Guillain-Barré Syndrome and Its Variants: A Case of Acute Motor-sensory Axonal Neuropathy in Jamaica
|
|
|
- Bernadette Payne
- 6 years ago
- Views:
Transcription
1 Guillain-Barré Syndrome and Its Variants: A Case of Acute Motor-sensory Axonal Neuropathy in Jamaica K Fletcher-Peddie 1, R Alfred 2, K Penn-Brown 3, F Gayle 1, DT Gilbert 1, V Elliot 1, TS Ferguson 1, 4 ABSTRACT This paper reports a case of a Jamaican young woman who experienced flaccid quadriparesis and bulbar weakness over a three-week period after a gastrointestinal illness. Nerve conduction studies confirmed an axonal type neuropathy consistent with the acute motor-sensory axonal neuropathy variant of the Guillain-Barré syndrome. Recovery, although evident, was slow and was augmented after a course of intravenous immunoglobulin. The patient was discharged from hospital after three months but was re-admitted one week later and eventually succumbed to complications of the illness. This case serves as a reminder that Guillain-Barré syndrome is now the most common cause of acute flaccid paralysis and should be considered early in all patients presenting with flaccid quadriparesis. Keywords: Acute motor-sensory axonal neuropathy, flaccid paresis, Guillain-Barré syndrome, Jamaica Síndrome de Guillain-Barré y Sus Variantes: Un Caso de la Neuropatía Axonal Sensorial Motor Aguda en Jamaica K Fletcher-Peddie 1, R Alfred 2, K Penn-Brown 3, F Gayle 1, DT Gilbert 1, V Elliot 1, TS Ferguson 1, 4 RESUMEN El presenta trabajo reporta el caso de una joven jamaicana que experimentó debilidad bulbar y cuadriparesia flácida por un período de tres semanas después de una enfermedad gastrointestinal. Los estudios de conducción nerviosa confirmaron una neuropatía de tipo axonal en correspondencia con la variante de la neuropatía axonal sensorial motora aguda del síndrome de Guillain-Barré. La recuperación, aunque evidente, fue lenta, y aumentó después de que se le aplicara inmunoglobulina intravenosa. La paciente fue dada de alta del hospital después de tres meses, pero fue ingresada de nuevo una semana más tarde, falleciendo finalmente a causa de las complicaciones de la enfermedad. Este caso sirve como recordatorio de que el síndrome de Guillain-Barré es ahora la causa más común de parálisis flácida aguda, y debe tenerse en cuenta temprano en todos los pacientes que acuden con cuadriparesia flácida. Palabras claves: Neuropatía axonal sensorial y motora aguda, paresia flácida, síndrome de Guillain-Barré, Jamaica West Indian Med J 2013; 62 (7): 658 From: 1 Department of Medicine, University Hospital of the West Indies, Kingston 7, Jamaica, 2 Scarborough General Hospital, Signal Hill, Tobago, 3 Spanish Town Hospital, St Catherine, Jamaica and 4 Tropical Medicine Research Institute (Epidemiology Research Unit), The University of the West Indies, Kingston 7, Jamaica. Correspondence: Dr R Alfred, Scarborough General Hospital, Signal Hill, Tobago, West Indies. rose24_tt@yahoo.com. INTRODUCTION Guillain-Barré syndrome (GBS) is characterized pathologically by inflammatory lesions throughout the peripheral nervous system (1). It represents an acute or subacute peripheral polyneuropathy characterized by symmetrical limb weakness occurring in the absence of identifiable causes of genetic, metabolic, or toxic origin. The characteristic presentation of the syndrome involves symmetrical paresis or paresthesia of an ascending nature, with diminished reflexes or areflexia and variable motor, sensory, or autonomic dysfunction (2). Guillain-Barré syndrome is now the most frequent cause of acute flaccid paralysis worldwide and has a guarded prognosis with up to 20% of patients experiencing severe long-term disability and up to 5% of patients dying even after receiving appropriate therapy (3). West Indian Med J 2013; 62 (7): 658
2 659 Fletcher-Peddie et al Diagnostic approach to GBS is based on clinical, laboratory, and electrophysiological criteria. The history is of paramount importance and is characterized by symmetric flaccid paresis associated with varying combinations of pain, paresthesia and numbness. The National Institute of Neurological Disorders and Stroke (NINDS) has defined the weakness as progressive (over a four-week period) in their diagnostic criteria developed to guide physicians in making the diagnosis (4). The Brighton Collaboration GBS Working Group (5) has defined key clinical and epidemiologic features required for case definitions for GBS. The Working Group has stated in their case definition that limb weakness in GBS should be bilateral and relatively symmetric (generally with progression from legs to arms and bulbar muscles), associated with decreased or absent deep tendon reflexes in weak limbs, a monophasic illness pattern, an interval between onset and nadir of weakness between 12 hours and 28 days, subsequent clinical plateau, electrophysiologic findings consistent with GBS, cytoalbuminologic dissociation (ie elevation of cerebrospinal fluid (CSF) protein level above laboratory normal value, CSF total white cell count < 50 cells/mm 3 and absence of an identified alternative diagnosis for weakness). There are three levels of diagnostic certainty (5). Level 1 includes all of the above, while levels 2 and 3 do not meet CSF or electrophysiological studies criteria, respectively. Guillain-Barré syndrome more commonly has a demyelinating type on histology, but variants exist. Histologically, GBS may be classified as having demyelinating and axonal subtypes, namely, acute inflammatory demyelinating polyneuropathy (AIDP), acute motor axonal neuropathy (AMAN) and acute motor-sensory axonal neuropathy (AMSAN). Acute motor-conduction-block neuropathy, another GBS variant, is believed to be a mild form of AMAN (2, 3). In Europe and North America, demyelinating GBS accounts for up to 90% of cases, but in other countries such as China and Japan, the axonal type GBS account for 30 65% of cases (3). In this paper, we present a case of axonal type GBS and discuss issues related to the presentation and diagnosis of GBS and its variants. CASE REPORT The case is that of a 27-year old Jamaican woman, of African descent, with no prior history of chronic illnesses. She was well up until one week prior to her initial admission to hospital, when after having a meal of chicken and rice at a local restaurant, she experienced gastrointestinal symptoms with diarrhoea and vomiting approximately six hours post consumption. Over the ensuing days, the diarrhoea stopped, but the vomiting continued and she was unable to tolerate oral rehydration fluid. She presented to a peripheral hospital one week later with confusion and new onset generalized tonic clonic seizures. She was afebrile, appeared dehydrated and had lethargy, but normal limb strength on examination. Laboratory investigations were significant for severe hyponatraemia and an elevated creatine kinase. She was treated with phenytoin and received amoxicillin/clavulanic acid for aspiration pneumonia. The hyponatraemia worsened despite hydration and she was then transferred to the University Hospital of the West Indies (UHWI) for further management. On presentation to UHWI (two weeks after her initial illness), she was found to be euvolaemic. Her urine was also noted to be dark. She was fully oriented, but had impaired short term memory and mild proximal weakness at the hips bilaterally. Her neck was supple. Over the following week her hyponatraemia was corrected with fluid restriction and hypertonic saline. An endocrinology consultation was requested and the endocrinology team felt that her electrolyte disturbance was a case of idiopathic syndrome of inappropriate antidiuretic hormone (SIADH) secretion. While in hospital, approximately three weeks after the diarrhoeal illness, she developed quadriparesis which progressed to complete paralysis over approximately two weeks. She also developed bulbar muscle involvement with dysarthria and dysphagia and required a nasogastric tube for feeding. Stool for campylobacter was negative but was done two weeks after initial illness so this might have been too late to make the diagnosis. Lumbar puncture revealed no albuminocytologic dissociation. Serum creatine kinase was initially elevated but normalized during hospitalization (Table 1). Thyroid function tests were normal. Serology for leptospirosis, HIV, HTLV-1, Hepatitis B and C were negative. An extensive collagen vascular screen, urine protein electrophoresis, urine aminolevulinic acid (ALA) and serum heavy metal screen (arsenic, mercury, bismuth, and antimony) were negative. Computed tomography and magnetic resonance imaging of the brain (Figs. 1A C) and cervical spine, including diffusion weighted image one month after she became quadriparetic, were negative for compressive lesions of the spinal cord or features of osmotic demyelination. Muscle biopsy of her thigh displayed severe atrophy with no perifasicular infil-trates or vacuoles or regeneration. Table 1 presents a sum-mary of laboratory results during hospitalization. Electromyography revealed moderate to abundant positive sharp waves and fibrillation potentials with absent fasciculation potentials and no voluntary motor unit action potentials (MUAP) in all muscles sampled. Nerve conduction studies revealed unelicitable F responses, compound muscle action potentials (CMAPs) and sensory nerve action potentials (SNAPs) at all peripheral (radial, median, ulnar, peroneal, tibial and sural) nerve stimulation sites tested. Findings on nerve conduction study (Figs. 2A C) were in keeping with an acute demyelinating and axonal sensorimotor illness.
3 Acute Motor-sensory Axonal Neuropathy in Jamaica 660 Table 1: Results of laboratory investigations Test Day #1 Day #3 Day #5 Day #6 Day #14 Day #20 Haemoglobin (mg/dl) Packed cell volume Platelet count (x 10 9 /Fl) White blood cell count (x10 9 /L) Sodium (mmol/l) Potassium (mmol/l) Chloride (mmol/l) Bicarbonate (mmol/l) Urea (mmol/l) Creatinine (ummol/l) Creatine phosphokinase (U/L) Erythrocyte sedimentation rate (mm/hr) 95 B Fig. 1A C: Magnetic resonance imaging of the brain one month after the patient became quadriparetic. CASE MANAGEMENT Initial supportive care included physical therapy, swallowing rehabilitation, prevention of decubitus ulcers via cushions and frequent turning in bed and bladder training. With the initial marked elevation of the creatine kinase levels, the possibility of a myopathy was entertained and pulse methyl prednisolone was administered at a dose of one gram per day for seven days but no improvement was noted. Four months after the onset of her illness, she was treated with a course of intravenous immunoglobulin 0.4 g/kg for five days. The late timing of this was based on financial constraints in procuring the nerve conduction studies.
4 661 Fletcher-Peddie et al Fig. 1D F: Cervical magnetic resonance imaging 10 weeks after initial diarrhoeal illness. Over the course of her hospitalization, there was mild improvement with swallowing capacity returning to almost normal and improved bowel and bladder function. She also had some improvement in motor function with her proximal muscle strength improving to grade 2/5 on the Medical Research Council (MRC) scale. Antiepileptic medications were started after her initial presentation with seizures. After the correction of her electrolyte abnormalities, these were tapered and then discontinued. She started rehabilitative physiotherapy and was discharged for home after 90 days in hospital. Approximately one week after discharge, the patient returned with recurrent seizures on a background of normal electrolytes and a urinary tract infection, confirmed by a positive urine culture. During this admission, she developed aspiration pneumonia and succumbed to her illness.
5 Acute Motor-sensory Axonal Neuropathy in Jamaica 662 Fig. 2A: Findings on nerve conduction studies.
6 663 Fletcher-Peddie et al Fig. 2B: Findings on nerve conduction studies.
7 Acute Motor-sensory Axonal Neuropathy in Jamaica 664 Fig. 2C: Electromyography.
8 665 Fletcher-Peddie et al Table 2: Neurophysiological criteria for AIDP, AMSAN and AMAN* AIDP Acute Inflammatory Demyelinating Polyneuropathy At least one of the following in each of at least two nerves, or at least two of the following in one nerve if all others inexcitable and dcmap > 10% LLN: Motor conduction velocity < 90% LLN (85% if dcmap <5 0% LLN) Distal motor latency >110% ULN (> 120% if dcmap < 100% LLN) pcmap/dcmap ratio < 0 5 and dcmap > 20% LLN F-response latency > 120% ULN AMSAN* Acute Motor-sensory Axonal Neuropathy None of the features of AIDP except one demyelinating feature allowed in one nerve if dcmap < 10% LLN Sensory action potential amplitudes < LLN AMAN* Acute Motor Axonal Neuropathy None of the features of AIDP except one demyelinating feature allowed in one nerve if dcmap < 10% LLN Sensory action potential amplitudes normal Inexcitable dcmap absent in all nerves or present in only one nerve with dcmap < 10% LLN dcmap = compound muscle action potential amplitude after distal stimulation; pcmap = compound muscle action potential amplitude after proximal stimulation; LLN = lower limit of normal; ULN = upper limit of normal. *In the original definitions the difference between AMSAN and AMAN proposed here is implied but not stipulated. *Source: 12 DISCUSSION Guillain-Barré syndrome is an acute polyneuropathy with various subtypes. Acute inflammatory demyelinating polyradiculoneuropathy, the classic demyelinating form of GBS, accounts for 90% of all GBS cases in the Western world. Acute motor axonal neuropathy and AMSAN are axonal forms of GBS that are more prevalent in Asia, South and Central America and often preceded by Campylobacter jejuni (C jejuni) infection, as proven by serological studies (7). The present case, as previously mentioned, had stool culture done late as the results of stool cultures usually do not remain positive beyond two weeks (6). More specific methods such as real time polymerase chain reaction (RT- PCR) and enzyme-linked immunosorbent assay (ELISA) techniques for campylobacter species are not offered at the University Hospital of the West Indies. While immunologic evidence is strongest for antecedent C jejuni infection, other infectious agents have been temporally associated with subsequent GBS and have included influenza viruses, Mycoplasma pneumoniae, human immunodeficiency virus, Epstein-Barr virus and cytomegalovirus (9). In rare cases, haematological malignancies (10) may also be linked to GBS. The relationship between vaccinations and GBS is not thought to be directly casual (5). Although host genetic or other phenotypic factors are likely to influence susceptibility to development of GBS in certain individuals, an association with specific HLA subtypes or other immunogenetic susceptibility factors has not been consistently identified by existing studies. Our literature review did not reveal any reports of an association of ethnicity with these HLA subtypes. The association between HLA-DR and -DQ and GBS is not strong, but some studies have found that polymorphisms of CD1E and CD1A genes may be linked to occurrence of GBS (11). The electrophysiologic evaluation of a suspected case of GBS remains a key extension of the clinical examination. Standard parameters of the motor nerve include the distal motor latencies, CMAP amplitudes, conduction velocities, waveform duration and morphology and F waves. Sensory nerve action potentials is the electrophysiologic correlate for the sensory nerve. The findings may be quite variable and beyond the nuances of GBS variants, and are often a function of the time during the disease course that the patient is evaluated. The hallmark of the classic GBS variant of AIDP rests in the basic pathophysiology of demyelination with occasional or variable secondary axonal degeneration. These patients exhibit prolonged distal latencies, slow conduction velocities, temporal dispersion, conduction block and prolonged F waves. At least three motor and sensory nerves with multi-site stimulation F waves and bilateral tibial H reflexes should be assessed on nerve conduction testing. Hughes and Cornblath outlined the electrophysiologic classification of GBS (12) [Table 2]. In that criterion, at least one of the defined markers of demyelination should be observed in each of at least two nerves. The entity of conduction block represents loss of myelin with neural conduction failure, which may lead to acute weakness and sensory loss. It is embodied in > 20% reduction in baseline to peak CMAP from proximal to distal stimulation sites. Conduction block may be seen in 74% of patients with AIDP within the first two weeks of their disease course. Approximately 40 60% of AIDP patients eventually demonstrate SNAP amplitude reduction or absence by the third or fourth week of the illness. This may be attributable to conduction block or secondary axonal degeneration (13).
9 Acute Motor-sensory Axonal Neuropathy in Jamaica 666 The variant AMSAN shows no electrophysiologic evidence of demyelination, instead exhibiting an axonal pattern of reduced or absent peak to baseline amplitude in sensory and motor with relatively preserved conduction velocity in excitable nerves. Nerve conduction studies in AMSAN reveal markedly diminished amplitudes or absent CMAP within 7 10 days of onset of the illness. Sensory nerve action potentials are also profoundly reduced or absent. Low amplitude or absent CMAPs do not necessarily imply axonal degeneration. Distal conduction block can account for distal reduced or absent CMAPs. In fact, it may be impossible to distinguish AIDP and AMSAN initially, purely on nerve conduction studies (14). The index case would have benefitted from serial nerve conduction studies to formally distinguish AIDP with secondary axonal loss from AMSAN, but her poor outcome leads one to clinically assume the latter diagnosis of AMSAN. The efficacy of plasmapheresis and intravenous immunoglobulin has been established in large international randomized trials and case reports, with corticosteroids proven ineffective (15). Despite reported improvement with immunoglobulin therapy (16), the prognosis and recovery of AMSAN is generally poorer than the other subtypes and the main stay of treatment is supportive care (17). This entails prompt diagnosis based on history and examination. One must address issues of swallowing, aspiration, ventilation, decubitus ulcers, limb physiotherapy, autonomic dysfunction, bladder and bowel care, analgesia, deep vein thrombosis prophylaxis, and education of involved family members and the patient. Poor prognostic factors include older age, rapid onset (less than seven days) prior to presentation, severe muscle weakness on admission, need for ventilatory support, an average distal motor response amplitude reduction to < 20% of normal, and preceding diarrhoeal illness (18). As realized from this case, the cause of demise in this illness may be related to the sequelae of complications. Supportive and rehabilitative care is of paramount importance. We acknowledge that several questions remain unanswered in this complicated case. The aetiology of her hyponatraemia might have been initially dehydration related to vomiting, but the persistence even in her euvolaemic state leads one to believe she may have had SIADH. This hyponatraemia may have led to her seizures. We are unsure of the cause of her dark urine. The elevation of her CPK makes this likely myoglobinuria, but confirmatory test were unavailable. The absence of cytoalbuminologic dissociation on her CSF does not exclude the diagnosis of GBS. The normalization of her CPK was also on the background of hydration and steroid use before the late timing of her muscle biopsy. One may wonder if the muscle atrophy may still represent an underlying chronic myopathy. Again, the axonal loss may indicate another differential of AIDP with secondary axonal loss but her poor outcome supports AMSAN. This case illustrates the need for complete evaluation with appropriate diagnostic tests in patients who present with an unclear diagnosis or experience an unexpected complication while in hospital. Working through the various differentials including osmotic demyelination, acute myopathy and GBS required investigations along disparate lines and as such delayed the diagnosis. Difficulty in obtaining the required investigations in our resource-limited setting also contributed to the delay in diagnosis. The final diagnosis serves as a reminder that GBS is now the most common cause of acute flaccid paralysis and should be considered early in all patients presenting with flaccid quadriparesis. REFERENCES 1. Prineas JW. Pathology of the Guillain Barre Syndrome. Ann Neurol 1981; 9: Seneviratne U. Guillain-Barré syndrome. Postgrad Med J 2000; 76: Yuki N, Hartung H. Review article: medical progress in Guillain Barre Syndrome. N Engl J Med 2012; 366: National Institute of Neurological Disorders and Stroke. NINDS Guillain-Barré syndrome information page. National Institute of Neurological Disorders and Stroke; Available from: disorders/gbs/gbs.htm 5. Sejvar J, Kohl K, Gidudu J, Amato A, Bakshi N, Baxter R et al. Guillain-Barré syndrome and Fisher syndrome: case definitions and guidelines for collection, analysis, and presentation of immunization safety data. Vaccine 2011; 29: Bloom S, Webster G, Marks D. Oxford Handbook of Gastroenterology and Hepatology. First edition. Oxford: Oxford University Press; Vucic S, Kiernan MC, Cornblath DR. Guillain-Barré syndrome: an update. J Clin Neurosci 2009; 16: Bessède E, Delcamp A, Sifré E, Buissonnière A, Mégraud F. New methods for detection of campylobacters in stool samples in comparison to culture. J Clin Microbiol 2011; 49: Tam CC, O Brien SJ, Rodrigues LC. Influenza, campylobacter and mycoplasma infections, and hospital admissions for Guillain Barre syndrome, England. Emerg Infect Dis 2006; 12: Wanschitz J, Dichtl W, Budka H, Loscher WN, Boesch S. Acute motor and sensory axonal neuropathy in Burkitt-like lymphoma. Muscle Nerve 2006; 34: Zhong M, Cai F. Current perspectives on Guillian-Barre Syndrome. World J Pediatric 2007; 3: Hughes RA, Cornblath DR. Guillain Barre Syndrome. Lancet 2005; 366: Haddden RD, Cornblath DR, Hughes RA, Zielasek J, Hartung HP, Toyka KV et al. Electrophysiological classification of Guillain Barre Syndrome: clinical associations and outcomes. Plasma Exchange/ Sandoglobin: Guillain-Barré Syndrome Trial Group. Ann Neurol 1998; 44: Van Den Bergh PY, Pieret F. Electrodiagnostic criteria for acute and chronic inflammatory demyelinating polyradiculopathy. Muscle Nerve 2004; 29: Rostásy KM, Huppke P, Beckers B, Brockmann K, Degenhardt V, Wesche B et al. Acute motor and sensory axonal neuropathy (AMSAN) in a 15-year-old boy presenting with severe pain and distal muscle weakness. Neuropediatrics 2005; 36: Hughes RA, Wijdicks EF, Benson E, Cornblath DR, Hahn AF, Meythaler JM et al. Supportive care for patients with Guillain-Barré syndrome. Arch Neurol 2005; 62: Rees JH, Soudain SE, Gregson NA, Hughes RA. Campylobacter jejuni infection and Guillain-Barré syndrome. N Engl J Med 1995; 333: Walgaard C, Lingsma HF, Ruts L, van Doorn PA, Steyerberg EW, Jacobs BC. Early recognition of poor prognosis in Guillain-Barre syndrome. Neurology 2011; 76: 968.
Supplementary Online Content
 Supplementary Online Content Stevens O, Claeys KG, Poesen K, Veroniek S, Van Damme P. Diagnostic challenges and clinical characteristics of hepatitis E virus associated Guillain- Barré syndrome. JAMA Neurol.
Supplementary Online Content Stevens O, Claeys KG, Poesen K, Veroniek S, Van Damme P. Diagnostic challenges and clinical characteristics of hepatitis E virus associated Guillain- Barré syndrome. JAMA Neurol.
Guillain-Barré Syndrome
 Guillain-Barré Syndrome Ouch! www.philippelefevre.com Guillain-Barré Syndrome Acute post-infective polyneuropathy Heterogeneous condition with several variant forms Lipid A Neuronal Ganglioside Pathogenesis
Guillain-Barré Syndrome Ouch! www.philippelefevre.com Guillain-Barré Syndrome Acute post-infective polyneuropathy Heterogeneous condition with several variant forms Lipid A Neuronal Ganglioside Pathogenesis
The Role of Cytomegalovirus, Haemophilus Influenzae and Epstein Barr Virus in Guillain Barre Syndrome
 ORIGINAL REPORT The Role of Cytomegalovirus, Haemophilus Influenzae and Epstein Barr Virus in Guillain Barre Syndrome Shahriar Nafissi 1, Zahra Vahabi 1, Maryam Sadeghi Ghahar 2, Ali Akbar Amirzargar 2,
ORIGINAL REPORT The Role of Cytomegalovirus, Haemophilus Influenzae and Epstein Barr Virus in Guillain Barre Syndrome Shahriar Nafissi 1, Zahra Vahabi 1, Maryam Sadeghi Ghahar 2, Ali Akbar Amirzargar 2,
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Clinical and electrophysiologic features of childhood Guillain-Barré syndrome in Northeast China
 Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
International Journal of Basic & Applied Physiology
 ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
Immunopathology of Guillain- Barré syndrome. L. Magy Service de Neurologie Centre de Référence 'Neuropathies Périphériques Rares' CHU Limoges, France
 Immunopathology of Guillain- Barré syndrome L. Magy Service de Neurologie Centre de Référence 'Neuropathies Périphériques Rares' CHU Limoges, France What is Guillain-Barré syndrome? An immune-mediated
Immunopathology of Guillain- Barré syndrome L. Magy Service de Neurologie Centre de Référence 'Neuropathies Périphériques Rares' CHU Limoges, France What is Guillain-Barré syndrome? An immune-mediated
Prediction of Functional Outcome in Axonal Guillain-Barre Syndrome Eun Jung Sung, MD, Dae Yul Kim, MD, Min Cheol Chang, MD, Eun Jae Ko, MD
 Original Article Ann Rehabil Med 2016;40(3):481-488 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.3.481 Annals of Rehabilitation Medicine Prediction of Functional Outcome in Axonal
Original Article Ann Rehabil Med 2016;40(3):481-488 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.3.481 Annals of Rehabilitation Medicine Prediction of Functional Outcome in Axonal
Immune Mediated Neuropathies
 Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Risk Factors of Respiratory Failure in Children with Guillain-Barré Syndrome
 Pediatrics and Neonatology (2012) 53, 295e299 Available online at www.sciencedirect.com journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Risk Factors of Respiratory Failure in Children
Pediatrics and Neonatology (2012) 53, 295e299 Available online at www.sciencedirect.com journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Risk Factors of Respiratory Failure in Children
Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome
 Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Electrophysiology in the Guillain-Barré Syndrome: Study of 30 Cases
 Journal of Bangladesh College of Physicians and Surgeons Vol. 24, No. 2, May 2006 Electrophysiology in the Guillain-Barré Syndrome: Study of 30 Cases NC KUNDU Summary: Thirty consecutive patients diagnosed
Journal of Bangladesh College of Physicians and Surgeons Vol. 24, No. 2, May 2006 Electrophysiology in the Guillain-Barré Syndrome: Study of 30 Cases NC KUNDU Summary: Thirty consecutive patients diagnosed
Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype Five Years after Initial Diagnosis
 Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
Miller Fisher Syndrome A variant of Guillan Barré Syndrome. Sarah I. Sheikh, BM BCh, MRCP
 Miller Fisher Syndrome A variant of Guillan Barré Syndrome Sarah I. Sheikh, BM BCh, MRCP History of GBS 1859 Jean Baptiste Octave Landry de Thézillat (1826-1865) published his observation on ascending
Miller Fisher Syndrome A variant of Guillan Barré Syndrome Sarah I. Sheikh, BM BCh, MRCP History of GBS 1859 Jean Baptiste Octave Landry de Thézillat (1826-1865) published his observation on ascending
Neuromuscular Respiratory Failure in Guillain-Barre Syndrome: Evaluation of Clinical and Electrodiagnostic Predictors
 Original Article Neuromuscular Respiratory Failure in Guillain-Barre Syndrome: Evaluation of Clinical and Electrodiagnostic Predictors Uma Sundar, Elizabeth Abraham, A Gharat, ME Yeolekar, Trupti Trivedi,
Original Article Neuromuscular Respiratory Failure in Guillain-Barre Syndrome: Evaluation of Clinical and Electrodiagnostic Predictors Uma Sundar, Elizabeth Abraham, A Gharat, ME Yeolekar, Trupti Trivedi,
Changes in the severity and subtype of Guillain-Barré syndrome admitted to a specialist Neuromedical ICU over a 25 year period
 J Neurol (2017) 264:564 569 DOI 10.1007/s00415-016-8380-0 ORIGINAL COMMUNICATION Changes in the severity and subtype of Guillain-Barré syndrome admitted to a specialist Neuromedical ICU over a 25 year
J Neurol (2017) 264:564 569 DOI 10.1007/s00415-016-8380-0 ORIGINAL COMMUNICATION Changes in the severity and subtype of Guillain-Barré syndrome admitted to a specialist Neuromedical ICU over a 25 year
Guillain-Barré syndrome and related disorders
 Guillain-Barré syndrome and related disorders Dr Benjamin Wakerley Department of Neurology Gloucestershire Royal Hospital Disclosures Novartis - educational grant Guillain-Barré syndrome and related disorders
Guillain-Barré syndrome and related disorders Dr Benjamin Wakerley Department of Neurology Gloucestershire Royal Hospital Disclosures Novartis - educational grant Guillain-Barré syndrome and related disorders
Dysphagia as initial manifestation of Guillan-Barrè Syndrome in a child Elda Pitrolo, Simona Santucci, Chiara Cuzzupè, Filippo De Luca
 Clinical Case Seminar A7(1-5 ) Dysphagia as initial manifestation of Guillan-Barrè Syndrome in a child Elda Pitrolo, Simona Santucci, Chiara Cuzzupè, Filippo De Luca Department of Human Pathology of Adulthood
Clinical Case Seminar A7(1-5 ) Dysphagia as initial manifestation of Guillan-Barrè Syndrome in a child Elda Pitrolo, Simona Santucci, Chiara Cuzzupè, Filippo De Luca Department of Human Pathology of Adulthood
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
LE SYNDROME DE GUILLAIN-BARRE
 FORMATION UNIVERSITAIRE SPECIFIQUE (FUS) Enseignement interuniversitaire MASTER DE SPECIALISATION EN MEDECINE INTERNE Samedi 19 dećembre 2015 Institute of Neurosciences LE SYNDROME DE GUILLAIN-BARRE Peter
FORMATION UNIVERSITAIRE SPECIFIQUE (FUS) Enseignement interuniversitaire MASTER DE SPECIALISATION EN MEDECINE INTERNE Samedi 19 dećembre 2015 Institute of Neurosciences LE SYNDROME DE GUILLAIN-BARRE Peter
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Paraparetic Guillain-Barré syndrome
 Paraparetic Guillain-Barré syndrome Bianca van den Berg, MD Christiaan Fokke, MD Judith Drenthen, MD Pieter A. van Doorn, MD, PhD Bart C. Jacobs, MD, PhD Correspondence to Dr. Jacobs: b.jacobs@erasmusmc.nl
Paraparetic Guillain-Barré syndrome Bianca van den Berg, MD Christiaan Fokke, MD Judith Drenthen, MD Pieter A. van Doorn, MD, PhD Bart C. Jacobs, MD, PhD Correspondence to Dr. Jacobs: b.jacobs@erasmusmc.nl
Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients
 Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients Shereen Zakarya Department of Neurology, Mansoura University ABSTRACT Objective: To study the clinical
Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients Shereen Zakarya Department of Neurology, Mansoura University ABSTRACT Objective: To study the clinical
Association of Campylobacter jejuni infection and Guillain- Barré syndrome: a cohort study in the northwest of Iran
 The Turkish Journal of Pediatrics 2008; 50: 443-448 Original Association of Campylobacter jejuni infection and Guillain- Barré syndrome: a cohort study in the northwest of Iran Mohammad Barzegar 1, Asghar
The Turkish Journal of Pediatrics 2008; 50: 443-448 Original Association of Campylobacter jejuni infection and Guillain- Barré syndrome: a cohort study in the northwest of Iran Mohammad Barzegar 1, Asghar
Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
 doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
Peripheral Neuropathies
 Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
ALBUMINOCYTOLOGICAL DISSOCIATION IN DIFFERENT ELECTROPHYSIOLOGICAL GBS VARIANTS
 O R I G I N A L A R T I C L E ALBUMINOCYTOLOGICAL DISSOCIATION IN DIFFERENT ELECTROPHYSIOLOGICAL GBS VARIANTS Ali ZohairNomani, Mansoor Iqbal, Haris Majid Rajput, Mazhar Badshah, Sumaira Nabi, Zakir Jan,
O R I G I N A L A R T I C L E ALBUMINOCYTOLOGICAL DISSOCIATION IN DIFFERENT ELECTROPHYSIOLOGICAL GBS VARIANTS Ali ZohairNomani, Mansoor Iqbal, Haris Majid Rajput, Mazhar Badshah, Sumaira Nabi, Zakir Jan,
A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging
 61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
A descriptive study of patients with Guillain-Barré syndrome: Experience from an Australian tertiary level hospital
 A descriptive study of patients with Guillain-Barré syndrome: Experience from an Australian tertiary level hospital Emma Foster 1, Luke Bonavia 1, Ashwin Subramaniam 2-4, Cameron Green 1, Ernest Butler
A descriptive study of patients with Guillain-Barré syndrome: Experience from an Australian tertiary level hospital Emma Foster 1, Luke Bonavia 1, Ashwin Subramaniam 2-4, Cameron Green 1, Ernest Butler
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Diagnosis of Guillain Barré syndrome in children and validation of the Brighton criteria
 J Neurol (2017) 264:856 861 DOI 10.1007/s00415-017-8429-8 ORIGINAL COMMUNICATION Diagnosis of Guillain Barré syndrome in children and validation of the Brighton criteria Joyce Roodbol 1,2 Marie-Claire
J Neurol (2017) 264:856 861 DOI 10.1007/s00415-017-8429-8 ORIGINAL COMMUNICATION Diagnosis of Guillain Barré syndrome in children and validation of the Brighton criteria Joyce Roodbol 1,2 Marie-Claire
Hyperreflexia in Guillain-Barré syndrome: relation with acute motor axonal neuropathy and anti-gm1 antibody
 18 Department of Neurology, Chiba University School of Medicine, Chiba, Japan S Kuwabara K Ogawara M Mori T Hattori Department of Neurology, Dokkyo University School of Medicine, Tochigi, Japan M Koga
18 Department of Neurology, Chiba University School of Medicine, Chiba, Japan S Kuwabara K Ogawara M Mori T Hattori Department of Neurology, Dokkyo University School of Medicine, Tochigi, Japan M Koga
Guillain-Barré Syndrome
 Guillain-Barré Syndrome A Laboratory Perspective Laura Dunn Biomedical Scientist (Trainee Healthcare Scientist) Diagnosis of GBS GBS is generally diagnosed on clinical grounds Basic laboratory studies
Guillain-Barré Syndrome A Laboratory Perspective Laura Dunn Biomedical Scientist (Trainee Healthcare Scientist) Diagnosis of GBS GBS is generally diagnosed on clinical grounds Basic laboratory studies
Detection of Autoantibodies against Gangliosides in Guillain-Barré Syndrome
 ISSN 1735-1383 Iran. J. Immunol. September 2010, 7 (3), 198-201 Hong-Liang Zhang, Su-Jie Gao, Yi Yang, Jiang Wu Detection of Autoantibodies against Gangliosides in Guillain-Barré Syndrome Article Type:
ISSN 1735-1383 Iran. J. Immunol. September 2010, 7 (3), 198-201 Hong-Liang Zhang, Su-Jie Gao, Yi Yang, Jiang Wu Detection of Autoantibodies against Gangliosides in Guillain-Barré Syndrome Article Type:
A comparison between plasmapheresis and intravenous immunoglobulin in children with Guillain Barré syndrome in Upper Egypt
 610471TAN0010.1177/1756285615610471Therapeutic Advances in Neurological DisordersK. Saad research-article2015 Therapeutic Advances in Neurological Disorders Original Research A comparison between plasmapheresis
610471TAN0010.1177/1756285615610471Therapeutic Advances in Neurological DisordersK. Saad research-article2015 Therapeutic Advances in Neurological Disorders Original Research A comparison between plasmapheresis
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment
 Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients
 Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients Chilvana Patel*, Surya Murthy Vishnubhakat**
Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients Chilvana Patel*, Surya Murthy Vishnubhakat**
Diagnosis and Management of Immune-mediated Neuropathies
 Continuing Medical Education 39 Diagnosis and Management of Immune-mediated Neuropathies Sung-Tsang Hsieh Abstract- Immune-mediate neuropathies, or inflammatory neuropathies are neuropathies due to the
Continuing Medical Education 39 Diagnosis and Management of Immune-mediated Neuropathies Sung-Tsang Hsieh Abstract- Immune-mediate neuropathies, or inflammatory neuropathies are neuropathies due to the
GUILLAIN-BARRE SYNDROME
 GUILLAIN-BARRE SYNDROME tarek.sharshar@rpc.aphp.fr University of Versailles Saint-Quentin en Yvelines Raymond Poincaré Teaching Hospital Garches - France STATEMENTS 1. Guillain-Barré Syndrome (GBS) is
GUILLAIN-BARRE SYNDROME tarek.sharshar@rpc.aphp.fr University of Versailles Saint-Quentin en Yvelines Raymond Poincaré Teaching Hospital Garches - France STATEMENTS 1. Guillain-Barré Syndrome (GBS) is
Guillain-Barré Syndrome: Natural history and prognostic factors: a retrospective review of 106 cases
 González-Suárez et al. BMC Neurology 2013, 13:95 RESEARCH ARTICLE Open Access Guillain-Barré Syndrome: Natural history and prognostic factors: a retrospective review of 106 cases Inés González-Suárez *,
González-Suárez et al. BMC Neurology 2013, 13:95 RESEARCH ARTICLE Open Access Guillain-Barré Syndrome: Natural history and prognostic factors: a retrospective review of 106 cases Inés González-Suárez *,
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Guillain-Barré syndrome and related disorders
 Guillain-Barré syndrome and related disorders Artículo Amato AA RESUMEN En 1859, Landry describió una neuropatía caracterizada por parálisis severa ascendente. Posteriormente, Guillain, Barré y Strohl
Guillain-Barré syndrome and related disorders Artículo Amato AA RESUMEN En 1859, Landry describió una neuropatía caracterizada por parálisis severa ascendente. Posteriormente, Guillain, Barré y Strohl
Evaluation of Peripheral Neuropathy. Evaluation of Peripheral Neuropathy - Introduction
 Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
The clinical spectrum of Malaysian patients with. Chronic inflammatory demyelinating polyneuropathy
 Neurology Asia 2004; 9 : 39 45 The clinical spectrum of Malaysian patients with chronic inflammatory demyelinating polyneuropathy Khean Jin GOH, Wai Keong NG, Nee Kong CHEW, Chong Tin TAN Division of Neurology,
Neurology Asia 2004; 9 : 39 45 The clinical spectrum of Malaysian patients with chronic inflammatory demyelinating polyneuropathy Khean Jin GOH, Wai Keong NG, Nee Kong CHEW, Chong Tin TAN Division of Neurology,
5.1 Alex.
 5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW
 Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Patogenesi e terapia della Neuropatia Motoria Multifocale
 26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
Guillain - Barre Syndrome - is an acute frequently severe and
 12 JAPI march 2013 VOL. 61 Original Article Clinical Profile of Guillain Barre Syndrome Shubhangi Vithal Dhadke 1, Vithal Narayan Dhadke 2, Sachin S Bangar 1, Milind B Korade 3 Abstract Objectives: To
12 JAPI march 2013 VOL. 61 Original Article Clinical Profile of Guillain Barre Syndrome Shubhangi Vithal Dhadke 1, Vithal Narayan Dhadke 2, Sachin S Bangar 1, Milind B Korade 3 Abstract Objectives: To
SEMESTER Suriname study. The Suriname Meningo- encephalitis Study (SMS) Introduction. SMS- protocol version 3.4. Principal investigators:
 SEMESTER Suriname study The Suriname Meningo- encephalitis Study (SMS) Principal investigators: E.C.M. van Gorp 1,2 and S. Vreden 3 Participating investigators: H. Alberga 4, M. Baptista 5, R. Cruden 4,
SEMESTER Suriname study The Suriname Meningo- encephalitis Study (SMS) Principal investigators: E.C.M. van Gorp 1,2 and S. Vreden 3 Participating investigators: H. Alberga 4, M. Baptista 5, R. Cruden 4,
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Guillain-Barré Syndrome in a Patient with Pneumococcal Meningitis
 Guillain-Barré Syndrome in a Patient with Pneumococcal Meningitis An Uncommon Complication of a Common Infection ACP Wisconsin, September 2017 Jesse Maupin, MD (PGY-2) University of Wisconsin Hospital
Guillain-Barré Syndrome in a Patient with Pneumococcal Meningitis An Uncommon Complication of a Common Infection ACP Wisconsin, September 2017 Jesse Maupin, MD (PGY-2) University of Wisconsin Hospital
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Correlative study between C-reactive protein, clinical severity, and nerve conduction studies in Guillain-Barrè syndrome
 Altaweel et al. The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2018) 54:4 https://doi.org/10.1186/s41983-018-0006-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Altaweel et al. The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2018) 54:4 https://doi.org/10.1186/s41983-018-0006-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
MOTOR NEURONE DISEASE
 MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
Infection-Associated Neurological Syndromes
 Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
Validity of Neurophysiological Study Inprediction of Severity of Guillain-Barre Syndrome and the Indication for Mechanical Ventilation
 IOSR Journal Of Pharmacy And Biological Sciences (IOSR-JPBS) e-issn:2278-3008, p-issn:2319-7676. Volume 14, Issue 1 Ser. II (Jan Feb 2019), PP 43-47 www.iosrjournals.org Validity of Neurophysiological
IOSR Journal Of Pharmacy And Biological Sciences (IOSR-JPBS) e-issn:2278-3008, p-issn:2319-7676. Volume 14, Issue 1 Ser. II (Jan Feb 2019), PP 43-47 www.iosrjournals.org Validity of Neurophysiological
1/22/2019. Nerve conduction studies. Learning objectives: Jeffrey Allen MD University of Minnesota Minneapolis, MN
 Jeffrey Allen MD University of Minnesota Minneapolis, MN February 9, 2019 Learning objectives: Describe electrophysiologic features of peripheral nerve demyelination Identify electrophysiology findings
Jeffrey Allen MD University of Minnesota Minneapolis, MN February 9, 2019 Learning objectives: Describe electrophysiologic features of peripheral nerve demyelination Identify electrophysiology findings
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment
 Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Guillain Barre Syndrome: A clinical observational study in Indian paediatric patients
 Guillain Barre Syndrome: A clinical observational study in Indian paediatric patients *Shikha Swaroop 1, Bakul B Javadekar 2 Sri Lanka Journal of Child Health, 2017; 46(3): 238-242 Abstract Background:
Guillain Barre Syndrome: A clinical observational study in Indian paediatric patients *Shikha Swaroop 1, Bakul B Javadekar 2 Sri Lanka Journal of Child Health, 2017; 46(3): 238-242 Abstract Background:
From the Department of Neurology, University Hospital Birmingham, Birmingham, UK
 Q J Med 2002; 95:717 721 Review QJM Treatment of Guillain-Barré syndrome J.B. WINER From the Department of Neurology, University Hospital Birmingham, Birmingham, UK Introduction Although there are earlier
Q J Med 2002; 95:717 721 Review QJM Treatment of Guillain-Barré syndrome J.B. WINER From the Department of Neurology, University Hospital Birmingham, Birmingham, UK Introduction Although there are earlier
CNS third year med students Summary of midterm material H Awad
 CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
Muscle Wasting & Weakness in Critical Illness
 Muscle Wasting & Weakness in Critical Illness Clin A/Prof Michael O Leary Intensive Care Service Royal Prince Alfred Hospital, Sydney Sydney Medical School, The University of Sydney Disclosures I have
Muscle Wasting & Weakness in Critical Illness Clin A/Prof Michael O Leary Intensive Care Service Royal Prince Alfred Hospital, Sydney Sydney Medical School, The University of Sydney Disclosures I have
AII-type: Select the most appropriate answer
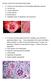 AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
Guillain-Barre Syndrome and its Prognosis with Hyponatremia
 Original Article RUHS Journal of Health Sciences, Volume 2 Number 4, October -December 2017 Guillain-Barre Syndrome and its Prognosis with Hyponatremia Jerin Romeol, Hemant Mahur2, D P Singh3, Nitesh Pansari4,
Original Article RUHS Journal of Health Sciences, Volume 2 Number 4, October -December 2017 Guillain-Barre Syndrome and its Prognosis with Hyponatremia Jerin Romeol, Hemant Mahur2, D P Singh3, Nitesh Pansari4,
Update: Plasmapheresis in Neurologic Disorders
 Update: Plasmapheresis in Neurologic Disorders Case Presentation A 62-year-old, right-hand-dominant male presented to the emergency department with a 3-day history of progressive weakness. Initially he
Update: Plasmapheresis in Neurologic Disorders Case Presentation A 62-year-old, right-hand-dominant male presented to the emergency department with a 3-day history of progressive weakness. Initially he
Three cases of acute distal demyelinating neuropathy with recovery
 https://helda.helsinki.fi Three cases of acute distal demyelinating neuropathy with recovery Österlund-Tauriala, Emilia 2017 Österlund-Tauriala, E & Partanen, J V 2017, ' Three cases of acute distal demyelinating
https://helda.helsinki.fi Three cases of acute distal demyelinating neuropathy with recovery Österlund-Tauriala, Emilia 2017 Österlund-Tauriala, E & Partanen, J V 2017, ' Three cases of acute distal demyelinating
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
Guillain-Barré Syndrome Beth A. Rosen. DOI: /pir
 Guillain-Barré Syndrome Beth A. Rosen Pediatrics in Review 2012;33;164 DOI: 10.1542/pir.33-4-164 The online version of this article, along with updated information and services, is located on the World
Guillain-Barré Syndrome Beth A. Rosen Pediatrics in Review 2012;33;164 DOI: 10.1542/pir.33-4-164 The online version of this article, along with updated information and services, is located on the World
IN CONTRAST to the chronic distal
 ORIGINAL CONTRIBUTION Alcohol-Related Acute Axonal Polyneuropathy A Differential Diagnosis of Guillain-Barré Syndrome Johannes C. Wöhrle, MD; Konstantinos Spengos, MD; Wolfgang Steinke, MD; Hans H. Goebel,
ORIGINAL CONTRIBUTION Alcohol-Related Acute Axonal Polyneuropathy A Differential Diagnosis of Guillain-Barré Syndrome Johannes C. Wöhrle, MD; Konstantinos Spengos, MD; Wolfgang Steinke, MD; Hans H. Goebel,
Electrodiagnostic studies comprising of electromyography (EMG) and nerve
 INTRODUCTION AND TERMINOLOGY Electrodiagnostic studies comprising of electromyography (EMG) and nerve conduction studies (NCS) are well-established objective methods for the diagnosis, quantification and
INTRODUCTION AND TERMINOLOGY Electrodiagnostic studies comprising of electromyography (EMG) and nerve conduction studies (NCS) are well-established objective methods for the diagnosis, quantification and
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Treatment of multifocal motor neuropathy with interferon-β1a
 Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
EUROPEAN JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH GUILLAIN-BARRÉ SYNDROME (GBS): A REVIEW
 ejpmr, 2016,3(2), 366-371 EUROPEAN JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.ejpmr.com SJIF Impact Factor 2.026 Review Article ISSN 3294-3211 EJPMR GUILLAIN-BARRÉ SYNDROME (GBS): A REVIEW Hemal
ejpmr, 2016,3(2), 366-371 EUROPEAN JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.ejpmr.com SJIF Impact Factor 2.026 Review Article ISSN 3294-3211 EJPMR GUILLAIN-BARRÉ SYNDROME (GBS): A REVIEW Hemal
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
doi: /brain/awt285 Brain 2014: 137;
 doi:10.1093/brain/awt285 Brain 2014: 137; 33 43 33 BRAIN A JOURNAL OF NEUROLOGY Diagnosis of Guillain-Barré syndrome and validation of Brighton criteria Christiaan Fokke, 1,2,3,4 Bianca van den Berg, 1,5
doi:10.1093/brain/awt285 Brain 2014: 137; 33 43 33 BRAIN A JOURNAL OF NEUROLOGY Diagnosis of Guillain-Barré syndrome and validation of Brighton criteria Christiaan Fokke, 1,2,3,4 Bianca van den Berg, 1,5
Clinical Profile of Guillain Barre Syndrome-Observations from a Tertiary Care Hospital of Bangladesh
 Original Article Clinical Profile of Guillain Barre Syndrome-Observations from a Tertiary Care Hospital of Bangladesh Habib R a, Saifuddin M b, Islam R c, Rahman A d, Bhowmik NB e, Haque MA f Abstract
Original Article Clinical Profile of Guillain Barre Syndrome-Observations from a Tertiary Care Hospital of Bangladesh Habib R a, Saifuddin M b, Islam R c, Rahman A d, Bhowmik NB e, Haque MA f Abstract
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
Clinical electrophysiological characteristics and prognosis of acute motor axonal neuropathy in Uygur children of Xinjiang.
 Biomedical Research 2017; 28 (22): 9696-9700 ISSN 0970-938X www.biomedres.info Clinical electrophysiological characteristics and prognosis of acute motor axonal neuropathy in Uygur children of Xinjiang.
Biomedical Research 2017; 28 (22): 9696-9700 ISSN 0970-938X www.biomedres.info Clinical electrophysiological characteristics and prognosis of acute motor axonal neuropathy in Uygur children of Xinjiang.
Pitfalls in electrodiagnosis of Guillain-Barré syndrome subtypes
 Pitfalls in electrodiagnosis of Guillain-Barré syndrome subtypes Antonino Uncini, Claudia Manzoli, Francesca Notturno, Margherita Capasso To cite this version: Antonino Uncini, Claudia Manzoli, Francesca
Pitfalls in electrodiagnosis of Guillain-Barré syndrome subtypes Antonino Uncini, Claudia Manzoli, Francesca Notturno, Margherita Capasso To cite this version: Antonino Uncini, Claudia Manzoli, Francesca
The Neurology of HIV Infection. Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University
 The Neurology of HIV Infection Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University HIV/AIDS Epidemiology World-wide pandemic, 40 million affected U.S.- Disproportionate
The Neurology of HIV Infection Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University HIV/AIDS Epidemiology World-wide pandemic, 40 million affected U.S.- Disproportionate
Case Number 1 Guillain-Barré Syndrome (GBS)
 Case Number 1 Guillain-Barré Syndrome (GBS) Maria Angela Grima Reviewed by: Dr. Nicola Aquilina Case summary: Demographic details: Mr. JS, male, Gudja Referred from: GP A 57-year-old Caucasian gentleman
Case Number 1 Guillain-Barré Syndrome (GBS) Maria Angela Grima Reviewed by: Dr. Nicola Aquilina Case summary: Demographic details: Mr. JS, male, Gudja Referred from: GP A 57-year-old Caucasian gentleman
role of antiganglioside antibodies
 J Neurol Neurosurg Psychiatry 2000;68:191 195 191 Department of Neurology, Chiba University School of Medicine, 1 8 1 Inohana, Chuo-ku, Chiba 260 8670, Japan S Kuwabara K Ogawara K Mizobuchi M Mori T Hattori
J Neurol Neurosurg Psychiatry 2000;68:191 195 191 Department of Neurology, Chiba University School of Medicine, 1 8 1 Inohana, Chuo-ku, Chiba 260 8670, Japan S Kuwabara K Ogawara K Mizobuchi M Mori T Hattori
Table 1: Nerve Conduction Studies (summarised)
 Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Central nervous system
 Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Pedro A. Mendez-Tellez, MD
 Critical Illness Polyneuropathy and Myopathy: Epidemiology and Risk Factors Pedro A. Mendez-Tellez, MD Johns Hopkins University Baltimore, Maryland, USA pmendez@jhmi.edu Conflict of Interest I have no
Critical Illness Polyneuropathy and Myopathy: Epidemiology and Risk Factors Pedro A. Mendez-Tellez, MD Johns Hopkins University Baltimore, Maryland, USA pmendez@jhmi.edu Conflict of Interest I have no
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
ORIGINAL CONTRIBUTION. Continuous Spectrum of Pharyngeal-Cervical-Brachial Variant of Guillain-Barré Syndrome
 ORIGINAL CONTRIBUTION Continuous Spectrum of Pharyngeal-Cervical-Brachial Variant of Guillain-Barré Syndrome Takahide Nagashima, MD, PhD; Michiaki Koga, MD, PhD; Masaaki Odaka, MD, PhD; Koichi Hirata,
ORIGINAL CONTRIBUTION Continuous Spectrum of Pharyngeal-Cervical-Brachial Variant of Guillain-Barré Syndrome Takahide Nagashima, MD, PhD; Michiaki Koga, MD, PhD; Masaaki Odaka, MD, PhD; Koichi Hirata,
Original Paper. Iran J Neurol 2014; 13(1): 7-12
 Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(1): 7-12 Correlations between cytomegalovirus, Epstein-Barr virus, anti-ganglioside antibodies, electrodiagnostic findings and functional
Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(1): 7-12 Correlations between cytomegalovirus, Epstein-Barr virus, anti-ganglioside antibodies, electrodiagnostic findings and functional
IVIG (intravenous immunoglobulin) Bivigam, Carimune NF, Flebogamma, Gammagard, Gammagard S/D, Gammaked, Gammaplex, Gamunex-C, Octagam, Privigen
 Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Seminar. Guillain-Barré syndrome
 Guillain-Barré syndrome Hugh J Willison, Bart C Jacobs, Pieter A van Doorn Guillain-Barré syndrome is the most common and most severe acute paralytic neuropathy, with about 100 000 people developing the
Guillain-Barré syndrome Hugh J Willison, Bart C Jacobs, Pieter A van Doorn Guillain-Barré syndrome is the most common and most severe acute paralytic neuropathy, with about 100 000 people developing the
Current treatment in Guillain-Barré Syndrome and myasthenia gravis
 4 rd Congress of the European Academy of Neurology Lisbon, Portugal, June 16-19, 2018 Teaching Course 10 Current treatments in neurology Level 1 Current treatment in Guillain-Barré Syndrome and myasthenia
4 rd Congress of the European Academy of Neurology Lisbon, Portugal, June 16-19, 2018 Teaching Course 10 Current treatments in neurology Level 1 Current treatment in Guillain-Barré Syndrome and myasthenia
Title: Revision to the Standardized Surveillance and Case Definition for Acute Flaccid Myelitis
 17-ID-01 Committee: Infectious Disease Title: Revision to the Standardized Surveillance and Case Definition for Acute Flaccid Myelitis I. Statement of the Problem Acute flaccid myelitis (AFM) is a syndrome
17-ID-01 Committee: Infectious Disease Title: Revision to the Standardized Surveillance and Case Definition for Acute Flaccid Myelitis I. Statement of the Problem Acute flaccid myelitis (AFM) is a syndrome
Guillain Barré Syndrome: Profile of 120 Patients with respect to Response to Various Modalities of Treatment
 IJPMR ORIGINAL ARTICLE 10.5005/jp-journals-10066-0022 Guillain Barré Syndrome Guillain Barré Syndrome: Profile of 120 Patients with respect to Response to Various Modalities of Treatment 1 Vishal A Chafale,
IJPMR ORIGINAL ARTICLE 10.5005/jp-journals-10066-0022 Guillain Barré Syndrome Guillain Barré Syndrome: Profile of 120 Patients with respect to Response to Various Modalities of Treatment 1 Vishal A Chafale,
GUILLAIN BARRÉ syndrome is the most common
 1374 THE NEW ENGLAND JOURNAL OF MEDICINE Nov. 23, 1995 CAMPYLOBACTER JEJUNI INFECTION AND GUILLAIN BARRÉ SYNDROME JEREMY H. REES, PH.D., M.R.C.P., SARA E. SOUDAIN, B.SC., NORMAN A. GREGSON, PH.D., AND
1374 THE NEW ENGLAND JOURNAL OF MEDICINE Nov. 23, 1995 CAMPYLOBACTER JEJUNI INFECTION AND GUILLAIN BARRÉ SYNDROME JEREMY H. REES, PH.D., M.R.C.P., SARA E. SOUDAIN, B.SC., NORMAN A. GREGSON, PH.D., AND
Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005)
 Section A: Case Definitions Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005) The current Case Definitions were drafted with available information at the time of writing. Case Definitions
Section A: Case Definitions Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005) The current Case Definitions were drafted with available information at the time of writing. Case Definitions
PMH: No medications; Immunizations UTD No hospitalizations or surgeries Speech Delay. Birth Hx: 24 WGA, NICU x6 months
 HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
HPI: 6 months of weakness and parathesias- originally in both feet x 2-3 months, then resolved. Now with parathesias and weakness in fingers x 1 week. Seen by podiatrist and given custom in-soles 1 month
Recognizing Guillain-Barré Syndrome in the Primary Care Setting
 Internet Journal of Allied Health Sciences and Practice Volume 5 Number 1 Article 5 1-1-2007 Recognizing Guillain-Barré Syndrome in the Primary Care Setting Kristi McClellan Mantay Eastern Virginia Medical
Internet Journal of Allied Health Sciences and Practice Volume 5 Number 1 Article 5 1-1-2007 Recognizing Guillain-Barré Syndrome in the Primary Care Setting Kristi McClellan Mantay Eastern Virginia Medical
