Effect of primary Phacoviscocanalostomy/ Viscocanalostomy on intraocular pressure of normal tension glaucoma patients: 3- year results
|
|
|
- Roy Barnett
- 6 years ago
- Views:
Transcription
1 Ho et al. BMC Ophthalmology (2017) 17:201 DOI /s y RESEARCH ARTICLE Open Access Effect of primary Phacoviscocanalostomy/ Viscocanalostomy on intraocular pressure of normal tension glaucoma patients: 3- year results Derek Kwun-hong Ho, Adesuwa Garrick, Seemeen Aazem and Divya Mathews * Abstract Background: The objective of this study was to evaluate the efficacy of Viscocanalostomy/Phacoviscocanalostomy (VC/PVC) in lowering intraocular pressure (IOP) in Normal Tension Glaucoma (NTG) patients. Methods: Retrospective electronic database review of patients who underwent VC/PVC for NTG between December 2009 and November 2011 at Stanley eye unit in Abergele Hospital. Goldmann applanation tonometry (GAT) was used for all IOP measurements which were taken at the time of listing for surgery and at 1 day, 1 week, 1 month, then 3-monthly up to 1 year, then half-yearly up to 3 years post operatively. Statistical analysis was performed using unpaired t-test. A P value of <0.05 was accepted as the level of significance. Results: Operations were performed on 94 eyes from 67 patients over the study period. The mean age at the time of surgery was 76.4 years. Pre-operative IOP was ± 2.19 mmhg (range mmhg). 3 year follow-up showed a mean IOP of ± 2.22 mmhg (range 8 18 mmhg). By year 3, 17 patients needed laser goniopuncture and 25 patients needed antiglaucoma drops. IOP was reduced by 24.4% at 3 years post-surgery, which was statistically significant (p < ). Conclusions: From our results, which show a 24.5% reduction in IOP at 3 years with 12% complication rate, we propose that a logical surgical management for NTG patients would be viscocanalostomy, thereby keeping trabeculectomy as an alternative. Keywords: Non-penetrating, Viscocanalostomy, Phacoviscocanalostomy, Normal tension glaucoma, Trabeculectomy Background Glaucoma is a progressive optic neuropathy which may be due, in part, to an elevated intraocular pressure (IOP) with pathognomonic changes in the optic disc and visual fields. Normal tension glaucoma (NTG), a type of primary open angle glaucoma, can be defined with the following criteria [1]. 1. A mean IOP off treatment consistently equal to or less than 21 mmhg on diurnal testing, with no single measurement greater than 24 mmhg. 2. Open drainage angles on gonioscopy * Correspondence: div_mat29@yahoo.co.uk Stanley Eye Unit, Abergele Hospital, Llanfair Road, Abergele, Conwy LL22 8DP, UK 3. Absence of any secondary cause for a glaucomatous optic neuropathy 4. Typical optic disc damage with glaucomatous cupping and loss of neuroretinal rim 5. Visual field defect compatible with the glaucomatous cupping (disc/field correlation) 6. Progression of glaucomatous damage. Apart from a low/normal IOP, NTG patients are more likely to have systemic microvascular or circulatory abnormalities, such as migraine, exaggerated vasospastic response to cold recovery test, higher incidence of cerebral vascular ischemia, systemic hypertension or hypotension, or other vascular abnormalities like disc haemorrhage and peripapillary atrophy [2]. The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Ho et al. BMC Ophthalmology (2017) 17:201 Page 2 of 6 Following a diagnosis of NTG, (as in all forms of glaucoma) the first line of treatment is antiglaucoma drops to reduce the IOP to low teens or, in some cases, single digits. Progression, despite treatment, warrants additional antiglaucoma drops. Surgical intervention is the next option should topical treatment fail to slow progression. In the past, trabeculectomy was the only surgical option for progressive glaucoma. More recently, the concept of nonpenetrating glaucoma surgery has gained interest for its potential to limit some of the complications associated with more invasive procedures to lower IOP [3]. In the mid 1990 s, Stegmann et al. introduced viscocanalostomy (VC) and reported successful results in glaucoma patients from Africa [4]. The advantage of doing VC is that it can also be combined with cataract surgery (PVC) with good surgical outcomes. In comparison, phacotrabeculectomy has more complications and requires more intervention / manipulation to ensure success [5]. In VC, entry into the anterior chamber is avoided. This prevents over filtration, hypotony and as a result fewer post-operative follow up visits. However, there have been debates on the longevity as well as the efficacy of VC [6]. Few publications reported on the efficacy of VC/PVC in NTG patients. The objective of this study was to evaluate the efficacy of VC/PVC in lowering IOP in NTG patients. Methods Patients who underwent VC/PVC as their primary glaucoma surgery for NTG between December 2009 and November 2011, at the Stanley eye unit in Abergele Hospital, were identified from the intranet database retrospectively with no control arm. The study followed the tenets of the Declaration of Helsinki. The indication for surgery was progressive optic neuropathy, or visual fields, in patients on maximum topical antiglaucoma drops or could not tolerate antiglaucoma drops, with IOP below 21 mmhg. All procedures were performed by a single surgeon (DM) under Subtenon s anaesthesia. VC/ PVC procedures were performed by the same surgeon as previously described [4]. Post-operative follow-up for non-complicated cases was on day 1, week 1, month 1 and then 3-monthly for the first year. In the immediate post-operative period, patients had topical steroids (G. prednisolone acetate 1%) on a reducing regimen and antibiotics (G. chloramphenicol 0.5%) for 4 weeks. IOP was measured with Goldmann Applanation Tonometry (GAT) at every visit and visual field was repeated 3 months after surgery. Laser goniopuncture (LGP) was performed if there was an increase in IOP. If an immediate drop in IOP was not achieved, antiglaucoma drops were commenced. Statistical analysis was performed using unpaired t-test and a P value of <0.05 was accepted as the level of significance. Results Ninety four eyes from 67 patients were identified, 30 of whom were male and 37 were female. The mean participant age was 76.4 ± 9.1 years (range years). Twenty five eyes had VC, of which 19 have previously undergone cataract operations, and 69 eyes had PVC. In total, 10 patients (11%) had inadvertent perforation of the Trabeculo-Descemet s Window (TDW). The average number of topical medication prior to surgery was 2.70 ± 0.91, with 8.9 ± 5.9 years on topical antiglaucoma medication (range from 2 months to 27 years). From the database we also identified additional 4 eyes who had previous trabeculectomy and 1 had vitrectomy/cataract surgery. These were excluded from the study. Mean pre-operative IOP was ± 2.19 mmhg (range mmhg). Post-operative IOP at 6 months was ± 2.05 mmhg (range 8 19 mmhg) with one patient needing laser gonio-puncture (LGP). At 12, 24 and 36 months, mean IOP was ± 2.35 mmhg (range 8 24 mmhg), ± 2.10 mmhg (range 9 18 mmhg) and ± 2.22 mmhg (range 8 18 mmhg) respectively (Fig. 1). This represents a 24.5% reduction in IOP over 3 years. Nine patients needed LGP and 4 patients were prescribed anti-glaucoma drops by year 1 as their IOP was suboptimal. By year 2, 16 patients were prescribed anti-glaucoma drops and 11 patients received LGP treatment. By the end of study period at year 3, 17 patients had LGP and 25 patients were given antiglaucoma drops (Table 1). There were 12 patients (13%) lost to follow-up by 12 months. This increased to 15 (16%) by year two and 19 (20%) by the end of the three-year study period. At 12 months, percentage decrease compared to the preoperative IOP was 24.8%, at 24 months the decrease was 26.0% and at 36 months 24.5%. Statistical analysis using unpaired t-test showed that IOP reduction was significant (p < ) (Table 1). The number of anti-glaucoma drops used at 36 months was 0.28 ± 0.58 compared to 2.66 ± 0.91 pre-operatively, 0.05 ± 0.22 at 12 months and 0.20 ± 0.46 at 24 months (Fig. 2). Fifty eight operated eyes (62%) were drop free at 36 months follow-up. As at 36 months follow-up, 17 eyes (18%) received LGP for sub-optimal IOP. Median time to perform LGP following VC/PVC was 12 months (range 6 36 months). Mean IOP by year 3 in this sub-group was ± 2.23 mmhg, reducing from the listing IOP of ± 1.90 mmhg, representing a reduction of 28%. 10 (59%) of these 17 eyes were also commenced on antiglaucoma drops, achieving an average IOP of ± 2.36 mmhg at 3 years. This compares to the 7 (41%) out of the 17 eyes, which maintained an average IOP of ± 2.12 mmhg without drops.
3 Ho et al. BMC Ophthalmology (2017) 17:201 Page 3 of 6 Fig. 1 Mean pre- and post-operative IOP following VC/PVC in NTG patients (m = month; yr. = years) 10 (11%) of 94 operated eyes had inadvertent intraoperative perforation of TDW. In this group, preoperative IOP was 18.4 ± 1.8 mmhg, reducing to 12.3 ± 1.7 mmhg at 6 months, 13.7 ± 1.9 mmhg at 12 months, 11.7 ± 2.8 mmhg at 24 months and 12.5 ± 2.7 mmhg at 36 months. Two patients needed LGP at 12 months and 4 were prescribed antiglaucoma drops by 36 months. Analysis using the unpaired t-test showed no statistical significance (p = 0.17) in IOP difference at 36 months, in the patients that had inadvertent perforation of the TDW and those that had an intact TDW, with 36 months IOP of 13.5 ± 2.1 mmhg. Comparing the pseudophakic patients who underwent VC and the patients who were rendered pseudophakic from their PVC surgeries, listing IOP for PVC patients was ± 2.33 mmhg while VC patients IOP was ± 1.96 mmhg (p = 0.97). By the end of the 3 year study period, final IOP were ± 2.22 mmhg and ± 2.36 mmhg for PVC and VC patients respectively (p = 0.27). This represents a reduction of 4.1 mmhg for PVC and 4.8 mmhg for VC cases (Fig. 3). No significant differences in post-operative IOP between the two groups were demonstrated. Overall, 1 patient needed conjunctiva resuturing at 1 week due to persistent leak. One patient required anterior chamber washout for hyphema 3 days post surgery and 1 other patient developed post operative cystoid macular oedema at 4 weeks. Four patients developed cystic blebs in spite of tight suturing of the flap possibly due to either thin superficial flaps or early suture dehiscence and scleral wound gape; however none of them required bleb refashioning. At 36 months, the average Mean deviation of visual field defect was ± (range 2.1 to 111.3) compared to an average of ± 6.76 (range to 1.88) before surgery. Visual field analysis using unpaired t-test gave a p-value of 0.11 (not statistically significant). Discussion The collaborative normal tension Glaucoma study reported slower rate of incident visual field loss in cases of 30% or more reduction in IOP in patients with NTG [7]. This is also supported in a paper by Bhandari et al. (8). Topical antiglaucoma drops and/laser trabeculoplasty should be used if IOP can be maintained at 30% or more below baseline [8, 9]. In a paper published by the NTG study group titled Intraocular pressure reduction in NTG patients, 57% of the patients achieved a 30% reduction in IOP with topical medication and/with laser trabeculoplasty while the other 43% needed as single fistulising procedure [10]. In contrast, Kamal and Hitchings are of the opinion that fistulising surgery with the use of an antiproliferative agent is the treatment most likely to achieve desired IOP reduction in NTG. They also recognise the risk of post-operative hypotony [1]. One might argue that our study involves a different cohort of patients, without any control group compared to other study populations making it difficult to interpret Table 1 Pre and post-operative IOP, with percentage reduction, at 12, 24 and 36 months Time Number of eyes (loss to follow-up) Mean IOP (SD) (mmhg) Percentage IOP reduction (%) Number of eyes received laser goniopuncture (LGP) Pre-op 94 (0) (±2.19) N/A N/A N/A 12 months 82 (12) (±2.35) 24.8% 9 (10%) 4 24 months 79 (15) (±2.10) 26.0% 11 (12%) months 75 (19) (±2.22) 24.5% 17 (18%) 20 Number of eyes receiving antiglaucoma drops
4 Ho et al. BMC Ophthalmology (2017) 17:201 Page 4 of 6 Fig. 2 Median number of anti-glaucoma medication prescribed to NTG patients pre- and post-operatively (m = month; yr. = years) the results. Bearing this in mind our results show that IOP reduction of 24.4% at 36 months with VC/PVC in NTG patients was comparable to that achieved with trabeculectomy. Hitchings et al. reports a reduction on IOP in NTG patients at just above 30% following trabeculectomy [11]. Similarly, Fontana et al. quotes a 25 30% reduction [12]. Membrey et al., at 2 years review, had a median reduction in IOP of 17 mmhg following trabeculectomy with 5 flourouracil and 15.3 mmhg following trabeculectomy with MMC [13]. The median results in our study was lower at 14 mmhg in year 1 and 3 with 13 mmhg in the 2nd year. LGP is done if IOP was increasing or if visual field progression was noticed. LGP has the potential to augment aqueous outflow through the TDW [14]. It is preferable to perform LGP rather than commencing topical medication ( rather too early than too late ) [14]. 17 (18%) of the 94 operated eyes had LGP by 3 years with a mean time to LGP from surgery of 19.9 ± 10.8 months. This is less than the 45% quoted for deep sclerectomy by Ambressin et al. with time to LGP from surgery of 12.4 ± 10 months. Our reduction in IOP post-lgp was also greater, at 28%, than the 20% quoted [15]. Ten patients (59%) were commenced on topical antiglaucoma medication as reduction in IOP following LGP was not sustained. Fistulising procedures have documented complications. Schultz et al. reported that hypotony occurred in 30% of patients during the post-operative follow-up period [16]. Others reported complications included choroidal effusion, hyphema, hypotony maculopathy, diplopia, bleb leak, blebitis. Song et al. acknowledges the potential complications of trabeculectomy but still maintain that it is the most effective method of achieving low IOPs [3]. One should remember that trabeculectomy also warrants frequent postoperative visits at least weekly in the early post-operative period [17]. And the further use of anti-proliferative agents at least once during the post-operative visit. This translates to a lot of clinic hours spent in the frequent review of these patients in comparison to day 1, 1 week, 4 weeks and 3 months post-operative visits for PVC/VC with no intervention in the form of needling or suture adjustment. Goniopunture may be needed forpvc/vcpatientsbutthis is usually one visit any time after 6 months post operatively. The time taken to perform the laser would be similar to do doing a YAG peripheral iridotomy. Fig. 3 Mean pre- and post-operative IOP following PVC and VC (m = month; yr. = years)
5 Ho et al. BMC Ophthalmology (2017) 17:201 Page 5 of 6 Ophthalmic surgeons have often raised concerns on the steep learning curve for PVC/VC. However, once mastered, PVC/VC takes no longer to complete than a trabeculectomy. In our surgeon s hands, both procedures take the same time. If perforation of the TDW did occur then a surgical Peripheral Iridotomy (PI) was performed as an additional step before completing the rest of the surgical steps of VC. This does not add any significant time to the surgery itself. Our complication rate was low. Ten eyes (11%) had inadvertent perforation of the TDW. Surgical PI was performed if the iris was presenting. Previous study by Park et al. documented micro-perforation rate of 21.4% and iris prolapsed from ruptured TDW in 5.9% [18]. Similar studies on Non-penetrating glaucoma surgery (NPGS) have reported tearing of the conjunctiva, hyphema, dellen, encapsulated bleb [19]. A recent paper by Grieshaber et al. reports complications following VC including choroidal detachment, gross hyphema and peripheral Descemet s detachment [20]. We acknowledge that there are a few weaknesses in the study. Firstly it is a retrospective study. In addition the patients in our study are from a different population, without any control group compared to other studies. This might make interpretation of our results with other study populations difficult. Postoperative evaluation including Tonometry was not masked and therefore subject to observer bias. The strengths of this retrospective study includes single surgeon, long term follow-up with a large number of patients compared to similar studies. Our study did not consider analysis of phakic versus pseudophakic eyes, as our participants included only 6 phakic eyes within the VC subgroup, compared to 88 pseudophakic eyes either from previous cataract operations or as a result of combined PVC surgeries. We considered the number of phakic eyes to be too low to draw any statistical conclusions with sufficient power. Not analysing visual acuity is one of the weaknesses of this study. However, visual acuity is not a reliable way of judging the success of glaucoma surgery. Also, visual field analysis in previous papers was carried out using various methods, making it difficult to directly compare the results of our visual field analysis. Membrey et al. observed that the use of MMC in trabeculectomy is associated with a greater risk on visual field progression despite a greater fall in IOP [11]. From our results, a logical surgical management for NTG patients would be viscocanalostomy keeping trabeculectomy as an alternative. We advocate viscocanalostomy for NTG patients where target IOP is in the mid-teens. In our practice, Trabeculectomy has its place in NTG patients where IOP of less than 12 mmhg is desirable. However, we advise cardiovascular workup and ensure compliance in such patients. Conclusions Our study on Viscocanalostomy / Phacoviscocanalostomy operations on 94 eyes with Normal Tension Glaucoma shows 24.4% IOP reduction at 3 years. We propose viscocanalostomy as the surgical management for NTG patients, thereby keeping trabeculectomy as an alternative. Abbreviations GAT: Goldmann applanation tonometry; IOP: Intraocular pressure; LGP: Laser goniopuncture; NPGS: Non-penetrating glaucoma surgery; NTG: Normal tension glaucoma; PI: Peripheral Iridotomy; PVC: Phacoviscocanalostomy; TDW: Trabeculo-Descemet s Window; VC: Viscocanalostomy Acknowledgments We would like to extend our thanks to Mr. C. S. Ng for his help and guidance on statistical analysis. Funding We report no funding. Availability of data and materials The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request. Authors contributions DM conceived of and designed the study. AG, DKHH and DM collected the data. DKHH performed statistical analysis. AG, DKHH, SA and DM contributed equally to the drafting, critical revision and final approval of the manuscript. Ethics approval and consent to participate This study was granted ethics approval from Wales Research Ethics Committee REC 5. REC reference number: 16/WA/0345. Consent for publication Not applicable. Competing interests The authors declare that they have no competing interest. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Received: 9 July 2017 Accepted: 1 November 2017 References 1. Kamal D, Hitchings R. Normal tension glaucoma a practical approach. Br J Ophthalmol. 1998;82(7): Daugeliene L, Yamamoto T, Kitazawa Y. Effect of trabeculectomy on visual field in progressive normal-tension glaucoma. Jpn J Ophthalmol. 1998;42(4): Song BJ, Caprioli J. New directions in the treatment of normal tension glaucoma. Indian J Ophthalmol. 2014;62(5): Stegmann R, Pienaar A, Miller D. Viscocanalostomy for open-angle glaucoma in black African patients. J Cataract Refract Surg. 1999;25(3): Paul C, Sengupta S, Paul A. Complications of Phacoemulsification vs Phacotrabeculectomy in the treatment of chronic angle closure glaucoma with concomitant cataract. Int J Innov Res Dev. 2013;2(9): Hondur A, Onol M, Hasanreisoglu B. Nonpenetrating glaucoma surgery: meta-analysis of recent results. J Glaucoma. 2008;17(2): Collaborative Normal-Tension Glaucoma Study Group. The effectiveness of intraocular pressure reduction in the treatment of normal-tension glaucoma. Am J Ophthalmol. 1998;126(4): Bhandari A, Crabb DP, Poinoosawmy D, et al. Effect of surgery on visual field progression in normal-tension glaucoma. Ophthalmology. 1997; 104(7):
6 Ho et al. BMC Ophthalmology (2017) 17:201 Page 6 of 6 9. Geijssen HC. Studies on normal pressure glaucoma. Amsterdam: Kugler; Schulzer M, The Normal Tension Glaucoma Study Group. Intraocular pressure reduction in normal-tension glaucoma patients. Ophthalmology. 1992;99(9): Hitchings RA, Wu J, Poinoosawmy D, et al. Surgery for normal tension glaucoma. Br J Ophthalmol. 1995;79(5): Fontana L, Viswanathan AC, Poinooswamy D, et al. Surgery for normal tension glaucoma. Target Intraocular Pressure and Visual Field Progression Acta Ophthalmol Scand Suppl. 1997;224: Membrey WL, Bunce C, Poinoosawmy DP, et al. Glaucoma surgery with or without adjunctive antiproliferatives in normal tension glaucoma: 2 visual field progression. Br J Ophthalmol. 2001;85(6): Tam DY, Barnebey HS, Ahmed II. Nd: YAG laser goniopuncture: indications and procedure. J Glaucoma. 2013;22(8): Ambresin A, Shaarawy T, Mermoud A. Deep sclerectomy with collagen implant in one eye compared with trabeculectomy in the other eye of the same patient. J Glaucoma. 2002;11(3): Schultz SK, Iverson SM, Shi W, et al. Safety and efficacy of achieving singledigit intraocular pressure targets with filtration surgery in eyes with progressive normal-tension glaucoma. J Glaucoma. 2016;25(2): Murdoch I. Post-operative management of trabeculectomy in the first three months. Community Eye Health. 2012;25(79 80): Park M, Tanito M, Nishikawa M, et al. Ultrasound biomicroscopy of intrascleral lake after viscocanalostomy and cataract surgery. J Glaucoma. 2004;13(6): Suominen S, Harju M, Ihanamäki T, et al. The effect of deep sclerectomy on intraocular pressure of normal-tension glaucoma patients: 1-year results. Acta Ophthalmol. 2010;88(1): Grieshaber MC, Peckar C, Pienaar A, et al. Long-term results of up to 12 years of over 700 cases of viscocanalostomy for open-angle glaucoma. Acta Ophthalmol. 2015;93(4): Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Glaucoma surgery with or without adjunctive antiproliferatives in normal tension glaucoma: 2 Visual field progression
 696 Glaucoma Unit, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK W L Membrey C Bunce D P Poinoosawmy F W Fitzke R A Hitchings Correspondence to: R A Hitchings roger.hitchings@virgin.net Accepted
696 Glaucoma Unit, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK W L Membrey C Bunce D P Poinoosawmy F W Fitzke R A Hitchings Correspondence to: R A Hitchings roger.hitchings@virgin.net Accepted
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA
 EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective cohort study
 Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
EXP11677SK. Financial Disclosure. None to be Declared EXP11677SK
 Financial Disclosure None to be Declared Presentation overview Glaucoma Surgical History Complications of trabeculectomy Express Device Specifications Surgical Steps Clinical advantages, indications and
Financial Disclosure None to be Declared Presentation overview Glaucoma Surgical History Complications of trabeculectomy Express Device Specifications Surgical Steps Clinical advantages, indications and
Glaucoma surgery with or without adjunctive antiproliferatives in normal tension glaucoma: 1 Intraocular pressure control and complications
 586 Glaucoma Unit, Moorfields Eye Hospital, City Road, London ECV 2PD W L Membrey D P Poinoosawmy C Bunce R A Hitchings Correspondence to: R A Hitchings Roger.Hitchings@virgin.net Accepted for publication
586 Glaucoma Unit, Moorfields Eye Hospital, City Road, London ECV 2PD W L Membrey D P Poinoosawmy C Bunce R A Hitchings Correspondence to: R A Hitchings Roger.Hitchings@virgin.net Accepted for publication
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of ab externo canaloplasty for primary open-angle glaucoma Primary open-angle glaucoma
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of ab externo canaloplasty for primary open-angle glaucoma Primary open-angle glaucoma
Combined phacoemulsification and viscocanalostomy with Ologen implant versus combined phacoemulsification and viscocanalostomy
 Gad et al. BMC Ophthalmology (2019) 19:45 https://doi.org/10.1186/s12886-019-1049-6 RESEARCH ARTICLE Combined phacoemulsification and viscocanalostomy with Ologen implant versus combined phacoemulsification
Gad et al. BMC Ophthalmology (2019) 19:45 https://doi.org/10.1186/s12886-019-1049-6 RESEARCH ARTICLE Combined phacoemulsification and viscocanalostomy with Ologen implant versus combined phacoemulsification
Long-term Results of Deep Sclerectomy with Small Collagen Implant in Korean
 pissn: 0-842 eissn: 202-82 Korean J Ophthalmol 20;27():4-8 http://dx.doi.org/0.4/kjo.27..4 Original Article Long-term Results of Deep Sclerectomy with Small Collagen Implant in Korean Seungsoo Rho,2, Sung
pissn: 0-842 eissn: 202-82 Korean J Ophthalmol 20;27():4-8 http://dx.doi.org/0.4/kjo.27..4 Original Article Long-term Results of Deep Sclerectomy with Small Collagen Implant in Korean Seungsoo Rho,2, Sung
MORE ON COMBINING OR NOT COMBINING...
 MORE ON COMBINING OR NOT COMBINING... A. GALAND* At the XVIII Congress of the European Society of Cataract and Refractive Surgeons (ESCRS) in Brussels, September 2 nd -6 th 2000, I was in charge of organizing
MORE ON COMBINING OR NOT COMBINING... A. GALAND* At the XVIII Congress of the European Society of Cataract and Refractive Surgeons (ESCRS) in Brussels, September 2 nd -6 th 2000, I was in charge of organizing
Clinical Study Deep Sclerectomy with Goniosynechiolysis Ab Interno for Chronic Glaucoma Associated with Peripheral Anterior Synechiae
 Ophthalmology Volume 2015, Article ID 625719, 5 pages http://dx.doi.org/10.1155/2015/625719 Clinical Study Deep Sclerectomy with Goniosynechiolysis Ab Interno for Chronic Glaucoma Associated with Peripheral
Ophthalmology Volume 2015, Article ID 625719, 5 pages http://dx.doi.org/10.1155/2015/625719 Clinical Study Deep Sclerectomy with Goniosynechiolysis Ab Interno for Chronic Glaucoma Associated with Peripheral
TRABECULECTOMY. Dr. Sandra M. Johnson, MD
 TRABECULECTOMY Dr. Sandra M. Johnson, MD FILTRATION OPTIONS Trabeculotomy, Schlemn s canal, internal Deep Non-penetrating Sclerectomy filtering to a scleral lake, or viscocanulostomy Trabeculectomy shunting
TRABECULECTOMY Dr. Sandra M. Johnson, MD FILTRATION OPTIONS Trabeculotomy, Schlemn s canal, internal Deep Non-penetrating Sclerectomy filtering to a scleral lake, or viscocanulostomy Trabeculectomy shunting
Glaucoma is the second leading cause of blindness
 Int J Ophthalmol, Vol. 10, No. 1, Jan.18, 2017 www.ijo.cn Clinical Research Ex-PRESS implantation with phacoemulsification in POAG versus CPACG Jie Lan 1,2, Da-Peng Sun 2, Jie Wu 2, Ya-Ni Wang 2, Li-Xin
Int J Ophthalmol, Vol. 10, No. 1, Jan.18, 2017 www.ijo.cn Clinical Research Ex-PRESS implantation with phacoemulsification in POAG versus CPACG Jie Lan 1,2, Da-Peng Sun 2, Jie Wu 2, Ya-Ni Wang 2, Li-Xin
Corporate Medical Policy
 Corporate Medical Policy Viscocanalostomy and Canaloplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: viscocanalostomy_and_canaloplasty 11/2011 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Viscocanalostomy and Canaloplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: viscocanalostomy_and_canaloplasty 11/2011 6/2017 6/2018 6/2017 Description
Trabeculectomy A Review and 2 Year Follow Up
 ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
Trabeculectomy combined with cataract extraction: a follow-up study
 British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
Viscocanalostomy and Canaloplasty. Description. Section: Other Effective Date: July 15, 2015
 Subject: Viscocanalostomy and Canaloplasty Page: 1 of 10 Last Review Status/Date: June 2015 Viscocanalostomy and Canaloplasty Description Glaucoma surgery is intended to reduce intraocular pressure (IOP)
Subject: Viscocanalostomy and Canaloplasty Page: 1 of 10 Last Review Status/Date: June 2015 Viscocanalostomy and Canaloplasty Description Glaucoma surgery is intended to reduce intraocular pressure (IOP)
TRABECULECTOMY THE BEST AND WORST CANDIDATES
 TRABECULECTOMY THE BEST AND WORST CANDIDATES MICHAEL F. OATS, MD OPHTHALMIC CONSULTANTS OF BOSTON ASCRS 2014 FINANCIAL DISCLOSURES None TRABECULECTOMY Performed for over 100 years Most commonly performed
TRABECULECTOMY THE BEST AND WORST CANDIDATES MICHAEL F. OATS, MD OPHTHALMIC CONSULTANTS OF BOSTON ASCRS 2014 FINANCIAL DISCLOSURES None TRABECULECTOMY Performed for over 100 years Most commonly performed
AC & ACG Instruction Course Surgical Treatments for PACG
 AC & ACG Instruction Course Surgical Treatments for PACG Presented by APGS Clement C.Y. THAM Professor, The Chinese University of Hong Kong Chief of Service, Hong Kong Eye Hospital Deputy Secretary-General,
AC & ACG Instruction Course Surgical Treatments for PACG Presented by APGS Clement C.Y. THAM Professor, The Chinese University of Hong Kong Chief of Service, Hong Kong Eye Hospital Deputy Secretary-General,
D uring recent years the role of non-penetrating surgery in
 599 CLINICAL SCIENCE A prospective randomised trial of viscocanalostomy with and without implantation of a reticulated hyaluronic acid implant (SKGEL) in open angle glaucoma C Lüke, T S Dietlein, P C Jacobi,
599 CLINICAL SCIENCE A prospective randomised trial of viscocanalostomy with and without implantation of a reticulated hyaluronic acid implant (SKGEL) in open angle glaucoma C Lüke, T S Dietlein, P C Jacobi,
Phacoemulsification versus Trabeculectomy in Medically Uncontrolled Chronic Angle- Closure Glaucoma without Cataract
 Phacoemulsification versus Trabeculectomy in Medically Uncontrolled Chronic Angle- Closure Glaucoma without Cataract Clement C. Y. Tham, FRCS, 1,2,3 Yolanda Y. Y. Kwong, FRCS, 1,2,3 Nafees Baig, FRCS,
Phacoemulsification versus Trabeculectomy in Medically Uncontrolled Chronic Angle- Closure Glaucoma without Cataract Clement C. Y. Tham, FRCS, 1,2,3 Yolanda Y. Y. Kwong, FRCS, 1,2,3 Nafees Baig, FRCS,
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3%
 The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
These devices, when FDA approved, are covered for patients with glaucoma that is not adequately controlled with medical therapy.
 Medical Policy Title: Aqueous Shunts and ARBenefits Approval: 10/26/2011 Devices for Glaucoma Effective Date: 01/01/2012 Document: ARB0168 Revision Date: Code(s): 66174, Transluminal dilation of aqueous
Medical Policy Title: Aqueous Shunts and ARBenefits Approval: 10/26/2011 Devices for Glaucoma Effective Date: 01/01/2012 Document: ARB0168 Revision Date: Code(s): 66174, Transluminal dilation of aqueous
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of microinvasive subconjunctival insertion of a trans-scleral gelatin stent for primary
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of microinvasive subconjunctival insertion of a trans-scleral gelatin stent for primary
Deep sclerectomy with supraciliary hema implant (Esnoper V-2000): results and complications
 Deep sclerectomy with supraciliary hema implant (Esnoper V-2000): results and complications Jordi Loscos, Xavier Valldeperas, Klaus Langhor, Àngels Parera, Pau Romera, Antoni Sabala & Julio de la Cámara
Deep sclerectomy with supraciliary hema implant (Esnoper V-2000): results and complications Jordi Loscos, Xavier Valldeperas, Klaus Langhor, Àngels Parera, Pau Romera, Antoni Sabala & Julio de la Cámara
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
Subject Index. Canaloplasty aqueous outflow system evaluation 110, 111 complications 118, 119 historical perspective 109, 110
 Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
TRABECULECTOMY-GUIDED DEEP SCLERECTOMY. A NOVEL TECHNIQUE. AHMED MOSTAFA ABDELRAHMAN, M.D., F.R.C.S. (Edin.) Assistant Professor of Ophthalmology
 TRABECULECTOMY-GUIDED DEEP SCLERECTOMY. A NOVEL TECHNIQUE. AHMED MOSTAFA ABDELRAHMAN, M.D., F.R.C.S. (Edin.) Assistant Professor of Ophthalmology Department of Ophthalmology, Cairo University. Purpose:
TRABECULECTOMY-GUIDED DEEP SCLERECTOMY. A NOVEL TECHNIQUE. AHMED MOSTAFA ABDELRAHMAN, M.D., F.R.C.S. (Edin.) Assistant Professor of Ophthalmology Department of Ophthalmology, Cairo University. Purpose:
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Viscocanalostomy and Canaloplasty
 Viscocanalostomy and Canaloplasty Policy Number: 9.03.26 Last Review: 9/2014 Origination: 9/2012 Next Review: 9/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for
Viscocanalostomy and Canaloplasty Policy Number: 9.03.26 Last Review: 9/2014 Origination: 9/2012 Next Review: 9/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for
Conventional trabeculectomy has so far remained the
 ORIGINAL STUDY Results of CO 2 Laser-assisted Deep Sclerectomy as Compared With Conventional Deep Sclerectomy Gabriel Greifner, MD,*w Sylvain Roy, MD, PhD,*z and Andre Mermoud, MD* Purpose: To evaluate
ORIGINAL STUDY Results of CO 2 Laser-assisted Deep Sclerectomy as Compared With Conventional Deep Sclerectomy Gabriel Greifner, MD,*w Sylvain Roy, MD, PhD,*z and Andre Mermoud, MD* Purpose: To evaluate
Surgery for COEXISTING CATARACT AND GLAUCOMA:
 Surgery for COEXISTING CATARACT AND GLAUCOMA: UNEASY RELATIONSHIP Session: 20-107 Monday, April 20, 2015 Time: 8:00 AM-9:30 AM Room 7B (San Diego Convention Center) Course Instructors Ahmad K Khalil Alan
Surgery for COEXISTING CATARACT AND GLAUCOMA: UNEASY RELATIONSHIP Session: 20-107 Monday, April 20, 2015 Time: 8:00 AM-9:30 AM Room 7B (San Diego Convention Center) Course Instructors Ahmad K Khalil Alan
Comparative Study between Non Penetrating Glaucoma Surgery with and without Implant
 Original Research Article Comparative Study between Non Penetrating Glaucoma Surgery with and without Implant Sudhir S Pendke 1, Ravi A Chauhan 1, Rahul V Gokhale 1, Sanchit S Bhalgat 2 1 MS (Ophthalmology),
Original Research Article Comparative Study between Non Penetrating Glaucoma Surgery with and without Implant Sudhir S Pendke 1, Ravi A Chauhan 1, Rahul V Gokhale 1, Sanchit S Bhalgat 2 1 MS (Ophthalmology),
Is NTG different from POAG?
 Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Corporate Medical Policy
 Corporate Medical Policy Aqueous Shunts and Devices for Glaucoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: aqueous_shunts_and_devices_for_glaucoma 3/2010 6/2017 6/2018 6/2017
Corporate Medical Policy Aqueous Shunts and Devices for Glaucoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: aqueous_shunts_and_devices_for_glaucoma 3/2010 6/2017 6/2018 6/2017
Clinical Study XEN Glaucoma Implant with Mitomycin C 1-Year Follow-Up: Result and Complications
 Hindawi Journal of Ophthalmology Volume 2017, Article ID 5457246, 5 pages http://dx.doi.org/10.1155/2017/5457246 Clinical Study XEN Glaucoma Implant with Mitomycin C 1-Year Follow-Up: Result and Complications
Hindawi Journal of Ophthalmology Volume 2017, Article ID 5457246, 5 pages http://dx.doi.org/10.1155/2017/5457246 Clinical Study XEN Glaucoma Implant with Mitomycin C 1-Year Follow-Up: Result and Complications
Early results of modified nonpenetrating deep sclerectomy and phacoemulsification in the treatment of open angle glaucoma and cataract
 European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 72-79 Early results of modified nonpenetrating deep sclerectomy and phacoemulsification in the treatment of open angle glaucoma and cataract
European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 72-79 Early results of modified nonpenetrating deep sclerectomy and phacoemulsification in the treatment of open angle glaucoma and cataract
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): June 4, 2013 Most Recent Review Date (Revised): March 25, 2014 Effective Date: June 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): June 4, 2013 Most Recent Review Date (Revised): March 25, 2014 Effective Date: June 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of ab interno supraciliary microstent insertion with phacoemulsification for primary
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of ab interno supraciliary microstent insertion with phacoemulsification for primary
Coexisting Cataract with Glaucoma & Role of Phacotrabeculectomy. Dr Mudit Agrawal
 Coexisting Cataract with Glaucoma & Role of Phacotrabeculectomy Dr Mudit Agrawal Glaucoma and cataract often occur together,especially in elderly and each condition can influence management of the other.
Coexisting Cataract with Glaucoma & Role of Phacotrabeculectomy Dr Mudit Agrawal Glaucoma and cataract often occur together,especially in elderly and each condition can influence management of the other.
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Cronicon EC OPHTHALMOLOGY. Research Article Trephine Assisted Trabeculectomy Technique. Idrees* Introduction
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
Viscocanalostomy and Canaloplasty
 Viscocanalostomy and Canaloplasty Policy Number: 9.03.26 Last Review: 9/2017 Origination: 9/2012 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for
Viscocanalostomy and Canaloplasty Policy Number: 9.03.26 Last Review: 9/2017 Origination: 9/2012 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for
THE CURRENT TREATMENT OF GLAUCOMA IS DIrected
 Three-Year Follow-up of the Tube Versus Trabeculectomy Study STEVEN J. GEDDE, JOYCE C. SCHIFFMAN, WILLIAM J. FEUER, LEON W. HERNDON, JAMES D. BRANDT, AND DONALD L. BUDENZ, ON BEHALF OF THE TUBE VERSUS
Three-Year Follow-up of the Tube Versus Trabeculectomy Study STEVEN J. GEDDE, JOYCE C. SCHIFFMAN, WILLIAM J. FEUER, LEON W. HERNDON, JAMES D. BRANDT, AND DONALD L. BUDENZ, ON BEHALF OF THE TUBE VERSUS
Trabeculectomy is the most commonly performed surgery
 ORIGINAL STUDY Standard Trabeculectomy and Ex-PRESS Miniature Glaucoma Shunt: A Comparative Study and Literature Review Elad Moisseiev, MD, Eran Zunz, MD, Rotem Tzur, MD, Shimon Kurtz, MD, and Gabi Shemesh,
ORIGINAL STUDY Standard Trabeculectomy and Ex-PRESS Miniature Glaucoma Shunt: A Comparative Study and Literature Review Elad Moisseiev, MD, Eran Zunz, MD, Rotem Tzur, MD, Shimon Kurtz, MD, and Gabi Shemesh,
Trabeculectomy with ologen implant versus trabeculectomy with mitomycin-c in primary open angle glaucoma: A 2-year study
 World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Available online at: http://www.wjpsonline.org/ Original Article Trabeculectomy with ologen implant versus trabeculectomy
World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Available online at: http://www.wjpsonline.org/ Original Article Trabeculectomy with ologen implant versus trabeculectomy
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Canaloplasty in One Eye Compared With Viscocanalostomy in the Contralateral Eye in Patients With Bilateral Open-angle Glaucoma
 ORIGINAL STUDY Canaloplasty in One Eye Compared With in the Contralateral Eye in Patients With Bilateral Open-angle Glaucoma Norbert Josef Koerber, MD, PhD*w Purpose: To compare the safety and efficacy
ORIGINAL STUDY Canaloplasty in One Eye Compared With in the Contralateral Eye in Patients With Bilateral Open-angle Glaucoma Norbert Josef Koerber, MD, PhD*w Purpose: To compare the safety and efficacy
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
THE ISTENT t TRABECULAR MICRO-BYPASS STENT: A CASE SERIES
 THE ISTENT t TRABECULAR MICRO-BYPASS STENT: A CASE SERIES VANDEWALLE E.*, ZEYEN T.*, STALMANS I.* ABSTRACT Purpose: To evaluate the safety and effectiveness of a trabecular micro-bypass stent, the istent
THE ISTENT t TRABECULAR MICRO-BYPASS STENT: A CASE SERIES VANDEWALLE E.*, ZEYEN T.*, STALMANS I.* ABSTRACT Purpose: To evaluate the safety and effectiveness of a trabecular micro-bypass stent, the istent
Messages From the Advanced Glaucoma Intervention Study
 Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
CO 2 Laser-assisted Sclerectomy Surgery, Part II: Multicenter Clinical Preliminary Study
 ORIGINAL STUDY CO 2 Laser-assisted Sclerectomy Surgery, Part II: Multicenter Clinical Preliminary Study Noa Geffen, MD,*w Yokrat Ton, MD,*w Joshua Degani, PhD,z and Ehud I. Assia, MD*w Purpose: To evaluate
ORIGINAL STUDY CO 2 Laser-assisted Sclerectomy Surgery, Part II: Multicenter Clinical Preliminary Study Noa Geffen, MD,*w Yokrat Ton, MD,*w Joshua Degani, PhD,z and Ehud I. Assia, MD*w Purpose: To evaluate
Citation BMC Ophthalmology, 2016, v. 16, article no. 64
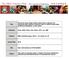 Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Aqueous Shunts and Stents for Glaucoma. (90321) (Formerly Aqueous Shunts for Glaucoma)
 Protocol Aqueous Shunts and Stents for Glaucoma (90321) (Formerly Aqueous Shunts for Glaucoma) Medical Benefit Effective Date: 01/01/13 Next Review Date: 01/14 Preauthorization* No Review Dates: 03/10,
Protocol Aqueous Shunts and Stents for Glaucoma (90321) (Formerly Aqueous Shunts for Glaucoma) Medical Benefit Effective Date: 01/01/13 Next Review Date: 01/14 Preauthorization* No Review Dates: 03/10,
CLASS-y Laser Treats Glaucoma
 Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Glaucoma. How is Glaucoma Diagnosed? Glaucoma Testing
 Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
Review of the Ahmed versus Baerveldt study 5-year treatment outcomes
 Perspective Page 1 of 5 Review of the Ahmed versus Baerveldt study 5-year treatment outcomes Victor Koh 1,2, Cecilia Maria Aquino 1, Paul Chew 1,2 1 Department of Ophthalmology, National University Hospital,
Perspective Page 1 of 5 Review of the Ahmed versus Baerveldt study 5-year treatment outcomes Victor Koh 1,2, Cecilia Maria Aquino 1, Paul Chew 1,2 1 Department of Ophthalmology, National University Hospital,
Long-term outcomes of argon laser photocoagulation in small size cyclodialysis cleft
 Han et al. BMC Ophthalmology (2015) 15:123 DOI 10.1186/s12886-015-0113-0 RESEARCH ARTICLE Open Access Long-term outcomes of argon laser photocoagulation in small size cyclodialysis cleft Jong Chul Han,
Han et al. BMC Ophthalmology (2015) 15:123 DOI 10.1186/s12886-015-0113-0 RESEARCH ARTICLE Open Access Long-term outcomes of argon laser photocoagulation in small size cyclodialysis cleft Jong Chul Han,
Baerveldt tube implantation following failed deep sclerectomy versus repeat deep sclerectomy.
 Baerveldt tube implantation following failed deep sclerectomy versus repeat deep sclerectomy. Authors: Bergin C, 1 Petrovic A, 1 Mermoud A, 2 Ravinet E, 2 Sharkawi E 1 1 Jules-Gonin Hôpital Ophtalmique,
Baerveldt tube implantation following failed deep sclerectomy versus repeat deep sclerectomy. Authors: Bergin C, 1 Petrovic A, 1 Mermoud A, 2 Ravinet E, 2 Sharkawi E 1 1 Jules-Gonin Hôpital Ophtalmique,
T rabeculectomy has been the filtration procedure of choice
 1012 SCIENTIFIC REPORT A randomised, prospective study comparing trabeculectomy with viscocanalostomy with adjunctive antimetabolite usage for the management of open angle glaucoma uncontrolled by medical
1012 SCIENTIFIC REPORT A randomised, prospective study comparing trabeculectomy with viscocanalostomy with adjunctive antimetabolite usage for the management of open angle glaucoma uncontrolled by medical
H E A L A C R O S S L I N K E D H A G L A U C O M A I N J E C TA B L E I M P L A N T Anteis Ophthalmology
 H E A L A C ROSS L I N K E D H A G L AU CO M A I N J ECTA B L E I M P L A N T Anteis Ophthalmology CONTENT 1 HEALAFLOW TECHNICAL SHEET 01 2 HEALAFLOW CHARACTERISTICS 02 3 HEALAFLOW GLAUCOMA FILTERING SURGERIES
H E A L A C ROSS L I N K E D H A G L AU CO M A I N J ECTA B L E I M P L A N T Anteis Ophthalmology CONTENT 1 HEALAFLOW TECHNICAL SHEET 01 2 HEALAFLOW CHARACTERISTICS 02 3 HEALAFLOW GLAUCOMA FILTERING SURGERIES
XEN GEL STENT MIGS 4/5/2018 OMAHA AND LINCOLN EYE AND LASER INSTITUTES XEN45 GEL STENT WHY ARE WE LOOKING FOR NEW INNOVATIONS IN GLAUCOMA SURGERY?
 XEN GEL STENT OMAHA AND LINCOLN EYE AND LASER INSTITUTES MARK R. YOUNG, M.D. April 7, 2018 QUESTION: Why are we looking for alternatives to current glaucoma treatment? Look at current surgical glaucoma
XEN GEL STENT OMAHA AND LINCOLN EYE AND LASER INSTITUTES MARK R. YOUNG, M.D. April 7, 2018 QUESTION: Why are we looking for alternatives to current glaucoma treatment? Look at current surgical glaucoma
Romanian Journal of Ophthalmology, Volume 59, Issue 4, October-December pp:
 Romanian Journal of Ophthalmology, Volume 59, Issue 4, October-December 2015. pp:243-247 GENERAL ARTICLE Intraoperative and postoperative complications in trabeculectomy, Clinical study Barac Ramona* **,
Romanian Journal of Ophthalmology, Volume 59, Issue 4, October-December 2015. pp:243-247 GENERAL ARTICLE Intraoperative and postoperative complications in trabeculectomy, Clinical study Barac Ramona* **,
Aqueous Shunts and Stents for Glaucoma
 Protocol Aqueous Shunts and Stents for Glaucoma (90321) Medical Benefit Effective Date: 04/01/14 Next Review Date: 01/15 Preauthorization No Review Dates: 03/10, 03/11, 07/11, 01/12, 09/12, 01/13, 01/14
Protocol Aqueous Shunts and Stents for Glaucoma (90321) Medical Benefit Effective Date: 04/01/14 Next Review Date: 01/15 Preauthorization No Review Dates: 03/10, 03/11, 07/11, 01/12, 09/12, 01/13, 01/14
Managing & Avoiding Post-Op Complications in Tube Surgeries
 Managing & Avoiding Post-Op Complications in Tube Surgeries K. Sheng Lim St. Thomas Hospital, London shenglim@gmail.com Current GDD Molteno 1969 Baerveldt 1990 Ahmed 1993 Current GDD GDD Plate Material
Managing & Avoiding Post-Op Complications in Tube Surgeries K. Sheng Lim St. Thomas Hospital, London shenglim@gmail.com Current GDD Molteno 1969 Baerveldt 1990 Ahmed 1993 Current GDD GDD Plate Material
Viscocanalostomy and Canaloplasty
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
V iscocanalostomy is a non-penetrating filtration procedure
 441 CLINICAL SCIENCE Five year results of viscocanalostomy T Shaarawy, C Nguyen, C Schnyder, A Mermoud... See end of article for authors affiliations... Correspondence to: André Mermoud, MD, Hôpital Ophtalmique
441 CLINICAL SCIENCE Five year results of viscocanalostomy T Shaarawy, C Nguyen, C Schnyder, A Mermoud... See end of article for authors affiliations... Correspondence to: André Mermoud, MD, Hôpital Ophtalmique
5-Fluorouracil as an Adjunct in Glaucoma Filtration Surgery in Younger Age Group
 Original Article 5-Fluorouracil as an Adjunct in Glaucoma Filtration Surgery in Younger Age Group Norin Iftikhar Bano, Tariq Mehmood Qureshi, Muhammad Tariq Khan, Harris Muzammil Ansari Pak J Ophthalmol
Original Article 5-Fluorouracil as an Adjunct in Glaucoma Filtration Surgery in Younger Age Group Norin Iftikhar Bano, Tariq Mehmood Qureshi, Muhammad Tariq Khan, Harris Muzammil Ansari Pak J Ophthalmol
Surgery for normal tension glaucoma
 42 British Journal of Ophthalmology 1995; 79: 42-46 ORIGINAL ARTICLES - Clinical science Moorfields Eye Hospital, City Road, London EClV 2PD R A Hitchings J Wu D Poinoosawmy A McNaught Correspondence to:
42 British Journal of Ophthalmology 1995; 79: 42-46 ORIGINAL ARTICLES - Clinical science Moorfields Eye Hospital, City Road, London EClV 2PD R A Hitchings J Wu D Poinoosawmy A McNaught Correspondence to:
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of trabecular stent bypass microsurgery for open-angle glaucoma Primary open-angle
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of trabecular stent bypass microsurgery for open-angle glaucoma Primary open-angle
PRINCIPLES AND TYPES OF GLAUCOMA SURGERIES
 PRINCIPLES AND TYPES OF GLAUCOMA SURGERIES DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING SAUD UNIVERSITY SAUDI ARABIA INTRODUCTION AQUEOUS
PRINCIPLES AND TYPES OF GLAUCOMA SURGERIES DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING SAUD UNIVERSITY SAUDI ARABIA INTRODUCTION AQUEOUS
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
Aqueous Shunts for the Treatment of Glaucoma
 TITLE: Aqueous Shunts for the Treatment of Glaucoma AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine University of California San
TITLE: Aqueous Shunts for the Treatment of Glaucoma AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine University of California San
Surgical outcomes of Trab and Tube for Uveitic glaucoma - Experience from a Tertiary Institution
 Surgical outcomes of Trab and Tube for Uveitic glaucoma - Experience from a Tertiary Institution Hye Jin Kwon, George YX Kong, William Tao, Lyndell Lim, Keith R Martin, Cathy Green, Jonathan Ruddle, Jonathan
Surgical outcomes of Trab and Tube for Uveitic glaucoma - Experience from a Tertiary Institution Hye Jin Kwon, George YX Kong, William Tao, Lyndell Lim, Keith R Martin, Cathy Green, Jonathan Ruddle, Jonathan
Optometrist's Guide to Glaucoma Surgery. Goals. Glaucoma Philosophy. I have no financial disclosures
 Optometrist's Guide to Glaucoma Surgery Anthony DeWilde, OD FAAO I have no financial disclosures 1 2 Goals Glaucoma Philosophy Glaucoma can be a visually debilitating disease. How glaucoma surgery works
Optometrist's Guide to Glaucoma Surgery Anthony DeWilde, OD FAAO I have no financial disclosures 1 2 Goals Glaucoma Philosophy Glaucoma can be a visually debilitating disease. How glaucoma surgery works
CHARTING THE NEW COURSE FOR MIGS
 CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure
 ORIGINAL ARTICLE Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure Jimmy S. M. Lai, 1 FRCS, FRCOphth, FHKAM (Ophthalmology), M.Med (Ophthalmology),
ORIGINAL ARTICLE Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure Jimmy S. M. Lai, 1 FRCS, FRCOphth, FHKAM (Ophthalmology), M.Med (Ophthalmology),
Contents Optic Nerve: The Glaucomatous Optic Nerve Optic Nerve: Clinical Examination Optic Nerve: Heidelberg Retinal Tomography
 Contents 1 Optic Nerve: The Glaucomatous Optic Nerve................... 1 1.1 Why Is the Optic Nerve Important in the Diagnosis and Management of Glaucoma?............................ 1 References.................................................
Contents 1 Optic Nerve: The Glaucomatous Optic Nerve................... 1 1.1 Why Is the Optic Nerve Important in the Diagnosis and Management of Glaucoma?............................ 1 References.................................................
Highlights On The Management Of Phacomorphic Glaucoma
 Highlights On The Management Of Phacomorphic Glaucoma Ahmed Aboueleinein What is phacomorphic glaucoma? It is a secondary angle closure glaucoma due to lens intumescence Advanced cataract or traumatic
Highlights On The Management Of Phacomorphic Glaucoma Ahmed Aboueleinein What is phacomorphic glaucoma? It is a secondary angle closure glaucoma due to lens intumescence Advanced cataract or traumatic
Challenging complications of valve implantation. Salah M Al-Mosallamy MD Assistant professor of ophthalmology 2014
 Challenging complications of valve implantation by Salah M Al-Mosallamy MD Assistant professor of ophthalmology 2014 PREDISPOSING FACTORS It is important to consider the case mix for these devices on dealing
Challenging complications of valve implantation by Salah M Al-Mosallamy MD Assistant professor of ophthalmology 2014 PREDISPOSING FACTORS It is important to consider the case mix for these devices on dealing
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE. Glaucoma: diagnosis and management of chronic open angle glaucoma and ocular hypertension
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Glaucoma: diagnosis and management of chronic open angle glaucoma and ocular hypertension 1.1 Short title Glaucoma 2 Background
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Glaucoma: diagnosis and management of chronic open angle glaucoma and ocular hypertension 1.1 Short title Glaucoma 2 Background
GLAUCOMA SURGICAL TREATMENTS
 GLAUCOMA SURGICAL TREATMENTS UnitedHealthcare Commercial Medical Policy Policy Number: OPT014 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS... 1 COVERAGE
GLAUCOMA SURGICAL TREATMENTS UnitedHealthcare Commercial Medical Policy Policy Number: OPT014 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS... 1 COVERAGE
Is Posner Schlossman Syndrome Benign?
 Is Posner Schlossman Syndrome Benign? Aliza Jap, FRCS (G), 1 Meenakshi Sivakumar, FRCS (Ed), M Med (Ophth), 2, Soon-Phaik Chee, FRCS (Ed), FRCOphth 2 Purpose: To determine the clinical course of patients
Is Posner Schlossman Syndrome Benign? Aliza Jap, FRCS (G), 1 Meenakshi Sivakumar, FRCS (Ed), M Med (Ophth), 2, Soon-Phaik Chee, FRCS (Ed), FRCOphth 2 Purpose: To determine the clinical course of patients
Aqueous Shunts and Stents for Glaucoma
 Aqueous Shunts and Stents for Glaucoma Policy Number: 9.03.21 Last Review: 1/2018 Origination: 9/2008 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Aqueous Shunts and Stents for Glaucoma Policy Number: 9.03.21 Last Review: 1/2018 Origination: 9/2008 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
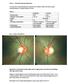 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
XEN-IMPLANT: MINIMALLY INVASIVE SURGERY FOR THE TREATMENT OF GLAUCOMA
 XEN-IMPLANT: MINIMALLY INVASIVE SURGERY FOR THE TREATMENT OF GLAUCOMA SAOO-Kongress 1.3.18 Dr. André Mermoud, Glaucoma Center, VISIO-Lausanne, Switzerland The 4 aims of any glaucoma surgery are: The 4
XEN-IMPLANT: MINIMALLY INVASIVE SURGERY FOR THE TREATMENT OF GLAUCOMA SAOO-Kongress 1.3.18 Dr. André Mermoud, Glaucoma Center, VISIO-Lausanne, Switzerland The 4 aims of any glaucoma surgery are: The 4
GLAUCOMA SURGICAL TREATMENTS
 GLAUCOMA SURGICAL TREATMENTS UnitedHealthcare Oxford Clinical Policy Policy Number: VISION 023.20 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
GLAUCOMA SURGICAL TREATMENTS UnitedHealthcare Oxford Clinical Policy Policy Number: VISION 023.20 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
Long term effect on IOP of a stainless steel glaucoma drainage implant (Ex-PRESS) in combined surgery with phacoemulsification
 425 EXTENDED REPORT Long term effect on IOP of a stainless steel glaucoma drainage implant (Ex-PRESS) in combined surgery with phacoemulsification C E Traverso, F De Feo, A Messas-Kaplan, P Denis, S Levartovsky,
425 EXTENDED REPORT Long term effect on IOP of a stainless steel glaucoma drainage implant (Ex-PRESS) in combined surgery with phacoemulsification C E Traverso, F De Feo, A Messas-Kaplan, P Denis, S Levartovsky,
Micro-Invasive Glaucoma Surgery (Aqueous Stents)
 Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Russ Trenary President & CEO.
 Russ Trenary President & CEO www.innfocusinc.com The InnFocus Winning Combination in Glaucoma Lowest IOP in studies IOP data below 14 mmhg with 3 year follow up. FDA requires 2 years max. SIBS material
Russ Trenary President & CEO www.innfocusinc.com The InnFocus Winning Combination in Glaucoma Lowest IOP in studies IOP data below 14 mmhg with 3 year follow up. FDA requires 2 years max. SIBS material
Surgical outcome of phacoemulsification combined with the Pearce trabeculect~m~ in patients with glaucoma
 Surgical outcome of phacoemulsification combined with the Pearce trabeculect~m~ in patients with glaucoma Louis R. Pasquale, M.D., S. Gregory Smith, M.D. ABSTRACT The safety and efficacy of phacoemulsification
Surgical outcome of phacoemulsification combined with the Pearce trabeculect~m~ in patients with glaucoma Louis R. Pasquale, M.D., S. Gregory Smith, M.D. ABSTRACT The safety and efficacy of phacoemulsification
Landmark Tube Trials
 SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
CLINICAL SCIENCES. Postoperative Complications After Glaucoma Surgery for Primary Angle-Closure Glaucoma vs Primary Open-Angle Glaucoma
 ONLINE FIRST CLINICAL SCIENCES Postoperative Complications After Glaucoma Surgery for Primary Angle-Closure Glaucoma vs Primary Open-Angle Glaucoma Yar-Li Tan, MRCS; Pei-Fang Tsou, MBBS; Gavin S. Tan,
ONLINE FIRST CLINICAL SCIENCES Postoperative Complications After Glaucoma Surgery for Primary Angle-Closure Glaucoma vs Primary Open-Angle Glaucoma Yar-Li Tan, MRCS; Pei-Fang Tsou, MBBS; Gavin S. Tan,
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Aqueous Shunts and Stents for Glaucoma
 Aqueous Shunts and Stents for Glaucoma Policy Number: 9.03.21 Last Review: 8/2018 Origination: 9/2008 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Aqueous Shunts and Stents for Glaucoma Policy Number: 9.03.21 Last Review: 8/2018 Origination: 9/2008 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
