Deep brain stimulation (DBS) in children with primary
|
|
|
- Maryann Stanley
- 5 years ago
- Views:
Transcription
1 J Neurosurg Pediatrics 14: , 2014 AANS, 2014 Interventional MRI guided deep brain stimulation in pediatric dystonia: first experience with the ClearPoint system Clinical article Philip A. Starr, M.D., Ph.D., 1 Leslie C. Markun, M.Sc., 1 Paul S. Larson, M.D., 1 Monica M. Volz, M.S.N., R.N., 1 Alastair J. Martin, Ph.D., 2 and Jill L. Ostrem, M.D. 3 Departments of 1 Neurological Surgery, 2 Radiology, and 3 Neurology, University of California, San Francisco, California Object. The placement of deep brain stimulation (DBS) leads in adults is traditionally performed using physiological confirmation of lead location in the awake patient. Most children are unable to tolerate awake surgery, which poses a challenge for intraoperative confirmation of lead location. The authors have developed an interventional MRI (imri) guided procedure to allow for real-time anatomical imaging, with the goal of achieving very accurate lead placement in patients who are under general anesthesia. Methods. Six pediatric patients with primary dystonia were prospectively enrolled. Patients were candidates for surgery if they had marked disability and medical therapy had been ineffective. Five patients had the DYT1 mutation, and mean age at surgery was 11.0 ± 2.8 years. Patients underwent bilateral globus pallidus internus (GPi, n = 5) or subthalamic nucleus (STN, n = 1) DBS. The leads were implanted using a novel skull-mounted aiming device in conjunction with dedicated software (ClearPoint system), used within a 1.5-T diagnostic MRI unit in a radiology suite, without physiological testing. The Burke-Fahn-Marsden Dystonia Rating Scale (BFMDRS) was used at baseline, 6 months, and 12 months postoperatively. Further measures included lead placement accuracy, quality of life, adverse events, and stimulation settings. Results. A single brain penetration was used for placement of all 12 leads. The mean difference (± SD) between the intended target location and the actual lead location, in the axial plane passing through the intended target, was 0.6 ± 0.5 mm, and the mean surgical time (leads only) was 190 ± 26 minutes. The mean percent improvement in the BFMDRS movement scores was 86.1% ± 12.5% at 6 months (n = 6, p = 0.028) and 87.6% ± 19.2% at 12 months (p = 0.028). The mean stimulation settings at 12 months were 3.0 V, 83 msec, 135 Hz for GPi DBS, and 2.1 V, 60 msec, 145 Hz for STN DBS). There were no serious adverse events. Conclusions. Interventional MRI guided DBS using the ClearPoint system was extremely accurate, provided realtime confirmation of DBS placement, and could be used in any diagnostic MRI suite. Clinical outcomes for pediatric dystonia are comparable with the best reported results using traditional frame-based stereotaxy. Clinical trial registration no.: NCT (ClinicalTrials.gov). ( Key Words dystonia deep brain stimulation interventional MRI functional neurosurgery pediatrics Abbreviations used in this paper: BFMDRS = Burke-Fahn- Marsden Dystonia Rating Scale; DBS = deep brain stimulation; GPi = globus pallidus internus; imri = interventional MRI; IPG = implantable pulse generator; STN = subthalamic nucleus. Deep brain stimulation (DBS) in children with primary dystonia can be highly effective for longterm symptom suppression. 1,4,6,8,18,21 Clinical outcome is critically dependent on exact lead placement in the posterior (motor) area of the internal pallidum, 26,28 but surgical methods to achieve excellent lead placement have not been standardized. In adults, the traditional method for DBS lead implantation involves physiological localization while patients are awake. 26 Physiological localization methods have included microelectrode recording and/or intraoperative test stimulation to assess for acute stimulation-induced adverse or therapeutic effects. 26 Since these methods often require the patient to be calm and cooperative for several hours of testing, they are not appropriate for most children. To address these issues, we have developed methods for implanting DBS leads using real-time interventional MRI (imri) guidance in conjunction with a skull-mounted aiming device. The procedure is performed within the isocenter of a high-field diagnostic magnet in a radiology suite. Our initial work on imri-guided DBS implantation, developed in adults with Parkinson s disease, 19,25 used a previously created skull-mounted aiming device (Nexframe, Medtronic Inc.). The Nexframe was not specifically designed for imri applications. Based on this experience, we developed a second-generation device (ClearPoint, MRI Interventions, Inc.), which has improved mechanical controls and an integrated software package intended to improve ease of use and accuracy of targeting. 11 In the present 400 J Neurosurg: Pediatrics / Volume 14 / October 2014
2 ClearPoint system for DBS in pediatric dystonia study, we used this imri device to demonstrate placement of DBS leads in children and found it to be associated with extremely high accuracy and excellent clinical outcome. This is the first report of DBS lead placement accuracy and clinical outcomes using the ClearPoint system. Methods Patient Selection and Clinical Characterization Patient characteristics are described in Table 1. Six pediatric patients with primary dystonia were prospectively enrolled (clinical trial registration no. NCT [ClinicalTrials.gov]). The study was approved by the UCSF institutional review board. Parental informed consent for the study was obtained in all cases. Patients were candidates for surgery if they had significant disability and medical therapy had been ineffective. Patients received bilateral globus pallidus internus (GPi, n = 5) or subthalamic nucleus (STN, n = 1) DBS. The patient undergoing STN stimulation was also part of a prospective study of STN DBS in primary dystonia. 20 The Burke-Fahn-Marsden Dystonia Rating Scale (BFMDRS) was administered at baseline, 6 months, and 12 months postoperatively. Further outcome measures included quality of life, adverse events, and stimulation settings. Surgical Procedure: Brain Leads The leads were implanted using a novel skull-mounted aiming device in conjunction with dedicated software (ClearPoint system), used within a 1.5-T diagnostic MRI scanner (Philips Intera, 60-cm bore diameter) in a radiology suite, with the patient under general anesthesia and without physiological testing. The main features of the ClearPoint system have been described in a previously published technical report on device performance in a phantom skull and in cadaver heads. 11 The primary hardware component of the ClearPoint system is the skull-mounted aiming device ( SmartFrame ), pictured in Fig. 1A. It has 4 degrees of freedom, with pitch (angulation in the sagittal plane) and roll (angulation in the coronal plane) controls for coarse angular adjustment, and X (right-left axis) and Y (anterior-posterior axis) controls for fine linear adjustment. The central MRI-visible alignment stem has a hollow lumen with an internal diameter of 2.1 mm for passage of a ceramic stylet within a Silastic peel-away sheath. After induction of anesthesia in a room adjacent to the MRI unit, the head is positioned in a 4-pin carbon fiber head holder (Malcolm-Rand, Integra Inc.), with flexible surface receiving coils on either side, and moved through the MRI bore so that the top of the head is accessible at the back. For children under 10 years of age, pressure applied to the head holder pins is reduced to avoid excessive bone penetration or fracture. After sterile prep, a drape is used that attaches by elastic cords at each end of the bore to maintain the sterile field during movements of the head between isocenter and the back of the bore (Fig. 1E). The head positioning and draping procedure are identical to those described in our previous report. 25 A cm MRI-visible marking grid is placed on each side of the scalp to span the coronal suture, and the J Neurosurg: Pediatrics / Volume 14 / October 2014 patient s head is returned to isocenter. A Gd-enhanced volumetric MRI scan is acquired and imported into ClearPoint software. An approximate target and safe trajectory to that target are selected (Fig. 1B), and the entry point is visualized on the software so as to show the intersection of the trajectory with the marking grid (Fig. 1C). The patient s head is moved to the back of the bore, where a sharp marking tool is used to penetrate the marking grid, skull, and scalp at the intended entry location (Fig. 1D), and then the marking grid is removed, a bicoronal incision is made, and 1.5-cm bur holes are drilled with an MRI-compatible high-speed drill (Anspach or Stryker). These drill kits also include a craniotome attachment, to allow the surgeon to perform urgent craniotomy in the MRI suite should a significant, surgically accessible hematoma evolve on serial MR images during the procedure. The dura and pia mater are coagulated and opened sharply, and the SmartFrames and Stimloc lead anchoring rings (Medtronic Inc.) are mounted over the bur holes. The mechanical remote controls are attached (Fig. 1E) and the head returned to the isocenter. Volumetric T1-weighted gradient echo sequences are obtained through the SmartFrames and imported into ClearPoint software for automated recognition of device position and trajectory. High-resolution imaging using T2-weighted fast spin echo and inversion-recovery fast spin echo images are obtained through the basal ganglia to provide optimal definition of target boundaries. The MRI sequences used have been previously described. 25 The target selection method is illustrated in Fig. 2. Alignment of the SmartFrame cannulas was then performed iteratively, initially using oblique axial scans through the alignment stem (Fig. 3A and B), in conjunction with the prescribed movements of the pitch and roll controls until the predicted radial placement error was less than 1.0 mm. Next, oblique sagittal and coronal scans (Fig. 3A and C) were acquired in conjunction with movement of the X and Y controls until the predicted radial error was less than 0.5 mm. (Measurement of radial error is further described below and in Fig. 4.) An overshoot was planned for each target; this overshoot was standardized for the STN target at 2 mm deep to the targeting plane and customized for the GPi target based on the measured distance between the targeting plane and the dorsal border of optic tract, typically 4 6 mm. A depth stop was placed on the ceramic stylet/peel-away sheath to reflect the intended overshoot, and the stylet/sheath was inserted to target. Oblique sagittal and coronal images were obtained through the trajectory at intermediate steps to confirm appropriate passage without hemorrhage. With both stylets at the target, a high-resolution axial T2-weighted MR image was used to confirm correct positioning (Fig. 3D). The ceramic stylet was removed and replaced with a quadripolar DBS lead (Model , Medtronic). After confirming correct lead depth using low-energy axial T2-weighted MRI, the patient s head was returned to the back of the bore for removal of the peel-away sheath, anchoring of the lead using the clip and cap of the Stimloc system, removal of the SmartFrames, and closure of the scalp. All patients were placed in a Kerlix head wrap for 1 week to protect the incisions. 401
3 P. A. Starr et al. TABLE 1: Patient characteristics and clinical outcomes* Medications (per day) BFMDRS MS/DS SF-36v2 Total Score Baseline 12 Mos Target Baseline 12 Mos Baseline 12 Mos Affected Body Regions DYT1 Status Duration of Disease (yrs) Age (yrs), Sex Patient No. none GPi 44/14 4/ trihexyphenidyl 22.5 mg; clonazepam 0.5 mg BID 1 9, M 2 DYT1+ M, N, T, RA, LA, RL, LL none none GPi 46/4 15.5/ N, T, RA, LA, RL, LL 2 13, F 6 not tested none GPi 68/15 0/ trihexyphenidyl 12 mg; Lioresal 20 mg; carbidopa/levodopa 30/300 mg 3 11, M 3 DYT1+ N, T, RA, LA, RL, LL trihexyphenidyl 12 mg; Lioresal 40 mg none STN 22.5/8 1/ , M 2 DYT1+ E, S, N, RA, RL, LL none GPi 36.5/12 0/ trihexyphenidyl 30 mg; clonazepam 1.5 mg; dexmethylphenidate hydrochloride 15 mg; diphenhydramine 12.5 mg 5 11, F 4 DYT1+ N, T, RA, LA, RL, LL 6 7, M 1 DYT1+ RA, T, RL, LL trihexyphenidyl 22.5 mg; Lioresal 55 mg none GPi 20/15 9/ mean (± SD) 11.0 (2.8) 3.0 (1.8) 39.5/11.3 (17.6)/(4.5) 4.9/2.3 (6.2)/(1.6) 53.5 (13.7) 81.7 (13.3) * BID = twice daily; DS = disability score; E = eyes; LA = left arm; LL = left leg; M = mouth; MS = movement score; N = neck; RA = right arm; RL = right leg; S = speech/swallowing; T = trunk; + = positive. Surgical Procedure: Pulse Generators and Lead Extenders The implantable pulse generators (IPGs) and lead extenders were placed in a separate inpatient or outpatient procedure 1 2 weeks after lead implantation. The reason for placing the IPGs in a separate procedure was logistical: lead placement occurred in a radiology suite, not an operating room, with a limited set of fully MRIcompatible surgical instruments. Placement of IPGs under the same anesthesia would have required transporting the patient to a waiting, open operating room set up by a separate nursing team. The free ends of the DBS leads were accessed via parietal incisions 3 5 cm posterior to the frontal bur hole. Four patients had bilateral, single-channel primary cell IPGs (Activa SCs, Medtronic) placed in the pectoral area, connected to the leads using 40-cm lead extenders (Model Medtronic). One patient requested bilateral Activa SCs placed in the abdomen with 60-cm lead extenders (for cosmetic reasons), and one requested a dual-channel rechargeable IPG (Activa RC) placed in the right chest using 40-cm lead extenders, to avoid having to return regularly for IPG replacement. Patients were again placed in a Kerlix head wrap for 1 week to protect the parietal incisions. Device Programming Neurostimulator programming was initiated 1 2 weeks after lead implantation. Each contact was activated separately in unipolar mode. Voltage-limiting adverse effects were noted. In all patients the stimulator was initially programmed using 1 contact in unipolar mode, typically at 60-msec pulse width using a frequency of 130 Hz. The initial contact chosen was the one for which clinical improvement was most apparent. If no therapeutic effect was noted in the initial programming session, then the contact within the posterior lateral GPi or dorsal STN, based on postoperative MRI, was chosen for chronic stimulation (typically Contact 1). The voltage was slowly increased over the first 2 4 weeks. Patients with GPi stimulators returned for follow-up programming visits every few months if needed, and if dystonia was not controlled at a voltage of 3.5 V, then generally a second contact was used or pulse width was increased. Additional considerations for STN programming have been previously described. 20 Evaluation of Lead Placement Accuracy We considered the most clinically relevant measure of lead placement accuracy to be the radial error, defined as the difference between the intended and actual lead trajectory, measured in the axial plane used for anatomical targeting (Fig. 4). We also calculated a trajectory error defined as the closest distance between the intended and actual lead trajectory (always perpendicular to the trajectories), since some prior papers on the accuracy of DBS placement use this measure preferentially. 3 The trajectory error is slightly smaller than the radial error, with the exact difference depending on the angle of placement with respect to the axial plane used for targeting (Fig. 4). Three-dimensional vector errors between the intended tip and actual tip location are less clinically relevant, as small lead misplacements (> 2 mm) along the 402 J Neurosurg: Pediatrics / Volume 14 / October 2014
4 ClearPoint system for DBS in pediatric dystonia Fig. 1. SmartFrame design, trajectory planning, and bore draping. A: Photograph of the SmartFrame. Colored knobs control the 4 degrees of freedom: pitch, roll, X, and Y. B: Trajectory plan for a GPi DBS case (yellow line), avoiding sulci, cortical veins, and lateral ventricle. The white rectangles on the scalp surface are part of the MRI-visible surface marking grid. C: Reconstruction in ClearPoint software of the surface marking grids, indicating the desired entry point selected in the trajectory planning step. D: The marking tool is used to mark the scalp and skull through the marking grids. E: SmartFrames mounted over bur holes, with mechanical remote controls attached, just before moving the patient s head to the isocenter. axis of implantation can easily be corrected by selection of a different active contact from the quadripolar lead. Statistical Analysis The difference between the BFMDRS movement scores at baseline compared with 12 months (on stimulation) were assessed using the Wilcoxon matched-pairs signed-rank test. Except for mean data pertaining to lead tip location and stimulation settings, and unless otherwise specified, mean values are presented ± SD. Results Surgical Experience and Lead Placement Accuracy A single brain penetration was used for placement of all 12 leads. The mean surgical time (leads only) was 190 ± 26 minutes. The mean radial error (as defined in Fig. 4) was 0.6 ± 0.5 mm. The mean trajectory error (defined in Fig. 4) was 0.54 ± 0.40 mm. For the lead implant with the largest radial error (1.8 mm), we noted upon anchoring the lead that the guidance sheath was slightly deflected by the edge of the dura. The mean lead tip location relative to the midcommissural point for GPi leads (n = 10) was as J Neurosurg: Pediatrics / Volume 14 / October 2014 follows: X = mm, Y = 3.13 mm, and Z = mm. The mean tip locations for the two STN leads were X = 11.1 mm, Y = mm, and Z = mm. DBS Parameters, Clinical Improvement, and Complications Individual stimulation settings at 12 months are provided in Table 2. The mean settings were 3.0 V, 83 msec, 135 Hz for GPi DBS) and 2.1 V, 60 msec, 145 Hz for STN DBS. Individual improvements in the BFMDRS movement scores are shown in Fig. 5 and Table 1. The mean percentage improvement in the BFMDRS movement score was 87.6% ± 19.2% (p = 0.028) at 12 months, and the mean percentage improvement in BFMDRS disability score was 77.2% ± 1.6% (p = 0.033) at 12 months. Quality of life (SF-36v2) scores improved by 52.6% (p = 0.027) overall at 12 months. Adverse events included the following single events: transient slurred speech, transient dyskinesia, an episode of unexplained nausea and dizziness, right knee pain, left shoulder pain, and an open circuit on one contact of one lead. There were no serious adverse events, no returns to the operating room within the 12-month follow-up period, and no hematomas seen on MRI after lead placement. 403
5 Duration of Hospitalization P. A. Starr et al. The mean length of hospital stay following imriguided lead placement was 3.3 ± 2.3 days. This duration of hospitalization did not differ from that (2.7 ± 0.8 days) documented for a cohort of 6 children with primary generalized dystonia of similar age range, in whom implantation was performed by the same surgeon but using traditional frame-based stereotaxy 1 prior to the introduction of the imri technique. The duration of hospital stay appears to be determined by factors other than surgical technique, such as the temporary increase in dystonic symptoms that may occur postoperatively as a result of the stress of surgery and anesthesia. 1 Discussion We used a novel skull-mounted guidance system, specifically designed for imri applications, to perform bilateral DBS implantation in a consecutive series of 6 pediatric patients with primary generalized dystonia. Aiming and advancing of the guidance sheath and DBS leads were performed at the isocenter of a 1.5-T diagnostic magnet in a radiology suite. We achieved a high placement accuracy, exceeding that of earlier hardware systems used for imri-guided DBS, 25 with clinical outcomes comparable to the best reported results for DBS in primary dystonia when using other surgical methods. Fig. 2. Targeting strategy showing the location of intended active contacts. A: GPi. The target is selected on the axial plane of the commissures by measuring the pallidocapsular border, dividing it into thirds, and drawing a 3- to 4-mm line perpendicular to the pallidocapsular border at the junction of its posterior one-third and anterior two-thirds. B: STN. The target is selected on the axial plane best showing the medial border of the STN and top of the red nuclei (RN), typically 4 mm inferior to the plane of the commissures. A line is drawn perpendicular to the midline, tangent to the anterior border of the RN, extending 2 mm lateral to the medial border of the STN. AC = anterior commissure; GPe = globus pallidus externus; LT = lamina terminalis; PC = posterior commissure; 3rd = third ventricle. Note that the lead tip is placed inferior to the selected target with an overshoot of 2 mm for the STN and 4 6 mm for the GPi (see Methods). imri Approach for Asleep DBS: Comparison With Other Methods Since the introduction of thalamic DBS for adults with tremor disorders 2 and STN or GPi DBS for individuals with advanced Parkinson s disease, 13,23 the predominant technique for implantation has involved physiological testing in awake patients as the final determinant of electrode position. However, this approach is not ideal for some patients who could benefit from DBS, such as children with dystonia or adults with Parkinson s disease or dystonia who have severe involuntary movements in the off-medication state or significant anxiety about the awake procedure. A number of centers have developed alternative approaches in which DBS implantation is performed under general anesthesia, and brain imaging rather than physiology is used to finalize the lead position. One approach is to use frame-based stereotaxy with the patient under general anesthesia in an operating room to place DBS electrodes, or permanent guide tubes, with immediate transport to an MRI suite for postoperative imaging to confirm location. 15,22 If the initial placement is considered inadequate, the patient may have the lead repositioned in the operating room while still under anesthesia. However, the initial placement is then subject to the accuracy limitations of standard stereotactic methods that use preoperative images registered to a frame system 14 and involves the logistical complexity of transporting a patient to multiple locations for a single surgery. Alternatively, intraoperative CT scanning has recently been used for asleep DBS, both for the stereotactic image acquisition and immediate intraoperative check of lead position. 3 The intraoperative CT scan is fused to a 404 J Neurosurg: Pediatrics / Volume 14 / October 2014
6 ClearPoint system for DBS in pediatric dystonia Fig. 3. SmartFrame alignment and confirmation of stylet placement. A: Photograph of the SmartFrame (mounted on skull model) showing the imaging planes used to align it to the target. The orange line shows the oblique axial plane imaged in B, and the green line is the intersection of the oblique sagittal and coronal planes shown in C. B: Oblique axial MR image used in conjunction with ClearPoint software to adjust pitch and roll controls. C: Oblique sagittal and coronal MR images used in conjunction with ClearPoint software, to adjust the X and Y controls. D: Intraoperative T2-weighted axial image through the GPi, showing the position of ceramic stylet and sheath (indicated by white arrows) used to guide the lead into the correct position (Patient 5). preoperative MR image for both target selection and final confirmation of lead placement. The technique is efficient, with short operating room times and no need to transport patients between the surgical suite and radiology suite on the day of surgery. However, the method is limited by the mechanical accuracy of frame-based stereotaxy14 as well as errors that may be introduced by suboptimal CT-MR fusion.27 The mean ± SEM trajectory error (closest distance between actual and intended trajectories) in a study of 119 electrode placements was 1.24 ± 0.87 mm, with a J Neurosurg: Pediatrics / Volume 14 / October 2014 range of mm3. When targeting errors in the present study are calculated identically (see Fig. 4), our trajectory error is substantially smaller: 0.54 ± 0.40 mm with a range of mm. ClearPoint Compared With Prior imri Techniques From 2004 to 2010, we performed imri-guided DBS placement using the Medtronic Nexframe skull-mounted aiming device,19,25 which was primarily designed for neuronavigation-guided DBS implantation9 rather than 405
7 P. A. Starr et al. Fig. 4. Schematic of the method for measuring radial error and trajectory error. The axial plane is the plane used for selecting the target. The radial error (r) equals the distance between the actual lead and the intended trajectory, where each intersects the plane of targeting. Trajectory error (t) equals the closest distance between the intended trajectory and the actual lead trajectory. 3 imri. The Nexframe device has 2 mechanical degrees of freedom. An MRI-visible alignment stem, inserted into the Nexframe, was employed for the imri environment. To analyze the accuracy of that system, we primarily used the radial error, the 2D difference between the intended and actual lead trajectories in the axial plane used to define the target. This is similar to, but slightly larger than, the trajectory error (Fig. 4). In 53 imri-guided lead implants that involved the Nexframe, mean (± SEM) radial error was 1.2 ± 0.65 mm. 25 Based on our experience with the Nexframe, we designed the ClearPoint system for imri DBS with a variety of improvements: an XY stage-mounted on the pitch/roll controls that provides for finer mechanical control after approximate initial alignment, an integrated software system, mechanical remote control for easy aiming of the device without reaching into the bore, and an MRI-visible alignment stem with a hollow lumen allowing delivery of devices through the alignment stem without the need to remove the alignment stem and replace it with guidance cannulas. The present study indicates that the accuracy of the ClearPoint system as used clinically, with a mean radial error of 0.6 ± 0.5 mm, is improved over that of the prior Nexframe system. This will need to be confirmed in a larger series utilizing the same brain target (STN) as the Nexframe imri study. 25 Of note, the mean radial error observed here in clinical use is very similar to that measured in preclinical phantom studies (0.5 ± 0.3 mm). 11 The improved accuracy of the ClearPoint system is probably related to the integration of successive imaging steps with progressively finer mechanical control of the aiming system. Following coarse angular adjustments with pitch/ roll controls, longitudinal MRI through the long axis of the alignment stem is used to make submillimeter linear TABLE 2: Active contact locations and stimulator settings at 12 months DBS Settings (lt brain) Active Contacts (lt brain)* DBS Settings (rt brain) Active Contacts (rt brain) Contacts V μsec Hz X Y Z Contacts V μsec Hz X Y Z Patient No. Target 1 GPi C C GPi C C GPi C C STN C GPi C C GPi C C * Measured with respect to the midcommissural point. 406 J Neurosurg: Pediatrics / Volume 14 / October 2014
8 ClearPoint system for DBS in pediatric dystonia Limitations The imri method of lead placement, similar to any other purely image-guided method, is totally dependent on high-resolution structural imaging to define target boundaries and on having MRI-based criteria for successful lead implantation. Here, as in prior reports, we found that optimal outcome for GPi DBS is associated with active contacts located near the intercommissural plane, 3 4 mm lateral to the pallidocapsular border at the junction of its posterior one-third and anterior two-thirds (Fig. 2). 26,28 Although technically simpler than awake microelectrode-guided stereotactic surgery, the unforgiving nature of target selection (no opportunity to physiologically refine an improperly selected target) mandates extreme care in the target selection step. This study documents results of imri-guided DBS using a 1.5-T narrow-bore MRI system, whereas 3.0-T widebore systems are increasingly common. The accuracy data reported here would not necessarily generalize to a 3.0-T or wider-bore system, with which image distortion effects may compromise the ability of the software to accurately reconstruct the position of the aiming device. 29 Users of ClearPoint systems with a magnetic field strength higher than 1.5 T, or a bore diameter greater than 60 cm, should carefully evaluate their own lead placement accuracy data. Fig. 5. Individual improvements in the BFMDRS movement score. adjustments of the X and Y controls. This level of fine mechanical control was impossible with the prior system. Clinical Outcomes Comparable to the Best Results Previously Reported Six case series, reporting a total of 75 patients, have provided 12-month outcome data using standardized rating scales for bilateral DBS in children with primary dystonia. 1,4,6,8,16,18 All of these studies used frame-based stereotaxy with targeting performed on MR images acquired prior to surgery and computationally registered to the frame axes. Improvements in the BFMDRS movement score from baseline to 12 months postimplantation ranged from 62% to 85%, except for one outlier study reporting substantially less benefit. 16 Our mean improvement of 87.6% ± 19.2% is comparable to the best results from the published literature, and the incidence of serious adverse events (prolonging hospitalization or requiring further surgery) was zero. Of note, none of our patients had fixed orthopedic deformity or extremely long (> 10 years) symptom duration, which would probably be associated with more limited improvement. 10,17 The one patient who underwent STN DBS (for DYT1-positive dystonia) had almost complete resolution of symptoms, at 12 months, with a decline in BFMDRS movement score from 22.5 to 1 (Table 1). J Neurosurg: Pediatrics / Volume 14 / October 2014 Application of the imri Method to Younger Children The purchase lengths of the screws used to mount the SmartFrame aiming device and Stimloc DBS lead anchoring ring are 4 mm and 5 mm, respectively. Since the frontal bone thickness in children under 10 years old is often less than 5 mm, 12 screws in younger patients may penetrate the full thickness of the skull. Should epidural bleeding occur due to screw penetration, this could be readily detected on subsequent MR images obtained after mounting the device, but no hematomas from screw placement were observed in the present series. For bilateral SmartFrame mounting with bur holes closer than 4.5 cm apart, there is a possibility for the control knobs on the devices to collide, depending on skull morphology and trajectory angles. After marking the scalp entry sites, it is advisable to place both SmartFrames over the intended entry sites to check for physical contact between the devices prior to drilling the bur holes. In most children, we prefer to place bilateral single channel pulse generators (Activa SC, Medtronic) rather than a larger, unilateral, dual-channel pulse generator, for the following reasons: 1) the lower profile of the singlechannel systems may reduce hardware-related complications; 24 2) battery life of two single-channel generators is generally longer than that of one dual-channel generator; 7 and 3) battery failure, if it affected both sides simultaneously, could result in a rapid recurrence of symptoms that constitute a medical emergency such as dystonic storm. 5 Conclusions Interventional MRI guided DBS is technically simple, extremely accurate, provides real-time confirmation of DBS placement, and can be used in any diagnostic MRI facility. Clinical outcomes are comparable with the best reported results of traditional frame-based stereotaxy. The method is dependent on excellent quality imaging. Acknowledgments We thank Salman Qasim, B.S., and Nathan Ziman, B.S., for technical assistance in preparing the manuscript. Disclosure This study was funded by a research grant from MRI Interventions, Inc., the manufacturer of ClearPoint. Three of the authors (P.A.S., P.S.L., and A.J.M.) designed the ClearPoint system in collaboration with MRI Interventions, Inc., and continue to receive research funding with salary support for further development and testing of the system. However, the authors hold no intellectual 407
9 P. A. Starr et al. property in this system, hold no ownership stake or stock options in MRI Interventions, Inc., and do not receive royalty payments from the company. Dr. Ostrem is a consultant for Medtronic, Abbvie, and Allergen. She received study-related support from MRI Interventions, and she receives non study-related support from St. Jude Medical and Ceregene. Author contributions to the study and manuscript preparation include the following. Conception and design: all authors. Acquisition of data: Starr, Markun, Larson, Volz, Martin. Analysis and interpretation of data: Starr, Markun, Martin. Drafting the article: Starr, Markun, Larson, Volz, Ostrem. Critically revising the article: all authors. Reviewed submitted version of manuscript: all authors. Approved the final version of the manuscript on behalf of all authors: Starr. Statistical analysis: Markun, Martin. Administrative/ technical/material support: Markun, Larson, Volz, Martin, Ostrem. Study supervision: Starr, Larson, Volz, Martin, Ostrem. References 1. Air EL, Ostrem JL, Sanger TD, Starr PA: Deep brain stimulation in children: experience and technical pearls. Clinical article. J Neurosurg Pediatr 8: , Benabid AL, Pollak P, Gao D, Hoffmann D, Limousin P, Gay E, et al: Chronic electrical stimulation of the ventralis intermedius nucleus of the thalamus as a treatment of movement disorders. J Neurosurg 84: , Burchiel KJ, McCartney S, Lee A, Raslan AM: Accuracy of deep brain stimulation electrode placement using intraoperative computed tomography without microelectrode recording. Clinical article. J Neurosurg 119: , Coubes P, Cif L, El Fertit H, Hemm S, Vayssiere N, Serrat S, et al: Electrical stimulation of the globus pallidus internus in patients with primary generalized dystonia: long-term results. J Neurosurg 101: , Frucht SJ: Treatment of movement disorder emergencies. Neurotherapeutics 11: , Ghosh PS, Machado AG, Deogaonkar M, Ghosh D: Deep brain stimulation in children with dystonia: experience from a tertiary care center. Pediatr Neurosurg 48: , Halpern CH, McGill KR, Baltuch GH, Jaggi JL: Longevity analysis of currently available deep brain stimulation devices. Stereotact Funct Neurosurg 89:1 5, Haridas A, Tagliati M, Osborn I, Isaias I, Gologorsky Y, Bressman SB, et al: Pallidal deep brain stimulation for primary dystonia in children. Neurosurgery 68: , Holloway KL, Gaede SE, Starr PA, Rosenow JM, Ramakrishnan V, Henderson JM: Frameless stereotaxy using bone fiducial markers for deep brain stimulation. J Neurosurg 103: , Isaias IU, Alterman RL, Tagliati M: Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration. Brain 131: , Larson PS, Starr PA, Bates G, Tansey L, Richardson RM, Martin AJ: An optimized system for interventional magnetic resonance imaging-guided stereotactic surgery: preliminary evaluation of targeting accuracy. Neurosurgery 70 (1 Suppl Operative):95 103, Letts M, Kaylor D, Gouw G: A biomechanical analysis of halo fixation in children. J Bone Joint Surg Br 70: , Limousin P, Krack P, Pollak P, Benazzouz A, Ardouin C, Hoffmann D, et al: Electrical stimulation of the subthalamic nucleus in advanced Parkinson s disease. N Engl J Med 339: , Maciunas RJ, Galloway RL Jr, Latimer JW: The application accuracy of stereotactic frames. Neurosurgery 35: , Maldonado IL, Roujeau T, Cif L, Gonzalez V, El-Fertit H, Vasques X, et al: Magnetic resonance-based deep brain stimulation technique: a series of 478 consecutive implanted electrodes with no perioperative intracerebral hemorrhage. Neurosurgery 65 (6 Suppl): , Marks W, Bailey L, Reed M, Pomykal A, Mercer M, Macomber D, et al: Pallidal stimulation in children: comparison between cerebral palsy and DYT1 dystonia. J Child Neurol 28: , Markun LC, Starr PA, Air EL, Marks WJ Jr, Volz MM, Ostrem JL: Shorter disease duration correlates with improved long-term deep brain stimulation outcomes in young-onset DYT1 dystonia. Neurosurgery 71: , Mehrkens JH, Borggraefe I, Feddersen B, Heinen F, Bötzel K: Early globus pallidus internus stimulation in pediatric patients with generalized primary dystonia: long-term efficacy and safety. J Child Neurol 25: , Ostrem JL, Galifianakis NB, Markun LC, Grace JK, Martin AJ, Starr PA, et al: Clinical outcomes of PD patients having bilateral STN DBS using high-field interventional MR-imaging for lead placement. Clin Neurol Neurosurg 115: , Ostrem JL, Racine CA, Glass GA, Grace JK, Volz MM, Heath SL, et al: Subthalamic nucleus deep brain stimulation in primary cervical dystonia. Neurology 76: , Parr JR, Green AL, Joint C, Andrew M, Gregory RP, Scott RB, et al: Deep brain stimulation in childhood: an effective treatment for early onset idiopathic generalised dystonia. Arch Dis Child 92: , Patel NK, Plaha P, Gill SS: Magnetic resonance imaging-directed method for functional neurosurgery using implantable guide tubes. Neurosurgery 61 (5 Suppl 2): , Siegfried J, Lippitz B: Bilateral chronic electrostimulation of ventroposterolateral pallidum: a new therapeutic approach for alleviating all parkinsonian symptoms. Neurosurgery 35: , Sillay KA, Larson PS, Starr PA: Deep brain stimulator hardware-related infections: incidence and management in a large series. Neurosurgery 62: , Starr PA, Martin AJ, Ostrem JL, Talke P, Levesque N, Larson PS: Subthalamic nucleus deep brain stimulator placement using high-field interventional magnetic resonance imaging and a skull-mounted aiming device: technique and application accuracy. Clinical article. J Neurosurg 112: , Starr PA, Turner RS, Rau G, Lindsey N, Heath S, Volz M, et al: Microelectrode-guided implantation of deep brain stimulators into the globus pallidus internus for dystonia: techniques, electrode locations, and outcomes. J Neurosurg 104: , Thani NB, Bala A, Swann GB, Lind CR: Accuracy of postoperative computed tomography and magnetic resonance image fusion for assessing deep brain stimulation electrodes. Neurosurgery 69: , Vayssiere N, Hemm S, Zanca M, Picot MC, Bonafe A, Cif L, et al: Magnetic resonance imaging stereotactic target localization for deep brain stimulation in dystonic children. J Neurosurg 93: , Watanabe Y, Lee CK, Gerbi BJ: Geometrical accuracy of a 3-tesla magnetic resonance imaging unit in Gamma Knife surgery. J Neurosurg 105 Suppl: , 2006 Manuscript submitted November 13, Accepted June 30, Part of this study was presented in abstract form at the Society for Movement Disorders, Sydney, Australia, June Please include this information when citing this paper: published online August 1, 2014; DOI: / PEDS Address correspondence to: Philip A. Starr, M.D., Ph.D., Department of Neurological Surgery, University of California, San Francisco, 779 Moffitt, 505 Parnassus Ave., San Francisco, CA starrp@neurosurg.ucsf.edu. 408 J Neurosurg: Pediatrics / Volume 14 / October 2014
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
SUPPLEMENTAL DIGITAL CONTENT
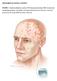 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep brain stimulation (DBS) has been shown to be
 clinical article J Neurosurg 124:908 916, 2016 Clinical outcomes using ClearPoint interventional MRI for deep brain stimulation lead placement in Parkinson s disease Jill L. Ostrem, MD, 1 Nathan Ziman,
clinical article J Neurosurg 124:908 916, 2016 Clinical outcomes using ClearPoint interventional MRI for deep brain stimulation lead placement in Parkinson s disease Jill L. Ostrem, MD, 1 Nathan Ziman,
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Pallidal Deep Brain Stimulation
 Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
P rimary generalised dystonia (PGD) is a movement disorder
 1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
Deep brain stimulation: What can patients expect from it?
 MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease
 CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
DBS Programming. Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18
 DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
Palladotomy and Pallidal Deep Brain Stimulation
 Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Surgical Management of Parkinson s Disease
 Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
Introduction of FIREFLY Technology
 Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
S ince the pioneering work of Benabid et and Pollak
 409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
As clinical experience with deep-brain stimulation (DBS) of
 ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. What is Parkinson s Disease?
 Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
The Surgical Management of Essential Tremor
 The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group
 Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
Parkinson disease: Parkinson Disease
 Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
2014 AAPM 56 th Annual Meeting
 2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech?
 Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Surgical Options. A History of Surgical Treatment. Patient selection. Essential Tremor (ET)
 Essential tremor (ET) is the most common movement disorder, impacting the lives of an estimated 10 million Americans and millions more worldwide. At this time, there is no cure for ET and only about 50%
Essential tremor (ET) is the most common movement disorder, impacting the lives of an estimated 10 million Americans and millions more worldwide. At this time, there is no cure for ET and only about 50%
National Institute for Health and Clinical Excellence
 National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
Troubleshooting algorithms for common DBS related problems in tremor and dystonia
 Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI
 Niederer 1 High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI Abstract In the past several decades the introduction of high-resolution, three-dimensional modeling techniques have
Niederer 1 High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI Abstract In the past several decades the introduction of high-resolution, three-dimensional modeling techniques have
Reformatted Imaging to Define the Intercommissural Line for CT -Guided Stereotaxic Functional Neurosurgery
 Reformatted Imaging to Define the Intercommissural Line for CT -Guided Stereotaxic Functional Neurosurgery 429 Richard E. Latchaw1.2 L. Dade Lunsford 1. 2 William H. Kennedi Functional stereotaxic neurosurgery
Reformatted Imaging to Define the Intercommissural Line for CT -Guided Stereotaxic Functional Neurosurgery 429 Richard E. Latchaw1.2 L. Dade Lunsford 1. 2 William H. Kennedi Functional stereotaxic neurosurgery
No Financial Disclosures
 Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri)
 1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
Citation for published version (APA): Contarino, M. F. (2013). Improving surgical treatment for movement disorders
 UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
Stereotactic Radiosurgery. Extracranial Stereotactic Radiosurgery. Linear accelerators. Basic technique. Indications of SRS
 Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation
 The Open Magnetic Resonance Journal, 2008, 1, 1-8 1 Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation X.A. Vasques 1-5, C. Tancu
The Open Magnetic Resonance Journal, 2008, 1, 1-8 1 Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation X.A. Vasques 1-5, C. Tancu
Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging
 J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
Deep Brain Stimulation to treat Parkinson s Disease
 Deep Brain Stimulation to treat Parkinson s Disease Reading this booklet can help you learn how Deep Brain Stimulation is used to help relieve symptoms of Parkinson s Disease. Your health care team will
Deep Brain Stimulation to treat Parkinson s Disease Reading this booklet can help you learn how Deep Brain Stimulation is used to help relieve symptoms of Parkinson s Disease. Your health care team will
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
10/13/2017. Disclosures. Deep Brain Stimulation in the Treatment of Movement Disorders. Deep Brain Stimulation: Objectives.
 Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery
 Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
ACR MRI Accreditation: Medical Physicist Role in the Application Process
 ACR MRI Accreditation: Medical Physicist Role in the Application Process Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives
ACR MRI Accreditation: Medical Physicist Role in the Application Process Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives
Biomedical Instrumentation
 Biomedical Instrumentation BME 523 (Fall 2009) Final Project Report Deep Brain Stimulation for Movement Disorder Diseases by HAO SU Submitted to Prof. Yitzhak Mendelson Date of Submission: December 18,
Biomedical Instrumentation BME 523 (Fall 2009) Final Project Report Deep Brain Stimulation for Movement Disorder Diseases by HAO SU Submitted to Prof. Yitzhak Mendelson Date of Submission: December 18,
Deep brain stimulation
 About insertion of a deep brain stimulator The deep brain stimulator sends electrical impulses to the brain interrupting the abnormal signals that are causing the symptoms. The impulses are adjusted by
About insertion of a deep brain stimulator The deep brain stimulator sends electrical impulses to the brain interrupting the abnormal signals that are causing the symptoms. The impulses are adjusted by
Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients
 J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
Activa RC and Activa PC
 Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
NCB Proximal Humerus Plating System
 NCB Proximal Humerus Plating System Surgical Technique The right locking option for tough fractures Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
NCB Proximal Humerus Plating System Surgical Technique The right locking option for tough fractures Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
Lecture XIII. Brain Diseases I - Parkinsonism! Brain Diseases I!
 Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Efficient Feature Extraction and Classification Methods in Neural Interfaces
 Efficient Feature Extraction and Classification Methods in Neural Interfaces Azita Emami Professor of Electrical Engineering and Medical Engineering Next Generation Therapeutic Devices 2 Where We Started:
Efficient Feature Extraction and Classification Methods in Neural Interfaces Azita Emami Professor of Electrical Engineering and Medical Engineering Next Generation Therapeutic Devices 2 Where We Started:
Cochlear Implants. Medical Procedures. for MED EL Implant Systems. AW33290_2.0 (English US)
 Cochlear Implants Medical Procedures for MED EL Implant Systems AW33290_2.0 (English US) This manual provides important instructions and safety information for MED EL Implant System users who have to undergo
Cochlear Implants Medical Procedures for MED EL Implant Systems AW33290_2.0 (English US) This manual provides important instructions and safety information for MED EL Implant System users who have to undergo
Intraoperative case studies. Portable full body 32-slice CT scanner
 Intraoperative case studies Portable full body 32-slice CT scanner Point-of-care CT imaging Your multi-departmental imaging solution Orthopedic surgery Arthroplasty Musculoskeletal disorders Hip replacement
Intraoperative case studies Portable full body 32-slice CT scanner Point-of-care CT imaging Your multi-departmental imaging solution Orthopedic surgery Arthroplasty Musculoskeletal disorders Hip replacement
Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years
 ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
Unrivaled, End-to-End
 PHANTOMS Unrivaled, End-to-End Stereotactic QA Industry-leading 0.1mm accuracy minimizes errors at each link in the stereotactic quality assurance chain. Stereotactic radiosurgery (SRS) is governed by
PHANTOMS Unrivaled, End-to-End Stereotactic QA Industry-leading 0.1mm accuracy minimizes errors at each link in the stereotactic quality assurance chain. Stereotactic radiosurgery (SRS) is governed by
Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic surgery
 ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
E ssential tremor is a commonly diagnosed movement
 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici
 DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration
 doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
Quality Assurance of Ultrasound Imaging in Radiation Therapy. Zuofeng Li, D.Sc. Murty S. Goddu, Ph.D. Washington University St.
 Quality Assurance of Ultrasound Imaging in Radiation Therapy Zuofeng Li, D.Sc. Murty S. Goddu, Ph.D. Washington University St. Louis, Missouri Typical Applications of Ultrasound Imaging in Radiation Therapy
Quality Assurance of Ultrasound Imaging in Radiation Therapy Zuofeng Li, D.Sc. Murty S. Goddu, Ph.D. Washington University St. Louis, Missouri Typical Applications of Ultrasound Imaging in Radiation Therapy
Basal ganglia motor circuit
 Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Deep Brain Stimulation
 Deep Brain Stimulation for Parkinson s Disease 2 Blair Ford, M.D. Associate Professor, Department of Neurology Columbia University Medical Center Scientific Editor for the Parkinson s Disease Foundation
Deep Brain Stimulation for Parkinson s Disease 2 Blair Ford, M.D. Associate Professor, Department of Neurology Columbia University Medical Center Scientific Editor for the Parkinson s Disease Foundation
Medium External Fixator Humeral Shaft Frame. Modular frame for upper extremity use.
 Medium External Fixator Humeral Shaft Frame. Modular frame for upper extremity use. Technique Guide Part of the Medium External Fixation System MRI Information Synthes Medium External Fixation devices
Medium External Fixator Humeral Shaft Frame. Modular frame for upper extremity use. Technique Guide Part of the Medium External Fixation System MRI Information Synthes Medium External Fixation devices
Cochlear Implants. Medical Procedures. for MED EL CI Systems. AW33290_5.0 (English US)
 Cochlear Implants Medical Procedures for MED EL CI Systems AW33290_5.0 (English US) This manual provides important instructions and safety information for MED EL CI System users who have to undergo a medical
Cochlear Implants Medical Procedures for MED EL CI Systems AW33290_5.0 (English US) This manual provides important instructions and safety information for MED EL CI System users who have to undergo a medical
Deep brain stimulation is a well-established procedure
 J Neurosurg 110:1283 1290, 2009 Avoiding the ventricle: a simple step to improve accuracy of anatomical targeting during deep brain stimulation Clinical article Lu d v i c Zr i n z o, M.D., M.Sc., F.R.C.S.Ed.
J Neurosurg 110:1283 1290, 2009 Avoiding the ventricle: a simple step to improve accuracy of anatomical targeting during deep brain stimulation Clinical article Lu d v i c Zr i n z o, M.D., M.Sc., F.R.C.S.Ed.
KneeAlign System Surgical Technique Guide
 KneeAlign System Surgical Technique Guide Table of Contents Step 1 System Assembly... 1 Step 2 System Assembly... 2 Step 3 System Assembly... 2 Step 4 System Assembly... 2 Step 5 Sensor Pairing... 2 Step
KneeAlign System Surgical Technique Guide Table of Contents Step 1 System Assembly... 1 Step 2 System Assembly... 2 Step 3 System Assembly... 2 Step 4 System Assembly... 2 Step 5 Sensor Pairing... 2 Step
A New Benchmark in Tibial Fixation
 PediLoc T I B I A S U R G I C A L T E C H N I Q U E A New Benchmark in Tibial Fixation Multiple plate designs for more options in osteotomies and fracture fixation Engineered from exclusive data resulting
PediLoc T I B I A S U R G I C A L T E C H N I Q U E A New Benchmark in Tibial Fixation Multiple plate designs for more options in osteotomies and fracture fixation Engineered from exclusive data resulting
ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease
 ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease Parkinson s Disease Cardinal Signs: Resting tremor Rigidity Bradykinesia Postural instability Other Symptoms Dystonia Dysphagia Autonomic
ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease Parkinson s Disease Cardinal Signs: Resting tremor Rigidity Bradykinesia Postural instability Other Symptoms Dystonia Dysphagia Autonomic
Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in
 1 Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in order to send signals into the brain to jam the abnormal
1 Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in order to send signals into the brain to jam the abnormal
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
PediLoc Tibia Surgical Technique
 PediLoc Tibia PediLoc Tibia Surgical Technique The technique description herein is made available to the healthcare professional to illustrate the author s suggested treatment for an uncomplicated procedure.
PediLoc Tibia PediLoc Tibia Surgical Technique The technique description herein is made available to the healthcare professional to illustrate the author s suggested treatment for an uncomplicated procedure.
External Distal Radius Fixator. Supplement to the 8 mm rod fixator system
 External Distal Radius Fixator. Supplement to the 8 mm rod fixator system Surgical technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation
External Distal Radius Fixator. Supplement to the 8 mm rod fixator system Surgical technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation
Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes
 Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
NewBridge. Laminoplasty Fixation INTERNATIONAL EDITION
 NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
Neurostimulation Systems
 Neurostimulation Systems Expanding the Array of Pain Control Solutions PROVEN EFFECTIVE FOR SIMPLE PAIN ITREL 3 SYSTEM For simple neuropathic pain Totally implantable for enhanced quality of life Easy
Neurostimulation Systems Expanding the Array of Pain Control Solutions PROVEN EFFECTIVE FOR SIMPLE PAIN ITREL 3 SYSTEM For simple neuropathic pain Totally implantable for enhanced quality of life Easy
chronic hyperkinetic condition of children with severe dystonia made it necessary to develop a short procedure that
 J Neurosurg 96:673 679, 2002 Comparison of atlas- and magnetic resonance imaging based stereotactic targeting of the globus pallidus internus in the performance of deep brain stimulation for treatment
J Neurosurg 96:673 679, 2002 Comparison of atlas- and magnetic resonance imaging based stereotactic targeting of the globus pallidus internus in the performance of deep brain stimulation for treatment
Lauren M. Burke, Warren D. Yu, Anthony Ho, Timothy Wagner, Joseph R. O Brien. Department of Orthopaedic Surgery George Washington University
 Lauren M. Burke, Warren D. Yu, Anthony Ho, Timothy Wagner, Joseph R. O Brien Department of Orthopaedic Surgery George Washington University O Brien: Consultant for Globus, Relivant, Stryker. Royalties:
Lauren M. Burke, Warren D. Yu, Anthony Ho, Timothy Wagner, Joseph R. O Brien Department of Orthopaedic Surgery George Washington University O Brien: Consultant for Globus, Relivant, Stryker. Royalties:
Electrical recording with micro- and macroelectrodes from the cerebellum of man
 Electrical recording with micro- and macroelectrodes from the cerebellum of man D. GRAHAM SLAUGHTER, M.D., BLAINE S. NASHOLD, Jn., M.D., AND GEORGE G. SOMJEN, M.D. The Division of Neurosurgery, and the
Electrical recording with micro- and macroelectrodes from the cerebellum of man D. GRAHAM SLAUGHTER, M.D., BLAINE S. NASHOLD, Jn., M.D., AND GEORGE G. SOMJEN, M.D. The Division of Neurosurgery, and the
Low-Profile Wrist Fixator. For stabilization of fractures of the distal radius.
 Low-Profile Wrist Fixator. For stabilization of fractures of the distal radius. Technique Guide Part of the External Fixation System Low-Profile Wrist Fixator Indications Intended for stabilization of
Low-Profile Wrist Fixator. For stabilization of fractures of the distal radius. Technique Guide Part of the External Fixation System Low-Profile Wrist Fixator Indications Intended for stabilization of
SURGICAL TECHNIQUE GUIDE TRESTLE. Anterior Cervical Plating System
 SURGICAL TECHNIQUE GUIDE TRESTLE Anterior Cervical Plating System 2 SURGICAL TECHNIQUE GUIDE SURGICAL TECHNIQUE GUIDE System Features Large window enables visualization of graft site and end plates Screw
SURGICAL TECHNIQUE GUIDE TRESTLE Anterior Cervical Plating System 2 SURGICAL TECHNIQUE GUIDE SURGICAL TECHNIQUE GUIDE System Features Large window enables visualization of graft site and end plates Screw
The American Approach to Depth Electrode Insertion December 4, 2012
 The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
1. POLICY: Magnetic Resonance Image Guided High Intensity Focused Ultrasound (MRgFUS) for Essential Tremor
 Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Positively Impacting Patient Outcomes With imri Suite
 In Practice Positively Impacting Patient Outcomes With imri Suite In Practice Something pretty amazing is happening in the middle of America s Dairyland. Neurosurgery tumor resection and deep brain stimulation
In Practice Positively Impacting Patient Outcomes With imri Suite In Practice Something pretty amazing is happening in the middle of America s Dairyland. Neurosurgery tumor resection and deep brain stimulation
Double Engine Orthopedic Bone Nail System Universal Humeral Nail
 Double Engine Orthopedic Bone Nail System ----------- Universal Humeral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic
Double Engine Orthopedic Bone Nail System ----------- Universal Humeral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic
Deep Brain Stimulation for Movement Disorders
 1 2 Deep Brain Stimulation for Movement Disorders Overview Deep brain stimulation (DBS) is a surgery to implant a device that sends electrical signals to brain areas responsible for body movement. Electrodes
1 2 Deep Brain Stimulation for Movement Disorders Overview Deep brain stimulation (DBS) is a surgery to implant a device that sends electrical signals to brain areas responsible for body movement. Electrodes
KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol
 KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol Sample referral sticker Referral Sticker Insert here Corin 17 Bridge Street Pymble NSW Australia 2073 P: +61 (0)2 9497 7400 F: +61 (0)2 9497 7498 E: KAS.customerservice@coringroup.com
KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol Sample referral sticker Referral Sticker Insert here Corin 17 Bridge Street Pymble NSW Australia 2073 P: +61 (0)2 9497 7400 F: +61 (0)2 9497 7498 E: KAS.customerservice@coringroup.com
QUICK REFERENCE GUIDE. The PreFix Fixator (92000 Series) ALWAYS INNOVATING
 21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
A Patient s Guide to SRS
 A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
AcUMEDr. Locking Proximal Humeral Plate. PoLARUSr PHPt
 AcUMEDr Locking Proximal Humeral Plate PoLARUSr PHPt PoLARUSr PHPt LOCKING PROXIMAL HUMERAL PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons,
AcUMEDr Locking Proximal Humeral Plate PoLARUSr PHPt PoLARUSr PHPt LOCKING PROXIMAL HUMERAL PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons,
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
TABLE OF CONTENTS. 2 (8144 Rev 2)
 1 (8144 Rev 2) TABLE OF CONTENTS Introduction Conventus CAGE TM - Proximal Humerus...3 Indications and Contraindications...4 Surgical Summary...5 Patient Positioning & Approach...6 Surgical Technique Plate
1 (8144 Rev 2) TABLE OF CONTENTS Introduction Conventus CAGE TM - Proximal Humerus...3 Indications and Contraindications...4 Surgical Summary...5 Patient Positioning & Approach...6 Surgical Technique Plate
