NRP Raising the Bar for Providers and Instructors
|
|
|
- Delphia Cook
- 5 years ago
- Views:
Transcription
1 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility may require more frequent renewal. 2. Any person who works with newborns is eligible to take an NRP Provider course; however, the course has little relevance for a person who has never seen a healthy term newborn at birth. 3. All learners may study, practice and demonstrate all NRP skills if desired, including intubation and emergency umbilical venous catheter placement. NRP does not certify or ensure competence to perform these skills in an actual resuscitation. 4. The recommended NRP instructor to learner ratio at a Provider course is 1 instructor: 3-4 learners. Programmatic Changes 1. Two new Performance Checklists: a. Lesson 1: Equipment Check b. Lesson 5: Laryngeal Mask Airway Placement 2. There is no more Renewal Course. Everyone takes a Provider Course tailored to learners needs. 3. Each institution determines its own policy about what happens if NRP provider status expires. 4. The Online Examination is required for the 6 th edition. The 5 th edition examination may be offered as a hard copy exam or online exam until December 31, No more hard copy examination is available after December Provider Course includes little or no lecture, uses course time for hands-on learning, immersive simulations, and constructive debriefings. a. The Performance Skills Stations are optional and used for learning, review, and practice. b. The NRP online examination and Integrated Skills Station (similar to Megacode) are required and used for evaluation. c. The Simulation and Debriefing component is required and used to improve teamwork and communication. 6. Teamwork and communication skills are just as important as cognitive and technical skills. The 10 NRP Key Behavioral Skills are Know your environment. Anticipate and plan. Assume the leadership role. Communicate effectively. Delegate workload optimally. Allocate attention wisely Use all available information. Use all available resources Call for help when needed. Maintain professional behavior. March 2011 Page 1 of 7
2 Science Changes 1. The following items are no longer optional in the birth setting, and should be available for every birth: a. Compressed air source b. Oxygen blender to mix oxygen and compressed air with flowmeter c. Pulse oximeter for neonatal use and oximeter probe d. Laryngeal mask airway (size 1) 2. There are 2 levels of post-resuscitation care (instead of 3 levels): a. Routine Care: For vigorous term babies with no risk factors and babies who have responded to the initial steps. Babies who required initial steps may not need to be separated from their mothers after birth to receive close monitoring and further stabilization. b. Post-resuscitation care: For babies who have depressed breathing or activity, and/or require supplemental oxygen. Require frequent evaluation. Some may transition to routine care; others will require ongoing support. Transfer to an intensive care nursery may be necessary. 3. Prior to beginning the steps in the NRP Flow Diagram, ask the OB provider for relevant perinatal history, including these questions: a. What is the gestational age? b. Is the fluid clear? c. How many babies are expected? d. Are there any additional risk factors? 4. At birth, answer 3 questions to determine the need for initial steps at the radiant warmer: a. Is the newborn term? b. Is the newborn breathing or crying? c. Does the newborn have good muscle tone? If any answer is No, the newborn should receive initial steps at the radiant warmer. 5. The vigorous meconium-stained newborn need not receive initial steps at the radiant warmer, but may receive routine care (with appropriate monitoring) with his mother. 6. Routine care of newborn staying with mother: a. Warm (skin-to-skin contact is recommended), clear airway by wiping the baby s mouth and nose if necessary, dry the newborn, provide ongoing evaluation of breathing, activity, and color. 7. Suctioning following birth (including bulb suctioning with a bulb syringe) should be reserved for babies who have obvious obstruction to spontaneous breathing or who require positivepressure ventilation. 8. After clearing the airway as necessary, drying and removing wet linen, repositioning, and stimulating, evaluate respirations and heart rate (not color). March 2011 Page 2 of 7
3 a. If HR is less than 100 bpm, or if newborn is apneic or gasping, begin positive-pressure ventilation. b. If HR is more than 100 bpm and respirations are labored, consider CPAP, especially for preterm newborns. 9. Subsequently, evaluation and decision-making are based on respirations, HR, and oxygenation (per pulse oximetry). 10. Resuscitation of term newborns may begin with 21% oxygen; resuscitation of preterm newborns may begin with a somewhat higher oxygen concentration. 11. Use pulse oximetry when: a. Resuscitation is anticipated b. PPV is required for more than a few breaths c. Central cyanosis is persistent, or you need to confirm your perception of central cyanosis d. Supplemental oxygen is administered 12. Place the oximeter probe on the newborn s right hand or wrist (measure pre-ductal saturation) and then connect it to the instrument. 13. Using pulse oximetry, supplemental oxygen concentration should be adjusted to achieve the target values for pre-ductal saturations summarized in the table on the NRP Flow Diagram. The table is used for both term and preterm babies. 14. Indications for positive-pressure ventilation: a. Apnea/gasping b. Heart rate below 100 bpm, even if breathing c. Persistent central cyanosis and low oxygen saturation, despite free-flow oxygen increased to 100%. 15. All positive-pressure devices, including the self-inflating bag, should have an integral pressure gauge, or if there is a site for attaching a pressure gauge (manometer), it should be attached. 16. When PPV begins, assess for rising heart rate and improving oxygen saturation (per pulse oximetry). If not evident (within 5-10 breaths), ask your assistant to assess bilateral breath sounds and chest movement. If these are not immediately evident, perform as many of the ventilation corrective steps as needed to achieve bilateral breath sounds and chest movement. 17. Note that the timeline down the side of the NRP Flow Diagram stops here, but it may take longer than 30 seconds to establish effective positive-pressure ventilation (defined by bilateral breath sounds and chest movement). March 2011 Page 3 of 7
4 18. Use MR SOPA to help you remember the ventilation corrective steps in order: M: Adjust the mask on the face. R: Reposition the head to ensure an open airway. Re-attempt ventilation. If not effective, S: Suction the mouth and nose O: Ventilate with the baby s mouth slightly open and lift the jaw forward. Re-attempt ventilation. If not effective, P: Gradually increase pressure every few breaths, (cautiously, and to a maximum of 40 cm H 2 0), until there are bilateral breath sounds and visible chest movement. If ventilation is still not effective, A: Consider airway alternative (endotracheal tube or laryngeal mask airway) 19. If the heart rate is below 60 bpm despite 30 seconds of effective positive-pressure ventilation (defined by audible bilateral breath sounds and chest movement) begin chest compressions. 20. When the heart rate is below 60 bpm, the oximeter may not function. When chest compressions begin, increase the oxygen concentration to 100% until the oximeter is giving a reliable signal and can guide the appropriate adjustment of supplemental oxygen. 21. Intubation is strongly recommended when chest compressions begin to help ensure effective ventilation. 22. The intubation procedure ideally should be completed within 30 seconds (not 20 seconds). Do not administer free-flow oxygen during the intubation procedure to an apneic newborn. 23. Interruption of chest compressions to check the heart rate may result in a decrease of perfusion pressure in the coronary arteries. Therefore, continue chest compressions and coordinated ventilations for at least seconds before stopping briefly to assess the heart rate. 24. If you anticipate the need to place an emergency umbilical venous catheter, continue chest compressions by moving to the head of the bed (near the infant s head) and continuing the 2- thumb technique. This is most easily accomplished if the newborn is intubated. March 2011 Page 4 of 7
5 25. The laryngeal mask airway has been shown to be an effective alternative for assisting ventilation. Use may be indicated when a. Facial or upper airway malformations render ventilation by mask ineffective. b. Positive-pressure ventilation with a face mask fails to achieve effective ventilation and intubation is not possible. 26. Epinephrine is indicated when the heart rate remains below 60 bpm after 30 seconds of effective assisted ventilation (preferably via endotracheal tube) and at least another seconds of coordinated chest compressions and effective ventilation. 27. The intratracheal route is associated with unreliable absorption and is likely to be ineffective. Nevertheless, since the endotracheal route is the most readily accessible, administration of a dose of epinephrine via an endotracheal tube may be considered while the intravenous route is being established. 28. Epinephrine administration (IV parameters unchanged; note new dose for intratracheal epinephrine) a. Recommended concentration: 1:10,000 (0.1 mg/ml) b. Recommended route: Intravenous (umbilical vein). Consider endotracheal route ONLY while IV access being obtained c. Give rapidly as quickly as possible. d. Recommended IV dose: ml/kg of 1:10,000 solution per umbilical vein in a 1-mL syringe. Follow IV administration of epinephrine with ml flush of normal saline. e. Recommended intratracheal dose: ml/kg of 1:10,000 solution per endotracheal tube in a 3-6 ml syringe. f. Check the newborn heart rate about 1 minute after administering epinephrine (longer if given endotracheally). Epinephrine dose may be repeated every 3-5 minutes. 29. Therapeutic hypothermia following perinatal asphyxia should be a. Used only for babies > 36 weeks gestation and who meet previously defined criteria for this therapy b. Initiated before 6 hours after birth c. Used only by centers with specialized programs equipped to provide the therapy 30. To help keep the preterm baby warm, a. Increase the temperature of the delivery room and the area where the baby will be resuscitated to approximately 25⁰C to 26⁰C (77⁰F-79⁰F) b. Use polyethylene plastic wrap for babies delivered at less than 29 weeks gestation (or 28 weeks and less). Use a sheet of plastic food wrap, a food-grade 1-gallon plastic bag, or a commercially available sheet of polyethylene plastic. c. Place a portable warming pad under layers of towels on the resuscitation table. March 2011 Page 5 of 7
6 Information for NRP Instructors 1. HealthStream is the vendor for the 6 th edition NRP online examination. The fee for the exam varies depending on how many exams are purchased and how the examination is accessed. If your institution uses HealthStream as its Learning Management System, your learners may receive the examination in the same way other hospital learning programs are obtained. If your institution is not a HealthStream client, you may purchase online examinations in small or large volume purchases. HealthStream will set up a website for your use. Individuals may also purchase an online examination with a personal credit card. For more information, visit and click on Online Examination. 2. Simulation training is dependent on good methodology, not technology; therefore, sophisticated electronic simulators are not necessary. 3. NRP Instructor Maintenance Requirements (includes Regional Trainers) a. Each current NRP instructor must own a personal copy of the NRP Instructor DVD: An Interactive Tool for Facilitation of Simulation-based Learning and complete the post-dvd education activity by January 1, Your DVD is licensed to one computer and cannot be used on multiple devices after launching the program. Launch it on the computer where it will be viewed! b. Each instructor must teach or co-teach at least 2 courses in the 2 years for which their instructor card is valid. c. Beginning in January 2013, every NRP instructor must take the online examination (Lessons 1 through 9) prior to their instructor status renewal date. Beginning in spring 2011, every instructor may take the online examination once/calendar year if desired at no charge; however, continuing education credit may be awarded only once every two years. 4. NRP Instructor eligibility a. Only registered nurses (including NNPs, CNMs, etc), physicians (MD or DO), respiratory therapists, and physician assistants are eligible to become NRP instructors. There are no exceptions and no waivers. Professionals who became NRP instructors by waiver in the past will maintain their instructor status as long as maintenance requirements are met. b. NRP instructor candidates are required to meet prerequisites prior to their NRP Instructor Course. Instructor candidates must have current NRP provider status (Lessons 1 through 9), produce a letter of recommendation and support from their manager/hospital administrator, pass the 6 th edition online examination in the 30 days before their Instructor Course (Lessons 1 through 9), watch the NRP Instructor DVD and complete the post-dvd education activity, and take the Instructor Self-Assessment, which is included in the NRP Instructor Manual th edition NRP materials will be available in May March 2011 Page 6 of 7
7 NRP Flow Diagram March 2011 Page 7 of 7
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Resuscitation efforts for Mom & Baby
 Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني
 Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Neonatal Resuscitation in What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011
 Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Steven Ringer MD PhD April 5, 2011
 Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
1 Pediatric Advanced Life Support Science Update What s New for 2010? 3 CPR. 4 4 Steps of BLS Survey 5 CPR 6 CPR.
 1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
Neonatal/Pediatric Cardiopulmonary Care
 Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Learning Station Competency Checklists
 Learning Station Competency Checklists Cardiac Arrest: Shockable Rhythm Team Dynamics Practice Demonstrates effective team dynamics (see, below) Performs manual maneuvers to open airway* Initiates assisted
Learning Station Competency Checklists Cardiac Arrest: Shockable Rhythm Team Dynamics Practice Demonstrates effective team dynamics (see, below) Performs manual maneuvers to open airway* Initiates assisted
EMERGENCY CARE. Advanced Patient Simulators 116 CALL US TOLL FREE AT
 EMERGENCY CARE Advanced Patient Simulators 116 CALL US TOLL FREE AT 800.882.6655 Our Code Blue III ALS training simulators allow you to teach high-performance, quality CPR by providing you with real-time
EMERGENCY CARE Advanced Patient Simulators 116 CALL US TOLL FREE AT 800.882.6655 Our Code Blue III ALS training simulators allow you to teach high-performance, quality CPR by providing you with real-time
EQUIPMENT: Nitrous Oxygen Delivery System:
 Policy: Nitrous Oxide Use in the Intrapartum and Immediate Postpartum Period for Obstetrical Patients in the Family Birth Place Approvers: CEO. CNO, Medical Staff President, Anesthesia Chair, OB Medical
Policy: Nitrous Oxide Use in the Intrapartum and Immediate Postpartum Period for Obstetrical Patients in the Family Birth Place Approvers: CEO. CNO, Medical Staff President, Anesthesia Chair, OB Medical
Code Blue III PLUS. Emergency Care Simulators
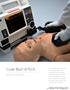 Code Blue III PLUS Emergency Care Simulators Our Code Blue III system teaches ALS skills using realistic code scenarios. Each step you take is monitored by software providing important feedback, not only
Code Blue III PLUS Emergency Care Simulators Our Code Blue III system teaches ALS skills using realistic code scenarios. Each step you take is monitored by software providing important feedback, not only
Neonatal Resuscitation
 Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The student guide to simulation
 CETL 2008 1 The following guide will introduce you to what the simulators can do But firstly a few words on communication Please verbally and non-verbally communicate with the simulator as if it were a
CETL 2008 1 The following guide will introduce you to what the simulators can do But firstly a few words on communication Please verbally and non-verbally communicate with the simulator as if it were a
Module 2: Facilitator instructions for Airway & Breathing Skills Station
 Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
NEONATOLOGY Healthy newborn. Neonatal sequelaes
 NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
ISPUB.COM. The Use of LMA in Newborn Resuscitation. R Vadhera INTRODUCTION VENTILATION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 1 Number 4 The Use of LMA in Newborn Resuscitation R Vadhera Citation R Vadhera. The Use of LMA in Newborn Resuscitation. The Internet Journal of
ISPUB.COM The Internet Journal of Anesthesiology Volume 1 Number 4 The Use of LMA in Newborn Resuscitation R Vadhera Citation R Vadhera. The Use of LMA in Newborn Resuscitation. The Internet Journal of
Pediatric Advanced Life Support Overview Judy Haluka BS, RCIS, EMT-P
 Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
MASTER SYLLABUS
 A. Academic Division: Health Sciences B. Discipline: Respiratory Care MASTER SYLLABUS 2018-2019 C. Course Number and Title: RESP 2330 Advanced Life Support Procedures D. Course Coordinator: Tricia Winters,
A. Academic Division: Health Sciences B. Discipline: Respiratory Care MASTER SYLLABUS 2018-2019 C. Course Number and Title: RESP 2330 Advanced Life Support Procedures D. Course Coordinator: Tricia Winters,
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Stabilization of the Newborn for Transport. Relevant Disclosure. Learning Objectives
 Stabilization of the Newborn for Transport Arlen Foulks, DO FAAP FACOP Medical Director, CCMH Level II NICU Medical Director, NeoFlight Assistant Professor of Pediatrics Neonatal Perinatal Medicine Section,
Stabilization of the Newborn for Transport Arlen Foulks, DO FAAP FACOP Medical Director, CCMH Level II NICU Medical Director, NeoFlight Assistant Professor of Pediatrics Neonatal Perinatal Medicine Section,
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Competency Indicators Pediatrics Registered Nurse
 Hospital Logo Competency Indicators Pediatrics Registered Nurse mployee Name: Review Key: = ducation Session valuation Key: Able to perform & document A: Airway assessment: mployee Describes unique airway
Hospital Logo Competency Indicators Pediatrics Registered Nurse mployee Name: Review Key: = ducation Session valuation Key: Able to perform & document A: Airway assessment: mployee Describes unique airway
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
10/13/2017. Newborn Care. Objectives. Cardiac Anatomy. Managing Transitional Physiology
 Newborn Care Managing Transitional Physiology Mary Coughlin MS, NNP, RNC-E President and Founder Caring Essentials Collaborative Boston, MA Objectives Upon completion of the learning session participants
Newborn Care Managing Transitional Physiology Mary Coughlin MS, NNP, RNC-E President and Founder Caring Essentials Collaborative Boston, MA Objectives Upon completion of the learning session participants
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Preface. The ACoRN Neonatal Society. ACoRN xiii
 Preface For most health professionals, few events are more challenging or stressful than caring for a sick or preterm baby. It is therefore not surprising that the management and stabilization of these
Preface For most health professionals, few events are more challenging or stressful than caring for a sick or preterm baby. It is therefore not surprising that the management and stabilization of these
A SYNOPSIS BY ILCOR PEDIATRIC TASK FORCE. Pediatric Basic Life Support, Pediatric Advanced Life Support and Neonatal Resuscitation 2015
 Vol. 2 - No.4 October - December 2015 83 Vol. 2 - No.4 October - December 2015 84 There is new evidence that when treating pediatric septic shock in specific settings, the use of restricted volume of isotonic
Vol. 2 - No.4 October - December 2015 83 Vol. 2 - No.4 October - December 2015 84 There is new evidence that when treating pediatric septic shock in specific settings, the use of restricted volume of isotonic
And Then There Were Two. Renae Buehner RNC, BSN Avera McKennan Labor and Delivery Unit Supervisor, Lead OB Flight RN
 And Then There Were Two Renae Buehner RNC, BSN Avera McKennan Labor and Delivery Unit Supervisor, Lead OB Flight RN Disclosures I have none She s coming in hot Assisting the maternal patient in a safe
And Then There Were Two Renae Buehner RNC, BSN Avera McKennan Labor and Delivery Unit Supervisor, Lead OB Flight RN Disclosures I have none She s coming in hot Assisting the maternal patient in a safe
Introduce the basics of the newborn resuscitation period Practice calculations for TPN orders Learn how to manage basic ventilator settings
 Introduce the basics of the newborn resuscitation period Practice calculations for TPN orders Learn how to manage basic ventilator settings Complex concepts you may be expected to know Not taught this
Introduce the basics of the newborn resuscitation period Practice calculations for TPN orders Learn how to manage basic ventilator settings Complex concepts you may be expected to know Not taught this
Department of Paediatrics Clinical Guideline. Advanced Paediatric Life Support. Sequence of actions. 1. Establish basic life support
 Advanced Paediatric Life Support Sequence of actions 1. Establish basic life support 2. Oxygenate, ventilate, and start chest compression: - Provide positive-pressure ventilation with high-concentration
Advanced Paediatric Life Support Sequence of actions 1. Establish basic life support 2. Oxygenate, ventilate, and start chest compression: - Provide positive-pressure ventilation with high-concentration
Guidelines Administrative Practice X Clinical Practice Professional Practice
 Guidelines Administrative Practice X Clinical Practice Professional Practice End Tidal CO 2 (EtCO2) Monitoring Using the Zoll Monitor/Defibrillator Page 1 of 4 Scope: Outcome: Respiratory Therapists (RT),
Guidelines Administrative Practice X Clinical Practice Professional Practice End Tidal CO 2 (EtCO2) Monitoring Using the Zoll Monitor/Defibrillator Page 1 of 4 Scope: Outcome: Respiratory Therapists (RT),
Airway Clearance Devices
 Print Page 1 of 11 Wisconsin.gov home state agencies subject directory department of health services Search Welcome» August 2, 2018 5:18 PM Program Name: BadgerCare Plus and Medicaid Handbook Area: Durable
Print Page 1 of 11 Wisconsin.gov home state agencies subject directory department of health services Search Welcome» August 2, 2018 5:18 PM Program Name: BadgerCare Plus and Medicaid Handbook Area: Durable
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Agency 71. Kansas Dental Board (Authorized by K.S.A and (Authorized by K.S.A and
 Agency 71 Kansas Dental Board Articles 71-4. CONTINUING EDUCATION REQUIREMENTS. 71-5. SEDATIVE AND GENERAL ANAESTHESIA. 71-11. MISCELLANEOUS PROVISIONS. Article 4. CONTINUING EDUCATION REQUIREMENTS 71-4-1.
Agency 71 Kansas Dental Board Articles 71-4. CONTINUING EDUCATION REQUIREMENTS. 71-5. SEDATIVE AND GENERAL ANAESTHESIA. 71-11. MISCELLANEOUS PROVISIONS. Article 4. CONTINUING EDUCATION REQUIREMENTS 71-4-1.
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
Nassau Regional Emergency Medical Services. Advanced Life Support Pediatric Protocol Manual
 Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Chapter 10. Objectives. Objectives 01/09/2013. Airway Management, Artificial Ventilation, and Oxygenation
 Chapter 10 Airway Management, Artificial Ventilation, and Oxygenation Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
Chapter 10 Airway Management, Artificial Ventilation, and Oxygenation Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Pediatric Assessment Triangle
 Pediatric Assessment Triangle Katherine Remick, MD, FAAP Associate Medical Director Austin Travis County EMS Pediatric Emergency Medicine Dell Children s Medical Center Objectives 1. Discuss why the Pediatric
Pediatric Assessment Triangle Katherine Remick, MD, FAAP Associate Medical Director Austin Travis County EMS Pediatric Emergency Medicine Dell Children s Medical Center Objectives 1. Discuss why the Pediatric
Carole Wegner RN, MSN And Lori Leiser CRT
 Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
These signs should lead to the administration of high concentrations of
 Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
In-hospital Resuscitation
 In-hospital Resuscitation Introduction This new section in the guidelines describes the sequence of actions for starting in-hospital resuscitation. Hospital staff are often trained in basic life support
In-hospital Resuscitation Introduction This new section in the guidelines describes the sequence of actions for starting in-hospital resuscitation. Hospital staff are often trained in basic life support
Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study
 D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
Medical Emergency Management for the Dental Clinic
 Medical Emergency Management for the Dental Clinic Revised: Spring 2017 1 Medical Emergency Management Florida State College at Jacksonville Dental Clinic Topic Page Emergency Equipment and Supplies 3
Medical Emergency Management for the Dental Clinic Revised: Spring 2017 1 Medical Emergency Management Florida State College at Jacksonville Dental Clinic Topic Page Emergency Equipment and Supplies 3
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
table of contents pediatric treatment guidelines
 table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
The assessment helps decide if the patient is an emergency, priority or non-urgent case.
 Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
It is important to point out and frequently remind learners that they are expected to complete ALL aspects of a normal assessment.
 Background The purpose of this document is to provide guidelines for faculty on various aspects of patient simulators to be emphasized to learners during orientation. We recommend that every learner be
Background The purpose of this document is to provide guidelines for faculty on various aspects of patient simulators to be emphasized to learners during orientation. We recommend that every learner be
San Benito County EMS Agency Section 700: Patient Care Procedures
 Purpose: To outline the steps EMTs & paramedics will take to manage possible life threats in any child or adult patient they encounter. This policy is in effect for all treatment protocols & is to be referred
Purpose: To outline the steps EMTs & paramedics will take to manage possible life threats in any child or adult patient they encounter. This policy is in effect for all treatment protocols & is to be referred
2. General Cardiac Arrest Protocol Medical Newborn/Neonatal. Protocol 8-3 Resuscitation 4. Medical Supraventricular
 PEDIATRIC CARDIAC SECTION: Pediatric Cardiovascular Emergencies REVISED: 06/2017 Section 8 1. Cardiac Arrest Unknown Rhythm (i.e. Protocol 8-1 BLS) 2. General Cardiac Arrest Protocol 8-2 3. Medical Newborn/Neonatal
PEDIATRIC CARDIAC SECTION: Pediatric Cardiovascular Emergencies REVISED: 06/2017 Section 8 1. Cardiac Arrest Unknown Rhythm (i.e. Protocol 8-1 BLS) 2. General Cardiac Arrest Protocol 8-2 3. Medical Newborn/Neonatal
Neonataal Cardiac Compressions ad. Professor of Pediatrics
 State of the Art Science to Support Neonataal Cardiac Compressions ad Medications Myra H. Wyckoff, MD Professor of Pediatrics UT Southwestern Medical Center at Dallas You are on call at your delivery hospital.
State of the Art Science to Support Neonataal Cardiac Compressions ad Medications Myra H. Wyckoff, MD Professor of Pediatrics UT Southwestern Medical Center at Dallas You are on call at your delivery hospital.
MASTER SYLLABUS
 MASTER SYLLABUS 2018-2019 A. Academic Division: Health Science B. Discipline: Respiratory Care C. Course Number and Title: RESP 2490 Practicum IV D. Course Coordinator: Tricia Winters, BBA, RRT, RCP Assistant
MASTER SYLLABUS 2018-2019 A. Academic Division: Health Science B. Discipline: Respiratory Care C. Course Number and Title: RESP 2490 Practicum IV D. Course Coordinator: Tricia Winters, BBA, RRT, RCP Assistant
Airway Management Essentials Self-Study Guide
 Airway Management Essentials Self-Study Guide Fourth Quarter 2010 Self-Study Guide Learning Objectives Cognitive Domain 1. Describe the various conditions that cause concern during treatment in the field
Airway Management Essentials Self-Study Guide Fourth Quarter 2010 Self-Study Guide Learning Objectives Cognitive Domain 1. Describe the various conditions that cause concern during treatment in the field
AIRWAY MANAGEMENT AND VENTILATION
 AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube)
 This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
Jefferson Tower Task Trainer List
 Jefferson Tower Task Trainer List Table of Contents Blue Phantom Ultrasound Central Line Training Model 2 Blue Phantom Femoral Vascular Access Training Model 3 Blue Phantom Thoracentesis Ultrasound Training
Jefferson Tower Task Trainer List Table of Contents Blue Phantom Ultrasound Central Line Training Model 2 Blue Phantom Femoral Vascular Access Training Model 3 Blue Phantom Thoracentesis Ultrasound Training
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Neonatal Intensive Care Unit Skills Checklist
 _ XXX-XX- Print Name Last 4 of SS # Date Completed Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
_ XXX-XX- Print Name Last 4 of SS # Date Completed Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
Physiological normal values (Depends on age, strain, health status, type of anesthesia, etc.)
 UBC Animal Care Guidelines This SOP will be used for: Inhalational anesthesia SOP: ACC-01-2017 Rodent Anesthesia Injectable anesthesia Submitted by: Shelly McErlane both inhalational and injectable anesthesia
UBC Animal Care Guidelines This SOP will be used for: Inhalational anesthesia SOP: ACC-01-2017 Rodent Anesthesia Injectable anesthesia Submitted by: Shelly McErlane both inhalational and injectable anesthesia
Pedi-Cap CO 2 detector
 Pedi-Cap CO 2 detector Presentation redeveloped for this program by Rosemarie Boland from an original presentation by Johnston, Adams & Stewart, (2006) Background Clinical methods of endotracheal tube
Pedi-Cap CO 2 detector Presentation redeveloped for this program by Rosemarie Boland from an original presentation by Johnston, Adams & Stewart, (2006) Background Clinical methods of endotracheal tube
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
ACoRN Workbook 2012 Update
 ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
TTC Catalog - Respiratory Care (RES)
 2018-2019 TTC Catalog - Respiratory Care (RES) RES 110 - Cardiopulmonary Science I This course focuses on assessment, treatment evaluation of patients with cardiopulmonary disease. RES 121 Restrictions:
2018-2019 TTC Catalog - Respiratory Care (RES) RES 110 - Cardiopulmonary Science I This course focuses on assessment, treatment evaluation of patients with cardiopulmonary disease. RES 121 Restrictions:
Stabilization and Transportation guidelines for Neonates and infants with Heart disease:
 Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
FANNP 28TH NATIONAL NNP SYMPOSIUM: CLINICAL UPDATE AND REVIEW OCTOBER 17-21, 2017
 Pulse Oximetry in the Delivery Room: Principles and Practice GS2 3 Jonathan P. Mintzer, MD, FAAP Assistant Professor of Pediatrics Stony Brook Children s Hospital, Division of Neonatal-Perinatal Medicine,
Pulse Oximetry in the Delivery Room: Principles and Practice GS2 3 Jonathan P. Mintzer, MD, FAAP Assistant Professor of Pediatrics Stony Brook Children s Hospital, Division of Neonatal-Perinatal Medicine,
Resuscitation Checklist
 Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
#6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure
 #6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure Objectives: Observe slide of artery and vein cross-section Auscultate heart sounds using a stethoscope Measure
#6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure Objectives: Observe slide of artery and vein cross-section Auscultate heart sounds using a stethoscope Measure
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Simulation 08: Cyanotic Preterm Infant in Respiratory Distress
 Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Delivery Room Resuscitation of Newborns with Congenital Anomalies
 Delivery Room Resuscitation of Newborns with Congenital Anomalies Anne Ades, MD, MSEd Director of Neonatal Education The Children s Hospital of Philadelphia Associate Professor of Clinical Pediatrics Perelman
Delivery Room Resuscitation of Newborns with Congenital Anomalies Anne Ades, MD, MSEd Director of Neonatal Education The Children s Hospital of Philadelphia Associate Professor of Clinical Pediatrics Perelman
