Survival Rates and Risk Factors for Cephalad and L5 S1 Adjacent Segment Degeneration after L5 Floating Lumbar Fusion : A Minimum 2-Year Follow-Up
|
|
|
- Martin Little
- 5 years ago
- Views:
Transcription
1 J Korean Neurosurg Soc 57 (2) : , 2015 Print ISSN On-line ISSN Copyright 2015 The Korean Neurosurgical Society Clinical Article Survival Rates and Risk Factors for Cephalad and L5 S1 Adjacent Segment Degeneration after L5 Floating Lumbar Fusion : A Minimum 2-Year Follow-Up Young-Seok Lee, M.D., Young-Baeg Kim, M.D., Ph.D., Seung-Won Park, M.D., Ph.D. Department of Neurosurgery, Chung-Ang University College of Medicine, Seoul, Korea Objective : Although the L5 S1 has distinct structural features in comparison with other lumbar spine segments, not much is known about adjacent segment degeneration (ASD) at the L5 S1 segment. The aim of study was to compare the incidence and character of ASD of the cephalad and L5 S1 segments after L5 floating lumbar fusion. Methods : From 2005 to 2010, 115 patients who underwent L5 floating lumber fusion were investigated. The mean follow-up period was 46.1 months. The incidence of radiological and clinical ASD of the cephalad and the L5 S1 segments was compared using survival analysis. Risk factors affecting ASD were analyzed using a log rank test and the Cox proportional hazard model. Results : Radiological ASD of the L5 S1 segment had a statistically significant higher survival rate than that of the cephalad segment (p=0.001). However, clinical ASD of the L5 S1 segment was significantly lower survival rates than that of the cephalad segment (p=0.038). Risk factor analysis showed that disc degeneration of the cephalad segment and preoperative spinal stenosis of the L5 S1 segment were risk factors. Conclusion : In L5 floating fusion, radiological ASD was more common in the cephalad segment and clinical ASD was more common in the L5 S1 segment. At the L5 S1 segment, the degree of spinal stenosis appears to be the most influential risk factor in ASD incidences, unlike the cephalad segment. Key Words : Radiological adjacent segment degeneration Clinical adjacent segment degeneration L5 S1 segment. INTRODUCTION Lumbar spinal fusion is effective for reducing low back pain and radiculopathy and maintaining spine stability. As techniques for spinal instrumentation and imaging have developed, lumbar spine fusion is more widely performed than before 5). However, adjacent segment degeneration (ASD) may occur following lumbar spine fusion because of increases in intervertebral stress and adjacent segment motions. ASD can be further categorized as radiological ASD (RASD), clinical ASD (CASD), and reoperation (i.e., additional decompression or arthrodesis). The rate of RASD is %; CASD, %; and reoperation, % 5,10,12,18,21). Although numerous studies have attempted to study ASD after lumbar spinal fusion, it is difficult to explain the relations between radiological outcomes and clinical symptoms in a consistent manner 4). And, many risk factors are known, including degeneration of the adjacent facet joint, fusion length, sagittal alignment, adjacent disc degeneration, lumbar stenosis, age, osteoporosis, sex, and postmenopausal state 1,8,12,18,21). The L5 S1 segment has distinctive biomechanical motions different from other lumbar segments 16,22). It is related to the function of the iliolumbar ligament, which supports and stabilizes the lumbosacral junction 6,15). Accordingly, the L5 S1 degeneration rate in patients who undergo L5 floating fusion (i.e., lumbar fusion stopped at L5) is %, which is lower than the rate of ASD in the proximal fusion level 5,6,14). Our experiences suggest that L5 radiculopathy is common after L5 floating fusion. Additionally, disc degeneration at the L5 S1 segment occurs frequently in cases when marked degeneration occurs at the L3 4 and L4 5 segments 2). Therefore, we attempted to study the radiological and clinical outcomes of ASD at the L5 S1 segment after L5 floating fusion. This study aimed to compare ASD at the cephalad and L5 S1 segments after L5 floating fusion and to elucidate the characteristics of ASD at the L5 S1 segment. Furthermore, Received : June 30, 2014 Revised : September 2, 2014 Accepted : September 4, 2014 Address for reprints : Young-Baeg Kim, M.D., Ph.D. Department of Neurosurgery, Chung-Ang University College of Medicine, 102 Heukseok-ro, Dongjak-gu, Seoul , Korea Tel : , Fax : , ybkim1218@cau.ac.kr This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. 108
2 Adjacent Segment Degeneration YS Lee, et al. this study aimed to identify the risk factors of ASD at the cephalad and the L5 S1 segments and any other factors affecting clinical outcomes. MATERIALS AND METHODS Between 2005 and 2010, L5 floating lumbar fusion was performed for 236 patients, and among them, 115 (44 male, 71 female) patients who were observed for more than 2 years were included in the study (Table 1). Patients treated with L5 floating lumbar fusion had severe low back pain and/or radiculopathy, which could not be improved through conservative management. Patients were excluded if operations were initiated because of acute fracture, malignancy, acute infection, preoperative spondylolisthesis 4 mm, or severe disc degeneration (Pfirrmann Classification) 20) in adjacent segments. All patients underwent transforaminal lumbar interbody fusion by a single surgeon (second author) following an identical procedure, and no decompression was performed in adjacent segments. Whitecloud s function scale was used to measure functional outcomes 6,24). ASD was defined as newly developed lesions in the adjacent segments of patients who did not have radiological and/or clinical changes within 6 months postoperatively 12). ASD was further categorized as RASD, CASD, and reoperation, and the cephalad ASD and L5 S1 segment ASD were separated. RASD was defined using plain radiography as follows : 1) instability : 10 angulations based on flexion/extension lateral radiographs; 2) listhesis >4 mm : anterior, posterior, or lateral translation on anteroposterior and lateral radiographs; and 3) an increase to grade 2 in disc degeneration based on the University of California at Los Angeles grading scale 6). Changes in the cephalad and L5 S1 segments were evaluated before and after surgery and at each follow-up using plain radiography. CASD was defined as newly developed back pain and/or radiculopathy in relation to the adjacent operation sites. The time to RASD, CASD, and reoperation were also measured. The osteoarthritis grade of the facet joint was evaluated based on preoperative computed tomography 23). Disc degeneration was evaluated using the Pfirrmann 5-grade classification 20), and spinal stenosis was evaluated using 4-grade classification on T2- weighted magnetic resonance imaging before surgery 7). The measurements and evaluations based on radiography were initially obtained by the first author as an independent observer, and the two other surgeons reviewed and confirmed the results. For RASD, CASD, and reoperation at the cephalad and L5 S1 Table 1. Patient population by initial diagnosis Diagnosis No. of cases Spinal stenosis 35 Degenerative spondylolisthesis 53 Isthmic spondylolisthesis 06 Degenerative scoliosis 05 Others 06 segments, the 36- and 60-month survival incidences were investigated using the Kaplan-Meier survivorship method. Using a log rank test, we compared RASD, CASD, and reoperation in the cephalad and L5 S1 segments with respect to the other factors. Moreover, the risk factors for RASD, CASD, and reoperation on the cephalad and L5 S1 segments were investigated using the Cox proportional hazard model. Correlation analysis was performed using a Spearman rank test to determine the contribution of independent variables to the measured functional outcome. All statistical analyses were conducted using SPSS version (SPSS Inc., Chicago, IL, USA), and a p value <0.05 was considered statistically significant. RESULTS Patient age at the time of operation was 58.2±10.0 years (range, years). The levels of operations were L4 5 (64 patients), L3 5 (43 patients), and L2 5 (8 patients). The mean follow-up period was 46.1 months (range, months). In 115 patients, 25 (21.7%) and 8 (7.0%) had cephalad and L5 S1 segment RASD, respectively. RASD was related to spinal instability (n=9, 36%) and spondylolisthesis (n=14, 56%), whereas L5 S1 segment RASD was mainly due to disc degeneration (n=6, 75%). CASD was found on the cephalad segment in 4 patients (3.5%) and on the L5 S1 segment in 12 patients (8.7%). The main symptom of cephalad segment CASD was back pain, and for L5 S1 segment CASD, it was either L5 radiculopathy (n=8) or back pain (n=4). Among patients with CASD, 2 cephalad segment cases (50%) and 5 L5 S1 segment cases (41.7%) were treated with reoperations (Table 2). Among 25 patients who had RASD at the cephalad segment, CASD was found in 4 patients (15.0%); however, CASD was not found among patients without RASD. Among 5 patients who had RASD at the L5 S1 segment, 3 patients (60.0%) had CASD. Moreover, 9 (8.4%) of 107 patients who did not have RASD when evaluated by plain radiography were found to have CASD (Table 3). The occurrence rates of RASD and CASD at the cephalad and L5 S1 segments were compared using the Kaplan-Meier survivorship method. The 36- and 60-month survival rates of RASD Table 2. The incidence and character of the RASD, CASD, and reoperation at the cephalad and caudad (L5 S1) segments L5 S1 segment RASD Instability Spondylolisthesis Disc degeneration CASD Back pain Radiculopathy Reoperation CASD : clinical adjacent segment degeneration, RASD : radiological adjacent segment degeneration 109
3 J Korean Neurosurg Soc 57 February 2015 Table 3. The prevalence of the RASD and CASD at the cephalad and caudad (L5 S1) segments CASD RASD RASD CASD : clinical adjacent segment degeneration, RASD : radiological adjacent segment degeneration Survival rate (%) Clinical ASD Censored 70 Survival rate (%) Radiological ASD Censored Survival times (months) Fig. 1. Kaplan-Meier survivorship curve. The survival rate of the cephalad and caudad (L5 S1) segments for radiological adjacent segment degeneration (ASD) (p=0.001). at the cephalad segment were 88.0% and 63.2%, respectively, whereas those of RASD at the L5 S1 segment were 95.9% and 91.9%, respectively; this implies that RASD is more common at the cephalad segment than at the L5 S1 segment level (p=0.001) (Fig. 1). Conversely, the 36- and 60-month survival rates of CASD at the cephalad segment were 99.1% and 91.7%, respectively, and 91.2% and 87.6% at the L5 S1 segment, respectively; this implies that CASD was more common at the L5 S1 segment than at the cephalad segment level (p=0.038) (Fig. 2). No differences were found in the patients undergoing reoperation between the two groups (p=0.288) (Table 4, Fig. 3). RASD, CASD, and reoperation based on sex, age (>60 years), level (single vs. multiple), subchondral bone mineral density (Tscore 2.5 criteria), disc degeneration (grade I/II/III vs. IV/V), spinal stenosis (none/mild vs. moderate/severe), and facet joint osteoarthritis (grade 0/1 vs. 2/3) were compared using a log rank Survival times (months) Fig. 2. Kaplan-Meier survivorship curve. The survival rate of the cephalad and caudad (L5 S1) segments for clinical adjacent segment degeneration (ASD) (p=0.038). Table 4. The survival rate of the cephalad and caudad (L5 S1) segments at 36 and 60 months Cephalad segment (%) Caudad (L5 S1) segment (%) p value RASD 0.001* 36 months months CASD 0.038* 36 months months Reoperation 0.288* 36 months months *Statistically significant difference (p<0.05). CASD : clinical adjacent segment degeneration, RASD : radiological adjacent segment degeneration test. The occurrence of RASD at the cephalad segment was significantly correlated to preoperative disc degeneration (p=0.010), and CASD was significantly related to disc degeneration and facet joint osteoarthritis before surgery (p=0.034, 0.049). In cases involving the L5 S1 segment, RASD, CASD, and reoperation were more common when spinal stenosis was higher than moderate (p=0.026, 0.015, 0.001, respectively) (Table 5). The Cox proportional hazard model analysis showed that disc degeneration [p=0.002; odds ratio (OR)=5.1; 95% confidence interval (CI), ] and occurrence of RASD at the cephalad segment and degree of spinal stenosis (p=0.008; OR=7.4; 95% CI, ) was significantly correlated with CASD at the L5 S1 segment. Based on Whitecloud s criteria for outcomes, 52 patients appeared to have excellent outcomes, 44 patients had good outcomes, 12 had fair outcomes, and 7 had poor outcomes. Factors 110
4 Adjacent Segment Degeneration YS Lee, et al. that were correlated with outcomes based on Spearman rank correlation were age [Spearman s rho (r)=0.20, p=0.029], segment level (r=0.25, p=0.008), disc degeneration before surgery on the cephalad and L5 S1 segments (r=0.25, p=0.007 and r=0.22, p= 0.017, respectively), spinal stenosis before surgery at the cephalad and L5 S1 segments (r=0.19, p=0.046 and r=0.19, p=0.042, respectively), and facet joint osteoarthritis grade at the cephalad segment (r=0.22, p=0.016). DISCUSSION Survival rate (%) Reoperation Censored Survival times (months) Fig. 3. Kaplan-Meier survivorship curve. The survival rate of the cephalad and caudad (L5 S1) segments for reoperation (p=0.288). The lumbosacral junction has distinctive structural and biomechanical characteristics that are different from those of other lumbar spine segments. During segmental flexion, the degree of flexion gradually increases as it approaches the lower lumbar segment, while the flexion angle decreases at the L5 S1 segment 16,19,22). This occurs because the posterior band of the iliolumbar ligament and the relative thicknesses of the L5 transverse process affect the range of motion of the lumbosacral segment and therefore maintain stability 13,17). Many authors have reported that ASD occurs more at the proximal segment than at the distal segment 3-5). However, Sears et al. 21) found that in 404 patients who underwent L5 floating fusion at 4 levels (excluding long segment fusion), cephalad ASD was found in 27 patients, caudal ASD in 27 patients, and both cephalad and caudal ASD in 5 patients, which showed that the rates of reoperation between the cephalad and L5 S1 segments ASD were identical. Similarly, our study found that reoperation on the lumbosacral junction was similar to that on the cephalad segment; however, because of the biomechanical influence of the lumbosacral junction, radiological and clinical outcomes were different in patients with cephalad segment involvement. ASD is caused by excessive mobility because of disc and facet joint degeneration on segments adjacent to fusion sites, which results in facet joint degeneration and induces spondylolisthesis and spinal instability leading to back pain 4). Furthermore, foramen and canal stenosis is caused by facet joint degeneration and hypertrophy, thickening of the ligamentum flavum, and disc degeneration, which leads to radiculopathy 6). In particular, foraminal stenosis is markedly more common than central or lateral recess stenosis in the L5 S1 segments 2). In our present study, back pain seemed to be the main symptom at the cephalad segment because of spinal instability and spondylolisthesis, and L5 radiculopathy seemed to be the main symptom due to foraminal stenosis in the L5 S1 segment. In cephalad segment ASD, clinical symptoms were found only in RASD patients. However, at the L5 S1 segment, clinical symptoms were found regardless of presence of RASD on plain radiographs. When RASD was evaluated based on plain radiography, sensitivity was 100% but specificity was only 18.9% at the cephalad segment. However, at the L5 S1 segment, sensitivity and specificity were 25% and 4.9%, respectively, indicating lower diagnostic values. Cheh et al. 4) reported sensitivity and specificity as 78.9% and 26.7%, respectively. This finding seems to have resulted from development of ASD in proximal areas of prior fusion (88.8%, 71 out of 80 cases). Instability occurs less frequently at L5 S1 because of the existence of the iliolumbar ligament. Furthermore, since L5 S1 is overlapped by the pubic bone on plain radiography, ill-defined radiographic images are produced, which Table 5. The result of prognostic factors analysis by the log rank test Risk factor 111 Reoperation CASD RASD Reoperation CASD RASD Sex Age Number of fusion levels BMD Disc degeneration * 0.010* Spinal stenosis * 0.015* 0.026* Facet joint * * *Statistically significant difference (p<0.05). CASD : clinical adjacent segment degeneration, RASD : radiological adjacent segment degeneration, BMD : bone mineral density
5 J Korean Neurosurg Soc 57 February 2015 may explain the low sensitivity and specificity. The cephalad segment has an especially high sensitivity and provides a clue regarding requirement of further evaluation. However, at the L5 S1 segment, plain radiography cannot provide sufficient information; therefore, additional tests are recommended. Similar results were found on comparative studies of RASD and CASD at the cephalad and L5 S1 segments. Kim et al. 9) reported that RASD was found at a rate of 55.9% with unilateral pedicle screw insertion and 72.9% with bilateral pedicle screw insertion in a minimum 10-year follow-up. Cheh et al. 4) reported that 42.6% (80 of 188 patients) had RASD in a minimum 5-year follow-up period, and among those, 56.3% (45 of 80 patients) had CASD. In this study, we investigated the occurrence rates of RASD and CASD at the cephalad and L5 S1 segments in L5 floating fusion and compared the results. After 5 years, 36.8% had RASD at the cephalad segment and 8.9% at the L5 S1 segment. The occurrence rates of CASD were 8.3% at the cephalad segment and 12.4% at the L5 S1 segment. In our study, the radiological and clinical survival rates were 92% and 88%, respectively, at the L5 S1 segment after 5 years. Ghiselli et al. 6) reported that the radiological survival rate was 90% for L4 5 fusion at 10 years after surgery. Other authors reported that among patients with L5 S1 involvement, only 3 5% needed to be operated on 6,12). However, the nonunion rate in the lumbosacral junction was 14.4% at 59 months, which was higher than the CASD and reoperation rate of the L5 S1 segment 11). Therefore, it is not necessary to additionally include the L5 S1 segment. Moreover, preservation of the L5 S1 segment reduces buttock stiffness and diffuses pressures concentrated on the cephalad adjacent segment to the caudad adjacent segment 14). Furthermore, fusion of the L5 S1 segment may involve longer operation, increased complications, subsequent degeneration of the sacroiliac joint, altered gait mechanics, and an increased pseudoarthrosis rate; this further supports the needlessness of including the L5 S1 segment 2). Ghiselli et al. 5) reported that reoperations were required in 16.5% of patients within 5 years and in 36.1% within 10 years, and that new diseases occurred in the adjacent level at an annual rate of 3.9%. Sears et al. 21) reported that 13% of patients required reoperations after 43 months from the initial surgery, and that new diseases were found in the adjacent sites at an annual rate of 2.2%. The prevalence for reoperation following L5 floating fusion at 10 years was 14.7%. In this study, 2.6% of patients with cephalad segment involvement and 6.3% of patients with L5 S1 segment involvement required reoperations within 5 years after surgery. This is partly because most of the patients in the study group had 1 2 level involvement, and since no patients underwent long-level fusion, ASD-related reoperations were required to a lesser extent. Numerous studies have investigated the risk factors for RASD, CASD, and reoperation. Age, disc and facet joint degeneration, and multiple levels are well-known factors 1,5,8,9,12,21). Among these factors that influence ASD, we found that factors affecting the cephalad and L5 S1 segments differ after L5 floating fusion. In our study, preoperative disc degeneration was the most significant factor for ASD at the cephalad segment with preoperative spinal stenosis at the L5 S1 segment. The present study has limitations. First, the study is retrospective, and the follow-up periods and evaluation time of the clinical outcomes were not consistent. Second, only 115 patients (48.7%) of 236 patients were followed up, and the mean follow-up period was 46 months, which is shorter than that in previous studies. Third, since the definitions of RASD and CASD were different depending on authors, it was difficult to make accurate comparisons with previous studies. Especially in cases involving clinical ASD, the diversity in treatment methods (i.e., medication and injection) and indication of surgery were difficult to define. Therefore, a long-term, randomized, prospective study on expanded groups of patients is warranted. CONCLUSION In L5 floating fusion, ASD at the L5 S1 and cephalad segments appear to have different characteristics. RASD was more common at the cephalad segment, and CASD was more common at the L5 S1 segment. Occurrences of spinal instability, spondylolisthesis, and back pain were the major symptoms at the cephalad segment, and preoperative disc degeneration was the most significant factor influencing the outcomes. However, disc degeneration and radiculopathy were the main symptoms at the L5 S1 segment, and the most significant factor was preoperative spinal stenosis. References 1. Ahn DK, Park HS, Choi DJ, Kim KS, Yang SJ : Survival and prognostic analysis of adjacent segments after spinal fusion. Clin Orthop Surg 2 : , Bridwell KH, Edwards CC 2nd, Lenke LG : The pros and cons to saving the L5-S1 motion segment in a long scoliosis fusion construct. Spine (Phila Pa 1976) 28 : S234-S242, Celestre PC, Montgomery SR, Kupperman AI, Aghdasi B, Inoue H, Wang JC : Lumbar clinical adjacent segment pathology : predilection for proximal levels. Spine (Phila Pa 1976) 39 : , Cheh G, Bridwell KH, Lenke LG, Buchowski JM, Daubs MD, Kim Y, et al. : Adjacent segment disease followinglumbar/thoracolumbar fusion with pedicle screw instrumentation : a minimum 5-year follow-up. Spine (Phila Pa 1976) 32 : , Ghiselli G, Wang JC, Bhatia NN, Hsu WK, Dawson EG : Adjacent segment degeneration in the lumbar spine. J Bone Joint Surg Am 86-A : , Ghiselli G, Wang JC, Hsu WK, Dawson EG : L5-S1 segment survivorship and clinical outcome analysis after L4-L5 isolated fusion. Spine (Phila Pa 1976) 28 : ; discussion 1280, Imagama S, Kawakami N, Matsubara Y, Kanemura T, Tsuji T, Ohara T : Preventive effect of artificial ligamentous stabilization on the upper adjacent segment impairment following posterior lumbar interbody fusion. Spine (Phila Pa 1976) 34 : , Kaito T, Hosono N, Mukai Y, Makino T, Fuji T, Yonenobu K : Induction of early degeneration of the adjacent segment after posterior lumbar in- 112
6 Adjacent Segment Degeneration YS Lee, et al. terbody fusion by excessive distraction of lumbar disc space. J Neurosurg Spine 12 : , Kim TH, Lee BH, Moon SH, Lee SH, Lee HM : Comparison of adjacent segment degeneration after successful posterolateral fusion with unilateral or bilateral pedicle screw instrumentation : a minimum 10-year follow-up. Spine J 13 : , Lawrence BD, Wang J, Arnold PM, Hermsmeyer J, Norvell DC, Brodke DS : Predicting the risk of adjacent segment pathology after lumbar fusion : a systematic review. Spine (Phila Pa 1976) 37 (22 Suppl) : S123- S132, Lee CS, Chung SS, Choi SW, Yu JW, Sohn MS : Critical length of fusion requiring additional fixation to prevent nonunion of the lumbosacral junction. Spine (Phila Pa 1976) 35 : E206-E211, Lee CS, Hwang CJ, Lee SW, Ahn YJ, Kim YT, Lee DH, et al. : Risk factors for adjacent segment disease after lumbar fusion. Eur Spine J 18 : , Leong JC, Luk KD, Chow DH, Woo CW : The biomechanical functions of the iliolumbar ligament in maintaining stability of the lumbosacral junction. Spine (Phila Pa 1976) 12 : , Liao JC, Chen WJ, Chen LH, Niu CC, Keorochana G : Surgical outcomes of degenerative spondylolisthesis with L5-S1 disc degeneration : comparison between lumbar floating fusion and lumbosacral fusion at a minimum 5-year follow-up. Spine (Phila Pa 1976) 36 : , Luk KD, Ho HC, Leong JC : The iliolumbar ligament. A study of its anatomy, development and clinical significance. J Bone Joint Surg Br 68 : , Miyasaka K, Ohmori K, Suzuki K, Inoue H : Radiographic analysis of lumbar motion in relation to lumbosacral stability. Investigation of moderate and maximum motion. Spine (Phila Pa 1976) 25 : , Ohmori K, Ishida Y, Takatsu T, Inoue H, Suzuki K : Vertebral slip in lumbar spondylolysis and spondylolisthesis. Long-term follow-up of 22 adult patients. J Bone Joint Surg Br 77 : , Park P, Garton HJ, Gala VC, Hoff JT, McGillicuddy JE : Adjacent segment disease after lumbar or lumbosacral fusion : review of the literature. Spine (Phila Pa 1976) 29 : , Pearcy M, Portek I, Shepherd J : Three-dimensional x-ray analysis of normal movement in the lumbar spine. Spine (Phila Pa 1976) 9 : , Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N : Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 26 : , Sears WR, Sergides IG, Kazemi N, Smith M, White GJ, Osburg B : Incidence and prevalence of surgery at segments adjacent to a previous posterior lumbar arthrodesis. Spine J 11 : 11-20, Tan Y, Aghdasi BG, Montgomery SR, Inoue H, Lu C, Wang JC : Kinetic magnetic resonance imaging analysis of lumbar segmental mobility in patients without significant spondylosis. Eur Spine J 21 : , Weishaupt D, Zanetti M, Boos N, Hodler J : MR imaging and CT in osteoarthritis of the lumbar facet joints. Skeletal Radiol 28 : , Whitecloud TS 3rd, Davis JM, Olive PM : Operative treatment of the degenerated segment adjacent to a lumbar fusion. Spine (Phila Pa 1976) 19 : ,
Spinal fusion has become a standard of care for numerous
 clinical article J Neurosurg Spine 25:46 5, 206 Risk of adjacent-segment disease requiring surgery after short lumbar fusion: results of the French Spine Surgery Society Series Caroline Scemama, MD, Baptiste
clinical article J Neurosurg Spine 25:46 5, 206 Risk of adjacent-segment disease requiring surgery after short lumbar fusion: results of the French Spine Surgery Society Series Caroline Scemama, MD, Baptiste
Spine and Fusion. Adjacent Segment Disease. 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D.
 Lumbar Posterior Hybrid Dynamic Stabilisation and Fusion Systems 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D. Spine and Fusion It has been more than a century since 1911 when Albee
Lumbar Posterior Hybrid Dynamic Stabilisation and Fusion Systems 36Ihsan SOLAROGLU M.D., M. Ozerk OKUTAN M.D., Gurdal NUSRAN M.D. Spine and Fusion It has been more than a century since 1911 when Albee
ASJ. Radiologic and Clinical Courses of Degenerative Lumbar Scoliosis (10 25 ) after a Short-Segment Fusion. Asian Spine Journal.
 Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Facet orientation in patients with lumbar degenerative spondylolisthesis
 35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
Association between bicortical screw fixation at upper instrumented vertebra and risk for upper instrumented vertebra fracture
 CLINICAL ARTICLE J Neurosurg Spine 26:638 644, 2017 Association between bicortical screw fixation at upper instrumented vertebra and risk for upper instrumented vertebra fracture Young-Seop Park, MD, 1
CLINICAL ARTICLE J Neurosurg Spine 26:638 644, 2017 Association between bicortical screw fixation at upper instrumented vertebra and risk for upper instrumented vertebra fracture Young-Seop Park, MD, 1
Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults Kosuke Sugiura, Toshinori Sakai, Fumitake Tezuka, Kazuta
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults Kosuke Sugiura, Toshinori Sakai, Fumitake Tezuka, Kazuta
Range of Motion According to the Fusion Level after Lumbar Spine Fusion: A Retrospective Study
 eissn2465-891x The Nerve.2018.4(2):55-59 The Nerve https://doi.org/10.21129/nerve.2018.4.2.55 CLINICAL ARTICLE www.thenerve.net Range of Motion According to the Fusion Level after Lumbar Spine Fusion:
eissn2465-891x The Nerve.2018.4(2):55-59 The Nerve https://doi.org/10.21129/nerve.2018.4.2.55 CLINICAL ARTICLE www.thenerve.net Range of Motion According to the Fusion Level after Lumbar Spine Fusion:
Two-year outcomes of transforaminal lumbar interbody fusion
 Journal of Orthopaedic Surgery 2011;19(2):135-40 Two-year outcomes of transforaminal lumbar interbody fusion Seng-Yew Poh, Wai-Mun Yue, Li-Tat John Chen, Chang-Ming Guo, William Yeo, Seang-Beng Tan Department
Journal of Orthopaedic Surgery 2011;19(2):135-40 Two-year outcomes of transforaminal lumbar interbody fusion Seng-Yew Poh, Wai-Mun Yue, Li-Tat John Chen, Chang-Ming Guo, William Yeo, Seang-Beng Tan Department
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Coflex TM for Lumbar Stenosis with
 Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions:
 Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra
 doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
Dingjun Hao, Baorong He, Liang Yan. Hong Hui Hospital, Xi an Jiaotong University College. of Medicine, Xi an, Shaanxi , China
 Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Clinical Features of Degenerative Scoliosis
 Clinical Features of Degenerative Scoliosis Yung Tae Kim, MD, Choon Sung Lee, MD, Jung Hwan Kim, MD*, Jong Min Kim, MD and Jai Hyung Park, MD Department of Orthopedic Surgery, Asan Medical Center, Ulsan
Clinical Features of Degenerative Scoliosis Yung Tae Kim, MD, Choon Sung Lee, MD, Jung Hwan Kim, MD*, Jong Min Kim, MD and Jai Hyung Park, MD Department of Orthopedic Surgery, Asan Medical Center, Ulsan
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Pasquale Donnarumma 1, Roberto Tarantino 1, Lorenzo Nigro 1, Marika Rullo 2, Domenico Messina 3, Daniele Diacinti 4, Roberto Delfini 1.
 Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
The Importance of Proximal Fusion Level Selection for Outcomes of Multi-Level Lumbar Posterolateral Fusion
 Original Article Clinics in Orthopedic Surgery 2015;7:77-84 http://dx.doi.org/10.4055/cios.2015.7.1.77 The Importance of Proximal Fusion Level Selection for Outcomes of Multi-Level Lumbar Posterolateral
Original Article Clinics in Orthopedic Surgery 2015;7:77-84 http://dx.doi.org/10.4055/cios.2015.7.1.77 The Importance of Proximal Fusion Level Selection for Outcomes of Multi-Level Lumbar Posterolateral
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late complications
 Int J Clin Exp Med 2015;8(4):5731-5738 www.ijcem.com /ISSN:1940-5901/IJCEM0006438 Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late
Int J Clin Exp Med 2015;8(4):5731-5738 www.ijcem.com /ISSN:1940-5901/IJCEM0006438 Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Haiting Wu 1, Qingjiang Pang 1 and Guoqiang Jiang 2. Clinical Report
 Clinical Report Medium-term effects of Dynesys dynamic stabilization versus posterior lumbar interbody fusion for treatment of multisegmental lumbar degenerative disease Journal of International Medical
Clinical Report Medium-term effects of Dynesys dynamic stabilization versus posterior lumbar interbody fusion for treatment of multisegmental lumbar degenerative disease Journal of International Medical
Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture: Severe Canal Compromise but Neurologically Intact Cases
 CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
Outcome of Two Fusion Methods In Isthmic and Degenerative Spondylolisthesis of the Lumbar Spine
 Outcome of Two Fusion Methods In Isthmic and Degenerative Spondylolisthesis of the Lumbar Spine Kyu Yeol Lee, MD, Sung Keun Sohn MD, Sung Wan Kim, MD, Sung Won Lee MD Department of Orthopaedic Surgery,
Outcome of Two Fusion Methods In Isthmic and Degenerative Spondylolisthesis of the Lumbar Spine Kyu Yeol Lee, MD, Sung Keun Sohn MD, Sung Wan Kim, MD, Sung Won Lee MD Department of Orthopaedic Surgery,
INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE.
 INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE. A PRELIMINARY REPORT F. POSTACCHINI, A. PALMESI LUMBAR VERTEBRAL INSTABILITY Still the subject of discussion Variously defined and interpreted Postacchini
INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE. A PRELIMINARY REPORT F. POSTACCHINI, A. PALMESI LUMBAR VERTEBRAL INSTABILITY Still the subject of discussion Variously defined and interpreted Postacchini
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis
 Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse of a Lumbar Spine Vertebral Body
 Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
ASJ. Outcome of Salvage Lumbar Fusion after Lumbar Arthroplasty. Asian Spine Journal. Introduction. Hussein Alahmadi, Harel Deutsch
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2014;8(1):13-18 Lumbar fusion http://dx.doi.org/10.4184/asj.2014.8.1.13 after lumbar arthroplasty 13 Outcome of Salvage Lumbar Fusion
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2014;8(1):13-18 Lumbar fusion http://dx.doi.org/10.4184/asj.2014.8.1.13 after lumbar arthroplasty 13 Outcome of Salvage Lumbar Fusion
VIPER PRIME System Cadaver Time Study
 VIPER PRIME System Cadaver Time Study White Paper August 24, 2017 1. INTRODUCTION Minimally invasive surgical techniques to perform spinal stabilization have gained popularity in recent years due to the
VIPER PRIME System Cadaver Time Study White Paper August 24, 2017 1. INTRODUCTION Minimally invasive surgical techniques to perform spinal stabilization have gained popularity in recent years due to the
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
ORIGINAL PAPER. Department of Orthopedic Surgery,Nagoya University Graduate School of Medicine,Nagoya,Japan 2
 Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_
 Orthopaedic Surgery (2009), Volume 1, No. 3, 176 183 ORIGINAL ARTICLE The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_030 176..183 Wei Liu MD,
Orthopaedic Surgery (2009), Volume 1, No. 3, 176 183 ORIGINAL ARTICLE The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_030 176..183 Wei Liu MD,
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis
 CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
Dynamic Radiographic Results of Different Semi-Rigid Fusion Devices for Degenerative Lumbar Spondylolisthesis: Dynamic Rod vs. Dynamic Screw Head
 DOI: 10.5137/1019-5149.JTN.9784-13.1 Received: 09.05.2013 / Accepted: 09.12.2013 Original Investigation Dynamic Radiographic Results of Different Semi-Rigid Fusion Devices for Degenerative Lumbar Spondylolisthesis:
DOI: 10.5137/1019-5149.JTN.9784-13.1 Received: 09.05.2013 / Accepted: 09.12.2013 Original Investigation Dynamic Radiographic Results of Different Semi-Rigid Fusion Devices for Degenerative Lumbar Spondylolisthesis:
Outcomes in Adult Scoliosis Patients Who Undergo Spinal Fusion Stopping at L5 Compared with Extension to the Sacrum
 96 Systematic Review Outcomes in Adult Scoliosis Patients Who Undergo Spinal Fusion Stopping at L5 Compared with Extension to the Sacrum Zeeshan M. Sardar 1 Jean A. Ouellet 1 Dena J. Fischer 2 Andrea C.
96 Systematic Review Outcomes in Adult Scoliosis Patients Who Undergo Spinal Fusion Stopping at L5 Compared with Extension to the Sacrum Zeeshan M. Sardar 1 Jean A. Ouellet 1 Dena J. Fischer 2 Andrea C.
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Long lumbar instrumented fusions have been described
 SPINE Volume 37, Number 16, pp 1407 1414 2012, Lippincott Williams & Wilkins SURGERY Upper Instrumented Vertebral Fractures in Long Lumbar Fusions What Are the Associated Risk Factors? Stephen J. Lewis,
SPINE Volume 37, Number 16, pp 1407 1414 2012, Lippincott Williams & Wilkins SURGERY Upper Instrumented Vertebral Fractures in Long Lumbar Fusions What Are the Associated Risk Factors? Stephen J. Lewis,
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis
 Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Int J Clin Exp Med 2015;8(4): /ISSN: /IJCEM Xiaokang Liu, Yingjie Liu, Xiaofeng Lian, Jianguang Xu
 Int J Clin Exp Med 2015;8(4):6097-6102 www.ijcem.com /ISSN:1940-5901/IJCEM0006352 Original Article Magnetic resonance imaging on disc degeneration changes after implantation of an interspinous spacer and
Int J Clin Exp Med 2015;8(4):6097-6102 www.ijcem.com /ISSN:1940-5901/IJCEM0006352 Original Article Magnetic resonance imaging on disc degeneration changes after implantation of an interspinous spacer and
Radiographic and Clinical Outcomes of Robot-Assisted Posterior Pedicle Screw Fixation: Two-Year Results from a Randomized Controlled Trial
 Original Article Yonsei Med J 2018 May;59(3):438-444 pissn: 0513-5796 eissn: 1976-2437 Radiographic and Clinical Outcomes of Robot-Assisted Posterior Pedicle Screw Fixation: Two-Year Results from a Randomized
Original Article Yonsei Med J 2018 May;59(3):438-444 pissn: 0513-5796 eissn: 1976-2437 Radiographic and Clinical Outcomes of Robot-Assisted Posterior Pedicle Screw Fixation: Two-Year Results from a Randomized
Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium
 Original Study Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium Tatsuya Yasuda, Tomohiko Hasegawa, Yu Yamato, Sho Kobayashi, Daisuke Togawa, Shin
Original Study Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium Tatsuya Yasuda, Tomohiko Hasegawa, Yu Yamato, Sho Kobayashi, Daisuke Togawa, Shin
ASJ. Asian Spine Journal. Seung-Pyo Suh 1, Young-Hoon Jo 2, Hae Won Jeong 2, Won Rak Choi 2, Chang-Nam Kang 2
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2017;11(3):463-471 Pseudarthrosis https://doi.org/10.4184/asj.2017.11.3.463 vs. adjacent segment disease 463 Outcomes of Revision Surgery
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2017;11(3):463-471 Pseudarthrosis https://doi.org/10.4184/asj.2017.11.3.463 vs. adjacent segment disease 463 Outcomes of Revision Surgery
Minimally Invasive Treatment (XLIF) of Adjacent Segment Disease after prior Lumbar Fusions
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 3 Number 4 Minimally Invasive Treatment (XLIF) of Adjacent Segment Disease after prior Lumbar Fusions W Rodgers, C Cox, E Gerber
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 3 Number 4 Minimally Invasive Treatment (XLIF) of Adjacent Segment Disease after prior Lumbar Fusions W Rodgers, C Cox, E Gerber
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Bone Cement-Augmented Percutaneous Short Segment Fixation : An Effective Treatment for Kummell s Disease?
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.1.54 J Korean Neurosurg Soc 58 (1) : 54-59, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.1.54 J Korean Neurosurg Soc 58 (1) : 54-59, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity: Technical Note Involving 13 Cases
 Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
Does Disc Space Height of Fused Segment Affect Adjacent Disc Degeneration in Anterior Lumbar Interbody Fusion? A Radiological Study
 Iranian Red Crescent Medical Journal ORIGINAL ARTICLE Does Disc Space Height of Fused Segment Affect Adjacent Disc Degeneration in Anterior Lumbar Interbody Fusion? A Radiological Study Sh Tang 1 *, W
Iranian Red Crescent Medical Journal ORIGINAL ARTICLE Does Disc Space Height of Fused Segment Affect Adjacent Disc Degeneration in Anterior Lumbar Interbody Fusion? A Radiological Study Sh Tang 1 *, W
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Adjacent segment disease after anterior cervical discectomy and fusion
 Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
The Kickstand Rod technique for correction of coronal imbalance in patients with adult spinal deformity: theory and technical considerations
 Case Report The Kickstand Rod technique for correction of coronal imbalance in patients with adult spinal deformity: theory and technical considerations Melvin C. Makhni 1, Meghan Cerpa 2, James D. Lin
Case Report The Kickstand Rod technique for correction of coronal imbalance in patients with adult spinal deformity: theory and technical considerations Melvin C. Makhni 1, Meghan Cerpa 2, James D. Lin
High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative spondylolisthesis
 Eur Spine J (2008) 17:188 192 DOI 10.1007/s00586-007-0492-x ORIGINAL ARTICLE High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative
Eur Spine J (2008) 17:188 192 DOI 10.1007/s00586-007-0492-x ORIGINAL ARTICLE High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative
2013 UCSF SPINE SYMPOSIUM RICHARD DEYO, MD MPH MICHAEL GROFF, MD
 2013 UCSF SPINE SYMPOSIUM RICHARD DEYO, MD MPH MICHAEL GROFF, MD OHSU Professor and the Kaiser- Permanente Endowed Professor of Evidence-Based Medicine in the Department of Family Medicine at Oregon Health
2013 UCSF SPINE SYMPOSIUM RICHARD DEYO, MD MPH MICHAEL GROFF, MD OHSU Professor and the Kaiser- Permanente Endowed Professor of Evidence-Based Medicine in the Department of Family Medicine at Oregon Health
The ABC s of LUMBAR SPINE DISEASE
 The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Outcome of Surgical Treatment of AO Type C Pelvic Ring Injury
 ORIGINAL ARTICLE Hip Pelvis 26(4): 269-274, 2014 http://dx.doi.org/10.5371/hp.2014.26.4.269 Print ISSN 2287-3260 Online ISSN 2287-3279 Outcome of Surgical Treatment of AO Type C Pelvic Ring Injury Do Hyeon
ORIGINAL ARTICLE Hip Pelvis 26(4): 269-274, 2014 http://dx.doi.org/10.5371/hp.2014.26.4.269 Print ISSN 2287-3260 Online ISSN 2287-3279 Outcome of Surgical Treatment of AO Type C Pelvic Ring Injury Do Hyeon
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Lumbar Disc Herniation Presented with Contralateral Symptoms
 Clinical Article J Korean Neurosurg Soc 60 (2) : 220-224, 2017 https://doi.org/10.3340/jkns.2016.1010.015 pissn 2005-3711 eissn 1598-7876 Lumbar Disc Herniation Presented with Contralateral Symptoms Pius
Clinical Article J Korean Neurosurg Soc 60 (2) : 220-224, 2017 https://doi.org/10.3340/jkns.2016.1010.015 pissn 2005-3711 eissn 1598-7876 Lumbar Disc Herniation Presented with Contralateral Symptoms Pius
Two Consecutive Levels of Unilateral Cervical Spondylolysis on Opposite Sides 두개의연속된척추에서반대쪽편측에발생한경추척추분리증
 Case Report pissn 1738-2637 / eissn 2288-2928 http://dx.doi.org/10.3348/jksr.2015.73.3.181 Two Consecutive Levels of Unilateral Cervical Spondylolysis on Opposite Sides 두개의연속된척추에서반대쪽편측에발생한경추척추분리증 Kyeong
Case Report pissn 1738-2637 / eissn 2288-2928 http://dx.doi.org/10.3348/jksr.2015.73.3.181 Two Consecutive Levels of Unilateral Cervical Spondylolysis on Opposite Sides 두개의연속된척추에서반대쪽편측에발생한경추척추분리증 Kyeong
Usefulness of Simple Rod Rotation to Correct Curve of Adolescent Idiopathic Scoliosis
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.6.534 J Korean Neurosurg Soc 58 (6) : 534-538, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.6.534 J Korean Neurosurg Soc 58 (6) : 534-538, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Is unilateral pedicle screw fixation superior than bilateral pedicle screw fixation for lumbar degenerative diseases: a meta-analysis
 Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Positional Magnetic Resonance Imaging. Description
 Subject: Positional Magnetic Resonance Imaging Page: 1 of 6 Last Review Status/Date: June 2015 Positional Magnetic Resonance Imaging Description Positional magnetic resonance imaging (MRI) allows imaging
Subject: Positional Magnetic Resonance Imaging Page: 1 of 6 Last Review Status/Date: June 2015 Positional Magnetic Resonance Imaging Description Positional magnetic resonance imaging (MRI) allows imaging
Static and dynamic cervical MRI: two useful exams in cervical myelopathy
 Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Lumbar Disc Degeneration Is an Equally Important Risk Factor as Lumbar Fusion for Causing Adjacent Segment Disc Disease
 Lumbar Disc Degeneration Is an Equally Important Risk Factor as Lumbar Fusion for Causing Adjacent Segment Disc Disease Raghu N. Natarajan, Gunnar B.J. Andersson Department of Orthopedic Surgery, Rush
Lumbar Disc Degeneration Is an Equally Important Risk Factor as Lumbar Fusion for Causing Adjacent Segment Disc Disease Raghu N. Natarajan, Gunnar B.J. Andersson Department of Orthopedic Surgery, Rush
ASJ. Magnification Error in Digital Radiographs of the Cervical Spine Against Magnetic Resonance Imaging Measurements. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Spondylolysis is a unilateral or bilateral defect in the. Spondylolysis outcomes in adolescents after direct screw repair of the pars interarticularis
 J Neurosurg Spine 21:329 333, 2014 AANS, 2014 Spondylolysis outcomes in adolescents after direct screw repair of the pars interarticularis Clinical article Laura A. Snyder, M.D., 1 Harry Shufflebarger,
J Neurosurg Spine 21:329 333, 2014 AANS, 2014 Spondylolysis outcomes in adolescents after direct screw repair of the pars interarticularis Clinical article Laura A. Snyder, M.D., 1 Harry Shufflebarger,
A Novel Classification and Minimally Invasive Treatment of Degenerative Lumbar Spinal Stenosis
 DOI: 10.5137/1019-5149.JTN.9173-13.2 Received: 28.08.2013 / Accepted: 11.02.2014 Original Investigation A Novel Classification and Minimally Invasive Treatment of Degenerative Lumbar Spinal Stenosis Guangfei
DOI: 10.5137/1019-5149.JTN.9173-13.2 Received: 28.08.2013 / Accepted: 11.02.2014 Original Investigation A Novel Classification and Minimally Invasive Treatment of Degenerative Lumbar Spinal Stenosis Guangfei
Dept. of Orthopaedic Surgery, Wakayama Medical University, Wakayama, Japan. Brigham and Women s Hospital, Harvard Medical School, Boston, MA, USA.
 Microendoscopic Decompression for Lumbar Spinal Stenosis with Degenerative Spondylolisthesis: the influence of spondylolisthesis stage (disc height and static and dynamic translation) on clinical outcomes
Microendoscopic Decompression for Lumbar Spinal Stenosis with Degenerative Spondylolisthesis: the influence of spondylolisthesis stage (disc height and static and dynamic translation) on clinical outcomes
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report
 Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Original Policy Date
 MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic Spondylolisthesis
 Case Reports in Orthopedics Volume 2015, Article ID 426940, 4 pages http://dx.doi.org/10.1155/2015/426940 Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic
Case Reports in Orthopedics Volume 2015, Article ID 426940, 4 pages http://dx.doi.org/10.1155/2015/426940 Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic
vertebra associated with dura) ectasia in
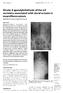 e287 Case Report Grade 4 spondylolisthesis of the L5 vertebra associated with dura) ectasia in neurofibromatosis Modi H N, Srinivasalu S, Suh S W, Yang J H ABSTRACT Spondylolisthesis associated with neurofibromatosis
e287 Case Report Grade 4 spondylolisthesis of the L5 vertebra associated with dura) ectasia in neurofibromatosis Modi H N, Srinivasalu S, Suh S W, Yang J H ABSTRACT Spondylolisthesis associated with neurofibromatosis
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
There is No Remarkable Difference Between Pedicle Screw and Hybrid Construct in the Correction of Lenke Type-1 Curves
 DOI: 10.5137/1019-5149.JTN.20522-17.1 Received: 11.04.2017 / Accepted: 12.07.2017 Published Online: 21.09.2017 Original Investigation There is No Remarkable Difference Between Pedicle Screw and Hybrid
DOI: 10.5137/1019-5149.JTN.20522-17.1 Received: 11.04.2017 / Accepted: 12.07.2017 Published Online: 21.09.2017 Original Investigation There is No Remarkable Difference Between Pedicle Screw and Hybrid
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases-
 Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
A Measure to Avoid Pleura Injuries in XLIF at Upper Lumbar Levels
 A Measure to Avoid Pleura Injuries in XLIF at Upper Lumbar Levels Takao Nakajima 1, Yong Kim 2, Masabumi Miyamoto 3 Dept. of Orthop. Surg., Nippon Medical School, Chiba Hokusoh Hospital 1 Dept. of Orthop.
A Measure to Avoid Pleura Injuries in XLIF at Upper Lumbar Levels Takao Nakajima 1, Yong Kim 2, Masabumi Miyamoto 3 Dept. of Orthop. Surg., Nippon Medical School, Chiba Hokusoh Hospital 1 Dept. of Orthop.
