Pectus excavatum is a chest wall deformity characterized
|
|
|
- Julian Ryan
- 5 years ago
- Views:
Transcription
1 Minimally Invasive Repair for Pectus Excavatum in Adults Swee H. Teh, MD, Angela M. Hanna, MD, Tuan H. Pham, MD, PhD, Adriana Lee, MD, Claude Deschamps, MD, Penny Stavlo, RN, and Christopher Moir, MD Divisions of Pediatric Surgery and Thoracic Surgery, Mayo Clinic, Rochester, Minnesota Background. The purpose of this study is to review the minimally invasive pectus excavatum repair in adults to determine the safety and effectiveness. Methods. An Institutional Review Board approved chart review identified patients 17 years or older who underwent minimally invasive pectus excavatum repair (MIPER) between January 1999 and January Results. Nineteen patients underwent MIPER. Indications for surgery were reduced exercise tolerance (13), dyspnea on exertion (17), improve self-perception (10), and chest pain (6). There were no intraoperative complications or conversions to open repair. Twelve patients (63%) required one strut and seven patients (37%) required two struts. Postoperative complications included self-resolving asymptomatic pneumothorax in six patients and pneumonia in one. Pain at six weeks postoperatively was mild to none in most patients and all had no pain at three months postoperatively except one patient with strut displacement. Two patients required removal of one of two struts due to displacement. The mean postoperative pectus index was significantly lower than preoperative value: 2.5 versus 4.6, p Among six patients with strut removal at two years postoperatively, two patients had mild recurrence of their deformity. Conclusions. Minimally invasive pectus excavatum repair can be performed safely in adults. This approach is technically more challenging in adults with one-third of the patients requiring two struts for optimal repair. The risk of strut displacement is higher than in the pediatric population. The long-term effectiveness and durability of this procedure in adults is still unknown. (Ann Thorac Surg 2008;85:1914 8) 2008 by The Society of Thoracic Surgeons Pectus excavatum is a chest wall deformity characterized by posterior displacement of the sternum. The etiology of this deformity is poorly understood. Most patients have the deformity throughout their childhood life and it worsens during the teenage growth spurt. Surgical correction offers a favorable outcome. Among the surgical approaches described, the minimally invasive pectus excavatum repair (MIPER) has recently received much attention, especially in children [1]. Many patients, however, enter into adulthood with persistence of their pectus excavatum deformity. There are limited reports on the suitability of this minimally invasive repair technique for young adults. The aim of this study is to review a single institution experience with adult repair to determine the safety and effectiveness of the minimally invasive approach. Material and Methods Patients and Data An Institutional Review Board approved retrospective review was performed to identify patients who were 17 years old or greater and underwent MIPER between January 1999 and January Individual consent for the Accepted for publication March 5, Address correspondence to Dr Moir, Mayo Clinic Rochester, Division of Pediatric Surgery, 200 Second Street SW, Rochester, MN 55905; moir.christopher@mayo.edu. study was waived because it was a retrospective review. Data on general demographics, clinical presentation, radiologic studies, severity of the deformity, surgical procedure, perioperative morbidity and mortality, and success of pectus repair were tabulated from detailed chart review. The severity of the deformity was assessed by the pectus index, the ratio of transverse diameter of the chest to the anteroposterior distance as measured from the anterior border of the vertebral body to the posterior border of the sternum [2]. This was assessed either by chest X-ray or computed tomographic computed tomographic scan. Pectus index of greater than 3 is classified as severe deformity. Indications for surgery were reduced exercise tolerance, dyspnea on exertion, poor self-perception, and chest pain (6). Operative Technique Preoperatively, thoracic epidural catheter was inserted for pain management. After induction of general anesthesia, a transverse skin marking was made outlining the anticipated placement of the strut bar to correct the pectus deformity. At the midclavicular point of the skin marking, a3to4cmtransverse skin incision was made bilaterally. Using electrocautery and blunt dissection, subcutaneous pockets around the incision were created just above the chest wall musculature. A trocar fitting a 5-mm thorascopic camera was inserted into the right hemithorax through the right inferolateral chest wall incision. Carbon 2008 by The Society of Thoracic Surgeons /08/$34.00 Published by Elsevier Inc doi: /j.athoracsur
2 Ann Thorac Surg TEH ET AL 2008;85: MIPER IN ADULTS dioxide insufflation to 6 mm Hg was administered through the trocar to partially deflate the right lung. Through the midclavicular transverse incision, and under direct thorascopic camera visualization, the right thoracic cavity was entered bluntly using either a large aortic aneurysmal clamp or pectus dissector instrument (Walter Lorenz Surgical, Jacksonville, FL). Again under direct vision from the thorascopic camera, the aneurysmal clamp or pectus dissector was tunneled across the sternum to the left hemithorax, and its tip bluntly exited the left hemithorax through the left midclavicular incision. An umbilical tape was secured to the aneurysmal clamp or pectus dissector. The clamp or dissector was withdrawn, and this resulted in tunneling of the umbilical tape from left to right. A strut, which was custom fashioned by hand intraoperatively to fit each individual s chest conformation and pectus defect, was secured to the right end of the umbilical tape. Guided by the umbilical tape, the strut was passed through the thorax from the right to the left incision in a concave-up position. The strut was flipped to a concave-down position to buttress the sternum and correct the pectus deformity. Once the strut is positioned to properly correct the deformity, it is secured to the chest wall with 0-prolene or wire sutures tied around the rib to anchor the bar to the rib. Many patients were identified preoperatively for two struts based on the severity of their deformity in addition to their age. Intraoperatively, if one strut did not correct the deformity satisfactorily then a second strut was placed either superior or inferior to the first bar in an identical fashion. Air in the chest cavity was evacuated by applying suction through the trocar as well as by giving the patient a few large tidal breaths. An immediate postoperative chest X-ray was performed to ascertain proper strut position as well as residual pneumothorax. Postoperative pain management was achieved through a combination of epidural, intravenous, and oral analgesics. Epidural was continued for the first 72 hours. Patient control analgesia was started when deemed necessary. Patients were dismissed from hospital when they were able to tolerate postoperative pain with oral analgesia, including nonsteroidal antiinflammatory drugs (ie, ibuprofen), acetaminophen, and oxycodone. Statistical Method Statistical analyses were performed using the JMP statistical package (JMP Software, Cary, NC). The paired Student t test was used to evaluate for statistical difference between groups, where a p value less than 0.05 was considered statistically significant. Standard error of the mean ( SE) is used to express value uncertainty, unless specified otherwise. Results Nineteen patients underwent minimally invasive pectus excavatum repair during the study period. There were 11 men and 8 women presenting at a mean age of 19.5 years (age 17, n 9; 18, n 3; 19, n 2; 20, n 1; 21, n 3; 42, 1915 Fig 1. Severity of pain at six weeks after minimally invasive repair of pectus excavatum in 19 adults. n 1.) The mean preoperative pectus index was (range, 3.2 to 15). The indications for surgery were reduced exercise tolerance (13), dyspnea on exertion (17), poor self-perception (10), and chest pain (6). Preoperative workup included pulmonary function tests in 12 patients, which revealed mild restrictive patterns but no major abnormalities, and echocardiogram in 4 patients, which were all normal. No patients had signs or symptoms of Marfan syndrome or other connective tissue disorders. Two patients had recurrence of the deformity after open repair elsewhere. One patient had an open repair at the age of 9 and developed relapse one year later with worsening chest pain. The other patient had open repair of his pectus excavatum at age 5 but had a recurrent deformity several years later with associated symptoms of dyspnea on exertion and chest pain. Both patients underwent minimally invasive repair for the excavatum at age 17 at our institution. Minimally invasive pectus excavatum repair was successfully performed in all patients. There were no intraoperative complications, and no patient required conversion to an open repair or blood transfusion. The mean operative time was hours (range, 1.0 to 5.16 hours), 63% (12 patients) required one strut and 37% (7 patients) required two struts in order to properly correct for the deformity. There were no perioperative deaths. One patient developed pneumonia and six patients were noted to have asymptomatic residual pneumothorax that resolved without chest tube placement. Thoracic epidural and oral analgesia, as described above satisfactorily controlled immediate postoperative pain. All patients reached satisfactory pain relief by oral analgesia prior to hospital dismissal. The mean hospital stay was 5.8 days (range, 4 to 8 days). At six weeks after surgery, all patients were evaluated with clinical exam and chest X-ray. Pain at six weeks postoperative was significant in four, moderate in four, mild in six, and none in five patients (Fig 1). Two of the GENERAL THORACIC
3 1916 TEH ET AL Ann Thorac Surg MIPER IN ADULTS 2008;85: Fig 2. Plot of the mean preoperative versus mean postoperative pectus index in all 19 adult patients who underwent minimally invasive pectus excavatum repair. four patients with significant pain were due to strut displacement. These two patients required premature removal of one of the two struts at one and seven months postoperatively. At three months postoperatively, all patients were pain free except one whose pain was secondary to strut displacement. Based on self-reporting, patients were satisfied with the results, where all the repairs were evaluated as good to excellent at mean follow-up of 27 months (range, 3 to 71 months). All 13 patients who had reduced exercise tolerance preoperatively reported improvement of the cardiorespiratory symptoms postoperatively. By objective measure, the mean postoperative pectus index was significantly lower as compared with the mean preoperative value: 2.5 versus 4.58, p (Fig 2). Six of the nineteen patients had their bar removed at the end of two years. Among these, 33% (two patients) were noted to have a mild recurrence of their pectus deformity. The first patient was an 18-year-old symptomatic female with a preoperative pectus index of 3.3 that improved postoperatively to 2.7. On follow-up at 13 months after strut removal, her pectus index had progressed from 2.7 to 2.9. This patient did opt for a redo repair, which due to adhesions and difficulty was converted to an open procedure. The second patient was a 19-year-old male whose preoperative pectus index was 3.9 and his postoperative pectus index was improved to 2.5. He had a progression of his pectus index to 2.68 at 16 months after strut removal. The other four patients were followed for a mean of six months without evidence of recurrence. Comment Pectus excavatum is often associated with children. When repair is not pursued or failed during childhood, the deformity persists into adulthood. Surgical repair is frequently delayed until after the teenage growth spurt when the chest wall growth decreases and the risk of recurrence is minimized. The deformity may cause several clinical symptoms that range from chest discomfort and reduced exercise tolerance to social withdrawal due to poor self-perception [3, 4]. Surgical repair of this deformity in early adulthood may offer the best corrective measure and has a lower hypothetical risk of recurrence because chest wall growth is minimal during this period. The surgical treatment of pectus excavatum has changed considerably in the last several decades, ranging from the open repair to the recently described minimally invasive technique known as the Nuss procedure [5]. The effectiveness of this procedure is based on the premise that the chest wall possesses the capability of remodeling and reconfiguration. The Nuss procedure has received much attention as it is minimally invasive, safe, avoids cartilage resection, has a shorter operating time, is highly effective in children, and offers excellent results in more than 90% of patients [5 7]. This procedure also improves the patient s self-perception and quality of life [4]. There are limited data to support the role of this repair in early adult patients with pectus excavatum. In one report by Coln and colleagues [8], eight patients aged 19 to 32 years underwent the Nuss procedure based on a chest wall index greater 3.25 or cardiac abnormalities identified on echocardiography. Only one bar was used in these patients with one to two lateral stabilizing bars. Mean operative time was 1.32 hours, mean hospital stay was four days, and pain medication was stopped between two and four weeks postoperatively in all patients except two who continued narcotics for two and four months. Late complications included one separation of a stabilizer bar requiring reoperation, and one bar displacement requiring reoperation. Follow-up was a mean of 22.1 months, and only four patients had undergone bar removal after one to two years. In these patients there was a good result with no loss of correction in a mean follow-up of 9.7 months after bar removal. The series is small with a short follow-up but shows good early results using only one bar that is removed after one to two years. Another series by Kim and colleagues [9] compared the results of the Nuss procedure in three different age groups: pediatrics less than 12 years (n 27), adolescents 12 to 20 years (n 12), and adults greater than 20 years (n 12). A pectus index greater than 3.0 was an indication for operation, in addition to recurrent pneumonia, arrhythmia, and dyspnea on exertion. In adolescents, three patients had one bar placed while nine had two bars and lateral stabilizers were used in ten patients. In adults, all patients but one had two bars placed and all had lateral stabilizers. Mean operative times were longer in the adolescent, and more so in the adult populations where the mean operative time was minutes. Additionally, mean hospital stay was increased, at days for adolescents and days for adults. In adults, 54.5% had chest pain for more than six months after the operation, one of whom ultimately underwent bar removal due to pain. Postoperative complications in the adolescent and adult groups were 58.3% in each
4 Ann Thorac Surg TEH ET AL 2008;85: MIPER IN ADULTS group, with bar rotation in 8.3% of adolescents and 33.3% of adults, one of whom ultimately underwent a Ravitch procedure for correction. There were three wound infections, where two patients developed empyema as a result necessitating bar removal, and one who required bar repositioning and musculocutaneous flap. Nine adolescents and four adults had bars removed at a mean of months. After bar removal, a follow up of months showed that all adolescents and adults had sustained results. The authors concluded that the bar displacement in adolescents is acceptable; however, in adults, even though post bar removal results are good, due to a high incidence of complications and reoperation the procedure is not recommended. Our series has demonstrated that this minimally invasive repair is indeed safe in adult patients without major operative morbidity. The operative duration is longer compared with children [6, 7]. Our mean operative time was 2.1 hours, mildly increased compared with the other reports in adults [9, 10]; however, there were two patients whose operative times were 5.07 and 5.16 hours. The first patient had undergone a previous open Ravitch repair, making dissection tedious and difficult. The second patient had a severe and lengthy deformity eventually requiring intraoperative placement of two struts to correct the angulation. The common immediate postoperative complications encountered in children were similarly seen in the adult population [1, 9, 10]. In our population, all pneumothoraces were small, limited, and resolved without chest tube placement. Postoperative pain could be managed effectively with epidural analgesia and subsequently with the combination of opiate and nonsteroidal antiinflammatory drugs. Of note, the postoperative pain was more marked in our adult patients as compared with children, where 21.1% of the patients still experienced a significant amount of intermittent pain at six weeks postoperative. This range is consistent with the previous reports in the adult population [9, 10]. The etiology of the continued pain in two of the four patients was secondary to strut displacement. The pain resolved when one of their two struts was removed surgically. It is also likely that in adults the chest wall is stiffer, harder to reconfigure by the strut, and therefore results in more pain. We also demonstrated that the pectus excavatum was successfully corrected in all patients with the minimally invasive technique, including two patients who had a recurrence from a failed open repair [10]. Seven of 19 patients (37%) required two struts for optimal correction. Many patients were considered to be candidates preoperatively for two struts based on the severity of their deformity in addition to their age. However, the final decision for two struts was made intraoperatively if one strut did not correct the deformity satisfactorily. Two of the seven patients experienced the complication of strut displacement causing significant pain and in these cases one strut was removed prematurely. We hypothesize that the higher complication rate encountered in patients who had two struts might be due to selection bias as these patients have a greater cephalocaudal axis extent of their 1917 deformity. The insertion of the second strut increased the risk of suboptimal contact of one of the bars to the undersurface of the sternum. This allowed some degree of mobility in the strut that has a suboptimal strut-sternal contact. Nuss and colleagues [5] also note that strut displacement occurs in 15% of patients without a stabilizer, 6% of patients with a stabilizer but without wiring, and only in 5% of patients with wiring of the stabilizer [1, 5]. Therefore, stabilizing techniques used in adults must be reinforced with wiring of the stabilizer. We used a technique similar to the wire-fixation technique where we tied the bar around the rib without a stabilizer. This was done in all but two patients, one who was early on in our experience before we incorporated this technique, and the other had undergone previous open Ravitch repair and we felt the bar had better stabilization with a stabilizer bar. The wire-fixation technique may be less costly, more time efficient, safer, and more effective to perform in children; however, it may not be suitable for adults with a stronger physique and severe pectus deformity. Typically bars have been left in place for two years. Among our patients, six of nineteen have had their bars removed, all as completion of the operation. Two of these patients have been noted to have a mild recurrence, one at one week and one at 16 months post strut removal. The first patient eventually underwent a redo repair that converted to an open procedure secondary to adhesions. The second patient had remained asymptomatic and has not required reoperation. As the result of this finding, we now have been opting to leave the strut in longer, up to three years. Most patients with severe pectus excavatum experience reduced exercise tolerance, dyspnea on exertion with shifting of the cardiac chambers, and compression of the heart marked radiologically [11]. It has been postulated that the respiratory symptoms seen in patients with pectus excavatum are secondary from alteration of the cardiac physiology during exercise. Zhao and colleagues [12] demonstrated that the exercise capacity during an upright position in these patients is affected by reduced venous filling of the heart and therefore results in reduction of stroke volume and peak oxygen uptake. Our series had 13 patients who reported reduced exercise tolerance, 17 reported dyspnea on exertion, and 6 complained of chest pain. Twelve patients underwent standard pulmonary function tests, which some reported mild restrictive patterns but did not reveal significant abnormality. Four patients were evaluated with an echocardiogram, all of which were normal. All of our 13 patients with reduced exercise tolerance preoperatively had resolved cardiopulmonary symptoms postoperatively, which is corroborated by other studies [9 11, 13, 14]. Minimally invasive pectus excavatum repair can be performed safely in adult patients. The operative and recovery time is longer and up to one third of adult patients may need a second strut to optimize the repair. The risk of strut displacement is higher than in children especially when a second strut is placed. We observed significant recurrence rate of the deformity in adults if the strut was removed in two years. Therefore, in this GENERAL THORACIC
5 1918 TEH ET AL Ann Thorac Surg MIPER IN ADULTS 2008;85: patient population, we are now leaving struts in for three years. Overall, the long-term effectiveness and durability of this procedure in adults is still unknown and longer follow-up is needed. References 1. Nuss D, Croitoru DP, Kelly RE Jr, Goretsky MJ, Nuss KJ, Gustin TS. Review and discussion of the complications of minimally invasive pectus excavatum repair. Eur J Pediatr Surg 2002;12: Daunt SW, Cohen JH, Miller SF. Age-related normal ranges for the Haller index in children. Pediatr Radiol 2004;34: Hebra A, Swoveland B, Egbert M, et al. Outcome analysis of minimally invasive repair of pectus excavatum: review of 251 cases. J Pediatr Surg 2000;35: Lawson ML, Cash TF, Akers R, et al. A pilot study of the impact of surgical repair on disease-specific quality of life among patients with pectus excavatum. J Pediatr Surg 2003; 38: Nuss D, Kelly RE Jr, Croitoru DP, Katz ME. A 10-year review of a minimally invasive technique for the correction of pectus excavatum. J Pediatr Surg 1998;33: Hosie S, Sitkiewicz T, Petersen C, et al. Minimally invasive repair of pectus excavatum--the Nuss procedure. A European multicentre experience. Eur J Pediatr Surg 2002;12: Miller KA, Woods RK, Sharp RJ, et al. Minimally invasive repair of pectus excavatum: a single institution s experience. Surgery 2001;130: Coln D, Gunning T, Ramsay M, Swygert T, Vera R. Early experience with the Nuss minimally invasive correction of pectus excavatum in adults. World J Surg 2002;26: Kim do H, Hwang JJ, Lee MK, Lee DY, Paik HC. Analysis of the Nuss procedure for pectus excavatum in different age groups. Ann Thorac Surg 2005;80: Miller KA, Ostlie DJ, Wade K, et al. Minimally invasive bar repair for redo correction of pectus excavatum. J Pediatr Surg 2002;37: Beiser GD, Epstein SE, Stampfer M, Goldstein RE, Noland SP, Levitsky S. Impairment of cardiac function in patients with pectus excavatum, with improvement after operative correction. N Engl J Med 1972;287: Zhao L, Feniberg MS, Gaides M, Ben-Dov I. Why is exercise capacity reduced in subjects with pectus excavatum? J Pediatr 2000;136: Quigley PM, Haller JA Jr, Jelus KL, Loughlin GM, Marcus CL. Cardiorespiratory function before and after corrective surgery in pectus excavatum. J Pediatr 1996;128(5 Pt 1): Haller JA Jr, Loughlin GM. Cardiorespiratory function is significantly improved following corrective surgery for severe pectus excavatum. Proposed treatment guidelines. J Cardiovasc Surg (Torino) 2000;41: Notice From the American Board of Thoracic Surgery Regarding Trainees and Candidates for Certification Who Are Called to Military Service Related to the War on Terrorism The Board appreciates the concern of those who have received emergency calls to military service. They may be assured that the Board will exercise the same sympathetic consideration as was given to candidates in recognition of their special contributions to their country during the Vietnam conflict and the Persian Gulf conflict with regard to applications, examinations, and interruption of training. If you have any questions about how this might affect you, please call the Board office at (312) Richard H. Feins, MD Chair The American Board of Thoracic Surgery 2008 by The Society of Thoracic Surgeons Ann Thorac Surg 2008;85: /08/$34.00 Published by Elsevier Inc
Pectus excavatum (PE) is one of the most common
 Analysis of the Nuss Procedure for Pectus Excavatum in Different Age Groups Do Hyung Kim, MD, Jung Joo Hwang, MD, Mi Kyeong Lee, RN, Doo Yun Lee, MD, and Hyo Chae Paik, MD Department of Thoracic and Cardiovascular
Analysis of the Nuss Procedure for Pectus Excavatum in Different Age Groups Do Hyung Kim, MD, Jung Joo Hwang, MD, Mi Kyeong Lee, RN, Doo Yun Lee, MD, and Hyo Chae Paik, MD Department of Thoracic and Cardiovascular
Nuss procedure for repair of pectus excavatum after failed Ravitch procedure in adults: indications and caveats
 Original Article Nuss procedure for repair of pectus excavatum after failed Ravitch procedure in adults: indications and caveats Gregor J. Kocher 1, Nathalie Gstrein 1, Dawn E. Jaroszewski 2, Mennatallah
Original Article Nuss procedure for repair of pectus excavatum after failed Ravitch procedure in adults: indications and caveats Gregor J. Kocher 1, Nathalie Gstrein 1, Dawn E. Jaroszewski 2, Mennatallah
What's new in pediatric surgery? A minimally invasive technique to correct pectus excavatum
 BUMC Proceedings 1999;12:25-28 What's new in pediatric surgery? A minimally invasive technique to correct pectus excavatum DALE COLN, MD Department of Surgery, BUMC An effective method for surgically repairing
BUMC Proceedings 1999;12:25-28 What's new in pediatric surgery? A minimally invasive technique to correct pectus excavatum DALE COLN, MD Department of Surgery, BUMC An effective method for surgically repairing
Short Nuss bar procedure
 Art of Operative Techniques Short Nuss bar procedure Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Skejby, Aarhus, Denmark; 2 Department of
Art of Operative Techniques Short Nuss bar procedure Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Skejby, Aarhus, Denmark; 2 Department of
P chondrosternal depression), the most common congenital
 Pectus Excavaturn Repair Claude Deschamps, MD ectus excavatum (also known as funnel chest or P chondrosternal depression), the most common congenital chest wall deformity, involves depression or inward
Pectus Excavaturn Repair Claude Deschamps, MD ectus excavatum (also known as funnel chest or P chondrosternal depression), the most common congenital chest wall deformity, involves depression or inward
Initial results with minimally invasive repair of pectus carinatum
 Initial results with minimally invasive repair of pectus carinatum Attila, MD Objective: Pectus carinatum is traditionally repaired by using some modification of the open Ravitch procedure, with its possible
Initial results with minimally invasive repair of pectus carinatum Attila, MD Objective: Pectus carinatum is traditionally repaired by using some modification of the open Ravitch procedure, with its possible
Current Management of Pectus Deformities. George W. Holcomb, III, M.D., MBA Surgeon-in-Chief Children s Mercy Hospital Kansas City, Missouri
 Current Management of Pectus Deformities George W. Holcomb, III, M.D., MBA Surgeon-in-Chief Children s Mercy Hospital Kansas City, Missouri Pectus Deformities Pectus Excavatum Pectus Carinatum Mixed Excavatum/Carinatum
Current Management of Pectus Deformities George W. Holcomb, III, M.D., MBA Surgeon-in-Chief Children s Mercy Hospital Kansas City, Missouri Pectus Deformities Pectus Excavatum Pectus Carinatum Mixed Excavatum/Carinatum
Pectus chest deformities are among the most common
 Repair of Pectus Chest Deformities in 320 Adult Patients: 21 Year Experience Dawn E. Jaroszewski, MD, and Eric W. Fonkalsrud, MD Department of Surgery and Division of Cardiothoracic Surgery, David Geffen
Repair of Pectus Chest Deformities in 320 Adult Patients: 21 Year Experience Dawn E. Jaroszewski, MD, and Eric W. Fonkalsrud, MD Department of Surgery and Division of Cardiothoracic Surgery, David Geffen
The Comparison Of Measurements On Chest X-Ray For Patients With Pectus Deformity. S Gurkok, O Genc, M Dakak, A Gozubuyuk, R Gorur, K Balkanli
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 5 Number 2 The Comparison Of Measurements On Chest X-Ray For Patients With Pectus Deformity S Gurkok, O Genc, M Dakak, A Gozubuyuk,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 5 Number 2 The Comparison Of Measurements On Chest X-Ray For Patients With Pectus Deformity S Gurkok, O Genc, M Dakak, A Gozubuyuk,
Single centre experience on short bar technique for pectus excavatum
 Featured Article Single centre experience on short bar technique for pectus excavatum Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Aarhus,
Featured Article Single centre experience on short bar technique for pectus excavatum Hans Kristian Pilegaard 1,2 1 Department of Cardiothoracic and Vascular Surgery, Aarhus University Hospital, Aarhus,
Management of postoperative infections after the minimally invasive pectus excavatum repair
 Journal of Pediatric Surgery (2005) 40, 1004 1008 www.elsevier.com/locate/jpedsurg Management of postoperative infections after the minimally invasive pectus excavatum repair Casey M. Calkins, Stephen
Journal of Pediatric Surgery (2005) 40, 1004 1008 www.elsevier.com/locate/jpedsurg Management of postoperative infections after the minimally invasive pectus excavatum repair Casey M. Calkins, Stephen
Moderators: Malgorzata Lutwin-Kawalec, MD, Dinesh K Choudhry, MD, FRCA. Institution: Nemours/AI DuPont Hospital for Children, Wilmington, DE
 PBLD Table # 17 A teenager with Factor V Leiden and pectus excavatum for a Nuss procedure: navigating recommendations for testing, perioperative risk of thrombosis and post-operative pain management. Moderators:
PBLD Table # 17 A teenager with Factor V Leiden and pectus excavatum for a Nuss procedure: navigating recommendations for testing, perioperative risk of thrombosis and post-operative pain management. Moderators:
Lorenz Bar Repair of Pectus Excavatum in the Adult Population: Should it be Done?
 Lorenz Bar Repair of Pectus Excavatum in the Adult Population: Should it be Done? Vanessa A. Olbrecht, MD, Meghan A. Arnold, MD, Rosemary Nabaweesi, MPH, MBChB, David C. Chang, PhD, MPH, Kimberly H. McIltrot,
Lorenz Bar Repair of Pectus Excavatum in the Adult Population: Should it be Done? Vanessa A. Olbrecht, MD, Meghan A. Arnold, MD, Rosemary Nabaweesi, MPH, MBChB, David C. Chang, PhD, MPH, Kimberly H. McIltrot,
Optoelectronic plethysmography demonstrates abrogation of regional chest wall motion dysfunction in patients with pectus excavatum after Nuss repair
 Journal of Pediatric Surgery (2012) 47, 160 164 www.elsevier.com/locate/jpedsurg Optoelectronic plethysmography demonstrates abrogation of regional chest wall motion dysfunction in patients with pectus
Journal of Pediatric Surgery (2012) 47, 160 164 www.elsevier.com/locate/jpedsurg Optoelectronic plethysmography demonstrates abrogation of regional chest wall motion dysfunction in patients with pectus
MODIFICATION OF THE NUSS PROCEDURE-PREVENTION OF INJURIES OF THE HEART AND MAJOR BLOOD VESSELS
 . Bali Medical Journal (BMJ) 20, Volume 1, Number 3: 88-92 MODIFICATION OF THE NUSS PROCEDURE-PREVENTION OF INJURIES OF THE HEART AND MAJOR BLOOD VESSELS Mirko Žganjer Children s Hospital Zagreb, Department
. Bali Medical Journal (BMJ) 20, Volume 1, Number 3: 88-92 MODIFICATION OF THE NUSS PROCEDURE-PREVENTION OF INJURIES OF THE HEART AND MAJOR BLOOD VESSELS Mirko Žganjer Children s Hospital Zagreb, Department
Corporate Medical Policy
 Corporate Medical Policy Surgical Treatment of Chest Wall Deformities (Congenital or File Name: Origination: Last CAP Review: Next CAP Review: Last Review: surgical_treatment_of_chest_wall_deformities_congenital_or_acquired
Corporate Medical Policy Surgical Treatment of Chest Wall Deformities (Congenital or File Name: Origination: Last CAP Review: Next CAP Review: Last Review: surgical_treatment_of_chest_wall_deformities_congenital_or_acquired
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Pectus excavatum is the most common congenital
 Nonprosthetic Surgical Repair of Pectus Excavatum Hiroshi Iida, MD, PhD, Yoshio Sudo, MD, PhD, Yasuyuki Yamada, MD, PhD, Yasushi Matsushita, MD, PhD, Kunihiro Eda, MD, PhD, and Yuho Inoue MD, PhD GENERAL
Nonprosthetic Surgical Repair of Pectus Excavatum Hiroshi Iida, MD, PhD, Yoshio Sudo, MD, PhD, Yasuyuki Yamada, MD, PhD, Yasushi Matsushita, MD, PhD, Kunihiro Eda, MD, PhD, and Yuho Inoue MD, PhD GENERAL
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Minimally Invasive Repair of Pectus Carinatum in Patients Unsuited to Bracing Therapy
 Korean J Thorac Cardiovasc Surg 2016;49:92-98 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Minimally Invasive Repair of Pectus Carinatum in Patients Unsuited to Bracing Therapy Clinical Research http://dx.doi.org/10.5090/kjtcs.2016.49.2.92
Korean J Thorac Cardiovasc Surg 2016;49:92-98 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Minimally Invasive Repair of Pectus Carinatum in Patients Unsuited to Bracing Therapy Clinical Research http://dx.doi.org/10.5090/kjtcs.2016.49.2.92
IN 1997 we reported our 10 years of experience with a
 Experience and Modification Update for the Minimally Invasive Nuss Technique for Pectus Excavatum Repair in 303 Patients By Daniel P. Croitoru, Robert E. Kelly, Jr, Michael J. Goretsky, M. Louise Lawson,
Experience and Modification Update for the Minimally Invasive Nuss Technique for Pectus Excavatum Repair in 303 Patients By Daniel P. Croitoru, Robert E. Kelly, Jr, Michael J. Goretsky, M. Louise Lawson,
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM
 For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
Uchiyama, Takayoshi; Nakao, Susumu; Citation Acta medica Nagasakiensia. 1978, 23
 NAOSITE: Nagasaki University's Ac Title Author(s) The Effect of Surgical Repair for P Function Tomita, Masao; Koga, Yasunori; Shib Onitsuka, Toshio; Sakoda, Koichiro; Shigehito; Nakamura, Yuzuru; Ayabe,
NAOSITE: Nagasaki University's Ac Title Author(s) The Effect of Surgical Repair for P Function Tomita, Masao; Koga, Yasunori; Shib Onitsuka, Toshio; Sakoda, Koichiro; Shigehito; Nakamura, Yuzuru; Ayabe,
Pulmonary function before and after the Nuss procedure in adolescents with pectus excavatum: correlation with morphological subtypes
 Jeong et al. Journal of Cardiothoracic Surgery (2015) 10:37 DOI 10.1186/s13019-015-0236-7 RESEARCH ARTICLE Open Access Pulmonary function before and after the Nuss procedure in adolescents with pectus
Jeong et al. Journal of Cardiothoracic Surgery (2015) 10:37 DOI 10.1186/s13019-015-0236-7 RESEARCH ARTICLE Open Access Pulmonary function before and after the Nuss procedure in adolescents with pectus
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Correlation Between Sternal Depression and Cardiac Rotation in Pectus Excavatum: Evaluation With Helical CT
 Pediatric Imaging Original Research Chu et al. CT of Pectus Excavatum Pediatric Imaging Original Research Zhi-gang Chu 1 Jian-qun Yu Zhi-gang Yang Li-qing Peng Hong-li Bai Xue-ming Li Chu ZG, Yu JQ, Yang
Pediatric Imaging Original Research Chu et al. CT of Pectus Excavatum Pediatric Imaging Original Research Zhi-gang Chu 1 Jian-qun Yu Zhi-gang Yang Li-qing Peng Hong-li Bai Xue-ming Li Chu ZG, Yu JQ, Yang
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Pseudo Heart Disease: 1/5 Norman Bethune Faculty of Medicine, Jilin University, China
 http://www.medicine-on-line.com Pseudo Heart Disease: 1/5 Case 060: Pseudo Heart Disease Author: Affiliation: Zhang Shu Norman Bethune Faculty of Medicine, Jilin University, China A 17 year-old girl presented
http://www.medicine-on-line.com Pseudo Heart Disease: 1/5 Case 060: Pseudo Heart Disease Author: Affiliation: Zhang Shu Norman Bethune Faculty of Medicine, Jilin University, China A 17 year-old girl presented
Reliability of a standardized protocol to calculate cross-sectional chest area and severity indices to evaluate pectus excavatum
 Journal of Pediatric Surgery (2006) 41, 1219 1225 www.elsevier.com/locate/jpedsurg Reliability of a standardized protocol to calculate cross-sectional chest area and severity indices to evaluate pectus
Journal of Pediatric Surgery (2006) 41, 1219 1225 www.elsevier.com/locate/jpedsurg Reliability of a standardized protocol to calculate cross-sectional chest area and severity indices to evaluate pectus
Thoracoscopic Lobectomy for Locally Advanced Lung Cancer. Masters of Minimally Invasive Thoracic Surgery Orlando September 19, 2014
 for Locally Advanced Lung Cancer Masters of Minimally Invasive Thoracic Surgery Orlando September 19, 2014 Thomas A. D Amico MD Gary Hock Endowed Professor and Vice Chair of Surgery Chief Thoracic Surgery
for Locally Advanced Lung Cancer Masters of Minimally Invasive Thoracic Surgery Orlando September 19, 2014 Thomas A. D Amico MD Gary Hock Endowed Professor and Vice Chair of Surgery Chief Thoracic Surgery
INTRODUCTION MATERIALS AND METHODS
 J Korean Med Sci 2003; 18: 360-4 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences The aim of this study was to compare clinical outcomes in pectus excavatum patients undergoing a Ravitch
J Korean Med Sci 2003; 18: 360-4 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences The aim of this study was to compare clinical outcomes in pectus excavatum patients undergoing a Ravitch
UW MEDICINE PATIENT EDUCATION DRAFT. What is pectus excavatum?
 UW MEDICINE PATIENT EDUCATION Modified Ravitch Procedure for Pectus Excavatum What to expect before, during, and after surgery This handout is for patients who are having a modified Ravitch procedure to
UW MEDICINE PATIENT EDUCATION Modified Ravitch Procedure for Pectus Excavatum What to expect before, during, and after surgery This handout is for patients who are having a modified Ravitch procedure to
Case Studies. Flail Chest Acute Pain Chest Wall Deformity Fracture Non-union
 Case Studies Flail Chest Acute Pain Chest Wall Deformity Fracture Non-union Tractor Roll Over Victim Multiple Rib Fractures, Hemothorax Surgeon s Name: John Mayberry, MD Facility Name/ Location: Oregon
Case Studies Flail Chest Acute Pain Chest Wall Deformity Fracture Non-union Tractor Roll Over Victim Multiple Rib Fractures, Hemothorax Surgeon s Name: John Mayberry, MD Facility Name/ Location: Oregon
Pectus Excavatum Reconstruction With Silicone Implants. Long-Term Results and a Review of the English-Language Literature
 REVIEW ARTICLES Pectus Excavatum Reconstruction With Silicone Implants Long-Term Results and a Review of the English-Language Literature Bart Jorrit Snel, MD,* Cees A. Spronk, MD, Paul M. N. Werker, MD,
REVIEW ARTICLES Pectus Excavatum Reconstruction With Silicone Implants Long-Term Results and a Review of the English-Language Literature Bart Jorrit Snel, MD,* Cees A. Spronk, MD, Paul M. N. Werker, MD,
Minimally invasive repair of pectus excavatum: A novel morphology-tailored, patient-specific approach
 Park et al General Thoracic Surgery Minimally invasive repair of pectus excavatum: A novel morphology-tailored, patient-specific approach Hyung Joo Park, MD, a Jin Yong Jeong, MD, a Won Min Jo, MD, a Jae
Park et al General Thoracic Surgery Minimally invasive repair of pectus excavatum: A novel morphology-tailored, patient-specific approach Hyung Joo Park, MD, a Jin Yong Jeong, MD, a Won Min Jo, MD, a Jae
Double-bar application decreases postoperative pain after the Nuss procedure
 Nagaso et al General Thoracic Surgery Double-bar application decreases postoperative pain after the Nuss procedure Tomohisa Nagaso, MD, a Junpei Miyamoto, MD, a Kiyokazu Kokaji, MD, b Ryohei Yozu, MD,
Nagaso et al General Thoracic Surgery Double-bar application decreases postoperative pain after the Nuss procedure Tomohisa Nagaso, MD, a Junpei Miyamoto, MD, a Kiyokazu Kokaji, MD, b Ryohei Yozu, MD,
Revision of failed, recurrent or complicated pectus excavatum after Nuss, Ravitch or cardiac surgery
 Brief Report on Thoracic Surgery Revision of failed, recurrent or complicated pectus excavatum after Nuss, Ravitch or cardiac surgery Dawn E. Jaroszewski 1, MennatAllah M. Ewais 1, Jesse J. Lackey 1, Kelly
Brief Report on Thoracic Surgery Revision of failed, recurrent or complicated pectus excavatum after Nuss, Ravitch or cardiac surgery Dawn E. Jaroszewski 1, MennatAllah M. Ewais 1, Jesse J. Lackey 1, Kelly
Alper Toker, MD. VATS decortication. Istanbul University, Istanbul Medical School Department of Thoracic Surgery
 VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
Pain management using patient controlled anaesthesia in adults post Nuss procedure: an analysis with respect to patient satisfaction
 Original Article on Thoracic Surgery Pain management using patient controlled anaesthesia in adults post Nuss procedure: an analysis with respect to patient satisfaction Shyamsunder Kolvekar 1, Hans Pilegaard
Original Article on Thoracic Surgery Pain management using patient controlled anaesthesia in adults post Nuss procedure: an analysis with respect to patient satisfaction Shyamsunder Kolvekar 1, Hans Pilegaard
Review Article Single Port Laparoscopic Orchidopexy in Children Using Surgical Glove Port and Conventional Rigid Instruments
 Cronicon OPEN ACCESS PAEDIATRICS Review Article Single Port Laparoscopic Orchidopexy in Children Using Surgical Glove Port and Conventional Rigid Instruments BEN DHAOU Mahdi 1, CHTOUROU Rahma 1 *, JALLOULI
Cronicon OPEN ACCESS PAEDIATRICS Review Article Single Port Laparoscopic Orchidopexy in Children Using Surgical Glove Port and Conventional Rigid Instruments BEN DHAOU Mahdi 1, CHTOUROU Rahma 1 *, JALLOULI
EVAR replaced standard repair in most cases. Why?
 EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery
 + The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery Elif GEZGINCI Gulhane Military Medical Academy School of Nursing Ankara 1 + 2 PREOPERATİVE + Preoperative (Patient
+ The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery Elif GEZGINCI Gulhane Military Medical Academy School of Nursing Ankara 1 + 2 PREOPERATİVE + Preoperative (Patient
PAPER. Video-Assisted Thoracic Surgery in the Treatment of Posttraumatic Empyema
 PAPER Video-Assisted Thoracic Surgery in the Treatment of Posttraumatic Empyema Lynette A. Scherer, MD; Felix D. Battistella, MD; John T. Owings, MD; Michael M. Aguilar, MD Background: Video-assisted thoracic
PAPER Video-Assisted Thoracic Surgery in the Treatment of Posttraumatic Empyema Lynette A. Scherer, MD; Felix D. Battistella, MD; John T. Owings, MD; Michael M. Aguilar, MD Background: Video-assisted thoracic
Routine chest drainage after patent ductus arteriosis ligation is not necessary
 Original Article Brunei Int Med J. 2010; 6 (3): 126-130 Routine chest drainage after patent ductus arteriosis ligation is not necessary Amy THIEN, Samuel Kai San YAPP, Chee Fui CHONG Department of Surgery,
Original Article Brunei Int Med J. 2010; 6 (3): 126-130 Routine chest drainage after patent ductus arteriosis ligation is not necessary Amy THIEN, Samuel Kai San YAPP, Chee Fui CHONG Department of Surgery,
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Critical Care Monitoring. Indications. Pleural Space. Chest Drainage. Chest Drainage. Potential space. Contains fluid lubricant
 Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Radiological Assessment of Children with Pectus Excavatum
 51 Original Article Radiological Assessment of Children with Pectus Excavatum Arturas Kilda 1, Algidas Basevicius 2, Vidmantas Barauskas 1, Saulius Lukosevicius 2 and Donatas Ragaisis 2 1 Department of
51 Original Article Radiological Assessment of Children with Pectus Excavatum Arturas Kilda 1, Algidas Basevicius 2, Vidmantas Barauskas 1, Saulius Lukosevicius 2 and Donatas Ragaisis 2 1 Department of
SURGERY FOR GIANT BULLOUS EMPHYSEMA
 SURGERY FOR GIANT BULLOUS EMPHYSEMA Dr. Carmine Simone Head, Division of Critical Care & Thoracic Surgeon Department of Surgery December 15, 2006 OVERVIEW Introduction Classification Patient selection
SURGERY FOR GIANT BULLOUS EMPHYSEMA Dr. Carmine Simone Head, Division of Critical Care & Thoracic Surgeon Department of Surgery December 15, 2006 OVERVIEW Introduction Classification Patient selection
The need for right ventricular outflow tract reconstruction
 Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Parenchymal air leak is a frequent complication after. Pleural Tent After Upper Lobectomy: A Randomized Study of Efficacy and Duration of Effect
 Pleural After Upper Lobectomy: A Randomized Study of Efficacy and Duration of Effect Alessandro Brunelli, MD, Majed Al Refai, MD, Marco Monteverde, MD, Alessandro Borri, MD, Michele Salati, MD, Armando
Pleural After Upper Lobectomy: A Randomized Study of Efficacy and Duration of Effect Alessandro Brunelli, MD, Majed Al Refai, MD, Marco Monteverde, MD, Alessandro Borri, MD, Michele Salati, MD, Armando
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Forces to be overcome in correction of pectus excavatum
 Forces to be overcome in correction of pectus excavatum Peter G. Weber, MD, Hans P. Huemmer, MD, and Bertram Reingruber, MD Objective: The Erlangen technique of funnel chest correction is carried out through
Forces to be overcome in correction of pectus excavatum Peter G. Weber, MD, Hans P. Huemmer, MD, and Bertram Reingruber, MD Objective: The Erlangen technique of funnel chest correction is carried out through
PREOPERATIVE CARDIOPULMONARY ASSESSMENT FOR LIVER TRANSPLANTATION James Y. Findlay Mayo Clinic College of Medicine, Rochester, MN, USA.
 PREOPERATIVE CARDIOPULMONARY ASSESSMENT FOR LIVER TRANSPLANTATION James Y. Findlay Mayo Clinic College of Medicine, Rochester, MN, USA Introduction Liver transplantation (LT) has gone from being a high-risk
PREOPERATIVE CARDIOPULMONARY ASSESSMENT FOR LIVER TRANSPLANTATION James Y. Findlay Mayo Clinic College of Medicine, Rochester, MN, USA Introduction Liver transplantation (LT) has gone from being a high-risk
Strattice Reconstructive Tissue Matrix used in the repair of rippling
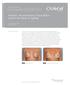 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
UAMS MEDICAL CENTER TRAUMA SERVICES MANUAL. REVIEWED: New PAGE: 1 of 7. RECOMMENDATION(S): Dr. Michael Sutherland APPROVAL: 04/28/2016
 REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
Laparoscopic Colorectal Surgery
 Laparoscopic Colorectal Surgery 20 th November 2015 Dr Adam Cichowitz General Surgeon Laparoscopic Colorectal Surgery Introduced in early 1990s Uptake slow Steep learning curve Requirement for equipment
Laparoscopic Colorectal Surgery 20 th November 2015 Dr Adam Cichowitz General Surgeon Laparoscopic Colorectal Surgery Introduced in early 1990s Uptake slow Steep learning curve Requirement for equipment
Comparative Study for the Efficacy of Small Bore Catheter in the Patients with Iatrogenic Pneumothorax
 Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Isolated Sternal Fracture S-M Yuan ABSTRACT. Isolated sternal fracture is rare and benign. A 36-year-old female presented had severe chest
 S-M Yuan ABSTRACT Isolated sternal fracture is rare and benign. A 36-year-old female presented had severe chest pain and mild dyspnea after her anterior chest wall was bluntly injured by the front seat
S-M Yuan ABSTRACT Isolated sternal fracture is rare and benign. A 36-year-old female presented had severe chest pain and mild dyspnea after her anterior chest wall was bluntly injured by the front seat
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Title: An Intrathoracic Scapular Prolapse with Hemorrhagic Shock after a. Authors: Takashi Eguchi, Ryoichi Kondo, Takayuki Shiina, and Kazuo
 Title: An Intrathoracic Scapular Prolapse with Hemorrhagic Shock after a Thoracotomy Authors: Takashi Eguchi, Ryoichi Kondo, Takayuki Shiina, and Kazuo Yoshida. Institution: Department of Thoracic Surgery,
Title: An Intrathoracic Scapular Prolapse with Hemorrhagic Shock after a Thoracotomy Authors: Takashi Eguchi, Ryoichi Kondo, Takayuki Shiina, and Kazuo Yoshida. Institution: Department of Thoracic Surgery,
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Peri-Operative Management: Guidelines for Inpatient Management of Children with Sickle Cell Disease
 Version 02 Approved by Interprofessional Patient Care Committee: September 16, 2016 1.0 Background Children with Sickle Cell are at risk of developing post-operative Acute Chest Syndrome. With improvements
Version 02 Approved by Interprofessional Patient Care Committee: September 16, 2016 1.0 Background Children with Sickle Cell are at risk of developing post-operative Acute Chest Syndrome. With improvements
Nuss Ravitch modified CPT Codes repair repair modify CPT Code repair repair Nuss codes repair modified Nuss modified Ravitch procedure
 Sep 1, 2013. Nuss procedure or the Ravitch technique (original or modified), typically requiring the removal of a portion of damaged.. CPT Codes. Description: Codes Covered When Medically Necessary. 21740.
Sep 1, 2013. Nuss procedure or the Ravitch technique (original or modified), typically requiring the removal of a portion of damaged.. CPT Codes. Description: Codes Covered When Medically Necessary. 21740.
Osteochondral Flap Repair
 Osteochondral Flap Repair System with Chondral Dart Surgical Technique Osteochondral Flap Repair Osteochondral Flap Repair System with Chondral Dart 1 2 For osteochondral fractures or OCD lesions that
Osteochondral Flap Repair System with Chondral Dart Surgical Technique Osteochondral Flap Repair Osteochondral Flap Repair System with Chondral Dart 1 2 For osteochondral fractures or OCD lesions that
In ESH we usually see blunt chest trauma but penetrating injuries also treated here (usually as single injuries, like stab wound)
 Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, radiofrequency, anesthetic considerations for, 479 489 Acute aortic syndrome, thoracic endovascular repair of, 457 462 aortic
Index Note: Page numbers of article titles are in boldface type. A Ablation, radiofrequency, anesthetic considerations for, 479 489 Acute aortic syndrome, thoracic endovascular repair of, 457 462 aortic
PEDICLE SCREW IMPACTATION IN THE AORTA AFTER DIRECT VERTEBRAL ROTATION
 PEDICLE SCREW IMPACTATION IN THE AORTA AFTER DIRECT VERTEBRAL ROTATION Alvarez, I; Carrillo, R; Carrascoso, J; Moreno, P. Spine Unit. Quiron University Hospital. Madrid; Burgos, J. H. Ramón y Cajal. Madrid;
PEDICLE SCREW IMPACTATION IN THE AORTA AFTER DIRECT VERTEBRAL ROTATION Alvarez, I; Carrillo, R; Carrascoso, J; Moreno, P. Spine Unit. Quiron University Hospital. Madrid; Burgos, J. H. Ramón y Cajal. Madrid;
LA TIMECTOMIA ROBOTICA
 LA TIMECTOMIA ROBOTICA Prof. Giuseppe Marulli UOC Chirurgia Toracica Università di Padova . The thymus presents a challenge to the surgeon not only as a structure that may be origin of benign and malignant
LA TIMECTOMIA ROBOTICA Prof. Giuseppe Marulli UOC Chirurgia Toracica Università di Padova . The thymus presents a challenge to the surgeon not only as a structure that may be origin of benign and malignant
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Trust Guidelines. Title: Guidelines for chest drain insertion
 Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
(SKILLS/HANDS-ON) Chest Tubes. Rebecca Carman, MSN, ACNP-BC. Amanda Shumway, PA-C. Thomas W. White, MD, FACS, CNSC
 (SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
(SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
CHILDHOOD MOTOCROSS TRUNCAL INJURIES: HIGH VELOCITY, FOCAL FORCE TO THE CHEST AND ABDOMEN: A Cohort Study For peer review only
 CHILDHOOD MOTOCROSS TRUNCAL INJURIES: HIGH VELOCITY, FOCAL FORCE TO THE CHEST AND ABDOMEN: A Cohort Study Journal: Manuscript ID: bmjopen-0-00 Article Type: Research Date Submitted by the Author: -Jul-0
CHILDHOOD MOTOCROSS TRUNCAL INJURIES: HIGH VELOCITY, FOCAL FORCE TO THE CHEST AND ABDOMEN: A Cohort Study Journal: Manuscript ID: bmjopen-0-00 Article Type: Research Date Submitted by the Author: -Jul-0
The Nuss procedure brought innovation to surgical treatment of pectus excavatum.
 General Thoracic Surgery Nagasao et al Stress distribution on the thorax after the Nuss procedure for pectus excavatum results in different patterns between adult and child patients Tomohisa Nagasao, MD,
General Thoracic Surgery Nagasao et al Stress distribution on the thorax after the Nuss procedure for pectus excavatum results in different patterns between adult and child patients Tomohisa Nagasao, MD,
The ABC s of Chest Trauma
 The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
SURGICAL PROCEDURE DESCRIPTIONS
 SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
Adult Hip Dysplasia David S. Feldman, MD
 Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006.
 Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
P keel ), or pigeon breast, is the term applied to
 Surgical Management of Pectus Carinatum Eric W. Fonkalsrud, MD ectus carinatum (from the Latin, chest with a P keel ), or pigeon breast, is the term applied to various protrusion deformities of the anterior
Surgical Management of Pectus Carinatum Eric W. Fonkalsrud, MD ectus carinatum (from the Latin, chest with a P keel ), or pigeon breast, is the term applied to various protrusion deformities of the anterior
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Pectus excavatum (PE) is the most common deformity
 Modified Nuss Procedure in Concurrent Repair of Pectus Excavatum and Open Heart Surgery Maria Grazia Sacco Casamassima, MD, Ling Ling Wong, MB BS, Dominic Papandria, MD, Fizan Abdullah, MD, PhD, Luca A.
Modified Nuss Procedure in Concurrent Repair of Pectus Excavatum and Open Heart Surgery Maria Grazia Sacco Casamassima, MD, Ling Ling Wong, MB BS, Dominic Papandria, MD, Fizan Abdullah, MD, PhD, Luca A.
Facing Surgery for Lung Cancer? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for Lung Cancer? Learn about minimally invasive da Vinci Surgery Treatments & Surgery Options: The treatment and surgical options for the most common lung cancer, non-small cell lung cancer,
Facing Surgery for Lung Cancer? Learn about minimally invasive da Vinci Surgery Treatments & Surgery Options: The treatment and surgical options for the most common lung cancer, non-small cell lung cancer,
ICU Management of Minimally Invasive Cardiac Surgery
 ICU Management of Minimally Invasive Cardiac Surgery Benjamin A. Kohl, MD, FCCM Chief of Critical Care, Aria-Jefferson Health Professor of Anesthesiology Thomas Jefferson University Sidney Kimmel Medical
ICU Management of Minimally Invasive Cardiac Surgery Benjamin A. Kohl, MD, FCCM Chief of Critical Care, Aria-Jefferson Health Professor of Anesthesiology Thomas Jefferson University Sidney Kimmel Medical
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Interruption of the thoracic sympathetic chain is associated
 Thoracoscopic Sympathicotomy King F. Kwong and Mark J. Krasna Interruption of the thoracic sympathetic chain is associated with alleviation of symptoms for a variety of maladies. Until fairly recently,
Thoracoscopic Sympathicotomy King F. Kwong and Mark J. Krasna Interruption of the thoracic sympathetic chain is associated with alleviation of symptoms for a variety of maladies. Until fairly recently,
Chest Wall Deformities
 CHAPTER 53 Chest Wall Deformities Michael Singh Dakshesh Parikh Brian Kenney Pectus Carinatum Pectus carinatum (PC), or pigeon chest, is a spectrum of anterior chest wall anomalies characterised by protrusion
CHAPTER 53 Chest Wall Deformities Michael Singh Dakshesh Parikh Brian Kenney Pectus Carinatum Pectus carinatum (PC), or pigeon chest, is a spectrum of anterior chest wall anomalies characterised by protrusion
Chest Wall Tumors and Reconstruction: Lateral Chest Wall. Dr. Robert Kelly
 Chest Wall Tumors and Reconstruction: Lateral Chest Wall Dr. Robert Kelly THORACIC PROGRAMME: ADVANCES IN CHEST WALL SURGERY AND OSTEOSYNTHESIS Dr. José Ribas Milanez de Campos Assistant, Professor, Department
Chest Wall Tumors and Reconstruction: Lateral Chest Wall Dr. Robert Kelly THORACIC PROGRAMME: ADVANCES IN CHEST WALL SURGERY AND OSTEOSYNTHESIS Dr. José Ribas Milanez de Campos Assistant, Professor, Department
Nonoperative management of pectus carinatum
 Journal of Pediatric Surgery (2006) 41, 40 45 www.elsevier.com/locate/jpedsurg Nonoperative management of pectus carinatum Ala Stanford Frey, Victor F. Garcia, Rebeccah L. Brown, Thomas H. Inge, Frederick
Journal of Pediatric Surgery (2006) 41, 40 45 www.elsevier.com/locate/jpedsurg Nonoperative management of pectus carinatum Ala Stanford Frey, Victor F. Garcia, Rebeccah L. Brown, Thomas H. Inge, Frederick
Goals and Objectives. Assessment Methods/Tools
 CA-3 CARDIOVASCULAR ANESTHESIA ROTATION Minneapolis Veterans Administration Medical Center (VAMC) Rotation Site Director: Dr. Karen Ringsred Rotation Duration: 4 weeks Introduction: The patients at the
CA-3 CARDIOVASCULAR ANESTHESIA ROTATION Minneapolis Veterans Administration Medical Center (VAMC) Rotation Site Director: Dr. Karen Ringsred Rotation Duration: 4 weeks Introduction: The patients at the
Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis
 Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
Pectus Carinatum. How is it Treated? Treatment options include either a pressure brace or surgery.
 What is Pectus? Pectus carinatum is when the breast bone or sternum and the rib cartilage stick out from your child s chest. It may also be called pigeon chest. It can be mild, moderate, or severe. It
What is Pectus? Pectus carinatum is when the breast bone or sternum and the rib cartilage stick out from your child s chest. It may also be called pigeon chest. It can be mild, moderate, or severe. It
CARDIOCHIRURGIA MINI-INVASIVA: INVASIVA: efficacia per il paziente efficienza per la sanita. Dott. Davide Ricci
 CARDIOCHIRURGIA MINI-INVASIVA: INVASIVA: efficacia per il paziente efficienza per la sanita Dott. Davide Ricci SC Cardiochirurgia U Universita degli Studi di Torino Minimally Invasive Surgical approaches
CARDIOCHIRURGIA MINI-INVASIVA: INVASIVA: efficacia per il paziente efficienza per la sanita Dott. Davide Ricci SC Cardiochirurgia U Universita degli Studi di Torino Minimally Invasive Surgical approaches
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
Financial and Other Disclosures
 Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
