Conflict of Interest Disclosure
|
|
|
- Angelina Rich
- 6 years ago
- Views:
Transcription
1 Inpatient Ketamine Infusion to Treat Acute Pain Crisis Refractory to Opioids in Sickle Cell Disease Robert Montgomery, DNP, RN-BC, ACNS-BC Associate Professor of Anesthesiology University of Colorado School of Medicine Clinical Coordinator Acute Pain Service University of Colorado Hospital East 17th Ave Aurora, CO Conflict of Interest Disclosure Pacira Pharmaceuticals: one time honoraria for serving on nursing advisory board Objectives Identify specific factors that complicate effective pain control during acute pain crises in sickle cell disease in the acute care setting Discuss the actual and potential beneficial effects of ketamine infusion for sickle cell disease patients with acute pain crises and with chronic pain Create a plan for using ketamine infusions to treat acute and chronic pain conditions in the acute care setting 1
2 Management of Sickle Cell Pain Crisis Effectively treat pain Parenteral opioid therapy (morphine, hydromorphone, fentanyl) IV PCA preferred AVOID meperidine (risk of seizures) NSAIDs, local heat, other adjunctive measures Medication offered around the clock, not PRN (use PCA or sustained-release, standing doses) Transition to oral short-acting opioid pain medication Be sure any other factors are recognized and addressed No evidenced based strategy: expert opinion Pain in Sickle Cell Disease Acute, intermittent, unpredictable, severe episodes called crisis Typical duration said to be 7-10 days Associated by some patients with death Onset may occur in early infancy Chronic pain may develop in adolescence and adulthood Not necessarily acute vaso-occlusion Other pain still occurs (e.g. injury, menses, SLE) To be distinguished from acute vaso-occlusion PAIN TYPE Nocioceptive Deep somatic Superficial somatic Visceral Neuropathic Pain in Sickle Cell Disease ORIGINS & SYNDROMES Vaso-occlusion, bone infarction, priapism- Leg ulcers Splenic/hepatic sequestration, splenic infarction, cholelithiasis Peripheral neuropathy Vaso-occlusion, neuropathies Central neuropathic CNS damage, central sensitization (?) Mixed Breakthrough Vaso-occlusion Incident (movement) Vaso-occlusion, skeletal damage Nonincident Transient flares of pain during analgesia Adapted from Niscola, Pain Medicine10:470,
3 Adult SCD Pain Common, but Managed at Home PiSCESdata from 31,017 daily pain diaries from 232 patients Crisis Utilization 3.5% Crisis No utilization 12.7% Pain Not Crisis 38.3% No Pain 45.5% Smith, Ann Intern Med148:94, 2008 Tissue infarction/fibrosis Everything else that affects humans: abnormal processing of nociceptive pain Central sensitization Allodynia: increased nociception to normally innocuous stimuli Hyperalgesia: excessive painful response to a painful stimulus Unfortunately, in SCD there are LOTS of such ongoing stimuli Chronic Pain in SCD Cheng, CurrPain Headache Rep14:213, 2010 Sickle Cell Pain and Catastrophizing Catastrophizing: High degree of aversion associated with pain-eliciting situations Pay more attention to pain sensations Ruminization, magnification of pain Helplessness when dealing with pain For sickle cell patients: Higher than in other pain groups (e.g. RA, spinal cord injury, back pain) Associated with depression and lower quality of life Worse in people with milder syndromes -?fewer chronic symptoms, less opportunity to adapt A Citero, Pain 133:39,
4 Challenges and Complexities Acute Sickle Cell Pain with Baseline Chronic Pain Chronic opioid therapy Significant opioid tolerance Poor response to parenteral opioid therapy Poor response to non-opioid adjuvants Opioid rotation ineffective or unavailable (allergy, intolerance, refusal) Opioid induced hyperalgesia (OIH) High readmission rates Poor or no outpatient management Poor medication compliance -opioid withdrawal Development of chronic neuropathic pain through sensitization of spinal neurons from repeated noxious stimuli Opioid Tolerant Patient Acute pain management in the opioid tolerant patient presents a significant challenge to nurses Opioid only based analgesic regimens are usually marginally effective and dose escalation increases patient risk and provider concern Multimodal analgesic techniques recommended by national practice guidelines are not always feasible or sufficient This situation results in poor quality pain management, patient suffering, and staff frustration and dissatisfaction 11 Opioid Induced Hyperalgesia (OIH) A state of nociceptive sensitization caused by exposure to opioids. The condition is characterized by a paradoxical response whereby a patient receiving opioids for the treatment of pain could actually become more sensitve to certain painful stimuli. Characteristics Worsening pain over time in spite of and because of increases in opioid dose Nociceptive sensitization Area of pain more diffuse Pain of lesser quality and harder to pinpoint 4
5 What is Ketamine IT IS NOT AN OPIOID It s a dissociative anesthetic that works as a NMDA receptor antagonist Used as an anesthetic -profound analgesia Produces catatonic state, psychotomimetic effects during recovery ( dissociative state) Analgesia maintained in sub-anesthetic low doses Can be very effective in crisis situation: tolerant patient with severe pain, unresponsive to high dose opioids 13 Ketamine Opioid tolerance and the development of neuropathic pain both involve activation of NMDA receptors Ketamine as an NMDA receptor antagonist may represent a 2-for-1 type intervention, helping to overcome tolerance to opioids as well as attenuating neural sensitization Through blockingthe N-methyl-D-aspartate (NMDA) receptor, ketamine impairs sensitization of spinal neurons to nociceptive stimuli and may, therefore, impede development of and blunt neuropathic pain. Mechanism of Action Inhibits binding of excitatory aminioacids (glutamate, aspartate) to the N-methyl-D-aspartate (NMDA) receptor in the CNS, blocking the transmission of painful stimuli NMDA antagonism produces analgesia, limits the development of opioid tolerance and hyperalgesia Elevates circulating epinepherineand norepinephrine leading to increased HR, BP, cardiac output, and vascular resistance No respiratory depressant effects when given in low doses 15 5
6 Mechanism of Action Strong pain stimuli activate NMDA receptors and produce hyperexcitability of dorsal root neurons This induces central sensitization - the windup phenomenon - and hyperalgesia NMDA antagonism can reverse/limit hyperalgesia and the wind-up phenomenon 16 NMDA Receptor and Tolerance Repeated μ opioid receptor activation via prolonged large dose opioid use leads to increased NMDA receptor activity and the development of tolerance Ketamine has been shown to block this increased NMDA activity and can prevent the development of tolerance 17 Himmelseher: Anesthesiology, Volume 102(1).January (350) 18 6
7 Fig. 2. In sensitization and opioid tolerance-related phenomena, pathologic pain is an expression of neuronal plasticity. After activation of intracellular kinase cascades, transcriptionindependent phosphorylation of key membrane receptors and channels, such the N-methyld-aspartate Nervous (NMDA) receptor, System is initiated. This increases Plasticity neuronal excitability for tens of minutes after cessation of the initiating stimulus. Long-term hypersensitivity is also regulated by mitogen-activated protein kinases (MAP kinases) viatranscription of gene products. Protein kinase (PK) C, a series of other protein kinase families, and nitric oxide (NO)/cGMP/PKG are activated allows after NMDA-mediated persistent increases in intracellular pain calcium (Ca2+) and or µ-opioid receptor binding to opioid receptors. Increased Ca2+ stimulates Ca2+/calmodulin, and Ca2+/calmodulin kinase (CaMK) pathways. These and inflammatory transmitters stimulate adenylcyclase camp PKA signaling. Several cascades then converge on MAP kinases, such as the extracellular continuous signal-regulated kinases (ERK). use These of processes opioids facilitate association to of key signaling molecules with postsynaptic density (PSD) proteins in the NMDA receptor. This leads to kinase phosphorylation of NMDA receptor subunits and up-regulation of NMDA receptor currents. Enhanced downstream signaling ensues and, in this vicious circle, potentiates NMDA receptor lower function and pain synaptic efficacy thresholds, and, thus, pain sensitization. In long-term hypersensitivity, CaMKand inflammation-related signaling kinases converge MAP kinases, such as p38map kinases, which is followed by phosphorylation of promoters with the initiation of gene cause transcription. The central campresponse element sensitization binding protein (CREB), MAP kinases, and CaMKIVmay also cause transcription viadirect phosphorylation of gene promoters. Intervention with ketamine blocks NMDA receptor currents and connected downstream signaling. Regarding pain sensitization and opioid phenomenon, a common mechanism underlying leading ketamine s preventive to action the appears Wind-Up to be the perturbation of increased assembly of PSD proteins tyrosine kinase NMDA receptor protein subunits. This reduces phosphorylation and functional NMDA receptor up-regulation. In the future, the cascades presented may evolve as important targets for new pain reducing drugs with similar but more specific phenomenon, responses than those caused by ketamine. and [triangle-headed upwards arrow] = pathophysiological increase or activation, [triangle-headed downwards arrow] = pathophysiological decrease or reduction, [up arrow] = increase or activation related to severe pain or opioid use, [down arrow] = decrease or reduction related to ketamine blockade. contribute to pathologic pain 19 Pharmacokinetics Metabolized and then conjugated in the liver before being excreted in the urine, with minimally active metabolites. Onset of 1-2 minutes Duration of action 60 minutes. Half-life is 2.5 hours 20 Selected Literature 3 Systematic Reviews: Carstensen & Moller 2010; Laskowski et al. 2011; Bell et al (Cochrane Review) Consistently found or showed a trend towards Reduced postop opioid needs and PONV Increased time to rescue analgesic Generally well tolerated Heterogeneity of trials acknowledged as a limitation UCH Ketamine MUE: Baumgartner & Lyda months; 95 patients; stopped in 11 patients, 4 for HTN/Tachy 43 patients (45%) required transfer from M-S unit Did not look at pain scores or opioid consumption 21 7
8 UCH Ketamine Study in Sickle Cell Disease Background Sickle cell disease (SCD) is characterized by hemolytic anemia and vasoocclusion, which can lead to acute and chronic pain (i.e. recurrent sickle cell pain crises) There are no current evidence-based treatment strategies for SCD pain A small subset of this population requires chronic opioid medications for pain control, which poses greater risk of opioid dependence, tolerance and opioid-induced hyperalgesia Anecdotal case reports suggest ketamine is a useful analgesic adjunct in decreasing pain scores and opioid consumption UCH Ketamine Study in Sickle Cell Disease Objectives Characterize the effects of ketamine infusion on inpatient opioid intake Characterize the effects of ketamine infusion on inpatient pain scores Compare opioid prescription dose requirements at admission and discharge UCH Ketamine Study in Sickle Cell Disease Population All adult patients with SCD who were admitted to the University of Colorado Hospital (UCH) Anschutz Inpatient Pavilion with chief complaint of a sickle cell pain crisis between January 2009 and December 2016 Patients whose pain was refractory to opioids and were treated with continuous ketamine infusion 8
9 UCH Ketamine Study in Sickle Cell Disease Data Collection Number of eligible ketamine infusion episodes and control episodes per patient Ketamine episodes: Data collected from day preceding initial ketamine infusion to discharge Non-ketamine episodes (control): Data collected from admission to discharge Total dose of opioids given each day for each ketamine and non-ketamine episode, converted to PO morphine equivalents per day (MED, mg) Pain scores using Numeric Rating Scale (0-10 pts), averaged for each day in each ketamine and non-ketamine episode Opioid prescription dosage (MED) at admission and discharge for each episode Incidence of discontinued ketamine infusions due to adverse side effects UCH Ketamine Study in Sickle Cell Disease Data Analysis Linear mixed-effects regression was used to analyze trends in opioid intake and pain scores over time with and without ketamine infusion Repeated measures were accounted for using random intercepts 9
10 70 Trends in Opioid Prescription Dosages 60 Proportions (%) Increased Unchanged Decreased Ketamine Non-ketamine UCH Ketamine Study in Sickle Cell Disease Population Characteristics 60 ketamine infusion episodes in 9 patients 12 non-ketamine infusion episodes in 6 patients Inpatient Opioid Intake Ketamine: Significant decrease in opioid dose by MED (SE=13.42 mg, p<0.0001) on average each day of the infusion Non-ketamine: Significant increase in opioid dose by 79.7 MED (SE=18.99, p<0.0001) on average each day of admission 10
11 UCH Ketamine Study in Sickle Cell Disease Pain Scores Ketamine: Significant decrease in pain scores by 0.11 pts/day (SE=0.024, p<0.0001) on average each day of the infusion Non-ketamine: Decrease in pain scores by pts/day (SE=0.031, p=0.21) on average each day of admission Opioid Prescriptions Ketamine infusion does not appear to reduce opioid dosage when admission MED was compared to discharge MED after ketamine infusion UCH Ketamine Study in Sickle Cell Disease Ketamine Discontinuations 6 ketamine infusions (9.62%) discontinued due to adverse side effects: Altered neurological state (hallucinations, confusion) Dizziness and lightheadedness Sedation UCH Ketamine Study in Sickle Cell Disease Conclusions Ketamine infusion beneficially serves as an analgesic adjunct in managing sickle cell pain by significantly reducing opioid intake and pain scores The use of ketamine may also help to reduce the risks of opioid tolerance and opioid-induced hyperalgesia Pain scores are more significantly reduced when managed with ketamine as an analgesic adjunct than with opioids and other analgesics alone 11
12 UCH Ketamine Study in Sickle Cell Disease Limitations Analyses include outlier episodes in ketamine and nonketamine infusion groups Non-ketamine infusion episodes were not identified for 3 patients Unreported pain scores from 14 ketamine infusion episodes and 2 non-ketamine infusion episodes Inconsistent time frame between ketamine and non-ketamine data collection UCH Nursing Guideline Low Dose Ketamine Infusion Analgesia Suitable candidates for analgesic dose ketamine are those with uncontrolled moderate to severe pain refractory to conventional therapies such as epidural infusion, IVPCA, nerve blocks, opioids, and non-opioid therapies. It may be particularly helpful for those with a history of chronic opioid use and tolerance, neuropathic pain, or intolerable side effects from conventional therapies. 35 Low Dose Ketamine Infusion Dosing There is great variance in individual response to intended and unintended effects Dose ranges are suggested starting and end points The patient response should guide dosing adjustments As with opioid drugs, the phrase the dose that works is the dose that works applies. The goal is maximize the beneficial effects of ketamine and minimize opioid escalation 36 12
13 What Do you Need to Watch For? BP greater than 180/100 HR greater than 120 PT excessively agitated or sedated Pt complaining of hallucinations Anxiety related side effects can be treated with lorazepam 37 Other Random Facts Telemetry and continuous pulse ox at all times. Pump must be checked by 2 RNs like PCAs You CAN NOT Y in any other meds into a ketamine line. Must be run through own line. Ptsshould be placed on a bed alarm. 38 When Do You Document BP, HR, pain level every 15min for the first hour Then 2 hrsx 2hrs Q4 hours for remainder of administration Check VS Q30min after any dose change
14 What Do You Document? BP, HR, O2, RR Pain intensity, sedation level Side effect/complications Evaluation of pt response to intervention. Pt and family education 40 What does it do? Ketamine Breakdown Sheet What do you need to know? How does it work? Ketamine is an N-methyl-D-aspartate (NMDA) receptor antagonist that works in the CNS NMDA antagonism produces analgesia and limits the development of opioid tolerance IV onset: 30 seconds and full effect in 1 min Duration: 60 min Half-life: 2.5 hours Adverse Effects Nausea and Vomiting Vivid Dreams Hallucinations Anxiety Hypertension Nystagmus Notes Acute Pain Service will manage the Ketamine infusion at a dose from1-30mg/hr. Concentration is 1mg/cc Max dose for any bolus is 5 mg Contraindications Absolute: Psychosis Relative: Poorly controlled hypertension, angina, congestive heart failure, stroke, PTSD, recent head injury Anxiety/hallucination Reduction Treatment of Choice Benzodiazepines usually lorazepam Monitoring Telemetry and continuous pulse ox at all times. Initiation of infusion: BP, HR, pain level every 15min for the first hour Then every 2 hrsx 1, then Q4 hours Q4 hours for remainder of administration Check VS 30min after any dose change Dose and pump must be checked by 2 RNs upon arrival to the floor with any rate changes, and at change of shift Documentation Blood pressure, heart rate, pulse ox, respiratory rate Pain intensity, sedation level Side effect/complications Evaluation of patient response to intervention. Patient and family education 14
15 UCH Ketamine Policy Final Thoughts References Baumgartner, L. Lyda, C. (2014). Incidence of Adverse Drug Effects Associated with Low-Dose Ketamine Infusions. Poster session presented at the meeting of Canadian Critical Care Conference, Whistler, British Columbia, Canada. Bell, R. F., Dahl, J. B., Moore, R. A., Kalso, E. A. (2006). Perioperative ketamine for acute postoperative pain. Cochrane Database of Systematic Reviews Issue 1. Art. No.: CD DOI: / CD pub2 Carstensen, M. & Moller, A. M., (2010). Adding ketamine to morphine for intravenous patient-controlled analgesia for acute postoperative pain: a qualitative review of randomized trials. British Journal of Anaesthesia, 104(4), Laskowski, K., Stirling, A., McKay, W. P., & Lim, H. J., (2011). A systematic review of intravenous ketamine for postoperative analgesia. Canadian Journal of Anesthesia, 58, Rackic, A. M., and Golembiewski, J. (2009). Low dose ketamine infusion for postoperative pain management. Journal of PerianesthesiaNursing 24(4),
What do we want for pain medications?
 New Trends in Pain Pharmacotherapy Dr. Chi Wai Cheung MBBS(HK), FHKCA, FHKAM(Anaesthesiology), Dip Pain Mgt(HKCA) Clinical Assistant Professor Department of Anaesthesiology The University of Hong Kong
New Trends in Pain Pharmacotherapy Dr. Chi Wai Cheung MBBS(HK), FHKCA, FHKAM(Anaesthesiology), Dip Pain Mgt(HKCA) Clinical Assistant Professor Department of Anaesthesiology The University of Hong Kong
Acute pain management in opioid tolerant patients. Muhammad Laklouk
 Acute pain management in opioid tolerant patients Muhammad Laklouk General principles An adequate review and assessment Provision of effective analgesia (including attenuation of tolerance and hyperalgesia)
Acute pain management in opioid tolerant patients Muhammad Laklouk General principles An adequate review and assessment Provision of effective analgesia (including attenuation of tolerance and hyperalgesia)
The Role of Ketamine in the Management of Complex Acute Pain
 The Role of Ketamine in the Management of Complex Acute Pain Dr James Bennett Consultant Anaesthetist Consultant Lead for Inpatient Pain Service East Sussex Healthcare NHS Trust STAPG Committee Member
The Role of Ketamine in the Management of Complex Acute Pain Dr James Bennett Consultant Anaesthetist Consultant Lead for Inpatient Pain Service East Sussex Healthcare NHS Trust STAPG Committee Member
SEEING KETAMINE IN A NEW LIGHT
 SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
Acute Pain NETP: SEPTEMBER 2013 COHORT
 Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Corporate Medical Policy
 Corporate Medical Policy Intravenous Anesthetics for the Treatment of Chronic Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravenous_anesthetics_for_the_treatment_of_chronic_pain
Corporate Medical Policy Intravenous Anesthetics for the Treatment of Chronic Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravenous_anesthetics_for_the_treatment_of_chronic_pain
Pain management. Coleman Palliative Care Conference: February 2016 Josh Baru MD Stacie Levine MD
 Pain management Coleman Palliative Care Conference: February 2016 Josh Baru MD Stacie Levine MD Case #1 61 yo man with history of Stage 3 colon cancer, s/p resection and adjuvant chemotherapy with FOLFOX
Pain management Coleman Palliative Care Conference: February 2016 Josh Baru MD Stacie Levine MD Case #1 61 yo man with history of Stage 3 colon cancer, s/p resection and adjuvant chemotherapy with FOLFOX
POST OPERATIVE PAIN MANAGEMENT: PAIN AND COMPLICATIONS
 POST OPERATIVE PAIN MANAGEMENT: PAIN AND COMPLICATIONS November 9, 2018 Aimee LaMere, CNP Molly McNaughton, CNP Leslie Weide, MSW, LICSW, ACM Disclosures: Conflict of interest statement: We certify that,
POST OPERATIVE PAIN MANAGEMENT: PAIN AND COMPLICATIONS November 9, 2018 Aimee LaMere, CNP Molly McNaughton, CNP Leslie Weide, MSW, LICSW, ACM Disclosures: Conflict of interest statement: We certify that,
Anaesthesia and Pain Management for Endo Exo Femoral Prosthesis (EEFP) Bridging the Gap from Surgery to Rehabilitation
 Anaesthesia and Pain Management for Endo Exo Femoral Prosthesis (EEFP) Bridging the Gap from Surgery to Rehabilitation Dr Ajay Kumar Senior Lecturer Macquarie and Melbourne University Introduction Amputee
Anaesthesia and Pain Management for Endo Exo Femoral Prosthesis (EEFP) Bridging the Gap from Surgery to Rehabilitation Dr Ajay Kumar Senior Lecturer Macquarie and Melbourne University Introduction Amputee
The Pain of Pain: or Patience for Patients
 The pain of pain or: Patience for Patients Alan Bielsky Objectives Discuss mechanisms of acute on chronic pain Explain the practical use of multimodal analgesia Detail different regimens that may benefit
The pain of pain or: Patience for Patients Alan Bielsky Objectives Discuss mechanisms of acute on chronic pain Explain the practical use of multimodal analgesia Detail different regimens that may benefit
Associate Professor Supranee Niruthisard Department of Anesthesiology Faculty of Medicine Chulalongkorn University January 21, 2008
 Associate Professor Supranee Niruthisard Department of Anesthesiology Faculty of Medicine Chulalongkorn University January 21, 2008 PAIN MECHANISMS Somatic Nociceptive Visceral Inflammatory response sensitizes
Associate Professor Supranee Niruthisard Department of Anesthesiology Faculty of Medicine Chulalongkorn University January 21, 2008 PAIN MECHANISMS Somatic Nociceptive Visceral Inflammatory response sensitizes
Intravenous lidocaine infusions. Dr Ian McConachie FRCA FRCPC
 Intravenous lidocaine infusions Dr Ian McConachie FRCA FRCPC Thank the organisers for inviting me. No conflicts or disclosures Lidocaine 1 st amide local anesthetic Synthesized in 1943 by Lofgren in Sweden.
Intravenous lidocaine infusions Dr Ian McConachie FRCA FRCPC Thank the organisers for inviting me. No conflicts or disclosures Lidocaine 1 st amide local anesthetic Synthesized in 1943 by Lofgren in Sweden.
Learning Objectives. Perioperative goals. Acute Pain in the Chronic Pain Patient for Ambulatory Surgery 9/8/16
 Acute Pain in the Chronic Pain Patient for Ambulatory Surgery Danielle Ludwin, MD Associate Professor of Anesthesiology Division of Regional and Orthopedic Anesthesia Columbia University Medical Center
Acute Pain in the Chronic Pain Patient for Ambulatory Surgery Danielle Ludwin, MD Associate Professor of Anesthesiology Division of Regional and Orthopedic Anesthesia Columbia University Medical Center
Collaboration. Opioids. Ketamine. epidural Best Practice. Waterloo Wellington HPC Protocol
 HPC hpcconnection.ca Neuro - axial Nursing cross sector Collaboration Analgesia Pharmacists Intractable patient centered Opioids Ketamine Interventional Consensus Anesthesia Physicians evidence based epidural
HPC hpcconnection.ca Neuro - axial Nursing cross sector Collaboration Analgesia Pharmacists Intractable patient centered Opioids Ketamine Interventional Consensus Anesthesia Physicians evidence based epidural
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Neuropathic Pain in Palliative Care
 Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Use of PCA devices in Difficult Populations
 Use of PCA devices in Difficult Populations Diane M. Santangelo MS RN ANP-C Stony Brook University Medical Center Acute Pain Service September 10, 2011 1 PCA technology? Why Bother? Costly Nurses complain:
Use of PCA devices in Difficult Populations Diane M. Santangelo MS RN ANP-C Stony Brook University Medical Center Acute Pain Service September 10, 2011 1 PCA technology? Why Bother? Costly Nurses complain:
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM. Is This Strictly a Pain Episode? Decision 7: Referrals
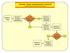 ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
Pain. November 1, 2006 Dr. Jana Pilkey MD, FRCP(C) Internal Medicine, Palliative Medicine
 Pain November 1, 2006 Dr. Jana Pilkey MD, FRCP(C) Internal Medicine, Palliative Medicine Objectives To be able to define pain To be able to evaluate pain To be able to classify types of pain To learn appropriate
Pain November 1, 2006 Dr. Jana Pilkey MD, FRCP(C) Internal Medicine, Palliative Medicine Objectives To be able to define pain To be able to evaluate pain To be able to classify types of pain To learn appropriate
Pain is a common complication
 Section Editors: Heather M. Hylton and Wendy H. Vogel Ketamine Protocol for Palliative Care in Cancer Patients With Refractory Pain BRIGHTON A. LOVEDAY, MSN, ANP-BC, AOCNP, ACHPN, APRN, and JILL SINDT,
Section Editors: Heather M. Hylton and Wendy H. Vogel Ketamine Protocol for Palliative Care in Cancer Patients With Refractory Pain BRIGHTON A. LOVEDAY, MSN, ANP-BC, AOCNP, ACHPN, APRN, and JILL SINDT,
Digital RIC. Rhode Island College. Linda M. Green Rhode Island College
 Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2013 The Relationship
Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2013 The Relationship
ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT
 ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT Jeff Gadsden, MD, FRCPC, FANZCA Associate Professor Duke University Department of Anesthesiology Regional Anesthesia and Acute Pain Medicine DISCLOSURES
ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT Jeff Gadsden, MD, FRCPC, FANZCA Associate Professor Duke University Department of Anesthesiology Regional Anesthesia and Acute Pain Medicine DISCLOSURES
Analgesic Drugs PHL-358-PHARMACOLOGY AND THERAPEUTICS-I. Mr.D.Raju,M.pharm, Lecturer
 Analgesic Drugs PHL-358-PHARMACOLOGY AND THERAPEUTICS-I Mr.D.Raju,M.pharm, Lecturer Mechanisms of Pain and Nociception Nociception is the mechanism whereby noxious peripheral stimuli are transmitted to
Analgesic Drugs PHL-358-PHARMACOLOGY AND THERAPEUTICS-I Mr.D.Raju,M.pharm, Lecturer Mechanisms of Pain and Nociception Nociception is the mechanism whereby noxious peripheral stimuli are transmitted to
Goals for sedation during mechanical ventilation
 New Uses of Old Medications Gina Riggi, PharmD, BCCCP, BCPS Clinical Pharmacist Trauma ICU Jackson Memorial Hospital Disclosure I do not have anything to disclose Objectives Describe the use of ketamine
New Uses of Old Medications Gina Riggi, PharmD, BCCCP, BCPS Clinical Pharmacist Trauma ICU Jackson Memorial Hospital Disclosure I do not have anything to disclose Objectives Describe the use of ketamine
Pain Management Strategies Webinar/Teleconference
 Pain Management Strategies Webinar/Teleconference Barry K. Baines, MD April 16, 2009 Objectives Describe the principles of pain management. Identify considerations in the use of opioids. Describe the benefits
Pain Management Strategies Webinar/Teleconference Barry K. Baines, MD April 16, 2009 Objectives Describe the principles of pain management. Identify considerations in the use of opioids. Describe the benefits
Opioid reduction strategies in an academic tertiary medical center
 Opioid reduction strategies in an academic tertiary medical center Terry Bosen, PharmD Medication Safety Program Director Vanderbilt University Medical Center Tennessee MME data per capita MME = Morphine
Opioid reduction strategies in an academic tertiary medical center Terry Bosen, PharmD Medication Safety Program Director Vanderbilt University Medical Center Tennessee MME data per capita MME = Morphine
PAIN TERMINOLOGY TABLE
 PAIN TERMINOLOGY TABLE TERM DEFINITION HOW TO USE CLINICALLY Acute Pain Pain that is usually temporary and results from something specific, such as a surgery, an injury, or an infection Addiction A chronic
PAIN TERMINOLOGY TABLE TERM DEFINITION HOW TO USE CLINICALLY Acute Pain Pain that is usually temporary and results from something specific, such as a surgery, an injury, or an infection Addiction A chronic
Analgesia for ERAS programs. Dr Igor Lemech VMO Anaesthetist Wagga Wagga Base Hospital
 Analgesia for ERAS programs Dr Igor Lemech VMO Anaesthetist Wagga Wagga Base Hospital Disclosure I have received honoraria from Mundipharma and MSD The new Wagga Wagga Rural Referral Centre Scope Analgesic
Analgesia for ERAS programs Dr Igor Lemech VMO Anaesthetist Wagga Wagga Base Hospital Disclosure I have received honoraria from Mundipharma and MSD The new Wagga Wagga Rural Referral Centre Scope Analgesic
1/21/14. Cancer Related Pain: Case-Based Pharmacology. Conflicts of Interest. Learning Objective
 Cancer Related Pain: Case-Based Pharmacology Jeannine M. Brant, PhD, APRN, AOCN Oncology Clinical Nurse Specialist Nurse Scientist Billings Clinic Conflicts of Interest Jeannine Brant has served on the
Cancer Related Pain: Case-Based Pharmacology Jeannine M. Brant, PhD, APRN, AOCN Oncology Clinical Nurse Specialist Nurse Scientist Billings Clinic Conflicts of Interest Jeannine Brant has served on the
GUIDELINES AND AUDIT IMPLEMENTATION NETWORK
 GUIDELINES AND AUDIT IMPLEMENTATION NETWORK General Palliative Care Guidelines The Management of Pain at the End Of Life November 2010 Aim To provide a user friendly, evidence based guide for the management
GUIDELINES AND AUDIT IMPLEMENTATION NETWORK General Palliative Care Guidelines The Management of Pain at the End Of Life November 2010 Aim To provide a user friendly, evidence based guide for the management
Opioid Induced Hyperalgesia (OIH)
 Opioid Induced Hyperalgesia (OIH) How to Receive Your CE Credits Read your selected course Completed the quiz at the end of the course with a 70% or greater. Complete the evaluation for your selected course.
Opioid Induced Hyperalgesia (OIH) How to Receive Your CE Credits Read your selected course Completed the quiz at the end of the course with a 70% or greater. Complete the evaluation for your selected course.
Multiple Choice Questions
 Multiple Choice Questions 25yo M presents without psychiatric or medical history, with complaint of tremor to the ER. He denies drinking alcohol but his friend at bedside takes you to the side and reports
Multiple Choice Questions 25yo M presents without psychiatric or medical history, with complaint of tremor to the ER. He denies drinking alcohol but his friend at bedside takes you to the side and reports
PERIOPERATIVE PAIN MANAGEMENT: WHAT S UP WITH METHADONE?
 PERIOPERATIVE PAIN MANAGEMENT: WHAT S UP WITH METHADONE? Sandra Z Perkowski, VMD, PhD, DACVAA University of Pennsylvania, School of Veterinary Medicine, Philadelphia, PA Pre-emptive and multimodal use
PERIOPERATIVE PAIN MANAGEMENT: WHAT S UP WITH METHADONE? Sandra Z Perkowski, VMD, PhD, DACVAA University of Pennsylvania, School of Veterinary Medicine, Philadelphia, PA Pre-emptive and multimodal use
Acute Pain Management in the Opioid Tolerant Patient. Objectives. Opioids. The participant will be able to define opioid tolerance
 Acute Pain Management in the Opioid Tolerant Patient Kathleen M. Colfer, MSN, RN-BC Clinical Nurse Specialist Acute Pain Management Service Department of Anesthesiology Thomas Jefferson University Hospital
Acute Pain Management in the Opioid Tolerant Patient Kathleen M. Colfer, MSN, RN-BC Clinical Nurse Specialist Acute Pain Management Service Department of Anesthesiology Thomas Jefferson University Hospital
MEDICAL POLICY SUBJECT: KETAMINE INFUSION THERAPY FOR THE TREATMENT OF CHRONIC PAIN SYNDROMES POLICY NUMBER: CATEGORY: Technology Assessment
 Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
Pre-op Interventions to Mitigate Post-op Acute and Chronic Pain
 Pre-op Interventions to Mitigate Post-op Acute and Chronic Pain H A R S H A S H A N T H A N N A. M D, M S C A S S O C I A T E P R O F E S S O R D E P A R T M E N T O F A N E S T H E S I A C H R O N I C
Pre-op Interventions to Mitigate Post-op Acute and Chronic Pain H A R S H A S H A N T H A N N A. M D, M S C A S S O C I A T E P R O F E S S O R D E P A R T M E N T O F A N E S T H E S I A C H R O N I C
NMDA-Receptor Antagonists and Opioid Receptor Interactions as Related to Analgesia and Tolerance
 Vol. 19 No. 1(Suppl.) January 2000 Journal of Pain and Symptom Management S7 Proceedings Supplement NDMA-Receptor Antagonists: Evolving Role in Analgesia NMDA-Receptor Antagonists and Opioid Receptor Interactions
Vol. 19 No. 1(Suppl.) January 2000 Journal of Pain and Symptom Management S7 Proceedings Supplement NDMA-Receptor Antagonists: Evolving Role in Analgesia NMDA-Receptor Antagonists and Opioid Receptor Interactions
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
General anesthesia. No single drug capable of achieving these effects both safely and effectively.
 General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General Anesthesia. Mohamed A. Yaseen
 General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
Choose a category. You will be given the answer. You must give the correct question. Click to begin.
 Instructions for using this template. Remember this is Jeopardy, so where I have written Answer this is the prompt the students will see, and where I have Question should be the student s response. To
Instructions for using this template. Remember this is Jeopardy, so where I have written Answer this is the prompt the students will see, and where I have Question should be the student s response. To
NMDA Receptor Antagonists. Tanyanun Ngam-ek-eu Samita Pirotesak Supervised by Assist.Prof. Nantthasorn Zinboonyahgoon
 NMDA Receptor Antagonists Tanyanun Ngam-ek-eu Samita Pirotesak Supervised by Assist.Prof. Nantthasorn Zinboonyahgoon NMDA Receptor N-metyl-D-aspartic-acid receptors Glutamate-gated cation channels with
NMDA Receptor Antagonists Tanyanun Ngam-ek-eu Samita Pirotesak Supervised by Assist.Prof. Nantthasorn Zinboonyahgoon NMDA Receptor N-metyl-D-aspartic-acid receptors Glutamate-gated cation channels with
Analgesic-Sedatives Drug Dose Onset
 Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
PART II: PREVENTING AND MANAGING COMPLICATIONS OF SICKLE CELL DISEASE
 PART II: PREVENTING AND MANAGING COMPLICATIONS OF SICKLE CELL DISEASE 1. PAIN Principles To educate patients, family and other caregivers about prevention, rapid identification and management of vaso-occlusive
PART II: PREVENTING AND MANAGING COMPLICATIONS OF SICKLE CELL DISEASE 1. PAIN Principles To educate patients, family and other caregivers about prevention, rapid identification and management of vaso-occlusive
Perioperative Pain Management
 Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Spinal Cord Injury Pain. Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018
 Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico
 Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico Balance is not that easy! Weaning Weaning is the liberation of a patient from
Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico Balance is not that easy! Weaning Weaning is the liberation of a patient from
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD
 Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
Chapter 19. Media Directory. Topical (Surface) Anesthesia. Spinal Anesthesia. Nerve-Block Anesthesia. Infiltration (Field-Block) Anesthesia
 Chapter 19 Drugs for Local and General Anesthesia Slide 18 Media Directory Lidocaine Animation Upper Saddle River, New Jersey 07458 All rights reserved. Topical (Surface) Anesthesia Creams, sprays, suppositories
Chapter 19 Drugs for Local and General Anesthesia Slide 18 Media Directory Lidocaine Animation Upper Saddle River, New Jersey 07458 All rights reserved. Topical (Surface) Anesthesia Creams, sprays, suppositories
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor
 Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
Results of a one-year, retrospective medication use evaluation. Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital
 Results of a one-year, retrospective medication use evaluation Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital Briefly review ketamine s history, mechanism of action, and unique properties
Results of a one-year, retrospective medication use evaluation Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital Briefly review ketamine s history, mechanism of action, and unique properties
Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143
 Sickle cell disease: managing acute painful episodes in hospital Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Sickle cell disease: managing acute painful episodes in hospital Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Overview of Essentials of Pain Management. Updated 11/2016
 0 Overview of Essentials of Pain Management Updated 11/2016 1 Overview of Essentials of Pain Management 1. Assess pain intensity on a 0 10 scale in which 0 = no pain at all and 10 = the worst pain imaginable.
0 Overview of Essentials of Pain Management Updated 11/2016 1 Overview of Essentials of Pain Management 1. Assess pain intensity on a 0 10 scale in which 0 = no pain at all and 10 = the worst pain imaginable.
The Fifth Vital Sign.
 Recognizing And Monitoring The Painful Patient Susan Clark, LVT, VTS(ECC) The Fifth Vital Sign. Pain control is part of the accepted standard of care in veterinary medicine. The ability to recognize the
Recognizing And Monitoring The Painful Patient Susan Clark, LVT, VTS(ECC) The Fifth Vital Sign. Pain control is part of the accepted standard of care in veterinary medicine. The ability to recognize the
Opioid Rotation. Dr Bruno Gagnon, M.D., M.Sc.
 Opioid Rotation Dr Bruno Gagnon, M.D., M.Sc. Associate Professor Department of Family Medicine and Emergency Medicine, Faculty of Medicine, Université Laval Consultant in Palliative Medicine CHU de Québec-Université
Opioid Rotation Dr Bruno Gagnon, M.D., M.Sc. Associate Professor Department of Family Medicine and Emergency Medicine, Faculty of Medicine, Université Laval Consultant in Palliative Medicine CHU de Québec-Université
Assay Sensitivity.
 Assay Sensitivity Michael C. Rowbotham, MD Professor of Neurology UCSF-Mount Zion Pain Management Center Senior Scientist and IRB Chair, CPMC Research Institute Michael.Rowbotham@ucsf.edu Outline What
Assay Sensitivity Michael C. Rowbotham, MD Professor of Neurology UCSF-Mount Zion Pain Management Center Senior Scientist and IRB Chair, CPMC Research Institute Michael.Rowbotham@ucsf.edu Outline What
Pain Pathways. Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH
 Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa
 CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.84 Subject: Policy: Purpose: Continuous Epidural Analgesia Acute or chronic pain relief provided to a patient
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.84 Subject: Policy: Purpose: Continuous Epidural Analgesia Acute or chronic pain relief provided to a patient
PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older)
 Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Seizure: the clinical manifestation of an abnormal and excessive excitation and synchronization of a population of cortical
 Are There Sharing Mechanisms of Epilepsy, Migraine and Neuropathic Pain? Chin-Wei Huang, MD, PhD Department of Neurology, NCKUH Basic mechanisms underlying seizures and epilepsy Seizure: the clinical manifestation
Are There Sharing Mechanisms of Epilepsy, Migraine and Neuropathic Pain? Chin-Wei Huang, MD, PhD Department of Neurology, NCKUH Basic mechanisms underlying seizures and epilepsy Seizure: the clinical manifestation
disease or in clients who consume alcohol on a regular basis. bilirubin
 NON-OPIOID Acetaminophen(Tylenol) Therapeutic class: Analgesic, antipyretic Aspirin (ASA, Acetylsalicylic Acid) Analgesic, NSAID, antipyretic Non-Opioid Analgesics COMMON USES WHAT I NEED TO KNOW AS A
NON-OPIOID Acetaminophen(Tylenol) Therapeutic class: Analgesic, antipyretic Aspirin (ASA, Acetylsalicylic Acid) Analgesic, NSAID, antipyretic Non-Opioid Analgesics COMMON USES WHAT I NEED TO KNOW AS A
Overview of Pain Types and Prevalence
 Pain Resource Nurse Overview of Pain Types and Prevalence Pain Resource Nurse Program Module 1 The Resource Center of the Alliance of State Pain Initiatives University of Wisconsin Board of Regents, 2011
Pain Resource Nurse Overview of Pain Types and Prevalence Pain Resource Nurse Program Module 1 The Resource Center of the Alliance of State Pain Initiatives University of Wisconsin Board of Regents, 2011
Analgesia for Patients with Substance Abuse Disorders. Lisa Jennings CN November 2015
 Analgesia for Patients with Substance Abuse Disorders Lisa Jennings CN November 2015 Definitions n Addiction: A pattern of drug use characterised by aberrant drug-taking behaviours & the compulsive use
Analgesia for Patients with Substance Abuse Disorders Lisa Jennings CN November 2015 Definitions n Addiction: A pattern of drug use characterised by aberrant drug-taking behaviours & the compulsive use
Sickle Cell Disease: How Should YOU Reassess Management & Treatment?
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/changing-conversation-sickle-cell-disease/sickle-cell-disease-howshould-you-reassess-management-treatment/10184/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/changing-conversation-sickle-cell-disease/sickle-cell-disease-howshould-you-reassess-management-treatment/10184/
Dr P.W.Buczkowski. Consultant in Anaesthesia & Pain Medicine. Royal Derby Hospital
 Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
SYLLABUS SPRING 2011 COURSE: NSC NEUROBIOLOGY OF PAIN
 SYLLABUS NSC 4358 NEUROBIOLOGY OF PAIN SPRING 2011 1 SYLLABUS SPRING 2011 COURSE: NSC 4358 001 NEUROBIOLOGY OF PAIN Instructor: Aage R. Møller PhD E-mail: AMOLLER@UTDALLAS.EDU Class schedule: Main Campus:
SYLLABUS NSC 4358 NEUROBIOLOGY OF PAIN SPRING 2011 1 SYLLABUS SPRING 2011 COURSE: NSC 4358 001 NEUROBIOLOGY OF PAIN Instructor: Aage R. Møller PhD E-mail: AMOLLER@UTDALLAS.EDU Class schedule: Main Campus:
Palliative Emergencies. Ken Stakiw
 Palliative Emergencies Ken Stakiw Disclosure None to disclose for this lecture Have received honoraria from a number of agencies and companies previously Intend to discuss some off label use of medications
Palliative Emergencies Ken Stakiw Disclosure None to disclose for this lecture Have received honoraria from a number of agencies and companies previously Intend to discuss some off label use of medications
Analgesia for Small Animals Pharmacology & Clinical Practice. Jill Maddison The Royal Veterinary College Hawkshead Lane, North Mymms, AL9 7TA, UK
 Analgesia for Small Animals Pharmacology & Clinical Practice Jill Maddison The Royal Veterinary College Hawkshead Lane, North Mymms, AL9 7TA, UK Colin Dunlop Advanced Anaesthesia Specialists Unit 13, 46-48
Analgesia for Small Animals Pharmacology & Clinical Practice Jill Maddison The Royal Veterinary College Hawkshead Lane, North Mymms, AL9 7TA, UK Colin Dunlop Advanced Anaesthesia Specialists Unit 13, 46-48
POST-OP MULTIMODAL PAIN MANAGEMENT. Maripat Welz-Bosna Reading Hospital Medical Center Department of Medicine Hospitalist Services/Pain Management
 POST-OP MULTIMODAL PAIN MANAGEMENT Maripat Welz-Bosna Reading Hospital Medical Center Department of Medicine Hospitalist Services/Pain Management Objectives Understand the basic neurobiology of the pain
POST-OP MULTIMODAL PAIN MANAGEMENT Maripat Welz-Bosna Reading Hospital Medical Center Department of Medicine Hospitalist Services/Pain Management Objectives Understand the basic neurobiology of the pain
MEDICAL POLICY. SUBJECT: KETAMINE INFUSION THERAPY FOR THE TREATMENT OF CHRONIC PAIN SYNDROMES POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
FDA hormone replacement therapy Web site 6
 TABLE OF CONTENTS Caring for pain at UIMCC 1-5 FDA hormone replacement therapy Web site 6 P&T Committee Formulary Action - September 2003 6 Caring for pain at UIMCC The International Association for the
TABLE OF CONTENTS Caring for pain at UIMCC 1-5 FDA hormone replacement therapy Web site 6 P&T Committee Formulary Action - September 2003 6 Caring for pain at UIMCC The International Association for the
Pain Management in Hospice and Palliative Care
 Pain Management in Hospice and Palliative Care A Case-based Approach JoAnne Nowak, M.D. Merrimack Valley Hospice Revised November 2011 Objectives Use a case study approach to stimulate discussion and illustrate
Pain Management in Hospice and Palliative Care A Case-based Approach JoAnne Nowak, M.D. Merrimack Valley Hospice Revised November 2011 Objectives Use a case study approach to stimulate discussion and illustrate
INTRAVENOUS LIDOCAINE INFUSIONS AND INTRALIPID RESCUE
 INTRAVENOUS LIDOCAINE INFUSIONS AND INTRALIPID RESCUE Acute Pain Service-LHSC VH and UH sites HISTORY Lidocaine and procaine used by IV infusion in the 1950s and 1960s for general analgesia Often continued
INTRAVENOUS LIDOCAINE INFUSIONS AND INTRALIPID RESCUE Acute Pain Service-LHSC VH and UH sites HISTORY Lidocaine and procaine used by IV infusion in the 1950s and 1960s for general analgesia Often continued
Pharmacology of Pain Transmission and Modulation
 Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Long Term Care Formulary HCD - 08
 1 of 5 PREAMBLE Opioids are an important component of the pharmaceutical armamentarium for management of chronic pain. The superiority of analgesic effect of one narcotic over another is not generally
1 of 5 PREAMBLE Opioids are an important component of the pharmaceutical armamentarium for management of chronic pain. The superiority of analgesic effect of one narcotic over another is not generally
Opioid Free Anesthesia
 Opioid Free Anesthesia Michael H Wilhelm, CRNA, APRN Opioid Free Anesthesia Michael H Wilhelm, CRNA, APRN 1 Why is pain important? Primary contributor to post-operative distress 56% of patients state that
Opioid Free Anesthesia Michael H Wilhelm, CRNA, APRN Opioid Free Anesthesia Michael H Wilhelm, CRNA, APRN 1 Why is pain important? Primary contributor to post-operative distress 56% of patients state that
SCOPING DOCUMENT FOR WHO Treatment Guidelines on pain related to cancer, HIV and other progressive life-threatening illnesses in adults
 SCOPING DOCUMENT FOR WHO Treatment Guidelines on pain related to cancer, HIV and other progressive life-threatening illnesses in adults BACKGROUND The justification for developing these guidelines lies
SCOPING DOCUMENT FOR WHO Treatment Guidelines on pain related to cancer, HIV and other progressive life-threatening illnesses in adults BACKGROUND The justification for developing these guidelines lies
Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe )
 PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
Analgesia is a labeled indication for all of the approved drugs I will be discussing.
 Comparative Opioid Pharmacology Disclosure Analgesia is a labeled indication for all of the approved drugs I will be discussing. I ve consulted with Glaxo (remifentanil), Abbott (remifentanil), Janssen
Comparative Opioid Pharmacology Disclosure Analgesia is a labeled indication for all of the approved drugs I will be discussing. I ve consulted with Glaxo (remifentanil), Abbott (remifentanil), Janssen
4/3/2018. Management of Acute Pain Crises. Five Mistakes I ve made and why you shouldn t
 Management of Acute Pain Crises Maggie O Connor, M.D. Retired Palliative Care Physician Hope is not the conviction that something will turn out well, but the certainty that something makes sense, regardless
Management of Acute Pain Crises Maggie O Connor, M.D. Retired Palliative Care Physician Hope is not the conviction that something will turn out well, but the certainty that something makes sense, regardless
Chapter 25. General Anesthetics
 Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Balanced Analgesia With NSAIDS and Coxibs. Raymond S. Sinatra MD, Ph.D
 Balanced Analgesia With NSAIDS and Coxibs Raymond S. Sinatra MD, Ph.D Prostaglandins and Pain The primary noxious mediator released from damaged tissue is prostaglandin (PG) PG is responsible for nociceptor
Balanced Analgesia With NSAIDS and Coxibs Raymond S. Sinatra MD, Ph.D Prostaglandins and Pain The primary noxious mediator released from damaged tissue is prostaglandin (PG) PG is responsible for nociceptor
2018 Learning Outcomes
 I. Pain Physiology and Anatomy (20%) A. Describe the basic anatomy of the nervous system. B. Describe the physiological mechanisms of neuronal function (eg- action potentials). C. Review the nociceptive
I. Pain Physiology and Anatomy (20%) A. Describe the basic anatomy of the nervous system. B. Describe the physiological mechanisms of neuronal function (eg- action potentials). C. Review the nociceptive
PAIN. Physiology of pain relating to pain management
 PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
UCSF: 150 years in the making
 Securing Hospital Approval for Ketamine use on the Wards: Challenges, Outcomes and Lessons Learned Acknowledgements Mark Schumacher Ph.D.,M.D. Professor and Chief, Division of Pain Medicine Dept. of Anesthesia
Securing Hospital Approval for Ketamine use on the Wards: Challenges, Outcomes and Lessons Learned Acknowledgements Mark Schumacher Ph.D.,M.D. Professor and Chief, Division of Pain Medicine Dept. of Anesthesia
Question 1. a) Aspiration and irrigation of the corpus cavernosum. b) Instillation of phenylephrine into the corpus cavernosum. c) IVF and morphine
 Question 1 A 16yo HbSS male, with a history of two prior episodes of priapism presents to the Emergency Department with a painful erection which started less than 2hours ago. What is the next best step
Question 1 A 16yo HbSS male, with a history of two prior episodes of priapism presents to the Emergency Department with a painful erection which started less than 2hours ago. What is the next best step
Neurobiology of Pain Adjuvant analgesia
 Neurobiology of Pain Adjuvant analgesia Jason Brooks Consultant Anaesthesia and Pain Management BCH March 2017 The Brief A broad overview of the abnormal and normal anatomy and physiology of pain pathways
Neurobiology of Pain Adjuvant analgesia Jason Brooks Consultant Anaesthesia and Pain Management BCH March 2017 The Brief A broad overview of the abnormal and normal anatomy and physiology of pain pathways
Lumbar Fusion. Reference Guide for PACU CLINICAL PATHWAY. All patient variances to the pathway are to be circled and addressed in the progress notes.
 Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Ketamine Nursing Self Learning Package
 Ketamine Nursing Self Learning Package Developed by Waterloo Wellington Ketamine Education Committee Reviewed by Dr. A. Moolman, Palliative Care Physician, MBChB, CCFP, LMCC, 6/4/2010 1 SECTION ONE Table
Ketamine Nursing Self Learning Package Developed by Waterloo Wellington Ketamine Education Committee Reviewed by Dr. A. Moolman, Palliative Care Physician, MBChB, CCFP, LMCC, 6/4/2010 1 SECTION ONE Table
Responding to The Joint Commission Alert on Safe Use of Opioids in Hospitals
 Responding to The Joint Commission Alert on Safe Use of Opioids in Hospitals Suzanne A Nesbit, PharmD, CPE Clinical Pharmacy Specialist, Pain Management The Johns Hopkins Hospital Objectives and Disclosures
Responding to The Joint Commission Alert on Safe Use of Opioids in Hospitals Suzanne A Nesbit, PharmD, CPE Clinical Pharmacy Specialist, Pain Management The Johns Hopkins Hospital Objectives and Disclosures
STARSHIP WITHDRAWAL OF ANALGESIA AND SEDATION
 STARSHIP WITHDRAWAL OF ANALGESIA AND SEDATION Patients receiving analgesia and/or sedation for longer than 5-7 days may suffer withdrawal if these drugs are suddenly stopped. To prevent this happening
STARSHIP WITHDRAWAL OF ANALGESIA AND SEDATION Patients receiving analgesia and/or sedation for longer than 5-7 days may suffer withdrawal if these drugs are suddenly stopped. To prevent this happening
OPIOID- INDUCED NEUROTOXICITY*
 OPIOID- INDUCED NEUROTOXICITY* Sriram Yennu MD, MS, FAAHPM Palliative Care, Rehabilitation and Integrative Medicine U.T. M.D. Anderson Cancer Center *Slide Deck courtesy Dept PRIM MDACC PATIENT #1: MRS
OPIOID- INDUCED NEUROTOXICITY* Sriram Yennu MD, MS, FAAHPM Palliative Care, Rehabilitation and Integrative Medicine U.T. M.D. Anderson Cancer Center *Slide Deck courtesy Dept PRIM MDACC PATIENT #1: MRS
Nociceptive Pain. Pathophysiologic Pain. Types of Pain. At Presentation. At Presentation. Nonpharmacologic Therapy. Modulation
 Learning Objectives Effective, Safe Analgesia An Approach to Appropriate Outpatient Chronic Pain Treatment By the end of this presentation, participants will be able to: Identify multiple factors that
Learning Objectives Effective, Safe Analgesia An Approach to Appropriate Outpatient Chronic Pain Treatment By the end of this presentation, participants will be able to: Identify multiple factors that
DRUGS THAT ACT IN THE CNS
 DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
Acute Postoperative Pain. David Radvinsky, MD March 24, 2016
 Acute Postoperative Pain David Radvinsky, MD March 24, 2016 Objectives 1. Discuss the multimodal approach to pain management and discuss the various classes of drugs based on receptor mechanism. 2. Give
Acute Postoperative Pain David Radvinsky, MD March 24, 2016 Objectives 1. Discuss the multimodal approach to pain management and discuss the various classes of drugs based on receptor mechanism. 2. Give
HIGH DOSE OPIOID THERAPY: ARE WE STILL TREATING PAIN?
 HIGH DOSE OPIOID THERAPY: ARE WE STILL TREATING PAIN? Sebastiano Mercadante, MD Director of Anesthesia and Intensive Care Unit & Pain Relief and Palliative Care Unit La Maddalena Cancer Center Professor
HIGH DOSE OPIOID THERAPY: ARE WE STILL TREATING PAIN? Sebastiano Mercadante, MD Director of Anesthesia and Intensive Care Unit & Pain Relief and Palliative Care Unit La Maddalena Cancer Center Professor
The Management of Pain in Children (and Adults)
 The Management of Pain in Children (and Adults) Myron Yaster, MD Richard J Traystman Professor, Departments of Anesthesiology, Critical Care Medicine, and Pediatrics The Johns Hopkins Medical Institutions
The Management of Pain in Children (and Adults) Myron Yaster, MD Richard J Traystman Professor, Departments of Anesthesiology, Critical Care Medicine, and Pediatrics The Johns Hopkins Medical Institutions
Objectives: What is your Definition of Pain? 8/16/2017
 Safe Opioid Management for the Seriously Ill Patient Sam Perna, D.O. Objectives: MDB1 1) Participants will understand the way the body s pain system works. 2) Participants will identify the elements of
Safe Opioid Management for the Seriously Ill Patient Sam Perna, D.O. Objectives: MDB1 1) Participants will understand the way the body s pain system works. 2) Participants will identify the elements of
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
