Multispecialty Applications / Professional Use Information
|
|
|
- Anna Owen
- 5 years ago
- Views:
Transcription
1 Multispecialty Applications / Professional Use Information
2 Multispecialty Applications Professional Use Information OmniPulse MAX TM 80 Watt Holmium Laser Model 1210-VHP OmniPulse TM 40 Watt Holmium Laser Model 1210 OmniPulse Jr. TM 30 Watt Holmium Laser Model Trimedyne, Inc Bake Parkway Irvine, CA USA P/N Multispecialty Applications / Professional Use Manual
3 Multispecialty Applications Professional Use Information OmniPulse MAX TM 80 Watt Holmium Laser Model 1210-VHP OmniPulse TM 40 Watt Holmium Laser Model 1210 OmniPulse Jr. TM 30 Watt Holmium Laser Model Trimedyne, Inc Bake Parkway Irvine, CA USA Multispecialty Applications / Professional Use Manual
4 Printed and bound in the United States of America. All rights reserved. No portion of this reference manual may be used or reproduced in any means without the written permission of Trimedyne, Inc. Making copies of any part of this manual for any purpose other than personal use is a violation of United States copyright laws. Permitted copies must carry the same copyright notices as the original. Though every effort has been made to ensure the accuracy of the information provided in this manual, the contents of this manual are subject to change without notice. For information, contact Trimedyne, Inc., Bake Parkway, Irvine, CA 92606, U.S.A. Voice +1 (949) ; Fax +1 (949) customerservice@trimedyne.com Copyright May 2003, P/N Published by Trimedyne, Inc. Trimedyne, OmniPulse MAX, OmniPulse, OmniPulse Jr., and the Trimedyne logo are trademarks of Trimedyne, Inc. Multispecialty Applications / Professional Use Manual i
5 Table of Contents 1 Introduction to Multispecialty Applications Dermatology and Plastic Surgery Indications Warnings Precautions Complications / Risks Contraindications Gastroenterological/ Gastrointestinal Surgery Indications Warnings Precautions Complications / Risks Contraindications General Surgery (Soft Tissue) Indications Warnings Precautions Complications / Risks Contraindications...20 Multispecialty Applications / Professional Use Manual ii
6 5 Genitourinary Surgery/Urology Indications Warnings Precautions Complications / Risks Contraindications Important Benign Prostatic Hyperplasia (BPH) Information: Gynecological Surgery Indications Warnings Precautions Complications / Risks Contraindications Lithotripsy and Percutaneous Urinary Lithotripsy Indications Warnings Precautions Complications / Risks Contraindications Orthopedic Surgery Indications Warnings Precautions Complications / Risks Contraindications...46 Multispecialty Applications / Professional Use Manual iii
7 9 Otorhinolaryngology (ENT) Surgery Indications Warnings Precautions Complications / Risks Contraindications Percutaneous Cervical, Lumbar, and Thoracic Disc Decompression / Discectomy Indications Warnings Precautions Complications / Risks Contraindications Recommended Laser Parameters for Endoscopic or Percutaneous Cervical or Thoracic Disc Decompression / Discectomy...58 Multispecialty Applications / Professional Use Manual iv
8 1 Introduction to Multispecialty Applications! Caution: Before using the Holmium:YAG Laser System clinically, the physician must become fully acquainted with the unique surgical effects produced by the laser. For example, its depth of tissue penetration may be different than that of Nd:YAG, Argon or CO 2 lasers. The information provided in this manual is not intended to be all-inclusive nor is it intended to replace physician training or experiments. The Trimedyne Holmium:YAG Laser Systems are designed for use in conjunction with Trimedyne Inc.'s Tapertip TM disposable holmium arthroscopic handpieces, the Omni TM Switchtip System arthroscopic laser handpieces, and other optical fiber delivery devices designed for use with Trimedyne Inc. s proprietary connector. Applications for these laser systems include incision, excision, resection, ablation, coagulation, hemostasis, and vaporization, with or without an endoscope, in the following indications: General Surgery of Soft Tissues Genitourinary Surgery / Urology Otorhinolanryngology (ENT) Surgery Gynecological Surgery Lithotripsy and Percutaneous Urinary Lithotripsy Orthopedic Surgery Percutaneous Cervical, Lumbar, and Thoracic Disc Decompression /Discectomy Therapeutic Dermatological, Therapeutic Plastic, and Aesthetic Surgical Procedures Gastroenterological / Gastrointestinal Surgery This Multispecialty Applications / Professional Use Information manual includes detailed information about each of these indications. It is also important to refer to the instructions for use accompanying each optical fiber delivery device. Multispecialty Applications / Professional Use Manual 1
9 Note: Please contact the Trimedyne Customer Service department or visit our website at for an updated listing of indications and to download the most recent Multispecialty Applications Professional Use Information manual. Endoscopes, which can be either flexible or rigid, may be used for visualization during laser procedures. The outer diameter of the fiber optic delivery device used will determine the minimum working channel requirement for insertion through the endoscope. During single eyepiece endoscopic procedures, use caution since depth perception may be altered. For additional information, the document ANSI Z , "For the Safe Use of Lasers in Healthcare Facilities," is recommended for reference. The laser system should be used only by physicians and staff who have been appropriately trained and who are thoroughly familiar with the instructions and safety precautions given in the operator manual. A review of the published literature is strongly encouraged. Multispecialty Applications / Professional Use Manual 2
10 2 Dermatology and Plastic Surgery For use with or without an endoscope with or without a working channel. Prior to use, physicians must be fully acquainted with endoscopic procedures. 2.1 Indications Incision, excision, resection, ablation, vaporization, coagulation and hemostasis of soft, mucosal, fatty, and cartilaginous tissues, with or without an endoscope, in therapeutic plastic, therapeutic dermatological, and aesthetic surgical procedures, including: Scars Tattoo removal Vascular lesions, including: Corns - Port wine stains - Hemangioma - Telangiectasia (facial, leg) - Rosacea Papillomas Basal cell carcinomas Lesions of skin and subcutaneous tissue Plantar warts Periungual and subungual warts Debridement of decubitus ulcer Skin tag vaporization Multispecialty Applications / Professional Use Manual 3
11 2.2 Warnings General Refer to the safety section of the operation manual for general laser-safety precautions. Specific 1. Holmium:YAG laser radiation (2.1 micrometers) will ablate biological tissues to depths different from the radiation of CO 2 (10.6 micrometers), Argon (514.5 nanometers), or Nd:YAG (1.064 micrometers) lasers. Extreme caution should be used until the physician is completely familiar with the biological interactions of the laser energy with tissues of various types. 2. Tissue perforation can occur if excessive laser energy is applied, whether through the use of excessive laser-beam power or the application of power for excessive periods of time. 3. Use the laser only on tissues that are fully observable. Do not use the laser if the desired operating field is obscured. 4. Aim the laser only at tissues intended for treatment; otherwise, damage to surrounding tissues may result. 5. Screen abnormalities, such as tumors, that are in close proximity to known arteries or veins by pretreatment work-ups to precisely locate these circulatory structures. 6. Use low energy and low pulse-rate settings until fully familiar with the capabilities of the laser system. If higher energies are required, increase the energy in the smallest available increments until the desired level is achieved. Smaller diameter fibers will require less energy and larger diameter fibers will require higher energy to achieve the same laser fluence. These starting energy recommendations apply regardless of the particular surgical fiber optic energy delivery system configuration. Refer to the instructions for use supplied with each surgical fiber for specific maximum operating parameters. Multispecialty Applications / Professional Use Manual 4
12 7. "Flash" fire can occur. Do not operate the laser system in the presence of flammable anesthetics or volatile substances such as alcohol or elevated levels of oxygen. Under no circumstances should flammable gases be present when operating the laser. 8. The risks of combustion, perforation and laser-induced hemorrhage, all of which could cause death, must be fully explained to the patient. 9. As with conventional endoscopic treatment, adverse reactions such as fever, chills, sepsis, edema and hemorrhage may occur following laser treatment. In extreme cases, death may occur due to procedural complications, concurrent illness or the application of laser radiation. 10. During surgical procedures, the use of a smoke evacuator or equivalent is recommended (as required) to minimize airborne particulates to avoid possible biohazard. 11. During surgical treatment over the eyelid area, it is recommended that the patient's eyes be protected by placing metal or other types of Holmium wavelength (2.1 µm) rated eye shields on top of the cornea. 2.3 Precautions 1. Use caution when treating patients who have had difficulty with previous endoscopic procedures. 2. Extra precautions should be taken when radiotherapy and laser therapy are to be used concurrently, including more stringent postoperative monitoring than usual. Clinical studies have shown that patients who have undergone radiotherapy present a greater risk of perforation or tissue erosion. 3. Discontinue laser therapy immediately if the patient develops any cardiopulmonary problems. 4. Trimedyne, Inc., has no clinical information or experience concerning the use of Ho:YAG laser systems on pregnant women or nursing mothers. 5. Patients who have experienced discomfort during previous laser treatment may require analgesics. 6. During single eyepiece endoscopic procedures, use caution since depth perception may be altered. Multispecialty Applications / Professional Use Manual 5
13 7. Remove the endoscope from the treatment area prior to lasing to avoid damage to the scope. 2.4 Complications / Risks 1. As is true of other forms of medical treatment, some of the complications that may be encountered in laser therapy are serious and could result in death. They include the following: a. Non-laser related Perforation Aspiration Induced hemorrhage Allergic reaction to medication Hypertension Arrhythmia Pain Gas overdistension, pneumothorax Air embolism b. Laser related Acute Induced hemorrhage Ulceration Perforation Multispecialty Applications / Professional Use Manual 6
14 Edema Pain Fever, leukocytosis Chills Chronic Delay in healing Perforation Stricture Delayed hemorrhage Sepsis 2. Pain: Short-lived pain may occur immediately following laser therapy and may persist for as long as 48 hours. 3. Fever and Leukocytosis: Immediately after laser therapy, the patient may experience fever and leukocytosis, which are commonly associated with tissue destruction. These generally resolve without treatment. Cultures are indicated to exclude the possibility of infection. 4. Bleeding: Patients may experience bleeding at the site of the laser therapy or from erosion of a tumor during or after laser therapy. Post treatment hematocrit is recommended to identify this potential complication. 5. Sepsis: Laser-ablated tissue may become infected after therapy. If a question of sepsis exists, a culture should be taken and other appropriate evaluations made. 6. Perforation: Perforation can occur as a result of excessive exposure to laser radiation. Perforation can also occur from tumor erosion, or as a result of endoscopic procedures. To clinically diagnose perforation, patients must be monitored postoperatively through physical signs, hematocrit and radiography. 7. Gas Overdistension, Pneumothorax: Patients may experience gastrointestinal distension or pneumothorax during or after therapy. Multispecialty Applications / Professional Use Manual 7
15 2.5 Contraindications Patients who are not good surgical candidates (e.g. intolerance to anesthetics, etc.). Obstruction of the desired operating field of view. Multispecialty Applications / Professional Use Manual 8
16 3 Gastroenterological/ Gastrointestinal Surgery For use with or without an endoscope with or without a working channel. Prior to use, physicians must be fully acquainted with endoscopic procedures. 3.1 Indications Incision, excision, resection, ablation, vaporization, coagulation, and hemostasis, with or without an endoscope, of gastroenterological/ gastrointestinal tissue, including: Cholecystectomy Lysis of adhesions Appendectomy Biopsy Pylorostenotomy Benign and malignant lesions Rectal polyps of sigmoid colon Gall bladder calculi Biliary/bile duct calculi Benign and malignant neoplasm Polyps Colitis Ulcers Multispecialty Applications / Professional Use Manual 9
17 Angiodysplasia Hemorrhoids Varices Esophagitis Esophageal ulcer Mallory-Weiss tear Gastric ulcer Duodenal ulcer Non-bleeding ulcer Gastric erosions Colorectal cancer Gastritis Bleeding tumors Pancreatitis Vascular malformations Telangiectasias Telangiectasias of the Osler-Weber-Rendu disease 3.2 Warnings General Refer to the safety section of the operation manual for general laser-safety precautions. Multispecialty Applications / Professional Use Manual 10
18 Specific 1. Holmium:YAG laser radiation (2.1 micrometers) will ablate biological tissues to depths different from the radiation of CO 2 (10.6 micrometers), Argon (514.5 nanometers), or Nd:YAG (1.064 micrometers) lasers. Extreme caution should be used until the physician is completely familiar with the biological interactions of the laser energy with tissues of various types. 2. Tissue perforation can occur if excessive laser energy is applied, whether through the use of excessive laser-beam power or the application of power for excessive periods of time. 3. Use the laser only on tissues that are fully observable. Do not use the laser if the desired operating field is obscured. 4. Aim the laser only at tissues intended for treatment; otherwise, damage to surrounding tissues may result. 5. Screen abnormalities, such as tumors, that are in close proximity to known arteries or veins by pretreatment work-ups to precisely locate these circulatory structures. 6. Use low energy and low pulse-rate settings until fully familiar with the capabilities of the laser system. If higher energies are required, increase the energy in the smallest available increments until the desired level is achieved. Smaller diameter fibers will require less energy and larger diameter fibers will require higher energy to achieve the same laser fluence. These starting energy recommendations apply regardless of the particular surgical fiber optic energy delivery system configuration. Refer to the instructions for use supplied with each surgical fiber for specific maximum operating parameters. 7. "Flash" fire can occur. Do not operate the laser system in the presence of flammable anesthetics or volatile substances such as alcohol or elevated levels of oxygen. Under no circumstances should flammable gases be present when operating the laser. 8. The risks of combustion, perforation and laser-induced hemorrhage, all of which could cause death, must be fully explained to the patient. 9. As with conventional endoscopic treatment, adverse reactions such as fever, chills, sepsis, edema and hemorrhage may occur following laser treatment. In extreme cases, death may occur due to procedural complications, concurrent illness or the application of laser radiation. Multispecialty Applications / Professional Use Manual 11
19 10. During surgical procedures, the use of a smoke evacuator or equivalent is recommended (as required) to minimize airborne particulates to avoid possible biohazard. 3.3 Precautions 1. Use caution when treating patients who have had difficulty with previous endoscopic procedures. 2. Extra precautions should be taken when radiotherapy and laser therapy are to be used concurrently, including more stringent postoperative monitoring than usual. Clinical studies have shown that patients who have undergone radiotherapy present a greater risk of perforation or tissue erosion. 3. Discontinue laser therapy immediately if the patient develops any cardiopulmonary problems. 4. Trimedyne, Inc., has no clinical information or experience concerning the use of Ho:YAG laser systems on pregnant women or nursing mothers. 5. Patients who have experienced discomfort during previous laser treatment may require analgesics. 6. During single eyepiece endoscopic procedures, use caution since depth perception may be altered. 7. Remove the endoscope from the treatment area prior to lasing to avoid damage to the scope. 3.4 Complications / Risks 1. As is true of other forms of medical treatment, some of the complications that may be encountered in laser therapy are serious and could result in death. They include the following: Multispecialty Applications / Professional Use Manual 12
20 a. Non-laser related Perforation Aspiration Induced hemorrhage Allergic reaction to medication Hypertension Arrhythmia Pain Gas overdistension, pneumothorax Air embolism b. Laser related Acute Induced hemorrhage Ulceration Perforation Edema Pain Fever, leukocytosis Chills Chronic Delay in healing Perforation Multispecialty Applications / Professional Use Manual 13
21 Stricture Delayed hemorrhage Sepsis 2. Pain: Short-lived pain may occur immediately following laser therapy and may persist for as long as 48 hours. 3. Fever and Leukocytosis: Immediately after laser therapy, the patient may experience fever and leukocytosis, which are commonly associated with tissue destruction. These generally resolve without treatment. Cultures are indicated to exclude the possibility of infection. 4. Bleeding: Patients may experience bleeding at the site of the laser therapy or from erosion of a tumor during or after laser therapy. Post treatment hematocrit is recommended to identify this potential complication. 5. Sepsis: Laser-ablated tissue may become infected after therapy. If a question of sepsis exists, a culture should be taken and other appropriate evaluations made. 6. Perforation: Perforation can occur as a result of excessive exposure to laser radiation. Perforation can also occur from tumor erosion, or as a result of endoscopic procedures. To clinically diagnose perforation, patients must be monitored postoperatively through physical signs, hematocrit and radiography. 7. Gas Overdistension, Pneumothorax: Patients may experience gastrointestinal distension or pneumothorax during or after therapy. 3.5 Contraindications Obstructions due to extrinsic compression Acute cholecystitis Jaundice Relative contraindications Obesity Multispecialty Applications / Professional Use Manual 14
22 4 General Surgery (Soft Tissue) For use with or without an endoscope with or without a working channel. Prior to use, physicians must be fully acquainted with endoscopic procedures. 4.1 Indications Incision, excision, resection, ablation, coagulation, hemostasis and vaporization, with or without an endoscope, in general surgery of soft tissue including: Skin incision Tissue dissection Excision of external tumors and lesions Complete or partial resection of internal organs Tumors and lesions Tissue ablation Mastectomy Hepatectomy Pancreatectomy Splenectomy Thyroidectomy Parathyroidectomy Herniorrhaphy Tonsillectomy Multispecialty Applications / Professional Use Manual 15
23 Lymphadenectomy Partial nephrectomy Pilonidal cystectomy Resection of lipoma Pelvic adhesiolysis Debridement of decubitus ulcers Hemorrhoids Pilodidal cyst removal and repair Debridement of statis ulcers Biopsy 4.2 Warnings General Refer to the safety section of the operation manual for general laser-safety precautions. Specific 1. Holmium:YAG laser radiation (2.1 micrometers) will ablate biological tissues to depths different from the radiation of CO 2 (10.6 micrometers), Argon (514.5 nanometers), or Nd:YAG (1.064 micrometers) lasers. Extreme caution should be used until the physician is completely familiar with the biological interactions of the laser energy with tissues of various types. 2. Tissue perforation can occur if excessive laser energy is applied, whether through the use of excessive laser-beam power or the application of power for excessive periods of time. 3. Use the laser only on tissues that are fully observable. Do not use the laser if the desired operating field is obscured. Multispecialty Applications / Professional Use Manual 16
24 4. Aim the laser only at tissues intended for treatment; otherwise, damage to surrounding tissues may result. 5. Screen abnormalities, such as tumors, that are in close proximity to known arteries or veins by pretreatment work-ups to precisely locate these circulatory structures. 6. Use low energy and low pulse-rate settings until fully familiar with the capabilities of the laser system. If higher energies are required, increase the energy in the smallest available increments until the desired level is achieved. Smaller diameter fibers will require less energy and larger diameter fibers will require higher energy to achieve the same laser fluence. These starting energy recommendations apply regardless of the particular surgical fiber optic energy delivery system configuration. Refer to the instructions for use supplied with each surgical fiber for specific maximum operating parameters. 7. "Flash" fire can occur. Do not operate the laser system in the presence of flammable anesthetics or volatile substances such as alcohol or elevated levels of oxygen. Under no circumstances should flammable gases be present when operating the laser. 8. The risks of combustion, perforation and laser-induced hemorrhage, all of which could cause death, must be fully explained to the patient. 9. As with conventional endoscopic treatment, adverse reactions such as fever, chills, sepsis, edema and hemorrhage may occur following laser treatment. In extreme cases, death may occur due to procedural complications, concurrent illness or the application of laser radiation. 10. During surgical procedures, the use of a smoke evacuator or equivalent is recommended (as required) to minimize airborne particulates to avoid possible biohazard. 4.3 Precautions 1. Use caution when treating patients who have had difficulty with previous endoscopic procedures. 2. Extra precautions should be taken when radiotherapy and laser therapy are to be used concurrently, including more stringent postoperative monitoring than usual. Clinical studies have shown that patients who have undergone radiotherapy present a greater risk of perforation or tissue erosion. Multispecialty Applications / Professional Use Manual 17
25 3. Discontinue laser therapy immediately if the patient develops any cardiopulmonary problems. 4. Trimedyne, Inc., has no clinical information or experience concerning the use of Ho:YAG laser systems on pregnant women or nursing mothers. 5. Patients who have experienced discomfort during previous laser treatment may require analgesics. 6. During single eyepiece endoscopic procedures, use caution since depth perception may be altered. 7. Remove the endoscope from the treatment area prior to lasing to avoid damage to the scope. 4.4 Complications / Risks 1. As is true of other forms of medical treatment, some of the complications that may be encountered in laser therapy are serious and could result in death. They include the following: a. Non-laser related Perforation Aspiration Induced hemorrhage Allergic reaction to medication Hypertension Arrhythmia Pain Gas overdistension, pneumothorax Air embolism Multispecialty Applications / Professional Use Manual 18
26 b. Laser related Acute Induced hemorrhage Ulceration Perforation Edema Pain Fever, leukocytosis Chills Chronic Delay in healing Perforation Stricture Delayed hemorrhage Sepsis 2. Pain: Short-lived pain may occur immediately following laser therapy and may persist for as long as 48 hours. 3. Fever and Leukocytosis: Immediately after laser therapy, the patient may experience fever and leukocytosis, which are commonly associated with tissue destruction. These generally resolve without treatment. Cultures are indicated to exclude the possibility of infection. 4. Bleeding: Patients may experience bleeding at the site of the laser therapy or from erosion of a tumor during or after laser therapy. Post treatment hematocrit is recommended to identify this potential complication. Multispecialty Applications / Professional Use Manual 19
27 5. Sepsis: Laser-ablated tissue may become infected after therapy. If a question of sepsis exists, a culture should be taken and other appropriate evaluations made. 6. Perforation: Perforation can occur as a result of excessive exposure to laser radiation. Perforation can also occur from tumor erosion, or as a result of endoscopic procedures. To clinically diagnose perforation, patients must be monitored postoperatively through physical signs, hematocrit and radiography. 7. Gas Overdistension, Pneumothorax: Patients may experience gastrointestinal distension or pneumothorax during or after therapy. 4.5 Contraindications Obstructions due to extrinsic compression Acute cholecystitis Jaundice Stone in the common bile duct The need for common bile duct exploration Relative contraindications Obesity Previous abdominal surgery Multispecialty Applications / Professional Use Manual 20
28 5 Genitourinary Surgery/Urology For use with or without an endoscope with or without a working channel. Prior to use, physicians must be fully acquainted with genitourinary/urology procedures. 5.1 Indications Incision, excision, resection, ablation, coagulation, hemostasis and vaporization, with or without an endoscope, of genitourinary/urology tissue including: Lesions of the external genitalia Condylomas Urethral and penile hemangioma 5.2 Warnings The Trimedyne holmium laser systems and fiber optic laser energy delivery systems are not licensed under a United States patent covering their use in laser resection or enucleation of the prostate, the treatment of strictures, or transurethral incision of the prostate. The following list of warnings is provided with the understanding that these devices are not recommended for such uses. General Refer to the safety section of the operation manual for general laser-safety precautions. Multispecialty Applications / Professional Use Manual 21
29 Specific 1. Holmium:YAG laser radiation (2.1 micrometers) will ablate biological tissues to depths different from the radiation of CO 2 (10.6 micrometers), Argon (514.5 nanometers), or Nd:YAG (1.064 micrometers) lasers. Extreme caution should be used until the physician is completely familiar with the biological interactions of the laser energy with tissues of various types. 2. Tissue perforation can occur if excessive laser energy is applied, whether through the use of excessive laser-beam power or the application of power for excessive periods of time. 3. Use the laser only on tissues that are fully observable. Do not use the laser if the desired operating field is obscured. 4. Aim the laser only at tissues intended for treatment; otherwise, damage to surrounding tissues may result. 5. Screen abnormalities, such as tumors, that are in close proximity to known arteries or veins by pretreatment work-ups to precisely locate these circulatory structures. 6. Use low energy and low pulse-rate settings until fully familiar with the capabilities of the laser system. If higher energies are required, increase the energy in the smallest available increments until the desired level is achieved. Smaller diameter fibers will require less energy and larger diameter fibers will require higher energy to achieve the same laser fluence. These starting energy recommendations apply regardless of the particular surgical fiber optic energy delivery system configuration. Refer to the instructions for use supplied with each surgical fiber for specific maximum operating parameters. 7. "Flash" fire can occur. Do not operate the laser system in the presence of flammable anesthetics or volatile substances such as alcohol or elevated levels of oxygen. Under no circumstances should flammable gases be present when operating the laser. 8. The risks of combustion, perforation and laser-induced hemorrhage, all of which could cause death, must be fully explained to the patient. 9. As with conventional endoscopic treatment, adverse reactions such as fever, chills, sepsis, edema and hemorrhage may occur following laser treatment. In extreme cases, death may occur due to procedural complications, concurrent illness or the application of laser radiation. Multispecialty Applications / Professional Use Manual 22
30 10. During surgical procedures, the use of a smoke evacuator or equivalent is recommended (as required) to minimize airborne particulates to avoid possible biohazard. 5.3 Precautions The Trimedyne holmium laser systems and fiber optic laser energy delivery systems are not licensed under a United States patent covering their use in laser resection or enucleation of the prostate, the treatment of strictures, or transurethral incision of the prostate. The following list of precautions is provided with the understanding that these devices are not recommended for such uses. 1. Use caution when treating patients who have had difficulty with previous endoscopic procedures. 2. Extra precautions should be taken when radiotherapy and laser therapy are to be used concurrently, including more stringent postoperative monitoring than usual. Clinical studies have shown that patients who have undergone radiotherapy present a greater risk of perforation or tissue erosion. 3. Discontinue laser therapy immediately if the patient develops any cardiopulmonary problems. 4. Trimedyne, Inc., has no clinical information or experience concerning the use of Ho:YAG Laser Systems on pregnant women or nursing mothers. 5. Patients who have experienced discomfort during previous laser treatment may require analgesics. 6. During single eyepiece endoscopic procedures, use caution since depth perception may be altered. 7. Remove the endoscope from the treatment area prior to lasing to avoid damage to the scope. Multispecialty Applications / Professional Use Manual 23
31 5.4 Complications / Risks The Trimedyne holmium laser systems and fiber optic laser energy delivery systems are not licensed under a United States patent covering their use in laser resection or enucleation of the prostate, the treatment of strictures, or transurethral incision of the prostate. The following list of complications is provided with the understanding that these devices are not recommended for such uses. 1. As is true of other forms of medical treatment, some of the complications that may be encountered in laser therapy are serious and could result in death. They include the following: a. Non-laser related Perforation Aspiration Induced hemorrhage Allergic reaction to medication Hypertension Arrhythmia Pain Gas overdistension, pneumothorax Air embolism Local and/or systemic infection Local hematoma Dissection Urinary tract infection Multispecialty Applications / Professional Use Manual 24
32 b. Laser related Acute Induced hemorrhage Ulceration Perforation Edema Pain Fever, leukocytosis Chills Discomfort during and/or after energy application Urinary retention Hematuria Dysuria Meatal stenosis Tissue adherence to reflective tip with resultant distal tip burn-out, melting and/or detachment Retrograde ejaculation Pain and/or continued symptoms of urinary outflow obstruction secondary to benign prostatic hyperplasia (BPH) Chronic Delay in healing Perforation Stricture Multispecialty Applications / Professional Use Manual 25
33 Delayed hemorrhage Sepsis Thermal damage to surrounding structures Impotence Retrograde ejaculation Pain and/or continued symptoms of urinary outflow obstruction secondary to benign prostatic hyperplasia (BPH) 2. Pain: Short-lived pain may occur immediately following laser therapy and may persist for as long as 48 hours. 3. Fever and Leukocytosis: Immediately after laser therapy, the patient may experience fever and leukocytosis, which are commonly associated with tissue destruction. These generally resolve without treatment. Cultures are indicated to exclude the possibility of infection. 4. Bleeding: Patients may experience bleeding at the site of the laser therapy or from erosion of a tumor during or after laser therapy. Post treatment hematocrit is recommended to identify this potential complication. 5. Sepsis: Laser-ablated tissue may become infected after therapy. If a question of sepsis exists, a culture should be taken and other appropriate evaluations made. 6. Perforation: Perforation can occur as a result of excessive exposure to laser radiation. Perforation can also occur from tumor erosion, or as a result of endoscopic or laparoscopic procedures. To clinically diagnose perforation, patients must be monitored postoperatively through physical signs, hematocrit and radiography. 7. Gas Overdistension, Pneumothorax: Patients may experience gastrointestinal distension or pneumothorax during or after therapy. Multispecialty Applications / Professional Use Manual 26
34 5.5 Contraindications The Trimedyne holmium laser systems and fiber optic laser energy delivery systems are not licensed under a United States patent covering their use in laser resection or enucleation of the prostate, the treatment of strictures, or transurethral incision of the prostate. The following list of contraindications is provided with the understanding that these devices are not recommended for such uses. Patients who are not good surgical candidates (e.g. intolerance to anesthetics, etc.) Obstruction of the desired operating field of view Patients with a known bleeding disorder Patients with a current or recent urinary tract infection not treated with antibiotics Patients having a prostate specific antigen (PSA) of 10 ng/ml or greater 5.6 Important Benign Prostatic Hyperplasia (BPH) Information: The Trimedyne holmium laser systems and fiber optic laser energy delivery devices are not licensed under a United States patent covering their use in laser resection or enucleation of the prostate, the treatment of strictures, or transurethral incision of the prostate. The following information is provided with the understanding that these devices are not recommended for such uses. Multispecialty Applications / Professional Use Manual 27
35 1. Usage information of the Holmium laser for the treatment of BPH from the medical literature: a. Incision 1 : Fiber was used to create a single incision from the ureteral orifice to the verumontanum and out to fat. Lasing was on the surface of the prostate. Fiber used was a 400 µm Ho:YAG bare fiber sheathed in a ureteral catheter. b. Resection 2 : Fiber was used to resect the prostate to form an effective cavity for voiding in the prostatic urethra, and to incise at the 5 o clock position from the bladder neck to the verumontanum to the base of the bladder using the left ureteral orifice as a landmark. A similar incision was made at the 7 o clock position using the right ureteral opening as a landmark. The median lobe was resected with a transverse incision between the aforementioned 2 incisions. The transverse incision was started at the verumontanum and continued under the median lobe along the capsule toward the bladder neck, using the verumontanum as a landmark, and then the resected tissue was floated in the bladder. The incision at the 5 o clock position was extended upward along the left lateral wall. When this upward incision reached the 3 o clock position, a downward incision was added at the 1 o clock position along the lateral wall. The left lobe was then resected and floated in the bladder. The right lobe was resected similarly. The incision at the 7 o clock position was extended upward to the 9 o clock position and then a downward incision was added at the 11 o clock position. Lasing was on the surface of the prostate. Fiber used was a 550 µm forward firing Ho:YAG laser fiber. 1 Cornford PA, Biyani CS, and Powell CS: Transurethral Incision of the Prostate Using the Holmium:YAG Laser: A Cathetherless Procedure. The Journal of Urology Vol. 159, , April Matsuoka K, Iida S, Tomiyasu K, Shimada A, Noda S: Transurethral Holmium Laser Resection of the Prostate. The Journal of Urology, Vol. 163, , February Multispecialty Applications / Professional Use Manual 28
36 c. Resection 3 : Fiber was used to incise deeply in the posterior and 7 o clock positions, and the median lobe BPH tissue was gradually undermined and resected. In a similar fashion, deep template incisions were made anteriorly (at 1 and 11 o clock) down to the level of the surgical capsule of the prostate, and were combined with similar incisions continued upward from the initial 5 and 7 o clock incision posteriorly, to undermine and resect gradually the prostatic lateral lobes bilaterally. Lasing was on the surface of the prostate. Fiber used was a 550 µm end firing silica glass Ho:YAG laser delivery fiber. d. Ablation 4 : Holmium ablation of the prostate is a simple, effective technique for small prostates. No information on fiber position is available from this article. Lasing was on the surface of the prostate. Fiber used was a side firing dual wavelength fiber. e. Vaporization 5 : Fiber was inserted through the working port of the cystoscope, which was advanced into the prostatic urethra in an antegrade fashion. Lasing was on the surface of the prostate. Fiber used was straight end firing or side firing 400, 600, or 1000 µm Ho:YAG fiber with a distal polished quartz internal reflection mechanism. 3 Kabalin JN, Gilling PJ, Fraundorfer MR: Application of the Holmium:YAG Laser for Prostatectomy. Journal of Clinical Laser Medicine & Surgery, Vol. 16, No. 1, Gilling PJ, Cass CB, Cresswell MD, Malcolm AR, Fraundorfer MR: The Use of the Holmium Laser in the Treatment of Benign Prostatic Hyperplasia. Journal of Endourology, Vol. 10, No. 5, October Kabalin JN: Holmium:YAG Laser Prostatectomy Canine Feasibility Study. Lasers in Surgery and Medicine 18: page (1996). Multispecialty Applications / Professional Use Manual 29
37 f. Vaporization 6 : Fiber was used to vaporize with the standard four-point necrosis at 2, 4, 8, and 10 o clock. Lasing was on the surface of the prostate. Fiber used was an end firing 550 µm Ho:YAG bare fiber or a side firing Ho:YAG fiber with a beam deflection of 70 and a 30 divergence. g. Enucleation 7,8,9,10 : Fiber was used to incise the bladder neck deeply at 5 and 7 o clock with the incisions brought to the level of the verumontanum on each side. The incisions were then joined distally and the lobe undermined to a depth determined by these previous incisions. The entire lobe was resected back toward the bladder neck, finally disarticulating it in one large fragment back into the bladder. The left lateral lobe was then undermined commencing at the verumontanum. The apex of the resection was first defined and then the bladder neck was incised deeply at the 1 o clock position. The upper and lower incisions were then joined and the entire lateral lobe peeled off the surgical capsule. The procedure was then repeated on the right side and any small remaining fragments of adenoma were removed to give a smooth cavity. Once the resection was completed, the lobes were morcellated using either the suprapubic or transurethral approach. Lasing was on the surface of the prostate. Fiber used was a 550 µm end firing Holmium fiber. 6 Mottet N, Anidjar M, Bourdon O, Louis JF, Teillac P, Costa P, Le Duc A: Randomized Comparison of Transurethral Electroresection and Holmium:YAG Laser Vaporization for Symptomatic Benign Prostatic Hyperplasia. Journal of Endourology, Vol. 13, No. 2, March Fraundorfer MR, Gilling PJ: Holmium:YAG Laser Enucleation of the Prostate Combined with Mechanical Morcellation: Preliminary Results. European Urology 1998, 33: Gilling PJ, Kennett K, Das AK, Thompson D, Fraundorfer MR: Holmium Laser Enucleation of the Prostate (HoLEP) Combined with Transurethral Tissue Morcellation: An Update of the Early Clinical Experience. Journal of Endourology, Vol. 12, No. 5, October Krahn HP (Winnipeg, Manitoba, Canada): Laser Enucleation of the Prostate (HoLEP) A Pilot Study. 10 Krahn HP (Winnipeg, Manitoba, Canada): Complications of Holmium Laser Enucleation of the Prostate (HoLEP). Multispecialty Applications / Professional Use Manual 30
38 h. Excision: More than one incision may be performed in order to excise prostatic tissue, thus excision and incision are used interchangeably in Holmium laser application. In addition, excision is synonymous to resection. Therefore, it is reasonable to believe that any information available to the Holmium incision or resection for the treatment of BPH also applies to the Holmium excision of the said treatment. i. Hemostasis: Hemostasis refers to the cauterization of blood vessels to control bleeding during surgery. Hemostasis is a peripheral effect of the other applications of Holmium:YAG energy, such as ablation, vaporization, incision, and resection. As iterated in Gilling P, et al: The Use of the Holmium Laser in the Treatment of Benign Prostatic Hyperplasia, Journal of Endourology, Vol. 10, No. 5, October 1996, the Holmium wavelength of 2.1 µm is strongly absorbed by water and has an absorption length of 0.4 mm, which is sufficient to ensure satisfactory hemostasis in prostatic tissue. 2. Any prostate tissue removed with the Holmium laser should be collected and evaluated by a pathologist for presence of any undifferentiated or poorly differentiated cell. 3. Patients should be advised to return for follow-up visits as determined by their physicians, including one at six months. Multispecialty Applications / Professional Use Manual 31
39 6 Gynecological Surgery For use with or without an endoscope with or without a working channel. Prior to use, physicians must be fully acquainted with gynecological procedures. 6.1 Indications Incision, excision, resection, ablation, coagulation, hemostasis and vaporization, with or without an endoscope, of soft tissue in gynecology during open and endoscopic procedures, including: Condyloma acuminata 6.2 Warnings General Refer to the safety section of the operation manual for general laser-safety precautions. Specific 1. Holmium:YAG laser radiation (2.1 micrometers) will ablate biological tissues to depths different from the radiation of CO 2 (10.6 micrometers), Argon (514.5 nanometers), or Nd:YAG (1.064 micrometers) lasers. Extreme caution should be used until the physician is completely familiar with the biological interactions of the laser energy with tissues of various types. 2. Tissue perforation can occur if excessive laser energy is applied, whether through the use of excessive laser-beam power or the application of power for excessive periods of time. Multispecialty Applications / Professional Use Manual 32
40 3. Use the laser only on tissues that are fully observable. Do not use the laser if the desired operating field is obscured. 4. Aim the laser only at tissues intended for treatment; otherwise, damage to surrounding tissues may result. 5. Screen abnormalities, such as tumors, that are in close proximity to known arteries or veins by pretreatment work-ups to precisely locate these circulatory structures. 6. Use low energy and low pulse-rate settings until fully familiar with the capabilities of the laser system. If higher energies are required, increase the energy in the smallest available increments until the desired level is achieved. Smaller diameter fibers will require less energy and larger diameter fibers will require higher energy to achieve the same laser fluence. These starting energy recommendations apply regardless of the particular surgical fiber optic energy delivery system configuration. Refer to the instructions for use supplied with each surgical fiber for specific maximum operating parameters. 7. "Flash" fire can occur. Do not operate the laser system in the presence of flammable anesthetics or volatile substances such as alcohol or elevated levels of oxygen. Under no circumstances should flammable gases be present when operating the laser. 8. The risks of combustion, perforation and laser-induced hemorrhage, all of which could cause death, must be fully explained to the patient. 9. As with conventional endoscopic treatment, adverse reactions such as fever, chills, sepsis, edema and hemorrhage may occur following laser treatment. In extreme cases, death may occur due to procedural complications, concurrent illness or the application of laser radiation. 10. During surgical procedures, the use of a smoke evacuator or equivalent is recommended (as required) to minimize airborne particulates to avoid possible biohazard. Multispecialty Applications / Professional Use Manual 33
41 6.3 Precautions 1. Use caution when treating patients who have had difficulty with previous endoscopic procedures. 2. Extra precautions should be taken when radiotherapy and laser therapy are to be used concurrently, including more stringent postoperative monitoring than usual. Clinical studies have shown that patients who have undergone radiotherapy present a greater risk of perforation or tissue erosion. 3. Discontinue laser therapy immediately if the patient develops any cardiopulmonary problems. 4. Trimedyne, Inc., has no clinical information or experience concerning the use of Ho:YAG laser systems on pregnant women or nursing mothers. 5. Patients who have experienced discomfort during previous laser treatment may require analgesics. 6. Patients should be monitored for fluid absorption, especially during prolonged procedures. 7. Hysteroscopic insufflation with air or CO 2 is not recommended during use of the Ho:YAG laser system during laser endometrial ablation. Visualization may be achieved via hysteroscopic distension of the uterus with saline or Ringers solution. 8. When fluid is being used for distension, monitor patient for electrolyte balance. 9. During single eyepiece endoscopic procedures, use caution since depth perception may be altered. 10. Remove the endoscope from the treatment area prior to lasing to avoid damage to the scope. 6.4 Complications / Risks 1. As is true of other forms of medical treatment, some of the potential complications that may be encountered in laser therapy are serious and could result in death. They include the following: Multispecialty Applications / Professional Use Manual 34
42 a. Non-laser related Perforation Aspiration Induced hemorrhage Allergic reaction to medication Hypertension Arrhythmia Pain Gas overdistension, pneumothorax Air embolism b. Laser related Acute Induced hemorrhage Ulceration Perforation Edema Pain Fever, leukocytosis Chills Chronic Delay in healing Multispecialty Applications / Professional Use Manual 35
43 Perforation Stricture Delayed hemorrhage Sepsis 2. Pain: Short-lived pain may occur immediately following laser therapy and may persist for as long as 48 hours. 3. Fever and Leukocytosis: Immediately after laser therapy, the patient may experience fever and leukocytosis, which are commonly associated with tissue destruction. These generally resolve without treatment. Cultures are indicated to exclude the possibility of infection. 4. Bleeding: Patients may experience bleeding at the site of the laser therapy or from erosion of a tumor during or after laser therapy. Post treatment hematocrit is recommended to identify this potential complication. 5. Sepsis: Laser-ablated tissue may become infected after therapy. If a question of sepsis exists, a culture should be taken and other appropriate evaluations made. 6. Perforation: Perforation can occur as a result of excessive exposure to laser radiation. Perforation can also occur from tumor erosion, or as a result of endoscopic procedures. To clinically diagnose perforation, patients must be monitored postoperatively through physical signs, hematocrit and radiography. 7. Gas Overdistension, Pneumothorax: Patients may experience gastrointestinal distension or pneumothorax during or after therapy. 6.5 Contraindications Invasive gynecological cancer Any medical condition which could contraindicate hysteroscopy, such as pelvic inflammatory disease Patients desiring future child bearing potential Obstructions due to extrinsic compression Multispecialty Applications / Professional Use Manual 36
44 7 Lithotripsy and Percutaneous Urinary Lithotripsy For use with or without an endoscope with or without a working channel. Prior to use, physicians must be fully acquainted with lithotripsy and percutaneous lithotripsy procedures. 7.1 Indications Incision, excision, resection, ablation, coagulation, hemostasis and vaporization, with or without an endoscope, in lithotripsy and percutaneous urinary lithotripsy, including fragmentation of: Urinary calculi Urethral calculi Kidney calculi Treatment of distal impacted fragment of steinstrasse when guide wires cannot be passed 7.2 Warnings General Refer to the safety section of the operation manual for general laser-safety precautions. Multispecialty Applications / Professional Use Manual 37
HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION.
 IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT LASER AT YOUR SIDE IN YOUR HANDS is a high power holmium laser
IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT LASER AT YOUR SIDE IN YOUR HANDS is a high power holmium laser
HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT
 IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT Manufactured by Asclepion Laser Technologies GmbH LASER AT
IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT Manufactured by Asclepion Laser Technologies GmbH LASER AT
Lasers in Urology. An Evidence-Based Approach to Choosing the Right Tool
 Lasers in Urology An Evidence-Based Approach to Choosing the Right Tool Today medical lasers and specifically designed optical fibers offer benefits in a variety of surgical applications. Selecting the
Lasers in Urology An Evidence-Based Approach to Choosing the Right Tool Today medical lasers and specifically designed optical fibers offer benefits in a variety of surgical applications. Selecting the
GREENLIGHT XPS LASER THERAPY SYSTEM: A SYSTEMATIC APPROACH TO VAPORIZATION
 TM GREENLIGHT XPS LASER THERAPY SYSTEM: A SYSTEMATIC APPROACH TO VAPORIZATION Gregg R. Eure, MD, FACS Urology of Virginia Virginia Beach, Virginia GREENLIGHT XPS TM A SYSTEMATIC APPROACH TO VAPORIZATION
TM GREENLIGHT XPS LASER THERAPY SYSTEM: A SYSTEMATIC APPROACH TO VAPORIZATION Gregg R. Eure, MD, FACS Urology of Virginia Virginia Beach, Virginia GREENLIGHT XPS TM A SYSTEMATIC APPROACH TO VAPORIZATION
SAFE EFFECTIVE EASY & VERSATILE PATIENT FRIENDLY. Laser wavelength highly absorbed by H 2
 biolitec in Urology SAFE Laser wavelength highly absorbed by H 2 O Allowing contact use for tactile feedback and control Less risk of complications EFFECTIVE High success rate even in outpatient setting
biolitec in Urology SAFE Laser wavelength highly absorbed by H 2 O Allowing contact use for tactile feedback and control Less risk of complications EFFECTIVE High success rate even in outpatient setting
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
Original Article - Lasers in Urology. Min Ho Lee, Hee Jo Yang, Doo Sang Kim, Chang Ho Lee, Youn Soo Jeon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
The holmium all-rounder for urology: Expert for stone and BPH treatment
 The holmium all-rounder for urology: Expert for stone and BPH treatment About StarMedTec Our goal is to meet the demands of doctors for efficient surgical lasers that cover a wide range of therapy options.
The holmium all-rounder for urology: Expert for stone and BPH treatment About StarMedTec Our goal is to meet the demands of doctors for efficient surgical lasers that cover a wide range of therapy options.
BENIGN PROSTATIC HYPERPLASIA (BPH) affects 70%
 JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
JOURNAL OF ENDOUROLOGY Volume 14, Number 2, March 2000 Mary Ann Liebert, Inc. Holmium Laser Enucleation of the Prostate With Tissue Morcellation: Initial United States Experience JEFFREY A. MOODY, M.D.,
Benign Prostatic Hyperplasia (BPH)
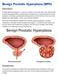 Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Benign Prostatic Hyperplasia (BPH) Definition Prostate gland enlargement is a common condition as men get older. Also called benign prostatic hyperplasia (BPH), prostate gland enlargement can cause bothersome
Lasers in Urology. Laser Tissue Interaction, November 28 th, Qureshi, Muhammad Mohsin. Biomedical in vivo Opto-scopy Laboratory
 Laser Tissue Interaction, November 28 th, 2016 Lasers in Urology Qureshi, Muhammad Mohsin Gwangju Institute of Science and Technology Biomedical in vivo Opto-scopy Laboratory 2 Content Introduction to
Laser Tissue Interaction, November 28 th, 2016 Lasers in Urology Qureshi, Muhammad Mohsin Gwangju Institute of Science and Technology Biomedical in vivo Opto-scopy Laboratory 2 Content Introduction to
TRANSURETHRAL RESECTION
 TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
TRANSURETHRAL PLASMA VAPORIZATION OF THE PROSTATE Procedure Guide
 TRANSURETHRAL PLASMA VAPORIZATION OF THE PROSTATE Procedure Guide 16299 1 PLASMA VAPORIZATION THERAPY PLASMA Vaporization PLASMA vaporization provides a safe, easy-to-use solution for TUR tissue-management
TRANSURETHRAL PLASMA VAPORIZATION OF THE PROSTATE Procedure Guide 16299 1 PLASMA VAPORIZATION THERAPY PLASMA Vaporization PLASMA vaporization provides a safe, easy-to-use solution for TUR tissue-management
Overview. Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia. Iain McAuley September 15, 2014
 Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
AURIGA. The innovative laser system for minimally invasive surgery
 AURIGA The innovative laser system for minimally invasive surgery The lasers that cover all your needs. AURIGA Wide range of laser applications Minimally invasive applications high performance AURIGA XL
AURIGA The innovative laser system for minimally invasive surgery The lasers that cover all your needs. AURIGA Wide range of laser applications Minimally invasive applications high performance AURIGA XL
P ROLIEVE. Thermodilatation System. The Prolieve System Patient Information is Directed to You, the Patient. A Transurethral Microwave Therapy Device
 P ROLIEVE Thermodilatation System A Transurethral Microwave Therapy Device The Prolieve System Patient Information is Directed to You, the Patient. Contents Why am I being treated with the Prolieve Thermodilatation
P ROLIEVE Thermodilatation System A Transurethral Microwave Therapy Device The Prolieve System Patient Information is Directed to You, the Patient. Contents Why am I being treated with the Prolieve Thermodilatation
Lasers in Gastroenterology, Otorhinolaryngology & Pulmonology
 Lasers in Gastroenterology, Otorhinolaryngology & Pulmonology Eloise Anguluan Laser-Tissue Interactions Fall Semester 2016 Gastroenterology the branch of medicine which deals with disorders of the stomach
Lasers in Gastroenterology, Otorhinolaryngology & Pulmonology Eloise Anguluan Laser-Tissue Interactions Fall Semester 2016 Gastroenterology the branch of medicine which deals with disorders of the stomach
Holmium laser enucleation of the prostate can be taught: the first learning experience
 Blackwell Science, LtdOxford, UK BJUBJU International1464-4096BJU International 909December 2002 3071 LEARNING HoLEP A. EL-HAKIM and M.M. ELHILALI 10.1046/j.1464-4096.2002.03071.x Original Article863869BEES
Blackwell Science, LtdOxford, UK BJUBJU International1464-4096BJU International 909December 2002 3071 LEARNING HoLEP A. EL-HAKIM and M.M. ELHILALI 10.1046/j.1464-4096.2002.03071.x Original Article863869BEES
Surgical Privileges Form: General surgery. Clinical Privileges Request. Date:.. Recommended (For committee use) Under Supervision
 Surgical Form: Clinical Request General surgery Applicant s Name:. License No. (If Any):... Scope of Practice:. Facility:.. Date:.. CATEGORY I: Basic Surgical skills 1. Insertion of Intravenous Line 2.
Surgical Form: Clinical Request General surgery Applicant s Name:. License No. (If Any):... Scope of Practice:. Facility:.. Date:.. CATEGORY I: Basic Surgical skills 1. Insertion of Intravenous Line 2.
Goals & Objectives by Year in Training: U-1
 Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY
 DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY NAME: DATE: Please check the box for each privilege requested. Applicants have the burden of producing information deemed adequate by
DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY NAME: DATE: Please check the box for each privilege requested. Applicants have the burden of producing information deemed adequate by
GENERAL GOALS & OBJECTIVES U-1. U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES
 GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size
 Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Benign enlargement of prostate (BEP), which is. Early Experiences with HoLEP. Original Article ABSTRACT INTRODUCTION. Bhandari BB*
 Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
Original Article Early Experiences with HoLEP Bhandari BB* * Consultant Urologist, Shree Birendra Army Hospital, Norvic International Hospital, Alka Hospital ABSTRACT introduction: Holmium Laser Enucleation
Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate
 Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
Singapore Med J 2016; 57(12): 676-680 doi: 10.11622/smedj.2016026 Early outcome of transurethral enucleation and resection of the prostate versus transurethral resection of the prostate Sundaram Palaniappan
HIGH-DEFINITION HYSTEROSCOPY FOR A HIGH STANDARD OF CARE.
 HIGH-DEFINITION HYSTEROSCOPY FOR A HIGH STANDARD OF CARE. Our next-generation TruClear hysteroscopes were designed with your technique and the patient experience in mind TruClear Elite Hysteroscope Mini
HIGH-DEFINITION HYSTEROSCOPY FOR A HIGH STANDARD OF CARE. Our next-generation TruClear hysteroscopes were designed with your technique and the patient experience in mind TruClear Elite Hysteroscope Mini
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
Be an artist of the new
 Be an artist of the new era. Dynamis Highest Performance Er:YAG and Nd:YAG Laser System Additional Surgical QCW Nd:YAG Laser Capability Complete Inside-to-Out Treatments Easy-to-Use Treatment Parameter
Be an artist of the new era. Dynamis Highest Performance Er:YAG and Nd:YAG Laser System Additional Surgical QCW Nd:YAG Laser Capability Complete Inside-to-Out Treatments Easy-to-Use Treatment Parameter
BIOPSY GUN. Delivered in sterile peel-open package. Device is made of Stainless Steel and PP material.
 BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj
 Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
Original Article Initial Experience of High Power Diode Laser for Vaporization of Prostate Muhammad Rafiq Zaki, Mujahid Hussain, Tahir Mehmood, Murtaza Hiraj Abstract Objectives: Prospective evaluation
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Holmium Laser Enucleation of the Prostate: Modified Morcellation Technique and Results
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.11.779 Voiding Dysfunction Holmium Laser Enucleation of the Prostate: Modified Morcellation Technique and Results Su Hyung Lee, Jong In Choi, Kyung
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.11.779 Voiding Dysfunction Holmium Laser Enucleation of the Prostate: Modified Morcellation Technique and Results Su Hyung Lee, Jong In Choi, Kyung
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
China Medical Technologies, Inc.
 China Medical Technologies, Inc. China Medical Technologies, Inc. (CMT) is a high-tech enterprise, trading on Nasdaq with the ticker CMED. We currently conduct our operations principally through our wholly-owned
China Medical Technologies, Inc. China Medical Technologies, Inc. (CMT) is a high-tech enterprise, trading on Nasdaq with the ticker CMED. We currently conduct our operations principally through our wholly-owned
Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 )
 Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
RATIONALE: The organs making up the urinary system consist of the kidneys, bladder, urethra, and ureters.
 Chapter 12 Section Review 12.1 1. A. Kidneys RATIONALE: The renal pelvis receives urine from the kidney, travels through the ureters on the way to the bladder, but urine is formed in the kidney. 2. C.
Chapter 12 Section Review 12.1 1. A. Kidneys RATIONALE: The renal pelvis receives urine from the kidney, travels through the ureters on the way to the bladder, but urine is formed in the kidney. 2. C.
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
3% Sorbitol Urologic Irrigating Solution in UROMATIC Plastic Container
 3% Sorbitol Urologic Irrigating Solution in UROMATIC Plastic Container Description 3% Sorbitol Urologic Irrigating Solution is a sterile, nonpyrogenic, nonhemolytic, electrically nonconductive solution
3% Sorbitol Urologic Irrigating Solution in UROMATIC Plastic Container Description 3% Sorbitol Urologic Irrigating Solution is a sterile, nonpyrogenic, nonhemolytic, electrically nonconductive solution
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Bladder Case # 1. Principal Diagnosis: Bladder Tumor, Suspect Transitional Cell Carcinoma. Secondary Diagnoses: 1. Hypertension. 2. Hyperlipidemia.
 DISCHARGE SUMMARY Bladder Case # 1 Date: 04/22/2010 Principal Diagnosis: Bladder Tumor, Suspect Transitional Cell Carcinoma. Secondary Diagnoses: 1. Hypertension. 2. Hyperlipidemia. Hospital Course: Mr.
DISCHARGE SUMMARY Bladder Case # 1 Date: 04/22/2010 Principal Diagnosis: Bladder Tumor, Suspect Transitional Cell Carcinoma. Secondary Diagnoses: 1. Hypertension. 2. Hyperlipidemia. Hospital Course: Mr.
Submitted: August 15, Accepted: September 10, Published: October 15, 2018.
 Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
Original Article doi: 10.22374/jeleu.v1i2.21 THULIUM LASER ENUCLEATION OF THE PROSTATE (THULEP) AS A TECHNIQUE FOR TREATMENT OF BPH: EVALUATION OF A SIX-YEAR EXPERIENCE AT A SINGLE INSTITUTION Mahmood
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
Issue Number: 0157 Date: 10/01/219
 Bulletin Changes to CCSD Schedule of Procedures Issue Number: 0157 Date: 10/01/219 The CCSD has reviewed requests to the CCSD Procedure Schedule for the months of December/January and has agreed on the
Bulletin Changes to CCSD Schedule of Procedures Issue Number: 0157 Date: 10/01/219 The CCSD has reviewed requests to the CCSD Procedure Schedule for the months of December/January and has agreed on the
Surgical Treatment of LUTS in Men with BPE
 Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Laser Applications in Dermatology & Orthopedics
 20161205 Laser Applications in Dermatology & Orthopedics Solchan Chung Advisor: prof. Jae Young Lee Biomimetic Materials Lab SMSE, GIST Dermatology 2 - Dermatology is the branch of medicine dealing with
20161205 Laser Applications in Dermatology & Orthopedics Solchan Chung Advisor: prof. Jae Young Lee Biomimetic Materials Lab SMSE, GIST Dermatology 2 - Dermatology is the branch of medicine dealing with
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH
 Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH The more you know, the better you ll feel. You ve likely had a discussion with your doctor about BPH 1. What follows are some
Control & confidence. You deserve both.
 Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
Learn more about BPH and Plasma therapy Control & confidence. You deserve both. YOUR GUIDE TO THE TREATMENT OF BPH Your doctor is always happy to offer all the guidance you need so that you feel completely
UNM SRMC UROLOGY CLINICAL PRIVILEGES.
 o o o Initial privileges (initial appointment) Renewal of privileges (reappointment) Expansion of privileges (modification) INSTRUCTIONS All new applicants must meet the following requirements as approved
o o o Initial privileges (initial appointment) Renewal of privileges (reappointment) Expansion of privileges (modification) INSTRUCTIONS All new applicants must meet the following requirements as approved
Holmium:YAG Laser for Treatment of Strictures of Vesicourethral Anastomosis after Radical Prostatectomy
 JOURNAL OF ENDOUROLOGY Volume 19, Number 4, May 2005 Mary Ann Liebert, Inc. Holmium:YAG Laser for Treatment of Strictures of Vesicourethral Anastomosis after Radical Prostatectomy BRUNOLF W. LAGERVELD,
JOURNAL OF ENDOUROLOGY Volume 19, Number 4, May 2005 Mary Ann Liebert, Inc. Holmium:YAG Laser for Treatment of Strictures of Vesicourethral Anastomosis after Radical Prostatectomy BRUNOLF W. LAGERVELD,
AccuracyMatters. Ultrasonic surgical aspiration system
 AccuracyMatters Ultrasonic surgical aspiration system High performance tissue ablation Vessel sparing, soft and hard tissue removal Adaptive radio frequency coagulation capability Easy to set up and break
AccuracyMatters Ultrasonic surgical aspiration system High performance tissue ablation Vessel sparing, soft and hard tissue removal Adaptive radio frequency coagulation capability Easy to set up and break
What is Laparoscopy All About?
 Disclaimer This movie is an educational resource only and should not be used to manage surgical health. All decisions about the management of Laparoscopy must be made in conjunction with your Physician
Disclaimer This movie is an educational resource only and should not be used to manage surgical health. All decisions about the management of Laparoscopy must be made in conjunction with your Physician
Lotus transducer Instructions for use
 Lotus transducer Instructions for use Instructions for use transducer Before using the product, please read the following information thoroughly Important This document provides instructions for using
Lotus transducer Instructions for use Instructions for use transducer Before using the product, please read the following information thoroughly Important This document provides instructions for using
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Treating BPH: Comparing Rezum UroLift and HoLEP
 Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
Treating BPH: Comparing Rezum UroLift and HoLEP Scott M. Cheney MD Mayo Clinic Arizona 2018 MFMER slide-1 Welcome to AZ 2018 MFMER slide-2 Outline Background on BPH, Rezum, Urolift, HoLEP AUA Guideline
PHOTOSELECTIVE POTASSIUM-TITANYL-PHOSPHATE LASER VAPORIZATION OF THE BENIGN OBSTRUCTIVE PROSTATE: OBSERVATIONS ON LONG-TERM OUTCOMES
 0022-5347/05/1744-1344/0 Vol. 174, 1344 1348, October 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000173913.41401.67 PHOTOSELECTIVE
0022-5347/05/1744-1344/0 Vol. 174, 1344 1348, October 2005 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2005 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000173913.41401.67 PHOTOSELECTIVE
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
MODULE 3: BENIGN PROSTATIC HYPERTROPHY
 MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
MODULE 3: BENIGN PROSTATIC HYPERTROPHY KEYWORDS: Prostatic hypertrophy, prostatic hyperplasia, PSA, voiding dysfunction, lower urinary tract symptoms (LUTS) At the end of this clerkship, the medical student
Thulium Laser versus Standard Transurethral Resection of the Prostate: A Randomized Prospective Trial
 european urology 53 (2008) 382 390 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Obstruction Thulium Laser versus Standard Transurethral Resection of the
european urology 53 (2008) 382 390 available at www.sciencedirect.com journal homepage: www.europeanurology.com Benign Prostatic Obstruction Thulium Laser versus Standard Transurethral Resection of the
Historical perspective
 Raj Santharam, MD GI Associates, LLC Clinical Assistant Professor of Medicine Medical College of Wisconsin Historical perspective FFS first widespread use in the early 1970 s Expansion of therapeutic techniques
Raj Santharam, MD GI Associates, LLC Clinical Assistant Professor of Medicine Medical College of Wisconsin Historical perspective FFS first widespread use in the early 1970 s Expansion of therapeutic techniques
October Cover Story: Less invasive surgeries are benefiting patients
 October Cover Story: Less invasive surgeries are benefiting patients From trauma surgeries to liposuction, Backus Hospital offers state-of-the-art minimally invasive techniques throughout many disciplines.
October Cover Story: Less invasive surgeries are benefiting patients From trauma surgeries to liposuction, Backus Hospital offers state-of-the-art minimally invasive techniques throughout many disciplines.
Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam
 Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam By Sarmad Aji, MD., FACS. A comprehensive review of the most commonly asked questions on the American Board of Surgery
Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam By Sarmad Aji, MD., FACS. A comprehensive review of the most commonly asked questions on the American Board of Surgery
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Transurethral Laser Technology: Treatments for BPH
 Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
Transurethral Laser Technology: Treatments for BPH Richard Lee, MD Departments of Urology and Public Health The New York Presbyterian Hospital Weill Medical College of Cornell University Background Traditional
Transurethral Resection of the Prostate (TURP) Transurethral Incision of the Prostate (TUIP) PROCEDURE EDUCATION LITERATURE
 Transurethral Resection of the Prostate (TURP) Transurethral Incision of the Prostate (TUIP) PROCEDURE EDUCATION LITERATURE We recommend that you read this handout carefully in order to prepare yourself
Transurethral Resection of the Prostate (TURP) Transurethral Incision of the Prostate (TUIP) PROCEDURE EDUCATION LITERATURE We recommend that you read this handout carefully in order to prepare yourself
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
In any operation. Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications.
 In any operation Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications. Abdominal operation I position for operation Supine Abdominal operation I position for
In any operation Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications. Abdominal operation I position for operation Supine Abdominal operation I position for
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Laparoscopic & Robotic Surgery in Pancreas Disease
 2007 년도대한췌담도학회추계학술대회 Session IV: Recent Updates in Pancreatobiliary Diseases Laparoscopic & Robotic Surgery in Pancreas Disease Department of Surgery, Yonsei University College of Medicine, Korea Woo-Jung
2007 년도대한췌담도학회추계학술대회 Session IV: Recent Updates in Pancreatobiliary Diseases Laparoscopic & Robotic Surgery in Pancreas Disease Department of Surgery, Yonsei University College of Medicine, Korea Woo-Jung
Chapter 47 1/8/2018. Urinary System Disorders. Urinary Tract Infections. Treatment
 Chapter 47 Urinary System Disorders Urinary Tract Infections Urinary tract infections (UTIs) are common Infection in one area can involve the entire system Microbes enter through the urethra. Catheterization,
Chapter 47 Urinary System Disorders Urinary Tract Infections Urinary tract infections (UTIs) are common Infection in one area can involve the entire system Microbes enter through the urethra. Catheterization,
Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011
 Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Urologic AMPUTATION OF PENIS Table 1 BIOPSY BLADDER Table 1 BIOPSY PENILE Table 1 BIOPSY URETERAL LESION Table 1 BLADDER DIVERTICULECTOMY
Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Urologic AMPUTATION OF PENIS Table 1 BIOPSY BLADDER Table 1 BIOPSY PENILE Table 1 BIOPSY URETERAL LESION Table 1 BLADDER DIVERTICULECTOMY
Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms
 Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Directions For Use. All directions should be read before use
 Directions For Use All directions should be read before use DEVICE DESCRIPTION: The CLEANER.XT Rotational Thrombectomy System is a percutaneous, 6Fr catheter based system (single piece construction) that
Directions For Use All directions should be read before use DEVICE DESCRIPTION: The CLEANER.XT Rotational Thrombectomy System is a percutaneous, 6Fr catheter based system (single piece construction) that
The SplitWire Percutaneous Transluminal Angioplasty Scoring Device. Instructions for Use
 The SplitWire Percutaneous Transluminal Angioplasty Scoring Device Instructions for Use Contents Contains one (1) SplitWire device. Sterile. Sterilized with ethylene oxide gas. Radiopaque. For single use
The SplitWire Percutaneous Transluminal Angioplasty Scoring Device Instructions for Use Contents Contains one (1) SplitWire device. Sterile. Sterilized with ethylene oxide gas. Radiopaque. For single use
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
Index Note: Page numbers of article titles are in boldface type. A Ablation, of prostate, holmium laser, 485 495 African prune tree (Pygeum africanum), 454 455 Alfuzosin, 445 446 Alpha-adrenergic agonists,
PATIENT SELECTION GUIDE. finding the right fit
 PATIENT SELECTION GUIDE finding the right fit IDENTIFYING PATIENTS Rezūm, a new minimally invasive treatment, is now available to offer patients as a first-line BPH therapy. BPH TREATMENT OPTIONS Behavior
PATIENT SELECTION GUIDE finding the right fit IDENTIFYING PATIENTS Rezūm, a new minimally invasive treatment, is now available to offer patients as a first-line BPH therapy. BPH TREATMENT OPTIONS Behavior
Agenda of Product Presenta0on. I. Introduc*on II. Laser Physics III. Key Advantages IV. Clinical Data V. Key Takeaways
 Agenda of Product Presenta0on I. Introduc*on II. Laser Physics III. Key Advantages IV. Clinical Data V. Key Takeaways 1 Applica0ons of DIOLAS LFD 3000 at a Glance Benign Prostatic Hyperplasia (BPH) Destruction
Agenda of Product Presenta0on I. Introduc*on II. Laser Physics III. Key Advantages IV. Clinical Data V. Key Takeaways 1 Applica0ons of DIOLAS LFD 3000 at a Glance Benign Prostatic Hyperplasia (BPH) Destruction
Reproduced with the kind permission of Health Press Ltd, Oxford
 Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Biodegradable spacer insertion to reduce rectal toxicity during radiotherapy for prostate cancer
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Biodegradable spacer insertion to reduce rectal toxicity during radiotherapy for prostate cancer Radiotherapy
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Biodegradable spacer insertion to reduce rectal toxicity during radiotherapy for prostate cancer Radiotherapy
Executive Summary. Non-drug local procedures for treatment of benign prostatic hyperplasia 1. IQWiG Reports - Commission No.
 IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
IQWiG Reports - Commission No. N04-01 Non-drug local procedures for treatment of benign prostatic hyperplasia 1 Executive Summary 1 Translation of the executive summary of the final report Nichtmedikamentöse
Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano
 Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
Dipartimento di Urologia Direttore Prof. Giorgio Guazzoni Mini-Invasive Treatment in Urological Diseases Dott. Alberto Saita Responsabile Endourologia Istituto Clinico Humanitas - Rozzano alberto.saita@humanitas.it
The SUM Program for Medical Transcription Training Career Development Series: Interpreting Anatomic Pathology Dictation
 The SUM Program for Medical Transcription Training Career Development Series: Interpreting Anatomic Pathology Dictation Table of Contents INTRODUCTION Anatomic Pathology by John H. Dirckx, M.D. Exercises
The SUM Program for Medical Transcription Training Career Development Series: Interpreting Anatomic Pathology Dictation Table of Contents INTRODUCTION Anatomic Pathology by John H. Dirckx, M.D. Exercises
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Transurethral Resection of Prostate (TURP)
 Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
For Reference Only GENERAL SURGERY 2013
 Summary of Services and Availability (by location) Each location has sufficient space, equipment, staffing and financial resources in place or available in sufficient time as required to support each requested
Summary of Services and Availability (by location) Each location has sufficient space, equipment, staffing and financial resources in place or available in sufficient time as required to support each requested
Cook Europe Shared Service Centre
 www.cookmedical.com Cook Europe Shared Service Centre Country Telephone E-mail Austria (+43) 1-795-67-121 oeorders@cook.ie Belgium ench (+32) 27-00-16-33 beorders@cook.ie Belgium Flemish (+32) 27-00-16-33
www.cookmedical.com Cook Europe Shared Service Centre Country Telephone E-mail Austria (+43) 1-795-67-121 oeorders@cook.ie Belgium ench (+32) 27-00-16-33 beorders@cook.ie Belgium Flemish (+32) 27-00-16-33
Name of Policy: Transurethral Microwave Thermotherapy
 Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Name of Policy: Transurethral Microwave Thermotherapy Policy #: 449 Latest Review Date: September 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Biodegradable spacer insertion to reduce rectal toxicity during radiotherapy for prostate cancer
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Biodegradable spacer insertion to reduce rectal toxicity during radiotherapy for prostate cancer Radiotherapy
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Biodegradable spacer insertion to reduce rectal toxicity during radiotherapy for prostate cancer Radiotherapy
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
ENDOBRONCHIAL ABLATIVE THERAPIES. Christopher Cortes, MD, FPCCP
 ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
Emergency Medicine Scope of Practice
 Emergency Medicine Scope of Practice All Physician Assistants working in Emergency Medicine will encounter a wide variety of non acute, urgent and emergent patient complaints and conditions. Given the
Emergency Medicine Scope of Practice All Physician Assistants working in Emergency Medicine will encounter a wide variety of non acute, urgent and emergent patient complaints and conditions. Given the
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
Instruction for Use of 3-stage Dilation Balloon Catheter JS-CE-SM-08-01, A/0
 Instruction for Use of 3-stage Dilation Balloon Catheter JS-CE-SM-08-01, A/0 Instruction for Use of 3-stage Dilation Balloon Catheter Product name 3-stage Dilation Balloon Catheter Product structure and
Instruction for Use of 3-stage Dilation Balloon Catheter JS-CE-SM-08-01, A/0 Instruction for Use of 3-stage Dilation Balloon Catheter Product name 3-stage Dilation Balloon Catheter Product structure and
