Comparison of Dynesys posterior stabilization and posterior lumbar interbody fusion for spinal stenosis L4L5
|
|
|
- Diane Wheeler
- 6 years ago
- Views:
Transcription
1 Acta Orthop. Belg., 2012, 78, ORIGINAL STUDY Comparison of Dynesys posterior stabilization and posterior lumbar interbody fusion for spinal stenosis L4L5 Shang-Won YU, Shih-Chieh YAng, Ching-Hou MA, Chin-Hsien WU, Cheng-Yo YEn, Yuan-Kun TU From E-Da Hospital/I-Shou University, Jiau-Shu Tsuen, Taiwan, R.O.C. The aim of this prospective randomized study was to compare the radiological and clinical outcome after treatment of lumbar spinal stenosis L4L5 with or without spondylolisthesis, with either posterior lumbar interbody fusion (PLIF) (26 patients) or Dynesys posterior stabilization (27 patients). Demographic characteristics were comparable in both groups. Dynesys stabilization resulted in significantly higher preservation of motion at the index level (p < 0.001), and significantly less (p < 0.05) hypermobility at the adjacent segments. Oswestry Disability Index (ODI) and VAS for back and leg pain improved significantly (p < 0.05) with both methods, but there was no significant difference between groups. Operation time, blood loss, and length of hospital stay were all significantly (p < 0.001) less in the Dynesys group. The latter benefits may be of particular importance for elderly patients, or those with significant comorbidities. Complications were comparable in both groups. Dynesys posterior stabilization was effective for treating spinal stenosis L4L5 with or without spondylolisthesis. Keywords : lumbar spine ; dynamic stabilization ; Dynesys ; posterior lumbar interbody fusion. INTRODUCTION Chronic lumbar back pain due to intervertebral disc degeneration and spinal canal stenosis has been typically treated by fusion of the affected levels if conservative treatment fails. Radiographic fusion rates have been reported to be greater than 95% ; however, successful clinical outcomes are reported in only approximately 70% of cases (22). Problems and potential complications with fusion include nonunion, instrumentation failure, infection and donor site pain. Moreover, increased movement at adjacent segments can occur after spinal fusion, and this hypermobility may increase the risk for adjacent segment disease (5,13,16,19). given the potential disadvantages of fusion, attention has been drawn to techniques which preserve motion. The Dynesys Spinal Stabilization System (Zimmer, Inc., Minneapolis, Mn, USA) uses pedicle screws, polyethylene-terephtalate cords, and polycarbonate urethane spacers to stabilize a functional spinal unit (32). The system is Shang-Won Yu, MD, Visiting Doctor. Shih-Chieh Yang, MD, PhD, Director Spine Division. Ching-Hou Ma, MD, Director Trauma Division. Chin-Hsien Wu, MD, Visiting Doctor. Cheng-Yo Yen, MD, Chairman Orthop. Dept. Yuan-Kun Tu, MD, PhD, Professor,Superintendant E-Da Hospital. Department of Orthopaedic Surgery, E-Da Hospital/I-Shou University, Jiau-Shu Tsuen, Taiwan, Republic of China. Correspondence : Shang-Won Yu, Department of Orthopedic Surgery, E-Da Hospital/I-Shou University, 1, E-Da Road, Jiau-Shu Tsuen, Yan-Chau Shiang, 824, Kaohsiung County, Taiwan, Republic of China. ysw6455@yahoo.com.tw 2012, Acta Orthopædica Belgica. No benefits or funds were received in support of this study
2 COMPARISOn OF DYnESYS POSTERIOR STABILIZATIOn AnD POSTERIOR LUMBAR InTERBODY FUSIOn 231 designed to stabilize the operated segment, while preserving some mobility, thus preserving a greater degree of lumbar mobility than with fusion (1). The Dynesys system is indicated for lumbar spinal stenosis with or without spondylolisthesis, and can be used for single or multisegmental disease (27,32). Many clinical studies performed over the past decade have indicated positive outcomes for patients with degenerative disc disease of the lumbar spine treated with the Dynesys system (2,14,18, 20,25,28,30). In addition, Di Silvestre et al (8) found posterior dynamic stabilization with the Dynesys system particularly useful in elderly patients because the technique was less surgically aggressive than fusion. However, Schwarzenbach et al (27) caution against its use in elderly patients with osteoporotic bone or with severe segmental macroinstability combined with degenerative spondylosis and advanced disc degeneration. Despite the positive results reported with the Dynesys stabilization system, there is concern over the effects of stabilization on adjacent segments. A number of cadaveric, in vivo, and modeling studies have provided conflicting results (1,4,7,15,17,24,29). To date, there have been no randomized studies directly comparing radiographic and clinical outcomes of posterior lumbar interbody fusion (PLIF) and Dynesys posterior dynamic stabilization for the treatment of lumbar spinal stenosis, with or without spondylolisthesis, and the effects of the procedures on adjacent segment mobility. Most reports about the advantages of the Dynesys system were retrospective, or compared the Dynesys system with historical series about fusion. In addition, reports on the use of the Dynesys system in Asian populations are rare. This is why the current study fills a hiatus. MATERIALS AND METHODS This prospective randomized case-controlled study was performed in a single institution, between September 2006 and March All patients were operated upon between September 2006 and February Enrolled patients were randomized to either Dynesys posterior dynamic stabilization or PLIF. The study was approved by the Institutional Review Board of the hospital, and all patients provided written informed consent for participation in the study and surgical procedures. Criteria for inclusion in the study were : 1) age 38 to 71 years, 2) spinal stenosis with or without grade I degenerative spondylolisthesis L4L5, 3) severe instability (dynamic view > 15, translation > 4 mm), 4) preoperative Oswestry Disability Index (ODI) > 40, 5), failure of 3 months of conservative treatment, and 6) skeletal maturity. Exclusion criteria were : 1) disease at a level other than L4L5, 2) more than one level of spinal stenosis, 3) > grade I spondylolisthesis, 4) degenerative scoliosis > 10, 5) systemic disease and/or receiving immunosuppressive medication, and 6) osteoporosis (Tscore < -2). All patients above 60 years of age received an osteoporosis evaluation. Those below 60 years of age did not receive an investigation unless they had a risk factor (e.g., metabolic disease, early hysterectomy) or clinical evidence of osteoporosis. In all cases, the presence of spinal stenosis was confirmed by magnetic resonance imaging (MRI). Treatment allocation was performed before initiation of enrollment. Permuted-block treatment allocation was used to assign participants to each group. A list of sequential numbers was generated using a permutedblock randomization procedure with a block size of 4 in SAS 9.0 (SAS Institute Inc., Cary, nc, USA), with each number randomly assigned to one group. Patients meeting the criteria were randomly assigned in a 1 :1 ratio to the Dynesys group or the PLIF group. All patients were fused or stabilized at the L4L5 level only. Dynesys implantation was performed according to the directions of the manufacturer (32). Simple decompression (interlaminar decompression or laminotomy) was performed in most cases ; however, for cases of severe stenosis or far lateral stenosis, extensive decompression, sometimes including facetectomy, was performed, followed by instrumentation with Dynesys. Each spacer added 1-2 mm to the disc height. Postoperatively, patients in the Dynesys group received a soft support brace (lumbar corset) for 3 months. Patients did not participate in a rehabilitation program, and were instructed that they should avoid bending but otherwise could maintain a normal lifestyle. PLIF was performed in a standard manner using Synthes Click X spinal implants. When required, extensive decompression and facetectomy were performed for easy cage insertion. Autologous bone chips obtained from the decompression were used within and around the cage, followed by pedicle screw instrumentation and fixation. Patients in the PLIF group received a hard plastic lumbar brace for 3 months. Although there is no evidence supporting the use of braces postoperatively, it is a routine practice in our country : a brace is believed
3 232 S.-W. YU, S.-C. YAng, C.-H. MA, C.-H. WU, C.-Y. YEn, Y.-K. TU to help patients feel secure after surgery. Patients did not participate in a rehabilitation program, and were instructed that they should avoid bending but otherwise could maintain a normal lifestyle. Primary outcome measures were comparison of radiographic results between Dynesys and PLIF surgery groups at the index, cranial, and caudal levels. Anteroposterior (AP) and sagittal radiographs were obtained preoperatively, and at each follow-up visit. Each radiograph was measured twice, separated by a 1 week interval, by two independent experienced spine surgeons to minimize human errors in measuring. The average value of the measurements was used for analysis. Lateral flexion and extension views were also taken. The range of motion (ROM) in the sagittal (flexionextension) view was obtained by the following formula : ROM sagittal = angle (extension) angle (flexion). Motion preservation (%) was defined as ROM (post - operatively) / ROM (preoperatively). Radiographic instability was defined as 1) flexion versus extension > 10, or 2) flexion versus extension at the spinal ridge > 3-4 mm. Screw loosening was based on the presence of the double-halo sign on plain radiographs as described by Dakhil-Jerew et al (6). Only screw loosening as evidenced by a double-halo sign was included in this study. Secondary outcome measures were in the first place changes in ODI and visual analogue scale (VAS) for back and leg pain. VAS scores were determined on a scale ranging from 0 (no pain) to 10 (worst pain imaginable). ODI and VAS scores were determined preoperatively and at each follow-up visit. Operation time, blood loss, length of hospital stay, and complications were also compared between the two groups. Patients were followed-up at 3 months, and at 1, 2, and 3 years post - operatively. Statistical analysis The per-protocol (PP) population was defined as randomized patients who followed the procedure throughout the study without major deviations. Patients who did not complete follow-up or had incomplete radiographic records were excluded from the analysis. Analysis of the primary and secondary outcomes was based on the PP population. Continuous and categorical variables were compared by the independent two-sample t-test and the chi-square / Fisher s exact test, respectively. Paired t- tests in both groups were used to analyze the results of improvement differences from baseline (pre-op) to the 3- year follow-up. Continuous variables were presented as mean ± standard deviation (SD), while categorical data were represented by number and percentage. All statistical assessments were two-sided and evaluated at the 0.05 level of significant difference. Statistical analyses were performed using SPSS 15.0 statistics software (SPSS Inc, Chicago, IL, USA). RESULTS A total of 60 patients meeting the inclusion criteria were prospectively recruited between September 2006 and February Patients were randomly assigned in a 1:1 ratio to the Dynesys group and the PLIF group : 30 versus 30. Four patients (6.7%) were subsequently excluded from the analysis because they were lost to follow-up, leaving 27 patients in the Dynesys group (10 males and 17 females ; mean age, ± 8.32 years) and 29 in the PLIF group (11 males and 18 females ; mean age, ± 6.98 years). Two out of 29 patients in the PLIF group did not have a complete followup radiographic record, while a third patient had a superficial infection which needed repeat débridement and antibiotics : all three were excluded. Thus, 53 patients (27 in the Dynesys group and 26 in the PLIF group) com pleted a follow-up of 3 years and were included in the final analysis of radiographic and clinical outcomes. A flow chart of patients in the study is presented in Fig. 1. The demographic and baseline characteristics of both groups (Table I) were similar (all, p > 0.05). Surgery was performed successfully in all patients, and all patients had unremarkable post - operative courses. Radiological outcome : motion and adjacent level instability Representative pre- and postoperative images of PLIF and Dynesys placement are shown in Fig. 3 and Fig. 4, respectively. Post-operative radiographs at 36-month follow-up detected instability at the cranial level after PLIF ; on the other hand after Dynesys no sign of adjacent instability L3L4 or L5S1 was seen, while the disc height of L4L5 (operated level) was partially restored and maintained.
4 COMPARISOn OF DYnESYS POSTERIOR STABILIZATIOn AnD POSTERIOR LUMBAR InTERBODY FUSIOn 233 Fig. 1. Study flow chart Table I. Patients demographics and baseline data Dynesys group (n = 27) PLIF group (n = 26) Demographic data Mean age (years) ± SD ± ± a Mean BMI (kg/m 2 ) ± SD ± ± a gender b Male 10 (37.0%) 11 (37.9%) Female 17 (63.0%) 18 (62.1%) Spondylolisthesis 11 (40.7%) 13 (44.8%) b Baseline data Mean ROM ( ) ± SD Operated level (L4-5) 7.56 ± ± a Cranial level (L3-4) 7.07 ± ± a Caudal level (L5-S1) 7.52 ± ± a Mean ODI ± SD ± ± a MeanVAS leg pain ± SD 7.22 ± ± a Mean VAS back pain ± SD 6.63 ± ± a PLIF : posterior lumbar interbody fusion ; BMI : body mass index ; ROM : range of motion ; ODI : Oswestry Disability Index ; VAS : visual analogue scale. p-values are based on a independent two-sample t-test or b chi-square test. p
5 234 S.-w. yu, S.-c. yang, c.-h. MA, c.-h. wu, c.-y. yen, y.-k. Tu Fig. 2a. Dynesys and PLIF : significantly less operation time with Dynesys. Fig. 2c. Dynesys and PLIF : significantly less hospital stay with Dynesys. Fig. 2b. Dynesys and PLIF : significantly less blood loss with Dynesys. The comparison of radiographic (primary) outcomes between the two groups is shown in Table III. A statistically significant decrease of the ROM at the operated level from preoperatively to the 3-year follow-up was observed in both the Dynesys group and the PLIF group (both, p < 0.001). These data suggest that both the Dynesys system and PLIF are able to stabilize an unstable segment, but the Dynesys group can maintain partial ROM after surgery. A significant difference in motion preservation at the operated level was found between the Dynesys and PLIF group at 3-year follow-up (65.06 ± 14.72% vs ± 10.21%, respectively ; p < 0.001). These data suggest that the Dynesys system can preserve a greater ROM than PLIF at the operated level. The percentage of cranial level motion preservation at 3-year follow-up was significantly different between the Dynesys and PLIF group ( ± 30.41% versus ± 47.12%, respectively ; p = 0.012). The percentage of caudal level motion preservation at 3-year follow-up was also significantly different between the Dynesys and PLIF group ( ± 25.42% versus ± 26.33%, respectively ; p = 0.032). Clinical outcome : ODI, VAS, operation time, blood loss, hospital stay, complications Statistically significant improvements in ODI and VAS leg and back pain scores (Table III) were found for both groups at the 3-year follow-up as compared to preoperative values (all : p < 0.05). However, the degree of improvement in all indices was similar between the Dynesys group and the PLIF group at 3-year follow-up (all : p > 0.05).
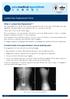
6 COMPARISOn OF DYnESYS POSTERIOR STABILIZATIOn AnD POSTERIOR LUMBAR InTERBODY FUSIOn 235 Table II. Complications by group Dynesys group (n = 27) PLIF group (n = 26) Radiological instability at cranial level 1 (3.7%) 6 (20.7%) at caudal level 0 (0.0%) 1 (3.4%) Re-operation 0 (0.0%) 3 (10.3%) Screw loosening 1 (3.7%) 1 (3.4%) Dural tear 0 (0.0%) 1 (3.4%) PLIF : posterior lumbar interbody fusion. Data are displayed as number (percentage). p-values are based on Fisher s exact test. p The operation time, blood loss, and length of hospital stay were all significantly less (Fig. 2) (all : p < 0.001) in the Dynesys group as compared to the PLIF group (78.56 ± minutes versus ± 9.99 minutes ; ± ml versus ± ml, and 5.48 ± 0.94 days versus 7.21 ± 0.90 days, respectively). Complications Fig. 3. A representative case of PLIF. Lateral plain radio - graphs showing : (a) pre-operative flexion ; (b) pre-operative extension : no instability at levels L3L4 and L5S1 ; (c) postoperative flexion at 36-month follow-up ; (d) postoperative extension at 36-month follow-up : instability (more than 15 ) was detected at the cranial level. There was no significant difference in complications such as radiographic instability, re-operation, screw loosening, and dural tears between the Dynesys and the PLIF group (Table II) (all : p > 0.05). One case of screw loosening in a Dynesys implantation was identified on radiographs taken 3 months postoperatively. The patient was asymptomatic, and no revision surgery was performed. One case of screw loosening also occurred in the PLIF group. The patient was asymptomatic, and successful fusion was achieved, thus no revision surgery was required. One dural tear also occurred in the PLIF group during interbody cage insertion, and was managed without further complications. In the Dynesys group, there was one case of radiographic instability at/or over the adjacent level. The patient experienced moderate back pain ; however, no subsequent surgery was required. In the PLIF group, however, there were 6 cases of radiographic instability, and 3 patients underwent reoperation of the adjacent levels.
7 236 S.-W. YU, S.-C. YAng, C.-H. MA, C.-H. WU, C.-Y. YEn, Y.-K. TU DISCUSSION Radiological outcome : motion and adjacent level instability Fig. 4. A representative case of Dynesys surgery. Radiographs showing : (a) preoperative extension ; (b) preoperative flexion : stenosis L4L5 for which the patient underwent Dynesys surgery ; (c) postoperative extension view at 36- month follow-up ; (d) postoperative flexion view at 36-month follow-up : no adjacent instability L3L4 or L5S1, and partial restoration of the disc height L4L5 (operated level). Dynesis resulted in higher preservation of motion at the index level. This finding is predicted by the design of the device, and consistent with reports in the literature. Contrary to fusion, which results in a solid connection of the operative levels, Dynesys stabilizes the index level, while the flexible cords and spacers allow a limited range of motion (32). Lee et al (14) reported the results of 20 consecutive patients treated with the Dynesys system, and found at a mean follow-up of ± 5.16 months that the system allowed preservation of motion of the stabilized segments and improvement of the clinical variables ODI and VAS for pain. Contrary to these findings, Schaeren et al (23) found no motion at the operated level in 19 Dynesis patients with a minimum 4-year follow-up. Dynesys led to less hypermobility (flexion/ extension) in the adjacent cranial segment. In the adjacent caudal segment almost no change of mobility was noted with Dynesys stabilization, whereas only a slight increase of mobility was noted with PLIF. Reports regarding the mobility and degeneration of adjacent segments after Dynesys implantation are conflicting. Fusion results in increased stress in adjacent segments and subsequent hypermobility and adjacent segment disease (3). Some authors have suggested that preservation of motion at the operative level can prevent degeneration at the adjacent segments by decreasing stress and resulting hypermobility (28). Beastall et al (1) studied 24 patients, treated with the Dynesys system, with positional magnetic resonance imaging preoperatively, and at 9 months postoperatively ; they found no significant increase in mobility at the adjacent levels. In a cadaveric study, Schmoelz et al (24) reported that Dynesys stabilization did not increase the mobility of adjacent segments. On the contrary, Schaeren et al (23) studied 19 Dynesys patients with a minimum 4-year follow-up and found new signs of degeneration in adjacent motion segments in 47% of the patients, a rate similar to that reported after lumbar fusion (21). Similarly, Kumar et al (12)
8 COMPARISOn OF DYnESYS POSTERIOR STABILIZATIOn AnD POSTERIOR LUMBAR InTERBODY FUSIOn 237 Radiological outcome Motion preservation (%) Table III. Radiological and clinical outcomes at 3-year follow-up Dynesys group (n = 27) PLIF group (n = 26) Operated level (L4-5) % ± 14.72* 15.99% ± 10.21* < 0.001** Cranial level (L3-4) % ± % ± 47.12* 0.012** Caudal level (L5-S1) % ± % ± 26.33* 0.032** Clinical outcome Oswestry Disability Index ± 8.63* ± 12.72* VAS leg pain ± 1.42* ± 1.55* VAS back pain ± 2.37* ± 2.77* PLIF : posterior lumbar interbody fusion ; VAS : visual analogue scale. Data are displayed as mean ± standard deviation. * Significant difference between pre- and postoperative condition in each group, p < ** Significant difference between Dynesys and PLIF groups using independent two-sample t-test, p < p studied 32 patients with the Dynesys system and also noted continued degeneration at the index and adjacent segments, but believed that the further changes may be a result of the natural progression of the disease. Liu et al (15) used a displacementcontrolled finite element analysis to evaluate the mechanical behavior of the lumbar spine after Dynesys placement and found preservation of motion and sufficient stability at the operated level, but greater ROM, annulus stress, and facet loading in the adjacent levels. Our results indicate less hypermobility in the cranial segment compared to PLIF, which is likely because Dynesys is able to share the load exhibited in L4L5, and does not carry an excessive load to L3L4. However, the Dynesys system is stiffer initially (at 3-months follow-up), and thus can carry more load to L3L4 in the beginning. As the system relaxes and adapts with time, the system becomes more flexible and the load on the cranial level decreases. In the caudal segment, the change of mobility in the sagittal plane was small for both systems ; the Dynesys group demonstrated almost no change, whereas the PLIF group demonstrated a slight increase in mobility. It is clear from the results of prior studies, as well as of our own, that long-term studies of adjacent segment mobility and disease after Dynesys implantation are mandatory. Clinical outcome. ODI, VAS, operation time, blood loss, hospital stay, complications While the majority of studies have indicated positive results with the Dynesys system, some reports have indicated that results are no better than those obtained with typical fusion. Würgler-Hauri et al (31) studied 37 patients with acquired lumbar stenosis, segmental instability, and degenerative disc disease who underwent lumbar microsurgical decompression and Dynesys implantation. They reported that patients experienced a reduction of radicular pain, but a worsening of lumbar pain and that 27% of patients mentioned a poor outcome. In addition, at 1-year, 19% of patients required revision surgery. grob et al (10) retrospectively studied 31 Dynesys patients, with at least 2-years of followup, with a mailed follow-up questionnaire. Within the 2-year period, 19% of patients either had or were scheduled for revision surgery, and only half of the patients stated that the operation had improved their overall quality of life ; less than half reported improvement in their functional capacity.
9 238 S.-W. YU, S.-C. YAng, C.-H. MA, C.-H. WU, C.-Y. YEn, Y.-K. TU In the current study, ODI and VAS for back and leg pain improved significantly in both groups at 3- year follow-up. This improvement was comparable between the two groups, indicating that both procedures are effective for the treatment of lumbar stenosis L4L5. This significant improvement in ODI and VAS with Dynesys stabilization is consistent with many reports in the literature (2,14,18,20, 25,28,30). However, at 3 months postoperatively the VAS back pain scores were better in the Dynesys group (data not shown), suggesting that the system provides better relief in the early postoperative period. Probably because the Dynesys device provides immediate stabilization of the diseased segment, and neutralizes the abnormal forces caused by the pathological bony and soft tissue changes which cause back pain (9,15,20,26,28,30,32). On the other hand, PLIF requires successful fusion to achieve a completely stable segment to eliminate back pain. The authors found that operation time was shorter in the Dynesys group, probably because there is no need for endplate preparation and insertion of an interbody device or bone grafting. Less blood loss in the Dynesys group is logical because insertion of the Dynesys device requires less bone and soft tissue dissection as compared to PLIF. Likewise, the shorter hospital stay in the Dynesys group is most likely due to the fact that the insertion of the device is less invasive as compared to PLIF (23,25,30). Although both Dynesys and PLIF require insertion of pedicle screws and rods (or spacers), Dynesys does not require insertion of an interbody fusion device or bone grafting, and is therefore relatively less invasive. Complications Complications were comparable in the two groups. One case of screw loosening after an L4L5 Dynesys implantation was identified on radio - graphs taken 3 months postoperatively. According to Dakhil-Jerew et al (6), Dynesys screw loosening should be confirmed with a double-halo sign. However, in our case, only a single-halo sign was detected, thus we believe that the screw and construct were secondarily stabilized by the soft tissues. Ko et al (11) studied screw loosening after implantation of the Dynesys system in 71 patients who underwent decompression for 1- or 2-level lumbar spondylosis. They found radiographic evidence of screw loosening in 19.7% of the patients (4.6% of screws) ; however, screw loosening had no adverse impact on clinical improvement. In our study, one case of screw loosening also occurred in the PLIF group, and no revision surgery was required. One dural tear occurred in the PLIF group during interbody cage insertion. Dural tear is a known complication of PLIF, whereas it is not likely to occur with implantation of the Dynesys system. Though there was no significant difference in adjacent level instability between the groups, there was one case of adjacent level instability in the Dynesys group as compared to 6 in the PLIF group. Of the 6 cases in the PLIF group, 3 patients underwent re-operation of the adjacent levels. We believe that this can be explained by the fact that PLIF increases load on adjacent levels, which speeds up further degeneration, especially in cranial segments, whereas the Dynesys seems to stabilize the index level without transferring excessive load to adjacent segments. Weaknesses Weaknesses of this study are : a short follow-up (3 years), potential errors in measuring radiographic mobility, stenosis not calculated as a percentage of the spinal canal, small patient numbers, no intention to treat analysis. REFERENCES 1. Beastall J, Karadimas E, Siddiqui M et al. The Dynesys lumbar spinal stabilization system : a preliminary report on positional magnetic resonance imaging findings. Spine 2007 ; 32 : Bordes-Monmeneu M, Bordes-Garcia V, Rodrigo- Baeza F, Saez D. [System of dynamic neutralization in the lumbar spine : experience on 94 cases.] (in Spanish). Neurocirugia 2005 ; 16 : Cakir B, Carazzo C, Schmidt R et al. Adjacent segment mobility after rigid and semirigid instrumentation of the lumbar spine. Spine 2009 ; 34 : Cheng BC, Gordon J, Cheng J, Welch WC. Immediate biomechanical effects of lumbar posterior dynamic stabilization above a circumferential fusion. Spine 2007 ; 32 :
10 COMPARISOn OF DYnESYS POSTERIOR STABILIZATIOn AnD POSTERIOR LUMBAR InTERBODY FUSIOn Chou WY, Hsu CJ, Chang WN, Wong CY. Adjacent segment degeneration after lumbar spinal posterolateral fusion with instrumentation in elderly patients. Arch Orthop Trauma Surg 2002 ; 122 : Dakhil-Jerew F, Jadeja H, Cohen A, Shepperd JA. Interobserver reliability of detecting Dynesys pedicle screw using plain X-rays : a study on 50 post-operative patients. Eur Spine J 2009 ; 18 : Delank KS, Gercek E, Kuhn S et al. How does spinal canal decompression and dorsal stabilization affect segmental mobility? A biomechanical study. Arch Orthop Trauma Surg 2010 ; 130 : Di Silvestre M, Lolli F, Bakaloudis G, Parisini P. Dynamic stabilization for degenerative lumbar scoliosis in elderly patients. Spine 2010 ; 35 : Fayyazi AH, Ordway NR, Park SA et al. Radio - stereometric analysis of postoperative motion after application of dynesys dynamic posterior stabilization system for treatment of degenerative spondylolisthesis. J Spinal Disord Tech 2010 ; 23 : Grob D, Benini A, Junge A, Mannion AF. Clinical experience with the Dynesys semirigid fixation system for the lumbar spine : surgical and patient-oriented outcome in 50 cases after an average of 2 years. Spine 2005 ; 30 : Ko CC, Tsai HW, Huang WC et al. Screw loosening in the Dynesys stabilization system : radiographic evidence and effect on outcomes. Neurosurg Focus 2010 ; 28 : E Kumar A, Beastall J, Hughes J et al. Disc changes in the bridged and adjacent segments after Dynesys dynamic stabilization system after two years. Spine 2008 ; 33 : Kumar MN, Baklanov A, Chopin D. Correlation between sagittal plane changes and adjacent segment degeneration following lumbar spine fusion. Eur Spine J 2001 ; 10 : Lee SE, Park SB, Jahng TA et al. Clinical experience of the dynamic stabilization system for the degenerative spine disease. J Korean Neurosurg Soc 2008 ; 43 : Liu CL, Zhong ZC, Shih SL et al. Influence of Dynesys system screw profile on adjacent segment and screw. J Spinal Disord Tech 2010 ; 23 : Miyakoshi N, Abe E, Shimada Y et al. Outcome of onelevel posterior lumbar interbody fusion for spondylolisthesis and postoperative intervertebral disc degeneration adjacent to the fusion. Spine 2000 ; 25 : Niosi CA, Zhu QA, Wilson DC et al. Biomechanical characterization of the three-dimensional kinematic behaviour of the Dynesys dynamic stabilization system : an in vitro study. Eur Spine J 2006 ; 15 : Nockels RP. Dynamic stabilization in the surgical management of painful lumbar spinal disorders. Spine 2005 ; 30 (16 Suppl) : S68-S Okuda S, Iwasaki M, Miyauchi A et al. Risk factors for adjacent segment degeneration after PLIF. Spine 2004 ; 29 : Putzier M, Schneider SV, Funk JF et al. The surgical treatment of the lumbar disc prolapse : nucleotomy with additional transpedicular dynamic stabilization versus nucleotomy alone. Spine 2005 ; 30 : E109-E Rahm MD, Hall BB. Adjacent-segment degeneration after lumbar fusion with instrumentation : a retrospective study. J Spinal Disord 1996 ; 9 : Resnick DK, Choudhri TF, Dailey AT et al. guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 5 : correlation between radiographic and functional outcome. J Neurosurg Spine 2005 ; 2 : Schaeren S, Broger I, Jeanneret B. Minimum four-year follow-up of spinal stenosis with degenerative spondylolisthesis treated with decompression and dynamic stabilization. Spine 2008 ; 33 : E636-E Schmoelz W, Huber JF, Nydegger T et al. Dynamic stabilization of the lumbar spine and its effects on adjacent segments : an in vitro experiment. J Spinal Disord Tech 2003 ; 16 : Schnake KJ, Schaeren S, Jeanneret B. Dynamic stabilization in addition to decompression for lumbar spinal stenosis with degenerative spondylolisthesis. Spine 2006 ; 31 : Schulte TL, Hurschler C, Haversath M et al. The effect of dynamic, semi-rigid implants on the range of motion of lumbar motion segments after decompression. Eur Spine J 2008 ; 17 : Schwarzenbach O, Berlemann U, Stoll TM, Dubois G. Posterior dynamic stabilization systems : DYnESYS. Orthop Clin North Am 2005 ; 36 : Stoll TM, Dubois G, Schwarzenbach O. The dynamic neutralization system for the spine : a multi-center study of a novel non-fusion system. Eur Spine J 2002 ; 11(Suppl 2) : S170-S Vaga S, Brayda-Bruno M, Perona F et al. Molecular MR imaging for the evaluation of the effect of dynamic stabilization on lumbar intervertebral discs. Eur Spine J 2009 ; 18(Suppl 1) : Welch WC, Cheng BC, Awad TE et al. Clinical outcomes of the Dynesys dynamic neutralization system : 1-year preliminary results. Neurosurg Focus 2007 ; 22 : E Würgler-Hauri CC, Kalbarczyk A, Wiesli M, Landolt H, Fandino J. Dynamic neutralization of the lumbar spine after microsurgical decompression in acquired lumbar spinal stenosis and segmental instability. Spine 2008 ; 33 : E66-E Zimmer Spine Inc. Dynesys Dynamic Stabilization System-Dynesys LIS Surgical Technique. Zimmer Spine Inc., Minneapolis.
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Haiting Wu 1, Qingjiang Pang 1 and Guoqiang Jiang 2. Clinical Report
 Clinical Report Medium-term effects of Dynesys dynamic stabilization versus posterior lumbar interbody fusion for treatment of multisegmental lumbar degenerative disease Journal of International Medical
Clinical Report Medium-term effects of Dynesys dynamic stabilization versus posterior lumbar interbody fusion for treatment of multisegmental lumbar degenerative disease Journal of International Medical
Original Article Intermediate-term clinical effects of Dynesys dynamic stabilization system on double-segmental lumbar disc herniation
 Int J Clin Exp Med 2017;10(8):12349-12354 www.ijcem.com /ISSN:1940-5901/IJCEM0056734 Original Article Intermediate-term clinical effects of Dynesys dynamic stabilization system on double-segmental lumbar
Int J Clin Exp Med 2017;10(8):12349-12354 www.ijcem.com /ISSN:1940-5901/IJCEM0056734 Original Article Intermediate-term clinical effects of Dynesys dynamic stabilization system on double-segmental lumbar
ProDisc-L Total Disc Replacement. IDE Clinical Study
 Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Dynamic Radiographic Results of Different Semi-Rigid Fusion Devices for Degenerative Lumbar Spondylolisthesis: Dynamic Rod vs. Dynamic Screw Head
 DOI: 10.5137/1019-5149.JTN.9784-13.1 Received: 09.05.2013 / Accepted: 09.12.2013 Original Investigation Dynamic Radiographic Results of Different Semi-Rigid Fusion Devices for Degenerative Lumbar Spondylolisthesis:
DOI: 10.5137/1019-5149.JTN.9784-13.1 Received: 09.05.2013 / Accepted: 09.12.2013 Original Investigation Dynamic Radiographic Results of Different Semi-Rigid Fusion Devices for Degenerative Lumbar Spondylolisthesis:
Coflex TM for Lumbar Stenosis with
 Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
ILIF Interlaminar Lumbar Instrumented Fusion. Anton Thompkins, M.D.
 ILIF Interlaminar Lumbar Instrumented Fusion Anton Thompkins, M.D. Anton Thompkins, M.D. EDUCATION: BS, Biology, DePauw University, Greencastle, IN MD, University of Cincinnati College of Medicine RESIDENCY:
ILIF Interlaminar Lumbar Instrumented Fusion Anton Thompkins, M.D. Anton Thompkins, M.D. EDUCATION: BS, Biology, DePauw University, Greencastle, IN MD, University of Cincinnati College of Medicine RESIDENCY:
Lumbar Single-Level Dynamic Stabilization with Semi-Rigid and Full Dynamic Systems: A Retrospective Clinical and Radiological Analysis of 71 Patients
 Original Article Clinics in Orthopedic Surgery 2017;9:310-316 https://doi.org/10.4055/cios.2017.9.3.310 Lumbar Single-Level Dynamic Stabilization with Semi-Rigid and Full Dynamic Systems: A Retrospective
Original Article Clinics in Orthopedic Surgery 2017;9:310-316 https://doi.org/10.4055/cios.2017.9.3.310 Lumbar Single-Level Dynamic Stabilization with Semi-Rigid and Full Dynamic Systems: A Retrospective
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis
 Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Lumbar Facet Joint Replacement
 Rome Spine 2011 THE SPINE TODAY International Congress Rome 6-7th December 2011 Lumbar Facet Joint Replacement Prof. Dr. Karin Büttner-Janz Past President International Society for the Advancement of Spine
Rome Spine 2011 THE SPINE TODAY International Congress Rome 6-7th December 2011 Lumbar Facet Joint Replacement Prof. Dr. Karin Büttner-Janz Past President International Society for the Advancement of Spine
INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE.
 INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE. A PRELIMINARY REPORT F. POSTACCHINI, A. PALMESI LUMBAR VERTEBRAL INSTABILITY Still the subject of discussion Variously defined and interpreted Postacchini
INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE. A PRELIMINARY REPORT F. POSTACCHINI, A. PALMESI LUMBAR VERTEBRAL INSTABILITY Still the subject of discussion Variously defined and interpreted Postacchini
ASJ. Outcome of Salvage Lumbar Fusion after Lumbar Arthroplasty. Asian Spine Journal. Introduction. Hussein Alahmadi, Harel Deutsch
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2014;8(1):13-18 Lumbar fusion http://dx.doi.org/10.4184/asj.2014.8.1.13 after lumbar arthroplasty 13 Outcome of Salvage Lumbar Fusion
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2014;8(1):13-18 Lumbar fusion http://dx.doi.org/10.4184/asj.2014.8.1.13 after lumbar arthroplasty 13 Outcome of Salvage Lumbar Fusion
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions:
 Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Dingjun Hao, Baorong He, Liang Yan. Hong Hui Hospital, Xi an Jiaotong University College. of Medicine, Xi an, Shaanxi , China
 Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
PARADIGM SPINE. Brochure. coflex-f Minimally Invasive Lumbar Fusion
 PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
Comparison of lumbar pedicular dynamic stabilisation systems versus fusion for the treatment of lumbar degenerative disc disease: A meta-analysis
 180 Acta Orthop. Belg., y.-j. 2017, huang, 83, 180-193 s.-j. zhao, q. zhang, l.-m. nong, n.-w. xu ORIGINAL STUDY Comparison of lumbar pedicular dynamic stabilisation systems versus fusion for the treatment
180 Acta Orthop. Belg., y.-j. 2017, huang, 83, 180-193 s.-j. zhao, q. zhang, l.-m. nong, n.-w. xu ORIGINAL STUDY Comparison of lumbar pedicular dynamic stabilisation systems versus fusion for the treatment
Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Spine and Fusion. Adjacent Segment Disease. 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D.
 Lumbar Posterior Hybrid Dynamic Stabilisation and Fusion Systems 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D. Spine and Fusion It has been more than a century since 1911 when Albee
Lumbar Posterior Hybrid Dynamic Stabilisation and Fusion Systems 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D. Spine and Fusion It has been more than a century since 1911 when Albee
ASJ. Radiologic and Clinical Courses of Degenerative Lumbar Scoliosis (10 25 ) after a Short-Segment Fusion. Asian Spine Journal.
 Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients
 Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Spinal fusion with decompressive laminectomy is
 J Neurosurg Spine 18:24 31, 2013 AANS, 2013 Posterior dynamic stabilization in the treatment of degenerative lumbar stenosis: validity of its rationale Clinical article Kee-Yong Ha, M.D., 1 Jun-Yeong Seo,
J Neurosurg Spine 18:24 31, 2013 AANS, 2013 Posterior dynamic stabilization in the treatment of degenerative lumbar stenosis: validity of its rationale Clinical article Kee-Yong Ha, M.D., 1 Jun-Yeong Seo,
Subject: Interspinous Decompression Devices for Spinal Stenosis (X Stop, Coflex) Guidance Number: MCG-222 Revision Date(s):
 Subject: Interspinous Decompression Devices for Spinal Stenosis (X Stop, Coflex) Guidance Number: MCG-222 Revision Date(s): Original Effective Date: 3/16/15 DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL
Subject: Interspinous Decompression Devices for Spinal Stenosis (X Stop, Coflex) Guidance Number: MCG-222 Revision Date(s): Original Effective Date: 3/16/15 DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Get back to: my life. Non-fusion treatment for lumbar spinal stenosis
 Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
Range of Motion According to the Fusion Level after Lumbar Spine Fusion: A Retrospective Study
 eissn2465-891x The Nerve.2018.4(2):55-59 The Nerve https://doi.org/10.21129/nerve.2018.4.2.55 CLINICAL ARTICLE www.thenerve.net Range of Motion According to the Fusion Level after Lumbar Spine Fusion:
eissn2465-891x The Nerve.2018.4(2):55-59 The Nerve https://doi.org/10.21129/nerve.2018.4.2.55 CLINICAL ARTICLE www.thenerve.net Range of Motion According to the Fusion Level after Lumbar Spine Fusion:
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Dept. of Orthopaedic Surgery, Wakayama Medical University, Wakayama, Japan. Brigham and Women s Hospital, Harvard Medical School, Boston, MA, USA.
 Microendoscopic Decompression for Lumbar Spinal Stenosis with Degenerative Spondylolisthesis: the influence of spondylolisthesis stage (disc height and static and dynamic translation) on clinical outcomes
Microendoscopic Decompression for Lumbar Spinal Stenosis with Degenerative Spondylolisthesis: the influence of spondylolisthesis stage (disc height and static and dynamic translation) on clinical outcomes
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up
 Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up Janek Frantzén M.D., Neurosurgeon Turku University Hospital, Finland ROME SPINE 2011 7.12.2011 1 Clinical Development
Bioactive glass S53P4 in spine surgery -results from a prospective 11-year-follow-up Janek Frantzén M.D., Neurosurgeon Turku University Hospital, Finland ROME SPINE 2011 7.12.2011 1 Clinical Development
Top spine papers of 2016
 Top spine papers of 2016 Ai Mukai, MD Texas Orthopedics, Sports & Rehabilitation University of Texas-Austin, PM&R Residency October 21, 2016 Top papers in spine? Top papers in Spine How do you define top?
Top spine papers of 2016 Ai Mukai, MD Texas Orthopedics, Sports & Rehabilitation University of Texas-Austin, PM&R Residency October 21, 2016 Top papers in spine? Top papers in Spine How do you define top?
The Role of Surgery in the Treatment of Low Back Pain and Radiculopathy. Christian Etter, MD, Spine Surgeon Zürich, Switzerland
 The Role of Surgery in the Treatment of Low Back Pain and Radiculopathy Christian Etter, MD, Spine Surgeon Zürich, Switzerland WW Fusion Volume by Disorder 2004E % Tumor/Trauma 11% Deformity 15% Degeneration
The Role of Surgery in the Treatment of Low Back Pain and Radiculopathy Christian Etter, MD, Spine Surgeon Zürich, Switzerland WW Fusion Volume by Disorder 2004E % Tumor/Trauma 11% Deformity 15% Degeneration
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Dynamic anterior cervical plating for multi-level spondylosis: Does it help?
 Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Minimally invasive transforaminal lumbar interbody
 Neurosurg Focus 35 (2):E13, 2013 AANS, 2013 Outcome following unilateral versus bilateral instrumentation in patients undergoing minimally invasive transforaminal lumbar interbody fusion: a single-center
Neurosurg Focus 35 (2):E13, 2013 AANS, 2013 Outcome following unilateral versus bilateral instrumentation in patients undergoing minimally invasive transforaminal lumbar interbody fusion: a single-center
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Fusion-segment of high-grade Lumbar Spondylolisthesis: 2-year follow-up
 730 Acta Orthop. Belg., 2016, 82, 730-736 x. li, l. xu, q. kong ORIGINAL STUDY Fusion-segment of high-grade Lumbar Spondylolisthesis: 2-year follow-up Xiaolong Li, Lian Xu, Qingquan Kong Department of
730 Acta Orthop. Belg., 2016, 82, 730-736 x. li, l. xu, q. kong ORIGINAL STUDY Fusion-segment of high-grade Lumbar Spondylolisthesis: 2-year follow-up Xiaolong Li, Lian Xu, Qingquan Kong Department of
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis
 Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases-
 Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative spondylolisthesis
 Eur Spine J (2008) 17:188 192 DOI 10.1007/s00586-007-0492-x ORIGINAL ARTICLE High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative
Eur Spine J (2008) 17:188 192 DOI 10.1007/s00586-007-0492-x ORIGINAL ARTICLE High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Int J Clin Exp Med 2015;8(4): /ISSN: /IJCEM Xiaokang Liu, Yingjie Liu, Xiaofeng Lian, Jianguang Xu
 Int J Clin Exp Med 2015;8(4):6097-6102 www.ijcem.com /ISSN:1940-5901/IJCEM0006352 Original Article Magnetic resonance imaging on disc degeneration changes after implantation of an interspinous spacer and
Int J Clin Exp Med 2015;8(4):6097-6102 www.ijcem.com /ISSN:1940-5901/IJCEM0006352 Original Article Magnetic resonance imaging on disc degeneration changes after implantation of an interspinous spacer and
Vertebral body fractures after transpsoas interbody fusion procedures
 The Spine Journal 11 (2011) 1068 1072 Case Report Vertebral body fractures after transpsoas interbody fusion procedures Justin E. Brier-Jones, BS a, Daniel K. Palmer, BS b, Serkan Inceoglu, PhD a, Wayne
The Spine Journal 11 (2011) 1068 1072 Case Report Vertebral body fractures after transpsoas interbody fusion procedures Justin E. Brier-Jones, BS a, Daniel K. Palmer, BS b, Serkan Inceoglu, PhD a, Wayne
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
PARADIGM SPINE. Interlaminar Technology. Interlaminar Implant
 PARADIGM SPINE Interlaminar Technology Interlaminar Implant SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options.
PARADIGM SPINE Interlaminar Technology Interlaminar Implant SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options.
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF)
 Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Technique Guide. NFlex. Semi-rigid rods for posterior lumbar stabilization.
 Technique Guide NFlex. Semi-rigid rods for posterior lumbar stabilization. Table of Contents Introduction NFlex 2 Indications and Contraindications 4 NFlex Principles 6 Surgical Technique Preoperative
Technique Guide NFlex. Semi-rigid rods for posterior lumbar stabilization. Table of Contents Introduction NFlex 2 Indications and Contraindications 4 NFlex Principles 6 Surgical Technique Preoperative
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
GECO 2010 LES-ARCS FRANCE LP-ESP II Elastic Spine PAD2 FH-ORTHOPEDICS
 GECO 2010 LES-ARCS FRANCE LP-ESP II Elastic Spine PAD2 FH-ORTHOPEDICS First results with 100 implanted LP-ESP after one year Klinikum Leer Departement of Spinal Surgery Germany Dr. med. Hamid Afshar Klinikum
GECO 2010 LES-ARCS FRANCE LP-ESP II Elastic Spine PAD2 FH-ORTHOPEDICS First results with 100 implanted LP-ESP after one year Klinikum Leer Departement of Spinal Surgery Germany Dr. med. Hamid Afshar Klinikum
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Pasquale Donnarumma 1, Roberto Tarantino 1, Lorenzo Nigro 1, Marika Rullo 2, Domenico Messina 3, Daniele Diacinti 4, Roberto Delfini 1.
 Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late complications
 Int J Clin Exp Med 2015;8(4):5731-5738 www.ijcem.com /ISSN:1940-5901/IJCEM0006438 Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late
Int J Clin Exp Med 2015;8(4):5731-5738 www.ijcem.com /ISSN:1940-5901/IJCEM0006438 Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late
Free Paper Session IX Spine II
 Free Paper Session IX Spine II 9. Oblique Lateral Interbody Fusion for L5-S Introduction: A minimally invasive modified anterior lumbar interbody fusion technique for the lumbosacral junction is described
Free Paper Session IX Spine II 9. Oblique Lateral Interbody Fusion for L5-S Introduction: A minimally invasive modified anterior lumbar interbody fusion technique for the lumbosacral junction is described
Anterior cervical interbody fusion with radiolucent carbon fiber cages : clinical and radiological results
 Acta Orthop. Belg., 2005, 71, 604-609 ORIGINAL STUDY Anterior cervical interbody fusion with radiolucent carbon fiber cages : clinical and radiological results Ibo VAN DER HAVEN, Piet J. M. VAN LOON, Ronald
Acta Orthop. Belg., 2005, 71, 604-609 ORIGINAL STUDY Anterior cervical interbody fusion with radiolucent carbon fiber cages : clinical and radiological results Ibo VAN DER HAVEN, Piet J. M. VAN LOON, Ronald
Lumbar Disc Replacement FAQs
 ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
Lumbar Disc Degeneration Is an Equally Important Risk Factor as Lumbar Fusion for Causing Adjacent Segment Disc Disease
 Lumbar Disc Degeneration Is an Equally Important Risk Factor as Lumbar Fusion for Causing Adjacent Segment Disc Disease Raghu N. Natarajan, Gunnar B.J. Andersson Department of Orthopedic Surgery, Rush
Lumbar Disc Degeneration Is an Equally Important Risk Factor as Lumbar Fusion for Causing Adjacent Segment Disc Disease Raghu N. Natarajan, Gunnar B.J. Andersson Department of Orthopedic Surgery, Rush
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Axial Lumbosacral Interbody Fusion. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Lumbar spinal stenosis is narrowing of the spinal canal that results in compression of the cauda
 1 CHAPTER 32: CLINICAL RESULTS OF THE IDE TRIAL OF X-STOP INTERSPINOUS SYSTEMS ELIZABETH YU AND JAMES ZUCHERMAN Lumbar spinal stenosis Lumbar spinal stenosis is narrowing of the spinal canal that results
1 CHAPTER 32: CLINICAL RESULTS OF THE IDE TRIAL OF X-STOP INTERSPINOUS SYSTEMS ELIZABETH YU AND JAMES ZUCHERMAN Lumbar spinal stenosis Lumbar spinal stenosis is narrowing of the spinal canal that results
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Available online at International Journal of Current Research Vol. 9, Issue, 05, pp , May, 2017 REVIEW ARTICLE
 z Available online at http://www.journalcra.com International Journal of Current Research Vol. 9, Issue, 05, pp.51434-51439, May, 2017 INTERNATIONAL JOURNAL OF CURRENT RESEARCH ISSN: 0975-833X REVIEW ARTICLE
z Available online at http://www.journalcra.com International Journal of Current Research Vol. 9, Issue, 05, pp.51434-51439, May, 2017 INTERNATIONAL JOURNAL OF CURRENT RESEARCH ISSN: 0975-833X REVIEW ARTICLE
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Clinical Study Adult s Degenerative Scoliosis: Midterm Results of Dynamic Stabilization without Fusion in Elderly Patients Is It Effective?
 Advances in Orthopedics Volume 2013, Article ID 365059, 7 pages http://dx.doi.org/10.1155/2013/365059 Clinical Study Adult s Degenerative Scoliosis: Midterm Results of Dynamic Stabilization without Fusion
Advances in Orthopedics Volume 2013, Article ID 365059, 7 pages http://dx.doi.org/10.1155/2013/365059 Clinical Study Adult s Degenerative Scoliosis: Midterm Results of Dynamic Stabilization without Fusion
The Fusion of Power and Performance.
 The Fusion of Power and Performance. Leading the Way in Lumbar Interbody Fusion with 1 Years of Clinical Results. The JAGUAR Lumbar I/F CAGE System, approved in the U.S. in February 1999, has revolutionized
The Fusion of Power and Performance. Leading the Way in Lumbar Interbody Fusion with 1 Years of Clinical Results. The JAGUAR Lumbar I/F CAGE System, approved in the U.S. in February 1999, has revolutionized
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Interlaminar Decompression & Stabilization. Reginald Davis, M.D., FAANS, FACS Director of Clinical Research
 Interlaminar Decompression & Stabilization Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Background Device meant to stabilize the spine without fusion following decompression
Interlaminar Decompression & Stabilization Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Background Device meant to stabilize the spine without fusion following decompression
Adjacent segment disease after anterior cervical discectomy and fusion
 Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse of a Lumbar Spine Vertebral Body
 Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Is unilateral pedicle screw fixation superior than bilateral pedicle screw fixation for lumbar degenerative diseases: a meta-analysis
 Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Clinical Experience With the Dynesys Semirigid Fixation System for the Lumbar Spine
 Clinical Experience With the Dynesys Semirigid Fixation System for the Lumbar Spine Surgical and Patient-Oriented Outcome in 50 Cases After an Average of 2 Years Dieter Grob, MD,* Arnoldo Benini, MD,*
Clinical Experience With the Dynesys Semirigid Fixation System for the Lumbar Spine Surgical and Patient-Oriented Outcome in 50 Cases After an Average of 2 Years Dieter Grob, MD,* Arnoldo Benini, MD,*
Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis
 Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Dynamic Stabilization and Sports. Low back pain is a common problem with 60-80% of the world s population suffering from
 Dynamic Stabilization and Sports Assoc. Prof. Dr. Olcay ESER Prof. Dr. Ali Fahir ÖZER Low back pain is a common problem with 60-80% of the world s population suffering from low back pain (1). Although
Dynamic Stabilization and Sports Assoc. Prof. Dr. Olcay ESER Prof. Dr. Ali Fahir ÖZER Low back pain is a common problem with 60-80% of the world s population suffering from low back pain (1). Although
) ACDF. (Japanese Orthopaedic Association,JOA) ACCF (175.4±12.1ml VS 201.3±80.4ml) ACDF JOA VAS (P=0.000),ACCF :A : X(2015)
 2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
Original Policy Date
 MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit
 Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Lumbar Dynamic. Reinhold Knebel Product Manager
 Lumbar Dynamic Reinhold Knebel Product Manager The DSS system provides options for dynamic and rigid stabilization to treat hypermobile segments and segments that require fusion. Allows pedicle displacement
Lumbar Dynamic Reinhold Knebel Product Manager The DSS system provides options for dynamic and rigid stabilization to treat hypermobile segments and segments that require fusion. Allows pedicle displacement
Caudal Vertebral Body Fractures Following Lateral Interbody Fusion in Nonosteoporotic Patients
 The Ochsner Journal 14:123 130, 2014 Ó Academic Division of Ochsner Clinic Foundation Caudal Vertebral Body Fractures Following Lateral Interbody Fusion in Nonosteoporotic Patients Gabriel C. Tender, MD
The Ochsner Journal 14:123 130, 2014 Ó Academic Division of Ochsner Clinic Foundation Caudal Vertebral Body Fractures Following Lateral Interbody Fusion in Nonosteoporotic Patients Gabriel C. Tender, MD
Effects of cord pretension and stiffness of the Dynesys system spacer on the biomechanics of spinal decompression- a finite element study
 Shih et al. BMC Musculoskeletal Disorders 2013, 14:191 RESEARCH ARTICLE Open Access Effects of cord pretension and stiffness of the Dynesys system spacer on the biomechanics of spinal decompression- a
Shih et al. BMC Musculoskeletal Disorders 2013, 14:191 RESEARCH ARTICLE Open Access Effects of cord pretension and stiffness of the Dynesys system spacer on the biomechanics of spinal decompression- a
