Chronic irritation, itching, and pain
|
|
|
- Camron Martin
- 5 years ago
- Views:
Transcription
1 SECOND OF 2 PARTS ON OFFICE MANAGEMENT OF BENIGN VULVAR CONDITIONS Chronic vulvar irritation, itching, and pain. What is the diagnosis? Five cases of dermatoses, vaginal abnormalities, and pain syndromes that may masquerade as infection Libby Edwards, MD, and Beth E. Goldbaum, MD IN THIS ARTICLE When a woman is reluctant to use local estrogen page 32 A teenager with vulvar pain and sores page 34 A case of inverse psoriasis page 36 Read Part 1: Chronic vulvar symptoms and dermatologic disruptions (May 2014), at obgmanagement.com Chronic irritation, itching, and pain are only rarely due to infection. These symptoms are more likely to be caused by dermatoses, vaginal abnormalities, and pain syndromes that may be difficult to diagnose. Careful evaluation should include a wet mount and culture to eliminate infection as a cause so that the correct diagnosis can be ascertained and treated. In Part 2 of this two-part series, we focus on five cases of vulvar dermatologic disruptions: atrophic vagina irritant and allergic contact dermatitis complex vulvar aphthosis desquamative inflammatory vaginitis inverse psoriasis. Dr. Edwards is Chief of Dermatology at Carolinas Medical Center, Charlotte, North Carolina. Dr. Goldbaum is Clinical Instructor of Obstetrics and Gynecology at Harvard Medical School, Boston, Massachusetts. The authors report no financial relationships relevant to this article. CASE 1 Introital burning and a fear of breast cancer A 56-year-old woman visits your office for management of recent-onset introital burning during sexual activity. She reports that her commercial lubricant causes irritation. Topical and oral antifungal therapies have not been beneficial. She has a strong family history of breast cancer. On examination, she exhibits small, smooth labia minora and experiences pain when a cotton swab is pressed against the vestibule. The vagina is also smooth, with scant secretions. Microscopically, these secretions are almost acellular, with no increase in white blood cells and no clue cells, yeast forms, or lactobacilli. The ph is greater than 6.5, and most epithelial cells are parabasal (FIGURE 1, page 32). You prescribe topical estradiol cream for vaginal use three nights per week, but when the patient returns 1 month later, her condition is unchanged. She explains that she never used the cream after reading the package insert, which reports a risk of breast cancer. Diagnosis: Atrophic vagina (not atrophic vaginitis, as there is no increase in white blood cells). Treatment: Re-estrogenization should relieve her symptoms. Several options for local estrogen replacement are available. Creams include estradiol CONTINUED ON PAGE OBG Management June 2014 Vol. 26 No. 6 obgmanagement.com
2 Benign vulvar conditions CONTINUED FROM PAGE 30 FIGURE 1 Atrophic vagina This wet mount of an atrophic vagina shows many parabasal cells with no lactobacilli and no increase in white blood cells. The risk of vaginal candidiasis is fairly high during the first 2 or 3 weeks of re-estrogenization (Estrace) and conjugated equine estrogen (Premarin), the latter of which is arguably slightly more irritating. These are prescribed at a starting dose of 1 g in the vagina three nights per week. After several weeks, they can be titrated to the lowest frequency that controls symptoms. The risk of vaginal candidiasis is fairly high during the first 2 or 3 weeks of reestrogenization, so patients should be warned of this possibility. Also consider prophylactic weekly fluconazole or an azole suppository two or three times a week for the first few weeks. Estradiol tablets (Vagifem) inserted in the vagina are effective, less messy, and more expensive, as is the estradiol ring ( Estring), which is inserted and changed quarterly. It is not unusual for a woman to avoid use of topical estrogen out of fear, or to use insufficient amounts only on the vulva, or to use it for only 1 or 2 weeks. 1 Women should be scheduled for a return visit to ensure they have been using the estrogen, their wet mount has normalized, and discomfort has cleared. When a woman is reluctant to use local estrogen We counsel women that small doses of vaginal estrogen used for limited periods of time are unlikely to influence their breast cancer risk and are the most effective treatment for symptoms of atrophy. Usually, this explanation is sufficient to reassure a woman that topical estrogen is safe. Otherwise, use of commercial personal lubricants (siliconebased lubricants are well tolerated) and moisturizers such as Replens and RePhresh can be comforting. The topical anesthetics lidocaine 2% jelly or lidocaine 5% ointment (which sometimes burns) can minimize pain with sexual activity for those requiring more than lubrication. Ospemifene (Osphena) is used by some clinicians in this situation, but this medication is labeled as a risk for all of the same contraindications as systemic estrogen, and it is much more expensive than topical estrogen. Ospemifene is an estrogen agonist/ antagonist. Although it is the only oral medication indicated for the treatment of menopause-related dyspareunia, the longterm effects on breast cancer risk are unknown. Also, it has an agonist effect on the endometrium and, again, the long-term risk is unknown. Fluconazole use is contraindicated with ospemifene, as is the use of any estrogen products. CASE 2 Recalcitrant itching, burning, and redness A 25-year-old woman reports anogenital itching, burning, and redness, which have been present for 3 months. She says she developed a yeast infection after antibiotic therapy for a dental infection; the yeast infection was treated with terconazole. She reports an allergic reaction to the terconazole, with immediate severe burning, redness, and swelling. The clobetasol cream she was given to use twice daily also caused burning, so she discontinued it. Her symptoms improved when she tried cool soaks and applied topical benzocaine gel as a local anesthetic. However, 32 OBG Management June 2014 Vol. 26 No. 6 obgmanagement.com
3 FIGURE 2 Contact dermatitis Redness and erosions are typical of an acute contact dermatitis, and eroded papules are especially common in contact dermatitis of benzocaine. 2 weeks later, she experienced increasing redness, itching, and burning. Although the benzocaine relieved these symptoms, it required almost continual reapplication for comfort. A physical examination of the vulva reveals generalized, poorly demarcated redness, edema, and superficial erosions (FIGURE 2). Diagnosis: Irritant contact dermatitis (as opposed to allergic contact dermatitis) associated with the use of terconazole and clobetasol. This was followed by allergic contact dermatitis in association with benzocaine. Treatment: Withdrawal of benzocaine, with reinitiation of cool soaks and a switch to clobetasol ointment rather than cream. Nighttime sedation allows the patient to sleep through the itching and gradually allows her skin to heal. Contact dermatitis is a fairly common cause of vulvar irritation, with two main types: Irritant contact dermatitis The most common form, it occurs in any individual exposed to an irritating substance in sufficient quantity or frequency. Irritant contact dermatitis is characterized mostly by sensations of rawness or burning and generally is caused by urine, feces, perspiration, friction, alcohols in topical creams, overwashing, and use of harsh soaps. Allergic contact dermatitis This form is characterized by itching, although secondary pain and burning from scratching and blistering can occur as well. Common allergens in the genital area include benzocaine, diphenhydramine (Benadryl), neomycin in triple antibiotic ointment (Neosporin), and latex. Allergic contact dermatitis occurs after 1 or 2 weeks of initial exposure or 1 or 2 days after re-exposure. The diagnosis of an irritant or allergic contact dermatitis can be based on a history of incontinence, application of high-risk substances, or inappropriate washing. Management generally involves discontinuation of all panty liners and topical agents except for water, with a topical steroid ointment used twice a day and pure petroleum jelly used as often as necessary for comfort. Nighttime sedation to allow a reprieve from rubbing and scratching may be helpful, and narcotic pain medications may be useful for the first 1 to 2 weeks of treatment. Women who fail to respond to treatment should be referred for patch testing by a dermatologist. CASE 3 Teenager with vulvar pain and sores A woman brings her 13-year-old daughter to your office for treatment of sudden-onset vulvar pain and sores. The child developed a sore throat and low-grade fever 3 days earlier, with vulvar pain and vulvar dysuria the next day. The pediatrician diagnosed a herpes simplex virus infection and prescribed oral acyclovir, but the girl s condition has not improved, and the mother believes her daughter s claims of sexual abstinence. The girl is otherwise healthy, aside from a history of trivial oral canker sores without arthritis, headaches, abdominal pain, eye pain, or vision changes. Physical examination of the vulva reveals Diagnosis of an irritant or allergic contact dermatitis can be based on a history of incontinence, application of highrisk substances, or inappropriate washing obgmanagement.com Vol. 26 No. 6 June 2014 OBG Management 33
4 Benign vulvar conditions Aphthae are uncommon and underrecognized on the vulva, and genital aphthae are usually much larger than oral aphthae FIGURE 3 Vulvar aphthae Well-demarcated ulcerations with a white fibrin base are pathognomonic of aphthae when they occur in an immunocompetent teenage girl. soft, painful, well-demarcated ulcers with a white fibrin base (FIGURE 3). Diagnosis: Complex aphthosis. Further testing is unnecessary. Treatment: Prednisone 40 mg/day plus hydrocodone in usual doses of 5/325, one or two tablets every 4 to 6 hours, as needed; topical petroleum jelly (especially before urination); and sitz baths. When the patient returns 1 week later, she is much improved. Aphthae are believed to be of hyperimmune origin, often precipitated by a viral syndrome. They are most common in girls aged 9 to 18 years. Vulvar aphthae are triggered by various viral infections, including Epstein- Barr. 2 The offending virus is not located in the ulcer proper, however, but is identified serologically. Aphthae are uncommon and underrecognized on the vulva, and genital aphthae are usually much larger than oral aphthae. Most patients initially are mistakenly evaluated and treated for sexually transmitted disease, but the large, welldemarcated, painful, nonindurated deep nature of the ulcer is pathognomonic for an aphthous ulcer. The presence of oral and genital aphthae does not constitute a diagnosis of Behçet disease, an often-devastating systemic inflammatory condition occurring almost exclusively in men in the Middle and Far East. The diagnosis of Behçet disease requires the identification of objective inflammatory disease of the eyes, joints, gastrointestinal tract, or neurologic system. True Behçet disease is incredibly uncommon in the United States. When it is diagnosed in Western countries, it takes an attenuated form, most often occurring in women who experience multisystem discomfort rather than identifiable inflammatory disease. End-organ damage is uncommon. Evaluation for Behçet disease in women with vulvar aphthae generally is not indicated, although a directed review of systems is reasonable. The rare patient who experiences frequent recurrence and symptoms of systemic disease should be referred to an ophthalmologist and other relevant specialists to evaluate for inflammatory disease. The treatment of vulvar aphthae consists of systemic corticosteroids such as prednisone 40 mg/day for smaller individuals and 60 mg/day for larger women, with follow-up to ensure a good response. Often, the prednisone can be discontinued when pain relents rather than continued through complete healing. Reassurance, without discussing Behçet disease, is paramount, as is pain control. The heavy application of petroleum jelly can decrease pain and prevent urine from touching the ulcer. Some patients experience recurrent ulcers. A second prescription of prednisone can be provided for immediate reinstitution with onset of symptoms. However, frequent recurrences may require ongoing suppressive medication, with dapsone being the usual first choice. Colchicine often is used, and thalidomide and tumor necrosis factor-a blockers (adalimumab, etanercept, and infliximab) also are extremely beneficial. 3,4 34 OBG Management June 2014 Vol. 26 No. 6 obgmanagement.com
5 FIGURE 4 Desquamative inflammatory vaginitis A B A. Note the redness of the introitus and the medial labia minora, with yellowish vaginal secretions visible at the introitus. B. This wet mount is notable for the marked increase in neutrophils and parabasal cells, with no lactobacilli. CASE 4 Increased neutrophils and no lactobacilli A 36-year-old woman visits your office reporting introital itching, vulvar dysuria, and superficial dyspareunia that have lasted 6 months. She has tried over-the-counter antifungal therapy, with only slight improvement while using the cream. Her health is normal otherwise, lacking pain syndromes or abnormalities suggestive of pelvic floor dysfunction. She experienced comfortable sexual activity until 6 months ago. The only abnormalities apparent on physical examination are redness of the vestibule, medial labia minora, and vaginal walls, with edema of the surrounding skin and no oral lesions (FIGURE 4A ). Copious vaginal secretions are visible at the introitus. A wet mount shows a marked increase in neutrophils with scattered parabasal cells (FIGURE 4B ). There are no clue cells, lactobacilli, or yeast forms. The patient s ph level is greater than 6.5. Routine and fungal cultures and molecular studies for chlamydia, trichomonas, and gonorrhea are returned as normal. o b g m a n a g e m e n t. c om Diagnosis: Desquamative inflammatory vaginitis. Treatment: Clindamycin vaginal cream, 1/2 to 1 full applicator nightly, with a weekly oral fluconazole tablet (200 mg is more easily covered by insurance) to prevent secondary candidiasis. You schedule a follow-up visit in 1 month. Desquamative inflammatory vaginitis (DIV) is described as noninfectious inflammatory vaginitis in a setting of normal estrogen and absence of skin disease of the mucous membranes of the vagina. The condition is characterized by an increase in white blood cells and parabasal cells, and absent lactobacilli, with relatively high vaginal ph. DIV is thought to represent an inflammatory dermatosis of the vaginal epithelium.5 Although some clinicians believe that DIV is actually lichen planus, the latter exhibits erosions as well as redness, nearly always affects the mouth and the vulva, and produces remarkable scarring. DIV does not erode, affect any other skin surfaces, or scar. Vol. 26 No. 6 June 2014 OBG Management CONTINUED ON PAGE 36 35
6 Benign vulvar conditions CONTINUED FROM PAGE 35 FIGURE 5 Inverse psoriasis vagina nightly, or it can be compounded at 100 or 200 mg, if needed. If the condition is recalcitrant, combination therapy can be used. When signs and symptoms abate, the frequency of use can be decreased, or hydrocortisone can be discontinued and restarted again with any recurrence of discomfort. Many clinicians also prescribe weekly fluconazole to prevent intercurrent candidiasis. CASE 5 5 Plaques on vulva and in skin folds Psoriasis of the vulva typically presents as a well-demarcated red, rough plaque that encompasses the dry, keratinized skin of the vulva, with maceration of skin folds suggestive of candidiasis. Other rare skin diseases that produce erosions and scarring also can be ruled out by the presence of erosions, absence of oral disease, and absence of other mucosal involvement. These diseases include cicatricial pemphigoid, pemphigus vulgaris, Stevens- Johnson syndrome, and toxic epidermal necrolysis. Infectious diseases characterized by inflammation are excluded by culture or molecular studies, and atrophic vaginitis and retained foreign bodies (especially retained tampons) can produce a similar picture. The vulvar itching and irritation that occur with DIV most likely represent an irritant contact dermatitis, with vaginal secretions serving as the irritant. How to treat DIV The management of DIV consists of either topical clindamycin cream (theoretically for its anti-inflammatory rather than antimicrobial properties) or intravaginal corticosteroids, especially hydrocortisone acetate. 6 Hydrocortisone can be tried at the low commercially available dose of 25-mg rectal suppositories, which should be inserted into the A 43-year-old woman reports a recalcitrant yeast infection of the vulva, with itching and irritation. She is overweight and diabetic, with mild stress incontinence. Physical examination reveals a fairly well-demarcated plaque of redness of the vulva and labiocrural folds, with satellite red papules and peripheral peeling (FIGURE 5). An examination of other skin surfaces reveals similar plaques in the gluteal cleft, umbilicus, and axillae as well as under the breasts. A fungal preparation of the vagina and skin is negative. You obtain a fungal culture and prescribe topical and oral antifungal therapy and see the patient again 1 week later. Her condition is unchanged. Diagnosis: You make a presumptive diagnosis of inverse psoriasis and do a confirmatory punch biopsy. Treatment: Clobetasol ointment applied to the skin folds, along with continuation of the topical miconazole cream. A week later, the patient s condition is remarkably improved, and her biopsy shows psoriasiform dermatitis. You reduce the potency of her corticosteroid, switching to desonide cream sparingly applied daily. Psoriasis is a common skin disease of immunologic origin. The skin is classically red and thick, with heavy white scale produced by rapid turnover of epithelium. However, there are several morphologic types of psoriasis, and anogenital psoriasis is most often of the inverse pattern. Inverse psoriasis preferentially affects skin folds and is frequently mistaken for (and often initially superinfected with) candidiasis. Scale is thin and unapparent, and there often is a shiny, 36 OBG Management June 2014 Vol. 26 No. 6 obgmanagement.com
7 glazed appearance to the skin. Tiny satellite lesions often are visible as well. A skin biopsy of inverse psoriasis often is not diagnostic, showing only nonspecific psoriasiform dermatitis; this does not disprove psoriasis. Psoriasis is a systemic condition and is associated with metabolic syndrome, carrying an increased risk of overweight, hypertension, diabetes, and cardiovascular disease. Management of these conditions is very important in the treatment of the patient overall. Unlike lichen planus and lichen sclerosus, scarring is rare with psoriasis, and squamous cell carcinoma generally is unassociated. 7,8 Anogenital psoriasis is treated with topical corticosteroids and, when needed, topical vitamin D preparations. Generally, inverse psoriasis is controlled with lowpotency topical corticosteroids, with management of secondary infection and irritants. Otherwise, ultraviolet light is a time-honored therapy for psoriasis but not practical for skin folds. It also is difficult for many patients to manage with a busy life. Systemic therapy, including methotrexate and oral retinoids are often used, as are newer biologic agents such as etanercept, adalimumab, infliximab, and ustekinumab. References 1. Kingsberg SA, Krychman ML. Resistance and barriers to local estrogen therapy in women with atrophic vaginitis. J Sex Med. 2013;10(6): Huppert JS, Gerber MA, Deitch HR, et al. Vulvar ulcers in young females: A manifestation of aphthosis. J Pediatr Adolesc Gynecol. 2006;19(3): O Neill ID. Efficacy of tumour necrosis factor-a antagonists in aphthous ulceration: Review of published individual patient data. J Eur Acad Dermatol Venereol. 2012;26(2): Sanchez-Cano D, Callejas-Rubio JL, Ruiz-Villaverde R, Ortego-Centeno N. Recalcitrant, recurrent aphthous stomatitis successfully treated with adalimumab. J Eur Acad Dermatol Venereol. 2009;23(2): Stockdale CK. Clinical spectrum of desquamative inflammatory vaginitis. Curr Infect Dis Rep. 2010;12(6): Sobel JD, Reichman O, Misra D, Yoo W. Prognosis and treatment of desquamative inflammatory vaginitis. Obstet Gynecol. 2011;117(4): Albert S, Neill S, Derrick EK, Calonje E. Psoriasis associated with vulvar scarring. Clin Exp Dermatol. 2004;29(4): Boffetta P, Gridley G, Lindelöf B. Cancer risk in a populationbased cohort of patients hospitalized for psoriasis in Sweden. J Invest Dermatol. 2001;117(6): An atlas of IMAGES IN GYN ULTRASOUND is building at obgmanagement.com Find this and last month s installment on hemorrhagic ovarian cysts, at obgmanagement.com Uterine adenomyosis: The globular uterus Michelle Stalnaker, MD, and Andrew M. Kaunitz, MD Department of Obstetrics and Gynecology University of Florida College of Medicine Jacksonville Drs. Stalnaker and Kaunitz interpret 15 dramatic ultrasound images, including color Doppler and 3-D imaging, that show adenomyosis identified by myometrial heterogeneity, increased vascularity, and asymmetric posterior myometrial thickening. obgmanagement.com Vol. 26 No. 6 June 2014 OBG Management 37
Conflicts of interest
 Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Kelly H. Tyler, MD, FACOG, FAAD S052 Gender Dermatology: Diagnosis and Treatment of Genital Skin Disorders Vulvar Dermatitis
 Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
Vulval dermatoses. Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough
 Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Cases of Non-Infectious Vulvovaginitis
 Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
Disorders of the vulva
 Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! **
 ** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! ** WHY AM I FILLING OUT THIS FORM? Your responses will help us to understand your experience. Please take your time and try to answer
** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! ** WHY AM I FILLING OUT THIS FORM? Your responses will help us to understand your experience. Please take your time and try to answer
4/3/2017 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS BACTERIAL VAGINOSIS EPIDEMIOLOGY OBJECTIVES
 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
Disclosures Dr. Lynette Margesson
 Management of Vulvar Pruritus 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and
Management of Vulvar Pruritus 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and
Topics in Women s Health. Ann Laros, MD University of Iowa
 Topics in Women s Health Ann Laros, MD University of Iowa Topics in Women s Health 1. Cervical cancer screening guidelines 2. ACHA Pap and STI data 3. Vulvar pearls 4. Genital HSV 2012 Cervical Cancer
Topics in Women s Health Ann Laros, MD University of Iowa Topics in Women s Health 1. Cervical cancer screening guidelines 2. ACHA Pap and STI data 3. Vulvar pearls 4. Genital HSV 2012 Cervical Cancer
Vaginitis. Antibiotics Changes in hormone levels due to pregnancy, breastfeeding, or menopause Douching Spermicides Sexual intercourse Infection
 WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Vaginitis Vaginitis is an inflammation of a woman s vagina. It is one of the most common reasons why women see their health care providers.
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Vaginitis Vaginitis is an inflammation of a woman s vagina. It is one of the most common reasons why women see their health care providers.
What are the symptoms of a vulval skin condition?
 Information for you Published in December 2013 Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting the vulva. If you are
Information for you Published in December 2013 Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting the vulva. If you are
Diagnosis and Management of Vulvar Disorders
 Diagnosis and Management of Vulvar Disorders Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics
Diagnosis and Management of Vulvar Disorders Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics
The use of CO2 laser for patients with Lichen sclerosus
 The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
ASCCP 2016 Annual Meeting. Post Test. Hope K. Haefner, MD The University of Michigan Center for Vulvar Diseases
 ASCCP 2016 Annual Meeting Post Test Hope K. Haefner, MD The University of Michigan Center for Vulvar Diseases haefner@umich.edu Disclosure Hope Haefner, MD was previously on the advisory board of Merck
ASCCP 2016 Annual Meeting Post Test Hope K. Haefner, MD The University of Michigan Center for Vulvar Diseases haefner@umich.edu Disclosure Hope Haefner, MD was previously on the advisory board of Merck
The Vulvar Lichen Disorders: Simplex, Sclerosus, Planus
 The Vulvar Lichen Disorders: Simplex, Sclerosus, Planus Paul Summers, M.D. Department of Obstetrics and Gynecology University of Utah School of Medicine Areas of Concern 1. Dermatopathology 2. Spongiotic
The Vulvar Lichen Disorders: Simplex, Sclerosus, Planus Paul Summers, M.D. Department of Obstetrics and Gynecology University of Utah School of Medicine Areas of Concern 1. Dermatopathology 2. Spongiotic
New Treatments for Vaginal Health. Sarah Azad, MD El Camino Women s Medical Group
 New Treatments for Vaginal Health There s Hope Sarah Azad, MD El Camino Women s Medical Group The Genitrourinary Syndrome of Menopause (GSM) Problems with genital health secondary to the changes that occur
New Treatments for Vaginal Health There s Hope Sarah Azad, MD El Camino Women s Medical Group The Genitrourinary Syndrome of Menopause (GSM) Problems with genital health secondary to the changes that occur
Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California.
 Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California? Disclosures Hope K. Haefner, MD is on the advisory board of Merck Co. Inc. Lynette
Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California? Disclosures Hope K. Haefner, MD is on the advisory board of Merck Co. Inc. Lynette
There are a variety of ways to address VVA. Keep yourself healthy, avoid irritants to the vulva and vagina, and use moisturizers and lubricants.
 What is VulvoVaginal Atrophy? VulvoVaginal Atrophy, or VVA for short, is also called genitourinary syndrome of menopause. VVA is a condition where the skin of the vagina and vulva becomes thin, dry and
What is VulvoVaginal Atrophy? VulvoVaginal Atrophy, or VVA for short, is also called genitourinary syndrome of menopause. VVA is a condition where the skin of the vagina and vulva becomes thin, dry and
Investigation and Management of Vaginal Discharge in Adult Women
 Investigation and Management of Vaginal Discharge in Adult Women SUMMARY POINTS A detailed history, including sexual history, should be taken to explore potential causes and guide investigation and management.
Investigation and Management of Vaginal Discharge in Adult Women SUMMARY POINTS A detailed history, including sexual history, should be taken to explore potential causes and guide investigation and management.
Case 1. Case Studies in Vulvovaginal Disease. Disclosures. What is your diagnosis? Case 1. Lichen sclerosus 10/19/2018
 Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
Year: Issue 1 Obs/Gyne The silent epidemic: Postmenopausal vaginal atrophy
 Year: 2013 - Issue 1 Obs/Gyne The silent epidemic: Postmenopausal vaginal atrophy By: Dr David W Sturdee, Immediate past President International Menopause Society and Hon Consultant Gynaecologist, Solihull
Year: 2013 - Issue 1 Obs/Gyne The silent epidemic: Postmenopausal vaginal atrophy By: Dr David W Sturdee, Immediate past President International Menopause Society and Hon Consultant Gynaecologist, Solihull
VIN/VAIN O C T O B E R 3 RD J M O R G A N
 VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
Vulvodynia and vestibulectomy
 Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
Vulvar Disease Clinical Cases
 Vulvar Disease Clinical Cases Hope K. Haefner, MD Professor University of Michigan Health System February 27, 2015 Cartagena Conflicts of Interest Hope Haefner, MD is on the Advisory Board of Merck Co.,
Vulvar Disease Clinical Cases Hope K. Haefner, MD Professor University of Michigan Health System February 27, 2015 Cartagena Conflicts of Interest Hope Haefner, MD is on the Advisory Board of Merck Co.,
Sexually Transmitted Infections. Kim Dawson October 2010
 Sexually Transmitted Infections Kim Dawson October 2010 Objectives: You will learn about: Sexually Transmitted Infections (STI s). How they are transferred. High risk behavior. The most common STI s. How
Sexually Transmitted Infections Kim Dawson October 2010 Objectives: You will learn about: Sexually Transmitted Infections (STI s). How they are transferred. High risk behavior. The most common STI s. How
Prescribing Information
 Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Innovations in the Management of Dyspareunia
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
FEMININE INTIMATE CARE
 FEMININE INTIMATE CARE The role of the pharmacist Dr Trudy Smith Vaginal Health Vagina sensitive area Just like GIT, also contain flora Vaginal flora Maintain healthy ph (4.5) Lactobacilli (aerobic) Automatic
FEMININE INTIMATE CARE The role of the pharmacist Dr Trudy Smith Vaginal Health Vagina sensitive area Just like GIT, also contain flora Vaginal flora Maintain healthy ph (4.5) Lactobacilli (aerobic) Automatic
Skin lesions & Abrasions
 Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
Vaginal involvement in genital erosive lichen planus
 Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
Lichen sclerosus. Lichen planus
 Lichen sclerosus Lichen planus Dr Fiona Lewis, Consultant Dermatologist, Heatherwood and Wexham Park NHS Foundation Trust & St John s Institute of Dermatology, GSTT Outline Typical features of lichen sclerosus
Lichen sclerosus Lichen planus Dr Fiona Lewis, Consultant Dermatologist, Heatherwood and Wexham Park NHS Foundation Trust & St John s Institute of Dermatology, GSTT Outline Typical features of lichen sclerosus
Dr Lilianne Scholtz (MBBCh)
 Dr Lilianne Scholtz (MBBCh) I have a discharge. It s itchy and it burns. My urine burns too. Diagnosis based on symptoms alone is accurate in ~34 % of women because symptoms are very non-specific Sobel
Dr Lilianne Scholtz (MBBCh) I have a discharge. It s itchy and it burns. My urine burns too. Diagnosis based on symptoms alone is accurate in ~34 % of women because symptoms are very non-specific Sobel
Vulvar and Vaginal Disorders Questionnaire
 1 Your Name: Vulvar and Vaginal Disorders Questionnaire Referring provider: To whom should we send a report about this visit: My physician: Don t send anyone a report Address/Phone: Ethnicity (circle):
1 Your Name: Vulvar and Vaginal Disorders Questionnaire Referring provider: To whom should we send a report about this visit: My physician: Don t send anyone a report Address/Phone: Ethnicity (circle):
Diseases of the vulva
 Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Scream Cream. Ingredients: Aminophylline 15-mg, Ergoloid mesylate 0.25-mg, Pentoxifylline 25-mg and L-Arginine 30-mg
 At LifeCare Pharmacy we understand that women have different needs at different stages of their lives. Maintaining a healthy and balanced lifestyle can be a difficult struggle. The chronic stress of overly
At LifeCare Pharmacy we understand that women have different needs at different stages of their lives. Maintaining a healthy and balanced lifestyle can be a difficult struggle. The chronic stress of overly
MYTHS OF STIs True or False
 MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
Prepubertal labial adhesions: Evaluation of a referral population
 Prepubertal labial adhesions: Evaluation of a referral population Janice L. Bacon, MD Columbia, SC OBJECTIVE: The purpose of this study was to assess patient demographics, clinical presentation, response
Prepubertal labial adhesions: Evaluation of a referral population Janice L. Bacon, MD Columbia, SC OBJECTIVE: The purpose of this study was to assess patient demographics, clinical presentation, response
Vulval disease in children
 Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
Complex Vaginitis Cases: Applying New Diagnostic Methods to Enhance Patient Outcomes ReachMD Page 1 of 5
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
HOW TO DIAGNOSE VULVAR DISEASES:
 HOW TO DIAGNOSE VULVAR DISEASES: Diagnostic approach. Normal findings. Maria Sol Peremateu, MD A wide spectrum of benign, premalignant, and malignant lesions may occur on the vulva. Some of the disorders
HOW TO DIAGNOSE VULVAR DISEASES: Diagnostic approach. Normal findings. Maria Sol Peremateu, MD A wide spectrum of benign, premalignant, and malignant lesions may occur on the vulva. Some of the disorders
GROUP 15 TOPICAL PREPARATIONS
 - 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
- 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
Vulval disease in children
 Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
The Case of Mrs. Virginia Jones* Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver, Canada
 Case title: Case authors: Case synopsis: The Case of Mrs. Virginia Jones* Dr. Leslie A. Sadownik Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver,
Case title: Case authors: Case synopsis: The Case of Mrs. Virginia Jones* Dr. Leslie A. Sadownik Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver,
Sexually Transmitted Diseases. Ch 24
 Sexually Transmitted Diseases Ch 24 Statistics THERE ARE CURRENTLY 65 MILLION PEOPLE LIVING WITH INCURABLE STDs IN THE U.S. THERE ARE 15 MILLION NEW CASES REPORTED EACH YEAR SOURCE: CDC, 2000 REPORTS WHY
Sexually Transmitted Diseases Ch 24 Statistics THERE ARE CURRENTLY 65 MILLION PEOPLE LIVING WITH INCURABLE STDs IN THE U.S. THERE ARE 15 MILLION NEW CASES REPORTED EACH YEAR SOURCE: CDC, 2000 REPORTS WHY
The Normal Vulva: Overview of Basic Dermatology Treatment
 The Normal Vulva: Overview of Basic Dermatology Treatment 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor
The Normal Vulva: Overview of Basic Dermatology Treatment 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor
An All Too Familiar Story
 All that itches is not yeast Michele Ambor Hutz NP An All Too Familiar Story A patient presents to her provider complaining of frequent yeast infections. The provider prescribes treatment without an exam
All that itches is not yeast Michele Ambor Hutz NP An All Too Familiar Story A patient presents to her provider complaining of frequent yeast infections. The provider prescribes treatment without an exam
Conflicts of interest. Genital Lichen Planus. Objectives. Lichen Planus. Genital Lichen Planus. Author Up To Date. Vulvar Lichen Planus Patterns
 Genital Lichen Planus Lynette J. Margesson MD FRCPC AAD Washington Mucous Membrane Symposium Saturday, March 2, 2019 Conflicts of interest Author Up To Date Little evidence based treatment Too few studies
Genital Lichen Planus Lynette J. Margesson MD FRCPC AAD Washington Mucous Membrane Symposium Saturday, March 2, 2019 Conflicts of interest Author Up To Date Little evidence based treatment Too few studies
Coding for Fitting and Insertion of a Pessary
 Coding for Fitting and Insertion of a Pessary A pessary is a device worn in the vagina for the treatment of pelvic organ prolapse or stress urinary incontinence. The pessary provides support of the vaginal
Coding for Fitting and Insertion of a Pessary A pessary is a device worn in the vagina for the treatment of pelvic organ prolapse or stress urinary incontinence. The pessary provides support of the vaginal
Anne Arundel Medical Center Informed Consent
 Informed Consent Title: Exploratory Trial of Autologous Platelet Rich Plasma (PRP) Intradermal Injections for the Treatment of Vulvar Lichen Sclerosus Investigator: Andrew Goldstein, M.D. Telephone Study
Informed Consent Title: Exploratory Trial of Autologous Platelet Rich Plasma (PRP) Intradermal Injections for the Treatment of Vulvar Lichen Sclerosus Investigator: Andrew Goldstein, M.D. Telephone Study
For topical use only. Not for oral, ophthalmic, or intravaginal use.
 DESOXIMETASONE Ointment USP, 0.25% For topical use only. Not for oral, ophthalmic, or intravaginal use. Rx only DESCRIPTION Desoximetasone ointment USP, 0.25% contains the active synthetic corticosteroid
DESOXIMETASONE Ointment USP, 0.25% For topical use only. Not for oral, ophthalmic, or intravaginal use. Rx only DESCRIPTION Desoximetasone ointment USP, 0.25% contains the active synthetic corticosteroid
Types of vaginal yeast
 Types of vaginal yeast You should seek medical care any time if you have pain. Although vaginal infections may cause unpleasant itching, they should not cause pain. Call for an appointment with your healthcare
Types of vaginal yeast You should seek medical care any time if you have pain. Although vaginal infections may cause unpleasant itching, they should not cause pain. Call for an appointment with your healthcare
In the August 2016 issue of OBG Management,
 GYN coding changes to note for your maximized reimbursement Revised ICD-10 gynecologic diagnostic codes go into effect October 1. Here is a look at the added, expanded, and revised codes you will need
GYN coding changes to note for your maximized reimbursement Revised ICD-10 gynecologic diagnostic codes go into effect October 1. Here is a look at the added, expanded, and revised codes you will need
- (Have NO cure yet, but are controllable) - (Can be cured if caught early enough)
 Myths or Facts of STD s 1. Most people with an STD experience painful symptoms. 2. Abstinence is the best way to prevent STD s. 3. If you get an STD once, and are treated, you can t get it again. 4. A
Myths or Facts of STD s 1. Most people with an STD experience painful symptoms. 2. Abstinence is the best way to prevent STD s. 3. If you get an STD once, and are treated, you can t get it again. 4. A
OBSTETRICS & GYNECOLOGY
 JANUARY 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Female Sexual Arousal
JANUARY 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Female Sexual Arousal
Asymptomatic Undiagnosed Lichen Sclerosus
 Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation
 Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation Ashley Christensen, BSN, 1 Michael Haugsdal, MD, 2 and Noelle Bowdler, MD 2 Keywords: Vulvovaginal irritation,
Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation Ashley Christensen, BSN, 1 Michael Haugsdal, MD, 2 and Noelle Bowdler, MD 2 Keywords: Vulvovaginal irritation,
PACKAGE LEAFLET: INFORMATION FOR THE USER. Flutarzole 0,05% w/w cream, Fluticasone propionate
 PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
WHITE PAPER SmartXide 2 V 2 LR. MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy
 WHITE PAPER SmartXide 2 V 2 LR MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy DEKA White Paper SMARTXIDE 2 V 2 LR November 2015 MonaLisa Touch Dual Probe Therapy
WHITE PAPER SmartXide 2 V 2 LR MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy DEKA White Paper SMARTXIDE 2 V 2 LR November 2015 MonaLisa Touch Dual Probe Therapy
CANDIDIASIS (WOMEN) Single Episode. Clinical Features. Diagnosis. Management
 CANDIDIASIS (WOMEN) What s new: Section on Management of Vulvovaginal Non-Albicans Candida Infection in Adults approved by GGC antimicrobial team Routine candida sensitivity testing has been discontinued,
CANDIDIASIS (WOMEN) What s new: Section on Management of Vulvovaginal Non-Albicans Candida Infection in Adults approved by GGC antimicrobial team Routine candida sensitivity testing has been discontinued,
Management of Complex Vulvovaginal Conditions. Hope K. Haefner, MD Professor Michigan Medicine February 9, 2018
 Management of Complex Vulvovaginal Conditions Hope K. Haefner, MD Professor Michigan Medicine February 9, 2018 Disclosures Hope K. Haefner, MD None Learning Objectives At the conclusion of this activity,
Management of Complex Vulvovaginal Conditions Hope K. Haefner, MD Professor Michigan Medicine February 9, 2018 Disclosures Hope K. Haefner, MD None Learning Objectives At the conclusion of this activity,
Lichen Sclerosus. Exceptional healthcare, personally delivered
 Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Management of Complex Vulvovaginal Conditions
 Management of Complex Vulvovaginal Conditions Hope K. Haefner, MD Professor Michigan Medicine August 10, 2018 None Disclosures Hope K. Haefner, MD 1 Learning Objectives At the conclusion of this activity,
Management of Complex Vulvovaginal Conditions Hope K. Haefner, MD Professor Michigan Medicine August 10, 2018 None Disclosures Hope K. Haefner, MD 1 Learning Objectives At the conclusion of this activity,
Eczema & Dermatitis Clinical features: Histopathological features: Classification:
 Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Common Superficial Fungal Infections
 How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
Sexually Transmitted Infections in the Adolescent Population. Abraham Lichtmacher MD FACOG Chief of Women s Services Lovelace Health System
 Sexually Transmitted Infections in the Adolescent Population Abraham Lichtmacher MD FACOG Chief of Women s Services Lovelace Health System STI in the Adolescent High school students nationwide, 34.2% were
Sexually Transmitted Infections in the Adolescent Population Abraham Lichtmacher MD FACOG Chief of Women s Services Lovelace Health System STI in the Adolescent High school students nationwide, 34.2% were
Vaginitis. Is vaginal discharge ever normal? Women with vaginal discharge. Vaginal symptoms are very common. Patient with chronic vaginal discharge
 Vaginitis Is the wet prep out of the building? No disclosures related to this topic Images are cited with permissions Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Health
Vaginitis Is the wet prep out of the building? No disclosures related to this topic Images are cited with permissions Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Health
STI s. (Sexually Transmitted Infections)
 STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
Prescribing Information. Taro-Clobetasol. Taro-Clobetasol
 Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
The Genital Skin During Menopause in Health and Disease
 The Genital Skin During Menopause in Health and Disease 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of
The Genital Skin During Menopause in Health and Disease 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of
STI Review. CALM: STI/HIV - Lesson One (Handout 3) Bacteria/ Transmission. Symptoms. Disease. Virus
 STI Review Bacteria/ Virus? Transmission Chlamydia Bacteria Unprotected vaginal or anal sex with a person who has Chlamydia Genital Herpes Virus By direct contact with the sores or blisters of an infected
STI Review Bacteria/ Virus? Transmission Chlamydia Bacteria Unprotected vaginal or anal sex with a person who has Chlamydia Genital Herpes Virus By direct contact with the sores or blisters of an infected
LTASEX.INFO STI SUMMARY SHEETS FOR EDUCATIONAL USE ONLY. COMMERCIAL USE RIGHTS RESERVED. COPYRIGHT 2013, JEROME STUART NICHOLS
 LTASEX.INFO STI SUMMARY SHEETS FOR EDUCATIONAL USE ONLY. COMMERCIAL USE RIGHTS RESERVED. COPYRIGHT 2013, JEROME STUART NICHOLS LTASEX.INFO! IN AIDS is a treatable complication of advanced HIV infection.
LTASEX.INFO STI SUMMARY SHEETS FOR EDUCATIONAL USE ONLY. COMMERCIAL USE RIGHTS RESERVED. COPYRIGHT 2013, JEROME STUART NICHOLS LTASEX.INFO! IN AIDS is a treatable complication of advanced HIV infection.
Make Love Not Warts Genital Warts
 Patricia Wong, MD 735 Cowper Street Palo Alto, CA 94301 650-473-3173 www.patriciawongmd.com Make Love Not Warts Genital Warts Genital warts are the most common sexually transmitted disease. The lifetime
Patricia Wong, MD 735 Cowper Street Palo Alto, CA 94301 650-473-3173 www.patriciawongmd.com Make Love Not Warts Genital Warts Genital warts are the most common sexually transmitted disease. The lifetime
Management of benign vulval dermatoses in primary care
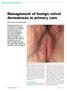 PRESCRIBING IN PRACTICE Management of benign vulval dermatoses in primary care MITESH PATEL AND DAVID NUNNS SPL Vulval dermatoses can be difficult to manage in primary care, and GPs need to be aware of
PRESCRIBING IN PRACTICE Management of benign vulval dermatoses in primary care MITESH PATEL AND DAVID NUNNS SPL Vulval dermatoses can be difficult to manage in primary care, and GPs need to be aware of
Company. Relationship. Content Area. Glaxo Smith Kline. Speaker. Over Active Bladder, Herpes
 Conflict of Interest Disclosure R. Mimi Secor, MS, NP, FAANP I disclose the following financial relationships with commercial entities that produce health care-related products or services relevant to
Conflict of Interest Disclosure R. Mimi Secor, MS, NP, FAANP I disclose the following financial relationships with commercial entities that produce health care-related products or services relevant to
Table of Contents. Injectable Gel with 0.3% Lidocaine
 Patient Brochure Table of Contents About Restylane-L 4 Safety 6 Post-Marketing Surveillance 9 About the Procedure 10 Troubleshooting 11 Injectable Gel with 0.3% Lidocaine 2 3 About Restylane-L Q What is
Patient Brochure Table of Contents About Restylane-L 4 Safety 6 Post-Marketing Surveillance 9 About the Procedure 10 Troubleshooting 11 Injectable Gel with 0.3% Lidocaine 2 3 About Restylane-L Q What is
Southern California Center for Sexual Health and Survivorship Medicine Inc, Newport Beach, CA 3
 The WISDOM survey: Physicians Level of Comfort Prescribing Treatment for Vulvar and Vaginal Atrophy (VVA) Symptoms in Women with a Predisposition or History of Breast Cancer Lisa Larkin, MD 1 ; Michael
The WISDOM survey: Physicians Level of Comfort Prescribing Treatment for Vulvar and Vaginal Atrophy (VVA) Symptoms in Women with a Predisposition or History of Breast Cancer Lisa Larkin, MD 1 ; Michael
STD. Are sexually transmitted infections (STIs) different from sexually transmitted diseases (STDs)?
 What are sexually transmitted diseases (STDs)? STD Sexually transmitted diseases are diseases that can be passed from person to person through sexual contact. Depending on the STD, sexual contact that
What are sexually transmitted diseases (STDs)? STD Sexually transmitted diseases are diseases that can be passed from person to person through sexual contact. Depending on the STD, sexual contact that
Sexually Transmitted. Diseases
 Sexually Transmitted Diseases How can I get an STD? Many STDs are carried and transmitted through semen and vaginal fluids. Some STDs can be spread through skin to skin contact Mother to child STDs: Signs
Sexually Transmitted Diseases How can I get an STD? Many STDs are carried and transmitted through semen and vaginal fluids. Some STDs can be spread through skin to skin contact Mother to child STDs: Signs
Photo Diagnosis. An illustrated quiz on problems seen in everyday practice ANSWERS ON PAGE 52. Provided by Dr. Benjamin Barankin, Edmonton, Alberta.
 An illustrated quiz on problems seen in everyday practice Case 1 A 67-year-old man had surgery on the chest two years ago after significant weight loss and night sweats. 2. What factors can increase the
An illustrated quiz on problems seen in everyday practice Case 1 A 67-year-old man had surgery on the chest two years ago after significant weight loss and night sweats. 2. What factors can increase the
Management of Menopausal Symptoms
 Management of Menopausal Symptoms Tammie Koehler DO, FACOG 1 Menopause Permanent cessation of menstruation that occurs after the loss of ovarian activity Determined to have occurred after 1 full year of
Management of Menopausal Symptoms Tammie Koehler DO, FACOG 1 Menopause Permanent cessation of menstruation that occurs after the loss of ovarian activity Determined to have occurred after 1 full year of
Sexually Transmissible Infections (STI) and Blood-borne Viruses (BBV) A guide for health promotion workers
 Sexually Transmissible Infections (STI) and Blood-borne Viruses (BBV) A guide for health promotion workers Sexual & Reproductive Health Western Australia Chlamydia (bacterial infection) Unprotected vaginal
Sexually Transmissible Infections (STI) and Blood-borne Viruses (BBV) A guide for health promotion workers Sexual & Reproductive Health Western Australia Chlamydia (bacterial infection) Unprotected vaginal
Learning Objectives. Peri menopause. Menopause Overview. Recommendation grading categories
 Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
How is it transferred?
 STI s What is a STI? It is a contagious infection that is transferred from one person to another through sexual intercourse or other sexually- related behaviors. How is it transferred? The organisms live
STI s What is a STI? It is a contagious infection that is transferred from one person to another through sexual intercourse or other sexually- related behaviors. How is it transferred? The organisms live
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
Lichen planus. Information for patients Gynaecology
 Lichen planus Information for patients Gynaecology page 2 of 8 What is lichen planus? Lichen planus is a non-cancerous, inflammatory skin condition that causes an itchy, non-infectious rash (small purple
Lichen planus Information for patients Gynaecology page 2 of 8 What is lichen planus? Lichen planus is a non-cancerous, inflammatory skin condition that causes an itchy, non-infectious rash (small purple
WELCOME. Training village
 WELCOME Training village PERFORM EASY AND PAINLESS VAGINAL DRYNESS TREATMENT WITH ELEA Dr Bertrand Durantet Aesthetic Doctor LYON France PART 1 FEATURES ON ELEA THE MAGNETIC SUPPORT THE FOOT PEDAL THE
WELCOME Training village PERFORM EASY AND PAINLESS VAGINAL DRYNESS TREATMENT WITH ELEA Dr Bertrand Durantet Aesthetic Doctor LYON France PART 1 FEATURES ON ELEA THE MAGNETIC SUPPORT THE FOOT PEDAL THE
What are some common conditions that affect the cornea?
 What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
Treating GSM without Estrogens. Lubrication and Vaginal Dilators
 Treating GSM without Estrogens Lubrication and Vaginal Dilators Hope K. Haefner, MD Michigan Medicine Ann Arbor, MI USA Disclosures/Conflicts of Interest Hope Haefner, MD has no disclosures or conflicts
Treating GSM without Estrogens Lubrication and Vaginal Dilators Hope K. Haefner, MD Michigan Medicine Ann Arbor, MI USA Disclosures/Conflicts of Interest Hope Haefner, MD has no disclosures or conflicts
Oral Medicine. Dr. Qianming Ian CHEN
 Oral Medicine Dr. Qianming Ian CHEN ORAL MEDICINE Oral medicine is the specialty of dentistry that is concerned with the oral health care of medically compromised patients and with the diagnosis and nonsurgical
Oral Medicine Dr. Qianming Ian CHEN ORAL MEDICINE Oral medicine is the specialty of dentistry that is concerned with the oral health care of medically compromised patients and with the diagnosis and nonsurgical
How to Prevent Sexually Transmitted Diseases
 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright owner. This includes
ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright owner. This includes
Persistent Genital Arousal Disorder (PGAD) in Women: Mental or Body
 Persistent Genital Arousal Disorder (PGAD) in Women: Mental or Body Irwin Goldstein MD Director, Sexual Medicine, Alvarado Hospital, San Diego, California Clinical Professor of Surgery, University of California,
Persistent Genital Arousal Disorder (PGAD) in Women: Mental or Body Irwin Goldstein MD Director, Sexual Medicine, Alvarado Hospital, San Diego, California Clinical Professor of Surgery, University of California,
SEXUAL PAIN Home messages, a summary from Presentations, moderated Posters and Podiums
 SEXUAL PAIN Home messages, a summary from Presentations, moderated Posters and Podiums María Luisa Banfi, MD Gynecologist, Sexologist Montevideo, Uruguay, South America CHICAGO 2012,SMS- ISSM, World Meeting
SEXUAL PAIN Home messages, a summary from Presentations, moderated Posters and Podiums María Luisa Banfi, MD Gynecologist, Sexologist Montevideo, Uruguay, South America CHICAGO 2012,SMS- ISSM, World Meeting
WOMENCARE. Herpes. Source: PDR.net Page 1 of 8. A Healthy Woman is a Powerful Woman (407)
 WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
MALE GENITAL (PENIS) LICHEN SCLEROSUS
 MALE GENITAL (PENIS) LICHEN SCLEROSUS What are the aims of this leaflet? This leaflet has been written to help you understand more about male genital lichen sclerosus (also known as balanitis xerotica
MALE GENITAL (PENIS) LICHEN SCLEROSUS What are the aims of this leaflet? This leaflet has been written to help you understand more about male genital lichen sclerosus (also known as balanitis xerotica
PAINFUL URINATION CAUSES & NATURAL REMEDY. Dr. Bestman Anyatonwu
 LIBRACIN NATURAL MEDICINE IND. LTD PAINFUL URINATION CAUSES & NATURAL REMEDY Dr. Bestman Anyatonwu MEANING Painful urination is a broad term that describes discomfort during urination. This pain may originate
LIBRACIN NATURAL MEDICINE IND. LTD PAINFUL URINATION CAUSES & NATURAL REMEDY Dr. Bestman Anyatonwu MEANING Painful urination is a broad term that describes discomfort during urination. This pain may originate
Burdensome Vaginal Infections: Best Diagnostic Practices for Driving Better Patient Outcomes
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions
 Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD Professor University of Michigan Health System Ann Arbor, Michigan February, 2017 Industry Support and Financial
Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD Professor University of Michigan Health System Ann Arbor, Michigan February, 2017 Industry Support and Financial
Vulvovaginal Complaints
 Curr Treat Options Peds (2016) 2:209 215 DOI 10.1007/s40746-016-0062-8 Pediatric Gynecology (L Breech and K Stambough, Section Editors) Vulvovaginal Complaints Chelsea Bayer, MD Laura Parks, MD * Address
Curr Treat Options Peds (2016) 2:209 215 DOI 10.1007/s40746-016-0062-8 Pediatric Gynecology (L Breech and K Stambough, Section Editors) Vulvovaginal Complaints Chelsea Bayer, MD Laura Parks, MD * Address
Summary. Accepted for publication 18 May Key words genital lichen planus, oral lichen planus, vulval lichen planus
 CLINICAL AND LABORATORY INVESTIGATIONS DOI 10.1111/j.1365-2133.2006.07480.x Prevalence of vulval lichen planus in a cohort of women with oral lichen planus: an interdisciplinary study P. Belfiore, O. Di
CLINICAL AND LABORATORY INVESTIGATIONS DOI 10.1111/j.1365-2133.2006.07480.x Prevalence of vulval lichen planus in a cohort of women with oral lichen planus: an interdisciplinary study P. Belfiore, O. Di
