Closed incision prophylactic negative pressure wound therapy in patients undergoing major complex abdominal wall repair
|
|
|
- Benjamin Lambert
- 5 years ago
- Views:
Transcription
1 Hernia (2017) 21: DOI /s ORIGINAL ARTICLE Closed incision prophylactic negative pressure wound therapy in patients undergoing major complex abdominal wall repair F. E. E. de Vries 1 J. J. Atema 1,2 O. Lapid 3 M. C. Obdeijn 3 M. A. Boermeester 1 Received: 29 August 2016 / Accepted: 1 May 2017 / Published online: 23 May 2017 Ó The Author(s) This article is an open access publication Abstract Purpose To evaluate if incisional prophylactic negative pressure wound therapy (pnpwt) reduces wound infections and other wound complications in high-risk patients undergoing major complex ventral abdominal wall repair. Methods Retrospective before after comparison nested in a consecutive series of patients undergoing elective major complex abdominal wall repair. Starting January 2014, pnpwt was applied on the closed incisional wound for a minimum of 5 days. To minimize selection bias, we compared two periods of 14 months before and after January Wound infections according to the Centre for Disease Control Surgical Site Infection classification as well as other wound complications were recorded. Results Thirty-two patients were included in the pnpwt group and 34 in the control group. The study group involved clean-contaminated and contaminated operations due to enterocutaneous fistula, enterostomies or infected mesh. Median duration of pnpwt was 5 days (IQR 5 7). Overall wound infection rate was 35%. pnpwt was associated with a significant decrease in postoperative wound infection rate (24 versus 51%; p = 0.029, OR 0.30 (95% CI )). Incisional wound infection rates dropped from 48 to 7% (p \ 0.01, OR 0.08 (95% CI ), whereas the number of subcutaneous abscesses & F. E. E. de Vries f.e.devries@amc.uva.nl Department of Surgery, Academic Medical Centre, PO Box 22660, 1100 DD Amsterdam, The Netherlands Department of Surgery, Onze Lieve Vrouwe Gasthuis, Amsterdam, The Netherlands Department of Plastic and Reconstructive Surgery, Academic Medical Centre, Amsterdam, The Netherlands was comparable in both groups. Moreover, less interventions were needed in the pnpwt group (p \ 0.001). Conclusions Closed incision pnpwt seems a promising solution to reduce the incidence of wound infections in complex abdominal wall surgery. Randomized controlled trials are needed to estimate more precisely the value and cost-effectiveness of pnpwt in this high-risk setting. Keywords Complex abdominal wall repair Prophylactic negative pressure Introduction Patients undergoing major complex abdominal wall repair (CAWR) are at high risk to develop wound complications [1, 2]. Some of these operations are contaminated or even dirty, for example in patients with enterocutaneous fistulas (ECF), enterostomies or infected mesh. Furthermore, abdominal wall reconstruction may require component separation techniques (CST), sometimes combined with the use of a mesh and flap reconstructions. Increased wound surface and the implantation of a foreign body can, therefore, increase the risk of wound complications. Last but not least, a considerable amount of these patients have a history of repeated abdominal surgery, recurrent hernias, long-lasting hospital stay and dependence of parenteral nutrition (PN). Altogether, their physical and nutritional condition is most often suboptimal and these patients are prone to wound complications. Reported rates of surgical site occurrences in this setting are 29 66% [3 10]. Surgical site infections (SSI) and other wound complications are associated with high morbidity, considerable mortality, longer hospital stay and increased health care costs [11]. Several patient characteristics such
2 584 Hernia (2017) 21: as smoking and obesity, but also operative characteristics such as length of operation and the level of contamination, are associated with an increased risk of developing SSI [11]. Over the last decades, several measures to reduce SSI have been implemented such as systemic antibiotic prophylaxis and antiseptic agents used to rinse the operative field [12, 13]. Since the introduction of negative pressure wound therapy (NPWT) in 1995, its popularity has grown and it has shown potential for several indications such as open bone fractures [14], diabetic ulcers [15] and the open abdomen [16]. First introduced in orthopaedic surgery in 2006 [17], prophylactic negative pressure wound therapy (pnpwt) has been suggested as a new method to prevent wound complications by its application on a closed incisional wound. NPWT consists of a closed, sealed system connected to a vacuum pump, which maintains negative pressure on the wound. The precise mechanism of pnpwt is unknown. Current hypothesis is that pnpwt creates a moist wound healing environment, drains exudate, reduces tissue edema, contracts the wound edges, mechanically stimulates the wound bed, and influences blood perfusion at the wound edge, which may lead to angiogenesis and the formation of granulation tissue [18]. Moreover, the sealed system might protect against micro-organisms from outside entering the wound. Conflicting results have been reported on the use of pnpwt. The aim of the present study was to evaluate if pnpwt reduces the incidence of wound infections and other wound complications in patients undergoing elective open major CAWR. Methods Study design and data collection This was a retrospective before after comparison nested in a consecutive series of patients undergoing CAWR at the Department of Surgery of the Academic Medical Center in Amsterdam, a tertiary university hospital in the Netherlands. The medical ethical committee of the hospital approved the study and for this type of study, formal consent was not required. Starting January 2014, the use of pnpwt for patients undergoing complex abdominal wall repair became a standard part of the procedure. To minimize selection bias, we compared two periods of 14 months before and 14 months after January 2014 to assess the effects of pnpwt. All data on operations performed between September 2012 and April 2015 by a single surgeon, more than 10 years specialized in complex abdominal wall surgery and lead of a specialized outpatient clinic for acute intestinal failure, were reviewed. Primary outcome was the incidence of superficial and deep wound infections. The wound infections were further subdivided into incisional wound infections and/or subcutaneous abscesses. Secondary outcomes were the appearance of other wound complications such as non-infected seroma, bleeding or hematoma, skin- or fat necrosis, wound dehiscence requiring (prolonged) NPWT, anastomotic leakage, intra-abdominal abscesses, ECF, the need for percutaneous or surgical interventions, emergency department visits after discharge, re-admissions and 30-day mortality. All adult patients undergoing midline elective open, CAWR according to the criteria of major complex abdominal wall surgery as described by Slater in 2014 [2] were included. Primary skin closure at the end of surgery (with or without flap rotation by a plastic surgeon) was a prerequisite. Data on patient demographics, risk factors for SSI, level of contamination, operative characteristics and post-operative complications (including SSI) were extracted from the clinical charts. Outcome and definitions Infections were scored from the clinical charts after the operative procedure and classified according to the Centre for Disease Control (CDC) SSI criteria (including superficial, deep and organ space infections). Next to this, superficial wound infections according to the CDC SSI criteria were scored for subcutaneous abscess and/or incisional wound infection. In case a culture was available these results were used, if no culture was available information from the clinical chart was used. The description of purulent drainage from a superficial incision or the need of opening the wound by the surgeon due to pain or tenderness, localized swelling, erythema or heat was scored as positive for wound infection. In case of bowel content leakage from either the anastomosis or bowel perforation which was proven by contrast radiography or relaparotomy, this was scored as leakage. If there was an unnatural communication between the gastro-intestinal tract and the skin, it was registered as an ECF. Intra-abdominal fluid collections with positive culture after drainage without signs of anastomotic leakage or bowel perforation were scored as an intra-abdominal abscess. Wound dehiscence needing postoperative therapeutic NPWT was recorded separately in the control group as well as in the pnpwt group. For the pnpwt group, this element was scored if NPWT was continued, after the first dressing change at postoperative day 5, because of dehiscence during pnpwt. Continuing pnpwt at the dressing change at postoperative day 5 because of severe edema but without any signs of dehiscence or infection was not scored as SSI. Bleeding or hematoma was recorded in the case of either active
3 Hernia (2017) 21: bleeding or a large hematoma, which needed radiologic drainage. We defined seroma as a subcutaneous fluid collection without any signs of infection or with negative culture results after drainage. Infected seroma was scored as a superficial SSI. Interventions were scored separately for intra-abdominal and extra-abdominal. Intra-abdominal interventions could be either radiologic percutaneous drainage or relaparotomy. Extra-abdominal interventions were scored for radiologic percutaneous subcutaneous drainage and the need for opening of the wound with or without antibiotics. Opening of the wound could be either spontaneously due to infection or as part of therapeutic drainage. Interventions were scored for infectious complications as well as non-infectious complications. Surgical technique Operative principles for CAWR did not change over the study period apart from the application of pnpwt. Infection prevention was performed according to the national guidelines and included hand hygiene, surgical site preparation with an alcohol and chlorhexidine based, nonaqueous, antiseptic agent and systemic prophylactic antibiotics min before incision. In case of presence of ECF segmental intestinal resection was performed. All patients had hand-sewn anastomoses. In patients where primary fascial closure was not possible, an open anterior CST was performed. An intra-abdominal sublay biological mesh (Strattice TM porcine dermal matrix, Acelity) was used in all cases with enterocutaneous or enteroatmospheric fistula and sometimes in other contaminated situations, such as infected synthetic mesh removal. In clean situations, a synthetic retrorectus light-weight polypropylene sublay Vypro Ò mesh (Ethicon/Johnson&Johnson) was used. Sometimes, in very large clean abdominal wall defects a double layer technique was used, including intraabdominal sublay Strattice TM dermal matrix and retrorectus light-weight polypropylene sublay Vypro Ò mesh, combined with a CST. On average, three 18 Fr suction drains were used 1 subfascial on top of the biological mesh and 2 subcutaneous to ensure active drainage of fluids and these were only removed when production was \30 ml/24 h. The fascia was closed with a monofilament polydioxanone suture (PDS loop). In case of large full thickness skin defects, a plastic surgeon performed a flap reconstruction. No skin grafts were used. All patients had subcutical closure before the skin was closed. The skin was closed with single polyester Mersilene Ò sutures (Ethicon); no staples were used. Up to January 2014, elastic Microfoam surgical bandage (3 M) was applied for 24 h. From January 2014, pnpwt (either Prevena TM (Acelity/KCI) or a home-made construction of Melolin non-adhesive wound dressing (Smith&Nephew) and V.A.C Ò Granufoam TM (Acelity/KCI) was used for at least 5 days with a negative pressure of 100 mmhg. After 5 days, the surgical team performed wound inspection. In case of severe edema and/or risk of wound dehiscence due to abdominal distension, pnpwt dressing was changed and prolonged for another 3 5 days. In case of a closed wound without any signs of edema or dehiscence, the pnpwt was removed. All patients wore a binder for 7 days continuously and thereafter for 3 months postoperative when mobilizing. Statistical analyses The pnpwt and the control group were compared using Chi-square (Fisher exact) test for categorical data and using Mann Whitney U test for not normal distributed numerical variables. Normal continuous numerical variables were compared using Students t test only if found normally distributed in a Q Q plot. Statistical analyses were performed with SPSS version A p value B 0.05 was considered statistically significant. Results Study population and operative characteristics During the 14-month period, from January 2014 until April 2015, 32 consecutive patients undergoing CAWR fulfilled the inclusion criteria and were treated with pnpwt. In the preceding 14 months, between September 2012 and January 1st 2014, a consecutive group of 34 patients formed the control group. Of these 66 consecutive patients, 36 (55%) were male, and the mean age at the time of operation was 59.4 [standard deviation (SD) 13.3] years. Baseline characteristics regarding co-morbidity known for increased risk of SSI, such as obesity or inflammatory bowel disease (IBD), did not significantly differ between both groups (Table 1). Overall, almost half of the included patients (44%) depended on PN. Seventy-seven percent (51/66) of the operations involved clean-contaminated or contaminated or dirty operations. The median number of previous abdominal surgeries was 4 (range 1 24). In 91% of the patients, a CST was performed, usually on both sides. Mean operation time (including anesthesia) was 438 (SD 153) minutes. Surgery was performed for the following reasons: resection of one or more enteric fistulas, restorations of bowel continuity, very large or recurrent hernias or recurrent hernia with infected mesh. Reconstruction by a plastic surgeon was required in 12 cases (18%). In Table 1, we summarize patient and operative characteristics for both the pnpwt and the control group. There were no statistical significant differences in operative characteristics between the two groups.
4 586 Hernia (2017) 21: Table 1 Patient and operative characteristics pnpwt (n = 32) Control (n = 34) p Gender (male:female) 20:12 16: Mean age at operation (SD) 58.9 (13.9) 59.7 (12.9) Mean BMI (SD) 26.9 (5.4) 27.7 (6.0) Mean ASA classification (SD) 2.34 (0.60) 2.18 (0.63) Diabetes (%) 8 (25) 6 (18) IBD (%) 3 (9) 4 (12) PN dependence (%) 14 (44) 15 (47) Corticosteroid use (%) 1 (3) 4 (12) Smoking (%) 6 (19) 5 (15) COPD (%) 6 (19) 2 (6) Previous abdominal operations (IQR) 4 (3 6) 4 (3 6) Range (1 24) (1 14) No of prior hernia repair (range) 0 (0 4) 0 (0 3) Duration of operation in minutes (SD) 453 (158) 424 (129) (Clean-) contaminated (or dirty) operation (%) 26 (81) 25 (74) Bowel anastomosis during operation (%) 22 (69) 21 (62) Enterocutaneous fistula present (%) 18 (56) 13 (38) Infected mesh removal (%) 11 (34) 5 (15) Mesh (any type) placement (%) 29 (91) 28 (82) Presence of enterostomy postoperative (%) 2 (6) 7 (21) Component separation technique (%) 29 (91) 31 (91) Plastic surgeon involved 7 (22) 5 (15) Median length of pnpwt (IQR) 5 (5 7) IBD inflammatory bowel disease, PN parenteral nutrition, COPD chronic obstructive pulmonary disease Outcome Table 2 summarizes outcomes of both groups. Overall SSI rate (including organ-space infections) was 47%. Six patients developed anastomotic leakage. In these patients, it was not possible to judge SSI; thus, these six patients were excluded from the wound infection analysis. The wound infection rate was 38% (23/66). We had no deep SSI. We found a significant decrease in superficial wound infections after surgery in the pnpwt group compared with the control group (24 versus 51%, p = 0.029, OR 0.30 (95% CI )). The number of incisional wound infections significantly decreased after the introduction of pnpwt (7 versus 48%, p \ 0.001, OR 0.08 (95% CI )), while the number of subcutaneous abscesses was comparable (5 versus 4). In the pnpwt group, all wound infections involved contaminated operations, whereas an additional three patients had wound infections after clean surgery in the control group. The number of patients needing subcutaneous drainage was comparable in both groups (22 versus 24%). However, (the need for) opening of the wound with or without antibiotics was significantly decreased after the introduction of pnpwt (7 versus 48%, p \ 0.001, OR 0.08 (95% CI ). The need for postoperative intra-abdominal interventions was comparable in both groups, including two relaparotomies for anastomotic leakage in the control group and 9 and 8 radiologic drainages, respectively, in intervention and control group. Six patients in the control group needed NPWT due to wound dehiscence compared with seven patients in the pnpwt group needing prolonged NPWT. Discussion pnpwt on a closed midline laparotomy skin incision significantly reduced wound infections in patients undergoing major complex abdominal wall repair (24 versus 51%, p = 0.029, OR 0.30 (95% CI )), and even more for incisional wound infections only (7 versus 48%, p \ 0.001, OR 0.08 (95% CI )). Although the number of intra-abdominal and radiologic subcutaneous interventions did not decrease, the number of wounds which spontaneously opened due to infection or were opened as part of incisional infection treatment was significantly decreased (p \ 0.001). In this cohort, pnpwt failed to reduce other wound complications, emergency department visits and re-admissions.
5 Hernia (2017) 21: Table 2 Postoperative outcome pnpwt (n = 32) (%) Control (n = 34) (%) p OR Surgical site infections (overall) 12 (38) 19 (56) Wound infection (superficial/deep according to CDC) 7 (24) (n = 29) 16 (51) (n = 31) (95% CI ) Incisional wound infection 2 (7) 15 (48) < (95% CI ) Subcutaneous abscesses 5 (17) 4 (13) Bowel content leakage 5 (16) 4 (12) Anastomotic leakage 2 (10) (n = 21) 4 (19) (n = 21) Transient small bowel laceration a 3 (9) 0 (0) Intra-abdominal abscess b 4 (13) 2 (6) Enterocutaneous fistula 3 (9) 3 (9) Non-infected seroma 5 (16) 7 (21) Bleeding/hematoma 4 (13) 6 (18) Wound dehiscence needing NPWT 6 (19) 7 (21) Necrosis partial skin/subcutis 1 (3) 3 (9) Interventions extra-abdominal Radiologic subcutaneous drainage 7 (22) 8 (24) Opening wound and/or antibiotics c 2 (7) (n = 29) 15 (48) (n = 31) < (95% CI ) Intervention for intra-abdominal complications Radiologic intra-abdominal drainage 9 (28) 8 (24) Relaparotomy 0 (0) 2 (6) Hospital stay days (IQR) 19 (9 35) 12 (8 22) Range (5 120) (2 105) Emergency department visit 9 (28) 13 (38) Re-admission 4 (13) 6 (18) day mortality 0 (0) 0 (0) Bold values indicate p-value significant if less than 0.05 a One patient had iatrogenic bowel perforation, two patients had a bowel perforation e.c.i b Intra-abdominal abscess without any signs of anastomotic leakage or bowel perforation c Spontaneously due to infection or therapeutic drainage As far as we know there are no randomized controlled trials published on pnpwt in abdominal surgery. We identified four controlled observational studies in patients undergoing ventral hernia repair [19 22]. Only two of them [20] found a significant benefit in reducing SSI. One study [20] involved large clean hernia repairs; another study [22] included both clean and clean-contaminated procedures. In contrast, Condé-Green et al. [19] found a significant difference in the number of wound complications as well as the number of skin dehiscence but failed to detect a difference in mere wound infections. In that study, all operations involved clean large ventral hernia repairs. The fourth study, Pauli et al. [21] focused on contaminated and infected hernias and do not find a difference in wound infections. Although the patient population in that study may seem comparable with our population, important differences exist when looking in more detail. Although Pauli et al. mentioned in their title high-risk abdominal wall reconstructions, they excluded patients undergoing anterior CST, patients with simultaneous colo- or enterocutaneous fistula takedown and patients undergoing simultaneous panniculectomy, and in particular these patients are at higher risk for SSI. In our study, almost half of the patients had one or more ECF and 91% underwent CST, therefore, representing a population at a much higher risk for wound infections. Hence, the discrepancy of their results with our findings may well be explained by the striking differences in included patient population. Recently, for all types of surgery a systematic review and meta-analysis on pnpwt has been performed [23]. An overall weighted average SSI rate of 6.61% in the pnpwt groups was found compared with 9.36% in the control groups, reflecting a relative reduction of 29.4%. A subgroup analysis of studies in abdominal surgery showed 13.54% SSI in the intervention group compared with 23.97% in the control group. Notably, the risk of SSI and subsequent SSI rates is much higher in complex and contaminated abdominal (wall) surgery such as encountered in the patients included in our study.
6 588 Hernia (2017) 21: In our patient group, of which 75% of the patients underwent bowel resection and/or anastomosis, it can be difficult to distinguish between intra-abdominal complications due to anastomotic leakage or perforation and organ space surgical site infections due to wound complications. So far, it is unlikely that pnpwt has any influence on the intra-abdominal postoperative situation in closed fascia settings. In our opinion, the influence of pnpwt on intraabdominal complications is negligible when the fascia is closed. As the aim of our study was to investigate the influence of pnpwt on wound infections, we chose to separately score intra-abdominal complications (bowel content leakage and intra-abdominal abscesses) and interventions for wound infections (superficial and deep). The first mentioned are more likely caused by anastomotic leakage, perforation or spillage of bowel content during the operation rather than due to wound complications. Moreover, we divided the superficial wound infections in subcutaneous abscesses and incisional wound infections. The reason is that the CDC SSI classification does not distinguish between these two different types of superficial infections. We found that a considerable number of patients in the pnpwt group had a subcutaneous abscess while not having an incisional SSI and, thus, a closed surgical incision wound. The reason might be that 91% of the patients underwent component separation technique, creating increased wound surface and dead space. Although retrospective cohort studies are prone to selection bias, we tried to minimize bias by comparing our intervention cohort with a cohort of patients operated within the same time span. In some of the previous studies, the choice for pnpwt or conventional dressings was based on the preference of the surgeon, which might create a higher risk of bias. In addition, we did not find any significant differences in baseline characteristics, reflecting comparable study groups. SSI cause an enormous burden on healthcare costs [24]. On the other hand, pnpwt also incurs additional costs. We identified three studies [25 27] on cost-effectiveness of pnpwt and these were all performed in a gynaecological population. Lewis et al. [26] found that the risk of wound complications must be reduced by 33% for pnpwt to achieve cost savings. For obese and morbid obese patients, required reduction was slightly less. Echebiri et al. [25] concluded that if surgical site infection rates are greater than 14%, pnpwt could be cost-beneficial depending on the degree of reduction in surgical site infections. At a surgical site infection rate of 30%, the rate must be reduced by 15% for pnpwt to become the preferred strategy. Although these studies involved a different patient group with clean surgery and, therefore, simply extrapolating these results cannot be done; these calculations do suggest that pnpwt is potentially cost-beneficial in our cohort. This study is limited by the retrospective and non-randomized design. It can be difficult to score wound complications from a patient chart. Next to this, there might be an interpreter bias as the one who did the data extraction was not blinded for the therapy. Last but not least, not all patients had an equal follow-up. As we are a tertiary hospital, some patients living far away might have returned to other hospitals in the country if wound complications occurred. Nevertheless, all patients had outpatient followup at least once after 30 days, so the number of wound complications missed is probably limited to exceptional very late ones. Closed incision prophylactic NPWT seems a promising solution to reduce the incidence of incisional wound infections in complex abdominal wall surgery. Randomized controlled trials are needed to estimate more precisely the value and cost-effectiveness of prophylactic NPWT in this high-risk setting. Compliance with ethical standards Conflict of interest M.A. Boermeester reports institutional grants from J&J/Ethicon, Acelity/KCI, LifeCell, Ipsen, Baxter, Mylan, Bard, outside the submitted work; advisory board member of J&J/Ethicon, Acelity/KCI and LifeCell. The other authors do not declare any conflicts of interest. Funding None. Ethical approval The medical ethical committee of the hospital approved the study. Human and animal rights This article does not contain any studies with human participants or animals performed by any of the authors. Informed consent The medical ethical committee waived the need of informed consent due to the retrospective design of the study. Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License ( which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. References 1. Kanters AE, Krpata DM, Blatnik JA et al (2012) Modified hernia grading scale to stratify surgical site occurrence after open ventral hernia repairs. J Am Coll Surg 215: Slater NJ, Montgomery A, Berrevoet F et al (2014) Criteria for definition of a complex abdominal wall hernia. Hernia 18: Basta MN, Fischer JP, Kovach SJ (2015) Assessing complications and cost-utilization in ventral hernia repair utilizing biologic mesh in a bridged underlay technique. Am J Surg 209: Garvey PB, Martinez RA, Baumann DP, Liu J, Butler CE (2014) Outcomes of abdominal wall reconstruction with acellular dermal
7 Hernia (2017) 21: matrix are not affected by wound contamination. J Am Coll Surg 219: Pinell-White XA, Gruszynski M, Losken A (2014) Ventral hernia repair after bowel surgery. Ann Plast Surg 72: Kim H, Bruen K, Vargo D (2006) Acellular dermal matrix in the management of high-risk abdominal wall defects. Am J Surg 192: Itani KMF, Rosen M, Vargo D, Awad SS, Denoto G, Butler CE (2012) Prospective study of single-stage repair of contaminated hernias using a biologic porcine tissue matrix: the RICH Study. Surgery 152: Iacco A, Adeyemo A, Riggs T, Janczyk R (2014) Single institutional experience using biological mesh for abdominal wall reconstruction. Am J Surg 208: Rosen MJ, Krpata DM, Ermlich B, Blatnik JA (2013) A 5-year clinical experience with single-staged repairs of infected and contaminated abdominal wall defects utilizing biologic mesh. Ann Surg 257: Slater NJ, Bokkerink WJV, Konijn V, Bleichrodt RP, van Goor H (2015) Safety and durability of 1-stage repair of abdominal wall defects with enteric fistulas. Ann Surg 261: CDC (2015) Surgical site infection. CDC, London, pp Allegranzi B, Bischoff P, de Jonge S et al (2016) New WHO recommendations on preoperative measures for surgical site infection prevention: an evidence-based global perspective. Lancet Infect Dis 3099: Allegranzi B, Zayed B, Bischoff P et al (2016) New WHO recommendations on intraoperative and postoperative measures for surgical site infection prevention: an evidence-based global perspective. Lancet Infect Dis 16:e288 e Stannard JP, Volgas DA, Stewart R, McGwin G, Alonso JE (2009) Negative pressure wound therapy after severe open fractures: a prospective randomized study. J Orthop Trauma 23: Canadian Agency for Drugs and Technologies in Health (2014) Negative pressure wound therapy for managing diabetic foot ulcers: a review of the clinical effectiveness, cost-effectiveness, and guidelines. CADTH Rapid Response Reports 16. Roberts DJ, Zygun DA, Grendar J et al (2012) Negative-pressure wound therapy for critically ill adults with open abdominal wounds. J Trauma Acute Care Surg 73: Meissner K (1999) Late radiogenic small bowel damage: guidelines for the general surgeon. Dig Surg 16: Borgquist O, Ingemansson R, Malmsjö M (2011) Individualizing the use of negative pressure wound therapy for optimal wound healing: a focused review of the literature. Ostomy Wound Manage 57: Condé-Green A, Chung TL, Holton LH et al (2012) Incisional negative-pressure wound therapy versus conventional dressings following abdominal wall reconstruction. Ann Plast Surg 71:1 20. Gassman A, Mehta A, Bucholdz E et al (2014) Positive outcomes with negative pressure therapy over primarily closed large abdominal wall reconstruction reduces surgical site infection rates. Hernia 19: Pauli EM, Krpata DM, Novitsky YW, Rosen MJ (2013) Negative pressure therapy for high-risk abdominal wall reconstruction incisions. Surg Infect 14: Soares KC, Baltodano PA, Hicks CW et al (2015) Novel wound management system reduction of surgical site morbidity after ventral hernia repairs: a critical analysis. Am J Surg 209: Semsarzadeh NN, Tadisina KK, Maddox J, Chopra K, Singh DP (2015) Closed incision negative-pressure therapy is associated with decreased surgical-site infections. Plast Reconstr Surg 136: de Lissovoy G, Fraeman K, Hutchins V, Murphy D, Song D, Vaughn BB (2009) Surgical site infection: incidence and impact on hospital utilization and treatment costs. Am J Infect Control 37: Echebiri NC, McDoom MM, Aalto MM, Fauntleroy J, Nagappan N, Barnabei VM (2015) Prophylactic use of negative pressure wound therapy after cesarean delivery. Obstet Gynecol 125: Lewis LS, Convery PA, Bolac CS, Valea FA, Lowery WJ, Havrilesky LJ (2014) Cost of care using prophylactic negative pressure wound vacuum on closed laparotomy incisions. Gynecol Oncol 132: Tuffaha HW, Gillespie BM, Chaboyer W, Gordon LG, Scuffham PA (2015) Cost-utility analysis of negative pressure wound therapy in high-risk cesarean section wounds. J Surg Res 195:
The Efficacy of NPWT on Primary Closed Incisions
 The Efficacy of NPWT on Primary Closed Incisions Pieter Zwanenburg Researcher / PhD Candidate Marja Boermeester Professor of Surgery, Academic Medical Center, Amsterdam Incisional Negative Pressure Wound
The Efficacy of NPWT on Primary Closed Incisions Pieter Zwanenburg Researcher / PhD Candidate Marja Boermeester Professor of Surgery, Academic Medical Center, Amsterdam Incisional Negative Pressure Wound
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Difficult Abdominal Closure. Mark A. Carlson, MD
 Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
Introduction. Efstathios Karamanos 1 Pridvi Kandagatla. Aamir Siddiqui 1
 World J Surg (2017) 41:914 918 DOI 10.1007/s00268-016-3835-0 ORIGINAL SCIENTIFIC REPORT Development and Validation of a Scoring System to Predict Surgical Site Infection After Ventral Hernia Repair: A
World J Surg (2017) 41:914 918 DOI 10.1007/s00268-016-3835-0 ORIGINAL SCIENTIFIC REPORT Development and Validation of a Scoring System to Predict Surgical Site Infection After Ventral Hernia Repair: A
REINFORCED BIOSCAFFOLDS
 REINFORCED BIOSCAFFOLDS Midline Incisional Open OviTex 1S Resorbable Clinical Case Study: Open Abdomen Incisional Herniorrhaphy in Contaminated (CDC Class IV) Operative Field Performed by Dr. Michael Sawyer,
REINFORCED BIOSCAFFOLDS Midline Incisional Open OviTex 1S Resorbable Clinical Case Study: Open Abdomen Incisional Herniorrhaphy in Contaminated (CDC Class IV) Operative Field Performed by Dr. Michael Sawyer,
34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH
 Case Presentation 34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH negative NKDA Case Presentation VS:
Case Presentation 34 yo M presented in ER of KCH at 7/06/10 Painful lump lt groin + vomiting Pain started 2 hrs before presentation. PMH known left inguinal hernia PSH negative NKDA Case Presentation VS:
ISPUB.COM. Abdominoplasty Combined With Treatment of Enterocutaneous Fistula. H Canter, E Hamaloglu INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Surgery Volume 11 Number 1 Abdominoplasty Combined With Treatment of Enterocutaneous Fistula H Canter, E Hamaloglu Citation H Canter, E Hamaloglu. Abdominoplasty Combined
ISPUB.COM The Internet Journal of Surgery Volume 11 Number 1 Abdominoplasty Combined With Treatment of Enterocutaneous Fistula H Canter, E Hamaloglu Citation H Canter, E Hamaloglu. Abdominoplasty Combined
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of reinforcement of a permanent stoma with mesh to prevent a parastomal hernia A
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of reinforcement of a permanent stoma with mesh to prevent a parastomal hernia A
2017 Americas Hernia Society Quality Collaborative Foundation. All rights reserved.
 The Americas Hernia Society Quality Collaborative (AHSQC) will submit the following measures below on behalf of its eligible professionals to the Center for Medicare and Medicaid Services as a Qualified
The Americas Hernia Society Quality Collaborative (AHSQC) will submit the following measures below on behalf of its eligible professionals to the Center for Medicare and Medicaid Services as a Qualified
Schematic of diagnosing surgical site infections
 Schematic of diagnosing surgical site infections Infection occurred within 30 days after an operation if no implant is in place within one year if an implant is in place eg. hip replacement Do NOT report
Schematic of diagnosing surgical site infections Infection occurred within 30 days after an operation if no implant is in place within one year if an implant is in place eg. hip replacement Do NOT report
Use of Biologics in Abdominal Wall Reconstruction
 Use of Biologics in Abdominal Wall Reconstruction Mike K. Liang Associate Professor of Surgery McGovern Medical School University of Texas Health Science Center Houston, Texas Disclosures No Financial
Use of Biologics in Abdominal Wall Reconstruction Mike K. Liang Associate Professor of Surgery McGovern Medical School University of Texas Health Science Center Houston, Texas Disclosures No Financial
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
Medieval times in surgery Still no solution for:
 Medieval times in surgery Still no solution for: The most frequent complications of the abdominal surgeon: Adhesions Postoperative ileus Incisional hernia Anastomotic leakage Wound infection Incidence
Medieval times in surgery Still no solution for: The most frequent complications of the abdominal surgeon: Adhesions Postoperative ileus Incisional hernia Anastomotic leakage Wound infection Incidence
SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION
 SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION Facts There were an estimated 157,500 surgical site infections associated with inpatient surgeries in 2011. SSIs were the most common healthcare-associated
SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION Facts There were an estimated 157,500 surgical site infections associated with inpatient surgeries in 2011. SSIs were the most common healthcare-associated
Open abdomen in trauma. Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland
 Open abdomen in trauma Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland Frequency and causes of open abdomen - in 23% (344/1531) after trauma laparotomies - damage control
Open abdomen in trauma Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland Frequency and causes of open abdomen - in 23% (344/1531) after trauma laparotomies - damage control
ACTIVE INCISION MANAGEMENT: A PLAN FOR PROTECTING YOUR SURGICAL RESULTS, YOUR PATIENTS AND YOUR HOSPITAL.
 ACTIVE INCISION MANAGEMENT: A PLAN FOR PROTECTING YOUR SURGICAL RESULTS, YOUR PATIENTS AND YOUR HOSPITAL. How active hands-on involvement in managing the incision healing process helps to protect your
ACTIVE INCISION MANAGEMENT: A PLAN FOR PROTECTING YOUR SURGICAL RESULTS, YOUR PATIENTS AND YOUR HOSPITAL. How active hands-on involvement in managing the incision healing process helps to protect your
Citation for published version (APA): de Vries, F. E. E. (2018). Treatment of the complex abdomen and acute intestinal failure
 UvA-DARE (Digital Academic Repository) Treatment of the complex abdomen and acute intestinal failure de Vries, F.E.E. Link to publication Citation for published version (APA): de Vries, F. E. E. (2018).
UvA-DARE (Digital Academic Repository) Treatment of the complex abdomen and acute intestinal failure de Vries, F.E.E. Link to publication Citation for published version (APA): de Vries, F. E. E. (2018).
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
7/2/2015. Incidence. *Mudge M et al, Br. J. Surg, 1985, 72:70-71
 Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Ventral Hernia Repair: Revisonal Surgery Natan Zundel MD FACS Professor of Surgery Vice-Chairman Department of Surgery FIU Herbert Wertheim College of Medicine. Miami Florida DISCLOSURE Ethicon Endosurgery
Colostomy & Ileostomy
 Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Case Report. XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect.
 Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
Case Report XCM Biologic Tissue Matrix. Components separation using sandwich technique for reconstruction of abdominal wall defect. XCM Biologic Tissue Matrix. Components separation using sandwich technique
Abdominal Wound Dehiscence. Presenter: T Mohammed Moderator: Dr H Pienaar
 Abdominal Wound Dehiscence Presenter: T Mohammed Moderator: Dr H Pienaar Introduction Wound Dehiscence is the premature "bursting" open of a wound along surgical suture. It is a surgical complication that
Abdominal Wound Dehiscence Presenter: T Mohammed Moderator: Dr H Pienaar Introduction Wound Dehiscence is the premature "bursting" open of a wound along surgical suture. It is a surgical complication that
One hundred percent fascial approximation with sequential abdominal closure of the open abdomen
 The American Journal of Surgery 192 (2006) 238 242 HowIdoit One hundred percent fascial approximation with sequential abdominal closure of the open abdomen C. Clay Cothren, M.D. a,b, *, Ernest E. Moore,
The American Journal of Surgery 192 (2006) 238 242 HowIdoit One hundred percent fascial approximation with sequential abdominal closure of the open abdomen C. Clay Cothren, M.D. a,b, *, Ernest E. Moore,
Vacuum-Assisted Closure of Perineal War Wound Related to Rectum
 Vacuum-Assisted Closure of Perineal War Wound Related to Rectum Nazım Gümüş, MD Plastic and Reconstructive Surgery Department, Adana Numune Research and Training Hospital, Adana, Turkey Correspondence:
Vacuum-Assisted Closure of Perineal War Wound Related to Rectum Nazım Gümüş, MD Plastic and Reconstructive Surgery Department, Adana Numune Research and Training Hospital, Adana, Turkey Correspondence:
PAPER. Short-term Outcomes With Small Intestinal Submucosa for Ventral Abdominal Hernia
 PAPER Short-term Outcomes With Small Intestinal Submucosa for Ventral Abdominal Hernia W. Scott Helton, MD; Piero M. Fisichella, MD; Robert Berger, MD; Santiago Horgan, MD; Nocif Joseph Espat, MD; Herand
PAPER Short-term Outcomes With Small Intestinal Submucosa for Ventral Abdominal Hernia W. Scott Helton, MD; Piero M. Fisichella, MD; Robert Berger, MD; Santiago Horgan, MD; Nocif Joseph Espat, MD; Herand
Farah S, Kiyingi A, Leinkram C. The Melbourne Hernia Clinic Masada Hospital 26 Balaclava Road St Kilda East Victoria, Australia 3168.
 Medium to Long term results following open intra-abdominal repair of large incisional hernias with a new composite polypropylene and silicone mesh, without components separation. Farah S, Kiyingi A, Leinkram
Medium to Long term results following open intra-abdominal repair of large incisional hernias with a new composite polypropylene and silicone mesh, without components separation. Farah S, Kiyingi A, Leinkram
ABSTRACT. KEY WORDS antibiotics; prophylaxis; hysterectomy
 Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Current Surgical Management of Enterocutaneous Fistulas
 LONDON NORTH WEST HOSPITALS Current Surgical Management of Enterocutaneous Fistulas THIS TALK Surgical prevention of ECF formation Preparing the patient for surgery The surgery to the bowel The surgery
LONDON NORTH WEST HOSPITALS Current Surgical Management of Enterocutaneous Fistulas THIS TALK Surgical prevention of ECF formation Preparing the patient for surgery The surgery to the bowel The surgery
Mesh Performance in Hernia Repair in 2017: A Surgical Review of Progress to Improve Outcomes
 SCIENCE. VALUE. INNOVATION. Mesh Performance in Hernia Repair in 2017: A Surgical Review of Progress to Improve Outcomes Bruce Abell, MD, Samir S. Awad, MD, MPH, J. Augusto Bastidas, MD, George DeNoto,
SCIENCE. VALUE. INNOVATION. Mesh Performance in Hernia Repair in 2017: A Surgical Review of Progress to Improve Outcomes Bruce Abell, MD, Samir S. Awad, MD, MPH, J. Augusto Bastidas, MD, George DeNoto,
COMPARISON BETWEEN SUTURING AND NON-SUTURING OF SUBCUTANEOUS TISSUE IN ELECTIVE ABDOMINAL SURGERIES
 COMPARISON BETWEEN SUTURING AND NON-SUTURING OF SUBCUTANEOUS TISSUE IN ELECTIVE ABDOMINAL SURGERIES *Amit Pal Singh Bawa, Kulwant Singh Ded and Rana Ranjit Singh Department of Surgery, Sri Guru Ramdas
COMPARISON BETWEEN SUTURING AND NON-SUTURING OF SUBCUTANEOUS TISSUE IN ELECTIVE ABDOMINAL SURGERIES *Amit Pal Singh Bawa, Kulwant Singh Ded and Rana Ranjit Singh Department of Surgery, Sri Guru Ramdas
Operative Management of Small Bowel Fistulae Associated with Open Abdomen
 Original Article Operative Management of Small Bowel Fistulae Associated with Open Abdomen Suvit Sriussadaporn, Sukanya Sriussadaporn, Kritaya Kritayakirana and Rattaplee Pak-art, Department of Surgery,
Original Article Operative Management of Small Bowel Fistulae Associated with Open Abdomen Suvit Sriussadaporn, Sukanya Sriussadaporn, Kritaya Kritayakirana and Rattaplee Pak-art, Department of Surgery,
Risk factors for future repeat abdominal surgery
 Langenbecks Arch Surg (2016) 401:829 837 DOI 10.1007/s00423-016-1414-3 ORIGINAL ARTICLE Risk factors for future repeat abdominal surgery Chema Strik 1 & Martijn W. J. Stommel 1 & Laura J. Schipper 1 &
Langenbecks Arch Surg (2016) 401:829 837 DOI 10.1007/s00423-016-1414-3 ORIGINAL ARTICLE Risk factors for future repeat abdominal surgery Chema Strik 1 & Martijn W. J. Stommel 1 & Laura J. Schipper 1 &
Artist s rendering. Count on STRATTICE. The Most Clinically Studied Biological Mesh for Complex Abdominal Wall Repair
 Artist s rendering Count on STRATTICE The Most Clinically Studied Biological Mesh for Complex Abdominal Wall Repair Count on STRATTICE #1 Biological Mesh **
Artist s rendering Count on STRATTICE The Most Clinically Studied Biological Mesh for Complex Abdominal Wall Repair Count on STRATTICE #1 Biological Mesh **
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
-primarily by apposition of the anterior rectus
 2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
4/30/2010. Options for abdominal wall reconstruction. Scott L. Hansen, MD
 Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Open Retromuscular Hernia Repair: Tips and Tricks from the Masters
 Open Retromuscular Hernia Repair: Tips and Tricks from the Masters Eric M. Pauli, MD FACS FASGE Associate Professor of Surgery Director of Endoscopic Surgery Penn State Hershey Medical Center Disclosures
Open Retromuscular Hernia Repair: Tips and Tricks from the Masters Eric M. Pauli, MD FACS FASGE Associate Professor of Surgery Director of Endoscopic Surgery Penn State Hershey Medical Center Disclosures
Discussion of Complex Clinical Scenarios and Variable Review ACS NSQIP Clinical Support Team
 Discussion of Complex Clinical Scenarios and Variable Review CS NSQIP Clinical Support Team SCR Open Q& Calls The CS NSQIP Clinical Team is trialing Open format Q& calls for NSQIP SCRs Participation in
Discussion of Complex Clinical Scenarios and Variable Review CS NSQIP Clinical Support Team SCR Open Q& Calls The CS NSQIP Clinical Team is trialing Open format Q& calls for NSQIP SCRs Participation in
Chapter I 7. Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial
 Chapter I 7 Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial Bastiaan R. Klarenbeek Roberto Bergamaschi Alexander
Chapter I 7 Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial Bastiaan R. Klarenbeek Roberto Bergamaschi Alexander
PERMACOL IMPLANT EVIDENCE SUMMARY
 PERMACOL IMPLANT EVIDENCE SUMMARY Use of Permacol surgical implant in a contaminated or infected field may lead to a weakening or breakdown of the implant. Treat any existing or suspected infection according
PERMACOL IMPLANT EVIDENCE SUMMARY Use of Permacol surgical implant in a contaminated or infected field may lead to a weakening or breakdown of the implant. Treat any existing or suspected infection according
Categorizing Wound Infections: A Comparison between ACS-NSQIP and an Institutional Surgical Secondary Events Database
 : A Comparison between ACS-NSQIP and an Institutional Surgical Secondary Events Database Luke V. Selby MD, Daniel D. Sjoberg MS, Danielle Cassella MA, Mindy Sovel MPH MS, David R. Jones MD, Vivian E. Strong
: A Comparison between ACS-NSQIP and an Institutional Surgical Secondary Events Database Luke V. Selby MD, Daniel D. Sjoberg MS, Danielle Cassella MA, Mindy Sovel MPH MS, David R. Jones MD, Vivian E. Strong
Masatoku Arai 1*, Shiei Kim 1, Hiromoto Ishii 1, Jun Hagiwara 1, Shigeki Kushimoto 2 and Hiroyuki Yokota 1
 Arai et al. World Journal of Emergency Surgery (2018) 1:9 https://doi.org/10.118/s1017-018-0200-7 RESEARCH ARTICLE Open Access The long-term outcomes of early abdominal wall reconstruction by bilateral
Arai et al. World Journal of Emergency Surgery (2018) 1:9 https://doi.org/10.118/s1017-018-0200-7 RESEARCH ARTICLE Open Access The long-term outcomes of early abdominal wall reconstruction by bilateral
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur
 VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
CleanCision. For hospital leaders who want to gain control over the sources of surgical site infection
 CleanCision For hospital leaders who want to gain control over the sources of surgical site infection Surgical site infection, especially in high risk abdominal and colorectal surgery, is a constant threat
CleanCision For hospital leaders who want to gain control over the sources of surgical site infection Surgical site infection, especially in high risk abdominal and colorectal surgery, is a constant threat
Proximal Loop Ileostomy-A Life Saving Approach in ComplicatedEnterocutaneous Fistulas
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 8 Ver. III (Aug. 2014), PP 58-67 Proximal Loop Ileostomy-A Life Saving Approach in ComplicatedEnterocutaneous
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 8 Ver. III (Aug. 2014), PP 58-67 Proximal Loop Ileostomy-A Life Saving Approach in ComplicatedEnterocutaneous
Vacuum-assisted close versus conventional treatment for postlaparotomy wound dehiscence
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.87.5.260 Annals of Surgical Treatment and Research Vacuum-assisted close versus conventional treatment for postlaparotomy
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.87.5.260 Annals of Surgical Treatment and Research Vacuum-assisted close versus conventional treatment for postlaparotomy
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
The use of peritoneal flaps in the repair of large incisional hernia
 The use of peritoneal flaps in the repair of large incisional hernia Marc Huyghe MD GZA St Augustinus Hospital (Antwerp) Mesh 2017 - Paris Peritoneal flap in the repair of incisional hernia - definition
The use of peritoneal flaps in the repair of large incisional hernia Marc Huyghe MD GZA St Augustinus Hospital (Antwerp) Mesh 2017 - Paris Peritoneal flap in the repair of incisional hernia - definition
Case Study. TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis.
 Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT
 STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
Optimizing Hernia Care (It is more than patching a hole!)
 Optimizing Hernia Care (It is more than patching a hole!) Bulent Cetindag M.D. Associate Professor of Surgery University of Iowa Carver College of Medicine Goal of Optimizing Three hundred fifty thousand
Optimizing Hernia Care (It is more than patching a hole!) Bulent Cetindag M.D. Associate Professor of Surgery University of Iowa Carver College of Medicine Goal of Optimizing Three hundred fifty thousand
Preoperative Optimization and Surgical Site Infection Reduction
 Preoperative Optimization and Surgical Site Infection Reduction David Evans, MD Medical Director of Trauma Services Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn
Preoperative Optimization and Surgical Site Infection Reduction David Evans, MD Medical Director of Trauma Services Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn
Preoperative Optimization and Surgical Site Infection Reduction
 Preoperative Optimization and Surgical Site Infection Reduction David Evans, MD Medical Director of Trauma Services Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn
Preoperative Optimization and Surgical Site Infection Reduction David Evans, MD Medical Director of Trauma Services Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn
PREVENA INCISION MANAGEMENT SYSTEM. Product Monograph
 PREVENA INCISION MANAGEMENT SYSTEM Product Monograph TABLE OF CONTENTS Introduction....4 PREVENA Incision Management System Description...4 Design of PREVENA Incision Dressings...5 Indications and Use...6
PREVENA INCISION MANAGEMENT SYSTEM Product Monograph TABLE OF CONTENTS Introduction....4 PREVENA Incision Management System Description...4 Design of PREVENA Incision Dressings...5 Indications and Use...6
For optimal incision management. The PREVENA Therapy portfolio of closed incision management solutions.
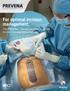 For optimal incision management. The PREVENA Therapy portfolio of closed incision management solutions. The PREVENA Incision Management System manages the surgical incision by: Helping to hold incision
For optimal incision management. The PREVENA Therapy portfolio of closed incision management solutions. The PREVENA Incision Management System manages the surgical incision by: Helping to hold incision
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: July 3,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: July 3,
PREVENA INCISION MANAGEMENT SYSTEM. Product Monograph
 PREVENA INCISION MANAGEMENT SYSTEM Product Monograph TABLE OF CONTENTS Introduction....4 PREVENA Incision Management System Description...4 Design of PREVENA Incision Dressings...5 Indications and Use...6
PREVENA INCISION MANAGEMENT SYSTEM Product Monograph TABLE OF CONTENTS Introduction....4 PREVENA Incision Management System Description...4 Design of PREVENA Incision Dressings...5 Indications and Use...6
The Case FOR Oncoplastic Surgery in Small Breasts. Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA
 The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
PREVENTION OF INCISIONAL HERNIA AFTER MIDLINE LAPAROTOMY FOR ABDOMINAL AORTIC ANEURYSM TREATMENT: A RANDOMIZED CONTROLLED TRIAL
 PREVENTION OF INCISIONAL HERNIA AFTER MIDLINE LAPAROTOMY FOR ABDOMINAL AORTIC ANEURYSM TREATMENT: A RANDOMIZED CONTROLLED TRIAL F. Muysoms 1, T. Vierendeels 2, M. Huyghe 3, M. Miserez 4, M. Ruppert 5,
PREVENTION OF INCISIONAL HERNIA AFTER MIDLINE LAPAROTOMY FOR ABDOMINAL AORTIC ANEURYSM TREATMENT: A RANDOMIZED CONTROLLED TRIAL F. Muysoms 1, T. Vierendeels 2, M. Huyghe 3, M. Miserez 4, M. Ruppert 5,
Process audit for SSI. CME on Infection Prevention & Control Breach Candy Hospital Trust
 Process audit for SSI CME on Infection Prevention & Control Breach Candy Hospital Trust Introduction SSIs are the most common healthcare-associated infection, accounting for 31% of all HAIs among hospitalized
Process audit for SSI CME on Infection Prevention & Control Breach Candy Hospital Trust Introduction SSIs are the most common healthcare-associated infection, accounting for 31% of all HAIs among hospitalized
Abdominal wall reconstruction with components separation and mesh reinforcement in complex hernia repair
 Nockolds et al. BMC Surgery 24, 4:25 http://www.biomedcentral.com/47-2482/4/25 RESEARCH ARTICLE Open Access Abdominal wall reconstruction with components separation and mesh reinforcement in complex hernia
Nockolds et al. BMC Surgery 24, 4:25 http://www.biomedcentral.com/47-2482/4/25 RESEARCH ARTICLE Open Access Abdominal wall reconstruction with components separation and mesh reinforcement in complex hernia
More than 150 consecutive open umbilical hernia repairs in a major Veterans Administration Medical Center
 The American Journal of Surgery (2008) 196, 647 651 The Association of VA Surgeons More than 150 consecutive open umbilical hernia repairs in a major Veterans Administration Medical Center Buckminster
The American Journal of Surgery (2008) 196, 647 651 The Association of VA Surgeons More than 150 consecutive open umbilical hernia repairs in a major Veterans Administration Medical Center Buckminster
Key words: Incisional Hernia, Laparoscopic IPOM, Onlay Mesh Repair, Preperitoneal Mesh Repair.
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4618 1. MBBS Woman Medical Officer Department of Urology Multan Institute of Kidney Diseases, Multan. 2. MBBS House Officer Department of Surgery
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4618 1. MBBS Woman Medical Officer Department of Urology Multan Institute of Kidney Diseases, Multan. 2. MBBS House Officer Department of Surgery
Robotic Ventral Hernia Repair and Endoscopic Component Separation: Outcomes
 SCIENTIFIC PAPER Robotic Ventral Hernia Repair and Endoscopic Component Separation: Outcomes Rodolfo J. Oviedo, MD, FACS, Jarrod C. Robertson, MD, Apurva Sunder Desai, BS ABSTRACT Background and Objectives:
SCIENTIFIC PAPER Robotic Ventral Hernia Repair and Endoscopic Component Separation: Outcomes Rodolfo J. Oviedo, MD, FACS, Jarrod C. Robertson, MD, Apurva Sunder Desai, BS ABSTRACT Background and Objectives:
Modern Management of the Open Abdomen A Cautionary Tale. Grand Rounds December 16, 2010 SUNY, Downstate
 Modern Management of the Open Abdomen A Cautionary Tale Grand Rounds December 16, 2010 SUNY, Downstate Case HPI: 41 yo M BIBA; stabbed in left back while walking out of a shopping center. PMH/PSH: GSW
Modern Management of the Open Abdomen A Cautionary Tale Grand Rounds December 16, 2010 SUNY, Downstate Case HPI: 41 yo M BIBA; stabbed in left back while walking out of a shopping center. PMH/PSH: GSW
Components separation, originally described
 IDEAS AND INNOVATIONS Use of Progressive Tension Sutures in Components Separation: Merging Cosmetic Surgery Techniques with Reconstructive Surgery Outcomes Jeffrey E. Janis, M.D. Dallas, Texas Summary:
IDEAS AND INNOVATIONS Use of Progressive Tension Sutures in Components Separation: Merging Cosmetic Surgery Techniques with Reconstructive Surgery Outcomes Jeffrey E. Janis, M.D. Dallas, Texas Summary:
Research Article Use and Indications of Human Acellular Dermis in Ventral Hernia Repair at a Community Hospital
 Plastic Surgery International Volume 2012, Article ID 918345, 5 pages doi:10.1155/2012/918345 Research Article Use and Indications of Human Acellular Dermis in Ventral Hernia Repair at a Community Hospital
Plastic Surgery International Volume 2012, Article ID 918345, 5 pages doi:10.1155/2012/918345 Research Article Use and Indications of Human Acellular Dermis in Ventral Hernia Repair at a Community Hospital
The use of synthetic mesh in patients undergoing ventral hernia repair during colorectal resection: Risk of infection and recurrence
 Asian Journal of Surgery (2012) 35, 149e153 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com ORIGINAL ARTICLE The use of synthetic mesh in patients undergoing ventral
Asian Journal of Surgery (2012) 35, 149e153 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com ORIGINAL ARTICLE The use of synthetic mesh in patients undergoing ventral
ISPUB.COM. S Saad, E Shakov, V Sebastian, A Saad INTRODUCTION METHODS CASE REPORT 2 CASE REPORT 3 CASE REPORT 1
 ISPUB.COM The Internet Journal of Surgery Volume 11 Number 1 The use of Wound Vacuum-assisted Closure (V.A.C. ) system in the treatment of Recurrent or Complex Pilonidal Cyst Disease: Experience in 4 Adolescent
ISPUB.COM The Internet Journal of Surgery Volume 11 Number 1 The use of Wound Vacuum-assisted Closure (V.A.C. ) system in the treatment of Recurrent or Complex Pilonidal Cyst Disease: Experience in 4 Adolescent
AIDA Study:Primary Onlay Mesh Augmentation following AAA Repair Prevents Incisional Hernia a Multicenter Randomized Trial
 AIDA Study:Primary Onlay Mesh Augmentation following AAA Repair Prevents Incisional Hernia a Multicenter Randomized Trial ES Debus, H. Diener Department for Vascular Medicine, University Heart Center Hamburg
AIDA Study:Primary Onlay Mesh Augmentation following AAA Repair Prevents Incisional Hernia a Multicenter Randomized Trial ES Debus, H. Diener Department for Vascular Medicine, University Heart Center Hamburg
PAPER. Long-term Complications Associated With Prosthetic Repair of Incisional Hernias
 PAPER Long-term Complications Associated With Prosthetic Repair of Incisional Hernias Geoffrey E. Leber, MD; Jane L. Garb, MS; Albert I. Alexander, MD; William P. Reed, MD Objective: To determine whether
PAPER Long-term Complications Associated With Prosthetic Repair of Incisional Hernias Geoffrey E. Leber, MD; Jane L. Garb, MS; Albert I. Alexander, MD; William P. Reed, MD Objective: To determine whether
Infection Control: Surgical Site Infections
 Infection Control: Surgical Site Infections Infectious Disease Epidemiology Section Office of Public Health Louisiana Dept of Health & Hospitals 800-256-2748 www.oph.dhh.louisiana.gov Your taxes at work
Infection Control: Surgical Site Infections Infectious Disease Epidemiology Section Office of Public Health Louisiana Dept of Health & Hospitals 800-256-2748 www.oph.dhh.louisiana.gov Your taxes at work
Managing Complications of Open Hernia Repair
 Managing Complications of Open Hernia Repair 20 Eric M. Pauli and Ryan M. Juza Introduction Abdominal wall hernias are becoming increasingly prevalent as the population ages, surgical management of intra-abdominal
Managing Complications of Open Hernia Repair 20 Eric M. Pauli and Ryan M. Juza Introduction Abdominal wall hernias are becoming increasingly prevalent as the population ages, surgical management of intra-abdominal
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
DO NOT DUPLICATE. Negative pressure wound therapy (NPWT) has revolutionized the
 Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Biodesign E NTEROCUTANEOUS FISTULA PLUG
 Offer a new alternative to patients who have enterocutaneous fistulas, even after standard treatments have been tried. Illustration by Lisa Clark Biodesign E NTEROCUTANEOUS FISTULA PLUG MEDICAL How is
Offer a new alternative to patients who have enterocutaneous fistulas, even after standard treatments have been tried. Illustration by Lisa Clark Biodesign E NTEROCUTANEOUS FISTULA PLUG MEDICAL How is
The Abdominal Compartment Syndrome
 The Abdominal Compartment Syndrome Andre R. Campbell, MD, FACS, FACP, FCCM Professor of Surgery, UCSF Endowed Chair of Surgical Education San Francisco General Hospital Outline Case presentations Review
The Abdominal Compartment Syndrome Andre R. Campbell, MD, FACS, FACP, FCCM Professor of Surgery, UCSF Endowed Chair of Surgical Education San Francisco General Hospital Outline Case presentations Review
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Supplementary Online Content
 Supplementary Online Content Bhangu A, Singh P, Lundy J, Bowley DM. Systemic review and meta-analysis of randomized clinical trials comparing primary vs delayed primary skin closure in contaminated and
Supplementary Online Content Bhangu A, Singh P, Lundy J, Bowley DM. Systemic review and meta-analysis of randomized clinical trials comparing primary vs delayed primary skin closure in contaminated and
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers
 A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
Vacuumed Assisted Closure
 Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
A Comparative Study between Onlay and Pre Peritoneal Mesh Repair in Management of Ventral Hernias
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. II (December. 2016), PP 63-67 www.iosrjournals.org A Comparative Study between Onlay
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. II (December. 2016), PP 63-67 www.iosrjournals.org A Comparative Study between Onlay
Laparoscopic umbilical herniorrhaphy: a novel technique of hernia neck closure and outcomes in the first 19 cases
 Original Article Page 1 of 7 Laparoscopic umbilical herniorrhaphy: a novel technique of hernia neck closure and outcomes in the first 19 cases Cheyenne Vetter 1, Yagan Pillay 2 1 Department of Family Medicine,
Original Article Page 1 of 7 Laparoscopic umbilical herniorrhaphy: a novel technique of hernia neck closure and outcomes in the first 19 cases Cheyenne Vetter 1, Yagan Pillay 2 1 Department of Family Medicine,
Management of Complex Wounds with Vacuum Assisted Closure
 Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection?
 ANNALS OF SURGERY Vol. 237, No. 3, 358 362 2003 Lippincott Williams & Wilkins, Inc. Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection? Chesley Richards,
ANNALS OF SURGERY Vol. 237, No. 3, 358 362 2003 Lippincott Williams & Wilkins, Inc. Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection? Chesley Richards,
A Case Report of a Repair of a Ruptured Incisional Hernia Using Polypropylene Mesh and Component Separation Technique A Rambhajan, T Bernard ABSTRACT
 A Case Report of a Repair of a Ruptured Incisional Hernia Using Polypropylene Mesh and Component Separation Technique A Rambhajan, T Bernard ABSTRACT Incisional hernias are a common complication of laparotomies
A Case Report of a Repair of a Ruptured Incisional Hernia Using Polypropylene Mesh and Component Separation Technique A Rambhajan, T Bernard ABSTRACT Incisional hernias are a common complication of laparotomies
Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts Correspondence to
 East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Open Ventral Hernia Repair
 Open Ventral Hernia Repair Hernia Center/Digestive Disease and Surgery Institute Table of Contents What is a Hernia? 1 What is a Ventral Hernia? 1 What are the Causes and Risk Factors for Developing a
Open Ventral Hernia Repair Hernia Center/Digestive Disease and Surgery Institute Table of Contents What is a Hernia? 1 What is a Ventral Hernia? 1 What are the Causes and Risk Factors for Developing a
Abdominal Wall Modification for the Difficult Ostomy
 Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Boonying Siribumrungwong, M.D., PhD.
 Comparison of Surgical Site Infection between Delayed Primary versus Primary Wound Closure in Complicated Appendicitis; A Multicenter Randomized Controlled Trial Boonying Siribumrungwong, M.D., PhD. Introduction
Comparison of Surgical Site Infection between Delayed Primary versus Primary Wound Closure in Complicated Appendicitis; A Multicenter Randomized Controlled Trial Boonying Siribumrungwong, M.D., PhD. Introduction
V.A.C. Therapy Patient Guide. Are you suffering from a wound? Ask your doctor about V.A.C. Therapy and whether it may be right for you.
 V.A.C. Therapy Patient Guide Are you suffering from a wound? Ask your doctor about V.A.C. Therapy and whether it may be right for you. kci1.com 800.275.4524 Table of Contents Wound Healing is a Process...2
V.A.C. Therapy Patient Guide Are you suffering from a wound? Ask your doctor about V.A.C. Therapy and whether it may be right for you. kci1.com 800.275.4524 Table of Contents Wound Healing is a Process...2
Chapter 14 8/23/2016. Surgical Wound Care. Wound Classifications. Wound Healing. Classified According to. Phases
 Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Surgical Site Infection in Obstetrics Practice
 ORIGINAL ARTICLE Surgical Site Infection in Obstetrics Practice Anila Ansar ABSTRACT Objective Study design Place & Duration of study Methodology To determine the frequency of surgical site infection (SSI),
ORIGINAL ARTICLE Surgical Site Infection in Obstetrics Practice Anila Ansar ABSTRACT Objective Study design Place & Duration of study Methodology To determine the frequency of surgical site infection (SSI),
ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM
 ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM DATA COLLECTION FORM Most Australian hospitals contribute data
ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM DATA COLLECTION FORM Most Australian hospitals contribute data
Session II 11:30 11:45 am. Wound Complications and How to Prevent Them Mark J. Berkowitz, MD Cleveland, Ohio. Disclosure: (n)
 Session II 11:30 11:45 am Wound Complications and How to Prevent Them Mark J. Berkowitz, MD Cleveland, Ohio Disclosure: (n) Wound Complications after ORIF of Calcaneus Fractures and How to Prevent Them
Session II 11:30 11:45 am Wound Complications and How to Prevent Them Mark J. Berkowitz, MD Cleveland, Ohio Disclosure: (n) Wound Complications after ORIF of Calcaneus Fractures and How to Prevent Them
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair
 Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair An inguinal hernia (hernia of the groin) is a weakness in the wall of the abdominal
Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair An inguinal hernia (hernia of the groin) is a weakness in the wall of the abdominal
