Brief Research Report Ultrasound-Guided Cervical Nerve Root Block: Spread of Solution and Clinical Effectpme_
|
|
|
- Isaac Paul
- 5 years ago
- Views:
Transcription
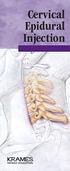
1 Pain Medicine 2011; 12: Wiley Periodicals, Inc. Brief Research Report Ultrasound-Guided Cervical Nerve Root Block: Spread of Solution and Clinical Effectpme_ Masanori Yamauchi, MD, PhD,* Daisuke Suzuki, PhD, Tomohisa Niiya, MD, PhD,* Hironori Honma, MD,* Nobuko Tachibana, MD,* Akihiko Watanabe, MD, PhD,* Mineko Fujimiya, MD, PhD, and Michiaki Yamakage, MD, PhD* Departments of *Anesthesiology and Anatomy, Sapporo Medical University School of Medicine, Sapporo, Japan Reprint requests to: Masanori Yamauchi, MD, PhD, Department of Anesthesiology, Sapporo Medical University School of Medicine, S1 W16, chuo-ku, Sapporo, Hokkaido , Japan. Tel: ; Fax: ; Disclosure Financial support was provided solely from institutional and departmental sources (Sapporo Medical University School of Medicine) for this study. None of the authors has any conflict of interest. We have not presented this study in any meetings. Abstract Objectives. We investigated the clinical effects and accuracy of ultrasound-guided cervical nerve root block. Additionally, spinal level and spread of injected solution were confirmed by anatomic dissection of fresh cadavers. Design Setting, Patients, and Interventions. Twelve patients diagnosed with mono-radiculopathy between C5 7 underwent ultrasound-guided nerve root block. An insulated needle was advanced with an in-plane approach using nerve stimulation and 2 ml of 0.375% ropivacaine with 4 mg of dexamethasone was injected using nerve stimulation. Ultrasound-guided C5 7 nerve root block was also performed in ten fresh cadavers. Blue dye (2 ml) was injected onto each nerve root and anatomic dissection was performed to confirm the exact spinal level and spread pattern of the dye. Results. Pain score before the procedure (65 [46 80], median [interquartile range]) was decreased to 25 [3 31] at 24 hours (P = 0.003) and 40 [28 66] at 30 days (P = 0.02) after the root block. Obvious side effects were not seen. All target nerve roots in patients and cadavers were correctly identified by ultrasound imaging. The needle tip did not reach the pedicle of the vertebral arch in the anteroposterior view of fluoroscopy, and spread pattern of contrast medium was extraforaminal and extraneural. Conclusions. This study suggests that injected solution by ultrasound-guided cervical nerve root block mainly spreads to the extraforaminal direction compared with conventional fluoroscopic technique. Therefore, present clinical study involves possibility of safer selective nerve root block with sufficient analgesic effects by ultrasound guidance, despite the absence of intraforaminal epidural spread of solution. Key Words. Cervical; Interventional; Nerve Block; Radiculopathy; Ultrasound Introduction Selective cervical nerve root block is widely performed to diagnose the spinal level of cervical radiculopathy and relieve radicular pain, headache, shoulder stiffness, or extremity pain [1 3]. Various complications associated with cervical nerve root block have been reported [4,5]. Intravascular injection may produce serious complications including central nervous system infarction and bleeding [6,7]. Fluoroscopic guidance is usually utilized for selective cervical nerve root block, and computed tomography (CT) [8] or magnetic resonance imaging guidance [9] is also employed in difficult cases. Although cervical nerve roots and vessels are identified more clearly by CT guidance than by fluoroscopy, cerebellar infarction and brainstem infarction have been reported even under CT guidance [10]. Recently, it has been reported that ultrasound-guided selective cervical nerve root block facilitated confirmation of nerves, vessels, needles, and injected solutions, and it is expected that a more appropriate procedure can be performed than that by fluoroscopic guidance alone [11 13]. However, there have not been many reports on the effects and features of ultrasound-guided selective cervical nerve root block, and the relation between needle tip position and spread pattern of local anesthetic is not known. In the present study, the authors clinically investigated the efficacy and accuracy of ultrasound-guided cervical nerve root block using nerve stimulation and fluoroscopy. The accuracy of determination of spinal level and spread of the injected solution was confirmed by dissection of fresh cadavers in an anatomic study. We 1190
2 Ultrasound-Guided Cervical Root Block investigated how local anesthetics spread by ultrasoundguided cervical nerve root block comparing with the conventional fluoroscopic technique, and that clinical effects and facility of the ultrasound-guided technique was also evaluated. Methods Clinical Study The protocol of this study was approved by the ethics committee of our hospital and written informed consent was obtained from all patients after receiving complete information prior to therapy. Twelve patients who were diagnosed with mono-cervical radiculopathy by history, distribution of paresthesia, physical examination, irregular alignment in cervical X-ray imaging and nerve root compression in magnetic resonance imaging were scheduled to undergo ultrasound-guided cervical nerve root block. Patients eligible for this prospective study were suffering from radicular pain or numbness between C5 7 areas and their symptoms had persisted for at least 2 months despite appropriate medication and conservative treatment. Patients were excluded if they met any of the following criteria: contraindications to regional block technique, cervical radiculopathy at multiple levels, age <18 or >80 years, pregnancy, and inability to comprehend pain scales. During the procedure, intravenous midazolam (2 mg) was administered as a requirement for patients sedation. The interventional procedure was performed by MaY under ultrasound guidance using a modified Narouze et al. technique [12]. Briefly, patients were placed supine on the radiographic table with the chin deviated approximately 0 30 away from the side, and a soft mat was inserted between the ipsilateral upper body and the table. The angle of the C-arm was adjusted to obtain the proper anteroposterior view of the cervical spine. First, C5 7 nerve roots were identified in ultrasound imaging (Micro- Maxx, SonoSite, Inc., Bothwell, WA, USA) by the shape of the transverse process; the C5th and C6th transverse processes both have obvious anterior and posterior tubercles, as opposed to the C7th transverse process, which has a rudimentary anterior tubercle and a prominent posterior tubercle [11,12]. Thus, we could define the C7 and C6 nerve roots at first, and then the C5 nerve root can be easily identified by moving the transducer cranially. The skin was prepared under strictly aseptic conditions with iodinated alcohol, and the ultrasound probe (HFL38, 13 6 MHz, 38-mm linear array, SonoSite, Inc.) was aseptically covered. Then a short axial view of the target nerve root surrounded by the anterior and posterior tubercles of the transverse process was visualized in ultrasound imaging in confirming location of vessels around the nerve root by color Doppler mode, and a 50-mm 22-G insulated needle (Hakko, Co., Tokyo, Japan) was gently introduced by an in-plane approach toward the posterior edge of the nerve root located at the inside of the posterior tubercle (Figure 1). The needle was connected to a constant voltage nerve stimulator (Stimuplex DIG, B-Braun/ Figure 1 Axial ultrasound imaging of C7 nerve root block (A), the fluoroscopic imaging during the block (B), and spread of contrast medium (C). C7 nerve root (C7) was partially surrounded by posterior tubercles (PT) of the transverse process, and a needle tip was introduced between C7 and PT. Contrast medium was spread to the peripheral direction and did not reach the epidural space (C). McGaw Medical, Bethlehem, PA, USA) that was set at 2 Hz with pulse width of 100 ms and a current of 0.8 ma. The needle position was considered acceptable if an evoked pickling paresthesia and motor response as twitch muscle contraction in the affected region was elicited between ma. After careful aspiration to exclude blood or cerebrospinal fluid, 0.5 ml of physiological saline was injected and the spread was confirmed by ultrasound imaging. Needle position was verified and the spread of 2 ml of contrast medium was examined with an anteroposterior fluoroscopic view and, if necessary, the needle position was adjusted (Figure 1). After careful aspiration, a total of 2 ml of a mixture of 0.375% ropivacaine and dexamethasone (4 mg) was slowly injected. All injections were performed under real-time ultrasound guidance. Finally, the needle was removed and light pressure was applied on the injection site for 2 minutes. Sensory and motor function scores at the dermatome where cervical nerve roots were blocked were assessed at 2, 6, and 1191
3 Yamauchi et al. 24 hours after the nerve block (0 = complete block, 1 = severe intense block, 2 = mild block, 3 = normal function). The next morning, all patients were discharged after confirming no complications or negative side effects and were instructed to continue their medication. Side effects and worsening of the symptoms of radiculopathy were recorded. Intensity of radicular pain was scored by the patient on a visual scale from 0 (no pain) to 100 mm (maximum intensity). In order to normalize the data, the percentages of pain relief given in the response to treatment were calculated using the following formula: ( pretreatment score posttreatment score) 100 pretreatment score The pain score was evaluated by the referring physician at 2, 6, and 24 hours while being in the hospital and 7 and 30 days in the ambulatory unit. Data were analyzed by Wilcoxon signed-rank test for paired values. A value of P < 0.05 was considered significant. The results are expressed as means standard deviation or median values [interquartile range]. Cadaver Study The protocol of this study was approved by the university s ethics committee, and fresh cadavers obtained with written informed consent prior to death were used. Ultrasound-guided cervical selective nerve block was performed in 10 randomly selected cadaveric specimens. We did not use nerve stimulation and fluoroscopic confirmation in the cadaver study. Specimens were kept in a freezer at -20 C and then thawed at room temperature 24 hours prior to the experiment. The experiment was performed at room temperature (22 C). C5 and C7 root block was performed at the same side and C6 root block was performed at the opposite side. Right C5 and C7 block and left C6 block were performed in the first cadaver. The right and left sides were changed in the next cadaver, and the blocks were alternately performed for all cadavers. After a 50-mm 22-G insulated needle had been advanced to the proper position under ultrasound guidance, 2 ml of blue dye was injected adjacent to each nerve root. Anatomic dissection around C5 7 and the cervical plexus was performed to confirm the exact spinal level and spread pattern of the dye. Results Clinical Study Twelve patients (seven men and five women) were enrolled in this study (Table 1), and no patients required sedation during procedure. The spinal levels of all nerve roots were correctly identified by ultrasound imaging, and there was no need to alter the needle position after fluoroscopic confirmation in any of the cases. Needle tip position was located at the inside of the transverse process of the target spinal level, not too medially into the foramen, in all patients. The needle tip did not reach the pedicle of the Table 1 vertebral arch in the anteroposterior view of fluoroscopy. Contrast medium clearly spread along the nerve roots as an extraneural pattern in 10 patients, spread along the scalene muscle like a myogram in two patients, and did not spread into the epidural space in all patients. An adequate response was evoked by nerve stimulation before injection of solution in all patients. Sensory and motor function scores were 0 or 1 for a few hours, and the motor functions had completely recovered to the preblocked level on the next day in all cases (Table 2). Pain score was significantly decreased almost half of the control state (65 mm) for 7 days (P < 0.01) and maintained about 40 mm for 30 days after the block (P < 0.05). Percentages of pain relief were also improved only 13% at 30 days (P < 0.05, Table 3). Side effects, such as intravascular injection revealed by fluoroscopy, inappropriate region block, respiratory or cardiovascular depression, local anesthetic toxicity, bruising and bleeding or hematoma at the injection site, worsening of symptoms, and other abnormalities were not seen. Cadaver Study Age of cadavers ranged years. All nerve roots were clearly visible in ultrasound imaging (Figure 2). Anatomic dissection proved that ultrasound identification of the spinal level was correct and the injected blue dye spread surrounding the nerve roots was located outside of the intervertebral foramen. There was no failed injection case. Discussion Demographic data N (m/f) 12 (7/5) Age (years) Body height (cm) Body weight (kg) Site of radiculopathy C5 4 cases C6 4 cases C7 4 cases Mean values standard deviation. The present clinical and anatomic studies showed that real-time ultrasound guidance can perform accurate and Table 2 Sensory and motor function scores after the nerve block 2 Hours 6 Hours 24 Hours Sensory score 0 (0 1.0) 2 ( ) 3 ( ) Motor function score 0 (0 1.0) 2 ( ) 3 ( ) Median values (interquartile range). 1192
4 Ultrasound-Guided Cervical Root Block Table 3 Results Pain score Pre 65 (46 80) 2 hours 0 (0 8) hours 0 (0 10) hours 25 (3 31) days 31 (12 38) days 40 (28 66) 0.02 Pain relief score (%) Pre 0 (0) 2 hours 100 (92 100) hours 100 (84 100) hours 59 (43 96) days 53 (10 80) days 13 (0 52) 0.02 Median values (interquartile range). Pre = precervical root block. P values were compared with Pre. safe cervical nerve root block, and that this technique provides lasting analgesic effect for 1 month. Therefore, ultrasound-guided cervical nerve root block could avoid intravascular or intraneuronal injection. However, the ultrasound-guided technique was different from conventional fluoroscopic technique; ultrasound guidance caused peripheral side nerve root injection. These findings indicate that ultrasound-guided cervical nerve root block is a feasible procedure compared with the fluoroscopic technique. Although fluoroscopically guided cervical nerve root block is widely known as a standard procedure, unintentional intravascular injection can cause fatal complications such as vertebral artery dissection or brain and spinal cord infarction [6,7]. The rate of complications from cervical nerve root block has been reported to be % [14,15], and most of the severe complications were caused by intravascular injection of a steroid or local anesthetic [16,17]. Intravascular puncture and intraneural injection may cause severe and irreversible nerve injury. Nakagawa et al. [11] and Narouze et al. [12] reported that ultrasound guidance enabled accurate and safe needle placement by identification of the C3 7 transverse process in the same manner as that in the present study. Both reports emphasized that ultrasound imaging could visualize the transverse process with nerve roots and vessels and would enable safer cervical nerve root block. The ultrasound technique can avoid radiation exposure and allergic reaction by the contrast medium. Elicited continuous twitch response can identify the needle position, and it is widely known that the needle tip-nerve distance can be roughly estimated by a stimulating current; over 0.8 ma indicates too far, ma indicates appropriate distance, and 0.5 ma or less indicates too near or position [18]. Thus, in addition to ultrasound confirmation of the needle tip, use of fluoroscopy and/or nerve stimulation would increase the safety margin of cervical nerve P root block in a difficult case. Although a needle tip position and spread of solution were more peripheral than usual conventional technique, hydrostatic pressure and osmotic effects lead to absorb the solution into the nerve fiber and intracellular fluid flow may spread local anesthetic and steroid toward the central lesion where compression or inflammation of the nerve root would occur. The limitations of this study should be considered. First, clinical effects of this procedure are still uncertain. The needle tip position advanced by ultrasound guidance would be relatively peripheral compared with that using the fluoroscopic technique. This extraforaminal injection is expected to reduce fatal side effects, and most patients in this study were satisfied with the effects and procedure. However, this ultrasound-guided technique does not enable steroid injection or pulsed radiofrequency treatment around the dorsal root ganglion, which may have advantages in long-term improvement of radicular pain [19]. Transforaminal epidural block is expected to improve radicular pain more effectively and for longer time than selective nerve root block [20]. Further prospective blind studies should be performed to assess the long-term effects of ultrasound-guided selective nerve root block compared with the long-term effects of other techniques. Another limitation of this study is that it is still uncertain whether intravascular injection can be avoided without fluoroscopy. Ultrasound-guided cervical nerve block enables confirmation of the vertebral and thyroid artery and avoidance of needle tip insertion into the arteries. Narouze et al. [12] showed that critical vessels could be visualized with high-resolution ultrasound system. To decrease risk of intravascular administration, test injection of the physiological saline, use of high-resolution linear ultrasound machine, or confirmation by Doppler mode is needed. The present Figure 2 Ultrasound imaging of C7 nerve root block in cadaver study. C7 nerve root (C7) was appeared from posterior tubercles (PT) of the transverse process. A needle (arrow head) was manipulated till touching the C
5 Yamauchi et al. cadaver study also has limitations. Although some studies have proved similar connective tissue, muscle and nerve characters of a fresh cadaver as in the in vivo body [21,22], spread of the injected solution may differ from that in clinical treatment. Detection of vessels by color Doppler and observation of physiological response are also impossible in a cadaver study. In this study, we kept specimens at room temperature after thawing for longer than 6 hours, and the influence of nerve, muscle and connective tissue characters was considered to be small [23]. Further study is needed to prove the relation between injected volume and spread around the nerve root. The present clinical study suggests that ultrasoundguided cervical nerve root block may enable safe selective nerve root block by identifying the correct spinal level and vessels. Therefore, despite the absence of intraforaminal epidural spread, this technique resulted in sufficient analgesic effect for radicular pain. The fresh cadaver study also showed that injected solution mainly spreads to the extraforaminal direction and that ultrasound-guided cervical nerve root block could avoid intraforaminal epidural block. Our results indicate that selective cervical nerve root block has the possibility to shift from fluoroscopic guidance to ultrasound guidance for its feasibility and portability. This study suggests that injected solution by ultrasoundguided cervical nerve root block mainly spreads to the extraforaminal direction compared with conventional fluoroscopic technique. Therefore, present clinical study involves the possibility that this ultrasound-guided technique would perform safer selective nerve root block with sufficient analgesic effects, despite the absence of intraforaminal epidural spread of solution. Further study with large number samples may shift technique of selective cervical nerve root block from fluoroscopic guidance to ultrasound guidance for its feasibility and portability. Acknowledgments We acknowledge Dr Mitsuhiro Aoki, Associate Professor in Department of Physical Therapy, School of Health Sciences, Sapporo Medical University, who provided invaluable assistance in performing this trial. References 1 Razzaq AA, O Brien D, Mathew B, Bartlett R, Taylor D. Efficacy and durability of fluoroscopically guided cervical nerve root block. Br J Neurosurg 2007;21: Martin DC, Willis ML, Mullinax LA, et al. Pulsed radiofrequency application in the treatment of chronic pain. Pain Pract 2007;7: Anderberg L, Annertz M, Rydholm U, Brandt L, Säveland H. Selective diagnostic nerve root block for the evaluation of radicular pain in the multilevel degenerated cervical spine. Eur Spine J 2006;15: Pobiel RS, Schellhas KP, Eklund JA, et al. Selective cervical nerve root blockade: Prospective study of immediate and longer term complications. Am J Neuroradiol 2009;30: Schellhas KP, Pollei SR, Johnson BA, et al. Selective cervical nerve root blockade: Experience with a safe and reliable technique using an anterolateral approach for needle placement. Am J Neuroradiol 2007;28: Wallace MA, Fukui MB, Williams RL, Ku A, Baghai P. Complications of cervical selective nerve root blocks performed with fluoroscopic guidance. Am J Roentgenol 2007;188: Brouwers PJ, Kottink EJ, Simon MA, Prevo RL. A cervical anterior spinal artery syndrome after diagnostic blockade of the right C6-nerve root. Pain 2001;91: Wagner AL. CT fluoroscopic-guided cervical nerve root blocks. Am J Neuroradiol 2005;26: Strobel K, Pfirrmann CW, Schmid M, et al. Cervical nerve root blocks: Indications and role of MR imaging. Radiology 2004;233: Suresh S, Berman J, Connell DA. Cerebellar and brainstem infarction as a complication of CT-guided transforaminal cervical nerve root block. Skeletal Radiol 2007;36: Nakagawa M, Shinbori H, Ohseto K. Ultrasoundguided and fluoroscopy-assisted selective cervical nerve root block. Masui 2009;58: Narouze SN, Vydyanathan A, Kapural L, Sessler DI, Mekhail N. Ultrasound-guided cervical selective nerve root block: A fluoroscopy-controlled feasibility study. Reg Anesth Pain Med 2009;34: Martinoli C, Bianchi S, Santacroce E, et al. Brachial plexus sonography: A technique for assessing the root level. AJR Am J Roentgenol 2002;179: Ma DJ, Gilula LA, Riew KD. Complications of fluoroscopically guided extraforaminal cervical nerve blocks. An analysis of 1036 injections. J Bone Joint Surg Am 2005;87: Furman MB, Giovanniello MT, O Brien EM. Incidence of intravascular penetration in transforaminal cervical epidural steroid injections. Spine 2003;28: Huntoon MA. Anatomy of the cervical intervertebral foramina: Vulnerable arteries and ischemic neurologic 1194
6 Ultrasound-Guided Cervical Root Block injuries after transforaminal epidural injections. Pain 2005;117: Baker R, Dreyfuss P, Mercer S, Bogduk N. Cervical transforaminal injection of corticosteroids into a radicular artery: A possible mechanism for spinal cord injury. Pain 2003;103: Quinn SF, Murtagh RC. T-guided nerve root sleeve block and ablation. AJR Am J Roentgenol 1988;151: Bigeleisen PE, Moayeri N, Groen GJ. Extraneural versus stimulation thresholds during ultrasoundguided supraclavicular block. Anesthesiology 2009;110: Rathmell JP, Aprill C, Bogduk N. Cervical transforaminal injection of steroids. Anesthesiology 2004;100: Inufusa A, An HS, Lim TH, et al. Anatomic changes of the spinal canal and intervertebral foramen associated with flexion-extension movement. Spine 1996;21: Farmer JC, Wisneski RJ. Cervical spine nerve root compression. An analysis of neuroforaminal pressures with varying head and arm positions. Spine 1994;19: Muraki T, Aoki M, Izumi T, et al. Lengthening of the pectoralis minor muscle during passive shoulder motions and stretching techniques: A cadaveric biomechanical study. Phys Ther 2009;89:
Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern?
 Pain Medicine 2016; 17: 1978 1984 doi: 10.1093/pm/pnw027 SPINE SECTION Original Research Article Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern? Seok Kang, MD, Seung
Pain Medicine 2016; 17: 1978 1984 doi: 10.1093/pm/pnw027 SPINE SECTION Original Research Article Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern? Seok Kang, MD, Seung
Technical Note NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE FLUOROSCOPIC VIEWS DURING CERVICAL RADIOFREQUENCY NEUROTOMY.
 Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Original Article Ultrasound-Guided Versus C-Arm Fluoroscopy Controlled Radiofrequency Ablation of the Cervical Facets
 Egyptian Journal of Neurosurgery Volume 31 / No. 3 / July September 2016 189-194 Original Article Ultrasound-Guided Versus C-Arm Fluoroscopy Controlled Radiofrequency Ablation of the Cervical Facets 1
Egyptian Journal of Neurosurgery Volume 31 / No. 3 / July September 2016 189-194 Original Article Ultrasound-Guided Versus C-Arm Fluoroscopy Controlled Radiofrequency Ablation of the Cervical Facets 1
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Ultrasound-Guided Cervical Selective Nerve Root Block. A Fluoroscopy-Controlled Feasibility Study
 ULTRASOUND ARTICLE Ultrasound-Guided Cervical Selective Nerve Root Block A Fluoroscopy-Controlled Feasibility Study Samer N. Narouze, MD, MS,* Amaresh Vydyanathan, MD,* Leonardo Kapural, MD, PhD,*Þ Daniel
ULTRASOUND ARTICLE Ultrasound-Guided Cervical Selective Nerve Root Block A Fluoroscopy-Controlled Feasibility Study Samer N. Narouze, MD, MS,* Amaresh Vydyanathan, MD,* Leonardo Kapural, MD, PhD,*Þ Daniel
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
A Patient s Guide to Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 2778 N. Webb Rd. Wichita, KS 67226 Phone: (316) 631-1600 Fax: (316) 631-1617 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Epidural Steroid Injections 2778 N. Webb Rd. Wichita, KS 67226 Phone: (316) 631-1600 Fax: (316) 631-1617 DISCLAIMER: The information in this booklet is compiled from
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
SPINE SECTION. Sang-Hoon Lee, MD, PhD,* Jin-Myung Kim, MS, Vincent Chan, MD, Hyo-Joon Kim, MD, PhD, and Hyoung-Ihl Kim, MD, PhD
 bs_bs_banner Pain Medicine 2013; 14: 5 13 Wiley Periodicals, Inc. SPINE SECTION Original Research Article Ultrasound-Guided Cervical Periradicular Steroid Injection for Cervical Radicular Pain: Relevance
bs_bs_banner Pain Medicine 2013; 14: 5 13 Wiley Periodicals, Inc. SPINE SECTION Original Research Article Ultrasound-Guided Cervical Periradicular Steroid Injection for Cervical Radicular Pain: Relevance
Cervical Epidural Injection
 Cervical Epidural Injection The Cervical Vertebrae The cervical vertebrae are the bones that support your neck and head. They form the top part of your spine. The tunnel made by these vertebrae is called
Cervical Epidural Injection The Cervical Vertebrae The cervical vertebrae are the bones that support your neck and head. They form the top part of your spine. The tunnel made by these vertebrae is called
CSNRBs are commonly performed under fluoroscopic
 Published August 26, 2010 as 10.3174/ajnr.A2230 ORIGINAL RESEARCH T. Wolter S. Knoeller A. Berlis C. Hader CT-Guided Cervical Selective Nerve Root Block with a Dorsal Approach BACKGROUND AND PURPOSE: Cervical
Published August 26, 2010 as 10.3174/ajnr.A2230 ORIGINAL RESEARCH T. Wolter S. Knoeller A. Berlis C. Hader CT-Guided Cervical Selective Nerve Root Block with a Dorsal Approach BACKGROUND AND PURPOSE: Cervical
Confirmation with Epidurogram Necessary?
 Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Facet Joint Syndrome / Arthritis
 Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
A Comparison between the Anterior and Posterior Approach to US-guided Shoulder Articular Injections for MR Arthrography 1
 A Comparison between the Anterior and Posterior Approach to US-guided Shoulder Articular Injections for MR Arthrography 1 Joo Yeon Ji, M.D. Purpose: To assess the feasibility of ultrasound-guided shoulder
A Comparison between the Anterior and Posterior Approach to US-guided Shoulder Articular Injections for MR Arthrography 1 Joo Yeon Ji, M.D. Purpose: To assess the feasibility of ultrasound-guided shoulder
Ultrasound-guided Pulsed Radiofrequency of the Third Occipital Nerve
 Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Musculoskeletal Imaging Original Research
 Musculoskeletal Imaging Original Research Wang et al. Fluoroscopically Guided Thoracic Foraminal Nerve Blocks Musculoskeletal Imaging Original Research Alfred Wang 1 Thomas K. Pilgram 2 Louis A. Gilula
Musculoskeletal Imaging Original Research Wang et al. Fluoroscopically Guided Thoracic Foraminal Nerve Blocks Musculoskeletal Imaging Original Research Alfred Wang 1 Thomas K. Pilgram 2 Louis A. Gilula
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Facet syndrome in the cervical (upper) spine
 Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
d EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: facet_joint_denervation 6/2009 4/2017 4/2018 4/2017 Description of Procedure or Service Facet joint denervation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: facet_joint_denervation 6/2009 4/2017 4/2018 4/2017 Description of Procedure or Service Facet joint denervation
PERCUTANEOUS FACET JOINT DENERVATION
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Radiofrequency Ablation 101
 Radiofrequency Ablation 101 Neuroscience Summit September 10, 2016 Chris Pratt, DO Texas Health Care Pain Management 1651 West Rosedale Street, Suite #205 Fort Worth, Texas 71604 What s in a name? Radiofrequency
Radiofrequency Ablation 101 Neuroscience Summit September 10, 2016 Chris Pratt, DO Texas Health Care Pain Management 1651 West Rosedale Street, Suite #205 Fort Worth, Texas 71604 What s in a name? Radiofrequency
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18
 Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
A Patient s Guide to Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is
A Patient s Guide to Pain Management: Epidural Steroid Injections 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is
Clinical Study. Pain Physician 2018; 21:E181-E186 ISSN Younghoon Jeon, MD, PhD 1 and Saeyoung Kim, MD, PhD 2
 Pain Physician 2018; 21:E181-E186 ISSN 2150-1149 Clinical Study Detection of Intravascular Injection During Cervical Transforaminal Epidural Injection: A Comparison of Digital Subtraction Angiography and
Pain Physician 2018; 21:E181-E186 ISSN 2150-1149 Clinical Study Detection of Intravascular Injection During Cervical Transforaminal Epidural Injection: A Comparison of Digital Subtraction Angiography and
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14 SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
Lumbar Epidural Injections. Treatment to Reduce Pain
 Lumbar Epidural Injections Treatment to Reduce Pain What Is a Lumbar Epidural Injection? Your doctor may have suggested you have a lumbar epidural injection. This procedure can help relieve low back and
Lumbar Epidural Injections Treatment to Reduce Pain What Is a Lumbar Epidural Injection? Your doctor may have suggested you have a lumbar epidural injection. This procedure can help relieve low back and
Chapter 4 describes the results of systematic literature review of the diagnostic validity
 Summary The main aim of this thesis was to contribute to the diagnostics of SI joint pain. We performed anatomical and clinical research next to a systematic literature review regarding diagnostic criteria
Summary The main aim of this thesis was to contribute to the diagnostics of SI joint pain. We performed anatomical and clinical research next to a systematic literature review regarding diagnostic criteria
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture. Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh Patel, MD
 -Pain Physician 2007; 10:747-752 ISSN 1533-3159 Technical Report Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh
-Pain Physician 2007; 10:747-752 ISSN 1533-3159 Technical Report Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh
A Patient s Guide to Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 2659 Professional Circle Suite 1110 Naples, FL 34119 Phone: 239-596-0100 Fax: 239-596-6737 DISCLAIMER: The information in this booklet
A Patient s Guide to Pain Management: Epidural Steroid Injections 2659 Professional Circle Suite 1110 Naples, FL 34119 Phone: 239-596-0100 Fax: 239-596-6737 DISCLAIMER: The information in this booklet
A Patient s Guide to Pain Management: Radiofrequency Ablation
 A Patient s Guide to Pain Management: Radiofrequency Ablation 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Pain Management: Radiofrequency Ablation 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis
 Pain Physician 2018; 21:67-72 ISSN 1533-3159 Prospective Observational Study Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis Min Cheol
Pain Physician 2018; 21:67-72 ISSN 1533-3159 Prospective Observational Study Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis Min Cheol
NERVOUS SYSTEM ANATOMY
 INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
 The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
Introduction of FIREFLY Technology
 Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons Cleveland Clinic Abu Dhabi
 Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Acute Brown-Sequard syndrome following brachial plexus avulsion injury. A report of two cases
 University of Malaya From the SelectedWorks of Mun Keong Kwan September, 2011 Acute Brown-Sequard syndrome following brachial plexus avulsion injury. A report of two cases Mun Keong Kwan Available at:
University of Malaya From the SelectedWorks of Mun Keong Kwan September, 2011 Acute Brown-Sequard syndrome following brachial plexus avulsion injury. A report of two cases Mun Keong Kwan Available at:
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Ultrasound guidance for interventional pain management
 Faculty Disclosure Ultrasound guidance for interventional pain management Dr. Roel Mestrum, MD, FIPP Anesthesiology, Intensive Care Medicine and Multidisciplinary Pain Centre Regionaal Ziekenhuis Heilig
Faculty Disclosure Ultrasound guidance for interventional pain management Dr. Roel Mestrum, MD, FIPP Anesthesiology, Intensive Care Medicine and Multidisciplinary Pain Centre Regionaal Ziekenhuis Heilig
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
INJECTION FOR YOUR BACK & NECK
 INJECTION FOR YOUR BACK & NECK CERVICAL EPIDURAL CERVICAL FACET BLOCKS LUMBAR EPIDURAL FACET BLOCKS ROOT BLOCKS INJECTIONS FOR YOUR BACK A lumbar caudal epidural steroid injection is an outpatient procedure
INJECTION FOR YOUR BACK & NECK CERVICAL EPIDURAL CERVICAL FACET BLOCKS LUMBAR EPIDURAL FACET BLOCKS ROOT BLOCKS INJECTIONS FOR YOUR BACK A lumbar caudal epidural steroid injection is an outpatient procedure
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
HISTORY AND CHIEF COMPLAINT:
 submitted by Keith M. Bartley, D.C. Jasper, IN 07/21/11 presented at Cox Seminar in Nashville, TN, on October 8 9, 2011 HISTORY AND CHIEF COMPLAINT: 01/21/11 55 year old male press operator for Jasper
submitted by Keith M. Bartley, D.C. Jasper, IN 07/21/11 presented at Cox Seminar in Nashville, TN, on October 8 9, 2011 HISTORY AND CHIEF COMPLAINT: 01/21/11 55 year old male press operator for Jasper
Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block
 Med. J. Cairo Univ., Vol. 84,. 1, December: 1525-153, 16 www.medicaljournalofcairouniversity.net Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block KHALED
Med. J. Cairo Univ., Vol. 84,. 1, December: 1525-153, 16 www.medicaljournalofcairouniversity.net Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block KHALED
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13)
 Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Neuroplasty or Epidural Adhesiolysis / Neurolysis
 Epidural injections are a very common treatment for neck, back and extremity pain. Back problems have become one of the most common medical conditions in our society today. Approximately 80 percent of
Epidural injections are a very common treatment for neck, back and extremity pain. Back problems have become one of the most common medical conditions in our society today. Approximately 80 percent of
USRA OF THE LOWER EXTREMITY
 USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE LOWER EXTREMITY Christian R. Falyar, CRNA, DNAP Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Cervical facet radiofrequency
 Techniques in Regional Anesthesia and Pain Management (2005) 9, 81-85 Cervical facet radiofrequency Ricardo Vallejo, MD, PhD, FIPP From the Millenium Pain Center, Bloomington, Illinois; and Illinois State
Techniques in Regional Anesthesia and Pain Management (2005) 9, 81-85 Cervical facet radiofrequency Ricardo Vallejo, MD, PhD, FIPP From the Millenium Pain Center, Bloomington, Illinois; and Illinois State
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto
 Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
The main causes of cervical radiculopathy include degeneration, disc herniation, and spinal instability.
 SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
NERVOUS SYSTEM ANATOMY
 NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block
 Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Karachi Spine - Pain and Minimally Invasive Spine Surgery Workshop. Lumbar Injections For Diagnosis and Treatment. Pain Management
 Lumbar Injections For Diagnosis and Treatment Pain Management Ovidiu Nicolae Palea Centrul de Diagnostic si Tratament ProVita Anesthesiology and Intensive Care 2009 decided to focus on Pain Management
Lumbar Injections For Diagnosis and Treatment Pain Management Ovidiu Nicolae Palea Centrul de Diagnostic si Tratament ProVita Anesthesiology and Intensive Care 2009 decided to focus on Pain Management
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Chapter 13. The Spinal Cord & Spinal Nerves. Spinal Cord. Spinal Cord Protection. Meninges. Together with brain forms the CNS Functions
 Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
CERVICAL SPINE TIPS A
 CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Improving the safety of transforaminal epidural steroid injections in the treatment of cervical radiculopathy.
 TRANSFORAMINAL NEEDLES Joseph Eldor, MD Pain Physician. 2011 May-Jun;14(3):285-93. Improving the safety of transforaminal epidural steroid injections in the treatment of cervical radiculopathy. Kloth DS,
TRANSFORAMINAL NEEDLES Joseph Eldor, MD Pain Physician. 2011 May-Jun;14(3):285-93. Improving the safety of transforaminal epidural steroid injections in the treatment of cervical radiculopathy. Kloth DS,
Clinical Effectiveness of Ultrasound-guided Costotransverse Joint Injection in Thoracic Back Pain Patients
 Brief Report Korean J Pain 2016 July; Vol. 29, No. 3: 197-201 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.3.197 Clinical Effectiveness of Ultrasound-guided Costotransverse Joint
Brief Report Korean J Pain 2016 July; Vol. 29, No. 3: 197-201 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.3.197 Clinical Effectiveness of Ultrasound-guided Costotransverse Joint
Origin of lumbar spinal roots and their relationship to intervertebral discs
 Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Infraclavicular brachial plexus blocks aim at the
 REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
2013 Coding Changes. Diagnostic Radiology. Nuclear Medicine
 2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Epidural Steroid Injection
 Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Epidural steroid injection
 Information sheet for adult patients undergoing: Epidural steroid injection for the Treatment of Pain What is the aim of this information sheet? The aim of this information sheet is to provide you with
Information sheet for adult patients undergoing: Epidural steroid injection for the Treatment of Pain What is the aim of this information sheet? The aim of this information sheet is to provide you with
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Department of Neurology/Division of Anatomical Sciences
 Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
The sacrum is a complex anatomical structure.
 A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
Case Report Inadvertent Subdural Injection during Cervical Transforaminal Epidural Steroid Injection
 Case Reports in Anesthesiology Volume 2013, Article ID 847085, 5 pages http://dx.doi.org/10.1155/2013/847085 Case Report Inadvertent Subdural Injection during Cervical Transforaminal Epidural Steroid Injection
Case Reports in Anesthesiology Volume 2013, Article ID 847085, 5 pages http://dx.doi.org/10.1155/2013/847085 Case Report Inadvertent Subdural Injection during Cervical Transforaminal Epidural Steroid Injection
The Spinal Cord & Spinal Nerves
 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
Back Pain Policies Summary
 Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Chapter 13: The Spinal Cord and Spinal Nerves
 Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS AND PAIN
 Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
