A Placebo-Controlled Trial of Itopride in Functional Dyspepsia
|
|
|
- Francis Hill
- 6 years ago
- Views:
Transcription
1 The new england journal of medicine original article A Placebo-Controlled Trial of Itopride in Functional Dyspepsia Gerald Holtmann, M.D., Nicholas J. Talley, M.D., Ph.D., Tobias Liebregts, M.D., Birgit Adam, M.D., and Christopher Parow, M.D. ABSTRACT From the Department of Gastroenterology, Hepatology and General Medicine, Royal Adelaide Hospital and University of Adelaide, Adelaide (G.H., T.L., B.A.); and the Department of Medicine, University of Sydney, Nepean Hospital, Penrith (N.J.T.) both in Australia; the Mayo Clinic College of Medicine, Rochester, Minn. (N.J.T.); and Global Scientific Support, Abbott, Ludwigshafen, Germany (C.P.). Address reprint requests to Dr. Holtmann at the Department of Gastroenterology, Hepatology and General Medicine, Royal Adelaide Hospital, North Terrace, Adelaide SA 5000, Australia, or at gholtman@mail.rah.sa.gov.au. N Engl J Med 2006;354: Copyright 2006 Massachusetts Medical Society. Background The treatment of patients with functional dyspepsia remains unsatisfactory. We assessed the efficacy of itopride, a dopamine D2 antagonist with acetylcholinesterase effects, in patients with functional dyspepsia. Methods Patients with functional dyspepsia were randomly assigned to receive either itopride (50, 100, or 200 mg ) or placebo. After eight weeks of treatment, primary efficacy end points were analyzed: the change from baseline in the severity of symptoms of functional dyspepsia (as assessed by the Leeds Dyspepsia Questionnaire), patients global assessment of efficacy (the proportion of patients without symptoms or with marked improvement), and the severity of pain or fullness as rated on a five-grade scale. Results We randomly assigned 554 patients; 523 had outcome data and could be included in the analyses. After eight weeks, 41 percent of the patients receiving placebo were symptom-free or had marked improvement, as compared with 57 percent, 59 percent, and 64 percent receiving itopride at a dose of 50, 100, or 200 mg, respectively (P<0.05 for all comparisons between placebo and itopride). Although the symptom score improved significantly in all four groups, an overall analysis revealed that itopride was significantly superior to placebo, with the greatest symptom-score improvement in the 100- and 200-mg groups ( 6.24 and 6.27, vs in the placebo group; P = 0.05). Analysis of the combined end point of pain and fullness showed that itopride yielded a greater rate of response than placebo (73 percent vs. 63 percent, P = 0.04). Conclusions Itopride significantly improves symptoms in patients with functional dyspepsia. (ClinicalTrials.gov number, NCT ) 832
2 Dyspepsia remains a common and costly problem in primary care and gastroenterology practice; in most patients who are examined, no structural lesions causing these symptoms are found. 1 Dyspepsia in the absence of a clinically identifiable structural lesion is referred to as functional dyspepsia, 2,3 in part because disturbed gastrointestinal function is believed to play a role in the development of symptoms. 4 Pharmacologic treatments for patients with functional dyspepsia remain unsatisfactory. 5 The results of controlled trials have generally been disappointing, and only small benefits relative to placebo have been found with histamine H 2 - receptor antagonists, 6 proton-pump inhibitors, 7 and Helicobacter pylori eradication. 8 Although several randomized, controlled trials and metaanalyses have demonstrated the superiority of cisapride over placebo, 9-11 the use of cisapride is now restricted in most countries because of cardiac side effects. In Japan, itopride, which is a dopamine D2 antagonist with acetylcholinesterase inhibitory actions, is often prescribed for patients with functional dyspepsia. Although this drug has been shown to stimulate gastric motility, 12 large, properly designed, randomized, controlled trials in patients with functional dyspepsia are lacking. In Japan, administration of 50 mg is standard practice. However, little is known regarding the dose response in other populations. For this reason, we aimed to study the efficacy of itopride in patients with functional dyspepsia in terms of symptom improvement and to compare various doses of itopride in terms of efficacy and safety in a white population. Methods Study Design and Patient Population Patients Outpatients who were considered to have functional dyspepsia on the basis of the Rome II criteria 3 were eligible for the trial. Functional dyspepsia was diagnosed if persistent or recurrent upper abdominal pain or discomfort was present. Discomfort was characterized by the presence of one or more symptoms that included early satiety, postprandial fullness, bloating, and nausea. Symptoms had to be present for at least 12 weeks within the preceding 12 months, without an identifiable structural or biochemical abnormality to which they could be attributed. Symptoms predominantly related to reflux (e.g., retrosternal pain, burning, and regurgitation) were considered features of gastroesophageal reflux disease, rather than of functional dyspepsia. Therefore, patients who had only reflux-related symptoms or who had predominantly reflux-related symptoms were not eligible for participation. Patients were recruited by 78 physicians in private practice in Germany and one tertiary university hospital, the University Hospital Essen, in Germany. Before patients could be included in the trial, they underwent physical examination, laboratory tests (including white-cell and red-cell counts, measurement of blood sugar during fasting, and liver-function tests), abdominal ultrasonography, and upper gastrointestinal endoscopy so that a structural cause for the symptoms could be ruled out. Patients were excluded if they were taking other medications that may alter gastric function, including macrolide antibiotics. Between and seven days (median, four) after a diagnosis of functional dyspepsia was established, gastrointestinal symptoms and the disease-specific quality of life were reevaluated to determine patients baseline status, and patients were randomly assigned to receive either placebo ( ) or one of doses of itopride (50, 100, or 200 mg ). The study medication was given in a double-blind fashion for eight weeks. The study was approved by the ethics committee of the University Hospital Essen and by the ethics committees of all local study centers. All the patients gave written informed consent. Randomization and Blinding The randomization code was generated with use of Proc Random (SAS, version 6.12). Since only two sizes of active tablet (50 mg and 100 mg) were used, patients received two tablets by means of a double-dummy technique. The study medication was packaged identically for the four dosage groups and was identifiable only by a randomization number. Medications were delivered to the centers in blocks of eight. Patients screening numbers were assigned at the initial visit and were used as individual identification numbers at each center during the screening phase. Patients who met all the inclusion and exclusion criteria were assigned a randomization number in ascending order and treated with the correspondingly identified study medication. 833
3 The new england journal of medicine Assessments Symptoms and Global Relief We used the validated Leeds Dyspepsia Questionnaire (LDQ) 13 to assess dyspeptic symptoms at baseline and after four and eight weeks of treatment. The LDQ, which is administered by an investigator in a face-to-face interview, measures eight dyspepsia symptoms on scales with six grades each (where a grade of 0 indicates not present, 1 very mild, 2 mild, 3 moderate, 4 severe, and 5 very severe); a summary score with a range of 0 to 40 represents the severity of dyspepsia. Patients global assessments of efficacy were evaluated at eight weeks with the use of a global scale with the following five grades: symptomfree, markedly improved, moderately improved, not changed, and deteriorated. Pain and fullness are considered to be the two most important symptoms of functional dyspepsia. We evaluated the severity of pain in the upper abdomen and the severity of fullness after eating as a combined end point. A positive response to treatment was prespecified as improvement by at least one grade on a five-grade scale (absent, very mild or mild, moderate, severe, or very severe) with respect to at least one of the two symptoms (pain or fullness) and no deterioration in the other symptom. Primary Outcome Variables Three primary efficacy criteria were used in this study and were tested in a prespecified order. The change in the summary LDQ score relative to baseline 13 after eight weeks of treatment was the first primary outcome variable. Patients global assessment of efficacy every two weeks was the second primary outcome variable. Finally, the composite response criterion with respect to the severity of pain in the upper abdomen and the severity of a feeling of excessive fullness after eating was evaluated as the third primary outcome variable. Disease-Specific Quality of Life To assess the effects of treatment on diseasespecific quality of life, we used the validated long version of the Nepean Dyspepsia Index (NDI) 14 and calculated a total quality-of-life score. The NDI quality-of-life score ranges from 0 to 99, with higher scores indicating worse quality of life. Compliance and Safety At each visit, patients returned their medication containers, and pills were counted. A patient who took between 80 percent and 120 percent (some patients were treating themselves off protocol under the erroneous assumption that more is better ) of the prescribed pills was considered to be compliant. At baseline and after four and eight weeks, a wide array of laboratory tests was performed, including liver-function and renal-function tests, hematologic tests, measurement of blood glucose, and measurement of serum prolactin. Twelve-lead resting electrocardiograms were obtained at the screening visit and after four and eight weeks of treatment. Statistical Analysis Sample sizes were determined prospectively with reference to other studies that used similar end points. A sample size of 100 patients per group was suitable to identify, with a power of 0.8, a standardized difference (the difference divided by the standard deviation) of 0.4 with an alpha significance level of 0.05 (two-sided). When the same alpha value was used in the testing of hypotheses according to a sequence determined a priori, a sample size of 100 patients per study group was also found suitable to identify a difference of 20 percentage points (40 percent vs. 60 percent) in response rates. All analyses was performed on an intention-to-treat basis, with the last observation carried forward in cases of premature study termination. The last-observationcarried-forward method was appropriate because no more than 10 percent of the observations were missing in each analysis. Missing items on the LDQ were completed before unblinding by means of a prospectively defined imputation technique. Treatment comparisons were made with the use of a hierarchical test system with an overall twosided alpha error rate of As the first of five hypotheses ordered a priori, the global hypothesis that there would be a treatment difference between the pooled active-treatment groups and the placebo group was evaluated by one-factorial analysis of variance (linear contrast of 3D0 + D1 + D2 + D3), where D0 denotes placebo, D1 50 mg of itopride, D2 100 mg of itopride, and D3 200 mg of itopride, testing the 834
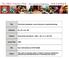
4 null hypothesis that the difference observed in the placebo group subtracted from the sum of the differences in the itopride groups equaled 0). Thus, the linear contrast compared the average changes in the LDQ score in the active-treatment groups with the changes in the LDQ score in the placebo group. Second, monotonic dose responses were tested in a parametric model (linear contrast of 3D0 1D1 + 1D2 + 3D3). Testing of the additional hypotheses involved pairwise comparisons of placebo with itopride, starting with the highest dose (linear contrasts of D3 D0, D2 D0, and D1 D0). This test procedure (which was stopped when the first test result provided a P value 0.05) is more conservative than the procedure described by Holm. 15 To investigate the clinical meaningfulness of the LDQ results, the same test procedure was repeated with Fisher s exact test and the Cochran Armitage test for the two binary outcomes: the response based on patients global assessment of efficacy and the response based on the LDQ pain and fullness items at week 8. In accordance with the main objective of the study namely, to analyze the overall effect of itopride on symptoms and to identify one (or two) doses for further study our analyses focused on the population of all patients with available LDQ data, and when data were missing, we used the last observation carried forward. Twenty-five patients with no efficacy data after treatment were excluded from the analyses. The statistical analyses were performed with SAS software (version 6.12). 16,17 This study was designed by the two senior authors (Drs. Holtmann and Talley) in cooperation with employees of the sponsor (Knoll, Germany), with advice from the statistician and a contract research organization that acted on behalf of the sponsor. The data were collected and analyzed by the contract research organization. The manuscript was written by the academic authors, with input and critical review from all persons involved in the design and data analysis. The academic authors vouch for the veracity and completeness of the data and data analyses. Results Study Population Six hundred six outpatients with a suspected diagnosis of functional dyspepsia were screened (Fig. 1). Fifty-two patients were excluded, leaving 554 patients who were randomly assigned. Six did not receive study medication, resulting in a study population of 548 patients. The patients ages ranged from 18 to 94 years (mean [±SD] age, 47.9±15.8 years). Overall, 63.5 percent of the patients were female. The baseline characteristics of the study population were similar among the groups (Table 1). Eighteen patients in the placebo group did not complete the eight-week treatment, whereas 37 patients in the itopride groups (12 assigned to 50 mg, 11 assigned to 100 mg, and 14 assigned to 200 mg ) did not complete treatment. In the itopride groups, 19 patients (4.7 percent) discontinued treatment prematurely because of adverse events, as compared with 10 patients (7.0 percent) in the placebo group. Response to Treatment Symptom-severity scores on the LDQ improved from baseline during treatment in all four study groups. Testing of the global hypothesis (that there would be a difference between the results in the placebo group and the pooled results in the itopride groups) revealed that itopride was significantly superior to placebo (Table 2 and Fig. 2). The test for a dose response did not reach statistical significance (P = 0.06). The difference between placebo and itopride given at a dose of 50 mg was not significant (P = 0.07), but the differences between placebo and itopride at a dose of 100 mg and between placebo and itopride at a dose of 200 mg were both significant, at P = Testing of all the a priori planned hypotheses for response rates with regard to patients global assessment of efficacy showed significance (Table 2 and Fig. 3). The overall response rate was 59.9 percent with active treatment (232 of 387 patients had a response), as compared with 41.2 percent with placebo (56 of 136 patients had a response) (P<0.001). There was a significant association between the dose of itopride and the response rate (P<0.001). The global hypothesis with regard to response rates according to the severity of pain and fullness on the LDQ yielded a significant discrimination between itopride and placebo, but results on subsequent 835
5 The new england journal of medicine Assessed for eligibility (606 patients) Excluded (52) Deviation from selection criteria (26) (13) Other reason (13) Randomly assigned (554) Analysis Follow-up Randomization Assigned to placebo (143) Received placebo (142) Did not receive placebo (1) Lost to follow-up (5) (3) Noncompliance (2) Discontinued study medication (13) Insufficient efficacy (2) Adverse events (6) Insufficient efficacy and adverse events (4) Occurrence of exclusion criteria (1) Completed study medication (124) Safety analysis (142) Efficacy analysis (136) Exclusion from analysis (6) LDQ data not available (6) Assigned to itopride, 50 mg 3 (139) Received assigned dosage (135) Did not receive assigned dosage (4) Lost to follow-up (5) (5) Discontinued study medication (7) Insufficient efficacy (1) Adverse events (4) Insufficient efficacy and adverse events (2) Completed study medication (123) Safety analysis (135) Efficacy analysis (127) Exclusion from analysis (8) LDQ data not available (8) Assigned to itopride, 100 mg 3 (136) Received assigned dosage (135) Did not receive assigned dosage (1) Lost to follow-up (3) (1) Noncompliance (2) Discontinued study medication (8) Insufficient efficacy (2) Adverse events (4) Insufficient efficacy and adverse events (2) Completed study medication (124) Safety analysis (135) Efficacy analysis (128) Exclusion from analysis (7) LDQ data not available (7) Assigned to itopride, 200 mg 3 (136) Received assigned dosage (136) Lost to follow-up (2) (1) Noncompliance (1) Discontinued study medication (12) Insufficient efficacy (5) Adverse events (6) Insufficient efficacy and adverse events (1) Completed study medication (122) Safety analysis (136) Efficacy analysis (132) Exclusion from analysis (4) LDQ data not available (4) Figure 1. Enrollment, Randomization, Follow-up, and Analysis. LDQ denotes the Leeds Dyspepsia Questionnaire. tests that assessed the dose response and that compared each dose group with placebo were not statistically significant (Table 2). At the end of treatment, the NDI quality-oflife scores were better among patients who were treated with active medication than among those who received placebo. The NDI quality-of-life score improved by a mean of 13.2±19.4 with placebo and by 18.0±21.9 with itopride (P = 0.02). However, differences between the various doses of itopride tested were not statistically significant. Only 112 of the 548 patients (20 percent) tested positive for H. pylori. Overall, 147 of the 436 patients who tested negative for H. pylori 836
6 Table 1. Characteristics of the Patients at Baseline.* Characteristic Placebo Itopride P Value 50 mg Three Times Daily 100 mg Three Times Daily 200 mg Three Times Daily No. of patients Age yr Mean 49.3± ± ± ± Range Sex no. (%) Female 89 (62.7) 87 (64.4) 78 (57.8) 94 (69.1) 0.28 Male 53 (37.3) 48 (35.6) 57 (42.2) 42 (30.9) Negative for Helicobacter pylori no. (%) Dysmotility-type dyspepsia no. (%) 118 (83.1) 113 (83.7) 106 (78.5) 99 (72.8) (28.2) 28 (20.7) 37 (27.4) 34 (25.0) 0.49 Ulcer-type dyspepsia no. (%) 46 (32.4) 54 (40.0) 38 (28.1) 49 (36.0) 0.20 Concomitant heartburn no. (%) 33 (23.2) 28 (20.7) 25 (18.5) 31 (22.8) 0.78 Concomitant irritable bowel syndrome no. (%) 18 (12.7) 22 (16.3) 21 (15.6) 18 (13.2) 0.79 Summary LDQ score 11.9± ± ± ± Nepean Dyspepsia Index 30.2± ± ± ± * Plus minus values are means ±SD. P values are for the comparison among all four study groups. The Leeds Dyspepsia Questionnaire (LDQ) measures eight dyspepsia symptoms on scales with six grades each (where a grade of 0 indicates not present, 1 very mild, 2 mild, 3 moderate, 4 severe, and 5 very severe); a summary score with a range of 0 to 40 represents the severity of dyspepsia. The Nepean Dyspepsia Index quality-of-life score ranges from 0 to 99, with higher scores indicating worse quality of life. (33.6 percent) reported severe or very severe epigastric pain, as compared with 25 of the 110 patients (22.7 percent) who had H. pylori infection (P = 0.02). H. pylori status had no significant influence on the outcome variables (data not shown). Overall, 89 of the 548 patients in the study population reported concomitant symptoms of gastroesophageal reflux disease during the initial clinical assessment. These symptoms did not dominate the clinical picture. Because of their significantly higher scores for epigastric pain and excessive fullness, patients with concomitant symptoms of gastroesophageal reflux disease had significantly higher severity scores on the LDQ than did patients without gastroesophageal reflux disease (18.9±5.7 vs. 10.8±5.6, P<0.001). Concomitant symptoms of gastroesophageal reflux disease were not associated with the response to therapy (data not shown). Adverse Events Adverse events during the treatment period were reported in 37.3 percent, 35.6 percent, 40.0 percent, and 39.0 percent of the patients treated with placebo and those treated with itopride at doses of 50, 100, and 200 mg, respectively. No relevant difference in the overall incidence of adverse events was seen with the use of itopride (38.2 percent), as compared with placebo (37.3 percent) (P = 0.9). The most frequently affected body system was the gastrointestinal tract, which accounted for adverse events in 14.1 percent of the patients in the placebo group and 12.6 percent, 11.1 percent, and 7.4 percent of the patients in the groups assigned to 50 mg, 100 mg, and 200 mg of itopride, respectively. Abdominal pain, diarrhea, nausea, and constipation were the most frequently reported events. Most adverse events were of mild or moderate 837
7 The new england journal of medicine Table 2. Primary Outcome Variables among 523 Patients.* Variable Change from Baseline in LDQ Score Patients Global Assessment of Efficacy Response Rates Severity of Pain and Fullness score P value no./total no. (%) P value no./total no. (%) P value Placebo 4.50± /136 (41.2) 86/136 (63.2) Itopride All doses, pooled 6.22± /387 (59.9) < /387 (72.9) mg 6.16± /127 (56.7) /132 (72.0) mg 6.24± /128 (58.6) /128 (74.2) mg 6.27± /132 (64.4) < /132 (72.0) 0.15 * Plus minus values are means ±SD. The Cochran Armitage test for a dose response in patients global assessment of efficacy revealed a significant dose-related effect (P<0.001), whereas the response rates based on the severity of pain or fullness (P = 0.11) and linear contrasts for monotonic dose responses according to the change in the Leeds Dyspepsia Questionnaire (LDQ) score (P = 0.06) were not significant. P values are for the comparison with placebo. Summary LDQ Score P<0.05 Placebo 50 mg 100 mg 200 mg Figure 2. Mean Changes from Baseline in the Summary Score for Symptom Severity on the Leeds Dyspepsia Questionnaire (LDQ). P<0.05 for the comparison between active treatment and placebo among all patients analyzed (n = 523). I bars represent the standard error. intensity and had resolved by the end of the study. Serious adverse events during the treatment period were seen in 2.8 percent of the patients in the placebo group and 1.2 percent of patients in the overall active-treatment group. They were not considered by the investigators to be related to the study medication. Prolactin levels significantly increased during treatment with 100 mg and 200 mg of itopride given, as compared with placebo (increase in the placebo group, 5.1 percent, vs. increases of 5.8 percent, 16.4 percent, and 20.7 percent in the groups assigned to 50 mg, 100 mg, and 200 mg of itopride, respectively). No clinical symptoms or signs were related to changes in the prolactin level. Treatment with itopride was not associated with any electrocardiographic changes; in particular, there was no prolongation of the corrected QT interval. Discussion Disturbances in gastrointestinal motility and sensory function are now believed to play a key role in the development of symptoms in patients with functional dyspepsia We assessed and compared the effects of doses of a benzamide, itopride, with placebo. In this eight-week study, itopride significantly improved symptoms in patients with functional dyspepsia. It is noteworthy that the improvement in the symptom score during treatment with any of the doses of itopride was approximately 50 percent greater than the improvement with placebo. Although the importance of the improvement in a symptom score might be questioned, the proportion of patients who had a global benefit was also significantly higher in the itopride groups than in the placebo group. Furthermore, itopride 838
8 Response Rate (% of patients) Placebo P=0.01 P= mg P< mg 200 mg Figure 3. Response Rates Based on Patients Global Assessment of Efficacy. Data are shown for all patients analyzed. The graph depicts the proportion of patients who reported that they were symptom-free or that their symptoms had markedly improved after eight weeks. was specifically associated with improvements in pain and fullness, which are believed to be key symptoms of functional dyspepsia. 2,3 We calculated that to achieve marked or complete improvement in symptoms in one patient, six patients would need to be treated. In comparison, when proton-pump inhibitors are used in patients with functional dyspepsia, the number needed to treat is nine. 7 Thus, itopride appears to be efficacious in the treatment of a common condition for which few effective alternative therapies are currently available. Itopride is thought to exert prokinetic effects by way of antidopaminergic and antiacetylcholinesterase actions 12 and probably to have effects on gastric accommodation and gastric hypersensitivity. In our study, we did not measure gastric emptying. Thus, we cannot determine whether gastric emptying was associated with the response to therapy. Stimulation of central dopamine receptors enhances prolactin release, and we observed increased prolactin levels during treatment with itopride. This effect was not associated with any clinical symptoms or signs during the eight-week period of therapy. In previous studies, an augmented increase in prolactin levels in patients with functional dyspepsia after stimulation of central serotoninergic receptors has been observed following treatment with buspirone that stimulates central serotoninergic 1A receptors. 12 Of note, the prolactin level was closely correlated with the degree of delayed solid-phase gastric emptying assessed scintigraphically. 21 Previous trials of treatments for functional dyspepsia have been criticized for various methodologic limitations. 22 The current trial was designed with a sufficient sample size, strict entry criteria, and application of valid outcome measures. The Rome II criteria were used to enroll patients; patients whose symptoms were predominantly those of gastroesophageal reflux disease were not eligible to participate. Nevertheless, there is remarkable overlap between functional dyspepsia and concomitant reflux symptoms. 23 Indeed, in our trial, 89 of the 548 patients who were randomly assigned to a study group also had some reflux symptoms. Although dyspepsia symptoms were significantly more severe, and scores for epigastric pain and excessive fullness were higher, among patients with reflux symptoms, their overall response to treatment was not different from that of patients who had no reflux symptoms. Therefore, it is reasonable to assume that the outcome of this study was not due to a favorable response to treatment with a prokinetic agent among patients with reflux. It is important to note that the trial was not powered a priori to achieve statistically significant results, in terms of pairwise comparisons between individual itopride doses and placebo. Instead, the sample size was calculated to identify a difference that was believed to be clinically significant. 7,8 In reality, the response to therapy was considerably better than expected. Trials longer than eight weeks are needed to confirm the current findings and to determine whether the benefits persist after treatment is stopped. In summary, the results of this multicenter, placebo-controlled trial suggest that itopride, a dopamine D2 antagonist with acetylcholinesterase effects, is superior to placebo in the treatment of functional dyspepsia. The exact mechanisms by which itopride improves symptoms remain to be established, and further clinical trials are needed to assess the efficacy and optimal duration of treatment in various populations. 839
9 Supported by Knoll, which is now owned by Abbott Laboratories, and by a grant (Ho 1193/4-1) from Deutsche Forschungsgemeinschaft. Dr. Holtmann reports having received consulting fees from Knoll. Dr. Talley reports having received research grant support from Axcan Pharmaceuticals, research support from Abbott Laboratories, and having been a consultant for Knoll. Dr. Parow is an employee of Abbott Laboratories. No other potential conflict of interest relevant to this article was reported. We are indebted to Dr. J. Schnitker (Institute for Applied Statistics [IAS], Bielefeld, Germany) and the IAS staff for the statistical analyses and monitoring of the study, to Drs. G. Boos and B. Matiba (Abbott, Ludwigshafen, Germany) for their contributions to the study design and the conduct of the trial, and to our colleagues who helped to recruit the patients. References 1. Richter JE. Dyspepsia: organic causes and differential characteristics from functional dyspepsia. Scand J Gastroenterol Suppl 1991;182: Talley NJ, Colin-Jones D, Koch KL, Koch M, Nyrén O, Stanghellini V. Functional dyspepsia: a classification with guidelines for diagnosis and management. Gastroenterol Int 1991;4: Talley NJ, Stanghellini V, Heading RC, Koch KL, Malagelada JR, Tytgat GN. Functional gastroduodenal disorders. Gut 1999;45:Suppl 2:II-37 II Talley NJ. Functional dyspepsia should treatment be targeted on disturbed physiology? Aliment Pharmacol Ther 1995; 9: Holtmann G, Talley NJ. Functional dyspepsia: current treatment recommendations. Drugs 1993;45: Talley NJ, McNeil D, Hayden A, Piper DW. Randomized, double-blind, placebocontrolled crossover trial of cimetidine and pirenzepine in nonulcer dyspepsia. Gastroenterology 1986;91: Moayyedi P, Delaney BC, Vakil N, Forman D, Talley NJ. The efficacy of proton pump inhibitors in nonulcer dyspepsia: a systematic review and economic analysis. Gastroenterology 2004;127: Laine L, Schoenfeld P, Fennerty MB. Therapy for Helicobacter pylori in patients with nonulcer dyspepsia: a meta-analysis of randomized, controlled trials. Ann Intern Med 2001;134: Talley NJ, Vakil NB, Moayyedi P. American Gastroenterological Association technical review on the evaluation of dyspepsia. Gastroenterology 2005;129: Dobrilla G, Comberlato M, Steele A, Vallaperta P. Drug treatment of functional dyspepsia: a meta-analysis of randomized controlled clinical trials. J Clin Gastroenterol 1989;11: Veldhuyzen van Zanten SJ, Jones MJ, Verlinden M, Talley NJ. Efficacy of cisapride and domperidone in functional (nonulcer) dyspepsia: a meta-analysis. Am J Gastroenterol 2001;96: Iwanaga Y, Miyashita N, Saito T, Morikawa K, Itoh Z. Gastroprokinetic effect of a new benzamide derivative itopride and its action mechanisms in conscious dogs. Jpn J Pharmacol 1996;71: Moayyedi P, Duffett S, Braunholtz D, et al. The Leeds Dyspepsia Questionnaire: a valid tool for measuring the presence and severity of dyspepsia. Aliment Pharmacol Ther 1998;12: Talley NJ, Haque M, Wyeth JW, et al. Development of a new dyspepsia impact scale: the Nepean Dyspepsia Index. Aliment Pharmacol Ther 1999;13: Holm S. A simple sequentially rejective multiple test procedure. Scand J Stat 1979;6: SAS/STAT software: changes and enhancements through Release Cary, N.C.: SAS Institute, SAS/STAT user s guide, vol. 1 and 2. Cary, N.C.: SAS Institute, Holtmann G, Gschossmann J, Neufang-Huber J, Gerken G, Talley NJ. Differences in gastric mechanosensory function after repeated ramp distensions in nonconsulters with dyspepsia and healthy controls. Gut 2000;47: Holtmann G, Talley NJ, Mitchell H, Hazell S. Antibody response to specific H. pylori antigens in functional dyspepsia, duodenal ulcer disease, and health. Am J Gastroenterol 1998;93: Zighelboim J, Talley NJ. What are functional bowel disorders? Gastroenterology 1993;104: [Erratum, Gastroenterology 1993;105:649.] 21. Dinan TG, Chua AS, Keeling PW. Serotonin and physical illness: focus on non-ulcer dyspepsia. Invicta Satellite Meeting: depression and the physically ill. J Psychopharmacol 1993;7(Suppl): Veldhuyzen van Zanten SJ, Cleary C, Talley NJ, et al. Drug treatment of functional dyspepsia: a systematic analysis of trial methodology with recommendations for design of future trials. Am J Gastroenterol 1996;91: Agreus L, Svardsudd K, Nyren O, Tibblin G. Irritable bowel syndrome and dyspepsia in the general population: overlap and lack of stability over time. Gastroenterology 1995;109: Copyright 2006 Massachusetts Medical Society. POWERPOINT SLIDES OF JOURNAL FIGURES AND TABLES At the Journal s Web site, subscribers can automatically create PowerPoint slides of Journal figures and tables. Click on a figure or table in the full-text version of any article at and then click on PowerPoint Slide for Teaching. A PowerPoint slide containing the image, with its title and reference citation, can then be downloaded and saved. 840
Validation of the gastrointestinal symptom score for the assessment of symptoms in patients with functional dyspepsia
 Aliment Pharmacol Ther 2005; 22: 357 363. doi: 10.1111/j.1365-2036.2005.02572.x Validation of the gastrointestinal symptom score for the assessment of symptoms in patients with functional dyspepsia B.
Aliment Pharmacol Ther 2005; 22: 357 363. doi: 10.1111/j.1365-2036.2005.02572.x Validation of the gastrointestinal symptom score for the assessment of symptoms in patients with functional dyspepsia B.
Dyspepsia is a problem commonly seen by primary
 Concise Review for Clinicians Nonulcer Dyspepsia: What It Is and What It Is Not G. RICHARD LOCKE III, MD Nonulcer dyspepsiais a description of persistent or recurrent upper abdominal pain or discomfort
Concise Review for Clinicians Nonulcer Dyspepsia: What It Is and What It Is Not G. RICHARD LOCKE III, MD Nonulcer dyspepsiais a description of persistent or recurrent upper abdominal pain or discomfort
June By: Reza Gholami
 ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
SUMMARY INTRODUCTION. Accepted for publication 7 August 2003
 Aliment Pharmacol Ther 2003; 18: 1099 1105. doi: 10.1046/j.1365-2036.2003.01767.x Efficacy of artichoke leaf extract in the treatment of patients with functional dyspepsia: a six-week placebo-controlled,
Aliment Pharmacol Ther 2003; 18: 1099 1105. doi: 10.1046/j.1365-2036.2003.01767.x Efficacy of artichoke leaf extract in the treatment of patients with functional dyspepsia: a six-week placebo-controlled,
Outline. Definition (s) Epidemiology Pathophysiology Management With an emphasis on recent developments
 Chronic Dyspepsia Eamonn M M Quigley MD FRCP FACP MACG FRCPI Lynda K and David M Underwood Center for Digestive Disorders Houston Methodist Hospital Houston, Texas Outline Definition (s) Epidemiology Pathophysiology
Chronic Dyspepsia Eamonn M M Quigley MD FRCP FACP MACG FRCPI Lynda K and David M Underwood Center for Digestive Disorders Houston Methodist Hospital Houston, Texas Outline Definition (s) Epidemiology Pathophysiology
Number of studies. Endoscopic finding. Number of subjects. Pooled prevalence 95% CI
 Clinical Approach to the Patient t with Dyspepsia William D. Chey, MD, FACG Professor of Medicine University of Michigan Prevalence of Endoscopic Findings in Individuals with Dyspepsia Systematic Review
Clinical Approach to the Patient t with Dyspepsia William D. Chey, MD, FACG Professor of Medicine University of Michigan Prevalence of Endoscopic Findings in Individuals with Dyspepsia Systematic Review
Functional Dyspepsia
 Functional Dyspepsia American College of Gastroenterology Boston Massachusetts, June 2015 Brian E. Lacy, PhD, MD, FACG Professor of Medicine Geisel School of Medicine at Dartmouth Chief, Section of Gastroenterology
Functional Dyspepsia American College of Gastroenterology Boston Massachusetts, June 2015 Brian E. Lacy, PhD, MD, FACG Professor of Medicine Geisel School of Medicine at Dartmouth Chief, Section of Gastroenterology
Management of Functional Dyspepsia (FD)
 Management of Functional Dyspepsia (FD) Amy S. Oxentenko, MD, FACG Program Director and Associate Chair, IM Associate Professor of Medicine Mayo Clinic, Rochester Outline Define functional dyspepsia (FD)
Management of Functional Dyspepsia (FD) Amy S. Oxentenko, MD, FACG Program Director and Associate Chair, IM Associate Professor of Medicine Mayo Clinic, Rochester Outline Define functional dyspepsia (FD)
Non-Ulcer Dyspepsia: what is it? What can we do with these patients? Overview. Dyspepsia Definition. Functional Dyspepsia. Dyspepsia the Basics
 Non-Ulcer : what is it? What can we do with these patients? Temporal Changes and Geographic Variations in Developing Peptic Ulcer Disease Gastric Cancer 1900 Eamonn M M Quigley MD FACG Alimentary Pharmabiotic
Non-Ulcer : what is it? What can we do with these patients? Temporal Changes and Geographic Variations in Developing Peptic Ulcer Disease Gastric Cancer 1900 Eamonn M M Quigley MD FACG Alimentary Pharmabiotic
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University
 CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
A Study on the Efficacy of Proton Pump Inhibitors in Helicobacter pylori- Negative Primary Care Patients with Dyspepsia in Japan
 Gut and Liver, Vol. 7, No. 1, January 2013, pp. 16-22 ORiginal Article A Study on the Efficacy of Proton Pump Inhibitors in Helicobacter pylori- Negative Primary Care Patients with Dyspepsia in Japan Tomoari
Gut and Liver, Vol. 7, No. 1, January 2013, pp. 16-22 ORiginal Article A Study on the Efficacy of Proton Pump Inhibitors in Helicobacter pylori- Negative Primary Care Patients with Dyspepsia in Japan Tomoari
HELICOBACTER PYLORI; PATIENTS WITH FUNCTIONAL DYSPEPSIA
 The Professional Medical Journal www.theprofesional.com ORIGINAL PROF-2404 1. Associate Professor and Health Sciences, (LUMHS) 2. MD, Consultant Physician,, Medical-III, Ward 06 Liaquat University Hospital,
The Professional Medical Journal www.theprofesional.com ORIGINAL PROF-2404 1. Associate Professor and Health Sciences, (LUMHS) 2. MD, Consultant Physician,, Medical-III, Ward 06 Liaquat University Hospital,
Functional Heartburn and Dyspepsia
 Functional Heartburn and Dyspepsia Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina Objectives Understand the means of diagnosing functional heartburn
Functional Heartburn and Dyspepsia Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina Objectives Understand the means of diagnosing functional heartburn
Setting The setting was primary care. The economic study was conducted in Canada.
 Treating Helicobacter pylori infection in primary care patients with uninvestigated dyspepsia: the Canadian adult dyspepsia empiric treatment - Helicobacter pylori positive (CADET-Hp) randomised controlled
Treating Helicobacter pylori infection in primary care patients with uninvestigated dyspepsia: the Canadian adult dyspepsia empiric treatment - Helicobacter pylori positive (CADET-Hp) randomised controlled
The PPI Doesn t Work, Now What? PPI Non-responsive Dyspepsia. Disclosures
 The PPI Doesn t Work, Now What? PPI Non-responsive Dyspepsia Lana Bistritz MD FRCPC Royal Alexandra Hospital GI Update 2016 Disclosures I have no relevant financial disclosures I will be discussing off
The PPI Doesn t Work, Now What? PPI Non-responsive Dyspepsia Lana Bistritz MD FRCPC Royal Alexandra Hospital GI Update 2016 Disclosures I have no relevant financial disclosures I will be discussing off
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 12, by Am. Coll. of Gastroenterology ISSN /03/$30.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 12, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Inc. doi:10.1016/j.amjgastroenterol.2003.07.003 An Update
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 12, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Inc. doi:10.1016/j.amjgastroenterol.2003.07.003 An Update
Functional Dyspepsia, Delayed Gastric Emptying and Impaired Quality of Life
 Gut Online First, published on December 1, 2005 as 10.1136/gut.2005.078634 Functional Dyspepsia, Delayed Gastric Emptying and Impaired Quality of Life NJ Talley 1, GR Locke III 1, BD Lahr 2, AR Zinsmeister
Gut Online First, published on December 1, 2005 as 10.1136/gut.2005.078634 Functional Dyspepsia, Delayed Gastric Emptying and Impaired Quality of Life NJ Talley 1, GR Locke III 1, BD Lahr 2, AR Zinsmeister
The Risk Factors and Quality of Life in Patients with Overlapping Functional Dyspepsia or Peptic Ulcer Disease with Gastroesophageal Reflux Disease
 Gut and Liver, Vol. 8, No. 2, March 2014, pp. 160-164 ORiginal Article The Risk Factors and Quality of Life in Patients with Overlapping Functional Dyspepsia or Peptic Ulcer Disease with Gastroesophageal
Gut and Liver, Vol. 8, No. 2, March 2014, pp. 160-164 ORiginal Article The Risk Factors and Quality of Life in Patients with Overlapping Functional Dyspepsia or Peptic Ulcer Disease with Gastroesophageal
F unctional gastrointestinal disorders (FGID) are clinical
 1445 IRRITABLE BOWEL SYNDROME Symptom patterns in functional dyspepsia and irritable bowel syndrome: relationship to disturbances in gastric emptying and response to a nutrient challenge in consulters
1445 IRRITABLE BOWEL SYNDROME Symptom patterns in functional dyspepsia and irritable bowel syndrome: relationship to disturbances in gastric emptying and response to a nutrient challenge in consulters
COMPARISON OF ONCE-A-DAY VERSUS TWICE-A-DAY CLARITHROMYCIN IN TRIPLE THERAPY FOR HELICOBACTER PYLORI ERADICATION
 Phil J Gastroenterol 2006; 2: 25-29 COMPARISON OF ONCE-A-DAY VERSUS TWICE-A-DAY CLARITHROMYCIN IN TRIPLE THERAPY FOR HELICOBACTER PYLORI ERADICATION Marianne P Collado, Ma Fatima P Calida, Peter P Sy,
Phil J Gastroenterol 2006; 2: 25-29 COMPARISON OF ONCE-A-DAY VERSUS TWICE-A-DAY CLARITHROMYCIN IN TRIPLE THERAPY FOR HELICOBACTER PYLORI ERADICATION Marianne P Collado, Ma Fatima P Calida, Peter P Sy,
Setting The setting was primary and secondary care. The economic study was carried out in the UK.
 Helicobacter pylori "test and treat" or endoscopy for managing dyspepsia: an individual patient data meta-analysis Ford A C, Qume M, Moayyedi P, Arents N L, Lassen A T, Logan R F, McColl K E, Myres P,
Helicobacter pylori "test and treat" or endoscopy for managing dyspepsia: an individual patient data meta-analysis Ford A C, Qume M, Moayyedi P, Arents N L, Lassen A T, Logan R F, McColl K E, Myres P,
Validation of a Four-Graded Scale for Severity of Heartburn in Patients with Symptoms of Gastroesophageal Reflux Disease
 Volume 11 Number 4 2008 VALUE IN HEALTH Validation of a Four-Graded Scale for Severity of Heartburn in Patients with Symptoms of Gastroesophageal Reflux Disease Ola Junghard, PhD, 1 Ingela Wiklund, PhD
Volume 11 Number 4 2008 VALUE IN HEALTH Validation of a Four-Graded Scale for Severity of Heartburn in Patients with Symptoms of Gastroesophageal Reflux Disease Ola Junghard, PhD, 1 Ingela Wiklund, PhD
receptor antagonists and prokinetics in dyspepsia: a critical review
 iv58 DYSPEPSIA MANAGEMENT H 2 antagonists and prokinetics in dyspepsia: a critical review P Bytzer... Drug treatment of with functional dyspepsia is controversial but H 2 antagonists have been the mainstay
iv58 DYSPEPSIA MANAGEMENT H 2 antagonists and prokinetics in dyspepsia: a critical review P Bytzer... Drug treatment of with functional dyspepsia is controversial but H 2 antagonists have been the mainstay
Assessment of symptomatic response as predictor of Helicobacter pylori status following eradication therapy in patients with ulcer
 618 University Department of Medicine and Therapeutics, Western Infirmary, Glasgow G11 6NT, UK K E L McColl A El-Nujumi L S Murray E M El-Omar A Dickson A W Kelman T E Hilditch Correspondence to: Professor
618 University Department of Medicine and Therapeutics, Western Infirmary, Glasgow G11 6NT, UK K E L McColl A El-Nujumi L S Murray E M El-Omar A Dickson A W Kelman T E Hilditch Correspondence to: Professor
Functional dyspepsia: recent advances in pathophysiology. Citation Hong Kong Practitioner, 1998, v. 20 n. 6, p
 Title Functional dyspepsia: recent advances in pathophysiology Author(s) Hu, HC; Lam, SK Citation Hong Kong Practitioner, 1998, v. 20 n. 6, p. 327-334 Issued Date 1998 URL http://hdl.handle.net/10722/45089
Title Functional dyspepsia: recent advances in pathophysiology Author(s) Hu, HC; Lam, SK Citation Hong Kong Practitioner, 1998, v. 20 n. 6, p. 327-334 Issued Date 1998 URL http://hdl.handle.net/10722/45089
MANAGEMENT OF DYSPEPSIA
 Review Article MANAGEMENT OF DYSPEPSIA Raeefuddin Ahmed* SUMMARY Upper gastro-intestinal motility disorders are not uncommon. While the exact prevalence in Pakistan is not known there are substantial number
Review Article MANAGEMENT OF DYSPEPSIA Raeefuddin Ahmed* SUMMARY Upper gastro-intestinal motility disorders are not uncommon. While the exact prevalence in Pakistan is not known there are substantial number
D yspepsia literally means bad digestion. Evaluation and treatment of dyspepsia REVIEW. M P Jones...
 25 REVIEW Evaluation and treatment of dyspepsia M P Jones... Dyspepsia is a common symptom. Dyspeptic symptoms may be caused by a variety of conditions such as peptic ulcer disease, gastro-oesophageal
25 REVIEW Evaluation and treatment of dyspepsia M P Jones... Dyspepsia is a common symptom. Dyspeptic symptoms may be caused by a variety of conditions such as peptic ulcer disease, gastro-oesophageal
Drug Class Review on Proton Pump Inhibitors
 Drug Class Review on Proton Pump Inhibitors Final Report Update 4 July 2006 Original Report Date: November 2002 Update 1 Report Date: April 2003 Update 2 Report Date: April 2004 Update 3 Report Date: May
Drug Class Review on Proton Pump Inhibitors Final Report Update 4 July 2006 Original Report Date: November 2002 Update 1 Report Date: April 2003 Update 2 Report Date: April 2004 Update 3 Report Date: May
Clinical Evaluation of Himcocid Suspension in Patients with Non-ulcer Dyspepsia
 [The Antiseptic (21): (98), 11, 49-411] Clinical Evaluation of Himcocid Suspension in Patients with Non-ulcer Dyspepsia Upadhyaya, B.N., Reader and Head, and Khagen Basumathy, Junior Resident Department
[The Antiseptic (21): (98), 11, 49-411] Clinical Evaluation of Himcocid Suspension in Patients with Non-ulcer Dyspepsia Upadhyaya, B.N., Reader and Head, and Khagen Basumathy, Junior Resident Department
Health-related anxiety and the effect of open-access endoscopy in US patients with dyspepsia
 Aliment Pharmacol Ther 23; 17: 835 84. doi: 1.146/j.269-2813.23.1497.x Health-related anxiety and the effect of open-access endoscopy in US patients with dyspepsia A. QUADRI & N. VAKIL University of Wisconsin
Aliment Pharmacol Ther 23; 17: 835 84. doi: 1.146/j.269-2813.23.1497.x Health-related anxiety and the effect of open-access endoscopy in US patients with dyspepsia A. QUADRI & N. VAKIL University of Wisconsin
Functional Dyspepsia
 Linköping University Medical Dissertations No. 792 Functional Dyspepsia Symptoms and Response to Omeprazole in the Short Term by Elisabeth Bolling-Sternevald Department of Biomedicine and Surgery, Faculty
Linköping University Medical Dissertations No. 792 Functional Dyspepsia Symptoms and Response to Omeprazole in the Short Term by Elisabeth Bolling-Sternevald Department of Biomedicine and Surgery, Faculty
Proton-pump inhibitors for the treatment of functional dyspepsia
 Therapeutic Advances in Gastroenterology Review Proton-pump inhibitors for the treatment of functional dyspepsia Hidekazu Suzuki, Sawako Okada and Toshifumi Hibi Ther Adv Gastroenterol (2011) 4(4) 219
Therapeutic Advances in Gastroenterology Review Proton-pump inhibitors for the treatment of functional dyspepsia Hidekazu Suzuki, Sawako Okada and Toshifumi Hibi Ther Adv Gastroenterol (2011) 4(4) 219
SUPPLEMENTARY INFORMATION Associated with
 Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Management of dyspepsia and of Helicobacter pylori infection
 Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
Sponsor / Company: sanofi-aventis and Proctor & Gamble Drug substance(s): Risedronate (HMR4003)
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: sanofi-aventis and
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: sanofi-aventis and
Maastricht Ⅴ /Florence
 2016 21 10 577 Maastricht Ⅴ /Florence 200001 2015 10 8 9 Maastricht V 1 / 2 3 4 / 5 Maastricht Ⅴ Interpretation of Management of Helicobacter pylori Infection the Maastricht Ⅴ / Florence Consensus Report
2016 21 10 577 Maastricht Ⅴ /Florence 200001 2015 10 8 9 Maastricht V 1 / 2 3 4 / 5 Maastricht Ⅴ Interpretation of Management of Helicobacter pylori Infection the Maastricht Ⅴ / Florence Consensus Report
Our evidence. Your expertise. SmartPill : The data you need to evaluate motility disorders.
 Our evidence. Your expertise. SmartPill : The data you need to evaluate motility disorders. SmartPill benefits your practice: Convenient performed right in your office Test standardization Provides direct
Our evidence. Your expertise. SmartPill : The data you need to evaluate motility disorders. SmartPill benefits your practice: Convenient performed right in your office Test standardization Provides direct
Functional Dyspepsia. Norbert Welkovics Heine van der Walt
 Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
Subgroups of Dyspepsia
 Chapter 2 Subgroups of Dyspepsia Bojan Tepeš Keywords: Dyspepsia, Organic dyspepsia, Functional dyspepsia, Diagnostic criteria, Postprandial distress syndrome, Epigastric pain syndrome Introduction Dyspepsia
Chapter 2 Subgroups of Dyspepsia Bojan Tepeš Keywords: Dyspepsia, Organic dyspepsia, Functional dyspepsia, Diagnostic criteria, Postprandial distress syndrome, Epigastric pain syndrome Introduction Dyspepsia
Patient-reported Outcomes
 3 Patient-reported Outcomes Ingela Wiklund Key points Many gastrointestinal diseases are symptomdriven, so the patient s perspective is particularly important in this area. Patient-reported outcomes (PROs)
3 Patient-reported Outcomes Ingela Wiklund Key points Many gastrointestinal diseases are symptomdriven, so the patient s perspective is particularly important in this area. Patient-reported outcomes (PROs)
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA o Patients of any age with ALARM signs should be referred through the 2-week referral system o Routine endoscopic investigation
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA o Patients of any age with ALARM signs should be referred through the 2-week referral system o Routine endoscopic investigation
A placebo-controlled trial of acotiamide for meal-related symptoms of functional dyspepsia
 Gut Online First, published on December 9, 2011 as 10.1136/gutjnl-2011-301454 Gastroduodenal 1 Sakura Life Clinic, Tokyo, Japan 2 Department of Comprehensive Medicine, Tohoku University Hospital, Sendai,
Gut Online First, published on December 9, 2011 as 10.1136/gutjnl-2011-301454 Gastroduodenal 1 Sakura Life Clinic, Tokyo, Japan 2 Department of Comprehensive Medicine, Tohoku University Hospital, Sendai,
Definition, Pathogenesis, and Management of That Cursed Dyspepsia
 Clinical Gastroenterology and Hepatology 2018;16:467 479 Definition, Pathogenesis, and Management of That Cursed Dyspepsia Pramoda Koduru, Malcolm Irani, and Eamonn M. M. Quigley IM F1 김영기 Dyspepsia Umbrella
Clinical Gastroenterology and Hepatology 2018;16:467 479 Definition, Pathogenesis, and Management of That Cursed Dyspepsia Pramoda Koduru, Malcolm Irani, and Eamonn M. M. Quigley IM F1 김영기 Dyspepsia Umbrella
Does the Injection of Botulinum Toxin Improve Symptoms in Patients With Gastroparesis?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Does the Injection of Botulinum Toxin
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Does the Injection of Botulinum Toxin
Chapter 1. General introduction and outline
 Chapter 1 General introduction and outline General introduction The function of the stomach comprises storage of ingested food, production of gastric secretion and mixing food with gastric secretion,
Chapter 1 General introduction and outline General introduction The function of the stomach comprises storage of ingested food, production of gastric secretion and mixing food with gastric secretion,
Yang K. Chen, MD* Prahalad Jajodia, MD Lino DeGuzman, MD Shahid A. Khan, MD Vaman S. Jakribettuu, MD*
 Randomized Controlled Trial Comparing Proton Pump Inhibitor- Based Eradication Regimen versus Low-Cost Eradication Regimen for Patients with Helicobacter pylori with Uninvestigated Dyspepsia Yang K. Chen,
Randomized Controlled Trial Comparing Proton Pump Inhibitor- Based Eradication Regimen versus Low-Cost Eradication Regimen for Patients with Helicobacter pylori with Uninvestigated Dyspepsia Yang K. Chen,
Investigating dyspepsia Rocco Maurizio Zagari, Lorenzo Fuccio, Franco Bazzoli
 DATE: 11/5/2008-10:27:27 ID:(BMJ)zagr584193 /(Jouve)bmj-001985 DOI: 10.1136/bmj.a1400 Topic(s): Type: InSection:review-article For the full versions of these articles see bmj.com CLINICAL REVIEW Investigating
DATE: 11/5/2008-10:27:27 ID:(BMJ)zagr584193 /(Jouve)bmj-001985 DOI: 10.1136/bmj.a1400 Topic(s): Type: InSection:review-article For the full versions of these articles see bmj.com CLINICAL REVIEW Investigating
Setting The setting was primary care. The economic study was carried out in Canada.
 Economic evaluation of Helicobacter pylori eradication in the CADET-Hp randomized controlled trial of H-pylori-positive primary care patients with uninvestigated dyspepsia Chiba N, Van Zanten S J, Escobedo
Economic evaluation of Helicobacter pylori eradication in the CADET-Hp randomized controlled trial of H-pylori-positive primary care patients with uninvestigated dyspepsia Chiba N, Van Zanten S J, Escobedo
H. Pylori and Dyspepsia
 Focus on CME at the University of Queen s ManitobaUniversity H. Pylori and Dyspepsia By Japie Louw, MB, ChB, FCP(SA), FRCPC, Med PhD Since its rediscovery in the early 1980 s, Helicobacter pylori (H. Pylori)
Focus on CME at the University of Queen s ManitobaUniversity H. Pylori and Dyspepsia By Japie Louw, MB, ChB, FCP(SA), FRCPC, Med PhD Since its rediscovery in the early 1980 s, Helicobacter pylori (H. Pylori)
Results. Subject Disposition and Demographics Of 37 enrolled subjects, 23 (62.2%) completed the study
 Poster 5-20 Effect of Gastric ph on the Bioavailability of in Healthy Subjects James Longstreth, PhD, Marijke H. Adams, PharmD, PhD, 2 Vasi Sperry, PhD, 3 Dan Kajdasz, PhD, 3 Carol R. Reed, MD 3 Longstreth
Poster 5-20 Effect of Gastric ph on the Bioavailability of in Healthy Subjects James Longstreth, PhD, Marijke H. Adams, PharmD, PhD, 2 Vasi Sperry, PhD, 3 Dan Kajdasz, PhD, 3 Carol R. Reed, MD 3 Longstreth
The full complete version includes LDQ-SF Overview information LDQ-SF Scoring/ Administration instructions LDQ-SF Complete Quesionnaire/Assessment
 This is a Sample version of the Leeds Dyspepsia Questionnaire- Short Form (LDQ-SF) The full version of Leeds Dyspepsia Questionnaire -Short Form (LDQ-SF) comes without sample watermark. The full complete
This is a Sample version of the Leeds Dyspepsia Questionnaire- Short Form (LDQ-SF) The full version of Leeds Dyspepsia Questionnaire -Short Form (LDQ-SF) comes without sample watermark. The full complete
J Neurogastroenterol Motil, Vol. 17 No. 3 July, 2011 DOI: /jnm Journal of Neurogastroenterology and Motility
 ㅋ JNM J Neurogastroenterol Motil, Vol. 17 No. 3 July, 2011 DOI: 10.5056/jnm.2011.17.3.279 Journal of Neurogastroenterology and Motility Original Article Functional Gastrointestinal Disorders Diagnosed
ㅋ JNM J Neurogastroenterol Motil, Vol. 17 No. 3 July, 2011 DOI: 10.5056/jnm.2011.17.3.279 Journal of Neurogastroenterology and Motility Original Article Functional Gastrointestinal Disorders Diagnosed
Dyspepsia prevalence and impact on quality of life among Rwandan healthcare workers: A cross-sectional survey
 Dyspepsia prevalence and impact on quality of life among Rwandan healthcare workers: A cross-sectional survey R Bitwayiki, 1,2 MBBS, MMed (IM); J T Orikiiriza, 3,4,5 MB ChB, MMed (Paed); F Kateera, 3 MB
Dyspepsia prevalence and impact on quality of life among Rwandan healthcare workers: A cross-sectional survey R Bitwayiki, 1,2 MBBS, MMed (IM); J T Orikiiriza, 3,4,5 MB ChB, MMed (Paed); F Kateera, 3 MB
Review article: pharmacology of esomeprazole and comparisons with omeprazole
 Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 5 9. Review article: pharmacology of esomeprazole and comparisons with omeprazole J. DENT Department of Gastroenterology, Hepatology and General Medicine, Royal
Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 5 9. Review article: pharmacology of esomeprazole and comparisons with omeprazole J. DENT Department of Gastroenterology, Hepatology and General Medicine, Royal
Do Changes in Visceral Sensory Function Determine the Development of Dyspepsia During Treatment With Aspirin?
 GASTROENTEROLOGY 2002;123:1451 1458 Do Changes in Visceral Sensory Function Determine the Development of Dyspepsia During Treatment With Aspirin? GERALD HOLTMANN,* JUERGEN GSCHOSSMANN,* LYDIA BUENGER,*
GASTROENTEROLOGY 2002;123:1451 1458 Do Changes in Visceral Sensory Function Determine the Development of Dyspepsia During Treatment With Aspirin? GERALD HOLTMANN,* JUERGEN GSCHOSSMANN,* LYDIA BUENGER,*
REVIEW ARTICLE: ENDPOINTS USED IN FUNCTIONAL DYSPEPSIA DRUG THERAPY TRIALS
 REVIEW ARTICLE: ENDPOINTS USED IN FUNCTIONAL DYSPEPSIA DRUG THERAPY TRIALS Daphne Ang, Nicholas J Talley, Magnus Simrén, Pieter Janssen, Guy E Boeckxstaens, Jan Tack To cite this version: Daphne Ang, Nicholas
REVIEW ARTICLE: ENDPOINTS USED IN FUNCTIONAL DYSPEPSIA DRUG THERAPY TRIALS Daphne Ang, Nicholas J Talley, Magnus Simrén, Pieter Janssen, Guy E Boeckxstaens, Jan Tack To cite this version: Daphne Ang, Nicholas
DOMPERIDONE BNF 4.6. Domperidone is a dopamine type 2-receptor antagonist. It is structurally related to the
 DOMPERIDONE BNF 4.6 Class: Prokinetic anti-emetic. Indications: Nausea and vomiting, dysmotility dyspepsia, gastro-oesophageal reflux. Pharmacology Domperidone is a dopamine type 2-receptor antagonist.
DOMPERIDONE BNF 4.6 Class: Prokinetic anti-emetic. Indications: Nausea and vomiting, dysmotility dyspepsia, gastro-oesophageal reflux. Pharmacology Domperidone is a dopamine type 2-receptor antagonist.
Effect of Itopride Hydrochloride on the Ileal and Colonic Motility in Guinea Pig In Vitro
 Yonsei Med J 49(3):472-478, 2008 DOI 10.3349/ymj.2008.49.3.472 Effect of Itopride Hydrochloride on the Ileal and Colonic Motility in Guinea Pig In Vitro Hyun Chul Lim, 1 Young Gyun Kim, 1 Jung Hyun Lim,
Yonsei Med J 49(3):472-478, 2008 DOI 10.3349/ymj.2008.49.3.472 Effect of Itopride Hydrochloride on the Ileal and Colonic Motility in Guinea Pig In Vitro Hyun Chul Lim, 1 Young Gyun Kim, 1 Jung Hyun Lim,
Association between clinical manifestations of complicated and uncomplicated peptic ulcer and visceral sensory dysfunction
 doi:10.1111/j.1440-1746.2010.06269.x GASTROENTEROLOGY jgh_6269 1162..1169 Association between clinical manifestations of complicated and uncomplicated peptic ulcer and visceral sensory dysfunction Montri
doi:10.1111/j.1440-1746.2010.06269.x GASTROENTEROLOGY jgh_6269 1162..1169 Association between clinical manifestations of complicated and uncomplicated peptic ulcer and visceral sensory dysfunction Montri
6/25/ % 20% 50% 19% Functional Dyspepsia Peptic Ulcer GERD Cancer Other
 Peptic Ulcer Disease and Dyspepsia John M. Inadomi, MD Professor of Medicine UCSF Chief, Clinical Gastroenterology San Francisco General Hospital Case History 49 y/o woman complains of several months of
Peptic Ulcer Disease and Dyspepsia John M. Inadomi, MD Professor of Medicine UCSF Chief, Clinical Gastroenterology San Francisco General Hospital Case History 49 y/o woman complains of several months of
Grigoris Leontiadis, MD PhD. McMaster University Upper Gastrointestinal and Pancreatic Diseases Cochrane Group
 Grigoris Leontiadis, MD PhD McMaster University Upper Gastrointestinal and Pancreatic Diseases Cochrane Group No relevant financial relationships with any commercial interests CDDW/CASL Meeting Session:
Grigoris Leontiadis, MD PhD McMaster University Upper Gastrointestinal and Pancreatic Diseases Cochrane Group No relevant financial relationships with any commercial interests CDDW/CASL Meeting Session:
Eamonn M.M. Quigley, John Keohane, Alimentary Pharmabiotic Centre, University College Cork, Cork, Ireland
 Authors and Disclosures www.medscape.com Eamonn M.M. Quigley, John Keohane, Alimentary Pharmabiotic Centre, University College Cork, Cork, Ireland From Current Opinion in Gastroenterology Dyspepsia Eamonn
Authors and Disclosures www.medscape.com Eamonn M.M. Quigley, John Keohane, Alimentary Pharmabiotic Centre, University College Cork, Cork, Ireland From Current Opinion in Gastroenterology Dyspepsia Eamonn
Systematic review: the methodological quality of trials affects estimates of treatment efficacy in functional (non-ulcer) dyspepsia
 Aliment Pharmacol Ther 2004; 19: 631 641. doi: 10.1111/j.1365-2036.2004.01878.x Systematic review: the methodological quality of trials affects estimates of treatment efficacy in functional (non-ulcer)
Aliment Pharmacol Ther 2004; 19: 631 641. doi: 10.1111/j.1365-2036.2004.01878.x Systematic review: the methodological quality of trials affects estimates of treatment efficacy in functional (non-ulcer)
Assessment of reflux symptom severity: methodological options and their attributes
 iv28 Assessment of reflux symptom severity: methodological options and their attributes P Bytzer... Despite major advances in our understanding of reflux disease, the management of this disorder still
iv28 Assessment of reflux symptom severity: methodological options and their attributes P Bytzer... Despite major advances in our understanding of reflux disease, the management of this disorder still
Real World Efficacy and Tolerability of Acotiamide in Relieving Multiple and Overlapping Symptoms in Patients of Functional Dyspepsia
 Archives of Gastroenterology and Hepatology Volume 1, Issue 1, 2018, PP: 1-6 Real World Efficacy and Tolerability of Acotiamide in Relieving Multiple and Overlapping Symptoms in Varsha Narayanan 1 *, Shailesh
Archives of Gastroenterology and Hepatology Volume 1, Issue 1, 2018, PP: 1-6 Real World Efficacy and Tolerability of Acotiamide in Relieving Multiple and Overlapping Symptoms in Varsha Narayanan 1 *, Shailesh
FUNCTIONAL GASTROINTESTINAL DISORDERS: RELATIONS BETWEEN PSYCHOSOCIAL FACTORS, SYMPTOMS AND SENSORIMOTOR DISTURBANCE
 FUNCTIONAL GASTROINTESTINAL DISORDERS: RELATIONS BETWEEN PSYCHOSOCIAL FACTORS, SYMPTOMS AND SENSORIMOTOR DISTURBANCE ETHELLE JEANETTE BENNETT BA (HONS) A thesis submitted in fulfilment of the requirements
FUNCTIONAL GASTROINTESTINAL DISORDERS: RELATIONS BETWEEN PSYCHOSOCIAL FACTORS, SYMPTOMS AND SENSORIMOTOR DISTURBANCE ETHELLE JEANETTE BENNETT BA (HONS) A thesis submitted in fulfilment of the requirements
Reflux of gastric contents, particularly acid, into the esophagus
 Heartburn Reflux of gastric contents, particularly acid, into the esophagus Patient assessment with GERD 1-signs and symptoms The hallmark of typical symptom of GERD is heartburn (restrosternal),acid regurgitation,
Heartburn Reflux of gastric contents, particularly acid, into the esophagus Patient assessment with GERD 1-signs and symptoms The hallmark of typical symptom of GERD is heartburn (restrosternal),acid regurgitation,
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA
 GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
Omeprazole delays gastric emptying in healthy volunteers: an effect prevented by tegaserod
 Aliment Pharmacol Ther 2005; 22: 59 65. doi: 10.1111/j.1365-2036.2005.02528.x Omeprazole delays gastric emptying in healthy volunteers: an effect prevented by tegaserod G. TOUGAS*,,D.L.EARNESTà, Y. CHEN*,
Aliment Pharmacol Ther 2005; 22: 59 65. doi: 10.1111/j.1365-2036.2005.02528.x Omeprazole delays gastric emptying in healthy volunteers: an effect prevented by tegaserod G. TOUGAS*,,D.L.EARNESTà, Y. CHEN*,
Nimish Vakil 1*, Anna Niklasson 2, Hans Denison 2 and Anna Rydén 2
 Vakil et al. BMC Gastroenterology 2014, 14:177 RESEARCH ARTICLE Open Access Symptom profile in partial responders to a proton pump inhibitor compared with treatment-naïve patients with gastroesophageal
Vakil et al. BMC Gastroenterology 2014, 14:177 RESEARCH ARTICLE Open Access Symptom profile in partial responders to a proton pump inhibitor compared with treatment-naïve patients with gastroesophageal
2.0 Synopsis. Choline fenofibrate capsules (ABT-335) M Clinical Study Report R&D/06/772. (For National Authority Use Only) Name of Study Drug:
 2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: (For National Authority Use Only) Name of Study Drug: Volume: Choline Fenofibrate (335) Name of Active Ingredient:
2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: (For National Authority Use Only) Name of Study Drug: Volume: Choline Fenofibrate (335) Name of Active Ingredient:
Clinical Study Synopsis
 Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Many patients with gastroesophageal reflux
 ... HEALTH ECONOMICS... Efficacy and Cost Effectiveness of Lansoprazole Versus Omeprazole in Maintenance Treatment of Symptomatic Gastroesophageal Reflux Disease Eva Vivian, PharmD; Anthony Morreale, PharmD,
... HEALTH ECONOMICS... Efficacy and Cost Effectiveness of Lansoprazole Versus Omeprazole in Maintenance Treatment of Symptomatic Gastroesophageal Reflux Disease Eva Vivian, PharmD; Anthony Morreale, PharmD,
F unctional dyspepsia and gastro-oesophageal reflux disease
 1370 GORD Prevalence of acid reflux in functional dyspepsia and its association with symptom profile J Tack, P Caenepeel, J Arts, K-J Lee, D Sifrim, J Janssens... See end of article for authors affiliations...
1370 GORD Prevalence of acid reflux in functional dyspepsia and its association with symptom profile J Tack, P Caenepeel, J Arts, K-J Lee, D Sifrim, J Janssens... See end of article for authors affiliations...
Helicobacter Pylori Testing HELICOBACTER PYLORI TESTING HS-131. Policy Number: HS-131. Original Effective Date: 9/17/2009
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
David Leff, DO. April 13, Disclosure. I have the following financial relationships to disclosure:
 David Leff, DO AOMA 94 th Annual Convention April 13, 2016 Disclosure I have the following financial relationships to disclosure: Speaker s Bureau: Allergan Labs, Takeda Pharmaceutical, Valeant Pharmaceutical
David Leff, DO AOMA 94 th Annual Convention April 13, 2016 Disclosure I have the following financial relationships to disclosure: Speaker s Bureau: Allergan Labs, Takeda Pharmaceutical, Valeant Pharmaceutical
FEATURE ARTICLE DYSPEPSIA MANAGEMENT IN A RESOURCE POOR SETTING
 FEATURE ARTICLE DYSPEPSIA MANAGEMENT IN A RESOURCE POOR SETTING A.C. Jemilohun 1 and J.O. Fadare 2 Ann Ibd. Pg. Med 2013. Vol.11, No.1 2-6 1. Department of Medicine, Ladoke Akintola University of Technology,
FEATURE ARTICLE DYSPEPSIA MANAGEMENT IN A RESOURCE POOR SETTING A.C. Jemilohun 1 and J.O. Fadare 2 Ann Ibd. Pg. Med 2013. Vol.11, No.1 2-6 1. Department of Medicine, Ladoke Akintola University of Technology,
Risk factors for un-investigated dyspepsia among primary care patients in northern Nigeria
 Risk factors for un-investigated dyspepsia among primary care patients in northern Nigeria *Solomon OA 1, Ajayi AO 2 1. Department of Family Medicine, University Teaching Hospital, Ado Ekiti, Nigeria 2.
Risk factors for un-investigated dyspepsia among primary care patients in northern Nigeria *Solomon OA 1, Ajayi AO 2 1. Department of Family Medicine, University Teaching Hospital, Ado Ekiti, Nigeria 2.
Authors and Disclosures
 Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
PFIZER INC. Study Initiation Date and Completion Dates: 09 March 2000 to 09 August 2001.
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
Clinical Study Synopsis
 Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Study population The study population comprised hypothetical patients with gastric and duodenal ulcer.
 Evaluation of the cost-effectiveness of Helicobacter pylori eradication triple therapy vs. conventional therapy for ulcers in Japan Ikeda S, Tamamuro T, Hamashima C, Asaka M Record Status This is a critical
Evaluation of the cost-effectiveness of Helicobacter pylori eradication triple therapy vs. conventional therapy for ulcers in Japan Ikeda S, Tamamuro T, Hamashima C, Asaka M Record Status This is a critical
Proton Pump Inhibitors (PPIs) (Sherwood Employer Group)
 Proton Pump Inhibitors (PPIs) (Sherwood Employer Group) BCBSKS will review Prior Authorization requests Prior Authorization Form: https://www.bcbsks.com/customerservice/forms/pdf/priorauth-6058ks-st-ippi.pdf
Proton Pump Inhibitors (PPIs) (Sherwood Employer Group) BCBSKS will review Prior Authorization requests Prior Authorization Form: https://www.bcbsks.com/customerservice/forms/pdf/priorauth-6058ks-st-ippi.pdf
2.0 Synopsis. ABT-711 M Clinical Study Report R&D/06/573. (For National Authority Use Only) to Part of Dossier: Volume:
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Depakote ER Name of Active Ingredient: Divalproex sodium (ABT-711) Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
2.0 Synopsis Abbott Laboratories Name of Study Drug: Depakote ER Name of Active Ingredient: Divalproex sodium (ABT-711) Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
Clinical Trial Synopsis
 Clinical Trial Synopsis Title of Study: A Phase III, Open-Label, Fixed-Dose Study to Determine the Safety of Long-Term Administration of TAK-375 in Subjects With Chronic Insomnia Protocol Number: Name
Clinical Trial Synopsis Title of Study: A Phase III, Open-Label, Fixed-Dose Study to Determine the Safety of Long-Term Administration of TAK-375 in Subjects With Chronic Insomnia Protocol Number: Name
Dr. LEUNG Lok Hang, Will
 Direct access endoscopy booking by family physicians: evaluating a new service model and clinical predictors of positive endoscopy findings at primary care setting Dr. LEUNG Lok Hang, Will Department of
Direct access endoscopy booking by family physicians: evaluating a new service model and clinical predictors of positive endoscopy findings at primary care setting Dr. LEUNG Lok Hang, Will Department of
KEYWORDS Dyspepsia, Acid Peptic Disease, Helicobacter Pylori, Urease, Giemsa, Peptic Ulcer, Non-Ulcer Dyspepsia.
 INCIDENCE OF HELICOBACTER PYLORI WITH ACID PEPTIC DISEASE AND MALIGNANT CONDITIONS OF UPPER GASTROINTESTINAL TRACT IN A TERTIARY CENTRE - A PROSPECTIVE STUDY Karunamoorthy Rajachidambaram 1, Dinkaran Kaarthesan
INCIDENCE OF HELICOBACTER PYLORI WITH ACID PEPTIC DISEASE AND MALIGNANT CONDITIONS OF UPPER GASTROINTESTINAL TRACT IN A TERTIARY CENTRE - A PROSPECTIVE STUDY Karunamoorthy Rajachidambaram 1, Dinkaran Kaarthesan
Committee Approval Date: October 14, 2014 Next Review Date: October 2015
 Medication Policy Manual Topic: esomeprazole-containing medications: - Nexium - Vimovo - esomeprazole strontium Policy No: dru039 Date of Origin: May 2001 Committee Approval Date: October 14, 2014 Next
Medication Policy Manual Topic: esomeprazole-containing medications: - Nexium - Vimovo - esomeprazole strontium Policy No: dru039 Date of Origin: May 2001 Committee Approval Date: October 14, 2014 Next
Review article: gastric acidity ) comparison of esomeprazole with other proton pump inhibitors
 Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 10 15. Review article: gastric acidity ) comparison of esomeprazole with other proton pump inhibitors J. G. HATLEBAKK Department of Medicine, Haukeland Sykehus,
Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 10 15. Review article: gastric acidity ) comparison of esomeprazole with other proton pump inhibitors J. G. HATLEBAKK Department of Medicine, Haukeland Sykehus,
Overuse of acid suppressant drugs in patients with chronic renal failure
 Nephrol Dial Transplant (2003) 18: 570 575 Original Article Overuse of acid suppressant drugs in patients with chronic renal failure Hans Strid, Magnus Simrén and Einar S. Björnsson Department of Internal
Nephrol Dial Transplant (2003) 18: 570 575 Original Article Overuse of acid suppressant drugs in patients with chronic renal failure Hans Strid, Magnus Simrén and Einar S. Björnsson Department of Internal
IBS: overview and assessment of pain outcomes and implications for inclusion criteria
 IBS: overview and assessment of pain outcomes and implications for inclusion criteria William D. Chey, MD Professor of Medicine University of Michigan What is the Irritable Bowel Syndrome Symptom based
IBS: overview and assessment of pain outcomes and implications for inclusion criteria William D. Chey, MD Professor of Medicine University of Michigan What is the Irritable Bowel Syndrome Symptom based
Article: Min, T and Ford, AC (2016) Efficacy of mesalazine in IBS. Gut, 65 (1). pp ISSN
 This is a repository copy of Efficacy of mesalazine in IBS. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/97338/ Version: Accepted Version Article: Min, T and Ford, AC (2016)
This is a repository copy of Efficacy of mesalazine in IBS. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/97338/ Version: Accepted Version Article: Min, T and Ford, AC (2016)
An evaluation of whole blood testing for Helicobacter pylori in general practice
 Aliment Pharmacol Ther 1998; 12: 641±645. An evaluation of whole blood testing for Helicobacter pylori in general practice N. J. TALLEY, J. R. LAMBERT*, S. HOWELL, H. H.-X. XIA, S. K. LIN* & L. AGREUS
Aliment Pharmacol Ther 1998; 12: 641±645. An evaluation of whole blood testing for Helicobacter pylori in general practice N. J. TALLEY, J. R. LAMBERT*, S. HOWELL, H. H.-X. XIA, S. K. LIN* & L. AGREUS
Does The Use Of Probiotics Treat Abdominal Pain In Children Between The Ages Of 4 And 18 With Irritable Bowel Syndrome?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Does The Use Of Probiotics Treat Abdominal
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Does The Use Of Probiotics Treat Abdominal
ORIGINAL ARTICLES ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:612 619 ORIGINAL ARTICLES ALIMENTARY TRACT Regurgitation Is Less Responsive to Acid Suppression Than Heartburn in Patients With Gastroesophageal Reflux
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:612 619 ORIGINAL ARTICLES ALIMENTARY TRACT Regurgitation Is Less Responsive to Acid Suppression Than Heartburn in Patients With Gastroesophageal Reflux
Medical Policy. MP Ingestible ph and Pressure Capsule
 Medical Policy BCBSA Ref. Policy: 2.01.81 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.20 Esophageal ph Monitoring 6.01.33 Wireless Capsule Endoscopy as a
Medical Policy BCBSA Ref. Policy: 2.01.81 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.20 Esophageal ph Monitoring 6.01.33 Wireless Capsule Endoscopy as a
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW
 PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
Helicobacter 2008;13:1-6. Am J Gastroent 2007;102: Am J of Med 2004;117:31-35.
 An Update on Helicobacter pylori and Its Treatment Trenika Mitchell, PharmD, BCPS Clinical Assistant Professor University of Kentucky College of Pharmacy October 18, 2008 Objectives Review the epidemiology
An Update on Helicobacter pylori and Its Treatment Trenika Mitchell, PharmD, BCPS Clinical Assistant Professor University of Kentucky College of Pharmacy October 18, 2008 Objectives Review the epidemiology
