Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia
|
|
|
- Octavia Chambers
- 5 years ago
- Views:
Transcription
1 Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia 1
2 Definition of hypothermia: Body temperature below 95 F / 35 C (ranges 34 36) Normal temperature is 98.6 F / 37 C Core temp 35 C to 37 C Peripheral tissue temp 31 C to 35 C Skin temp 28 C to 32 C Elderly normal is 0.5 C / 97.7 F or 36.5 C 2
3 Which statements are correct concerning perioperative hypothermia: Hypothermia develops with a characteristic pattern. Core temperature decreases o C during the first hour of surgery. The second phase of temperature loss is characterized by 2 or 3 h of a slower, linear, decrease in core temperature. The third phase of temperature loss is characterized by a rapid temperature decrease of 2-3 o C. 3
4 Which statements are correct regarding perioperative hypothermia: Hypothermia develops with a characteristic pattern. Core temperature decreases o C during the first hour of surgery. The second phase of temperature loss is characterized by 2 or 3 h of a slower, linear, decrease in core temperature. The third phase of temperature loss is characterized by a rapid temperature decrease of 2-3 o C. 4
5 How does perioperative hypothermia occur Develops with a characteristic pattern. Core temperature decreases o C during the first hour of surgery. Redistribution of blood from the core to the peripheral circulation contributes 81% to this initial decrease in temperature 5
6 The second phase of temperature loss is characterized by 2 or 3 h of a slower, linear, decrease in core temperature. Core temperature decreases an additional 0.4 o C/hr +/- 0.3 C, with redistribution contributing 43%. 6
7 Lastly, patient enters a plateau phase during which core temperature remains constant Redistribution contributes 65% to the entire heat loss during the first 3 h of anesthesia 7
8 8
9 Body heat content is not normally distributed evenly. Instead, tonic thermoregulatory vasoconstriction maintains a core-to-peripheral temperature gradient. Induction of general anesthesia inhibits vasoconstriction, allowing a core-toperipheral redistribution of body heat. 9
10 Induction of GA produces vasodilation GA reduces the vasoconstriction threshold temperature (core temperature that triggers a thermoregulatory response) to well below core temperature Inhibiting centrally mediated thermoregulatory constriction Anesthetics directly cause vasodilation 10
11 After one hour of anesthesia core temperature decreases ~ 1.6 o C During the subsequent 2 h core temperature decreases ~ 1.1 o C - 2 o C 11
12 12
13 Redistribution hypothermia in the obese patient: Is increased Is decreased Does not occur Is consistent with a very thin patients 13
14 Redistribution hypothermia in the obese patient: Is increased Is decreased Does not occur Is consistent with a very thin patients 14
15 Obese patients redistribute core temperature less than those of normal weight Normally have thermoregulatory problems dissipating metabolic heat due to excess adipose. Consequently, they spend much of their time in vasodilation. The result is that their peripheral tissue temperature is higher than normal, which reduces core-to-peripheral flow of heat after induction of anesthesia. 15
16 The Linear Phase of heat loss is defined as: The second portion of the hypothermia curve Results from heat loss exceeding metabolic heat production of approximately 0.5 o C/hr Heat loss mediated by radiation, conduction, convection and evaporation Heat loss from radiation contributes most to heat loss during this phase. 16
17 The Linear Phase of heat loss is defined as: The second portion of the hypothermia curve Results from heat loss exceeding metabolic heat production of approximately 0.5 o C/hr Heat loss mediated by radiation, conduction, convection and evaporation Heat loss from radiation contributes most to heat loss during this phase. 17
18 70% of the body s heat loss to the environment Occurs via infrared radiation Loss of body heat to cooler objects in the room No physical contact with objects required for radiant heat loss to occur Prevented by simple covering 18
19 Loss of heat to air currents flowing over the body Wind-chill effect Cool, drafty operating rooms (Laminar flow rooms) Second major source of heat loss during anesthesia and surgery Simple covering helps prevent convective loss 19
20 Loss of heat to cooler objects the body is touching, Accounts for 5% of heat loss in OR Operating tables Small losses unless patient is wet which can increase conduction loss 25-fold Mechanism by which cold IV fluids and blood products decrease body temperature 20
21 1L crystalloid infused at room temperature (20 C) causes patient to expend 17 kcal to warm the fluid to 37 C Approximately 25% of a patient s hourly caloric production which can t be increased in the anesthetized patient Body temperature will fall ~ 0.2 C/L of crystalloid infused at room temperature 21
22 Blood products Infusion of 2-4 units of cold blood can decrease core temp by almost 1 C 22
23 Loss from sweating, insensible fluid losses, airway humidification of dry gases, evaporation from large wound surfaces Normally, a small factor Respiratory evaporative losses are less than 10% Losses from extensive wounds can become significant 23
24 Core temperature that triggers a thermoregulatory response Response modified by Thermosensivity (gain) :proportional response Magnitude of change relative to goal temperature Maximal response Further change in core temp elicits no increase in response 24
25 No autonomic response within this range 0.2 o C range for normal adults Core temperatures beyond this range will elicit response Vasoconstriction / shivering for cold Vasodilation / sweating for heat 25
26 Cooling of core body temperature by IV fluids is the result of which type of heat: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 26
27 Cooling of core body temperature by IV fluids is the result of which type of heat: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 27
28 Loss of body temperature from the OR table reflection which type of heat loss: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 28
29 Loss of body temperature from the OR table is a result of which type of heat loss: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 29
30 Loss of body temperature from the surgical incision is a result of which type of heat loss: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 30
31 Loss of body temperature from the surgical incision is a result of which type of heat loss: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 31
32 The major cause of heat loss during anesthesia is via what mechanism: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 32
33 The major cause of heat loss during anesthesia is via what mechanism: 1. Conduction 2. Convection 3. Radiation 4. Evaporation 33
34 Perioperative heat loss that results from the application of skin prep solutions is an example of what type of heat transfer? 1. Conduction 2. Convection 3. Radiation 4. Evaporation 34
35 Perioperative heat loss that results the application of skin prep solutions is an example of what type of heat transfer? 1. Conduction 2. Convection 3. Radiation 4. Evaporation 35
36 Heat loss varies according to which skin preparation is used. Which skin preparation will cause the greatest heat loss? 1. Water 2. Chlorhexidine 3. Hibiclens 4. Alcohol 5. Betadine 36
37 Heat loss varies according to which skin preparation is used. Which skin preparation will cause the greatest heat loss? 1. Water 2. Chlorhexidine 3. Hibiclens 4. Alcohol 5. Betadine 37
38 The decrease in mean body temperature in a 70 kg patient ranges from to o C/m 2 The greater surface area covered the greater the heat loss. 38
39 The final phase of the hypothermia curve is characterized by which of the following: 1. Reversal of redistribution hyperthermia 2. Constant core temperature 3. Slowly decreasing core temperature C/h 4. Characterized by a passive or active plateau 39
40 The final phase of the hypothermia curve is characterized by which of the following: 1. Reversal of redistribution hyperthermia 2. Constant core temperature 3. Slowly decreasing core temperature C/h 4. Characterized by a passive or active plateau 40
41 Passive Plateau A passive plateau results when metabolic heat production equals heat loss, without activating thermoregulatory defenses. 41
42 Active Plateau Patients who become sufficiently hypothermic trigger thermoregulatory vasoconstriction and develop an actively maintained plateau. The difference between a passive plateau and active plateau is that an active plateau depends on thermoregulatory vasoconstriction to decrease heat loss and to alter distribution of heat within the body. In this regard, core temperature is maintained much as it is normally. A core temperature between 34 and 35 C is necessary to trigger thermoregulatory vasoconstriction during anesthesia 42
43 Steady State temperature regulation is interrupted during anesthesia 1. Anesthesia significantly decreases metabolic heat production. 2. Heat loss may be abnormally high because of: 2. Cool operating room environment 3. administration of cool intravenous and irrigating fluids 4. evaporative and radiative losses from within surgical incisions. 3. Behavioral compensations are not available to unconscious patients 4. Autonomic responses are impaired, at least until patients become quite hypothermic. 43
44 Neuraxial anesthesia inhibits thermoregulatory control by: 1. Blocking the PNS 2. Preventing Shivering 3. Acting on central mechanisms 4. Decreasing behavioral control 5. All the above 6. None of the above 44
45 Neuraxial anesthesia inhibits thermoregulatory control by: 1. Blocking the PNS 2. Preventing Shivering 3. Acting on central mechanisms 4. Decreasing behavioral control 5. All of the above 6. None of the above 45
46 Redistribution decreases core temperature about twice as much during regional as during general anesthesia. True or False 46
47 Redistribution decreases core temperature about twice as much during regional as during general anesthesia. True or False 47
48 Redistribution decreases core temperature about half as much during major conduction anesthesia as during general anesthesia. Patients don t feel cold and do not complain 48
49 Metabolic heat production remains near normal Start linear hypothermia phase at a higher temperature due to a decreased loss to redistribution in initial phase 49
50 During relatively short procedures, hypothermia is likely to be greater in patients administered general anesthesia. Patients administered regional anesthesia will generally start the linear hypothermia phase at a relatively high temperature because they initially lost less to redistribution. Furthermore, hypothermia may develop at a reduced rate during neuraxial anesthesia because metabolic heat production remains near normal. 50
51 After long and large operations, the opposite pattern is likely to prevail because in patients administered general anesthesia a core temperature plateau will develop, whereas those undergoing neuraxial anesthesia often continue to become hypothermic. Whether core hypothermia is worse with general or regional anesthesia is thus likely to depend largely on the duration and magnitude of surgery. 51
52 52
53 After neuraxial block, an initial core temperature drop is caused by vasodilation in the lower body and heat redistribution from the core to the periphery, similar to that observed during general anesthesia. Afterward, temperature continues to decrease linearly as a result of enhanced heat loss through vasodilated skin. Unlike during general anesthesia, core temperature might never reach a plateau phase during central neuraxial block and could continue to decrease unless active warming is started. This is because neuraxial block inhibits vasoconstriction and shivering in the lower part of the body. Lack of thermal sensation from the blocked areas overrides the hypothalamus, and therefore, the patient fails to feel cold and to report it to the anesthesiologist. When general and epidural anesthesia are combined, the decrease in vasoconstriction as a result of the latter does not allow a core temperature plateau to be reached and results in lower body temperatures than with general anesthesia alone. 53
54 During neuraxial anesthesia, body temperature is negatively correlated with block level and with patient s age. Elderly patients are at increased risk of developing hypothermia while undergoing regional anesthesia as a result of a decreased temperature threshold for shivering. Surprisingly, duration and magnitude of the surgery do not seem to predict the extent of hypothermia nor does room temperature. Identifying patients who are at risk for developing hypothermia during neuraxial block can be difficult, and anesthesiologists could fail to estimate its presence based only on clinical grounds. As a result of the potential for significant temperature loss, temperature should be monitored during most neuraxial anesthetics. However, most anesthesiologists do not measure this variable during regional anesthesia. In a recent survey, only 33% of the participating clinicians reported they monitored body temperature while conducting regional anesthesia. 54
55 Combined Neuraxial and General Anesthesia. The patients at greatest risk for inadvertent perioperative hypothermia are those in whom regional and general anesthesia are combined. The reason is that these patients will initially become rapidly hypothermic because of redistribution to all four extremities. During the linear phase, they will continue to cool, but at the relatively higher rate associated with general anesthesia. Three additional factors contribute to hypothermia during combined regional general anesthesia. 55
56 The first is that neuraxial anesthesia per se reduces the vasoconstriction threshold. General anesthesia does also, but the epidural effect is superimposed on the general anesthetic effect. As a result, vasoconstriction occurs later and at a lower core temperature in patients administered both epidural and general anesthesia. The second factor is that general anesthesia inhibits the shivering that might otherwise increase heat production during neuraxial anesthesia. The third and most important factor is that peripheral nerve block prevents vasoconstriction in the legs. As a result, vasoconstriction once initiated centrally is relatively ineffective, and core temperature continues to decrease. 56
57 The principle defenses against hypothermia include all the following except: 1. Skin vasomotor activity 2. Non-shivering thermogenesis 3. Shivering 4. Modulation of pre-optic area of the posterior hypothalamus 57
58 The principle defenses against hypothermia include all the following except: 1. Skin vasomotor activity 2. Non-shivering thermogenesis 3. Shivering 4. Modulation of pre-optic area of the posterior hypothalamus 58
59 Preoptic area anterior hypothalamic nuclei (POAHN) Receives input from afferent peripheral and central receptors (includes the hypothalamus itself) 10/21/
60 Anterior hypothalamus Promotes heat loss Vasodilation sweating Posterior hypothalamus Promotes heat conservation Decrease blood flow Piloerection Shivering Promotes heat production Increase secretion thyroid hormone Epinephrine and norepinephrine secretion increase the BMR 10/21/
61 Vigorous shivering increases metabolic heat production up to % above basal level
62 Vigorous shivering increases metabolic heat production up to % above basal level
63 Vigorous shivering increases Oxygen consumption up to % above basal level
64 Vigorous shivering increases Oxygen consumption up to % above basal level
65 May increase O2 requirments by % 65
66 Shivering is an involuntary, oscillatory muscular activity that augments metabolic heat production. Vigorous shivering increases metabolic heat production up to 600% above basal level. 66
67 Which statement about shivering is false: 1. Shivering is elicited when the preoptic region of the hypothalamus is cooled. 2. Shivering is uncomfortable and worsens post-op pain. 3. Shivering is associated with a marked decrease in catecholamine levels. 4. Shivering is rare in the elderly. 67
68 Which statement about shivering is false: 1. Shivering is elicited when the preoptic region of the hypothalamus is cooled. 2. Shivering is uncomfortable and worsens post-op pain. 3. Shivering is associated with a marked decrease in catecholamine levels. 4. Shivering is rare in the elderly. 68
69 Which are the most effective measure to decrease intraoperative hypothermia is: 1. Warming pre-operatively 2. Warming intra- operatively pre-induction 3. Warming intra- operatively post-induction 4. Warming postoperatively 69
70 Which are the most effective measure to decrease intraoperative hypothermia is: 1. Warming pre-operatively 2. Warming intra- operatively pre-induction 3. Warming intra- operatively post-induction 4. Warming postoperatively 70
71 Post induction warming -The overall heat loss during this relatively short time is relatively small, and therefore, warming the patient after induction does not control the initial temperature drop. On the contrary, warming started before induction limits the redistribution of heat by reducing the temperature gradient between the core and peripheral compartments. This strategy is simple and is probably worthwhile in the patients who are most likely to experience the complications of intraoperative hypothermia. 71
72 Pulmonary artery catheter, is considered a gold standard for core temperature measurement and is often used as a reference for other monitoring devices. 72
73 Esophageal temperature readings can artifactually decrease during thoracotomy and rapid infusion of cold fluids and can be effected by the temperature of the inspired gases. The optimal position for the thermistor is in the lower esophagus, approximately 45 cm from the nose and 12 to 16 cm distally to the point where heart and breath sounds are best heard. complications such as esophageal perforations and burns are possible 73
74 Nasopharyngeal temperature can be measured with an esophageal probe positioned above the palate and is reasonably close to brain and core temperature. Its use has been suggested during use of a laryngeal mask. Bladder urinary catheter probe Not effective measure during low UOP and lower abdominal surgeries Rectal temp Affected by stool and bacteria that produce heat Does not reflect acute changes in core temperature 74
75 Temperatures at different skin locations can differ considerably, and at least 4 distinct monitoring sites are necessary to obtain an estimate of the average skin temperature. Axillary temperature is thought to be relatively close to the core value and can probably be a reasonable choice if other core temperature measurements are impractical. Careful probe location is essential at this site, and even then, significant inaccuracy is still possible. 75
76 76
77 77
78 The hypothalamic set point temperature normally average about 98.6 F. All of the following factors can alter the set point except? 1. Skin temperature 2. Pyrogens 3. Antipyretics 4. Thyroxin 78
79 The hypothalamic set point temperature normally average about 98.6 F. All of the following factors can alter the set point except? 1. Skin temperature 2. Pyrogens 3. Antipyretics 4. Thyroxin 79
80 Pyrogens released from toxic bacteria or degenerating tissues of the body can increase the set-point temperature. Fever-reducing medication such as ASA, ibuprofen and tylenol are called antipyretics Thyroxine can increase metabolic rate and therefore increase the rate of heat production, but does not change the set-point temp of the hypothalamus. A decrease in skin temperature causes the setpoint temperature to increase, and the set-point temperature decreases when the skin is hot. 80
81 Most of the heat loss from an unclothed person at room temperature occurs by which of the following mechanisms? 1. Conduction to air 2. Conduction to objects 3. Convection 4. Evaporation 5. Radiation 81
82 Most of the heat loss from an unclothed person at room temperature occurs by which of the following mechanisms? 1. Conduction to air 2. Conduction to objects 3. Convection 4. Evaporation 5. Radiation 82
83 About 60% of the body heat is lost by radiation. Loss of heat by radiation means loss in the form of infrared heat waves, which is a type of electromagnetic wave. All objects radiate heat waves; thus, heat waves are radiated from the walls of rooms and other objects toward the body is greater than the temperature of surrounding objects, more heat radiates from the body than is radiated to the body 83
84 Which of the following mechanisms cause heat loss from a normal person when the environmental temperature is 106 F and the relative humidity is less than 10%. 1. Conduction 2. Convection 3. Evaporation 4. Radiation 84
85 Which of the following mechanisms cause heat loss from a normal person when the environmental temperature is 106 F and the relative humidity is less than 10%. 1. Conduction 2. Convection 3. Evaporation 4. Radiation 85
86 Evaporation is the only means of heat loss when the air temperature is greater than the body temperature Each gram of water that evaporates from the surface of the body causes 0.58 kilocalories of heat to be lost from the body Even when the body is not sweating, water evaporates insensiblhy from the skin and lungs at a rate of 450 to 600ml/day, which is about 12 to 16 kilocalories of heat loss per hour. 86
87 A scuba diver explores an underwater lava flow where temperature is 102 F. Which of the following profiles best describes the mechanisms of heat loss that are effective in this man? 1. Evaporation 2. Radiation 3. Convection 4. Conduction 5. None of the above 6. All of the above 87
88 A scuba diver explores an underwater lava flow where temperature is 102 F. Which of the following profiles best describes the mechanisms of heat loss that are effective in this man? 1. Evaporation 2. Radiation 3. Convection 4. Conduction 5. None of the above are correct 6. All of the above are correct 88
89 None of the mechanisms of heat loss are effective when a person is placed in water that has a temperature greater than body temperature. Instead, the body temperature becomes equal to the water temperature. 89
90 Which of the following sets of changes occurs at point W, compared with point V? 1. Shivering 2. Sweating 3. Vasoconstriction 4. Vasodilation 105F 103F W 101F Y 99F V 98F Hours Diagram shows the effect of changing the set-point of the hypothalamic temperature controller. The red line indicates the body temperature, and the blue line represents the hypothalamic set-point temperature. 90 X
91 Which of the following sets of changes occurs at point W, compared with point V? 1. Shivering 2. Sweating 3. Vasoconstriction 4. Vasodilation 105F 103F 101F 99F 98F V W X Y Hours 91
92 When the hypothalamic set-point temperature is greater than the body temperature, the person feels cold, and exhibits responses that lead to an elevation of body temperature. These responses include shivering and vasoconstriction as well as piloerection and epinephrine secretion. Shivering increases heat production. The increase in epinephrine secretion causes an immediate increase in the rate of cellular metabolism, which is an effect called chemical thermogenesis. Vasoconstriction of the skin blood vessels decreases heat loss through the skin. 92
93 Which of the following sets of changes occurs at point Y, compared with point V? 1. Shivering 2. Sweating 3. Vasoconstriction 4. Vasodilation Diagram shows the effect of changing the set-point of the hypothalamic temperature controller. The red line indicates the body temperature, and the blue line represents the hypothalamic set-point temperature. 105F 103F 101F 99F 98F V W X Y Hours 93
94 Which of the following sets of changes occurs at point Y, compared with point V? 1. Shivering 2. Sweating 3. Vasoconstriction 4. Vasodilation 105F 103F 101F 99F 98F V W X Y Hours 94
95 When the hypothalamic set point temperature is lower than the body temperature, the person feels hot, and exhibits responses that cause body temperature to decrease These responses include sweating and vasodilation Sweating increases heat loss from the body by evaporation Vasodialtion of skin blood vessels facilitates heat loss from the body by increasing the skin blood flow. 95
96 Which of the following sets of changes occurs at point X, compared with point Y? 1. Shivering 2. Sweating 3. Vasoconstriction 4. Vasodilation Diagram shows the effect of changing the set-point of the hypothalamic temperature controller. The red line indicates the body temperature, and the blue line represents the hypothalamic set-point temperature. 105F X 103F 101F 99F 98F V W Y Hours 96
97 Which of the following sets of changes occurs at point X, compared with point Y? 1. Shivering 2. Sweating 3. Vasoconstriction 4. Vasodilation 105F 103F 101F 99F 98F V W X Y Hours 97
98 When the hypothalamic set-point temperature is equal to the body temperature, the body exhibits neither heat loss nor heat conservation mechanisms, even when the body temperature is far above normal Therefore, the person does not feel not even when the body temperature does not feel hot even when body temperature is 104 F 98
99 A 54 year old man is admitted to the emergency department after being found lying in his yard near a running lawnmower on a hot summer day. His body temperature is 106 F, blood pressure is normal, and heart rate is 160 beats/min. Which of the following sets of changes is most likely to be present in this man? 1. Sweating 2. Hyperventilation 3. Vasodilation of skin 99
100 A 54 year old man is admitted to the emergency department after being found lying in his yard near a running lawnmower on a hot summer day. His body temperature is 106 F, blood pressure is normal, and heart rate is 160 beats/min. Which of the following sets of changes is most likely to be present in this man? 1. Sweating 2. Hyperventilation 3. Vasodilation of skin 100
101 This patient is suffering from heat stroke. Patients with heat stroke exhibit tachypnea and hyperventilation caused by direct CNS stimulation, acidosis, or hypoxia. The blood vessels in the skin are vasodilated, and the skin is warm. Sweating ceases in patients with true heatstroke, most likely because the high temperature itself causes damage to the anterior hypothalamic-preoptic area. The nerve impulses from this area are transmitted in the autonomic pathways to the spinal cord and then through sympathetic outflow to the skin to cause sweating. 101
102 What is the definition of kcal? 1. Amount of heat needed to raise the temperature of 1 kg of water by 1 o C 2. Amount of heat needed to raise the temperature of 10 kg of water by 1 o C 3. Amount of heat needed to raise the temperature of 1 kg of water by 10 o C 4. Amount of heat needed to raise the temperature of 10 kg of water by 100 o C 102
103 What is the definition of kcal? 1. Amount of heat needed to raise the temperature of 1 kg of water by 1 o C 2. Amount of heat needed to raise the temperature of 10 kg of water by 1 o C 3. Amount of heat needed to raise the temperature of 1 kg of water by 10 o C 4. Amount of heat needed to raise the temperature of 10 kg of water by 100 o C 103
104 The average 70kg adult produces 70kcal of heat/hr (average 1680 kcal/day) During anesthesia 70 kg adult produces 42kcal of heat/hr For every 58 kcal heat loss, there is a 1 o C decrease in body temperature Approximately q 2 hrs you will loose 1 o C 104
105 Which is not a complication of hypothermia? 1. Increased surgical blood loss 2. Decreased UOP 3. Shivering 4. Appearance of J wave at QRS-ST junction 5. PE 105
106 Which is not a complication of hypothermia? 1. Increased surgical blood loss 2. Decreased UOP 3. Shivering 4. Appearance of J wave at QRS-ST junction 5. PE 106
107 ANS Initial sympathetic stimulation and compensatory mechanisms < 32ºC to 33ºC (90-92) Compensatory mechanisms fail 22ºC to 24ºC (72 76) poikilothermic 107
108 Skin Peripheral vasoconstriction Piloerection Shivering 108
109 Metabolism s 6 to 8% for every 1º C in temperature Early Hyponatremia (cold diuresis) Hyperkalemia Hyperglycemia (inhibition of insulin release and block of its cellular uptake) Late Metabolic acidosis 109
110 CV system Initial stimulation HR, BP, CO, vasoconstriction (catecholamine release) Increase in circulating levels of norepinephrine of 100 to 700 % Leads to cardiac work load Temperature < 33º C (91.4) Depression of CV system, HR, BP, CO decrease < 31º C (88) Atrial and ventricular irritability < 30º C (86) Bradycardia and V-fib 19º C to 20º C (66 68F) Asystole 110
111 EKG changes 32C (90F) PR interval increases Broadening QRS complex Lengthening QT interval Appearance of J wave at QRS-ST junction Usually in lateral precordial leads 111
112 EKG of severely hypothermic patient--29ºc; asteriks show hump where QRS joins ST segment. This is J wave, also called Osborne wave. 112
113 Increased postoperative release of norepinephrine has been observed in patients who were hypothermic during surgery as compared with patients whose temperature was maintained at a normal value. This catecholamine release was associated with increased blood pressure and heart rate and with peripheral vasoconstriction. Although the observed hemodynamic changes were moderate, ischemia resulting from increased myocardial oxygen consumption is possible in high-risk patients. Besides, cold-induced catecholamine release could result in coronary constriction, offering an additional explanation to the observed incidence of myocardial ischemia. The available evidence suggests that avoidance of intraoperative hypothermia could be part of a strategy aimed at minimizing stress-related sympathetic activation with its cardiac complications. 113
114 Respiratory System Initial increase in respiratory effort Followed by respiratory depression with decreasing temperature Hypothermia-induced bronchodilation occurs, increasing anatomic and physiologic deadspace Diminished hypoxic pulmonary vasoconstriction and responsiveness to hypoxemia and hypercarbia < 30ºC (86F) bronchial secretions increase Pulmonary edema develops at 24ºC (76F) Increased O2 requirement with shivering of 400% to 700% 114
115 Left shift of oxyhemoglobin dissociation curve Reduced release of oxygen at a given po 2 O 2 consumption d 4% for each 0.5ºC drop in temperature Alkalosis Acidosis 115
116 Normal Hypothermia 116
117 CNS mentation, amnesia, obtundation, loss of pupillary and deep tendon reflexes, loss of brain activity CBF and CMRO 2 If shivering present CMRO 2 will >100% without in blood flow Peripheral nerve conduction slowed impairing nerve conduction Autonomic system depressed 117
118 Renal function Early: cold diuresis (diuresis continues due to impaired renal tubular sodium reabsorption) Late: oliguria and azotemia Muscles GI Shivering between 33ºC to 35ºC (34F 93F) Diminishes below 33ºC Stops below 30ºC Decreased gastric motility (full stomach) Decreased hepatic clearance 118
119 Coagulation disturbances Hemo-concentration Increased blood viscosity When energy is added to a liquid, the movement of the molecules increases. The increasing speed allows the molecules to slide past each other with greater ease. Week hydrogen bonds are formed between Hydrogen and Oxygen molecules in the blood which increase viscosity. Decreased O2 availability (left shift of oxyhemoglobin dissociation curve) Platelet dysfunction Platelet numbers remain normal Function impaired Reduced release of thromboxane A 2 Disruption of fibrinolytic system Clot formation impaired Disseminated intravascular coagulation 119
120 Other complications Decreased immune system response Increased infection Delayed healing / prolonged time until suture removal Delayed recovery from anesthesia Increased hospital stay cost up to $
121 Pharmacologic effects of drugs Decreased hepatic metabolism Prolonged drug metabolism probably contributes to delayed postanesthetic recovery of hypothermic patients. Decreased renal excretion Prolonged action Although few drugs have been investigated so far, it has been shown that low body temperature decreases the clearance of vecuronium, atracurium, and propofol. Inhalation agents MAC decreases 7% for each 1ºC decrease in body temperature 121
122 Normothermia Shorter hospital stay Hypothermia Decreased wound healing (vasocontriction, tissue hypoxia, inhibitory effect on immune system macrophage aggregation to site Only last a few hours, this is most critical for the establishment of bacterial growth Decreased time to suture removal Decreased collegen deposition and increased protein breakdown Decreased time of solid food ingestion 122
123 ADULT Exhibit 80% vasoconstriction response to hypothermia Exhibit 40% response to shivering ELDERLY Exhibit 55% vasoconstriction response to hypothermia Exhibit 10% response to shivering 123
124 Preoperative skin warming Adjusted ambient temperature in the OR Intraoperative temperature monitoring Heated and humidified anesthesia circuits Forced-air warming blankets Warmed intravenous fluids and blood products Postoperative mechanical ventilation Prevention and treatment of postoperative shivering Anticipation and treatment of rewarming vasodilation 124
125 All are appropriate management of perioperative hypothermia in a patient undergoing a AAA except? 1. Lower body bair hugger 2. Upper body bair hugger 3. Fluid warmer 4. Pre-operative α-2 agonist 125
126 All are appropriate management of perioperative hypothermia in a patient undergoing a AAA except? 1. Lower body Bair Hugger 2. Upper body Bair Hugger 3. Fluid warmer 4. Pre-operative α-2 agonist 126
127 Lower body bair hugger placed during cross clamping will exacerbate the tissue oxygen demand-supply imbalance Increased risk of thermal injury with warming blankets 127
128 Patient arrives to PACU with a temp 35 o C. The patient is tachypneic, hypertensive and shivering. Which of the following are appropriate treatments for this patient: 1. Forced air rewarming device cc LR fluid bolus 3. 4L Oxygen via OFM 4. Demerol 50 mg IV 5. 1,3,4 6. All of the above 128
129 Patient arrives to PACU with a temp 35 o C. The patient is tachypneic, hypertensive and shivering. Which of the following are appropriate treatments for this patient: 1. Forced air rewarming device cc LR fluid bolus 3. 4L Oxygen via OFM 4. Demerol 50 mg IV 5. 1,3,4 6. All of the above 129
130 Rewarming vasodilation Can produce acute hypotension, reflex tachycardia and myocardial ischemia Must vigorous fluid replacement essential to prevent this Vasodilator therapy as necessary 130
131 Intrathecal Fentanyl decreased shivering Bair Hugger decreased temperature during spinal anesthesia Lower vs upper vs both Use of ketamine to reduce shivering Kappa recepters 131
Energy Metabolism and Body Temperature
 Energy Metabolism and Body Temperature Hui-ping Wang( 王会平 ), PhD Dept. of Physiology, Zhejiang University School of Medicine wanghuiping@zju.edu.cn Part I Energy metabolism Definition The metabolic processes
Energy Metabolism and Body Temperature Hui-ping Wang( 王会平 ), PhD Dept. of Physiology, Zhejiang University School of Medicine wanghuiping@zju.edu.cn Part I Energy metabolism Definition The metabolic processes
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Chapter 12. Temperature Regulation
 Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Dr.A.VASUKINATHAN THERMOREGULATION AND ANAESTHESIA:
 Dr.A.VASUKINATHAN In homeothermic species a thermoregulatory system co-ordinates defenses against cold and heat to maintain internal body temperature within a narrow range, thus optimizing normal physiologic
Dr.A.VASUKINATHAN In homeothermic species a thermoregulatory system co-ordinates defenses against cold and heat to maintain internal body temperature within a narrow range, thus optimizing normal physiologic
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded)
 People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
03RC1- Greif. Temperature Monitoring. Robert Greif - 1 -
 03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
The cold never bother me anymore. R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit
 The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
Temperature Monitoring Locations: For TEMP 01, any temperature measurement coming from a physiologic monitor will suffice (peripheral or core).
 Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Thermal Injury. Thermal Injury Presentation CCFP (EM) Rounds. Topics Hypothermia. Resources Ch Tinitinelli
 Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Metabolism ANS 215 Physiology and Anatomy of Domesticated Animals
 Metabolism ANS 215 Physiology and Anatomy of Domesticated Animals I. Body Temperature A. Chemical reaction of the body and therefore body functions are affected by body temperature 1. Each species has
Metabolism ANS 215 Physiology and Anatomy of Domesticated Animals I. Body Temperature A. Chemical reaction of the body and therefore body functions are affected by body temperature 1. Each species has
Regulation of Body Temperature. Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY
 Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation
 Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
a central pulse located at the apex of the heart Apical pulse Apical-radial pulse a complete absence of respirations Apnea
 Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
THERMOREGULATION PHARMACOLOGY 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1
 THERMOREGULATION DIVISION OF PHYSIOLOGY DEPARTMENT OF ANATOMY, PHYSIOLOGY AND PHARMACOLOGY FACULTY OF VETERINARY MEDICINE IPB 2017 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1 Regulation
THERMOREGULATION DIVISION OF PHYSIOLOGY DEPARTMENT OF ANATOMY, PHYSIOLOGY AND PHARMACOLOGY FACULTY OF VETERINARY MEDICINE IPB 2017 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1 Regulation
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care
 Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
For more information about how to cite these materials visit
 Author(s): Louis D Alecy, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Louis D Alecy, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Thermoregulation 2015 WMA
 1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
Hypothermia Induction Methods
 Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
All Things Cold: Hypothermia, Altitude Illness and Frostbite. Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine
 All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
Bill Hall, MD Mesa County EMS System
 Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
Infusion of Warm Fluid During Abdominal Surgery Prevents Hypothermia and Postanaesthetic Shivering
 I.J. Engineering and Manufacturing 2011, 5, 26-30 Published Online October 2011 in MECS (http://www.mecs-press.net) DOI: 10.5815/ijem.2011.05.04 Available online at http://www.mecs-press.net/ijem Infusion
I.J. Engineering and Manufacturing 2011, 5, 26-30 Published Online October 2011 in MECS (http://www.mecs-press.net) DOI: 10.5815/ijem.2011.05.04 Available online at http://www.mecs-press.net/ijem Infusion
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
General anesthesia. No single drug capable of achieving these effects both safely and effectively.
 General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida
 Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
Introduction. Dr. Carmen E. Rexach Physiology Mt SAC Biology Department
 Introduction Dr. Carmen E. Rexach Physiology Mt SAC Biology Department What is physiology? Definition Study of body s vital functions Used to refer to healing Structure vs function Mechanists approach
Introduction Dr. Carmen E. Rexach Physiology Mt SAC Biology Department What is physiology? Definition Study of body s vital functions Used to refer to healing Structure vs function Mechanists approach
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest. Objectives: U.S. stats
 Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
HEAT STROKE. Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC
 HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
Lujain Hamdan. Ayman Musleh & Yahya Salem. Mohammed khatatbeh
 12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
Medical APMLE. Podiatry and Medical.
 Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
LESSON 2. Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE?
 LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
Homeostasis. Achievement Criteria. Excellence Criteria. Demonstrate understanding of how an animal maintains a stable internal environment 10/02/2016
 Homeostasis Demonstrate understanding of how an animal maintains a stable internal environment Biology 3.4 AS91604 Achievement Criteria Explain the purpose of the homeostatic mechanism Be able to explain
Homeostasis Demonstrate understanding of how an animal maintains a stable internal environment Biology 3.4 AS91604 Achievement Criteria Explain the purpose of the homeostatic mechanism Be able to explain
Chapter 24 Cholesterol, Energy Balance and Body Temperature. 10/28/13 MDufilho
 Chapter 24 Cholesterol, Energy Balance and Body Temperature 10/28/13 MDufilho 1 Metabolic Role of the Liver Hepatocytes ~500 metabolic functions Process nearly every class of nutrient Play major role in
Chapter 24 Cholesterol, Energy Balance and Body Temperature 10/28/13 MDufilho 1 Metabolic Role of the Liver Hepatocytes ~500 metabolic functions Process nearly every class of nutrient Play major role in
Homeostasis. - Homeostasis literally means same state and it refers to the process of keeping the internal body environment in a steady state.
 www.sureshkumarbio.wordpress.com Form 4 : Chapter 2 : Cell Structure and Cell Organisation Homeostasis - Homeostasis literally means same state and it refers to the process of keeping the internal body
www.sureshkumarbio.wordpress.com Form 4 : Chapter 2 : Cell Structure and Cell Organisation Homeostasis - Homeostasis literally means same state and it refers to the process of keeping the internal body
HOMEOSTASIS 37 C. ph of % blood sugar
 HOMEOSTASIS ph of 7.35 37 C 0.1% blood sugar Homeostasis an equilibrium (steady state) between an organism s various physiological functions, and between the organism and the environment. This is a balance
HOMEOSTASIS ph of 7.35 37 C 0.1% blood sugar Homeostasis an equilibrium (steady state) between an organism s various physiological functions, and between the organism and the environment. This is a balance
Therapeutic Hypothermia
 Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
Body Temperature Regulation and Fever
 C H A P T E R 7 4 Body Temperature Regulation and Fever NORMAL BODY TEMPERATURES Body Core Temperature and Skin Temperature. The temperature of the deep tissues of the body the core of the body usually
C H A P T E R 7 4 Body Temperature Regulation and Fever NORMAL BODY TEMPERATURES Body Core Temperature and Skin Temperature. The temperature of the deep tissues of the body the core of the body usually
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST
 THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
Induced Hypothermia for Cardiac Arrest. Heather Hand RN,CCRN,CNRN,ATCN,LNC
 Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Post-Cardiac Arrest Syndrome. MICU Lecture Series
 Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Postoperative hypothermia in geriatric patients undergoing arthroscopic shoulder surgery
 Anesth Pain Med 2019;14:112-116 https://doi.org/10.17085/apm.2019.14.1.112 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received May 18, 2018 Revised 1st, July 12, 2018 2nd, August 4, 2018 Accepted
Anesth Pain Med 2019;14:112-116 https://doi.org/10.17085/apm.2019.14.1.112 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received May 18, 2018 Revised 1st, July 12, 2018 2nd, August 4, 2018 Accepted
Introduction1. Introduction2. Introduction3. Thermoregulation2. Thermoregulation1
 Introduction1 Pharmacologic Options for Reducing the Shivering Response to Therapeutic Hypothermia Cerebral ischemia occurs when there is inadequate blood flow to the brain for more than 5 minutes. As
Introduction1 Pharmacologic Options for Reducing the Shivering Response to Therapeutic Hypothermia Cerebral ischemia occurs when there is inadequate blood flow to the brain for more than 5 minutes. As
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure.
 B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
Autonomic Nervous System
 Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Targeted Temperature Management: Normothermia for Neuroprotection
 Targeted Temperature Management: Normothermia for Neuroprotection I. Rationale Elevated body temperature is associated with increased cerebral metabolic rate and associated metabolic demand, which can
Targeted Temperature Management: Normothermia for Neuroprotection I. Rationale Elevated body temperature is associated with increased cerebral metabolic rate and associated metabolic demand, which can
Sleep and the Heart. Sleep Stages. Sleep and the Heart: non REM 8/31/2016
 Sleep and the Heart Overview of sleep Hypertension Arrhythmias Ischemic events CHF Pulmonary Hypertension Cardiac Meds and Sleep Sleep Stages Non-REM sleep(75-80%) Stage 1(5%) Stage 2(50%) Stage 3-4*(15-20%)
Sleep and the Heart Overview of sleep Hypertension Arrhythmias Ischemic events CHF Pulmonary Hypertension Cardiac Meds and Sleep Sleep Stages Non-REM sleep(75-80%) Stage 1(5%) Stage 2(50%) Stage 3-4*(15-20%)
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which research field below employs a variety of tools from other fields, including engineering,
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which research field below employs a variety of tools from other fields, including engineering,
The Surgical Patient. Objectives:
 The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
Basic Principles of Animal Form and Function Anatomy/Physiology Animal form and function are correlated at all levels of organization
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Basic Principles of Animal Form and Function Anatomy/Physiology Form and function are related Animal form and function are correlated at all levels of organization Evolution
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Basic Principles of Animal Form and Function Anatomy/Physiology Form and function are related Animal form and function are correlated at all levels of organization Evolution
Temp. regulation in homeotherms i.e. Birds & Mammals.
 Temp. regulation in homeotherms i.e. Birds & Mammals. Elephant 36oC, Man 37oc, Rat, Horse, Cow 38oC, Cat, Pigs, Dogs, Sheep 39oC Rabbit, Chicken 41oc, Sparrow 43oC In general Monotherms } } 30 36oC Marsupials
Temp. regulation in homeotherms i.e. Birds & Mammals. Elephant 36oC, Man 37oc, Rat, Horse, Cow 38oC, Cat, Pigs, Dogs, Sheep 39oC Rabbit, Chicken 41oc, Sparrow 43oC In general Monotherms } } 30 36oC Marsupials
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Cardiothoracic Fellow Expectations Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center
 The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Instituting preventive warming measures for patients who are normothermic. A variety of measures may be used, unless contraindicated.
 Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Langara College Spring archived
 COURSE DETAILS Department of Human Kinetics and Recreation Human Kinetics 1191 Anatomy & Physiology II Term: 2007-10 Sections: 001, 002, 003 Lecture/Seminar/Lab Hrs: 2: 0: 2 Credits: 3 Schedule: Section
COURSE DETAILS Department of Human Kinetics and Recreation Human Kinetics 1191 Anatomy & Physiology II Term: 2007-10 Sections: 001, 002, 003 Lecture/Seminar/Lab Hrs: 2: 0: 2 Credits: 3 Schedule: Section
PATIENT CARE MANUAL. Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation
 PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
Anesthesia Monitoring
 Anesthesia Monitoring Horatiu V. Vinerean, DVM, DACLAM Anesthesia Monitoring Anesthesia can be divided into four progressive phases. The signs relating to a certain phase are based upon the presence or
Anesthesia Monitoring Horatiu V. Vinerean, DVM, DACLAM Anesthesia Monitoring Anesthesia can be divided into four progressive phases. The signs relating to a certain phase are based upon the presence or
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
May 2013 Anesthetics SLOs Page 1 of 5
 May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
TEMPERATURE MANAGEMENT
 TEMPERATURE MANAGEMENT Unintentional Hypothermia and the Maintenance of Normothermia Ian Sampson, M.D. SURGICAL CARE IMPROVEMENT PROJECT Temperature Management SCIP INF 7: Colorectal surgery patients with
TEMPERATURE MANAGEMENT Unintentional Hypothermia and the Maintenance of Normothermia Ian Sampson, M.D. SURGICAL CARE IMPROVEMENT PROJECT Temperature Management SCIP INF 7: Colorectal surgery patients with
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Spinal anesthesia significantly impairs thermoregulation
 MISCELLANEOUS Effect of Preoperative Forced-Air Warming on Hypothermia in Elderly Patients Undergoing Transurethral Resection of the Prostate Youn Yi Jo, Young Jin Chang, Yong Beom Kim, Sehwan Lee, Hyun
MISCELLANEOUS Effect of Preoperative Forced-Air Warming on Hypothermia in Elderly Patients Undergoing Transurethral Resection of the Prostate Youn Yi Jo, Young Jin Chang, Yong Beom Kim, Sehwan Lee, Hyun
INDUCED HYPOTHERMIA A Hot Topic. R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences
 INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
Department of Anaesthesiology, Erasmus University Medical Center, Rotterdam, The Netherlands
 Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED
 ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
Sara Pitoni, Helen L. Sinclair and Peter J.D. Andrews. Presented by : R4 蔡為民 Supervised by : Dr. 楊煦星
 Sara Pitoni, Helen L. Sinclair and Peter J.D. Andrews Presented by : R4 蔡為民 Supervised by : Dr. 楊煦星 The incidence of out-of-hospital sudden cardiac arrest in industrial countries is reported to be between
Sara Pitoni, Helen L. Sinclair and Peter J.D. Andrews Presented by : R4 蔡為民 Supervised by : Dr. 楊煦星 The incidence of out-of-hospital sudden cardiac arrest in industrial countries is reported to be between
Homeostasis. homeo: same/steady stasis: state
 Homeostasis Homeostasis homeo: same/steady stasis: state Homeostasis Homeostasis is about staying the same THE MAINTENANCE OF STATIC OR CONSTANT CONDITIONS IN THE INTERNAL ENVIRONMENT Conditions at external
Homeostasis Homeostasis homeo: same/steady stasis: state Homeostasis Homeostasis is about staying the same THE MAINTENANCE OF STATIC OR CONSTANT CONDITIONS IN THE INTERNAL ENVIRONMENT Conditions at external
THERMOREGULATION 05 JUNE 2013
 THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
HYPOTHERMIA IN TRAUMA. Kevin Palmer EMT-P, DiMM
 HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
THERMOREGULATION AND SET POINT. BPK 422: Physiological Basis of Temperature Regulation By: Edwin Leung () & Lily Gan () Fall 2015 December 2, 2015
 THERMOREGULATION AND SET POINT BPK 422: Physiological Basis of Temperature Regulation By: Edwin Leung () & Lily Gan () Fall 2015 December 2, 2015 SUPPORTING POINT HYPOTHESIS Core temperatures are defended
THERMOREGULATION AND SET POINT BPK 422: Physiological Basis of Temperature Regulation By: Edwin Leung () & Lily Gan () Fall 2015 December 2, 2015 SUPPORTING POINT HYPOTHESIS Core temperatures are defended
General Anesthesia. Mohamed A. Yaseen
 General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
Homeostasis 1 of 26 Boardworks Ltd 2011
 Homeostasis 1 of 26 Boardworks Ltd 2011 2 of 26 Boardworks Ltd 2011 A day at the sauna 3 of 26 Boardworks Ltd 2011 How does the body react to change? Saving energy? 4 of 26 Boardworks Ltd 2011 Sayid has
Homeostasis 1 of 26 Boardworks Ltd 2011 2 of 26 Boardworks Ltd 2011 A day at the sauna 3 of 26 Boardworks Ltd 2011 How does the body react to change? Saving energy? 4 of 26 Boardworks Ltd 2011 Sayid has
A day at the sauna. Boardworks Ltd How does the body react to change?
 1 of 40 2 of 40 A day at the sauna 3 of 40 How does the body react to change? Saving energy? 4 of 40 Sayid has decided to save energy by staying in bed all day. How much of his energy do you think this
1 of 40 2 of 40 A day at the sauna 3 of 40 How does the body react to change? Saving energy? 4 of 40 Sayid has decided to save energy by staying in bed all day. How much of his energy do you think this
Chapter 29. Vital Signs
 Chapter 29 Vital Signs Vital Signs Temperature, pulse, respiratory rate, blood pressure Pain Oxygen saturation also frequently measured Vital signs are used to: Monitor patient s condition Identify problems
Chapter 29 Vital Signs Vital Signs Temperature, pulse, respiratory rate, blood pressure Pain Oxygen saturation also frequently measured Vital signs are used to: Monitor patient s condition Identify problems
Anesthesia Monitoring. D. J. McMahon rev cewood
 Anesthesia Monitoring D. J. McMahon 150114 rev cewood 2018-01-19 Key Points Anesthesia Monitoring: - Understand the difference between guidelines & standards - ASA monitoring Standard I states that an
Anesthesia Monitoring D. J. McMahon 150114 rev cewood 2018-01-19 Key Points Anesthesia Monitoring: - Understand the difference between guidelines & standards - ASA monitoring Standard I states that an
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
MEASURING AND RECORDING PATIENT VITAL SIGNS
 MEASURING AND RECORDING PATIENT VITAL SIGNS ABSTRACT: Vital sign measurements are effective tools to assess if a patient is ill. They are quick, simple measurements and reliable indicators of a person
MEASURING AND RECORDING PATIENT VITAL SIGNS ABSTRACT: Vital sign measurements are effective tools to assess if a patient is ill. They are quick, simple measurements and reliable indicators of a person
Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy
 Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy Ryohei Miyazaki 1, Kengo Hayamizu 1 and Sumio Hoka 2** Abstract Background:
Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy Ryohei Miyazaki 1, Kengo Hayamizu 1 and Sumio Hoka 2** Abstract Background:
Chapter V. Evaluation of the Effects of d-fenfluramine on the Cutaneous Vasculature and Total Metabolic Heat Production
 Chapter V. Evaluation of the Effects of d-fenfluramine on the Cutaneous Vasculature and Total Metabolic Heat Production Experiments presented in this chapter were designed to investigate the possible mechanisms
Chapter V. Evaluation of the Effects of d-fenfluramine on the Cutaneous Vasculature and Total Metabolic Heat Production Experiments presented in this chapter were designed to investigate the possible mechanisms
NOTES: CH 40 Introduction to Human Anatomy & Physiology
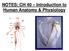 NOTES: CH 40 Introduction to Human Anatomy & Physiology THE HUMAN BODY Anatomy Physiology (= structures) (= functions or processes) Characteristics of LIFE: 1) Made up of 1 or more CELLS. 2) Obtain and
NOTES: CH 40 Introduction to Human Anatomy & Physiology THE HUMAN BODY Anatomy Physiology (= structures) (= functions or processes) Characteristics of LIFE: 1) Made up of 1 or more CELLS. 2) Obtain and
Feline Anesthesia Fluid Therapy Treatment of Anesthetic Complications
 Feline Anesthesia Fluid Therapy Treatment of Anesthetic Complications Rebecca A. Krimins, DVM, MS April 29, 2018 DCVR Annual Spring Symposium Email: drkrimins@gmail.com Cat Anesthesia There is no single
Feline Anesthesia Fluid Therapy Treatment of Anesthetic Complications Rebecca A. Krimins, DVM, MS April 29, 2018 DCVR Annual Spring Symposium Email: drkrimins@gmail.com Cat Anesthesia There is no single
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Therapeutic Hypothermia and Pharmacologic Considerations. Genelle Butz, PharmD Director of Pharmacy CarolinaEast Medical Center August 6, 2013
 Therapeutic Hypothermia and Pharmacologic Considerations Genelle Butz, PharmD Director of Pharmacy CarolinaEast Medical Center August 6, 2013 Disclosures Disclosure tatement: I have no financial or personal
Therapeutic Hypothermia and Pharmacologic Considerations Genelle Butz, PharmD Director of Pharmacy CarolinaEast Medical Center August 6, 2013 Disclosures Disclosure tatement: I have no financial or personal
Perioperative Heat Balance Daniel 1. Sessler, M. D. *
 578 REVIEW ARTICLE Michael M. Todd, M.D., Editor Anesthesiology 2000, 92:578-96 0 2000 American Society of Anesthesiologists, Inc. Lippincott Williams Sr Wilkins, Inc. Perioperative Heat Balance Daniel
578 REVIEW ARTICLE Michael M. Todd, M.D., Editor Anesthesiology 2000, 92:578-96 0 2000 American Society of Anesthesiologists, Inc. Lippincott Williams Sr Wilkins, Inc. Perioperative Heat Balance Daniel
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
