Single-stage debridement and instrumentation for pyogenic spinal infections
|
|
|
- Thomas Hawkins
- 5 years ago
- Views:
Transcription
1 Neurosurg Focus 17 (6):E5, 2004 Single-stage debridement and instrumentation for pyogenic spinal infections ALFRED T. OGDEN, M.D., AND MICHAEL G. KAISER, M.D. Department of Neurological Surgery, Columbia University, New York, New York Surgical intervention is indicated for pyogenic vertebral discitis and osteomyelitis in patients in whom medical therapy has failed, and in those with neurological compromise, mechanical instability, epidural abscess, or intractable pain. Surgical management has evolved to include single-stage operations for debridement and stabilization as well as more aggressive reconstruction strategies with respect to instrumentation. A review of the literature demonstrates excellent outcomes with single-stage operations and placement of hardware wherever it is required. Using this method, the authors have treated 16 patients without a single incidence of recurrent infection or hardware failure after almost 2 years of follow up. KEY WORDS spinal infection osteomyelitis erythrocyte sedimentation rate C-reactive protein spinal instrumentation debridement The vertebrae are the most common sites for hematogenously acquired osteomyelitis. 38 Most patients with PVDO can be treated conservatively with long-term antibiotic therapy. 3,4,6,7,9,20,21,35,36 Surgical debridement is usually reserved for patients in whom medical management of the disease has failed, those with neurological compromise, unstable mechanical deformity, an epidural abscess, or intractable pain. 11,13,14,24,28,31 The decision whether to intercede surgically is often colored by the medical comorbidities endemic in this patient population. The patient s overall constitution is particularly important in these cases, given the extensive surgery often needed to stabilize the spine after debridement. Because hardware placed for fusion operations in noninfected patients has been shown to increase postoperative infection rates, many practitioners have expressed understandable concern about the placement of instrumentation in an infected patient. Historically, many have preferred to prescribe bed rest and prolonged external bracing rather than placing internal constructs. Others have advocated a staged operation with a period of antibiotic therapy bridging the debridement and instrumentation procedures. 2,12,19,22 The desire to effect more rapid mobilization has led to a progressively more aggressive strategy with regard to placement of instrumentation. In recent series excellent outcomes have been demonstrated for single-stage procedures in which hardware placement is performed within and adjacent to debrided areas, and these studies have not shown significantly increased rates of infection recurrence. 15,17,28 Abbreviations used in this paper: CRP = C-reactive protein; ESR = erythrocyte sedimentation rate; PVDO = pyogenic vertebral discitis and osteomyelitis. SPINAL INFECTIONS Common Pathogens In North America, spinal infections are typically the result of methicillin-sensitive Staphylococcus aureus that spreads hematogenously in individuals with medical conditions that predispose them to infections. 3,4,6,7,9,20,21,35,36 Gram-negative rods account for another large percentage and are the most prevalent infecting organisms in the intravenous drug using population. 33 Brucellar vertebral osteomyelitis is common in countries where unpasteurized milk is consumed, 3 and even in first world countries, tuberculous vertebral osteomyelitis comprises up to 40% of the cases in some series. 7,9,23 Clinical Presentation and Evaluation Back pain is frequently the only presenting symptom, which means that many cases of PVDO go undiagnosed for prolonged periods of time. Fever and an elevated white blood cell count are usually not present, and the diagnosis is often made when symptoms of back pain result in radiographic evaluation. When PVDO is suspected, the serum ESR and CRP level should be assayed because elevated values on these tests are more than 80% sensitive for this diagnosis. 4,7 The majority of patients with spinal infections can be treated effectively with a 6- to 8-week course of antibiotic drugs and careful monitoring of neurological status, with treatment tailored to the causative organism. 3,4,6, 7,9,20,21,35,36 Blood cultures are positive for bacteria in 50 to 72% of these cases. 3,21,23 When blood cultures are unrevealing, a computerized tomography guided biopsy procedure should be the first option chosen, because this will yield Neurosurg. Focus / Volume 17 / December,
2 A. T. Ogden and M. G. Kaiser an organism between 52 and 68% of the time, and this yield is not greatly increased in specimens obtained during open procedures. 8,21 Medical Management and Follow-Up Protocol At our institution, patients with PVDO receive a 6- to 8- week course of intravenously delivered antibiotic medications, which after a time can be converted to an oral regimen in selected cases. Once an antibiotic regimen is started, patients are assessed with weekly serum ESR and CRP testing and monitored for evidence of neurological decline. The best data regarding ESR and CRP responses to antibiotic therapy are found in pediatric series of acute nonsurgically treated PVDO. In such cases, the ESR should begin to decrease in the 2nd week and to normalize within 3 to 5 weeks, whereas CRP levels should respond more rapidly, decreasing in the first couple of days and normalizing in 1 to 2 weeks. 30,37 In adults, ESR trends are confounded by comorbid medical conditions and the nonspecific elevation in the rate that often occurs with age. In one study of PVDO in adults, 50% of patients who failed to demonstrate a significant decrease in the ESR after 1 month still achieved clinical cures with conservative management. 5 Nevertheless, the ESR is a useful tool in the management of adult PVDO, and the authors of most studies on this disease view a 50 to 66% reduction in the ESR as compatible with eradication of infection. 4,32 There are no published series of medically managed PVDO in adults in whom systematic follow-up review was performed using CRP testing. Surgical Intervention Most authors advocate surgical debridement in cases of failure of medical therapy, neurological compromise, or unstable mechanical deformity. 11,13,14,24,28,31 The presence of an epidural abscess independent of a neurological deficit is a relatively strong indication to operate, although treatment of epidural abscesses with antibiotic drugs alone can be successful in selected cases. 10,18,27,29 The vast majority of PVDO cases involve the anterior and/or middle spinal column. Although an epidural abscess with no significant structural deformity can be treated with simple laminectomy and evacuation, the majority of cases require an approach that allows extensive anterior debridement and reconstruction, followed by placement of a stabilization construct. This presents a conflict between the desire to place adequate instrumentation and concern over placement of a foreign body in an infected individual. These issues must be viewed in the context of the consequences of subjecting patients who are often medically ill to a second operation, prolonged periods of immobility, and weeks to months of external bracing. Authors of retrospective series have reported outcomes obtained using strategies that reflect a continuum of treatment rationales. Investigators have advocated anterior stabilization with allograft or autograft combined with bed rest and bracing, or anterior stabilization with no instrumentation followed by a period of treatment with antibiotic drugs and a second stage for placement of a posterior construct. More recently, the trend has been to perform aggressive debridement with anterior, posterior, or circumferential stabilization at the time of the initial surgery. Some authors have also advocated removal of hardware after there is evidence of fusion to avoid the possibility of reinfection from instrumentation colonized by bacteria. Although there are no prospective data to establish the relative risks and benefits of single-stage compared with two-stage operations, the numerous retrospective series described later and in Table 1 have shown excellent outcomes with the single-stage approach. Literature Review In most series in which single-stage procedures for anterior spinal infections have been described, anterior debridement with placement of allograft or autograft has been used, combined with placement of a posterior stabilizing construct. This approach is based on the premise that instrumentation placed posteriorly involves a second operating field that is not (at least directly) contaminated. The first report in which this strategy was used was published by Fountain 13 in Fountain presented a mixed series of patients, one of whom had destructive PVDO and who was treated with anterior corpectomy and fusion as well as posterior stabilization with Harrington rods. Although the details pertaining to the follow-up review in this individual are lacking, the fusion was apparently successful and the patient was out of bed within 14 days of the procedure. Abramovitz, et al., 1 reported a mixed series of surgically treated spinal infections in which three patients received anterior decompression and fusion with posterior placement of Harrington rods. After a follow-up duration of 1 to 9 months, two patients were ambulatory, with early evidence of bone fusion, and one had died. No other relevant follow-up data were reported. The first series describing the consistent placement of posterior instrumentation at the time of debridement was published in 1988 by Redfern, et al. 26 These authors reported on six patients with PVDO who underwent posterior placement of a Banks Dervin rod in the same operation as a debridement procedure. Two of these patients also received anterior placement of an autologous rib strut graft. Although one patient died of pneumonia 25 days postsurgery and one died of unrelated cardiac causes 6 months later, the remaining four had excellent outcomes. There was one case of troublesome delayed wound healing but no evidence of recurrent infection. In 1993, Graziano and Sidhu 14 reported results obtained in seven patients with PVDO of the thoracic and lumbar spine who were treated with anterior corpectomy and placement of an anterior nonvascularized autogenous strut graft. Six of these patients were stabilized with a posterior fixation construct at the same surgery. The results were excellent, with no recurrence of infection, no pseudarthroses, and evidence of strut graft incorporation in all patients after a mean 25-month follow-up duration. In 1996, Rath, et al., 25 reported on a series of 43 patients with thoracic or lumbar PVDO who were treated entirely via a posterior approach. Eighteen of these patients underwent a single-stage procedure with anterior placement of autologous bone graft and posterior fixation with a transpedicular screw/rod construct. Twenty-one underwent a two-stage procedure consisting of an initial debridement, placement of gentamicin-impregnated methyl methacrylate chains in the debridement cavity, and posterior fixation, followed by an anterior fusion and removal of the 2 Neurosurg. Focus / Volume 17 / December, 2004
3 Single-stage debridement and fixation for spinal infection TABLE 1 Literature review of single-stage operations for PVDO* Reop Deaths, Authors No. of Ant Pst Superf Deep Recurrent Hdw/Graft Graft Rate Med & Year Patients Instr Fix WI WI PVDO Rev Extr (%) Causes Redfern, et al., Graziano & Sidhu, NA NA Rath, et al., NA NA Carragee, Dietze, et al., Safran, et al., NA NA Rezai, et al., Przybylski, et al., Hee, et al., NA Liljenqvist, et al., * Ant = anterior; extr = extrusion; fix = fixation; hdw = hardware; instr = instrumentation; med = medical; NA = not applicable; pst = posterior; recur = recurrent; rev = revision; superf = superficial; WI = wound infection. methyl methacrylate implants 2 to 3 weeks later. In the interim, patients were placed on bed rest and received intravenously administered antibiotic drugs. The authors reported no difference in outcome or morbidity rates between the two groups. There was one nonfusion in the single-stage group and there was one recurrence in the two-stage group. The recurrence occurred in one of the two patients in whom methyl methacrylate had been implanted to bridge osseous defects. In 1997, Dietze, et al., 11 reported the first series in which instrumentation was placed anteriorly, adjacent to the area of debridement. Of 20 patients with surgically treated spinal infections, 15 received instrumentation. There were four cases involving the cervical spine that were treated with anterior debridement, simultaneous arthrodesis, and placement of anterior Caspar vertebral body plates; and there were 11 cases involving the thoracic and lumbar levels that were treated with anterior debridement, arthrodesis, and posterior fixation for which either hook/rod or pedicle screw/rod constructs were used. All operations were single-stage procedures except in five of the lumbar cases, in which there was a 3- to 5-day respite between anterior decompression and arthrodesis with posterior fixation. At the time of the report, the authors had provided follow-up care for a mean of 16 months, during which time three patients were lost to follow-up review and one patient who had multiple medical comorbidities died of septic shock. The authors reported surgical complications in four patients, including one superficial wound infection, one deep wound infection, one pseudarthrosis from a telescoped cervical interbody fibular allograft, and one dislodged lumbar interbody humeral graft that had to be replaced surgically. There were no recurrent spinal infections during the follow-up period. In 1997, Carragee 5 reported on a series of 17 consecutive patients with thoracic and lumbar PVDO who were followed for 2 years after anterior debridement and posterior fixation. There were eight significant postoperative complications, including two instrumentation failures and one wound dehiscence, and four patients died of medical complications. There were no recurrent infections, and ESRs returned to normal levels in 15 of the 17 patients. In two patients with inflammatory arthritis, ESRs were Neurosurg. Focus / Volume 17 / December, 2004 halved during the follow-up period but remained in the supernormal range. In 1998, Safran, et al., 31 reported on a series of 10 patients with thoracic and lumbar PVDO who were treated with single-stage anterior corpectomy and arthrodesis. There was one repeated operation to replace an extruded anterior bone graft. After a mean follow-up duration of 30 months, all patients were ambulatory, had attained a bone fusion, and displayed no evidence of recurrent infection. In 1999, Rezai, et al., 28 reported on a series of 57 consecutive patients with PVDO of the cervical, thoracic, or lumbar spine, 37 of whom were treated surgically. Of these, 26 underwent an anterior approach, receiving autograft or allograft, with 14 undergoing placement of anterior instrumentation alone and four undergoing anterior and posterior instrumentation. Four patients who underwent a posterior approach received fixation with hook/rod constructs. Patients were followed for a mean duration of 36 months, with none lost to follow up. Patients were treated with external bracing for 3 to 6 months postsurgery. Two patients experienced wound dehiscence that eventually healed; one patient had a superficial infection at the halo pin site. Two patients with cervical lesions who received grafts without instrumentation required a repeated operation to secure extruded bone grafts. One patient required a repeated operation to replace a screw, and another, who was noncompliant with antibiotic therapy, underwent repeated surgery for graft collapse. There was one patient who suffered a recurrent cervical infection but who nonetheless attained a solid fusion. This patient was successfully treated with abscess drainage, removal of the hardware, and another course of antibiotic medications. In 2001, Przybylski and Sharan 24 presented a series of 17 consecutive patients with PVDO who were treated surgically. Two patients had cervical disease, one thoracic, and 14 lumbar. All patients underwent single-stage anterior debridement and fixation, although the patient with cervical disease was the only one who received anterior instrumentation. Patients were followed for 12 to 44 months and wore external bracing for 2 to 3 months. There were two deaths in the immediate postoperative period, one caused by pneumonia and multiorgan failure and the other by myocardial infarction. There was 3
4 one wound dehiscence that healed by secondary intention without surgical debridement; there was one late superficial infection of a drain site that was treated with intravenous antibiotic medications. After surgical treatment of a thoracolumbar lesion, a paraspinal abscess and a new cervical PVDO developed 17 and 28 months, respectively, after the initial operation in one patient. His instrumentation was removed, a solid fusion was found, and results of the intraoperative cultures were negative. Another patient had a late deep wound infection that was treated with drainage, local wound care, and intravenously administered antibiotic drugs. Her hardware was removed several months later. Levels of CRP had normalized in all of the surviving patients after 3 months, except in three with chronic PVDO. In 2002, Hee, et al., 15 reported on a series of 21 patients treated via anterior approaches for 11 lumbar lesions, nine thoracic lesions, and one cervical lesion. Anterior fusion was performed in all cases, with five patients receiving a titanium mesh cage packed with autograft instead of a bone strut graft. Anterior stabilization instrumentation was used in two patients and posterior instrumentation and fusion were performed in 10 others by using hook/rod or pedicle screw/rod constructs. Two of these posterior fusions were delayed for 1 to 2 weeks. All patients wore rigid external braces until fusion was demonstrated on x- ray films; patients were followed for a mean duration of 67 months. Three patients died of septic shock in the immediate perioperative period. In two patients recurrent PVDO with progressive kyphosis developed, requiring a repeated operation; in one patient a dislodged hook was found; and in another a pseudarthrosis and wound infection developed. The authors found that, compared with patients who received posterior fixation, those who did not experienced faster procedures and less blood loss, but had higher complication rates and were twice as slow to attain fusion. Patients who received titanium cages spent less time in braces and had shorter hospital stays and lower complication rates. In 2003, Liljenqvist, et al., 17 reported on a series of 20 patients with thoracic or lumbar PVDO who all underwent single-stage operations consisting of anterior debridement and reconstruction in which an expandable titanium cage was used, along with posterior fixation in which a pedicle screw/rod construct was used. All patients were followed for a mean duration of 26 months with serial radiographs and serum CRP testing. Eight patients were mobilized with no external support, whereas 12 patients wore a brace for 3 to 6 months. Three patients died during the follow-up period, two of sepsis in the postoperative period and one of a myocardial infarction that occurred after discharge. There was one common iliac vein injury that required intraoperative repair. There were two repeated operations for hardware malpositioning that had produced neurological symptoms. There were four superficial wound infections requiring surgical debridement but no deep wound infections or cases of recurrent PVDO. The CRP values had completely normalized in 11 of 20 at follow-up review, and ranged from 0.7 to 2.3 mg/dl in the remaining nine. In 2003, Shad, et al., 34 presented a series of five patients with a small cervical PVDO, all of whom were treated with anterior corpectomy and plate fixation. In four of A. T. Ogden and M. G. Kaiser the five patients the causative pathogen was S. aureus. When the authors removed and cultured the hardware after successful fusion and cure, S. epidermidis grew in each case. Current Management Protocols The majority of spinal infections can be managed medically without surgical intervention. A diagnosis is made based on the results of radiographic studies and is confirmed by elevated serum ESRs and CRP levels. Identification of the pathogenic organism is accomplished using blood cultures or computerized tomography guided biopsy sampling. Surgery is reserved for patients with neurological compromise, failed medical management, unstable mechanical deformity, epidural abscess, or intractable pain. In reviewing our own series of patients who were surgically treated for PVDO over the last 3 years, we have identified 16 consecutive patients who underwent singlestage placement of both anterior and posterior instrumentation after debridement. Two of these patients died in the perioperative period, and four were lost to follow up. The remaining patients were followed with weekly ESR and CRP testing during antibiotic treatment, and they underwent ESR and CRP assessments 1 month after termination of antibiotic therapy. After 1 to 2 years of follow-up review, all ESRs and CRP values were normal or close to normal, and all patients demonstrated stable constructs on dynamic plain x-ray films. There were no hardware revisions and no recurrences. CONCLUSIONS A definitive recommendation regarding the optimal surgical strategy for PVDO is not possible given the retrospective nature of the literature and the inherent heterogeneity among case series. Still, it would appear that single-stage operations do not predispose patients to recurrent infection, at least not during a follow-up duration of 1 to 2 years. Although no study has been conducted to examine systematically the benefits of early mobilization in this population, it is logical to assume lower rates of complications such as pneumonia and deep venous thrombosis in patients undergoing single-stage operations. There are no obvious advantages to rigorous avoidance of hardware placement into debridement cavities. Indeed, the sporadic cases of extrusion of anteriorly placed grafts reported in series in which only posterior hardware was placed indicates that anterior plate placement or fixation should be used if possible. Interestingly, in rare cases in which reexploration is performed for recurrent infection, a solid arthrodesis is often observed. This may result from the enhanced inflammatory response produced by an infectious process that is active during the initial phase of bone healing. 16 Complete eradication of infection should be verified by postoperative normalization of ESRs and CRP levels. Trends in these values are greatly affected by concomitant medical conditions and the inflammatory response to surgery. Follow-up magnetic resonance imaging may be useful as well, but interpretation of these images is made difficult by the presence of enhancing noninfected granulation tissue and artifacts from the hardware. The benefits of hardware removal after fusion are unclear, and the one 4 Neurosurg. Focus / Volume 17 / December, 2004
5 Single-stage debridement and fixation for spinal infection small series in which hardware colonization by a skin flora that was not the original pathogen was reported does not support the systematic removal of hardware after debridement and stabilization for PVDO. References 1. Abramovitz JN, Batson RA, Yablon JS: Vertebral osteomyelitis. The surgical management of neurologic complications. Spine 11: , Arnold PM, Baek PN, Bernardi RJ, et al: Surgical management of nontuberculous thoracic and lumbar vertebral osteomyelitis: report of 33 cases. Surg Neurol 47: , Belzunegui J, Del Val N, Intxausti JJ, et al: Vertebral osteomyelitis in northern Spain. Report of 62 cases. Clin Exp Rheumatol 17: , Beronius M, Bergman B, Andersson R: Vertebral osteomyelitis in Goteborg, Sweden: a retrospective study of patients during Scand J Infect Dis 33: , Carragee EJ: Instrumentation of the infected and unstable spine: a review of 17 cases from the thoracic and lumbar spine with pyogenic infections. J Spinal Disord 10: , Carrega G, Arena S, Bartolacci V, et al: [Non-tubercular vertebral osteomyelitis: diagnosis and therapy of 45 patients from a single Italian centre.] Infez Med 11: , 2003 (Ita) 7. Chelsom J, Solberg CO: Vertebral osteomyelitis at a Norwegian university hospital : clinical features, laboratory findings and outcome. Scand J Infect Dis 30: , Colmenero JD, Jimenez-Mejias ME, Reguera JM, et al: Tuberculous vertebral osteomyelitis in the new millennium: still a diagnostic and therapeutic challenge. Eur J Clin Microbiol Infect Dis 23: , Colmenero JD, Jimenez-Mejias ME, Sanchez-Lora FJ, et al: Pyogenic, tuberculous, and brucellar vertebral osteomyelitis: a descriptive and comparative study of 219 cases. Ann Rheum Dis 56: , Darouiche RO, Hamill RJ, Greenberg SB, et al: Bacterial spinal epidural abscess. Review of 43 cases and literature survey. Medicine 71: , Dietze DD Jr, Fessler RG, Jacob RP: Primary reconstruction for spinal infections. J Neurosurg 86: , Emery SE, Chan DP, Woodward HR: Treatment of hematogenous pyogenic vertebral osteomyelitis with anterior debridement and primary bone grafting. Spine 14: , Fountain SS: A single-stage combined surgical approach for vertebral resections. J Bone Joint Surg Am 61: , Graziano GP, Sidhu KS: Salvage reconstruction in acute and late sequelae from pyogenic thoracolumbar infection. J Spinal Disord 6: , Hee HT, Majd ME, Holt RT, et al: Better treatment of vertebral osteomyelitis using posterior stabilization and titanium mesh cages. J Spinal Disord Tech 15: , Kon T, Cho TJ, Aizawa T, et al: Expression of osteoprotegerin, receptor activator of NF- B ligand (osteoprotegerin ligand) and related proinflammatory cytokines during fracture healing. J Bone Miner Res 16: , Liljenqvist U, Lerner T, Bullmann V, et al: Titanium cages in the surgical treatment of severe vertebral osteomyelitis. Eur Spine J 12: , Lyu RK, Chen CJ, Tang LM, et al: Spinal epidural abscess successfully treated with percutaneous, computed tomographyguided, needle aspiration and parenteral antibiotic therapy: case report and review of the literature. Neurosurgery 51: , Matsui H, Hirano N, Sakaguchi Y: Vertebral osteomyelitis: an analysis of 38 surgically treated cases. Eur Spine J 7:50 54, McHenry MC, Easley KA, Locker GA: Vertebral osteomyelitis: long-term outcome for 253 patients from 7 Clevelandarea hospitals. Clin Infect Dis 34: , Nolla JM, Ariza J, Gomez-Vaquero C, et al: Spontaneous pyogenic vertebral osteomyelitis in nondrug users. Semin Arthritis Rheum 31: , Osenbach RK, Hitchon PW, Menezes AH: Diagnosis and management of pyogenic vertebral osteomyelitis in adults. Surg Neurol 33: , Perronne C, Saba J, Behloul Z, et al: Pyogenic and tuberculous spondylodiskitis (vertebral osteomyelitis) in 80 adult patients. Clin Infect Dis 19: , Przybylski GJ, Sharan AD: Single-stage autogenous bone grafting and internal fixation in the surgical management of pyogenic discitis and vertebral osteomyelitis. J Neurosurg Spine 94: 1 7, Rath SA, Neff U, Schneider O, et al: Neurosurgical management of thoracic and lumbar vertebral osteomyelitis and discitis in adults: a review of 43 consecutive surgically treated patients. Neurosurgery 38: , Redfern RM, Miles J, Banks AJ, et al: Stabilisation of the infected spine. J Neurol Neurosurg Psychiatry 51: , Reihsaus E, Waldbaur H, Seeling W: Spinal epidural abscess: a meta-analysis of 915 patients. Neurosurg Rev 23: , Rezai AR, Woo HH, Errico TJ, et al: Contemporary management of spinal osteomyelitis. Neurosurgery 44: , Rigamonti D, Liem L, Sampath P, et al: Spinal epidural abscess: contemporary trends in etiology, evaluation, and management. Surg Neurol 52: , Roine I, Faingezicht I, Arguedas A, et al: Serial serum C-reactive protein to monitor recovery from acute hematogenous osteomyelitis in children. Pediatr Infect Dis J 14:40 44, Safran O, Rand N, Kaplan L, et al: Sequential or simultaneous, same-day anterior decompression and posterior stabilization in the management of vertebral osteomyelitis of the lumbar spine. Spine 23: , Sapico FL: Microbiology and antimicrobial therapy of spinal infections. Orthop Clin North Am 27:9 13, Sapico FL, Montgomerie JZ: Vertebral osteomyelitis in intravenous drug abusers: report of three cases and review of the literature. Rev Infect Dis 2: , Shad A, Shariff S, Fairbank J, et al: Internal fixation for osteomyelitis of cervical spine: the issue of persistence of culture positive infection around the implants. Acta Neurochir 145: , Stefanovski N, Van Voris LP: Pyogenic vertebral osteomyelitis: report of a series of 23 patients. Contemp Orthop 31: , Torda AJ, Gottlieb T, Bradbury R: Pyogenic vertebral osteomyelitis: analysis of 20 cases and review. Clin Infect Dis 20: , Unkila-Kallio L, Kallio MJ, Eskola J, et al: Serum C-reactive protein, erythrocyte sedimentation rate, and white blood cell count in acute hematogenous osteomyelitis of children. Pediatrics 93:59 62, Waldvogel FA, Medoff G, Swartz MN: Osteomyelitis: a review of clinical features, therapeutic considerations and unusual aspects. 3. Osteomyelitis associated with vascular insufficiency. N Engl J Med 282: , 1970 Manuscript received October 15, Accepted in final form November 4, Address reprint requests to: Michael G. Kaiser, M.D., The Neurological Institute, 710 West 168th Street, 4th Floor, New York, New York Neurosurg. Focus / Volume 17 / December,
Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery
 The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
Posterior lumbar interbody fusion with an autogenous iliac crest bone graft in the treatment of pyogenic spondylodiscitis
 Spine Posterior lumbar interbody fusion with an autogenous iliac crest bone graft in the treatment of pyogenic spondylodiscitis J. S. Lee, K. T. Suh From the Pusan National University Hospital, Pusan,
Spine Posterior lumbar interbody fusion with an autogenous iliac crest bone graft in the treatment of pyogenic spondylodiscitis J. S. Lee, K. T. Suh From the Pusan National University Hospital, Pusan,
POSTOPERATIVE COMPLICATIONS IN OPERATED CASES OF PYOGENIC SPONDYLODISCITIS
 Original Article Orthopaedics POSTOPERATIVE COMPLICATIONS IN OPERATED CASES OF PYOGENIC SPONDYLODISCITIS Ravikumar T V 1, Shivprasad M S 2, Yashavatha Kumar 1, Vinay Jain K 3, Mahesh 1 1 -Assistant Professor,
Original Article Orthopaedics POSTOPERATIVE COMPLICATIONS IN OPERATED CASES OF PYOGENIC SPONDYLODISCITIS Ravikumar T V 1, Shivprasad M S 2, Yashavatha Kumar 1, Vinay Jain K 3, Mahesh 1 1 -Assistant Professor,
Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion and Posterior Instrumentation
 Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity. Department of Spine, General Hospital of Lanzhou Command, Gansu, China
 Int Surg 2017;102:171 177 DOI: 10.9738/INTSURG-D-15-00051.1 Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity Xu Lan, Jian-Zhong Xu, Xue-Mei Liu, Bao-Feng Ge Department of Spine,
Int Surg 2017;102:171 177 DOI: 10.9738/INTSURG-D-15-00051.1 Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity Xu Lan, Jian-Zhong Xu, Xue-Mei Liu, Bao-Feng Ge Department of Spine,
SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY).
 SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY). TRANSVERSECTOMY). Patricia Álvarez González, Javier Pizones Arce, Felisa SánchezS nchez-mariscal, Lorenzo ZúñZ úñiga
SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY). TRANSVERSECTOMY). Patricia Álvarez González, Javier Pizones Arce, Felisa SánchezS nchez-mariscal, Lorenzo ZúñZ úñiga
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit
 Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Anterior Versus Posterior Fixation for the Treatment of Lumbar Pyogenic Vertebral Osteomyelitis
 Anterior Versus Posterior Fixation for the Treatment of Lumbar Pyogenic Vertebral Osteomyelitis Meng Si, MD; Zhi-ping Yang, MD; Zhen-feng Li, MD; Qiang Yang, MD; Jian-min Li, MD abstract Full article available
Anterior Versus Posterior Fixation for the Treatment of Lumbar Pyogenic Vertebral Osteomyelitis Meng Si, MD; Zhi-ping Yang, MD; Zhen-feng Li, MD; Qiang Yang, MD; Jian-min Li, MD abstract Full article available
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
In the adult population, vertebral discitis and osteomyelitis. Posterior fixation without debridement for vertebral body osteomyelitis and discitis
 Posterior fixation without debridement for vertebral body osteomyelitis and discitis Neurosurg Focus 37 (2):E6, 2014 AANS, 2014 Ahmed S. Mohamed, M.D., 1 Jung Yoo, M.D., 1 Robert Hart, M.D., 1 Brian T.
Posterior fixation without debridement for vertebral body osteomyelitis and discitis Neurosurg Focus 37 (2):E6, 2014 AANS, 2014 Ahmed S. Mohamed, M.D., 1 Jung Yoo, M.D., 1 Robert Hart, M.D., 1 Brian T.
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Dynamic anterior cervical plating for multi-level spondylosis: Does it help?
 Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Treatment Of Spondylodiscitis, Epidural Abscess And Spondylitis A Retrospective Study Of 20 Cases With Exclusion Of TB Cases
 BMH Med. J. 2019;6(1):4-12. Research Article Treatment Of Spondylodiscitis, Epidural Abscess And Spondylitis A Retrospective Study Of 20 Cases With Exclusion Of TB Cases Suresh S Pillai 1, Arunkumar C
BMH Med. J. 2019;6(1):4-12. Research Article Treatment Of Spondylodiscitis, Epidural Abscess And Spondylitis A Retrospective Study Of 20 Cases With Exclusion Of TB Cases Suresh S Pillai 1, Arunkumar C
Spinal Fusion. North American Spine Society Public Education Series
 Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Surgical treatment of tuberculous spondylodiscitis
 European Review for Medical and Pharmacological Sciences 2012; 1(Suppl 2): 79-85 Surgical treatment of tuberculous spondylodiscitis E. POLA, B. ROSSI, L.A. NASTO, D. COLANGELO, C.A. LOGROSCINO Division
European Review for Medical and Pharmacological Sciences 2012; 1(Suppl 2): 79-85 Surgical treatment of tuberculous spondylodiscitis E. POLA, B. ROSSI, L.A. NASTO, D. COLANGELO, C.A. LOGROSCINO Division
Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony
 Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony Martino, MD University of South Alabama, Department of
Anterior Corpectomy with Expandable Titanium Cages for Thoraco Lumbar Fractures Audrey Paulzak, MD Pat O'Brien, BS W. George Rusyniak, MD Anthony Martino, MD University of South Alabama, Department of
ASJ. Evaluation of Outcome of Transpedicular Decompression and Instrumented Fusion in Thoracic and Thoracolumbar Tuberculosis. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2017;11(1):31-36 Transpedicular decompression https://doi.org/10.4184/asj.2017.11.1.31 in potts spine Evaluation of Outcome of Transpedicular
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2017;11(1):31-36 Transpedicular decompression https://doi.org/10.4184/asj.2017.11.1.31 in potts spine Evaluation of Outcome of Transpedicular
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Management of Skip-Lesions in Dialysis-Related Cervical Spondyloarthropathy
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Management of Skip-Lesions in Dialysis-Related Cervical Spondyloarthropathy S Chandela, J Llena, J Houten Citation S Chandela, J Llena,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Management of Skip-Lesions in Dialysis-Related Cervical Spondyloarthropathy S Chandela, J Llena, J Houten Citation S Chandela, J Llena,
Pseuarthrosis Post Cervical Surgery
 Pseuarthrosis Post Cervical Surgery Don Moore, MD Center for Spine Health Cleveland Clinic May 12, 2018 Pseudarthrosis Post Cervical Surgery Patient factors Surgeon factors Efficacy of index procedure
Pseuarthrosis Post Cervical Surgery Don Moore, MD Center for Spine Health Cleveland Clinic May 12, 2018 Pseudarthrosis Post Cervical Surgery Patient factors Surgeon factors Efficacy of index procedure
Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D.
 J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
Transpedicular Curettage and Drainage of Infective Lumbar Spondylodiscitis: Technique and Clinical Results
 Original Article Clinics in Orthopedic Surgery 2012;4:200-208 http://dx.doi.org/10.4055/cios.2012.4.3.200 Transpedicular Curettage and Drainage of Infective Lumbar Spondylodiscitis: Technique and Clinical
Original Article Clinics in Orthopedic Surgery 2012;4:200-208 http://dx.doi.org/10.4055/cios.2012.4.3.200 Transpedicular Curettage and Drainage of Infective Lumbar Spondylodiscitis: Technique and Clinical
Treatment of thoracolumbar burst fractures by vertebral shortening
 Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Pyogenic spinal infection can be thought of as a
 Case Report 651 Pyogenic Spondylitis Presenting with Skip Lesions Po-Liang Lai, MD; Hsieh-Shong Leu 1, MD MSc; Chi-Chien Niu, MD; Wen-Jer Chen, MD; Lih-Huei Chen, MD We report on a 65-year-old man who
Case Report 651 Pyogenic Spondylitis Presenting with Skip Lesions Po-Liang Lai, MD; Hsieh-Shong Leu 1, MD MSc; Chi-Chien Niu, MD; Wen-Jer Chen, MD; Lih-Huei Chen, MD We report on a 65-year-old man who
Surgical Management of Cervical Spondyloarthropathy in Hemodialysis Patients
 The Open Orthopaedics Journal, 2010, 4, 39-43 39 Open Access Surgical Management of Cervical Spondyloarthropathy in Hemodialysis Patients Panayiotis Spinos 1, Charalambos Matzaroglou *,2, Meni Partheni
The Open Orthopaedics Journal, 2010, 4, 39-43 39 Open Access Surgical Management of Cervical Spondyloarthropathy in Hemodialysis Patients Panayiotis Spinos 1, Charalambos Matzaroglou *,2, Meni Partheni
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Diagnosis and Treatment of Tuberclous Spondylitis and Pyogenic Spondylitis in Atypical Cases
 Asian Spine Journal Vol. 1, No. 2, pp 75~79, 2007 Diagnosis and Treatment of Tuberclous Spondylitis and Pyogenic Spondylitis in Atypical Cases Jae Sung Ahn, June Kyu Lee Department of Orthopedic Surgery,
Asian Spine Journal Vol. 1, No. 2, pp 75~79, 2007 Diagnosis and Treatment of Tuberclous Spondylitis and Pyogenic Spondylitis in Atypical Cases Jae Sung Ahn, June Kyu Lee Department of Orthopedic Surgery,
Treatment of Tuberculous Spondylitis with Anterior Stabilization and Titanium Cage
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 444, pp. 60 65 2006 Lippincott Williams & Wilkins Treatment of Tuberculous Spondylitis with Anterior Stabilization and Titanium Cage Anastasios G. Christodoulou,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 444, pp. 60 65 2006 Lippincott Williams & Wilkins Treatment of Tuberculous Spondylitis with Anterior Stabilization and Titanium Cage Anastasios G. Christodoulou,
Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion
 Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Spinal epidural abscess is uncommon but has the potential
 J Neurosurg Spine 14:765 770, 2011 Prospective evaluation of a clinical decision guideline to diagnose spinal epidural abscess in patients who present to the emergency department with spine pain Clinical
J Neurosurg Spine 14:765 770, 2011 Prospective evaluation of a clinical decision guideline to diagnose spinal epidural abscess in patients who present to the emergency department with spine pain Clinical
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Lateral Mass and Pedicle Screws Fixation of Cervical Spine
 Lateral Mass and Pedicle Screws Fixation of Cervical Spine Anderson Spine 1991 Paul A Anderson University of Wisconsin AAOS Biomedical Engineering Committee Co-chair ASTM F05-24 Purpose Anatomy Surgical
Lateral Mass and Pedicle Screws Fixation of Cervical Spine Anderson Spine 1991 Paul A Anderson University of Wisconsin AAOS Biomedical Engineering Committee Co-chair ASTM F05-24 Purpose Anatomy Surgical
Codes for Back and Spinal Procedures
 20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
20930 Allograft for spine surgery only; morselized 20931 Allograft for spine surgery only; structural 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process,
For pyogenic spondylitis, conservative management
 SPINE Volume 41, Number 17, pp E1022 E1029 ß 2016 Wolters Kluwer Health, Inc. All rights reserved CLINICAL CASE SERIES Posterior Only Approach for Lumbar Pyogenic Spondylitis With Short Instrumentation
SPINE Volume 41, Number 17, pp E1022 E1029 ß 2016 Wolters Kluwer Health, Inc. All rights reserved CLINICAL CASE SERIES Posterior Only Approach for Lumbar Pyogenic Spondylitis With Short Instrumentation
Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach
 Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach Darryl Lau, MD and Dean Chou, MD Department of Neurological Surgery
Posterior Thoracic Corpectomies with Cage Reconstruction for Metastatic Spinal Tumors: Comparing the MiniOpen Approach to the Open Approach Darryl Lau, MD and Dean Chou, MD Department of Neurological Surgery
Advantages of MISS. Disclosures. Thoracolumbar Trauma: Minimally Invasive Techniques. Minimal Invasive Spine Surgery 11/8/2013.
 3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
3 rd Annual UCSF Techniques in Complex Spine Surgery Program Thoracolumbar Trauma: Minimally Invasive Techniques Research Support: Stryker Disclosures Murat Pekmezci, MD Assistant Clinical Professor UCSF/SFGH
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Late Infection of Spinal Instrumentation
 Abstract Late Infection of Spinal Instrumentation Jae-Ik Shim, M.D., Taik-Seon Kim, M.D., Sung-Jong Lee, M.D., Suk-Ha Lee, M.D., Dong-Ki Lee, M.D., Yoen-Sik Yu, M.D., Yun-Yeup Kim, M.D. Department of Orthopaedic
Abstract Late Infection of Spinal Instrumentation Jae-Ik Shim, M.D., Taik-Seon Kim, M.D., Sung-Jong Lee, M.D., Suk-Ha Lee, M.D., Dong-Ki Lee, M.D., Yoen-Sik Yu, M.D., Yun-Yeup Kim, M.D. Department of Orthopaedic
Preliminary Report of Instrumentation in Tuberculous Lumbosacral Spine
 Doi:http://dx.doi.org/10.5704/MOJ.1411.004 Preliminary Report of Instrumentation in Tuberculous Lumbosacral Spine, MRCS Department of Orthopaedic Surgery, Yangon Orthopaedic Hospital, Yangon, Myanmar ABSTRACT
Doi:http://dx.doi.org/10.5704/MOJ.1411.004 Preliminary Report of Instrumentation in Tuberculous Lumbosacral Spine, MRCS Department of Orthopaedic Surgery, Yangon Orthopaedic Hospital, Yangon, Myanmar ABSTRACT
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis
 Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
1105 two (2) vertebrae... 1, add on per additional vertebra
 SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
Two Level Vertebral Osteomyelitis Without Spinal Epidural Abscess Secondary to Spinal and Epidural Anesthesia: Two Case
 Article ID: WMC003938 ISSN 2046-1690 Two Level Vertebral Osteomyelitis Without Spinal Epidural Abscess Secondary to Spinal and Epidural Anesthesia: Two Case Corresponding Author: Dr. Ergun Karavelioglu,
Article ID: WMC003938 ISSN 2046-1690 Two Level Vertebral Osteomyelitis Without Spinal Epidural Abscess Secondary to Spinal and Epidural Anesthesia: Two Case Corresponding Author: Dr. Ergun Karavelioglu,
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Traumatic thoracic spinal fracture dislocation with minimal or no cord injury
 J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
Case Study: Jordan. Conditions Treated Cleidocranial Dysostosis. Age Range During Treatment 13 Years 14 Years
 Case Study: Jordan Conditions Treated Cleidocranial Dysostosis Age Range During Treatment 13 Years 14 Years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery &
Case Study: Jordan Conditions Treated Cleidocranial Dysostosis Age Range During Treatment 13 Years 14 Years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery &
To study the outcomes of posterior decompression and fixation of tuberculosis of dorsolumbar spine
 2017; 3(3): 691-695 ISSN: 2395-1958 IJOS 2017; 3(3): 691-695 2017 IJOS wwworthopapercom Received: 15-05-2017 Accepted: 16-06-2017 Dr Manish Shah Assistant Professor, Department of Dr Kushal Suthar Dr Ravindra
2017; 3(3): 691-695 ISSN: 2395-1958 IJOS 2017; 3(3): 691-695 2017 IJOS wwworthopapercom Received: 15-05-2017 Accepted: 16-06-2017 Dr Manish Shah Assistant Professor, Department of Dr Kushal Suthar Dr Ravindra
Replacement Code for Interbody Cage for Disc
 +22851 vs. +20931 October 22, 2015 We ve been told we cannot bill +22851 and +20931 with the ACDF code, 22551. Is this true? It is true if you are thinking about reporting +22851 (intervertebral device)
+22851 vs. +20931 October 22, 2015 We ve been told we cannot bill +22851 and +20931 with the ACDF code, 22551. Is this true? It is true if you are thinking about reporting +22851 (intervertebral device)
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Discitis and osteomyelitis accounts for approximately
 Neurosurg Focus 37 (2):E5, 2014 AANS, 2014 Direct lateral retroperitoneal approach for the surgical treatment of lumbar discitis and osteomyelitis Karthik Madhavan, M.D., 1 Steven Vanni, D.C., D.O., 1
Neurosurg Focus 37 (2):E5, 2014 AANS, 2014 Direct lateral retroperitoneal approach for the surgical treatment of lumbar discitis and osteomyelitis Karthik Madhavan, M.D., 1 Steven Vanni, D.C., D.O., 1
The incidence of osteomyelitis of the spine has been
 SPINE Volume 42, Number 17, pp 1339 1346 ß 2017 Wolters Kluwer Health, Inc. All rights reserved. SURGERY Prognostic Factors for Failure of Antibiotic Treatment in Patients With Osteomyelitis of the Spine
SPINE Volume 42, Number 17, pp 1339 1346 ß 2017 Wolters Kluwer Health, Inc. All rights reserved. SURGERY Prognostic Factors for Failure of Antibiotic Treatment in Patients With Osteomyelitis of the Spine
Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up
 Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up Janek Frantzén M.D., Neurosurgeon Turku University Hospital, Finland ROME SPINE 2011 7.12.2011 1 Clinical Development
Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up Janek Frantzén M.D., Neurosurgeon Turku University Hospital, Finland ROME SPINE 2011 7.12.2011 1 Clinical Development
Spine Postoperative Infections: Risk Factors
 Spine Postoperative Infections: Risk Factors Tomás Funes 1, 2 MD, Donato Pacione1 MD, Stephen Kalhorn 1 MD, Pablo Jalón 2 MD, Anthony Frempong-Boadu1 MD, Juan José Mezzadri 2 MD, PhD 1 Department of Neurosurgery,
Spine Postoperative Infections: Risk Factors Tomás Funes 1, 2 MD, Donato Pacione1 MD, Stephen Kalhorn 1 MD, Pablo Jalón 2 MD, Anthony Frempong-Boadu1 MD, Juan José Mezzadri 2 MD, PhD 1 Department of Neurosurgery,
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
Ankle and subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT
 Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Extended indications of percutaneous endoscopic lavage and drainage for the treatment of lumbar infectious spondylitis
 Eur Spine J (2014) 23:846 853 DOI 10.1007/s00586-013-3157-y ORIGINAL ARTICLE Extended indications of percutaneous endoscopic lavage and drainage for the treatment of lumbar infectious spondylitis Shih-Chieh
Eur Spine J (2014) 23:846 853 DOI 10.1007/s00586-013-3157-y ORIGINAL ARTICLE Extended indications of percutaneous endoscopic lavage and drainage for the treatment of lumbar infectious spondylitis Shih-Chieh
Single-stage approach of posterior debridement, allograft and internal fixation in management of lumbosacral tuberculosis.
 Biomedical Research 2017; 28 (3): 1448-1452 Single-stage approach of posterior debridement, allograft and internal fixation in management of lumbosacral tuberculosis. Jiawen Wu 1, Juanjuan Wang 2, Ming
Biomedical Research 2017; 28 (3): 1448-1452 Single-stage approach of posterior debridement, allograft and internal fixation in management of lumbosacral tuberculosis. Jiawen Wu 1, Juanjuan Wang 2, Ming
Case Report Rapidly Progressive Spontaneous Spinal Epidural Abscess
 Case Reports in Infectious Diseases Volume 2016, Article ID 7958291, 4 pages http://dx.doi.org/10.1155/2016/7958291 Case Report Rapidly Progressive Spontaneous Spinal Epidural Abscess Abdurrahman Aycan,
Case Reports in Infectious Diseases Volume 2016, Article ID 7958291, 4 pages http://dx.doi.org/10.1155/2016/7958291 Case Report Rapidly Progressive Spontaneous Spinal Epidural Abscess Abdurrahman Aycan,
Comparison of clinical, radiological and functional outcome of short segment V/S long segment posterior fixation of tuberculosis of spine
 2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
Single-stage posterior debridement and single-level instrumented fusion for spontaneous infectious spondylodiscitis of the lumbar spine
 Acta Orthop. Belg., 2011, 77, 816-822 ORIGINAL STUDY Single-stage posterior debridement and single-level instrumented fusion for spontaneous infectious spondylodiscitis of the lumbar spine Liang ZHANg,
Acta Orthop. Belg., 2011, 77, 816-822 ORIGINAL STUDY Single-stage posterior debridement and single-level instrumented fusion for spontaneous infectious spondylodiscitis of the lumbar spine Liang ZHANg,
Osteoarthrosis, unspecified whether generalized or localized, lower leg. Osteoarthrosis, localized, not specified whether primary or secondary, pelvic
 Page 1 Appendix TABLE E-1 Codes (and Definitions) in Humana Database Used for Study Inclusion and Exclusion of Patients Who Underwent,, or 1 to 2-Level Inclusion ICD-9-P-8154 Total knee replacement ICD-9-D-71596
Page 1 Appendix TABLE E-1 Codes (and Definitions) in Humana Database Used for Study Inclusion and Exclusion of Patients Who Underwent,, or 1 to 2-Level Inclusion ICD-9-P-8154 Total knee replacement ICD-9-D-71596
Evaluation of Role of Anterior Debridement and Decompression of Spinal Cord and Instrumentation in Treatment of Tubercular Spondylitis
 Asian Spine Journal Vol. 6, No. 3, pp 183~193, 2012 Anterior Debridment Decompression and Instrumentation in Tubercular Spondylitis / 183 http://dx.doi.org/10.4184/asj.2012.6.3.183 Evaluation of Role of
Asian Spine Journal Vol. 6, No. 3, pp 183~193, 2012 Anterior Debridment Decompression and Instrumentation in Tubercular Spondylitis / 183 http://dx.doi.org/10.4184/asj.2012.6.3.183 Evaluation of Role of
Original Article Clinics in Orthopedic Surgery 2015;7:
 Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
Single stage posterior instrumentation and anterior interbody fusion for tuberculosis of dorsal and lumbar spines
 Original Article interbody fusion for tuberculosis of dorsal Pandey BK 1, Sangondimath GM 2, Chhabra HS 2 1 Department of Orthopaedics, Kathmandu Medical College Teaching Hospital, Sinamangal, Kathmandu,
Original Article interbody fusion for tuberculosis of dorsal Pandey BK 1, Sangondimath GM 2, Chhabra HS 2 1 Department of Orthopaedics, Kathmandu Medical College Teaching Hospital, Sinamangal, Kathmandu,
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine.
 Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis
 29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
Curative effect comparison of anterior and posterior approach in debridement combined with bone graft fusion for the treatment of spinal tuberculosis.
 Biomedical Research 2017; 28 (11): 4832-4836 ISSN 0970-938X www.biomedres.info Curative effect comparison of anterior and posterior approach in debridement combined with bone graft fusion for the treatment
Biomedical Research 2017; 28 (11): 4832-4836 ISSN 0970-938X www.biomedres.info Curative effect comparison of anterior and posterior approach in debridement combined with bone graft fusion for the treatment
J Korean Soc Spine Surg 2014 Jun;21(2): Originally published online June 30, 2014;
 Journal of Korean Society of Spine Surgery Spinal Epidural Abscess and Psoas Abscess Combined with Pyogenic Spondylodiscitis Following Vertebroplasty - A Case Report - Jin Sung Park, M.D., Dong Hee Kim,
Journal of Korean Society of Spine Surgery Spinal Epidural Abscess and Psoas Abscess Combined with Pyogenic Spondylodiscitis Following Vertebroplasty - A Case Report - Jin Sung Park, M.D., Dong Hee Kim,
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
Anterior-only instrumentation and grafting after L5 corpectomy for non-traumatic lesions
 Acta Orthop. Belg., 2010, 76, 94-99 ORIGINAL STUDY Anterior-only instrumentation and grafting after L5 corpectomy for non-traumatic lesions Li-Yang DAI, Lei-Sheng JIANG From Xinhua Hospital, Shanghai Jiaotong
Acta Orthop. Belg., 2010, 76, 94-99 ORIGINAL STUDY Anterior-only instrumentation and grafting after L5 corpectomy for non-traumatic lesions Li-Yang DAI, Lei-Sheng JIANG From Xinhua Hospital, Shanghai Jiaotong
Evaluation of implant stabilization in tubercular Spondylodiscitis: a prospective study
 International Journal of Research in Medical Sciences Maila SK et al. Int J Res Med Sci. 2015 Oct;3(10):2647-2653 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150807
International Journal of Research in Medical Sciences Maila SK et al. Int J Res Med Sci. 2015 Oct;3(10):2647-2653 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150807
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
Although unstable thoracolumbar injuries are a common
 ORIGINAL ARTICLE Anterior-Only Stabilization of Three-Column Thoracolumbar Injuries Rick C. Sasso, MD, Natalie M. Best, BS, Thomas M. Reilly, MD, and Robert A. McGuire, Jr., MD Objective: The optimal treatment
ORIGINAL ARTICLE Anterior-Only Stabilization of Three-Column Thoracolumbar Injuries Rick C. Sasso, MD, Natalie M. Best, BS, Thomas M. Reilly, MD, and Robert A. McGuire, Jr., MD Objective: The optimal treatment
PARAPLEGIA. B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture.
 16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Spinal infection. Outline ANATOMY 6/2/2017. Anatomy Pathogen
 Outline Spinal infection Pramot Tanutit, M.D. Department of Radiology, Songklanagarind Hospital Faculty of Medicine, Prince of Songkla University Anatomy Pathogen Pyogenic spondylodiscitis Tuberculous
Outline Spinal infection Pramot Tanutit, M.D. Department of Radiology, Songklanagarind Hospital Faculty of Medicine, Prince of Songkla University Anatomy Pathogen Pyogenic spondylodiscitis Tuberculous
Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June Section: Surgery Last Reviewed Date: June 2013
 Medical Policy Manual Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June 2007 Section: Surgery Last Reviewed Date: June 2013 Policy No: 157 Effective Date: August 1, 2013 IMPORTANT REMINDER
Medical Policy Manual Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June 2007 Section: Surgery Last Reviewed Date: June 2013 Policy No: 157 Effective Date: August 1, 2013 IMPORTANT REMINDER
CT-guided percutaneous intraspinal needle aspiration for the diagnosis and treatment of epidural collections
 CT-guided percutaneous intraspinal needle aspiration for the diagnosis and treatment of epidural collections Poster No.: P-0064 Congress: ESSR 2013 Type: Scientific Exhibit Authors: G. Petrocheilou, I.
CT-guided percutaneous intraspinal needle aspiration for the diagnosis and treatment of epidural collections Poster No.: P-0064 Congress: ESSR 2013 Type: Scientific Exhibit Authors: G. Petrocheilou, I.
Utility of magnetic resonance imaging in the follow-up of children affected by acute osteomyelitis.
 Curr Pediatr Res 017; 1 (): 354-358 ISSN 0971-903 www.currentpediatrics.com Utility of magnetic resonance imaging in the follow-up of children affected by acute osteomyelitis. Valentina Fabiano 1, Giulia
Curr Pediatr Res 017; 1 (): 354-358 ISSN 0971-903 www.currentpediatrics.com Utility of magnetic resonance imaging in the follow-up of children affected by acute osteomyelitis. Valentina Fabiano 1, Giulia
INFECTION & INFLAMMATION IMAGING
 INFECTION & INFLAMMATION IMAGING Radiopharmaceutical Drug Interactions & Other Interesting Case Studies MICHELLE RUNDIO, CNMT NCT MBA PCI NUCLEAR IN-111 WHITE BLOOD CELL IMAGING Interactions, Imaging Parameters
INFECTION & INFLAMMATION IMAGING Radiopharmaceutical Drug Interactions & Other Interesting Case Studies MICHELLE RUNDIO, CNMT NCT MBA PCI NUCLEAR IN-111 WHITE BLOOD CELL IMAGING Interactions, Imaging Parameters
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
MR imaging is the preferred imaging method of diagnosing
 ORIGINAL RESEARCH T.J. Kowalski K.F. Layton E.F. Berbari J.M. Steckelberg P.M. Huddleston J.T. Wald D.R. Osmon Follow-Up MR Imaging in Patients with Pyogenic Spine Infections: Lack of Correlation with
ORIGINAL RESEARCH T.J. Kowalski K.F. Layton E.F. Berbari J.M. Steckelberg P.M. Huddleston J.T. Wald D.R. Osmon Follow-Up MR Imaging in Patients with Pyogenic Spine Infections: Lack of Correlation with
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Congenital deformity of the spine-therapy. Werner Lack*, Georg Grabmeier**
 Congenital deformity of the spine-therapy Werner Lack*, Georg Grabmeier** *free spine surgeons of Austria, **SMZ-East, Vienna Conservative therapy in clear cases of progression (2 hemi vertebrae, unilateral
Congenital deformity of the spine-therapy Werner Lack*, Georg Grabmeier** *free spine surgeons of Austria, **SMZ-East, Vienna Conservative therapy in clear cases of progression (2 hemi vertebrae, unilateral
Thoracolumbar fractures. Treatment options. A long trip.
 Thoracolumbar fractures. Treatment options. A long trip. MIS SURGERY. WHY NOT? Murcia. October 5, 2012. Dr. Pedro Cortés García. Spinal Unit. Orthopaedic department. Canary Islands University Hospital
Thoracolumbar fractures. Treatment options. A long trip. MIS SURGERY. WHY NOT? Murcia. October 5, 2012. Dr. Pedro Cortés García. Spinal Unit. Orthopaedic department. Canary Islands University Hospital
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Cervical Pseudarthrosis: Diagnosis and Revision Strategies
 Cervical Pseudarthrosis: Diagnosis and Revision Strategies William C. Welch, M.D., F.A.C.S., F.I.C.S. Professor of Neurological Surgery Chief, Neurological Surgery, Pennsylvania Hospital University of
Cervical Pseudarthrosis: Diagnosis and Revision Strategies William C. Welch, M.D., F.A.C.S., F.I.C.S. Professor of Neurological Surgery Chief, Neurological Surgery, Pennsylvania Hospital University of
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 2.417, ISSN: , Volume 3, Issue 11, December 2015
 MANAGEMENT OF PATHOLOGICAL FRACTURE SHAFT HUMERUS SECONDARY TO BACTERIAL OSTEOMYELITIS: A CASE REPORT DR. NARENDRA SINGH KUSHWAHA* DR.SHAH WALIULLAH** DR.VINEET KUMAR*** DR.VINEET SHARMA**** *Asst. Professor,
MANAGEMENT OF PATHOLOGICAL FRACTURE SHAFT HUMERUS SECONDARY TO BACTERIAL OSTEOMYELITIS: A CASE REPORT DR. NARENDRA SINGH KUSHWAHA* DR.SHAH WALIULLAH** DR.VINEET KUMAR*** DR.VINEET SHARMA**** *Asst. Professor,
Anterior cervical dynamic ABC plating with single level corpectomy and fusion in forty-two patients
 (2003) 41, 153 ± 158 ã 2003 International Society All rights reserved 1362 ± 4393/03 $25.00 www.nature.com/sc Original Article Anterior cervical dynamic ABC plating with single level corpectomy and fusion
(2003) 41, 153 ± 158 ã 2003 International Society All rights reserved 1362 ± 4393/03 $25.00 www.nature.com/sc Original Article Anterior cervical dynamic ABC plating with single level corpectomy and fusion
A U X I L I A R Y C O N N E C T O R S Surgical Technique
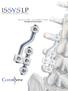 A U X I L I A R Y C O N N E C T O R S Surgical Technique AUXILIARY CONNECTORS ISSYS LP Auxiliary Connectors The ISSYS LP auxiliary connectors were designed to provide medial-lateral variability for the
A U X I L I A R Y C O N N E C T O R S Surgical Technique AUXILIARY CONNECTORS ISSYS LP Auxiliary Connectors The ISSYS LP auxiliary connectors were designed to provide medial-lateral variability for the
PRIMARY STUDIES EN BLOC VERSUS DEBULKING
 PRIMARY STUDIES EN BLOC VERSUS DEBULKING I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary outcome VI Results secondary and other outcome(s) VII Critical appraisal of
PRIMARY STUDIES EN BLOC VERSUS DEBULKING I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary outcome VI Results secondary and other outcome(s) VII Critical appraisal of
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Perioperative Complications of Pedicle Subtraction Osteotomy
 630 Original Article GLOBAL SPINE JOURNAL THIEME Perioperative Complications of Pedicle Subtraction Osteotomy Michael D. Daubs 1 Darrel S. Brodke 2 Prokopis Annis 2 Brandon D. Lawrence 2 1 Division of
630 Original Article GLOBAL SPINE JOURNAL THIEME Perioperative Complications of Pedicle Subtraction Osteotomy Michael D. Daubs 1 Darrel S. Brodke 2 Prokopis Annis 2 Brandon D. Lawrence 2 1 Division of
J Korean Soc Spine Surg 2016 Sep;23(3): Originally published online September 30, 2016;
 Journal of Korean Society of Spine Surgery Multifocal Extensive Spinal Tuberculosis Accompanying Isolated Involvement of Posterior Elements - A Case Report - Dong-Eun Shin, M.D., Sang-June Lee, M.D., Young
Journal of Korean Society of Spine Surgery Multifocal Extensive Spinal Tuberculosis Accompanying Isolated Involvement of Posterior Elements - A Case Report - Dong-Eun Shin, M.D., Sang-June Lee, M.D., Young
