A Novel Classification and Minimally Invasive Treatment of Degenerative Lumbar Spinal Stenosis
|
|
|
- David Skinner
- 5 years ago
- Views:
Transcription
1 DOI: / JTN Received: / Accepted: Original Investigation A Novel Classification and Minimally Invasive Treatment of Degenerative Lumbar Spinal Stenosis Guangfei Gu, Hailong Zhang, Shisheng He, Qingsong Fu, Xiaobing CaI, Xu Zhou, Xiaolong Shen, Xin Gu Shanghai Tenth People s Hospital, Tongji University School of Medicine, Department of Orthopedics, Shanghai, China ABSTRACT AIm: We conducted a novel classification system of degenerative lumbar spinal stenosis (DLSS) based on clinical manifestations and imaging (computed tomography and magnetic resonance imaging) features. We chose different minimally invasive surgical procedures according to our system. Clinical parameters and radiological findings will be assessed in the article. MaterIal and Methods: A retrospective study was conducted on 96 patients undergoing minimally invasive surgery for DLSS. We chose different surgical procedures according to our novel classification system based on clinical manifestations, imaging features, and concurrence with other spinal diseases. Clinical parameters and radiological findings were assessed pre- and postoperatively. Results: The mean follow up period was 24 months (range, 15~36 months). There was a statistically significant improvement in the Visual Analogue Scale (VAS) score of low back pain and leg pain after surgery (p<0.05). According to the Japanese Orthopaedic Association (JOA) scores, the operation efficacy was excellent in 57 cases, good in 36 cases, and fair in 3 cases. According to Bridwell s criterion, the fusion rate was 96% (48/50) in patients who underwent fusion surgery. There were no cages or pedicle screws related complications. ConclusIon: Minimally invasive surgical treatment of DLSS has satisfactory outcomes according to the novel classification, but further long-term, prospective, randomized controlled studies involving a larger study group are needed to validate the long-term efficacy. Keywords: Decompression, Degenerative lumbar spinal stenosis, Minimally invasive surgery, Transforaminal lumbar interbody fusion Introduction Spinal stenosis is a narrowing of the spinal canal with encroachment on the neural structures by surrounding bone and soft tissue (9). Patients with spinal stenosis typically present with intermittent neurogenic claudication, or a combination of lower extremity pain, tension and weakness that occurs with walking or standing but is relieved with sitting down or lumbar flexion. The pathoanatomy of degenerative lumbar spinal stenosis (DLSS) is very complicated, including bulging discs, zygapophyseal joint hypertrophy, buckling or hypertrophy of the ligaments, and spondylolisthesis as a result of the degenerative cascade (3). To our knowledge, how to do the individualized surgery for lumbar stenosis is still controversial. In this article, we conducted a novel classification system of DLSS based on clinical manifestations and imaging (Computed Tomography (CT) and Magnetic Resonance Imaging (MRI)) features. We chose different minimally invasive surgical procedures according to our system. Clinical parameters and radiological findings will be assessed in the article. qr code Corresponding author: Shisheng He guguangfei@aliyun.com Turk Neurosurg 1
2 Material and Methods The Novel Classification System We used a novel classification system of DLSS based on clinical manifestations, and imaging (CT and MRI) features. According to the clinical manifestations, DLSS is divided into 3 types. Type I: intermittent claudication without leg pain. Type II: intermittent claudication with asymmetric radicular pain. Type III: intermittent claudication with bilateral radicular pain. According to the imaging (CT and MRI) features, DLSS is also divided into 3 types (Figure 1A-E). Type A: unilateral spinal stenosis (including lateral recess and nerve root canal) with or without central spinal stenosis. Type B: bilateral spinal stenosis (including lateral recess and nerve root canal) with or without central spinal stenosis. Type C: the other status, including lumbar spinal stenosis caused by calcification of huge lumbar disc herniation, severe DLSS and multiple-level ( 3) DLSS. Inclusion Criteria 1) The clinical indications were leg pain and/or leg numbness inducing intermittent claudication rather than back pain, 2) Preoperative imaging examines including radiographs (anteroposterior, lateral and flexion-extension views), CT and MRI showed consistency with the clinical manifestations, 3) No obvious improvement after 6-month conservative treatment before consideration for surgical intervention. Exclusion Criteria 1) The patients have associated dynamic segmental instability (Meyerding grade more than grade II) and (or) degenerative scoliosis (Cobb 30 ) (14), 2) Lumbar spinal stenosis caused by calcification of huge lumbar disc herniation, severe DLSS and multiple-level ( 3) DLSS, 3) Patients who had previous back disease involving trauma, infection or pathologic causes, 4) Patients who cannot tolerate the surgery. A total of 96 patients, 42 males and 54 females, presented with DLSS from March 2009 to December The ages ranged from 41 to 81 years (mean 62.6 years). The disease duration was months (mean 47.1 months). According to the aforementioned classification criteria, all patients were classified as follows: clinical classification: type I 32 cases, type II 38 cases, type III 26 cases; imaging classification: type A 36 cases, type B, 60 cases, type C 0 cases; 32 patients had concurrent lumbar instability, 8 cases were associated with scoliosis (Cobb< 30 ) (3) and 12 cases were simultaneously associated with instability and scoliosis (Table I). We chose different surgical procedures according to our classification A B C D E Figure 1: The patients were divided into 3 groups (type A, B, C) according to the imaging manifestation of lumbar spinal stenosis; A) Type A, unilateral lateral lumbar spinal stenosis; B) Type B, bilateral lateral lumbar spinal stenosis; D) Type C, severe lumbar spinal stenosis; C) Type C, lumbar spinal stenosis caused by calcification of huge disc herniation; E) Type C, multiple-level lumbar spinal stenosis ( 3). 2 Turk Neurosurg
3 system (Figure 2) and all the procedures were performed by the same surgeon group. Ethical approval for this study was obtained from the Research Ethics Committee, Shanghai Tenth People s Hospital, Tongji University School of Medicine, with number 2012-RES-042. Surgical techniques were as follows: a) Unilateral approach for bilateral decompression through an expandable tubular retractor. Under general anaesthesia, the patient was evenly placed in a prone position on a radiolucent operating table. The incision was marked by connecting a line between the outer portions of the superior and inferior pedicles (approximately 2.5 cm off midline) with help of a special localizer (Figure 3A-D) designed by the authors. A 3 cm longitudinal incision was made on the symptomatic side or the severe stenosis side according to images. After the skin and thoracolumbar fascia were dissected, the soft tissue was gradually separated by the retractor. Adequate decompression was achieved by cutting the inferior portion of the lamina, hypertrophied superior and inferior articular processes, and ligamenta flava (12). After one side of approach had been completely decompressed, the operating table or the expandable tubular retractor was tilted about 15 to observe the contralateral side. The basal part of the spinous process of the caudal half of the cranial lamina and a small cranial portion of the caudal lamina were removed with a rongeur. Then, the contralateral lamina was carefully removed with a rongeur leaving the ligamentum flavum in place as protection for the dural sac and the nerve root. Following sufficient resection of the bony segment, the ligamentum flavum was removed en bloc with a curette, while protecting the dural sac and contralateral nerve root with a patty. We confirmed adequate decompression of the contralateral side with recognition of the inner aspect of the pedicle on the contralateral side (15). All procedures were accomplished under direct visualization without microscope or microendoscope. b) Bilateral decompression via bilateral approach through an expandable tubular retractor The decompression would be performed on the contralateral side after approach side had been finished. The details were the same as above mentioned. c) Transforaminal lumbar interbody fusion (TLIF) and percutaneous pedicle screw fixation (PPSF) after decompression. After decompression, transforaminal lumbar interbody fusion and percutaneous pedicle screw fixation were performed through an expandable tubular retractor. Before cage insertion, the vertebral endplates were carefully prepared with disc space reamers and shavers. Sufficient autologous bone graft obtained from the resected lamina and facet was packed in the anterior disc space. A single PEEK cage (Capstone Medtronic Sofamor Danek, Memphis, TN, USA) filled with autologous bone was inserted obliquely across the disc space. No additional contralateral facet fusion was performed in the patients. Percutaneous pedicle screws and a rod were placed on the contralateral side to distract the disc space and then the screw-rod connections in the distracted position were provisionally tightened (10). Percutaneous pedicle screws were mounted through the Sextant system (Medtronic Sofamor Danek, Memphis, TN, USA) with the aid of a G-arm fluoroscope. The number of patients for each surgical procedure is listed in Table I. Clinical and Radiological Evaluation The operation time, intra-operative blood loss and complications were recorded. Radiographs (anteroposterior and lateral images) were taken 3 days after surgery to confirm the position of instruments. A CT scan was obtained from patients undergoing decompression without fixation 3 days after surgery. Out-patient follow-ups (clinical and radiological evaluation) were on the 3rd, 6th, and 12th month after surgery. Phone call follow-ups (clinical evaluation) were made every half year, 12 Table I: Demographic Data and Clinical Characteristics Demographic data Patients included 96 Age, mean years (range) 63.4yrs (range, 41~81yrs) Duration of symptoms (months) 47.1 m Clinical variables No. patients Gender Male 42 Female 54 Type according to the clinical manifestations Type I 32 Type II 38 Type III 26 Type according to the imagings Type A 36 Type B 60 Type C 0 Concurrent with other spinal diseases Lumbar instability 32 Scoliosis 8 Instability and scoliosis 12 Surgical procedures Single segment 52 Procedure a 38 Procedure b 14 Procedure c 28 Double segments 44 Procedure a+ Procedure a 28 Procedure a+ Procedure b 12 Procedure b+ Procedure b 4 Procedure c 22 Turk Neurosurg 3
4 Figure 2: Surgical procedures for degenerative lumbar spinal stenosis according to the novel typing system. A B C D Figure 3: A) The spinal localizer consists of 19 horizontal crossbars and 4 longitudinal rods. There is about 1 cm between each crossbar and some different marks are made on the crossbars. Two longitudinal rods can also be distinguished with different marks. B) The locator is placed on the patient s back with the center in the midline over the approximate spinal levels of interest preoperatively. C) A represents the pedicles of L4 and L5, B is the intervertebral space of L4-5, C is the superior articular process of S1. D) The incision was marked by connecting a line between the outer portions of the superior and inferior pedicles. 4 Turk Neurosurg
5 months after surgery. Visual Analogue Scale/Score (VAS) for low back pain and leg pain was recorded before surgery, at the 6th month after surgery and at the last follow-up respectively. The Oswestry disability index (ODI) was used to assess how the patient s leg (or back) trouble had affected the ability to manage in daily life. The clinical improvement rate was assessed by the Japanese Orthopaedic Association (JOA) score with a maximum possible score of 29 points pre- and postoperatively. [The JOA improvement rate was calculated as (post-operative JOA scores- preoperative JOA scores) / (29- preoperative JOA scores) 100%. Operation efficacy was then determined by the clinical improvement rate as excellent 75%, 50% good<75%, 25% fair<50%, and poor<25% or postoperative JOA scores lower than preoperative scores. On the 3rd, 6th, 12th months after surgery, radiographs (anteroposterior and lateral images) were obtained to evaluate the fusion status. A CT scan with two-dimensional reconstruction was performed when it was difficult to confirm the fusion status by radiographs. 2 independent, experienced spine surgeons, who were not part of the surgical team, performed the radiographic assessment of fusion. The fusion status was assessed according to Bridwell s posterior fusion grades using plain radiographs (2, 4), namely, grade I: solid trabeculated transverse process and facet fusions bilaterally, grade II: thick fusion mass on one side, difficult to visualize on the other side, grade III: suspected lucency or defect in the fusion mass, grade IV: definite resorption of graft with fatigue of instrumentation. The fusion was defined as grade I or grade II. Statistical Assessments The software of SPSS 17.0 (SPSS, USA) was used to statistical analysis. Quantifiable data were expressed as x? s. Student s t test was used for the comparison of continuous variables. P values below 0.05 were accepted for significance. Results The operation time and intra-operative blood loss are illustrated in Table II. In 1 patient who also had severe osteoporosis, the interbody cage sunk into the upper vertebral body. The cage was removed and the interbody space was then fused with autologous bone graft. Dural tear occurred in 1 patient. The overlying fascia was closed tightly without additional exposure and repair in this patient. Postoperatively, the patients remained strictly supine in bed and cerebrospinal fluid leakage lasted 4 days without any neurological sequelae or wound complication. Delayed healing of the incision was found in 3 cases, which was considered to be a result of excessive traction during the operation. The wound healed 15~18 days after surgery with antibiotics and dressing change. The mean follow-up was 24 months with a range of 15~36 months. The VAS score of low back pain before surgery was (6.6±1.0), and (2.8±0.7) and (2.6±0.7) at six months after surgery and the last follow-up respectively. The VAS score of leg pain before surgery was (7.8±1.0), and were (2.3±0.7) and (2.0±0.7) at six months and the last follow-up respectively. ODI (%) were (67.7±6.5), (19.0±2.7) and (16.8±1.7) before surgery, at six months after surgery, and the last follow-up respectively. VAS score and ODI showed statistically significant improvements after surgery (P<0.05). JOA scores before surgery and the last follow-up after surgery were (7.9±1.7) and (24.3±1.7) respectively. According to the JOA scores, the operation efficacy was excellent in 57 cases, good in 36 cases, and fair in 3 cases. 50 patients who also had lumbar instability underwent transforaminal lumbar interbody fusion and percutaneous pedicle screw fixation after decompression (Figure 4A-O). Postoperative radiographs showed one pair of screws was overlong and penetrating the front cortical bone of the vertebra in 1 patient (Figure 5A,B), and no additional symptoms (such as abdominal pain) were observed during the follow-up period in this patient. According to the Bridwell s criterion, there were 36 grade I cases (72%), 12 grade II cases(24%), and 2 grade III cases (4%). The patients of grade III are still in follow up. Discussion Spinal stenosis is a narrowing of the spinal canal by a combination of bone and soft tissues, which causes mechanical compression of spinal nerve roots. The compression of these nerve roots can be asymptomatic, but it can also become symptomatic, resulting in weakness, reflex alterations, gait disturbances, bowel or bladder dysfunction, motor and sensory changes, radicular pain or atypical leg pain, and neurogenic claudication (1, 13). DLSS typically starts with a normal canal and changes such as bulging discs, zygapophyseal joint hypertrophy, buckling or hypertrophy of Table II: Operation Time (min) and Intra-Operative Blood Loss (ml) of the Procedures Procedure a (n=38) Single segment (n=52) Procedure b (n=14) Procedure c (n=28) Procedure a + Procedure a (n=28) Double segments (n=44) Procedure a + Procedure b (n=12) Procedure b + Procedure b (n=4) Procedure c (n=22) Operation time (min) 55.4± ± ± ± ± ± ±24.5 Intra-operative blood loss (ml) 88.0± ± ± ± ± ± ±74.1 Note: Procedure a: Unilateral approach for bilateral decompression; procedure b: Bilateral approach for bilateral decompression; procedure c: Transforaminal lumbar interbody fusion (TLIF) and percutaneous pedicle screw fixation (PPSF) after decompression. Turk Neurosurg 5
6 A B C D E F G H I J K L M N O Figure 4: A 62-year-old man was admitted to our hospital for low back pain and intermittent claudication for almost 2 years. According to our classification system, he was classified as type II for clinical manifestations and type B for imaging features. The patient also had lumbar instability. We chose the unilateral approach for bilateral decompression, transforaminal lumbar interbody fusion and percutaneous pedicle screw fixation. A, B, C, D, E, F, G) The preoperative image data (X-ray, CT and MRI) showed lumbar stenosis combined with instability in L4/5 level. H, I) AP and lateral radiographs showing the internal fixation and cage on the third day after surgery; J, K) Three months after surgery; L, M) CT scan showing a solid fusion and satisfactory decompression six months after surgery; N, O) AP and lateral radiographs showing a solid fusion 12 months after surgery. A B Figure 5: Postoperative X ray and CT showed one pair of screws was overlong and penetrating the front cortical bone of the vertebra in 1 patient in group A. 6 Turk Neurosurg
7 the ligaments, and spondylolisthesis develop as a result of the degenerative cascade. DLSS can anatomically involve the central canal, lateral recess, foramina or any combination of these locations. Central canal stenosis may result from a decrease in the anteroposterior, transversal or combined diameter secondary to loss of disc height with or without ligamentum flavum buckling or hypertrophy, disc protrusion, hypertrophic zygapophyseal joints, and degenerative spondylolisthesis (5). The same processes, including decreased disc height, facet joint hypertrophy (with or without spondylolisthesis) and/or vertebral endplate osteophytosis, can also result in lateral recess stenosis. Foraminal stenosis can be either antero-posterior resulting from a combination of disc-space narrowing and overgrowth of structures anterior to the facet joint capsule, and/or vertical resulting from posterolateral osteophytes from the vertebral endplates protruding into the foramen along with a laterally bulging annulus fibrosis or herniated disc that compresses the nerve root against the superior pedicle (7). The pathoanatomy of spinal stenosis is very complicated, and how to choose minimally invasive surgical procedures for lumbar spinal stenosis is still controversial. Our suggestions (Figure 5) are as follows: unilateral approach for bilateral decompression applies to patients with a clinical manifestations classification of type I or type II and associated with an images classification of type A or most of type B. However, in certain cases with an images classification of type B, the contralateral decompression should be performed if unilateral approach for contralateral decompression was difficult or insufficient. For patients with clinical manifestations classification of type I or type III and images classification of type B, a bilateral approach for bilateral decompression was necessary. For patients with images classification of type C, open surgery could be a safe and optimal option. For those patients who also had lumbar instability (6), transforaminal lumbar interbody fusion and percutaneous pedicle screw fixation should be performed after decompression. Patients with combined scoliosis should be treated as degenerative scoliosis if the Cobb angle is 30. If the Cobb angle is <30 without symptoms of instability, the patients could be treated as simple DLSS but it should be noted that articular facets on the concave side should be carefully preserved. In some cases, internal fixation and short level fusion were needed to prevent aggravation of scoliosis and instability. We performed contralateral decompression after adequate decompression approach side had been achieved. The operating table or the expandable tubular retractor was tilted about 15 to observe the contralateral side. The root of spinous process was partly excised to visualize the contralateral structures. In order to protect the dural sac and nerve root, we first decompressed to the contralateral pedicle beyond the surface of ligamentum flavum. The bilateral approach for bilateral decompression should be performed if the unilateral approach for contralateral decompression was difficult or insufficient. For patients combined with preoperative lumbar instability or intraoperative iatrogenic instability during operation, minimally invasive transforaminal lumbar interbody fusion (MIS- TLIF) should be performed. Currently, numerous studies (8, 11) have reported that MIS-TLIF was similar to open TLIF in respect of long-term clinical outcomes and fusion rates. However, MIS- TLIF has the additional benefits of less postoperative pain, early rehabilitation, shorter hospitalization, and fewer complications. Study by Shunwu et al. (12) showed that serum creatine kinase was significantly lower in the MIS- TLIF group than in the open group on the third postoperative day and the average postoperative ODI and VAS scores were significantly reduced in both groups. However, the scores in the minimally invasive group improved more compared with the open group. In our study, VAS scores and ODI after surgery were both significantly improved as well. According to the JOA scores, the operation efficacy was excellent in 57 cases, good in 36 cases, fair in 3 cases. According to the Bridwell s criterion, the fusion rate was 96% (48/50) in patients who underwent fusion surgery. There were no complications related to the cages or pedicle screws. There were a few limitations of this study. First, the number of cases included in this study was relatively low. Second, this was a retrospective study without any control group, and the potential interference factors such as the surgeon s habits, the operation conditions and so on could not be excluded. Third, postoperative CT scans were not performed in all patients, and deviations may have existed when assessing the fusion status. Further studies are needed to make clear that minimally invasive surgery for DLSS associated with severe instability, with degenerative scoliosis (Cobb 30 ), lumbar spinal stenosis caused by calcification of huge lumbar disc herniation, and multiple-level ( 3) DLSS is beneficial. Conclusion Minimally invasive surgical treatment of DLSS has satisfactory outcomes according to the novel classification, but further long-term, prospective, randomized controlled studies involving a larger study group are needed to validate the long-term efficacy. Acknowledgement We thank Xia Zhang, a nurse in our hospital, for her excellent daily work in our surgery. References 1. Botwin KP, Gruber RD: Lumbar spinal stenosis: Anatomy and pathogenesis. Phys Med Rehabil Clin N Am 14:1-15, Bridwell KH, Lenke LG, McEnery KW, Baldus C, Blanke K: Anterior fresh frozen structural allografts in the thoracic and lumbar spine. Do they work if combined with posterior fusion and instrumentation in adult patients with kyphosis or anterior column defects? Spine 20: , Costa F, Sassi M, Cardia A, et al: Degenerative lumbar spinal stenosis: Analysis of results in a series of 374 patients treated with unilateral laminotomy for bilateral microdecompression. Journal of Neurosurgery Spine 7: , Eck KR, Lenke LG, Bridwell KH, Gilula LA, Lashgari CJ, Riew KD: Radiographic assessment of anterior titanium mesh cages. J Spinal Disord 13(6): , 2000 Turk Neurosurg 7
8 5. Genevay S, Atlas SJ: Lumbar spinal stenosis. Best Pract Res Clin Rheumatol 24(2): , Hanley EN Jr: The indications for lumbar spinal fusion with and without instrumentation. Spine 20:143S-153S, Jenis LG, An HS: Spine update. Lumbar foraminal stenosis. Spine 25(3): , Lau D, Lee JG, Han SJ, Lu DC, Chou D: Complications and perioperative factors associated with learning the technique of minimally invasive transforaminal lumbar interbody fusion (TLIF). J Clin Neurosci 18: , Manchikanti L, Cash KA, McManus CD, Pampati V, Abdi S: Preliminary results of a randomized, equivalence trial of fluoroscopic caudal epidural injections in managing chronic low back pain: Part 4--Spinal stenosis. Pain Physician 11: , Park Y, Ha JW, Lee YT, Oh HC, Yoo JH, Kim HB: Surgical outcomes of minimally invasive transforaminal lumbar interbody fusion for the treatment of spondylolisthesis and degenerative segmental instability. Asian Spine J 5(4): , Peng CW, Yue WM, Poh SY, Yeo W, Tan SB: Clinical and radiological outcomes of minimally invasive versus open transforaminal lumbar interbody fusion. Spine 34: , Shunwu F, Xing Z, Fengdong Z, Xiangqian F: Minimally invasive transforaminal lumbar interbody fusion for the treatment of degenerative lumbar diseases. Spine (Phila Pa 1976) 35(17): , Simotas AC, Dorey FJ, Hansraj KK, Cammisa F Jr: Nonoperative treatment for lumbar spinal stenosis. Clinical and outcome results and a 3-year survivorship analysis. Spine (Phila Pa 1976) 25: , Tribus CB: Degenerative lumbar scoliosis: Evaluation and management. J Am Acad Orthop Surg 11: , Yang SM, Park HK, Chang JC, Kim RS, Park SQ, Cho SJ: Minimum 3-year outcomes in patients with lumbar spinal stenosis after bilateral microdecompression by unilateral or bilateral laminotomy. J Korean Neurosurg Soc 54(3): , Turk Neurosurg
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
JCSC INTRODUCTION. Rudolf Morgenstern, MD, PhD
 Diagnosis The lumbar lateral X-ray images in forward flexion and extension showed an anterior displacement of 10 mm in extension and of 6 mm in flexion measured with the methonline ML Comm JCSC DEGENERATIVE
Diagnosis The lumbar lateral X-ray images in forward flexion and extension showed an anterior displacement of 10 mm in extension and of 6 mm in flexion measured with the methonline ML Comm JCSC DEGENERATIVE
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse of a Lumbar Spine Vertebral Body
 Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Original Article Clinics in Orthopedic Surgery 2015;7:
 Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
INTRODUCTION. Jun-Ho Lee 1, Hyeun-Sung Kim 2, Jee-Soo Jang 2, Il-Tae Jang 3, Seong Hoon Oh 1, Jin-Uk Kim 1. Clinical Article
 Journal of Minimally Invasive Spine JMISST Surgery and Technique 1(1):5-10, 2016 Clinical Article eissn 2508-2043 http://dx.doi.org/10.21182/jmisst.2016.00066 www.jmisst.org Realizable Minimally Invasive
Journal of Minimally Invasive Spine JMISST Surgery and Technique 1(1):5-10, 2016 Clinical Article eissn 2508-2043 http://dx.doi.org/10.21182/jmisst.2016.00066 www.jmisst.org Realizable Minimally Invasive
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Is unilateral pedicle screw fixation superior than bilateral pedicle screw fixation for lumbar degenerative diseases: a meta-analysis
 Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Moo Sung Kang, Jeong Yoon Park, Kyung Hyun Kim, Sung Uk Kuh, Dong Kyu Chin, Keun Su Kim, and Yong Eun Cho
 BioMed Research International, Article ID 919248, 6 pages http://dx.doi.org/10.1155/2014/919248 Clinical Study Minimally Invasive Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw Fixation:
BioMed Research International, Article ID 919248, 6 pages http://dx.doi.org/10.1155/2014/919248 Clinical Study Minimally Invasive Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw Fixation:
T.L.I.F. Surgical Technique. Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System.
 Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Original Investigation. Peng Luo 1*, Rong-Xue Shao 2*, Ai-Min Wu 1, Hua-Zi Xu 1, Yong-Long ChI 1, Yan LIn 1 ABSTRACT
 DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
Peggers Super Summaries: The Aging Spine
 Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Same Segment Early Recurrence in Surgery of Lumbar Canal Stenosis- Role of Dissectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. II (August. 2016), PP 34-40 www.iosrjournals.org Same Segment Early Recurrence in Surgery
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. II (August. 2016), PP 34-40 www.iosrjournals.org Same Segment Early Recurrence in Surgery
This procedure lacks scientific evidence of effectiveness, and is not covered.
 ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
L-VARLOCK. Posterior Lumbar Cage with adjustable lordosis. S urgical T echnique
 L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
PARADIGM SPINE. Brochure. coflex-f Minimally Invasive Lumbar Fusion
 PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
T.L.I.F. Transforaminal Lumbar Interbody Fusion
 T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report
 Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Current Spine Procedures
 SPINE BOOT CAMP: WHAT YOU DON T KNOW MAY COST YOU! David Abraham, M.D. The Reading Neck and Spine Center Reading, PA Current Spine Procedures Epidural/Transforaminal Injections Lumbar Procedures Laminectomy
SPINE BOOT CAMP: WHAT YOU DON T KNOW MAY COST YOU! David Abraham, M.D. The Reading Neck and Spine Center Reading, PA Current Spine Procedures Epidural/Transforaminal Injections Lumbar Procedures Laminectomy
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Zheng Li, Fubing Liu, Shuhao Liu, Zixian Chen, Chun Jiang, Zhenzhou Feng, and Xiaoxing Jiang
 BioMed Research International Volume 2016, Article ID 7261027, 6 pages http://dx.doi.org/10.1155/2016/7261027 Clinical Study Miniopen Transforaminal Lumbar Interbody Fusion with Unilateral Fixation: A
BioMed Research International Volume 2016, Article ID 7261027, 6 pages http://dx.doi.org/10.1155/2016/7261027 Clinical Study Miniopen Transforaminal Lumbar Interbody Fusion with Unilateral Fixation: A
SURGICAL TECHNIQUE MANUAL. InterFuse T
 1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
Yoshinao Koike, Yoshihisa Kotani, Hidemasa Terao, Yoshiaki Hosokawa, Hideyuki Kobayashi, Yusuke Kameda, Hideaki Fukaya
 Comparative Analysis of Physical Function and Quality of Life Parameters in Two Surgical Modalities for Single-level Degenerative Spondylolisthesis: OLIF with Percutaneous Posterior Fixation in Lateral
Comparative Analysis of Physical Function and Quality of Life Parameters in Two Surgical Modalities for Single-level Degenerative Spondylolisthesis: OLIF with Percutaneous Posterior Fixation in Lateral
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Int J Clin Exp Med 2017;10(6): /ISSN: /IJCEM
 Int J Clin Exp Med 2017;10(6):9424-9431 www.ijcem.com /ISSN:1940-5901/IJCEM0048266 Original Article Learning curve of microendoscopy-assisted minimally invasive transforaminal lumbar interbody fusion:
Int J Clin Exp Med 2017;10(6):9424-9431 www.ijcem.com /ISSN:1940-5901/IJCEM0048266 Original Article Learning curve of microendoscopy-assisted minimally invasive transforaminal lumbar interbody fusion:
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_
 Orthopaedic Surgery (2009), Volume 1, No. 3, 176 183 ORIGINAL ARTICLE The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_030 176..183 Wei Liu MD,
Orthopaedic Surgery (2009), Volume 1, No. 3, 176 183 ORIGINAL ARTICLE The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_030 176..183 Wei Liu MD,
Efficacy of minimally invasive transforaminal lumbar interbody fusion for single-segment lumbar degenerative disease.
 Biomedical Research 2016; 27 (4): 1309-1315 ISSN 0970-938X www.biomedres.info Efficacy of minimally invasive transforaminal lumbar interbody fusion for single-segment lumbar degenerative disease. Aiguo
Biomedical Research 2016; 27 (4): 1309-1315 ISSN 0970-938X www.biomedres.info Efficacy of minimally invasive transforaminal lumbar interbody fusion for single-segment lumbar degenerative disease. Aiguo
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique
 Case Report Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique Shaishav Bhagat 1, Alexander Z. E. Durst
Case Report Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique Shaishav Bhagat 1, Alexander Z. E. Durst
QF-78. S. Tanaka 1, T.Yokoyama 1, K.Takeuchi 1, K.Wada 2, T. Tanaka 2, S.Abrakawa 2, G.Kumagai 2, T.Asari 2, A.Ono 2, Y.
 QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
Corporate Medical Policy
 Corporate Medical Policy Interspinous and Interlaminar Stabilization/Distraction Devices File Name: Origination: Last CAP Review: Next CAP Review: Last Review: interspinous_and_interlaminar_stabilization-distraction_devices
Corporate Medical Policy Interspinous and Interlaminar Stabilization/Distraction Devices File Name: Origination: Last CAP Review: Next CAP Review: Last Review: interspinous_and_interlaminar_stabilization-distraction_devices
MRI Measurement of Neuroforaminal Dimension at the Index and Supradjacent Levels after Anterior Lumbar Interbody Fusion: A Prospective Study
 Original Article Clinics in Orthopedic Surgery 2013;5:49-54 http://dx.doi.org/10.4055/cios.2013.5.1.49 MRI Measurement of Neuroforaminal Dimension at the Index and Supradjacent Levels after Anterior Lumbar
Original Article Clinics in Orthopedic Surgery 2013;5:49-54 http://dx.doi.org/10.4055/cios.2013.5.1.49 MRI Measurement of Neuroforaminal Dimension at the Index and Supradjacent Levels after Anterior Lumbar
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Compression of the lumbar nerve roots and subsequent leg
 INVITED REVIEW ARTICLE Lumbar Decompression Using a Tubular Retractor System Sapan D. Gandhi, BS,* Christopher K. Kepler, MD, MBA,w and D. Greg Anderson, MDw Summary: Spinal stenosis and intervertebral
INVITED REVIEW ARTICLE Lumbar Decompression Using a Tubular Retractor System Sapan D. Gandhi, BS,* Christopher K. Kepler, MD, MBA,w and D. Greg Anderson, MDw Summary: Spinal stenosis and intervertebral
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
ASJ. Radiologic and Clinical Courses of Degenerative Lumbar Scoliosis (10 25 ) after a Short-Segment Fusion. Asian Spine Journal.
 Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Coflex TM for Lumbar Stenosis with
 Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Spinal Stenosis Surgical
 Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Restoration of coronal imbalance in the
 INSTRUMENTATION AND TECHNIQUE Provisional Ipsilateral Expandable Rod for Disc Space Distraction in Minimally Invasive Transforaminal Lumbar Interbody Fusion: Operative Technique Luis M. Tumialán, MD* Justin
INSTRUMENTATION AND TECHNIQUE Provisional Ipsilateral Expandable Rod for Disc Space Distraction in Minimally Invasive Transforaminal Lumbar Interbody Fusion: Operative Technique Luis M. Tumialán, MD* Justin
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
VTI INTERFUSE T SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK. 1/20
 VTI INTERFUSE T SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK. 1/20 CONTENTS InterFuse T Product Description Indications for Use X-Ray Marker Locations Product Specifications Instrument Set 3 4 5 STEP
VTI INTERFUSE T SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK. 1/20 CONTENTS InterFuse T Product Description Indications for Use X-Ray Marker Locations Product Specifications Instrument Set 3 4 5 STEP
Technique Guide. StenoFix. Interspinous distraction after surgical decompression.
 Technique Guide StenoFix. Interspinous distraction after surgical decompression. Table of Contents Introduction StenoFix 2 Indications and Contraindications 4 Surgical Technique Preoperative Planning
Technique Guide StenoFix. Interspinous distraction after surgical decompression. Table of Contents Introduction StenoFix 2 Indications and Contraindications 4 Surgical Technique Preoperative Planning
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis
 Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Free Paper Session IX Spine II
 Free Paper Session IX Spine II 9. Oblique Lateral Interbody Fusion for L5-S Introduction: A minimally invasive modified anterior lumbar interbody fusion technique for the lumbosacral junction is described
Free Paper Session IX Spine II 9. Oblique Lateral Interbody Fusion for L5-S Introduction: A minimally invasive modified anterior lumbar interbody fusion technique for the lumbosacral junction is described
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra
 doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis
 Image-Guided Minimally Invasive Lumbar Last Review Status/Date: June 2013 Page: 1 of 10 Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis Description Image-guided minimally
Image-Guided Minimally Invasive Lumbar Last Review Status/Date: June 2013 Page: 1 of 10 Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis Description Image-guided minimally
Bony framework of the vertebral column Structure of the vertebral column
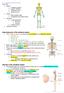 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
INTERVERTEBRAL BODY FUSION DEVICE. Surgical Technique
 INTERVERTEBRAL BODY FUSION DEVICE Surgical Technique Joint Spine Sports Med MectaLIF Oblique & Posterior Surgical Technique 2 INDEX 1. INTRODUCTION 4 1.1 Materials & Markers 5 2. INDICATIONS 6 3. CONTRAINDICATIONS
INTERVERTEBRAL BODY FUSION DEVICE Surgical Technique Joint Spine Sports Med MectaLIF Oblique & Posterior Surgical Technique 2 INDEX 1. INTRODUCTION 4 1.1 Materials & Markers 5 2. INDICATIONS 6 3. CONTRAINDICATIONS
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis. Original Policy Date
 MP 7.01.107 Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed
MP 7.01.107 Image-Guided Minimally Invasive Lumbar Decompression (IG-MLD) for Spinal Stenosis Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
REFERENCE DOCTOR Thoracolumbar Trauma MIS Options. Hyeun Sung Kim, MD, PhD,
 Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
