FOLLOWING the serendipitous discovery of lipid rescue
|
|
|
- Muriel Eaton
- 5 years ago
- Views:
Transcription
1 Lipid Resuscitation of Bupivacaine Toxicity Long-chain Triglyceride Emulsion Provides Benefits over Long- and Medium-chain Triglyceride Emulsion Zhengqian Li, B.S.,* Yun Xia, M.D., Ph.D., Xiaoxi Dong, M.D., Hongfei Chen, B.S.,* Fangfang Xia, B.S.,* Xianqin Wang, Ph.D., Huimin Dong, M.D.,* Zhousheng Jin, B.S.,* Xili Ding, B.S.,* Thomas J. Papadimos, M.D., M.P.H.,# Xuzhong Xu, M.D. ABSTRACT Background: The superiority of Intralipid, a long-chain triglyceride (LCT) emulsion versus Lipovenoes, a long- and medium-chain triglyceride (LCT/MCT) emulsion, in reversing local anesthetic-induced cardiac arrest is poorly defined and needs to be determined. Methods: The study included two parts: in experiment A, bupivacaine (20 mg/kg) was injected to produce asystole. Either Intralipid 20% (LCT group, n 30) or Lipovenoes 20% (LCT/MCT group, n 30) with epinephrine was infused immediately. Return of spontaneous circulation and recurrence of asystole after resuscitation were recorded. In experiment B, 80 rats using the same model and resuscitation protocol were divided into 10 groups: LCT 0, LCT 15, LCT 30, LCT 60, and LCT 120 and LCT/MCT 0, LCT/MCT 15, LCT/ MCT 30, LCT/MCT 60, and LCT/MCT 120 (n 8 each; the subscripts represent respective observation period). LCT 15 LCT 120 and LCT/MCT 15 LCT/MCT 120 groups received Intralipid 20% or Lipovenoes 20%, respectively. Plasma and myocardial bupivacaine and triglyceride concentrations, as well as myocardial bioenergetics, were determined. * Research Associate, Professor and Chairman, Department of Anesthesiology, The First Affiliated Hospital, Wenzhou Medical College, Zhejiang, China. Resident Physician, Department of Anesthesiology, The First Affiliated Hospital, Wenzhou Medical College, Zhejiang, China, and Department of Anesthesiology, Ruian People s Hospital, Zhejiang, China. Associate Professor, # Professor Clinical, Department of Anesthesiology, the Ohio State University Medical Center, Columbus, Ohio. Experimentalist, Analysis and Testing Center, Wenzhou Medical College, Zhejiang, China. Received from the Department of Anesthesiology, The First Affiliated Hospital, Wenzhou Medical College, Zhejiang, China. Submitted for publication February 15, Accepted for publication August 2, Supported by the key department foundation from The First Affiliated Hospital, Wenzhou Medical College. Address correspondence to Dr. Xu: Department of Anesthesiology, The First Affiliated Hospital of Wenzhou Medical College, 2 Fuxue Road, Wenzhou City, Zhejiang Province, China xuzhong@263.net. Information on purchasing reprints may be found at or on the masthead page at the beginning of this issue. ANESTHESIOLOGY s articles are made freely accessible to all readers, for personal use only, 6 months from the cover date of the issue. Copyright 2011, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins. What We Already Know about This Topic Intravenous lipid emulsion is an effective treatment for local anesthetic-induced cardiovascular collapse Intravenous lipid emulsions contain long-chain triglycerides and long- and medium-chain triglycerides, components which are essential to its benefits in this setting What This Article Tells Us That Is New Long-chain triglyceride emulsion in rats with local anestheticinduced cardiovascular collapse was superior to long- and medium-chain triglyceride emulsion and was associated with fewer recurrences of asystole after resuscitation and lower myocardial bupivacaine concentrations Results: In experiment A, 24 rats in LCT group and 23 in LCT/MCT group achieved return of spontaneous circulation (P 0.754); among them, 2 (8.3%) and 8 (34.8%) rats suffered a repeated asystole, respectively (P 0.027). In experiment B, plasma and myocardial bupivacaine concentrations in LCT 15 and LCT 60 groups were lower than LCT/ MCT 15 and LCT/MCT 60 groups, respectively. Furthermore, the plasma bupivacaine level in LCT/MCT 60 group was higher than LCT/MCT 30 group (P 0.003). Conclusions: LCT emulsion may be superior to LCT/MCT emulsion in treating bupivacaine-related cardiotoxicity as it was associated with fewer recurrences of asystole after resuscitation and lower myocardial bupivacaine concentrations. FOLLOWING the serendipitous discovery of lipid rescue from local anesthetic-induced cardiac arrest by Weinberg et al. 1 in 1998, a growing body of reported data has provided evidence for the efficacy of lipid rescue in both laboratory models and humans, thereby establishing intravenous lipid emulsion as an effective treatment for local anesthetic-induced cardiovascular collapse. 2 3 This article is accompanied by an Editorial View. Please see: Killoran PV, Cattano D: From bedside to bench and back: Perfecting lipid emulsion therapy for local anesthetic toxicity. ANESTHESIOLOGY 2011; 115: Anesthesiology, V 115 No December 2011 Downloaded From: on 07/23/2018
2 Lipid Reverses Bupivacaine-induced Cardiac Arrest Intravenous lipid emulsions containing long-chain triglycerides (LCTs) and long- and medium-chain triglycerides (LCTs/MCTs) are widely used in clinical scenarios. The two formulation types of commercially available lipid emulsions most commonly used are Intralipid (a 100% LCT emulsion; Huarui Pharmaceuticals Co., Ltd., Wuxi, China) and Lipovenoes (a 50:50 wt:wt mixed LCT/MCT emulsion; Huarui Pharmaceuticals Co., Ltd.). Intralipid contains 100% soybean oil 200 g/l, phosphatide 12 g/l, and glycerol 22 g/l, whereas Lipovenoes consists of a mixture of 50% soybean oil and 50% medium chain triglycerides 200 g/l, phosphatide 12 g/l, and glycerol 25 g/l. Most of the published work to date has focused on LCT emulsions, Intralipid 4 9 and Liposyn III. 10 Recently there have been several reported cases of successful resuscitation using Medialipid 20%, which contains 50/50 LCTs/ MCTs. Clear recommendations on lipid therapy have now been published by both the Association of Anesthetists of Great Britain and Ireland and American Society of Regional Anesthesia and Pain Medicine. 2 Specifically, both professional societies currently recommend administration of an initial bolus dose of 1.5 ml/kg followed by an infusion of 15 ml kg 1 h 1. If cardiovascular stability is not attained or deteriorates, rebolusing at 5-min intervals and doubling the infusion rate should be considered. Nevertheless, the recommendations do not address the choice of lipid emulsions. The exact mechanism of lipid rescue remains unclear. Currently, the most favored theoretical mechanism is the lipid sink theory, in which the lipophilic local anesthetics are bound by lipid, thus reducing tissue content of the toxin. 1 An alternative mechanism is the lipid flux theory, whereby lipid emulsions supply the mitochondria with sufficient substrate to enable energy production, which counters the impaired fatty acid delivery caused by local anesthetics. 13 Furthermore, there are reports of differences in speed of hydrolysis and oxidation, 14 the binding affinity of bupivacaine, 15 the production of ketone bodies, 16 and metabolic pathways of transport and utilization 17 between LCT and LCT/MCT emulsions. Some authors also believe that they may have different effects on bupivacaine-induced cardiotoxicity because of their different particle sizes (430 nm vs. 280 nm, respectively). 18 We hypothesize that LCT emulsions provide similar return of spontaneous circulation (ROSC), fewer recurrences of asystole after ROSC, and lower myocardial bupivacaine concentrations than did LCT/MCT emulsions. Accordingly, a double-blind prospective randomized animal study was undertaken with the primary aim of establishing the rate of mortality after ROSC following administration of LCT (Intralipid, 20%) or LCT/MCT (Lipovenoes, 20%) emulsions in an established rat model of bupivacaine cardiotoxicity, and secondarily, to determine the rate of ROSC and survival at an endpoint of 120 min. In addition, plasma and myocardial bupivacaine and triglyceride concentrations, as well as myocardial bioenergetics, were determined to account for the possible difference between them. Materials and Methods Two experiments were performed. In experiment A, the effects of two commercially available lipid emulsions of different compositions, on the recovery from bupivacaine toxicity in a cardiac rat model, were evaluated. In experiment B, plasma and cardiac tissue bupivacaine concentrations under the two lipid emulsion treatments at predetermined time levels were analyzed, as were triglyceride levels and myocardial bioenergetics. All studies were conducted with the approval of Wenzhou Medical College s Animal Care and Use Committee (Wenzhou, China). Experimental Animals Healthy male Sprague-Dawley rats, 7 to 8 weeks old, were purchased from Shanghai Slac Laboratory Animal Co., Ltd. (Shanghai, China), and housed in plastic cages (4 rats per cage) at the animal center of Wenzhou Medical College in a standard 12-h reverse day/night cycle at an ambient temperature of 26 C. The rats had an ad libitum diet of stock laboratory diet (Beijing Keao-Xieli Feedstuff Co., Ltd., Beijing, China) and tap water. They had a recovery period of 1 to 2 weeks following transportation to Wenzhou Medical College before experiments. After the animals had exhibited adequate weight gain, rats age 8 10 weeks, weighing g, were entered into subsequent studies. Experimental Model The rats were fasted for 12 h before the experiments, with free access to water. All experiments commenced at or before 9 AM. On the day of the experiment, rats were anesthetized with an intraperitoneal injection of chloral hydrate (350 mg/ kg). They were then intubated via tracheotomy and mechanically ventilated with 1% to 2% sevoflurane in 100% oxygen, using a rodent volume-controlled ventilator (HX-300, TME Technology Co., Ltd., Chengdu, China): tidal volume 8 ml/kg, respiratory rate breaths/min, inspiratory: expiratory ratio 2:3. The right internal jugular vein, the left femoral vein, and femoral artery were cannulated. Body temperature was maintained at 38 to 39 C with a heating lamp held at a safe distance. Electrocardiography, using three subcutaneous needle electrodes, and the arterial pressure were recorded continuously throughout the duration of the protocol by a MedLab data archiving and retrieval system using U/4C051 (Nanjing Medease Science and Technology Co., Ltd., Jiangsu, China). After completion of invasive procedures, all animals were then allowed to stabilize for 15 min at 0.5% sevoflurane and 100% oxygen, after which baseline heart rate, mean arterial pressure, and rate-pressure product (RPP) were recorded. Bupivacaine Arrest and Resuscitation Protocol At the end of the stabilization period, sevoflurane was discontinued and immediately thereafter 20 mg/kg bupivacaine 1220
3 PERIOPERATIVE MEDICINE hydrochloride (Sigma-Aldrich Co., St. Louis, MO) was injected as an intravenous bolus over 20 s via the venous cannula in the right femoral vein. The dose of 20 mg/kg was elected based on the work of Weinberg et al. 6 All rats developed asystole by the end of the bupivacaine infusion, and this was taken as time zero. Cardiopulmonary resuscitation with mechanical ventilation and manually performed external chest compressions (approximately 30% anterior-posterior chest diameter at 200 compressions/min) were instituted immediately upon the onset of cardiac arrest (time zero). At the same time, animals were entered in a lipid infusion protocol as determined by prior randomization, and received Intralipid 20% for the LCT group, or Lipovenoes 20% for the LCT/MCT group, as a 5 ml/kg bolus over 30 s followed by a continuous infusion of 1.0 ml kg 1 min 1 for 3 min, via the right femoral vein and the right internal jugular vein, respectively. This lipid therapy regimen was based on the work of Di Gregorio et al. 9 and Hiller et al. 19 with some modifications to optimize recovery in this model of bupivacaine overdose. Total dosing of 8 ml/kg was elected in accordance with the clinical recommendation of Weinberg A bolus of 10 g/kg epinephrine (Shanghai Harvest Pharmaceutical Co., Ltd., Shanghai, China) was then administered over the subsequent 5 s at 1-min intervals until ROSC, with a maximum cumulative dose of 100 g/kg. Chest compressions were delivered until a native RPP more than 20% of baseline value for 1 min or longer, which was our criterion for ROSC. 9 All chest compressions were stopped at the 15-min point regardless of RPP, and subjects were evaluated for sustained or nonsustained recovery until the 20-min point. Ventilation with 100% oxygen was continued throughout the 20 min of resuscitation efforts. Cardiopulmonary resuscitation was not recommenced after initial ROSC in animals subsequently developing a second period of cardiac arrest. All intravenous fluids were prepared and preheated to 37 C before infusion by personnel that did not participate in resuscitation efforts. Coordinated resuscitation efforts with clear division of roles were conducted according to the recommendation of Smith 22 with the following modifications: (1) provider one initiated specific lipid therapy and epinephrine administration, (2) provider two performed external chest compressions, and (3) provider three managed the airway and assessed native RPP during resuscitation. The two types of lipid emulsions have the same visual appearance, and all providers were blinded regarding the group. Experiment A Grouping of Animals and Setup. Sixty rats were randomly allocated by the random table method before the study into LCT group and LCT/MCT group, with 30 animals in each group. The animal experimental procedures were conducted using the aforementioned bupivacaine arrest and resuscitation protocol. LCT and LCT/MCT groups received Intralipid 20% or Lipovenoes 20%, respectively. All surviving rats in both groups were observed for 120 min. Data Acquisition. ROSC and rats surviving at 120 min were recorded. We then calculated the rate of ROSC, survival at 120 min, and mortality after resuscitation (rate of ROSC number of rats displaying ROSC/total number of rats; survival at 120 min number of rats survived at 120-min/total number of rats; mortality after resuscitation cases of repeated asystole after ROSC/cases of initial ROSC). We also continuously recorded the systolic blood pressure, mean arterial pressure, heart rate, and RPP until the termination of the observation period, at which time we calculated the RPP recovery ratio (RPP recovery ratio RPP of survival rats at specific time points/baseline RPP value). Time to first heartbeat, time to ROSC, and the cumulative dose of epinephrine were recorded. Experiment B Grouping of Animals and Setup. A second group of 80 rats were assigned to 10 groups (eight animals per group) based on differing observation time using the random table method. The groups were defined as LCT 0, LCT 15, LCT 30, LCT 60, and LCT 120 and LCT/MCT 0, LCT/MCT 15, LCT/ MCT 30, LCT/MCT 60, and LCT/MCT 120. After asystole, LCT 15 LCT 120 groups and LCT/MCT 15 LCT/MCT 120 groups received Intralipid 20% or Lipovenoes 20%, respectively. Monitoring and evaluation of hemodynamic status and airway management were conducted continuously during cardiopulmonary resuscitation and throughout respective observation period. At the end of the observation period, all the surviving animals in LCT 15 LCT 120 and LCT/ MCT 15 LCT/MCT 120 groups were killed with cervical dislocation anda4mlblood sample was immediately taken by needle aspiration of the cardiac apex. The same sampling method was used for all animals in LCT 0 and LCT/MCT 0 groups upon the onset of cardiac arrest (without lipid emulsions infusion). The blood plasma was separated by centrifugation (for 10 min at 3,000 revolutions per minute) and cardiac tissues were rinsed to remove any residual blood. Finally, all samples were then stored at 70 C until analysis was performed. Data Acquisition. ROSC and rat survival to the end of their respective observation periods were recorded. For all groups, the plasma and cardiac tissue bupivacaine concentrations were analyzed similar to previous reports 23 from this laboratory by high-performance liquid chromatography/mass spectrometry. Cardiac tissue sample preparation for triglyceride determination was conducted using the Song 24 procedure. Both plasma and tissue samples were then examined by a fully automatic Architect C 8000 Analyzer (Abbott Laboratories, Chicago, IL). Adenosine triphosphate (ATP), adenosine diphosphate (ADP), and adenosine monophosphate from heart tissue were measured by high-performance liquid chromatography. Sample preparation was conducted using the Stehr 25 procedure. Measurements were performed on an 1221
4 Lipid Reverses Bupivacaine-induced Cardiac Arrest Agilent 1100 series high-performance liquid chromatography (Agilent Technologies, Inc., Santa Clara, CA) equipped with UV-visible detection (wavelength range from 190 to 600 nm). Separations were carried out on a Hypersil ODS-2 column ( mm, 5 m; Dalian Elite Analytical Instrument Co., Ltd., Dalian, China) at 30 C. The mobile phase was a mixture of eluent A and B (ph 6.0, 99:1, v:v) at a flow rate of 1.0 ml/min. Eluent A was phosphate buffer (12 MM Na 2 HPO 4 and 88 MM NaH 2 PO 4,pH 6.0) and eluent B was a mixture of 85% eluent A and 15% acetonitrile. An injection volume of 20 l was used applying a 7725i Rheodyne manual injector (Agilent Technologies, Inc.) for both standard samples and tissue extract samples. The detection wavelength was set at 254 nm. Equally treated external standards of known concentrations were used to check retention times and to permit sample quantification based on the analysis of peak area. The adenylate energy charge was calculated according to the formula: energy charge (ATP 0.5 ADP) (ATP ADP adenosine monophosphate) 1. Statistical Analysis Power analysis was based on results of preliminary data comparing mortality after ROSC between groupings. In our preliminary study, 16 rats received lipid emulsions immediately after bupivacaine-induced asystole (n 8 for mintralipid treatment; n 8 for Lipovenoes treatment). One of seven (14.3%) animals displaying initial ROSC developed a second cardiac arrest after intralipid administration, whereas 3 of 6 (50%) survivors suffered a repeated asystole after Lipovenoes administration. Sample size calculations showed that a chi-square test with a type I error (two-sided) of 0.05 will have 88% power to detect a 35.7% difference in mortality after ROSC between the two groups, when the sample size in each group is 29. To account for potential attrition, we enrolled 30 rats per group. Considering a survival of 75% (6 of 8) at 120-min endpoint for intralipid treatment and 37.5% (3 of 8) for Lipovenoes treatment shown in the preliminary experiment, eight rats were enrolled in each group so as to avoid a small number of survivors, which may statistically lead to inaccurate results obtained from determination of myocardial bupivacaine and triglyceride levels. Data were tested for normal distribution using the Shapiro Wilk test and the Kolmogorov Smirnov test. Continuous variables were presented using means and SDs or medians and interquartile values, and in the case of categorical variables, frequencies were used. In experiment A, values for baseline parameters, times to ROSC, and times to first heartbeat were compared by Student t test, and the cumulative epinephrine dose was analyzed using the Wilcoxon and Mann Whitney U test. Dichotomous outcomes were analyzed with Fisher exact test. Continuous hemodynamic variables in animals surviving at 120 min were compared across time by two-way repeated measures ANOVA, with Bonferroni correction posttesting when significance was achieved (P 0.05). Time-to-event data were studied with Kaplan Meier analysis and compared using the log-rank test. In experiment B, baseline parameters were analyzed by one-way ANOVA. The comparison of bupivacaine, triglyceride, and adenine-nucleotides between groups with the same observation time was evaluated by Student t test. As primary outcome variables, bupivacaine among the same emulsiontreated groups was compared using an initial Kruskal Wallis H-test. If significance was achieved for differences, subanalysis according to the Bonferroni correction was applied. All statistical analysis was performed with SPSS for Windows Table 1. Baseline Values of Weight and Haemodynamic Metrics for LCT and LCT/MCT Groups in Experiment A and for LCT and LCT/MCT Groups in Experiment B Experiment Group n Weight (g) MAP (mmhg) Heart Rate (Beat/Min) RPP (mmhg Beat/Min) Experiment A LCT ,648 LCT/MCT ,429 P value Experiment B LCT ,971 LCT ,398 LCT ,660 LCT ,006 LCT ,703 LCT/MCT ,818 LCT/MCT ,794 LCT/MCT ,652 LCT/MCT ,795 LCT/MCT ,328 P value Values are given as mean SD. Baseline values for major parameters showed no difference between LCT and LCT/MCT groups in experiment A and among 10 groups in experiment B. Subscript numbers in experiment B represent respective observation period. LCT long-chain triglyceride; MAP mean artery pressure; MCT medium-chain triglyceride; RPP rate-pressure product (systolic blood pressure heart rate). 1222
5 PERIOPERATIVE MEDICINE Table 2. Resuscitation Outcomes for LCT and LCT/MCT Groups in Experiment A Characteristics (version 14.0; SPSS, Chicago, IL). Statistical significance was considered as P Results LCT (n 30) LCT/MCT (n 30) P Value Rate of ROSC 80.0% (24) 76.7% (23) (%) Survival to 73.3% (22) 50.0% (15) min (%) Mortality after 8.3% (2) 34.8% (8) resuscitation (%) Times to ROSC (s) Times to first heartbeat (s) Epinephrine cumulative dose ( g/kg) 40 (30, 62.5) 50 (30, 92.5) Normal data are given as mean SD, whereas non-normal data are expressed as median and interquartile values. LCT long-chain triglyceride; MCT medium-chain triglyceride; ROSC return of spontaneous circulation. Experiment A Characteristics of Study Subjects. Body weight, baseline values of mean arterial blood pressure, heart rate, or RPP before intervention did not differ significantly between LCT and LCT/MCT groups (table 1). Resuscitation Outcomes. The LCT and LCT/MCT groups displayed similar ROSC (24 and 23 animals respectively, 80.0% vs. 76.7%, P 0.754). More importantly, 8 of 23 animals displaying initial ROSC in LCT/MCT group subsequently developed a second period of intractable cardiac arrest compared with only 2 of 24 in LCT group (8.3% vs. 34.8%, P 0.027). Almost all of repeated cardiac arrest occurred in the period from 10 to 45 min. Therefore, 22 animals in LCT group survived to protocol termination, compared with 15 animals in LCT/MCT group (73.3% vs. 50.0%, P 0.063). There were no significant differences between LCT and LCT/MCT groups in respect to time to ROSC (P 0.264), time to first heartbeat (P 0.086), and cumulative dose of epinephrine (P 0.529) (table 2). Death distribution and Kaplan Meier survival curves of rats that exhibited ROSC in LCT and LCT/MCT groups are presented in figure 1. The median survival time of animals displaying initial ROSC was 120 (interquartile, 0) min and 120 (interquartile, 91) min in LCT and LCT/MCT groups, respectively (chi-square test 4.643, P 0.031). Hemodynamic Measures. Hemodynamic parameters heart rate (fig. 2), systolic blood pressure (fig. 3), and RPP (fig. 4) in animals surviving to protocol termination are presented graphically. LCT emulsions produced superior conditions in terms of heart rate (F 22.69, P 0.001), systolic blood pressure (F 4.35, P 0.044), and RPP (F 17.87, P 0.001) than did LCT/MCT emulsions. The graphical disparity reported primarily occurred at the midpoint of the observation period, and the curves of both groups flatten out gradually in the later periods. LCT emulsions resulted in a more complete recovery of RPP at 15 (P 0.004), 30 (P 0.001), and 60 min (P 0.001) than did LCT/MCT emulsions. RPP recovery ratio for the min did not differ between the groups (P 0.05) (fig. 5). Experiment B Characteristics of Study Subjects. In experiment B, there were 6, 5, 6, and 6 surviving rats in LCT 15, LCT 30, LCT 60, and LCT 120 groups, respectively, and 4, 4, 4, and 5 in LCT/ MCT 15, LCT/MCT 30, LCT/MCT 60, and LCT/MCT 120 Fig. 1. Death distribution (A) and Kaplan Meier survival curves (B) of rats exhibiting return of spontaneous circulation (ROSC) in long-chain triglyceride and long- and medium-chain triglyceride groups. (A) Eight of 23 animals displaying return of spontaneous circulation in the long- and medium-chain triglyceride group died at min (75% CI: 19.9, 31.1) after the onset of initial asystole, whereas 2 of 24 in the long-chain triglyceride group died at 10 min and 27 min, respectively. (B) The median survival time of rats exhibiting return of spontaneous circulation in the long-chain triglyceride group was longer than that in the long- and medium-chain triglyceride group (chi-square test 4.643, P 0.031). LCT long-chain triglyceride; MCT medium-chain triglyceride. 1223
6 Lipid Reverses Bupivacaine-induced Cardiac Arrest Fig. 2. Heart rate versus time for rats that survived to 120 min. Long-chain triglyceride emulsions produced superior heart rate recovery (F 22.69, P 0.001) than did long- and medium-chain triglyceride emulsions. N 22 for long-chain triglyceride group and 15 for long- and medium-chain triglyceride group. Data are mean and error bars SD. LCT longchain triglyceride; MCT medium-chain triglyceride. groups, respectively. Baseline body weight and hemodynamic parameters (heart rate, mean arterial pressure, and RPP) were similar among the 10 groups (table 1). Bupivacaine Measurement. The concentrations of bupivacaine in cardiac tissue and plasma are presented graphically in figure 6. Data indicate a lower bupivacaine level in the LCT 15 group ( g/g; g/ml; cardiac tissue content, plasma concentration, respectively) than the LCT/MCT 15 group ( g/g; g/ml), and in the LCT 60 group ( g/g; g/ml) than the LCT/MCT 60 group ( g/g; g/ml). Mean SD; P 0.05 for all shown results. LCT emulsion-treated groups showed a monotonously decreased plasma bupivacaine, whereas LCT/MCT emulsion-treated Fig. 4. Rate-pressure product versus time for rats that survived to 120 min. Long-chain triglyceride emulsions produced superior rate-pressure product recovery (F 17.87, P 0.001) than did long- and medium-chain triglyceride emulsions. N 22 for long-chain triglyceride group and 15 for long- and medium-chain triglyceride group. Data are mean and error bars SD. LCT long-chain triglyceride; MCT medium-chain triglyceride; RPP rate-pressure product. groups exhibit an overall decline with an unexpected plasma concentration rebound that was g/ml in the LCT/MCT 60 group and g/ml in the LCT/ MCT 30 group, P Triglyceride Level. There was no difference in the triglyceride content of cardiac tissue between groups with the same observation time (P 0.05) (fig. 6B). No difference in plasma triglyceride levels was found between LCT 0 and LCT/MCT 0, as well as between LCT 15 and LCT/MCT 15 groups (P 0.05) (fig. 6D). There was a steady decline from the 15-min point (LCT/MCT 15 ) to the 120-min point (LCT/MCT 120 ). It was lower in the LCT/MCT 120 group as compared to the LCT 120 group (P 0.001). Myocardial Bioenergetics. No major differences in the myocardial bioenergetics between groups with the same observation time was observed, including ATP, ADP, adenosine monophosphate, and energy charge (fig. 7). Fig. 3. Systolic blood pressure versus time for rats that survived to 120 min. Long-chain triglyceride emulsions produced superior systolic blood pressure recovery (F 4.35, P 0.044) than did long- and medium-chain triglyceride emulsions. N 22 for long-chain triglyceride group and 15 for long- and medium-chain triglyceride group. Data are mean and error bars SD. LCT long-chain triglyceride; MCT medium-chain triglyceride. Fig. 5. Effects of lipid emulsions on rate-pressure product recovery ratio at 15, 30, 60, 90, and 120 min induced by 20 ml/kg intravenous bupivacaine. Asterisks represent significance of differences between long-chain triglyceride (n 22) and long- and medium-chain triglyceride (n 15) groups at 15, 30, and 60 min. ** P 0.01; *** P Data are mean and error bars SD. LCT long-chain triglyceride; MCT medium-chain triglyceride; RPP rate-pressure product. 1224
7 PERIOPERATIVE MEDICINE Fig. 6. Bupivacaine and triglyceride level of surviving rats before and after lipid emulsions rescue treatment. The cardiac tissue and plasma concentration of bupivacaine (A, C) and triglyceride (B, D) were compared between groups with the same observation time. ** P 0.01 between long-chain triglyceride 15-min group and long- and medium-chain triglyceride 15-min group; *** P between long-chain triglyceride 60-min group and long- and medium-chain triglyceride 60-min group; ## P 0.01 between long- and medium-chain triglyceride 30-min group and long- and medium-chain triglyceride 60-min group; P between long-chain triglyceride 120-min group and long- and medium-chain triglyceride 120-min group. N 8, 6, 5, 6, and 6 in long-chain triglyceride min groups and 8, 4, 4, 4, and 5 in long- and medium-chain triglyceride min groups, respectively. Data are mean and error bars SD. LCT long-chain triglyceride; MCT medium-chain triglyceride. Discussion This rodent model demonstrated that both LCT and LCT/ MCT emulsions reversed the cardiac arrest induced by the intravenous injection of 20 mg/kg bupivacaine. They produced the relatively similar rates of ROSC (P 0.754). There was, however, a significant difference in mortality after resuscitation was observed between the LCT and LCT/MCT groups (8.3% vs. 34.8%, P 0.027). With respect to survival at 120 min, it approached significance (P 0.063); we had powered the study to find a 35.7% difference (.88), but we only found a 23.3% difference. Thus, the null hypothesis regarding survival may not have been rejected (potential Type II error). In addition, the RPP recovery ratio during the period from 15 to 60 min were also much higher in LCT group. The concentrations of bupivacaine in cardiac tissue and arterial plasma were significantly lower in LCT 15 and LCT 60 groups than those in LCT/MCT 15 and LCT/ MCT 60 groups, respectively. Epinephrine is a first-line drug for treating cardiac arrest because its -agonist activity increases diastolic pressure and coronary perfusion pressure. 26 Recent work by Harvey et al. 5 demonstrated that epinephrine was necessary for return of spontaneous circulation in lipid-based resuscitation from local anesthetic-induced cardiac arrest. This finding is consistent with our previous work in the isolated rat heart model of bupivacaine toxicity, wherein lipid emulsion combined with epinephrine produced superior coronary flow and RPP value than resuscitation with lipid emulsion alone. 27 The results in experiment B indicate that both treatments resulted in a sharp decline in total myocardial bupivacaine concentration during the initial 30 min after asystole, a time period during which cardiac tissue bupivacaine content decreased by 90.4% after LCT emulsion treatment and by 93.0% after LCT/MCT emulsion treatment. Overall, the similar measurements at 0 min and 30 min suggested they may exert their curative effects in a 30-min time period. Thereafter, it was observed that the plasma bupivacaine concentration dramatically increased in the LCT/MCT 60 group relative to the LCT/MCT 30 group, whereas it exhibited an extended decline after LCT emulsion treatment, which indi- 1225
8 Lipid Reverses Bupivacaine-induced Cardiac Arrest Fig. 7. Myocardial bioenergetics measurements. (A) Adenosine triphosphate (ATP), (B) adenosine diphosphate (ADP), (C) adenosine monophosphate (AMP), and (D) energy charge (EC) [(ATP 0.5 ADP) (ATP ADP AMP) 1 ] revealed no significant differences between groups with the same observation time. N 8, 6, 5, 6, and 6 in long-chain triglyceride min groups and 8, 4, 4, 4, and 5 in long- and medium-chain triglyceride min groups, respectively. Data are mean and error bars SD. LCT long-chain triglyceride; MCT medium-chain triglyceride. cated a longer action time when LCT emulsion was compared to LCT/MCT emulsion. The half-life may have accounted for this observation: the estimated half-life was 33 min for LCTs and 17 min for MCTs, 28 for which clearing of the plasma LCT/MCT was completed earlier than LCT. 14 More studies suggest that a substantial amount of exogenous fatty acids reach both hepatic and nonhepatic tissues as intact triacylglycerol without preceding lipolysis in the plasma compartment. 29 On the basis of the lipid sink hypothesis and the profound liver-targeting property for lipid emulsions, it can be hypothesized that the redistribution and metabolism of lipid emulsion upon hemodynamic recovery may have allowed subsequent hepatic release of bupivacaine that was incorporated within the core of LCT/MCT lipid emulsion. This hypothesis may explain the distinct effects in hemodynamic parameters during the period from 15 to 60 min as well as the deaths after resuscitation concentrated in min in LCT/MCT group in experiment A. However, we did not measure the hepatic bupivacaine content, and this is a possibility for future research. In addition to the above, the high lipid solubility of local anesthetics and the difference in the high binding capacity of the lipid emulsions explained their distinct efficacy. Mazoit et al., 15 using the shake-flask method in vitro to measure the extent of emulsification of lipophilic local anesthetics, found that the extent of local anesthetic binding to Intralipid 20% was roughly 2.5 times more than Medialipide 20% (B-Braun, Boulogne, France). This indicated that LCT emulsions were more efficient than LCT/MCT emulsions in binding to long-acting local anesthetics. Compared with the LCT/MCT 15 group, the lower cardiac tissue bupivacaine content in the LCT 15 group may chiefly result from the better capacity of LCT lipid emulsion to bind bupivacaine and an ensuing livertargeting transport of lipid-soluble bupivacaine. The Lipovenoes in our protocol is similar to the Medialipid used by Mazoit et al., as both of them are lipid emulsions containing equal proportions of LCTs and MCTs (although made by different manufacturers). Under normal aerobic conditions, fatty acids are the preferred substrate for cardiomyocyte, generating about 80 90% of ATP. 32 Lipid emulsions could theoretically increase intracellular fatty acid content, by impeding a local anesthetic s inhibition of acylcarnitine and ATP synthesis 7,13 in the cardiomyocyte, thereby improving ATP production cardiac function. Carnitine is needed to transport long-chain fatty 1226
9 PERIOPERATIVE MEDICINE acids into the mitochondria. 33 Conversely, medium-chain fatty acids can enter the mitochondria by simple diffusion independent of the carnitine enzyme system. 34 Thus, specificity for rapid oxidation, without deposition in fat stores, 14 carnitine-independent transport to the site of oxidation, and the ability to supply energy with higher ketone bodies make MCTs theoretically a preferable choice from an energyrelated perspective. Unfortunately, the theoretical benefits of LCT/MCT lipid emulsions are not borne out in practice. No difference in ATP, ADP, adenosine monophosphate, and energy charge throughout the duration of the protocol was observed in experiment B, which was similar with that of Stehr s research data from an isolated rat heart model. 25 Our investigation has several limitations. First, our small animal model necessitated that each animal in experiment B had to be sacrificed at its assigned sampling time point. Thus, repeated measures for each animal were not possible. Nonetheless, we stringently controlled the animal profiles including the animal source, strain, sex, age, body weight, housing condition, and experimental environment to reduce the error as much as possible. Second, the dosing protocols of key study drugs (lipid emulsions, epinephrine) that we used may not be the optimal. However, the regimen we used was found in preliminary experiments used to optimize recovery in this model of bupivacaine intoxication. The effective reversal of cardiovascular symptoms and our highly successful resuscitation suggest validation of our model. A third limitation regards the power of our study. While we were powered to find a 35.7% difference, we, nonetheless, still present a solid basis for further experimentation and discussion, especially in light of the fact that our work supports Weinberg s 6,7,9,19 and confirms his studies. In conclusion, LCT emulsion may be the choice of lipid resuscitation from bupivacaine toxicity as it provided less mortality after resuscitation, lower myocardial bupivacaine concentrations, and superior hemodynamic recovery than did LCT/MCT emulsion in an intact rat model of bupivacaine-induced cardiovascular collapse, which we would attribute to the differences of lipid sink effect, rather than to the lipid flux theory. LCT emulsion s superiorities showed in the present study may further strengthen the guidelines for the management of severe local anesthetic toxicity with lipid emulsion. Further research may be warranted regarding the comparison of LCT and LCT/MCT emulsions in another humanized animal model, although it is unlikely that LCT/ MCT emulsions will show any benefit over LCT emulsions. The authors thank Lianbo Yu, Ph.D., Biostatistical Scientist, Center for Biostatistics, Columbus, Ohio, and Hongying Shi, Ph.D., Assistant Professor, Department of Preventive Medicine, Wenzhou Medical College, Wenzhou, Zhejiang, China, for analyzing the data. References 1. Weinberg GL, VadeBoncouer T, Ramaraju GA, Garcia-Amaro MF, Cwik MJ: Pretreatment or resuscitation with a lipid infusion shifts the dose-response to bupivacaine-induced asystole in rats. ANESTHESIOLOGY 1998; 88: Neal JM, Bernards CM, Butterworth JF 4th, Di Gregorio G, Drasner K, Hejtmanek MR, Mulroy MF, Rosenquist RW, Weinberg GL: ASRA practice advisory on local anesthetic systemic toxicity. Reg Anesth Pain Med 2010; 35: Rothschild L, Bern S, Oswald S, Weinberg G: Intravenous lipid emulsion in clinical toxicology. Scand J Trauma Resusc Emerg Med 2010; 18:51 4. Rosenblatt MA, Abel M, Fischer GW, Itzkovich CJ, Eisenkraft JB: Successful use of a 20% lipid emulsion to resuscitate a patient after a presumed bupivacaine-related cardiac arrest. ANESTHESIOLOGY 2006; 105: Harvey M, Cave G, Prince G, Lahner D: Epinephrine injection in lipid-based resuscitation from bupivacaine-induced cardiac arrest: Transient circulatory return in rabbits. Anesth Analg 2010; 111: Weinberg GL, Di Gregorio G, Ripper R, Kelly K, Massad M, Edelman L, Schwartz D, Shah N, Zheng S, Feinstein DL: Resuscitation with lipid versus epinephrine in a rat model of bupivacaine overdose. ANESTHESIOLOGY 2008; 108: Weinberg GL, Ripper R, Murphy P, Edelman LB, Hoffman W, Strichartz G, Feinstein DL: Lipid infusion accelerates removal of bupivacaine and recovery from bupivacaine toxicity in the isolated rat heart. Reg Anesth Pain Med 2006; 31: Cave G, Harvey M, Prince G, Lahner D, Desmet J: Effect of hypertonic saline on electrocardiography QRS duration in rabbit model of bupivacaine toxicity resuscitated by intravenous lipid. Anaesthesia 2010; 65: Di Gregorio G, Schwartz D, Ripper R, Kelly K, Feinstein DL, Minshall RD, Massad M, Ori C, Weinberg GL: Lipid emulsion is superior to vasopressin in a rodent model of resuscitation from toxin-induced cardiac arrest. Crit Care Med 2009; 37: Warren JA, Thoma RB, Georgescu A, Shah SJ: Intravenous lipid infusion in the successful resuscitation of local anesthetic-induced cardiovascular collapse after supraclavicular brachial plexus block. Anesth Analg 2008; 106: Ludot H, Tharin JY, Belouadah M, Mazoit JX, Malinovsky JM: Successful resuscitation after ropivacaine and lidocaine-induced ventricular arrhythmia following posterior lumbar plexus block in a child. Anesth Analg 2008; 106: Charbonneau H, Marcou TA, Mazoit JX, Zetlaoui PJ, Benhamou D: Early use of lipid emulsion to treat incipient mepivacaine intoxication. Reg Anesth Pain Med 2009; 34: Weinberg GL, Palmer JW, VadeBoncouer TR, Zuechner MB, Edelman G, Hoppel CL: Bupivacaine inhibits acylcarnitine exchange in cardiac mitochondria. ANESTHESIOLOGY 2000; 92: Johnson RC, Young SK, Cotter R, Lin L, Rowe WB: Mediumchain-triglyceride lipid emulsion: Metabolism and tissue distribution. Am J Clin Nutr 1990; 52: Mazoit JX, Le Guen R, Beloeil H, Benhamou D: Binding of longlasting local anesthetics to lipid emulsions. ANESTHESIOLOGY 2009; 110: Dennison AR, Ball M, Crowe PJ, White K, Hands L, Watkins RM, Kettlewell M: The metabolic consequences of infusing emulsions containing medium chain triglycerides for parenteral nutrition: A comparative study with conventional lipid. Ann R Coll Surg Engl 1986; 68: Cotter R, Johnson RC, Young SK, Lin LI, Rowe WB: Competitive effects of long-chain-triglyceride emulsion on the metabolism of medium-chain-triglyceride emulsions. Am J Clin Nutr 1989; 50: Candela D, Louart G, Bousquet PJ, Muller L, Nguyen M, Boyer JC, Peray PA, Goret L, Ripart J, Lefrant JY, de La Coussaye JE: Reversal of bupivacaine-induced cardiac electrophysiologic changes by two lipid emulsions in anesthetized and mechanically ventilated piglets. Anesth Analg 2010; 110: Hiller DB, Gregorio GD, Ripper R, Kelly K, Massad M, Edelman L, Edelman G, Feinstein DL, Weinberg GL: Epinephrine 1227
10 Lipid Reverses Bupivacaine-induced Cardiac Arrest impairs lipid resuscitation from bupivacaine overdose: A threshold effect. ANESTHESIOLOGY 2009; 111: Weinberg GL: Reply to Drs. Goor, Groban and Butterworth Lipid rescue: Caveats and recommendations for the silverbullet (letter). Reg Anesth Pain Med 2004; 29: Weinberg G, Hertz P, Newman J: Lipid, not propofol, treats bupivacaine overdose. Anesth Analg 2004; 99: Smith HM, Jacob AK, Segura LG, Dilger JA, Torsher LC: Simulation education in anesthesia training: A case report of successful resuscitation of bupivacaine-induced cardiac arrest linked to recent simulation training. Anesth Analg 2008; 106: Chen Y, Xia Y, Liu L, Shi T, Shi K, Wang Q, Chen L, Papadimos TJ, Xu X: Lipid emulsion reverses bupivacaineinduced asystole in isolated rat hearts: Concentration-response and time-response relationships. ANESTHESIOLOGY 2010; 113: Song Z, Deaciuc I, Song M, Lee DY, Liu Y, Ji X, McClain C: Silymarin protects against acute ethanol-induced hepatotoxicity in mice. Alcohol Clin Exp Res 2006; 30: Stehr SN, Ziegeler JC, Pexa A, Oertel R, Deussen A, Koch T, Hübler M: The effects of lipid infusion on myocardial function and bioenergetics in l-bupivacaine toxicity in the isolated rat heart. Anesth Analg 2007; 104: Ali B, Zafari AM: Narrative review: Cardiopulmonary resuscitation and emergency cardiovascular care: review of the current guidelines. Ann Intern Med 2007; 147: Liu L, Xia Y, Chen Y, Wang Q, Shi T, Wang F, Small RH, Xu X: The comparative effects of lipid, epinephrine, and their combination in the reversal of bupivacaine-induced asystole in the isolated rat heart. Anesth Analg 2011 [Epub ahead of print] 28. Sailer D, Müller M: Medium chain triglycerides in parenteral nutrition. JPEN J Parenter Enteral Nutr 1981; 5: Calder PC, Deckelbaum RJ: New metabolic pathways and roles for lipids and lipid emulsions. Curr Opin Clin Nutr Metab Care 1998; 1: Qi K, Seo T, Jiang Z, Carpentier YA, Deckelbaum RJ: Triglycerides in fish oil affect the blood clearance of lipid emulsions containing long- and medium-chain triglycerides in mice. J Nutr 2006; 136: Jang JH, Kim CK, Choi HG, Sung JH: Preparation and evaluation of 2-(allylthio)pyrazine-loaded lipid emulsion with enhanced stability and liver targeting. Drug Dev Ind Pharm 2009; 35: Collins-Nakai RL, Noseworthy D, Lopaschuk GD: Epinephrine increases ATP production in hearts by preferentially increasing glucose metabolism. Am J Physiol 1994; 267: H Mitchell ME: Carnitine metabolism in human subjects. I. Normal metabolism. Am J Clin Nutr 1978; 31: Koletzko B, Goulet O, Hunt J, Krohn K, Shamir R: 1. Guidelines on Paediatric Parenteral Nutrition of the European Society of Paediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) and the European Society for Clinical Nutrition and Metabolism (ESPEN), Supported by the European Society of Paediatric Research (ESPR). J Pediatr Gastroenterol Nutr 2005; 41 Suppl 2:S
Lipid Rescue: An Effective Therapy for Bupivacaine Cardiotoxicity and its Application Beyond Cardiotoxicity and Beyond Local Anesthetics
 Lipid Rescue: An Effective Therapy for Bupivacaine Cardiotoxicity and its Application Beyond Cardiotoxicity and Beyond Local Anesthetics Kenneth Drasner, M.D. Professor of Clinical Anesthesia University
Lipid Rescue: An Effective Therapy for Bupivacaine Cardiotoxicity and its Application Beyond Cardiotoxicity and Beyond Local Anesthetics Kenneth Drasner, M.D. Professor of Clinical Anesthesia University
Measurement of the efficacy of 2% lipid in reversing bupivacaine- induced asystole in isolated rat hearts
 Chen et al. BMC Anesthesiology 2014, 14:60 RESEARCH ARTICLE Open Access Measurement of the efficacy of 2% lipid in reversing bupivacaine- induced asystole in isolated rat hearts Hongfei Chen 1, Yun Xia
Chen et al. BMC Anesthesiology 2014, 14:60 RESEARCH ARTICLE Open Access Measurement of the efficacy of 2% lipid in reversing bupivacaine- induced asystole in isolated rat hearts Hongfei Chen 1, Yun Xia
Prevention and Treatment Patrick Levelle, MD
 Prevention and Treatment Patrick Levelle, MD LOCAL ANESTHETIC TOXICITY 1. PERIPHERAL NERVE BLOCKS 2. ROLE OF THE PERIANESTHESIA RN 3. LOCAL ANESTHETIC TOXICITY Use of Lipid Emulsion Regional and Peripheral
Prevention and Treatment Patrick Levelle, MD LOCAL ANESTHETIC TOXICITY 1. PERIPHERAL NERVE BLOCKS 2. ROLE OF THE PERIANESTHESIA RN 3. LOCAL ANESTHETIC TOXICITY Use of Lipid Emulsion Regional and Peripheral
The Effects of Lidocaine on Bupivacaine-Induced Cardiotoxicity in the Isolated Rat Heart
 Physiol. Res. 59 (Suppl. 1): S65-S69, 2010 The Effects of Lidocaine on Bupivacaine-Induced Cardiotoxicity in the Isolated Rat Heart I. KŘIKAVA 1, J. JARKOVSKÝ 3, P. ŠTOURAČ 1, M. NOVÁKOVÁ 2, P. ŠEVČÍK
Physiol. Res. 59 (Suppl. 1): S65-S69, 2010 The Effects of Lidocaine on Bupivacaine-Induced Cardiotoxicity in the Isolated Rat Heart I. KŘIKAVA 1, J. JARKOVSKÝ 3, P. ŠTOURAČ 1, M. NOVÁKOVÁ 2, P. ŠEVČÍK
Local Anaesthetic Systemic Toxicity (LAST)
 Local Anaesthetic Systemic Toxicity (LAST) Part II Course, June 2012 Dr Michael Barrington St Vincent s Hospital, Melbourne History LAST quickly became noted as a serious complication after introduction
Local Anaesthetic Systemic Toxicity (LAST) Part II Course, June 2012 Dr Michael Barrington St Vincent s Hospital, Melbourne History LAST quickly became noted as a serious complication after introduction
Regional Anaesthesia for Children
 Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration
 Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration Investigators: Salvatore Cutuli, Eduardo Osawa, Rinaldo Bellomo Affiliations: 1. Department
Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration Investigators: Salvatore Cutuli, Eduardo Osawa, Rinaldo Bellomo Affiliations: 1. Department
LIPID: Will the Traditional Antidote Replace
 LIPID: Will the Traditional Antidote Replace Evvah Karakılıç MD, PhD. Ankara Numune Education and Research Hospital Department of Emergency Medicine Intravenous lipid emulsions Routinely used for nutritional
LIPID: Will the Traditional Antidote Replace Evvah Karakılıç MD, PhD. Ankara Numune Education and Research Hospital Department of Emergency Medicine Intravenous lipid emulsions Routinely used for nutritional
Erik S. Litonius, MD,* Tomohisa Niiya, MD, PhD,* Pertti J. Neuvonen, MD, PhD, and Per H. Rosenberg, MD, PhD*
 Intravenous Lipid Emulsion Only Minimally Influences Bupivacaine and Mepivacaine Distribution in Plasma and Does Not Enhance Recovery from Intoxication in Pigs Erik S. Litonius, MD,* Tomohisa Niiya, MD,
Intravenous Lipid Emulsion Only Minimally Influences Bupivacaine and Mepivacaine Distribution in Plasma and Does Not Enhance Recovery from Intoxication in Pigs Erik S. Litonius, MD,* Tomohisa Niiya, MD,
Intravenous Lipid Emulsion for Local Anesthetic Toxicity: A Review of the Literature
 Toxicology Reviews Intravenous Lipid Emulsion for Local Anesthetic Toxicity: A Review of the Literature Kristen L. Felice, PharmD, Heather M. Schumann, PharmD University of Illinois at Chicago College
Toxicology Reviews Intravenous Lipid Emulsion for Local Anesthetic Toxicity: A Review of the Literature Kristen L. Felice, PharmD, Heather M. Schumann, PharmD University of Illinois at Chicago College
Hemodynamic changes with high infusion rates of lipid emulsion. Experimental study in swine 1
 1 - ORIGINAL ARTICLE MODELS, BIOLOGICAL Hemodynamic changes with high infusion rates of lipid emulsion. Experimental study in swine 1 Artur Udelsmann I, Marcos De Simone Melo II DOI: http://dx.doi.org/10.1590/s0102-865020150110000001
1 - ORIGINAL ARTICLE MODELS, BIOLOGICAL Hemodynamic changes with high infusion rates of lipid emulsion. Experimental study in swine 1 Artur Udelsmann I, Marcos De Simone Melo II DOI: http://dx.doi.org/10.1590/s0102-865020150110000001
Do surgical trainees know how to administer local anaesthetic and deal with toxicity?
 Do surgical trainees know how to administer local anaesthetic and deal with toxicity? How junior surgeons measure up against their anaesthetic counterparts. N Blucher Core Surgical Trainee 1 D Pefanis
Do surgical trainees know how to administer local anaesthetic and deal with toxicity? How junior surgeons measure up against their anaesthetic counterparts. N Blucher Core Surgical Trainee 1 D Pefanis
Treatment of Local Anesthetic Cardiac Toxicity. AAQ Montreal 16 Avril 2013 Guy Weinberg, MD Chicago, IL
 Treatment of Local Anesthetic Cardiac Toxicity AAQ Montreal 16 Avril 2013 Guy Weinberg, MD Chicago, IL Topics for Today LAST LIPID FUTURE CHALLENGES Classic Treatments for LAST Have Miserable Outcomes
Treatment of Local Anesthetic Cardiac Toxicity AAQ Montreal 16 Avril 2013 Guy Weinberg, MD Chicago, IL Topics for Today LAST LIPID FUTURE CHALLENGES Classic Treatments for LAST Have Miserable Outcomes
The Structure of Bupivacaine and How it Relates to Cardiotoxicity and Lipid Rescue. By: Sean Zajdel SRNA
 The Structure of Bupivacaine and How it Relates to Cardiotoxicity and Lipid Rescue By: Sean Zajdel SRNA The basic action of an anesthetic in the body is largely a function of the drug s chemical structure
The Structure of Bupivacaine and How it Relates to Cardiotoxicity and Lipid Rescue By: Sean Zajdel SRNA The basic action of an anesthetic in the body is largely a function of the drug s chemical structure
INTRAVENOUS LIDOCAINE INFUSIONS AND INTRALIPID RESCUE
 INTRAVENOUS LIDOCAINE INFUSIONS AND INTRALIPID RESCUE Acute Pain Service-LHSC VH and UH sites HISTORY Lidocaine and procaine used by IV infusion in the 1950s and 1960s for general analgesia Often continued
INTRAVENOUS LIDOCAINE INFUSIONS AND INTRALIPID RESCUE Acute Pain Service-LHSC VH and UH sites HISTORY Lidocaine and procaine used by IV infusion in the 1950s and 1960s for general analgesia Often continued
Update in Poison Management. Update in Poison Management. Antidote Use. Fomepizole. Pediatric Ingestions 1. No financial disclosures
 Update in Poison Management No financial disclosures Robert J. Hoffman, MD,MS FACMT, FACEP, FAAEM, FAAP Department of Emergency Medicine Albert Einstein College of Medicine New York, New York Update in
Update in Poison Management No financial disclosures Robert J. Hoffman, MD,MS FACMT, FACEP, FAAEM, FAAP Department of Emergency Medicine Albert Einstein College of Medicine New York, New York Update in
Lipid rescue: the use of lipid emulsions to treat local anaesthetic toxicity
 Lipid rescue: the use of lipid emulsions to treat local anaesthetic toxicity Kruger CJ, MBChB Marwick PC, MBChB Levin AI, MBChB, DA, MMed, PhD, FCA Department of Anaesthesiology and Critical Care, Stellenbosch
Lipid rescue: the use of lipid emulsions to treat local anaesthetic toxicity Kruger CJ, MBChB Marwick PC, MBChB Levin AI, MBChB, DA, MMed, PhD, FCA Department of Anaesthesiology and Critical Care, Stellenbosch
Effects of Amiodarone in a Swine Model of Nortryptiline Toxicity
 Toxicology Investigations Effects of Amiodarone in a Swine Model of Nortryptiline Toxicity Fermin Barrueto, Jr., MD a, Indira Murr, MD b, Andrew Meltzer, MD a, Kori Brewer, PhD b, and William Meggs, MD,
Toxicology Investigations Effects of Amiodarone in a Swine Model of Nortryptiline Toxicity Fermin Barrueto, Jr., MD a, Indira Murr, MD b, Andrew Meltzer, MD a, Kori Brewer, PhD b, and William Meggs, MD,
Sign up to receive ATOTW weekly
 PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
Epinephrine Impairs Lipid Resuscitation from Bupivacaine Overdose
 Anesthesiology 2009; 111:498 505 Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Epinephrine Impairs Lipid Resuscitation from Bupivacaine Overdose A
Anesthesiology 2009; 111:498 505 Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Epinephrine Impairs Lipid Resuscitation from Bupivacaine Overdose A
CHEWING THE FAT Intravenous Lipid Emulsions Non nutritive uses
 09 September 2016 No. 21 CHEWING THE FAT Intravenous Lipid Emulsions Non nutritive uses J Carim Moderator: P Govender School of Clinical Medicine Discipline of Anaesthesiology and Critical Care CONTENT
09 September 2016 No. 21 CHEWING THE FAT Intravenous Lipid Emulsions Non nutritive uses J Carim Moderator: P Govender School of Clinical Medicine Discipline of Anaesthesiology and Critical Care CONTENT
Biphasic Clinical Summaries
 Biphasic Clinical Summaries Defibrillation of Ventricular Fibrillation and Ventricular Tachycardia Background Physio-Control conducted a multi-centered, prospective, randomized and blinded clinical trial
Biphasic Clinical Summaries Defibrillation of Ventricular Fibrillation and Ventricular Tachycardia Background Physio-Control conducted a multi-centered, prospective, randomized and blinded clinical trial
Local anesthetic systemic toxicity (LAST) is a rare
 Intravenous Fat Emulsion for Treatment of Local Anesthetic Systemic Toxicity: Best Practice and Review of the Literature Ana M. Nedialkov, DNP, CRNA, ARNP Tony Umadhay, PhD, CRNA Jorge A. Valdes, DNP,
Intravenous Fat Emulsion for Treatment of Local Anesthetic Systemic Toxicity: Best Practice and Review of the Literature Ana M. Nedialkov, DNP, CRNA, ARNP Tony Umadhay, PhD, CRNA Jorge A. Valdes, DNP,
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
1 Recognition. 2 Immediate management. 3 Treatment. 4 Follow-up. AAGBI Safety Guideline. Management of Severe Local Anaesthetic Toxicity
 AAGBI Safety Guideline Management of Severe Local Anaesthetic Toxicity 1 Recognition 2 Immediate management 3 Treatment Signs of severe toxicity: Sudden alteration in mental status, severe agitation or
AAGBI Safety Guideline Management of Severe Local Anaesthetic Toxicity 1 Recognition 2 Immediate management 3 Treatment Signs of severe toxicity: Sudden alteration in mental status, severe agitation or
Citation Acta medica Nagasakiensia. 1984, 29
 NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
Levosimendan is superior to epinephrine on coronary flow for lipid-base resuscitation of bupivacaine-induced asystole in the isolated rat heart
 Chen et al. BMC Anesthesiology (2018) 18:174 https://doi.org/10.1186/s12871-018-0627-0 RESEARCH ARTICLE Open Access Levosimendan is superior to epinephrine on coronary flow for lipid-base resuscitation
Chen et al. BMC Anesthesiology (2018) 18:174 https://doi.org/10.1186/s12871-018-0627-0 RESEARCH ARTICLE Open Access Levosimendan is superior to epinephrine on coronary flow for lipid-base resuscitation
Local Anesthetic Toxicity: Optimal Management to Avoid Neurotoxic Injury and Treat Cardiac Arrest
 Page 1 Local Anesthetic Toxicity: Optimal Management to Avoid Neurotoxic Injury and Treat Cardiac Arrest Kenneth Drasner, M.D. San Francisco, California Continued reports of major and minor neurologic
Page 1 Local Anesthetic Toxicity: Optimal Management to Avoid Neurotoxic Injury and Treat Cardiac Arrest Kenneth Drasner, M.D. San Francisco, California Continued reports of major and minor neurologic
RESEARCH IN BASIC SCIENCE
 RESEARCH IN BASIC SCIENCE Effect of High-Dose Sodium Bicarbonate on the Vasopressor Effects of Epinephrine During Cardiopulmonary Resuscitation Barry E. Bleske, Pharm.D., Eric W Warren, Pharm.D., Ted L.
RESEARCH IN BASIC SCIENCE Effect of High-Dose Sodium Bicarbonate on the Vasopressor Effects of Epinephrine During Cardiopulmonary Resuscitation Barry E. Bleske, Pharm.D., Eric W Warren, Pharm.D., Ted L.
Improved regional anesthesia techniques and less
 Local Anesthetic-Induced Cardiac Toxicity: A Survey of Contemporary Practice Strategies Among Academic Anesthesiology Departments William Corcoran, MD* John Butterworth, MD Robert S. Weller, MD* Jonathan
Local Anesthetic-Induced Cardiac Toxicity: A Survey of Contemporary Practice Strategies Among Academic Anesthesiology Departments William Corcoran, MD* John Butterworth, MD Robert S. Weller, MD* Jonathan
Bryan D. Hayes, PharmD, FAACT University of
 Session Title: Pearls for the Critically Ill Poisoned Patient Bryan D. Hayes, PharmD, FAACT Session overview Managing the critically ill poisoned patient is challenging, particularly toxin-induced shock.
Session Title: Pearls for the Critically Ill Poisoned Patient Bryan D. Hayes, PharmD, FAACT Session overview Managing the critically ill poisoned patient is challenging, particularly toxin-induced shock.
LA SYSTEMIC TOXICITY(LAST) AND INTRAVENOUS LIPID EMULSION (ILE) (IN COLLABORATION WITH MALAYSIAN SIGRA)
 LA SYSTEMIC TOXICITY(LAST) AND INTRAVENOUS LIPID EMULSION (ILE) (IN COLLABORATION WITH MALAYSIAN SIGRA) DR LING KWONG UNG, ANAESTHETIST, RAMSAY-SIME DARBY MEDICAL CENTRE, ARA DAMANSARA, MALAYSIA. lingkupisces@yahoo.com
LA SYSTEMIC TOXICITY(LAST) AND INTRAVENOUS LIPID EMULSION (ILE) (IN COLLABORATION WITH MALAYSIAN SIGRA) DR LING KWONG UNG, ANAESTHETIST, RAMSAY-SIME DARBY MEDICAL CENTRE, ARA DAMANSARA, MALAYSIA. lingkupisces@yahoo.com
Case Report ECMO for Cardiac Rescue after Accidental Intravenous Mepivacaine Application
 Hindawi Publishing Corporation Case Reports in Pediatrics Volume 2012, Article ID 491692, 5 pages doi:10.1155/2012/491692 Case Report ECMO for Cardiac Rescue after Accidental Intravenous Mepivacaine Application
Hindawi Publishing Corporation Case Reports in Pediatrics Volume 2012, Article ID 491692, 5 pages doi:10.1155/2012/491692 Case Report ECMO for Cardiac Rescue after Accidental Intravenous Mepivacaine Application
Efficacy of the Valsalva Maneuver on Needle Projection Pain and Hemodynamic Responses During Spinal Puncture
 156 Research Paper International Journal of Medical Sciences 2011; 8(2):156-160 Ivyspring International Publisher. All rights reserved. Efficacy of the Valsalva Maneuver on Needle Projection Pain and Hemodynamic
156 Research Paper International Journal of Medical Sciences 2011; 8(2):156-160 Ivyspring International Publisher. All rights reserved. Efficacy of the Valsalva Maneuver on Needle Projection Pain and Hemodynamic
 C CONFERENCIAS MAGISTRALES Vol. 36. Supl. 1 Abril-Junio 213 pp S81-S94 Lipid Rescue From Bench to Bedside Meg A Rosenblatt, MD* * Professor of Anesthesiology and Orthopaedics. Icahn School of Medicine
C CONFERENCIAS MAGISTRALES Vol. 36. Supl. 1 Abril-Junio 213 pp S81-S94 Lipid Rescue From Bench to Bedside Meg A Rosenblatt, MD* * Professor of Anesthesiology and Orthopaedics. Icahn School of Medicine
DEVICE DURING STANDARD ACTIVE DECOMPRESSION
 USE OF AN IMPEDANCE THRESHOLD DEVICE DURING STANDARD AND/OR ACTIVE COMPRESSION DECOMPRESSION ITD Bibliography 1. Aufderheide TP, Pirrallo RG, et al. Clinical evaluation of an inspiratory impedance threshold
USE OF AN IMPEDANCE THRESHOLD DEVICE DURING STANDARD AND/OR ACTIVE COMPRESSION DECOMPRESSION ITD Bibliography 1. Aufderheide TP, Pirrallo RG, et al. Clinical evaluation of an inspiratory impedance threshold
MORE HEARTBEAT THAN A. Enhanced CPR. Better neurologic outcomes. Steve Dunn, Ph.D., Professor, University of Wisconsin Oshkosh
 MORE THAN A HEARTBEAT Enhanced CPR. Better neurologic outcomes. Steve Dunn, Ph.D., Professor, University of Wisconsin Oshkosh Thanks to the ResQPOD and a dedicated EMS team, Steve survived sudden cardiac
MORE THAN A HEARTBEAT Enhanced CPR. Better neurologic outcomes. Steve Dunn, Ph.D., Professor, University of Wisconsin Oshkosh Thanks to the ResQPOD and a dedicated EMS team, Steve survived sudden cardiac
WITH ISOBARIC BUPIVACAINE (5 MG/ML)
 , 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
, 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
TRANSPARENCY COMMITTEE OPINION. 19 March Date of the Marketing Authorisation (national procedure): 18 December 1997
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 19 March 2008 INTRALIPIDE 20 PER CENT, emulsion for infusion 100 ml in Excel container (PE/PP) (CIP: 355 096-5) 250
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 19 March 2008 INTRALIPIDE 20 PER CENT, emulsion for infusion 100 ml in Excel container (PE/PP) (CIP: 355 096-5) 250
WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR
 RECOVER 2011 1 of 7 WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR 1. Basic Demographics Worksheet author(s) Ann Peruski Date Submitted for review: 18 Apr 2011 Mailing address: 6995
RECOVER 2011 1 of 7 WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR 1. Basic Demographics Worksheet author(s) Ann Peruski Date Submitted for review: 18 Apr 2011 Mailing address: 6995
2015 AHA Guidelines: Pediatric Updates
 2015 AHA Guidelines: Pediatric Updates Advances in Pediatric Emergency Medicine December 9, 2016 Karen O Connell, MD, MEd Associate Professor of Pediatrics and Emergency Medicine Emergency Medicine and
2015 AHA Guidelines: Pediatric Updates Advances in Pediatric Emergency Medicine December 9, 2016 Karen O Connell, MD, MEd Associate Professor of Pediatrics and Emergency Medicine Emergency Medicine and
Lipid Rescue Resuscitation from Local Anaesthetic Cardiac Toxicity
 Toxicol Rev 2006; 25 (3): 139-145 REVIEW ARTICLE 1176-2551/06/0003-0139/$39.95/0 2006 Adis Data Information BV. All rights reserved. Lipid Rescue Resuscitation from Local Anaesthetic Cardiac Toxicity Guy
Toxicol Rev 2006; 25 (3): 139-145 REVIEW ARTICLE 1176-2551/06/0003-0139/$39.95/0 2006 Adis Data Information BV. All rights reserved. Lipid Rescue Resuscitation from Local Anaesthetic Cardiac Toxicity Guy
But unfortunately, the first sign of cardiovascular disease is often the last. Chest-Compression-Only Resuscitation Gordon A.
 THE UNIVERSITY OF ARIZONA Sarver Heart Center 1 THE UNIVERSITY OF ARIZONA Sarver Heart Center 2 But unfortunately, the first sign of cardiovascular disease is often the last 3 4 1 5 6 7 8 2 Risk of Cardiac
THE UNIVERSITY OF ARIZONA Sarver Heart Center 1 THE UNIVERSITY OF ARIZONA Sarver Heart Center 2 But unfortunately, the first sign of cardiovascular disease is often the last 3 4 1 5 6 7 8 2 Risk of Cardiac
16. Exercise Energetics
 16. Exercise The performance of muscular exercise not only throws a strain on the musculoskeletal system itself but it also tests the reserves of virtually every system in the body. Exercising muscles
16. Exercise The performance of muscular exercise not only throws a strain on the musculoskeletal system itself but it also tests the reserves of virtually every system in the body. Exercising muscles
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Advanced Resuscitation - Child
 C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
A dose-response curve for the negative bias pressure of an intrathoracic pressure regulator during CPR
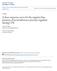 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 10-2005 A dose-response curve for the negative bias pressure of an intrathoracic
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 10-2005 A dose-response curve for the negative bias pressure of an intrathoracic
Rintaro Hoshino 1, Yoshinori Kamiya 1,2*, Yuka Fujii 3,4 and Tsunehisa Tsubokawa 3,5
 Hoshino et al. JA Clinical Reports (2017) 3:9 DOI 10.1186/s40981-017-0077-6 CASE REPORT Open Access Lipid emulsion injection-induced reversal of cardiac toxicity and acceleration of emergence from general
Hoshino et al. JA Clinical Reports (2017) 3:9 DOI 10.1186/s40981-017-0077-6 CASE REPORT Open Access Lipid emulsion injection-induced reversal of cardiac toxicity and acceleration of emergence from general
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
SAS Audit and Research Prize Submission January 2013
 1 Dr Johann Willers Associate Specialist in Anaesthesia and Intensive Care Department of Anaesthesia and Intensive Care Western Sussex Hospitals NHS Trust Worthing Hospital Lyndhurst Road Worthing West
1 Dr Johann Willers Associate Specialist in Anaesthesia and Intensive Care Department of Anaesthesia and Intensive Care Western Sussex Hospitals NHS Trust Worthing Hospital Lyndhurst Road Worthing West
HealthCare Training Service
 HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
P V Praveen Kumar 1*, P. Archana 2. Original Research Article. Abstract
 Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Comparison Of 0.5%Bupivacaine And 0.5% Bupivacaine Plus Buprenorphine in Brachial Plexus Block
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
Therapeutic hypothermia Transcutaneous pacing Sodium bicarbonate Rx Calcium, Magnesium Fluids and Pressors Antiarrhythmic Rx Epi/Vasopressin O 2
 Resuscitation Arsenal Therapeutic hypothermia Transcutaneous pacing Sodium bicarbonate Rx Calcium, Magnesium Fluids and Pressors Antiarrhythmic Rx Epi/Vasopressin O 2 /intubation Shock CPR ` 1994-96 Standing
Resuscitation Arsenal Therapeutic hypothermia Transcutaneous pacing Sodium bicarbonate Rx Calcium, Magnesium Fluids and Pressors Antiarrhythmic Rx Epi/Vasopressin O 2 /intubation Shock CPR ` 1994-96 Standing
Validity of the lipid sink as a mechanism for the reversal of local anesthetic systemic
 1 Validity of the lipid sink as a mechanism for the reversal of local anesthetic systemic toxicity: A physiologically based pharmacokinetic model study Ilin Kuo, MS. Research Assistant, Department of Chemical
1 Validity of the lipid sink as a mechanism for the reversal of local anesthetic systemic toxicity: A physiologically based pharmacokinetic model study Ilin Kuo, MS. Research Assistant, Department of Chemical
Peripheral nerve blocks offer considerable anesthetic
 Combined Lipid Emulsion and ACLS Resuscitation Following Bupivacaine- and Hypoxia-Induced Cardiovascular Collapse in Unanesthetized Swine CDR Brent A. Bushey, CRNA, MS, NC, USN Victor H. Auld, CRNA, MSN
Combined Lipid Emulsion and ACLS Resuscitation Following Bupivacaine- and Hypoxia-Induced Cardiovascular Collapse in Unanesthetized Swine CDR Brent A. Bushey, CRNA, MS, NC, USN Victor H. Auld, CRNA, MSN
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Intralipid for Amniotic Fluid Embolism (AFE)?
 Intralipid for Amniotic Fluid Embolism (AFE)? Joseph Eldor, MD. Vladimir Kotlovker, MD Theoretical Medicine Institute, P.O.Box. 27476, Jerusalem 91273, Israel csen_international@csen.com Weinberg et al.
Intralipid for Amniotic Fluid Embolism (AFE)? Joseph Eldor, MD. Vladimir Kotlovker, MD Theoretical Medicine Institute, P.O.Box. 27476, Jerusalem 91273, Israel csen_international@csen.com Weinberg et al.
4 Development of an ESR online-method for the monitoring of in vitro fat digestion
 4 Development of an ESR online-method for the monitoring of in vitro fat digestion 4.1 Introduction When regarding the oral administration of lipid-based nanocapsules, gastrointestinal digestion will play
4 Development of an ESR online-method for the monitoring of in vitro fat digestion 4.1 Introduction When regarding the oral administration of lipid-based nanocapsules, gastrointestinal digestion will play
Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical Trial
 J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
The ABC of CAB- Circulation, Airway, Breathing: PALS/Resuscitation Update
 The ABC of CAB- Circulation, Airway, Breathing: PALS/Resuscitation Update Jennifer K. Lee, MD Johns Hopkins University Dept. of Anesthesia, Division of Pediatric Anesthesia Disclosures I have research
The ABC of CAB- Circulation, Airway, Breathing: PALS/Resuscitation Update Jennifer K. Lee, MD Johns Hopkins University Dept. of Anesthesia, Division of Pediatric Anesthesia Disclosures I have research
Guidelines Administrative Practice X Clinical Practice Professional Practice
 Guidelines Administrative Practice X Clinical Practice Professional Practice End Tidal CO 2 (EtCO2) Monitoring Using the Zoll Monitor/Defibrillator Page 1 of 4 Scope: Outcome: Respiratory Therapists (RT),
Guidelines Administrative Practice X Clinical Practice Professional Practice End Tidal CO 2 (EtCO2) Monitoring Using the Zoll Monitor/Defibrillator Page 1 of 4 Scope: Outcome: Respiratory Therapists (RT),
Advanced Resuscitation - Adult
 C02A Resuscitation 2017-03-23 17 years & older Office of the Medical Director Advanced Resuscitation - Adult Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
C02A Resuscitation 2017-03-23 17 years & older Office of the Medical Director Advanced Resuscitation - Adult Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
Update of CPR AHA Guidelines
 Update of CPR AHA Guidelines Donald Hal Shaffner Course objective is to have an updated understanding of the American Heart Association s treatment algorithms for the management of cardiac decompensation
Update of CPR AHA Guidelines Donald Hal Shaffner Course objective is to have an updated understanding of the American Heart Association s treatment algorithms for the management of cardiac decompensation
UNIVERSITY OF BOLTON SCHOOL OF SPORT AND BIOMEDICAL SCIENCES SPORT PATHWAYS WITH FOUNDATION YEAR SEMESTER TWO EXAMINATIONS 2015/2016
 LH8 UNIVERSITY OF BOLTON SCHOOL OF SPORT AND BIOMEDICAL SCIENCES SPORT PATHWAYS WITH FOUNDATION YEAR SEMESTER TWO EXAMINATIONS 2015/2016 INTRODUCTION TO HUMAN PHYSIOLOGY MODULE NO: SRB3008 Date: Monday
LH8 UNIVERSITY OF BOLTON SCHOOL OF SPORT AND BIOMEDICAL SCIENCES SPORT PATHWAYS WITH FOUNDATION YEAR SEMESTER TWO EXAMINATIONS 2015/2016 INTRODUCTION TO HUMAN PHYSIOLOGY MODULE NO: SRB3008 Date: Monday
Intralipid for Bone cement implantation syndrome (BCIS)?
 Intralipid for Bone cement implantation syndrome (BCIS)? Joseph Eldor, MD. Vladimir Kotlovker, MD Theoretical Medicine Institute, P.O.Box. 27476, Jerusalem 91273, Israel csen_international@csen.com Abstract
Intralipid for Bone cement implantation syndrome (BCIS)? Joseph Eldor, MD. Vladimir Kotlovker, MD Theoretical Medicine Institute, P.O.Box. 27476, Jerusalem 91273, Israel csen_international@csen.com Abstract
WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR
 RECOVER 2011 1 of 6 WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR 1. Basic Demographics Worksheet author(s) Kate Hopper Mailing address: Dept Vet Surgical & Radiological Sciences Room
RECOVER 2011 1 of 6 WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR 1. Basic Demographics Worksheet author(s) Kate Hopper Mailing address: Dept Vet Surgical & Radiological Sciences Room
Lipid Therapy for Cardiac Arrest (PICO #ALS-834)
 Lipid Therapy for Cardiac Arrest (PICO #ALS-834) TFQO: Clif Calloway, COI #214 EVREV 1: Eric Lavonas, COI #240 EVREV 1: Mohammed Alhelai, COI #4 Taskforce: ALS COI Disclosure Dallas 2015 Eric Lavonas,
Lipid Therapy for Cardiac Arrest (PICO #ALS-834) TFQO: Clif Calloway, COI #214 EVREV 1: Eric Lavonas, COI #240 EVREV 1: Mohammed Alhelai, COI #4 Taskforce: ALS COI Disclosure Dallas 2015 Eric Lavonas,
Carnitine and sports medicine: Use or abuse?
 Carnitine and sports medicine: Use or abuse? Eric P. Brass, M.D., Ph.D. Professor of Medicine, UCLA School of Medicine Director, Harbor-UCLA Center for Clinical Pharmacology Disclosure: Dr. Brass is a
Carnitine and sports medicine: Use or abuse? Eric P. Brass, M.D., Ph.D. Professor of Medicine, UCLA School of Medicine Director, Harbor-UCLA Center for Clinical Pharmacology Disclosure: Dr. Brass is a
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator
 Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Comparision of Intravenous Bolus Phenylephrine and Ephedrine for Prevention of Post Spinal Hypotension in Cesarean Sections
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. II (July. 2015), PP 99-103 www.iosrjournals.org Comparision of Intravenous Bolus Phenylephrine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. II (July. 2015), PP 99-103 www.iosrjournals.org Comparision of Intravenous Bolus Phenylephrine
Feasibility of Leadless Cardiac Pacing Using Injectable. Magnetic Microparticles
 Supplementary Information for Feasibility of Leadless Cardiac Pacing Using Injectable Magnetic Microparticles Menahem Y. Rotenberg, Hovav Gabay, Yoram Etzion and Smadar Cohen. Correspondence to: scohen@bgu.ac.il,
Supplementary Information for Feasibility of Leadless Cardiac Pacing Using Injectable Magnetic Microparticles Menahem Y. Rotenberg, Hovav Gabay, Yoram Etzion and Smadar Cohen. Correspondence to: scohen@bgu.ac.il,
Pharmacokinetics of propofol when given by intravenous
 Br. J. clin. Pharmac. (199), 3, 144-148 Pharmacokinetics of propofol when given by intravenous infusion DENIS J. MORGAN', GWEN A. CAMPBELL2,* & DAVID P. CRANKSHAW2 'Victorian College of Pharmacy, 381 Royal
Br. J. clin. Pharmac. (199), 3, 144-148 Pharmacokinetics of propofol when given by intravenous infusion DENIS J. MORGAN', GWEN A. CAMPBELL2,* & DAVID P. CRANKSHAW2 'Victorian College of Pharmacy, 381 Royal
Local anesthetics are widely and commonly used throughout
 SPECIAL ARTICLE ASRA Practice Advisory on Local Anesthetic Systemic Toxicity Joseph M. Neal, MD,* Christopher M. Bernards, MD,* John F. Butterworth, IV, MD,Þ Guido Di Gregorio, MD,þ Kenneth Drasner, MD,
SPECIAL ARTICLE ASRA Practice Advisory on Local Anesthetic Systemic Toxicity Joseph M. Neal, MD,* Christopher M. Bernards, MD,* John F. Butterworth, IV, MD,Þ Guido Di Gregorio, MD,þ Kenneth Drasner, MD,
Epinephrine Cardiovascular Emergencies Symposium 2018
 Epinephrine Cardiovascular Emergencies Symposium 218 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN High Quality
Epinephrine Cardiovascular Emergencies Symposium 218 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN High Quality
The evaluation of cardiovascular response to exercise in healthy Turkish children
 The Turkish Journal of Pediatrics 2009; 51: 472-477 Original The evaluation of cardiovascular response to exercise in healthy Turkish children Hülya Akdur 1, Ahmet Bilge Sözen 2, Zerrin Yiğit 3, Funda
The Turkish Journal of Pediatrics 2009; 51: 472-477 Original The evaluation of cardiovascular response to exercise in healthy Turkish children Hülya Akdur 1, Ahmet Bilge Sözen 2, Zerrin Yiğit 3, Funda
INTRAVENOUS lipid emulsion (LE) has been reported
 Lipid Emulsion Reverses Levobupivacaine-induced Responses in Isolated Rat Aortic Vessels Seong-Ho Ok, M.D.,* Ju-Tae Sohn, M.D., Ji-Seok Baik, M.D., Jae-Gak Kim, M.D., Sang-Seung Park, M.D., Hui-Jin Sung,
Lipid Emulsion Reverses Levobupivacaine-induced Responses in Isolated Rat Aortic Vessels Seong-Ho Ok, M.D.,* Ju-Tae Sohn, M.D., Ji-Seok Baik, M.D., Jae-Gak Kim, M.D., Sang-Seung Park, M.D., Hui-Jin Sung,
Labor Epidural: Local Anesthetics and Beyond
 Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Pilot Of Spontaneous Breathing Vs. Ventilated Model For Hemorrhage And Resuscitation In The Rabbit
 Article ID: WMC001137 Pilot Of Spontaneous Breathing Vs. Ventilated Model For Hemorrhage And Resuscitation In The Rabbit Author(s):Dr. Jonathan S. Jahr, MD, Dr. Robert A. Gunther, PhD, Dr. Bernd Driessen,
Article ID: WMC001137 Pilot Of Spontaneous Breathing Vs. Ventilated Model For Hemorrhage And Resuscitation In The Rabbit Author(s):Dr. Jonathan S. Jahr, MD, Dr. Robert A. Gunther, PhD, Dr. Bernd Driessen,
Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries and Perineal Surgeries
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Perioperative Fluid Management in ERPs
 Perioperative Fluid Management in ERPs Robert H. Thiele, M.D. Assistant Professor University of Virginia First Do No Harm Intravenous fluids should be considered a pharmacotherapeutic agent Just like all
Perioperative Fluid Management in ERPs Robert H. Thiele, M.D. Assistant Professor University of Virginia First Do No Harm Intravenous fluids should be considered a pharmacotherapeutic agent Just like all
Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant
 Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Use of the Intubating Laryngeal Mask Airway
 340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
Blood Transfusion Practice Indicated by Paediatric Intensive Care Specialists in Response to Four Clinical Scenarios
 Original articles Blood Transfusion Practice Indicated by Paediatric Intensive Care Specialists in Response to Four Clinical Scenarios E. NAHUM, J. BEN-ARI, T. SCHONFELD Paediatric Intensive Care Unit,
Original articles Blood Transfusion Practice Indicated by Paediatric Intensive Care Specialists in Response to Four Clinical Scenarios E. NAHUM, J. BEN-ARI, T. SCHONFELD Paediatric Intensive Care Unit,
Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines
 Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines www.circ.ahajournals.org Elham Pishbin. M.D Assistant Professor of Emergency Medicine MUMS C H E S Advanced Life Support
Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines www.circ.ahajournals.org Elham Pishbin. M.D Assistant Professor of Emergency Medicine MUMS C H E S Advanced Life Support
Biostatistics and Epidemiology Step 1 Sample Questions Set 2. Diagnostic and Screening Tests
 Biostatistics and Epidemiology Step 1 Sample Questions Set 2 Diagnostic and Screening Tests 1. A rare disorder of amino acid metabolism causes severe mental retardation if left untreated. If the disease
Biostatistics and Epidemiology Step 1 Sample Questions Set 2 Diagnostic and Screening Tests 1. A rare disorder of amino acid metabolism causes severe mental retardation if left untreated. If the disease
What works? What doesn t? What s new? Terry M. Foster, RN
 What works? What doesn t? What s new? Terry M. Foster, RN 2016 Changes Updated every 5 years Last update was 2010 All recommendations have been heavily researched with studies involving large number of
What works? What doesn t? What s new? Terry M. Foster, RN 2016 Changes Updated every 5 years Last update was 2010 All recommendations have been heavily researched with studies involving large number of
Advanced Resuscitation - Adolescent
 C02B Resuscitation 2017-03-23 10 up to 17 years Office of the Medical Director Advanced Resuscitation - Adolescent Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia
C02B Resuscitation 2017-03-23 10 up to 17 years Office of the Medical Director Advanced Resuscitation - Adolescent Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia
Support for Acetaminophen 1000 mg Over-the-Counter Dose:
 Support for Acetaminophen 1000 mg Over-the-Counter Dose: The Dental Impaction Pain Model and Efficacy and Safety Results from McNeil Randomized, Double-Blind, Single-Dose Study of Acetaminophen 1000 mg,
Support for Acetaminophen 1000 mg Over-the-Counter Dose: The Dental Impaction Pain Model and Efficacy and Safety Results from McNeil Randomized, Double-Blind, Single-Dose Study of Acetaminophen 1000 mg,
Factors Affecting the Inosine Monophosphate Content of Muscles in Taihe Silkies Chickens
 1359 Factors Affecting the Inosine Monophosphate Content of Muscles in Taihe Silkies Chickens G. H. Chen*, H. F. Li 1, X. S. Wu, B. C. Li, K. Z. Xie, G. J. Dai, K. W. Chen 1, X. Y. Zhang 1 and K. H. Wang
1359 Factors Affecting the Inosine Monophosphate Content of Muscles in Taihe Silkies Chickens G. H. Chen*, H. F. Li 1, X. S. Wu, B. C. Li, K. Z. Xie, G. J. Dai, K. W. Chen 1, X. Y. Zhang 1 and K. H. Wang
Local anaesthetics. Dr JM Dippenaar
 Local anaesthetics Dr JM Dippenaar Chemical structure Lipophilic phenol ring + Amide/Ester bridge + Hydrophilic chain Local anesthetic drugs Amides Esters Lignocaine Cocaine Bupivacaine PABA esters Ropivacaine
Local anaesthetics Dr JM Dippenaar Chemical structure Lipophilic phenol ring + Amide/Ester bridge + Hydrophilic chain Local anesthetic drugs Amides Esters Lignocaine Cocaine Bupivacaine PABA esters Ropivacaine
Application of ultrasound in goal-directed fluid management of anesthesia in elderly patients.
 Biomedical Research 2017; Special Issue: S482-S486 ISSN 0970-938X www.biomedres.info Application of ultrasound in goal-directed fluid management of anesthesia in elderly patients. Baoyong Li, Limin Zhang,
Biomedical Research 2017; Special Issue: S482-S486 ISSN 0970-938X www.biomedres.info Application of ultrasound in goal-directed fluid management of anesthesia in elderly patients. Baoyong Li, Limin Zhang,
June 2011 Bill Streett-Training Section Chief
 Capnography 102 June 2011 Bill Streett-Training Section Chief Terminology Capnography: the measurement and numerical display of end-tidal CO2 concentration, at the patient s airway, during a respiratory
Capnography 102 June 2011 Bill Streett-Training Section Chief Terminology Capnography: the measurement and numerical display of end-tidal CO2 concentration, at the patient s airway, during a respiratory
Dr Ahmad Shaltut Othman Anaesthesiologist & Intensivist Hosp Sultanah Bahiyah Alor Setar
 FEEDING WITH FISH OIL Dr Ahmad Shaltut Othman Anaesthesiologist & Intensivist Hosp Sultanah Bahiyah Alor Setar New horizons in clinical nutrition from Support to Therapy Landmarks in Parenteral Nutrition
FEEDING WITH FISH OIL Dr Ahmad Shaltut Othman Anaesthesiologist & Intensivist Hosp Sultanah Bahiyah Alor Setar New horizons in clinical nutrition from Support to Therapy Landmarks in Parenteral Nutrition
Medical Biochemistry and Molecular Biology department
 Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
The Hypotensive Poisoned Patient. Robert S. Hoffman, MD Director, NYC PCC
 The Hypotensive Poisoned Patient Robert S. Hoffman, MD Director, NYC PCC Some Definitions Hypotension = Low blood pressure Failure of macrocirculation Shock = Poor tissue perfusion Failure of microcirculation
The Hypotensive Poisoned Patient Robert S. Hoffman, MD Director, NYC PCC Some Definitions Hypotension = Low blood pressure Failure of macrocirculation Shock = Poor tissue perfusion Failure of microcirculation
Unexpected Cardiac Arrest In The Anesthetized Child
 Unexpected Cardiac Arrest In The Anesthetized Child Historical Background Jeffrey Morray, MD Outcomes for anesthetized children have improved over the past 50 years, as reflected in anesthesia-related
Unexpected Cardiac Arrest In The Anesthetized Child Historical Background Jeffrey Morray, MD Outcomes for anesthetized children have improved over the past 50 years, as reflected in anesthesia-related
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
