Conclusion: PPNB with one percent lignocaine. is a safe analgesic procedure to perform in
|
|
|
- Lilian Stokes
- 5 years ago
- Views:
Transcription
1 Original Article Singapore Med J 2011, 52(10) 752 Incidence of complications after transrectal ultrasonography-guided biopsy of the prostate in a local tertiary institution Wu M W F, Sevilla E M, Raman L, Consigliere D, Siow W Y, Tiong H Y ABSTRACT Introduction: This study aimed to evaluate the risk of complications for patients who received periprosthetic nerve block (PPNB) with one percent lignocaine before transrectal ultrasonography (TRUS) biopsy of the prostate. Conclusion: PPNB with one percent lignocaine is a safe analgesic procedure to perform in patients undergoing TRUS biopsy. Keywords: complications, periprostatic nerve block, transrectal prostate biopsy Singapore Med J 2011; 52(10): Department of Urology, National University Health System, 1E Kent Ridge Road, NUHS Tower Block Level 8, Singapore Wu MAW, MBBS, MMed, MRCSE Registrar Sevilla EM, MD Medical Officer Raman L, MD Research Scientist Consigliere D, MBBS, FAMS Senior Consultant Siow WY, MBBS, FAMS Consultant Tiong HY, MD, FAMS Consultant Correspondence to: Dr Tiong Ho Yee Tel: (65) Fax: (65) cfsthy@nus. edu.sg Methods: From 2008 to 2009, data on 526 consecutive patients who underwent prostate biopsy was prospectively recorded and analysed. 475 (90.3 percent) patients received PPNB with 10 ml of one percent lignocaine (Group I), which was carried out under TRUS-guidance and prior to biopsy. 51 (9.7 percent) patients received diclofenac (100 mg) intramuscular injections or no analgesia (Group 2). Complications were defined as any adverse effects after biopsy. Serious complications were defined as those requiring hospitalisation or invasive/operative procedures for treatment. Results: At baseline, both groups were comparable. The mean prostate -specific antigen level in Group I was higher than that in Group 2 (48.6 +/ versus /- 4.3 ng/ml; p -value is 0.04). There was no perioperative mortality. Post -procedural complications were reported in 23.4 percent (n is I I I) of patients in Group I and 25.5 percent (n is 13) in Group 2 (p -value is 0.27). Serious complications were reported in 2.5 percent (n is 12) and 7.1 percent (n is 3) of Group I and 2 patients (p -value is 0.10), respectively. Both univariable and logistic regression revealed age below 65 years and pre -procedure complaints of lower urinary tract symptoms as independent predictors for complications (p -values are 0.02 and 0.006, respectively). INTRODUCTION Transrectal ultrasonography (TRUS)-guided biopsy of the prostate is widely regarded as the gold standard for diagnosing prostate cancer. It is usually performed in the outpatient setting, as it is a considered a minor and safe procedure. Although it is well tolerated by most men, a considerable number of patients do complain of discomfort and pain. Various studies show that 65%-90% of patients complain of mild discomfort to severe pain.(') Irani et al reported that up to 19% of patients would not undergo a repeat procedure without any form of anaesthesia(2) Periprostatic nerve block (PPNB) was first introduced by Nash et alo) in 1996 and since then, various prospective clinical studies, including a meta - analysis, have shown that PPNB significantly reduces the pain score in patients when compared to a placebo"," or other forms of analgesia such as intramuscular injections or rectal administration of non -steroidal anti- inflammatory drugs (NSAIDs) and intrarectal local anaesthesia.(4'6'7) The most common complications after a TRUS biopsy are haematuria, urinary tract infections (UTIs), rectal bleeding and acute retention of urine. Some complications are serious enough to warrant hospitalisation and/or operative procedures for treatment. The rate of serious complications was 0.5%-6.6% in different studies:81 ' Recent studies have re -highlighted the emerging significance of TRUS complications("2' as increasing number of biopsies and repeat biopsies are performed in an era of prostate -specific antigen (PSA) screening. Following our initial evaluationv") and
2 Singapore Med J 2011; 52(10) 753 subsequent introduction of PPNB to clinical practice, we prospectively evaluated the risk of complications for patients who received PPNB with 1% lignocaine before the TRUS biopsy, and compared it with patients who received intramuscular diclofenac or no analgesia. METHODS An Institutional Review Board (IRB)-approved database was developed to audit complications post-trus prostate biopsy after the introduction of PPNB at our institution. A total of 526 consecutive patients who underwent TRUS biopsy of the prostate from January 2008 to September 2009 were prospectively enrolled in our study. Indications for the biopsy were elevated serum PSA and/ or abnormal digital rectal examination of the prostate. Anticoagulant or antiplatelet medications were stopped one week before the biopsy. Antibiotic prophylaxis with oral ciprotioxacin 500 mg was started one day before the biopsy and continued twice daily for a total of three days. A Dulcolax suppository (Boehringer, Ingelheim, Germany) was self-administered by the patients on the morning of the biopsy. The clinicians performing the procedures discussed with all the patients undergoing a TRUS-guided prostate biopsy concerning their preferred analgesia during the biopsy. The choice of analgesia was dependent on the clinician -patient discussion prior to the procedure. Group 1 consisted of 475 (90.3%) patients who had PPNB with 1% lignocaine performed under TRUS-guidance prior to the biopsy. Group 2 comprised 51 (9.7%) patients who had intramuscular injection of 100 mg diclofenac before the biopsy or no analgesia at all due to drug allergies. Only three patients in Group 2 opted for no analgesia. For PPNB in Group 1, the patient was placed in the left lateral decubitus position. TRUS was performed using a Falcon 2101 Ultrasound Scanner with a MHz transducer probe (BK Medical, Peabody, MA, USA). PPNB was performed by infiltrating 5 ml of 1% lignocaine to the neurovascular bundle on each side of the prostate using the outer sheath of the 18 -gauge biopsy needle. With the US in the sagittal view, injection was given in the neurovascular bundle at the base of the prostate just lateral to the junction between the prostate and the seminal vesicle, as described earlier.(6) The syringe was aspirated before injection to ensure that a vascular structure was not entered. Proper positioning of the needle was confirmed by observing the separation of the seminal vesicle and prostate from the rectal wall caused by the injection. Patients in Group 2 proceeded directly to biopsy either with no analgesia or minutes after analgesia. Before biopsy, the prostate volume was measured by the non-planimetric ellipsoid formula. The presence of hypoechoic areas or calcifications on TRUS was noted on a standardised report form. Systematic core biopsies of the prostate were taken using an automatic spring -loaded biopsy gun with an 18 -gauge Tru-Cut biopsy needle (CR Bard Inc, Covington, GA, USA). The number of core biopsies taken depended on the individual clinician's decision. All procedures were performed in the above standardised technique on an outpatient basis. All patients were reviewed 2-3 weeks after the procedure, and any complications reported during the visit were recorded in the clinical case notes. Complications that were additionally self -reported by the patients after the biopsy, including unscheduled post -procedure outpatient visits and phone calls to the outpatient clinic, were also captured in the clinical notes. Serious complications were defined as those requiring hospitalisation or interventions, including intravenous antibiotics, cystoscopic procedures or operations for treatment. These were recorded in the same unified outpatient and inpatient records. Demographic data, PSA value, clinical and US parameters of the prostate, number of cores taken and complications were recorded for each patient in a computerised database by a dedicated database administrator, who reviewed all the clinical records and investigational results of the patients one month after the prostate biopsy. Statistical analysis was performed using the Statistical Package for the Social Sciences version 17 (SPSS, Chicago, IL, USA). Chi-square test was performed for categorical variables, and Student's t -test and ANOVA were used for analysis of continuous variables. Univariable and multivariable logistic regression were performed to assess the associated risk factors for post -procedural complications. A p -value < 0.05 was considered statistically significant. RESULTS At baseline, the two groups were comparable in terms of demographics, clinical and US parameters of the prostate and the number of cores taken for biopsy (Table I). In particular, there were no significant differences in the mean prostate volumes of both groups (44.2 ± 1.0 vs ± 4.0 ml, p = 0.85). However, the mean PSA level in Group 1 was higher than that in Group 2 (48.6 ± 13.8 vs ± 4.3 ng/ml, p = 0.04). Table II shows no statistically significant difference between the two groups in the histological outcomes of the biopsy, with prostate cancer diagnosed in 27.4% (n = 130) of Group 1 and 33.3% (n = 17) of Group 2 patients (p = 0.41).
3 Group (1.9) (2.0) Singapore Med J 2011; 52(10) 754 Table I. Baseline demographic, clinical and ultrasonographic characteristics of patients in Group I Group 2 (without PPNB). (with PPNB) and Patient characteristic No. (%) p -value Group I (n = 475) Group 2 (n = 51) Mean age ± SD (yrs) 65.7 ± ± Race Chinese 404 (85.1) 41 (80.4) 0.95 Malay 33 (6.9) 3 (5.9) 0.26 Indian 12 (2.5) Others 26 (5.5) 6 (11.8) 0.27 Diabetes mellitus 81 (17.1) 6(11.8) 0.22 On antiplatelet medications 40 (8.4) 5 (9.8) 0.45 On anticoagulant medications 5 (1.1) Compliant to pre -medications* 427 (89.9) 39 (76.5) 0.94 LUTS pre -procedure 168 (35.4) 14 (27.5) 0.77 Mean PSA level ± SD (ng/ml) 48.6 ± ± Abnormal digital rectal examination 113 (23.8) 13 (25.0) 0.23 Mean prostate volume on TRUS ± SD (ml) 44.2 ± ± Mean no. of cores taken ± SD 11.0± ± No. of repeat biopsies 30 (6.3) 5 (9.8) 0.49 * Pre -medications: antibiotics and suppository t Statistically significant PPNB: periprostatic nerve block; SD: standard deviation; LUTS: lower urinary tract symptoms; PSA: prostate -specific antigen; TRUS:transrectal ultrasonography Table Ill. Demographic and clinical parameters of patients with complications (n = I l l). I Table II. Histological outcome of TRUS biopsy of patients in Group I (with PPNB) and Group 2 (without PPNB). Parameter No. (%) Histological outcome No. of patients (%) p -value Mean age ± SD (yrs) 63.9 ± 9.2 Group 2 (n = 475) (n = 51) Mean PSA level ± SD (ng/ml) ± Benign prostatic hyperplasia 263 (55.4) 24 (47.1) 0.94 Mean prostate volume on TRUS ± SD (ml) ± only Mean no.of cores taken ± SD ± 1.66 Prostatitis documented 94 (19.8) 9 (17.6) 0.91 Diabetes mellitus 18 (16.4) Cancer detected 130 (27.4) 17 (33.3) 0.41 On antiplatelet medications 10 (9.1) Note: Some patients showed a combination of mutiple On anticoagulant medications 2 (1.8) histological outcomes No. of repeat biopsies 5 (4.5) PPNB: periprostatic nerve block; TRUS: transrectal ultrasonography SD: standard deviation; PSA: prostate -specific antigen; TRUS: transrectal ultrasonography The total complication rate reported in the two groups was 23.6% (n = 124). Table III shows the demographics and clinical parameters of patients who had complications. The overall complication rate (proportion of patients with at least one complication) was 23.4% (n = 111) in Group 1 patients and 25.5% (n = 13) in Group 2 (p = 0.27). The most commonly reported specific complications in both groups were gross haematuria and UTIs (Table IV). As there were patients complication, the different who reported more than one specific there was an overlap of patients in reported specific complications. The proportion of patients with gross haematuria in Group 2 (n = 9) was significantly higher than that in Group 1 (n = 36) (21.4% vs. 7.6%, p = 0.002). There was no significant difference between the two groups with regard to all other specific complications. No perioperative mortality was noted across the board. The total serious complication rate (proportion of patients with at least one serious complication) for the two groups was 2.9% (n = 15). Serious complications were reported in 2.5% (n = 12) and 7.1% (n = 3) of Group 1 and 2 patients, respectively (p = 0.104), and only these patients were admitted for treatment. Table IV shows the breakdown of specific serious complications, with some patients having more than one serious specific complication. Due to the small number of patients in both groups, statistical comparison between the specific serious complications was not performed.
4 Singapore Med J 2011; 52(10) 755 Table IV. Specific complications/serious complications of patients in Group I (with PPNB) and Group 2 (without PPNB). Complication* No. of patients (%) Group I (n = 475) Group 2 (n = 51) p -value Gross haematuria 36 (7.6) 9 (21.4) Acute urinary retention 27 (5.7) 2 (4.8) 0.89 Haematospermia 23 (4.8) I (2.4) Urinary tract infection 12 (2.5) I Rectal bleeding 5 (1.1) I Serious complication* Gross haematuria 4 (0.8) 3 (5.9) Acute urinary retention 4 (0.8) 0 Urinary tract infection 4 (0.8) 0 Rectal bleeding 2 (0.4) (2.4) 0.29 (2.4) 0.47 * There was an overlap of patients with different specific complications/serious complications (i.e. some patients reported more than one complication). t Statistically significant PPNB: periprostatic nerve block Clinical, US and demographic risk factors were analysed for their association with overall complications using both univariable and multivariable models, as shown in Tables V and VI. The mean age group of patients who had complications was significantly lower than those without complications (63.8 ± 9.4 vs ± 8.3 years, p = 0.01), although the difference was clinically small. On univariable analysis, age < 65 years (p = 0.03, odds ratio [OR] 1.56, 95% confidence level [CI] ) and pre - procedure complaints of lower urinary tract symptoms (LUTS) (p = 0.009, OR 1.73, 95% CI ) were significantly associated with overall complications. Multivariable logistic regression using these two factors in combination with PPNB confirmed age < 65 years and pre -procedure complaints of LUTS as independent predictors for overall complications (p = 0.02, OR 1.67, 95% CI and p = 0.006, OR 1.80, 95% CI , respectively). The number of patients with serious complications was too small for meaningful analysis with the univariable and multivariable models. DISCUSSION Several studies have already shown that PPNB reduces pain from TRUS prostate biopsy (47) Our previous study has ascertained that the pain score was lower in the PPNB group (diclofenac 3.70 ± 2.36 and PPNB 2.24 ± 1.63).(4) In our current population, the mean pain score for patients in the PPNB group (Group 1) was 1.16 ± and that for Group 2 was 1.46 ± (p = 0.004). Pain score was Table V. Univariable analysis of risk factors for overall complications. Variable OR; 95% CI p -value Age (yrs) < ; > ; Race Chinese 0.68; Others 1.48; History of diabetes mellitus No 1.07; Yes 0.96; On anticoagulation medication No 0.61; Yes 1.63; On antiplatelet medication No 0.83; Yes 1.20; Compliance to pre -medication No 1.37; Yes 0.73; Presence of LUTS pre -procedure No 0.58; Yes 1.73; PSA level (ng/ml) < ; > ; Indication for TRUS biopsy Abnormal DRE and raised PSA 1.49; Abnormal DRE or raised PSA 0.67; Periprosthetic nerve block given No 1.54; Yes 0.65; TRUS finding of hypoechoic nodules No 1.00; Yes 1.00; TRUS finding of calcifications No 0.51; Yes 1.98; TRUS prostate volume < ; > ; Total no. of cores taken ; > ; TRUS prostate biopsy was a repeat procedure No 1.95; Yes 0.51; OR: odds ratio; CI: confidence interval; LUTS: lower urinary tract symptoms; PSA: prostate -specific antigen;trus: transrectal ultrasonography; DRE: digital rectal examination measured using the Wong -Baker FACES Pain Rating Scale, and none of the patients in this study had pain score > 3. The use of PPNB as an analgesia will become more widespread, since it is a relatively easy and quick procedure to perform just prior to biopsy. With this effective form of analgesia, patients would find TRUS
5 Singapore Med J 2011; 52(10) 756 Table VI. Multivariable analysis of risk factors for overall complications. Variable OR; 95% CI p -value Age (yrs) < ; > ; LUTS Yes 1.80; No 0.56; Administration of PPNB Yes 1.55; No 0.65; OR: odds ratio; CI: confidence interval; LUTS: lower urinary tract symptoms; PPNB: periprostatic nerve block biopsy to be more acceptable, especially when a repeat biopsy or a higher number of cores is required for a more accurate diagnosis. In this prospective follow-up study, we have shown that the risk of overall complications and serious complications was not significantly increased following the introduction of PPNB into our clinical practice compared to intramuscular injection of diclofenac or no analgesia. The predictable course and the close proximity of the prostatic neurovascular bundles to the rectal wall mean that they can be easily targeted and accessed by a US -guided needle for the injection of a local anaesthetic. However, there have been reported concerns that the injection of a local anaesthesia may increase bacteriuria and that more needle passes may cause greater rectal bleeding, both of which are already common in TRUS biopsies.(") Although there are many published studies on the efficacy of PPNB in relieving pain from TRUS prostate biopsy, few other publications have specifically addressed complications from PPNB. The overall and serious complication rates of 23.6% and 2.9%, respectively, from this series are comparable to those reported in other studies.") With regard to PPNB, our finding of no increased overall complications is consistent with that of two other published reports.(13,14) Obek et al studied 100 patients who underwent TRUS biopsy with PPNB as analgesia in a prospective randomised trial, and concluded that there was no increased risk of urethral bleeding.(") In a paper by Turgut et al, adverse effects associated with PPNB were reported to be mainly pain secondary to the needle puncture, lignocaine-associated problems and radiological changes in the prostate post biopsy. Only 1.5% of the 200 patients experienced post -procedure urinary incontinence; they also concluded that PPNB is a safe and effective analgesia for patients undergoing TRUS b opsy. (14) No significant difference in specific complications (UTIs or rectal bleeding) between the PPNB and non- PPNB groups was found. Interestingly, the proportion of patients reporting gross haematuria in the non-ppnb (Group 2) was significantly higher when compared to that in Group 1 (21.4% vs. 7.6%), although the proportions of patients on antiplatelet or anticoagulation medications were equivalent between the two groups. The reason for this is unclear, as injections of the neurovascular bundles are relatively distant from the urethra. We do not routinely administer apical lignocaine injections to the prostate. However, the vast majority of cases with haematuria are self -resolving with conservative treatment and do not have serious implications. Maan et al reported no statistically significant difference in the incidence of haematuria or overall bleeding in patients who continued taking aspirin before and after the procedure, and concluded that aspirin does not have to be discontinued before the biopsy."5' Despite this finding, all our patients who were on antiplatelet or anticoagulation medications were advised to discontinue them before biopsy, and this was confirmed before biopsy was performed. When univariable and multivariable logistic regressions were performed, younger age and the presence of LUTS were found to be independent predictors for complications. In particular, age < 65 years was found to be significantly predictive of reported overall complications. However, the clinical difference may actually be smaller, as the mean ages of those who had complications and those without were close (63.8 ± 9.4 vs ± 8.3 years, p = 0.010). One possible reason may be that younger patients are more likely to self - report complications compared to older patients. The presence of LUTS was an independent predictor of complications. The odds of patients with LUTS developing complications after prostate biopsy was 1.80 (95% CI ) compared to patients who denied any LUTS, i.e. the 'true' PSA-screened patients. Hence, patients who undergo PSA screening probably are at a low risk of complications from TRUS biopsy. Therefore, with the pain issues addressed by PPNB, TRUS biopsy can become a truly acceptable follow-up investigation for patients identified by PSA screening. Although the mean PSA level of the PPBN group was higher (48.6 ± 13.8 vs ± 4.3, p = 0.04) compared to the group without PPNB, the complication rate between the two groups is not significantly different. A higher PSA value can be attributed to either a larger prostate volume, the presence of prostate cancer or prostatitis, and this could translate to greater risk for complications; however, in our study, this was not evident.
6 Singapore Med J 2011; 52(10) 757 Despite the link between complications and LUTS, TRUS prostate volume was not a significant predictor of complications, and there was no significant difference in the mean prostate volume between patients with and without complications (45.2 ± 21.5 vs ± 21.6 ml, 5. respectively, p = 0.58). There is evidence to suggest that prostate volume is not the best indicator of bladder outlet obstruction, but other parameters, such as degree of 6. intravesical prostatic protrusion are more predictive of bladder outlet obstruction and LUTS. This is currently the subject of our ongoing research.i 6 "' 7. We acknowledge that there is a lack of randomisation in the study. The administration of PPNB did not allow for blinding. The number of patients in Group 1 (n = 475) was significantly higher, as we have adopted PPNB as the standard of care for TRUS biopsy in our institution. Hence, most patients would be offered this method of pain relief. However, we believe our results reflect the real -life clinical practice of introducing PPNB into clinical urological outpatients, with careful prospective recording of complications to document the safety of a new procedure. This study reflects the 'true' complication rate, with the patient's and clinician's choice of PPNB taken into account. In addition, by 12. Hadway P, Barrett LK, Waghorn DJ, et al. Urosepsis and documenting both self -reported complications and bacteraemia caused by antibiotic -resistant organisms after transrectal ultrasonography-guided prostate biopsy. BJU Int serious complications, we believe that a complete 2009; 104: picture of morbidity arising from PPNB and TRUS 13. Obek C, Onal B, Ozkan B, et al. Is periprostatic local anesthesia biopsy has been represented. This is important with the increasing attention given to post -biopsy complications, against the background of likely increasing advocates for transrectal ultrasound guided prostate biopsy associated with increased infectious or hemorrhagic complications? A prospective randomized trial. J Urol 2002; 168: Turgut AT, Olytictioglu E, Kosar P, Geyik PO, Kosar of PSA screening."8' In conclusion, our study shows that U. Complications and limitations related to periprostatic PPNB with 1% lignocaine is a safe analgesic procedure to perform in patients undergoing TRUS biopsy, as it does not significantly increase the risk of overall and serious complications when compared to patients who did not have PPNB. local anesthesia before TRUS-guided prostate biopsy. J Clin Ultrasound 2008; 36: Maan Z, Cutting CW, Patel U, et al. Morbidity of transrectal ultrasonography-guided prostate biopsies in patients after the continued use of low -dose aspirin. BJU Int 2003; 91: Mariappan P, Brown DJ, McNeill AS. Intravesical prostatic protrusion is better than prostate volume in predicting the outcome of trial without catheter in white men presenting with REFERENCES acute urinary retention: a prospective clinical study. J Urol 2007; 1. Collins GN, Lloyd SN, Hehir M, McKelvie GB. Multiple 178: Discussion 577. transrectal ultrasound -guided prostatic biopsies --true morbidity 17. Lim KB, Ho H, Foo KT, Wong MY, Fook-Chong S. Comparison and patient acceptance. Br J Urol 1993; 71: of intravesical prostatic protrusion, prostate volume and serum 2. Irani J, Fournier F, Bon D, et al. Patient tolerance of transrectal prostatic-specific antigen in the evaluation of bladder outlet ultrasound -guided biopsy of the prostate. Br J Urol 1997; obstruction. Int J Urol 2006; 13: : Schroder FH, Hugosson J, Roobol MJ, et al. Screening and 3. Nash PA, Bruce JE, Indudhara R, Shinohara K. Transrectal prostate -cancer mortality in a randomized European study. N ultrasound guided prostatic nerve blockade eases systematic Engl J Med 2009; 360: needle biopsy of the prostate. J Urol 1996; 155: Tiong HY, Liew LC, Samuel M, Consigliere D, Esuvaranathan K. A meta -analysis of local anesthesia for transrectal ultrasound - guided biopsy of the prostate. Prostate Cancer Prostatic Dis 2007; 10: Walker AE, Schelvan C, Rockall AG, Rickards D, Kellett MJ. Does pericapsular lignocaine reduce pain during transrectal ultrasonography-guided biopsy of the prostate? BJU Int 2002; 90: Bhomi KK, Lim HH, Consigliere DT, Tiong HY. Control of pain during transrectal ultrasound -guided prostate biopsy: a prospective study comparing two methods. Urol Int 2007; 79: Lynn NN, Collins GN, Brown SC, O'Reilly PH. Periprostatic nerve block gives better analgesia for prostatic biopsy. BJU Int 2002; 90: Ecke TH, Gunia S, Bartel P, et al. Complications and risk factors of transrectal ultrasound guided needle biopsies of the prostate evaluated by questionnaire. Urol Oncol 2008; 26: Raaijmakers R, Kirkels WJ, Roobol MJ, Wildhagen MF, Schrder FH. Complication rates and risk factors of 5802 transrectal ultrasound -guided sextant biopsies of the prostate within a population -based screening program. Urology 2002; 60: Rodriguez LV, Terris MK..Risks and complications of transrectal ultrasound guided prostate needle biopsy: a prospective study and review of the literature. J Urol 1998; 160 (6 Pt 1): Lange D, Zappav igna C, Hamidizadeh R, et al. Bacterial sepsis after prostate biopsy --a new perspective. Urology 2009; 74:
TRANSRECTAL ULTRASOUND-GUIDED PROSTATE BIOPSY, PERIPROSTATIC LOCAL ANESTHESIA AND PAIN TOLERANCE
 & TRANSRECTAL ULTRASOUND-GUIDED PROSTATE BIOPSY, PERIPROSTATIC LOCAL ANESTHESIA AND PAIN TOLERANCE Mustafa Hiroš 1 *, Mirsad Selimović 1, Hajrudin Spahović 1, Sabina Sadović 1, Ediba Spužić-Čelić 2 1 Urology
& TRANSRECTAL ULTRASOUND-GUIDED PROSTATE BIOPSY, PERIPROSTATIC LOCAL ANESTHESIA AND PAIN TOLERANCE Mustafa Hiroš 1 *, Mirsad Selimović 1, Hajrudin Spahović 1, Sabina Sadović 1, Ediba Spužić-Čelić 2 1 Urology
Getting to Diagnosis. Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust
 Getting to Diagnosis Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust GP Visit Symptoms Reduced urinary flow Difficulty starting/stopping Urgency Frequency Nocturia Because a friend/relative
Getting to Diagnosis Debbie Victor Uro-Oncology CNS Royal Cornwall Hospitals Trust GP Visit Symptoms Reduced urinary flow Difficulty starting/stopping Urgency Frequency Nocturia Because a friend/relative
Transrectal ultrasound-guided biopsy for the diagnosis of prostate cancer
 Transrectal ultrasound-guided for the diagnosis of prostate cancer Adrian Haşegan Clinica de Urologie, Spitalul Clinic Judeţean de Urgenţă Sibiu Facultatea de Medicină Sibiu Abstract Transrectal ultrasound-guided
Transrectal ultrasound-guided for the diagnosis of prostate cancer Adrian Haşegan Clinica de Urologie, Spitalul Clinic Judeţean de Urgenţă Sibiu Facultatea de Medicină Sibiu Abstract Transrectal ultrasound-guided
Major Complications and Associated Risk Factors of Transrectal Ultrasound Guided Prostate Needle Biopsy: A Retrospective Study of 1875 Cases in Taiwan
 ORIGINAL ARTICLE Major Complications and Associated Risk Factors of Transrectal Ultrasound Guided Prostate Needle Biopsy: A Retrospective Study of 1875 Cases in Taiwan I-Ni Chiang, 1 Shang-Jen Chang, 2
ORIGINAL ARTICLE Major Complications and Associated Risk Factors of Transrectal Ultrasound Guided Prostate Needle Biopsy: A Retrospective Study of 1875 Cases in Taiwan I-Ni Chiang, 1 Shang-Jen Chang, 2
Prostate gold seed fiducial implantation by radiation oncologists: A report on feasibility
 Prostate gold seed fiducial implantation by radiation oncologists: A report on feasibility Poster No.: R-0006 Congress: Type: Authors: Keywords: DOI: 2014 CSM Scientific Exhibit C. Jayaratne, A. Brown,
Prostate gold seed fiducial implantation by radiation oncologists: A report on feasibility Poster No.: R-0006 Congress: Type: Authors: Keywords: DOI: 2014 CSM Scientific Exhibit C. Jayaratne, A. Brown,
Thuchchai Pipitpanpipit, M.D.
 ARC Journal of Urology Volume 1, Issue 2, 2016, PP 15-19 www.arcjournals.org Prospective Randomized Controlled Study of the Results of Medication with Oral versus Oralcefixime to Prevent Transient Bacteraemia
ARC Journal of Urology Volume 1, Issue 2, 2016, PP 15-19 www.arcjournals.org Prospective Randomized Controlled Study of the Results of Medication with Oral versus Oralcefixime to Prevent Transient Bacteraemia
THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE BIOPSIES IN IMPROVING THE DIAGNOSTIC ABILITY IN PROSTATE CANCER
 Clinical Urology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 222-226, May - June, 2001 THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE
Clinical Urology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 222-226, May - June, 2001 THE SIGNIFICANCE OF HYPOECHOIC LESION DIRECTED AND TRANSITION ZONE
PATIENT SELECTION GUIDE. finding the right fit
 PATIENT SELECTION GUIDE finding the right fit IDENTIFYING PATIENTS Rezūm, a new minimally invasive treatment, is now available to offer patients as a first-line BPH therapy. BPH TREATMENT OPTIONS Behavior
PATIENT SELECTION GUIDE finding the right fit IDENTIFYING PATIENTS Rezūm, a new minimally invasive treatment, is now available to offer patients as a first-line BPH therapy. BPH TREATMENT OPTIONS Behavior
Prostate cancer diagnosis: should patients with prostate specific antigen >10 ng/ml have stratified prostate biopsy protocols?
 Cancer Detection and Prevention 32 (2009) 34 38 www.elsevier.com/locate/cdp Prostate cancer diagnosis: should patients with prostate specific antigen >0 ng/ml have stratified prostate biopsy protocols?
Cancer Detection and Prevention 32 (2009) 34 38 www.elsevier.com/locate/cdp Prostate cancer diagnosis: should patients with prostate specific antigen >0 ng/ml have stratified prostate biopsy protocols?
Shrestha A, Chalise PR, Sharma UK, Gyawali PR, Shrestha GK, Joshi BR. Department of Surgery, TU Teaching Hospital, Maharajgunj, Kathmandu, Nepal
 Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
NIH Public Access Author Manuscript J Urol. Author manuscript; available in PMC 2010 May 4.
 NIH Public Access Author Manuscript Published in final edited form as: J Urol. 2009 December ; 182(6): 2819 2824. doi:10.1016/j.juro.2009.08.086. Intravesical Prostatic Protrusion in Men in Olmsted County,
NIH Public Access Author Manuscript Published in final edited form as: J Urol. 2009 December ; 182(6): 2819 2824. doi:10.1016/j.juro.2009.08.086. Intravesical Prostatic Protrusion in Men in Olmsted County,
Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy?
 Original Article Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy? Sherif Azab 1, Ayman Osama 2, Mona Rafaat 3 1 Urology Department, Faculty
Original Article Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy? Sherif Azab 1, Ayman Osama 2, Mona Rafaat 3 1 Urology Department, Faculty
Review of Clinical Manifestations of Biochemicallyadvanced Prostate Cancer Cases
 Original Article Review of Clinical Manifestations of Biochemicallyadvanced Prostate Cancer Cases Edmund Chiong, 1,2 Alvin Fung Wean Wong, 2 Yiong Huak Chan 3 and Chong Min Chin, 1,2 1 Department of Surgery,
Original Article Review of Clinical Manifestations of Biochemicallyadvanced Prostate Cancer Cases Edmund Chiong, 1,2 Alvin Fung Wean Wong, 2 Yiong Huak Chan 3 and Chong Min Chin, 1,2 1 Department of Surgery,
Transperineal ultrasound-guided biopsy of the prostate gland
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient biopsy of the prostate gland affix patient label What is a transperineal (TP) ultrasound-guided prostate
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient biopsy of the prostate gland affix patient label What is a transperineal (TP) ultrasound-guided prostate
Is Prostate Biopsy Essential to Diagnose Prostate Cancer in the Older Patient with Extremely High Prostate-Specific Antigen?
 www.kjurology.org http://dx.doi.org/1.4111/kju.1.3..8 Urological Oncology Is Prostate Biopsy Essential to Diagnose Prostate Cancer in the Older Patient with Extremely High Prostate-Specific Antigen? Jee
www.kjurology.org http://dx.doi.org/1.4111/kju.1.3..8 Urological Oncology Is Prostate Biopsy Essential to Diagnose Prostate Cancer in the Older Patient with Extremely High Prostate-Specific Antigen? Jee
Prostate Biopsy in the Left Lateral Decubitus Position is Less Painful than Prostate Biopsy in the Lithotomy Position: A Randomized Controlled Trial
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.87 Urological Oncology Prostate Biopsy in the Left Lateral Decubitus Position is Less Painful than Prostate Biopsy in the Lithotomy Position: A
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.87 Urological Oncology Prostate Biopsy in the Left Lateral Decubitus Position is Less Painful than Prostate Biopsy in the Lithotomy Position: A
Attending for your Prostate Scan
 Attending for your Prostate Scan Patient Information The aim of this booklet is to give you enough information: To help you prepare for your hospital visit To give properly informed consent for the procedure
Attending for your Prostate Scan Patient Information The aim of this booklet is to give you enough information: To help you prepare for your hospital visit To give properly informed consent for the procedure
Dichotomous Estimation of Prostate Volume: A Diagnostic Study of the Accuracy of the Digital Rectal Examination
 pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 December 31(3): 220-225 http://dx.doi.org/10.5534/wjmh.2013.31.3.220 Original Article Dichotomous Estimation of Prostate Volume: A Diagnostic
pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 December 31(3): 220-225 http://dx.doi.org/10.5534/wjmh.2013.31.3.220 Original Article Dichotomous Estimation of Prostate Volume: A Diagnostic
RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, PATIENTS WITH BENIGN PROSTATIC HYPERPLASIA
 American Urological Association symptom index for BPH RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, AND DISEASE-SPECIFIC QUALITY OF LIFE QUESTION IN PATIENTS WITH
American Urological Association symptom index for BPH RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, AND DISEASE-SPECIFIC QUALITY OF LIFE QUESTION IN PATIENTS WITH
The TRUS guided prostate extended biopsy in the detection of prostate cancer
 Mædica - a Journal of Clinical Medicine ORIGIN RIGINAL PAPERS The TRUS guided prostate extended biopsy in the detection of prostate cancer Assoc. Prof. V. AMBERT, MD, PhD; A. ATEIA, MD; I. CHIRA, MD, PhD;
Mædica - a Journal of Clinical Medicine ORIGIN RIGINAL PAPERS The TRUS guided prostate extended biopsy in the detection of prostate cancer Assoc. Prof. V. AMBERT, MD, PhD; A. ATEIA, MD; I. CHIRA, MD, PhD;
INTEROBSERVER VARIATION OF PROSTATIC VOLUME ESTIMATION WITH DIGITAL RECTAL EXAMINATION BY UROLOGICAL STAFFS WITH DIFFERENT EXPERIENCES
 Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology DIGITAL RECTAL EXAMINATION BY UROLOGICAL STAFFS Vol. 30 (6): 466-471, November - December, 2004 INTEROBSERVER
Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology DIGITAL RECTAL EXAMINATION BY UROLOGICAL STAFFS Vol. 30 (6): 466-471, November - December, 2004 INTEROBSERVER
Are extended biopsies really necessary to improve prostate cancer detection?
 (2003) 6, 250 255 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Are extended biopsies really necessary to improve prostate cancer detection? R Damiano*,1, R
(2003) 6, 250 255 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Are extended biopsies really necessary to improve prostate cancer detection? R Damiano*,1, R
PERIPROSTATIC LOCAL ANESTHESIA IN TRANSRECTAL ULTRASOUND-GUIDED PROSTATE BIOPSY: IS IT POSSIBLE TO IMPROVE PAIN TOLERANCE?
 Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (4): 323-329, July - August, 2002 PERIPROSTATIC LOCAL ANESTHESIA IN TRANSRECTAL ULTRASOUND-GUIDED
Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (4): 323-329, July - August, 2002 PERIPROSTATIC LOCAL ANESTHESIA IN TRANSRECTAL ULTRASOUND-GUIDED
Key Words: prostatic neoplasms, biopsy, infection, sepsis, treatment outcome
 Infection/Inflammation The Impact of Repeat Biopsies on Infectious Complications in Men with Prostate Cancer on Active Surveillance Behfar Ehdaie,* Emily Vertosick,* Massimiliano Spaliviero,* Anna Giallo-Uvino,*
Infection/Inflammation The Impact of Repeat Biopsies on Infectious Complications in Men with Prostate Cancer on Active Surveillance Behfar Ehdaie,* Emily Vertosick,* Massimiliano Spaliviero,* Anna Giallo-Uvino,*
Efficacy of a short prophylaxis with tranexamic acid on hemostasis during transrectal prostate biopsy in patients taking oral anti-platelet treatment
 JBUON 2016; 21(3): 680-684 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Efficacy of a short prophylaxis with tranexamic acid on hemostasis during
JBUON 2016; 21(3): 680-684 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Efficacy of a short prophylaxis with tranexamic acid on hemostasis during
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Increasing Awareness, Diagnosis, and Treatment of BPH, LUTS, and EP
 Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
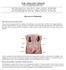
A schematic of the rectal probe in contact with the prostate is show in this diagram.
 Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
= 0.62, P <0.001) with important clinical exceptions. There was negative correlation between the PV and Qmax (r s
 Original Article 60 Relationships between Prostatic Volume and Intravesical Prostatic Protrusion on Transabdominal Ultrasound and Benign Prostatic Obstruction in Patients with Lower Urinary Tract Symptoms
Original Article 60 Relationships between Prostatic Volume and Intravesical Prostatic Protrusion on Transabdominal Ultrasound and Benign Prostatic Obstruction in Patients with Lower Urinary Tract Symptoms
Prostate Cancer 3/15/2017. CEUS of the Prostate. The Prostate Cancer Screening Dilemma Data. Incidence: 161,360 Deaths: 26,730
 Prostate Cancer CEUS of the Prostate 2017 Data Incidence: 161,360 Deaths: 26,730 Third leading cause of cancer death in men (after lung & Professor of Radiology & Urology colon Ca) Co-Director, Jefferson
Prostate Cancer CEUS of the Prostate 2017 Data Incidence: 161,360 Deaths: 26,730 Third leading cause of cancer death in men (after lung & Professor of Radiology & Urology colon Ca) Co-Director, Jefferson
european urology 53 (2008)
 european urology 53 (2008) 967 975 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Topical Prilocaine-Lidocaine Cream Combined with Peripheral Nerve Block Improves
european urology 53 (2008) 967 975 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Topical Prilocaine-Lidocaine Cream Combined with Peripheral Nerve Block Improves
Increasing Hospital Admission Rates for Urological Complications After Transrectal Ultrasound Guided Prostate Biopsy
 Increasing Hospital Admission Rates for Urological Complications After Transrectal Ultrasound Guided Prostate Biopsy Robert K. Nam,*, Refik Saskin, Yuna Lee, Ying Liu, Calvin Law, Laurence H. Klotz, D.
Increasing Hospital Admission Rates for Urological Complications After Transrectal Ultrasound Guided Prostate Biopsy Robert K. Nam,*, Refik Saskin, Yuna Lee, Ying Liu, Calvin Law, Laurence H. Klotz, D.
An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms
 Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Hypoechoic Rim of Chronically Inflamed Prostate, as Seen at TRUS: Histopathologic Findings
 Hypoechoic Rim of Chronically Inflamed Prostate, as Seen at TRUS: Histopathologic Findings Hak Jong Lee, MD 1 Ghee Young Choe, MD 2 Chang Gyu Seong, MD 3 Seung Hyup Kim, MD 4 Index terms: Prostate Prostate,
Hypoechoic Rim of Chronically Inflamed Prostate, as Seen at TRUS: Histopathologic Findings Hak Jong Lee, MD 1 Ghee Young Choe, MD 2 Chang Gyu Seong, MD 3 Seung Hyup Kim, MD 4 Index terms: Prostate Prostate,
One Stop Prostate Biopsy Protocol Author Consultation Date Approved
 One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
One Stop Prostate Biopsy Protocol Author Consultation Date Approved Urology Nurse Practioner PROTOCOL FOR MEN ATTENDING A ONE STOP PROSTATE BIOPSY CLINIC RATIONALE Prostate cancer is the most common cancer
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
Developing a new score system for patients with PSA ranging from 4 to 20 ng/ ml to improve the accuracy of PCa detection
 DOI 10.1186/s40064-016-3176-3 RESEARCH Open Access Developing a new score system for patients with PSA ranging from 4 to 20 ng/ ml to improve the accuracy of PCa detection Yuxiao Zheng, Yuan Huang, Gong
DOI 10.1186/s40064-016-3176-3 RESEARCH Open Access Developing a new score system for patients with PSA ranging from 4 to 20 ng/ ml to improve the accuracy of PCa detection Yuxiao Zheng, Yuan Huang, Gong
Screening for Prostate Cancer
 Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
The Chances of Subsequent Cancer Detection in Patients with a PSA > 20 ng/ml and an Initial Negative Biopsy
 Research Article TheScientificWorldJOURNAL (2009) 9, 343 348 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.47 The Chances of Subsequent Cancer Detection in Patients with a PSA > 20 ng/ml and an Initial
Research Article TheScientificWorldJOURNAL (2009) 9, 343 348 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.47 The Chances of Subsequent Cancer Detection in Patients with a PSA > 20 ng/ml and an Initial
Clinical Studies with Speman in Cases of Benign Enlargement of Prostate
 [The Indian Practitioner (1971): 6, 281] Clinical Studies with Speman in Cases of Benign Enlargement of Prostate Agarwal, V.K., M.S., F.I.C.S., Professor of Surgery, and Gupta, R.K., M.B.,B.S., Research
[The Indian Practitioner (1971): 6, 281] Clinical Studies with Speman in Cases of Benign Enlargement of Prostate Agarwal, V.K., M.S., F.I.C.S., Professor of Surgery, and Gupta, R.K., M.B.,B.S., Research
Chapter 4: Research and Future Directions
 Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate
 Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Implantation of fiducial markers for image guidance in prostate radiotherapy: patient-reported toxicity
 The British Journal of Radiology, 82 (2009), 941 945 Implantation of fiducial markers for image guidance in prostate radiotherapy: patient-reported toxicity 1 Ş İĞDEM, MD, 2 H AKPINAR, MD, 1 G ALÇO,MD,
The British Journal of Radiology, 82 (2009), 941 945 Implantation of fiducial markers for image guidance in prostate radiotherapy: patient-reported toxicity 1 Ş İĞDEM, MD, 2 H AKPINAR, MD, 1 G ALÇO,MD,
10 5 cfu/ml logistic regression duration of catheterisation, sex,
 Table I: data extraction on study characteristics Study study population outcome urine sampling definition of bacteriuria statistical model odds ratios of the candidate for for culture Inclusion criteria
Table I: data extraction on study characteristics Study study population outcome urine sampling definition of bacteriuria statistical model odds ratios of the candidate for for culture Inclusion criteria
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
Individualized prostate biopsy strategy for Chinese patients with different prostate-specific antigen levels
 DOI: 10.1111/j.1745-7262.2008.00345.x www.asiaandro.com. Clinical Experience. Individualized prostate biopsy strategy for Chinese patients with different prostate-specific antigen levels Bo Dai 1,4, Ding-Wei
DOI: 10.1111/j.1745-7262.2008.00345.x www.asiaandro.com. Clinical Experience. Individualized prostate biopsy strategy for Chinese patients with different prostate-specific antigen levels Bo Dai 1,4, Ding-Wei
Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate volume matter?
 ORIGINAL ARTICLE Gulhane Med J 2018;60: 14-18 Gülhane Faculty of Medicine 2018 doi: 10.26657/gulhane.00010 Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate
ORIGINAL ARTICLE Gulhane Med J 2018;60: 14-18 Gülhane Faculty of Medicine 2018 doi: 10.26657/gulhane.00010 Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate
Effect of patient position on pain scales during transrectal ultrasound-guided prostate biopsy
 Original Article - Urological Oncology Korean J Urol 2015;56:449-454. pissn 2005-6737 eissn 2005-6745 Effect of patient position on pain scales during transrectal ultrasound-guided prostate biopsy Yeong
Original Article - Urological Oncology Korean J Urol 2015;56:449-454. pissn 2005-6737 eissn 2005-6745 Effect of patient position on pain scales during transrectal ultrasound-guided prostate biopsy Yeong
MRI in the Enhanced Detection of Prostate Cancer: What Urologists Need to Know
 MRI in the Enhanced Detection of Prostate Cancer: What Urologists Need to Know Michael S. Cookson, MD, FACS Professor and Chair Department of Urology Director of Prostate and Urologic Oncology University
MRI in the Enhanced Detection of Prostate Cancer: What Urologists Need to Know Michael S. Cookson, MD, FACS Professor and Chair Department of Urology Director of Prostate and Urologic Oncology University
Can men with prostates sized 80 ml or larger be managed conservatively?
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Serum Prostate-Specific Antigen as a Predictor of Prostate Volume in the Community: The Krimpen Study
 european urology 51 (2007) 1645 1653 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Hyperplasia Serum Prostate-Specific Antigen as a Predictor of Prostate
european urology 51 (2007) 1645 1653 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Hyperplasia Serum Prostate-Specific Antigen as a Predictor of Prostate
Preoperative Gleason score, percent of positive prostate biopsies and PSA in predicting biochemical recurrence after radical prostatectomy
 JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
Histopathological Study of Transrectal Ultrasound Guided Biopsies of Prostate
 ORIGINAL ARTICLE Histopathological Study of Transrectal Ultrasound Guided Biopsies of Prostate in Patients With Raised Serum Prostate Specific Antigen Prabha Rathour 1, Hetal Jani 2, Urvi Parikh 3, Hansa
ORIGINAL ARTICLE Histopathological Study of Transrectal Ultrasound Guided Biopsies of Prostate in Patients With Raised Serum Prostate Specific Antigen Prabha Rathour 1, Hetal Jani 2, Urvi Parikh 3, Hansa
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Owing to the widespread use of prostate specific antigen (PSA)
 ORIGINAL RESEARCH Subsequent prostate cancer detection in patients with prostatic intraepithelial neoplasia or atypical small acinar proliferation Moamen M. Amin, MD; Suganthiny Jeyaganth, MSc; Nader Fahmy,
ORIGINAL RESEARCH Subsequent prostate cancer detection in patients with prostatic intraepithelial neoplasia or atypical small acinar proliferation Moamen M. Amin, MD; Suganthiny Jeyaganth, MSc; Nader Fahmy,
BJUI. Evaluation of a novel precision template-guided biopsy system for detecting prostate cancer
 2008 The Authors. Journal compilation 2008 BJU International Original Article TEMPLATE-BASED PROSTATE BIOPSY SYSTEM MEGWALU et al. BJUI BJU INTERNATIONAL Evaluation of a novel precision template-guided
2008 The Authors. Journal compilation 2008 BJU International Original Article TEMPLATE-BASED PROSTATE BIOPSY SYSTEM MEGWALU et al. BJUI BJU INTERNATIONAL Evaluation of a novel precision template-guided
@Original Contribution
 Pergamon Ultrasound in Med. & Biol., Vol. 21, No. 1, pp. 11-16, 1995 Copyright 0 1995 Elsevier Science Ltd P&ted in the USA. All rights reserved 0301.5629/95 $9.50 + 00 0301-5629(94)00084-O @Original Contribution
Pergamon Ultrasound in Med. & Biol., Vol. 21, No. 1, pp. 11-16, 1995 Copyright 0 1995 Elsevier Science Ltd P&ted in the USA. All rights reserved 0301.5629/95 $9.50 + 00 0301-5629(94)00084-O @Original Contribution
The Role of TURP in the Detection of Prostate Cancer in BPH Patients with Previously Negative Prostate Biopsy
 www.kjurology.org DOI:10.4111/kju.2010.51.5.313 Urological Oncology The Role of TURP in the Detection of Prostate Cancer in BPH Patients with Previously Negative Prostate Biopsy Dae Keun Kim, Sang Jin
www.kjurology.org DOI:10.4111/kju.2010.51.5.313 Urological Oncology The Role of TURP in the Detection of Prostate Cancer in BPH Patients with Previously Negative Prostate Biopsy Dae Keun Kim, Sang Jin
BLADDER PROSTATE PENIS TESTICLES BE YO ND YO UR CA NC ER
 BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
EUROPEAN UROLOGY 58 (2010)
 EUROPEAN UROLOGY 58 (2010) 551 558 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Prostate Cancer Prevention Trial and European Randomized Study of Screening
EUROPEAN UROLOGY 58 (2010) 551 558 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Prostate Cancer Prevention Trial and European Randomized Study of Screening
Prostate Biopsy Michael Holmes. FRACS (Urology)
 Prostate Biopsy Michael Holmes FRACS (Urology) Why have a Prostate biopsy? A prostate biopsy will have been recommended if your PSA. was elevated The rectal examination was abnormal or wrong The PSA is
Prostate Biopsy Michael Holmes FRACS (Urology) Why have a Prostate biopsy? A prostate biopsy will have been recommended if your PSA. was elevated The rectal examination was abnormal or wrong The PSA is
UV-2005/01. Chronic Prostatitis and Chronic Pelvic Pain Syndrom (CP/CPPS) Karl-Bickleder-Str. 44C Straubing - Germany
 SYNOPSIS UV-2005/01 Title: Short Title: Indication: Phase: Study Code: Study Director Co-ordinating Investigator: Study Centres: Multicentre, randomised, double-blind, placebo-controlled clinical study
SYNOPSIS UV-2005/01 Title: Short Title: Indication: Phase: Study Code: Study Director Co-ordinating Investigator: Study Centres: Multicentre, randomised, double-blind, placebo-controlled clinical study
The Royal Marsden. Prostate case study. Presented by Mr Alan Thompson Consultant Urological Surgeon
 Prostate case study Presented by Mr Alan Thompson Consultant Urological Surgeon 2 Part one Initial presentation A 62 year old male solicitor attends your GP surgery. He has rarely seen you over the last
Prostate case study Presented by Mr Alan Thompson Consultant Urological Surgeon 2 Part one Initial presentation A 62 year old male solicitor attends your GP surgery. He has rarely seen you over the last
ONCOLOGY LETTERS 8: , 2014
 1834 Systematic 12 and 13 core transrectal ultrasound or magnetic resonance imaging guided biopsies significantly improve prostate cancer detection rate: A single center 13 year experience GONG CHENG *,
1834 Systematic 12 and 13 core transrectal ultrasound or magnetic resonance imaging guided biopsies significantly improve prostate cancer detection rate: A single center 13 year experience GONG CHENG *,
Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer
 ORIGINAL ARTICLE Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer Chang-Chi Chang, Junne-Yih Kuo*, Kuang-Kuo Chen, Alex Tong-Long Lin, Yen-Hwa Chang, Howard
ORIGINAL ARTICLE Transurethral Prostatic Resection for Acute Urinary Retention in Patients with Prostate Cancer Chang-Chi Chang, Junne-Yih Kuo*, Kuang-Kuo Chen, Alex Tong-Long Lin, Yen-Hwa Chang, Howard
or more transrectal ultrasonography (TRUS)-guided ng/ml and 39% if it was 20.0 ng/ml. of >10 ng/ml have prostate cancer [3], many other
![or more transrectal ultrasonography (TRUS)-guided ng/ml and 39% if it was 20.0 ng/ml. of >10 ng/ml have prostate cancer [3], many other or more transrectal ultrasonography (TRUS)-guided ng/ml and 39% if it was 20.0 ng/ml. of >10 ng/ml have prostate cancer [3], many other](/thumbs/92/108155308.jpg) BJU International (1999), 83, 34 38 Elevated serum prostate specific antigen levels in conjunction with an initial prostatic biopsy negative for carcinoma: who should undergo a repeat biopsy? G.C. DURKAN
BJU International (1999), 83, 34 38 Elevated serum prostate specific antigen levels in conjunction with an initial prostatic biopsy negative for carcinoma: who should undergo a repeat biopsy? G.C. DURKAN
PSA Screening and Prostate Cancer. Rishi Modh, MD
 PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Trans-rectal Ultrasound Scan and Biopsy (TRUSS)
 Trans-rectal Ultrasound Scan and Biopsy (TRUSS) What is the prostate gland? The prostate is a small gland the size of a walnut. It is found at the base of the bladder and surrounds the urethra (water pipe).
Trans-rectal Ultrasound Scan and Biopsy (TRUSS) What is the prostate gland? The prostate is a small gland the size of a walnut. It is found at the base of the bladder and surrounds the urethra (water pipe).
AUCKLAND REGIONAL UROLOGY GUIDELINES AND REFERRAL RECOMMENDATIONS
 AUCKLAND REGIONAL UROLOGY GUIDELINES AND REFERRAL RECOMMENDATIONS This document outlines the urological conditions currently funded at Auckland District Health Board (ADHB), Counties Manukau District Health
AUCKLAND REGIONAL UROLOGY GUIDELINES AND REFERRAL RECOMMENDATIONS This document outlines the urological conditions currently funded at Auckland District Health Board (ADHB), Counties Manukau District Health
Executive Summary. Non-drug local procedures for treatment of benign prostatic hyperplasia 1. IQWiG Reports - Commission No.
 IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
The diagnostic value of abdominal ultrasound, urine cytology and prostate-specific antigen testing in the lower urinary tract symptoms clinic
 ORIGINAL PAPER The diagnostic value of abdominal ultrasound, urine cytology and prostate-specific antigen testing in the lower urinary tract symptoms clinic N. S. Patel, 1 C. Blick, 1 P. V. S. Kumar, 2
ORIGINAL PAPER The diagnostic value of abdominal ultrasound, urine cytology and prostate-specific antigen testing in the lower urinary tract symptoms clinic N. S. Patel, 1 C. Blick, 1 P. V. S. Kumar, 2
Diagnostic Value of Finger-guided Prostate Nodule Biopsy Combined With Systemic Random Biopsy
 ORIGINAL ARTICLE Diagnostic Value of Finger-guided Prostate Nodule Biopsy Combined With Systemic Random Biopsy I-Ni Chiang, 1,2 Shang-Jen Chang, 3 Yeong-Shiau Pu, 1,2 Kuo-How Huang, 1,2 Hong-Jen Yu, 1,2
ORIGINAL ARTICLE Diagnostic Value of Finger-guided Prostate Nodule Biopsy Combined With Systemic Random Biopsy I-Ni Chiang, 1,2 Shang-Jen Chang, 3 Yeong-Shiau Pu, 1,2 Kuo-How Huang, 1,2 Hong-Jen Yu, 1,2
Ultrasound-guided transrectal extended prostate biopsy: a prospective study
 DOI: 10.1111/j.1745-7262.2005.00019.x. Original Article. Ultrasound-guided transrectal extended prostate biopsy: a prospective study Mohammed Ahmed Al-Ghazo, Ibrahim Fathi Ghalayini, Ismail Ibrahim Matalka
DOI: 10.1111/j.1745-7262.2005.00019.x. Original Article. Ultrasound-guided transrectal extended prostate biopsy: a prospective study Mohammed Ahmed Al-Ghazo, Ibrahim Fathi Ghalayini, Ismail Ibrahim Matalka
Title: Prostate Specific Antigen (PSA) for Prostate Cancer Screening: A Clinical Review
 Title: Prostate Specific Antigen (PSA) for Prostate Cancer Screening: A Clinical Review Date: November 26, 2007 Context and policy issues: Prostate cancer is the most common tumor in men, and is one of
Title: Prostate Specific Antigen (PSA) for Prostate Cancer Screening: A Clinical Review Date: November 26, 2007 Context and policy issues: Prostate cancer is the most common tumor in men, and is one of
Cancer. Description. Section: Surgery Effective Date: October 15, 2016 Subsection: Original Policy Date: September 9, 2011 Subject:
 Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
Transperineal Biopsy of the Prostate
 Transperineal Biopsy of the Prostate Department of Urology Patient Information What What is a is Prostate? a Prostate? The Prostate is an organ forming part of the male reproductive system. It is located
Transperineal Biopsy of the Prostate Department of Urology Patient Information What What is a is Prostate? a Prostate? The Prostate is an organ forming part of the male reproductive system. It is located
Title of Research Thesis:
 Eastern Michigan University By Fatai Osinowo Adviser s Name: Dr. Stephen Sonstein, PhD Title of Research Thesis: A sub-analyses from the Benign Prostatic Hyperplasia (BPH) Registry and Patient survey:
Eastern Michigan University By Fatai Osinowo Adviser s Name: Dr. Stephen Sonstein, PhD Title of Research Thesis: A sub-analyses from the Benign Prostatic Hyperplasia (BPH) Registry and Patient survey:
Introduction. Key Words: high-grade prostatic intraepithelial neoplasia, HGPIN, radical prostatectomy, prostate biopsy, insignificant prostate cancer
 Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Prostate Gland Volume and Its Relationship to Complications of Benign Prostatic Enlargement
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 6 Ver. II (Jun. 2015), PP 33-37 www.iosrjournals.org Prostate Gland Volume and Its Relationship
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 6 Ver. II (Jun. 2015), PP 33-37 www.iosrjournals.org Prostate Gland Volume and Its Relationship
Having a transperineal prostate biopsy
 Having a transperineal prostate biopsy This leaflet should help to answer some of your questions about having a transperineal prostate biopsy. If you have any further questions, please speak to a doctor
Having a transperineal prostate biopsy This leaflet should help to answer some of your questions about having a transperineal prostate biopsy. If you have any further questions, please speak to a doctor
Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano
 Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
PSA To screen or not to screen? Darrel Drachenberg, MD, FRCSC
 PSA To screen or not to screen? Darrel Drachenberg, MD, FRCSC Disclosures Faculty / Speaker s name: Darrel Drachenberg Relationships with commercial interests: Grants/Research Support: None Speakers Bureau/Honoraria:
PSA To screen or not to screen? Darrel Drachenberg, MD, FRCSC Disclosures Faculty / Speaker s name: Darrel Drachenberg Relationships with commercial interests: Grants/Research Support: None Speakers Bureau/Honoraria:
Setting The setting was hospital. The economic analysis was conducted in Toronto, Montreal and Laval, Canada.
 Electromotive drug administration of lidocaine as an alternative anesthesia for transurethral surgery Jewett M A, Valiquette L, Sampson H A, Katz J, Fradet Y, Redelmeier D A Record Status This is a critical
Electromotive drug administration of lidocaine as an alternative anesthesia for transurethral surgery Jewett M A, Valiquette L, Sampson H A, Katz J, Fradet Y, Redelmeier D A Record Status This is a critical
Computer simulated additional deep apical biopsy enhances cancer detection in palpably benign prostate gland
 Blackwell Publishing AsiaMelbourne, AustraliaIJUInternational Journal of Urology0919-81722006 Blackwell Publishing Asia Pty Ltd? 200613?12901295Original ArticleAdditional apical biopsy in prostatic gland
Blackwell Publishing AsiaMelbourne, AustraliaIJUInternational Journal of Urology0919-81722006 Blackwell Publishing Asia Pty Ltd? 200613?12901295Original ArticleAdditional apical biopsy in prostatic gland
CHAPTER 6. M.D. Eckhardt, G.E.P.M. van Venrooij, T.A. Boon. hoofdstuk :49 Pagina 89
 hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
Elevated PSA. Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017
 Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Prostate Case Scenario 1
 Prostate Case Scenario 1 H&P 5/12/16: A 57-year-old Hispanic male presents with frequency of micturition, urinary urgency, and hesitancy associated with a weak stream. Over the past several weeks, he has
Prostate Case Scenario 1 H&P 5/12/16: A 57-year-old Hispanic male presents with frequency of micturition, urinary urgency, and hesitancy associated with a weak stream. Over the past several weeks, he has
Clinical Study Single Dose of Levofloxacin versus Three Dosages for Prophylaxis in Prostate Biopsy
 International Scholarly Research Notices, Article ID 875670, 4 pages http://dx.doi.org/10.1155/2014/875670 Clinical Study Single Dose of Levofloxacin versus Three Dosages for Prophylaxis in Prostate Biopsy
International Scholarly Research Notices, Article ID 875670, 4 pages http://dx.doi.org/10.1155/2014/875670 Clinical Study Single Dose of Levofloxacin versus Three Dosages for Prophylaxis in Prostate Biopsy
Does a New Ultrasound Probe Change the Complication Rates of Transrectal Ultrasound-guided Needle Biopsies of the Prostate?
 Does a New Ultrasound Probe Change the Complication Rates of Transrectal Ultrasound-guided Needle Biopsies of the Prostate? THORSTEN H. ECKE 1, HOLGER GERULLIS 2,3, CHRISTOPH J. HEUCK 4, PETER BARTEL 1,
Does a New Ultrasound Probe Change the Complication Rates of Transrectal Ultrasound-guided Needle Biopsies of the Prostate? THORSTEN H. ECKE 1, HOLGER GERULLIS 2,3, CHRISTOPH J. HEUCK 4, PETER BARTEL 1,
Ultrasonographically Guided Biopsy of the Prostate Gland
 Review Article Ultrasonographically Guided Biopsy of the Prostate Gland Andrew L. Altman, MD, Martin I. Resnick, MD Abbreviations BPH, benign prostatic hyperplasia; PIN, prostatic intraepithelial neoplasia;
Review Article Ultrasonographically Guided Biopsy of the Prostate Gland Andrew L. Altman, MD, Martin I. Resnick, MD Abbreviations BPH, benign prostatic hyperplasia; PIN, prostatic intraepithelial neoplasia;
Original Article - Lasers in Urology. Min Ho Lee, Hee Jo Yang, Doo Sang Kim, Chang Ho Lee, Youn Soo Jeon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
The Effect of Intrarectal Lidocaine Gel Instillation before Transrectal Ultrasound Guided Prostate Biopsy
 Original Article ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2016.11.3.97 Urogenit Tract Infect 2016;11(3):97-102 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2016.11.3.97&domain=pdf&date_stamp=2016-12-25
Original Article ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2016.11.3.97 Urogenit Tract Infect 2016;11(3):97-102 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2016.11.3.97&domain=pdf&date_stamp=2016-12-25
Central European Journal of Urology
 38 O R I G I N A L P A P E R UROLOGICAL ONCOLOGY Comparing use of lidocaine periprostatic nerve block and diclofenac suppository alone for patients undergoing transrectal ultrasound guided prostate biopsy
38 O R I G I N A L P A P E R UROLOGICAL ONCOLOGY Comparing use of lidocaine periprostatic nerve block and diclofenac suppository alone for patients undergoing transrectal ultrasound guided prostate biopsy
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet. Under review
 Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
You have been booked for a. Flexible Cystoscopy. Under Local Anaesthetic
 You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
Benign prostatic hyperplasia (BPH) is one of the
 MISCELLANEOUS Safety and Efficacy of Bipolar Versus Monopolar Transurethral Resection of the Prostate: A Comparative Study Erkan Hirik, 1 Aliseydi Bozkurt, 1 Mehmet Karabakan, 1 * Huseyin Aydemir, 2 Binhan
MISCELLANEOUS Safety and Efficacy of Bipolar Versus Monopolar Transurethral Resection of the Prostate: A Comparative Study Erkan Hirik, 1 Aliseydi Bozkurt, 1 Mehmet Karabakan, 1 * Huseyin Aydemir, 2 Binhan
BJUI. Avoidable iatrogenic complications of urethral catheterization and inadequate intern training in a tertiary-care teaching hospital
 . JOURNAL COMPILATION 2009 BJU INTERNATIONAL Lower Urinary Tract IATROGENIC COMPLICATIONS OF URETHRAL CATHETERIZATION AND INADEQUATE INTERN TRAINING THOMAS et al. BJUI BJU INTERNATIONAL Avoidable iatrogenic
. JOURNAL COMPILATION 2009 BJU INTERNATIONAL Lower Urinary Tract IATROGENIC COMPLICATIONS OF URETHRAL CATHETERIZATION AND INADEQUATE INTERN TRAINING THOMAS et al. BJUI BJU INTERNATIONAL Avoidable iatrogenic
