Venous, Arterial, and Neuropathic Lower-Extremity Wounds: Clinical Resource Guide
|
|
|
- Aleesha McDowell
- 6 years ago
- Views:
Transcription
1 Venous, Arterial, and Neuropathic Lower-Extremity Wounds: Clinical Resource Guide The Wound, Ostomy and Continence Nurses Society suggests the following format for bibliographic citations: Wound, Ostomy and Continence Nurses Society. (2017). Venous, arterial, and neuropathic lower-extremity wounds: Clinical resource guide. Mt. Laurel, NJ: Author. Copyright 2017 by the Wound, Ostomy and Continence Nurses Society (WOCN ). Date of publication: 10/10/17. No part of this publication may be reproduced, photocopied, or republished in any form, in whole or in part, without written permission of the WOCN Society.
2 Contents Contributors... 3 Introduction... 4 Purpose... 4 Assessment: Lower-Extremity Venous Disease (LEVD), Lower-Extremity Arterial Disease (LEAD), and Lower-Extremity Neuropathic Disease (LEND)... 5 History/Risk Factors... 5 Comorbid Conditions... 5 Wound Location... 6 Wound Characteristics... 6 Surrounding Skin... 6 Nails... 7 Complications... 7 Perfusion/Sensation of the Lower Extremity... 7 Pain... 7 Peripheral Pulses... 8 Common Non-Invasive Vascular Tests... 8 Screen for Loss of Protective Sensation... 8 Measures to Improve Venous Return... 9 Measures to Improve Tissue Perfusion... 9 Measures to Prevent Trauma... 9 Topical Therapy Goals Considerations/Options Adjunctive Therapy Indications for Referral to Other Healthcare Providers for Additional Evaluation and Treatment References
3 Contributors Originated By: Wound Committee, WOCN Society Original Publication Date: November 2009 Updated/Revised: April 2013: Wound Committee, WOCN Society September 2017: Phyllis A. Bonham, PhD, MSN, RN, CWOCN, DPNAP, FAAN Clinical Editor, WOCN Society Chair, Wound Guidelines Task Force, WOCN Society 3
4 Venous, Arterial, and Neuropathic Lower-Extremity Wounds: Clinical Resource Guide Introduction This Clinical Resource Guide updates the previous document, A Quick Reference Guide for Lower-Extremity Wounds: Venous, Arterial, and Neuropathic, which was developed by the Wound Committee of the Wound, Ostomy and Continence Nurses Society (WOCN, 2013). The guide is a synopsis of content derived from the WOCN Society s Clinical Practice Guideline Series for managing lower-extremity wounds due to venous, arterial, or neuropathic disease. Refer to the complete version of each Clinical Practice Guideline for more detailed, evidence-based information about the management of wounds in patients with lower-extremity venous, arterial, or neuropathic disease (WOCN, 2011, 2012, 2014): The guidelines are available in print or as an electronic mobile app from the WOCN Society s Bookstore ( Guideline for management of wounds in patients with lower-extremity venous disease (2011). Guideline for management of wounds in patients with lower-extremity neuropathic disease (2012). Guideline for management of wounds in patients with lower-extremity arterial disease (2014). Purpose This guide provides an overview of common assessment findings and key characteristics of the three most common types of lower-extremity wounds (i.e., venous, arterial, neuropathic). In addition, it includes a summary of the following information: measures to improve venous return and tissue perfusion; measures to prevent trauma; goals, considerations, and options for topical therapy; adjunctive therapies; and indications for referral to other healthcare providers for additional evaluation and treatment. 4
5 Lower-Extremity Venous Disease (LEVD) Wounds (WOCN, 2011) Advanced age. Obesity. Pregnancy. Thrombophilia. Systemic inflammation. Anticardiolipin antibody. Venous thromboembolism (VTE); phlebitis. Varicose veins. Pulmonary embolus. Sedentary lifestyle or occupation; reduced mobility. Simultaneous insufficiency of two out of three venous systems. Trauma; surgeries; leg fractures. Impaired calf muscle pump. Restricted range of motion of the ankle. Family history of venous disease. Injection drug user. Previous wound. Congestive heart failure. Lymphedema. Orthopedic procedures. Rheumatoid arthritis. Venous, Arterial, and Neuropathic Lower-Extremity Wounds: Clinical Resource Guide Lower-Extremity Arterial Disease (LEAD) Lower-Extremity Neuropathic Disease (LEND) Wounds (WOCN, 2014) Wounds (WOCN, 2012) Assessment: History/Risk Factors Advanced age. Smoking/tobacco use. Diabetes. Hyperlipidemia. Hypertension. Elevated homocysteine. Chronic renal insufficiency. Family history of cardiovascular disease. Ethnicity. Persistent Chlamydia pneumoniae infection. Periodontal disease. Assessment: Comorbid Conditions Cardiovascular disease; cerebrovascular disease; vascular procedures or surgeries. Sickle cell anemia. Obesity; metabolic syndrome. Arthritis. Spinal cord injury. Migraine. Atrial fibrillation. Human immunodeficiency virus (HIV). Low testosterone. 5 Advanced age; heredity. Alcoholism. Diabetes longer than 10 years; poor diabetes control; impaired glucose tolerance. Hansen s disease (leprosy); Charcot-Marie-Tooth disease. Smoking/tobacco use. Human immunodeficiency virus/acquired immunodeficiency syndrome and related drug therapies. Hypertension. Obesity. Raynaud s disease; scleroderma. Hyperthyroidism; hypothyroidism. Chronic obstructive pulmonary disease. Spinal cord injury; neuromuscular diseases. Abdominal, pelvic, and orthopedic procedures. Paraneoplastic disorders. Acromegaly/height. Exposure to heavy metals (e.g., lead, mercury, arsenic). Malabsorption syndrome due to bariatric surgery; celiac disease; vitamin deficiency (B 12, folate, niacin, thiamine); pernicious anemia. Loss of protective sensation; rigid foot deformities; gait abnormalities; history of previous ulcer/amputation. Lower-extremity arterial disease. Kidney disease.
6 Lower-Extremity Venous Disease (LEVD) Wounds (WOCN, 2011) The most typical location is superior to the medial malleolus, but wounds can be anywhere on the lower leg including back of the leg/posterior calf. Base: Ruddy red; granulation tissue and/or yellow adherent or loose slough may be present. Size: Variable; can be large. Depth: Usually shallow. Edges: Irregular; undermining or tunneling are uncommon. Exudate: Moderate to heavy. Infection: Not common. Edema: Pitting or non-pitting; worsens with prolonged standing or sitting with legs dependent. Scarring from previous wounds. Ankle flare; varicose veins. Hemosiderosis (i.e., brown staining). Lipodermatosclerosis. Atrophie blanche. Maceration; crusting; scaling. Temperature: Normally warm to touch. Localized elevation of skin temperature (greater than 4 F) measured at the ankle with a noncontact infrared thermometer is predictive of a wound. Lower-Extremity Arterial Disease (LEAD) Wounds (WOCN, 2014) Assessment: Wound Location Areas exposed to pressure, repetitive trauma, or rubbing from footwear are the most common locations: Lateral malleolus. Mid-tibial area (shin). Phalangeal heads, toe tips, or web spaces. Heels. Assessment: Wound Characteristics Base: Pale; granulation rarely present; necrosis common; eschar may be present. Size: Variable; often small. Depth: May be deep. Edges: Rolled; smooth; punched-out appearance; undermining may be present. Exudate: Minimal. Infection: Frequent (signs may be subtle). Pain: Common. Non-healing; wound often precipitated by minor trauma. Assessment: Surrounding Skin Pallor on elevation. Dependent rubor. Shiny, taut, thin, dry, and fragile. Hair loss over lower extremity. Atrophy of skin, subcutaneous tissue, and muscle. Edema: Atypical of arterial disease; localized edema may indicate infection. Temperature: Skin feels cool to touch. Lower-Extremity Neuropathic Disease (LEND) Wounds (WOCN, 2012) Plantar foot surface is the most typical location. Other common locations include: o Pressure points/sites of painless trauma/repetitive stress, over bony prominences (e.g., heels). o Metatarsal head (e.g., first metatarsal head and interphalangeal joint of great toe). o Dorsal and distal aspects of toes, inter-digital areas, interphalangeal joints. o Midfoot/fore-foot: Collapse of mid-foot structures with rocker-bottom foot suggests Charcot fracture. Base: Pale or pink; necrosis/eschar may be present. Size: Variable. Depth: Variable from shallow to exposed bone/tendon. Edges: Well-defined; smooth; undermining may be present. Shape: Usually round or oblong. Exudate: Usually small to moderate; foul odor and purulence indicate infection. Normal skin color. Anhidrosis; xerosis; fissures; maceration; tinea pedis. Callus over bony prominences (might cover a wound) and periwound; hemorrhage into a callus indicates ulceration underneath. Musculoskeletal/structural foot deformities. Erythema and induration may indicate infection/cellulitis. Edema: Unilateral edema with increased erythema, warmth, and a bounding pulse may indicate Charcot fracture. Temperature: Skin warm to touch; localized elevation of skin temperature greater than 2 C indicates inflammation. Diabetic skin markers: Dermopathy, necrobiosis lipoidica, acanthosis nigricans, bullosis diabeticorum. 6
7 Lower-Extremity Venous Disease (LEVD) Wounds (WOCN, 2011) Lower-Extremity Arterial Disease (LEAD) Wounds (WOCN, 2014) Lower-Extremity Neuropathic Disease (LEND) Wounds (WOCN, 2012) Assessment: Nails N/A Dystrophic. Dystrophic; hypertrophy. Onychomycosis; paronychia. Assessment: Complications Venous dermatitis (e.g., erythema, itching, vesicles, weeping, scaling, crusting, afebrile). Infection/Cellulitis (e.g., pain, erythema, swelling, induration, bulla, fever, leukocytosis). Variceal bleeding. Tinea pedis. Venous thromboembolism. Leg pain may be variable (e.g., severe, throbbing). Pain may be accompanied by complaints of leg heaviness. Leg pain worsens with dependency. Elevation relieves pain. Infection/Cellulitis (e.g., pain, edema, periwound fluctuance; or only a faint halo of erythema around the wound). Osteomyelitis (e.g., probe to bone). Gangrene (wet or dry). Assessment Perfusion/Sensation of the Lower Extremity: Pain Intermittent claudication is a classical sign and indicates 50% of the vessel is occluded (i.e., cramping, aching, fatigue, weakness, and/or pain in the calf, thigh, or buttock that occurs after walking/exercise and typically is relieved with 10 minutes rest). Resting, positional, or nocturnal pain may be present; resting pain indicates 90% of the vessel is occluded. Elevation exacerbates pain. Dependency relieves pain. Neuropathy and paresthesia may occur from ischemic nerve dysfunction. Acute limb ischemia: A sudden onset of the 6 P s (i.e., pain, pulselessness, pallor, paresthesia, paralysis, and polar [coldness]) indicates an acute embolism; and warrants an immediate referral to a vascular surgeon. Critical limb ischemia (CLI): Chronic rest pain; rest pain of the forefoot/toes. Ischemic non-healing wounds or gangrene are limb threatening with a high mortality rate and warrant referral to a vascular surgeon. Infection/Cellulitis. Arterial ischemia. Osteomyelitis. Charcot fracture (e.g., swelling, pain, erythema, localized temperature elevation of 3 7 C compared to an unaffected area). Gangrene. Pain may be superficial, deep, aching, stabbing, dull, sharp, burning, or cool. Decreased or altered sensitivity to touch occurs. Altered sensation not described as pain (e.g., numbness, warmth, prickling, tingling, shooting, pins and needles; stocking-glove pattern ) may be present. Pain may be worse at night. Allodynia (i.e., intolerance to normally painless stimuli such as bed sheets touching feet/legs) may occur. 7
8 Lower-Extremity Venous Disease Lower-Extremity Arterial Disease (LEVD) Wounds (WOCN, 2011) (LEAD) Wounds (WOCN, 2014) Assessment Perfusion/Sensation of the Lower Extremity: Peripheral Pulses Pulses are present and palpable. Pulses are absent or diminished (i.e., dorsalis pedis, posterior tibial). Femoral or popliteal bruits may be heard. Capillary refill: Normal (less than 3 seconds). Venous refill time: Shortened (less than 20 seconds). Ankle brachial index (ABI): Within normal limits ( ). Duplex scanning with ultrasound: Most reliable non-invasive test to diagnose anatomical and hemodynamic abnormalities and detect venous reflux. 8 Lower-Extremity Neuropathic Disease (LEND) Wounds (WOCN, 2012) Pulses are present and palpable. If co-existing LEAD is present: Pulses are absent or diminished (i.e., dorsalis pedis, posterior tibial); and femoral or popliteal bruits may be heard. Assessment Perfusion/Sensation of the Lower Extremity: Common Non-Invasive Vascular Tests Capillary refill: Abnormal (more than 3 seconds). Venous refill time: Prolonged (greater than 20 seconds). Ankle brachial index (ABI): o Non-compressible arteries: Unable to obliterate the pulse signal at cuff pressure greater than 250 mmhg. o Elevated: Greater than o Normal: Equal to/or greater than 1.00 o LEAD: Equal to/or less than o Borderline: Equal to/or less than o Severe ischemia: Equal to/or less than o Critical ischemia: Equal to/or less than Transcutaneous oxygen (TcPO2): Less than 40 mmhg is hypoxic; less than 30 mmhg is CLI. Toe brachial index (TBI): Less than 0.64 indicates LEAD. Toe pressure (TP): Less than 30 mmhg (less than 50 mmhg if diabetes present) indicates CLI. Assess for peripheral, sensory neuropathy using a 5.07/10 g Semmes-Weinstein monofilament. Capillary and venous refill times: Normal. ABI: LEAD, which often co-exists with neuropathic disease and diabetes should be ruled out. The ABI can be elevated greater than 1.30 or arteries can be non-compressible (i.e., unable to obliterate the pulse signal at cuff pressure greater than 250 mmhg), which indicates calcified ankle arteries. In such cases, a TP or TBI is indicated. o TBI: Less than 0.64 indicates LEAD. o TP: Less than 50 mmhg (if diabetes is present) indicates CLI and failure to heal. TcPO2: Less than 40 mmhg is hypoxic; less than 30 mmhg is CLI. Assessment Perfusion/Sensation of the Lower Extremity: Screen for Loss of Protective Sensation Assess light pressure sensation using a 5.07/ 10 g Semmes-Weinstein monofilament. Assess vibratory sensation using a 128 Hz tuning fork. Check deep tendon reflexes at the ankle and knee with a reflex hammer. Inability to feel the monofilament, diminished vibratory perception, and diminished reflexes indicate a loss of protective sensation and an increased risk of wounds. Assess light pressure sensation using a 5.07/10 g Semmes- Weinstein monofilament. Assess vibratory sensation using a 128 Hz tuning fork. Check deep tendon reflexes at the ankle and knee with a reflex hammer. Inability to feel the monofilament, diminished vibratory perception, and diminished reflexes indicate a loss of protective sensation and an increased risk of wounds.
9 Lower-Extremity Venous Disease (LEVD) Wounds (WOCN, 2011) Measures to Improve Venous Return Use compression therapy: mmhg compression at the ankle, if ABI is equal to/or greater than 0.80: o Multi-layer compression systems are more effective than single layer systems. o Consider intermittent pneumatic compression for patients who are immobile or need higher levels of compression than can be provided by wraps or stockings. Elevate legs above heart level: 30 minutes, 4 times per day. Consider medications (e.g., pentoxifylline) to improve blood flow. Increase exercise: Walking, calf muscle exercise, toe lifts, ankle flexion exercises. Avoid constricting garments, crossing legs, prolonged standing, and high heeled shoes. Stop smoking/tobacco use. Manage weight; healthy nutrition. Surgically obliterate damaged veins: Subfascial endoscopic perforator surgery (SEPS). Screen patients for LEAD by Doppler-derived ABI prior to application of compression stockings/bandages/wraps. Mixed venous/arterial disease: o Use reduced compression (23 30 mmhg) for patients with LEVD, wounds, and edema if ABI is less than 0.80 and equal to/or greater than o Do not apply compression if ABI is less than Lower-Extremity Arterial Disease (LEAD) Lower-Extremity Neuropathic Disease Wounds (WOCN, 2014) (LEND) Wounds (WOCN, 2012) Measures to Improve Tissue Perfusion Revascularize if possible. Revascularize if ischemic. Change lifestyle: Stop smoking/tobacco use; avoid Stop smoking/tobacco use. secondhand smoke, restrictive garments, and cold Maintain tight glucose/glycemic control; control temperatures. hypertension. Maintain proper hydration/nutrition. Engage in exercise that is adapted to prevent Maintain legs in a neutral or dependent position. injury. Increase physical activity: Walking; supervised Consider medications, as indicated. exercise minutes, 3 times per week. Use medications to control hypertension, hyperlipidemia, homocysteine levels, and diabetes; antiplatelets to improve blood cell movement through narrowed vessels. Control or reduce weight if obese. Measures to Prevent Trauma Use proper footwear; wear socks/stockings with shoes; obtain professional nail/callus care. Use pressure redistribution/offloading products/devices for heels, toes, and bony prominences, especially if bedbound or chairbound. Avoid chemical, thermal, and mechanical injury (e.g., no bare feet even in the house; no hot soaks or heating pads; no medicated corn pads). Self-inspect the lower extremities daily; promptly report injuries to the healthcare provider. Use reduced compression for mixed venous/arterial disease if the ABI is less than Do not apply compression if ABI is less than 0.50, ankle pressure is less than 70 mmhg, or TP is less than 50 mmhg. 9 Reduce shear stress and offload the at-risk neuropathic foot, and/or wounds (e.g., bedrest, total contact casts, walking splints, orthopedic shoes); use assistive devices for support, balance, and additional offloading. Use proper footwear; obtain routine professional nail/callus care. Use pressure redistribution/offloading products/devices for heels, toes, and bony prominences, especially if in bed or chairbound. Avoid chemical, thermal, and mechanical injury (e.g., no bare feet even in the house; no hot soaks or heating pads; no medicated corn pads; wear socks/stockings with shoes). Self-inspect the lower extremities on a daily basis.
10 Lower-Extremity Venous Disease (LEVD) Wounds (WOCN, 2011) Reduce and control edema. Attain/maintain intact skin; protect the periwound skin from drainage; absorb/manage exudate. Prevent trauma/injury. Prevent, promptly identify, and manage complications (e.g., infection/cellulitis; dermatitis/eczema). Promote wound healing; maintain moist wound surface. Reduce pain. Use absorptive dressings to control exudate. Treat infection: Use culture-guided antibiotic/antimicrobial therapy. o Consider topical antimicrobial/antibiotics for superficial infection. o Deep tissue infection/cellulitis warrants systemic treatment. Remove devitalized tissue. Avoid known skin irritants and allergens, tapes, and adhesives in patients with venous dermatitis/eczema. Use emollients such as petrolatum to manage dry, scaly skin. Consider use of barrier products to protect the periwound skin from excessive drainage and maceration. Identify and treat dermatitis/eczema (e.g., topical steroids 1 2 weeks). Consider topical analgesics for painful wound care/debridement. Lower-Extremity Arterial Disease (LEAD) Wounds (WOCN, 2014) Topical Therapy: Goals Prevent trauma/injury. Prevent, promptly identify, and manage complications (e.g., infection/cellulitis). Promote wound healing. Minimize pain. Preserve limb. Topical Therapy: Considerations/Options Avoid occlusive dressings: Use dressings that permit easy, frequent visualization of the wound. Aggressively treat infection. Dry, non-infected wounds with stable, fixed eschar, necrosis; or a stable blister: o Maintain, keep dry, protect, no debridement. o Assess perfusion status and signs of infection. Infected, necrotic wounds: o Refer for revascularization/surgical removal of necrotic tissue and antibiotic therapy. o Do not rely on topical antibiotics as the sole therapy to treat infected, ischemic wounds. o Promptly institute culture-guided systemic antibiotics for patients with CLI and evidence of limb infection or cellulitis, and/or infected wounds. Open/draining wounds with necrotic tissue: o Consider a closely monitored trial of autolytic or enzymatic debridement. Open/draining wounds with exposed bones or tendons: o Consider a carefully monitored trial of moist, nonocclusive, absorbent, dressings. Open/draining, non-necrotic wounds: o Consider moist wound healing with non-occlusive, absorbent dressings. Lower-Extremity Neuropathic Disease (LEND) Wounds (WOCN, 2012) Prevent trauma/injury. Prevent, promptly identify, and manage complications (e.g., infection/cellulitis or osteomyelitis). Promote wound healing. Keep the periwound dry while maintaining a moist wound bed. Minimize pain. Preserve limb. Use dressings that maintain a moist surface, absorb exudate, and allow easy visualization. Use occlusive dressings cautiously. Aggressively treat infection/cellulitis, including fungal infection. Do not rely on topical antimicrobials alone to treat cellulitis, but they could be used in conjunction with systemic antimicrobials; use of antimicrobials should be culture-guided. Debride focal callus to reduce pressure. Debride avascular/necrotic tissue in nonischemic wounds. 10
11 Lower-Extremity Venous Disease (LEVD) Wounds (WOCN, 2011) Skin substitutes. Electrical stimulation. Ultrasound. Dermatology referral for unresponsive dermatitis/eczema after 2 weeks of appropriate therapy. Vascular/surgical referral for: o Infection/Cellulitis. o Non-healing wound after 4 weeks of appropriate therapy. o Venous thromboembolism. o Variceal bleeding. o Intractable pain. o Atypical appearance or location of wound. Lower-Extremity Arterial Disease (LEAD) Wounds (WOCN, 2014) Adjunctive Therapy Hyperbaric oxygen therapy. Arterial flow augmentation (i.e., intermittent pneumatic compression). Electrotherapy. Low frequency ultrasound. Spinal cord stimulation. Lower-Extremity Neuropathic Disease (LEND) Wounds (WOCN, 2012) Hyperbaric oxygen therapy. Skin substitutes. Topical negative pressure. Growth factor therapy. Surgery to correct structural deformities. Surgical debridement/implantation of antibiotic beads, spacers, or gels. Pain management specialists. Indications for Referral to Other Healthcare Providers for Additional Evaluation and Treatment Vascular/surgical referral: o Infected, ischemic wounds: Clinical signs of infection/cellulitis or suspected osteomyelitis. o Atypical appearance or location of wound. o Intractable pain. o Wounds and/or edema in mixed venous/arterial disease that fail to respond to compression therapy or worsen. o Absence of both dorsalis pedis and posterior tibial pulses. o ABI less than 0.90 plus one or more of the following: Wound fails to improve with 2 to 4 weeks of appropriate therapy, severe ischemic pain, and/or intermittent claudication. o ABI less than o ABI greater than 1.30 or non-compressible arteries. Urgent vascular/surgical referral for symptoms of acute limb ischemia; CLI (ABI less than 0.40; ankle pressure less than 50 mmhg; TP less than 30 mmhg/or less than 50 mmhg if diabetes present; TcPO2 less than 30 mmhg); and/or gangrene. Refer patients who smoke/use tobacco and have a loss of protective sensation to foot care specialists and for tobacco cessation education/counselling. Refer patients with gait abnormalities to a qualified pedorthic professional for shoe or device customization. Vascular/surgical referral: o Infection/Cellulitis or suspected osteomyelitis (i.e., probe to the bone). o Atypical appearance or location of wound. o Symptoms/new onset of Charcot fracture. o Musculoskeletal/structural foot deformities. o ABI less than 0.90 and no response to 2 to 4 weeks of conservative wound care. o ABI less than o ABI greater than 1.30 or non-compressible arteries. Urgent vascular/surgical referral for symptoms of acute limb ischemia, CLI, and/or gangrene. 11
12 References Wound, Ostomy and Continence Nurses Society. (2011). Guideline for management of wounds in patients with lower-extremity venous disease. WOCN Clinical Practice Guideline Series 4. Mt. Laurel, NJ: Author. Wound, Ostomy and Continence Nurses Society. (2012). Guideline for management of wounds in patients with lower-extremity neuropathic disease. WOCN Clinical Practice Guideline Series 3. Mt. Laurel, NJ: Author. Wound, Ostomy and Continence Nurses Society. (2013). A quick reference guide for lowerextremity wounds: Venous, arterial, and neuropathic. Mt. Laurel, NJ: Author. Wound, Ostomy and Continence Nurses Society. (2014). Guideline for management of wounds in patients with lower-extremity arterial disease. WOCN Clinical Practice Guideline Series 1. Mt. Laurel, NJ: Author. 12
10/9/2015. Differential Assessment of Lower Extremity Wounds. Disclosure Statement. Program Objectives
 3M 2015. All Rights Reserved 3M 2015. All Rights Reserved 2 3M 2015. All Rights Reserved 3 Differential Assessment of Lower Extremity Wounds Presented by: Lynn Peterson RN, BSN, CWOCN 3M Health Care November
3M 2015. All Rights Reserved 3M 2015. All Rights Reserved 2 3M 2015. All Rights Reserved 3 Differential Assessment of Lower Extremity Wounds Presented by: Lynn Peterson RN, BSN, CWOCN 3M Health Care November
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Lower Extremity Venous Disease (LEVD)
 Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Arterial & Venous Ulcers. A Comprehensive Review Assessment & Management
 Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Address: Left Leg. other: Nails: thick yellow brittle fungus abnormal thick yellow brittle fungus abnormal
 South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Peripheral Arterial Disease Extremity
 Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
Rapid Foot Screening
 GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Person s Name: ID Number: Date:
 South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
Organization of Wound Care Nurses
 Organization of Wound Care Nurses www.woundcarenurses.org Lower extremity arterial disease refers to disorders affecting the leg arteries Also known as PVD, PAOD, and PAD Cardiovascular Disease (CVD) is
Organization of Wound Care Nurses www.woundcarenurses.org Lower extremity arterial disease refers to disorders affecting the leg arteries Also known as PVD, PAOD, and PAD Cardiovascular Disease (CVD) is
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
The Diabetic Foot Latest Statistics
 The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT
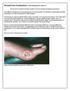 Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
Aetiology Macroangiopathy occurs mainly distally ie Popliteal artery There is arterial wall calcification Microangiopathy is less common
 DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital
 Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Pressure Ulcer Staging. Staging of Wounds are based on the deepest level of tissue damage
 Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Our Vision NADA BoD Strategic Planning Session -
 Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Diabetes Foot and Skin Care. Diabetes and the feet. Foot problems: Major cause of morbidity and mortality
 Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Frank K. Galbraith D.P.M. Dr. Frank Galbraith
 Frank K. Galbraith D.P.M. Dr. Frank Galbraith Ingrown Toenails Paronychia (infected toenail) Onychomycosis (fungal nails) From improper trimming, leaving nail sharp corners Curved nails Thick (Hypertrophic)
Frank K. Galbraith D.P.M. Dr. Frank Galbraith Ingrown Toenails Paronychia (infected toenail) Onychomycosis (fungal nails) From improper trimming, leaving nail sharp corners Curved nails Thick (Hypertrophic)
Clinical Examination of VASCULAR PATIENTS. Stephanie Hirst & Alexander Sunde
 Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Advanced Clinical Solutions. Pressure Ulcer. Carilex Medical Group 1
 Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
Diabetes - Foot Care
 Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Leg Ulcer Case Study
 Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Recognizing Pressure Injury
 Recognizing Pressure Injury Karen Zulkowski, DNS, RN Hawaii Recorded on March 8, 2017 1 A Little About Myself Executive editor of the Journal of the World Council of Enterostomal Therapists (JWCET) and
Recognizing Pressure Injury Karen Zulkowski, DNS, RN Hawaii Recorded on March 8, 2017 1 A Little About Myself Executive editor of the Journal of the World Council of Enterostomal Therapists (JWCET) and
Wound Care per HHVNA Wound Product Formulary
 Venous Ulcers ABI of 0.9-1.2 = normal blood flow An ABI MUST be obtained prior to inititiation of compression therapy. Compression is the Gold Standard of care to promote wound of venous ulcers. Elevation
Venous Ulcers ABI of 0.9-1.2 = normal blood flow An ABI MUST be obtained prior to inititiation of compression therapy. Compression is the Gold Standard of care to promote wound of venous ulcers. Elevation
Bacterial Burden (Bioburden) The metabolic load imposed by bacteria in tissue.
 Glossary Ankle Brachial Index (ABI) Is a numerical figure which indicates a quantifiable pressure index. The pressure index is determined by means of Doppler Ultra Sound. The ABI is obtained by dividing
Glossary Ankle Brachial Index (ABI) Is a numerical figure which indicates a quantifiable pressure index. The pressure index is determined by means of Doppler Ultra Sound. The ABI is obtained by dividing
Treat the whole patient, not just the hole in the patient! 3/21/2017 CAN YOU CONNECT THE DOTS?? PHILOSOPHY OBJECTIVES
 CAN YOU CONNECT THE DOTS?? Boone Hospital Wound Healing Center Kimberly Jamison, MD, FACP, FAPWCA, PCWC Kim Mitchell, RN, BSN OBJECTIVES Describe the basic concepts of chronic wound care to ensure an optimal
CAN YOU CONNECT THE DOTS?? Boone Hospital Wound Healing Center Kimberly Jamison, MD, FACP, FAPWCA, PCWC Kim Mitchell, RN, BSN OBJECTIVES Describe the basic concepts of chronic wound care to ensure an optimal
Lower Leg Ulceration. Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network;
 Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
How to manage leg ulcers in the elderly
 How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease
 Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide
 Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide Diabetes, Obesity & Nutrition Strategic Clinical Network Version 1.0 Acknowledgement This healthcare provider s guide has been adapted from
Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide Diabetes, Obesity & Nutrition Strategic Clinical Network Version 1.0 Acknowledgement This healthcare provider s guide has been adapted from
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY CLINICAL GUIDELINES TABLE OF CONTENTS. Diabetes Mellitus and Podiatric Care 2
 NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY 2012-2013 CLINICAL GUIDELINES TABLE OF CONTENTS CONDITION PAGE(S) Diabetes Mellitus and Podiatric Care 2 Fractures 3-4 Heel Pain (Posterior) Retrocalcaneal
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY 2012-2013 CLINICAL GUIDELINES TABLE OF CONTENTS CONDITION PAGE(S) Diabetes Mellitus and Podiatric Care 2 Fractures 3-4 Heel Pain (Posterior) Retrocalcaneal
Localized collection of pus in a cavity
 Localized collection of pus in a cavity Loss of feeling or sensation induced to permit surgery Common example: Injection given to numb up the toe prior to performing an ingrown toenail procedure Mechanical
Localized collection of pus in a cavity Loss of feeling or sensation induced to permit surgery Common example: Injection given to numb up the toe prior to performing an ingrown toenail procedure Mechanical
Due to Perimed s commitment to continuous improvement of our products, all specifications are subject to change without notice.
 A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
Helen Gelly, MD, FUHM, FCCWS
 Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre.
 Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Preventing Foot Ulcers in the Neuropathic Diabetic Foot. Glossary of Terms
 Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
National Clinical Conference 2018 Baltimore, MD
 National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
AGONY FEET. The. of the. Prevention and management of diabetic foot ulcers
 The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
Arterial Leg Ulcer Clinical Pathway
 Waterloo Wellington Integrated Wound Care Program Evidence-Based Wound Care Arterial Leg Ulcer Clinical Pathway 0-7 Days Expected Outcomes Notes Patient admitted to service/facility Most Responsible Physician(MRP)/Nurse
Waterloo Wellington Integrated Wound Care Program Evidence-Based Wound Care Arterial Leg Ulcer Clinical Pathway 0-7 Days Expected Outcomes Notes Patient admitted to service/facility Most Responsible Physician(MRP)/Nurse
Peripheral Neuropathy
 Peripheral Neuropathy Neuropathy affects 30-50% of patient population with diabetes and this prevalence tends to increase proportionally with duration of diabetes and dependant on control. Often presents
Peripheral Neuropathy Neuropathy affects 30-50% of patient population with diabetes and this prevalence tends to increase proportionally with duration of diabetes and dependant on control. Often presents
10/19/2017. Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI. Consultant with J&J-Depuy-Synthesis
 Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Total Contact Cast System
 Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
I also call this lecture
 I also call this lecture GO BUCKS!!! My Background Cornerstone University Grand Rapids, MI Kent State University College of Podiatric Medicine (OCPM) Florida Hospital East Orlando 3 year surgical residency
I also call this lecture GO BUCKS!!! My Background Cornerstone University Grand Rapids, MI Kent State University College of Podiatric Medicine (OCPM) Florida Hospital East Orlando 3 year surgical residency
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
EDUCATION. Peripheral Artery Disease
 EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
Perfusion Assessment in Chronic Wounds
 Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
How can DIABETES affect my FEET? Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014
 Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014 Dr. Michael Yan, MD, CCFP Clinical Lecturer, Department of Family Medicine, University of
Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014 Dr. Michael Yan, MD, CCFP Clinical Lecturer, Department of Family Medicine, University of
Podiatry in Practice. Alan M. Singer, DPM, FACFAS
 Podiatry in Practice Alan M. Singer, DPM, FACFAS Podiatry in Practice Alan Singer, D.P.M. UNIVERSITY PODIATRY GROUP Onychomycosis Anti-fungals Onychocryptosis (Ingrown Nails) Ingrown Nails Partial Nail
Podiatry in Practice Alan M. Singer, DPM, FACFAS Podiatry in Practice Alan Singer, D.P.M. UNIVERSITY PODIATRY GROUP Onychomycosis Anti-fungals Onychocryptosis (Ingrown Nails) Ingrown Nails Partial Nail
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy.
 Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Successful Wound Management Strategies : An Introduction. Alex Khan, APRN ACNS-BC. Organization of Wound Care Nurses
 Successful Wound Management Strategies : An Introduction Alex Khan, APRN ACNS-BC Organization of Wound Care Nurses www.woundcarenurses.org Goals & Objectives The role and importance of wound care management
Successful Wound Management Strategies : An Introduction Alex Khan, APRN ACNS-BC Organization of Wound Care Nurses www.woundcarenurses.org Goals & Objectives The role and importance of wound care management
Diabetes Mellitus and the Associated Complications
 Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Disclosures. Critical Limb Ischemia. Vascular Testing in the CLI Patient. Vascular Testing in Critical Limb Ischemia UCSF Vascular Symposium
 Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
WOUND MANAGEMENT. A Clinical Perspective. Furqan Alex Khan, APRN ACNS-BC MSN
 WOUND MANAGEMENT A Clinical Perspective Furqan Alex Khan, APRN ACNS-BC MSN alexkhan@prohealthcare.us Ket Harris Davis, APRN FNP-C DNP keturahnp@keturah-hms.com. Objectives Understand types of wounds Discuss
WOUND MANAGEMENT A Clinical Perspective Furqan Alex Khan, APRN ACNS-BC MSN alexkhan@prohealthcare.us Ket Harris Davis, APRN FNP-C DNP keturahnp@keturah-hms.com. Objectives Understand types of wounds Discuss
DIABETES AND FOOTCARE
 DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
The Peripheral Vascular System
 The Peripheral Vascular System Anatomy and Physiology Arteries Arteries contain 3 concentric layers of tissue: - the intima - the media - the adventitia The intima The endothelium of the intima has metabolic
The Peripheral Vascular System Anatomy and Physiology Arteries Arteries contain 3 concentric layers of tissue: - the intima - the media - the adventitia The intima The endothelium of the intima has metabolic
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
DIABETIC FOOT BOOK THE. A guide to keeping it simple and preventing complications. Practice genii. the Diabetic Foot Book
 DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS
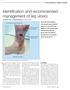 Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Bed Sores No More! Pressure Injuries Risk Factors and Updated Staging Methodology. Nicolle Samuels, MSPT, CLT-LANA, CWS, CKTP
 Bed Sores No More! Pressure Injuries Risk Factors and Updated Staging Methodology Nicolle Samuels, MSPT, CLT-LANA, CWS, CKTP Objectives Understand updated definitions as well as staging and classification
Bed Sores No More! Pressure Injuries Risk Factors and Updated Staging Methodology Nicolle Samuels, MSPT, CLT-LANA, CWS, CKTP Objectives Understand updated definitions as well as staging and classification
2 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?)
 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Ann Rambusch, MSN, HCS D, HCS O, RN June 28, 2016 1 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Understanding NPUAP
Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Ann Rambusch, MSN, HCS D, HCS O, RN June 28, 2016 1 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Understanding NPUAP
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Pressure Ulcer. Patient information leaflet. Category I. Category II. Category III. Category IV. Unstageable. Deep Tissue Injury
 Pressure Ulcers Patient information leaflet Pressure Ulcer Category I Category II Category III Category IV Unstageable Deep Tissue Injury Introduction This leaflet is about pressure ulcers and includes
Pressure Ulcers Patient information leaflet Pressure Ulcer Category I Category II Category III Category IV Unstageable Deep Tissue Injury Introduction This leaflet is about pressure ulcers and includes
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Pressure Injury Staging Update 2016
 Pressure Injury Staging Update 2016 A Review of the New Changes for Pressure Injury Documentation and Staging Jeanne Terefenko, BSN, RN, CWOCN Ext. 5855 Pressure Ulcer Staging Updates: In April, 2016,
Pressure Injury Staging Update 2016 A Review of the New Changes for Pressure Injury Documentation and Staging Jeanne Terefenko, BSN, RN, CWOCN Ext. 5855 Pressure Ulcer Staging Updates: In April, 2016,
Additional Information S-55
 Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Diabetic Foot Pathophysiology. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Garland Green, MD Interventional Cardiologist. Impact of PAD: Prevalence, Risk Factors, Testing, and Medical Management
 Garland Green, MD Interventional Cardiologist Impact of PAD: Prevalence, Risk Factors, Testing, and Medical Management Peripheral Arterial Disease Affects over 8 million Americans Affects 12% of the general
Garland Green, MD Interventional Cardiologist Impact of PAD: Prevalence, Risk Factors, Testing, and Medical Management Peripheral Arterial Disease Affects over 8 million Americans Affects 12% of the general
Project I - Background Worksheet. Team Members: Kira Brown, Paige Fallu. Clinical problem Diabetic Foot Ulcers
 Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
