD 38:25 222, 2 Printed in U.S.A. Investigation
Montpellier and Nimes University Hospital. 2nd International Workshop on Clinical Pharmacology of Anticancer Drugs Madrid, September the 13th and 14th
 Association of NR1I2, CYP3A5 and ABCB1 genetic polymorphisms with variability of temsirolimus pharmacokinetics and toxicity in patients with metastatic bladder cancer Litaty MBATCHI, Matthieu GASSIOT,
Association of NR1I2, CYP3A5 and ABCB1 genetic polymorphisms with variability of temsirolimus pharmacokinetics and toxicity in patients with metastatic bladder cancer Litaty MBATCHI, Matthieu GASSIOT,
Mycophénolate mofétil
 Mycophénolate mofétil O OH CH 3 O O-desmethyl O glucosides OH CH 3 OCH 3 CH 3 CYP 3A UGT2B7 C O HO O HO AcMPAG (acyl-glucuronide) ACTIF TOXIQUE O O CH 3 OCH 3 Mycophenolate (MPA) OH COOH UGT enzymes COOH
Mycophénolate mofétil O OH CH 3 O O-desmethyl O glucosides OH CH 3 OCH 3 CH 3 CYP 3A UGT2B7 C O HO O HO AcMPAG (acyl-glucuronide) ACTIF TOXIQUE O O CH 3 OCH 3 Mycophenolate (MPA) OH COOH UGT enzymes COOH
Pharmacogenomics and Pharmacokinetics ^
 Pharmacogenomics and Pharmacokinetics ^ avid F. Kisor, B.S., Pharm.. Profeor of Pharmacokinetics epartment of Pharmaceutical and Biomedical Sciences Raabe College of Pharmacy Ohio Northern University Learning
Pharmacogenomics and Pharmacokinetics ^ avid F. Kisor, B.S., Pharm.. Profeor of Pharmacokinetics epartment of Pharmaceutical and Biomedical Sciences Raabe College of Pharmacy Ohio Northern University Learning
Classification of Inhibitors of Hepatic Organic Anion Transporting Polypeptides (OATPs): Influence of Protein Expression on Drug Drug Interactions
 pubs.acs.org/jmc Classification of Inhibitors of Hepatic Organic Anion Transporting Polypeptides (OATPs): Influence of Protein Expression on Drug Drug Interactions Maria Karlgren,*,, Anna Vildhede, Ulf
pubs.acs.org/jmc Classification of Inhibitors of Hepatic Organic Anion Transporting Polypeptides (OATPs): Influence of Protein Expression on Drug Drug Interactions Maria Karlgren,*,, Anna Vildhede, Ulf
Application of Physiologically Based Pharmacokinetic Modeling in. Understanding Bosutinib Drug-Drug Interactions: Importance of Intestinal
 TITLE: Application of Physiologically Based Pharmacokinetic Modeling in Understanding Bosutinib Drug-Drug Interactions: Importance of Intestinal P-Glycoprotein AUTHORS: Shinji Yamazaki, Cho-Ming Loi, Emi
TITLE: Application of Physiologically Based Pharmacokinetic Modeling in Understanding Bosutinib Drug-Drug Interactions: Importance of Intestinal P-Glycoprotein AUTHORS: Shinji Yamazaki, Cho-Ming Loi, Emi
Kinetic Characterization of Rat Hepatic Uptake of 16 Actively Transported Drugs
 9-9556//39-88 84$25. DRUG METOLISM ND DISPOSITION Vol. 39, No. Copyright 2 by The merican Society for Pharmacology and Experimental Therapeutics 4477/37552 DMD 39:88 84, 2 Printed in U.S.. Kinetic Characterization
9-9556//39-88 84$25. DRUG METOLISM ND DISPOSITION Vol. 39, No. Copyright 2 by The merican Society for Pharmacology and Experimental Therapeutics 4477/37552 DMD 39:88 84, 2 Printed in U.S.. Kinetic Characterization
Causes and Consequences of Variability in Drug Transporter Activity in Pediatric Drug Therapy
 Supplement Article Causes and Consequences of Variability in Drug Transporter Activity in Pediatric Drug Therapy The Journal of Clinical Pharmacology (2016), 56(S7) S173 S192 C 2016, The American College
Supplement Article Causes and Consequences of Variability in Drug Transporter Activity in Pediatric Drug Therapy The Journal of Clinical Pharmacology (2016), 56(S7) S173 S192 C 2016, The American College
Importance of Multi-P450 Inhibition in Drug Drug Interactions: Evaluation of Incidence, Inhibition Magnitude, and Prediction from in Vitro Data
 pubs.acs.org/crt Importance of Multi-P450 Inhibition in Drug Drug Interactions: Evaluation of Incidence, Inhibition Magnitude, and Prediction from in Vitro Data Nina Isoherranen,* Justin D. Lutz, Sophie
pubs.acs.org/crt Importance of Multi-P450 Inhibition in Drug Drug Interactions: Evaluation of Incidence, Inhibition Magnitude, and Prediction from in Vitro Data Nina Isoherranen,* Justin D. Lutz, Sophie
A unified in vivomodelingapproach for quantitative prediction of the impact of gene polymorphism and drug interactions on drug exposure
 A unified in vivomodelingapproach for quantitative prediction of the impact of gene polymorphism and drug interactions on drug exposure Sylvain Goutelle, Michel Tod, Laurent Bourguignon, Nathalie Bleyzac,
A unified in vivomodelingapproach for quantitative prediction of the impact of gene polymorphism and drug interactions on drug exposure Sylvain Goutelle, Michel Tod, Laurent Bourguignon, Nathalie Bleyzac,
Simultaneous Assessment of Uptake and Metabolism in Rat Hepatocytes: A Comprehensive Mechanistic Model S
 Supplemental material to this article can be found at: http://jpet.aspetjournals.org/content/suppl/2/2/2/jpet..872.dc 52-3/2/34-2 5$25. THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 34,
Supplemental material to this article can be found at: http://jpet.aspetjournals.org/content/suppl/2/2/2/jpet..872.dc 52-3/2/34-2 5$25. THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 34,
Prediction of the Effects of Renal Impairment on the Clearance for Organic Cation Drugs that. undergo Renal Secretion: A Simulation-Based Study
 DMD Fast Forward. Published on February 28, 2018 as DOI: 10.1124/dmd.117.079558 This article has not been copyedited and formatted. The final version may differ from this version. Prediction of the Effects
DMD Fast Forward. Published on February 28, 2018 as DOI: 10.1124/dmd.117.079558 This article has not been copyedited and formatted. The final version may differ from this version. Prediction of the Effects
Proteomic Quantification of Kidney Transporters: Methodological Challenges, Interindividual Variability and Application in IVIVE
 Proteomic Quantification of Kidney Transporters: Methodological Challenges, Interindividual Variability and Application in IVIVE Bhagwat Prasad, Ph.D. University of Washington, Seattle, WA (bhagwat@uw.edu)
Proteomic Quantification of Kidney Transporters: Methodological Challenges, Interindividual Variability and Application in IVIVE Bhagwat Prasad, Ph.D. University of Washington, Seattle, WA (bhagwat@uw.edu)
Endogenous Biomarkers for OATP1B: Preclinical to Clinical Translations. Yurong Lai, PhD Drug Metabolism Gilead Sciences
 Endogenous Biomarkers for OATP1B: Preclinical to Clinical Translations Yurong Lai, PhD Drug Metabolism Gilead Sciences Outlines Current strategies to assess clinical DDIs for OATP inhibitor Endogenous
Endogenous Biomarkers for OATP1B: Preclinical to Clinical Translations Yurong Lai, PhD Drug Metabolism Gilead Sciences Outlines Current strategies to assess clinical DDIs for OATP inhibitor Endogenous
Saliva Versus Plasma Bioequivalence of Rusovastatin in Humans: Validation of Class III Drugs of the Salivary Excretion Classification System
 Drugs R D (2015) 15:79 83 DOI 10.1007/s40268-015-0080-1 ORIGINAL RESEARCH ARTICLE Saliva Versus Plasma Bioequivalence of Rusovastatin in Humans: Validation of Class III Drugs of the Salivary Excretion
Drugs R D (2015) 15:79 83 DOI 10.1007/s40268-015-0080-1 ORIGINAL RESEARCH ARTICLE Saliva Versus Plasma Bioequivalence of Rusovastatin in Humans: Validation of Class III Drugs of the Salivary Excretion
Physiologically Based Pharmacokinetic Model of the CYP2D6 Probe Atomoxetine: Extrapolation to Special Populations and Drug-Drug Interactions s
 Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2017/08/31/dmd.117.076455.dc1 1521-009X/45/11/1156 1165$25.00 https://doi.org/10.1124/dmd.117.076455 DRUG
Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2017/08/31/dmd.117.076455.dc1 1521-009X/45/11/1156 1165$25.00 https://doi.org/10.1124/dmd.117.076455 DRUG
Evaluation of alteration in hepatic and intestinal BCRP function in. vivo due to ABCG2 c.421c>a polymorphism based on PBPK analysis.
 Evaluation of alteration in hepatic and intestinal BCRP function in vivo due to ABCG2 c.421c>a polymorphism based on PBPK analysis of rosuvastatin AZUSA FUTATSUGI, KOTA TOSHIMOTO, TAKASHI YOSHIKADO, YUICHI
Evaluation of alteration in hepatic and intestinal BCRP function in vivo due to ABCG2 c.421c>a polymorphism based on PBPK analysis of rosuvastatin AZUSA FUTATSUGI, KOTA TOSHIMOTO, TAKASHI YOSHIKADO, YUICHI
Drug Interactions, from bench to bedside
 Drug Interactions, from bench to bedside Candidate to Market, The Paterson Institute for Cancer Research, Manchester, UK Michael Griffin PhD Overview of presentation To understand the importance of drug-drug
Drug Interactions, from bench to bedside Candidate to Market, The Paterson Institute for Cancer Research, Manchester, UK Michael Griffin PhD Overview of presentation To understand the importance of drug-drug
1.* Dosage. A. Adults
 3-Hydroxy-3-Methylglutaryl Coenzyme A (HMG-CoA) Reductase Inhibitors [Developed, November 1994; Revised, October 1996; September 1997; September 1998; October 1999; November 1999; August 2000; September
3-Hydroxy-3-Methylglutaryl Coenzyme A (HMG-CoA) Reductase Inhibitors [Developed, November 1994; Revised, October 1996; September 1997; September 1998; October 1999; November 1999; August 2000; September
Management of Post-transplant hyperlipidemia
 Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Erik Mogalian, Polina German, Chris Yang, Lisa Moorehead, Diana Brainard, John McNally, Jennifer Cuvin, Anita Mathias
 Evaluation of Transporter and Cytochrome P450-Mediated Drug-Drug Interactions Between Pan-Genotypic HCV NS5A Inhibitor GS-5816 and Phenotypic Probe Drugs Erik Mogalian, Polina German, Chris Yang, Lisa
Evaluation of Transporter and Cytochrome P450-Mediated Drug-Drug Interactions Between Pan-Genotypic HCV NS5A Inhibitor GS-5816 and Phenotypic Probe Drugs Erik Mogalian, Polina German, Chris Yang, Lisa
Introduction to Pharmacokinetics (PK) Anson K. Abraham, Ph.D. Associate Principal Scientist, PPDM- QP2 Merck & Co. Inc., West Point, PA 5- June- 2017
 Introduction to Pharmacokinetics (PK) Anson K. Abraham, Ph.D. Associate Principal Scientist, PPDM- QP2 Merck & Co. Inc., West Point, PA 5- June- 2017 1 Outline Definition & Relevance of Pharmacokinetics
Introduction to Pharmacokinetics (PK) Anson K. Abraham, Ph.D. Associate Principal Scientist, PPDM- QP2 Merck & Co. Inc., West Point, PA 5- June- 2017 1 Outline Definition & Relevance of Pharmacokinetics
Introduction. Drug Design, Development and Therapy. Choon Ok Kim 1 Eun Sil Oh 2 Hohyun Kim 3 Min Soo Park 1,4. Original Research
 Drug Design, Development and Therapy open access to scientific and medical research Open Access Full Text Article Original Research Pharmacokinetic interactions between glimepiride and rosuvastatin in
Drug Design, Development and Therapy open access to scientific and medical research Open Access Full Text Article Original Research Pharmacokinetic interactions between glimepiride and rosuvastatin in
Metformin: Mechanistic Absorption Modeling and IVIVC Development
 Metformin: Mechanistic Absorption Modeling and IVIVC Development Maziar Kakhi *, Ph.D. FDA Silver Spring, MD 20993 Maziar.kakhi@fda.hhs.gov Viera Lukacova, Ph.D. Simulations Plus Lancaster, CA 93534 viera@simulations-plus.com
Metformin: Mechanistic Absorption Modeling and IVIVC Development Maziar Kakhi *, Ph.D. FDA Silver Spring, MD 20993 Maziar.kakhi@fda.hhs.gov Viera Lukacova, Ph.D. Simulations Plus Lancaster, CA 93534 viera@simulations-plus.com
Yvonne Y. Lau, Hideaki Okochi, Yong Huang, and Leslie Z. Benet
 0090-9556/06/3407-1175 1181$20.00 DRUG METABOLISM AND DISPOSITION Vol. 34, No. 7 Copyright 2006 by The American Society for Pharmacology and Experimental Therapeutics 9076/3121398 DMD 34:1175 1181, 2006
0090-9556/06/3407-1175 1181$20.00 DRUG METABOLISM AND DISPOSITION Vol. 34, No. 7 Copyright 2006 by The American Society for Pharmacology and Experimental Therapeutics 9076/3121398 DMD 34:1175 1181, 2006
