For pyogenic spondylitis, conservative management
|
|
|
- Asher Farmer
- 5 years ago
- Views:
Transcription
1 SPINE Volume 41, Number 17, pp E1022 E1029 ß 2016 Wolters Kluwer Health, Inc. All rights reserved CLINICAL CASE SERIES Posterior Only Approach for Lumbar Pyogenic Spondylitis With Short Instrumentation and Prolonged Suction Drainage Yong-Min Kim, MD and Seung-Myung Choi, MD Study design. A single-institution, single-surgeon retrospective review. Objective. To assess the efficacy of posterior only approach with short instrumentation and prolonged suction drainage in managing lumbar pyogenic spondylitis. Summary of Background Data. Several methods of posterior surgical treatment for pyogenic spondylitis have been reported, there have been few reports regarding the efficacy of posterior only approach with short instrumentation including even inflamed segment. Methods. Thirty-three patients with lumbar pyogenic spondylitis who underwent posterior decompression and lumbar interbody fusion with short instrumentation including the inflamed segment and catheter drainage were enrolled. Clinically infection control (erythrocyte sedimentation rate and C-reactive protein normalization time) and onset of ambulation were reviewed. Moreover, achievement of fusion and changes of sagittal alignment were investigated radiologically. Results. In all 33 cases, infection was controlled successfully without any recurrence. There was no breakage of implant. Postoperative interval to normalization of erythrocyte sedimentation rate was average 69.4 days and C-reactive protein was 25.4 days, respectively. Ambulation was started at average 5.8 postoperative days. Successful interbody fusion was confirmed radiologically in all the cases at a mean of 5.4 months. Sagittal angle of fixed segment was average 6.9 degrees of lordosis before operation, which became more lordotic to 11.5 degrees From the Department of Orthopedic Surgery, School of Medicine, Chungbuk National University, Cheongju, Korea. Acknowledgment date: September 10, First revision date: November 17, Second revision date: December 21, Acceptance date: February 2, The device(s)/drug(s) is/are FDA-approved or approved by corresponding national agency for this indication. NIH funds were received in support of this work. No relevant financial activities outside the submitted work. Address correspondence and reprint requests to Seung-Myung Choi, MD, Department of Orthopedic Surgery, Chungbuk National University Hospital, 776, 1sunhwan-ro, Heungdeok-gu, Cheongju-si, Chungcheongbuk-do, , Republic of Korea; davidchoi1530@gmail.com DOI: /BRS just after operation, but decreased to 4.7 degrees of lordosis at the final follow up. Actually final sagittal alignment was almost same as preoperative status (P ¼ 0.24). Conclusion. By achieving favorable clinical and radiological results, short instrumentation and prolonged suction drainage with posterior only approach seemed to be an effective method in managing lumbar pyogenic spondylitis. Key words: early ambulation, lumbar pyogenic spondylitis, maintenance, posterior only approach, prolonged suction drainage, sagittal alignment, short instrumentation, solid fusion. Level of Evidence: 3 Spine 2016;41:E1022 E1029 For pyogenic spondylitis, conservative management with antibiotic therapy is tried first but surgery may be necessary if the infection is not controlled by conservative way, or if neurological deficit and/or instability is present. An anterior approach is advantageous by performing direct extirpation of the lesion and bone grafting, but requires long-term bed rest and often results in kyphotic deformity. On the other hand, posterior approach using instrumentation provides spinal stability, although it has been regarded as inappropriate to be used in infectionrelated conditions because of the risk that the metal devices would be an obstacle on infection treatment. In a previous report, we showed that prolonged drainage resulted in successful results in patients with deep wound infections after short posterior lumbar instrumentation. 1 Based on this experience, we managed lumbar pyogenic spondylitis with similar approach that is, long-term drainage and antibiotic regimen after extirpation of infectious lesion. MATERIALS A total of 33 patients who underwent short instrumentation and catheter drainage after extirpation of infectious lesion via posterior only approach at our institute between October 1997 and January 2011 were enrolled. Indications were pyogenic spondylodiscitis that had not responded to antibiotic treatment, apparent, or impending neurologic E September 2016
2 TABLE 1. Clinical Profiles of the Patients Who Underwent Posterior Instrumentation and Fusion With Transpedicular Screw System Sex Age (Yrs) Infection Level Destruction Grade compromise by abscess, so on and progressive bony destruction around the disc in previously ambulatory subjects with rather competent general condition. Mean age of 33 patients was 63.7 years (range, yrs) (Table 1). The mean postoperative follow-up period was 43.7 months (range, months). Initial erythrocyte sedimentation rate (ESR) was average 64.7 mm/h and C- reactive protein (CRP) was 9.8 mg/dl. Epidural Abscess Psoas Abscess Posterior Column Abscess Infected Vertebrae Preoperatively, the extent of vertebral body destruction, presence of an epidural abscess, or a psoas abscess was assessed on MRI (Table 1). Twenty-five patients had singlesegment infection and eight patients had multilevel involvement (two disc levels were affected in seven patients and three discs in one patient). Extent of Vertebral Body Destruction A new classification of the extent of vertebral body destruction from grade I to grade IV using the sagittal and coronal MRI images was developed. Grade I was defined as infection confined to the intervertebral disc space only, grade II as involvement of the end plate and vertebral body less than 1/3 of vertebral height, grade III as more than 1/3 and less than 2/3. Grade IV is the severest, destruction more than 2/3 of vertebral height (Figure 1(A C)). To determine the Fixation Level 1 M 70 L2-5 II, III, I L2-5 Lt. L2-S1, Rt. (þ) L2-S1 L3-S1 2 M 55 L5-S1 II L4-S1 Lt. L5-S1 ( ) L5-S1 3 F 67 L3-4 II L3-4 Both L3-4 ( ) L3 5 4 F 77 L2-3 III L1-4 Rt. L2-4 ( ) L2-4 5 F 59 L4-S1 I, I L4-S1 Both L4-5 (þ) L4-S1 6 F 63 L5-S1 III L5-S1 ( ) ( ) L5-S1 7 M 42 L5-S1 I L5-S1 Lt. L5-S1 ( ) L5-S1 8 M 60 L4-5 II L4-5 Lt. L4-S1, Rt. ( ) L4-S1 L4 9 F 72 L4-5 III L4-5 Lt. L4-S1 (þ) L4-S1 10 M 50 L4-5 I L4-S1 Lt. L4-S1, Rt. ( ) L4-S1 L5-S1 11 F 66 L4-5 II L4-5 Both L4-5 ( ) L4-S1 12 M 75 L3-4 I L3-4 Rt. L3-4 ( ) L M 53 L2-3 III L2-3 Rt. L2-3 (þ) L M 69 L1-2 III L1-2 Rt. L3-5 ( ) T12-L3 15 M 69 L3-4 III L3-4 Rt. L3-5 (þ) L F 68 L4-5 II L4-5 ( ) ( ) L3-S1 17 M 68 L2-3 I ( ) ( ) ( ) L M 70 L3-5 I, I L3-5 Lt. L3-5 (þ) L2-S1 19 F 74 L4-S1 I, I L4-S1 Lt. L4-S1 (þ) L4-S1 20 F 61 L4-5 II L4-5 ( ) ( ) L4-S1 21 F 69 L4-5 I ( ) ( ) ( ) L M 60 L1-2 I ( ) Rt. L1-2 ( ) L M 64 L3-5 I, I L2-5 ( ) (þ) L3-S1 24 F 68 L4-S1 I, I L4-S1 Rt. L4-5, Lt. L4- (þ) L4-S1 S1 25 F 70 L4-5 I L4-5 Rt. L4-5 ( ) L F 52 L4-5 II L4-5 Lt. L4-5 ( ) L4-S1 27 M 58 L4-S1 I, I L4-S1 Rt. L5-S1 (þ) L4-S1 28 F 68 L5-S1 III L4-S1 ( ) ( ) L5-S1 29 M 56 L2-3 II L2-3 Rt. L2-3 ( ) L M 65 L4-5 I ( ) ( ) ( ) L F 64 L3-4 II L3-5 ( ) ( ) L F 61 L4-S1 I, I L4-S1 Both L4-S1 (þ) L4-S1 33 F 59 L2-3 II L2-3 ( ) ( ) L2-4 Spine E1023
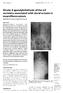
3 Figure 1. A, The author s grading of destruction in the vertebral body. The MR images show grade II (B) and III (C) destruction of the body. reliability of the proposed new classification, Kendall coefficient of concordance was used to qualify the intraobserver and interobserver agreement by two spine specialists, who were independent of this study. The intraobserver and interobserver reliability showed good to excellent agreement ( , , respectively). To determine the validity, Spearman correlation between the scale according to the extent of vertebral body destruction and the preoperative Cobb angle of inflamed segment was calculated showing a positive correlation (r ¼ 0.659, P ¼ 0.01). Epidural Abscess Epidural abscess was observed in 29 among 33 patients (Figure 2 (A B)). In most patients, it was seen within the infected segment (one disc and two adjacent bodies). However, six patients had farther extension of epidural abscess over adjacent, intact disc. Psoas Abscess Psoas abscess was identified in 23 patients. Among which 16 patients had psoas abscess within the infected segment (bilateral in five and unilateral in 11). The other seven patients had psoas abscess extending beyond intact disc (bilateral in three patients and unilateral in four patients). METHODS Surgical Procedures At first, autogenic cancellous bone as large amount as possible was obtained from unilateral posterior superior iliac spine and stored in a bowl mixed with appropriate antibiotics. Via conventional posterior approach, subtotal laminectomy and discectomy were done like ordinary posterior lumbar interbody fusion (PLIF) procedure. All of the identifiable infected tissues were extirpated with curette and forceps mainly. The epidural abscess was drained using a thin suction tip. Drainage of the psoas abscess was performed by opening the outer fibrous ring of the intervertebral disc with a right-angled hemostat. After those procedures, posterior instrument was fixed in the lordotic position. Previously obtained cancellous autograft mixed with selective antibiotic based on culture studies or empirical choice (gentamicin and cefazolin) for culturenegative was packed into the intervertebral space. Figure 2. Case 13: Imaging studies obtained in a 53-year-old man with pyogenic spondylitis of the L2 3 intervertebral disc space. A, Preoperative radiographs reveal definite bony destruction on L2 and L3. B, Preoperative MR imaging shows grade III destruction of the body, epidural abscess in T2 weight sagittal image, right psoas abscess, and involvement of posterior column in axial image. E September 2016
4 In 14 of the 33 patients, the only infected segment was included in the fixation. In 19 patients, fixation from one or two levels above or below the affected vertebrae was carried out either because an epidural abscess extended beyond the infected segment requiring extensive laminectomy or intervertebral body destruction was too severe to be treated with screw fixation of the affected vertebrae alone. Spinal instrumentation systems applied were Diapason and Xia Spine (Stryker Spine, Cestus, France) in 21 patients and seven patients respectively, and Click X (Synthes-Dupey Spine, Kirkel, Germany) in remaining five patients. All of those were made of Ti6AI4 V alloy having the same biomechanical properties that is, in terms of antibiotic effectiveness, bacterial adherence, and glycocalyx formation. Two pairs of 400 ml evacuator with No. 15 F PVC drainage tubes (four in total) were utilized for the drainage of the intervertebral disc space abscess and epidural abscess. When daily amount of drainage diminishes into below 10 cc for more than two consecutive days, the drainage catheters were gradually pulled out and removed over several days. According to the antibiotic sensitivity of the bacteria, appropriate antibiotics were injected intravenously. According to the ESR and CRP, antibiotic therapy period was determined. In patients causative bacteria were not identified, two of the general antibiotics, cephalosporin and gentamicin, were prescribed. From postoperative second or third day, custom-made rigid thoracic lumbar sacral orthosis (TLSO) brace for thoracolumbar and lumbar sacral orthosis (LSO) for lumbar spine infections were applied for 6 weeks; strictly for the first 3 weeks, thereafter temporary disuse during sleeping time was allowed. between two lines drawn to the superior endplate of the superior vertebral body and the inferior endplate of the inferior vertebral body, was used to assess the sagittal alignment. Fusion Fusion was assessed based on the presence of bridging trabeculae between the bone graft and the adjacent vertebral bodies on the lateral views by two radiologists who were independent of surgeries. Statistical Analysis All data normality was determined with a Kolmogorov- Smirnov test. Paired t test was used to compare the changes in pre- and postoperative ESR and CRP values. Linear mixed model was applied (i) to analyze the sagittal alignment of fixed segment in terms of preoperative, immediate postoperative, and final follow-up state and (ii) to compare the difference between those of the ISFG in the 14 patients and the SSFG in the 19 patients. The null hypothesis was that neither correction loss in sagittal alignment for preoperative state compared with those for last follow up nor difference between the two groups would be shown. The differences in the mean times taken for the ESR and CRP to become normal and ambulation start day in an orthosis between the patients with and without an epidural abscess or psoas abscess were analyzed respectively using the Mann- Whitney U test. The level of significance was set at P < RESULTS Clinical Results Assessment Clinical Assessment Infection Control The ESR and CRP values obtained during admission and outpatient visits after surgery were used as an indicator of infection control. Rehabilitation and Complications Initiation date of ambulation after surgery and occurrence of postoperative complications were reviewed. Radiological Assessment Sagittal Alignment Changes in sagittal alignment of the fixed segment were measured on the lateral plain radiographs before surgery, immediately after surgery, and at the last follow up. In 14 patients in which inflamed segment are the same with fixed segment (inflamed segment fixation group, ISFG), the alignment of inflamed segment was assessed. In 19 patients in which required fixation of additional segment, the alignment of the spanned fixed segment was measured (spanned segment fixation group, SSFG). The Cobb angle, the angle Bacterial Identification and Antibiotic Treatment Causative microorganism was identified in 17 patients, whereas in the other 16 patients, no causative bacteria were identified (Table 2). The IV antibiotics were administered for a mean of 33.9 days (4.8 weeks) after surgery (range, days). Oral antibiotics were not routinely utilized after intravenous antibiotics, however in some patients with delayed normalization time of ESR and CRP, oral antibiotics course followed IV antibiotics for 4 to 6 weeks according to guidance of the infectious disease consultant. ESR and CRP The mean time taken for the ESR to become normal was 69.4 days (range, days, P < 0.01), almost times times longer than that for the CRP, 25.4 days (range, days, P < 0.01). With regard to the presence or absence of epidural abscess, psoas abscess, there was no statistically significant difference in the mean times taken for the ESR and CRP to become normal respectively (P > 0.05). Drainage Total drainage volume was on average 580 cc (range, cc). The period of indwelling drainage was mean 15.8 days (range, 6 32 days). Daily drainage volume decreased Spine E1025
5 TABLE 2. Factors About Infection Control No Organism Initial ESR (mm/hr) Normal ESR (day) Initial CRP (mg/dl) Normal CRP (day) Amount of H/V Insertion day of H/V 1 MSSA ( ) Enterobacter Staphylococcus UTI epidermidis 5 ( ) ( ) MRSA ( ) S. agalactiae MRSA MRSA S.epidermidis ( ) ( ) MRSA ( ) ( ) MRSA ( ) S.epidermidis ( ) MRSA MRSA ( ) ( ) MRSA ( ) ( ) ( ) S.epidermidis MRSA ( ) MRSA H/V indicates hemo-vac; MRSA, methicillin-resistant Staphylococcus Aureus; MSSA, methicillin-susceptible Staphylococcus Aureus; UTI, urinary tract infection. gradually but more than 30 cc was maintained for mean 4.5 days (range, 2 10 days). Ambulation and Complications Ambulation in an orthosis was started at a mean of 5.8 postoperative days (range, 2 19 days). There was no statistically significant in ambulation start day between patients with epidural abscess or not, and psoas abscess or not respectively (P > 0.05). No recurrence of infection or occurrence of complications such as instrument breakage was noted. Radiological Results Fusion Bridging of the trabeculae between the adjacent vertebral bodies across the graft bone that had been packed into the infected disc space was identified on the radiographs at a mean of 5.4 postoperative months in all the patients. Sagittal Alignment Regarding changes in the inflamed segment fixation group (ISFG), the mean amount of Cobb angle correction was 4.18; from of lordosis on average (range, 158 of kyphosis to 228 of lordosis) preoperatively to of lordosis on average (range, 58 of kyphosis to 308 of lordosis) immediately after surgery. Thereafter, the mean Cobb angle changed by 5.48 to kyphosis; of lordosis (range, 88 of kyphosis to 228 of lordosis) at the last follow-up. Totally, there was no significant difference between the preoperative and final results (P ¼ 0.11). Regarding the changes of those in the SSFG, the Cobb angle was improved from preoperative mean 6.98 of lordosis (range, of kyphosis to of lordosis) to of E September 2016
6 Figure 3. Lateral radiographs of a patient with spondylodiscitis in L2 L3 showing development of sagittal alignment after posterior instrumentation to one level above and below the affected vertebrae. A, Preoperative Cobb angle of inflamed segement. B, Postoperative Cobb angle of spanned fixed segment revealing restoration of lordosis. C, Cobb angle at the last follow-up showing maintanence of the lordotic alignment despite 1.98 of loss of correction. lordosis (range, 7.48 of kyphosis to 288 of lordosis) just after surgery. However, gradual loss of correction to kyphosis occurred afterwards and the result was 4.78 of lordosis (range, of kyphosis to 228 of lordosis) (Figure 3 (A C)). There was no statistic difference between the preoperative and final results (P ¼ 0.24). The mean Cobb angle change from before surgery to the last follow up was 1.38 of kyphosis for the ISFG and 2.28 of kyphosis for the SSFG, however did not show significant difference (P ¼ 0.26) and the two groups had similar tendency with their changes from the preoperative, postoperative, and to the last follow-up. Lordosis increased after the fixation then decreased gradually, but maintained the at least preoperative state at the last follow up (Figure 4). In the nine patients, including Grade III destruction, corresponded to SSFG, mean Cobb angle change from before surgery to the last follow-up was 5.48 of kyphosis although the difference was not significant (P ¼ 0.31). DISCUSSION Surgical treatment of spinal infection has developed in tandem with various approaches. Many authors reported that correction of kyphotic deformity was achieved and implant-related complications rarely occurred in the cases treated with anterior fusion combined with anterior instrumentation or posterior instrumentation. 2 9 Recently, various authors obtained promising results with posterior instrumentation and fusion or even minimal invasive instrumentation without anterior debridement in infectious spondylitis and emphasized the importance of stabilization of a diseased segment and appropriate antibiotic therapy. Although various posterior approach through a single posterior incision have been described, to our best knowledge; however, there are few report concerning the clear indication of posterior only approach without anterior procedures in regards to extent of vertebral body destruction, presence and extension of epidural abscess, psoas abscess. Furthermore, we found no report on whether long instrumentation to the uncontaminated level, where screws were not placed in the infected vertebrae could provide better results in terms of infection control, correction, and maintenance of kyphotic correction than instrumentation at the inflamed segment directly where there were the risk of the chance of spreading the infection and loss of correction. Even in patients with epidural abscess, psoas abscess, our approach showed good results in terms of hematological and clinical values. Prolonged drainage of remained abscess using suction drainage tubes and massive debridement of epidural space, psoas muscle may be an effective treatment strategy to decompress the epidural space and prevent the infected-related secondary process. 15,19 Few reports have discussed evaluating the change of sagittal alignment with posterior instrumentation only and our result is comparable with those in other reports including combined anterior and posterior approach. 9,16,20,21 Lee et al 20 reported that maintenance of kyphosis correction with only 1.88 of kyphotic angle loss at the final follow up from the postoperative state could be obtained (through posterior lumbar interbody Spine E1027
7 Figure 4. Devleopment of sagittal alignment. Mean Cobb angle at the last follow up shows difference of 1.38 compared with preoperative angle in the inflamed segment fixation group (ISFG). Sagittal alignment of spanned segment fixation group (SSFG) shows similar pattern. No significant difference of change was seen between two groups (P ¼ 0.26). fusion and pedicle screw fixation in pyogenic discitis). Although the operative technique we used in this study was similar to theirs, loss of kyphosis correction at the last follow up was more common (5.48 of Cobb angle loss) in our study cohorts. We attributed this to the fact that (1) the measuring methods were different; lordotic angle was measured from the upper end-plate of T12 to the upper end-plate of S1 in their study, and from upper endplate of the superior vertebral body and the lower endplate of the inferior vertebral body at fixed segment in our study; (2) the sites of infection were all in singlelevel and lower lumbar vertebra in their series but a total of 8 of 31 our patients were infected in the multilevels and a total of seven thoracolumbar junction and upper lumbar areas were affected; (3) there were more patients with advanced vertebral body destruction than those with discitis (Grade I according to our classification in our study); (4) a pedicle screw was not applied directly to the infected vertebral body, therefore, longer and more stable fixation would be achieved in their study than our study where pedicle screw was inserted including inflamed segment. However, there was no statistic difference between the preoperative and final results of sagittal alignment in the presence series and most of all, our approach demonstrated the successful fusion and complete recovery without recurrence of infection even in severe patients despite loss of kyphotic angle correction. We felt that short instrumentation including the inflamed segment could provide enough stability needed for controlling the infection and screws placed in the inflamed vertebrae may not spread the infection. However, in the patients with extent of the vertebral body destruction was more than 1/3 and less than 2/3 of body height (Grade III), in which loss of degree of kyphosis correction from before the surgery to the last follow up tended to be higher than those in lower grade, longer fixation more than 2 levels above and below the lesion would be needed. When body destruction was more severe (Grade IV), as other articles suggested, fixation with sparing the lesion or a combined anterior and posterior approach with autologous bone graft or titanium mesh cage also would provide stronger stability for restoration and maintenance of the kyphotic correction. 2 9,12,13,21,22 With regard to risk that the implant would be an obstacle on infection treatment, the adhesive strength and formation of a biofilm by bacteria could be subdued with preoperative antibiotic therapy and the occurrence of inflammation could be prevented by necrosis debridement thoroughly before the insertion of an instrument. 20,23 25 Continuous use of drainage and antibiotics before the formation of a biofilm by bacteria would block their growth. In our opinion, proper use of antibiotics and suction drainage is essential for the treatment of anterior lesions via posterior approaches. CONCLUSION We believe that short instrumentation and catheter drainage with posterior only approach would be one of the effective methods that resulted in successful treatment of infection and stability to facilitate early mobilization. Key Points Posterior spinal instrumentation can afford great spinal stability enabling early ambulation. For pyogenic infections, instrumentation has not been applied in fear of aggravation of the infection. We managed pyogenic spondylitis via posterior approach using prolonged suction drainage and short instrumentation, achieving successful control of the infection, solid fusion, early ambulation, and maintenance of sagittal alignment. References 1. Kim YM, Won JH, Seo JB, et al. Pyogenic L4-5 spondylitis managed with percutaneous drainage followed by posterior lumbar interbody fusion: a case report. J Korean Soc Spine Surg 2001;8: Buyukbebeci O, Karakurum G, Guleç A, et al. Tuberculous osteomyelitis of the lumbosacral region: a spinal epidural abscess with presacral extension. Arch Orthop Trauma Surg 2004;124: Chen W-J, Wu C-C, Jung C-H, et al. Combined anterior and posterior surgeries in the treatment of spinal tuberculous spondylitis. Clin Orthop 2002;398: Kim D-J, Yun Y-H, Moon S-H, et al. Posterior instrumentation using compressive laminar hooks and anterior interbody arthrodesis for the treatment of tuberculosis of the lower lumbar spine. Spine 2004;29:E E September 2016
8 5. Sundararaj GD, Babu N, Amritanand R, et al. Treatment of haematogenous pyogenic vertebral osteomyelitis by singlestage anterior debridement, grafting of the defect, and posterior instrumentation. J Bone Joint Surg Br 2007;89: Ha K-Y, Shin J-H, Kim K-W, et al. The fate of anterior autogenous bone graft after anterior radical surgery with or without posterior instrumentation in the treatment of pyogenic lumbar spondylodiscitis. Spine 2007;32: Fukuta S, Miyamoto K, Masuda T, et al. Two-stage (posterior and anterior) surgical treatment using posterior spinal instrumentation for pyogenic and tuberculotic spondylitis. Spine 2003;28: E302 E Hirakawa A, Miyamoto K, Ohno Y, et al. Two-stage (posterior and anterior) surgical treatment of spinal osteomyelitis due to atypical mycobacteria and associated thoracolumbar kyphoscoliosis in a nonimmunocompromised patient. Spine 2008;33:E Klöckner C, Valencia R. Sagittal alignment after anterior debridement and fusion with or without additional posterior instrumentation in the treatment of pyogenic and tuberculous spondylodiscitis. Spine 2003;28: Güven O, Kumano K, Yalçin S, et al. A single stage posterior approach and rigid fixation for preventing kyphosis in the treatment of spinal tuberculosis. Spine 1994;19: Sundararaj GD, Behera S, Ravi V, et al. Role of posterior stabilisation in the management of tuberculosis of the dorsal and lumbar spine. J Bone Joint Surg Br 2003;85: Fushimi K, Miyamoto K, Fukuta S, et al. The surgical treatment of pyogenic spondylitis using posterior instrumentation without anterior debridement. J Bone Joint Surg Br 2012;94: Lin C-P, Ma H-L, Wang S-T, et al. Surgical results of long posterior fixation with short fusion in the treatment of pyogenic spondylodiscitis of the thoracic and lumbar spine: a retrospective study. Spine 2012;37:E Suh KT, Park WW, Kim S-J, et al. Posterior lumbar interbody fusion for adult isthmic spondylolisthesis: a comparison of fusion with one or two cages. J Bone Joint Surg Br 2008;90: Tschoeke SK, Kayser R, Gulow J, et al. Single-stage epidural catheter lavage with posterior spondylodesis in lumbar pyogenic spondylodiscitis with multilevel epidural abscess formation. J Neurol Surg Part Cent Eur Neurosurg 2014;75: Deininger MH, Unfried MI, Vougioukas VI, et al. Minimally invasive dorsal percutaneous spondylodesis for the treatment of adult pyogenic spondylodiscitis. Acta Neurochir (Wien) 2009;151: Nasto LA, Colangelo D, Mazzotta V, et al. Is posterior percutaneous screw-rod instrumentation a safe and effective alternative approach to TLSO rigid bracing for single-level pyogenic spondylodiscitis? Results of a retrospective cohort analysis. Spine J Off J North Am Spine Soc 2014;14: Ha K-Y, Kim Y-H, Seo J-Y, et al. Percutaneous posterior instrumentation followed by direct lateral interbody fusion for lumbar infectious spondylitis. J Spinal Disord Tech 2013;26: E Cottle L, Riordan T. Infectious spondylodiscitis. J Infect 2008;56: Lee JS, Suh KT. Posterior lumbar interbody fusion with an autogenous iliac crest bone graft in the treatment of pyogenic spondylodiscitis. J Bone Joint Surg Br 2006;88: Kuklo TR, Potter BK, Bell RS, et al. Single-stage treatment of pyogenic spinal infection with titanium mesh cages. J Spinal Disord Tech 2006;19: Korovessis P, Repantis T, Iliopoulos P, et al. Beneficial influence of titanium mesh cage on infection healing and spinal reconstruction in hematogenous septic spondylitis: a retrospective analysis of surgical outcome of twenty-five consecutive cases and review of literature. Spine 2008;33:E Oga M, Arizono T, Takasita M, et al. Evaluation of the risk of instrumentation as a foreign body in spinal tuberculosis. Clinical and biologic study. Spine 1993;18: Eysel P, Hopf C, Vogel I, et al. Primary stable anterior instrumentation or dorsoventral spondylodesis in spondylodiscitis? Results of a comparative study. Eur Spine J 1997;6: Maimaiti F, Sheng W, Guo H, et al. Surgical treatment of lumbar pyogenic spondylitis. Chin J Reparative Reconstr Surg 2012;26: Spine E1029
Posterior lumbar interbody fusion with an autogenous iliac crest bone graft in the treatment of pyogenic spondylodiscitis
 Spine Posterior lumbar interbody fusion with an autogenous iliac crest bone graft in the treatment of pyogenic spondylodiscitis J. S. Lee, K. T. Suh From the Pusan National University Hospital, Pusan,
Spine Posterior lumbar interbody fusion with an autogenous iliac crest bone graft in the treatment of pyogenic spondylodiscitis J. S. Lee, K. T. Suh From the Pusan National University Hospital, Pusan,
Surgical treatment of tuberculous spondylodiscitis
 European Review for Medical and Pharmacological Sciences 2012; 1(Suppl 2): 79-85 Surgical treatment of tuberculous spondylodiscitis E. POLA, B. ROSSI, L.A. NASTO, D. COLANGELO, C.A. LOGROSCINO Division
European Review for Medical and Pharmacological Sciences 2012; 1(Suppl 2): 79-85 Surgical treatment of tuberculous spondylodiscitis E. POLA, B. ROSSI, L.A. NASTO, D. COLANGELO, C.A. LOGROSCINO Division
Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion and Posterior Instrumentation
 Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Original Paper Med Princ Pract 2003;12:92 96 DOI: 10.1159/000069113 Received: April 21, 2002 Revised: August 3, 2002 Surgical Treatment of Thoracic and Lumbar Tuberculosis by Anterior Interbody Fusion
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture: Severe Canal Compromise but Neurologically Intact Cases
 CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit
 Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Preliminary Report of Instrumentation in Tuberculous Lumbosacral Spine
 Doi:http://dx.doi.org/10.5704/MOJ.1411.004 Preliminary Report of Instrumentation in Tuberculous Lumbosacral Spine, MRCS Department of Orthopaedic Surgery, Yangon Orthopaedic Hospital, Yangon, Myanmar ABSTRACT
Doi:http://dx.doi.org/10.5704/MOJ.1411.004 Preliminary Report of Instrumentation in Tuberculous Lumbosacral Spine, MRCS Department of Orthopaedic Surgery, Yangon Orthopaedic Hospital, Yangon, Myanmar ABSTRACT
J Korean Soc Spine Surg 2016 Sep;23(3): Originally published online September 30, 2016;
 Journal of Korean Society of Spine Surgery Multifocal Extensive Spinal Tuberculosis Accompanying Isolated Involvement of Posterior Elements - A Case Report - Dong-Eun Shin, M.D., Sang-June Lee, M.D., Young
Journal of Korean Society of Spine Surgery Multifocal Extensive Spinal Tuberculosis Accompanying Isolated Involvement of Posterior Elements - A Case Report - Dong-Eun Shin, M.D., Sang-June Lee, M.D., Young
Anterior Versus Posterior Fixation for the Treatment of Lumbar Pyogenic Vertebral Osteomyelitis
 Anterior Versus Posterior Fixation for the Treatment of Lumbar Pyogenic Vertebral Osteomyelitis Meng Si, MD; Zhi-ping Yang, MD; Zhen-feng Li, MD; Qiang Yang, MD; Jian-min Li, MD abstract Full article available
Anterior Versus Posterior Fixation for the Treatment of Lumbar Pyogenic Vertebral Osteomyelitis Meng Si, MD; Zhi-ping Yang, MD; Zhen-feng Li, MD; Qiang Yang, MD; Jian-min Li, MD abstract Full article available
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
J Korean Soc Spine Surg 2014 Jun;21(2): Originally published online June 30, 2014;
 Journal of Korean Society of Spine Surgery Spinal Epidural Abscess and Psoas Abscess Combined with Pyogenic Spondylodiscitis Following Vertebroplasty - A Case Report - Jin Sung Park, M.D., Dong Hee Kim,
Journal of Korean Society of Spine Surgery Spinal Epidural Abscess and Psoas Abscess Combined with Pyogenic Spondylodiscitis Following Vertebroplasty - A Case Report - Jin Sung Park, M.D., Dong Hee Kim,
Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery
 The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
ASJ. Evaluation of Outcome of Transpedicular Decompression and Instrumented Fusion in Thoracic and Thoracolumbar Tuberculosis. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2017;11(1):31-36 Transpedicular decompression https://doi.org/10.4184/asj.2017.11.1.31 in potts spine Evaluation of Outcome of Transpedicular
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2017;11(1):31-36 Transpedicular decompression https://doi.org/10.4184/asj.2017.11.1.31 in potts spine Evaluation of Outcome of Transpedicular
Single-stage approach of posterior debridement, allograft and internal fixation in management of lumbosacral tuberculosis.
 Biomedical Research 2017; 28 (3): 1448-1452 Single-stage approach of posterior debridement, allograft and internal fixation in management of lumbosacral tuberculosis. Jiawen Wu 1, Juanjuan Wang 2, Ming
Biomedical Research 2017; 28 (3): 1448-1452 Single-stage approach of posterior debridement, allograft and internal fixation in management of lumbosacral tuberculosis. Jiawen Wu 1, Juanjuan Wang 2, Ming
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity. Department of Spine, General Hospital of Lanzhou Command, Gansu, China
 Int Surg 2017;102:171 177 DOI: 10.9738/INTSURG-D-15-00051.1 Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity Xu Lan, Jian-Zhong Xu, Xue-Mei Liu, Bao-Feng Ge Department of Spine,
Int Surg 2017;102:171 177 DOI: 10.9738/INTSURG-D-15-00051.1 Surgical Treatment of Lower Cervical Tuberculosis With Kyphosis Deformity Xu Lan, Jian-Zhong Xu, Xue-Mei Liu, Bao-Feng Ge Department of Spine,
REFERENCE DOCTOR Thoracolumbar Trauma MIS Options. Hyeun Sung Kim, MD, PhD,
 Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Yongchun Zhou 1, Weiwei Li 1*, Jun Liu 1, Liqun Gong 1 and Jing Luo 2*
 Zhou et al. BMC Surgery (2018) 18:71 https://doi.org/10.1186/s12893-018-0405-4 RESEARCH ARTICLE Open Access Comparison of single posterior debridement, bone grafting and instrumentation with single-stage
Zhou et al. BMC Surgery (2018) 18:71 https://doi.org/10.1186/s12893-018-0405-4 RESEARCH ARTICLE Open Access Comparison of single posterior debridement, bone grafting and instrumentation with single-stage
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Hongqi Zhang *, Kefeng Zeng, Xinghua Yin, Jia Huang, Mingxing Tang and Chaofeng Guo
 Zhang et al. Journal of Orthopaedic Surgery and Research (2015) 10:150 DOI 10.1186/s13018-015-0292-7 RESEARCH ARTICLE Open Access Debridement, internal fixation, and reconstruction using titanium mesh
Zhang et al. Journal of Orthopaedic Surgery and Research (2015) 10:150 DOI 10.1186/s13018-015-0292-7 RESEARCH ARTICLE Open Access Debridement, internal fixation, and reconstruction using titanium mesh
W.-Y. YU, C. LOU, F.-J. LIU, D.-W. HE. Introduction. Abstract. OBJECTIVE: Spinal tuberculosis,
 European Review for Medical and Pharmacological Sciences Clinical efficacy of one stage posterior debridement joint graft fixation for lumbar vertebral fractures in spinal tuberculosis patients with compression
European Review for Medical and Pharmacological Sciences Clinical efficacy of one stage posterior debridement joint graft fixation for lumbar vertebral fractures in spinal tuberculosis patients with compression
POSTOPERATIVE COMPLICATIONS IN OPERATED CASES OF PYOGENIC SPONDYLODISCITIS
 Original Article Orthopaedics POSTOPERATIVE COMPLICATIONS IN OPERATED CASES OF PYOGENIC SPONDYLODISCITIS Ravikumar T V 1, Shivprasad M S 2, Yashavatha Kumar 1, Vinay Jain K 3, Mahesh 1 1 -Assistant Professor,
Original Article Orthopaedics POSTOPERATIVE COMPLICATIONS IN OPERATED CASES OF PYOGENIC SPONDYLODISCITIS Ravikumar T V 1, Shivprasad M S 2, Yashavatha Kumar 1, Vinay Jain K 3, Mahesh 1 1 -Assistant Professor,
Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion
 Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Yongchun Zhou, Zongrang Song, Jing Luo, Jijun Liu, Yunfei Huang, Yibin Meng, Wentao Wang and Dingjun Hao *
 Zhou et al. BMC Musculoskeletal Disorders (2016) 17:66 DOI 10.1186/s12891-016-0921-2 RESEARCH ARTICLE Open Access The efficacy of local continuous chemotherapy and postural drainage in combination with
Zhou et al. BMC Musculoskeletal Disorders (2016) 17:66 DOI 10.1186/s12891-016-0921-2 RESEARCH ARTICLE Open Access The efficacy of local continuous chemotherapy and postural drainage in combination with
INTRODUCTION.
 www.jkns.or.kr http://dx.doi.org/1.334/jkns.212.51.4.23 J Korean Neurosurg Soc 51 : 23-27, 212 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 212 The Korean Neurosurgical Society Clinical Article
www.jkns.or.kr http://dx.doi.org/1.334/jkns.212.51.4.23 J Korean Neurosurg Soc 51 : 23-27, 212 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 212 The Korean Neurosurgical Society Clinical Article
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up
 Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up Janek Frantzén M.D., Neurosurgeon Turku University Hospital, Finland ROME SPINE 2011 7.12.2011 1 Clinical Development
Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up Janek Frantzén M.D., Neurosurgeon Turku University Hospital, Finland ROME SPINE 2011 7.12.2011 1 Clinical Development
VLIFT System Overview. Vertebral Body Replacement System
 VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Contact Fusion Cage. Surgical Technique
 Contact Fusion Cage Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by a surgeon experienced
Contact Fusion Cage Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by a surgeon experienced
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Curative effect comparison of anterior and posterior approach in debridement combined with bone graft fusion for the treatment of spinal tuberculosis.
 Biomedical Research 2017; 28 (11): 4832-4836 ISSN 0970-938X www.biomedres.info Curative effect comparison of anterior and posterior approach in debridement combined with bone graft fusion for the treatment
Biomedical Research 2017; 28 (11): 4832-4836 ISSN 0970-938X www.biomedres.info Curative effect comparison of anterior and posterior approach in debridement combined with bone graft fusion for the treatment
Treatment of thoracolumbar burst fractures by vertebral shortening
 Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Solitaire Anterior Spinal System
 Surgical Technique Solitaire Anterior Spinal System Independent Stabilization for the Anterior Column Available in Titanium and Contents Introduction... Page 1 Design Features... Page 2 Instruments...
Surgical Technique Solitaire Anterior Spinal System Independent Stabilization for the Anterior Column Available in Titanium and Contents Introduction... Page 1 Design Features... Page 2 Instruments...
Diagnosis and Treatment of Tuberclous Spondylitis and Pyogenic Spondylitis in Atypical Cases
 Asian Spine Journal Vol. 1, No. 2, pp 75~79, 2007 Diagnosis and Treatment of Tuberclous Spondylitis and Pyogenic Spondylitis in Atypical Cases Jae Sung Ahn, June Kyu Lee Department of Orthopedic Surgery,
Asian Spine Journal Vol. 1, No. 2, pp 75~79, 2007 Diagnosis and Treatment of Tuberclous Spondylitis and Pyogenic Spondylitis in Atypical Cases Jae Sung Ahn, June Kyu Lee Department of Orthopedic Surgery,
Surgical technique. synex. The vertebral body replacement with ratchet mechanism.
 Surgical technique synex. The vertebral body replacement with ratchet mechanism. Table of contents Indications and contraindications 2 Implants 3 Surgical technique 4 Cleaning of instruments 10 Optional
Surgical technique synex. The vertebral body replacement with ratchet mechanism. Table of contents Indications and contraindications 2 Implants 3 Surgical technique 4 Cleaning of instruments 10 Optional
C-THRU Anterior Spinal System
 C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
GIZA Surgical Technique
 GIZA Surgical Technique Vertebral Body Replacement System Manufactured by Titanium alloy material provides mechanical integrity during insertion and distraction, x-ray visibility, and biocompatibility*
GIZA Surgical Technique Vertebral Body Replacement System Manufactured by Titanium alloy material provides mechanical integrity during insertion and distraction, x-ray visibility, and biocompatibility*
The vertebral body replacement with ratchet mechanism. Synex. Surgical Technique
 The vertebral body replacement with ratchet mechanism Synex Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products.
The vertebral body replacement with ratchet mechanism Synex Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products.
Ang Deng, Hong-Qi Zhang, Ming-Xing Tang, Shao-Hua Liu, Qi-Le Gao, Yu-Xiang Wang, Chao-Feng Guo, Xi-Yang Wang
 Int J Clin Exp Med 2016;9(2):3953-3959 www.ijcem.com /ISSN:1940-5901/IJCEM0016644 Original Article One-stage combined posterior and anterior approaches for active tuberculosis of the subaxial cervical
Int J Clin Exp Med 2016;9(2):3953-3959 www.ijcem.com /ISSN:1940-5901/IJCEM0016644 Original Article One-stage combined posterior and anterior approaches for active tuberculosis of the subaxial cervical
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
In the adult population, vertebral discitis and osteomyelitis. Posterior fixation without debridement for vertebral body osteomyelitis and discitis
 Posterior fixation without debridement for vertebral body osteomyelitis and discitis Neurosurg Focus 37 (2):E6, 2014 AANS, 2014 Ahmed S. Mohamed, M.D., 1 Jung Yoo, M.D., 1 Robert Hart, M.D., 1 Brian T.
Posterior fixation without debridement for vertebral body osteomyelitis and discitis Neurosurg Focus 37 (2):E6, 2014 AANS, 2014 Ahmed S. Mohamed, M.D., 1 Jung Yoo, M.D., 1 Robert Hart, M.D., 1 Brian T.
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Thoracoscopic transdiaphragmatic approach for anterior body reconstruction of L2 burst fracture
 Thoracoscopic transdiaphragmatic approach for anterior body reconstruction of L2 burst fracture Jongtae Park MD Department of neurosurgery, School of medicine, Wonkwang University, Iksan, Korea Technical
Thoracoscopic transdiaphragmatic approach for anterior body reconstruction of L2 burst fracture Jongtae Park MD Department of neurosurgery, School of medicine, Wonkwang University, Iksan, Korea Technical
SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY).
 SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY). TRANSVERSECTOMY). Patricia Álvarez González, Javier Pizones Arce, Felisa SánchezS nchez-mariscal, Lorenzo ZúñZ úñiga
SURGICAL INDICATIONS AND COMPLICATIONS OF CAPENER TECHNIQUE (COSTO-TRANSVERSECTOMY). TRANSVERSECTOMY). Patricia Álvarez González, Javier Pizones Arce, Felisa SánchezS nchez-mariscal, Lorenzo ZúñZ úñiga
Synex System TECHNIQUE GUIDE. An expandable vertebral body replacement device
 Synex System TECHNIQUE GUIDE An expandable vertebral body replacement device Original Instruments and Implants of the Association for the Study of Internal Fixation AO ASIF Synex System Overview The Synex
Synex System TECHNIQUE GUIDE An expandable vertebral body replacement device Original Instruments and Implants of the Association for the Study of Internal Fixation AO ASIF Synex System Overview The Synex
There is No Remarkable Difference Between Pedicle Screw and Hybrid Construct in the Correction of Lenke Type-1 Curves
 DOI: 10.5137/1019-5149.JTN.20522-17.1 Received: 11.04.2017 / Accepted: 12.07.2017 Published Online: 21.09.2017 Original Investigation There is No Remarkable Difference Between Pedicle Screw and Hybrid
DOI: 10.5137/1019-5149.JTN.20522-17.1 Received: 11.04.2017 / Accepted: 12.07.2017 Published Online: 21.09.2017 Original Investigation There is No Remarkable Difference Between Pedicle Screw and Hybrid
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
Comparison of clinical, radiological and functional outcome of short segment V/S long segment posterior fixation of tuberculosis of spine
 2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
2018; 2(4): 104-108 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(4): 104-108 Received: 20-08-2018 Accepted: 21-09-2018 Dr. Mitul Mistry Assistant Professor,
SYNEX The vertebral body replacement with ratchet mechanism
 SYNEX The vertebral body replacement with ratchet mechanism Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image
SYNEX The vertebral body replacement with ratchet mechanism Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image
ASJ. Radiologic and Clinical Courses of Degenerative Lumbar Scoliosis (10 25 ) after a Short-Segment Fusion. Asian Spine Journal.
 Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June Section: Surgery Last Reviewed Date: June 2013
 Medical Policy Manual Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June 2007 Section: Surgery Last Reviewed Date: June 2013 Policy No: 157 Effective Date: August 1, 2013 IMPORTANT REMINDER
Medical Policy Manual Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June 2007 Section: Surgery Last Reviewed Date: June 2013 Policy No: 157 Effective Date: August 1, 2013 IMPORTANT REMINDER
nva Anterior Lumbar Interbody Fusion System
 nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
PARADIGM SPINE. Anterior Cervical Fusion Cage. Cervical Interbody Fusion
 PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Spinal Terminology Basics
 Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
OPERATIVE TECHNIQUE. CONSTRUX Mini PTC. Mini PTC Spacer System
 OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic Spondylolisthesis
 Case Reports in Orthopedics Volume 2015, Article ID 426940, 4 pages http://dx.doi.org/10.1155/2015/426940 Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic
Case Reports in Orthopedics Volume 2015, Article ID 426940, 4 pages http://dx.doi.org/10.1155/2015/426940 Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic
MRI findings in proven Mycobacterium tuberculosis (TB) spondylitis
 CASE ORIGINAL REPORT ARTICLE MRI findings in proven Mycobacterium tuberculosis (TB) spondylitis D J Kotzé, MB ChB L J Erasmus, MB ChB Department of Diagnostic Radiology, University of the Free State, Bloemfontein
CASE ORIGINAL REPORT ARTICLE MRI findings in proven Mycobacterium tuberculosis (TB) spondylitis D J Kotzé, MB ChB L J Erasmus, MB ChB Department of Diagnostic Radiology, University of the Free State, Bloemfontein
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
SynCage. Surgical Technique. This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
 SynCage Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning This description alone
SynCage Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning This description alone
Posterior wedge osteotomy and debridement for Andersson lesion with severe kyphosis in ankylosing spondylitis
 Liang et al. Journal of Orthopaedic Surgery and Research (2017) 12:54 DOI 10.1186/s13018-017-0556-5 RESEARCH ARTICLE Open Access Posterior wedge osteotomy and debridement for Andersson lesion with severe
Liang et al. Journal of Orthopaedic Surgery and Research (2017) 12:54 DOI 10.1186/s13018-017-0556-5 RESEARCH ARTICLE Open Access Posterior wedge osteotomy and debridement for Andersson lesion with severe
Vertebral column decancellation for the management of sharp angular spinal deformity
 Eur Spine J (2011) 20:1703 1710 DOI 10.1007/s00586-011-1771-0 ORIGINAL ARTICLE Vertebral column decancellation for the management of sharp angular spinal deformity Yan Wang Lawrence G. Lenke Received:
Eur Spine J (2011) 20:1703 1710 DOI 10.1007/s00586-011-1771-0 ORIGINAL ARTICLE Vertebral column decancellation for the management of sharp angular spinal deformity Yan Wang Lawrence G. Lenke Received:
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
L-VARLOCK. Posterior Lumbar Cage with adjustable lordosis. S urgical T echnique
 L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
The Fusion of Power and Performance.
 The Fusion of Power and Performance. Leading the Way in Lumbar Interbody Fusion with 1 Years of Clinical Results. The JAGUAR Lumbar I/F CAGE System, approved in the U.S. in February 1999, has revolutionized
The Fusion of Power and Performance. Leading the Way in Lumbar Interbody Fusion with 1 Years of Clinical Results. The JAGUAR Lumbar I/F CAGE System, approved in the U.S. in February 1999, has revolutionized
Idiopathic scoliosis Scoliosis Deformities I 06
 What is Idiopathic scoliosis? 80-90% of all scolioses are idiopathic, the rest are neuromuscular or congenital scolioses with manifest primary diseases responsible for the scoliotic pathogenesis. This
What is Idiopathic scoliosis? 80-90% of all scolioses are idiopathic, the rest are neuromuscular or congenital scolioses with manifest primary diseases responsible for the scoliotic pathogenesis. This
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Kyung Hee University Spine Centre Kyung Hee University Hospital at Gang Dong Seoul, South Korea
 Report for APSS-Depuy-Synthes Clinical Fellowship 2013 Centre: Kyung Hee University Spine Centre Kyung Hee University Hospital at Gang Dong Seoul, South Korea Supervisor: Prof Kim Ki-Tack Fellow: Dr Tony
Report for APSS-Depuy-Synthes Clinical Fellowship 2013 Centre: Kyung Hee University Spine Centre Kyung Hee University Hospital at Gang Dong Seoul, South Korea Supervisor: Prof Kim Ki-Tack Fellow: Dr Tony
SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS
 STUDY SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS *Hashem, N.; **A Subai, N. *Faculty of Medicine, Ains Shams University, Egypt ^Department of Orthopedics,
STUDY SHORT SEGMENT FIXATION THORACOLUMBAR UNSTABLE BURST FRACTURES USING DC PLATES & PEDICLE SCREWS *Hashem, N.; **A Subai, N. *Faculty of Medicine, Ains Shams University, Egypt ^Department of Orthopedics,
Osteoporotic Compression Fracture of Spine Treated With Posterior Instrumentation and Transpedicular Bone Grafting
 http://dx.doi.org/10.5704/moj.1211.003 Osteoporotic Compression Fracture of Spine Treated With Posterior Instrumentation and Transpedicular Bone Grafting Foead AI, MS Orth, Thanapipatsiri S*, MD, Pichaisak
http://dx.doi.org/10.5704/moj.1211.003 Osteoporotic Compression Fracture of Spine Treated With Posterior Instrumentation and Transpedicular Bone Grafting Foead AI, MS Orth, Thanapipatsiri S*, MD, Pichaisak
Surgical Technique INTERSOMATIC CERVICAL CAGE
 R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
Primary Posterior Fixation For Tuberculosis Of The Spine
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 10 Number 1 B Jadav, M Prabhakar Citation B Jadav, M Prabhakar.. The Internet Journal of Orthopedic Surgery. 2007 Volume 10 Number 1. Abstract
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 10 Number 1 B Jadav, M Prabhakar Citation B Jadav, M Prabhakar.. The Internet Journal of Orthopedic Surgery. 2007 Volume 10 Number 1. Abstract
Surgical treatment of preschool childhood spinal thoracic tuberculosis: two case reports and technical note
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Surgical treatment of preschool childhood spinal thoracic tuberculosis: two case reports and technical note Mehmet Nuri Erdem, Anas
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Surgical treatment of preschool childhood spinal thoracic tuberculosis: two case reports and technical note Mehmet Nuri Erdem, Anas
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Single stage posterior instrumentation and anterior interbody fusion for tuberculosis of dorsal and lumbar spines
 Original Article interbody fusion for tuberculosis of dorsal Pandey BK 1, Sangondimath GM 2, Chhabra HS 2 1 Department of Orthopaedics, Kathmandu Medical College Teaching Hospital, Sinamangal, Kathmandu,
Original Article interbody fusion for tuberculosis of dorsal Pandey BK 1, Sangondimath GM 2, Chhabra HS 2 1 Department of Orthopaedics, Kathmandu Medical College Teaching Hospital, Sinamangal, Kathmandu,
PILLAR AL. Anterior Lumbar Interbody Fusion (ALIF) and Partial Vertebral Body Replacement (pvbr) PEEK Spacer System OPERATIVE TECHNIQUE
 PILLAR AL PEEK Spacer System Anterior Lumbar Interbody Fusion (ALIF) and Partial Vertebral Body Replacement (pvbr) OPERATIVE TECHNIQUE Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE TECHNIQUE 3 OPERATIVE
PILLAR AL PEEK Spacer System Anterior Lumbar Interbody Fusion (ALIF) and Partial Vertebral Body Replacement (pvbr) OPERATIVE TECHNIQUE Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE TECHNIQUE 3 OPERATIVE
Treatment Of Spondylodiscitis, Epidural Abscess And Spondylitis A Retrospective Study Of 20 Cases With Exclusion Of TB Cases
 BMH Med. J. 2019;6(1):4-12. Research Article Treatment Of Spondylodiscitis, Epidural Abscess And Spondylitis A Retrospective Study Of 20 Cases With Exclusion Of TB Cases Suresh S Pillai 1, Arunkumar C
BMH Med. J. 2019;6(1):4-12. Research Article Treatment Of Spondylodiscitis, Epidural Abscess And Spondylitis A Retrospective Study Of 20 Cases With Exclusion Of TB Cases Suresh S Pillai 1, Arunkumar C
Late Infection of Spinal Instrumentation
 Abstract Late Infection of Spinal Instrumentation Jae-Ik Shim, M.D., Taik-Seon Kim, M.D., Sung-Jong Lee, M.D., Suk-Ha Lee, M.D., Dong-Ki Lee, M.D., Yoen-Sik Yu, M.D., Yun-Yeup Kim, M.D. Department of Orthopaedic
Abstract Late Infection of Spinal Instrumentation Jae-Ik Shim, M.D., Taik-Seon Kim, M.D., Sung-Jong Lee, M.D., Suk-Ha Lee, M.D., Dong-Ki Lee, M.D., Yoen-Sik Yu, M.D., Yun-Yeup Kim, M.D. Department of Orthopaedic
nvp Posterior Lumbar Interbody Fusion System
 nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvt Transforaminal Lumbar Interbody Fusion System
 nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
vertebra associated with dura) ectasia in
 e287 Case Report Grade 4 spondylolisthesis of the L5 vertebra associated with dura) ectasia in neurofibromatosis Modi H N, Srinivasalu S, Suh S W, Yang J H ABSTRACT Spondylolisthesis associated with neurofibromatosis
e287 Case Report Grade 4 spondylolisthesis of the L5 vertebra associated with dura) ectasia in neurofibromatosis Modi H N, Srinivasalu S, Suh S W, Yang J H ABSTRACT Spondylolisthesis associated with neurofibromatosis
The effect of body mass index on lumbar lordosis on the Mizuho OSI Jackson spinal table
 35 35 40 The effect of body mass index on lumbar lordosis on the Mizuho OSI Jackson spinal table Authors Justin Bundy, Tommy Hernandez, Haitao Zhou, Norman Chutkan Institution Orthopaedic Department, Medical
35 35 40 The effect of body mass index on lumbar lordosis on the Mizuho OSI Jackson spinal table Authors Justin Bundy, Tommy Hernandez, Haitao Zhou, Norman Chutkan Institution Orthopaedic Department, Medical
To study the outcomes of posterior decompression and fixation of tuberculosis of dorsolumbar spine
 2017; 3(3): 691-695 ISSN: 2395-1958 IJOS 2017; 3(3): 691-695 2017 IJOS wwworthopapercom Received: 15-05-2017 Accepted: 16-06-2017 Dr Manish Shah Assistant Professor, Department of Dr Kushal Suthar Dr Ravindra
2017; 3(3): 691-695 ISSN: 2395-1958 IJOS 2017; 3(3): 691-695 2017 IJOS wwworthopapercom Received: 15-05-2017 Accepted: 16-06-2017 Dr Manish Shah Assistant Professor, Department of Dr Kushal Suthar Dr Ravindra
CROSS -FUSE P E E K V B R / I B F SYST E M
 S U R G I C A L T E C H N I Q U E CROSS -FUSE P E E K V B R / I B F SYST E M S U R G I C A L S Y S T E M O V E R V I E W 2 CROSS-FUSE P E E K V B R / I B F S Y S T E M S U R G I C A L T E C H N I Q U E
S U R G I C A L T E C H N I Q U E CROSS -FUSE P E E K V B R / I B F SYST E M S U R G I C A L S Y S T E M O V E R V I E W 2 CROSS-FUSE P E E K V B R / I B F S Y S T E M S U R G I C A L T E C H N I Q U E
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
