Disclosures. The Challenge of CPP. Goals of this lecture 6/24/2013
|
|
|
- Jane Osborne
- 5 years ago
- Views:
Transcription
1 2 Chronic Pelvic Pain.. Relief for clinicians, and for patients Rebecca Jackson, MD Professor Obstetrics & Gynecology University of California, San Francisco Disclosures I have no affiliation with any pharmaceutical companies, etc. I will discuss off-label use of drugs. The Challenge of CPP Frustrated (or desperate) patients want a definitive diagnosis and treatment right now Lack of clear national guidelines Lack of understanding of CPP among GYNs (and PCP s) Lack of understanding among pain MDs of the pelvis High utilization of services often without improvement in patient pain or functioning Goals of this lecture Give you hope (and skills necessary) that you can help many women with CPP Concentrate on interconnected, multi-factorial nature of CPP How to create a therapeutic relationship Stepwise algorithm for diagnosis AND treatment Treatment focus: trigger points, pelvic floor dysfunction, vulvodynia, neuropathic pain 1
2 6 Syllabus Note Syllabus includes slides that will not be addressed in lecture but are included for reference These slides are marked with REF Overview of CPP Affects physical and sexual function, and emotional well-being Severely impacts quality of life Multiple systems interact and contribute to the pathophysiology of CPP In many cases a direct cause of CPP cannot be identified Increased risk of a history of abuse, depression, and anxiety, which exacerbate painful symptoms What CPP patients want 1. Personalized care 2. To feel understood and taken seriously 3. Explanation of the cause 4. Reassurance Set clear expectations Ask for her goals/concerns (and acknowledge them) Set realistic expectations: 1. Improvement in pain/function; not pain free 2. You will look for conditions that can be treated, but even if can t make clear diagnosis, you have options to help with pain 3. This will take awhile. Multiple visits. Multiple treatment modalities 4. If she wants relief, she will have to work at it. (PT, exercises etc) 5. Visits scheduled, not during flares 6. Outline next steps, but don t be pushed into an immediate diagnosis 7. You will partner with her throughout to help her improve 8. Pain contract for opiates (if necessary) 2
3 Differential Diagnosis! Gynecologic Urinary tract Mental health issues (cause increased pain) Endometriosis* Interstitial cystitis* Somatization Adenomyosis* Recurrent UTI Substance abuse Post-PID syndrome Urethral diverticulum Physical and sexual abuse, PTSD Vulvodynia, vulvar vestibulitis Chronic urethral syndrome Depression, Anxiety Pelvic adhesions (maybe?) Neoplasia Musculoskeletal Pelvic congestion (maybe?) Radiation cystitis Pelvic floor myalgia* Ovarian remnant syndrome Gastrointestinal tract Myofascial pain (trigger point neuralgia)* Leiomyoma (pressure) Irritable bowel syndrome* Hernia Endosalpingiosis Chronic constipation Abnormal posture Neoplasia Inflammatory bowel disease Fibromyalgia Fallopian tubal prolapse (post-hyst) Diverticular colitis Chronic abdominal wall pain Tuberculous salpingitis Chronic intermittent bowel obstruction Neurologic Neuralgia of pelvic/pudendal nerves* Benign cystic mesothelioma Neoplasia (post-surgical or ob) Postoperative peritoneal cysts Celiac disease Herniated disc Neuropathic pain (diabetes) * Most common It s all connected Gyn GI Depression, anxiety, PTSD, IPV, h/o abuse: Exacerbate painful symptoms Mental Health Issues Primary etiology of pain can be Gyn, GI, GU or M-S Musculoskeletal GU Musculoskeletal Initial insult can cause musculoskeletal dysfunction that can persist after initial insult resolves, or can feedback and make primary visceral symptoms worse Stepwise approach to Eval & Treatment Step 1: Address Mental Health Treat depression if present Counseling if h/o abuse Step 2: Eval and treat musculo-skel issues Step 3: Choose possible diagnosis and treat empirically Step 4: If not improved: Consider another diagnosis/trtment Add other meds (TCA, gabapentin) Re-address M-S issues: physical therapy if not yet tried Order of steps not important: Do in whatever order makes sense for given patient The CPP History & PE Not just for getting to diagnosis but also. Powerful therapeutic tool Careful history, close listening, thorough (but sensitive) PE build rapport, trust Therapeutic benefit from the telling of one s story (therefore, use written history forms only as adjunct) Reflect back what you have heard Discuss concerns, fears 3
4 Point to it Relation to BM, voiding? If intermitt: how long is each episode? Did anything happen that may have brought it on? Particularly Important Questions to Ask of Women With Chronic Pelvic Pain CPP: History Clues Timing relative to menses, urination, BM Most endometriosis initially includes dysmenorrhea (may progress to continuous, non-cyclic pain) Quality of pain Squeezing, cramps: visceral Sharp, shooting, lancinating: somatic Cyclic pain is usually gynecologic but both IBS and interstitial cystitis can be worsened with menses What do you think is the cause? Chronic Pelvic Pain. Howard, Fred; MS, MD Obstetrics & Gynecology. 101(3): , March CPP: History Urinary symptoms Dysuria, frequency, nocturia, incomplete voiding Pain worse with full bladder? GI symptoms Dyschezia, nausea, diarrhea, constipation, mucus stools, hematochezia, melena Pain relieved by bowel movements? Musculoskeletal symptoms LBP, joint pain, sciatica Effect of movement on pain CPP Physical Exam Goals Identify underlying pathology Reproduce pain Establish trust, minimize fear Not just a pelvic exam! Observe gait/posture, thorough exam of abd wall, pelvic floor muscles, vaginal introitus 4
5 CPP: Before Leaving Get More Information!! Pain diary with menstrual calendar Voiding diary Bladder questionnaires Medical record review Back to the Stepwise approach Step 1: Address Mental Health Treat depression if present Counseling if h/o abuse Step 2: Eval and treat musculo-skel issues Step 3: Choose possible diagnosis and treat empirically Step 4: If not improved: Consider another diagnosis/trtment Add other meds (TCA, gabapentin) Re-address M-S issues: physical therapy if not yet tried Order of steps not important: Do in whatever order makes sense for given patient 1. Address mental health issues Pain has impact on quality of life and functional capacity Women become isolated and have difficulty communicating needs Relationships become strained Pre-existing psych issues such as PTSD exacerbated by pain Anxiety, depression, IPV, h/o of abuse are common act to exacerbate pain Assess quality of life (REF) In the past month, how much has your pelvic pain kept you from doing your usual activities such as self-care, work or recreation? (scale 1-5) How much has your pelvic pain interfered with your quality of life? How much have the treatments you have received for your pelvic pain improved your quality of life? How do you cope with your pain? How does your partner, family etc. respond when you are in pain? 20 5
6 Sensitive History IPV, h/o abuse, sexual functioning, depression Frame it: remember, these pts may distrust medical system, think you are trying to say their pain is in their heads I would like to ask you questions about the rest of your life to help me understand how the pain is affecting you. This will help me know how best to treat you. I ask these questions of all my patients Emotional Health (REF) Screen for current or prior physical or sexual violence, including events in childhood "At any time, has a partner hit, kicked, or otherwise hurt or threatened you?" Has your partner or a former partner every hit or hurt you? Has he or she ever threatened to hurt you? Do you ever feel afraid of your partner? Have you ever been forced to have sex when you didn t want to? Depression (12-35%) During the past month, have you been bothered by little interest or pleasure in doing things? During the past month, have you been bothered by feeling down or hopeless? Assess sexual functioning (68% have dysfunction) Desire, frequency, satisfaction, orgasm and discomfort Treating Sexual Pain (REF) Learn about your body Explore your pleasure spots Educate your partner Connect with your partner in sexual and nonsexual ways Prepare for sex: relax the PF muscles, use lubricants, take time for arousal Reinvent your sex life Avoid painful activities 1. Address mental health issues SSRI for depression Counseling (especially cognitivebehavioral therapy) for h/o abuse, difficulty coping with pain Address sexual pain Heather Howard, PhD Sexual Rehab.org 6
7 Myofascial Pelvic Pain Syndrome 2. Evaluate and treat musculoskeletal issues 28 muscles have direct attachments to the pelvis! Inciting event: injury/trauma, visceral condition (IBS, EM, EC), referred pain from viscera, poor posture Leads to: Short, tight, tender pelvic floor muscles and pain in pelvis, vagina, vulva, rectum, or bladder, or referred to thighs, buttocks, or lower abdomen. Many experts believe that many, if not most, women with chronic pelvic pain have some degree of MPPS Trigger points are the hallmark of myofascial pain Even without classic trigger points, muscular pain prominent in many women with CPP (regardless of etiology) Pelvic Floor Myalgia Findings Pain is aching, throbbing, or heaviness Low back, sacral pain; can radiate to hip, thigh Often worse with prolonged standing Levators are tense, tender on vaginal exam Management Pelvic physical therapy and biofeedback Neuropathic pain medications (gabapentin, TCAs) Vaginal or abdominal wall trigger point injections Relaxation therapy (breathing, visualization) Ice, heat (to the vagina!) Carnett s Sign Differentiates pain originating from the abdominal wall versus peritoneal cavity (Suleiman et al., 2001) The patient raises her head and shoulders from the examination table while the provider palpates the tender area on the abdomen. Positive Carnett s sign: pain remains unchanged or increases when the abdominal muscles are tensed. 28 7
8 12-point Unimanual Unidigit Examining Pelvic Floor Muscles Vaginal Exam Palpate in 4 quadrants x 3 depths Single finger NO abdominal palpation Just beyond hymen 12:00 urethra, 6:00 rectum 3:00/9:00 obturator internus Mid-vagina 12:00 bladder base, 6:00 rectum 3:00/9:00 puborectalis Just before cervix 12:00 bladder, 6:00 rectum/cul-de-sac 3:00/9:00 pubo/iliococcygeus Does this reproduce your pain? 30 A couple patients yo with CPP x 1.5 yr, band across her lower abd, thinks it started with IUD placement. IUD removed 3 mos ago, no change. Of note, had leg injury and walks with cane yo with CPP many yrs, now w 10/10 flare. RLQ. s/p hyst (no relief), s/p l/s 1 yr ago adhesions but o/w nl. Percoset with some relief. Thinks its due to ovarian cysts b/c had some on earlier u/s. Both had. Myofascial Trigger Points Trigger points are hyperirritable palpable nodules that are taut bands of muscle fibers (Tough et al., 2007) When palpated the pain usually radiates to another location Found in abdominal wall, perineum and pelvic floor locations Abdominal wall and vagina share T10-12 dermatomes with pelvic organs: Pain from trigger points referred to pelvic organs See also: Lavelle, E., Lavelle, W., & Smith, H. (2007). Myofascial trigger points. Anesthesiology Clinics, 25,
9 Trigger Point Injection Therapy Local anesthetic injection(s) directly into trigger point (TP). Thought to interrupt pain pathway 93% success by 5 th injection in abdomen (Kuan, 2006) Agent: Lidocaine 1%, Bupivicaine 0.25%, Plus /minus triamcinolone 10mg (caution corticosteroids) Volume: 2 to 10 cc. (use 2 cc if multiple trigger point, larger volume if only one. Beware lido toxicity limit to <15-20 cc) 22 or 25 gauge needle, long enough to reach the TP. Find the TP with the needle: TP=maximal burning pain Weekly injections, stop if no relief at all. Continue if any relief. Best if combined with physical therapy 33 Langford, Neurourology and Urodynamics Volume 26, Issue 1, pages 59 62, January 2007 Intravaginal trigger points can be accessed with trumpet pudendal needle guide Botulinum toxin A few small studies of injections into levator ani show benefit Consider it experimental Risk of major side effects: urinary or fecal incontinence or retention Another patient. 25 yo with CPP and known endometriosis (l/s proven), much improved with continuous OCP but still w significant dysparunea and pain that affects her QOL. She had. 9
10 Myofascial pain treatment Anti-inflammatories, ice to vagina, vulva Refer patients to physical therapists specializing in pelvic floor muscle work (advanced training) Myofascial release Biofeedback Home exercise program Abdominal breathing, rescue poses, stretching exercises Choose possible diagnosis & treat empirically These 5 diagnoses account for most known causes of CPP: 1. IBS 2. Interstitial Cystitis 3. Endometriosis 4. Adenomyosis 5. Vulvodynia/vulvar vestibulitis See American Physical Therapy website for referrals Irritable Bowel Syndrome(IBS) Pain or discomfort for 3 days/month in the prior 3 months with 2 or more of: Improvement with defecation Onset associated with a change in frequency of stool Onset associated with a change in appearance of stool Symptoms lending support to diagnosis >3 bm per day or <3 bm per week Lumpy/hard or loose/watery stool, mucus passage Urgency or incomplete emptying Bloating or distension Symptoms may be precipitated by meals or certain foods Caveats: Can be worse with menses so don t r/o if pain is cyclic Rome III Diagnostic Criteria Treatment for IBS (REF) Dietary recommendations: Elimination diet Fiber Mainstay of treatment Eat at regular times Watch dairy products Drink plenty of fluids Pain/gas/bloating: antispasmodic (dicyclomine, hyoscyamine) Constipation: increased fiber and psyllium Diarrhea: loperamide Stress reduction Exercise regularly Antidepressants Alosetron (diarrhea) or lubiprostone (constipation) CAM: acupuncture, herbs, probiotics, hypnosis, peppermint oil 10
11 Interstitial Cystitis (IC) Symptoms/Signs Urgency, frequency, nocturia, bladder pain Pain worse on filling bladder; better on voiding May also have dyspareunia, urge incontinence Bladder tenderness + pelvic floor tenderness Absence of objective evidence of another disease that could cause the symptoms Diagnosis of IC: PUF Questionnaire (pain/urgency/freq) Max score = 35 PPV 91% (vs. KCL sensitivity) if score > 20 Lowest threshold for diagnosis is score >12 Parsons CL et al. Urology 2002;59: and 60: PUF questionnaire avail online: search: PUF Interstitial cysitis Treatments for IC Start with: Oral sodium pentosan polysulfate (PPS) 100mg TID (Elmiron) Eliminate bladder irritants: acidic foods, artificial sweeteners, caffeine, tea, chocolate Stop Smoking Bladder training Physical therapy, stretching Refer to urogyn if not effective: Intravesical treatments Hydrodistension under general anesthesia: mainstay of treatment Dimethylsulfoxide Q1-2wks x 4-8 times: remission not cure BCG (Bacillus Calmette-Guerin) 6 weekly treatments TENS Endometriosis (EM): Presentation Classical EM occurs in a minority of patients Dysmenorrhea Dyspareunia Perimenstrual tenesmus, diarrhea, dysuria, hematuria, sacral backache Commonly, continuous CPP is the sole complaint (although many will give h/o of significant dysmenorrhea) Bimanual exam may show: Uterosacral ligament nodularity, fixed uterine retroflexion Stenotic cervical os, deviated cervix Corpus and adnexal tenderness Tender pelvic floor Endometriosis (EM): Role of L/S Conventional wisdom EM requires a surgical diagnosis Recent trend Empirical diagnosis of women likely to have EM is safer and more cost-effective than laparoscopy If history consistent and pain improved with either continuous hormonal methods or with GnRH agonist, assume endometriosis Reserve laparoscopy to treat endometriosis in setting of infertility, desiring pregnancy (improved fertility rates after surgical trtment) and for endometriomas 11
12 Endometriosis, empiric therapy NSAID + Continuous OC x2 3 mo Yes Continue OC* Complete* 6 9 mo Improved? No GnRHa x2 mo Pain Improved? # Yes # Both pain score and functionality improve *Or transition to DMPA,?Implanon, LNG-IUS, (or OC) No Consider L/S, other diagnoses, Musc skel eval/trt Adenomyosis Presentation Endometrial glands, stroma within myometrium Symptoms Onset usually in late 30s-40s New onset dysmenorrhea; constant CPP possible Sometimes: dyspareunia Irregular vaginal bleeding No bowel or bladder symptoms unless EM osis Signs Uterus enlarged, boggy and tender No adnexal tenderness Adenomyosis: Diagnosis/Treatment Diagnosis Pathologic diagnosis. More recently, MRI being used. However, unclear clinical utility, can simply start empiric therapy. Treatment: Ovarian suppression: OCs, Patch, DMPA, Implanon Levonorgestrel IUD If fail hysterectomy Medical management often ineffective for controlling pain of adenomyosis. (works for bleeding) Unlike for other pelvic pain syndromes, hysterectomy for adenomyosis is often curative b/c symptoms confined to uterus Vulvodynia Incidence: 3-5% of reproductive age women Risk Factors: Vulvovaginal infection OC use Physical, emotional or sexual trauma Comorbid disorders: IC IBS Fibromyalgia/Chronic Fatigue Syndrome Psychosocial and sexual impairment 48 12
13 Vulvodynia: Q Tip Test 49 Diagnosis of Vulvodynia & Vestibulodynia 50 Purpose: identify and map changes in sensation including allodynia Gently touch with a q-tip Start at the thigh and work down to perineum bilaterally Include clitoris and perianal areas Proceed from labia majora to labia minora then the vestibule Chronic Vulvar Pain PE No visible findings Erythema Hyperalgesia Allodynia R/O Infectious, inflammatory, neoplastic and neurologic cause Vulvodynia Generalized pain Burning, stabbing, stinging, etc. Vestibulodynia Pain at vestibule only Provoked Burning Treat accordingly Vulvar Vestibule 51 Treatments: Vulvodynia & Vestibulodynia 52 Behavioral: Avoidance of vulvar irritants, constipation, sitz bath bid followed by vaseline, Ice/cool for burning, after sex Meds: No meds clearly superior, may need to try several, Start with topical lidocaine or topical gabapentin 6%. 3 mos trial; Other meds: Oral TCA s, Anticonvulsants, SSNRI s, Opioids; Topical: estradiol cream (if atrophic), compounded antidepressants, anticonvulasants Pelvic floor therapy, biofeedback very important Psychotherapy, CBT, Sex therapy Nerve blocks, Nuerostimulation Surgery? For generalized vulvodynia, surgery contraindicated. For localized vestibulitis, vestibulectomy has been shown effective 13
14 4. If no improvement Consider another diagnosis/trtment Add other meds (TCA, gabapentin) Re-address M-S issues: physical therapy if not yet tried When pain is a disease and not a symptom After 4-6 months, pain can become an illness, not just a symptom Central Sensitization = Maladaptation: an amplification of neural signaling within the central nervous system that elicits pain hypersensitivity Inciting event might have been treated, pain persists Treatment focuses not on cure but on managing the pain Treating Pain: Medications Analgesics: NSAIDS (try at least 3) Opioids (short course) Topical anesthetics* Antidepressants Tricyclics* SSRI s/snri s* Anticonvulsants gabapentin pregabalin Muscle relaxants Vaginal preparations (valium, anti-depressant, anticonvulsant) Refer to pain management nerve blocks neurotoxin: OnabotulinumtoxinA* medication consult 55 Treatment of Neuropathic Pain Mainly helpful in women with daily pain Clinical depression is present SSRI (e.g., fluoxetine) or SNRI (e.g., venlafaxine) Advance to primary care dosing limits Clinical depression not prominent Gabapentin mg QHS, adv to 900 mg TID TCA: nortriptyline 10 mg QHS, adv weekly to 50 mg Sleep problems Herbals, antihistamines Short acting sleeping meds: e.g., zolpidem *Off label use 14
15 Integrative Approach Mind/body interventions: breathing exercises, imagery, MBSR, laughter yoga, etc. Movement therapies: yoga, Tai Chi, Feldenkrais, etc. Nutrition: anti-inflammatory diet/herbs, multivitamins, B complex, fish oil, calcium/magnesium, herbal tonics Alternative providers: TCM, craniosacral, chiropractic, energy medicine, strain/counter strain, etc. 57 Take It Home Spend time to establish trust Set realistic goals with your patient: improved function vs. complete remission Think beyond making a diagnosis Manage the reactive depression that can make the perception of pain much worse Pelvic floor dysfunction is common and perpetuates the pain cycle. Treat with pelvic PT plus/minus trigger point injections If your first empiric therapy is ineffective, don t give up. Revisit other diagnoses, depression and musculo-skeletal issues. Build a community: physical therapist, pain consultant 60 What CPP patients want 1. Personalized care 2. To feel understood and taken seriously 3. Explanation of the cause 4. Reassurance Although we often can t give them #3, we can explain the interconnectedness of pelvic organs, muscles and pain pathways. Patients don t really come to us because they are in pain, they come to us because they are suffering. Ling, APS Conference
16 Resources International Pelvic Pain Society National Vulvodynia Association Endometriosis.org Sexuality Information and Education Council of US Interstitial Cystitis Association Irritable Bowel Syndrome: see NIDDK/NIH American Physical Therapy Association American Chronic Pain Association UCSF Chronic Pelvic Pain Clinic 61 References ACOG Committee on Practice Bulletins--Gynecology ACOG Practice Bulletin No. 51. Chronic pelvic pain. Obstet Gynecol Mar;103(3): Jarrell F, et al. Consensus guidelines for the management of chronic pelvic pain J Obstet Gynaecol Can. 2005;27(8): Howard FM. Chronic pelvic pain. Ob Gynecol. 2003;101: Abercrombie PD, Learman LA. Providing Holistic Care for Women with Chronic Pelvic Pain. J Obstet Gynecol Neonatal Nurs Aug 3. (Entire issue devoted to chronic pelvic pain) 16
Priscilla Abercrombie, RN, NP, PhD, AHN-BC HS Clinical Professor Obstetrics, Gynecology & Reproductive Sciences UCSF Community Health Systems UCSF
 Priscilla Abercrombie, RN, NP, PhD, AHN-BC HS Clinical Professor Obstetrics, Gynecology & Reproductive Sciences UCSF Community Health Systems UCSF Chronic Pelvic Pain Clinic UCSF Osher Center for Integrative
Priscilla Abercrombie, RN, NP, PhD, AHN-BC HS Clinical Professor Obstetrics, Gynecology & Reproductive Sciences UCSF Community Health Systems UCSF Chronic Pelvic Pain Clinic UCSF Osher Center for Integrative
Chronic Pelvic Pain.. Relief for clinicians, and for patients
 Chronic Pelvic Pain.. Relief for clinicians, and for patients Rebecca Jackson, MD Professor Obstetrics & Gynecology University of California, San Francisco Disclosures I have no financial disclosures I
Chronic Pelvic Pain.. Relief for clinicians, and for patients Rebecca Jackson, MD Professor Obstetrics & Gynecology University of California, San Francisco Disclosures I have no financial disclosures I
Chronic Pelvic Pain Case Study
 Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
Case L.M. Question 1 4/17/2013. Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin
 Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre
 PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
Chronic Pelvic Pain. Bridget Kamen, MD Obstetrics and Gynecology, Confluence Health. I have no disclosures
 Chronic Pelvic Pain Bridget Kamen, MD Obstetrics and Gynecology, Confluence Health I have no disclosures Objectives A little epidemiology Understand there are both gynecologic and non-gynecologic causes
Chronic Pelvic Pain Bridget Kamen, MD Obstetrics and Gynecology, Confluence Health I have no disclosures Objectives A little epidemiology Understand there are both gynecologic and non-gynecologic causes
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery
 Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
Chronic Pelvic Pain. Miss Sanjay Kumari Consultant Gynaecologist
 Chronic Pelvic Pain Miss Sanjay Kumari Consultant Gynaecologist Headache in Pelvis Confusion and lack of clarity What we think? But to me it s a pain that you ve tried in every way to solve, by surgery,
Chronic Pelvic Pain Miss Sanjay Kumari Consultant Gynaecologist Headache in Pelvis Confusion and lack of clarity What we think? But to me it s a pain that you ve tried in every way to solve, by surgery,
Chronic Pelvic Pain. AP099, December 2010
 AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
Pelvic Pain: Diagnosis and Management
 Pelvic Pain: Diagnosis and Management Mr N Pisal Consultant Gynaecologist Advanced Laparoscopic Surgeon www.london-gynaecology.com History LMP Dysmenorrhoea / Dyspareunia Cyclical pain related to menstrual
Pelvic Pain: Diagnosis and Management Mr N Pisal Consultant Gynaecologist Advanced Laparoscopic Surgeon www.london-gynaecology.com History LMP Dysmenorrhoea / Dyspareunia Cyclical pain related to menstrual
Case Study (continued) Abdominal and Pelvic Pain. Learning Objectives. Case Study. Signs &Symptoms. Triage Questions to Assess Acute Pelvic Pain
 Learning Objectives Discuss common causes of acute pelvic pain Discuss common causes of chronic pelvic pain Abdominal and Pelvic Pain Identify triage questions to differentiate urgent vs. non urgent presentations
Learning Objectives Discuss common causes of acute pelvic pain Discuss common causes of chronic pelvic pain Abdominal and Pelvic Pain Identify triage questions to differentiate urgent vs. non urgent presentations
Chronic pelvic pain has many different characteristics. Signs and symptoms may include:
 Pelvic Pain in Women Pelvic pain in women refers to pain in the lowest part of your abdomen and pelvis. If asked to locate your pain, you might sweep your hand over that entire area rather than point to
Pelvic Pain in Women Pelvic pain in women refers to pain in the lowest part of your abdomen and pelvis. If asked to locate your pain, you might sweep your hand over that entire area rather than point to
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website:
 Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
Endometriosis: An Overview
 Endometriosis: An Overview www.bcwomens.ca Welcome to the BC Women s Centre for Pelvic Pain and Endometriosis. This handout will give you some basic information about endometriosis. It will also explain
Endometriosis: An Overview www.bcwomens.ca Welcome to the BC Women s Centre for Pelvic Pain and Endometriosis. This handout will give you some basic information about endometriosis. It will also explain
CHRONIC PELVIC PAIN AS WE UNDERSTAND IT TODAY. Dr. Sonia Wartan Consultant in Pain Medicine
 CHRONIC PELVIC PAIN AS WE UNDERSTAND IT TODAY Dr. Sonia Wartan Consultant in Pain Medicine Clinical Lead of Chronic Pain Services Chronic Pelvic MDT Clinic Royal Gwent Hospital Acute Pain Specific disease/injury
CHRONIC PELVIC PAIN AS WE UNDERSTAND IT TODAY Dr. Sonia Wartan Consultant in Pain Medicine Clinical Lead of Chronic Pain Services Chronic Pelvic MDT Clinic Royal Gwent Hospital Acute Pain Specific disease/injury
Management of Gynae Problems in Primary Care David Griffiths FRCOG The Great Western Hospital Swindon. A brief overview
 Management of Gynae Problems in Primary Care David Griffiths FRCOG The Great Western Hospital Swindon A brief overview Pelvic Pain Challenge to the physician In UK 1 Million sufferers 20% of all gynae
Management of Gynae Problems in Primary Care David Griffiths FRCOG The Great Western Hospital Swindon A brief overview Pelvic Pain Challenge to the physician In UK 1 Million sufferers 20% of all gynae
Role of Physiotherapy in the Management of Persistent Pelvic Pain. Brigitte Fung Physiotherapist Kwong Wah Hospital
 Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Objectives. Scope of the Problem. How Many Women who Have a Hysterectomy for CPP have Endometriosis on Pathology?
 Objectives Discuss the epidemiology Explore the neurobiology Introduce CPP as a systemic condition Run through the diagnostics Review therapies Chronic Pelvic Pain Dr. Jen Gunter MD, FRCS(C), FACOG, DABPM,
Objectives Discuss the epidemiology Explore the neurobiology Introduce CPP as a systemic condition Run through the diagnostics Review therapies Chronic Pelvic Pain Dr. Jen Gunter MD, FRCS(C), FACOG, DABPM,
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Interstitial Cystitis
 Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Uterine prolapse & Fistulas. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
Pelvic Pain Assessment Form
 Pelvic Pain Assessment Form Physician: Initial History and Physical Examination Date: This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Pelvic Pain Assessment Form Physician: Initial History and Physical Examination Date: This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Interstitial Cystitis - Painful Bladder Syndrome
 Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
MANAGEMENT OF VISCERAL PAIN
 MANAGEMENT OF VISCERAL PAIN William D. Chey, MD, FACG Professor of Medicine University of Michigan 52 year old female with abdominal pain 5 year history of persistent right sided burning/sharp abdominal
MANAGEMENT OF VISCERAL PAIN William D. Chey, MD, FACG Professor of Medicine University of Michigan 52 year old female with abdominal pain 5 year history of persistent right sided burning/sharp abdominal
Pelvic Pain Assessment Form
 Pelvic Pain Assessment Form Physician : Date: Initial History and Physical Examination This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Pelvic Pain Assessment Form Physician : Date: Initial History and Physical Examination This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Provenance Rehabilitation Pelvic Intake Form
 Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
Introduction to GYN Specialties
 Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
IBS. Patient INFO. A Guide to Irritable Bowel Syndrome
 Patient INFO IBS A Guide to Irritable Bowel Syndrome The information provided by the AGA Institute is not medical advice and should not be considered a replacement for seeing a medical professional. About
Patient INFO IBS A Guide to Irritable Bowel Syndrome The information provided by the AGA Institute is not medical advice and should not be considered a replacement for seeing a medical professional. About
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Endometriosis د. نجمه محمود كلية الطب جامعة بغداد فرع النسائية والتوليد
 Endometriosis د. نجمه محمود كلية الطب جامعة بغداد فرع النسائية والتوليد Objectives:- To know what is endometriosis The sites where it occur To explain its itiology & pathogenesis To know the clinical features
Endometriosis د. نجمه محمود كلية الطب جامعة بغداد فرع النسائية والتوليد Objectives:- To know what is endometriosis The sites where it occur To explain its itiology & pathogenesis To know the clinical features
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
Is one of the most common chronic disorders. causing patients to seek medical treatment.
 ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
Practical Approaches to the Patient with Chronic Pain
 Practical Approaches to the Patient with Chronic Pain M. Jean Uy- Kroh, MD, FACOG Assistant Professor Of Surgery, CCLCM Director of Chronic Pelvic Pain Program Women s Health Institute Cleveland, Ohio
Practical Approaches to the Patient with Chronic Pain M. Jean Uy- Kroh, MD, FACOG Assistant Professor Of Surgery, CCLCM Director of Chronic Pelvic Pain Program Women s Health Institute Cleveland, Ohio
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
Moneli Golara Consultant Obstetrician and Gynaecologist Barnet Hospital Royal Free NHS Trust
 Moneli Golara Consultant Obstetrician and Gynaecologist Barnet Hospital Royal Free NHS Trust Endometriosis one of the most common conditions requiring treatment Growth of endometrial like tissue outside
Moneli Golara Consultant Obstetrician and Gynaecologist Barnet Hospital Royal Free NHS Trust Endometriosis one of the most common conditions requiring treatment Growth of endometrial like tissue outside
10/15/2012. Pelvic Pain and Dysfunction
 Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Abdominal and Pelvic Pain
 Objectives Abdominal and Pelvic Pain By the end of this lecture, participants will be able to: Identify common causes of acute abdominal and pelvic pain Identify common causes of chronic abdominal and
Objectives Abdominal and Pelvic Pain By the end of this lecture, participants will be able to: Identify common causes of acute abdominal and pelvic pain Identify common causes of chronic abdominal and
PELVIC PAIN QUESTIONNAIRE
 PELVIC PAIN QUESTIONNAIRE Name: DOB: / / Are you currently: Single Married Separated Divorced Re-married De-Facto Who do you live with? What type of employment are you currently in? How long? INFORMATION
PELVIC PAIN QUESTIONNAIRE Name: DOB: / / Are you currently: Single Married Separated Divorced Re-married De-Facto Who do you live with? What type of employment are you currently in? How long? INFORMATION
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 301.681.3400 OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is surgery to remove the uterus. It is a very common type of surgery for women in the United States. Removing your uterus means
301.681.3400 OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is surgery to remove the uterus. It is a very common type of surgery for women in the United States. Removing your uterus means
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders What are functional GI disorders?
 The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD and Kellie Bunn, PA-C What are functional GI
The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD and Kellie Bunn, PA-C What are functional GI
Dysmenorrhoea Gynaecology د.شيماءعبداالميرالجميلي. Aetiology of secondary dysmenorrhea
 30-11-2014 Gynaecology Dysmenorrhoea د.شيماءعبداالميرالجميلي Dysmenorrhoea is defined as painful menstruation. It is experienced by 45 95 per cent of women of reproductive age.primary Spasmodic Dysmenorrhea
30-11-2014 Gynaecology Dysmenorrhoea د.شيماءعبداالميرالجميلي Dysmenorrhoea is defined as painful menstruation. It is experienced by 45 95 per cent of women of reproductive age.primary Spasmodic Dysmenorrhea
PELVIC PAIN IN GYNECOLOGY
 PELVIC PAIN IN GYNECOLOGY Pelvic pain is an important part of clinical practice for who any clinician who provides health care for women. It can be acute, recurrent or chronic. Differential Diagnosis:
PELVIC PAIN IN GYNECOLOGY Pelvic pain is an important part of clinical practice for who any clinician who provides health care for women. It can be acute, recurrent or chronic. Differential Diagnosis:
Case 1. Case Studies in Vulvovaginal Disease. Disclosures. What is your diagnosis? Case 1. Lichen sclerosus 10/19/2018
 Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
What is Irritable Bowel Syndrome (IBS)?
 What is Irritable Bowel Syndrome (IBS)? Irritable bowel syndrome (IBS) is a health issue found in your intestines (gut). IBS can cause symptoms such as: Belly pain. Cramping. Gas. Bloating (or swelling)
What is Irritable Bowel Syndrome (IBS)? Irritable bowel syndrome (IBS) is a health issue found in your intestines (gut). IBS can cause symptoms such as: Belly pain. Cramping. Gas. Bloating (or swelling)
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
IBS - Definition. Chronic functional disorder of GI generally characterized by:
 IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
An Approach to Abdominal Pain
 An Approach to Abdominal Pain objectives Should know the different types of abd pain Is acute or chronic? Hx taking skills with knowing the key questions Important abdominal pain signs A good differential
An Approach to Abdominal Pain objectives Should know the different types of abd pain Is acute or chronic? Hx taking skills with knowing the key questions Important abdominal pain signs A good differential
8/29/2016 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW. LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES
 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
Pelvic Pain Tool Box NO FINANCIAL DISCLOSURES OBJECTIVES. Chronic Pelvic Pain. Treating Chronic Pelvic Pain 6/4/2018
 Pelvic Pain Tool Box Shanti Mohling, MD, FACOG Director of Gynecology Associate Director Fellowship in Minimally Invasive Gynecologic Surgery University of Tennessee College of Medicine, Chattanooga NO
Pelvic Pain Tool Box Shanti Mohling, MD, FACOG Director of Gynecology Associate Director Fellowship in Minimally Invasive Gynecologic Surgery University of Tennessee College of Medicine, Chattanooga NO
IC - THE GYNECOLOGISTS PERSPECTIVE Diagnosis & the relationship of IC to Endometriosis, Vulvodynia, Vulvar Vestibulitis & IBS
 Guest Lecture Series Transcript IC - THE GYNECOLOGISTS PERSPECTIVE Diagnosis & the relationship of IC to Endometriosis, Vulvodynia, Vulvar Vestibulitis & IBS Featuring: Dr. Bruce Kahn, MD, FACOG Department
Guest Lecture Series Transcript IC - THE GYNECOLOGISTS PERSPECTIVE Diagnosis & the relationship of IC to Endometriosis, Vulvodynia, Vulvar Vestibulitis & IBS Featuring: Dr. Bruce Kahn, MD, FACOG Department
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
32 OBG Management July 2010 Vol. 22 No. 7 obgmanagement.com
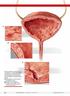 A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
Female Symptom Monitor
 Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
Information About Your Pain Please describe your pain problem (use a separate sheet of paper if needed) :
 Patient History Date: This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be a diagnostic tool. Contact Information Name: Birth Date: Referring
Patient History Date: This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be a diagnostic tool. Contact Information Name: Birth Date: Referring
Fibromyalgia summary. Patient leaflets from the BMJ Group. What is fibromyalgia? What are the symptoms?
 Patient leaflets from the BMJ Group Fibromyalgia summary We all get aches and pains from time to time. But if you have long-term widespread pain across your whole body, you may have a condition called
Patient leaflets from the BMJ Group Fibromyalgia summary We all get aches and pains from time to time. But if you have long-term widespread pain across your whole body, you may have a condition called
Vulvodynia and vestibulectomy
 Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
Sexual Concerns. Mental Health Topics
 Sexual Concerns A lot of people have concerns about their sex life. Common concerns and problems that affect one or both sex partners Talk to your partner about your include: sexual concerns. n Little
Sexual Concerns A lot of people have concerns about their sex life. Common concerns and problems that affect one or both sex partners Talk to your partner about your include: sexual concerns. n Little
Dysmenorrhea. Erin Eppsteiner, M.D. Department of Ob/Gyn The University of Iowa Roy J & Lucille A Carver College of Medicine
 Dysmenorrhea Erin Eppsteiner, M.D. Department of Ob/Gyn The University of Iowa Roy J & Lucille A Carver College of Medicine Objectives Be able to recognize primary and secondary dysmenorrhea Be familiar
Dysmenorrhea Erin Eppsteiner, M.D. Department of Ob/Gyn The University of Iowa Roy J & Lucille A Carver College of Medicine Objectives Be able to recognize primary and secondary dysmenorrhea Be familiar
FEMALE SYMPTOM MONITOR
 FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
Female Symptom Monitor
 Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
At the outset, we want to clear up some terminology issues. IBS is COPYRIGHTED MATERIAL. What Is IBS?
 1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
How does interstitial cystitis begin?
 Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
MULTIDISCIPLINARY APPROACH TO PELVIC PAIN. The Desert Women s Care Pelvic Pain program has is organized around four key goals
 MULTIDISCIPLINARY APPROACH TO PELVIC PAIN Approximately 15 20% of women aged 18 50 years have chronic pain of greater than twelve months duration. There are numerous causes for pelvic pain and 25 50% of
MULTIDISCIPLINARY APPROACH TO PELVIC PAIN Approximately 15 20% of women aged 18 50 years have chronic pain of greater than twelve months duration. There are numerous causes for pelvic pain and 25 50% of
Cases For Teaching Second Year Medical Students. Head and neck and neuroanatomy. 2- What is the anatomical explanation for her symptoms?
 Head and neck and neuroanatomy Case 1: (RECURRENT LARYNGEAL NERVE INJURY) A 35-year-old woman complains of a 2-month history of hoarseness of her voice and some choking while drinking liquids. She denies
Head and neck and neuroanatomy Case 1: (RECURRENT LARYNGEAL NERVE INJURY) A 35-year-old woman complains of a 2-month history of hoarseness of her voice and some choking while drinking liquids. She denies
Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary vulvar clinic Vestibulectomy
 From Pain to Pleasure Surgical Treatment of Vestibulodynia Päivi Tommola Specialist in Gynecology 13.10.2010 GKS Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary
From Pain to Pleasure Surgical Treatment of Vestibulodynia Päivi Tommola Specialist in Gynecology 13.10.2010 GKS Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information
 Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
Intentions and Format of the Class
 Intentions and Format of the Class To give you a not so common sense understanding of your pelvis. Including Anatomy Dysfunction (when things don t work right) Exercise (Yoga Asanas) that promote pelvic
Intentions and Format of the Class To give you a not so common sense understanding of your pelvis. Including Anatomy Dysfunction (when things don t work right) Exercise (Yoga Asanas) that promote pelvic
Name: Date: DOB: Full Address: Phone: Home: Cell: Occupation: Emerg. contact and phone: Relationship to pt.
 Client Registration Name: Date: DOB: Email: Full Address: Phone: Home: Cell: Occupation: Emerg. contact and phone: Relationship to pt. How did you hear about ALIGN? ALIGN Integration Movement does not
Client Registration Name: Date: DOB: Email: Full Address: Phone: Home: Cell: Occupation: Emerg. contact and phone: Relationship to pt. How did you hear about ALIGN? ALIGN Integration Movement does not
Support Information Advocacy Education Research CHRONIC PELVIC PAIN. w w w. p e l v i c p a i n. o r g. u k. w w w. p e l v i c p a i n. o r g.
 Support Information Advocacy Education Research The Pelvic Pain Support Network would be pleased to hear from clinicians and researchers with an interest in this field. For further information please contact:
Support Information Advocacy Education Research The Pelvic Pain Support Network would be pleased to hear from clinicians and researchers with an interest in this field. For further information please contact:
CLEAR COVERAGE HYSTERECTOMY CHECKLISTS
 CLEAR COVERAGE HYSTERECTOMY CHECKLISTS Click on the link below to access the checklist sheet. Abnormal Uterine Bleeding Adenomyosis Chronic Abdominal or Pelvic Pain Endometriosis Fibroids General Guidelines
CLEAR COVERAGE HYSTERECTOMY CHECKLISTS Click on the link below to access the checklist sheet. Abnormal Uterine Bleeding Adenomyosis Chronic Abdominal or Pelvic Pain Endometriosis Fibroids General Guidelines
Interstitial Cystitis/ Bladder Pain Syndrome
 page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
Your first consultation: questions your doctor may ask you
 BY ELLEN T JOHNSON, ROS WOOD, AND LONE HUMMELSHOJ Endometriosis can be difficult to diagnose, so your gynaecologist will need your help if s/he is to build up a useful picture of your symptoms. Completing
BY ELLEN T JOHNSON, ROS WOOD, AND LONE HUMMELSHOJ Endometriosis can be difficult to diagnose, so your gynaecologist will need your help if s/he is to build up a useful picture of your symptoms. Completing
Long-term pelvic pain:
 Long-term pelvic pain: information for you aashara Published November 005 by the RCOG Title amended October 00 Contents Page number Key points 1 About this information What is long-term pelvic pain? What
Long-term pelvic pain: information for you aashara Published November 005 by the RCOG Title amended October 00 Contents Page number Key points 1 About this information What is long-term pelvic pain? What
Vulvodynia What a Health Practitioner Should Know
 Vulvodynia What a Health Practitioner Should Know Catherine M. Leclair, MD Associate Professor Director, Program in Vulvar Health Objective: To present a clinically based approach to vulvodynia Identify
Vulvodynia What a Health Practitioner Should Know Catherine M. Leclair, MD Associate Professor Director, Program in Vulvar Health Objective: To present a clinically based approach to vulvodynia Identify
Pathogenesis of Chronic Pelvic Pain
 Pathogenesis of Chronic Pelvic Pain Yong-Chul Kim Department of anesthesia and pain medicine, Seoul National University College of Medicine 1 Overview Anatomy Nerve innervation CPP by pathology CPP by
Pathogenesis of Chronic Pelvic Pain Yong-Chul Kim Department of anesthesia and pain medicine, Seoul National University College of Medicine 1 Overview Anatomy Nerve innervation CPP by pathology CPP by
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE?
 PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
Chronic Abdominal Pain. Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016
 Chronic Abdominal Pain Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016 Disclosures Speaker Bureau for Allergan Pharmaceuticals Abdominal Pain - Definitions Acute occurring for several
Chronic Abdominal Pain Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016 Disclosures Speaker Bureau for Allergan Pharmaceuticals Abdominal Pain - Definitions Acute occurring for several
Dr Hannah Blakely. Dr Ben Sharp. Ms Julee Binns. Sara Widdowson. 7:15-8:15 Breakfast Session: Oxford Women's Health
 Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
Primary Care Gynaecology Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
 Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
Medical History Form M Clear Passage Physical Therapy
 OFFICE USE ONLY: Accept / Qualified / Decline Date Intro Sent: Date MHF Rec d: Date Reviewed: By: Medical History Form M Clear Passage Physical Therapy Please use black ink. Print rather than using cursive,
OFFICE USE ONLY: Accept / Qualified / Decline Date Intro Sent: Date MHF Rec d: Date Reviewed: By: Medical History Form M Clear Passage Physical Therapy Please use black ink. Print rather than using cursive,
Lower back pain and hemorrhoids
 Lower back pain and hemorrhoids Beverly Hill Proctologists Primary Menu they begin in the front of our pelvic cavities and terminate in the back of the tailbone pain with hemorrhoids. Can hemorrhoids cause
Lower back pain and hemorrhoids Beverly Hill Proctologists Primary Menu they begin in the front of our pelvic cavities and terminate in the back of the tailbone pain with hemorrhoids. Can hemorrhoids cause
Sexological aspects of genital pain
 Sexological aspects of genital pain Annamaria Giraldi, professor, MD, PHD Sexological Clinic, Psychiatric Centre Copenhagen 1 Disclosures Speaker: Eli Lilly, Pfizer Consultant: Eli Lilly,Palatin 2 Agenda
Sexological aspects of genital pain Annamaria Giraldi, professor, MD, PHD Sexological Clinic, Psychiatric Centre Copenhagen 1 Disclosures Speaker: Eli Lilly, Pfizer Consultant: Eli Lilly,Palatin 2 Agenda
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
Presenter. Irritable Bowel Syndrome. Objectives. Introduction. Rome Criteria. Irritable Bowel Syndrome 2/28/2018
 Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Palm Beach Obstetrics & Gynecology, PA
 Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Endometriosis The lining of the uterus is
Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Endometriosis The lining of the uterus is
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic Pain. What you need to know. 139 Dumaresq Street Campbelltown Phone Fax
 Pelvic Pain What you need to know 139 Dumaresq Street Campbelltown Phone 4628 5292 Fax 4628 0349 www.nureva.com.au September 2015 PELVIC PAIN This is a common problem and most women experience some form
Pelvic Pain What you need to know 139 Dumaresq Street Campbelltown Phone 4628 5292 Fax 4628 0349 www.nureva.com.au September 2015 PELVIC PAIN This is a common problem and most women experience some form
ICD-10 Common Codes for Pelvic Rehab Providers
 ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
Prof. Salma Rouf Prof. ObGyn, DMCH Joint Secretary, OGSB
 Prof. Salma Rouf Prof. ObGyn, DMCH Joint Secretary, OGSB To facilitate and improve the understanding of chronic pelvic pain To provide evidence based guidelines for management Pain is by definition, a
Prof. Salma Rouf Prof. ObGyn, DMCH Joint Secretary, OGSB To facilitate and improve the understanding of chronic pelvic pain To provide evidence based guidelines for management Pain is by definition, a
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE
 PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
