Risk factors related to the failure of venous leg ulcers to heal with compression treatment
|
|
|
- Darcy McGee
- 6 years ago
- Views:
Transcription
1 From the American Venous Forum Risk factors related to the failure of venous leg ulcers to heal with compression treatment Dragan J. Milic, PhD, a Sasa S. Zivic, MD, a Dragan C. Bogdanovic, MD, b Nevena D. Karanovic, PhD, c and Zoran V. Golubovic, PhD, b Nis, Republic of Serbia Background: Compression therapy is the most widely used treatment for venous leg ulcers and it was used in different forms for more than 400 years. Published healing rates of venous ulcers obtained with compression therapy vary widely from 40-95%. According to numerous studies, it has been suggested that the application of external pressure to the calf muscle raises the interstitial pressure resulting in improved venous return and reduction in the venous hypertension. Several risk factors have been identified to be correlated with the failure of venous leg ulcers to heal with compression therapy (longer ulcer duration; large surface area; fibrinous deposition present on >50% of the wound surface and an Ankle Brachial Pressure Index (ABPI) of <0.85. Methods: An open prospective single-center study was performed in order to determine possible risk factors associated with the failure of venous ulcers to heal when treated with multi-layer high compression bandaging system for 52 weeks. In the study, 189 patients (101 women, 88 men; mean age 61 years) with venous leg ulcers (ulcer surface >5 cm 2 ; duration >3 months) were included. The study excluded patients with arterial disease (ABPI <0.8), heart insufficiency with ejection fraction (EF) <35, pregnancy, cancer disease, rheumatoid arthritis, and diabetes. Based on clinical opinion and available literature, the following were considered as potential risk factors: sex, age, ulceration surface, time since ulcer onset, previous operations, history of deep vein thrombosis, body mass index (BMI), reduction in calf circumference >3 cm during the first 50 days of treatment, walking distance during the day <200 meters, calf:ankle circumference ratio <1.3, fixed ankle joint, history of surgical wound debridement, >50% of wound covered with fibrin, depth of the wound >2 cm. Results: Within 52 weeks of limb-compression therapy, 24 (12.7%) venous ulcers had failed to heal. A small ulceration surface (<20 cm 2 ), the duration of the venous ulcer <12 months, a decrease in calf circumference of more than 3 cm, and emergence of new skin islets on >10% of wound surface during the first 50 days of treatment were favorable prognostic factors for ulcer healing. A large BMI (>33 kg/m 2 ), short walking distance during the day (<200 m), a history of wound debridement, and ulcers with deepest presentation (>2 cm) were indicators of slow healing. Calf:ankle circumference ratio <1.3, fixed ankle joint, and reduced ankle range of motion were the only independent parameters associated with non-healing (P <.001). Conclusion: The results obtained in this study suggest that non-healing venous ulcers are related to the impairment of the calf muscle pump. (J Vasc Surg 2009;49: ) Chronic venous insufficiency and venous leg ulcers are a major health problem because of their high prevalence and associated high cost of care. Compression therapy is the most widely used treatment for venous leg ulcers and it was used in different forms for more than 400 years. 1 The mechanism of action of compression therapy in the treatment of venous leg ulcers is not completely understood. According to numerous studies, it has been suggested that the application of external pressure to the calf muscle raises the interstitial pressure resulting in improved venous return and reduction in the venous hypertension. 2,3 Published healing rates of venous ulcers obtained with compression therapy vary widely from 40-95% Several risk factors have been identified to be correlated with the failure of venous leg ulcers to heal with compression therapy (longer From the Clinic for Vascular Surgery, Clinical Center Nis, a Medical School, University of Nis, b University Megatrend. c Competition of interest: none. Presented at the Twentieth Annual Meeting of the American Venous Forum, Feb 20-23, 2008, Charleston, SC. Reprint requests: Dragan J. Milic, PhD, Vascular Clinic Clinical Centre Nis, Bulevar Nemanjica 72A/25, Nis, Republic of Serbia ( dmilic@ptt.rs OR drmilic@beotel.net) /$36.00 Copyright 2009 by the Society for Vascular Surgery. doi: /j.jvs ulcer duration, large surface area, fibrinous deposition present on 50% of the wound surface, and an Ankle Brachial Pressure Index [ABPI] of 0.85). 11 The purpose of this study was to identify possible risk factors related to the failure of venous leg ulcers to heal with compression treatment. METHODS An open prospective single-center study was performed in order to determine possible risk factors associated with the failure of venous ulcers to heal when treated with multi-layer high compression bandaging system for 52 weeks. Patients aged at least 16-years-old with leg ulceration of venous etiology were screened for inclusion in the trial. Before inclusion in the study, all patients underwent color duplex scan examination (CDS) and ABPI measurements. CDS examinations were performed using Siemens Sonoline Sienna (Erlangen, Germany) ultrasonography scan device with a 7 MHz probe. Venous compressibility and flow characteristics were the key elements to exclude thrombosis. The direction of flow was assessed in a reverse Trendelenburg position during Valsalva maneuver. A cuff inflation-deflation method with rapid cuff deflation in the
2 JOURNAL OF VASCULAR SURGERY Volume 49, Number 5 Milic et al 1243 Table I. Demographic and clinical characteristics of patients by outcome groups Characteristic Healed by week 26 (n 95) Healed by week 27 to 52 (n 70) P Total healed (n 165) Not healed (n 24) P Ulceration surface 20 cm 2 24 (25) 47 (67) (43) 13 (54).306 Wound duration 12 months 31 (33) 49 (70) (48) 14 (58).368 Female gender 51 (54) 37 (53) (53) 13 (54).939 Age (years) Previous operations 38 (40) 33 (47) (43) 10 (42).900 Deep vein thrombosis 38 (40) 21 (30) (36) 9 (37).868 BMI (12) 19 (27) (18) 3 (12).773 Reduction in calf circumference 73 (77) 37 (53) (67) 12 (50).112 Daily walking distance 200 m 5 (5) 12 (17) (10) 2 (8).765 Calf:ankle circumference ratio (10) 12 (17) (13) 18 (75).001 Fixed ankle joint and ROM 20 5 (5) 7 (10) (7) 16 (67).001 Ulcer recurrence 95 (100) 70 (100) 165 (100) 24 (100) Wound debrided surgically 11 (12) 18 (26) (18) 3 (12).771 Wound covered with fibrin 50% 11 (12) 34 (49) (27) 8 (33).538 Lipodermatosclerosis 84 (88) 61 (87) (88) 24 (100).082 Depth of the wound 2 cm 8 (8) 20 (29) (17) 5 (21).577 Emergence of new skin islets 29 (30) 9 (13) (23) 2 (8).100 Values are given as number (percent) or mean SD. BMI, Body mass index; ROM, range of motion; SD, standard deviation. standing position was performed to induce reflux. The presence of reflux was determined by the direction of flow (significant flow toward the feet was suggestive of reflux). A reflux time of 0.5 seconds has been used to diagnosis the presence of reflux. The study excluded patients with an ABPI 0.8 (27 patients), patients with heart insufficiency with an ejection fraction (EF) 35 (1 patient), pregnancy (1 patient), cancer disease (3 patients), rheumatoid arthritis (2 patients), and diabetes (11 patients). Thirteen patients with unidentified cause of leg ulcer were also excluded from the study. Only patients with verified venous ulcers (ulcer surface 5 cm 2 ; duration 3 months) were included in the study. Wound size was determined by measurement (maximal length and width) as well as by computerized process consists of mapping the two-dimensional digital image onto the polygonal mesh. The margins of a wound were outlined on a computer screen and the enclosed wound area was automatically determined. Digital images were taken with the Sony Cyber Shot (Kohda, Japan) digital camera T10. The digital image included a 5 cm-long calibration marker positioned below the wound surface. The wound area was evaluated every 15 days. Two hundred fifty-eight patients were considered for the study and 200 were included. Eleven patients were lost during the study and 189 patients (101 women, 88 men; mean age 61 years) with venous leg ulcers completed the study. Based on clinical opinion and available literature, the following were considered as potential risk factors: sex, age (years), ulceration surface (cm 2 ), time since ulcer onset (months), previous operations (stripping, superficial endoscopic perforator vein surgery [SEPS]), history of deep vein thrombosis, body mass index (BMI), reduction in calf circumference 3 cm during the first 50 days of treatment, walking distance 200 meters during the day, calf:ankle circumference (CAC) ratio 1.3, fixed ankle joint and reduced ankle range of motion (ROM) ( 20 ), ulcer recurrence, history of surgical wound debridement, 50% of wound covered with fibrin, depth of the wound 2 cm, and emergence of new skin islets on more than 10% of ulcer surface during the first 50 days of treatment. Time since ulcer onset, previous operations, history of surgical wound debridement, and history of deep vein thrombosis (DVT) were determined according to medical documentation. The BMI was calculated at the beginning of the treatment. The depth of the wound was measured using a cotton-tipped applicator that was inserted into the deepest portion of the wound. The applicator was marked with the pen at skin level and the distance was measured from the tip to the mark. Calf and ankle circumference were measured in the recumbent position with the maximal (calf) and minimal (ankle) point determined visually. Calf: ankle ratio was determined at the beginning of the treatment and afterwards every 30 days. Walking distance during the day was determined according to the patient s daily activities and patients who had predominantly inactive and sessile lifestyle were considered to walk less than 200 meters per day. The wound surface covered with fibrin and surface of new skin islets were determined using a sheet of transparency film that was placed over the wound, and the boundary of the entire wound and wound surface covered with fibrin or surface of new skin islets were drawn with a marking pen on the film. The surfaces were analyzed and ratio was calculated. Ankle ROM was determined with the patient in the supine position by goniometry during maximal voluntary plantar flexion and dorsiflexion of the ankle. ROM was determined as the sum of plantar flexion and dorsiflexion. The study was approved by relevant authorities and written consent was obtained by all patients included in the study. The same treatment team comprised of three doctors and three medical nurses treated all patients. The patients
3 1244 Milic et al JOURNAL OF VASCULAR SURGERY May 2009 were treated at the Clinic for Vascular Surgery, Clinical Centre of Nis (Serbia) on an ambulatory basis with the primary endpoint of the study being complete ulcer healing at 26 and 52 weeks. After ulcer healing, patients were instructed to continue to wear Tubulcus elastic stockings (35 mm Hg, Laboratoires Innothera, Arcueil, France) in order to avoid recurrence. During the treatment, patients were monitored by the study team at least once a week. Treatment regimen. The standard regimen was to debride the wound. This was a normally simple mechanical debridement with sterile gauze in order to remove slough and other dead tissue. According to the extent of the wound, exudation dressings were changed from 1 to 7 days. Extensive wound exudation was treated with crystal acidum boricum (after debridement, acidum boricum was applied over the wound in a thin layer) and in patients with no exudation, dry dressings were performed. No antibiotics were used and patients in both groups received only aspirin (100 mg). After wound debridement and dressing bandaging systems were applied, the bandaging system was applied as follows: - First and second layer were cotton gauze without tension (50% overlap) and cotton crepe bandage. - Third layer in the treatment group consisted of readymade tubular compression device (Tubulcus) that exerts graduated pressure with the highest compression (30-40 mm Hg) at the ankle, diminishing up the calf, and corresponds to class III compression stockings. It is open-toed and has no heel. Because it is a tubular, knitted, ready-made device, the appropriate pressure is exerted regardless of the fitter s skill. Tubulcus can be reused and laundered at 60 C. Device size was determined for each patient according to the circumferences of the leg measured at the ankle and the largest part of the calf (5 sizes - S, M, L, XL, and XXL - were available). The circumference of the limb was measured every 4 weeks during the treatment and according to these measurements a new pair of Tubulcus was applied. If the measurements of the limb stayed in the initial size, Tubulcus was changed after 6 months. - The fourth layer was medium-stretch elastic bandage (100% stretch) 15 cm wide and 5 m long (Niva, Novi Sad, Serbia) in a spiral with a 50% overlap. The elastic bandages were applied with the patient in the recumbent position and the foot in dorsal flexion. One pair of elastic bandages was changed regularly every 3 months. The patient was advised to walk 30 minutes after bandaging. The bandaging systems were worn day and night. Although compliance was not formally assessed, there were no withdrawals from the study because of noncompliance. Endpoints and statistical analyses. Primary endpoint of the study was complete ulcer healing at 26 and 52 weeks. In cases where the original ulcer closed but a new area developed on the same limb while the original ulcer was still present, the limb was considered to be open until this new area of ulceration had also closed. The definition of ulcer closure was the point at which complete epithelialization of the reference limb occurred. After 52 weeks of treatment, statistical data were collected and analyzed. The patients were classified in 3 groups: (1) patients with unhealed ulcers, (2) patients with ulcers that healed in less than 26 weeks, and (3) patients with ulcers that healed from 26 to 52 weeks (Table I). Analysis of potential risk factors associated with the failure of a venous leg ulcer to heal with compression treatment was performed between the patients with healed and unhealed ulcers (Table II). Also, analysis of risk factors were performed between the patients with healed ulcers taking into account time for healing ( 26 weeks and weeks) in order to define possible indicators of slow healing and favorable prognostic factors for ulcer healing (Table III). Statistical methods. To assess the magnitude of the effects of given risk factor, single variable logistic regression was performed to estimate odds ratios (ORs) with 95% confidence intervals (CIs). The age was used as continuous, and all other factors as categorical variables. Reported P values are for the Wald statistics, calculated as the estimated regression coefficient divided by its standard error. To calculate adjusted ORs, multivariate logistic regression was performed using unconditional Enter method, where all other risk factors, except the risk factor of interest, were held constant. Independent-samples t test was used to compare means between two groups. Mantel- Haenszel 2 test and Fisher exact test were performed for the frequencies comparison. Statistical analyses were conducted using SPSS Version 10.0 software (SPSS Inc, Chicago, Ill). RESULTS One hundred eighty-nine patients treated for a venous leg ulcer completed the study. One hundred one patients (53.4%) were women, and 88 patients (46.6%) were men. The mean patient s age at the first office visit was 61.4 years (range, years). After 52 weeks of limb compression therapy, 24 ulcers (12.7%) had failed to heal. The healing rate at 26 and 52 weeks of limb compression therapy was 50.26% and 87.3%, respectively. The median number of previous episodes of ulceration was 4.7 (range, 2-11), the median size of the ulcer was 29.3 cm 2 (range, cm 2 ), and 83.6% of ulcers were medial, 13.2% were lateral, 2.1% were circumferential, and 1.1% were a combination. The median duration of the ulcer was 6.2 years (range, 4 months-17 years). Sixty-eight patients (36%) had previous DVT. Pain, edema, pigmentation, and lipodermatosclerosis were present in all 189 patients (100%). Eighty-one patients (42.9%) had previously undergone some surgical procedure (stripping of greater saphenous vein [GSV] was performed in 72 patients (38.1%) and 9 patients (4.8%) underwent SEPS procedure). Mean time from operation until inclusion in the study was 8.9 years (range, 20 months 29 years). During the observation period, neither
4 JOURNAL OF VASCULAR SURGERY Volume 49, Number 5 Milic et al 1245 Table II. Influence of the risk factors on the failure of a venous leg ulcer to heal Risk factor Unadjusted OR (95% CI) P Adjusted OR (95% CI) P Ulceration surface 20 cm ( ) ( ).70 Wound duration 12 months 1.49 ( ) ( ).40 Female gender 1.03 ( ) ( ).22 Age (years) 1.00 ( ) ( ).19 Previous operations 0.95 ( ) ( ).66 Deep vein thrombosis 1.08 ( ) ( ).58 BMI ( ) ( ).74 Reduction in calf circumference 0.50 ( ) ( ).96 Daily walking distance 200 m 0.79 ( ) ( ).92 Calf:ankle circumference ratio ( ) ( ).001 Fixed ankle joint and ROM ( ) ( ).001 Wound debrided surgically 0.67 ( ) ( ).28 Wound covered with fibrin 50% 1.33 ( ) ( ).38 Depth of the wound 2 cm 1.29 ( ) ( ).61 Emergence of new skin islets 0.30 ( ) ( ).39 OR, Odds ratio; CI, confidence interval; BMI, body mass index; ROM, range of motion. Table III. Influence of the risk factors on the prolonged time of a venous leg ulcer to heal Risk factor Unadjusted OR (95% CI) P Adjusted OR (95% CI) P Ulceration surface 20 cm ( ) ( ).002 Wound duration 12 months 4.82 ( ) ( ).011 Female gender 0.97 ( ) ( ).36 Age (years) 0.99 ( ) ( ).27 Previous operations 1.34 ( ) ( ).16 Deep vein thrombosis 0.64 ( ) ( ).29 BMI ( ) ( ).04 Reduction in calf circumference 0.34 ( ) ( ).002 Daily walking distance 200 m 3.72 ( ) ( ).53 Calf:ankle circumference ratio ( ) ( ).09 Fixed ankle joint and ROM ( ) ( ).11 Wound debrided surgically 2.64 ( ) ( ).30 Wound covered with fibrin 50% 7.21 ( ) ( ).001 Depth of the wound 2 cm 4.35 ( ) ( ).44 Emergence of new skin islets 0.34 ( ) ( ).004 OR, Odds ratio; CI, confidence interval; BMI, body mass index; ROM, range of motion. surgery nor sclerotherapy was performed in the patients included in the study. There were no deaths or major complications during the treatment period. The CEAP classification was as follows: (a) Clinical-all included limbs had active ulceration (C6); (b) Etiologic: 58.7% of the patients had primary chronic venous insufficiency (CVI) while 41.3% of the patients were classified as secondary CVI. Secondary etiology was based on ultrasound scan findings. (c) Anatomic: perforating vein reflux was documented at duplex scanning in 90 patients (47.6%). Association of perforating vein reflux with superficial venous reflux was noted in 32 patients (16.9%). The combination of both superficial and deep reflux with perforating vein reflux was observed in 17 (9%). Deep vein reflux was noted in 50 patients (26.5%). (d) Pathophysiologic: the pathophysiology identified was reflux in all 189 limbs (100%). Risk factors associated with prolonged healing time and non-healing of venous ulcers using compression treatment and statistical analysis. To assess the magnitude of the effects of given risk factor on prolonged time of a venous leg ulcer to heal, only data for healed patients were included in logistic regression models and healed within 26 weeks/healed by week 27 to 52 was set as dichotomous dependent variable. Unadjusted analyses revealed several significant associations between failure of wounds to heal within 26 weeks and the measured risk factors. Ulceration area greater than 20 cm 2,wound duration longer than 12 months, BMI value higher than 33 kg/m 2, daily walking distance shorter than 200 meters, history of surgical wound debridement, 50% of wound surface covered with fibrin, and depth of the wound greater than 2 cm significantly increased the odds of not healing within 26 weeks. In contrast, reduction in calf circumference for more than 3 cm during the first 50 days of treatment and emergence of new skin islets on more than 10% of wound surface signif-
5 1246 Milic et al JOURNAL OF VASCULAR SURGERY May 2009 icantly reduced the risk of not healing within 26 weeks. Sex, age, previous operations, DVT, CAC ratio less than 1.3, and fixed ankle joint with reduced ankle ROM were not associated with prolonged time of a venous leg ulcer to heal. The association between the failure of wounds to heal within 26 weeks and daily walking distance shorter than 200 meters, surgical wound debridement, and depth of the wound greater than 2 cm became attenuated after adjustment for other risk factors (Table III). Unadjusted and adjusted analysis revealed significant associations between failure of wounds to heal within 1 year and the CAC ratio less than 1.3 and fixed ankle joint with reduced ankle ROM. All other risk factors were not associated with the failure of wounds to heal (Table II). According to statistical analysis, all examined risk factors could be classified in four groups: 1. Factors with no influence on ulcer healing (sex, age, previous operations, ulcer recurrence). 2. Favorable prognostic factors for ulcer healing (ulceration surface 20 cm 2, time since ulcer onset 12 months, reduction in calf circumference 3 cm during the first 50 days of treatment, and emergence of new skin islets on more than 10% of ulcer surface). 3. Indicators of slow healing (ulceration surface 20 cm 2, time since ulcer onset 12 months, BMI 33 kg/m 2, walking distance shorter than 200 meters during the day, history of surgical wound debridement, 50% of wound covered with fibrin, depth of the wound 2 cm). 4. Risk factors associated with non-healing (CAC ratio 1.3, fixed ankle joint, and reduced ROM). DISCUSSION The goals of compression therapy in the treatment of venous leg ulcerations are ulcer healing, reduction of pain and edema, and prevention of recurrence. 12 Published healing rates of venous ulcers obtained with compression therapy vary widely from 40-95% Unfortunately, a significant number of venous ulcers remain refractory to compression treatment. A possible way to predict nonhealing venous leg ulcers is to examine prognostic risk factors that are consistently found in a number of published studies (large wound area and wound of long duration). Patients who possess either or both of these factors are at risk for not healing. 4,13,14 The results of our study do not support these findings. Large and long lasting ulcers could be healed although more time is needed. A decrease in wound size during the first 50 days of treatment is a favorable prognostic factor for healing. According to some studies, approximately 50-70% of patients with venous ulcers and a decrease in wound size during the first month of compression therapy will be healed after 6 months of treatment. 4 Although some studies 15 have shown that younger age is a favorable prognostic factor for ulcer healing, we could not prove such a relation. Margolis et al 14 found that venous stripping and the presence of fibrin on more than 50% of the wound surface were the factors associated with the failure of a venous leg ulcer to heal. Our study didn t find any correlation between surgical procedures and ulcer healing while fibrin on more than 50% of the wound surface was an indicator of slow healing. The most difficult ulcers to treat with compression therapy showing non-healing tendency in our study were the ulcers with deepest presentation ( 2 cm in depth) and ulcers with history of surgical debridement. The reason for this is, in our opinion, complete destruction of skin structures and lack of growth factors present in dermis making the healing process more difficult. The emergence of new skin islets on the wound surface, a favorable factor for ulcer healing in our study, never happened in these patients. A reduction in calf circumference for more than 3 cm during the first 50 days of compression treatment was a favorable factor for fast ulcer healing ( 26 weeks). This was especially notable for the patients with calf circumference larger than 40 cm at the beginning of the treatment. In obese patients, more time is needed for ulcer closure and high BMI ( 33 kg/m 2 ) was an indicator of slow healing. Short walking distance during the day ( 200 meters) was also an indicator of slow healing. We think that main reason for this is immobility of these patients and inactivity of their muscle pump. It may be prudent to introduce intermittent pneumatic compression in the treatment of these patients in order to stimulate muscle pump and to improve ulcer healing. Our study of 1 year of compression treatment is longer than many other studies and this may be the reason in the discrepancy of risk factors. If the analysis had been carried out with non-healing at 6 months of compression treatment, then some risk factors do align with other studies. 4,13,14 The only independent parameters associated with nonhealing of venous ulcers when treated with compression therapy were CAC ratio 1.3 and fixed ankle joint with reduced ankle ROM (P.001). Fixed ankle joint and reduced ankle ROM is well described as a significant factor in venous ulceration development. Limited ROM was significantly correlated to EF and residual volume fraction measured by air plethysmographic measurement indicating the importance of calf pump function in the development of venous ulceration. 16 Our study strongly supports these findings. One of the main contributors to decreased ankle ROM in patients with CVI is probably inactivity. Bed rest and prolonged inactivity may lead to muscle atrophy, contracture, and degenerative joint disease. Pain with ankle motion could also cause a decrease in voluntary ankle flexion and extension. 16 CAC ratio 1.3 was also an indicator of non-healing venous ulcers. The vast majority of patients included in our study ( 60%) had CAC ratio between the values of 1.6 and 1.9 and over 80% of patients had CAC ratio between the values of 1.4 and 2.2.
6 JOURNAL OF VASCULAR SURGERY Volume 49, Number 5 Milic et al 1247 In our study, patients with the lowest CAC ratio ( ) were the most difficult to treat. It is interesting that the healing process was more difficult also in those patients who developed a low CAC ratio during the compression treatment ( 1.2). This could be an indicator of the patient s inactivity during the treatment. Also, this could mean that too excessive pressure was implemented for too long a time leading to calf muscle atrophy. We think that in this case, compression system with lower interface pressure values should be implemented. Our results emphasize the importance of the calf muscle pump in the development of venous ulcers, which is in concordance with many published studies indicating the importance of calf muscle pump dysfunction CONCLUSION The results obtained in this study suggest that nonhealing venous ulcers are related to the impairment of the calf muscle pump. Further trials are necessary to identify the best treatment options especially for non-healing ulcers. AUTHOR CONTRIBUTIONS Conception and design: MD, ZS, ZG Analysis and interpretation: MD, ZS, DB, ZG Data collection: MD, ZS Writing the article: MD, DB Critical revision of the article: MD, ZS, DB, NK, ZG Final approval of the article: MD, ZS, DB, NK, ZG Statistical analysis: DB Obtained funding: NK, ZG Overall responsibility: MD REFERENCES 1. Kiev J, Kerstein MD. Venous insufficiency and graded compression therapy. Wounds 1993;5: Bergan JJ, Schmid-Schönbein GW, Smith PD, Nicolaides AN, Boisseau MR, Eklof B. Chronic venous disease. N Engl J Med 2006;355: Eberhardt RT, Raffetto JD. Chronic venous insufficiency. Circulation 2005;111: Kikta MJ, Schuler JJ, Meyer JP Jr, Durham JR, Eldrup-Jorgensen J, Schwarcz TH, Flanigan DP. A prospective, randomized trial of Unna s boots versus hydroactive dressing in the treatment of venous stasis ulcers. J Vasc Surg 1988;7: Milic DJ, Zivic SS, Bogdanovic DC, Perisic ZD, Milosevic ZD, Jankovic RJ, et al. A randomized trial of the Tubulcus multilayer bandaging system in the treatment of extensive venous ulcers. J Vasc Surg 2007; 46: Mayberry JC, Moneta GL, Taylor LM Jr, Porter JM. Fifteen year results of ambulatory compression therapy for chronic venous ulcer. Surgery 1991;109: Nelson EA, Harper DR, Ruckley CV, Prescott RJ, Gibson B, Dale JJ. A randomized trial of single layer and multi-layer bandages in the treatment of chronic venous ulceration. Phlebology 1995;1: Marston WA, Carlin RE, Passman MA, Farber MA, Keagy BA. Healing rates and cost efficacy of outpatient compression treatment for leg ulcers associated with venous insufficiency. J Vasc Surg 1999;30: Partsch H, Damstra RJ, Tazelaar DJ, Schuller-Petrovic S, Velders AJ, de Rooij MJ, et al. Multicentre, randomised controlled trial of four-layer bandaging versus short-stretch bandaging in the treatment of venous leg ulcers. Vasa 2001;30: Blecken SR, Villavicencio JL, Kao TC. Comparison of elastic versus nonelastic compression in bilateral venous ulcers: a randomized trial. J Vasc Surg 2005;42: Margolis DJ, Berlin JA, Strom BL. Which venous leg ulcers will heal with limb compression bandages? Am J Med 2000;109: Abu-Own A, Scurr JH, Coleridge Smith PD. Effect of leg elevation on the skin microcirculation in chronic venous insufficiency. J Vasc Surg 1994;20: Fletcher A, Cullum N, Sheldon TA. A systematic review of compression treatment for venous leg ulcers. BMJ 1997;315: Margolis DJ, Berlin JA, Strom BL. Risk factors associated with the failure of a venous leg ulcer to heal. Arch Dermatol 1999;135: Skene AI, Smith JM, Doré CJ, Charlett A, Lewis JD. Venous leg ulcers: a prognostic index to predict time to healing. BMJ 1992;305: Back TL, Padberg FT Jr, Araki CT, Thompson PN, Hobson RW 2nd. Limited range of motion is a significant factor in venous ulceration. J Vasc Surg 1995;22: Araki CT, Back TL, Padberg FT, Thompson PN, Jamil Z, Lee BC, et al. The significance of calf muscle pump function in venous ulceration. J Vasc Surg 1994;20:872-7; discussion Neglén P, Raju S. A rational approach to detection of significant reflux with duplex Doppler scanning and air plethysmography. J Vasc Surg 1993;17: Welkie JF, Comerota AJ, Kerr RP, Katz ML, Jayheimer EC, Brigham RA. The hemodynamics of venous ulceration. Ann Vasc Surg 1992; 6:1-4. Submitted Aug 31, 2008; accepted Nov 15, 2008.
A randomized trial of the Tubulcus multilayer bandaging system in the treatment of extensive venous ulcers
 From the American Venous Forum A randomized trial of the Tubulcus multilayer bandaging system in the treatment of extensive venous ulcers Dragan J. Milic, PhD, a Sasa S. Zivic, MD, a Dragan C. Bogdanovic,
From the American Venous Forum A randomized trial of the Tubulcus multilayer bandaging system in the treatment of extensive venous ulcers Dragan J. Milic, PhD, a Sasa S. Zivic, MD, a Dragan C. Bogdanovic,
Prospective evaluation of chronic venous insufficiency based on foot venous pressure measurements and air plethysmography findings
 Prospective evaluation of chronic venous insufficiency based on foot venous pressure measurements and air plethysmography findings Masato Fukuoka, MD, Takaki Sugimoto, MD, and Yutaka Okita, MD, Kobe, Japan
Prospective evaluation of chronic venous insufficiency based on foot venous pressure measurements and air plethysmography findings Masato Fukuoka, MD, Takaki Sugimoto, MD, and Yutaka Okita, MD, Kobe, Japan
chronic venous disorders, varicose vein, CEAP classification, lipodermatosclerosis, Klippel- Trenaunay syndrome DVT CVD
 Online publication August 27, 2009 chronic venous disorders: CVD CEAP 4 CEAP CVD J Jpn Coll Angiol, 2009, 49: 201 205 chronic venous disorders, varicose vein, CEAP classification, lipodermatosclerosis,
Online publication August 27, 2009 chronic venous disorders: CVD CEAP 4 CEAP CVD J Jpn Coll Angiol, 2009, 49: 201 205 chronic venous disorders, varicose vein, CEAP classification, lipodermatosclerosis,
2013 Vol. 24 No
 2013 Vol. 24 No. 3 333 1 2 2013 24 3 317-322 1 2 1 2 2012 8 6 57 333 Table 1 Compression bandages available in Japan Classification Feature Name Distributor Short stretch non-cohesive Comprilan Terumo
2013 Vol. 24 No. 3 333 1 2 2013 24 3 317-322 1 2 1 2 2012 8 6 57 333 Table 1 Compression bandages available in Japan Classification Feature Name Distributor Short stretch non-cohesive Comprilan Terumo
elastic stockings or inelastic bandages for ulcer treatment
 ICC - Compression session May 14, 2015 elastic stockings or inelastic bandages for ulcer treatment Giovanni Mosti; Lucca; Italy DISCLOSURE: NO CONFLICT OF INTEREST leg ulcers 31.619 patients venous 47.6
ICC - Compression session May 14, 2015 elastic stockings or inelastic bandages for ulcer treatment Giovanni Mosti; Lucca; Italy DISCLOSURE: NO CONFLICT OF INTEREST leg ulcers 31.619 patients venous 47.6
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device
 VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
pressure of compression stockings matters (clinical importance of pressure)
 Classification of Compression Stockings ICC Meeting, Copenhagen, May 17, 2013. pressure of compression stockings matters (clinical importance of pressure) Giovanni Mosti; Lucca, Italy disclosure no conflict
Classification of Compression Stockings ICC Meeting, Copenhagen, May 17, 2013. pressure of compression stockings matters (clinical importance of pressure) Giovanni Mosti; Lucca, Italy disclosure no conflict
Calf compression pressure required to achieve venous closure from supine to standing positions
 Calf compression pressure required to achieve venous closure from supine to standing positions Bernhard Partsch, MD, and Hugo Partsch, MD, Vienna, Austria Background: Compression therapy needs to narrow
Calf compression pressure required to achieve venous closure from supine to standing positions Bernhard Partsch, MD, and Hugo Partsch, MD, Vienna, Austria Background: Compression therapy needs to narrow
Compression therapy is the primary treatment for. Elastic Multilayer Bandages for Chronic Venous Insufficiency: Features of Our Technique
 Ann Vasc Dis Vol.5, No.3; 2012; pp 347 351 2012 Annals of Vascular Diseases doi: 10.3400/avd.oa.12.00020 Original Article Elastic Multilayer Bandages for Chronic Venous Insufficiency: Features of Our Technique
Ann Vasc Dis Vol.5, No.3; 2012; pp 347 351 2012 Annals of Vascular Diseases doi: 10.3400/avd.oa.12.00020 Original Article Elastic Multilayer Bandages for Chronic Venous Insufficiency: Features of Our Technique
New Guideline in venous ulcer treatment: dressing, medication, intervention
 New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
Increased blood flow. natural healing response. generates a. Wound Healing. Providing increased blood circulation to promote wound healing from inside
 Increased blood flow generates a natural healing response Wound Healing Providing increased blood circulation to promote wound healing from inside Increased blood circulation generates a natural healing
Increased blood flow generates a natural healing response Wound Healing Providing increased blood circulation to promote wound healing from inside Increased blood circulation generates a natural healing
Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA, CPC
 Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA, CPC Advisor, APMA Coding Committee Advisor, APMA MACRA Task Force Expert Panelist, Codingline Fellow, American
Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA, CPC Advisor, APMA Coding Committee Advisor, APMA MACRA Task Force Expert Panelist, Codingline Fellow, American
Venous Insufficiency Ulcer
 Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
Chronic Venous Disease: A Complex Disorder. A N Nicolaides
 Chronic Venous Disease: A Complex Disorder A N Nicolaides Emeritus Professor of Vascular Surgery, Imperial College, London. Hon. Professor of Surgery, University of Nicosia Medical School, Cyprus Disclosures
Chronic Venous Disease: A Complex Disorder A N Nicolaides Emeritus Professor of Vascular Surgery, Imperial College, London. Hon. Professor of Surgery, University of Nicosia Medical School, Cyprus Disclosures
Efficacy of Velcro Band Devices in Venous and. Mixed Arterio-Venous Patients
 Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
The influence of wound geometry on the measurement of wound healing rates in clinical trials
 The influence of wound geometry on the measurement of wound healing rates in clinical trials Daniel R. Gorin, MD, Paul R. Cordts, MD, Wayne W. LaMorte, MD, PhD, MPH, and James O. Menzoian, MD, Boston,
The influence of wound geometry on the measurement of wound healing rates in clinical trials Daniel R. Gorin, MD, Paul R. Cordts, MD, Wayne W. LaMorte, MD, PhD, MPH, and James O. Menzoian, MD, Boston,
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Classification for elastic tubes, medical socks and soft bandaging?
 Classification for elastic tubes, medical socks and soft bandaging? Dr. Martin Abel Head of Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG Copenhagen, 17.05.2013 1 Standard Bandages in UK
Classification for elastic tubes, medical socks and soft bandaging? Dr. Martin Abel Head of Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG Copenhagen, 17.05.2013 1 Standard Bandages in UK
2017 Florida Vascular Society
 Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
How does compression really work?
 How does compression really work? Felizitas Pannier Private Practice Phlebology & Dermatology, Bonn, Germany Many thanks to Hugo Partsch, Horst Gerlach and Hans-Jürgen Thomä for some of the pictures Compression
How does compression really work? Felizitas Pannier Private Practice Phlebology & Dermatology, Bonn, Germany Many thanks to Hugo Partsch, Horst Gerlach and Hans-Jürgen Thomä for some of the pictures Compression
Tsunehisa Sakurai, MD, Masahiro Matsushita, MD, Naomichi Nishikimi, MD, and Yuji Nimura, MD, Nagoya, Japan
 Hemodynamic assessment of femoropopliteal venous reflux in with primary varicose veins patients Tsunehisa Sakurai, MD, Masahiro Matsushita, MD, Naomichi Nishikimi, MD, and Yuji Nimura, MD, Nagoya, Japan
Hemodynamic assessment of femoropopliteal venous reflux in with primary varicose veins patients Tsunehisa Sakurai, MD, Masahiro Matsushita, MD, Naomichi Nishikimi, MD, and Yuji Nimura, MD, Nagoya, Japan
Inelastic versus elastic leg compression in chronic venous insufficiency: A comparison limb size and venous hemodynamics
 Inelastic versus elastic leg compression in chronic venous insufficiency: A comparison limb size and venous hemodynamics of Richard K. Spence, MD, and Elizabeth Cahall, RN, BSN, Camden, N.J., and Staten
Inelastic versus elastic leg compression in chronic venous insufficiency: A comparison limb size and venous hemodynamics of Richard K. Spence, MD, and Elizabeth Cahall, RN, BSN, Camden, N.J., and Staten
Chronic Venous Insufficiency Compression and Beyond
 Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Dr Paul Thibault. Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology
 Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
A short review of diagnosis and compression therapy of chronic venous. insufficiency, Clinical picture and diagnosis A B S T R A C T WORDS
 A short review of diagnosis and compression therapy of chronic venous insufficiency N. Kecelj Leskovec, M. D. Pavlovi}, and T. Lunder A B S T R A C T Introduction: Chronic venous insufficiency (CVI) is
A short review of diagnosis and compression therapy of chronic venous insufficiency N. Kecelj Leskovec, M. D. Pavlovi}, and T. Lunder A B S T R A C T Introduction: Chronic venous insufficiency (CVI) is
The Influence of Dressings on Venous Ulcer Healing--A Randomised Trial
 Eur J Vasc Endovasc Surg 13, 174-179 (1997) The Influence of Dressings on Venous Ulcer Healing--A Randomised Trial M. C. Stacey*, A. G. Jopp-Mckay, P. Rashid, S. E. Hoskin and P. J. Thompson University
Eur J Vasc Endovasc Surg 13, 174-179 (1997) The Influence of Dressings on Venous Ulcer Healing--A Randomised Trial M. C. Stacey*, A. G. Jopp-Mckay, P. Rashid, S. E. Hoskin and P. J. Thompson University
Consider the impact of Venous Disease Review elements in the workup and diagnosis of Venous Disease Review treatment considerations
 Gregory Bohn, MD FACS Clinical Symposium on Advances in Skin and Wound Care September 9-12, 2011 Gaylord National Washington, DC Consider the impact of Venous Disease Review elements in the workup and
Gregory Bohn, MD FACS Clinical Symposium on Advances in Skin and Wound Care September 9-12, 2011 Gaylord National Washington, DC Consider the impact of Venous Disease Review elements in the workup and
Additional Information S-55
 Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing?
 Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing? Susan Whitelaw RVT, RDMS PURPOSE Duplex imaging of the lower extremity veins is performed to assess the deep
Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing? Susan Whitelaw RVT, RDMS PURPOSE Duplex imaging of the lower extremity veins is performed to assess the deep
Velcro Compression Devices
 Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options
 Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Chronic Venous Insufficiency
 Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING
 HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
OHTAC Recommendation. Endovascular Laser Treatment for Varicose Veins. Presented to the Ontario Health Technology Advisory Committee in November 2009
 OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015
 Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015 Anatomy of Perforating veins Cadaveric studies 1 have shown >60 vein perforating veins from superficial to deep Normal
Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015 Anatomy of Perforating veins Cadaveric studies 1 have shown >60 vein perforating veins from superficial to deep Normal
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Good bye slippage a new fusion to tackle bandage slippage on the foot. Presenters: Josefin Damm & Andreas Nilsson
 Good bye slippage a new fusion to tackle bandage slippage on the foot Presenters: Josefin Damm & Andreas Nilsson Disclaimer/Conflict of Interest Josefin Damm: Co-inventor of Lundatex products, co-founder
Good bye slippage a new fusion to tackle bandage slippage on the foot Presenters: Josefin Damm & Andreas Nilsson Disclaimer/Conflict of Interest Josefin Damm: Co-inventor of Lundatex products, co-founder
NCVH. Ultrasongraphy: State of the Art Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW
 Ultrasongraphy: State of the Art 2015 NCVH New Cardiovascular Horizons Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW Anil K. Chagarlamudi, M.D. Cardiovascular
Ultrasongraphy: State of the Art 2015 NCVH New Cardiovascular Horizons Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW Anil K. Chagarlamudi, M.D. Cardiovascular
Leg ulcers. Causes and management. OBJECTIVE This article outlines the assessment and management of patients with leg ulceration.
 THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
Arterial & Venous Ulcers. A Comprehensive Review Assessment & Management
 Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
From the American Venous Forum
 From the American Venous Forum Digital venous photoplethysmography in the seated position is a reproducible noninvasive measure of lower limb venous function in patients with isolated superficial venous
From the American Venous Forum Digital venous photoplethysmography in the seated position is a reproducible noninvasive measure of lower limb venous function in patients with isolated superficial venous
Best Practice: What can Physical Therapists do to Create Change? Purpose
 Best Practice: Assessment & Intervention for Patients with Wounds in Home Health What can Physical Therapists do to Create Change? Mitchell Brotsky, Kira D Annunzio Advisor: Tony D Alonzo Arcadia University
Best Practice: Assessment & Intervention for Patients with Wounds in Home Health What can Physical Therapists do to Create Change? Mitchell Brotsky, Kira D Annunzio Advisor: Tony D Alonzo Arcadia University
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
JOURNAL OF WOUND CARE. VOLUME 8. NUMBER 9. October A comparison of sub-bandage pressures produced with two multi-layer bandaging systems
 JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The effect of graded compression elastic stockings on the lower leg venous system during daily activity
 The effect of graded compression elastic stockings on the lower leg venous system during daily activity Chad L. Buhs, MD, Phillip J. Bendick, PhD, and John L. Glover, MD, Royal Oak, Mich Purpose: We evaluated
The effect of graded compression elastic stockings on the lower leg venous system during daily activity Chad L. Buhs, MD, Phillip J. Bendick, PhD, and John L. Glover, MD, Royal Oak, Mich Purpose: We evaluated
THE IMPACT OF MODIFYING OCCUPATIONAL RISK FACTORS ON THE OUTCOME OF TREATMENT OF CHRONIC VENOUS ULCER.
 Egyptian Journal of Occupational Medicine, 2011; 35 (2) : 277-287 THE IMPACT OF MODIFYING OCCUPATIONAL RISK FACTORS ON THE OUTCOME OF TREATMENT OF CHRONIC VENOUS ULCER. By Refaat T. M.*, Ewis A. A.*, Osman
Egyptian Journal of Occupational Medicine, 2011; 35 (2) : 277-287 THE IMPACT OF MODIFYING OCCUPATIONAL RISK FACTORS ON THE OUTCOME OF TREATMENT OF CHRONIC VENOUS ULCER. By Refaat T. M.*, Ewis A. A.*, Osman
Deep axial reflux, an important contributor to skin changes or ulcer in chronic venous disease
 Deep axial reflux, an important contributor to skin changes or ulcer in chronic venous disease Gudmundur Danielsson, MD, PhD, a Bo Eklof, MD, PhD, b Andrew Grandinetti, PhD, c Fedor Lurie, MD, PhD, a and
Deep axial reflux, an important contributor to skin changes or ulcer in chronic venous disease Gudmundur Danielsson, MD, PhD, a Bo Eklof, MD, PhD, b Andrew Grandinetti, PhD, c Fedor Lurie, MD, PhD, a and
4-layer compression bandaging system (includes microbe binding wound contact layer) Latex-free, 4-layer compression bandaging system
 JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
Venous Reflux Duplex Exam
 Venous Reflux Duplex Exam GWENDOLYN CARMEL, RVT PHYSIOLOGIST, DEPARTMENT OF VASCULAR SURGERY NEW JERSEY VETERANS HEALTHCARE CENTER EAST ORANGE, NJ PURPOSE: To identify patterns of incompetence and which
Venous Reflux Duplex Exam GWENDOLYN CARMEL, RVT PHYSIOLOGIST, DEPARTMENT OF VASCULAR SURGERY NEW JERSEY VETERANS HEALTHCARE CENTER EAST ORANGE, NJ PURPOSE: To identify patterns of incompetence and which
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Self Management with Compression
 Self Management with Compression Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University
Self Management with Compression Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University
Treatment of Chronic Venous Ulcers Using New Four Layers Compressive Bandage Dressing
 ORIGINAL ARTICLE J Nepal Med Assoc 215;53(199):156-61 CC S BY NC OPEN ACCESS Treatment of Chronic Venous Ulcers Using New Four Layers Compressive Bandage Dressing Kaushal K Tiwari, 1 Krishna G Shrestha,
ORIGINAL ARTICLE J Nepal Med Assoc 215;53(199):156-61 CC S BY NC OPEN ACCESS Treatment of Chronic Venous Ulcers Using New Four Layers Compressive Bandage Dressing Kaushal K Tiwari, 1 Krishna G Shrestha,
Venous Disease and Leg Ulcers. Edward G Mackay MD St. Petersburg, FL NCVH 2015 Orlando, FL
 Venous Disease and Leg Ulcers Edward G Mackay MD St. Petersburg, FL NCVH 2015 Orlando, FL Disclosures Stocks Endoshape Sapheon Medical Advisory Board BTG, Boston Scientific Venous Leg Ulcer Most common
Venous Disease and Leg Ulcers Edward G Mackay MD St. Petersburg, FL NCVH 2015 Orlando, FL Disclosures Stocks Endoshape Sapheon Medical Advisory Board BTG, Boston Scientific Venous Leg Ulcer Most common
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: February 15, 2017 Next Review: February, 2019 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: February 15, 2017 Next Review: February, 2019 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Four Layer Versus Actico Cohesive Short Stretch Bandage Background
 Four Layer Versus Actico Cohesive Short Stretch Bandage Background Cochrane Systematic Review 6/2/01 "Five small studies found no difference in healing between multi-layer high compression (4-layer bandage
Four Layer Versus Actico Cohesive Short Stretch Bandage Background Cochrane Systematic Review 6/2/01 "Five small studies found no difference in healing between multi-layer high compression (4-layer bandage
Lower Extremity Venous Disease (LEVD)
 Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
N.S. Theivacumar, R.J. Darwood, M.J. Gough*
 Eur J Vasc Endovasc Surg (2009) 37, 477e481 Endovenous Laser Ablation (EVLA) of the Anterior Accessory Great Saphenous Vein (): Abolition of Sapheno-Femoral Reflux with Preservation of the Great Saphenous
Eur J Vasc Endovasc Surg (2009) 37, 477e481 Endovenous Laser Ablation (EVLA) of the Anterior Accessory Great Saphenous Vein (): Abolition of Sapheno-Femoral Reflux with Preservation of the Great Saphenous
Priorities Forum Statement
 Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Leg ulcers are non-healing
 Clinical Chronic REVIEW WOUNDS Doppler assessment: getting it right Full leg ulcer assessments are important in order to identify the aetiology of patients leg ulcer and Doppler ultrasounds form a part
Clinical Chronic REVIEW WOUNDS Doppler assessment: getting it right Full leg ulcer assessments are important in order to identify the aetiology of patients leg ulcer and Doppler ultrasounds form a part
Distribution and quantification of venous reflux in lower extremity chronic venous stasis disease with duplex scanning
 Distribution and quantification of venous reflux in lower extremity chronic venous stasis disease with duplex scanning Michael S. Weingarten, MD, FACS, Charles C. Branas, MPH, RVT, Michael Czeredarczuk,
Distribution and quantification of venous reflux in lower extremity chronic venous stasis disease with duplex scanning Michael S. Weingarten, MD, FACS, Charles C. Branas, MPH, RVT, Michael Czeredarczuk,
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Inelastic bandages maintain their hemodynamic effectiveness over time despite significant pressure loss
 From the American Venous Forum Inelastic bandages maintain their hemodynamic effectiveness over time despite significant pressure loss Giovanni Mosti, MD, a and Hugo Partsch, MD, PhD, b Lucca, Italy; and
From the American Venous Forum Inelastic bandages maintain their hemodynamic effectiveness over time despite significant pressure loss Giovanni Mosti, MD, a and Hugo Partsch, MD, PhD, b Lucca, Italy; and
Compression Bulletin 30
 0 Compression Bulletin 30 In this issue: Editor s choice Management of chronic venous disease: Clinical practice guidelines of the European Society for Vascular Surgery (ESVS) Members of the European Society
0 Compression Bulletin 30 In this issue: Editor s choice Management of chronic venous disease: Clinical practice guidelines of the European Society for Vascular Surgery (ESVS) Members of the European Society
A rational approach to detection of significant reflux with duplex Doppler scanning and air plethysmography
 A rational approach to detection of significant reflux with duplex Doppler scanning and air plethysmography Peter Negl6n, MD, PhD,* and Seshadri Raju, MD, Al-Ain, United Arab Emirates, and Jackson, Miss.
A rational approach to detection of significant reflux with duplex Doppler scanning and air plethysmography Peter Negl6n, MD, PhD,* and Seshadri Raju, MD, Al-Ain, United Arab Emirates, and Jackson, Miss.
First Coast Service Options (FCSO) Medicare Policy Primer
 First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
Deep Vein Thrombosis
 Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema. Original Policy Date
 MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
pump The significance of calf muscle function in venous ulceration
 The significance of calf muscle function in venous ulceration pump Clifford T. Arald, PhD, Thomas L. Back, MS, RVT, Frank T. Padberg, MD, Peter N. Thompson, MD, Zafar Jamil, MD, Bing C. Lee, MD, Walter
The significance of calf muscle function in venous ulceration pump Clifford T. Arald, PhD, Thomas L. Back, MS, RVT, Frank T. Padberg, MD, Peter N. Thompson, MD, Zafar Jamil, MD, Bing C. Lee, MD, Walter
Promoting best practice in leg ulcer management
 Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
The Early Venous Reflux Ablation (EVRA) ulcer study
 The Early Venous Reflux Ablation (EVRA) ulcer study MS Gohel, F Heatley, X Liu, A Bradbury, R Bulbulia, N Cullum, DM Epstein, I Nyamekye, KR Poskitt, S Renton MS, J Warwick, AH Davies on behalf of the
The Early Venous Reflux Ablation (EVRA) ulcer study MS Gohel, F Heatley, X Liu, A Bradbury, R Bulbulia, N Cullum, DM Epstein, I Nyamekye, KR Poskitt, S Renton MS, J Warwick, AH Davies on behalf of the
The postthrombotic syndrome in relation to venous hemodynamics, as measured by means of duplex scanning and straingauge plethysmography
 The postthrombotic syndrome in relation to venous hemodynamics, as measured by means of duplex scanning and straingauge plethysmography José H. Haenen, RVT, Mirian C.H. Janssen, MD, Herman van Langen,
The postthrombotic syndrome in relation to venous hemodynamics, as measured by means of duplex scanning and straingauge plethysmography José H. Haenen, RVT, Mirian C.H. Janssen, MD, Herman van Langen,
Venous Ulcers. A Little Basic Science. An Aggressive Prescription to Aid Healing. Why do venous ulcers occur? Ambulatory venous hypertension!
 UCSF Vascular Symposium April 26-28, 2012 San Francisco, California True statements about the management of venous ulcers include: An Aggressive Prescription to Aid Healing Anthony J. Comerota, MD, FACS,
UCSF Vascular Symposium April 26-28, 2012 San Francisco, California True statements about the management of venous ulcers include: An Aggressive Prescription to Aid Healing Anthony J. Comerota, MD, FACS,
Venous Leg Ulcers? The prevalence of active leg ulcers in western countries. How Do I Treat. Mary s ulcer. What types of leg ulcers are there?
 Focus on CME at the xxx University of Toronto How Do I Treat Venous Leg Ulcers? David H. Keast, MSc, MD, FCFP Presented at Primary Care Today, Satellite Symposia, October 3, 2003 The prevalence of active
Focus on CME at the xxx University of Toronto How Do I Treat Venous Leg Ulcers? David H. Keast, MSc, MD, FCFP Presented at Primary Care Today, Satellite Symposia, October 3, 2003 The prevalence of active
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat?
 Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
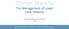
JOURNAL OF VASCULAR SURGERY Volume 50, Number 3 Amsler et al 669 Table I. Design of trials Trial Design Endpoint set at [weeks] Interface pressure [mm
![JOURNAL OF VASCULAR SURGERY Volume 50, Number 3 Amsler et al 669 Table I. Design of trials Trial Design Endpoint set at [weeks] Interface pressure [mm JOURNAL OF VASCULAR SURGERY Volume 50, Number 3 Amsler et al 669 Table I. Design of trials Trial Design Endpoint set at [weeks] Interface pressure [mm](/thumbs/74/70265537.jpg) From the American Venous Forum REVIEW ARTICLES In search of optimal compression therapy for venous leg ulcers: A meta-analysis of studies comparing divers bandages with specifically designed stockings
From the American Venous Forum REVIEW ARTICLES In search of optimal compression therapy for venous leg ulcers: A meta-analysis of studies comparing divers bandages with specifically designed stockings
Compression Bulletin 03 Knowledge Management Published under the auspices of the IUP October 2002
 Compression Bulletin 03 Knowledge Management Published under the auspices of the IUP October 2002 Robert Stemmer Library on Compression Therapy Compression Therapy of the Extremities This book, available
Compression Bulletin 03 Knowledge Management Published under the auspices of the IUP October 2002 Robert Stemmer Library on Compression Therapy Compression Therapy of the Extremities This book, available
Date: A. Venous Health History Form. Patient please complete questions Primary Care Physician:
 E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
Date: A. Venous Health History Form. Patient please complete questions Primary Care Physician:
 E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
Current Management of C0s patient
 Current Management of C0s patient M. Perrin Vascular Surgery, Lyon, France 1 AIM of the PRESENTATION - 1 st to estimate the prevalence of C 0s patient - 2 d to evaluate its current management - 3d to suggest
Current Management of C0s patient M. Perrin Vascular Surgery, Lyon, France 1 AIM of the PRESENTATION - 1 st to estimate the prevalence of C 0s patient - 2 d to evaluate its current management - 3d to suggest
Leg ulceration is a chronic. An evaluation of lower limb 3d scanning and compression hosiery. Product Research/Audit. Abstract
 An evaluation of lower limb 3d scanning and compression hosiery Abstract KEY WORDS Venous ulcers Compression Bespoke hosiery Prevention Aims: To evaluate the effect of bespoke compression hosiery (Therapeutic
An evaluation of lower limb 3d scanning and compression hosiery Abstract KEY WORDS Venous ulcers Compression Bespoke hosiery Prevention Aims: To evaluate the effect of bespoke compression hosiery (Therapeutic
Dr Peter Chapman-Smith
 Dr Peter Chapman-Smith Phlebologist NZ Stem Cell Treatment Centre, Whangarei 12:00-12:30 Healing Those Heartsink Leg Ulcers Healing Those Heartsink Leg Ulcers Practice Nurses Presentation GPCME Christchurch
Dr Peter Chapman-Smith Phlebologist NZ Stem Cell Treatment Centre, Whangarei 12:00-12:30 Healing Those Heartsink Leg Ulcers Healing Those Heartsink Leg Ulcers Practice Nurses Presentation GPCME Christchurch
Management of Post-Thrombotic Syndrome
 Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Imperial College, London, UK
 Eur J Vasc Endovasc Surg 33, 483e487 (07) doi:10.1016/j.ejvs.06.11.033, available online at http://www.sciencedirect.com on Immediate Hemodynamic Effect of the Additional Use of the SCD EXPRESSÔ Compression
Eur J Vasc Endovasc Surg 33, 483e487 (07) doi:10.1016/j.ejvs.06.11.033, available online at http://www.sciencedirect.com on Immediate Hemodynamic Effect of the Additional Use of the SCD EXPRESSÔ Compression
UNDERSTANDING VEIN PROBLEMS
 UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
Case. Wounds. Fundamentals of Ulcer Care. Dr. Mark Meissner Wound Case Study. Compression and Ulcer Healing Cullum NA, Cochrane Reviews 2001
 Case Wounds Mark H. Meissner, MD University of Washington School of Medicine 65 yr old male physician Recurrent R medial malleolar ulcer over 5 years New R lateral malleolar ulcer Intermittently wearing
Case Wounds Mark H. Meissner, MD University of Washington School of Medicine 65 yr old male physician Recurrent R medial malleolar ulcer over 5 years New R lateral malleolar ulcer Intermittently wearing
Solving the Compliance Riddle with Compression Garments
 Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA Editorial Advisory Board, WOUNDS Consulting Editor, Podiatry Management APMA Coding Committee Expert Panelist,
Solving the Compliance Riddle with Compression Garments Jeffrey D. Lehrman, DPM, FASPS, MAPWCA Editorial Advisory Board, WOUNDS Consulting Editor, Podiatry Management APMA Coding Committee Expert Panelist,
Most incompetent calf perforating veins are found in association with superficial venous reflux
 Most incompetent calf perforating veins are found in association with superficial venous reflux Wesley P. Stuart, FRCSEd, a Amanda J. Lee, PhD, b Paul L. Allan, MD, c C. Vaughan Ruckley, ChM, a and Andrew
Most incompetent calf perforating veins are found in association with superficial venous reflux Wesley P. Stuart, FRCSEd, a Amanda J. Lee, PhD, b Paul L. Allan, MD, c C. Vaughan Ruckley, ChM, a and Andrew
Lower Extremity Venous Insufficiency Evaluation
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND
 GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
Description and Management of C0s patient. M. Perrin, Vascular Surgery, Lyon, France
 Description and Management of C0s patient M. Perrin, Vascular Surgery, Lyon, France 1 No disclosure of interest to declare for this presentation 2 AIM of the PRESENTATION 1 st to estimate the prevalence
Description and Management of C0s patient M. Perrin, Vascular Surgery, Lyon, France 1 No disclosure of interest to declare for this presentation 2 AIM of the PRESENTATION 1 st to estimate the prevalence
S Shivakumar, Gopi Tupkar, N Ravishankar and Divakar. The Pharma Innovation Journal 2017; 6(7):
 2017; 6(7): 120-128 ISSN (E): 2277-7695 ISSN (P): 2349-8242 NAAS Rating 2017: 5.03 TPI 2017; 6(7): 120-128 2017 TPI www.thepharmajournal.com Received: 20-05-2017 Accepted: 21-06-2017 S Shivakumar Gopi
2017; 6(7): 120-128 ISSN (E): 2277-7695 ISSN (P): 2349-8242 NAAS Rating 2017: 5.03 TPI 2017; 6(7): 120-128 2017 TPI www.thepharmajournal.com Received: 20-05-2017 Accepted: 21-06-2017 S Shivakumar Gopi
AWMA MODULE ACCREDITATION. Module Three: Assessment and Management of Lower Leg Ulceration
 AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
