NEURO - Unit 2. The Patient with Neurological Trauma
|
|
|
- Muriel Wiggins
- 5 years ago
- Views:
Transcription
1 NEURO - Unit 2 The Patient with Neurological Trauma
2 Student Learning Goals Differentiate among common head traumas and explain: concussion, contusion, epidural hematoma, subdural hematoma, intracerebral hemorrhage and penetrating injuries. Describe nursing care for the patient with a head injury. Discuss brain tumors, symptoms and treatment. Explain the physical effects of spinal cord injuries. Identify one result of injury to each division of the spine. Describe the medical and surgical treatment during the acute phase of spinal cord injury. List the data to be included in the nursing assessment of the patient with a spinal cord injury. Describe spinal shock. Discuss the symptoms, cause and nursing care for the patient experiencing autonomic dysreflexia. Describe nursing care for the patient with spinal cord injury.
3 Head Injury: Types Scalp injuries Concussion Contusion Hematoma Intracerebral hemorrhage Penetrating injuries
4 May see: Lacerations of scalp Contusions of scalp Abrasions of scalp Hematomas of scalp May bleed profusely Scalp Injuries May or may not be associated with skull or brain injuries
5 CONCUSSION Trauma with no visible injury to the skull or brain Brief loss of consciousness (< 5 min.) May have Headache Amnesia about event N & V No permanent damage Recurrent injury can be a problem
6 CONTUSION Bruising and bleeding in the brain tissue More serious than concussion Risk with contusion is Edema & increased bleeding Why is this a problem?
7 A collection of blood 2 classifications: Subdural HEMATOMA Usually venous bleeding and slow forming Blood collects below the dura Epidural Usually arterial bleeding and rapid forming Blood collects above the dura
8
9 Subdural Hematoma 3 types Acute Within 24 hours Subacute More than 24 hours, less than one week Chronic Weeks to months
10 Epidural Hematoma Generally bleeding due to tear in middle meningeal artery Initially unconscious, then lucid briefly, then unconscious as pressure increases May see rapid increase in ICP Why?
11 Intracerebral Hemorrhage From lesions within the tissue of the brain itself What else do we call this? Can result from head trauma as well Penetrating Injuries Sharp objects penetrate the skull and brain tissue See: Brain Injury Wound contamination
12 Head Injury Surgical treatment Directed at evacuating hematomas and débriding damaged tissue
13 Head Injury: Nursing Care Nursing Diagnosis & Interventions Ineffective Tissue Perfusion - Cerebral Ineffective Breathing Pattern Risk for Injury Risk for Infection Impaired Physical Mobility Disturbed Body Image and Ineffective Role Performance
14 NURSING CARE Neuro checks Note sx. of ICP Fluid management Bedrest Quiet environment HOB Low - mid fowlers Nursing care that decreases ICP Avoid neck/hip flexion Limit suctioning Spacing of nursing care
15 ?Critical Thinking Questions? How does increased ICP affect respirations? Why would the patient lose consciousness when the ICP goes up?
16 Critical Thinking Question An 18-year-old man was admitted to the emergency department as a result of a motor vehicle accident. He appeared alert and was talking clearly to his parents in between x-ray examinations and laboratory tests. He had a moderate laceration on his forehead, which was sutured. As the nurse was applying a dressing, she noticed that his pupils were unequal. What should the nurse do next? What diagnosis may be likely?
17 General info Brain Tumors Some are primary tumors Some are metastatic Not all malignant Benign tumors can be a problem Why? Cause and risk factors Causes generally unknown Some congenital; others may be related to heredity Drug/environmental factors may play a role in development
18 Brain Tumors Signs and symptoms Directly related to area of brain invaded by the tumor Visual disturbances and headache New-onset seizure activity Difficulties with balance and coordination Medical treatment Surgery often followed by radiation with or without chemotherapy
19 Brain Tumors: Nursing Care Nursing Diagnosis/Nursing Interventions Acute Pain Disturbed Thought Processes Disturbed Sensory Perception Impaired Physical Mobility and Self-Care Deficit Ineffective Coping
20 Chapter 29 Spinal Cord Injury
21
22 BACKGROUND ASSESSMENT How is a diagnosis of incomplete spinal cord injury determined? What are possible psychosocial effects of a complete spinal cord injury?
23 Diagnostic Tests and Procedures Neurologic examination Initial evaluation provides the nurse with a baseline assessment of function and problems Ongoing assessment: To monitor the effects of neurologic injury To detect related complications To determine patient s need for assistance in activities of daily living Focuses on the motor and sensory systems Movement, muscle strength, reflex activiry
24 Diagnostic Tests and Procedures Imaging studies Radiography Detects vertebral compression, fractures, or problems with alignment Computed tomography (CT) Noninvasive examination of the specific levels of the spinal cord to be visualized, bony vertebrae, and the spinal nerves Magnetic resonance imaging (MRI) Produces precise, clear images of internal structures Myelogram Visualizes the spinal cord and vertebrae
25 Spinal Cord Injury (SCI) Head and neck permit movement in various directions Because the thoracic vertebrae is not flexible, the neck and cervical spine are vulnerable to injury
26 Spinal Cord Injuries may be classified: By Location/Level of Cord affected Cervical Thoracic Lumbar As Open or Closed By extent of damage to the cord Complete transection Incomplete transection
27 Effects of Spinal Cord Injury (SCI) Factors include extent of cut and level of injury Sometimes cannot be fully determined initially symptoms of spinal cord edema may mimic partial or complete transection With incomplete spinal cord injuries some function remains below the level of the injury Specific tracts may be involved, causing particular patterns of neurologic dysfunction
28 Patterns of Injury and Neurological Dysfunction
29 Effects of Spinal Cord Injury The higher the level of injury, the more encompassing the neurologic dysfunction Quadriplegia High cervical spine injuries; loss of motor and sensory function in all four extremities Paraplegia Injuries at or below T2 may cause paralysis of the lower part of the body
30 Respiratory Impairment Injuries at or above the level of C5 Called High Cervical May result in instant death Often die before reach hospital Ventilator dependent Cervical injuries below the level of C4 spare the diaphragm can involve impairment of intercostal and abdominal muscles
31 Degree of Functional Loss with Level of SCI See Table 29-3 Key is Respiratory Muscles involvement? Diaphragm vs. intercostals affected Where does full use of arms begin? What about lower extremities?
32
33
34
35
36 Spinal Shock An immediate, transient response to injury May appear as early as minutes May persist days, weeks, months Reflex activity below the level of the injury temporarily ceases
37 Symptoms Spinal Shock Below level of injury Immediate flaccid paralysis Loss of all sensation Loss of reflex activity Loss of autonomic function As it resolves see spastic involuntary movements Tx: General support of body systems
38 Autonomic Dysreflexia One of most serious and potentially dangerous complications of SCI Exaggerated response of autonomic nervous system to noxious (painful) stimuli Occurs with injury at or above the level of T6 As Spinal Shock resolves Risk for Autonomic Dysreflexia increases
39 Autonomic Dysreflexia What happens? Excessive stimulation of sensory receptors below the level of the injury precipitates autonomic dysreflexia. The sympathetic nervous system is stimulated, but an appropriate parasympathetic modulation response cannot be elicited because of the spinal cord injury that separates the two divisions of the autonomic nervous system
40 Autonomic Dysreflexia Sympathetic stim > Arterioles constrict: Leads to severe hypertension Can lead to seizure or stroke Regulatory vasodilation Only takes place above level of injury Sweating, flushing, nasal congestion, pounding headache Hypertension > vagal stim Bradycardia Vagal stim would dilate but cannot below level of SCI
41 Autonomic Dysreflexia Triggers Triggered by various stimuli distended bladder Constipation/fecal impaction renal calculi ejaculation uterine contractions may be caused by pressure sores, skin rash, enemas, or even sudden position changes
42 Autonomic Dysreflexia Nursing Care: Prevention: Avoid bladder distention How? Avoid bowel distention How? Topical Anesthetic agents for pressure sores Emergent Situation Raise HOB; sit patient up > lowers BP Relief of cause
43 Spasticity Most SCI pts. experience this Muscle spasms may be incapacitating can hamper efforts at rehabilitation Hyperactive reflexes accompany Generally see gradual reduction in 1 2 years Meds can help what type?
44 Impaired Sensory and Motor Function Impaired motor function can affect: mobility self-care And increases risk for complications r/t immobility Loss of sensation puts patient at risk for skin breakdown other injuries because pressure and pain are not perceived
45 Impaired Bladder Function During spinal shock all bladder and bowel function ceases Indwelling cath > intermittent cath Once spinal shock resolves, reflex activity returns May see spastic bladder Bladder retraining individualized
46 Impaired Bowel Function Initially may need gastric decompression Usually peristalsis returns w/i 3 days Most SCI pts can maintain bowel function the large bowel musculature has its own neural center that responds to distention by the fecal mass Bowel retraining programs For regular evacuation
47 Impaired Temperature Regulations May lose these regulatory mechanisms What regulatory mechanisms? May be unable to adapt to temperature extremes Especially tetraplegics Why?
48 Impaired Sexual Function Spinal levels S2, S3, and S4 control sexual function Injury at or above these levels results in sexual dysfunction Ability to achieve erection and ejaculation is variable Women resumes normal menses
49 Impaired Skin Integrity Pressure ulcers common r/t Immobility Loss of Sensation Locations most vulnerable??? Portals for infection Interrupt rehab efforts and wheelchair training Complete SCI interrupts vasomotor tone of the vascular system results in vasodilation and pooling of blood in the periphery; impedes perfusion of the skin; and encourages the development of pressure sores
50 Altered Self-Concept and Body Image SCI has tremendous impact Every aspect of life can be affected Timing of information impt. Prevent from overwhelming Often met with shock, disbelief and denial Take suicidal threats seriously Facilitate independence and control
51 OH NO!! Mr Studinski, 20 YO, was canoeing with several friends when they Came across a rope swing along the river. Mr Studinski failed To check the depth of the water before swinging himself high Over the river bed and diving into the water. The water level was 6. The pt comes to us with a c6 spinal cord injury and an epidural Hematoma. He is unconscious at this time. Dr. Spinalson is the md. Vitals: 142/75, 98, 98.5, 20. No home meds. Lab work: HGB 12.4, BUN 16, HCT 1.0, PT 12.4, NA 128, K 3.8. Currently in room With distraught family. MD waiting on CT results and will devise Course of treatment. NS running at 50ml/hr. No other meds ordered At this time. Diet NPO. Activity Bedrest. NKA.
52 Medical Treatment in the Acute Phase
53 Goals in Acute Phase Save patient s life Prevent further injury Preserve function
54 Saving the Patient s Life Establish Airway Use Jaw-thrust method of opening the airway Conventional head-tilt chin-lift: inappropriate with spinal injury; increases risk of cord damage Neck flexion avoided even that caused by a pillow or other support, must be avoided
55 Saving the Patient s Life Once airway is open administer 100% oxygen by mask and manual resuscitator Placement of endotracheal or tracheostomy tube allows direct access to the airway and facilitates optimal oxygenation Any injury that compromises ventilation must be treated immediately
56 Preventing Further Cord Injury Traction Immobilization with skeletal traction Gardner-Wells tongs Secured just above the ears; doesn t actually penetrate skull Crutchfield tongs Halo vest Applied directly to the skull just behind the hairline immobilizes and aligns cervical vertebrae usually placed during surgery that is done to internally stabilize fractures and relieve the compression of nerve roots Allows mobility OOB or Ambulatory
57
58
59 Preventing Further Cord Injury Special beds and cushions Kinetic bed, such as the Roto Rest bed, continually rotates the patient from side to side Overlay air mattresses: flotation devices placed on standard hospital beds Air-fluidized and flotation beds may be used after the spine has been stabilized Stryker wedge frame: canvas and metal frame bed that may be used to help turn the patient Types of cushions include those inflated with air, flotation devices, and gel pads
60
61 Preventing Further Cord Injury Drug therapy Methylprednisolone Reduces the damage to the cellular membrane Administered within the first 8 hours of injury Completely paralyzed patients often regain about 20% of function Partially paralyzed have regained up to 75% of function
62 Preserving Cord Function Early surgical intervention to repair cord damage Cord compression by bony fragments, compound vertebral fractures, and gunshot and stab wounds Surgery within the first 24 hours is most desirable Laminectomy Involves removing all or part of the posterior arch of the vertebra Alleviates cord compression/nerve root compression Spinal fusion If multiple vertebrae are involved Placing a piece of donor bone into area between the involved vertebrae
63 Nursing Care in Acute Phase Monitor respiratory status level of consciousness pupils motor and sensory function vital signs intake and output
64 Nursing Care in Acute Phase Obtain Health History Present Illness Past Medical Hx. Review of Systems S&S related to neuro dysfunction Functional Assessment Physical Exam
65 Functional Assessment Patient s self-care abilities Patient s roles and responsibilities as a family member Occupation, hobbies, usual activity pattern, habits, and diet Emotional response to the spinal injury Usual coping strategies Spiritual beliefs; other sources of support
66 Physical Examination Record the patient s reported height and weight Take vital signs Be alert for Spinal Shock Level of responsiveness, posture, and spontaneous movements Examine pupils for size, equality, reaction to light Respiratory effort and breath sounds
67 Physical Examination Inspect the skin for lacerations, bruises, pressure ulcers Inspect abdomen; auscultate for bowel sounds Inspect extremities for open fractures or abnormal positions Range of motion Ability to perceive sharp and dull sensation use a dermatome chart
68
69 Nursing Diagnosis/Interventions Ineffective Breathing Pattern Risk for Injury and Disturbed Sensory Perception Risk for Autonomic Dysreflexia Risk for Disuse Syndrome Bowel Incontinence Impaired Urinary Elimination
70 Nursing Diagnosis/Interventions Risk for Infection Ineffective Thermoregulation Feeding/Dressing/Grooming Self-Care Deficit Sexual Dysfunction Ineffective Coping Ineffective Therapeutic Regimen Management
71 Rehabilitation Activities that assist individual to achieve highest possible level of self-care and independence Begins on admission During Acute Phase Focus on preventing further disability and avoiding complications The interdisciplinary team addresses all aspects of function Physician, nurse, physical therapist, occupational therapist, speech therapist, dietitian, social worker, psychologist, and counselor Patient and family must be emotionally and physically prepared to make adjustments
72 CRITICAL THINKING QUESTION A nurse working the night shift on a medical-surgical unit looks up from the nurses station to see a patient walking toward the elevator. Evidently, the patient removed the traction device being used to treat his high cervical (C2, C3) fractures sustained in a fall off a porch. The Gardner-Wells tongs are still attached to his skull. He insists he is leaving to go get a drink. What should the nurse do?
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc. Copyright 2014, 2011, 2006 by Saunders, an imprint of Elsevier, Inc.
 Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Injuries to the head and spine
 Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
Autonomic Dysreflexia
 Autonomic Dysreflexia A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review date October 2016 This document has been developed to provide health service providers
Autonomic Dysreflexia A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review date October 2016 This document has been developed to provide health service providers
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition
 Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
TBI are twice as common in males High potential for poor outcome Deaths occur at three points in time after injury
 Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 EPC Ch 24 Quiz w-key Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following best explains the presentation and prognosis of
EPC Ch 24 Quiz w-key Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following best explains the presentation and prognosis of
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
1. Spinal cord injury mild flexion-extension whiplash ~ complete transection with permanent quadriplegia
 Wk 5. Management of Clients with Neurologic Trauma 1. Spinal cord injury mild flexion-extension whiplash ~ complete transection with permanent quadriplegia most common in cervical, lower thoracic-upper
Wk 5. Management of Clients with Neurologic Trauma 1. Spinal cord injury mild flexion-extension whiplash ~ complete transection with permanent quadriplegia most common in cervical, lower thoracic-upper
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
Shepherd Center: A Catastrophic Care Hospital. The Jane Woodruff Pavilion
 Shepherd Center: A Catastrophic Care Hospital The Jane Woodruff Pavilion Acute Management of SCI & Prevention of Secondary Complications Joycelyn Craig, BSN, RN, CRRN SCI Nurse Education Manager FACTS
Shepherd Center: A Catastrophic Care Hospital The Jane Woodruff Pavilion Acute Management of SCI & Prevention of Secondary Complications Joycelyn Craig, BSN, RN, CRRN SCI Nurse Education Manager FACTS
What is a spinal cord injury?
 Spinal Cord Injury What is a spinal cord injury? A spinal cord injury (SCI) is when the spinal cord is damaged Such damage causes 2 things: - loss or change of movement (paralysis) - loss or change of
Spinal Cord Injury What is a spinal cord injury? A spinal cord injury (SCI) is when the spinal cord is damaged Such damage causes 2 things: - loss or change of movement (paralysis) - loss or change of
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
10/6/2017. Notice. Traumatic Brain Injury & Head Trauma
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Injuries to the Head and Spine
 Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Most hypertensive: headache, vomiting, seizures, changes in mental status, fever, changes EKG
 Wk 2. Management of Clients with Stroke 1. Stroke neurologic changes by interruption in blood supply to brain 1) Etiology Ischemia: thrombosis or embolism thrombotic strokes > embolic strokes (1) Thrombosis
Wk 2. Management of Clients with Stroke 1. Stroke neurologic changes by interruption in blood supply to brain 1) Etiology Ischemia: thrombosis or embolism thrombotic strokes > embolic strokes (1) Thrombosis
8th Annual NKY TBI Conference 3/28/2014
 Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Acute spinal cord injury
 Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Slide 1. Slide 2. Slide 3. Introduction CHAPTER 10:CLIENTS WITH SPINAL CORD INJURY PART I. Introduction - page 252(pathophysiology)
 Slide 1 CHAPTER 10:CLIENTS WITH SPINAL CORD INJURY PART I PT 151 Slide 2 Introduction - page 252(pathophysiology) Traumatic SCI occurs when an external force, such as fracture of the vertebrae or penetration
Slide 1 CHAPTER 10:CLIENTS WITH SPINAL CORD INJURY PART I PT 151 Slide 2 Introduction - page 252(pathophysiology) Traumatic SCI occurs when an external force, such as fracture of the vertebrae or penetration
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men years old
 1 2 3 4 5 6 7 Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men 16-30 years old Mechanism of Injury: Vehicle crashes: 48% : 21%
1 2 3 4 5 6 7 Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men 16-30 years old Mechanism of Injury: Vehicle crashes: 48% : 21%
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Activity Three: Where s the Bleeding?
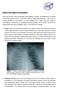 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Sir William Asher ANATOMY
 SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injury. North American Spine Society Public Education Series
 Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Spinal Trauma. General Rehabilitation of Patient with Spinal Trauma. Common Spinal Injuries. Important Anatomical Structures at each Vertebral Level
 Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Paraplegia: Exercise and Health Considerations. By: Juli and Trina
 Paraplegia: Exercise and Health Considerations By: Juli and Trina What is paraplegia? Paraplegia is impairment of motor and/or sensory function to the lower extremities, and sometimes the lower trunk Complete
Paraplegia: Exercise and Health Considerations By: Juli and Trina What is paraplegia? Paraplegia is impairment of motor and/or sensory function to the lower extremities, and sometimes the lower trunk Complete
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Neurosurgery (Orthopaedic PGY-1) Goals. Objectives
 Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Spinal Cord Injury. The nerves that go from the spinal cord to the arms, legs, chest, and abdomen are called peripheral nerves.
 Spinal Cord Injury Introduction Spinal cord injuries can be very devastating. More than 10,000 Americans experience spinal cord injuries each year, mainly due to auto or falling accidents. More than 200,000
Spinal Cord Injury Introduction Spinal cord injuries can be very devastating. More than 10,000 Americans experience spinal cord injuries each year, mainly due to auto or falling accidents. More than 200,000
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
A Patient s Guide to Dropped Head Syndrome
 A Patient s Guide to Dropped Head Syndrome 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
A Patient s Guide to Dropped Head Syndrome 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION
 LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL SERVICES Basic EMT Practical Examination Cardiac Arrest Management
 Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre.
 Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Hockey New South Wales Head Injury Guidelines Effective November
 Hockey New South Wales Effective November 2011 1 Table of Contents Part 1: Guidelines Statement 3 Head Injuries 3 Two Types of Head Injuries 3 Symptoms of Head Injuries 3 Head Injury Notifications 3 Important
Hockey New South Wales Effective November 2011 1 Table of Contents Part 1: Guidelines Statement 3 Head Injuries 3 Two Types of Head Injuries 3 Symptoms of Head Injuries 3 Head Injury Notifications 3 Important
Spinal Injured patients getting adequate rehabilitation
 Starts on day one Requires specially trained staff and team effort Should be done according to the environment in which the patient has to return Major goal of rehabilitation is to reduce disability by
Starts on day one Requires specially trained staff and team effort Should be done according to the environment in which the patient has to return Major goal of rehabilitation is to reduce disability by
Chiropractic Glossary
 Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours
 Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Muscle spasm Diminished bowel sounds Nausea/vomiting
 3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
Malignant Spinal cord Compression. Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania
 Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
CARE OF SPINAL CORD INJURY VICTIMS
 CARE OF SPINAL CORD INJURY VICTIMS Dr THIERRY ALBERT Centre de Rééducation et de Réadaptation pour Adulte de COUBERT Route de Liverdy, Coubert 77257 Brie comte robert, cedex talbert@ugecamif.fr Spinal
CARE OF SPINAL CORD INJURY VICTIMS Dr THIERRY ALBERT Centre de Rééducation et de Réadaptation pour Adulte de COUBERT Route de Liverdy, Coubert 77257 Brie comte robert, cedex talbert@ugecamif.fr Spinal
Head Injury Guidelines POL 5700
 Issued by: WHS Effective Date: 1 st Oct 13 Rev: A Page 1 of 5 1. PURPOSE Concussion - Important information What is a concussion? A concussion is an injury to the brain. A blow to the head usually causes
Issued by: WHS Effective Date: 1 st Oct 13 Rev: A Page 1 of 5 1. PURPOSE Concussion - Important information What is a concussion? A concussion is an injury to the brain. A blow to the head usually causes
STROKE INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
Emergency First Response (EFR) Skills Assessment Sheets V4 June 2017
 Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
Activity and Exercise
 Activity and Exercise Chapter 44 Ra'eda Almashaqba 1 Activity and Exercise refers to the persons rotten of exercise, activity, leisure, and recreation Include: 1. Activity of daily living 2. The type,
Activity and Exercise Chapter 44 Ra'eda Almashaqba 1 Activity and Exercise refers to the persons rotten of exercise, activity, leisure, and recreation Include: 1. Activity of daily living 2. The type,
CERVICAL STRAIN AND SPRAIN
 CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN (Whiplash)
 CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
Stroke. Objectives: After you take this class, you will be able to:
 Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Traumatic Spinal Cord Injury. 39 th CANP Annual Educational Conference March 18 th, :00pm-6:15pm Carl Wherry, ACNP-bc Amanda Severson, ACNP-bc
 Traumatic Spinal Cord Injury 39 th CANP Annual Educational Conference March 18 th, 2016 5:00pm-6:15pm Carl Wherry, ACNP-bc Amanda Severson, ACNP-bc Disclosures No conflicts of interest to disclose. Introduction
Traumatic Spinal Cord Injury 39 th CANP Annual Educational Conference March 18 th, 2016 5:00pm-6:15pm Carl Wherry, ACNP-bc Amanda Severson, ACNP-bc Disclosures No conflicts of interest to disclose. Introduction
Chapter 28 - Head and Spine Injuries
 1 2 3 4 National EMS Education Standard Competencies (1 of 4) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured
1 2 3 4 National EMS Education Standard Competencies (1 of 4) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
Chapter Goal. Learning Objectives 9/12/2012. Chapter 36. Geriatrics. Use assessment findings to formulate management plan for geriatric patients
 Chapter 36 Geriatrics Chapter Goal Use assessment findings to formulate management plan for geriatric patients Learning Objectives Describe dependent & independent living environments Identify local resources
Chapter 36 Geriatrics Chapter Goal Use assessment findings to formulate management plan for geriatric patients Learning Objectives Describe dependent & independent living environments Identify local resources
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Chapter 31. Objectives. Objectives 01/09/2013. Head Trauma
 Chapter 31 Head Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Chapter 31 Head Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Traction. Process of drawing or pulling apart. May involve distraction and gliding. Pulling 2 articulating surfaces away from each other
 Traction Process of drawing or pulling apart May involve distraction and gliding Pulling 2 articulating surfaces away from each other Axis Traction in line with the long axis of a part Types of Traction
Traction Process of drawing or pulling apart May involve distraction and gliding Pulling 2 articulating surfaces away from each other Axis Traction in line with the long axis of a part Types of Traction
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
A Patient's Guide to Cervical Laminectomy
 Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
Introduction A laminectomy is a surgical procedure to relieve pressure on the spinal cord due to spinal stenosis. In spinal stenosis, bone spurs press against the spinal cord, leading to a condition called
ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY INFORMATION
 ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY INFORMATION WHAT IS ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure
ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY INFORMATION WHAT IS ANTERIOR CERVICAL DISCECTOMY AND FUSION (ACDF) SURGERY? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW
 Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Inova. Spine Institute
 Inova Spine Institute At Inova Spine Institute, you ll find a wide range of treatment alternatives, from physical therapy and rehabilitation to pain management. For patients who require surgery, Inova
Inova Spine Institute At Inova Spine Institute, you ll find a wide range of treatment alternatives, from physical therapy and rehabilitation to pain management. For patients who require surgery, Inova
Lumbar Epidural Injections. Treatment to Reduce Pain
 Lumbar Epidural Injections Treatment to Reduce Pain What Is a Lumbar Epidural Injection? Your doctor may have suggested you have a lumbar epidural injection. This procedure can help relieve low back and
Lumbar Epidural Injections Treatment to Reduce Pain What Is a Lumbar Epidural Injection? Your doctor may have suggested you have a lumbar epidural injection. This procedure can help relieve low back and
SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012
 SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012 INTRODUCTION Mortal condition recognised since antiquity First described in the Edwin Smith papyrus 2500BC An ailment not
SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012 INTRODUCTION Mortal condition recognised since antiquity First described in the Edwin Smith papyrus 2500BC An ailment not
Concussion or Mild Traumatic Brain Injury
 Concussion or Mild Traumatic Brain Injury Concussion or Mild Traumatic Brain Injury Table of Contents What is concussion... 2 Causes... 3 Symptoms..3-4 When to get treatment...4-5 Daily activities. 5 Return
Concussion or Mild Traumatic Brain Injury Concussion or Mild Traumatic Brain Injury Table of Contents What is concussion... 2 Causes... 3 Symptoms..3-4 When to get treatment...4-5 Daily activities. 5 Return
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Head Trauma Inservice (October)
 John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
Wounds and Injuries of the Spinal Column and Cord
 Wounds and Injuries of the Spinal Column and Cord Chapter 20 Wounds and Injuries of the Spinal Column and Cord Introduction Combat injuries of the spinal column, with or without associated spinal cord
Wounds and Injuries of the Spinal Column and Cord Chapter 20 Wounds and Injuries of the Spinal Column and Cord Introduction Combat injuries of the spinal column, with or without associated spinal cord
The Surgical Patient. Objectives:
 The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
HEAD INJURY. Dept Neurosurgery
 HEAD INJURY Dept Neurosurgery INTRODUCTION PATHOPHYSIOLOGY CLINICAL CLASSIFICATION MANAGEMENT - INVESTIGATIONS - TREATMENT INTRODUCTION Most head injuries are due to an impact between the head and another
HEAD INJURY Dept Neurosurgery INTRODUCTION PATHOPHYSIOLOGY CLINICAL CLASSIFICATION MANAGEMENT - INVESTIGATIONS - TREATMENT INTRODUCTION Most head injuries are due to an impact between the head and another
Skin and Temperature Management following Spinal Cord Injury. North West Regional Spinal Injuries Centre Southport & Ormskirk NHS Trust
 Skin and Temperature Management following Spinal Cord Injury Functions of the skin The skin is the largest organ of the integumentary system The skin is the interface with the environment and plays an
Skin and Temperature Management following Spinal Cord Injury Functions of the skin The skin is the largest organ of the integumentary system The skin is the interface with the environment and plays an
The Spine.
 The Spine www.fisiokinesiterapia.biz Characteristics of Vertebrae Cervical Spine 1 and 2 Sacrum and Coccyx Curves Lordotic in the Spine Kyphotic Lordotic Ligamentous Support Muscles of the Spine Spinal
The Spine www.fisiokinesiterapia.biz Characteristics of Vertebrae Cervical Spine 1 and 2 Sacrum and Coccyx Curves Lordotic in the Spine Kyphotic Lordotic Ligamentous Support Muscles of the Spine Spinal
Recognition & Treatment of Malignant Spinal Cord Compression Study Day
 Recognition & Treatment of Malignant Spinal Cord Compression Study Day 11 th May 2017 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk Clinical
Recognition & Treatment of Malignant Spinal Cord Compression Study Day 11 th May 2017 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk Clinical
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
