Social changes, evolution in dentistry, and changes
|
|
|
- Melvin Quinn
- 6 years ago
- Views:
Transcription
1 Naert 9/21/04 2:37 PM Page 695 A 10-year Randomized Clinical Trial on the Influence of Splinted and Unsplinted Oral Implants Retaining Mandibular Overdentures: Peri-implant Outcome Ignace Naert, DDS, PhD 1 /Ghada Alsaadi, DDS 2 /Daniel van Steenberghe, MD, DDS, PhD, Dr hc 3 / Marc Quirynen, DDS, PhD 4 Purpose: This randomized controlled clinical trial aimed to evaluate the efficacy of splinted implants versus unsplinted implants in overdenture therapy over a 10-year period. Materials and Methods: The study sample comprised 36 completely edentulous patients, 17 men and 19 women (mean age 63.7 years). In each patient, 2 implants (Brånemark System, Nobel Biocare, Göteborg, Sweden) were placed in the interforaminal area. Three to 5 months after placement, they were connected to standard abutments. The patients were then rehabilitated with ball-retained overdentures, magnet-retained overdentures, or bar-retained overdentures (the control group). Patients were followed for 4, 12, 60, and 120 months post abutment connection. Group means as well as linear regression models were fitted with attachment type and time as classification variables and corrected for simultaneous testing (Tukey). Results: After 10 years, 9 patients had died and 1 was severely ill. Over 10 years, no implants failed. Mean Plaque Index, Bleeding Index, change in attachment level, Periotest values, and marginal bone level at the end of the follow-up period were not significantly different among the groups. Discussion: The annual marginal bone loss, excluding the first months of remodeling, was comparable with that found around healthy natural teeth. Conclusion: The fact that no implants failed and that overall marginal bone loss after the first year of bone remodeling was limited suggested that implants in a 2- implant mandibular overdenture concept have an excellent prognosis in this patient population, irrespective of the attachment system used. INT J ORAL MAXILLOFAC IMPLANTS 2004;19: Key words: dental implants, dental prostheses 1 Chairman, Department of Prosthetic Dentistry/BIOMAT Research Group, School of Dentistry, Oral Pathology and Maxillofacial Surgery, Faculty of Medicine, Catholic University of Leuven, Leuven, Belgium. 2 Master Student, Department of Prosthetic Dentistry, School of Dentistry, Oral Pathology and Maxillofacial Surgery, Faculty of Medicine, Catholic University of Leuven, Leuven, Belgium. 3 Chairman, Department of Periodontology, School of Dentistry, Oral Pathology and Maxillofacial Surgery, Faculty of Medicine, Catholic University of Leuven, Leuven, Belgium; P-I Brånemark Chair, School of Dentistry, Oral Pathology and Maxillofacial Surgery, Faculty of Medicine, Catholic University of Leuven, Leuven, Belgium. 4 Professor, Department of Periodontology, School of Dentistry, Oral Pathology and Maxillofacial Surgery, Faculty of Medicine, Catholic University of Leuven, Leuven, Belgium. Correspondence to: Prof I. Naert, Department of Prosthetic Dentistry/BIOMAT Research Group, School of Dentistry, Oral Pathology and Maxillofacial Surgery, Faculty of Medicine, Catholic University of Leuven (K.U. Leuven), Kapucijnenvoer, 7, B-3000 Leuven, Belgium. Fax: Ignace.Naert@med.kuleuven.ac.be Social changes, evolution in dentistry, and changes in prosthetic techniques have led to higher patient expectations regarding esthetics, function, and oral comfort. This is also the case for completely edentulous patients. 1,2 However, the main problem with the mandibular complete denture is lack of stability, since the resorption degree of jawbone is about 4 times that of the maxilla. 3 Jemt and associates 4 were among the first to report on the possibility of using overdentures supported by 2 implants to improve mandibular denture retention. Studies have been carried out over the last 2 decades to evaluate the benefits of implant-supported overdenture therapy. It has already been established, through medium- to long-term studies, that the survival of root-form titanium implants is very high in mandibular overdenture therapy. 5 13, magnet, and ball attachments and rigid and The International Journal of Oral & Maxillofacial Implants 695
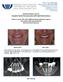
2 Naert 9/21/04 2:37 PM Page 696 Table 1 Variables Among the 3 Groups nonrigid telescopic copings have been used to retain mandibular overdentures. The type of attachment influences the retention and stability of the denture. 14 A few studies have compared the clinical outcomes of splinted and unsplinted attachment systems. 9,15 18 None of these studies lasted more than 5 years, and none except that of Naert and colleagues 9 reported on the efficacy of the treatment according to a randomized controlled design. This study aimed to evaluate the effectiveness of splinted and unsplinted implants retaining a mandibular overdenture over a 10-year period. MATERIALS AND METHODS Mean age (y) Gender (male/female) 7/5 5/7 5/7 Mean period of edentulism (y) Mean bone height in the canine region (mm) Bone quality* Class Class Bone quality* Class A Class B Class C Class D *No. of patients in each class. There were no significant differences for the variables tested between the 3 groups (P.05). Patient Selection and Implants Thirty-six completely edentulous patients (19 women and 17 men; mean age, 63.7 years; range, 36 to 85 years) were selected for this study. The population represented a consecutive group of patients treated at the University Hospitals, Catholic University of Leuven, Belgium. Exclusion criteria were insufficient bone volume to place 2 implants with a minimum length of 10 mm, saggital mandibular retrusion, psychologic problems with the acceptance of a conventional removable denture, gagging reflexes, less than 1 year of edentulism in the mandible, the absence of a maxillary complete denture, and administrative or physical considerations that would seriously affect the surgical procedure or constitute a hindrance for longitudinal follow-up. Functional problems were the main reason that patients presented for treatment. The patients complained about lack of retention or stability of their existing mandibular dentures, which, from a technical point of view, were deemed to be well made. At the inception, all patients underwent an initial examination, including recording of their medical and dental histories and evaluation of their existing dentures. Each patient was provided with 2 turned, screw-type implants made of commercially pure titanium (Brånemark System, Nobel Biocare, Göteborg, Sweden) in the mandibular left and right canine areas. 19 The periodontist used a drill template to assist placement in prosthetically optimal locations. Surgical treatment was performed according to a standard technique. 20 Jawbone quality and degree of jawbone resorption were evaluated by the surgeon at the time of implant placement. Bone height in the canine regions was assessed on panoramic radiographs. The alveolar crest was also evaluated tactilely during drilling. Assessment of the alveolar crest both radiographically and clinically facilitated classification according to the Lekholm and Zarb index. 21 Abutment Connection and Loading Three to five months after implant placement, transmucosal standard abutments (Brånemark System; Nobel Biocare) were connected. The final length of the abutment was selected at the time of impression making. The tops of the abutments were 1 to 2 mm above the mucosal margin. Before prosthesis fabrication, a randomized procedure allocated the 36 patients into 3 groups of equal size, each with a different attachment system. The characteristics of the 3 patient groups are shown in Table 1. The bar group (Fig 1a) was considered the reference or control group. Patients in this group were provided with an egg-shaped Dolder bar (Cendres et Métaux, Biel, Switzerland) splinting the 2 implants. In the magnet group (Fig 1b), 2 openfield magnets (art. no 1102; Dyna Engineering BV, Bergen op Zoom, The Netherlands) were used as the attachment system. In the ball group (Fig 1c), 2 ball attachments (art. no. SDCB ; Nobel Biocare) retained the overdenture. All overdentures were carefully evaluated for occlusion and articulation on an articulator and intraorally. The aim was to achieve a balanced occlusion without anterior tooth contact in centric relation. The interabutment distance ranged from 12 to 29 mm (mean 19.5 mm), depending on the jaw size and anatomy. Follow-up Patients were examined at the time of abutment connection and at follow-up visits 4, 12, 60, and 120 months after abutment connection. At each follow-up visit several peri-implant parameters were recorded: 696 Volume 19, Number 5, 2004
3 Naert 9/21/04 2:37 PM Page 697 Figs 1a to 1c Clinical views of (a) the ovoid bar, (b) the open-field magnets, and (c) the ball attachments used with their corresponding overdentures. a b c Using the Plaque Index (PI), the presence or absence of plaque at the abutment was scored at 4 sites (mesiobuccal, mesiolingual, distobuccal, and distolingual) by visual inspection (0 = no plaque, 4 = plaque on all surfaces of one implant, and 8 = plaque on all surfaces of both implants). The 8 subscores for each patient were used to calculate the patient s final mean score. The final scores varied from 0 (no plaque on both implants) to 1 (plaque on all surfaces of both implants). The bleeding tendency of the soft tissue surrounding the abutments was assessed at the same 4 sites by gently running a Merritt-B periodontal probe (Hu-Friedy; B. Ofrictin, Heidelberg, Germany) 1 mm into the gingival sulcus strictly parallel with the axial wall of the abutment. The Bleeding Index (BI) was used to assess bleeding (0 = no bleeding, 1 = bleeding on all surfaces of both implants). If bleeding became visible within 20 seconds, a BI score was given. Probing pocket depth was measured with a Merritt-B periodontal probe (Fig 2). Six measurements were made for each implant. For the bar group, the bar was removed each time. 22 Recession, defined as the distance between the top of the abutment and the margin of the soft tissue (Fig 2), was simultaneously measured at the same 6 sites assessed for PPD. 22 Fig 2 Diagram of the peri-implant parameters. IAJ = implantabutment junction; REC = recession (ie, the distance between the top of the abutment and the margin of the soft tissue); PPD = probing pocket depth; AL = attachment level (ie, the distance between the IAJ and the tip of the periodontal probe inserted into the pocket, calculated by the formula AL = [PPD + REC] abutment length); MBL = marginal bone level (ie, the distance between the marginal bone level and the IAJs measured on longcone radiographs). Adapted from Quirynen and associates 22 by permission of the author. The International Journal of Oral & Maxillofacial Implants 697
4 Naert 9/21/04 2:37 PM Page 698 Attachment level was calculated using the formula: (probing pocket depth + recession) abutment length. Negative values indicated that the tip of the probe did not reach the implant-abutment junction, which indicated the clinical attachment level of the abutment. 22 The rigidity of the implant-bone continuum was systematically assessed at each follow-up visit by means of a Periotest device (Siemens, Bensheim, Germany). This device measures the damping capacity of the implant-bone continuum. It consists of a handpiece connected to a unit that analyses the bracing time of a rod applied to a surface. 23 The values were only accepted when 2 consecutive measurements did not deviate more than 1 unit from each other. Periotest values can range from 8 (very stable) to +50 (very mobile). The marginal bone level was measured mesially and distally for each implant on intraoral radiographs. The radiographs were made with a parallel long-cone technique, which allowed standardization of consecutive radiographs. 24 The reference was set at the implant-abutment junction (Fig 2). A digital-sliding caliper with an accuracy of 0.01 mm (Mitutoyo, Tokyo, Japan) was used for the measurements at a 4 magnification. Radiographic follow-up of marginal bone level changes between baseline and 1, 5, and 10 years postloading, was performed for both implants in each patient. As the patient was considered a statistical unit, the mean marginal bone level of 2 implants was calculated. The intraexaminer variability of radiographically determined bone height scores was 0.2 mm [SE = 0.07 and SD = 0.42]. 9 Baseline for PI, BI, and attachment level was defined at 4 months post abutment connection, while the baseline for marginal bone level and the Periotest values was set at the time of abutment connection. To investigate the correlation between BI and marginal bone loss, the baseline marginal bone level was considered 4 months post abutment connection, not at abutment connection. To explore the correlation between attachment level and marginal bone level, only proximal measurements were used (ie, buccal and lingual site measurements were excluded). Again, 4 months post abutment connection was used as the baseline for both marginal bone level and attachment level in this instance. Implant Failure An implant was considered a failure if A peri-implant radiolucency could be detected on the intraoral radiographs. An individual implant showed the slightest signs of mobility, corresponding to a Periotest value of +5. The patient showed subjective signs of pain or infection that prompted implant removal. Attachment and marginal bone levels were not used as success criteria but rather to determine prognosis. Statistical Analysis Attachment types and elapsed time were inserted into a linear mixed model (PROC MIXED) as classification variables. The model incorporated a compound symmetric error structure model for observations of the same patient over time and to correct for confounding variables. Compound symmetry means that correlations between the observations of same patient are considered the same; the difference in time is disregarded. P values for comparisons between group means were adjusted for simultaneous hypothesis testing according to the Tukey method for multiple comparisons. Correlation coefficients and linear regression models (PROC REG) were fitted to the data as well. P values indicated whether the null hypothesis of no linear relation between the 2 variables under consideration had been refuted. The overall threshold for significance ( ) was set at.05 to detect the level of significance. The box-and-whisker plot design was bounded by the following values: the full horizontal line in the box represented the mean; the dashed line, the median; the rectangle stretches, from the 25th to the 75th percentile (the 25th percentile is the value that is at which 25% of the observations are smaller than that value, the 75th percentile is that value of which 75% of the observations are smaller). The lines extending the rectangle are called the whiskers. They are considered to represent all values that are not outliers. An outlier is defined as a value larger than the 75th percentile (75th percentile 25th percentile) or smaller than the 25th percentile 1.5 (75th percentile 25th percentile). Hence, the whiskers extend to the farthest data point that still lies in the interval bounded by these 2 formulas. SAS Version 8 for Windows was used (SAS Institute, Cary, NC). Graphing was done using R version Volume 19, Number 5, 2004
5 Naert 9/21/04 2:37 PM Page PI change 0.0 BI change Fig 3 Box-and-whisker plot for PI changes from the baseline at years 1, 5, and 10 for the 3 different groups. Fig 4 Box-and-whisker plot for BI changes from the baseline at years 1, 5, and 10 for the 3 different groups. RESULTS Patient Dropout Because of the randomization procedure, patient characteristics between the 3 different groups did not significantly differ from one another. The reasons for patient dropout at year 10 are presented in the Discussion section. The remaining 26 patients respected the follow-up schedule over the entire 10- year period. Implant Outcome Overall, 73 implants were placed; 54 were standard 3.75-mm-wide implants, 2 were standard 5-mmwide implants, and the remaining 17 were self-tapping implants 3.75 mm wide. Implants of various lengths (10, 13, 15, 18, and 20 mm) were used (for details see Naert and associates 9,25 ). None of the implants failed during the observation period. One failed at the time of abutment surgery and was replaced by a new one, which healed uneventfully. Peri-implant Outcome The mean PI scores at year 10 were 0.39 for the bar group, 0.31 for the magnet group, and 0.18 for the ball group. There was no significant difference between the 3 groups over time. However, a significant decrease in PI appeared at year 10 compared to year 5 when the 3 groups were taken together (P =.02). The mean PI changes between baseline and year 10 were 0.13 for the bar group, 0.17 for the magnet group, and 0 for the ball group (Fig 3). These values were not significantly different from each other. The mean BI scores at year 10 were 0.41 for the bar group, 0.21 for the magnet group, and 0.11 for ball group. The BI changes from baseline to 1 year, 5 years, and 10 years for the 3 groups are shown in Fig 4. The mean BI changes between year 10 and baseline were for the bar group, 0.09 for the magnet group, and 0.15 for the ball group. Neither the BI over time nor the changes from baseline was significantly different between the 3 groups. The mean attachment level changes between baseline and years 1, 5, and 10, for the 3 groups are shown in Fig 5. No significant differences in mean attachment level changes between the 3 groups over time were found (P.05). The mean attachment level changes between baseline and year 10 were 1.07 mm for the bar group, 0.1 mm for the magnet group, and 1.13 mm for the ball group. Figure 6 reveals the Periotest score changes between baseline and years 1, 5, and 10 for the 3 different groups. No significant differences were found between the 3 groups over time. However, mean Periotest values at year 10 were significantly lower than those measured at the baseline in all 3 groups (P.001). The mean Periotest value at year 10 for the 3 groups together was 5.2, and the mean difference between baseline and year 10 was 1.7. Table 2 shows that there was a slight marginal bone loss over time. The changes in marginal bone level between baseline (abutment connection) and years 1, 5, and 10 for the 3 different groups are shown in Fig 7. No significant differences between the 3 groups were found over time (P =.1). The mean marginal bone level was located significantly more apically at years 1, 5, and 10 than at baseline (P.001). The mean marginal bone loss between baseline and year 10 was 1.15 mm for the bar group, 0.53 mm for the magnet group, and 0.9 mm for the ball groups. No significant differences were found The International Journal of Oral & Maxillofacial Implants 699
6 Naert 9/21/04 2:37 PM Page 700 Attachment level change (mm) Periotest value change Fig 5 Box-and-whisker plot for attachment level changes from the baseline at years 1, 5, and 10 for the 3 different groups. Six sites per patient were measured. Fig 6 Box-and-whisker plot for Periotest value changes from the baseline at years 1, 5, and 10 for the 3 different groups. Table 2 Frequency Distribution of Bone Loss Categories at Year 5 and 10* No. of implants Bone loss (mm?) Year 5 Year to to to to > *Data per individual implant. between the 3 groups. Excluding the first year of bone remodeling, marginal bone loss was 0.53 mm for the bar group, 0.32 mm for the magnet group, and 0.29 mm for the ball group. A linear regression did not show correlation between the BI and the marginal bone loss over the 10-year period when the 3 groups were taken together (P =.77). A linear regression for attachment level for distal and mesial sites (4 sites) and marginal bone level over time is presented in Fig 8. A significant correlation (P =.004) was found between both parameters (correlation coefficient = 0.36). DISCUSSION A total of 10 patients (27.7%) dropped out. Nine patients died, and 1 was unable to complete 10 years of follow-up because of severe illness. This might be predictable for a prospective study in which the mean age at the time of patient inception was quite high (63.7 years). No implant failures occurred after loading; this corroborates the preliminary and the 5-year data of the same study population. 9,25 The mean PI and BI scores and the attachment level data were not significantly different between groups. Karabuda and associates 26 found no significant difference between the bar and ball attachment types used for implant-supported overdentures with respect to soft tissue health. 27 They reported a 100% survival rate for 2 implants supporting a mandibular overdenture with ball or bar attachment for 5 years. No differences in marginal bone loss were observed either bar and ball attachments. In the current study, a remarkable significant decrease in mean PI scores was seen at year 10 compared to year 5. The reason for this outcome remains speculative. No correlation was found between bleeding tendency and marginal bone loss. This is in agreement with previous observations made at the University of Leuven. 28,29 However, a significant correlation was observed between the attachment level and the marginal bone level. This follows previous observations reporting correlation coefficients of 0.6 and 0.7, respectively. 5,28,30 The overall annual bone loss up to year 10, excluding the first months of remodeling, was nearly 0.04 mm; this corroborates previous results as well. 5,28,31 This value is comparable with the annual bone loss around healthy natural teeth 32 and falls within the criteria for implant success suggested by Albrektsson and colleagues. 33 The mean Periotest values were not significantly different between the 3 different groups, but a decrease in Periotest values over time was observed, which is in agreement with previous observations. 9,34 36 This might be explained by an increase in bone contact and mineralization with time at loaded implant-bone interfaces, as has been demonstrated radiographically Volume 19, Number 5, 2004
7 Naert 9/21/04 2:37 PM Page 701 Bone level change (mm) Fig 7 Box-and-whisker plot for marginal bone level changes from the baseline at years 1, 5, and 10 for the 3 different groups. Fig 8 Linear regression for attachment level and marginal bone level over time at mesial and distal sites only (P =.004). In an in vitro study, Tokuhisa and coworkers 37 compared the load transfer between the 3 attachment systems (bar, magnet, and ball) retaining a mandibular overdenture. They reported that the bar attachment induced the greatest axial force and bending moment on both the loading- and non loading-side implants, and the ball attachment the least. This contradicts the present clinical in vivo findings. CONCLUSIONS From this 10-year randomized controlled clinical trial involving 36 edentulous patients, several conclusions can be formulated. The implant-retained overdenture supported by 2 implants in the mandible had a success rate of 100% for loaded implants. The peri-implant clinical parameters differed only slightly between splinted and unsplinted implants retaining mandibular overdentures. Excluding the first year of bone remodeling, the overall annual marginal bone loss was less than 0.04 mm. No correlation was found between bleeding on probing and marginal bone loss during the 10-year period. Although the Periotest value was not significantly different between the 3 groups, the boneimplant rigidity increased over time. ACKNOWLEDGMENTS The authors thank Nobel Biocare, Göteborg, Sweden, for providing the ball attachments, Dyna Engineering, and Bergen of Zoom, The Netherlands, for the magnet attachments. REFERENCES 1. Vigild M. Benefit related assessment of treatment need among institutionalised elderly people. Gerodontology 1993;10: Zarb GA, Schmitt A. Implant prosthodontic treatment options for the edentulous patient. J Oral Rehabil 1995;22: Tallgren A. The continuing reduction of the residual alveolar ridges in complete denture wearers: A mixed-longitudinal study covering 25 years. J Prosthet Dent 1972;27: Stålblad PÅ, Jansson T, Zarb G. Osseointegration in overdenture therapy. Preliminary comments. In: Prosthetic Reconstructions on Osseointegrated Implants [Proceedings of the Gothenburg Conference, Sept 1983.] Swed Dent J 1985;9(suppl 28): Quirynen M, Naert I, van Steenberghe D, Teerlinck J, Dekeyser C, Theuniers G. Periodontal aspects of osseointegrated fixtures supporting an overdenture. A 4-year retrospective study. J Clin Periodontol 1991;18: Mericske-Stern R, Steinlin Schaffner T, Marti P, Geering AH. Peri-implant mucosal of ITI implants supporting overdentures. A five-year longitudinal study. Clin Oral Implants Res 1994;5: Makkonen TA, Holmberg S, Niemi L, Olsson C, Tammisalo T, Peltola J. A 5-year prospective clinical study of Astra Tech dental implants supporting fixed bridges or overdentures in the edentulous mandible. Clin Oral Implants Res 1997;8: Naert I, Hooghe M, Quirynen M, van Steenberghe D. The reliability of implant-retained hinging overdentures for the fully edentulous mandible. An up to 9-year longitudinal study. Clin Oral Investig 1997;1: Naert I, Gizani S, Vuylsteke M, van Steenberghe D. A 5- year randomized clinical trial on the influence of splinted and unsplinted oral implants in the mandibular overdenture therapy. Part I: Peri-implant outcome. Clin Oral Implants Res 1998;9: Jemt T, Chai J, Harnett J, et al. A 5-year prospective multicenter follow-up report on overdentures supported by osseointegrated implants. Int J Oral Maxillofac Implants 1996;11: The International Journal of Oral & Maxillofacial Implants 701
8 Naert 9/21/04 2:37 PM Page Walmsley AD, Frame JW. Implant supported overdentures The Birmingham experience. J Dent 1997;25(suppl 1):S43 S Meijer HJA, Raghoebar GM, van t Hof MA, Geetman ME, van Oort RP. Implant-retained mandibular overdentures compared with complete dentures; A 5-years follow-up study of clinical aspects and patient satisfaction. Clin Oral Implants Res 1999;10: Meijer HJ, Geertman ME, Raghoebar GM, Kwakman JM. Implant-retained mandibular overdentures: 6-year results of a multicenter clinical trial on 3 different implant systems. J Oral Maxillofac Surg 2001;59: Davis DM, Packer ME. The maintenance requirements of mandibular overdentures stabilized by Astra Tech implants using three different attachment mechanisms balls, magnets, and bars; 3-year results. Eur J Prosthodont Restorative Dent 2000;8: Mericske-Stern R. Clinical evaluation of overdenture restorations supported by osseointegrated titanium implants: A retrospective study. Int J Oral Maxillofac Implants 1990;5: Bergendal T, Engquist B. Implant-supported overdentures: A longitudinal prospective study. Int J Oral Maxillofac Implants 1998;13: Oetterli M, Kiener P, Mericske-Stern R. A longitudinal study on mandibular implants supporting an overdenture: The influence of retention mechanism and anatomic-prosthetic variables on periimplant parameters. Int J Prosthodont 2001;14: Von Wowern N, Gotfredsen K. Implant-supported overdentures, a prevention of bone loss in edentulous mandibles? A 5-year follow-up study. Clin Oral Implants Res 2001;12: Naert I, De Clercq M, Theuniers G, Schepers E. Overdentures supported by osseointegrated fixtures for the edentulous mandible: A 2.5-year report. Int J Oral Maxillofac Implants 1988;3: Adell R, Lekholm U, Brånemark P-I. Surgical procedures. In: Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue- Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, 1985: Lekholm U, Zarb GA. Patient selection and preparation. In Brånemark P-I, Zarb GA, Albrektsson T. Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence,1985: Quirynen M, Naert I, van Steenberghe D, Duchateau L, Darius P. Periodontal aspects of Brånemark and IMZ implants supporting overdentures. A comparative study. In: Laney WR, Tolman DE (eds). Proceedings of the Second International Congress on Tissue Integration in Oral Orthopaedic and Maxillofacial Reconstruction, Sept 1990, Rochester, MN. Chicago: Quintessence, 1992: Schulte W, d Hoedt B, Lukas D, Maunz M, Steppeler M. Periotest measuring periodontal characteristics Correlation with periodontal bone loss. J Periodontal Res 1992;27: Strid KG. Radiographic procedures. In: Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, 1985: Naert I, Quirynen M, Hooghe M, van Steenberghe D. A comparative prospective study of splinted and unsplinted Brånemark implants in mandibular overdenture therapy: A preliminary report. J Prosthet Dent 1994;71: Karabuda C, Tosun T, Ermis E, Ozdemir T. Comparison of 2 retentive systems for implant-supported overdentures: Soft tissue management and evaluation of patient satisfaction. J Periodontol 2002;73: Gotfredsen K, Holm B. Implant-supported mandibular overdentures retained with ball or bar attachments: A randomized prospective 5-year study. Int J Prosthodont 2000; 13: Quirynen M, van Steenberghe D, Jacobs R, Schotte A, Darius P. The reliability of pocket probing around screw-type implants. Clin Oral Implants Res 1991;2: Quirynen M, Naert I, van Steenberghe D, Nys L. A study of 589 consecutive implants supporting complete fixed prostheses. Part I: Periodontal aspects. J Prosthet Dent 1992;68: Kelly GP, Cain RJ, Knowles JW, et al. Radiographs in clinical periodontal trials. J Periodontol 1975;46: Behneke A, Behneke N, d Hoedt B. A 5-year longitudinal study of the clinical effectiveness of ITI solid-screw implants in the treatment of mandibular edentulism. Int J Oral Maxillofac Implants 2002;17: Lavstedt S, Bolin A, Henrikson CO. Proximal alveolar bone loss in a longitudinal radiographic investigation. II. A 10- year follow-up study of an epidemiologic material. Acta Odontol Scand 1986;44: Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: A review and proposed criteria of success. Int J Oral Maxillofac Implants 1986;1: Teerlinck J, Quirynen M, Darius P, van Steenberghe D. Periotest: An objective clinical diagnosis of bone apposition toward implants. Int J Oral Maxillofac Implants 1991;6: van Steenberghe D, Tricio J, Naert I, Nys M. Damping characteristics of bone-to-implant interfaces. A clinical study with the Periotest device. Clin Oral Implants Res 1995;6: Tricio J, van Steenberghe D, Rosenberg D, Duchateau L. Implant stability related to insertion torque force and bone density: An in vitro study. J Prosthet Dent 1995;74: Tokuhisa M, Matsushita Y, Koyano K. In vitro study of a mandibular implant overdenture retained with ball, magnet, or bar attachments: Comparison of load transfer and denture stability. Int J Prosthodont 2003;16: Volume 19, Number 5, 2004
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report
 Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
REVIEWS. 10 Stomatologija, Baltic Dental and Maxillofacial Journal, 2008, Vol. 10, No. 1 SUMMARY
 Maxillary complete denture outcome with two-implant supported mandibular overdentures. A systematic review Vygandas Rutkunas, Hiroshi Mizutani, Vytaute Peciuliene, Ruta Bendinskaite, Tomas Linkevicius
Maxillary complete denture outcome with two-implant supported mandibular overdentures. A systematic review Vygandas Rutkunas, Hiroshi Mizutani, Vytaute Peciuliene, Ruta Bendinskaite, Tomas Linkevicius
Rehabilitation of an Edentulous Patient with Implant Supported Overdenture
 10.5005/jp-journals-10031-1036 CASE REPORT Rehabilitation of an Edentulous Patient with Implant Supported Overdenture Swapnali Mhatre, Sabita M Ram, Janani Mahadevan, Malika Karthik ABSTRACT The conventional
10.5005/jp-journals-10031-1036 CASE REPORT Rehabilitation of an Edentulous Patient with Implant Supported Overdenture Swapnali Mhatre, Sabita M Ram, Janani Mahadevan, Malika Karthik ABSTRACT The conventional
An osseointegrated oral implant is characterized
 Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate Loading Protocol: An In-Vivo Study
 J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
The use of two interforaminal implants to retain/
 Immediate Loading of Unsplinted Implants in the Anterior Mandible for Overdentures: 3-Year Results Phillip Roe, DDS, MS 1 /Joseph Y. K. Kan, DDS, MS 2 / Kitichai Rungcharassaeng, DDS, MS 3 /Jaime L. Lozada,
Immediate Loading of Unsplinted Implants in the Anterior Mandible for Overdentures: 3-Year Results Phillip Roe, DDS, MS 1 /Joseph Y. K. Kan, DDS, MS 2 / Kitichai Rungcharassaeng, DDS, MS 3 /Jaime L. Lozada,
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation
 The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
At present, there are several
 CLINICAL USE OF NEW MAGNETIC ATTACHMENTS FOR IMPLANT-SUPPORTED OVERDENTURES Takehiro Fujimoto, DDS, PhD Atsushi Niimi, DDS, DMSc Itsuki Murakami, DDS, MS, PhD Minoru Ueda, DDS, PhD KEY WORDS Brånemark
CLINICAL USE OF NEW MAGNETIC ATTACHMENTS FOR IMPLANT-SUPPORTED OVERDENTURES Takehiro Fujimoto, DDS, PhD Atsushi Niimi, DDS, DMSc Itsuki Murakami, DDS, MS, PhD Minoru Ueda, DDS, PhD KEY WORDS Brånemark
Mandibular Implant-Retained Overdentures with two Different Implant Designs. Ibrahim R. Eltorky
 Mandibular Implant-Retained Overdentures with two Different Implant Designs Ibrahim R. Eltorky Associate professor of Prosthodontics, Faculty of Dentistry, Tanta University, Egypt. ibrahim_eltorky@yahoo.com
Mandibular Implant-Retained Overdentures with two Different Implant Designs Ibrahim R. Eltorky Associate professor of Prosthodontics, Faculty of Dentistry, Tanta University, Egypt. ibrahim_eltorky@yahoo.com
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction
 Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction Corina-Marinela Cristache 1, Ionela-Ruxandra Sfeatcu 2, Mihai Burlibaºa 3, Gheorghe Cristache
Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction Corina-Marinela Cristache 1, Ionela-Ruxandra Sfeatcu 2, Mihai Burlibaºa 3, Gheorghe Cristache
Mandibular implant-supported hybrid prostheses
 Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
JOMI on CD-ROM, 1990 Mar ( ): The Applicability of Osseointegrated Oral Imp
 The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
Fixed Partial Dentures /FPDs/, Implant Supported. in implant prosthodontics
 Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants
 The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Evaluation of supported overdenture by implant and magnet
 * * 26 Evaluation of supported overdenture by implant and magnet Arab H.R * Assistant Professor, Dep. Of Periodontics, School of Dentistry, Mashhad University of Medical Sciences, Mashhad, Iran. Tamizi
* * 26 Evaluation of supported overdenture by implant and magnet Arab H.R * Assistant Professor, Dep. Of Periodontics, School of Dentistry, Mashhad University of Medical Sciences, Mashhad, Iran. Tamizi
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers
 Original Article The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers Emre Mumcu, Hakan Bilhan and Onur Geckili Department
Original Article The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers Emre Mumcu, Hakan Bilhan and Onur Geckili Department
Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants
 Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants Alan B. Carr, DMD, MS 1 /Yong-Geun Choi, DDS, MPH, MPH 2 / Steven E. Eckert, DDS, MS 1 /Ronald P. Desjardins, DMD, MS 3
Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants Alan B. Carr, DMD, MS 1 /Yong-Geun Choi, DDS, MPH, MPH 2 / Steven E. Eckert, DDS, MS 1 /Ronald P. Desjardins, DMD, MS 3
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Saudi Journal of Oral and Dental Research. DOI: /sjodr. ISSN (Print) Dubai, United Arab Emirates Website:
 DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
Fixed full-arch implant-supported acrylic resin prostheses
 Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
The evaluation of long-term treatment results for
 Long-Term Results After Placement of Dental Implants: Longitudinal Study of 1,964 Implants over 16 Years Nicole Noack, MD*/Jürgen Willer, DMD**/Jürgen Hoffmann, MD, DMD*** In a retrospective study, Kaplan-Meier
Long-Term Results After Placement of Dental Implants: Longitudinal Study of 1,964 Implants over 16 Years Nicole Noack, MD*/Jürgen Willer, DMD**/Jürgen Hoffmann, MD, DMD*** In a retrospective study, Kaplan-Meier
Overdenture: A Way of Preventive Prosthodontics
 CASE REPORT Overdenture: A Way of Preventive Prosthodontics Gorakhnath B Shinde 1 and Wadkar AP 2 Quick Response Code ABSTRACT: doi:... 1 Post Graduate Student 2 Professor and PG Guide Department of Prosthodontics
CASE REPORT Overdenture: A Way of Preventive Prosthodontics Gorakhnath B Shinde 1 and Wadkar AP 2 Quick Response Code ABSTRACT: doi:... 1 Post Graduate Student 2 Professor and PG Guide Department of Prosthodontics
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
STABILITY OF IMPLANTS AND NATURAL TEETH MONTHS OF FUNCTION AS DETERMINED BY THE PERIOTEST OVER 60 CLINICAL
 CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2011.3.4.190 A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis In-Ho Kang,
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2011.3.4.190 A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis In-Ho Kang,
University of Groningen
 University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
EMG activity of the masseter muscle in implant supported overdenture wearers during chewing of hard and soft food
 Journal of Oral Rehabilitation 2002 29; 986 991 EMG activity of the masseter muscle in implant supported overdenture wearers during chewing of hard and soft food H. C. KARKAZIS Department of Removable
Journal of Oral Rehabilitation 2002 29; 986 991 EMG activity of the masseter muscle in implant supported overdenture wearers during chewing of hard and soft food H. C. KARKAZIS Department of Removable
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study
 A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized Balanced Occlusion
 Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
 C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function
 Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
While the protocol for direct bone-to-implant
 Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
The biologic predictability of dental implants has
 Prosthetic Complications with Dental Implants: From an Up-to-8-year Experience in Private Practice Rabah Nedir, DMD 1 /Mark Bischof, DMD 2 /Serge Szmukler-Moncler, DMD, PhD 3 / Urs C. Belser, DMD 4 /Jacky
Prosthetic Complications with Dental Implants: From an Up-to-8-year Experience in Private Practice Rabah Nedir, DMD 1 /Mark Bischof, DMD 2 /Serge Szmukler-Moncler, DMD, PhD 3 / Urs C. Belser, DMD 4 /Jacky
There is overwhelming evidence that implant-retained
 CLINICAL Two-Year Success Rate of Implant-Retained Mandibular Overdentures by Novice General Dentistry Residents Hans Malmstrom, DDS 1 * Jin Xiao, DDS, MS, PhD 1 Georgios Romanos, DDS, PhD 1,2 Yan-Fang
CLINICAL Two-Year Success Rate of Implant-Retained Mandibular Overdentures by Novice General Dentistry Residents Hans Malmstrom, DDS 1 * Jin Xiao, DDS, MS, PhD 1 Georgios Romanos, DDS, PhD 1,2 Yan-Fang
Prosthetic RehabilitationofaPatientwithAlzheimersDiseaseusingaCombinedBallBarandClipRetainedImplantSupportedOverdentureA Case Report
 Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
(Assist. Prof), Dept. Of Prosthodontics, Govt. Dental College Thiruvananthapuram(Kerala).India
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. IV (February. 2017), PP 95-99 www.iosrjournals.org A Simple Technique to Rehabilitate
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 2 Ver. IV (February. 2017), PP 95-99 www.iosrjournals.org A Simple Technique to Rehabilitate
Radiographic Stent for Simplified Placement of Implants in the Mandible
 10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
The clinical use of endosseous implants has
 A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Uppers are from Mars, Lowers from Venus Clarifying Overdentures
 Uppers are from Mars, Lowers from Venus Clarifying Overdentures M. Nader Sharifi, D.D.S., M.S. Thomas P. Hinman Dental Meeting Atlanta, GA March 23, 2017 About Your Speaker: M. Nader Sharifi, D.D.S., M.S.
Uppers are from Mars, Lowers from Venus Clarifying Overdentures M. Nader Sharifi, D.D.S., M.S. Thomas P. Hinman Dental Meeting Atlanta, GA March 23, 2017 About Your Speaker: M. Nader Sharifi, D.D.S., M.S.
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Etiology, risk factors and management of implant fractures
 Journal section: Oral Surgery Publication Types: Review doi:10.4317/medoral.15.e504 Etiology, risk factors and management of implant fractures Arturo Sánchez-Pérez 1, Mª José Moya-Villaescusa 1, Alfonso
Journal section: Oral Surgery Publication Types: Review doi:10.4317/medoral.15.e504 Etiology, risk factors and management of implant fractures Arturo Sánchez-Pérez 1, Mª José Moya-Villaescusa 1, Alfonso
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
 Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
Since the introduction of osseointegrated dental implants
 CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
The earliest methods used
 RESEARCH EVALUATION OF THE PERIOTEST AS A DIAGNOSTIC TOOL FOR DENTAL IMPLANTS A. Norman Cranin, DDS, D.Eng Jack DeGrado, DDS Marc Kaufman, DDS Mylene Baraoidan, DDS Robert DiGregorio, PharmD George Batgitis,
RESEARCH EVALUATION OF THE PERIOTEST AS A DIAGNOSTIC TOOL FOR DENTAL IMPLANTS A. Norman Cranin, DDS, D.Eng Jack DeGrado, DDS Marc Kaufman, DDS Mylene Baraoidan, DDS Robert DiGregorio, PharmD George Batgitis,
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Initially, Brånemark System (Nobel Biocare AB,
 Clinical Application of Narrow Brånemark System Implants for Single-Tooth Restorations Giovanni Polizzi, MD, DDS*/Sandro Fabbro, MD**/Marco Furri, DDS**/ Irene Herrmann, DDS***/Sergio Squarzoni, MD****
Clinical Application of Narrow Brånemark System Implants for Single-Tooth Restorations Giovanni Polizzi, MD, DDS*/Sandro Fabbro, MD**/Marco Furri, DDS**/ Irene Herrmann, DDS***/Sergio Squarzoni, MD****
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Medical interventions involving surgical procedures
 Mechanical and Technical Risks in Implant Therapy Giovanni E. Salvi, PD, Dr Med Dent 1 /Urs Brägger, Prof Dr Med Dent 2 Purpose: To systematically appraise the impact of mechanical/technical risk factors
Mechanical and Technical Risks in Implant Therapy Giovanni E. Salvi, PD, Dr Med Dent 1 /Urs Brägger, Prof Dr Med Dent 2 Purpose: To systematically appraise the impact of mechanical/technical risk factors
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
There are many longitudinal investigations
 A 3-Arm Study of Early Loading of Rough-Surfaced Implants in the Completely Edentulous Maxilla and in the Edentulous Posterior Maxilla and Mandible: Results After 1 Year of Loading Thomas Nordin, DDS 1
A 3-Arm Study of Early Loading of Rough-Surfaced Implants in the Completely Edentulous Maxilla and in the Edentulous Posterior Maxilla and Mandible: Results After 1 Year of Loading Thomas Nordin, DDS 1
Ankylos. Scientific Summary
 Ankylos Scientific Summary Implanting TissueCare For over 25 years, the Ankylos implant system stands for stable, long-term esthetics. The results from numerous publications and long-term clinical experience
Ankylos Scientific Summary Implanting TissueCare For over 25 years, the Ankylos implant system stands for stable, long-term esthetics. The results from numerous publications and long-term clinical experience
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Osseointegrated titanium implants are now accepted in clinical dentistry for
 Treatment Planning and Placement of Implants in the Posterior Maxillae: Report of 732 Consecutive Nobelpharma Implants Oded Bahat, BDS, MSD One to nine Nobelpharma osseointegrated implants were placed
Treatment Planning and Placement of Implants in the Posterior Maxillae: Report of 732 Consecutive Nobelpharma Implants Oded Bahat, BDS, MSD One to nine Nobelpharma osseointegrated implants were placed
EFFECT OF IMPLANTS ON MAXIMUM BITE FORCE
 CLINICAL EFFECT OF IMPLANTS ON MAXIMUM BITE FORCE IN EDENTULOUS PATIENTS Mansour Rismanchian, DMD, MS; Farshad Bajoghli, DMD, MS; Zahra Mostajeran, DDS; Akbar Fazel, DMD, MS; P. sadr Eshkevari, DDS One
CLINICAL EFFECT OF IMPLANTS ON MAXIMUM BITE FORCE IN EDENTULOUS PATIENTS Mansour Rismanchian, DMD, MS; Farshad Bajoghli, DMD, MS; Zahra Mostajeran, DDS; Akbar Fazel, DMD, MS; P. sadr Eshkevari, DDS One
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
