With the establishment of evaluation
|
|
|
- Damon Cain
- 5 years ago
- Views:
Transcription
1 J Periodontol December 2009 Comparative Analysis of Peri-Implant Marginal Bone Loss Based on Microthread Location: A 1-Year Prospective Study After Loading Dong-Wook Song,* Dong-Won Lee,* Chong-Kwan Kim, Kwang-Ho Park, and Ik-Sang Moon* Background: The purpose of the present study was to investigate the short-term effects of microthread location on peri-implant marginal bone levels. Methods: Two types of implants, one with microthreads placed at the implant top (group A) and the other with microthreads placed 0.5 mm below the implant top (group B), were placed adjacent to each other in the partially edentulous areas of 20 patients. In total, 40 implants were placed. Bone loss around each implant was analyzed after 1 year of functional loading, and gingival parameters (modified plaque index and modified sulcus bleeding index) of the peri-implant soft tissue were evaluated. Bone losses after loading and gingival parameters were compared using the paired t test. Results: The average bone loss was 0.16 (SD: 0.19) mm in group A and 0.30 (SD: 0.22) mm in group B after 1-year of functional loading. The paired t test revealed a significant difference in crestal bone loss between groups A and B in individual patients (P = 0.004). No significant differences were found between the two groups for the gingival parameters. Conclusions: Less peri-implant bone loss was observed around implants with microthreads placed at the implant top (group A) compared to those in which microthreads were placed below the top (group B). These results indicated that the microthreads acted to stabilize the peri-implant marginal bone, and their locations played an important role in the stabilization process. J Periodontol 2009;80: KEY WORDS Alveolar bone loss; dental implants; dental radiography; prospective studies. * Department of Periodontology, Gangnam Severance Dental Hospital, College of Dentistry, Yonsei University, Seoul, Korea. Department of Periodontology, College of Dentistry, Yonsei University. Department of Oral and Maxillofacial Surgery, Gangnam Severance Dental Hospital, College of Dentistry, Yonsei University. With the establishment of evaluation criteria for implant success and survival, 1 the importance of the marginal bone level in assessing the dental implant response to loading has come into focus. Marginal bone loss can result from surgical trauma during implant placement, overloading, or establishment of biologic width. Studies 2-6 were conducted on the design and surface treatment of implants to minimize this problem. A 4-year radiographic study 7 on microthreaded implants revealed that surface texture, retentive elements at the implant neck, and the implant abutment interface design play crucial roles in maintaining peri-implant marginal bone. It was also stated that the implant abutment interface design profoundly affects the stress distribution in marginal bone, and a conical interface design decreases the peak bone implant interfacial shear stress compared to a flattop interface. 8 Surface roughness may also increase resistance to shear stress at the implant bone interface, affecting the implant holding power. 9 Additionally, retentive elements such as microthreads at the implant neck are necessary to preserve and maintain the peri-implant marginal bone. 7,10-13 Placing microthreads at the implant neck greatly increases the ability of an implant to resist axial loads, and the doi: /jop
2 Effect of Microthread Location on Marginal Bone Loss Volume 80 Number 12 mechanical stimulus provided by the microthreads helps to preserve periimplant marginal bone. 10 In animal experiments, implants with microthreads at the implant neck had a higher degree of bone-to-implant contact. 11 Furthermore, clinical studies 7,12 showed minimal bone resorption and stable peri-implant marginal bone around implants with microthreads at the implant neck. A 3-year clinical study 13 conducted by our group, which compared peri-implant marginal bone loss in microthreaded and non-microthreaded implants, found that microthreads at the implant neck were associated with less peri-implant marginal bone loss. Previously published studies 11,13 focused on the presence or absence of microthreads and, thus, did not provide insight into the effect of the microthread location on peri-implant marginal bone. In a clinical study using implants with different thread locations, Jung et al. 14 demonstrated that bone loss occurred differently depending on the thread location, and periimplant marginal bone levels stabilized at the level of the first thread. Therefore, it is possible that the microthread location might also have the same effect on the stabilization of marginal bone levels. The present study was conducted to investigate this relationship. MATERIALS AND METHODS This study was approved by the Institutional Review Board of Yonsei University. Patients were informed of the study procedures, and all provided written informed consent. Implants The implants used in this study were screw-shaped, threaded implants made of commercially pure titanium with a sand-blasted, large grit, acid-etched (SLA) surface. The point on the implant neck at which surface treatment began was designated as the top of the fixture (Figs. 1A and 1B). Originally, the most coronal location of the microthreads was 0.5 mm below the top of the fixture (group B; Fig. 1B). However, the design of the implant was changed: the location of the microthreads was moved up to the top of the fixture (group A; Fig. 1A). Other than the location of the microthreads, all other designs were identical between the two types of implants, and they were both available when the clinical research was performed. Patient Selection A pilot study was conducted prior to this investigation to determine the appropriate number of cases for statistically significant results. Twenty implants of each 1938 Figure 1. Schematic presentation of implants. A) Implants in group A. B) Implants in group B. group were arbitrarily chosen from independent patients not involved in the current research, and marginal bone loss after 1 year of functional loading was measured. A sample calculation revealed that 18 cases were necessary to obtain statistically significant results (the difference between the mean of groups A and B = 0.20; SD 1 = 0.19; SD 2 = 0.23; a = 0.05; b = 0.20). Twenty cases were selected with an anticipated dropout rate of 10%. i Patients who required implant therapy were recruited between March 2006 and July 2007 to the Department of Periodontology, Gangnam Severance Hospital, and were selected as subjects for this study. Most patients were in good general health, and the two patients who had diabetes and hypertension were well controlled with medication. In total, 11 males and nine females (mean age: 53.7 years; age range: 37 to 78 years) participated in the study. Treatment Procedure All surgeries were performed using a two-stage method. Implants from each group were placed adjacent to each other in the partially edentulous area of each patient. The implants were placed 0.5 mm subcrestally per the manufacturer s guidelines, and special attention was paid to ensure that there was 1mm of bone remaining both buccally and lingually. The mesio-distal location of each implant was randomly determined. The location and characteristics of each type of implant are illustrated in Table 1. The second surgery was performed 3 and 6 months later for mandibular and maxillary implants, respectively. The prostheses were delivered 3 weeks after the second Implantium, Dentium, Seoul, Korea. i MedCalc for Windows, version , MedCalc Software, Mariakerke, Belgium.
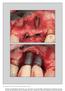
3 J Periodontol December 2009 Song, Lee, Kim, Park, Moon Table 1. Distribution of the Locations and Dimensions of Implants Subject Group Tooth # Fixture Diameter/ Length (mm) 1 A /8 B /8 2 A /8 B /8 3 A /8 B /8 4 A /10 B /10 5 A /10 B /10 6 A /12 B /10 7 A 2 4.3/8 B 3 4.3/8 8 A 5 4.3/8 B 6 4.3/8 9 A 9 4.3/8 B /10 10* A /10 B /10 11 A /10 B /10 12 A 3 4.3/10 B 4 4.3/10 13* A 2 4.3/10 B 4 3.8/10 14 A 2 4.8/8 B 3 4.3/12 15 A /10 B /8 16 A /10 B /10 17 A /8 B /10 18 A /8 B /10 19 A 3 4.3/10 B 4 4.3/10 20 A /10 B /12 * In two patients, the implants were not placed immediately adjacent to each other and were splinted to fabricate three- or four-unit bridges. surgery. Prostheses were mostly two-unit bridges, except in two patients (Table 1). Patients were recalled every 3 months for oral hygiene evaluation, professional plaque control, and a review of self-performed oral hygiene instructions. Radiographs The taking and measurement of radiographs followed previous protocols established by our group. 13,15-18 In brief, periapical radiographs were taken 1 day after implant placement, immediately after the second surgery, immediately after prosthesis delivery, and 1 year after functional loading. Radiographs were taken with an extension cone paralleling device # using the parallel cone technique (70 kv, 8 ma, and seconds). A 5.5-mm spherical metal bearing was placed to aid length measurement. All films were developed using the same automatic processor** following the manufacturer s instructions. Films were digitized using a digital scanner at an input resolution of 2,400 dots per inch with a 256 gray scale. Measurement of Marginal Bone Level Change After digitization, all images were transferred to a personal computer. The same monitor, set to a resolution of 1, pixels per inch, was used to examine the digitized radiographs. The room was kept dark throughout the computer-assisted radiographicmeasurement process. Bone loss was measured by comparing the radiographs taken immediately after prosthesis delivery to those taken 1 year after functional loading (Fig. 2). The marginal bone height was measured as the distance between the reference point and the most apical point of the marginal bone level. The reference point was the border between the polished surface and the SLA surface of the fixture. Calibration was performed using the known thread-pitch distance of the implants (1 pitch = 0.64 mm). A 5.5-mm spherical metal bearing was used for calibration when the threads were not clearly visible on the radiographs. Measurements were taken to the nearest 0.01 mm using computer software. ii Bone loss was measured at the mesial and distal peri-implant sites, and their average values were used. Measurements were made by a single operator (DWS). To test intraobserver variability, the marginal bone loss on 40 randomly selected radiographs was measured twice, with a 1-week interval. The statistical significance of the differences between the first and Kodak Insight, film speed F, Kodak, Rochester, NY. # Extension Cone Paralleling Kit, Rinn, Elgin, IL. ** Periomat, Durr Dental, Bietigheim-Bissingen, Germany. Epson GT-12000, Epson, Nagano, Japan. Processor: Intel Celeron D, Intel, Santa Clara, CA; operating system: Windows XP Professional 2002, Microsoft, Redmond, WA. Flatron 775FT Plus, LG, Seoul, Korea. ii UTHSCSA Image Tool, Version 3.00, University of Texas Health Science Center at San Antonio, San Antonio, TX. 1939
4 Effect of Microthread Location on Marginal Bone Loss Volume 80 Number 12 second measurements was assessed using the paired t test. Pearson correlation coefficients were calculated to analyze the correlation between the two sets of measurements. No significant differences were found between the first and second measurements in the paired t test (P = 0.43; 95% confidence interval: to 0.01). Both showed a high correlation, with a Pearson correlation coefficient of 0.97 (P <0.0001; 95% confidence interval: 0.93 to 0.98). Follow-Up Parameters At the 1-year follow-up visit, implants were evaluated for pain, discomfort, and implant-related infection. An implant was deemed as surviving when it was stable, functional, and asymptomatic. To rule out the possible influence of inflammatory changes of the periimplant tissues on the surrounding marginal bone, the modified plaque index (mpi) and modified sulcus bleeding index (mbi) were measured at four aspects around each implant. 19 Averages of the four obtained mpi and mbi values were calculated to represent the respective values for each implant. Statistical Analyses The null hypothesis was defined as: 1) no difference between the mean marginal bone loss of groups A and B during the examination period; and 2) no difference between the mean mpi and mbi of both groups. The Kolmogorov-Smirnov test was used to test the normality of the distribution. The paired t test was used to analyze differences in peri-implant marginal bone loss and gingival parameters between the two groups. Computer software was used to process the data. Values were deemed statistically significant at P < Figure 2. Intraoral radiographs of implants in groups A (a) and B (b). A) At prosthesis delivery. B) One year after functional loading. RESULTS Clinical Examination No remarkable complications were found during the observation period. None of the subjects complained of pain, and mobility was not observed in any of the implants. No implants were lost in this study, and complications associated with the prostheses were also not found. Marginal Bone Level Changes The marginal bone loss for each type of implant is illustrated in Table 2. The Kolmogorov-Smirnov test revealed a normal distribution in both groups (group A: P = 0.064; group B: P = 0.377). The average bone loss in groups A and B showed a statistically significant difference (P = ). A box plot of the marginal bone loss around implants from groups A and B is illustrated in Figure 3. Evaluation of Peri-Implant Soft Tissues The peri-implant soft tissues revealed little tendency to bleed after probing and were clinically healthy. The mpi and mbi for each type of implant is illustrated in Tables 3 and 4, respectively. No significant differences were found between the two groups for either the mpi or mbi (mpi: P = 0.419; mbi: P = 0.186). DISCUSSION This prospective study investigated whether the microthread location at the implant neck affected the peri-implant marginal bone level. To minimize variability from load or bone quality, implants from groups A and B were placed adjacent to each other in the edentulous area of each patient. We used computer software to accurately and reliably analyze periapical radiographs taken immediately after prosthesis connection and 1 year after functional loading to study the influence of microthreads on changes in marginal bone under load. 20 Less bone loss was observed in group A than in group B (0.16 [SD: 0.19] mm versus 0.30 [SD: 0.22] mm), and no significant differences were found between the two groups for the gingival parameters. Bone loss at the mesial and distal peri-implant sites was within the success criteria established by Albrektsson et al. 1 Numerous animal experiments 21,22 and clinical studies 14,23-27 demonstrated that a smooth implant neck without retentive elements facilitates significant marginal bone resorption. Such bone loss may be due to a lack of mechanical stimulus around the implant; elements such as a rough surface and microthreads at the implant neck are necessary to avoid such problems. 10 In a clinical study 14 involving various implant systems, bone loss usually occurred at the most apical point of the smooth portion of the implant neck, immediately above the first thread. At the level of the first thread, the peri-implant marginal bone remained stable. SPSS for Windows, release 13.0, SPSS, Chicago, IL.
5 J Periodontol December 2009 Song, Lee, Kim, Park, Moon Table 2. Marginal Bone Loss (mm) Around Implants in Groups A and B Type of Implant Subject Group A Group B Average SD Median % confidence interval for the mean 0.07 to to 0.32 A photoelastic study 28 demonstrated that threads generated compressive stresses in the supporting tissues, and the thread location on the implant body affected the pattern of load transfer. A literature review 29 on peri-implant marginal bone loss indicated that the first thread converted the shear force placed on the implant into a compressive force. According to one study, 30 bone is most resistant to compressive strength and is 30% and 65% less resistant to tensile and shear strength, respectively. This transformation Figure 3. Box plot of marginal bone loss around implants in groups A and B. Asterisks represent the outside value that is defined as a value larger than the upper quartile plus 1.5 times the interquartile range. of the shear stress acting on the peri-implant marginal bone to compressive strength reduces excessive stress and decreases microdamage to the marginal bone. The reported marginal bone loss around microthreaded implants after 1 year of functional loading are varied and range from 0.05 to 0.6 mm. 7,12,31,32 It was speculated that the presence or absence of the microthread might be the proper explanation for the diversity in the reported bone loss. 13 In the present study, the average bone loss around implants with microthreads placed 0.5 mm below the top of the neck (group B) was greater than that observed around implants in which the microthreads were placed at the implant top (group A). One possible explanation is that implants with microthreads placed below the top lacked retentive features above the microthread level and, therefore, lacked the ability to distribute stress concentrated at the implant neck. Thus, these implants may have transferred this stress to the periimplant marginal bone. If such stress exceeds the threshold that the peri-implant marginal bone can withstand, fatigue microdamage occurs, leading to bone resorption. 33 Therefore, microthreads, which act to distribute stress, placed at the level of the marginal bone exert optimal effects for maintaining periimplant marginal bone stability. The incorporation of retentive elements such as microthreads to rough-surface implants provides various advantages including increased implant-to-bone contact and improved stress distribution. 10,11,33 However, 1941
6 Effect of Microthread Location on Marginal Bone Loss Volume 80 Number 12 Table 3. mpi of Implants in Groups A and B Type of Implant Subject Group A Group B Average SD Median % confidence interval for the mean 0.55 to to 0.78 Table 4. mbi of Implants in Groups A and B Type of Implant Subject Group A Group B Average SD Median % confidence interval for the mean 0.40 to to 0.69 the exposure of rough-surface implants to the oral environment can accelerate biofilm formation and facilitate plaque retention, increasing the risk of periimplant mucositis and peri-implantitis. 34,35 Therefore, such potential biologic complications related to microthreads should be taken into account when formulating a treatment plan for patients with a high susceptibility to peri-implantitis. 35 Unlike the study by Jung et al., 14 in which marginal bone loss occurred to the level of the first thread, the present investigation showed less bone loss in most subjects, to a level slightly coronal to the first microthread. Also, whereas the aforementioned study 14 used external hex-type implants with a flat-top implant abutment interface, the present study used implants with an internal conical seal design and a conical implant abutment interface. According to a previous study 8 using finite-element analysis, the peak interfacial shear stress occurs at the top marginal bone in flat-top interfaces but more apically in conical interfaces. The magnitude and location of the peak stress in marginal bone is crucial. According 1942
7 J Periodontol December 2009 Song, Lee, Kim, Park, Moon to Saint Venant s principle, load distribution change on the end of a structure alters the stresses only near the end. 8 Thus, an implant abutment junction that is closer to the alveolar crest will produce greater stress and strain compared to one that is farther away, which, in turn, may lead to bone loss. The bone-loss pattern of group B, in which marginal bone resorption occurred at a level coronal to the first microthread, may have been influenced by the internal conical seal design, which decreases the stress and strain on the marginal bone by axially distributing stresses applied to the implant. The effects of platform switching may also account for the lesser amount of bone loss observed. The abutments that were used in this investigation were smaller in diameter than the fixtures, and the fixtures had a horizontal offset and a bevel at the top, placing the implant abutment interface farther from the crestal bone. This feature prevents inflammation arising from the implant abutment interface from reaching bone, contributing to a decrease in overall alveolar bone loss. 36,37 Taken together, the bone-loss pattern observed in this study could be a result of the presence of microthreads at the implant neck and a combination of other factors such as the internal conical design and platform switching. Inflammation of the peri-implant tissues can adversely affect the integrity of the peri-implant marginal bone. To investigate the influence of peri-implant tissues on marginal bone, the mpi and mbi of the implant prostheses were measured 1 year after functional loading. No significant differences in gingival parameters were found between the two groups. This could be explained by the study design, which involved placing the two different implant types adjacent to each other in an attempt to provide the same conditions for both groups. The mpi and mbi measured 1 year after functional loading cannot be said to perfectly reflect the health of the peri-implant soft tissues during that time period. However, considering the similarities between the mpi and mbi of the two groups, it can be presumed that inflammation of the peri-implant tissues affected both groups to the same degree. Thus, the difference in the marginal bone loss between the two types of implants was due to differences in the microthread location. This study also showed that microthreads stabilized the level of the marginal bone. Therefore, placing microthreads as far coronally as possible along the bone-to-implant interface could help maintain the marginal bone. CONCLUSIONS The aim of this study was to investigate the effects of microthread location on peri-implant marginal bone levels. The average bone loss was 0.16 (SD: 0.19) mm in group A and 0.30 (SD: 0.22) mm in group B after 1 year of functional loading. The paired t test revealed a significant difference in crestal bone loss between groups A and B in individual patients (P = 0.004). No significant differences were found between the two groups for the gingival parameters. Less peri-implant bone loss was observed in the implants with microthreads placed at the implant top (group A) compared to those in which microthreads were placed below the top (group B). These results indicate that microthreads act to stabilize the peri-implant marginal bone, and their location plays an important role in the stabilization process. ACKNOWLEDGMENTS Drs. Song and Lee contributed equally to the research in this study. The authors report no conflicts of interest related to this study. REFERENCES 1. Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: A review and proposed criteria of success. Int J Oral Maxillofac Implants 1986;1: Esposito M, Hirsch JM, Lekholm U, Thomsen P. Biological factors contributing to failures of osseointegrated oral implants. (II). Etiopathogenesis. Eur J Oral Sci 1998;106: Isidor F. Histological evaluation of peri-implant bone at implants subjected to occlusal overload or plaque accumulation. Clin Oral Implants Res 1997;8: Cochran DL, Hermann JS, Schenk RK, Higginbottom FL, Buser D. Biologic width around titanium implants. A histometric analysis of the implanto-gingival junction around unloaded and loaded nonsubmerged implants in the canine mandible. J Periodontol 1997;68: Abrahamsson I, Berglundh T, Wennström J, Lindhe J. The peri-implant hard and soft tissues at different implant systems. A comparative study in the dog. Clin Oral Implants Res 1996;7: Berglundh T, Lindhe J. Dimension of the periimplant mucosa. Biological width revisited. J Clin Periodontol 1996;23: Norton MR. Marginal bone levels at single tooth implants with a conical fixture design. The influence of surface macro- and microstructure. Clin Oral Implants Res 1998;9: Hansson S. Implant-abutment interface: Biomechanical study of flat top versus conical. Clin Implant Dent Relat Res 2000;2: Wilke HJ, Claes L, Steinemann S. The influence of various titanium surfaces on the interface shear strength between implants and bone. In: Heimke G, Soltesz U, Lee AJC, eds. Clinical Implant Materials: Advances in Biomaterials. Amsterdam: Elsevier Science Publishers; 1990;9: Hansson S. The implant neck: Smooth or provided with retention elements. A biomechanical approach. Clin Oral Implants Res 1999;10: Rasmusson L, Kahnberg KE, Tan A. Effects of implant design and surface on bone regeneration and implant stability: An experimental study in the dog mandible. Clin Implant Dent Relat Res 2001;3:
8 Effect of Microthread Location on Marginal Bone Loss Volume 80 Number Palmer RM, Palmer PJ, Smith BJ. A 5-year prospective study of astra single tooth implants. Clin Oral Implants Res 2000;11: Lee DW, Choi YS, Park KH, Kim CS, Moon IS. Effect of micro-thread on the maintenance of marginal bone level: A 3-year prospective study. Clin Oral Implants Res 2007;18: Jung YC, Han CH, Lee KW. A 1-year radiographic evaluation of marginal bone around dental implants. Int J Oral Maxillofac Implants 1996;11: Lee DW, Kim CK, Park KH, Cho KS, Moon IS. Noninvasive method to measure the length of soft tissue from the top of the papilla to the crestal bone. J Periodontol 2005;76: Lee DW, Park KH, Moon IS. Dimension of keratinized mucosa and the interproximal papilla between adjacent implants. J Periodontol 2005b;76: Lee DW, Park KH, Moon IS. Dimension of interproximal soft tissue between adjacent implants in two distinctive implant systems. J Periodontol 2006;77: Lee DW, Huh JK, Park KH, Chai JK, Kim CK, Moon IS. Comparison of interproximal soft tissue height for single implants and contra-lateral natural teeth. Clin Oral Implants Res 2009;20: Mombelli A, van Oosten MA, Schürch E Jr., Lang NP. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol 1987;2: Wyatt CCL, Bryant SR, Avivi-Arber L, Chaytor DV, Zarb GA. A computer-assisted measurement technique to assess bone proximal to oral implants on intraoral radiographs. Clin Oral Implants Res 2001;12: Pilliar RM, Deporter DA, Watson PA, Valiquette N. Dental implant design effect on bone remodeling. J Biomed Mater Res 1991;25: al-sayyed A, Deporter DA, Pilliar RM, et al. Predictable crestal bone remodelling around two porous-coated titanium alloy dental implant designs. A radiographic study in dogs. Clin Oral Implants Res 1994;5: Quirynen M, Naert I, van Steenberghe D. Fixture design and overload influence marginal bone loss and fixture success in the Brånemark system. Clin Oral Implants Res 1992;3: Andersson B. Implants for single-tooth replacement. A clinical and experimental study on the Brånemark CeraOne System. Swed Dent J Suppl 1995;108: Engquist B, Nilson H, Åstrand P. Single-tooth replacement by osseointegrated Brånemark implants. A retrospective study of 82 implants. Clin Oral Implants Res 1995;6: Hämmerle CHF, Brägger U, Bürgin W, Lang NP. The effect of subcrestal placement of the polished surface of ITI implants on marginal soft and hard tissues. Clin Oral Implants Res 1996;7: Malevez CH, Hermans M, Daelemans PH. Marginal bone levels at Brånemark system implants used for single tooth restoration. The influence of implant design and anatomical region. Clin Oral Implants Res 1996;7: Kinni ME, Hokama SN, Caputo AA. Force transfer by osseointegrated implant devices. Int J Oral Maxillofac Implants 1987;2: Oh TJ, Yoon J, Misch CE, Wang HL. The causes of early implant bone loss: Myth or science? J Periodontol 2002;73: Guo XE. Mechanical properties of cortical bone and cancellous bone tissue. In: Cowin SC, ed. Bone Mechanics Handbook. Boca Raton, FL: CRC Press; 2001;10: Puchades-Roman L, Palmer RM, Palmer PJ, Howe LC, Ide M, Wilson RF. A clinical, radiographic, and microbiologic comparison of astra tech and Brånemark single tooth implants. Clin Implant Dent Relat Res 2000;2: Engquist B, Åstrand P, Dahlgren S, Engquist E, Feldmann H, Gröndahl K. Marginal bone reaction to oral implants: A prospective comparative study of astra tech and Brånemark system implants. Clin Oral Implants Res 2002;13: Isidor F. Influence of forces on peri-implant bone. Clin Oral Implants Res 2006;17: Teughels W, Assche NV, Sliepen I, Quirynen M. Effect of material characteristics and/or surface topography on biofilm development. Clin Oral Implants Res 2006; 17: Cosyn J, Sabzevar MM, De Wilde P, De Rouck T. Twopiece implants with turned versus microtextured collars. J Periodontol 2007;78: Jung RE, Jones AA, Higginbottom FL, et al. The influence of non-matching implant and abutment diameters on radiographic crestal bone levels in dogs. J Periodontol 2008;79: Cochran DL, Bosshardt DD, Grize L, et al. Bone response to loaded implants with non-matching implant-abutment diameters in the canine mandible. J Periodontol 2009;80: Correspondence: Dr. Ik-Sang Moon, Department of Periodontology, Gangnam Severance Dental Hospital, College of Dentistry, Yonsei University, Seoul, Korea. Fax: ; ismoon@yuhs.ac. Submitted June 9, 2009; accepted for publication July 16,
Effect of thread size on the implant neck area: preliminary results at 1 year of function
 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Effect of microthread on the maintenance of marginal bone level: a 3-year prospective study
 Dong-Won Lee Young-Shill Choi Kwang-Ho Park Chang-Sung Kim Ik-Sang Moon Effect of microthread on the maintenance of marginal bone level: a 3-year prospective study Authors affiliations: Dong-Won Lee, Young-Shill
Dong-Won Lee Young-Shill Choi Kwang-Ho Park Chang-Sung Kim Ik-Sang Moon Effect of microthread on the maintenance of marginal bone level: a 3-year prospective study Authors affiliations: Dong-Won Lee, Young-Shill
Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function
 Jung-Joo Kim n Dong-Won Lee n Chong-Kwan Kim Kwang-Ho Park Ik-Sang Moon Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function Authors
Jung-Joo Kim n Dong-Won Lee n Chong-Kwan Kim Kwang-Ho Park Ik-Sang Moon Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function Authors
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
The peri-implant mucosa has
 Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
To achieve esthetic success with implant restorations,
 Case Series Influence of the Tooth- and Implant-Side Marginal Bone Level on the Interproximal Papilla Dimension in a Single Implant With a Microthread, Conical Seal, and Platform-Switched Design Hee-Jun
Case Series Influence of the Tooth- and Implant-Side Marginal Bone Level on the Interproximal Papilla Dimension in a Single Implant With a Microthread, Conical Seal, and Platform-Switched Design Hee-Jun
Tae-Hyung Kim. The Graduate School. Yonsei University. Department of Dental Science
 Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The 2B-3D rule for implant planning, placement and restoration
 IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs
 Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Replacement of missing teeth by means of
 Peri-Implant Bone Level Around Implants with Platform-Switched Abutments Stefan Fickl, Dr Med Dent 1 /Otto Zuhr, Dr Med Dent 2 /Jamal M. Stein, Dr Med Dent 3 / Markus B. Hürzeler, Prof Dr Med Dent 2,4
Peri-Implant Bone Level Around Implants with Platform-Switched Abutments Stefan Fickl, Dr Med Dent 1 /Otto Zuhr, Dr Med Dent 2 /Jamal M. Stein, Dr Med Dent 3 / Markus B. Hürzeler, Prof Dr Med Dent 2,4
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study
 Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Michael P. Hänggi,* Daniel C. Hänggi, John D. Schoolfield, Jürg Meyer,* David L. Cochran, and Joachim S. Hermann
 J Periodontol May 2005 Crestal Bone Changes Around Titanium Implants. Part I: A Retrospective Radiographic Evaluation in Humans Comparing Two Non-Submerged Implant Designs With Different Machined Collar
J Periodontol May 2005 Crestal Bone Changes Around Titanium Implants. Part I: A Retrospective Radiographic Evaluation in Humans Comparing Two Non-Submerged Implant Designs With Different Machined Collar
High Crown to Implant Ratio as Stress Factor in Short Implants Therapy
 10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
BONE LEVEL IMPLANT SCIENTIFIC OVERVIEW
 BONE LEVEL IMPLANT SCIENTIFIC OVERVIEW STUDY OVERVIEW ON STRAUMANN BONE LEVEL IMPLANT Pre-clinical studies Topic Objective Study Setup, Principal Investigator Property tests Biomechanical stability Ultimate
BONE LEVEL IMPLANT SCIENTIFIC OVERVIEW STUDY OVERVIEW ON STRAUMANN BONE LEVEL IMPLANT Pre-clinical studies Topic Objective Study Setup, Principal Investigator Property tests Biomechanical stability Ultimate
A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report of two cases
 Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Alfredo Montes Imeri, D.D.S.
 Proximal bone levels of plateau-designed, press fit implants adjacent to a natural teeth and implants A THESIS SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY: Alfredo
Proximal bone levels of plateau-designed, press fit implants adjacent to a natural teeth and implants A THESIS SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY: Alfredo
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
Soft tissue responses to differential shapes of the implant abutment
 대한치주과학회지 : Vol. 36, No. 1, 2006 Soft tissue responses to differential shapes of the implant abutment Soo-Yong Ahn 1, Chong-Hyun Han 2, Seong-Joo Heo 3, Tae-Il Kim 1, Yang-Jo Seol 1, Yong-Moo Lee 1, Young
대한치주과학회지 : Vol. 36, No. 1, 2006 Soft tissue responses to differential shapes of the implant abutment Soo-Yong Ahn 1, Chong-Hyun Han 2, Seong-Joo Heo 3, Tae-Il Kim 1, Yang-Jo Seol 1, Yong-Moo Lee 1, Young
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Peri-implant health and peri-implant bone stability after immediate implant placement
 2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Since the introduction of osseointegrated dental implants
 CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Effect of varying horizontal mismatched implants on crestal bone level and peri-implant soft tissue: An in vivo study
 2018; 4(2): 141-148 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(2): 141-148 2018 IJADS www.oraljournal.com Received: 05-02-2018 Accepted: 09-03-2018 Dr. Renu Gupta Head of Department, Department
2018; 4(2): 141-148 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(2): 141-148 2018 IJADS www.oraljournal.com Received: 05-02-2018 Accepted: 09-03-2018 Dr. Renu Gupta Head of Department, Department
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
Review. The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang*
 The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang* The success of dental implants is highly dependent on integration between the implant
The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang* The success of dental implants is highly dependent on integration between the implant
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
INTRODUCTION MATERIAL AND METHODS
 Original Research Loss of Interdental Crestal Bone Comparison Following Immediate and Delayed Loading after Delayed Placement of Dental Implants in Mandible - A Clinical Study Potharaju Santhi Priya 1,
Original Research Loss of Interdental Crestal Bone Comparison Following Immediate and Delayed Loading after Delayed Placement of Dental Implants in Mandible - A Clinical Study Potharaju Santhi Priya 1,
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
More than pure esthetics. The natural and strong solution.
 More than pure esthetics. The natural and strong solution. Expand your patient pool with an innovative solution. With the Straumann PURE Ceramic Implant, clinicians have an additional option to convince
More than pure esthetics. The natural and strong solution. Expand your patient pool with an innovative solution. With the Straumann PURE Ceramic Implant, clinicians have an additional option to convince
Changes in Crestal Bone Levels for Immediately Loaded Implants
 Changes in Crestal Bone Levels for Immediately Loaded Implants Roy H. Yoo, DMD 1 /Sung-Kiang Chuang, DMD, MD 2 /Mohammed S. Erakat, DMD 3 / Meghan Weed, BS 4 /Thomas B. Dodson, DMD, MPH 5 Purpose: The
Changes in Crestal Bone Levels for Immediately Loaded Implants Roy H. Yoo, DMD 1 /Sung-Kiang Chuang, DMD, MD 2 /Mohammed S. Erakat, DMD 3 / Meghan Weed, BS 4 /Thomas B. Dodson, DMD, MPH 5 Purpose: The
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Complication incidence of two implant systems up to six years: a comparison between internal and external connection implants
 Complication incidence of two implant systems up to six years: a comparison between internal and external connection implants Sung-Wook Chae 1, Young-Sung Kim 1,2, Yong-Moo Lee 3, Won-Kyung Kim 1, Young-Kyoo
Complication incidence of two implant systems up to six years: a comparison between internal and external connection implants Sung-Wook Chae 1, Young-Sung Kim 1,2, Yong-Moo Lee 3, Won-Kyung Kim 1, Young-Kyoo
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Replacement of missing teeth with
 A simple surgical technique to maximise prosthetic results Timothy Kosinski presents a technique to help minimise surgical risk, as well as helping the dentist to understand anatomy and proper implant
A simple surgical technique to maximise prosthetic results Timothy Kosinski presents a technique to help minimise surgical risk, as well as helping the dentist to understand anatomy and proper implant
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
An osseointegrated oral implant is characterized
 Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Comparative study of single-thread, double-thread, and triple-thread dental implant: a three-dimensional finite element analysis
 ISSN 1 746-7233, England, UK World Journal of Modelling and Simulation Vol. 3 (2007) No. 4, pp. 310-314 Comparative study of single-thread, double-thread, and triple-thread dental implant: a three-dimensional
ISSN 1 746-7233, England, UK World Journal of Modelling and Simulation Vol. 3 (2007) No. 4, pp. 310-314 Comparative study of single-thread, double-thread, and triple-thread dental implant: a three-dimensional
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
Cumulative survival rate of Astra Tech implants: a retrospective analysis
 Research Article Journal of Periodontal J Periodontal Implant Sci 2011;41:86-91 doi: 10.5051/jpis.2011.41.2.86 Cumulative survival rate of Astra Tech implants: a retrospective analysis Jung-Soo Kim 1,
Research Article Journal of Periodontal J Periodontal Implant Sci 2011;41:86-91 doi: 10.5051/jpis.2011.41.2.86 Cumulative survival rate of Astra Tech implants: a retrospective analysis Jung-Soo Kim 1,
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
Analysis of Short-term Success Rate and Healing Patterns of Implantium Implant
 Analysis of Short-term Success Rate and Healing Patterns of Implantium Implant Gyung-Joon Chae 1, Sung-Min Chung 2, Ui-Won Jung 1, Kyoo-Sung Cho 1, Jung-Kyu Chai 1, Chong-Kwan Kim 1, Seong-Ho Choi 1, and
Analysis of Short-term Success Rate and Healing Patterns of Implantium Implant Gyung-Joon Chae 1, Sung-Min Chung 2, Ui-Won Jung 1, Kyoo-Sung Cho 1, Jung-Kyu Chai 1, Chong-Kwan Kim 1, Seong-Ho Choi 1, and
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
RYAN J. DONOVAN UNIVERSITY OF FLORIDA
 CRESTAL BONE CHANGES AROUND IMPLANTS WITH A REDUCED ABUTMENT DIAMETER PLACED NON-SUBMERGED AND IN AT SUBCRESTAL POSITIONS: A 1-YEAR RADIOGRAPHIC EVALUATION By RYAN J. DONOVAN A THESIS PRESENTED TO THE
CRESTAL BONE CHANGES AROUND IMPLANTS WITH A REDUCED ABUTMENT DIAMETER PLACED NON-SUBMERGED AND IN AT SUBCRESTAL POSITIONS: A 1-YEAR RADIOGRAPHIC EVALUATION By RYAN J. DONOVAN A THESIS PRESENTED TO THE
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
ANTHOGYR IN-HOUSE DATA
 ANTHOGYR IN-HOUSE DATA Interim report on the axiom clinical study January 2010 Interim clinical evaluation of the axiom implant (dia. 4x10mm) : tissue stabilisation and maintenance of bone level 2 Introduction
ANTHOGYR IN-HOUSE DATA Interim report on the axiom clinical study January 2010 Interim clinical evaluation of the axiom implant (dia. 4x10mm) : tissue stabilisation and maintenance of bone level 2 Introduction
In the early years of modern implantology, the Brånemark
 Influence of Two Different Machined-Collar Heights on Crestal Bone Loss Mariano Herrero-Climent, MD, DDS, MSc, PhD 1 /Manuel María Romero Ruiz, MD, DDS, MSc 2 / Carmen María Díaz-Castro, DDS, MSc 3 /Pedro
Influence of Two Different Machined-Collar Heights on Crestal Bone Loss Mariano Herrero-Climent, MD, DDS, MSc, PhD 1 /Manuel María Romero Ruiz, MD, DDS, MSc 2 / Carmen María Díaz-Castro, DDS, MSc 3 /Pedro
The following resources related to this article are available online at jada.ada.org ( this information is current as of July 11, 2011):
 Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Astra Tech Implant System. Scientific Summary
 Astra Tech Implant System Scientific Summary Why we do what we do? Our vision of a world where everyone eats, speaks and smiles with confidence permeates and inspires everything we do. We believe in an
Astra Tech Implant System Scientific Summary Why we do what we do? Our vision of a world where everyone eats, speaks and smiles with confidence permeates and inspires everything we do. We believe in an
Immediate Loading of a Multi-Threaded Implant
 Immediate Loading of a Multi-Threaded Implant Dr. Jonathan Yahav, DDS (Northwestern University, Chicago, IL) Aye Myat, BS in Biological Sciences (University of Illinois at Chicago, Chicago IL) Khasim Ali
Immediate Loading of a Multi-Threaded Implant Dr. Jonathan Yahav, DDS (Northwestern University, Chicago, IL) Aye Myat, BS in Biological Sciences (University of Illinois at Chicago, Chicago IL) Khasim Ali
5 Professor and Chair, Department of Periodontics, Dental
 Biologic Width Around Different Implant-Abutment Interface Configurations. A Radiographic Evaluation of the Effect of Horizontal Offset and Concave Abutment Profile in the Canine Mandible Santiago J. Caram,
Biologic Width Around Different Implant-Abutment Interface Configurations. A Radiographic Evaluation of the Effect of Horizontal Offset and Concave Abutment Profile in the Canine Mandible Santiago J. Caram,
Research Article. ISSN (Print)
 Scholars Journal of Dental Sciences (SJDS) Sch. J. Dent. Sci., 2015; 2(2B):199-204 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources) www.saspublisher.com
Scholars Journal of Dental Sciences (SJDS) Sch. J. Dent. Sci., 2015; 2(2B):199-204 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources) www.saspublisher.com
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
CRESTAL BONE PRESERVATION WITH PLATFORM SWITCHING
 www.djas.co.in ISSN No-2321-1482 DJAS 4(III), 135-143, 2016 All rights are reserved REVIEW ARTICLE Dental JOURNAL of Advance Studies CRESTAL BONE PRESERVATION WITH PLATFORM SWITCHING 1 2 3 Manjit kumar,
www.djas.co.in ISSN No-2321-1482 DJAS 4(III), 135-143, 2016 All rights are reserved REVIEW ARTICLE Dental JOURNAL of Advance Studies CRESTAL BONE PRESERVATION WITH PLATFORM SWITCHING 1 2 3 Manjit kumar,
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized Balanced Occlusion
 Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Radiological assessment of peri-implant bone loss: a 12-month retrospective study.
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.3.e430 Radiological assessment of peri-implant bone loss: a 12-month retrospective study. AJ. Flichy-Fernández 1, J. Ata-Ali 2,
Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.3.e430 Radiological assessment of peri-implant bone loss: a 12-month retrospective study. AJ. Flichy-Fernández 1, J. Ata-Ali 2,
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Over the past few decades, an improved
 RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
The high clinical success rate of endosseous
 Clinical Evaluation of Short, Machined-Surface Implants Followed for 12 to 92 Months Georges Tawil, DDS, DSc.Od 1 /Roland Younan, DCD, DES 2 Purpose: Bone resorption following tooth loss often limits the
Clinical Evaluation of Short, Machined-Surface Implants Followed for 12 to 92 Months Georges Tawil, DDS, DSc.Od 1 /Roland Younan, DCD, DES 2 Purpose: Bone resorption following tooth loss often limits the
MARGINAL TISSUE RESPONSE TO DIFFERENT IMPLANT NECK DESIGN
 ORIGINAL ARTICLE DOI:10.4047/jkap.2008.46.6.602 MARGINAL TISSUE RESPONSE TO DIFFERENT IMPLANT NECK DESIGN Hanna Eun Kyong Bae 1, BDS, MDS, Moon-Kyu Chung 1, DDS, PhD, In-Ho Cha 2, DDS, PhD, Dong-Hoo Han
ORIGINAL ARTICLE DOI:10.4047/jkap.2008.46.6.602 MARGINAL TISSUE RESPONSE TO DIFFERENT IMPLANT NECK DESIGN Hanna Eun Kyong Bae 1, BDS, MDS, Moon-Kyu Chung 1, DDS, PhD, In-Ho Cha 2, DDS, PhD, Dong-Hoo Han
synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions
 synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions INTRODUCTION synocta Meso abutment for cement-retained restorations 1 The synocta Meso abutments, available
synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions INTRODUCTION synocta Meso abutment for cement-retained restorations 1 The synocta Meso abutments, available
Five-year retrospective radiographic follow-up study of dental implants with sandblasting with large grit, and acid etching-treated surfaces
 ORIGINAL ARTICLE http://dx.doi.org/.515/jkaoms.015.41.6.317 pissn 347550 eissn 345930 Fiveyear retrospective radiographic followup study of dental implants with sandblasting with large grit, and acid etchingtreated
ORIGINAL ARTICLE http://dx.doi.org/.515/jkaoms.015.41.6.317 pissn 347550 eissn 345930 Fiveyear retrospective radiographic followup study of dental implants with sandblasting with large grit, and acid etchingtreated
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Dentascan Evaluation of Hard Tissue Changes around Implants Placed in Healed Sockets: A Cross-sectional Study
 JDSOR ORIGINAL ARTICLE Dentascan Evaluation of Hard Tissue Changes around 10.5005/jp-journals-10039-1099 Implants Placed in Healed Sockets Dentascan Evaluation of Hard Tissue Changes around Implants Placed
JDSOR ORIGINAL ARTICLE Dentascan Evaluation of Hard Tissue Changes around 10.5005/jp-journals-10039-1099 Implants Placed in Healed Sockets Dentascan Evaluation of Hard Tissue Changes around Implants Placed
Dental Implant Treatment Planning and Restorative Considerations
 Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
