PERIOPERATIVE HYPOTHERMIA PREVENTION IN BURN PATIENTS
|
|
|
- Doreen McKinney
- 5 years ago
- Views:
Transcription
1 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care practices based upon the available medical literature and clinical expertise at the time of development. They should not be considered to be accepted protocol or policy, nor are intended to replace clinical judgment or dictate care of individual patients. PERIOPERATIVE HYPOTHERMIA PREVENTION IN BURN PATIENTS SUMMARY Perioperative hypothermia is associated with serious morbidity including blood loss, surgical wound infections, and death. Maintaining euthermia in the burn patient is especially challenging due to the need for significant and prolonged skin exposure to facilitate debridement and skin grafting. Thermoregulation in the operative setting can be accomplished through environmental warming (adjusting the room temperature), cutaneous warming (blankets, forced-air and warm-water circulating devices), and internal warming (intravascular catheters and esophageal warming catheters). RECOMMENDATIONS Level 1 None Level 2 Burn operating rooms should be pre-warmed to at least 24.2 C (76 F) and adjusted according to the patient s total body surface area (TBSA), patient response, and procedure length. All adult burn patients should receive warmed intravenous fluids if >500 mls is administered. All adult burn patients with injuries greater than 10% TBSA should be placed on a waterfluidized warming blanket. Level 3 Esophageal or intravascular warming devices should be considered for patients who: Have greater than 20% TBSA partial and/or full thickness burns Have an anticipated operative time greater than 3 hours Esophageal warming devices may be considered EXCEPT in patients with esophageal pathology or with extensive head/neck edema that interferes with safe esophageal intubation for 5 days post-operatively Esophageal warming devices can be set to a maximum of 42 C Intravascular warming catheters should be considered for placement the day prior to planned surgery and removed as soon as no longer clinically indicated. Intravascular warming devices can be set to a maximum of 42 C Forced air warming devices should not be placed directly on burn wounds INTRODUCTION Perioperative hypothermia is associated with significant morbidity (including increased blood loss and surgical wound infections) and potential mortality. Maintaining euthermia in the burn patient is especially challenging due to the need for prolonged and sometimes extensive skin exposure to facilitate debridement and skin grafting. Thermoregulation in the operative setting can be accomplished through a variety of techniques including environmental warming (adjusting the temperature of the operating room), cutaneous EVIDENCE DEFINITIONS Class I: Prospective randomized controlled trial. Class II: Prospective clinical study or retrospective analysis of reliable data. Includes observational, cohort, prevalence, or case control studies. Class III: Retrospective study. Includes database or registry reviews, large series of case reports, expert opinion. Technology assessment: A technology study which does not lend itself to classification in the above-mentioned format. Devices are evaluated in terms of their accuracy, reliability, therapeutic potential, or cost effectiveness. LEVEL OF RECOMMENDATION DEFINITIONS Level 1: Convincingly justifiable based on available scientific information alone. Usually based on Class I data or strong Class II evidence if randomized testing is inappropriate. Conversely, low quality or contradictory Class I data may be insufficient to support a Level I recommendation. Level 2: Reasonably justifiable based on available scientific evidence and strongly supported by expert opinion. Usually supported by Class II data or a preponderance of Class III evidence. Level 3: Supported by available data, but scientific evidence is lacking. Generally supported by Class III data. Useful for educational purposes and in guiding future clinical research. 1 Approved 03/29/2018
2 warming (blankets, forced-air and warm-water circulating devices), and internal warming (intravascular catheters and esophageal warming catheters). This guideline details the morbidity associated with hypothermia in burn patients with the specific focus of preventing hypothermia in the perioperative setting. BACKGROUND The hypothalamus normally regulates temperature through efferent responses. Behavioral responses require a conscious state not possible during general anesthesia. Autonomic responses can lead to vasoconstriction or perspiration which may be significantly altered during general anesthesia. This occurs primarily due to the vasodilatory effects of anesthesia opposing normal thermoregulatory mechanisms (1,2). Primary hypothermia is caused by environmental exposure to cold, whereas secondary hypothermia results from inadequate physiologic heat production. Advanced Trauma Life Support (ATLS) classifies core temperature hypothermia as mild (32 35 C), moderate (30 32 C), or severe (<30 C). In contrast to severe environmental hypothermia, which is associated with a mortality rate of <25%, even moderate hypothermia associated with severe traumatic injury is associated with a nearly 100% mortality risk (3). Burn patients are at increased risk for hypothermia due to unprotected and prolonged body surface exposure and loss of protective thermoregulation provided by normally intact skin (2). The risk for hypothermia increases exponentially during the resuscitation phase and surgical intervention. Hypothermia can lead to increased wound infections, prolonged hospital length of stay, and worsened post-operative discomfort. Myocardial morbidity may occur with only mild hypothermia. Burn patients undergoing excision of large burn wounds are at risk for increased blood loss, coagulopathy and death (1). Maintaining euthermia aids in the extubation process and decreases the risk of shivering (4). This morbidity does not end with the operating room as burn patients may remain hypothermic post-operatively and require ongoing monitoring and treatment in a critical care setting (5). The morbidity and mortality associated with hypothermia necessitate aggressive intervention, most especially during the critical operative phase of burn treatment. Williams et al. described three warming categories. First, maintaining a warm environment allows for endogenous heat production. Second, active cutaneous warming of the body s surface can be accomplished through multiple modalities. Third, internal rewarming of the body s core is possible using intravascular warming catheters and esophageal heat exchange devices (EHED) (5,6). Regardless of the modality selected, accurate monitoring of core temperature is essential (7). LITERATURE REVIEW The massive inflammatory response to a major burn leads to increased oxygen consumption, catabolism, and resting energy expenditure. Burn-induced hypermetabolism leads to ineffective thermoregulation. Anesthesia administration exacerbates this response and intensifies the heat loss through redistribution of circulating volume. Hypothermia adds further to the metabolic stress. Burn injuries result in increased evaporative losses and often require extended operative times (8). The first approach in preventing intraoperative hypothermia is to warm the environment. Unfortunately, there is extensive heterogeneity within the literature addressing warming of the operating room. Research involving orthopedic surgery suites heated to 25 C and general surgery suites heated to 24 C reveal decreased vasoconstriction and better maintenance of core body temperature. Increasing ambient temperature in the operating room is a common practice in burn surgery. Temperature settings are based on the age and severity of the burns and range between 26.4 C and 37.4 C. The effects of these temperatures are exacerbated when donning surgical garb and are oppressive for the staff, creating an environment that hinders performance. Despite the challenges of warming the operating room and maintaining the heated environment for the duration of the case, the benefit to burn patients makes this an important, and cost effective, intervention (8,9). Skin surface warming is another well-studied intervention to prevent intraoperative hypothermia. Active cutaneous warming is accomplished using water-circulating, resistive and radiant heat, and forced-air 2 Approved 03/29/2018
3 warming (FAW). This modality does not raise core temperature directly, but is effective through increasing the temperature in the peripheral tissue. Applying layers, such as blankets or surgical drapes, offers passive cutaneous warming through insulation. Under body warming devices are not as effective as over body devices due to the reduced efficiency of perfusion to dependent areas. Unfortunately, intraoperative vasoconstriction reduces the efficacy of all cutaneous warming therapies (1). FAW devices are used to prevent and treat hypothermia through surface warming (2). FAW is the most commonly employed modality for skin surface warming (1). Several models are available with different size and shape disposable blankets (7). FAW are composed of an intake system for floor-level air, with an intake filter, blowers, and connecting hoses. This modality has been widely studied and remains the most commonly used. More recently, FAW devices have been criticized due to concern for contamination inside the equipment that can subsequently be emitted, placing patients at risk for infection (10). Furthermore, Williams et al. proposed that FAW systems worsen hypothermia due to water vaporization occurring on the moist surface of larger open burns (6). There are specific risks associated with the use of FAW to include fire, contamination, burn injury, and interference with anesthesia monitoring equipment (7). Additionally, there is increasing concern that air flow may also increase the risk of surgical site infections (SSI). One suspected cause is the potential for bacteria to collect in hoses and the warming unit intake. Additionally, the forced air emission creates airflow disturbances within the operating suite. This interruption of filtered air may permit unwanted dust particles to settle on wounds. Some surgeons delay using these warming devices until the patient is completely prepped and draped, while others no longer utilize them at all. The creator of the Bair Hugger FAW device himself indicated that more recent studies directly correlate use of the FAW and surgical implant contamination. He recommended to discontinue all use of these devices in implant surgery until further studies can be completed (11). A critical literature review by Kellam et al. identified numerous methodological inconsistencies in the available literature leading to a lack of convincing scientific evidence to support the elimination of FAW devices in the perioperative phase (2). Even though bacteria were located within the hoses and intake systems, a causal link between this method and an increase in SSIs was not established. The Federal Drug Administration (FDA) investigated health care provider safety concerns by collecting data from a variety of sources. They were unable to identify a valid correlation between FAW devices and SSIs. Therefore, the FDA continues to recommend FAW as an intervention for preventing hypothermia (12). Fluid warming is recommended for all intraoperative intravenous fluid administration in a volume of greater than 500 ml and provides direct core warming (4). There are several types of fluid warmers to include dry systems, countercurrent exchange, water bath, convective air, and insulator systems (1). Efficacy of fluid warming is impacted by the method selected, rate of administration, and length of tubing (1). Esophageal heat exchange was first described in 1993, but regulating temperature using the gastrointestinal tract was described as far back as the 1950 s. Esophageal temperature is not affected by environmental temperature or any surface warming (13,14). Instead, esophageal warming depends on the natural insulation of the esophagus, fluid temperature and flow rate (13). Esophageal heat exchange devices (EHED) are 60 cm long, flexible, non-sterile silicone tubes inserted into the esophagus and connected to a closed system water circulation device for patient warming and cooling. The device has three ports; one for water infusion, one for water exit for recirculation, and one for gastric emptying (6). EHEDs can be used for warming in the operative and critical care settings with response monitored by core temperature probes. They are inserted in a manner similar to an orogastric tube, through the mouth and into the esophagus (15,16). The EHED is felt to be superior to intravenous heat exchange devices because of the risks for infection and injury associated with invasive catheters. However, it is felt to be insufficient when used alone and is suggested to be used in conjunction with surface warming. Though described more extensively for the induction of hypothermia, research describing its use for preventing or treating hypothermia is limited to a few small case studies (6,13,16,17). 3 Approved 03/29/2018
4 The most invasive method for prevention and treatment of perioperative hypothermia is the intravascular rewarming catheter. It is a unique tool utilized in both the OR and the ICU setting. It has the advantage of warming or cooling the patient from the inside out. Several different types of catheters are on the market and most systems warm the patient through a closed loop system within a balloon that sits within a central venous catheter. The catheter is connected to a regulation system which remotely senses changes in a patient s core temperature and automatically adjusts the temperature to the set target temperature (5). Most systems pump normal saline through the catheter and balloon. As venous blood passes over the balloon, the blood (and patient) is either warmed or cooled. Catheters are placed in either the femoral, internal jugular, or subclavian vein (18-21). Intravascular catheter placement is performed much like a central venous catheter. Once in place, the balloon is inflated to the manufacturer s recommendations. Catheter diameter ranges from 8.5 Fr to 9.3 Fr and length ranges from 20 to 50 cm. Most catheters have 1 to 3 lumens and some include a lumen for fluid and drug administration. Once in place, the thermal regulation system can warm or cool from ºC per hour. Desired temperature is usually achieved within 60 minutes. Certain systems such as the Zoll Thermogard XP have monitoring capabilities that can track patient and system data and electronically transfer it to the patients medical record (19-21). Catheters can stay in place for up to 7 days, but, as with any central venous catheter, should be removed as soon as they are not needed clinically (19-22). Intravascular catheters are placed within the venous system and do not require arterial access. They are placed just like a central venous catheter and do not require additional training for insertion. The system is a closed circuit with sensors located within the balloon if the balloon was to malfunction. The machines are portable and can be moved from the OR to the ICU or vice versa (20). Risks of insertion are much the same as a central venous catheter insertion including misplacement, infection, catheter-related venous thrombosis, hematoma, pneumothorax, and risk to surrounding structures (21-23). There are distinct benefits for the burn patient (and the burn surgery staff) including decreased risk of complications associated with hypothermia, decreased operative times and improved outcomes (21-23). REFERENCES 1. Bindu B, Bindra A, Rath G. Temperature management under general anesthesia: Compulsion or option. Journal of Anaesthesiology Clinical Pharmacology 2017; 33(3): Kellam M, Dieckmann L, Austin P. Forced-Air warming devices and the risk of surgical infection. Journal of Association of Perioperative Nurses 2013; 98(4): American College of Surgeons. Advanced Trauma Life Support. 7th ed. Chicago: American College of Surgeons; pp Ma H, Bingjie L, Dong S, Li X, Cui Y et al. Warming infusion improves perioperative outcomes of elderly patients who underwent bilateral hip replacement. Medicine 2017; 96:13(e6490), 4 pgs. 5. Vaity C, Al-Subaie N, Cecconi M. Cooling devices for targeted temperature management post cardiac arrest. Critical Care 2015; 19: Williams D, Leslie G, Kyriazis D, O Donovan B, Bowes J et al. Use of an esophageal heat exchanger to maintain core temperature during burn excisions and to attenuate pyrexia on the burns intensive care unit. Case Reports in Anesthesiology 2016; Article ID , 6 pgs. 7. Wu X. The safe and efficient use of forced-air warming systems. Journal of Association of Perioperative Nurses 2013; 97(3): Bittner E, Shank E, Woodson L, Martyn L, Jeevendra J. Acute and perioperative care of the burn-injured patient. Anesthesiology 2015; 122(2): Rizzo J, Rowan M, Driscoll I, Chan R, Chung K. Perioperative temperature management during burn care. Journal of Burn Care and Research 2016; e277-e Reed M, Kimberger O, McGovern P, Albrecht M. Forced-Air warming design: Evaluation of intake filtration, internal microbial buildup, and airborne-contamination emissions. Journal of the American Association of Nurse Anesthetist 2013; 81(4): Augustine S. Another perspective on forced-warming and the risk of surgical site infection: Letters to the editor. Journal of Association of Perioperative Nurses 2014; 99(3): Approved 03/29/2018
5 12. Maisel W. (August 20, 2017). US Food and Drug Administration. Information about the use of forced air thermal regulating systems- Letter to health care providers. Accessed February 28, 2018 from https// 13. Kalasbail P, Makarova N, Garrett F, Sessler D. Heating and cooling rates with an esophageal heat exchange device. Anesthesia and Analgeisa 2018; 126(4): Vaicys E, Eason A, Schieber J, Kulstad E. Therapeutic hypothermia induction via an esophageal routea computer simulation. The American Journal of Emergency Medicine 2012; 30: Esophageal Cooling Device: A new approach to patient temperature management. (2015). ECD-081 Rev B. Advanced Cooling Therapy Inc. Chicago, Ill. 16. Kulstad E, Naiman M, Shanley P, Garrett F, Haryu T et al. Temperature modulation with an esophageal heat transfer device- A pediatric swine model study. BioMed Central Anesthesiology 2015; 15: Kulstad E, Metzger A, Courtney DM, Rees J, Shanley P et al. Induction, maintenance, and reversal of therapeutic hypothermia with an esophageal heat transfer device. Resuscitation 2013; 84: Kulstad E, Courtney DM, Waller D. Induction of therapeutic hypothermia via the esophagus: A proof of concept study. World Journal of Emergency Medicine 2012; 3(2): Hegazy A, Lapierre D, Butler R, Althenayan E. Temperature control in critically ill patients with a novel esophageal cooling device: A case series. BioMed Central Anesthesiology 2015; 15:152; 6 pgs. 20. Alsius Corporation, Irvine, California 21. Prunet B, Asencio Y, Lacroix G, et al. Maintenance of normothermia during burn surgery with an intravascular temperature control system: a nonrandomised controlled trial. Injury 2012; 43: Corallo J, King B, Pizano L, Namias N, Schulman C. Core warming of a burn patient during excision to prevent hypothermia. Burns 2008; 34: Davis J, Rodriguez L, Quintana O, Varas R, Pizano L, et al. Use of a warming catheter to achieve normothermia in large burns. Journal of Burn Care and Research 2013; 34: Surgical Critical Care Evidence-Based Medicine Guidelines Committee Primary Author: Scott Zenoni, MD, Susan Smith, PhD, ARNP-C Editor: Michael L. Cheatham, MD Last revision date: March 29, 2018 Please direct any questions or concerns to: webmaster@surgicalcriticalcare.net 5 Approved 03/29/2018
The cold never bother me anymore. R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit
 The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Instituting preventive warming measures for patients who are normothermic. A variety of measures may be used, unless contraindicated.
 Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
3M Bair Hugger System is Safe and Effective Patient Warming Therapy - Response to Misstatements in Lawsuits, September 2016
 3M Bair Hugger System is Safe and Effective Patient Warming Therapy - Response to Misstatements in Lawsuits, September 2016 3M is sympathetic to patients who experience surgical site infections. Any surgery
3M Bair Hugger System is Safe and Effective Patient Warming Therapy - Response to Misstatements in Lawsuits, September 2016 3M is sympathetic to patients who experience surgical site infections. Any surgery
Temperature Monitoring Locations: For TEMP 01, any temperature measurement coming from a physiologic monitor will suffice (peripheral or core).
 Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
Hypothermia Induction Methods
 Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
TEMPERATURE MANAGEMENT
 TEMPERATURE MANAGEMENT Unintentional Hypothermia and the Maintenance of Normothermia Ian Sampson, M.D. SURGICAL CARE IMPROVEMENT PROJECT Temperature Management SCIP INF 7: Colorectal surgery patients with
TEMPERATURE MANAGEMENT Unintentional Hypothermia and the Maintenance of Normothermia Ian Sampson, M.D. SURGICAL CARE IMPROVEMENT PROJECT Temperature Management SCIP INF 7: Colorectal surgery patients with
03RC1- Greif. Temperature Monitoring. Robert Greif - 1 -
 03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
Neurotrauma: The Place for Cooling
 Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Resistive Heating during Off-Pump Coronary Bypass Surgery
 (Acta Anaesth. Belg., 2007, 58, 27-31) Resistive Heating during Off-Pump Coronary Bypass Surgery S. ENGELEN, J.BERGHMANS, S.BORMS, M.SUY-VERBURG and D. HIMPE Summary : Background : Maintaining normothermia
(Acta Anaesth. Belg., 2007, 58, 27-31) Resistive Heating during Off-Pump Coronary Bypass Surgery S. ENGELEN, J.BERGHMANS, S.BORMS, M.SUY-VERBURG and D. HIMPE Summary : Background : Maintaining normothermia
Department of Anaesthesiology, Erasmus University Medical Center, Rotterdam, The Netherlands
 Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy
 Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy Ryohei Miyazaki 1, Kengo Hayamizu 1 and Sumio Hoka 2** Abstract Background:
Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy Ryohei Miyazaki 1, Kengo Hayamizu 1 and Sumio Hoka 2** Abstract Background:
SARASOTA MEMORIAL HOSPITAL. INITIATION AND MAINTAINANCE OF Normothermia/Temperature Managment
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Temperature Management ThermoGard XP or Arctic Sun (crc26) DATE: REVIEWED: PAGES: 5/15 5/18 1 of 8 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: Critical
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Temperature Management ThermoGard XP or Arctic Sun (crc26) DATE: REVIEWED: PAGES: 5/15 5/18 1 of 8 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: Critical
British Journal of Anaesthesia 101 (5): (2008) doi: /bja/aen272 Advance Access publication September 26, 2008
 British Journal of Anaesthesia 101 (5): 627 31 (2008) doi:10.1093/bja/aen272 Advance Access publication September 26, 2008 CLINICAL PRACTICE Effect of prewarming on post-induction core temperature and
British Journal of Anaesthesia 101 (5): 627 31 (2008) doi:10.1093/bja/aen272 Advance Access publication September 26, 2008 CLINICAL PRACTICE Effect of prewarming on post-induction core temperature and
New Therapeutic Hypothermia Techniques
 New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
Targeted Temperature Management: Normothermia for Neuroprotection
 Targeted Temperature Management: Normothermia for Neuroprotection I. Rationale Elevated body temperature is associated with increased cerebral metabolic rate and associated metabolic demand, which can
Targeted Temperature Management: Normothermia for Neuroprotection I. Rationale Elevated body temperature is associated with increased cerebral metabolic rate and associated metabolic demand, which can
Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS
 Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS PRACTICE POINTS Give the right blood product to the right patient at the right time. Failure to correctly check the patient or the pack can be fatal. At the
Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS PRACTICE POINTS Give the right blood product to the right patient at the right time. Failure to correctly check the patient or the pack can be fatal. At the
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
HYPOTHERMIA IN TRAUMA. Kevin Palmer EMT-P, DiMM
 HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
Appendix E: Overview of Vascular
 Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
Postoperative hypothermia and patient outcomes after elective cardiac surgery
 doi:10.1111/j.1365-2044.2011.06784.x ORIGINAL ARTICLE Postoperative hypothermia and patient outcomes after elective cardiac surgery D. Karalapillai, 1 D. Story, 2 G. K. Hart, 3,4 M. Bailey, 5 D. Pilcher,
doi:10.1111/j.1365-2044.2011.06784.x ORIGINAL ARTICLE Postoperative hypothermia and patient outcomes after elective cardiac surgery D. Karalapillai, 1 D. Story, 2 G. K. Hart, 3,4 M. Bailey, 5 D. Pilcher,
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Postoperative hypothermia in geriatric patients undergoing arthroscopic shoulder surgery
 Anesth Pain Med 2019;14:112-116 https://doi.org/10.17085/apm.2019.14.1.112 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received May 18, 2018 Revised 1st, July 12, 2018 2nd, August 4, 2018 Accepted
Anesth Pain Med 2019;14:112-116 https://doi.org/10.17085/apm.2019.14.1.112 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received May 18, 2018 Revised 1st, July 12, 2018 2nd, August 4, 2018 Accepted
Mild hypothermia causes numerous serious
 Insufficiency in a New Temporal-Artery Thermometer for Adult and Pediatric Patients Mohammad-Irfan Suleman, MD*, Anthony G. Doufas, MD, PhD*, Ozan Akça, MD*, Michel Ducharme, PhD, and Daniel I. Sessler,
Insufficiency in a New Temporal-Artery Thermometer for Adult and Pediatric Patients Mohammad-Irfan Suleman, MD*, Anthony G. Doufas, MD, PhD*, Ozan Akça, MD*, Michel Ducharme, PhD, and Daniel I. Sessler,
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Central Venous Access Devices. Stephanie Cunningham Amy Waters
 Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
IV Fluids. Nursing B23. Objectives. Serum Osmolality
 IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
3/6/2017. Endovascular Selective Cerebral Hypothermia First-in-Human Experience
 Endovascular Selective Cerebral Hypothermia First-in-Human Experience Ronald Jay Solar, Ph.D. San Diego, CA 32 nd Annual Snowmass Symposium March 5-10, 2017 Introduction Major limitations in acute ischemic
Endovascular Selective Cerebral Hypothermia First-in-Human Experience Ronald Jay Solar, Ph.D. San Diego, CA 32 nd Annual Snowmass Symposium March 5-10, 2017 Introduction Major limitations in acute ischemic
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
NK8s, Thermogard.pdf. Shyama Marshall RN, BSN Clinical Nurse II, Neuroscience ICU UCI Medical Center
 Shyama Marshall RN, BSN Clinical Nurse II, Neuroscience ICU UCI Medical Center 1 Introduction/Background One of the challenges to registered nurses is hypothermia in burn ICU patients and uncontrollable
Shyama Marshall RN, BSN Clinical Nurse II, Neuroscience ICU UCI Medical Center 1 Introduction/Background One of the challenges to registered nurses is hypothermia in burn ICU patients and uncontrollable
Frostbite. Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department
 Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
IV Fluids Nursing B23 Objectives Serum Osmolality 275 to 295 Isotonic
 1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
2011 Arizant Healthcare Inc. All Rights Reserved A 01/ Arizant Healthcare Inc. All Rights Reserved A 01/11
 Infection Prevention Division Essentials EDU Learning Program UNINTENDED HYPOTHERMIA: THE IMPORTANCE OF MAINTAINING NORMOTHERMIA Disclosure Sponsored by Arizant Healthcare Inc., a 3M company 3M Health
Infection Prevention Division Essentials EDU Learning Program UNINTENDED HYPOTHERMIA: THE IMPORTANCE OF MAINTAINING NORMOTHERMIA Disclosure Sponsored by Arizant Healthcare Inc., a 3M company 3M Health
Cold Injuries: An Update on Hypothermia and Frostbite
 Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Unit 11. Objectives. Indications for IV Therapy. Intravenous Access Devices & Common IV Fluids. 3 categories. Maintenance Replacement Restoration
 Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
Case Presentation. Cooling. Case Presentation. New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation
 New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
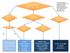 Suspected Hypothermia Temp
Suspected Hypothermia Temp
Cardiothoracic Fellow Expectations Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center
 The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
Inadvertent Perioperative Hypothermia During Orthopedic Surgery
 Inadvertent Perioperative Hypothermia During Orthopedic Surgery Publish date: July 12, 2018 Authors: Chandrakanth Boddu, MD Joseph Cushner Giles R. Scuderi, MD Author Affiliation Disclosures Authors Disclosure
Inadvertent Perioperative Hypothermia During Orthopedic Surgery Publish date: July 12, 2018 Authors: Chandrakanth Boddu, MD Joseph Cushner Giles R. Scuderi, MD Author Affiliation Disclosures Authors Disclosure
Temperature control in critically ill patients with a novel esophageal cooling device: a case series
 Hegazy et al. BMC Anesthesiology (2015) 15:152 DOI 10.1186/s12871-015-0133-6 RESEARCH ARTICLE Open Access Temperature control in critically ill patients with a novel esophageal cooling device: a case series
Hegazy et al. BMC Anesthesiology (2015) 15:152 DOI 10.1186/s12871-015-0133-6 RESEARCH ARTICLE Open Access Temperature control in critically ill patients with a novel esophageal cooling device: a case series
Dr.A.VASUKINATHAN THERMOREGULATION AND ANAESTHESIA:
 Dr.A.VASUKINATHAN In homeothermic species a thermoregulatory system co-ordinates defenses against cold and heat to maintain internal body temperature within a narrow range, thus optimizing normal physiologic
Dr.A.VASUKINATHAN In homeothermic species a thermoregulatory system co-ordinates defenses against cold and heat to maintain internal body temperature within a narrow range, thus optimizing normal physiologic
American College of Surgeons Critical Care Review Course 2012: Infection Control
 American College of Surgeons Critical Care Review Course 2012: Infection Control Overview: I. Central line associated blood stream infection (CLABSI) II. Ventilator associated pneumonia (VAP) I. Central
American College of Surgeons Critical Care Review Course 2012: Infection Control Overview: I. Central line associated blood stream infection (CLABSI) II. Ventilator associated pneumonia (VAP) I. Central
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
Central Venous Catheter Insertion: Assisting
 Approved by: Central Venous Catheter Insertion: Assisting Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Santiago Ensenat Medical Director, Neonatology Neonatal
Approved by: Central Venous Catheter Insertion: Assisting Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Santiago Ensenat Medical Director, Neonatology Neonatal
USE OF FOSPHENYTOIN (CEREBYX ) AND INTRAVENOUS PHENYTOIN (DILANTIN ) IN ADULT PATIENTS
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
Preventing CLABSI & CAUTI Preventive Measures for Central Line Associated Bloodstream Infection & Catheter Associated UTI
 Preventing CLABSI & CAUTI Preventive Measures for Central Line Associated Bloodstream Infection & Catheter Associated UTI Kaiser Permanente For Internal use only Objectives By the end of this lesson, you
Preventing CLABSI & CAUTI Preventive Measures for Central Line Associated Bloodstream Infection & Catheter Associated UTI Kaiser Permanente For Internal use only Objectives By the end of this lesson, you
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation
 Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Insertion of a totally implantable vascular access device (TIVAD)
 Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Victoria Chapman BS, RN, HP (ASCP)
 Victoria Chapman BS, RN, HP (ASCP) Considerations: Age Sex Body Composition Hydration Status Chemotherapy Use Access History Considerations: Immunosuppression Use Chemotherapy Frequency of plasma exchanges
Victoria Chapman BS, RN, HP (ASCP) Considerations: Age Sex Body Composition Hydration Status Chemotherapy Use Access History Considerations: Immunosuppression Use Chemotherapy Frequency of plasma exchanges
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
IV therapy. By: Susan Mberenga, RN, MSN. Copyright 2016, 2013, 2010, 2006, 2002 by Saunders, an imprint of Elsevier Inc.
 IV therapy By: Susan Mberenga, RN, MSN 1 IV Therapy Types of solutions Isotonic Hypotonic Hypertonic Caution: Too rapid or excessive infusion of any IV fluid has the potential to cause serious problems
IV therapy By: Susan Mberenga, RN, MSN 1 IV Therapy Types of solutions Isotonic Hypotonic Hypertonic Caution: Too rapid or excessive infusion of any IV fluid has the potential to cause serious problems
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Veins that are firm to
 Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
It s the solution that counts. 3M skin antiseptic products
 It s the solution that counts 3M skin antiseptic products SoluPrepTM Brand The impact of surgical site infections Surgical site infections (SSIs) are a major burden on healthcare systems, providers and
It s the solution that counts 3M skin antiseptic products SoluPrepTM Brand The impact of surgical site infections Surgical site infections (SSIs) are a major burden on healthcare systems, providers and
The Evidence Base. Stephan A. Mayer, MD. Columbia University New York, NY
 Hypothermic for Cardiac Arrest The Evidence Base Stephan A. Mayer, MD Director, Neuro-ICU Columbia University New York, NY Disclosures Columbia University Clinical Trials Pilot Award Radiant Medical, Inc.
Hypothermic for Cardiac Arrest The Evidence Base Stephan A. Mayer, MD Director, Neuro-ICU Columbia University New York, NY Disclosures Columbia University Clinical Trials Pilot Award Radiant Medical, Inc.
Vaxcel Implantable Ports Valved and Non-Valved. A Patient s Guide
 Vaxcel Implantable Ports Valved and Non-Valved A Patient s Guide Vaxcel Implantable Port This pamphlet provides some answers to questions you may have about your implantable port and how to care for it
Vaxcel Implantable Ports Valved and Non-Valved A Patient s Guide Vaxcel Implantable Port This pamphlet provides some answers to questions you may have about your implantable port and how to care for it
Clinical experience with an active intravascular rewarming technique for near-severe hypothermia associated with traumatic injury
 Kiridume et al. Journal of Intensive Care 2014, 2:11 CASE REPORT Open Access Clinical experience with an active intravascular rewarming technique for near-severe hypothermia associated with traumatic injury
Kiridume et al. Journal of Intensive Care 2014, 2:11 CASE REPORT Open Access Clinical experience with an active intravascular rewarming technique for near-severe hypothermia associated with traumatic injury
Prevention of Hypothermia During Interventional Cardiology Procedures in Adults
 ISPUB.COM The Internet Journal of Anesthesiology Volume 23 Number 2 Prevention of Hypothermia During Interventional Cardiology Procedures in Adults K Wagner, C Smith, K Quan Citation K Wagner, C Smith,
ISPUB.COM The Internet Journal of Anesthesiology Volume 23 Number 2 Prevention of Hypothermia During Interventional Cardiology Procedures in Adults K Wagner, C Smith, K Quan Citation K Wagner, C Smith,
All Things Cold: Hypothermia, Altitude Illness and Frostbite. Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine
 All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
How and why I give IV fluid Disclosures SCA Fluids and public health 4/1/15. Andrew Shaw MB FRCA FCCM FFICM
 How and why I give IV fluid Andrew Shaw MB FRCA FCCM FFICM Professor and Chief Cardiothoracic Anesthesiology Vanderbilt University Medical Center 2015 Disclosures Consultant for Grifols manufacturer of
How and why I give IV fluid Andrew Shaw MB FRCA FCCM FFICM Professor and Chief Cardiothoracic Anesthesiology Vanderbilt University Medical Center 2015 Disclosures Consultant for Grifols manufacturer of
Acute And perioperative care of the burn-injured patient. Anesthesiology, V 122, No 2
 Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Cold Injuries: Frostbite and Hypothermia. Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University
 Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program
 PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
The University of Toledo Medical Center and its Medical Staff
 Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
Central Line Care and Management
 Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
SYMBOLOGY. = Manufacturer. = Manufacturing Serial Number. = Manufacturing Lot Number = Catalog Number LOT REF. = Do not resterilize Single Use Only
 damage or expenses directly or indirectly arising from use of this product. This warranty is in lieu of and excludes all other warranties not expressly set forth herein, whether express or implied by operation
damage or expenses directly or indirectly arising from use of this product. This warranty is in lieu of and excludes all other warranties not expressly set forth herein, whether express or implied by operation
Therapeutic Hypothermia for Post Cardiac Arrest Plan Initial Orders
 Arrest Plan Initial Orders Weight Allergies Therapeutic Hypothermia Guidelines ***Required to continue with ordering Plan.*** Strict Intake and Output q1h, throughout cooling and re warming. Set Up for
Arrest Plan Initial Orders Weight Allergies Therapeutic Hypothermia Guidelines ***Required to continue with ordering Plan.*** Strict Intake and Output q1h, throughout cooling and re warming. Set Up for
IV Link Staff. Infection Prevention & Control A Learning Package for IV Link Staff
 IV Link Staff Infection Prevention & Control A Learning Package for IV Link Staff Purpose This learning package provides key infection prevention messages and direction for knowledge that you require as
IV Link Staff Infection Prevention & Control A Learning Package for IV Link Staff Purpose This learning package provides key infection prevention messages and direction for knowledge that you require as
SCIP-Inf-10. Pediatric Warming Solutions. Complete. Pediatric Warming
 Pediatric Warming Solutions SCIP-Inf-10 goals achieve Complete Pediatric Warming You know the importance of keeping your littlest patients warm, so why trust them to anyone but the leader in patient warming?
Pediatric Warming Solutions SCIP-Inf-10 goals achieve Complete Pediatric Warming You know the importance of keeping your littlest patients warm, so why trust them to anyone but the leader in patient warming?
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Quality ID #76: Prevention of Central Venous Catheter (CVC) - Related Bloodstream Infections National Quality Strategy Domain: Patient Safety
 Quality ID #76: Prevention of Central Venous Catheter (CVC) - Related Bloodstream Infections National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Quality ID #76: Prevention of Central Venous Catheter (CVC) - Related Bloodstream Infections National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
ECMO vs. CPB for Intraoperative Support: How do you Choose?
 ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
The Impact of Healthcare Associated Infection (HCAI)
 Instructions for use Save this presentation Feel free to add or delete slides as necessary, change information to suit local needs and as new guidance or evidence is published Disclaimer: Whilst the working
Instructions for use Save this presentation Feel free to add or delete slides as necessary, change information to suit local needs and as new guidance or evidence is published Disclaimer: Whilst the working
Chapter 23 Unit 28. Therapeutic Modalities
 Chapter 23 Unit 28 Therapeutic Modalities Chapter Objectives Discuss the purpose of therapeutic modalities Explain the legal implications associated with the use of therapeutic modalities List the different
Chapter 23 Unit 28 Therapeutic Modalities Chapter Objectives Discuss the purpose of therapeutic modalities Explain the legal implications associated with the use of therapeutic modalities List the different
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute pain, outcomes assessment of evidence-based guidelines and registries, 124 125 Adverse event tracking, improved, with anesthesia
Index Note: Page numbers of article titles are in boldface type. A Acute pain, outcomes assessment of evidence-based guidelines and registries, 124 125 Adverse event tracking, improved, with anesthesia
Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia
 Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia 1 Definition of hypothermia: Body temperature below 95 F / 35 C (ranges 34 36) Normal temperature is 98.6
Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia 1 Definition of hypothermia: Body temperature below 95 F / 35 C (ranges 34 36) Normal temperature is 98.6
Induced Hypothermia for Cardiac Arrest. Heather Hand RN,CCRN,CNRN,ATCN,LNC
 Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
CIE Biology GCSE. 9: Transport in animals. Notes.
 CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
Therapeutic hypothermia
 INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
Quality ID#164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clincial Care
 Quality ID#164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clincial Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Quality ID#164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clincial Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
SENSATION and CS300 Smaller meets faster. IABP System
 SENSATION and CS300 Smaller meets faster IABP System Cardiac Assist SENSATION and CS300 3 Cardiac Assist SENSATION and CS300 5 Smaller The SENSATION 7Fr. Fiber-Optic IAB Catheter Faster The CS300 with
SENSATION and CS300 Smaller meets faster IABP System Cardiac Assist SENSATION and CS300 3 Cardiac Assist SENSATION and CS300 5 Smaller The SENSATION 7Fr. Fiber-Optic IAB Catheter Faster The CS300 with
SYSTEM-WIDE POLICY & PROCEDURE MANUAL. Policy Title: Hypothermia Post Cardiac Arrest Policy Number: PC-124. President & CEO Page 1 of 9
 Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart. O Wenker, L Chaloupka, R Joswiak, D Thakar, C Wood, G Walsh
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST
 THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
ISPUB.COM. Intravenous Infusion Sets (IV Set) In Anesthesia Practice: A Survey On Their Use And A Look Into The Future. A Hadzic, J Vloka INTRODUCTION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 4 Number 4 Intravenous Infusion Sets (IV Set) In Anesthesia Practice: A Survey On Their Use And A Look Into The A Hadzic, J Vloka Citation A Hadzic,
ISPUB.COM The Internet Journal of Anesthesiology Volume 4 Number 4 Intravenous Infusion Sets (IV Set) In Anesthesia Practice: A Survey On Their Use And A Look Into The A Hadzic, J Vloka Citation A Hadzic,
Intravascular Ultrasound
 Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Initial placement 20FR Guidewire PEG kit REORDER NO:
 Initial placement 20FR Guidewire PEG kit REORDER NO: 00710802 INSTRUCTIONS FOR USE 1 of 5 These products have been manufactured not to include latex. Intended Use: The Initial placement 20FR Guidewire
Initial placement 20FR Guidewire PEG kit REORDER NO: 00710802 INSTRUCTIONS FOR USE 1 of 5 These products have been manufactured not to include latex. Intended Use: The Initial placement 20FR Guidewire
CASE PRIMERS. Pediatric Anesthesia Fellowship Program. Laryngotracheal Reconstruction (LTR) Tufts Medical Center
 CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
