Low frequency ultrasound debridement (Sonoca-185) in acute wound management: a case study
|
|
|
- Gloria Holland
- 5 years ago
- Views:
Transcription
1 Low frequency ultrasound debridement (Sonoca-185) in acute wound management: a case study Citation: Shannon, M.K., Williams, A. and Bloomer, M. 2012, Low frequency ultrasound debridement (Sonoca-185) in acute wound management: a case study, Wound practice and research, vol. 20, no. 4, pp , Cambridge Publishing Reproduced with permission from the Editor of Wound Practice and Research. Downloaded from DRO: DRO Deakin Research Online, Deakin University s Research Repository Deakin University CRICOS Provider Code: 00113B
2 Low-frequency ultrasound debridement (Sonoca-185) in acute wound management: A case study Shannon MK, Williams A & Bloomer M Abstract There are numerous evidence-based wound debridement techniques that promote wound healing. However, some of these techniques may cause discomfort and pain for the patient and can be costly for the health care provider. A new, non-invasive wound debridement technique known as low-frequency ultrasonic debridement (LFUD) has been used for the removal of unhealthy tissue and bacterial load in wound management in the clinical setting. This paper reports the use of LFUD by a skin integrity clinical nurse consultant (CNC) as an adjuvant wound debridement and healing technique in a patient with a parastomal abscess. LFUD was found to benefit this patient in terms of expedited wound healing and increased comfort, enabling the patient to have a successful skin graft that led to complete wound closure and discharge from hospital in a timely manner. Keywords: debridement, wound bed preparation, antibacterial, wound healing, ultrasound, nurse-led intervention. What is already known Successful wound healing requires wound bed preparations and promotion of granulation and healing. Numerous techniques exist that aim to facilitate wound healing, with advantages and disadvantages for the patient and clinician already known. Meagan K Shannon* MN, DipMngmnt, DipCritCare, RN Skin Integrity Clinical Nurse Consultant Peninsula Health, VIC, Australia Tel mshannon@phcn.vic.gov.au Allison Williams RN, PhD Associate Professor, School of Nursing and Midwifery, Faculty of Medicine, Nursing and Health Sciences, Monash University VIC, Australia Melissa Bloomer MN(Hons), MNP, MPET, GCDE, GCPET, Crit Care Cert, BN, RN, FACN School of Nursing and Midwifery, Faculty of Medicine, Nursing and Health Sciences, Monash University, VIC, Australia *Corresponding author What this paper adds LFUD is a new technique available to skin integrity clinicians that results in efficient wound bed preparation, promotes healing by stimulating the inflammatory process and healing cascade, whilst also having an antimicrobial effect. This treatment offers an alternative to surgical/sharp debridement and an adjunct to wound care and management and potentially results in reduced length of stay and increased patient comfort. Introduction Wound bed preparation is vital for wound healing. Studies have shown that wound healing is improved with correct wound bed preparation, which includes appropriate debridement, infection control and moisture management 1-4. There are numerous debridement techniques available to remove devitalised, infected and/or necrotic tissue from the wound bed to promote wound healing. These include conservative and sharp wound debridement, autolytic, enzymatic, mechanical, chemical, biological or parasitic debridement and, more recently, low-frequency ultrasound debridement (LFUD). In the case study reported in this paper, LFUD technique was used to prepare the wound bed and aid in wound closure for a patient with a parastomal abscess. This new wound management initiative was a two-year project that commenced in October 2010 and was funded by the Department of Health, Victoria, Australia, in collaboration between the skin integrity and podiatry services in a metropolitan public hospital in Victoria. Literature review Research on conservative and sharp wound debridement, which involves the use of scalpel, scissors, or laser to cut Wound Practice and Research 200
3 away dead tissue, has shown that all have advantages and disadvantages 2,5. Sharp debridement is performed in an aseptic environment and is considered fast-acting and selective as it creates a blood-rich, clean wound surface in which granulating tissue can form 6-8. However, as opposed to conservative debridement, it can be painful for the patient and costly, especially if an operating room is required 5. Autolytic debridement is achieved by using the body s own enzymes via wound products such as transparent films, hydrogels and hydrocolloids that rehydrate and liquefy necrotic tissue, and is usually painless 5. Research has shown that this method is effective for wound healing by removing black, necrotic tissue and slough, but is considered a slow process 5-9, thus increasing the risk of infection 5. Enzymatic debridement utilises plant enzymes and ureas to rapidly digest necrotic tissue proteins. However, the need for a medical prescription and secondary dressings make this an expensive option and the treatment may produce inflammation and/ or discomfort for the patient 6. Mechanical debridement of necrotic tissue, which includes hydrotherapy, allows a dressing to proceed from moist to wet and then is manually removed to debride necrotic tissue 7. As this technique is nonselective, it may traumatise healthy or granulating healing tissue which may cause maceration or infection, and while it is relatively cheap, it can be time-consuming and painful 5-8. Chemical debridement is a technique that utilises bacteriocidal and bacteriostatic agents which can be cytotoxic to healthy granulation tissue and may be rendered inactive in a wound that contains blood or pus 5-7. Studies have demonstrated that this method remains controversial as benefits need to be closely observed against any disadvantageous effects on wound healing 9,10. Biological or parasitic debridement usually consists of sterile maggot larvae (Lucilia sericata) being introduced into a wound to secrete proteinase enzymes that help degrade necrotic tissue, digest bacteria and stimulate formation of granulation tissue 5. While it is relatively cheap and fast, it can be painful and unpleasant, and is contraindicated in patients with life-threatening, deep-tracking wounds and bleeding abnormalities 5,6,7,10,11. Other wound management therapies, such as negative pressure wound therapy (NPWT), can complement acute and chronic wound healing, with research supporting its effectiveness 12. This therapy was used in conjunction with LFUD in this case study. Figure 1. LFUD Sonoca-185. LFUD (Figure 1) is a relatively new technique used for wound debridement and to improve wound healing by perpetuating the wound healing cascade. LFUD was introduced to alleviate the pressure on operating rooms, decrease patient length of stay, enable debridement for patients who are unable to tolerate an anaesthetic, and facilitate follow-up and ongoing care in the community by a multidisciplinary team 13,14. This technique removes unhealthy tissue, decreases bacterial load or bioburden, and is considered non-invasive because it uses ultrasound waves (frequencies >20,000 cycles per second) in much the same way as dentists remove plaque 15. It has been reported that LFUD has numerous advantages, which include excellent wound bed preparation with antibacterial capabilities, minimal blood loss, improved patient safety and comfort, and cost savings due to decreased use of antibiotics, prevention of amputation and improved wound outcomes, particularly for patients who do not respond to standard wound care Compared to traditional conservative wound treatment, LFUD can expedite healing by removing impediments to healing whilst preserving a healthy, granulating wound bed that helps support successful skin closure via other surgical means such as skin grafting 20. LFUD technology has been used outside Australia for many years. Currently, there is no Australian published data on the use of LFUD 13,14. International research has shown that most LFUD studies have included either patients with chronic leg or diabetic foot ulcers except one study 15 that included patients with four large, non-healing surgical wounds which were debrided in preparation for skin closure via skin grafting. This study reported 107 LFUD treatments (range 6 15) on 17 patients over eight months. The outcome was that 53% of patient wounds had complete healing, 35% had at least a 50% reduction in wound size, and 12% experienced a 20 30% reduction in wound size. After commencing LFUD treatments, no patients required antibiotic treatment. The choice of wound debridement technique is dependent on the patient, availability of resources, the skill or qualification of the clinician, and cost. Each individual patient requires a considered assessment prior to the use of any debridement technique to ensure best practice for best patient outcomes. LFUD procedure The LFUD consists of a generator and a sonotrobe hand piece (Figure 2) attached to tubing connected to a sterile 500-millilitre bag of normal saline. A foot pedal connected to the generator is used to disperse the ultrasound to the sonotrobe head. Debridement is achieved via normal saline being streamed through the tubing to the sonotrobe head with high-frequency ultrasound waves 17 to create cavitation or oscillating micro-gas bubbles of the saline 18. The streaming, steady mechanical forces applied to all exposed surfaces disturbs the wound tissue where unhealthy tissue is washed or suctioned away and healthy tissue is stretched and tipped into an inflammatory process or healing cascade, ultimately Wound Practice and Research 201
4 and a total hip replacement in July 2010, complicated by infection and requiring inpatient rehabilitation for almost two months. Whilst an inpatient at rehabilitation recovering from the hip surgery, she developed abdominal pain, nausea, vomiting and fever with an increased white cell count and pus in the colostomy site requiring readmission to the acute hospital. Figure 2. Sonotrobes. debriding and healing at the same time 13,18. Amplitude or speed of the ultrasound waves can be adjusted on the generator according to the patient s tolerance, debridement and/or antibacterial needs 13,17. The period of debridement is calculated by the surface area of the wound divided by three, giving a minimum treatment time for antibacterial effect 13. The clinician may choose to continue treatment over the estimated time to remove all visible unhealthy tissue depending on the patient s tolerance. It is typical to initially treat the wound with a topical anaesthetic, such as Emla cream, to reduce sensitivity and improve patient tolerance. For example, neuropathic wounds may require no anaesthetic agents. Considerations when using LFUD There are three different styles of sonotrobe heads (Figure 3) which can be used to debride the wound: hoof, double ball and spatula. The hoof creates a shower head spray, the spatula creates a one-directional spray and the double ball creates a circular, multidirectional spray 14. The clinician makes the decision on which type of head to use based on the type of wound. For example, a cavity wound requires multidirectional spray; therefore the double ball would be preferred. An undulated flat surfaced wound would require a shower spray; therefore the hoof may be used. The spatula head is useful for large, flat-surfaced wounds. Infection control principles and personal protection measures are observed at all times when utilising the LFUD technique. Due to the potential spray associated with the LFUD technique, a one-metre clearance zone is maintained, shield mask and gown are highly recommended and appropriate wipe down of the clearance zone using recommended infection control wipes or detergents to prevent cross-infection is essential 14. The case study The patient is a 66-year-old, married female living at home with her husband. She has a history of Crohn's disease, with a bowel resection in 1997 and colostomy formation in 2003, chronic obstructive pulmonary disease, cholecystectomy, anaemia, asthma and gastro-oesophageal reflux disease. In 2008 she underwent a parastomal hernia repair with mesh, Investigation revealed a fistula into the abdominal wall had developed with infection around the stoma site. A laparotomy was performed and the parastomal abscess was drained. Four days later, the abdominal mesh inserted during a previous hernia repair was removed and the stoma was re-sited. On admission, her blood chemistry was within normal limits except an elevated white cell count and neutrophils. Her haemoglobin was slightly below accepted levels at 10.1 g/dl with total protein and calcium also below the recommended levels. The patient was considered to be within the healthy weight range for her age as assessed by a dietitian. Wound swabs showed small gram-positive and negative bacilli with a lot of degenerative cell debris. The patient s medication regimen post-laparotomy is detailed in Table 1. Negative pressure wound therapy (NPWT) was applied at all times in between LFUD debridement treatments at 80 mm/ Hg using sterile gauze as the medium of choice and changed twice weekly. The NPWT aided exudate management, increased the vascular supply and assisted with development of granulation tissue on the wound bed. Rationale for LFUD Surgical debridement was the first choice for this patient prior to the use of LFUD due to the complexity of the patient s wound. NPWT had been used on the wound for less than four weeks and discussions were held with the covering general surgical team in regards to goals and outcomes for this patient. A skin integrity clinical nurse consultant (CNC) referral was made four weeks after the laparotomy and revision of stoma (Figure 4). This referral was made to expedite timely debridement for this patient as there were concerns over multiple and subsequent anaesthetics and Figure 3. Sonotrobe heads hoof, ball and spatula. Wound Practice and Research 202
5 Table 1. The case study patient s medication regimen. Medication Dose Route Frequency Ceftriaxone 1 gm IV Daily Metronidazole 500 mg IV Three times per day Prednisolone 15 mg Orally Mane Aspirin 100 mg Orally Mane Enoxaparin sodium 20 mg Subcutaneous Daily Frusemide 40 mg Orally or IV Mane Humira 40 mg Subcutaneous Fortnightly Oxycodone IR 5 10 mg Orally PRN four hourly Oxycontin SR 5 mg Orally Twice per day Ondansetron 4 8 mg Orally or IV Three times per day Maxalon 10 mg Orally or IV Four times per day delays in operating room bookings necessary for sharp wound debridement. The skin integrity CNC was given responsibility to care for this patient s wound in consultation with the general surgical team. Following patient consent, the initial LFUD treatment was of 48 minutes in duration due to the size of the wound and the amount of devitalised tissue. The hoof sonotrobe head was chosen for the directional spray. As the pain experienced by the patient was minimal, the amplitude was set to a maximum effect of 100% for debridement with the normal saline flow (lavage) set at 20%. The patient was given oral opiate pain relief of Oxycodone 5 mg. Concurrent suction was used to control any saline splash and general infection control principles were adhered to. Undermining of the bridge tissue was noted between the old stoma site and laparotomy site. Improvement was seen in the abdominal swelling (Figure 5), periwound (surrounding skin) and overall skin integrity from first sighting, which was four weeks post-admission date. NPWT was used to continue to support granulation and management of exudate post-lfud treatment. The second treatment of LFUD was of 47 minutes' duration using the hoof and double ball sonotrobe head with concurrent suction. The hoof was used on the flat surfaces of the wound and the double ball head was used in the cavity and sinus areas that were exposed upon treatment. Bridge tissue was necrotic and required extensive debridement. LFUD revealed a large proximal right sinus of 8 centimetres (cm). There was noted undermining of the right side of the wound by 2.5 cm (very close to the stoma) and a proximal undermining flap of 4 cm (Figure 6). For this treatment, the amplitude was decreased to 80% and the saline flow was increased to 40% due to the patient experiencing 7/10 pain in the sinus and cavity areas. Wound Practice and Research 203
6 Figure 4. First view of wound post-laparotomy and revision of stoma. The third treatment of LFUD was of 35 minutes' duration. The right proximal wound depth decreased by 3 cm to measure 5 cm in depth, the right side of wound of 2.5 cm depth was resolved (very close to the stoma) and the proximal flap remained 4 cm deep (Figure 7). The hoof sonotrobe head was used for the flat surfaces of the wound and the double ball sonotrobe head was used for the undermining cavity and sinus areas. Amplitude was adjusted to 100% with flow adjusted to 40% according to the patient s tolerance and suction was simultaneously applied. The double ball revealed a 4 cm left distal tunnel. This section of wound treatment was limited due to the patient s severe pain. The final LFUD treatment was of 25 minutes' duration using the hoof sonotrobe head with amplitude of 80% and a flow of 25% that had been adjusted to the patient s pain tolerance. Due to the lower flow rate, shorter treatment time duration and smaller wound size, suction was not required (Figure 8). Outcomes The patient's length of stay was 66 days with the four LFUD treatments occurring over a 10-day period. NPWT was continued for just under nine weeks. There was successful wound healing of over 60% within five days of commencing LFUD. Within another three days the wound size had decreased by almost another 50%. The patient returned to rehabilitation care and gained sufficient wound granulation Figure 6. Post second LFUD treatment of 47 minutes' duration. tissue with maintenance NPWT to have the wound surgically grafted 12 days after the final LFUD treatment. Recovery was uneventful post-skin graft and the patient was discharged home. Discussion Whilst the LFUD technique was valuable for this patient s wound management, the time taken to use this technique by the skin integrity CNC must be acknowledged. We recommend a combination of LFUD and conservative sharps wound debridement to manage such a large wound based on our experience in this case study. The conservative sharps wound debridement would remove the bulk of the obvious unhealthy tissue and allow the LFUD to remove the last of the unhealthy tissue without damaging the wound bed whilst still having the benefits of an antimicrobial effect and instigation of the healing cascade. Despite this, LFUD proved to be an optimal technique for wound debridement and wound bed preparation in conjunction with NPWT for this patient as the outcome was complete wound closure with skin graft and discharge home. Conclusion The use of LFUD as an adjunct in the healing or improving of chronic wounds was supported by this case study. The outcome for this patient with a parastomal abscess has been positive as complete wound closure was obtained. The LFUD achieved all the expected outcomes for this wound in that the Figure 5. Post first LFUD treatment of 48 minutes' duration. Figure 7. Post third LFUD treatment of 35 minutes' duration. Wound size decreased by over 60%. Wound Practice and Research 204
7 Figure 8. Post fourth LFUD treatment of 25 minutes' duration. Wound size decreased by almost another 50%. wound bed preparation was acceptable for skin grafting by removing unhealthy tissue and bioburden, while controlling the patient s level of discomfort and pain. The patient required minimal medication including anaesthetic agents and analgesics, and no intra-hospital transfer was required with cost benefits for the treating hospital. In addition, treatment time leading to health benefits for the patient was reduced. Given the wound care for this patient was led by the skin integrity CNC and the ability to utilise the LFUD in the clinical setting, there was the capacity to maintain a degree of flexibility with treatment times, thus allowing for other patient care needs. agents in treating surgical wounds healing by secondary intention. York: NHS Centre for Reviews and Dissemination, Ayello EA & Cuddigan JE. Debridement: Controlling the necrotic/cellular burden. Adv Skin Wound Care 2004; 17(2): Baharestani M. The clinical relevance of debridement. In: Baharestani M, Gottrup F, Holstein P & Vanscheidt W (eds). The clinical relevance of debridement. Berlin: Springer-Verlag, 1999, pp Guy H & Grothier L. Using negative pressure therapy in wound healing. Nurs Times 2012; 108(36): HealthPACT Review S Health Scanning Technology Prioritising Summary. Low frequency ultrasound debridement. Australian and New Zealand Horizon Scanning Network (February 2007). 14. Medi-Group Australia, Accessed 25 September Breuing KH, Bayer L, Newalder MA & Dennis PO. Early experience using low frequency ultrasound in chronic wounds. Ann Plast Surg 2005; 55(2): Peschen M, Weichenthal M, Schopf E & Vanschiedt W. Low frequency ultrasound treatment of chronic venous leg ulcers in an outpatient therapy. Acta Derm Venerol 1997; 77: Ennis WJ, Formann P, Mozen N, Massey J, Conner-Kerr T & Meneses P. Ultrasound therapy for recalcitrant diabetic foot ulcers: Results of a randomised, double-blind, controlled, multicenter study. Ostomy Wound Manag 2005; 51(8): Tan J, Abisi S, Smith A & Burnand KG. A painless Method of Ultrasonically Assisted Debridement of Chronic Leg Ulcers: A Pilot Study. Eur J Vasc Endovasc 2007; 33: Weichenthal M, Mohr P, Stegmann W & Breitbart EW. Low-frequency ultrasound treatment of chronic venous ulcers. Wound Repair Regen 1997; 5(1): Hierner R, Degreef H, Vranckx JJ, Garmyn M, Massage P & van Brussel M. Skin grafting and wound healing the dermato-plastic team approach. Clin Dermatol 2005; (3): Whilst LFUD is identified as an excellent modality for wound debridement, the need to continue embracing other well-known debridement techniques has not been ignored. Instead, LFUD is now considered to be another arsenal for skin integrity services and can be used as an adjunct in the debridement and antibacterial management of wounds. Further research to support the use of LFUD with and without NPWT and in combination with other methods of debridement is recommended. References 1. Panuncialman J & Falanga V. The science of wound bed preparation. Surg Clin N Am 2009; Schultz GS, Sibbald RG, Falanga V et al. Wound bed preparation: A systematic approach to wound management. Wound Repair Regen 2003; 11(Suppl 1):S Sibbald R G, Goodman L, Woo KY et al. Special considerations in wound bed preparation 2011: An update. Adv Skin Wound Care 2011 Sept; Sibbald RG, Orsted H, Schultz G, Coutts P & Keast D. Preparing the wound bed: Focus on infection and inflammation. Ostomy Wound Manag 2003; 49(11): Smith F, Dryburgh N, Donaldson J & Mitchell M. Debridement for surgical wounds. Cochrane Database Syst Rev, The Cochrane Collaboration, John Wiley & Sons Ltd. Edinburgh Napier University Accessed 22 October Carville K. Wound Care Manual. 5th edn. Australia: Silver Chain Foundation, Caliano C, Cobb M, Davis K et al. Wound Care an Incredibly Visual Pocket Guide. Philadelphia: Lippincott Williams & Wilkins, Lewis R, Whiting P, ter Reit G, O Meara S & Glanville J. A rapid systematic review of the clinical effectiveness and cost effectiveness of debriding Wound Practice and Research 205
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Emil Schmidt Wound Care specialist SDHB - Otago
 Prospective randomised trial of low frequency ultrasound debridement (LFUD) in management of lower limb wounds Krysa J, Schmidt E, Thomson I, van Rij A Emil Schmidt Wound Care specialist SDHB - Otago Background
Prospective randomised trial of low frequency ultrasound debridement (LFUD) in management of lower limb wounds Krysa J, Schmidt E, Thomson I, van Rij A Emil Schmidt Wound Care specialist SDHB - Otago Background
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Surgical site infections have been
 For patients undergoing complex abdominal or bowel surgery, the risk of infection and the resultant dehiscence if an infection occurs can pose a great challenge LINDSEY BULLOUGH Tissue Viability Nurse,
For patients undergoing complex abdominal or bowel surgery, the risk of infection and the resultant dehiscence if an infection occurs can pose a great challenge LINDSEY BULLOUGH Tissue Viability Nurse,
DEBRIDEMENT. In This Chapter. Chapter 8. Necrotic Tissue Eschar Slough Types of Debridement When Not to Debride...
 Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL. of the infection risk in chronic wound
 Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Embrace the Call to Wound Prevention and Care
 CONCLUSION Embrace the Call to Wound Prevention and Care A challenging career Be part of an interprofessional team Help patients, families, communities Commit to lifelong learning To cure occasionally,
CONCLUSION Embrace the Call to Wound Prevention and Care A challenging career Be part of an interprofessional team Help patients, families, communities Commit to lifelong learning To cure occasionally,
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Post-surgical wound management of pilonidal cysts by using a haemoglobin spray
 Post-surgical wound management of pilonidal cysts by using a haemoglobin spray Nesat Mustafi 1 & Peter Engels 2 1 Wound center, Nordwest Hospital, Frankfurt, Germany, 2 Bergisch Gladbach, Germany Objective:
Post-surgical wound management of pilonidal cysts by using a haemoglobin spray Nesat Mustafi 1 & Peter Engels 2 1 Wound center, Nordwest Hospital, Frankfurt, Germany, 2 Bergisch Gladbach, Germany Objective:
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Debridement: treatment, options and selection.
 This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
Sarah Medrano, RN, BSN, WOCN; and Mary Jo Beneke, RN, BS, CWOCN Yuma Regional Medical Center, Yuma, Arizona
 Sound Evidence coustic Pressure Wound Therapy to ebride Unstageable Pressure Ulcers in the cute Care Setting: Case Series Sarah Medrano, RN, BSN, WCN; and Mary Jo Beneke, RN, BS, CWCN Yuma Regional Medical
Sound Evidence coustic Pressure Wound Therapy to ebride Unstageable Pressure Ulcers in the cute Care Setting: Case Series Sarah Medrano, RN, BSN, WCN; and Mary Jo Beneke, RN, BS, CWCN Yuma Regional Medical
Debridement within the context of the EWMA s debridement guidelines. Emil Schmidt WCNS SDHB - Otago
 Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
NPWT Case Series EXPERIENCES WITH INVIA MOTION. Precious life Progressive care. Invia Motion Negative Pressure Wound Therapy
 NPWT Case Series EXPERIENCES WITH INVIA MOTION Invia Motion Negative Pressure Wound Therapy Precious life Progressive care npwt_case_booklet_a4.indd 1 18.12.13 13:17 Chronic sacral pressure ulcer Case
NPWT Case Series EXPERIENCES WITH INVIA MOTION Invia Motion Negative Pressure Wound Therapy Precious life Progressive care npwt_case_booklet_a4.indd 1 18.12.13 13:17 Chronic sacral pressure ulcer Case
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude
 Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Use of an outside force to remove nonviable. Wound Debridement Guide South West Regional Wound Care Program Last Updated March 12,
 Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers
 A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
Pressure Ulcers: 3 Keys to Pressure Ulcer Management. Evidence Based Prevention & Management. I have no financial conflicts of interest
 Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Essity Internal. Taking the fear out of wound infection: conquering everyday issues
 Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
Genadyne A4 and foam to treat a postoperative debridment flank abscess
 Genadyne A4 and foam to treat a postoperative debridment flank abscess Michael S. DO, The Wound Healing Center Indianapolis, IN Cynthia Peebles RN D.O.N., Becky Beck RN Heartland at Prestwick NH Avon,
Genadyne A4 and foam to treat a postoperative debridment flank abscess Michael S. DO, The Wound Healing Center Indianapolis, IN Cynthia Peebles RN D.O.N., Becky Beck RN Heartland at Prestwick NH Avon,
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur
 VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
The word debridement derives from the
 Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Overview. Holistic Approach 07/04/2014. My Resident Has a Chronic Wound. Wound Causes Factors that impair wound healing Wound Assessment
 My Resident Has a Chronic Wound Now What??? Jolene Heil RN ET MClScWH April 8, 2014 Overview Wound Causes Factors that impair wound healing Wound Assessment Holistic Approach What is the cause of the wound?
My Resident Has a Chronic Wound Now What??? Jolene Heil RN ET MClScWH April 8, 2014 Overview Wound Causes Factors that impair wound healing Wound Assessment Holistic Approach What is the cause of the wound?
Consensus guidance for the use of debridement techniques in the UK
 Consensus guidance for the use of debridement techniques in the UK In Autumn 2010, a multidisciplinary group of clinicians met in Manchester to discuss the issue of debridement in wound management. There
Consensus guidance for the use of debridement techniques in the UK In Autumn 2010, a multidisciplinary group of clinicians met in Manchester to discuss the issue of debridement in wound management. There
TIME CONCEPT AND LOCAL WOUND MANAGEMENT
 TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
o Venous edema o Stasis ulcers o Varicose veins (not including spider veins) o Lipodermatosclerosis
 Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Fundamentals Of Wound Management. Julie Hewish Senior Tissue Viability Nurse
 Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Pressure Ulcer Prevention Guidelines
 EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
The Risk. Background / Bias. Integrating Wound Care into a Limb Preservation Initiative 4/24/2009
 Stimulating Wound Granulation: Advances in NPWT and other Measures (Wound Bed Preparation) Charles Andersen MD, FACS, FAPWCA Clinical Prof of Surgery UW, USUHS Chief Vascular/Endovascular/ Limb Preservation
Stimulating Wound Granulation: Advances in NPWT and other Measures (Wound Bed Preparation) Charles Andersen MD, FACS, FAPWCA Clinical Prof of Surgery UW, USUHS Chief Vascular/Endovascular/ Limb Preservation
RN Cathy Hammond. Specialist Wound Management Service at Nurse Maude Christchurch
 RN Cathy Hammond Specialist Wound Management Service at Nurse Maude Christchurch 14:00-14:55 WS #141: Wound Infection - What You Need to Know 15:05-16:00 WS #153: Wound Infection - What You Need to Know
RN Cathy Hammond Specialist Wound Management Service at Nurse Maude Christchurch 14:00-14:55 WS #141: Wound Infection - What You Need to Know 15:05-16:00 WS #153: Wound Infection - What You Need to Know
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Many patients with chronic wounds. Case reports. The use of Prontosan in combination with Askina Calgitrol : an independent case series
 Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Management of Complex Wounds with Vacuum Assisted Closure
 Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
ACOFP 55th Annual Convention & Scientific Seminars. New Physicians and Residents: Introduction to Wound Care. Katherine Lincoln, DO, FAAFP
 8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
Clinical Policy Title: Debridement of diabetic foot ulcers
 Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
QUICK GUIDE SNAP THERAPY SYSTEM
 QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
Wound and Ostomy Care: Basics and Troubleshooting
 Wound and Ostomy Care: Basics and Troubleshooting Catherine Clarey-Sanford, PhD, RN, CWOCN Conflict of Interest No conflict of interest exists No commercial interest No financial benefits Specific wound
Wound and Ostomy Care: Basics and Troubleshooting Catherine Clarey-Sanford, PhD, RN, CWOCN Conflict of Interest No conflict of interest exists No commercial interest No financial benefits Specific wound
CASE 1: TYPE-II DIABETIC FOOT ULCER
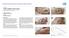 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Use of Non-Contact Low Frequency Ultrasound in Wound Care
 Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
South West Regional Wound Care Toolkit F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE)
 F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE) F.5 SURGICAL WOUND (CLOSED AND OPEN) 5.1 Background to Etiology Closed surgical wounds are well-approximated with a palpable healing ridge
F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE) F.5 SURGICAL WOUND (CLOSED AND OPEN) 5.1 Background to Etiology Closed surgical wounds are well-approximated with a palpable healing ridge
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine
 Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Negative Pressure Wound Therapy (NPWT)
 Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Chapter 14 8/23/2016. Surgical Wound Care. Wound Classifications. Wound Healing. Classified According to. Phases
 Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
The Georgetown Team Approach to Diabetic Limb Salvage: 2013
 The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study
 The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study Woundmanagement Summary In the treatment of patients with chronic
The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study Woundmanagement Summary In the treatment of patients with chronic
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Ray Norris, Rachel Henchy
 Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Basic Dressing Categories
 Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
CLINICAL EVIDENCE Negative Pressure Wound Therapy (NPWT)
 CLINICAL EVIDENCE Negative Pressure Wound Therapy (NPWT) Endoform forms part of the NPWT strategy Endoform fits seamlessly with NPWT approaches. Utilize Endoform within the wound bed to help stabilize,
CLINICAL EVIDENCE Negative Pressure Wound Therapy (NPWT) Endoform forms part of the NPWT strategy Endoform fits seamlessly with NPWT approaches. Utilize Endoform within the wound bed to help stabilize,
THERAPIES. HAND IN HAND. Need safe and efficient infection prevention and management? 1 The Cutimed. Closing wounds. Together.
 Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
Northumbria Healthcare NHS Foundation Trust. Laparoscopic Cholecystectomy. Issued by the Department of Upper Gastrointestinal Surgery
 Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
Using a combination of surgical debridement, negative pressure wound therapy and hyperbaric oxygen therapy
 Using a combination of surgical debridement, negative pressure wound therapy and hyperbaric oxygen therapy KEY WORDS Hyperbaric oxygen therapy Negative pressure wound therapy Surgical debridement Ulceration
Using a combination of surgical debridement, negative pressure wound therapy and hyperbaric oxygen therapy KEY WORDS Hyperbaric oxygen therapy Negative pressure wound therapy Surgical debridement Ulceration
1/5. Introduction. Primary endpoint Time to reach readiness for closure by surgical intervention or left for closure by secondary intention
 1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
Table of Contents. Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings
 Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Prontosan. Clean. Easy Wound Healing. Wound Cleansing
 Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Wound Management in the Elderly
 Wound Management in the Elderly Stephanie Yates, MSN, ANP, ANP-BC, CWOCN Nurse Practitioner/CNS Duke University Medical Center Durham, NC stephanie.yates@duke.edu Skin Condition Key quality indicator To
Wound Management in the Elderly Stephanie Yates, MSN, ANP, ANP-BC, CWOCN Nurse Practitioner/CNS Duke University Medical Center Durham, NC stephanie.yates@duke.edu Skin Condition Key quality indicator To
Small Bowel and Colon Surgery
 Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
