Thoracic Paravertebral Block Manoj K. Karmakar, F.R.C.A.*
|
|
|
- Noah Parsons
- 5 years ago
- Views:
Transcription
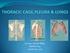
1 REVIEW ARTICLE David C. Warltier, M.D., Ph.D., Editor Anesthesiology 2001; 95: American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Thoracic Paravertebral Block Manoj K. Karmakar, F.R.C.A.* THORACIC paravertebral block (TPVB) is the technique of injecting local anesthetic adjacent to the thoracic vertebra close to where the spinal nerves emerge from the intervertebral foramina. This results in ipsilateral somatic and sympathetic nerve blockade in multiple contiguous thoracic dermatomes above and below the site of injection. 1 3 It is effective in treating acute 2 8 and chronic 3,9,10 pain of unilateral origin from the chest and abdomen. Bilateral use of TPVB has also been described Our understanding of the safety and efficacy of TPVB has improved significantly in the last two decades, prompting its use in children 12,17 23 and neonates 20,22 and for surgical anesthesia. 11,14,16,24 26 History Hugo Sellheim of Leipzig ( ) pioneered paravertebral block in 1905, and used the technique to produce abdominal analgesia. Arthur Lawen refined Sellheim s technique in 1911 and called it paravertebral conduction anesthesia. 29 Kappis developed the technique comparable to the one in present-day use 27 and in 1919, produced surgical anesthesia for abdominal surgery. 30 After its initial popularity, TPVB was neglected until 1979, when Eason and Wyatt 3 revisited TPVB and rekindled interest by describing a catheter technique. The last two decades have seen renewed interest in this form of afferent nerve blockade. Sabanathan, Richardson and Lönnqvist are three researchers who recently have contributed substantially to improving our understanding of this almost-forgotten technique. Anatomy The thoracic paravertebral space (TPVS) is a wedgeshaped space 31 that lies on either side of the vertebral *Associate Professor. Received from the Department of Anesthesia & Intensive Care, The Chinese University of Hong Kong, Shatin, Hong Kong. Submitted for publication May 25, Accepted for publication February 12, Support was provided solely from institutional and/or departmental sources. Address reprint requests to Dr. M. K. Karmakar: Department of Anesthesia & Intensive Care, The Chinese University of Hong Kong, Prince of Wales Hospital, Shatin, New Territories, Hong Kong. Address electronic mail to: karmakar@cuhk.edu.hk. Individual article reprints may be purchased through the Journal Web site, column (fig. 1). It is wider on the left than on the right. 32 The parietal pleura forms the anterolateral boundary, while the base is formed by the posterolateral aspect of the vertebral body, the intervertebral disc, the intervertebral foramen and its contents. 3,31 The superior costotransverse ligament, which extends from the lower border of the transverse process above to the upper border of the transverse process below, forms the posterior wall of the TPVS. The apex of the space is continuous, with the intercostal space lateral to the tips of the transverse processes. 3,31 Interposed between the parietal pleura and the superior costotransverse ligament is a fibroelastic structure, 33 the endothoracic fascia (figs. 1 and 2), which is the deep fascia of the thorax 35,37,38 and lines the inside of the thoracic cage. 33,35 38 In the paravertebral location, the endothoracic fascia is closely applied to the ribs 31 and fuses medially with the periosteum at the midpoint of the vertebral body. 36 An intervening layer of loose connective tissue, the subserous fascia, is found between the parietal pleura and the endothoracic fascia. The endothoracic fascia thus divides the TPVS into two potential fascial compartments, the anterior extrapleural paravertebral compartment and the posterior subendothoracic paravertebral compartment (fig. 1). 37,38 The TPVS contains fatty tissue, 31,33 within which lies the intercostal (spinal) nerve, the dorsal ramus, the intercostal vessels, the rami communicantes, and, anteriorly, the sympathetic chain. 3,31 The spinal nerves in the TPVS are segmented into small bundles lying freely among the fat and devoid of a fascial sheath, which makes them exceptionally susceptible to local anesthetic block. 39 The intercostal nerve and vessels are located behind the endothoracic fascia, 40,41 while the sympathetic trunk is located anterior to it 36,41 in the TPVS (fig. 1). Communications of the Thoracic Paravertebral Space The TPVS is continuous with the intercostal space laterally, 36,37,39,42 45 the epidural space medially via the intervertebral foramen, 31,42,45,46 and the contralateral paravertebral space via the prevertebral 34,37 and epidural space. 31 The cranial extension of the TPVS is still not defined, but we have observed radiologic spread of 771
2 772 MANOJ K. KARMAKAR Fig. 1. Anatomy of the thoracic paravertebral space. contrast medium into the cervical region after thoracic paravertebral injection. The origin of the psoas major muscle forms the caudal boundary, 47 and inferior (lumbar) spread through the TPVS is thought to be unlikely. 47 Ipsilateral thoracolumbar anesthesia, 48 radiologic spread of contrast below the diaphragm, 45 and thoracolumbar spread of colored dye in cadavers 49 have been described, and there is disagreement about the caudal limit of spread. 1 The endothoracic fascia is continuous inferiorly with the fascia transversalis of the abdomen dorsal to the diaphragm through the medial and lateral arcuate ligaments and the aortic hiatus. 35,38 An injection in the lower TPVS posterior to the endothoracic fascia 50 can spread inferiorly through the medial and lateral arcuate ligaments 50,51 to the retroperitoneal space behind the fascia transversalis, where the lumbar spinal nerves lie, 50 and is the anatomic basis of the technique of extended unilateral anesthesia. 51 Fig. 2. Saggital section through the thoracic paravertebral space showing a needle that has been advanced above the transverse process. Techniques of Thoracic Paravertebral Block Several different techniques exist for TPVB. It can be performed with the patient in the sitting, lateral, or prone position. The sitting position allows easy identification of landmarks, and the patients are often more comfortable. The classical technique, which is most commonly used, involves eliciting loss of resistance. 3 At the appropriate dermatome under aseptic precautions, the needle (22-gauge, 8 10-cm short beveled spinal needle, or a Tuohy needle if a catheter is to be placed) is inserted cm lateral to the most cephalad aspect of the spinous process and advanced perpendicular to the skin in all planes to contact the transverse process 3 of the vertebra below at a variable depth (2 4 cm) depending on the build of the individual. If bone is not encountered at this depth, it is possible that the needle tip is lying between adjacent transverse processes. It is imperative to locate the transverse process before advancing the needle any further to prevent inadvertent deep insertion and possible pleural puncture. This is accomplished by withdrawing the needle to the subcutaneous plane and redirecting it cephalad and caudad to the same depth until bone is encountered. If bone is still not encountered, the needle is advanced a further centimeter and the above process repeated until the transverse process is contacted. The needle is then walked above the transverse process (fig. 2) and gradually advanced until a loss of resistance 3 to air or saline, or a subtle pop is felt as the needle tip traverses the thin superior costotransverse ligament, usually within cm from the superior edge of the transverse process. After gentle aspiration, local anesthetic is injected in small aliquots or a catheter is inserted so that 1 3 cm of the distal end of the catheter lies within the TPVS. The same technique is used with modification in children, 17,18,30,52,53 and two simple equations help predict
3 THORACIC PARAVERTEBRAL BLOCK 773 the lateral distance for needle insertion and the skin-to- TPVS depth (both in millimeters): [10.2 (0.12 weight in kilograms)] and [ (weight in kilograms)], respectively. 53 Various investigators also redirect their needle medially 29 to contact the vertebra, advance caudal to the transverse process, 26,46,54 or elicit paresthesia. 10,54,55 Medial redirection is not recommended because of the potential for epidural or intrathecal injection. Unlike epidural space location, where a definite give is felt as the needle tip traverses the firm ligamentum flavum, TPVS location using loss of resistance is subjective and indefinite 28,56 and may not be appreciated as a definite give. 23 Difficulty is also commonly encountered during catheter insertion and may require manipulation of the needle 3,23 or injection of saline to create a salinefilled cavity before passing a catheter. Very easy passage of the catheter may indicate interpleural placement. 43 The needle may be advanced by a fixed predetermined distance (1 2 cm) 2,26 once the needle is walked off the transverse process without eliciting loss of resistance. 2,11,26 This variation has been used very effectively with low risk of complication, including pneumothorax. 2,11,26 The use of a depth marker is recommended if a nongraduated needle is used to avoid pleural or pulmonary puncture. Fluoroscopy 46 and contrast chest radiography 28,46,57 are often used as supplementary methods to confirm the position of the needle or catheter. Contrast injected into the TPVS produces either a longitudinal or a cloud-like spread localized to the paravertebral region as depicted on frontal chest radiograph. 57 Radiologic images are not always readily identifiable, 56 and spread can vary in the same patient having repeated injections. 46 A pressure measurement technique was recently advocated. 56 Pressure in the erector spinae muscle is higher during inspiration than during expiration. 56 Once the superior costotransverse ligament is traversed and the TPVS entered, there is a sudden lowering of pressure, and expiratory pressure then exceeds inspiratory pressure: pressure inversion. 56 These objective signs are described as an easy and reproducible method of locating the TPVS. 56 Negative pressure during both phases of respiration would indicate interpleural placement. 58 A modification of the classical approach is the medial approach 59 in which the needle is inserted 1 cm from the midline and advanced perpendicularly to contact the lamina rather than the transverse process followed by lateral redirection to slip off the lamina into the TPVS. 59,60 Developed initially to avoid intrathecal injection by directing the needle away from the intervertebral foramen, 59 this approach has been associated with complications relating to dural puncture. 60,61 A recent variation of the medial approach is the paravertebral peridural block, 34 in which the needle is inserted 3 4 cm lateral to the midline and advanced at a 45 angle to the coronal plane with medial direction to contact the lamina. The needle is then redirected laterally by gradual increments in the angle of entry to the coronal plane until the needle is walked off the lamina into the TPVS. 34 Retrospective analyses using the paravertebral peridural block technique report a high success rate and low incidence of complications. 34 Thoracic paravertebral catheters can also be safely, accurately, and easily placed under direct vision during thoracic surgery from within the chest. 21,22,62 The original description by Sabanathan et al. 62 involves reflecting the parietal pleura from the posterior wound margin on to the vertebral bodies to create an extrapleural paravertebral pocket into which a percutanously inserted catheter is placed against the angles of the exposed ribs. This method has been refined to ensure accurate placement of the catheter in the TPVS by tunneling the tip through a small defect created by the surgeon in the extrapleural fascia, 63 rather than laying it adjacent to the vertebral bodies. 62 The anatomy of the extrapleural fascia is not clear, 63 and the endothoracic fascia may have been referred to as the extrapleural fascia. This method, which requires an open chest, has been combined very effectively with preincisional percutaneous thoracic paravertebral injection to provide both intraoperative and postoperative analgesia after thoracic surgery. 7,64 Videoassisted placement of a paravertebral catheter under direct vision during thoracoscopic surgery has also been described. 15 Mechanism and Spread of Anesthesia A thoracic paravertebral injection may remain localized to the level injected, 65 or it may spread to the contiguous levels above and below, 37,42,45 the intercostal space laterally, 42,45,46 the epidural space medially, 31,45,46 or a combination of the above to affect ipsilateral somatic 1,2,5,48,66 and sympathetic nerves, 1,66 including the posterior primary ramus 3 in multiple contiguous thoracic dermatomes. There are no published data that compare the effects of volume or dose of local anesthetic on the dermatomal distribution of TPVB. Eason and Wyatt 3 found that at least four intercostal spaces could be covered by a single 15-ml injection of 0.375% bupivacaine. More recently, 15 ml of bupivacaine 0.5% injected into the TPVS has been shown to produce mean unilateral somatic block over 5 (range, 1 9) dermatomes and sympathetic block over 8 (range, 6 10) dermatomes. 1 Similarly, 1.5 mg/kg bupivacaine 0.5% produced sensory loss at the level of injection with a mean superior spread of 1.4 (range, 0 4) dermatomes and a mean inferior spread of 2.8 (range, 0 7) dermatomes. 48 In children, 0.25 ml/kg (SD, 0.12) of contrast medium injected into the TPVS produces radiologic spread over 5.7 segments (SD, 1.6). 57 Thoracic paraverte-
4 774 MANOJ K. KARMAKAR Table 1. Advantages of Thoracic Paravertebral Block Technical Simple and easy to learn Safer and easier than thoracic epidural Palpation of rib not necessary and scapula does not interfere with block Safe to perform in sedated and ventilated patients Catheter placement under direct vision during thoracic surgery is safe and accurate Chest drain loss of local anesthetic is four times lower than that of interpleural block bral anesthesia does not appear to be gravity-dependent, but there is a tendency for preferential caudal spread of somatic 1,2,5,48 and sympathetic blockade. 1 There is controversy about epidural spread and its contribution to the extension of TPVB. Radioopaque contrast medium infused postoperatively through an extrapleural paravertebral catheter placed intraoperatively under direct vision remains confined to the paravertebral space. 8,67 In contrast, varying degrees of epidural spread has been shown to occur after 70% of percutaneous paravertebral injections, 46 which is mostly unilateral, 46 and the volume involved is considered too small to produce clinically significant epidural block. 68 Cadaveric dissection also confirms that only a small proportion of the injectate enters the epidural space 42 and remains confined to the side of injection. The vertebral attachment of the endothoracic fascia attenuates prevertebral spread 36,40 and may also influence epidural spread or mass movement of drug after an extrapleural paravertebral compartment injection. Clinically, sensory anesthesia is predominantly ipsilateral and greater after epidural spread than after only paravertebral spread. 46 Current evidence therefore suggests that ipsilateral epidural spread of discrete amounts of local anesthetic occurs after thoracic paravertebral injection, which contributes to the extension of a TPVB. Bilateral symmetrical anesthesia 11,46,69 72 is described and may be caused by extensive epidural spread 46 or inadvertent intrathecal injection into the dural sleeve, 61 and may occur more commonly with the median injection technique 59,61 or the use of large volumes of injectate ( 25 ml) 70 Segmental contralateral anesthesia 2,57 adjacent to the site of injection occurs in 1.1% of paravertebral injections 68 and may be caused by either prevertebral spread 34,37,57,73 or epidural spread 31,65 to the contralateral TPVS. Bilateral sympathetic blockade may occur in the absence of bilateral sensory blockade 34 caused by prevertebral spread 34,37,73 to the contralateral sympathetic chain, which is more anteriorly placed in the TPVS and also more sensitive to local anesthetic agents. This may be one explanation for bilateral Horner syndrome reported after unilateral TPVB. 46 Ipsilateral lumbar spinal nerves are also occasionally involved, 1,48 and this may be caused by an extended subendothoracic fascial spread to the retroperitoneal space (vide supra) or epidural spread. There are no published data comparing the distribution of anesthesia after a single-site versus a multiple-site percutaneous thoracic paravertebral injection. Current evidence suggests that a single-site injection of % bupivacaine, ml or 0.3 ml/kg. 1,3,72 is as effective as a multiple-site injection of 0.5% bupivacaine, 3 4 ml per site, 11,14,16,26 in producing unilateral anesthesia over four to five thoracic dermatomes. The effect of increasing the volume of local anesthetic injected into a single site is not known but may predispose to bilateral sensory blockade. 70 Therefore, if a wide unilateral thoracic block (i.e., 5 dermatomes) is desired, it may be preferable to inject at multiple contiguous sites 11,14,26 or at two separate sites several dermatomes apart. 3 This may be one of the reasons why TPVB is not commonly used. Indications Thoracic paravertebral block offers several technical and clinical advantages (table 1) and is indicated for anesthesia and analgesia when the afferent pain input is predominantly unilateral from the chest and abdomen. Reported indications are listed in table 2. Bilateral TPVB has also been used perioperatively during thoracic, 12,15 major abdominal vascular, 13 and breast 11,16 surgeries. Contraindications Clinical Single injection produces multidermatomal ipsilateral somatic and sympathetic nerve block Reliably blocks the posterior primary ramus Abolishes cortical responses to thoracic dermatomal stimulation Inhibits stress and pressor response to surgical stimuli Maintains hemodynamic stability Reduces opioid requirements Low incidence of complication Preserves bladder sensation Preserves lower limb motor power Promotes early mobilization No additional nursing vigilance required Infection at the site of needle insertion, empyema, allergy to local anesthetic drugs, and tumor occupying the TPVS are some of the few contraindications. A coagulopathy, bleeding disorder or therapeutic anticoagulation are considered as relative contraindications for TPVB. 28 One must exercise caution in patients with kyphoscoliosis and patients who have had previous thoracotomy. Chest deformity in the former may predispose
5 THORACIC PARAVERTEBRAL BLOCK 775 Table 2. Reported Indications for Thoracic Paravertebral Block Postoperative analgesia Thoracic surgery Breast surgery Cholecystectomy Renal and ureteric surgery Herniorrhaphy Appendicectomy Video-assisted thoracoscopic surgery Minimally invasive cardiac surgery Surgical anesthesia Breast surgery Herniorrhaphy Chest wound exploration in a single lung transplant recipient Acute postherpetic neuralgia Chronic pain management: benign and malignant neuralgia Miscellaneous Fractured ribs Therapeutic control of hyperhydrosis Liver capsule pain after blunt abdominal trauma to thecal or pleural puncture, whereas obliteration of the TPVS by scar tissue and adhesion of the lung to the chest wall 74 in the latter may predispose to pleural and pulmonary puncture. TPVB can be used in patients undergoing pleurectomy as long as the parietal pleura over the TPVS medial to the angle of the rib is left intact. 15,75 Drugs Used and Dosage There are no published data that describe an optimal dose or concentration of local anesthetic for either single-shot injection or continuous thoracic paravertebral infusion. For a multiple level TPVB, 3 4 ml of bupivacaine 0.5% 11,14,26 or ropivacaine 0.5% 25 with epinephrine (2.5 g/ml) is injected at each segment. On the other hand, for a single-level thoracic paravertebral injection and continuous thoracic paravertebral infusion, bupivacaine 1,3,18,20,22,48,76 79 and lidocaine 8,52,80 with or without epinephrine are used, and the commonly reported dosage schedules in adults and children are outlined in table 3. Pharmacokinetics In adults, the commonly used bolus dose of 20 ml 0.5% bupivacaine results in a mean (SEM) maximum concentration of 1.45 (0.32) g/ml in a median time of 25 min (range, min). 76 Peak arterial plasma concentration and time to peak concentration were compared in 20 patients undergoing thoracotomy after bupivacaine 0.25% (1 mg/kg) with or without epinephrine (5 g/ml). 77 The time to peak concentration was 5 min (range, 5 20 min) in both groups, and there were small differences in peak plasma concentrations that were not statistically significant. 77 After continuous infusion of bupivacaine 0.5% at 0.1 ml kg 1 h 1 for 120 h, there was a gradual increase to a mean (SEM) peak total bupivacaine concentration of 4.92 (0.7) g/ml at 48 h (range, 5 96 h), after which there was a small but insignificant decrease in concentration. 76 There were no clinical signs of toxicity, and bupivacaine levels as high as 7.48 g/ml were measured in one patient. 76 Other investigators have also reported progressive accumulation of bupivacaine in plasma during continuous thoracic paravertebral infusion without clinical signs of toxicity, 78,79,81 although bupivacaine levels have often exceeded the threshold for central nervous system toxicity (2 4.5 g/ml). 80 This may account for the few reported cases of postoperative confusion that resolved after temporary cessation of the infusion. 82 In children with a median age of 5.3 weeks, a loading dose of 1.25 mg/kg of bupivacaine 0.25% resulted in mean (SD) maximum serum bupivacaine concentration of 1.03 (0.56) g/ml in a median time of 10 min (range, min). 22 Lidocaine 1% with epinephrine (5 g/ml) as a 0.5-ml/kg loading dose in children aged 1 month to12 yr resulted in peak plasma concentrations ranging between 1.7 and 3.0 g/ml within min after injection. 52 A continuous infusion of bupivacaine (0.25% at 0.5 mg kg 1 h 1 ) in small infants resulted in a mean (SD) maximum serum bupivacaine concentration of 2.0 (0.63) g/ml in 24 h with no clinical toxicity. 22 There was wide variation in bupivacaine concentrations (range, g/ml) between individual infants. 22 In a follow-up study of even smaller infants (median age, 1.5 weeks) given half the dose of bupivacaine (0.125%, 0.25 mg kg 1 h 1 ) with epinephrine (2.5 g/ml) as a continuous infusion, the mean (SD) serum bupivacaine concentration at 48 h was 1.60 (0.67) g/ml, and no patient showed clinical signs of toxicity. 20 Bupivacaine concentration exceeded 3 g/ml in three patients at h. 20 In the only report describing the pharmacokinetics of lidocaine 1% at 0.25 ml kg 1 h 1 for thoracic paravertebral infusion in children over a 10-h period, plasma concentration ranged from 2.1 to 3.2 g/ml. 52 Although total bupivacaine level increases steadily during prolonged thoracic paravertebral infusion, free bupivacaine concentrations remain unchanged. 79 This may be a result of the increase in 1 -acid glycoprotein concentrations postoperatively 79,83 offering protection against bupivacaine toxicity by increasing the binding of bupivacaine. There is also a greater increase in the S- bupivacaine enantiomer, 76,81 which is associated with lower toxicity than the R-bupivacaine enantiomer. Because of concerns of systemic accumulation and potential for toxicity with bupivacaine, various investigators have recently resorted to using lidocaine for prolonged thoracic paravertebral infusion in adults. 8,80 At the same infusion rate (0.1 ml kg 1 h 1 ), lidocaine 1% produces analgesia after thoracotomy, which is superior to placebo 8 and equianalgesic to bupivacaine 0.25% 8 and 0.5%. 80
6 776 MANOJ K. KARMAKAR Lidocaine, with a shorter elimination half-life and lower cardiotoxicity than bupivacaine, 52 may prove to be an attractive alternative. Failure Rate and Complications Thoracic paravertebral block is technically easy to learn, 10,11 has a high success rate 10,11,34 regardless of the number of blocks performed, 11 and does not appear to be operator-dependent. 11 The failure rate varies from 6.8 to 10%, 11,68,72 which is comparable with that of other commonly used regional anesthetic techniques 68 and reflects the technical difficulty in accurately identifying the TPVS. Based on published data, it is difficult to quote the true complication rate of TPVB, but it appears to be relatively low. 10,11,34,68,84 Richardson and Sabanathan estimated it to be 5%, 84 whereas Coveney et al. 11 retrospectively reviewed 156 consecutive cases of TPVB using the multiple-injection technique and noted that complications occurred in only four cases (2.6%). Lönnqvist et al. 68 prospectively evaluated complications after paravertebral (thoracic and lumbar) blocks in 367 patients (319 adults, 48 children) and observed the following frequency of complications: vascular puncture, 3.8%; hypotension, 4.6%; pleural puncture, 1.1%; and pneumothorax, 0.5%. Inadvertent pleural puncture 3,46,68 is uncommon 34,68 and may 11,34,60,68,85 or may not 46,68 result in a pneumothorax, which is usually minor and managed conservatively. 11,60,85 If it does occur, pleural puncture can be converted to interpleural analgesia. 18 Clues that suggest pleural puncture are a definite pleural pop sensation, 68 irritating cough, 46,60 or sharp pain in the chest 11,60 or shoulder 11 during the procedure. Air is not aspirated 46 unless the lung is inadvertently punctured or air that may have entered the pleural cavity via the needle during removal of the stylet is aspirated. Such patients need to be closely monitored for the possible development of pneumothorax. Radiologically, interpleural injection (contrast) is seen to move with respiration, 46 does not define any specific anatomical plane, 45 rapidly disperses, 45 and spreads to the diaphragmatic angle or horizontal fissure. 46 A unique case of clicking pneumothorax is also described. 85 This clinical entity is seen most commonly with small left apical pneumothoraces and is characterized by the Hamman sign, a clicking, bubbling, or crunching noise heard on auscultation near the apex of the heart in certain postures. 85 Pulmonary hemorrhage has been reported after percutaneous TPVB in a patient who had undergone previous thoracic surgery, 74 which highlights the need for caution in patients with altered paravertebral anatomy. Hypotension is uncommon 1,34,68 after TPVB in normovolemic patients because of unilateral sympathetic blockade, 1,66 but TPVB may unmask hypovolemia and result in hypotension. Interestingly, hypotension does not appear to be a problem even after bilateral TPVB. 13,68 Some patients develop hypotension as part of a vaso-vagal episode. 86 Transient seizure after inadvertent intravascular 71 and rapid supplementary 68 injection of plain bupivacaine highlights the need to use epinephrine-containing solutions, although this may rarely produce clinical signs of systemic epinephrine absorption. 11 Dural puncture related complications such as intrathecal injection, 34,61 spinal anesthesia, 60 and postural headache 60 appear to be exclusive to the medial approach to the TPVS 34,60,61 and are probably related to the closer proximity of the needle to the dural cuff and intervertebral foramen. Transient ipsilateral 22,34,46,72 or bilateral 46 Horner syndrome can also develop. The former is likely to be caused by spread of local anesthetic to the ipsilateral stellate ganglion or the preganglionic fibers originating from the first few segments of the thoracic spinal cord, whereas the latter may be caused by contralateral paravertebral spread via the prevertebral 34,37,57 or epidural 31,65 route. Ipsilateral sensory changes in the arm 11,34 may also develop as a result of spread of local anesthetic to the T1 component of the brachial plexus in the thorax or the C8 component where it originates between C7 and T1, although further spread to the brachial plexus in the neck cannot be excluded. Bilateral symmetrical anesthesia 69 and ipsilateral thoracolumbar anesthesia 1,48,50 can also occur as described above. Segmental thoracic pain that lasted for 3 months after the block may be a result of intercostal nerve trauma during catheter insertion. 69 Neurologic complications that have resulted in significant morbidity are myelopathy after paravertebral injection of efocaine (three cases) 87 and Brown Sequard paralysis after paravertebral alcohol injection (one case). 88 No fatality directly related to TPVB has been reported to date. Application of Thoracic Paravertebral Block Pain Relief after Thoracic Surgery Continuous thoracic paravertebral infusion of local anesthetic via a catheter placed under direct vision at thoracotomy is a safe, simple, and effective method of providing analgesia after thoracotomy. 4,6 8,19,20,22,62,64,82,89 91,92 In children it has been used very effectively as the sole analgesic technique, 19,20,22,23 but in adults it is usually used in conjunction with adjunct medication (opioid or nonsteroidal antiinflammatory drugs) to provide optimal pain relief after thoracotomy. 4,6,8,64,89 Although supplementary analgesics are required, opioid requirements are significantly reduced. 6,8,90 A continuous thoracic paravertebral infusion of local anesthetic in conjunction with adjunct medications provides very effective pain relief with few side effects. 7,8,64,82 Pain relief is superior to placebo 8,90 and intravenous patient-controlled mor-
7 THORACIC PARAVERTEBRAL BLOCK 777 phine, 6 and is comparable to interpleural analgesia, 4,89 lumbar epidural morphine, 82 and thoracic epidural administration of bupivacaine 5 or a bupivacaine fentanyl mixture. 91,92 Thoracic paravertebral analgesia preserves respiratory function better 4,89 and produces fewer side effects 4 than interpleural analgesia. Hypotension 5 and urinary retention 5,91 are also less frequent than with thoracic epidural analgesia. Continuous thoracic paravertebral infusion of local anesthetic provides better pain control after thoracotomy than an intermittent bolus regimen. 93 It reduces the postoperative decline in respiratory function, 8,90 augments the recovery of respiratory mechanics, 90 and reduces the generation of chronic postthoracotomy neuralgia. 94 A balanced analgesic regimen, which includes preoperative pain prophylaxis (opioid and nonsteroidal antiinflammatory drug premedication with preincisional TPVB) in conjunction with postoperative thoracic paravertebral infusion of bupivacaine, regular nonsteroidal antiinflammatory drug, and on-demand opioid, is very effective in patients undergoing thoracotomy. 7,64 It prevents the postoperative increase in plasma cortisol, 7 preserves preoperative respiratory function, 7 and is superior to a balanced analgesic regimen with thoracic epidural bupivacaine. 64 Pain Relief after Multiple Fractured Ribs Thoracic paravertebral block provides effective pain relief in patients with unilateral multiple fractured ribs 2,3,37,66,95 and has been used as repeated percutaneous injections, 2 regular top ups via an indwelling catheter, 3,95 or as a continuous infusion. 66 A single thoracic paravertebral injection of 25 ml (SD, 5) of bupivacaine 0.5% produces pain relief for a mean duration of 9.9 h (SD, 1.2). 2 It has also been shown to improve respiratory parameters and arterial blood gas tensions. 2 Used in a patient with associated head injury, TPVB circumvents the need for sedation and ventilation and allows continuous central neurologic assessment. 73,95 McKnight and Marshall 66 described ipsilateral flat nipple (monoplatythela) as an objective sign of a functioning TPVB in one such patient. In patients with associated lumbar spinal injury, the segmental thoracic nerve blockade spares the lumbar and sacral nerve roots, allowing regular peripheral neurologic assessment for signs of spinal cord compression. 73 There is a lack of comparative data, and TPVB has been overshadowed by epidural, interpleural, and intercostal nerve block for managing pain in patients with blunt chest trauma. Although no direct comparison can be made, TPVB offers technical and clinical advantages in patients with unilateral multiple fractured ribs and deserves more attention and investigation in the future. Anesthesia for Breast Surgery Thoracic paravertebral injection of local anesthetic at multiple levels (C7 T6) 11,14,26 or as a single injection at T4 72 in conjunction with intraoperative sedation is safe and effective for surgical anesthesia in a majority of patients undergoing major breast surgery 11,14,16,25,26,72 and is associated with minimal complications 11,26 and a high degree of patient satisfaction. 14 Weltz et al. 14 reported that the block (4 ml, 0.5% bupivacaine with 1:400,000 epinephrine injected at each level, C7 T7) provides postoperative analgesia for an average of 23 h (range, 9 38 h). TPVB has significantly improved the quality of recovery after major breast surgery. 11,16,72 Compared with patients who undergo only general anesthesia, patients who receive TPVB have a shorter recovery time, 72 experience less postoperative pain, 16,72 require fewer analgesics, 11,72 and also have less painful restricted movement of the shoulder. 72 They also experience less postoperative nausea and vomiting, 11,72 tend to mobilize earlier, 72 and are discharged significantly earlier from hospital. 11 The use of TPVB in patients undergoing ambulatory breast cancer surgery has costsaving potential. 14 Anesthesia for Inguinal Herniorrhaphy Paravertebral injection of local anesthetic at multiple thoracic and lumbar segments, 24,96 or as a single injection at T11 behind the endothoracic fascia, 50,51 produces ipsilateral thoracolumbar anesthesia effective for inguinal herniorrhaphy. Klein et al. 96 used multiple paravertebral injections at T10 L2 using 5 ml of bupivacaine 0.5% with epinephrine (2.5 g/ml) at each level and produced surgical anesthesia with few side effects, which in conjunction with intraoperative sedation was adequate for inguinal herniorrhaphy. The block also provided long-lasting postoperative analgesia, and the time to first opioid requirement was h. 96 Wassef et al. 24 reported that paravertebral block of the ipsilateral T12 L2 nerve roots is more successful than field block for surgical anesthesia during inguinal herniorrhaphy. In addition, the paravertebral block not only required fewer needle insertions and total amount of local anesthetic than the field block, but was also devoid of side effects and was acceptable to the patients. 24 Saito et al. 51 described extended unilateral anesthesia for inguinal herniorrhaphy. In this variation of the paravertebral technique, the needle is inserted more laterally (5 cm from the midline), and loss of resistance is used to locate the space beneath the endothoracic fascia. 51 A single injection of 12 ml 2% mepivacaine posterior to the endothoracic fascia at T11 results in extended thoracolumbar anesthesia over an average of seven dermatomes, which was effective for herniorrhaphy in 60% of patients studied. 51 The efficacy of paravertebral block makes it a potential choice for outpatient inguinal herniorrhaphy and warrants further investigation.
8 778 MANOJ K. KARMAKAR Table 3. Drug and Dosage for Thoracic Paravertebral Block Age Group Drug Concentration (%) Bolus Dose Infusion Rate (ml kg 1 h 1 ) Adults Bupivacaine ml or 0.3 ml/kg 0.1 Lidocaine ml 0.1 Children Bupivacaine epinephrine 0.5 ml/kg 0.2 Lidocaine 1 epinephrine 0.5 ml/kg 0.25 Pain Relief after Cholecystectomy and Renal Surgery Data on the use of TPVB in patients undergoing cholecystectomy and renal surgery via a subcostal incision are limited, and the results are inconclusive. Giesecke et al. 97 reported that a single preincisional thoracic paravertebral injection of bupivacaine 0.5%, 20 ml before cholecystectomy, attenuates the stress response to surgical stimuli during isoflurane anesthesia and provides complete pain relief for 1 6 h. In contrast, Bigler et al. 69 reported that TPVB with 0.5% bupivacaine, a 15-ml bolus dose followed by an infusion of 5 ml/h postoperatively, is inadequate as the only analgesic after cholecystectomy, whereas a thoracic epidural infusion of bupivacaine 0.5% (5 ml/h) and morphine (0.2 mg/h) produced total pain relief. Pain scores were higher in the paravertebral group, as was the use of systemic morphine. 69 The author is unaware of any published data evaluating the analgesic efficacy of TPVB in adults undergoing renal surgery. In children, Lönnqvist and Olsson 17 retrospectively compared the analgesic efficacy of a continuous thoracic paravertebral infusion with that of lumbar epidural infusion of bupivacaine. They reported that the requirement for supplementary morphine was lower and the number of children with no need for supplementary morphine was higher in patients treated with a TPVB. 17 Chronic Pain Management Thoracic paravertebral block has been used to manage benign 1,3,9,10,48,56 and malignant 3,55,59 neuralgia involving the thoracic dermatomes, and long-term results have been more favorable in the former group of patients. Kirvelä and Antila 10 used a single thoracic paravertebral injection of bupivacaine 0.5%, ml, to relieve chronic postoperative (postthoracotomy and postmastectomy) pain. 10 Initial results were good in 99% of blocks, but the long-term pain relief in the postthoracotomy group was better than in the postmastectomy group. 10 In the postthoracotomy group, pain relief lasted a month after 58%, at least 2 months after 30%, more than 4 months after 8%, and more than 5 months after 3% of blocks, as opposed to less than a month in 88% of blocks performed for chronic postmastectomy pain. 10 Ferrandiz et al. 9 also managed postthoracotomy pain syndrome using TPVB and achieved complete pain relief in 50% of patients who were pain free for a variable time after thoracotomy, which the investigators called free time, as opposed to 33% of patients who had long-term postthoracotomy pain with no free time. Neurolytic TPVB, because of the high risk of neurologic damage, is limited to the management of intractable thoracic pain in cancer patients with poor prognosis, but preliminary results using 1 4 ml of 7% phenol per spinal segment has demonstrated limited long-term benefits. 55 Miscellaneous Applications Thoracic paravertebral block has been used in several other situations, including pain management after appendectomy, 68,71 video-assisted thoracoscopic surgery, 15,98 and minimally invasive cardiac surgery. 99 It has also been used to manage acute postherpetic neuralgia, 85,100 control liver capsule pain after blunt abdominal trauma, 101 control hyperhydrosis, 28 manage reflex sympathetic dystrophy of the chest, 34 relieve angina pectoris, 88 and explore a chest wound in a single lung transplant recipient. 102 Conclusions Thoracic paravertebral block is a technically simple, easy-to-learn technique with few contraindications and is associated with a low overall incidence of complications. TPVB produces unilateral somatic and sympathetic nerve blockade, which suppresses the neuroendocrine stress response to surgery and is adequate for surgical anesthesia in patients undergoing major breast surgery and inguinal herniorrhaphy. It has significantly improved the quality of recovery after major breast surgery. Continuous TPVB as part of a balanced analgesic regimen provides effective pain relief with very few side effects after thoracotomy, which is comparable to thoracic epidural analgesia the gold standard and should be considered a safe alternative. The same efficacy has not been demonstrated after cholecystectomy or renal surgery, but one may expect a significant opioid-sparing effect. A single thoracic paravertebral injection is also effective for pain control in patients with multiple fractured ribs and benign thoracic neuralgia. The role of bilateral thoracic paravertebral block is still to be defined. Based on published data, one can recommend that this simple yet highly versatile regional anesthetic analgesic technique should be in the repertoire of every anesthesiologist and more widely applied.
9 THORACIC PARAVERTEBRAL BLOCK 779 References 1. Cheema SP, Ilsley D, Richardson J, Sabanathan S: A thermographic study of paravertebral analgesia. Anaesthesia 1995; 50: Gilbert J, Hultman J: Thoracic paravertebral block: A method of pain control. Acta Anaesthesiol Scand 1989; 33: Eason MJ, Wyatt R: Paravertebral thoracic block-a reappraisal. Anaesthesia 1979; 34: Richardson J, Sabanathan S, Mearns AJ, Shah RD, Goulden C: A prospective, randomized comparison of interpleural and paravertebral analgesia in thoracic surgery. Br J Anaesth 1995; 75: Matthews PJ, Govenden V: Comparison of continuous paravertebral and extradural infusions of bupivacaine for pain relief after thoracotomy. Br J Anaesth 1989; 62: Carabine UA, Gilliland H, Johnston JR, McGuigan J: Pain relief for thoracotomy: Comparison of morphine requirements using an extrapleural infusion of bupivacaine. Reg Anesth 1995; 20: Richardson J, Sabanathan S, Mearns AJ, Evans CS, Bembridge J, Fairbrass M: Efficacy of pre-emptive analgesia and continuous extrapleural intercostal nerve block on post-thoracotomy pain and pulmonary mechanics. J Cardiovasc Surg (Torino) 1994; 35: Barron DJ, Tolan MJ, Lea RE: A randomized controlled trial of continuous extra-pleural analgesia post-thoracotomy: Efficacy and choice of local anaesthetic. Eur J Anaesthesiol 1999; 16: Ferrandiz M, Aliaga L, Catala E, Villar-Landeira JM: Thoracic paravertebral block in chronic postoperative pain (letter). Reg Anesth 1994; 19: Kirvela O, Antila H: Thoracic paravertebral block in chronic postoperative pain. Reg Anesth 1992; 17: Coveney E, Weltz CR, Greengrass R, Iglehart JD, Leight GS, Steele SM, Lyerly HK: Use of paravertebral block anesthesia in the surgical management of breast cancer: Experience in 156 cases. Ann Surg 1998; 227: Karmakar MK, Booker PD, Franks R: Bilateral continuous paravertebral block used for postoperative analgesia in an infant having bilateral thoracotomy. Paediatr Anaesth 1997; 7: Richardson J, Vowden P, Sabanathan S: Bilateral paravertebral analgesia for major abdominal vascular surgery: A preliminary report. Anaesthesia 1995; 50: Weltz CR, Greengrass RA, Lyerly HK: Ambulatory surgical management of breast carcinoma using paravertebral block. Ann Surg 1995; 222: Soni AK, Conacher ID, Waller DA, Hilton CJ: Video-assisted thoracoscopic placement of paravertebral catheters: A technique for postoperative analgesia for bilateral thoracoscopic surgery. Br J Anaesth 1994; 72: Klein SM, Bergh A, Steele SM, Georgiade GS, Greengrass RA: Thoracic paravertebral block for breast surgery. Anesth Analg 2000; 90: Lönnqvist PA, Olsson GL: Paravertebral vs epidural block in children: Effects on postoperative morphine requirement after renal surgery. Acta Anaesthesiol Scand 1994; 38: Lönnqvist PA: Continuous paravertebral block in children. Initial experience. Anaesthesia 1992; 47: Eng J, Sabanathan S: Continuous paravertebral block for postthoracotomy analgesia in children. J Pediatr Surg 1992; 27: Cheung SL, Booker PD, Franks R, Pozzi M: Serum concentrations of bupivacaine during prolonged continuous paravertebral infusion in young infants. Br J Anaesth 1997; 79: Downs CS, Cooper MG: Continuous extrapleural intercostal nerve block for post thoracotomy analgesia in children. Anaesth Intensive Care 1997; 25: Karmakar MK, Booker PD, Franks R, Pozzi M: Continuous extrapleural paravertebral infusion of bupivacaine for post-thoracotomy analgesia in young infants. Br J Anaesth 1996; 76: Johnson CM: Continuous paravertebral block in children (letter). Anaesthesia 1993; 48: Wassef MR, Randazzo T, Ward W: The paravertebral nerve root block for inguinal herniorrhaphy: A comparison with the field block approach. Reg Anesth Pain Med 1998; 23: D Ercole FJ, Scott D, Bell E, Klein SM, Greengrass RA: Paravertebral blockade for modified radical mastectomy in a pregnant patient. Anesth Analg 1999; 88: Greengrass R, O Brien F, Lyerly K, Hardman D, Gleason D, D Ercole F, Steele S: Paravertebral block for breast cancer surgery. Can J Anaesth 1996; 43: Richardson J: Fin-de-siecle renaissance of paravertebral analgesia. Pain Rev 1997; 4: Richardson J, Lönnqvist PA: Thoracic paravertebral block. Br J Anaesth 1998; 81: Atkinson RS, Rushman GB, Lee JA: A Synopsis of Anaesthesia. Bristol, IOP Publishing Limited, 1987, pp Lönnquist PA, Richardson J: Use of paravertebral blockade in children. Tech Reg Anesth Pain Manag 1999; 3: MacIntosh R, Bryce-Smith R: Local Analgesia and Abdominal Surgery. Edinburgh, E&S Livingstone, 1962, pp Kittredge RD: Computed tomographic evaluation of the thoracic prevertebral and paravertebral spaces. J Comput Tomogr 1983; 7: Im JG, Webb WR, Rosen A, Gamsu G: Costal pleura: Appearances at high-resolution CT. Radiology 1989; 171: Tenicela R, Pollan SB: Paravertebral-peridural block technique: A unilateral thoracic block. Clin J Pain 1990; 6: Dugan DJ, Samson PC: Surgical significance of the endothoracic fascia: The anatomic basis for empyemectomy and other extrapleural technics. Am J Surg 1975; 130: Moore DC, Bush WH, Scurlock JE: Intercostal nerve block: A roentgenographic anatomic study of technique and absorption in humans. Anesth Analg 1980; 59: Karmakar MK, Kwok WH, Kew J: Thoracic paravertebral block: Radiological evidence of contralateral spread anterior to the vertebral bodies. Br J Anaesth 2000; 84: Karmakar MK, Chung DC: Variability of a thoracic paravertebral block: Are we ignoring the endothoracic fascia? (letter). Reg Anesth Pain Med 2000; 25: Nunn JF, Slavin G: Posterior intercostal nerve block for pain relief after cholecystectomy: Anatomical basis and efficacy. Br J Anaesth 1980; 52: Moore DC: Intercostal nerve block: Spread of india ink injected to the rib s costal groove. Br J Anaesth 1981; 53: Pernkopf E: Thorax, abdomen and extremities, Atlas of Topographical and Applied Human Anatomy. Edited by Ferner H. Baltimore, Urban and Schwarzenberg, 1980, pp Conacher ID: Resin injection of thoracic paravertebral spaces. Br J Anaesth 1988; 61: Mowbray A, Wong KK, Murray JM: Intercostal catheterisation: An alternative approach to the paravertebral space. Anaesthesia 1987; 42: Murphy DF: Continuous intercostal nerve blockade: An anatomical study to elucidate its mode of action. Br J Anaesth 1984; 56: Conacher ID, Kokri M: Postoperative paravertebral blocks for thoracic surgery: A radiological appraisal. Br J Anaesth 1987; 59: Purcell-Jones G, Pither CE, Justins DM: Paravertebral somatic nerve block: A clinical, radiographic, and computed tomographic study in chronic pain patients. Anesth Analg 1989; 68: Lönnqvist PA, Hildingsson U: The caudal boundary of the thoracic paravertebral space: A study in human cadavers. Anaesthesia 1992; 47: Richardson J, Jones J, Atkinson R: The effect of thoracic paravertebral blockade on intercostal somatosensory evoked potentials. Anesth Analg 1998; 87: Saito T, Den S, Tanuma K, Tanuma Y, Carney E, Carlsson C: Anatomical bases for paravertebral anesthetic block: Fluid communication between the thoracic and lumbar paravertebral regions. Surg Radiol Anat 1999; 21: Saito T, Gallagher ET, Yamada K, Tanuma K, Ogawa R: Broad unilateral analgesia (letter). Reg Anesth 1994; 19: Saito T, Gallagher ET, Cutler S, Tanuma K, Yamada K, Saito N, Maruyama K, Carlsson C: Extended unilateral anesthesia: New technique or paravertebral anesthesia? Reg Anesth 1996; 21: Lönnqvist PA: Plasma concentrations of lignocaine after thoracic paravertebral blockade in infants and children. Anaesthesia 1993; 48: Lönnquist PA, Hesser U: Depth from the skin to the thoracic paravertebral space in infants and children. Paediatr Anaesth 1994; 4: Katz J: Thoracic paravertebral nerve, Atlas of Regional Anesthesia. Edited by Katz J. Norwalk, Appleton & Lange, 1994, pp Antila H, Kirvela O: Neurolytic thoracic paravertebral block in cancer pain: A clinical report. Acta Anaesthesiol Scand 1998; 42: Richardson J, Cheema SP, Hawkins J, Sabanathan S: Thoracic paravertebral space location: A new method using pressure measurement. Anaesthesia 1996; 51: Lönnquist PA, Hesser U: Radiological and clinical distribution of thoracic paravertebral blockade in infants and children. Paediatr Anaesth 1993; 3: Kawamata M, Omote K, Namiki A, Miyabe M: Measurement of intercostal and pleural pressures by epidural catheter. Anaesthesia 1994; 49: Shaw WM, Hollis NY: Medial approach for paravertebral somatic nerve block. JAMA 1952; 148: Sharrock NE: Postural headache following thoracic somatic paravertebral nerve block. ANESTHESIOLOGY 1980; 52: Evans PJ, Lloyd JW, Wood GJ: Accidental intrathecal injection of bupivacaine and dextran. Anaesthesia 1981; 36: Sabanathan S, Smith PJ, Pradhan GN, Hashimi H, Eng JB, Mearns AJ: Continuous intercostal nerve block for pain relief after thoracotomy. Ann Thorac Surg 1988; 46: Berrisford RG, Sabanathan SS: Direct access to the paravertebral space at thoracotomy (letter). Ann Thorac Surg 1990; 49: Richardson J, Sabanathan S, Jones J, Shah RD, Cheema S, Mearns AJ: A prospective, randomized comparison of preoperative and continuous balanced epidural or paravertebral bupivacaine on post-thoracotomy pain, pulmonary function and stress responses. Br J Anaesth 1999; 83: MacIntosh RR, Mushin WW: Observations on the epidural space. Anaesthesia 1947; 2: McKnight CK, Marshall M: Monoplatythela and paravertebral block (letter). Anaesthesia 1984; 39: Eng J, Sabanathan S: Site of action of continuous extrapleural intercostal nerve block. Ann Thorac Surg 1991; 51:387 9
Continuing Education in Anaesthesia, Critical Care & Pain Advance Access published August 17, 2010
 Continuing Education in Anaesthesia, Critical Care & Pain Advance Access published August 17, 2010 Paravertebral block SQM Tighe MBBS, FRCA Michelle D Greene BMedSci, MBBS, FRCA Nirmal Rajadurai MBBS,
Continuing Education in Anaesthesia, Critical Care & Pain Advance Access published August 17, 2010 Paravertebral block SQM Tighe MBBS, FRCA Michelle D Greene BMedSci, MBBS, FRCA Nirmal Rajadurai MBBS,
Perioperative Pain Management
 Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
THORACIC paravertebral blockade (TPVB) is a
 Magnetic Resonance Imaging Analysis of the Spread of Local Anesthetic Solution after Ultrasound-guided Lateral Thoracic Paravertebral Blockade A Volunteer Study Daniela Marhofer, M.D.,* Peter Marhofer,
Magnetic Resonance Imaging Analysis of the Spread of Local Anesthetic Solution after Ultrasound-guided Lateral Thoracic Paravertebral Blockade A Volunteer Study Daniela Marhofer, M.D.,* Peter Marhofer,
Multiple fractured ribs (MFR) cause severe pain
 Continuous Thoracic Paravertebral Infusion of Bupivacaine for Pain Management in Patients With Multiple Fractured Ribs* Manoj K. Karmakar, MD; Lester A.H. Critchley, MD; Anthony M.-H. Ho, MD, FCCP; Tony
Continuous Thoracic Paravertebral Infusion of Bupivacaine for Pain Management in Patients With Multiple Fractured Ribs* Manoj K. Karmakar, MD; Lester A.H. Critchley, MD; Anthony M.-H. Ho, MD, FCCP; Tony
Paraspinal Blocks a new paradigm in truncal analgesia
 Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
nerve blocks in the diagnosis and therapy of visceral disease
 Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Newcastle upon Tyne Hospitals NHS Foundation Trust. RVI Paravertebral Continuous Infusion Guideline
 The Newcastle upon Tyne Hospitals NHS Foundation Trust RVI Paravertebral Continuous Infusion Guideline Version No.: 1 Effective From: 11 August 2016 Review date: 11 August 2019 Date Ratified 25 July 2016
The Newcastle upon Tyne Hospitals NHS Foundation Trust RVI Paravertebral Continuous Infusion Guideline Version No.: 1 Effective From: 11 August 2016 Review date: 11 August 2019 Date Ratified 25 July 2016
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Epidural anaesthesia and analgesia
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
PLEURAE and PLEURAL RECESSES
 PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
Ultrasound-guided thoracic paravertebral puncture and placement of catheters in human cadavers: where do catheters go?
 British Journal of Anaesthesia 106 (2): 246 54 (2011) Advance Access publication 25 November 2010. doi:10.1093/bja/aeq309 REGIONAL ANAESTHESIA Ultrasound-guided thoracic paravertebral puncture and placement
British Journal of Anaesthesia 106 (2): 246 54 (2011) Advance Access publication 25 November 2010. doi:10.1093/bja/aeq309 REGIONAL ANAESTHESIA Ultrasound-guided thoracic paravertebral puncture and placement
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Single Dose Preemptive Thoracic Paravertebral Block For Postoperative Pain Relief After Cholecystectomy
 10 Single Dose Preemptive Thoracic Paravertebral Block For Postoperative Pain Relief After Cholecystectomy Tarek Atef Tawfic *, MD; Mohamed Medhat Khalil *, MD *Lecturer of anaesthesia, faculty of medicine,
10 Single Dose Preemptive Thoracic Paravertebral Block For Postoperative Pain Relief After Cholecystectomy Tarek Atef Tawfic *, MD; Mohamed Medhat Khalil *, MD *Lecturer of anaesthesia, faculty of medicine,
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Intercostal Muscles LO4
 Intercostal Muscles LO4 4 List the structures, from superficial to deep, in an intercostal space. Describe their relationships to each other, to the associated neurovascular bundle and to the pleural cavity.
Intercostal Muscles LO4 4 List the structures, from superficial to deep, in an intercostal space. Describe their relationships to each other, to the associated neurovascular bundle and to the pleural cavity.
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA
 FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA TECHNIQUES Abdominal Wall TAP Rectus Sheath Quadratus Lumborum Erector Spinae Chest PECS I & II Erector Spinae TECHNIQUES Knee Ipack/LIA Hip Fascia Iliaca
FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA TECHNIQUES Abdominal Wall TAP Rectus Sheath Quadratus Lumborum Erector Spinae Chest PECS I & II Erector Spinae TECHNIQUES Knee Ipack/LIA Hip Fascia Iliaca
Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives
 1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES
 SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
Paravertebral Blocks in Breast Cancer Surgery: Is There adifferenceinpostoperativepain,nausea,andvomiting?
 Ann Surg Oncol (2012) 19:548 552 DOI 10.1245/s10434-011-1899-5 ORIGINAL ARTICLE BREAST ONCOLOGY Paravertebral Blocks in Breast Cancer Surgery: Is There adifferenceinpostoperativepain,nausea,andvomiting?
Ann Surg Oncol (2012) 19:548 552 DOI 10.1245/s10434-011-1899-5 ORIGINAL ARTICLE BREAST ONCOLOGY Paravertebral Blocks in Breast Cancer Surgery: Is There adifferenceinpostoperativepain,nausea,andvomiting?
Paravertebral policy. The Acute pain Management Dept, UCLH
 UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
How and why to do an epidural in dogs and cats? Which Indications and which drugs?
 AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
Ultrasound Guided Thoracic Paravertebral Block versus Blind Landmark Technique for Breast Surgery. Does it Really Different?
 Med. J. Cairo Univ., Vol. 84, No. 3, December: 235-24, 216 www.medicaljournalofcairouniversity.net Ultrasound Guided Thoracic Paravertebral Block versus Blind Landmark Technique for Breast Surgery. Does
Med. J. Cairo Univ., Vol. 84, No. 3, December: 235-24, 216 www.medicaljournalofcairouniversity.net Ultrasound Guided Thoracic Paravertebral Block versus Blind Landmark Technique for Breast Surgery. Does
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Influence of Intrapleural Infusion of Marcaine on Post Thoracotomy Pain
 ORIGINAL ARTICLE Tanaffos (2007) 6(1), 47-51 2007 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Influence of Intrapleural Infusion of Marcaine on Post Thoracotomy Pain Hamid
ORIGINAL ARTICLE Tanaffos (2007) 6(1), 47-51 2007 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Influence of Intrapleural Infusion of Marcaine on Post Thoracotomy Pain Hamid
Australian Safety and Efficacy Register of New Interventional Procedures-Surgical ASERNIP-S REPORT NO. 47. January 2006
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures-Surgical Paravertebral Blocks for Anaesthesia and Analgesia: A Systematic Review ASERNIP-S REPORT NO. 47 January 2006
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures-Surgical Paravertebral Blocks for Anaesthesia and Analgesia: A Systematic Review ASERNIP-S REPORT NO. 47 January 2006
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
Dr. K.Raja Sekhar, Dr. B. Venu Gopalan, Asst. Professor.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 52-57 www.iosrjournals.org A Comparative Study of Bupivacaine with
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 52-57 www.iosrjournals.org A Comparative Study of Bupivacaine with
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion
 Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Epidural Analgesia in Labor - Whats s New
 Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
Thoracic paravertebral block
 British Journal of Anaesthesia 1998; 81: 230 238 REVIEW ARTICLE Thoracic paravertebral block J. RICHARDSON AND P. A. LÖNNQVIST Paravertebral nerve block produces ipsilateral analgesia through injection
British Journal of Anaesthesia 1998; 81: 230 238 REVIEW ARTICLE Thoracic paravertebral block J. RICHARDSON AND P. A. LÖNNQVIST Paravertebral nerve block produces ipsilateral analgesia through injection
cardiac plexus is continuous with the coronary and no named branches pain from the heart and lungs
 Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
The goal of this article is to describe the. Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation.
 Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
Regional Anesthesia. Fatiş Altındaş Dept. of Anesthesiology
 Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
ANATOMY OF THE PLEURA. Dr Oluwadiya KS
 ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
thoracic cage inlet and outlet landmarks of the anterior chest wall muscles of the thoracic wall sternum joints ribs intercostal spaces diaphragm
 Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Tarek M Sarhan, Assistant professor of Anesthesiology, Faculty of Medicine, Alexandria University
 7 ANALGESIA FOR TRACHEOESOPHAGEAL FISTULA REPAIR IN NEONATES : A COMPARISON OF SINGLE SHOT THORACIC PARAVERTEBRAL BLOCK AND EPIDURAL BLOCK WITH ROPIVACAINE Tarek M Sarhan, Assistant professor of Anesthesiology,
7 ANALGESIA FOR TRACHEOESOPHAGEAL FISTULA REPAIR IN NEONATES : A COMPARISON OF SINGLE SHOT THORACIC PARAVERTEBRAL BLOCK AND EPIDURAL BLOCK WITH ROPIVACAINE Tarek M Sarhan, Assistant professor of Anesthesiology,
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Benefits of peripheral nerve blocks in breast surgery
 10 August 2018 No. 13 Benefits of peripheral nerve blocks in breast surgery Salem Bobaker Moderator: S Jithoo School of Clinical Medicine Discipline of Anaesthesiology and Critical Care Content INTRODUCTION...
10 August 2018 No. 13 Benefits of peripheral nerve blocks in breast surgery Salem Bobaker Moderator: S Jithoo School of Clinical Medicine Discipline of Anaesthesiology and Critical Care Content INTRODUCTION...
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics
 Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
NERVOUS SYSTEM ANATOMY
 INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th & 12 th Eds.)
 PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
PARA VERTEBRAL BLOCK DURING CHOLECYSTECTOMY EFFECTS ON CIRCULATORY AND HORMONAL RESPONSES
 Br. J. Anaesth. (988), 6, 652-656 PARA VERTEBRAL BLOCK DURING CHOLECYSTECTOMY EFFECTS ON CIRCULATORY AND HORMONAL RESPONSES K. GIESECKE, B. HAMBERGER, P.-O. JARNBERG AND C. KLINGSTEDT Paravertebral block
Br. J. Anaesth. (988), 6, 652-656 PARA VERTEBRAL BLOCK DURING CHOLECYSTECTOMY EFFECTS ON CIRCULATORY AND HORMONAL RESPONSES K. GIESECKE, B. HAMBERGER, P.-O. JARNBERG AND C. KLINGSTEDT Paravertebral block
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Types of blocks. Clinical considerations 8/11/2009. Let s Discuss Sympathetic Blocks. Stellate Celiac plexis Lumbar sympathetic Hypogastric
 Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
Abdomen: Introduction. Prof. Oluwadiya KS
 Abdomen: Introduction Prof. Oluwadiya KS www.oluwadiya.com Abdominopelvic Cavity Abdominal Cavity Pelvic Cavity Extends from the inferior margin of the thorax to the superior margin of the pelvis and the
Abdomen: Introduction Prof. Oluwadiya KS www.oluwadiya.com Abdominopelvic Cavity Abdominal Cavity Pelvic Cavity Extends from the inferior margin of the thorax to the superior margin of the pelvis and the
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
GI module Lecture: 9 د. عصام طارق. Objectives:
 GI module Lecture: 9 د. عصام طارق Objectives: To list structures forming posterior abdominal wall. To follow aorta & its main branches. To describe IVC & its main tributaries. To list nerves of posterior
GI module Lecture: 9 د. عصام طارق Objectives: To list structures forming posterior abdominal wall. To follow aorta & its main branches. To describe IVC & its main tributaries. To list nerves of posterior
Paravertebral block versus unilateral spinal anesthesia for inguinal hernia repair - A comparative clinical trial
 ORIGINAL ARTICLE e-issn: 2349-0659 p-issn: 2350-0964 doi: 10.21276/apjhs.2017.4.4.40 aravertebral block versus unilateral spinal anesthesia for inguinal hernia repair - A comparative clinical trial Eeshwar
ORIGINAL ARTICLE e-issn: 2349-0659 p-issn: 2350-0964 doi: 10.21276/apjhs.2017.4.4.40 aravertebral block versus unilateral spinal anesthesia for inguinal hernia repair - A comparative clinical trial Eeshwar
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
NERVOUS SYSTEM ANATOMY
 NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. Comparative Assessment of Sequential organ failure Assessment (SOFA) score and Multiple Organ Dysfunction Score (Mode) in Outcome Prediction among ICU Patients. 2. Comparison of Backpain after
S.No. 1. Comparative Assessment of Sequential organ failure Assessment (SOFA) score and Multiple Organ Dysfunction Score (Mode) in Outcome Prediction among ICU Patients. 2. Comparison of Backpain after
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Regional Anaesthesia of the Thoracic Limb
 Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain.
 Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Regional Anesthesia. procedure if required. However, many patients prefer to receive sedation either during the
 1 Regional Anesthesia Regional anaesthesia (or regional anesthesia) is anesthesia affecting only a large part of the body, such as a limb or the lower half of the body. Regional anaesthetic techniques
1 Regional Anesthesia Regional anaesthesia (or regional anesthesia) is anesthesia affecting only a large part of the body, such as a limb or the lower half of the body. Regional anaesthetic techniques
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
NEW KIDS ON THE BLOCK: THE NEW ERA OF REGIONAL ANESTHESIA PLANE BLOCKS
 2017 CSA Fall Anesthesia Conference NEW KIDS ON THE BLOCK: THE NEW ERA OF REGIONAL ANESTHESIA PLANE BLOCKS Michael Barrington, MB BS, FANZCA, PhD Senior Staff Anaesthetist, St Vincent s Hospital, Melbourne.
2017 CSA Fall Anesthesia Conference NEW KIDS ON THE BLOCK: THE NEW ERA OF REGIONAL ANESTHESIA PLANE BLOCKS Michael Barrington, MB BS, FANZCA, PhD Senior Staff Anaesthetist, St Vincent s Hospital, Melbourne.
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Bilateral thoracic paravertebral block: potential and practice
 British Journal of Anaesthesia 106 (2): 164 71 (2011) doi:10.1093/bja/aeq378 REVIEW ARTICLE Bilateral thoracic paravertebral block: potential and practice J. Richardson 1 *,P.A.Lönnqvist 2 and Z. Naja
British Journal of Anaesthesia 106 (2): 164 71 (2011) doi:10.1093/bja/aeq378 REVIEW ARTICLE Bilateral thoracic paravertebral block: potential and practice J. Richardson 1 *,P.A.Lönnqvist 2 and Z. Naja
Combined spinalepidural. epidural analgesia in labour (review) By Neda Taghizadeh
 Combined spinalepidural versus epidural analgesia in labour (review) By Neda Taghizadeh Cochrane review Cochrane collaboration was founded in 1993 and is named after Archie Cochrane (1909-1988), British
Combined spinalepidural versus epidural analgesia in labour (review) By Neda Taghizadeh Cochrane review Cochrane collaboration was founded in 1993 and is named after Archie Cochrane (1909-1988), British
Single Needle Thoracic Paravertebral Block with Ropivacaine and Dexmeditomidine for Radical Mastectomy: Experience in 25 Cases
 Research Article imedpub Journals http://www.imedpub.com DOI: 10.21767/2471-982X.100013 Single Needle Thoracic Paravertebral Block with Ropivacaine and Dexmeditomidine for Radical Mastectomy: Experience
Research Article imedpub Journals http://www.imedpub.com DOI: 10.21767/2471-982X.100013 Single Needle Thoracic Paravertebral Block with Ropivacaine and Dexmeditomidine for Radical Mastectomy: Experience
WITH ISOBARIC BUPIVACAINE (5 MG/ML)
 , 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
, 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
British Journal of Anaesthesia 96 (4): (2006) doi: /bja/ael020 Advance Access publication February 13, 2006
 British Journal of Anaesthesia 96 (4): 418 26 (2006) doi:10.1093/bja/ael020 Advance Access publication February 13, 2006 REVIEW ARTICLE A comparison of the analgesic efficacy and side-effects of paravertebral
British Journal of Anaesthesia 96 (4): 418 26 (2006) doi:10.1093/bja/ael020 Advance Access publication February 13, 2006 REVIEW ARTICLE A comparison of the analgesic efficacy and side-effects of paravertebral
Department of Neurology/Division of Anatomical Sciences
 Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
In the Last Three Lectures We Already Discussed the Importance of the Thoracic Cage.
 -This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
-This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
Pain Management Clinic ISIC
 Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
A Frame of Reference for Anatomical Study. Anatomy and Physiology Mr. Knowles Chapter 1 Liberty Senior High School
 A Frame of Reference for Anatomical Study Anatomy and Physiology Mr. Knowles Chapter 1 Liberty Senior High School Anatomical Terms of Direction and Position Created for communicating the direction and
A Frame of Reference for Anatomical Study Anatomy and Physiology Mr. Knowles Chapter 1 Liberty Senior High School Anatomical Terms of Direction and Position Created for communicating the direction and
Regional anaesthesia in paediatric day case surgery. PA Lönnqvist Karolinska Institutet Karolinska University Hospital Stockholm, Sweden
 Regional anaesthesia in paediatric day case surgery PA Lönnqvist Karolinska Institutet Karolinska University Hospital Stockholm, Sweden Ambulatory surgery in children Out-patient surgery in children did
Regional anaesthesia in paediatric day case surgery PA Lönnqvist Karolinska Institutet Karolinska University Hospital Stockholm, Sweden Ambulatory surgery in children Out-patient surgery in children did
Group of students. - Rawan almujabili د. محمد المحتسب - 1 P a g e
 - 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
- 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
