Inverse Association of Serum 25-Hydroxyvitamin D With Markers of Inflammation and Suppression of Osteoclastic Activity in Hemodialysis Patients
|
|
|
- Kristian Goodwin
- 5 years ago
- Views:
Transcription
1 Dialysis Inverse Association of Serum 25-Hydroxyvitamin D With Markers of Inflammation and Suppression of Osteoclastic Activity in Hemodialysis Patients Theodoros Eleftheriadis, 1,2 Georgia Antoniadi, 1 Vassilios Liakopoulos, 1 Ioannis Stefanidis, 1 Grammati Galaktidou 2 1 Nephrology Department, Medical School, University of Thessaly, Larissa, Greece 2 Research Institute, Theagenion Anticancer Hospital, Thessaloniki, Greece Keywords. hemodialysis, inflammation, bone metabolism, vitamin D Introduction. In hemodialysis patients, 25-hydroxyvitamin D conversion to active 1,25-dihydroxyvitamin D by the kidneys is very limited. The expression of both vitamin D receptor and 1α-hydroxylase in cells of the immune system and in both osteoblasts and osteoclasts makes it possible that 25-hydroxyvitamin D could play an important role in both inflammation and bone metabolism acting in a autocrine and/or paracrine way in these patients. Materials and Methods. Thirty-three hemodialysis patients not under vitamin D receptor agonist treatment were enrolled into the study. Serum levels of 25-hydroxyvitamin D, C-reactive protein (CRP), interleukin-6 (IL-6), receptor activator of nuclear factor-κb ligand (RANKL), and osteoprotegerin, as well as intact parathyroid hormone (PTH) were assessed by immunoassays. Results. Regarding inflammation, 25-hydroxyvitamin D inversely correlated with both CRP and IL-6. Regarding bone metabolism, 25-hydroxyvitamin D was positively related to osteoprotegerin, but negatively to the RANKL. The latter could be the result of PTH suppression by 25-hydroxyvitamin D, since 25-hydroxyvitamin D negatively correlated with PTH, which in turn was positively related to RANKL. Conclusions. Serum 25-hydroxyvitamin D is inversely correlated with markers of inflammation and may suppress osteoclastic activity in hemodialysis patients. Original Paper IJKD 2012;6: INTRODUCTION According to the central dogma about vitamin D metabolism and action, vitamin D is produced in the skin or absorbed from dietary sources. After its conversion to 25-hydroxyvitamin D in the liver, vitamin D is transported to the kidneys where it is converted by 1α-hydroxylase to its active form, 1,25-dihydroxyvitamin D. Active vitamin D is indeed not a vitamin, it is a hormone that plays a central role in bone metabolism by increasing calcium and phosphorus absorption in the gastrointestinal tract, stimulating calcium reabsorption in the distal tubule and stimulating osteoclastic activity. 1 Vitamin D metabolism is heavily disturbed in hemodialysis patients. Its reduced activation by the kidneys results in very low circulating levels of 1,25-dihydroxyvitamin D, whereas 25-hydroxyvitamin D deficiency is also a common finding. 2-4 Because of the central dogma about vitamin D metabolism and action, much attention is being paid to active vitamin D receptor (VDR) agonists administration in hemodialysis patients primarily for the treatment of secondary 129
2 hyperparathyroidism. 5 On the contrary, and despite the Kidney Disease Outcomes Quality Initiative guidelines that recommend supplementation with vitamin D2, if the serum level of 25-hydroxyvitamin D is less than 30 ng/ml our sense is that 25-hydroxyvitamin D insufficiency is frequently overlooked. 6 The significance of serum 25-hydroxyvitamin D in patients with chronic kidney failure has been supported by clinical data. In patients with chronic kidney failure, low serum levels of 25-hydroxyvitamin D and not of 1,25-dihydroxyvitamin D was a negative prognostic factor for both progression to end-stage renal disease and death. 7 In hemodialysis patients, 25-hydroxyvitamin D deficiency was associated with sudden cardiac death and overall mortality. 8 The same has been confirmed in peritoneal dialysis patients and in the general population, as well. 9,10 Such findings challenge the central dogma about vitamin D metabolism and action. It seems that vitamin D does not act exclusively in bone metabolism, which is also supported by the presence of the VDR in a wide variety of tissues. The expression of 1α-hydroxylase in extrarenal cells also challenges the central dogma regarding the exclusive endocrine action of vitamin D, suggesting that autocrine and/or paracrine actions are also possible through local 25-hydroxyvitamin D activation. 1,11 Among the cells that express VDR are dendritic cells, macrophages, and stimulated T cells and B cells The same cells also express the enzyme 1α-hydroxylase. Various mediators of inflammation have been shown to increase 1α-hydroxylase expression, and consequently in case of inflammation very high concentrations of 1,25-dihydroxyvitamin D can be produced locally At the bone level, 1,25-dihydroxyvitamin D increases the expression of the receptor activator of nuclear factor-κb ligand (RANKL) in osteoblasts The RANK, which is the receptor for the RANKL on preosteoclasts, induces them to become mature osteoclasts and start bone resorption. 23 On the other hand, 1,25-dihydroxyvitamin D also induces osteoblasts to produce osteoprotegerin, which acts as a decoy receptor that binds and neutralizes RANKL and thus inhibits osteoclastogenesis and osteoclastic activity and induces osteoclast apoptosis. 23 The finding that both osteblasts and osteoclasts express 1α-hydroxylase supports that 25-hydroxyvitamin D can act in the bone in an autocrine and/or paracrine way, without the need of previous activation by the kidneys. 24,25 The aim of the present study was to evaluate the role of serum 25-hydroxyvitamin D in inflammation that characterizes hemodialysis patients, 26 as well as its possible effect on bone metabolism that is heavily disturbed in this population. 27 MATERIALS AND METHODS Patients Thirty-three hemodialysis patients (mean age, 62.8 ± 9.4 years; 20 men and 13 women) were enrolled into this observational laboratory study. The cause of end-stage renal disease was diabetes mellitus in 13 patients, primary glomerulonephritis in 5, interstitial nephritis in 3, hypertension in 3, obstructive nephropathy in 2, autosomal dominant polycystic kidney disease in 2, and unknown in 5. The patients underwent regular hemodialysis via an arteriovenous fistula. Polysulfone low-flux dialysis membranes and a bicarbonate dialysis solution containing 1.25 mmol/l or 1.5 mmol/l of calcium were used. The low calcium dialysis solution was used in case of high serum calcium or very low serum parathyroid hormone (PTH) levels. Hemodialysis sessions (4 hours) had been performed 3 times a week and for at least 1 year prior to the study. The KT/V according to the second-generation natural logarithmic formula, based on the single-pool urea kinetic model, was 1.21 ± At the time of blood collection, serum calcium level was 9.48 ± 0.56 mg/ dl, serum phosphorous was 5.97 ± 1.90 mg/dl, and serum albumin was 3.94 ± 0.32 g/dl. None of the patients was a smoker or suffered from infection, malignancy, or autoimmune disease and none had a history of parathyroidectomy. Because our aim was to investigate the role of serum 25-hydroxyvitamin D in inflammation and bone metabolism, patients treated with VDR activators were excluded from the study. Additionally, none of the patients were receiving corticosteroids, cytotoxic drugs, warfarin, anticonvulsants, antidepressants, hormone replacement therapy, biphosphonates, or cinacalcet for at least 6 months prior to the study. Sevelamer hydrochloride (Renagel, Genzyme Pharmaceuticals, Naarden, Netherlands) or lanthanum carbonate (Fosrenol, Shire Pharmaceuticals Group, Chineham, 130
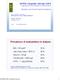
3 Basingstoke, UK) were used as phosphate binders. An informed consent was obtained from each individual enrolled into the study and the hospital ethics committee gave its approval to the study protocol. Methods Blood samples were drawn in the morning before the onset of the second dialysis session of the week and the serum was stored at -80 C. Immunoassays for measuring 25-hydroxyvitamin D and intact PTH were performed in an ELECSYS 2010 automatic analyser (Roche Diagnostics GmbH, Mannheim, Germany). C-reactive protein (CRP) was measured using the Cobas Integra 400 automatic analyzer (Roche Diagnostics GmbH, Mannheim, Germany). Interleukin-6 (IL-6) was assessed by means of an enzyme-linked immunosorbent assay (Biosource Europe SA, Nivelles, Belgium). The RANKL and osteoprotegerin were also measured with an enzyme-linked immunosorbent assay using two commercially available kits (Human srankl [total] enzyme-linked immunosorbent assay, BioVendor GmbH, Heidelberg, Germany and Osteoprotegerin enzyme-linked immunosorbent assay, Biomedica Medizinprodukte GmbH & Co KG, Wien, Austria). Statistical Analyses Mean values and standard deviations were calculated for each continuous variable. The normal distribution of the evaluated variables was assessed using the 1-sample Kolmogorov-Smirnov test; 25-hydroxyvitamin D, osteoprotegerin, IL-6, and intact PTH values were normally distributed, but not the CRP and RANKL levels. For evaluating relationship among normally distributed variables, the Pearson correlation coefficient was calculated, whereas the Spearman rho was calculated in case of nonparametric data. A relationship was considered significant when the 2-sided P value was less than.05. RESULTS The mean serum 25-hydroxyvitamin D level was ± 5.34 ng/ml. Twenty-eight of the 33 patients (84.8%) had serum 25-hydroxyvitamin D levels less than 30 ng/ml. The mean CRP level was ± mg/l and the mean IL-6 level was ± pg/ml. Of the 33 patients, 15 (45.5%) had increased CRP values, ie, greater than 5 mg/l. The mean serum values for were ± pmol/l for the RANKL, ± 3.96 pmol/l for osteoprotegerin, and ± pg/ml for intact PTH. Serum 25-hydroxyvitamin D inversely correlated with CRP (r = , P =.04). An inverse relationship was also detected between 25-hydroxyvitamin D and IL-6 (r = , P =.008; Figure 1). As expected, serum CRP correlated with serum IL-6 (r = 0.576, P <.001). Serum 25-hydroxyvitamin D inversely correlated with serum intact PTH (r = , P =.02), but directly correlated with serum osteoprotegerin (r = 0.366, P =.04; Figure 2). Figure 1. Relationship between 25-hydroxyvitamin D and interleukin-6. Serum 25-hydroxyvitamin D inversely correlated with the serum marker of inflammation, interleukin-6 (r = , P =.008). Figure 2. Relationship between 25-hydroxyvitamin D and osteoprotegerin. Serum 25-hydroxyvitamin D positively correlated with serum osteoprotegerin (r = 0.366, P =.04). 131
4 An inverse correlation was found between serum 25-hydroxyvitamin D and serum RANKL (r = , P =.005). Serum intact PTH was not significantly related with serum osteoprotegerin (r = , P =.834), but it correlated with RANKL (r = 0.439, P =.01). DISCUSSION In the present study, the associations of serum 25-hydroxyvitamin D with markers of inflammation and with the two major proteins that control osteoclastic activity, the RANKL and the osteoprotegerin, were investigated. These questions are of particular interest in hemodialysis patients because inflammation is common in this population, 26 which is also characterized by heavily disturbed bone metabolism. 27 The expression of both VDR and 1α-hydroxylase in the cells of the immune system and in both osteoblasts and osteclasts, 12-19,24,25 combined with the drastic decreased conversion of 25-hydroxyvitamin D to active 1,25-dihydroxyvitamin D by the kidneys of hemodialysis patients, 2 means that the autocrine and paracrine action of 25-hydroxyvitamin D in these two systems could be important. Not surprisingly, 25-hydroxyvitamin D insufficiency was very common in the cohort of our patients, since its serum level was bellow the recommended limit of 30 ng/ml (85% of the patients). 6 The very high incidence of 25-hydroxyvitamin D insufficiency in hemodialysis patients was detected by previous studies as well. 3,4 Regarding inflammation, increased serum CRP levels in approximately half of our patients reconfirmed that inflammation is a common finding in hemodialysis patients. 26 Besides their central role in the treatment of secondary hyperparathyroidism, 5 the beneficial effect of active vitamin D agonists on various other aspects, and particularly on inflammation in patients with chronic kidney failure, has been confirmed. 28 In vitro studies showed that active VDR agonists decrease cytokine production by human blood mononuclear cells after various inflammatory stimuli, 29,30 and in the clinic, administration of an active VDR agonist decreased CRP in patients with kidney failure. 31 However, the available data about the association of serum 25-hydroxyvitamin D with inflammation in hemodialysis patients are scarce. The present study showed that serum 25-hydroxyvitamin D was negatively correlated with the markers of inflammation, CRP and IL-6, in hemodialysis patients. This capacity of 25-hydroxyvitamin D to attenuate inflammation in hemodialysis patients is very important because inflammation has been incriminated for malnutrition, 32 erythropoietin resistance, 33,34 atherosclerosis, 35 impaired immune response, and death in this population. Regarding the effect of serum 25-hydroxyvitamin D on bone metabolism, the present study supports that 25-hydroxyvitamin D may suppress osteoclastic activity, since it is positively related to osteoprotegerin, but negatively to RANKL. The positive relationship of serum 25-hydroxyvitamin D with serum osteoprotegerin was expected, but the negative relationship of serum 25-hydroxyvitamin D with serum RANKL is against to what is known from in vitro studies The answer could be in the effect of 25-hydroxyvitamin D on PTH. As expected, serum intact PTH level was increased in hemodialysis patients. In addition, serum intact PTH positively correlated with serum RANKL. It is known that PTH increases bone resorption by increasing RANKL expression in osteoblasts. 22,39,40 Additionally, in the cohort of our patients, serum 25-hydroxyvitamin D was negatively related with serum intact PTH. The suppression of PTH by 1,25-dihydroxyvitamin D is established. 41,42 However, the expression of 1α-hydroxylase in the parathyroid glands supports that 25-hydroxyvitamin D could suppress PTH by acting in an autocrine way. 43 The latter has also been confirmed by clinical studies and could be responsible for the negative correlation between 25-hydroxyvitamin D and RANKL detected in the present study It is possible that in vivo 25-hydroxyvitamin D suppresses RANKL expression indirectly through the suppression of intact PTH expression. Additionally, there are in vivo experimental data suggesting that vitamin D suppresses RANKL independently of its effect on PTH production. In parathyreoidectomized rats constantly infused with PTH, pharmacological or toxic doses of 1,25-dihydroxyvitamin D stimulate bone resorption by inducing RANKL, but a certain range of physiological doses of the vitamin inhibits PTH-induced bone resorption possibly by suppressing the PTH/PTHrP receptor-mediated signaling. 47 Furthermore, it has been experimentally confirmed that 25-hydroxyvitamin D depletion 132
5 induces RANKL-mediated osteoclastogenesis and bone loss. 48 The design of the present study could not exclude the possibility that the negative relationship between serum 25-hydroxyvitamin D and markers of inflammation could result from decreased vitamin D intake due to inflammation-induced malnutrition. 32 However, our patients were stable, did not suffered from other than the hemodialysis inflammatory conditions, and mostly had normal serum albumin values. Additionally, there are plenty of clinical and experimental data, already mentioned in the present text, that support the anti-inflammatory properties of VDR agonists. Another problem with the interpretation of the results of the present study is that besides osteoblasts, other cell types, particularly of the immune system, are also sources of serum osteoprotegerin and RANKL. However, these molecules, even if are expressed in immune cells, affect osteoclastic activity. In inflammatory diseases the participation of activated lymphocytes in pathological bone erosion, mainly through RANKL expression by activated T cells, is established. 49 Another study showed that both B and T lymphocytes play a significant role in basal bone turnover, since T cells help B cells to produce the 65% of the total osteoprotegerin in bone marrow in mice. B-cell knockout mice were found to be osteoporotic and deficient in bone marrow osteoprotegerin, phenomena that are reversed by B-cell reconstitution. 50 The last limitation of this study to be discussed here is that hemodialysis patients with very high serum intact PTH levels were not present in this study, because those treated with VDR agonists for secondary hyperparathyroidism were excluded. Nonetheless, this was the only way to isolate the effect of serum 25-hydroxyvitamin D on the evaluated parameters. Unfortunately, this exclusion criterion limited the number of the patients enrolled in the study. CONCLUSIONS The associations detected in the present study suggest that in hemodialysis patients, 25-hydroxyvitamin D, acting in an autocrine and/or paracrine way, ameliorates inflammation. In addition, regarding bone metabolism, 25-hydroxyvitamin D exerts an anabolic effect. Correction of 25-hydroxyvitamin D insufficiency, which is very common in this population, is expected to offer great benefit. However, larger, prospective, interventional studies, based on the administration of 25-hydroxyvitamin D in hemodialysis patients, are required for definite conclusions. CONFLICT OF INTEREST None declared. REFERENCES 1. Holick MF. Vitamin D deficiency. N Engl J Med. 2007;357: Al-Badr W, Martin KJ. Vitamin D and kidney disease. Clin J Am Soc Nephrol. 2008;3: Gonzalez EA, Sachdeva A, Oliver DA, Martin KJ. Vitamin D insufficiency and deficiency in chronic kidney disease. A single center observational study. Am J Nephrol. 2004;24: Wolf M, Shah A, Gutierrez O, et al. Vitamin D levels and early mortality among incident hemodialysis patients. Kidney Int. 2007;72: Martin KJ, Gonzalez EA. Vitamin D analogs: actions and role in the treatment of secondary hyperparathyroidism. Semin Nephrol. 2004;24: [No author listed]. K/DOQI clinical practice guidelines for bone metabolism and disease in chronic kidney disease. Am J Kidney Dis. 2003;42:S Ravani P, Malberti F, Tripepi G, et al. Vitamin D levels and patient outcome in chronic kidney disease. Kidney Int. 2009;75: Drechsler C, Pilz S, Obermayer-Pietsch B, et al. Vitamin D deficiency is associated with sudden cardiac death, combined cardiovascular events, and mortality in haemodialysis patients. Eur Heart J. 2010;31: Wang AY, Lam CW, Sanderson JE, et al. Serum 25-hydroxyvitamin D status and cardiovascular outcomes in chronic peritoneal dialysis patients: a 3-y prospective cohort study. Am J Clin Nutr. 2008;87: Mertens PR, Muller R. Vitamin D and cardiovascular risk. Int Urol Nephrol. 2010;42: Jones G. Expanding role for vitamin D in chronic kidney disease: importance of blood 25-OH-D levels and extrarenal 1alpha-hydroxylase in the classical and nonclassical actions of 1alpha,25-dihydroxyvitamin D(3). Semin Dial. 2007;20: Provvedini DM, Tsoukas CD, Deftos LJ, Manolagas SC. 1,25-dihydroxyvitamin D3 receptors in human leukocytes. Science. 1983;221: Rigby WF, Stacy T, Fanger MW. Inhibition of T lymphocyte mitogenesis by 1,25-dihydroxyvitamin D3 (calcitriol). J Clin Invest. 1984;74: Rigby WF, Denome S, Fanger MW. Regulation of lymphokine production and human T lymphocyte activation by 1,25-dihydroxyvitamin D3. Specific inhibition at the level of messenger RNA. J Clin Invest. 1987;79:
6 15. Mahon BD, Wittke A, Weaver V, Cantorna MT. The targets of vitamin D depend on the differentiation and activation status of CD4 positive T cells. J Cell Biochem. 2003;89: Adams JS, Sharma OP, Gacad MA, Singer FR. Metabolism of 25-hydroxyvitamin D3 by cultured pulmonary alveolar macrophages in sarcoidosis. J Clin Invest. 1983;72: Monkawa T, Yoshida T, Hayashi M, Saruta T. Identification of 25-hydroxyvitamin D3 1alpha-hydroxylase gene expression in macrophages. Kidney Int. 2000;58: Fritsche J, Mondal K, Ehrnsperger A, Andreesen R, Kreutz M. Regulation of 25-hydroxyvitamin D3-1 alpha-hydroxylase and production of 1 alpha,25- dihydroxyvitamin D3 by human dendritic cells. Blood. 2003;102: Liu PT, Stenger S, Li H, et al. Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response. Science. 2006;311: Kitazawa S, Kajimoto K, Kondo T, Kitazawa R. Vitamin D3 supports osteoclastogenesis via functional vitamin D response element of human RANKL gene promoter. J Cell Biochem. 2003;89: Hofbauer LC, Dunstan CR, Spelsberg TC, Riggs BL, Khosla S. Osteoprotegerin production by human osteoblast lineage cells is stimulated by vitamin D, bone morphogenetic protein-2, and cytokines. Biochem Biophys Res Commun. 1998;250: Horwood NJ, Elliott J, Martin TJ, Gillespie MT. Osteotropic agents regulate the expression of osteoclast differentiation factor and osteoprotegerin in osteoblastic stromal cells. Endocrinology. 1998;139: Boyce BF, Xing L. Functions of RANKL/RANK/OPG in bone modeling and remodeling. Arch Biochem Biophys. 2008;473: Atkins GJ, Anderson PH, Findlay DM, et al. Metabolism of vitamin D3 in human osteoblasts: evidence for autocrine and paracrine activities of 1 alpha,25-dihydroxyvitamin D3. Bone. 2007;40: Kogawa M, Findlay DM, Anderson PH, et al. Osteoclastic metabolism of 25(OH)-vitamin D3: a potential mechanism for optimization of bone resorption. Endocrinology. 2010;151: Eleftheriadis T, Antoniadi G, Liakopoulos V, Kartsios C, Stefanidis I. Disturbances of acquired immunity in hemodialysis patients. Semin Dial. 2007;20: Malluche HH, Langub MC, Monier-Faugere MC. The role of bone biopsy in clinical practice and research. Kidney Int Suppl. 1999;73:S Eleftheriadis T, Antoniadi G, Liakopoulos V, Antoniadis N, Stefanidis I, Galaktidou G. Vitamin D receptor activators and response to injury in kidney diseases. J Nephrol. 2010;23: Muller K, Haahr PM, Diamant M, Rieneck K, Kharazmi A, Bendtzen K. 1,25-Dihydroxyvitamin D3 inhibits cytokine production by human blood monocytes at the posttranscriptional level. Cytokine. 1992;4: Eleftheriadis T, Antoniadi G, Liakopoulos V, Kartsios C, Stefanidis I, Galaktidou G. Paricalcitol reduces basal and lipopolysaccharide-induced (LPS) TNF-alpha and IL-8 production by human peripheral blood mononuclear cells. Int Urol Nephrol. 2010;42: Alborzi P, Patel NA, Peterson C, et al. Paricalcitol reduces albuminuria and inflammation in chronic kidney disease: a randomized double-blind pilot trial. Hypertension. 2008;52: Stenvinkel P, Heimburger O, Lindholm B, Kaysen GA, Bergstrom J. Are there two types of malnutrition in chronic renal failure? Evidence for relationships between malnutrition, inflammation and atherosclerosis (MIA syndrome). Nephrol Dial Transplant. 2000;15: Eleftheriadis T, Kartsios C, Liakopoulos V, et al. Does hepcidin affect erythropoiesis in hemodialysis patients? Acta Haematol. 2006;116: Eleftheriadis T, Liakopoulos V, Antoniadi G, Kartsios C, Stefanidis I. The role of hepcidin in iron homeostasis and anemia in hemodialysis patients. Semin Dial. 2009;22: Zimmermann J, Herrlinger S, Pruy A, Metzger T, Wanner C. Inflammation enhances cardiovascular risk and mortality in hemodialysis patients. Kidney Int. 1999;55: Eleftheriadis T, Kartsios C, Yiannaki E, et al. Chronic inflammation and T cell zeta-chain downregulation in hemodialysis patients. Am J Nephrol. 2008;28: Eleftheriadis T, Kartsios C, Yiannaki E, et al. Chronic inflammation and CD16+ natural killer cell zeta-chain downregulation in hemodialysis patients. Blood Purif. 2008;26: Eleftheriadis T, Liakopoulos V, Antoniadi G, Stefanidis I, Galaktidou G. Indoleamine 2,3-dioxygenase is increased in hemodialysis patients and affects immune response to hepatitis B vaccination. Vaccine. 2011;29: Lee SK, Lorenzo JA. Parathyroid hormone stimulates TRANCE and inhibits osteoprotegerin messenger ribonucleic acid expression in murine bone marrow cultures: correlation with osteoclast-like cell formation. Endocrinology. 1999;140: Huang JC, Sakata T, Pfleger LL, et al. PTH differentially regulates expression of RANKL and OPG. J Bone Miner Res. 2004;19: Russell J, Lettieri D, Sherwood LM. Suppression by 1,25(OH)2D3 of transcription of the pre-proparathyroid hormone gene. Endocrinology. 1986;119: Slatopolsky E, Weerts C, Thielan J, Horst R, Harter H, Martin KJ. Marked suppression of secondary hyperparathyroidism by intravenous administration of 1,25-dihydroxy-cholecalciferol in uremic patients. J Clin Invest. 1984;74: Segersten U, Correa P, Hewison M, et al. 25-hydroxyvitamin D(3)-1alpha-hydroxylase expression in normal and pathological parathyroid glands. J Clin Endocrinol Metab. 2002;87: Bjorkman M, Sorva A, Tilvis R. Responses of parathyroid hormone to vitamin D supplementation: a systematic review of clinical trials. Arch Gerontol Geriatr. 2009;48: Gracia-Iguacel C, Gallar P, Qureshi AR, et al. Vitamin D deficiency in dialysis patients: effect of dialysis modality and implications on outcome. J Ren Nutr. 2010;20:
7 46. Jean G, Vanel T, Terrat JC, Chazot C. Prevention of secondary hyperparathyroidism in hemodialysis patients: the key role of native vitamin D supplementation. Hemodial Int. 2010;14: Ueno Y, Shinki T, Nagai Y, Murayama H, Fujii K, Suda T. In vivo administration of 1,25-dihydroxyvitamin D3 suppresses the expression of RANKL mrna in bone of thyroparathyroidectomized rats constantly infused with PTH. J Cell Biochem. 2003;90: Anderson PH, Sawyer RK, Moore AJ, May BK, O Loughlin PD, Morris HA. Vitamin D depletion induces RANKLmediated osteoclastogenesis and bone loss in a rodent model. J Bone Miner Res. 2008;23: Nakashima T, Takayanagi H. The dynamic interplay between osteoclasts and the immune system. Arch Biochem Biophys. 2008;473: Li Y, Toraldo G, Li A, et al. B cells and T cells are critical for the preservation of bone homeostasis and attainment of peak bone mass in vivo. Blood. 2007;109: Correspondence to: Theodoros Eleftheriadis, MD, PhD Department of Nephrology, Medical School, University of Thessaly, Neo Ktirio, Mezourlo Hill, Larissa, Greece Tel: teleftheriadis@yahoo.com Received September 2011 Revised November 2011 Accepted November
Plasma Serotonin and Markers of Bone Formation and Bone Resorption in Hemodialysis Patients
 Dialysis Plasma Serotonin and Markers of Bone Formation and Bone Resorption in Hemodialysis Theodoros Eleftheriadis, 1,2 Georgia Antoniadi, 1 Vassilios Liakopoulos, 1 Theodora Sparopoulou, 2 Ioannis Stefanidis,
Dialysis Plasma Serotonin and Markers of Bone Formation and Bone Resorption in Hemodialysis Theodoros Eleftheriadis, 1,2 Georgia Antoniadi, 1 Vassilios Liakopoulos, 1 Theodora Sparopoulou, 2 Ioannis Stefanidis,
PART FOUR. Metabolism and Nutrition
 PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 21, 2005 Maria Mesquita, 1 Eric Wittersheim, 2 Anne Demulder, 2 Max Dratwa, 1 Pierre Bergmann 3 Bone Cytokines and Renal Osteodystrophy
PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 21, 2005 Maria Mesquita, 1 Eric Wittersheim, 2 Anne Demulder, 2 Max Dratwa, 1 Pierre Bergmann 3 Bone Cytokines and Renal Osteodystrophy
Role of High-sensitivity C-reactive Protein as a Marker of Inflammation in Pre-dialysis Patients of Chronic Renal Failure
 ORIGINAL ARTICLE JIACM 2009; 10(1 & 2): 18-22 Abstract Role of High-sensitivity C-reactive Protein as a Marker of Inflammation in Pre-dialysis Patients of Chronic Renal Failure N Nand*, HK Aggarwal**,
ORIGINAL ARTICLE JIACM 2009; 10(1 & 2): 18-22 Abstract Role of High-sensitivity C-reactive Protein as a Marker of Inflammation in Pre-dialysis Patients of Chronic Renal Failure N Nand*, HK Aggarwal**,
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Kobe University Repository : Kernel
 Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
02/27/2018. Objectives. To Replace or Not to Replace: Nutritional Vitamin D in Dialysis.
 To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
Outline. The Role of Vitamin D in CKD. Essential Role of Vitamin D. Mechanism of Action of Vit D. Mechanism of Action of Vit D 7/16/2010
 Outline The Role of Vitamin D in CKD Priscilla How, Pharm.D., BCPS Assistant Professor National University of Singapore Principal Clinical Pharmacist National University Hospital (Pharmacy and Nephrology,
Outline The Role of Vitamin D in CKD Priscilla How, Pharm.D., BCPS Assistant Professor National University of Singapore Principal Clinical Pharmacist National University Hospital (Pharmacy and Nephrology,
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Elecsys bone marker panel. Optimal patient management starts in the laboratory
 bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
The hart and bone in concert
 The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
PART ONE. Peritoneal Kinetics and Anatomy
 PART ONE Peritoneal Kinetics and Anatomy Advances in Peritoneal Dialysis, Vol. 22, 2006 Paul A. Fein, Irfan Fazil, Muhammad A. Rafiq, Teresa Schloth, Betty Matza, Jyotiprakas Chattopadhyay, Morrell M.
PART ONE Peritoneal Kinetics and Anatomy Advances in Peritoneal Dialysis, Vol. 22, 2006 Paul A. Fein, Irfan Fazil, Muhammad A. Rafiq, Teresa Schloth, Betty Matza, Jyotiprakas Chattopadhyay, Morrell M.
Effects of Diabetes Mellitus, Age, and Duration of Dialysis on Parathormone in Chronic Hemodialysis Patients. Hamid Nasri 1, Soleiman Kheiri 2
 Saudi J Kidney Dis Transplant 2008;19(4):608-613 2008 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Effects of Diabetes Mellitus, Age, and
Saudi J Kidney Dis Transplant 2008;19(4):608-613 2008 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Effects of Diabetes Mellitus, Age, and
Malnutrition and inflammation in peritoneal dialysis patients
 Kidney International, Vol. 64, Supplement 87 (2003), pp. S87 S91 Malnutrition and inflammation in peritoneal dialysis patients PAUL A. FEIN, NEAL MITTMAN, RAJDEEP GADH, JYOTIPRAKAS CHATTOPADHYAY, DANIEL
Kidney International, Vol. 64, Supplement 87 (2003), pp. S87 S91 Malnutrition and inflammation in peritoneal dialysis patients PAUL A. FEIN, NEAL MITTMAN, RAJDEEP GADH, JYOTIPRAKAS CHATTOPADHYAY, DANIEL
New biological targets for CKD- MBD: From the KDOQI to the
 New biological targets for CKD- MBD: From the KDOQI to the KDIGO Guillaume JEAN, MD. Centre de Rein Artificiel, 42 avenue du 8 mai 1945, Tassin la Demi-Lune, France. E-mail : guillaume-jean-crat@wanadoo.fr
New biological targets for CKD- MBD: From the KDOQI to the KDIGO Guillaume JEAN, MD. Centre de Rein Artificiel, 42 avenue du 8 mai 1945, Tassin la Demi-Lune, France. E-mail : guillaume-jean-crat@wanadoo.fr
( ) , (Donabedian, 1980) We would not choose any treatment with poor outcomes
 ..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
PART FOUR. Metabolism and Nutrition
 PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 23, 2007 Alicja E. Grzegorzewska, Monika Mĺot Michalska Serum Level of Intact Parathyroid Hormone and Other Markers of Bone Metabolism
PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 23, 2007 Alicja E. Grzegorzewska, Monika Mĺot Michalska Serum Level of Intact Parathyroid Hormone and Other Markers of Bone Metabolism
Protocol GTC : A Randomized, Open Label, Parallel Design Study of Sevelamer Hydrochloride (Renagel ) in Chronic Kidney Disease Patients.
 Protocol GTC-68-208: A Randomized, Open Label, Parallel Design Study of Sevelamer Hydrochloride (Renagel ) in Chronic Kidney Disease Patients. These results are supplied for informational purposes only.
Protocol GTC-68-208: A Randomized, Open Label, Parallel Design Study of Sevelamer Hydrochloride (Renagel ) in Chronic Kidney Disease Patients. These results are supplied for informational purposes only.
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment
 Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE ON MAINTENANCE DIALYSIS THERAPY
 UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
2017 KDIGO Guidelines Update
 2017 KDIGO Guidelines Update Clinic for Hemodialysis Clinical Center University of Sarajevo 13 th Congress of the Balkan cities Association of Nephrology, Dialysis, and Artificial Organs Transplantation
2017 KDIGO Guidelines Update Clinic for Hemodialysis Clinical Center University of Sarajevo 13 th Congress of the Balkan cities Association of Nephrology, Dialysis, and Artificial Organs Transplantation
Hyperphosphatemia is associated with a
 TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
J.Bacchetta has documented that she has received grants for research activities from Amgen, Crinex, Sandoz.
 J.Bacchetta has documented that she has received grants for research activities from Amgen, Crinex, Sandoz. Epidemiological, immune and metabolic aspects of vitamin D in CKD Justine Bacchetta, MD, PhD
J.Bacchetta has documented that she has received grants for research activities from Amgen, Crinex, Sandoz. Epidemiological, immune and metabolic aspects of vitamin D in CKD Justine Bacchetta, MD, PhD
Clinical Guideline Bone chemistry management in adult renal patients on dialysis
 Clinical Guideline Bone chemistry management in adult renal patients on dialysis This guidance covers how to: Maintain serum phosphate 0.8 to 1.7mmol/L 1 Maintain serum corrected calcium 2.1 to 2.5mmol/L
Clinical Guideline Bone chemistry management in adult renal patients on dialysis This guidance covers how to: Maintain serum phosphate 0.8 to 1.7mmol/L 1 Maintain serum corrected calcium 2.1 to 2.5mmol/L
Advances in Peritoneal Dialysis, Vol. 29, 2013
 Advances in Peritoneal Dialysis, Vol. 29, 2013 Takeyuki Hiramatsu, 1 Takahiro Hayasaki, 1 Akinori Hobo, 1 Shinji Furuta, 1 Koki Kabu, 2 Yukio Tonozuka, 2 Yoshiyasu Iida 1 Icodextrin Eliminates Phosphate
Advances in Peritoneal Dialysis, Vol. 29, 2013 Takeyuki Hiramatsu, 1 Takahiro Hayasaki, 1 Akinori Hobo, 1 Shinji Furuta, 1 Koki Kabu, 2 Yukio Tonozuka, 2 Yoshiyasu Iida 1 Icodextrin Eliminates Phosphate
Ipovitaminosi D e metabolismo calcio-fosforo in dialisi peritoneale. Maurizio Gallieni Università degli Studi di Milano
 Ipovitaminosi D e metabolismo calcio-fosforo in dialisi peritoneale Maurizio Gallieni Università degli Studi di Milano G Ital Nefrol 2018 - ISSN 1724-5990 Nutrients 2017, 9, 328 Vitamin D deficiency (
Ipovitaminosi D e metabolismo calcio-fosforo in dialisi peritoneale Maurizio Gallieni Università degli Studi di Milano G Ital Nefrol 2018 - ISSN 1724-5990 Nutrients 2017, 9, 328 Vitamin D deficiency (
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Parathyroid hormone (serum, plasma)
 Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients
 Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
SCIENTIFIC DISCUSSION
 European Medicines Agency London, 01 June 2007 Product Name : Renagel Procedure No: EMEA/H/C/000254/II/56 SCIENTIFIC DISCUSSION 1/11 1. Introduction Renagel (sevelamer), a non-absorbed, calcium and metal-free
European Medicines Agency London, 01 June 2007 Product Name : Renagel Procedure No: EMEA/H/C/000254/II/56 SCIENTIFIC DISCUSSION 1/11 1. Introduction Renagel (sevelamer), a non-absorbed, calcium and metal-free
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Glycaemic control and serum intact parathyroid hormone levels in diabetic patients on haemodialysis therapy
 Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
Phosphate binders and metabolic acidosis in patients undergoing maintenance hemodialysis sevelamer hydrochloride, calcium carbonate, and bixalomer
 Hemodialysis International 2015; 19:5459 Phosphate binders and metabolic acidosis in patients undergoing maintenance hemodialysis sevelamer hydrochloride, calcium carbonate, and bixalomer Toru SANAI, 1
Hemodialysis International 2015; 19:5459 Phosphate binders and metabolic acidosis in patients undergoing maintenance hemodialysis sevelamer hydrochloride, calcium carbonate, and bixalomer Toru SANAI, 1
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience
 Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Renal Association Clinical Practice Guideline in Mineral and Bone Disorders in CKD
 Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
Variable Included. Excluded. Included. Excluded
 Table S1. Baseline characteristics of patients included in the analysis and those excluded patients because of missing baseline serumj bicarbonate levels, stratified by dialysis modality. Variable HD patients
Table S1. Baseline characteristics of patients included in the analysis and those excluded patients because of missing baseline serumj bicarbonate levels, stratified by dialysis modality. Variable HD patients
Vitamin D. Vitamin functioning as hormone. Todd A Fearer, MD FACP
 Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
Normal kidneys filter large amounts of organic
 ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
Contents. Authors Name: Christopher Wong: Consultant Nephrologist Anne Waddington: Renal Pharmacist Eimear Fegan : Renal Dietitian
 Cheshire and Merseyside Renal Units Guidelines on the Management of Chronic Kidney Disease - Mineral Bone Disorder (adapted from Greater Manchester) Authors Name: Christopher Wong: Consultant Nephrologist
Cheshire and Merseyside Renal Units Guidelines on the Management of Chronic Kidney Disease - Mineral Bone Disorder (adapted from Greater Manchester) Authors Name: Christopher Wong: Consultant Nephrologist
Marie-Claude Monier-Faugere, Hanna Mawad, and Hartmut H. Malluche
 Opposite Effects of Calcitriol and Paricalcitol on the Parathyroid Hormone-(1-84)/Large Carboxy-Terminal- Parathyroid Hormone Fragments Ratio in Patients with Stage 5 Chronic Kidney Disease Marie-Claude
Opposite Effects of Calcitriol and Paricalcitol on the Parathyroid Hormone-(1-84)/Large Carboxy-Terminal- Parathyroid Hormone Fragments Ratio in Patients with Stage 5 Chronic Kidney Disease Marie-Claude
FGF23 (and Klotho): what s new? Brief introduction to FGF23. Introduction to FGF23. FGF23: phosphorylation pathways. FGF23: phosphorylation pathways
 (and Klotho): what s new? Brief introduction to Justine Bacchetta, MD, PhD Reference Center for Rare Renal Diseases Long Beach, CA, 2017 Calcium and phosphate metabolism 1-25 vitamin D Introduction to
(and Klotho): what s new? Brief introduction to Justine Bacchetta, MD, PhD Reference Center for Rare Renal Diseases Long Beach, CA, 2017 Calcium and phosphate metabolism 1-25 vitamin D Introduction to
New vitamin D analogs
 Kidney International, Vol. 63, Supplement 85 (2003), pp. S83 S87 New vitamin D analogs EDUARDO SLATOPOLSKY, JANE FINCH, and ALEX BROWN Renal Division, Department of Internal Medicine, Washington University
Kidney International, Vol. 63, Supplement 85 (2003), pp. S83 S87 New vitamin D analogs EDUARDO SLATOPOLSKY, JANE FINCH, and ALEX BROWN Renal Division, Department of Internal Medicine, Washington University
Attivazione selettiva dei VDR nella CKD-MBD: dalla conservativa alla dialisi
 Attivazione selettiva dei VDR nella CKD-MBD: dalla conservativa alla dialisi Mario Cozzolino, MD, PhD, FERA Dipartimento di Scienze della Salute Università di Milano UO Nefrologia e Dialisi Laboratorio
Attivazione selettiva dei VDR nella CKD-MBD: dalla conservativa alla dialisi Mario Cozzolino, MD, PhD, FERA Dipartimento di Scienze della Salute Università di Milano UO Nefrologia e Dialisi Laboratorio
Should cinacalcet be used in patients who are not on dialysis?
 Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Modern Medical Laboratory Journal - ISSN X
 Original Article Mod Med Lab. 2017; 1(1): 17-17 22 Modern Medical Laboratory Journal - ISSN 2371-770X An Investigation of the Relationship between Beta-2 Microglobulin (β2m) and Inflammatory Factors (Serum
Original Article Mod Med Lab. 2017; 1(1): 17-17 22 Modern Medical Laboratory Journal - ISSN 2371-770X An Investigation of the Relationship between Beta-2 Microglobulin (β2m) and Inflammatory Factors (Serum
2.0 Synopsis. Paricalcitol Capsules M Clinical Study Report R&D/15/0380. (For National Authority Use Only)
 2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-358/Zemplar (paricalcitol) Capsules Name of Active Ingredient: paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-358/Zemplar (paricalcitol) Capsules Name of Active Ingredient: paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
DIALYSIS. Original Paper. Parvin Soltani, 1 Pardis Ketabi Moghaddam, 2 Farshid Haghverdi, 1 Ali Cheraghi 2
 DIALYSIS A Randomized Clinical Trial of the Effect of Pentoxifylline on C-Reactive Protein Level and Dialysis Adequacy in Endstage Renal Disease Patients on Maintenance Hemodialysis Parvin Soltani, 1 Pardis
DIALYSIS A Randomized Clinical Trial of the Effect of Pentoxifylline on C-Reactive Protein Level and Dialysis Adequacy in Endstage Renal Disease Patients on Maintenance Hemodialysis Parvin Soltani, 1 Pardis
Supplementary Information to Chapter 36
 REVIEW ON VITAMIN-D NEW INSIGHTS Elmer Verner McCollum (1879-1967) was the first to discover the antirachitic vitamin which he named as vitamin D in the early part of 20th century (1919). He had earlier
REVIEW ON VITAMIN-D NEW INSIGHTS Elmer Verner McCollum (1879-1967) was the first to discover the antirachitic vitamin which he named as vitamin D in the early part of 20th century (1919). He had earlier
silent epidemic,. (WHO),
 Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
Disclosures. Topics. Staging and GFR. K-DOQI Staging of Chronic Kidney Disease. Definition of Chronic Kidney Disease. Chronic Kidney Disease
 Disclosures Chronic Kidney Disease Consultant: Baxter Healthcare J. Kevin Tucker, M.D. Brigham and Women s Hospital Massachusetts General Hospital Topics Staging of chronic kidney disease (CKD) How to
Disclosures Chronic Kidney Disease Consultant: Baxter Healthcare J. Kevin Tucker, M.D. Brigham and Women s Hospital Massachusetts General Hospital Topics Staging of chronic kidney disease (CKD) How to
1. Reggie J. Divina, M.D. (1) 2. Fe S. Felicilda, M.D., DPBCN (1,2) 3. Rufino E. Chan, M.D. (1) 4. Luisito O. Llido, M.D.
 82 TITLE: Nutritional status of hemodialysis patients in the Philippines: a cross sectional survey in four out- patient dialysis centers Submitted: January 10, 2010 Posted: August 30, 2010 AUTHOR(S) 1.
82 TITLE: Nutritional status of hemodialysis patients in the Philippines: a cross sectional survey in four out- patient dialysis centers Submitted: January 10, 2010 Posted: August 30, 2010 AUTHOR(S) 1.
FOCUS ON CARDIOVASCULAR DISEASE
 The Consequences of Vitamin D Deficiency: FOCUS ON CARDIOVASCULAR DISEASE Vitamin D deficiency is a global health problem. With all the medical advances of the century, vitamin D deficiency is still epidemic.
The Consequences of Vitamin D Deficiency: FOCUS ON CARDIOVASCULAR DISEASE Vitamin D deficiency is a global health problem. With all the medical advances of the century, vitamin D deficiency is still epidemic.
Impact of serum FGF23 levels on blood pressure of patients with chronic kidney disease
 European Review for Medical and Pharmacological Sciences 2018; 22: 721-725 Impact of serum FGF23 levels on blood pressure of patients with chronic kidney disease J.-X. LI, G.-Q. YU, Y.-Z. ZHUANG Department
European Review for Medical and Pharmacological Sciences 2018; 22: 721-725 Impact of serum FGF23 levels on blood pressure of patients with chronic kidney disease J.-X. LI, G.-Q. YU, Y.-Z. ZHUANG Department
Designed to be taken at facility only 3 times per week. Greater convenience for patients & caregivers and compliance for providers
 MV-ONE PLUS is a novel antioxidative nutraceutical especially formulated for patients with chronic kidney disease (CKD). MV-ONE PLUS has been designed as a supplement to address vitamin D deficiency and
MV-ONE PLUS is a novel antioxidative nutraceutical especially formulated for patients with chronic kidney disease (CKD). MV-ONE PLUS has been designed as a supplement to address vitamin D deficiency and
Pediatric Nutrition and Kidney Disease
 Pediatric Nutrition and Kidney Disease Loai Eid, MD, MSHS, FAAP Consultant Pediatric Nephrologist Pediatric Nephrology & Hypertension Division Chief Dubai Hospital - DHA 26 th October, 2017 Objectives
Pediatric Nutrition and Kidney Disease Loai Eid, MD, MSHS, FAAP Consultant Pediatric Nephrologist Pediatric Nephrology & Hypertension Division Chief Dubai Hospital - DHA 26 th October, 2017 Objectives
A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication
 Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Prevalence of malnutrition in dialysis
 ESPEN Congress Cannes 2003 Organised by the Israel Society for Clinical Nutrition Education and Clinical Practice Programme Session: Nutrition and the Kidney Malnutrition and Haemodialysis Doctor Noël
ESPEN Congress Cannes 2003 Organised by the Israel Society for Clinical Nutrition Education and Clinical Practice Programme Session: Nutrition and the Kidney Malnutrition and Haemodialysis Doctor Noël
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Secondary hyperparathyroidism in chronic kidney disease recent paradigm shift in clinical management
 Secondary hyperparathyroidism in chronic kidney disease recent paradigm shift in clinical management Complete this course and earn 1 CME POINT Dr. HO Chung Ping MBBS (HK), MRCP, FRCP (Glas, Edin), FHKCP,
Secondary hyperparathyroidism in chronic kidney disease recent paradigm shift in clinical management Complete this course and earn 1 CME POINT Dr. HO Chung Ping MBBS (HK), MRCP, FRCP (Glas, Edin), FHKCP,
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis
 Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
Vitamin D receptor gene polymorphism and serum levels of Fetuin-A, Vitamin D and ipth in the hemodialysis patients
 In The Name of GOD Vitamin D receptor gene polymorphism and serum levels of Fetuin-A, Vitamin D and ipth in the hemodialysis patients Authors & Affiliations: 1-jamal hallajzadeh; Maraghe University of
In The Name of GOD Vitamin D receptor gene polymorphism and serum levels of Fetuin-A, Vitamin D and ipth in the hemodialysis patients Authors & Affiliations: 1-jamal hallajzadeh; Maraghe University of
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients
 Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
Skeletal. Parathyroid hormone-related protein Analyte Information
 Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
chapter 1 & 2009 KDIGO
 http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
Setting the standard
 SCLEROSTIN in NEPHROLOGY MOST REFERENCED OPTIMIZED FOR CLINICAL SAMPLES Setting the standard for clinical research. SCLEROSTIN A BONE-RELATED PROTEIN URINE PROTOCOL AVAILABLE Sclerostin ELISA - Assay Characteristics
SCLEROSTIN in NEPHROLOGY MOST REFERENCED OPTIMIZED FOR CLINICAL SAMPLES Setting the standard for clinical research. SCLEROSTIN A BONE-RELATED PROTEIN URINE PROTOCOL AVAILABLE Sclerostin ELISA - Assay Characteristics
... . : ... PTH.
 IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Comparison of Fetuin-A, Vitamin D, Monounsaturated Fatty Acid, and Vascular Calcification on Plain Radiography Between Dialysis Modalities
 DIALYSIS Comparison of Fetuin-A, Vitamin D, Monounsaturated Fatty Acid, and Vascular Calcification on Plain Radiography Between Dialysis Modalities Hye In Kim, 1 Won Suk An 1, 2 1 Department of Internal
DIALYSIS Comparison of Fetuin-A, Vitamin D, Monounsaturated Fatty Acid, and Vascular Calcification on Plain Radiography Between Dialysis Modalities Hye In Kim, 1 Won Suk An 1, 2 1 Department of Internal
Guidelines and new evidence on CKD - MBD treatment
 Guidelines and new evidence on CKD - MBD treatment Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia ERA-EDTA CME course IV Congress of Nephrology of B&H, April 25, 2015, Sarajevo,
Guidelines and new evidence on CKD - MBD treatment Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia ERA-EDTA CME course IV Congress of Nephrology of B&H, April 25, 2015, Sarajevo,
Drugs Affecting Bone. Rosa McCarty PhD. Department of Pharmacology & Therapeutics
 Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
IL-17 in health and disease. March 2014 PSO13-C051n
 IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
Month/Year of Review: September 2012 Date of Last Review: September 2010
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 1.393, ISSN: , Volume 2, Issue 7, August 2014
 HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
Bone and Mineral. Comprehensive Menu for the Management of Bone and Mineral Related Diseases
 Bone and Mineral Comprehensive Menu for the Management of Bone and Mineral Related Diseases Innovation to Assist in Clinical Diagnosis and Treatment DiaSorin offers a specialty line of Bone and Mineral
Bone and Mineral Comprehensive Menu for the Management of Bone and Mineral Related Diseases Innovation to Assist in Clinical Diagnosis and Treatment DiaSorin offers a specialty line of Bone and Mineral
Serum Hepcidin in Haemodialysis Patients: Associations with Iron Status and Microinflammation
 The Journal of International Medical Research 2011; 39: 1961 1967 Serum Hepcidin in Haemodialysis Patients: Associations with Iron Status and Microinflammation Y XU, XQ DING, JZ ZOU, ZH LIU, SH JIANG AND
The Journal of International Medical Research 2011; 39: 1961 1967 Serum Hepcidin in Haemodialysis Patients: Associations with Iron Status and Microinflammation Y XU, XQ DING, JZ ZOU, ZH LIU, SH JIANG AND
CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015)
 CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015) Dr Simon Steddon, Consultant Nephrologist, Guy s and St Thomas NHS Foundation Trust, London Dr Edward Sharples,
CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015) Dr Simon Steddon, Consultant Nephrologist, Guy s and St Thomas NHS Foundation Trust, London Dr Edward Sharples,
Bsml Polymorphism of the Vitamin D Receptor Gene in Hyperparathyroid or Hypoparathyroid Dialysis Patients
 Clinical Chemistry / BSMI POLYMORPHISM OF THE VITAMIN D RECEPTOR GENE Bsml Polymorphism of the Vitamin D Receptor Gene in Hyperparathyroid or Hypoparathyroid Dialysis Patients Jacopo Tagliabue, MD,1 Marco
Clinical Chemistry / BSMI POLYMORPHISM OF THE VITAMIN D RECEPTOR GENE Bsml Polymorphism of the Vitamin D Receptor Gene in Hyperparathyroid or Hypoparathyroid Dialysis Patients Jacopo Tagliabue, MD,1 Marco
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
IRA-International Journal of Applied Sciences ISSN Vol. 03 Issue 02 (May, 2016) Paper DOI:
 IRA-International Journal of Applied Sciences ISSN 2455-4499 Vol. 03 Issue 02 (May, 2016) Paper DOI: https://dx.doi.org/10.21013/jas.v3.n2.p8 Pathophysiology of Giant Cell Formation in Giant Cell Tumor
IRA-International Journal of Applied Sciences ISSN 2455-4499 Vol. 03 Issue 02 (May, 2016) Paper DOI: https://dx.doi.org/10.21013/jas.v3.n2.p8 Pathophysiology of Giant Cell Formation in Giant Cell Tumor
Medical journals have recently. Vitamin D Defi ciency in Dialysis Patients and Its Effect on Various Disease Markers. Methods
 Patients and Its Effect on Various Disease Markers Adel B. Korkor, MD; Christine M. Bretzmann, PharmD; Daniel C. Eastwood, MS Drs. Korkor and Bretzmann are with Purity Dialysis Centers, Delafi eld, Wisconsin;
Patients and Its Effect on Various Disease Markers Adel B. Korkor, MD; Christine M. Bretzmann, PharmD; Daniel C. Eastwood, MS Drs. Korkor and Bretzmann are with Purity Dialysis Centers, Delafi eld, Wisconsin;
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
The discovery of Vitamin D and the elimination of rickets has been considered as one of Medicine s Greatest Achievements.
 The discovery of Vitamin D and the elimination of rickets has been considered as one of Medicine s Greatest Achievements. SIR EDWARD MELLANBY 1 8 8 4-1 9 5 5 A D I E T C H A R A C T E R I S T I C O F S
The discovery of Vitamin D and the elimination of rickets has been considered as one of Medicine s Greatest Achievements. SIR EDWARD MELLANBY 1 8 8 4-1 9 5 5 A D I E T C H A R A C T E R I S T I C O F S
Bone Disorders in CKD
 Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Conversion from conventional to nocturnal hemodialysis improves vitamin D levels
 http://www.kidney-international.org & 2007 International Society of Nephrology Conversion from conventional to nocturnal hemodialysis improves vitamin D levels SJ Nessim 1, SV Jassal 1, SV Fung 1 and CT
http://www.kidney-international.org & 2007 International Society of Nephrology Conversion from conventional to nocturnal hemodialysis improves vitamin D levels SJ Nessim 1, SV Jassal 1, SV Fung 1 and CT
Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis
 ORIGINAL ARTICLE Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis Masaki Ohya 1, Haruhisa Otani 2,KeigoKimura 3, Yasushi Saika 4, Ryoichi Fujii 4, Susumu
ORIGINAL ARTICLE Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis Masaki Ohya 1, Haruhisa Otani 2,KeigoKimura 3, Yasushi Saika 4, Ryoichi Fujii 4, Susumu
Dialysis: the long case
 Dialysis: the long case Prof Mark Brown St George Public Hospital, Kogarah The case SD 1. What significant things have been omitted from the history? 2. Physical findings 70 RTA; mitral regurg murmur;
Dialysis: the long case Prof Mark Brown St George Public Hospital, Kogarah The case SD 1. What significant things have been omitted from the history? 2. Physical findings 70 RTA; mitral regurg murmur;
Impact of elevated C-reactive protein levels on erythropoiesisstimulating agent (ESA) dose and responsiveness in hemodialysis patients
 NDT Advance Access published October 7, 2008 Nephrol Dial Transplant (2008) 1 of 7 doi: 10.1093/ndt/gfn543 Original Article Impact of elevated C-reactive protein levels on erythropoiesisstimulating agent
NDT Advance Access published October 7, 2008 Nephrol Dial Transplant (2008) 1 of 7 doi: 10.1093/ndt/gfn543 Original Article Impact of elevated C-reactive protein levels on erythropoiesisstimulating agent
8/22/1395 Dr. F. Moeinzadeh
 1 How I treat CKD Dr. Firouzeh Moeinzadeh Táá áàtçà ÑÜÉyxááÉÜ Éy axñ{üéäézç \áyt{tç hç äxüá àç Éy `xw vtä fv xçvxá 2 Aim of this lesson How I diagnosis a CKD patient? How I follow a CKD patient? How I
1 How I treat CKD Dr. Firouzeh Moeinzadeh Táá áàtçà ÑÜÉyxááÉÜ Éy axñ{üéäézç \áyt{tç hç äxüá àç Éy `xw vtä fv xçvxá 2 Aim of this lesson How I diagnosis a CKD patient? How I follow a CKD patient? How I
Klotho: renal and extra-renal effects
 Klotho: renal and extra-renal effects Juan F. Navarro-González, MD, PhD, FASN Nephrology Service and Research Division University Hospital Nuestra Señora de Candalaria Santa Cruz de Tenerife. Spain Klotho:
Klotho: renal and extra-renal effects Juan F. Navarro-González, MD, PhD, FASN Nephrology Service and Research Division University Hospital Nuestra Señora de Candalaria Santa Cruz de Tenerife. Spain Klotho:
