Introduction to Viral Haemorrhagic Fevers
|
|
|
- Deborah Magdalene Bishop
- 5 years ago
- Views:
Transcription
1 Introduction to Viral Haemorrhagic Fevers Linus Ndegwa, MPHE, HCS Infection Control, Manager Global Disease Detection-GDD Centers for Disease Control and Prevention-Kenya
2 Session Objectives To explain viruses that cause haemorrhagic fevers (Ebola, Marburg, Yellow Fever) To discuss circumstances associated with VHF outbreaks To discuss preventive measures
3 What is Viral Hemorrhagic Fever?-1 Acute infection that often begins as non-specific illness Difficult to distinguish clinically from other febrile diseases, especially in the early phases Spectrum of severity, but frequently progresses to shock, multi organ-system failure, and death(severe multisystem syndrome) Damage to overall vascular system Pathogenesis of severe cases involves a lethal combination of increased capillary permeability, impaired coagulation and often impaired cardiac function
4 What is Viral Hemorrhagic Fever?-2 Hemorrhage actually seen in a minority of cases and is not usually large in volume Host as well as viral genetics probably play key roles in spectrum of disease Symptoms often accompanied by hemorrhage Rarely life threatening in itself Includes conjunctivitis, petechial, echymosis
5 VHF Taxonomy ARENAVIRIDAE: Lassa fever South American HF (Argentine, Bolivian, Venezuelan, Brazilian) BUNYAVIRIDAE: PHLEBOVIRUS NAIROVIRUS HANTAVIRUS Rift Valley fever Crimean Congo HF HF with renal syndrome Hantavirus pulmonary syndrome FILOVIRIDAE: Ebola HF Marburg HF FLAVIVIRIDAE:Yellow fever Dengue HF Kyasanur Forest disease Omsk HF
6 Classification Arenaviridae Bunyaviridae Filoviridae Flaviviridae Junin Crimean- Congo H.F. Ebola Kyasanur Forest Disease Machupo Hantavirus Marburg Omsk H.F. Sabia Guanarito Lassa Rift Valley fever Yellow Fever Dengue
7 Filoviridae Ebola virus Zaire (Zaire ebolavirus) Sudan Côte d Ivoire Bundibugyo Reston Lloviu (Cueva del Lloviu, in Spain) Marburg virus
8 Filoviridae Transmission Reservoir is UNKNOWN Bats implicated with Marburg Aerosol transmission Non-human primates (gorillas, chimps, monkeys) infected in the wild, but develop severe disease like humans. Thus likely represent a another chance dead-end host, not true reservoir Inter-human transmission through direct contact with blood/body secretions. Usually two components: Human to human transmission in the community: Intimate contact Ritual burial practices Nosocomial transmission Reuse of needles and syringes Exposure to infectious tissues, excretions, and hospital wastes
9 Sudan Guinea Sierra Leone Liberia Côte d Ivoire Uganda Gabon Republic of the Congo Democratic Republic of the Congo Key Zaire Taï Forest Sudan Sudan and Bundibugyo Kilometers 2000
10 Filoviridae Epidemiology-1 Marburg Africa Case fatality 23-33% Ebola Case fatality 53-88% Zaire 70-80% Sudan 50-60% Bundibugyo 24%(?) Côte d'ivoire 1 case, survived Reston 0? (Appears nonpathogenic to humans, but limited experience) Philippines Llovio 0? (sequences from bats only evidence)
11 Filoviridae Epidemiology-2 Pattern of disease is UNKOWN Affects all ages Infection:case ratio of Ebola perhaps lower than other VHFs Occasional epidemics in Africa, although rarely exported Mortality high, no specific therapy, no vaccine Primary management strategy is early detection and isolation of infected individuals Public health often overrides individual concern
12
13 Pathophysiology Filovirus entry is mediated by the viral spike glycoprotein (GP), which attaches viral particles to the cell surface, delivers them to endosomes and catalyses fusion between viral and endosomal membranes 2. Additional host factors: Endosomal compartment are probably required for viral membrane fusion.
14 Ebola clinical disease Most severe hemorrhagic fever Incubation period: 5 21 days Abrupt onset Fever, chills, malaise, dizziness, exhaustion and myalgia More severe: Bleeding under skin, in internal organs, orifices DIC Death around day 7 11 Painful recovery Laboratory findings: similar to other VHFs, although coagulation enzymes usually normal DDX: As for other VHFs
15
16
17
18
19
20
21 IDSR Case Definition Standard case definition Suspected case: Illness with onset of fever and no response to usual causes of fever in the area, and at least one of the following signs: bloody diarrhoea, bleeding from gums, bleeding into skin (purpura), bleeding into eyes and urine. Confirmed case: A suspected case with laboratory confirmation (positive IgM antibody, positive PCR or viral isolation), or epidemiologic link to confirmed cases or outbreak. Note: During an outbreak, these case definitions may be changed to correspond to the local event The DDSR hotlines are active. They are and
22 Surveillance Goals Early detection of cases and outbreaks, rapid investigation, and early laboratory verification of the aetiology of all suspected cases. Investigation of all suspected cases with contact tracing. During epidemics, most infected patients do not show haemorrhagic symptoms and a specific case definition according to the suspected or confirmed disease should be used.
23 Respond to Alert Threshold-1 If a single case is suspected: Report case-based information immediately to the appropriate levels and DDSR. Suspected cases should be placed in isolation and VHF Precautions strictly implemented. Standard precautions should be enhanced throughout the healthcare setting. Collect specimen to confirm the case(s). Conduct case-contact follow-up and active case search for additional cases.
24 Respond to Action Threshold-2 If a single case is confirmed: Maintain strict VHF infection control practices throughout the outbreak. Mobilize the community for early detection and care of cases and conduct community education about how the disease is transmitted and how to implement infection control in the home care setting and during funerals.
25 Respond to Action Threshold-3 Conduct case contact follow-up and active searches for additional cases that may not come to the health care setting. Request additional help from other levels as needed. Establish isolation ward to handle additional cases that may come to the health centre.
26 Laboratory Diagnosis-1 Specimen must be sent to KEMRI which is the WHO recognized reference lab. Besides, Ebola material can only be handled in a biosafety level 4 and above lab. Acute disease ELISA-based detection of viral specific antigen and IgM antibodies in serum Isolation of virus from blood early in the disease (moderate CPE) PCR
27 Laboratory Diagnosis-2 Surveillance ELISA-based detection of IgG antibodies Post-mortem Demonstration of antigen in tissue biopsy by immunohistochemistry
28
29
30 1201 cases (suspected/ confirmed) 814 confirmed 672 deaths
31
32 Nairobi KQ routes
33 Treatment Treat and manage the patient with Supportive treatment Ribavirin Not approved by FDA Effective in some individuals Arenaviridae and Bunyaviridae only Convalescent-phase plasma Argentine HF, Bolivian HF and Ebola Strict isolation of affected patients is required Report to health authorities
34 Prevention and Control If human case occurs Decrease person-to-person transmission Isolation of infected individuals Protective clothing Disposable gowns, gloves, masks and shoe covers, protective eyewear when splashing might occur, or if patient is disoriented or uncooperative WHO and CDC developed manual Infection Control for Viral Hemorrhagic Fevers In the African Health Care Setting
35 Prevention and Control Anyone suspected of having a VHF must use a chemical toilet Disinfect and dispose of instruments Use a 0.5% solution of sodium hypochlorite (1:10 dilution of bleach)
36 VHF Isolation
37 Session Objectives To discuss isolation management To outline required isolation practices for VHF To discuss how to implement cascaded isolation for various categories of VHF cases
38 Isolation management The measures to be undertaken should include: Setting up of minimum level of standard precautions for use of all patients regardless of their infection status, at the identified high-risk areas. Setting up of isolation facilities and barrier nursing/infection prevention and control. Establishment of safe handling and disposal of used needles and syringes. Use of safe burial practices and disposal of bodies
39 Isolation management To reduce the risk of Ebola/VHF transmission in a health care setting, use the VHF isolation precautions, which should include the following. Isolation of the patient. Wearing of protective clothing that should comprise of a scrub suit gown, apron, two pairs of gloves, mask, headcover, eyewear and rubber boots. Cleaning and disinfecting spills, waste and reusable equipments. Using of safe disposal method for non- reusable supplies and infectious waste.
40 Isolation management Provision of information about the risk of viral transmission on health care. Provision of information to families and community about prevention of viral infection and care of patients. The staff will require training to strengthen their skills for using the VHF isolation precautions. Since there may be not adequate time to conduct training, it is recommended that all health care personnel in the affected areas should be alerted of VHF isolation precautions.
41 History of Isolation Practices 1950 s - Infection Disease Hospitals begin to shut down (except for TBsanitariums) 1960 s - TB Hospitals also begin to shut down Centers for Disease Control publish first manual on Isolation Techniques for Use in Hospitals
42 History of Isolation Practices Cont 1970 CDC published a detailed manual titled Isolation Techniques A revised edition appeared in Seven isolation categories were recognised namely: - Strict isolation, Respiratory isolation, Protective isolation, Enteric precautions, Wound and Skin Precautions, Discharge Precautions and Blood Precautions. By mid 70s; 93% of US Hospitals had adopted the Isolation system. In 1980 s Hospitals were experiencing new endemic and epidemic nosocomial infectious problems. Some caused by Multi-drug resistant microorganisms and others caused by newly recognised pathogen requiring different isolation precautions.
43 History of Isolation Practices Cont d 1983 CDC guideline for Isolation, Precautions in Hospitals was published (Isolation Precautions). Hospital Infection Control Committee were given choice between category specific or disease specific isolation. Health worker is in charge of own decision on selected isolation precaution to follow. Category specific sections was modified: New categories were: Strict Isolation, Contact,Isolation, Respiratory Isolation, Tuberculosis (AFB) Isolation, Enteric Precautions, Drainage/Secretions and Body fluid precautions
44 7 Categories of Isolation Blood and Body Fluid Precautions Strict Isolation Contact Isolation Respiratory Isolation TB Isolation Enteric Isolation Drainage and Secretion Isolations N.B. Disease were lumped into categories based on epidemiological features of the disease (resulted in under or over isolation)
45 History of Isolation Practices Cont d 1985-Universal Precautions come into being HIV HBV Blood borne pathogens Body Substance Isolation
46 History of Isolation Practices Cont d 1990 s - HICPAC Isolation System Two tiered system Standard Precautions Transmission-based precautions Contact Droplet Airborne
47 History of Isolation Practices Cont d Slight Modification The Two tiered system has been modified into Standard and Expanded Precautions These are accepted practices that should be implemented by all health care providers when coming into contact blood, blood products or other bodily fluids irrespective of a patients suspected or confirmed infectious status.
48 History of Isolation Practices Cont d Components of Standard Precautions Hand Hygiene Protective Attire Appropriate Instrument Processing Prevention of Sharp Injuries Management of Medical Wastes Clean Environments Newly Added Respiratory Hygiene & Cough Ettiquette
49 History of Isolation Practices Cont d Components of Expanded Precautions Transmission-based precautions Contact Precautions Droplet Precautions Airborne Precautions (Renamed Airborne Infection Isolation AII) Newly Added Protective Environment for Allogeneic HSCT and other vulnerable patients
50 Key Points About PPE Don before contact with the patient, generally before entering the room Use carefully don t spread contamination Remove and discard carefully, either at the doorway or immediately outside patient room; remove respirator outside room Immediately perform hand hygiene
51 Are there any questions?
52 Annexes
53 Sequence* for Donning PPE Gown first Mask or respirator Goggles or face shield Gloves *Combination of PPE will affect sequence be practical
54 How to Don a Gown Select appropriate type and size Opening is in the back Secure at neck and waist If gown is too small, use two gowns Gown #1 ties in front Gown #2 ties in back
55 Sequence of Putting on PPE ( Donning ) 60
56 How to Don a Mask Place over nose, mouth and chin Fit flexible nose piece over nose bridge Secure on head with ties or elastic Adjust to fit
57 How to Don a Particulate Respirator Select a fit tested respirator Place over nose, mouth and chin Fit flexible nose piece over nose bridge Secure on head with elastic Adjust to fit Perform a fit check: Inhale respirator should collapse Exhale check for leakage around face
58
59 How to Don Eye and Face Protection Position goggles over eyes and secure to the head using the ear pieces or headband Position face shield over face and secure on brow with headband Adjust to fit comfortably
60 How to Don Gloves Don gloves last Select correct type and size Insert hands into gloves Extend gloves over isolation gown cuffs
61 A HW dressed in Full Personal Protective Equipment
62 How to Safely Use PPE Keep gloved hands away from face Avoid touching or adjusting other PPE Remove gloves if they become torn; perform hand hygiene before donning new gloves Limit surfaces and items touched
63 PPE Use in Healthcare Settings: How to Safely Remove PPE
64 Contaminated and Clean Areas of PPE Contaminated outside front Areas of PPE that have or are likely to have been in contact with body sites, materials, or environmental surfaces where the infectious organism may reside. Clean inside, outside back, ties on head and back. Areas of PPE that are not likely to have been in contact with the infectious organism
65 Sequence for Removing PPE Gloves Face shield or goggles Gown Mask or respirator
66 Where to Remove PPE At doorway, before leaving patient room or in anteroom* Remove respirator outside room, after door has been closed* *Ensure that hand hygiene facilities are available at the point needed, e.g., sink or alcohol-based hand rub
67 How to Remove Gloves (1) Grasp outside edge near wrist Peel away from hand, turning glove inside-out Hold in opposite gloved hand
68 How to Remove Gloves (2) Slide ungloved finger under the wrist of the remaining glove Peel off from inside, creating a bag for both gloves Discard
69 Removing gloves 4 5 6
70 Remove Goggles or Face Shield Grasp ear or head pieces with ungloved hands Lift away from face Place in designated receptacle for reprocessing or disposal
71 Removing Isolation Gown Unfasten ties Peel gown away from neck and shoulder Turn contaminated outside toward the inside Fold or roll into a bundle Discard
72 Removing a Mask Untie the bottom, then top, tie Remove from face Discard
73 Removing a Particulate Respirator Lift the bottom elastic over your head first Then lift off the top elastic Discard
74 Sequence of Taking off PPE ( Doffing ) 79
75 Hand Hygiene Perform hand hygiene immediately after removing PPE. If hands become visibly contaminated during PPE removal, wash hands before continuing to remove PPE Wash hands with soap and water or use an alcoholbased hand rub PPE Use in Healthcare Settings *Ensure that hand hygiene facilities are available at the point needed, e.g., sink or alcohol-based hand rub
76 Standard and Expanded Isolation Precautions
77 Standard Precautions Previously called Universal Precautions Assumes blood and body fluid of ANY patient could be infectious Recommends PPE and other infection control practices to prevent transmission in any healthcare setting Decisions about PPE use determined by type of clinical interaction with patient
78 PPE for Standard Precautions (1) Gloves Use when touching blood, body fluids, secretions, excretions, contaminated items; for touching mucus membranes and non-intact skin. Gowns Use during procedures and patient care activities when contact of clothing/ exposed skin with blood/body fluids, secretions, or excretions is anticipated.
79 PPE for Standard Precautions (2) Mask and goggles or a face shield Use during patient care activities likely to generate splashes or sprays of blood, body fluids, secretions, or excretions
80 PPE for Expanded Precautions Expanded Precautions include Contact Precautions Droplet Precautions Airborne Infection Isolation Protective Isolation precautions
81 Use of PPE for Expanded Precautions Contact Precautions Gown and gloves for contact with patient or environment of care (e.g., medical equipment, environmental surfaces) In some instances these are required for entering patient s environment Droplet Precautions Surgical masks within 3 feet of patient Airborne Infection Isolation Particulate respirator* *Negative pressure isolation room also required
82 Hand Hygiene Required for Standard and Expanded Precautions Perform Immediately after removing PPE Between patient contacts Wash hands thoroughly with soap and water or use alcohol-based hand rub
83 Bunyaviridae Rift Valley Fever virus Crimean-Congo Hemorrhagic Fever virus Hantavirus
84 Bunyaviridae Transmission Arthropod vector Exception Hantaviruses RVF Aedes mosquito CCHF Ixodid tick Hantavirus Rodents Less common Aerosol Exposure to infected animal tissue
85 Bunyaviridae Epidemiology RVF - Africa and Arabian Peninsula 1% case fatality rate CCHF - Africa, Eastern Europe, Asia 30% case fatality rate Hantavirus - North and South America, Eastern Europe, and Eastern Asia 1-50% case fatality rate
86 Bunyaviridae Humans RVF Incubation period 2-5 days 0.5% - Hemorrhagic Fever CCHF Incubation period 3-7 days Hemorrhagic Fever days following clinical signs Hantavirus Incubation period 7 21 days HPS and HFRS
87 Flaviviridae Dengue virus Yellow Fever virus Omsk Hemorrhagic Fever virus Kyassnur Forest Disease virus
88 Flaviviridae Transmission Arthropod vector Yellow Fever and Dengue viruses Aedes aegypti Sylvatic cycle Urban cycle Kasanur Forest Virus Ixodid tick Omsk Hemorrhagic Fever virus Muskrat urine, feces, or blood
89 Flaviviridae Epidemiology Yellow Fever Virus Africa and Americas Case fatality rate varies Dengue Virus Asia, Africa, Australia, and Americas Case fatality rate 1-10% Kyasanur Forest virus India Case fatality rate 3 5% Omsk Hemorrhagic Fever virus Europe Case fatlity rate 0.5 3%
90 Flaviviridae Humans Yellow Fever Incubation period 3 6 days Short remission Dengue Hemorrhagic Fever Incubation period 2 5 days Infection with different serotype Kyasanur Forest Disease Omsk Hemorrhagic Fever Lasting sequela
91 Acute Haemorrhagic Fever Syndrome Suspected case: Acute onset of fever of less than 3 weeks duration in a severely ill patient AND any 2 of the following; hemorrhagic or purpuric rash; epistaxis ; haematemesis; haemoptysis ; blood in stool; other hemorrhagic manifestations with no known predisposing factors Confirmed case: A suspected case with laboratory confirmation or epidemiologic link to confirmed cases or outbreak. Note: During an outbreak, case definitions may be changed to correspond to the local event.
92 VHF Case Definition Any person who has an unexplained illness with fever and bleeding or who died after an unexplained severe illness with fever and bleeding from all body openings
93 Yellow Fever Case Definition Suspected case: A person with acute onset of fever followed by jaundice within two weeks of onset of first symptoms. Hemorrhagic manifestations and renal failure may occur. Confirmed case: A suspected case with laboratory confirmation (positive IgM antibody or viral isolation) or epidemiologic link to confirmed cases or outbreaks
94 Rift Valley Fever Case Definition Suspected case: A person with an acute febrile illness (axillary temperature >37.5 ºC or oral/anal temperature of > 38. ºC) of more than 48 hours duration that does not respond to antibiotic or antimalarial therapy, and is associated with abrupt onset of any 1 or more of the following: Exhaustion, backache, muscle pains, headache (often severe), discomfort when exposed to light, and nausea/vomiting With: Direct contact with sick or dead animal or its products and/or Recent travel (during last week) to, or living in an area where, after heavy rains, livestock die or abort, and where RVF virus activity is suspected/confirmed And /or: Nausea/vomiting, diarrhea or abdominal pain with 1 or more of the following: Severe pallor (or Hb < 8 gm/dl) Confirmed case: Any patient who, after clinical screening, is positive for anti-rvf IgM ELISA antibodies (typically appear from fourth to sixth day after onset of symptoms) or tests positive on Reverse Transcriptase Polymerase Chain Reaction (RT-PCR)
Viral Hemorrhagic Fevers CDC, AFIP
 CDC, AFIP Diverse group of illnesses caused by RNA viruses from 4 families: Arenaviridae, Bunyaviridae, Filoviridae, Flaviridae Differ by geographic occurrence and vector/reservoir Share certain clinical
CDC, AFIP Diverse group of illnesses caused by RNA viruses from 4 families: Arenaviridae, Bunyaviridae, Filoviridae, Flaviridae Differ by geographic occurrence and vector/reservoir Share certain clinical
Viral hemorrhagic fevers (VHFs) By : Assis. Prof Nader Alaridah MD, PhD
 Viral hemorrhagic fevers (VHFs) By : Assis. Prof Nader Alaridah MD, PhD Overview Viral hemorrhagic fevers (VHFs) are a group of illnesses caused by four families of viruses. Arenaviridae, Bunyaviridae,
Viral hemorrhagic fevers (VHFs) By : Assis. Prof Nader Alaridah MD, PhD Overview Viral hemorrhagic fevers (VHFs) are a group of illnesses caused by four families of viruses. Arenaviridae, Bunyaviridae,
18/08/2016. Safe Patient Care Keeping our Residents Safe. Let s play dress up: Why, when and who? Overview
 Safe Patient Care Keeping our Residents Safe 2016 Let s play dress up: Why, when and who? Personal Protective Equipment, practical of donning and doffing, also including Respiratory Hygiene Jo O Hora,
Safe Patient Care Keeping our Residents Safe 2016 Let s play dress up: Why, when and who? Personal Protective Equipment, practical of donning and doffing, also including Respiratory Hygiene Jo O Hora,
The Chain of Infection
 The Chain of Infection As healthcare professionals, it is important to understand two things about infection: 1.the various ways infection can be transmitted 2. the ways the infection chain can be broken
The Chain of Infection As healthcare professionals, it is important to understand two things about infection: 1.the various ways infection can be transmitted 2. the ways the infection chain can be broken
UTSW/BioTel EMS TRAINING BULLETIN October EMS TB Ebola Virus Disease (EVD)
 UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
Summary of current outbreak in Guinea, Liberia and Sierra Leone
 ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
Media centre Ebola virus disease
 1 of 6 10/15/2014 10:59 AM Media centre Ebola virus disease Fact sheet N 103 Updated September 2014 Key facts Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, is a severe, often fatal
1 of 6 10/15/2014 10:59 AM Media centre Ebola virus disease Fact sheet N 103 Updated September 2014 Key facts Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, is a severe, often fatal
Viral Hemorrhagic Fevers
 Viral Hemorrhagic Fevers (VHFs) http://www.ncrr.nih.gov/publications/ncrr_reporter/summer-fall2009/images/essential_2.jpg Definition Viral hemorrhagic fevers (VHFs) refer to a group of illnesses that are
Viral Hemorrhagic Fevers (VHFs) http://www.ncrr.nih.gov/publications/ncrr_reporter/summer-fall2009/images/essential_2.jpg Definition Viral hemorrhagic fevers (VHFs) refer to a group of illnesses that are
Viral Hemorrhagic Fever
 Viral Hemorrhagic Fever Overview Organism History Epidemiology Transmission Disease in Humans Disease in Animals Prevention and Control What is Viral Hemorrhagic Fever? Severe multisystem syndrome Diffuse
Viral Hemorrhagic Fever Overview Organism History Epidemiology Transmission Disease in Humans Disease in Animals Prevention and Control What is Viral Hemorrhagic Fever? Severe multisystem syndrome Diffuse
Ebola Virus Disease (EVD) Essential information
 Ebola Virus Disease (EVD) Essential information Ebola Virus Disease (EVD) Origins The Ebola virus is named after the Ebola River in what was Zaire (now Democratic Republic of Congo) where the first outbreak
Ebola Virus Disease (EVD) Essential information Ebola Virus Disease (EVD) Origins The Ebola virus is named after the Ebola River in what was Zaire (now Democratic Republic of Congo) where the first outbreak
Ebola Virus Patient Advisory
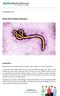 22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
VIRAL HEMORRHAGIC FEVER (VHF)
 VIRAL HEMORRHAGIC FEVER (VHF) REPORTING INFORMATION Class A: Report immediately via telephone the case or suspected case and/or a positive laboratory result to the local public health department where
VIRAL HEMORRHAGIC FEVER (VHF) REPORTING INFORMATION Class A: Report immediately via telephone the case or suspected case and/or a positive laboratory result to the local public health department where
EBOLA VIRUS AWARENESS
 EBOLA VIRUS AWARENESS Yvonne S. Butler, MD Assistant Professor; Obstetrics and Gynecology Global Women s Health Program Liberia Chevron-Liberia / BIPAI Partnership Baylor College of Medicine Texas Children
EBOLA VIRUS AWARENESS Yvonne S. Butler, MD Assistant Professor; Obstetrics and Gynecology Global Women s Health Program Liberia Chevron-Liberia / BIPAI Partnership Baylor College of Medicine Texas Children
Appendix B: Provincial Case Definitions for Reportable Diseases
 Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Hemorrhagic fevers caused by: i) Ebola virus and ii) Marburg virus and iii) Other viral causes including
Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Hemorrhagic fevers caused by: i) Ebola virus and ii) Marburg virus and iii) Other viral causes including
Marburg and Lassa viruses ศาสตราจารย ดร.พ ไลพ นธ พ ธว ฒนะ
 Marburg and Lassa viruses ศาสตราจารย ดร.พ ไลพ นธ พ ธว ฒนะ ศ นย ความร วมม อการว จ ยไข หว ดใหญ ภาคว ชาจ ลช วว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล มหาว ทยาล ยมห ดล Situation analysis of laboratory based surveillance
Marburg and Lassa viruses ศาสตราจารย ดร.พ ไลพ นธ พ ธว ฒนะ ศ นย ความร วมม อการว จ ยไข หว ดใหญ ภาคว ชาจ ลช วว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล มหาว ทยาล ยมห ดล Situation analysis of laboratory based surveillance
WHO SOUTHERN SUDAN HEALTH UPDATE May 2004
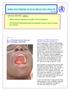 WHO SOUTHERN SUDAN HEALTH UPDATE SPECIAL EDITION: EBOLA Ebola outbreak confirmed in Yambio, Western Equatoria World Health Organization leads international response team to contain the outbreak Photo by:
WHO SOUTHERN SUDAN HEALTH UPDATE SPECIAL EDITION: EBOLA Ebola outbreak confirmed in Yambio, Western Equatoria World Health Organization leads international response team to contain the outbreak Photo by:
Provider Health & Safety Alert Ebola Virus Disease September 30, 2014
 Provider Health & Safety Alert Ebola Virus Disease September 30, 2014 With the announcement of the first confirmed case of Ebola Virus Disease (EVD) in Dallas Texas, there could be interactions with individuals
Provider Health & Safety Alert Ebola Virus Disease September 30, 2014 With the announcement of the first confirmed case of Ebola Virus Disease (EVD) in Dallas Texas, there could be interactions with individuals
12 June The average EVD case fatality rate has been around 50 per cent.
 12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
Ebola. Wessex CPD Event 14/11/14. Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre Tel:
 Ebola Wessex CPD Event 14/11/14 Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre wessex@phe.gov.uk Tel: 0345 055 2022 Outline Background About the current outbreak Situation in the UK Clinical management
Ebola Wessex CPD Event 14/11/14 Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre wessex@phe.gov.uk Tel: 0345 055 2022 Outline Background About the current outbreak Situation in the UK Clinical management
Dr. Johnmark Opondo MB. ChB. (Nairobi UON), MPH ( Emory) Deputy Medical Health Officer Saskatoon Health Region
 Dr. Johnmark Opondo MB. ChB. (Nairobi UON), MPH ( Emory) Deputy Medical Health Officer Saskatoon Health Region OBJECTIVES 1. To understand the basic science behind EVD 2. To review the issues behind the
Dr. Johnmark Opondo MB. ChB. (Nairobi UON), MPH ( Emory) Deputy Medical Health Officer Saskatoon Health Region OBJECTIVES 1. To understand the basic science behind EVD 2. To review the issues behind the
Questions and Answers on Ebola
 Updated: August 26, 2014 The 2014 Ebola outbreak is the largest Ebola outbreak in history and the first in West Africa. The current outbreak is affecting four countries in West Africa: Guinea, Liberia,
Updated: August 26, 2014 The 2014 Ebola outbreak is the largest Ebola outbreak in history and the first in West Africa. The current outbreak is affecting four countries in West Africa: Guinea, Liberia,
Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red
 Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red In this document: Summary Key Messages Ebola Cases and Deaths (West Africa) Ebola in U.S. Health Workers (in Liberia)
Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red In this document: Summary Key Messages Ebola Cases and Deaths (West Africa) Ebola in U.S. Health Workers (in Liberia)
Confronting Ebola. Keeping NY patients and healthcare workers safe and healthy
 Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
Marburg virus disease
 Marburg virus disease Fact sheet available at http://www.who.int/mediacentre/factsheets/fs_marburg/en/ Updated 20 October 2017 Key facts Marburg virus disease (MVD), formerly known as Marburg haemorrhagic
Marburg virus disease Fact sheet available at http://www.who.int/mediacentre/factsheets/fs_marburg/en/ Updated 20 October 2017 Key facts Marburg virus disease (MVD), formerly known as Marburg haemorrhagic
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS
 INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
Chapter 7 8/23/2016. Asepsis and Infection Control. Asepsis. Asepsis (Cont.) Microorganisms. Infection control and prevention
 Chapter 7 Asepsis and Infection Control All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Asepsis Microorganisms Tiny microscopic entities capable
Chapter 7 Asepsis and Infection Control All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Asepsis Microorganisms Tiny microscopic entities capable
A BSL-1 lab houses activities that require only standard microbial practices. These include:
 BSL-1 A BSL-1 lab houses activities that require only standard microbial practices. These include: Work should be performed on an open lab bench or table Spills must be decontaminated immediately Infectious
BSL-1 A BSL-1 lab houses activities that require only standard microbial practices. These include: Work should be performed on an open lab bench or table Spills must be decontaminated immediately Infectious
MODULE B. Objectives. Infection Prevention. Infection Prevention. N.C. Nurse Aide I Curriculum
 DHSR/HCPR/CARE NAT I Curriculum - July 2013 1 N.C. Nurse Aide I Curriculum MODULE B Infection Prevention Objectives Relate the chain of infection to the work of a nurse aide in long-term care facilities.
DHSR/HCPR/CARE NAT I Curriculum - July 2013 1 N.C. Nurse Aide I Curriculum MODULE B Infection Prevention Objectives Relate the chain of infection to the work of a nurse aide in long-term care facilities.
CHAPTER 7 Medical/Surgical Asepsis and Infection Control
 CHAPTER 7 Medical/Surgical Asepsis and Infection Control 1 Slide 1 Microorganisms Microscopic. Naturally present on and in the human body and environment. Some microorganisms (pathogens) cause specific
CHAPTER 7 Medical/Surgical Asepsis and Infection Control 1 Slide 1 Microorganisms Microscopic. Naturally present on and in the human body and environment. Some microorganisms (pathogens) cause specific
EBOLA 101. Update for EMS System Stakeholders. Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Nor Cal EMS Version 10/25/2014
 EBOLA 101 Update for EMS System Stakeholders Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Nor Cal EMS Version 10/25/2014 Conference 1 Version #1 Date 10/25/14 Content good for current situation 10/25/14
EBOLA 101 Update for EMS System Stakeholders Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Nor Cal EMS Version 10/25/2014 Conference 1 Version #1 Date 10/25/14 Content good for current situation 10/25/14
Emerging Infectious Diseases
 Emerging Infectious Diseases Dr Arthur Jackson Consultant in Infectious Diseases September 2014 The time has come to close the book on infectious diseases. We have basically wiped out infection in the
Emerging Infectious Diseases Dr Arthur Jackson Consultant in Infectious Diseases September 2014 The time has come to close the book on infectious diseases. We have basically wiped out infection in the
Infection Control Blood Borne Pathogens. Pines Behavioral Health
 Infection Control Blood Borne Pathogens Pines Behavioral Health Definition: Infection control is preventing the spread of germs that cause illness and infection. Infection control starts with understanding
Infection Control Blood Borne Pathogens Pines Behavioral Health Definition: Infection control is preventing the spread of germs that cause illness and infection. Infection control starts with understanding
Chapter 13. Preventing Infection. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE
 LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE For Residents & Instructors ggbha.org Updated 6/18/2018 This learning module must be reviewed by residents
LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE For Residents & Instructors ggbha.org Updated 6/18/2018 This learning module must be reviewed by residents
Genus Ebolavirus is 1 of 3 members of the Filoviridae family (filovirus), along with genus Marburgvirus and genus Cuevavirus.
 EBOLA VIRUS Ebola virus disease (EVD) is a severe, often fatal illness, with a case fatality rate of up to 90%. It is one of the world s most virulent diseases.the infection is transmitted by direct contact
EBOLA VIRUS Ebola virus disease (EVD) is a severe, often fatal illness, with a case fatality rate of up to 90%. It is one of the world s most virulent diseases.the infection is transmitted by direct contact
Chapter 11 PREVENTING INFECTION. Elsevier items and derived items 2010 by Mosby, Inc. an affiliate of Elsevier Inc. All rights reserved
 Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
بسم اهلل الرحمن الرحيم
 بسم اهلل الرحمن الرحيم INFECTION CONTROL MEASURES AGAINST H1N1 VIRUS; PHASE II Microbiology Diagnostics and Infection Control UNIT () Mansoura University Hospitals Prof. Mohammad Abou el-ela Director of
بسم اهلل الرحمن الرحيم INFECTION CONTROL MEASURES AGAINST H1N1 VIRUS; PHASE II Microbiology Diagnostics and Infection Control UNIT () Mansoura University Hospitals Prof. Mohammad Abou el-ela Director of
APPLIED EDUCATIONAL SYSTEMS. Infection Control. Health Science and Technology Education. Table of Contents
 Infection Control and Technology Education Microorganisms Microorganisms are small living bodies that are not visible to the naked eye. Nonpathogens - maintain body processes Pathogens cause infection
Infection Control and Technology Education Microorganisms Microorganisms are small living bodies that are not visible to the naked eye. Nonpathogens - maintain body processes Pathogens cause infection
The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
 Health & Safety Manual Health Promotion & Wellness ROUTINE PRACTICES PROCEDURES INTRODUCTION The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
Health & Safety Manual Health Promotion & Wellness ROUTINE PRACTICES PROCEDURES INTRODUCTION The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
Chapter 12. Preventing Infection. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Ebola Virus Disease. Global Epidemiology and Surveillance in Hong Kong. as of 13 August 2014
 Ebola Virus Disease Global Epidemiology and Surveillance in Hong Kong as of 13 August 2014 Ebola Virus Disease (EVD) Ebola virus disease (EVD), (formerly known as Ebola haemorrhagic fever) is a severe,
Ebola Virus Disease Global Epidemiology and Surveillance in Hong Kong as of 13 August 2014 Ebola Virus Disease (EVD) Ebola virus disease (EVD), (formerly known as Ebola haemorrhagic fever) is a severe,
The Ebola Virus. By Emilio Saavedra
 The Ebola Virus By Emilio Saavedra Etiological Agents: Ebolavirus is the etiologic agent. [1] There are four main families of viruses that are agents of Ebola (hemorrhagic fever). [1] These four families
The Ebola Virus By Emilio Saavedra Etiological Agents: Ebolavirus is the etiologic agent. [1] There are four main families of viruses that are agents of Ebola (hemorrhagic fever). [1] These four families
Infection Prevention and Control Induction Program. GRICG May 2015
 Infection Prevention and Control Induction Program GRICG May 2015 What is an infection? An infection occurs when invading microorganisms cause ill health Viruses Bacteria Fungi Parasites Prions Pain, tenderness,
Infection Prevention and Control Induction Program GRICG May 2015 What is an infection? An infection occurs when invading microorganisms cause ill health Viruses Bacteria Fungi Parasites Prions Pain, tenderness,
Infection Control Sec. 1, Unit 5 Part 1
 Infection Control Sec. 1, Unit 5 Part 1 Introduction Infections are a significant cause of illness, disease and death for residents that reside in certain living situations including nursing facilities.
Infection Control Sec. 1, Unit 5 Part 1 Introduction Infections are a significant cause of illness, disease and death for residents that reside in certain living situations including nursing facilities.
Information for Primary Care: Managing patients who require assessment for Ebola virus disease Updated 17 Oct 2014
 Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE
 PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers
 EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers VERSION 2 Interim Guidelines for Evaluation of US Patients Suspected of Having Ebola Virus Disease (EVD) This is a rapidly
EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers VERSION 2 Interim Guidelines for Evaluation of US Patients Suspected of Having Ebola Virus Disease (EVD) This is a rapidly
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
Infection Control in the School Setting. It s In Your Hands
 Infection Control in the School Setting It s In Your Hands What is an Infection? A condition resulting from the presence of, and invasion by, germs (microorganisms) For Infection to Occur an Organism Must:
Infection Control in the School Setting It s In Your Hands What is an Infection? A condition resulting from the presence of, and invasion by, germs (microorganisms) For Infection to Occur an Organism Must:
What employees should know about UNIVERSAL PRECAUTIONS. They re work practices that help prevent contact with blood and certain other body fluids.
 What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
Diseases that are commonly transmitted by exposure to blood. Most common are: Hepatitis B and C HIV
 Diseases that are commonly transmitted by exposure to blood Most common are: Hepatitis B and C HIV applies to all persons who may reasonably anticipate contact with blood or other potentially infectious
Diseases that are commonly transmitted by exposure to blood Most common are: Hepatitis B and C HIV applies to all persons who may reasonably anticipate contact with blood or other potentially infectious
Infectious Disease Control Oi Orientation. Providence Health & Services
 Infectious Disease Control Oi Orientation ti Providence Health & Services Infection Control Who is at risk of infection & why? Exposures and Outcomes What tools do we use to reduce risk? Surveillance Analysis
Infectious Disease Control Oi Orientation ti Providence Health & Services Infection Control Who is at risk of infection & why? Exposures and Outcomes What tools do we use to reduce risk? Surveillance Analysis
Communicable Diseases. Detection and Prevention
 Communicable Diseases Detection and Prevention Communicable Diseases Communicable Disease an infectious disease transmissible by direct contact (person to person) indirect means (body fluids, objects touched
Communicable Diseases Detection and Prevention Communicable Diseases Communicable Disease an infectious disease transmissible by direct contact (person to person) indirect means (body fluids, objects touched
Infection Prevention and Control Annual Education Authored by: Infection Prevention and Control Department
 Infection Prevention and Control Annual Education 2017 Authored by: Infection Prevention and Control Department Objectives After you complete this Computer-Based Learning (CBL) module, you should be able
Infection Prevention and Control Annual Education 2017 Authored by: Infection Prevention and Control Department Objectives After you complete this Computer-Based Learning (CBL) module, you should be able
Isolation Precautions. Pornrith Pisuttimarn, M.D.
 Isolation Precautions Pornrith Pisuttimarn, M.D. YEAR DOCUMENT ISSUED 1970 Isolation Techniques for Use in Hospitals, 1 st ed. 1975 Isolation Techniques for Use in Hospitals, 2 nd ed. 1983 CDC Guideline
Isolation Precautions Pornrith Pisuttimarn, M.D. YEAR DOCUMENT ISSUED 1970 Isolation Techniques for Use in Hospitals, 1 st ed. 1975 Isolation Techniques for Use in Hospitals, 2 nd ed. 1983 CDC Guideline
SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/ April Swine Flu-Information Sheet
 SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/09 Swine Flu-Information Sheet To date 2 cases of swine Influenza A (H1N1) have been confirmed in individuals in Scotland. Other
SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/09 Swine Flu-Information Sheet To date 2 cases of swine Influenza A (H1N1) have been confirmed in individuals in Scotland. Other
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING
 Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
EBOLA FACTS. During this outbreak, most of the disease has spread through human-to-human transmission.
 EBOLA FACTS Ebola virus disease (formerly known as Ebola haemorrhagic fever) is a severe and often fatal illness, with a fatality rate of up to 90%. It is one of the world s most dreaded diseases. However,
EBOLA FACTS Ebola virus disease (formerly known as Ebola haemorrhagic fever) is a severe and often fatal illness, with a fatality rate of up to 90%. It is one of the world s most dreaded diseases. However,
CDC Ebola Response Team
 Ebola Preparations from the Healthcare Epidemiologists Perspective August 25th, 2014 CDC Ebola Response Team Barbara Knust, DVM, MPH Epidemiology Team Lead Tim Uyeki, MD Clinical Team Lead Nancy Cornish,
Ebola Preparations from the Healthcare Epidemiologists Perspective August 25th, 2014 CDC Ebola Response Team Barbara Knust, DVM, MPH Epidemiology Team Lead Tim Uyeki, MD Clinical Team Lead Nancy Cornish,
Infection Control Precautions during the Clinical Management of Injecting Drug Users with Possible, Probable or Confirmed Anthrax
 Infection Control Precautions during the Clinical Management of Injecting Drug Users with Possible, Probable or Confirmed Anthrax (Adapted from guidance developed by Health Protection Scotland and HPA
Infection Control Precautions during the Clinical Management of Injecting Drug Users with Possible, Probable or Confirmed Anthrax (Adapted from guidance developed by Health Protection Scotland and HPA
Infection Control Standard Precautions and Isolation
 Infection Control Standard Precautions and Isolation Michael Bell, M.D. Division of Healthcare Quality Promotion Centers for Disease Control and Prevention History of Infection Control Precautions in the
Infection Control Standard Precautions and Isolation Michael Bell, M.D. Division of Healthcare Quality Promotion Centers for Disease Control and Prevention History of Infection Control Precautions in the
Infection Control Update
 Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION
 TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
Prevention and Control of Healthcare-Associated Norovirus
 Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
Statements about Ebola: True or false? Part 1 Commented version for trainers only!
 Statements about Ebola: True or false? Part 1 Commented version for trainers only! The questions and answers are designed to revise key messages of the training. If necessary, you may adapt the questions
Statements about Ebola: True or false? Part 1 Commented version for trainers only! The questions and answers are designed to revise key messages of the training. If necessary, you may adapt the questions
Doc: 1.9. Course: Patient Safety Solutions. Topic: Infection prevention and control. Summary
 Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Universal Precautions
 Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Infection Prevention and Control (IPC)
 Infection Prevention and Control (IPC) Standard Operating Procedure for CHICKENPOX (VARICELLA ZOSTER VIRUS) in a healthcare setting WARNING This document is uncontrolled when printed. Check local intranet
Infection Prevention and Control (IPC) Standard Operating Procedure for CHICKENPOX (VARICELLA ZOSTER VIRUS) in a healthcare setting WARNING This document is uncontrolled when printed. Check local intranet
Infection Control and Asepsis. Copyright 2010, 2006 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Infection Control and Asepsis 1 Introduction to Infection Control Nosocomial infections are acquired by patients in some kind of health care facility Center for Disease Control (CDC), the Joint Commission,
Infection Control and Asepsis 1 Introduction to Infection Control Nosocomial infections are acquired by patients in some kind of health care facility Center for Disease Control (CDC), the Joint Commission,
UNIVERSAL PRECAUTIONS BLOODBORNE PATHOGENS WHAT SCHOOL STAFF NEED TO KNOW
 UNIVERSAL PRECAUTIONS BLOODBORNE PATHOGENS WHAT SCHOOL STAFF NEED TO KNOW BELMONT PUBLIC SCHOOLS SEPTEMBER 2017 OBJECTIVES Provide school staff with education regarding the safe handling of all bodily
UNIVERSAL PRECAUTIONS BLOODBORNE PATHOGENS WHAT SCHOOL STAFF NEED TO KNOW BELMONT PUBLIC SCHOOLS SEPTEMBER 2017 OBJECTIVES Provide school staff with education regarding the safe handling of all bodily
Epidemiology and Risk of Infection in outpatient Settings
 Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Epidemiology and Risk of Infection in outpatient Settings
 Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Ebola Virus Diseases
 CDC/Dr F A Murphy Frequently Asked Questions on Ebola Virus Diseases Frequently asked questions on Ebola virus disease World Health Organization 2014 All rights reserved. Requests for publications, or
CDC/Dr F A Murphy Frequently Asked Questions on Ebola Virus Diseases Frequently asked questions on Ebola virus disease World Health Organization 2014 All rights reserved. Requests for publications, or
EDUCATIONAL COMMENTARY EMERGING INFECTIOUS DISEASES WITH GLOBAL IMPACT
 Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn CE Credits under Continuing Education on
Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn CE Credits under Continuing Education on
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT
 AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
PRESS STATEMENT ON MARBURG VIRUS DISEASE
 THE REPUBLIC OF UGANDA MINISTRY OF HEALTH PRESS STATEMENT ON MARBURG VIRUS DISEASE Hon. Dr. Jane Ruth Aceng Minister of Health October 19, 2017 PRESS STATEMENT ON MARBURG HEMORRHAGIC FEVER The Ministry
THE REPUBLIC OF UGANDA MINISTRY OF HEALTH PRESS STATEMENT ON MARBURG VIRUS DISEASE Hon. Dr. Jane Ruth Aceng Minister of Health October 19, 2017 PRESS STATEMENT ON MARBURG HEMORRHAGIC FEVER The Ministry
Infection Control Handout
 Modes of Transmission Contact Routes Direct Contact Transmission Indirect Contact Transmission Droplet Transmission Indirect contact contamination Clothes Soiled bed linen Personal care products Personal
Modes of Transmission Contact Routes Direct Contact Transmission Indirect Contact Transmission Droplet Transmission Indirect contact contamination Clothes Soiled bed linen Personal care products Personal
Respiratory Protection and Swine Influenza
 PAGE 1 TechUpdate Respiratory Protection and Swine Influenza Frequently asked Questions The U.S. Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) have recently issued
PAGE 1 TechUpdate Respiratory Protection and Swine Influenza Frequently asked Questions The U.S. Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) have recently issued
SARS Infection Control in Healthcare Settings
 SARS Infection Control in Healthcare Settings William A. Rutala, Ph.D., M.P.H. University of North Carolina (UNC) Hospitals and UNC School of Medicine Infection Control Considerations Hospitals must protect
SARS Infection Control in Healthcare Settings William A. Rutala, Ph.D., M.P.H. University of North Carolina (UNC) Hospitals and UNC School of Medicine Infection Control Considerations Hospitals must protect
EMS Infectious Disease Playbook Risk Based PPE Usage - Mike Deitschman, MPH, CPH, NDHP, NRP Executive Director South Dakota Healthcare Coalition
 EMS Infectious Disease Playbook Risk Based PPE Usage - Mike Deitschman, MPH, CPH, NDHP, NRP Executive Director South Dakota Healthcare Coalition Current EMS Projects Todays training Partnering with EMS
EMS Infectious Disease Playbook Risk Based PPE Usage - Mike Deitschman, MPH, CPH, NDHP, NRP Executive Director South Dakota Healthcare Coalition Current EMS Projects Todays training Partnering with EMS
*NCCT is approved as a provider of continuing education programs in the clinical laboratory sciences by the ASCLS P.A.C.E. Program, provider #122.
 COURSE DESCRIPTION Viral hemorrhagic fevers are serious infections with a high case fatality rate and the propensity to spread to caretakers of infected persons, either family members or healthcare workers,
COURSE DESCRIPTION Viral hemorrhagic fevers are serious infections with a high case fatality rate and the propensity to spread to caretakers of infected persons, either family members or healthcare workers,
CE Unit. Viruses and Vaccines
 CE Unit Viruses and Vaccines DO NOT WRITE What is a virus? Have you ever had a virus? What is a vaccine? How is a virus different from bacteria? What are the deadliest viruses? 10. Dengue fever 50 million
CE Unit Viruses and Vaccines DO NOT WRITE What is a virus? Have you ever had a virus? What is a vaccine? How is a virus different from bacteria? What are the deadliest viruses? 10. Dengue fever 50 million
Preventing Disease Transmission
 Chapter 4 Preventing Disease Transmission KNOWLEDGE OBJECTIVES 1. Describe how the immune system works. 2. Identify four ways in which diseases are transmitted, and give an example of how each can occur.
Chapter 4 Preventing Disease Transmission KNOWLEDGE OBJECTIVES 1. Describe how the immune system works. 2. Identify four ways in which diseases are transmitted, and give an example of how each can occur.
USE OF PERSONAL PROTECTION EQUIPMENT. Standard and Isolation precautions Ana M. Bonet 6/2017
 USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Infection Prevention and Control - General Orientation
 Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Bloodborne Pathogens. General
 Bloodborne Pathogens General Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Determine your risk of exposure Protect yourself from exposure through prevention
Bloodborne Pathogens General Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Determine your risk of exposure Protect yourself from exposure through prevention
The Struggle with Infectious Disease. Lecture 5
 The Struggle with Infectious Disease Lecture 5 Tropical Diseases Life and infectious disease began in the rift valley/rain forest of Eastern Africa Peoples migrated North to temperate regions Tropical
The Struggle with Infectious Disease Lecture 5 Tropical Diseases Life and infectious disease began in the rift valley/rain forest of Eastern Africa Peoples migrated North to temperate regions Tropical
Infection Control for Anesthesia Personnel
 Infection Control for Anesthesia Personnel 2017 A leading cause of death and increased morbidity for hospitalized ptns Hospitals, nursing homes, long-term care facilities, home care settings Higher rate
Infection Control for Anesthesia Personnel 2017 A leading cause of death and increased morbidity for hospitalized ptns Hospitals, nursing homes, long-term care facilities, home care settings Higher rate
At the end of this session, the participants will be able to:
 At the end of this session, the participants will be able to: Verbalize definitions related to infection control List modes of transmission of infections and portals of entry of bacteria Explain universal
At the end of this session, the participants will be able to: Verbalize definitions related to infection control List modes of transmission of infections and portals of entry of bacteria Explain universal
SUBJECT: Management of Human Body Fluids/Waste (Bloodborne Pathogens)
 Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
Acting in an Emergency (Video- Acting in an emergency and preventing disease transmission)
 CHAPTER 2 Acting in an Emergency (Video- Acting in an emergency and preventing disease transmission) Lesson Objectives 1. Explain how bloodborne pathogens may be transmitted from an infected person to
CHAPTER 2 Acting in an Emergency (Video- Acting in an emergency and preventing disease transmission) Lesson Objectives 1. Explain how bloodborne pathogens may be transmitted from an infected person to
Guidelines for Management, Prevention and Control of Crimean-Congo Hemorrhagic Fever (CCHF) December 2005
 Epidemic Investigation Cell (EIC) Public Health Laboratories Division National Institute of Health, Islamabad, Pakistan Tel: 051-9255237, 9255117 Fax: 9255125, 9255099 E-mail: edoffice@apollo.net.pk Guidelines
Epidemic Investigation Cell (EIC) Public Health Laboratories Division National Institute of Health, Islamabad, Pakistan Tel: 051-9255237, 9255117 Fax: 9255125, 9255099 E-mail: edoffice@apollo.net.pk Guidelines
2017 Infection Prevention and Control/Flu/TB/Basics Test Answer Key
 Name: School: Instructor: Date: 2017 Infection Prevention and Control/Flu/TB/Basics Test Answer Key For questions about this test, contact Infection Prevention and Control at 678-312-3308. 1. When do you
Name: School: Instructor: Date: 2017 Infection Prevention and Control/Flu/TB/Basics Test Answer Key For questions about this test, contact Infection Prevention and Control at 678-312-3308. 1. When do you
BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM
 Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Orion ISO Universal Precautions Employee Training Module
 Orion ISO Universal Precautions Employee Training Module Pathogens are disease-causing microorganisms. Bloodborne pathogens are viruses or bacteria present in human blood and body fluids which can infect
Orion ISO Universal Precautions Employee Training Module Pathogens are disease-causing microorganisms. Bloodborne pathogens are viruses or bacteria present in human blood and body fluids which can infect
skin and/or clothing Gloves: protect the hands Goggles: protect the eyes
 Infection control measures Refers to policies and procedures used to minimize the risk of spreading infections, Infection control especially in hospitals and health care facilities. Is a multi- disciplinary
Infection control measures Refers to policies and procedures used to minimize the risk of spreading infections, Infection control especially in hospitals and health care facilities. Is a multi- disciplinary
Worker Protection and Infection Control for Pandemic Flu
 Factsheet #2 What Workers Need to Know About Pandemic Flu Worker Protection and Infection Control for Pandemic Flu An influenza pandemic will have a huge impact on workplaces throughout the United States.
Factsheet #2 What Workers Need to Know About Pandemic Flu Worker Protection and Infection Control for Pandemic Flu An influenza pandemic will have a huge impact on workplaces throughout the United States.
Palliative Care in Ebola
 Palliative Care in Ebola CHALLENGES IN DELIVERY AND EXPERIENCES FROM THE CURRENT OUTBREAK Background Ebola: filovirus from the family filoviridae Named after the Ebola River in DRC (then Zaire) where first
Palliative Care in Ebola CHALLENGES IN DELIVERY AND EXPERIENCES FROM THE CURRENT OUTBREAK Background Ebola: filovirus from the family filoviridae Named after the Ebola River in DRC (then Zaire) where first
Bloodborne Pathogens For School Employees
 Bloodborne Pathogens For School Employees Waynesboro Public Schools Bloodborne Pathogens Training and Annual Review Created on May 5, 2010 Reviewed/Revised April 6, 2017 Introduction In an educational
Bloodborne Pathogens For School Employees Waynesboro Public Schools Bloodborne Pathogens Training and Annual Review Created on May 5, 2010 Reviewed/Revised April 6, 2017 Introduction In an educational
