Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration
|
|
|
- Vivian Gilbert
- 5 years ago
- Views:
Transcription
1 doi: /brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and Michele Tagliati 1 1 Department of Neurology and 2 Department of Neurosurgery, Mount Sinai School of Medicine, New York, NY 10029, USA Correspondence to: Michele Tagliati, MD, Associate Professor of Neurology, Mount Sinai School of Medicine, 5 East 98th Street,Box1139,NewYork,NY10029,USA michele.tagliati@mssm.edu Pallidal deep brain stimulation (DBS) is currently the most effective treatment for advanced, medically refractory dystonia. However, factors predicting clinical outcome are not well defined.we reviewed the clinical records of 39 consecutive patients with medically refractory primary dystonia who underwent pallidal DBS implants. Thirty-five patients were implanted bilaterally and four unilaterally. Seven patients had fixed skeletal deformities (FSD). The Burke-Fahn-Marsden Dystonia Rating Scale (BFMDRS) scores at baseline, 3 and 12 months after DBS were used to evaluate clinical outcome.we investigated the outcome predictive role of several demographic and clinical factors. FSD patients had a significantly inferior outcome at 12 months, mostly affected by axial scores. All other patients (n = 32) showed a remarkable improvement (median BFMDRS percentage improvement = 87.8). Only disease duration showed a significant correlation with DBS outcome at 3 and 12 months. No other demographic and baseline clinical features predicted DBS outcome. This study confirms that patients with primary, medically refractory dystonia are generally outstanding candidates for pallidal DBS, with the possible exception of axial FSD. Patients with shorter duration of disease may expect a better general outcome. No particular predictive value should be assigned to age at onset, age at surgery, severity of disease, DYT1 status and the presence of phasic or tonic involuntary movements. Keywords: deep brain stimulation; globus pallidus; dystonia; outcome predictors; disease duration Abbreviations: BFMDRS = Burke-Fahn-Marsden Dystonia Rating Scale; DBS = deep brain stimulation; FSD = fixed skeletal deformities Received March 12, Revised April 29, Accepted May 15, Advance Access publication June 20, 2008 Introduction Dystonia is a movement disorder characterized by patterned, directional and often sustained muscle contractions that produce abnormal postures or repetitive movements (Tarsy and Simon, 2006). Primary dystonias are by definition unaccompanied by other neurological abnormalities and have no known cause, aside from a few genetic mutations identified to date (Geyer and Bressman, 2006). With the notable exception of dopa-responsive dystonia, pharmacological treatment of primary generalized dystonia is mostly unsatisfactory. As a consequence, surgical attempts to relieve dystonic spasm have targeted both peripheral and CNS structures (Tagliati et al., 2003). Chronic stimulation of the globus pallidus internus is a safe and effective treatment for advanced, disabling dystonia (Vidailhet et al., 2005; Kupsch et al., 2006). Despite these successful results, the indications of pallidal stimulation for dystonia remain highly empirical. Current experience suggests that primary dystonias respond better than most secondary dystonias (Tagliati et al., 2004), and patients carrying the DYT1 mutation have been reported to be particularly good candidates for this procedure (Coubes et al., 2000; Tagliati et al., 2004). To add uncertainty to patient selection for deep brain stimulation (DBS) in dystonia, the clinical outcome predictors are still poorly defined. The influence on DBS results of factors like age, disease duration and severity, symptom distribution and history of ablative procedures has not been accurately evaluated, due in part to the relatively small size and variable clinical presentation of the studied cohorts. In order to better define demographic and clinical outcome predictors of pallidal stimulation for primary dystonia, large and homogeneous study populations are needed. To this purpose, we reviewed DBS results obtained ß The Author (2008). Published by Oxford University Press on behalf ofthe Guarantors of Brain. Allrights reserved. For Permissions, please journals.permissions@oxfordjournals.org
2 1896 Brain (2008), 131,1895^1902 I.U.Isaiaset al. in a large cohort of primary dystonia patients implanted by the same neurosurgeon (R.L.A.) and followed almost exclusively by the same neurologist (M.T.). Methods Subjects Thirty-nine consecutive patients with medically refractory primary dystonia who underwent stereotactic pallidal DBS surgery between December 2000 and January 2007 were included in the study. Similar to previous series (Vidailhet et al., 2005), patients were diagnosed with primary dystonia if they: (i) exhibited a normal neurological examination except for dystonia; (ii) lacked a history of known aetiologies of dystonia such as static encephalopathy, head trauma, ischaemic insults, meningitis/encephalitis and neuroleptic treatments and (iii) had an anatomically normal brain MRI. DBS surgery was offered if they suffered with severe disability despite optimal medical management. Patients with untreated psychiatric disturbances or cognitive dysfunction were not offered surgery. Patients with secondary dystonia or history of prior central ablative procedures (i.e. thalamotomy/pallidotomy) were excluded from this study. Thirty-five patients had early-onset dystonia (526 years) (Geyer and Bressman, 2006). Twenty-five tested positive for the DYT1 gene defect. Thirty-five were implanted bilaterally; four were treated unilaterally based on the anatomical distribution of their symptoms. Seven patients had fixed skeletal deformities (FSD), in all cases scoliosis, at the time of surgery. This group was analysed separately and compared to the rest of the cohort. Table 1 summarizes the demographical characteristics of the two subgroups (i.e. those with and without FSD) in our study. Clinical evaluation and outcomes measures We reviewed retrospectively the clinical records of all 39 subjects, including videotaped evaluations, with the approval of the Mount Sinai School of Medicine (MSSM) Institutional Review Board (IRB # ). The severity of dystonia was evaluated at baseline (2 weeks before surgery) and 3 and 12 months postoperatively using the Burke-Fahn- Marsden Dystonia Rating Scale (BFMDRS) (Burke et al., 1985). Postoperatively, patients were evaluated only while actively stimulated. Results were normalized by calculating the percentage change of the BFMDRS according to the formula: Baseline BFMDRS score Postoperative BFMDRS score 100 Baseline BFMDRS score Medications taken into account were: dopaminergic drugs (levodopa, dopamine agonists), anticholinergics, antispasmodic drugs (baclofen) and benzodiazepines. Twelve patients were receiving botulinum toxin injections before surgery. Injections were suspended during the first 12 months of stimulation. In addition to the BFMDRS scores, we also recorded the presence of phasic movements and/or tonic posturing in each body segment. A body segment that exhibited rapid, repetitive movements was categorized as phasic ; a segment exhibiting sustained contractions and abnormal postures was categorized as tonic (Ahlskog et al., 2000). We reserved the term fixed for chronic dystonic contractions associated with tendonous or skeletal deformities. Patients were then divided into predominantly phasic or predominantly tonic groups based on the number of body segments exhibiting those respective symptom subtypes. In order to determine preoperative predictors of response to pallidal DBS, we analysed the correlation of the postoperative percent change in the BFMDRS with several demographic (age at surgery, gender) and clinical features at baseline. The clinical features examined included age at onset of dystonia, disease duration, presence of the DYT1 gene mutation, presence/absence of skeletal deformities, degree of motor disability and predominance of axial symptoms. Neurosurgical procedure and DBS programming All subjects included in this study underwent microelectrode-guided, frame-based stereotactic implantation of DBS leads (model 3387, Medtronic) by one surgeon (R.L.A.), as described previously (Shils et al., 2002; Alterman et al., 2007). Postoperative brain MRI was routinely performed to confirm placement of the leads in the posteroventral globus pallidus internus. In accordance with the United States Food and Drug Administration Humanitarian Device Exemption regulating the use of DBS for dystonia (HDE# H020007), starting in 2004 patients were operated upon with the approval of either the Beth Israel Medical Center, NY (April September 2004) or the MSSM IRB (February 2005 to January 2007). Device programming was conducted in a standardized fashion. As previously published (Alterman et al., 2007), we systematically analysed the four available contacts on each lead in monopolar configuration in order to map clinical responses (when present) and the tolerability of stimulation. Ventral contacts (0 and 1) were preferentially, Table 1 Demographic characteristics of the two subgroups of patients included in the study N Sex (M/F) Age at onset Age at surgery Disease duration DYT1+ (n) FSD 7 6/ (6^19) (15^ 63) (7^ 44) 3 PTD 32 20/ (3^50) (10 ^58) (1^ 40) 22 FSD = fixed skeletal deformities; PTD = primary torsion dystonia without FSD. Data are reported as Mean SD (range) unless otherwise specified.
3 Outcome predictors of DBS for dystonia Brain (2008), 131,1895^ but not exclusively, used for initial therapy. Adjustments were performed thereafter in order to maximize clinical benefit and/or reduce adverse effects (Kumar, 2002). Statistical analysis Statistical analyses were performed with the JMP Õ statistical package, version 5.1 (SAS Institute, Inc., Cary, NC, USA). ChiSquare was used to test demographic homogeneity among groups regarding gender and DYT1 status. Average BFMDRS percentage improvement of the FSD group was compared with the rest of the sample by means of Wilcoxon tests. To look for factors that were predictive of improvement both at 3 and at 12 months, we used the Spearman correlation coefficient for quantitative variables (age at onset, age at surgery, disease duration and total scores or subscores for the movement and disability scales) and the Wilcoxon test for categorical variables (gender, skeletal deformities, DYT1 status, phasic/tonic dystonia predominance). Variables relating to improvement after surgery were included in stepwise multiple linear regression. Statistical tests were two-tailed and P50.05 was considered to be statistically significant. Results The baseline clinical characteristics of the study cohort are summarized in Tables 2 and 3. The cohort had homogeneous features, with the exception of FSD patients, who exhibited higher axial scores at baseline (mean SD; versus , P50.05). No other clinical or demographic differences at baseline were found between patient groups. Following surgery and device activation, every patient experienced a progressive improvement in motor function, which is reflected in their BFMDRS motor and disability score percentage changes (Table 2). Dystonic patients with FSD had a significantly poorer outcomes at 12 months (P50.01; Fig. 1). This was due to the poor resolution of limb and particularly axial symptoms (Table 3). Therefore, we excluded this subgroup of patients from further outcome analysis, focusing on the remaining 32 patients without FSD. Among demographic features, only the patient s age at surgery correlated with clinical outcome at 3 and 12 months (P50.01). Patients older than 21 years at surgery (n = 17) improved, on average, 38 percentage points less than patients younger than 21 (n = 15) 3 months after surgery (P50.01) and 15 percentage points less at 1 year (P50.01). Total and segmental BFMDRS scores at baseline, 3 and 12 months after surgery are listed in Tables 2 and 3. There was no correlation between BFMDRS score or segmental subscores at baseline and DBS outcomes at 3 months and 12 months. Among clinical variables, only disease duration significatively correlated with clinical outcome at 3(P50.01) and 12 months (P50.05). In addition, disease duration also showed a significant negative correlation with disability scores at 12 months (P50.05, Spearman test). Patients with disease duration longer than 15 years (n = 12) improved 49% less than patients with shorter disease duration (n = 20) at 3 months (P50.001) and 13% less at 1 year (P50.05; Fig. 2A and B). As disease duration and age at surgery are related, we used multiple regression analysis to identify, which factor had a stronger predictive value. Disease duration was the only resulting independent variable correlated with DBS outcome (P50.001; Fig. 2C). DYT1-positive patients (n = 22) were, on average, younger at symptom onset ( years versus , P50.01) and younger at surgery ( years versus , P50.01) than DYT1-negative patients (n = 10). There were no other significant differences in the demographic or baseline clinical characteristics of these two groups, with the exception of a higher prevalence of speech and swallowing involvement in DYT1-negative subjects (7/10 versus 7/22; P50.05). DYT1-positive patients exhibited a greater BFMDRS percentage improvement both at 3 months ( versus , P50.05) and 1-year ( versus , P50.05; Fig. 3A and B) after surgery. However, when patients were stratified by disease duration, this difference was lost (Fig. 3C F). Seven patients presented with predominantly phasic symptoms; 25 had predominantly tonic dystonia. We found no outcome disparity between phasic predominant and tonic predominant patients at either 3 or 12 months of follow-up. Twenty-six subjects (81%) were taking one or more medications before surgery. In addition, one patient had a functioning baclofen pump (which was explanted after surgery). One year after surgery, nine patients (28%) had completely discontinued medications. No demographical or baseline clinical features predicted medication reduction or their discontinuation. Stimulation settings at 12 months were grossly similar to those used at 3 months of follow up. We predominantly used a monopolar configuration both at 3 (68/74 leads; 33 single, 35 double) and 12 months (67/74 leads; 19 single, 44 double, 4 triple); the rest of the electrodes were set at a bipolar configuration (one simple bipolar and five tripolar at 3 months; two simple bipolar, five tripolar at 12 months). At 3 months, mean voltage was 2.8 V (0.4 SD), mean pulse width was ms (71.6 SD) and mean frequency was 82.7 (32.2 SD). At 12 months, mean voltage was 3.0V (0.4 SD), mean pulse width was ms (72.0 SD) and mean frequency was 76.9 Hz (26.9 SD). There were no intraoperative haemorrhages and no adverse neurological sequelae were observed. Nine patients experienced adverse events including five device infections (two of these in the same patient); in each case, the infected device components were removed and re-implanted following an appropriate course of intravenous antibiotics. There were two extension cable fractures, one scalp erosion
4 Table 2 Clinical features at baseline and at 3 and 12 months post-dbs BFMDRS total score % BFMDRS improvement % drugs reduction Disability score Baseline 3 months 12 months 3 months 12 months 3 months 12 months Baseline 3 months 12 months FSD (28^77) (8.5^39) (11^36) (37^70) # (50 ^76) (0 ^ 67) (0^92.5) (3^21) (2^10) (3^13) PTD (9^81.5) (0^56.5) (0^21) (0^100) (50 ^100) (0^100) (0^100) (3^24) (1^16) (0^10) FSD = fixed skeletal deformities; PTD = primary torsion dystonia without FSD. Data are reported as Mean SD (range). The total score for the movement subscale of the Burke-Fahn- Marsden Dystonia Rating Scale (BFMDRS), which can range from 0 to 120, is the sum of individual scores of nine body regions and represents the severity of motor disability related to dystonia. The total disability score can range from 0 to 30 and is the sum of individual ratings for seven activities: speech, handwriting, and the degree of dependence with respect to hygiene, dressing and feeding, swallowing and walking. A high score indicates worse disability. P50.05; P50.01; # P Table 3 BFMDRS sub-scores at baseline, 3 and 12 months Face Speech and Swallowing Axial Limbs Baseline 3 months 12 months Baseline 3 months 12 months Baseline 3 months 12 months Baseline 3 months 12 months FSD (n =3) (n =7) (n =7) # (n = 7) PTD (n = 11) (n = 14) (n = 25) (n =32) FSD = fixed skeletal deformities; PTD = primary torsion dystonia without FSD. Data are reported as Mean SD (no. of patients with symptoms). P50.05; P50.01; # P Brain (2008), 131,1895^1902 I.U.Isaiaset al. Downloaded from at Pennsylvania State University on March 4, 2014
5 Outcome predictors of DBS for dystonia Brain (2008), 131,1895^ Fig. 1 (A) Average Burke-Fahn-Marsden Dystonia Rating Scale (BFMDRS) percentage change at 3 and 12 months after surgery. FSD = fixed skeletal deformities; PTD = Primary torsion dystonia without skeletal deformities. Patients with FSD had a significantly pooreroutcomeat12monthsfollow-up( P50.05). (B) Average BFMDRS motor subscores percentage change at 12 months follow-up. Results in patients with FSD (gray bars) were limited by comparatively poorer outcome in axial ( P50.01) and limbs subscores ( P50.05). Error bars = Standard error. without infection and three lead revisions. In all cases there were no long-term neurological repercussions. There were no complications related to revision surgery. Discussion This retrospective study confirms previous reports showing that pallidal DBS is a safe and effective therapy for medication refractory primary dystonia (Yianni et al., 2003; Coubes et al., 2004; Vidailhet et al., 2005, 2007; Kupsch et al., 2006; Alterman et al., 2007). Patients without FSD showed a remarkable 85% average improvement in their BFMDRS scores, which is higher than that reported by others (Yianni et al., 2003; Vidailhet et al., 2005; Kupsch et al., 2006). This may due to the fact that our population had much shorter disease duration than did patients in these other studies, a clinical factor that appears to be significantly correlated to DBS outcome. Patients with FSD showed a relatively poorer outcomes 12 months after surgery (61%), as their results were negatively weighed by Fig. 2 Effect of disease duration on Burke-Fahn-Marsden Dystonia Rating Scale (BFMDRS) percentage improvement in 32 patients with primary dystonia without skeletal deformities. Patients with disease duration longer than 15 years (n =12) improved significantly less than patients with shorter disease duration (n = 20) both at 3 months (2a, P50.001) and at 1-year follow-up (2b, P50.05). Disease duration was the only independent factor significantly correlated with DBS outcome at one-year follow up (2c; r 2 =0.32,P50.01). the axial BFMDRS subscores, whose improvement was limited to 40%. Despite the consistent positive results reported with surgical therapy for torsion dystonia, surgical outcome
6 1900 Brain (2008), 131,1895^1902 I.U.Isaiaset al. Fig. 3 Boxplot distribution of Burke-Fahn-Marsden Dystonia Rating Scale (BFMDRS) percentage improvements at 3 months (A, C, E) and 12 months (B, D, F) for DYT1-positive(n = 22) and negative subjects (n = 10) without fixed skeletal deformities. DYT1-positive subjects showed significantly better outcomes than DYT1-negative subjects at 3 months (A) and1year(b) afterpallidaldbs( P50.05). However, this difference became less prominent and lost statistical significance when subjects were stratified by disease duration. Results observed in subjects with less than 15 years disease duration are displayed in boxplot C (3 months follow-up) and D (1 year follow-up). Results observed in subjects with more than 15 years disease duration are displayed in boxplot E (3 months follow-up) and F (1 year follow-up). BFMDRS percentage improvement was consistently lower in subjects with longer duration of disease independent of DTY1 status. In each figure the horizontal line represents the grand mean of the population. FSD = fixed skeletal deformities. predictors have been addressed sparingly. When thalamotomy was the preferred surgical treatment (Cooper, 1976; Tasker et al., 1988), the best results were reported in patients with idiopathic disease, predominant distal limbs involvement and little or no axial dystonia (Cooper, 1976; Tasker et al., 1988). The more contemporary literature regarding DBS initially suggested that the DYT1 gene mutation is a positive outcome predictor (Coubes et al., 2000, 2004;
7 Outcome predictors of DBS for dystonia Brain (2008), 131, 1895^ Yianni et al., 2003). However, two prospective studies failed to associate pallidal DBS results with any pre-surgical variable, except possibly the presence of phasic or hyperkinetic movements (Vidailhet et al., 2005, 2007; Kupsch et al., 2006). The most remarkable result emerging from our study is the negative influence of disease duration on outcome. In particular, disease duration longer than 15 years seems to strongly predict a slower improvement and overall worse (though still satisfactory) DBS outcome. A negative influence of disease duration was previously suggested, but not clearly demonstrated possibly because of the variable clinical background of the cohort (Yianni et al., 2003). Other studies failed to find a correlation between duration of disease and outcome, in one case possibly due to selection criteria that specifically excluded patients with short disease durations (Kupsch et al., 2006), and in another to the relatively advanced median age of the study population (Vidailhet et al., 2005). The predictive role of disease duration is of particular interest in light of current models proposing that the therapeutic effect of DBS is mediated by a gradual brain reorganization or plasticity (Vitek, 2002; Detante et al., 2004; Krauss et al., 2004; Tisch et al., 2007). It is tempting to speculate that the severity of aberrant plasticity in dystonia may be correlated with disease duration, making complete resolution of symptoms by DBS more difficult the more longstanding the aberrancy. Neither age at surgery nor severity of disease correlated with clinical outcome in our cohort. While we confirmed the particularly favourable DBS results previously described in younger patients (Coubes et al., 2004; Alterman et al., 2007), multiple regression analysis showed that age at surgery served merely as a proxy for disease duration. The fact that disease severity at baseline, as measured by the BFMDRS, did not correlate with clinical outcome, suggests that patients with disabling, medically refractory, primary dystonia should be evaluated for DBS regardless of their baseline BFMDRS scores. Patients carrying the DYT-1 gene mutation were significantly younger at surgery and showed higher percentage improvement than those with sporadic primary dystonia at both the 3 and 12 month follow-ups. The faster improvement seems clinically most relevant, with DYT1- positive improving an average 53 percentage points more than DYT1-negative patients at 3 months, but only 13 percentage points more at 12 months. Nevertheless, this apparent difference in response was lost when the groups were stratified by disease duration. Therefore, it appears that the younger age and shorter disease duration of DYT1-positive patients at the time of surgery may have contributed to the widely held impression that DYT1- positive subjects respond best to pallidal DBS (Coubes et al., 2000; Yianni et al., 2003; Tagliati et al., 2004). There were no significant differences in clinical outcome between patients with predominantly tonic (or sustained) versus phasic dystonia, another clinical feature previously suggested as a possible outcome predictor for pallidal DBS (Vercueil et al., 2001, Volkmann and Benecke, 2002; Kupsch et al., 2003, 2006; Tagliati et al., 2004; Vidailhet et al., 2005;Wang et al., 2006). The discrepancy of our results with those reported in the literature may stem from two factors. First, patients with phasic movements have been noted to improve faster (in the order of minutes or hours) than patients with tonic symptoms (Volkmann and Benecke, 2002; Krauss et al., 2004; Vidailhet et al., 2005; Hung et al., 2007), a difference that would not have been captured at 3 months follow-up. Second, our exclusion from analysis of patients with FSD may have eliminated patients who would otherwise have been classified as predominantly tonic and would have probably resulted in our confirming these previous findings. Consequently, we propose that no particular long-term predictive value should be associated with phasic or tonic dystonia, unless fixed contractures or skeletal deformities are present. Of course, such secondary orthopaedic changes are more likely with longer disease duration. While patients with FSD showed poorer outcomes 12 months after surgery than those without, they still may benefit significantly from pallidal DBS. Indeed, some of these patients showed further improvement when skeletal deformities were surgically corrected. In conclusion, we confirm that patients with primary, medically refractory dystonia are generally outstanding candidates for pallidal DBS. Our results suggest that DBS for primary dystonia should be entertained before the occurrence of fixed contractures or axial deformities. Patients with disease duration shorter than 15 years may expect to improve faster and achieve a better general outcome than those with longer disease duration. We find no particular predictive value of age at onset of dystonia, severity of disease at baseline, DYT1 status or phasic/tonic predominance of dystonic symptoms. Acknowledgements The authors thank Drs Michael Okun and Edward Drasby for follow-up evaluations of three patients living in another state. They also would like to thank Adam Koss for his critical reading of the manuscript. The study was funded in part by a grant of the Bachmann-Strauss Foundation for Dystonia and Parkinson s disease. Drs M.T. and R.A. received speaking honoraria and consulting fees from Medtronic Inc., not related to the conduction of this study. References Ahlskog JE. Approach to the patients with a movement disorder: basic principles of neurologic diagnosis. In: Adler CH, Ahlskog JE, editors. Parkinson s disease and movement disorders: diagnosis and treatment. Totowa, NJ: Humana Press; p Alterman RL, Miravite J, Weiss D, Shils JL, Bressman SB, Tagliati M. Sixty hertz pallidal deep brain stimulation for primary torsion dystonia. Neurology 2007; 69: Burke RE, Fahn S, Marsden CD, Bressman SB, Moskowitz C, Friedman J. Validity and reliability of a rating scale for the primary torsion dystonia. Neurology 1985; 35: 73 7.
8 1902 Brain (2008), 131,1895^1902 I.U.Isaiaset al. Cooper IS. 20-year follow up of the neurosurgical treatment of dystonia musculorum deformans. Adv Neurol 1976; 14: Coubes P, Cif L, El Fertit H, Hemm S, Vayssiere N, Serrat S, et al. Electrical stimulation of the globus pallidus internus in patients with primary generalized dystonia: long-term results. J Neurosurg 2004; 101: Coubes P, Roubertie A, Vayssiere N, Hemm S, Echenne B. Treatment of DYT1-generalised dystonia by stimulation of the internal globus pallidus. Lancet 2000; 355: Detante O, Vercueil L, Thobois S, Broussolle E, Costes N, Lavenne F, et al. Globus pallidus internus stimulation in primary generalized dystonia: a H2 15O PET study. Brain 2004; 127: Geyer HL, Bressman SB. The diagnosis of dystonia. Lancet Neurol 2006; 5: Hung SW, Hamani C, Lozano AM, Poon YY, Piboolnurak P, Miyasaki JM, et al. Long-term outcome of bilateral pallidal deep brain stimulation for primary cervical dystonia. Neurology 2007; 68: Krauss JK, Yianni J, Loher JT, Aziz TZ. Deep brain stimulation for dystonia. J Clin Neurophysiol 2004; 21: Kumar R. Methods for programming and patient management with deep brain stimulation of the globus pallidus for the treatment of advanced Parkinson s disease and dystonia. Mov Disord 2002; 17 (Suppl 3): S Kupsch A, Benecke R, Müller J, Trottenberg T, Schneider GH, Poewe W, et al. Pallidal deep-brain stimulation in primary generalized or segmental dystonia. N Engl J Med 2006; 355: Kupsch A, Kuehn A, Klaffke S, Meissner W, Harnack D, Winter C, et al. Deep brain stimulation in dystonia. J Neurol 2003; 250: Shils J, Tagliati M, Alterman R. Neurophysiological monitoring during neurosurgery for movement disorders. In: Deletis V, Shils J, editors. Neurophysiology in neurosurgery. San Diego: Academic Press; p Tagliati M, Blatt K, Bressman S. Generalized Torsion Dystonia. In: Noseworthy J, editor. Neurological therapeutics: principles and practice. Chapter 237. London: Martin Dunitz, Ltd; Tagliati M, Shils J, Sun C, Alterman R. Deep brain stimulation for dystonia. Expert Rev Med Devices 2004; 1: Tarsy D, Simon DK. Dystonia. N Engl J Med 2006; 355: Tasker RR, Doorly T, Yamashiro K. Thalamotomy in generalized dystonia. Adv Neurol 1988; 50: Tisch S, Rothwell JC, Limousin P, Hariz MI, Corcos DM. The physiological effects of pallidal deep brain stimulation in dystonia. IEEE Trans Neural Syst Rehabil Eng 2007; 15: Vercueil L, Pollak P, Fraix V, Caputo E, Moro E, Benazzouz A, et al. Deep brain stimulation in the treatment of severe dystonia. J Neurol 2001; 248: Vidailhet M, Vercueil L, Houeto JL, Krystkowiak P, Benabid AL, Cornu P, et al. Bilateral deep-brain stimulation of the Globus Pallidus in primary generalized dystonia. N Engl J Med 2005; 352: Vidailhet M, Vercueil L, Houeto JL, Krystkowiak P, Lagrange C, Yelnik J, et al. Bilateral, pallidal, deep-brain stimulation in primary generalized dystonia: a prospective 3 year follow-up study. Lancet Neurol 2007; 6: Vitek JL. Pathophysiology of dystonia: a neuronal model. Mov Disord 2002; 17: Volkmann J, Benecke R. Deep brain stimulation for dystonia: a patients selection and evaluation. Mov Disord 2002; 17: Wang S, Liu X, Yianni J, Green AL, Joint C, Stein JF, et al. Use of surface electromyography to assess and select patients with idiopathic dystonia for bilateral pallidal stimulation. J Neurosurg 2006; 105: Yianni J, Bain P, Giladi N, Auca M, Gregory R, Joint C, et al. Globus pallidus internus deep brain stimulation for dystonic conditions: a prospective audit. Mov Disord 2003; 18:
Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech?
 Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Review Article Dystonia and the Role of Deep Brain Stimulation
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia
 original article Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia Marie Vidailhet, M.D., Ph.D., Laurent Vercueil, M.D., Jean-Luc Houeto, M.D., Ph.D., Pierre Krystkowiak,
original article Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia Marie Vidailhet, M.D., Ph.D., Laurent Vercueil, M.D., Jean-Luc Houeto, M.D., Ph.D., Pierre Krystkowiak,
ORIGINAL CONTRIBUTION. Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia
 ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging
 J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years
 ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
Bilateral, pallidal, deep-brain stimulation in primary generalised dystonia: a prospective 3 year follow-up study
 Bilateral, pallidal, deep-brain stimulation in primary generalised dystonia: a prospective 3 year follow-up study Marie Vidailhet, Laurent Vercueil, Jean-Luc Houeto, Pierre Krystkowiak, Christelle Lagrange,
Bilateral, pallidal, deep-brain stimulation in primary generalised dystonia: a prospective 3 year follow-up study Marie Vidailhet, Laurent Vercueil, Jean-Luc Houeto, Pierre Krystkowiak, Christelle Lagrange,
P rimary generalised dystonia (PGD) is a movement disorder
 1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
Citation for published version (APA): Contarino, M. F. (2013). Improving surgical treatment for movement disorders
 UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
Deep brain stimulation in the treatment of dyskinesia and dystonia
 Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
The Canadian multicentre study of deep brain stimulation for cervical dystonia
 doi:10.1093/brain/awm229 The Canadian multicentre study of deep brain stimulation for cervical dystonia Brain (2007), 130, 2879^2886 Zelma H. T. Kiss, 1 Kristina Doig-Beyaert, 1 Michael Eliasziw, 1,2 Joseph
doi:10.1093/brain/awm229 The Canadian multicentre study of deep brain stimulation for cervical dystonia Brain (2007), 130, 2879^2886 Zelma H. T. Kiss, 1 Kristina Doig-Beyaert, 1 Michael Eliasziw, 1,2 Joseph
No Financial Disclosures
 Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in
 1 Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in order to send signals into the brain to jam the abnormal
1 Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in order to send signals into the brain to jam the abnormal
The Canadian multicentre study of deep brain stimulation for cervical dystonia
 Brain Advance Access published September 28, 2007 doi:10.1093/brain/awm229 Brain (2007) Page 1 of 8 The Canadian multicentre study of deep brain stimulation for cervical dystonia Zelma H. T. Kiss, 1 Kristina
Brain Advance Access published September 28, 2007 doi:10.1093/brain/awm229 Brain (2007) Page 1 of 8 The Canadian multicentre study of deep brain stimulation for cervical dystonia Zelma H. T. Kiss, 1 Kristina
Treatment of Dystonia with Deep Brain Stimulation
 Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Treatment of Dystonia with Deep Brain Stimulation Jill L. Ostrem* and Philip A. Starr *Department of Neurology,
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Treatment of Dystonia with Deep Brain Stimulation Jill L. Ostrem* and Philip A. Starr *Department of Neurology,
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Deep brain stimulation: What can patients expect from it?
 MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
SUPPLEMENTAL DIGITAL CONTENT
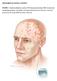 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
doi: /brain/awt009 Brain 2013: 136; Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years
 doi:10.1093/brain/awt009 Brain 2013: 136; 761 769 761 BRAIN A JOURNAL OF NEUROLOGY Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years Richard A. Walsh, 1,2
doi:10.1093/brain/awt009 Brain 2013: 136; 761 769 761 BRAIN A JOURNAL OF NEUROLOGY Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years Richard A. Walsh, 1,2
Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life
 J Neurosurg 107:29 36, 2007 Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life GALIT KLEINER-FISMAN, M.D., 1 GRACE
J Neurosurg 107:29 36, 2007 Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life GALIT KLEINER-FISMAN, M.D., 1 GRACE
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Parkinson's Disease Center and Movement Disorders Clinic
 Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
Deep brain stimulation for dystonia
 Hu and Stead Translational Neurodegeneration 2014, 3:2 Translational Neurodegeneration REVIEW Deep brain stimulation for dystonia Wei Hu * and Matt Stead * Open Access Abstract Deep brain stimulation (DBS)
Hu and Stead Translational Neurodegeneration 2014, 3:2 Translational Neurodegeneration REVIEW Deep brain stimulation for dystonia Wei Hu * and Matt Stead * Open Access Abstract Deep brain stimulation (DBS)
10/13/2017. Disclosures. Deep Brain Stimulation in the Treatment of Movement Disorders. Deep Brain Stimulation: Objectives.
 Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
The phenomenology and treatment of idiopathic adult-onset truncal dystonia: a retrospective review
 Ehrlich and Frucht Journal of Clinical Movement Disorders (2016) 3:15 DOI 10.1186/s40734-016-0044-9 RESEARCH ARTICLE Open Access The phenomenology and treatment of idiopathic adult-onset truncal dystonia:
Ehrlich and Frucht Journal of Clinical Movement Disorders (2016) 3:15 DOI 10.1186/s40734-016-0044-9 RESEARCH ARTICLE Open Access The phenomenology and treatment of idiopathic adult-onset truncal dystonia:
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici
 DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
Globus pallidus internus stimulation in primary generalized dystonia: a H 2 15 O PET study
 DOI: 10.1093/brain/awh213 Brain (2004), 127, 1899 1908 Globus pallidus internus stimulation in primary generalized dystonia: a H 2 15 O PET study Olivier Detante, 1,3 Laurent Vercueil, 1 Stéphane Thobois,
DOI: 10.1093/brain/awh213 Brain (2004), 127, 1899 1908 Globus pallidus internus stimulation in primary generalized dystonia: a H 2 15 O PET study Olivier Detante, 1,3 Laurent Vercueil, 1 Stéphane Thobois,
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Dystonia. The condition can vary from very mild to severe. Dystonia may get worse over time or it may stay the same or get better.
 Dystonia What are movement disorders? Movement disorders are conditions that cause involuntary body movements. With all movement disorders, abnormal signals from the brain cause patients to have trouble
Dystonia What are movement disorders? Movement disorders are conditions that cause involuntary body movements. With all movement disorders, abnormal signals from the brain cause patients to have trouble
Pallidal Deep-Brain Stimulation in Primary Generalized or Segmental Dystonia
 The new england journal of medicine original article Pallidal Deep-Brain Stimulation in Primary Generalized or Segmental Dystonia Andreas Kupsch, M.D., Reiner Benecke, M.D., Jörg Müller, M.D., Thomas Trottenberg,
The new england journal of medicine original article Pallidal Deep-Brain Stimulation in Primary Generalized or Segmental Dystonia Andreas Kupsch, M.D., Reiner Benecke, M.D., Jörg Müller, M.D., Thomas Trottenberg,
I n 1991 Benabid et al introduced deep brain stimulation
 PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
Troubleshooting algorithms for common DBS related problems in tremor and dystonia
 Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep brain stimulation for camptocormia in dystonia and Parkinson s disease
 J Neurol (2011) 258:96 103 DOI 10.1007/s00415-010-5695-0 ORIGINAL COMMUNICATION Deep brain stimulation for camptocormia in dystonia and Parkinson s disease Hans-Holger Capelle Christoph Schrader Christian
J Neurol (2011) 258:96 103 DOI 10.1007/s00415-010-5695-0 ORIGINAL COMMUNICATION Deep brain stimulation for camptocormia in dystonia and Parkinson s disease Hans-Holger Capelle Christoph Schrader Christian
Dystonia is characterized by sustained muscle
 This article has been updated from its originally published version to replace Figure 2 and update the legend. See the corresponding erratum notice, DOI: 10.3171/10.3171/ 2013.11.JNS13844a, for full details.
This article has been updated from its originally published version to replace Figure 2 and update the legend. See the corresponding erratum notice, DOI: 10.3171/10.3171/ 2013.11.JNS13844a, for full details.
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
Pallidal Deep Brain Stimulation
 Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak, MD, PhD D.
 ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
Changes in Cortical and Pallidal Oscillatory Activity during the Execution of a Sensory Trick in Patients with Cervical Dystonia
 Changes in Cortical and Pallidal Oscillatory Activity during the Execution of a Sensory Trick in Patients with Cervical Dystonia Joyce KH Tang 1 Neil Mahant 2 Danny Cunic 2 Robert Chen 2 Elena Moro 2 Anthony
Changes in Cortical and Pallidal Oscillatory Activity during the Execution of a Sensory Trick in Patients with Cervical Dystonia Joyce KH Tang 1 Neil Mahant 2 Danny Cunic 2 Robert Chen 2 Elena Moro 2 Anthony
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
Deep brain stimulation (DBS) has been
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
Which patients with dystonia benefit from deep brain stimulation? A metaregression of individual patient outcomes
 1 Lysholm Department of Neuroradiology, National Hospital for Neurology & Neurosurgery, London, UK 2 Unit of Functional Neurosurgery, Sobell Department of Motor Neuroscience, UCL Institute of Neurology,
1 Lysholm Department of Neuroradiology, National Hospital for Neurology & Neurosurgery, London, UK 2 Unit of Functional Neurosurgery, Sobell Department of Motor Neuroscience, UCL Institute of Neurology,
E ssential tremor is a commonly diagnosed movement
 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
Dystonia: Title. A real pain in the neck. in All the Wrong Places
 Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation
 The Open Magnetic Resonance Journal, 2008, 1, 1-8 1 Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation X.A. Vasques 1-5, C. Tancu
The Open Magnetic Resonance Journal, 2008, 1, 1-8 1 Cerebral Magnetic Resonance Imaging Feasibility in Patients with Implanted Neurostimulation System for Deep Brain Stimulation X.A. Vasques 1-5, C. Tancu
Parkinson disease: Parkinson Disease
 Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
National Institute for Health and Clinical Excellence
 National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
 Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
Professor Tim Anderson
 Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Source: *Dystonia facts medically edited by: Charles Patrick Davis, MD, PhD
 Source: http://www.medicinenet.com/script/main/art.asp?articlekey=349 Dystonia facts* *Dystonia facts medically edited by: Charles Patrick Davis, MD, PhD Dystonia is a disorder of muscle control; it can
Source: http://www.medicinenet.com/script/main/art.asp?articlekey=349 Dystonia facts* *Dystonia facts medically edited by: Charles Patrick Davis, MD, PhD Dystonia is a disorder of muscle control; it can
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
Name of Policy: Deep Brain Stimulation
 Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II
 Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Dr Barry Snow. Neurologist Auckland District Health Board
 Dr Barry Snow Neurologist Auckland District Health Board Dystonia and Parkinson s disease Barry Snow Gowers 1888: Tetanoid chorea Dystonia a movement disorder characterized by sustained or intermittent
Dr Barry Snow Neurologist Auckland District Health Board Dystonia and Parkinson s disease Barry Snow Gowers 1888: Tetanoid chorea Dystonia a movement disorder characterized by sustained or intermittent
DBS Programming. Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18
 DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
Deep brain stimulation for dystonia
 1 AP-HP, Department of Neurology, Groupe Hospitalier Pitié-Salpêtrière, Paris, France 2 Centre de Recherche de l Institut du Cerveau et de la Moelle épinière (CRICM), CNRS UMR 7225, UPMC Université Paris
1 AP-HP, Department of Neurology, Groupe Hospitalier Pitié-Salpêtrière, Paris, France 2 Centre de Recherche de l Institut du Cerveau et de la Moelle épinière (CRICM), CNRS UMR 7225, UPMC Université Paris
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Professor Tim Anderson
 Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Deep Brain Stimulation. Is It Right for You?
 Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Malignant Neuroleptic Syndrome following Deep Brain Stimulation Surgery of Globus Pallidus Pars Internus in Cerebral Palsy
 Korean J Crit Care Med 2016 February 31(1):34-38 / ISSN 2383-4870 (Print) ㆍ ISSN 2383-4889 (Online) Case Report Malignant Neuroleptic Syndrome following Deep Brain Stimulation Surgery of Globus Pallidus
Korean J Crit Care Med 2016 February 31(1):34-38 / ISSN 2383-4870 (Print) ㆍ ISSN 2383-4889 (Online) Case Report Malignant Neuroleptic Syndrome following Deep Brain Stimulation Surgery of Globus Pallidus
Original Policy Date
 MP 7.01.48 Deep Brain Stimulation Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index
MP 7.01.48 Deep Brain Stimulation Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index
The motor regulator. 1) Basal ganglia/nucleus
 The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
Journal of Anesthesia & Pain Medicine
 Case Report To spasm, or Not to Spasm, That is the Question Journal of Anesthesia & Pain Medicine John C McDonald BA 1 and Terence K Gray DO 1,2* 1 Mercy Pain Center, Mercy Hospital, Portland, Maine, USA
Case Report To spasm, or Not to Spasm, That is the Question Journal of Anesthesia & Pain Medicine John C McDonald BA 1 and Terence K Gray DO 1,2* 1 Mercy Pain Center, Mercy Hospital, Portland, Maine, USA
THE MEDICAL AND SURGICAL TREATMENT OF DYSTONIA
 THE MEDICAL AND SURGICAL TREATMENT OF DYSTONIA Samuel Frank, MD Beth Israel Deaconess Medical Center Boston, MA Dystonia may present as an isolated disorder or as part of another disease process. The clinical
THE MEDICAL AND SURGICAL TREATMENT OF DYSTONIA Samuel Frank, MD Beth Israel Deaconess Medical Center Boston, MA Dystonia may present as an isolated disorder or as part of another disease process. The clinical
Surgical Management of Parkinson s Disease
 Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
Deep Brain Stimulation
 Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep brain stimulation (DBS) in children with primary
 J Neurosurg Pediatrics 14:400 408, 2014 AANS, 2014 Interventional MRI guided deep brain stimulation in pediatric dystonia: first experience with the ClearPoint system Clinical article Philip A. Starr,
J Neurosurg Pediatrics 14:400 408, 2014 AANS, 2014 Interventional MRI guided deep brain stimulation in pediatric dystonia: first experience with the ClearPoint system Clinical article Philip A. Starr,
Rapid assessment of gait and speech after subthalamic deep brain stimulation
 SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
Palladotomy and Pallidal Deep Brain Stimulation
 Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Patient selection for surgery: Hyperkinetic movement disorders
 Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
Deep Brain Stimulation. Description
 Subject: Deep Brain Stimulation Page: 1 of 20 Last Review Status/Date: September 2013 Deep Brain Stimulation Description Deep brain stimulation (DBS) involves the stereotactic placement of an electrode
Subject: Deep Brain Stimulation Page: 1 of 20 Last Review Status/Date: September 2013 Deep Brain Stimulation Description Deep brain stimulation (DBS) involves the stereotactic placement of an electrode
Deep Brain Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor
 Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor Karen L. Francis, PhD* Waneen W. Spirduso, EdD Tim Eakin, PhD Pamela Z.
Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor Karen L. Francis, PhD* Waneen W. Spirduso, EdD Tim Eakin, PhD Pamela Z.
Neurodegeneration with brain iron accumulation : clinical, radiographic and genetic heterogeneity and corresponding therapeutic options
 Acta neurol. belg., 2007, 107, 26-31 Neurodegeneration with brain iron accumulation : clinical, radiographic and genetic heterogeneity and corresponding therapeutic options Frederik CLEMENT 1,3, David
Acta neurol. belg., 2007, 107, 26-31 Neurodegeneration with brain iron accumulation : clinical, radiographic and genetic heterogeneity and corresponding therapeutic options Frederik CLEMENT 1,3, David
Aid to Programming: Algorithm and Check List for Electrode Configurations. Patient name: Medical Record No.
 1 Aid to Programming: Algorithm and Check List for Electrode Configurations Patient name: Medical Record No. Date of Birth: Month Day Year Diagnosis: DBS target: DBS side: The designations for the contacts
1 Aid to Programming: Algorithm and Check List for Electrode Configurations Patient name: Medical Record No. Date of Birth: Month Day Year Diagnosis: DBS target: DBS side: The designations for the contacts
Lecture XIII. Brain Diseases I - Parkinsonism! Brain Diseases I!
 Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Clinical Policy Title: Deep brain stimulation
 Clinical Policy Title: Deep brain stimulation Clinical Policy Number: 09.03.02 Effective Date: July 1, 2015 Initial Review Date: February 18, 2015 Most Recent Review Date: February 6, 2018 Next Review
Clinical Policy Title: Deep brain stimulation Clinical Policy Number: 09.03.02 Effective Date: July 1, 2015 Initial Review Date: February 18, 2015 Most Recent Review Date: February 6, 2018 Next Review
A lthough levodopa treatment remains the gold standard
 1640 PAPER Stimulation of the subthalamic nucleus in Parkinson s disease: a 5 year follow up W M M Schüpbach, N Chastan, M L Welter, J L Houeto, V Mesnage, A M Bonnet, V Czernecki, D Maltête, A Hartmann,
1640 PAPER Stimulation of the subthalamic nucleus in Parkinson s disease: a 5 year follow up W M M Schüpbach, N Chastan, M L Welter, J L Houeto, V Mesnage, A M Bonnet, V Czernecki, D Maltête, A Hartmann,
Specialised Services Policy: CP28 Deep Brain Stimulation
 Specialised Services Policy: CP28 Deep Brain Stimulation Document Author: Specialist Services Planning Manager for Neurosciences and Complex Conditions Executive Lead: Director of Planning Approved by:
Specialised Services Policy: CP28 Deep Brain Stimulation Document Author: Specialist Services Planning Manager for Neurosciences and Complex Conditions Executive Lead: Director of Planning Approved by:
Alim-Louis Benabid and Mahlon DeLong win the 2014 Lasker~DeBakey Clinical Medical Research Award
 Alim-Louis Benabid and Mahlon DeLong win the 2014 Lasker~DeBakey Clinical Medical Research Award The 2014 Lasker~DeBakey Clinical Medical Research Award recognizes the extraordinary efforts of two physician-scientists,
Alim-Louis Benabid and Mahlon DeLong win the 2014 Lasker~DeBakey Clinical Medical Research Award The 2014 Lasker~DeBakey Clinical Medical Research Award recognizes the extraordinary efforts of two physician-scientists,
Citation for published version (APA): Zutt, R. (2018). Myoclonus: A diagnostic challenge. [Groningen]: Rijksuniversiteit Groningen.
![Citation for published version (APA): Zutt, R. (2018). Myoclonus: A diagnostic challenge. [Groningen]: Rijksuniversiteit Groningen. Citation for published version (APA): Zutt, R. (2018). Myoclonus: A diagnostic challenge. [Groningen]: Rijksuniversiteit Groningen.](/thumbs/96/128260656.jpg) University of Groningen Myoclonus Zutt, Rodi IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document
University of Groningen Myoclonus Zutt, Rodi IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Value Units
 Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Patient selection for surgery: Parkinson s disease
 Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Clinical Policy Title: Deep brain stimulation
 Clinical Policy Title: Deep brain stimulation Clinical Policy Number: 09.03.02 Effective Date: July 1, 2015 Initial Review Date: February 18, 2015 Most Recent Review Date: March 15, 2017 Next Review Date:
Clinical Policy Title: Deep brain stimulation Clinical Policy Number: 09.03.02 Effective Date: July 1, 2015 Initial Review Date: February 18, 2015 Most Recent Review Date: March 15, 2017 Next Review Date:
Deep Brain Stimulation. Description. Section: Surgery Effective Date: April 15, 2015
 Subject: Deep Brain Stimulation Page: 1 of 22 Last Review Status/Date: March 2015 Deep Brain Stimulation Description Deep brain stimulation (DBS) involves the stereotactic placement of an electrode into
Subject: Deep Brain Stimulation Page: 1 of 22 Last Review Status/Date: March 2015 Deep Brain Stimulation Description Deep brain stimulation (DBS) involves the stereotactic placement of an electrode into
Linköping University Post Print. Patient-specific models and simulations of deep brain stimulation for postoperative follow-up
 inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
