Clinical and morphological aspects of the implant/soft tissue interface
|
|
|
- Julius Robinson
- 5 years ago
- Views:
Transcription
1 Clinical and morphological aspects of the implant/soft tissue interface Rodrigo F. Neiva, DDS, a Kathleen G. Neiva, DDS, b Tae-Ju Oh, DDS, MS, a and Hom-Lay Wang, DDS, MSD a a Department of Periodontics/Prevention/Geriatrics, and b Department of Cariology/ Restorative Science/Endodontics, School of Dentistry, University of Michigan, Ann Arbor, MI, USA Purpose: This paper is aimed to describe clinical and morphological aspects of the soft tissue implant/soft tissue interface and to provide guidelines for assessment of peri-implant mucosal health. Materials and Methods: Critical appraisal of the current literature regarding the interface between dental implants and the peri-implant mucosa is performed. Results: The articles reviewed agree that smooth titanium surfaces are highly compatible with oral soft tissues. The biological seal that is formed by the mucosa surrounding dental implants is established to provide protection against microbial invasion. Implant design may influence the location of the biological seal, but not the formation of the seal. Non-keratinized peri-implant mucosa does not seem to predispose peri-implant disease. Keartinized mucosa seems to be desirable for hygiene procedures and esthetics, but not necessary for implant success. Assessment of peri-implant mucosal health has shown to be a predictable indicator of peri-implant disease. Conclusion: Studies have consistently shown that biologic seal is formed between the oral cavity and the underlying tissues after implant placement, providing protection against the microbial challenge. However, future studies are needed in order to clarify the importance of the biological seal for implant success. (Int Chin J Dent 2002; 2: ) Clinical Significance: Since dental implant penetrate into the oral cavity, the interface between dental implants and oral soft tissues allows the formation of a biologic seal. This biologic seal has the ability to protect the underneath structures by closing the pathway of communication between the oral environment and the alveolar bone. Assessment of the integrity of this interface aids in early detection of peri-implant pathologies, and may prevent future implant bone loss. In addition, the implant/soft tissue interface may provide esthetics that implant supported restoration needs. Key words: biological width, dental implants, mucositis, peri-implant mucosa. INTRODUCTION The replacement of missing teeth by means of endosseous dental implants has become an important part of dentistry. Over the last two decades, research has validated the success of osseointegrated implants as a 151
2 viable replacement for partial and complete edentulism. Although techniques and materials have been developed which are capable of a high degree of clinical success, the ultimate long-term success of implants is dependent upon the efforts of both the patient and dentist in maintaining the health of the peri-implant tissues. Dental implants have two distinct interfaces with oral tissues. First, there is the peri-mucosal interface where soft tissue meets the implant, creating a biological seal. Secondly, the endosseous interface exists where alveolar bone is in close proximity with the titanium surface, providing stability and rigidity to the implant. Since the soft tissues reform around dental implants as a result of a healing process following implant placement, they are called peri-implant mucosa, not gingiva. The aim of this paper is to review the literature regarding the interface between the implant and peri-implant mucosa, which is divided into epithelium and connective tissue. EPITHELIUM Epithelial tissues have the capacity to proliferate and to move on surfaces. Following implant/abutment placement, epithelial migration from adjacent soft tissues begins. The epithelium moves in apico-coronal direction as soon as it reaches the implant surface, giving rise to a junctional epithelium about 2 mm long. 1-3 The formation of a junctional epithelium in the implant/mucosal interface can be considered the first barrier of defense against oral microflora. Figs. 1a and 1b illustrate the relationship between implant and surrounding soft tissue. JE oct ict MM cje oct aje ict a b Fig. 1. a. Diagram illustrates the relationship between implant and surrounding soft tissue interface. b. Histological sections of the implant/peri-implant mucosal interface. JE: Junctional epithelium; oct: Outer connective tissue; ict: Inner connective tissue; MM: Mucosal margin; cje: Coronal junctional epithelium; aje: Apical juctional epithelium; ict: Inner connective tissue. 152
3 Donley et al. suggested that junctional epithelium cells adjacent to a titanium implant to form a hemidesmosomal type of attachment to the implant surface similar to that of a natural tooth. 4 On the other hand, Meffert et al. suggested that the junctional hemidesmosomal arrangement may not be predictable in a metallic system. 5 Research has shown that once epithelial cells have reached the implant surface, their attachment occurs directly via a basal lamina (<200 nm) and hemidesmosomes. 6-8 Kawahara et al. hypothesized another form of attachment, where a glycoprotein layer of approximately 200 nm forms between the cell wall, without direct epithelium/implant contact. 9,10 Lekholm and Adell, however, have discussed the fact that the seal is probably viable and adequate in function based on the fact that there were minimal histologic inflammatory reactions in the underlying connective tissues. 11,12 The surface topography has also shown to play a role in the soft tissue attachment to titanium surfaces, since polished surfaces have shown higher compatibility to fibroblasts when compared to rough surfaces A prerequisite to a successful dental implant should be obtaining a peri-implant mucosal seal to the implant surface. 19,20 Failure to achieve or maintain this seal results in the apical migration of the epithelium into the bone/implant interface and possibly caused partially or completely encapsulation of the endosseous implant. 21,22 In a natural dentition, the junctional epithelium provides a seal at the base of the sulcus against the penetration of chemical and bacterial substances. If the seal is disrupted and/or the fibers apical to the epithelium are destroyed, the epithelium migrates apically, forming a periodontal pocket after cleavage of the soft tissue from the radicular surface. The importance of the biologic seal should be emphasized due to the absence of cementum and fiber insertion into the implant surface which may cause formation of a "peri-implant pocket" extending into the osseous structures. The characteristics of the soft tissues adjacent to teeth and implants were listed in Table 1. Table 1. Soft tissues adjacent to teeth and implants. Attachment Orientation of collagen fibers Source of blood supply Biological width/seal Teeth Basal lamina Perpendicular Periosteum, PDL JE: 0.97 mm 70 and hemidesmosomes CT: 1.07 mm 70 Implants Basal lamina Parallel Periosteum JE: 1.88 mm 1 and hemidesmosomes CT: 1.05 mm 1 PDL: Periodontal ligament; JE: Junctional epithelium; CT: Connective tissue. CONNECTIVE TISSUE For the connective tissue attachment to the implant, collagen fibers form a tight cuff around the implant abutment. The length of the connective tissue attachment ranges from 1.3 to 1.8 mm, 1,23 and is also dependent on the design of the implant (one- or two-part implant). There have been reports in the literature that the use of a plasma spray surface promotes connective tissue adherence with fibers inserted 153
4 functionally at 90 into the plasma sprayed surface of the implant. 15,24 However, most reports have shown that connective tissue fibers are not inserted into the implant surface. Dense bundles of thick collagen fibers are oriented only longitudinally due to a lack of fiber insertion. 25,26 The connective tissue of the peri-implant mucosa can be subdivided into two distinct zones. The outer zone located under the junctional epithelium, composed of collagen Types I and III, is responsible for the transformation of collagen. The inner supracrestal connective tissue zone, composed mainly of Type I collagen, is responsible for mechanical resistance and stability of the peri-implant mucosa. 25,27 The connective tissue surrounding dental implants possess fewer capillaries as compared to the connective tissue surrounding natural teeth. 28 The blood supply of the peri-implant mucosa is composed of terminal branches of larger vessels originating from the periosteum of the alveolar bone, while the vasculature of the gingiva and the supracrestal connective tissue at teeth is derived from the supraperiosteal vessels lateral of the alveolar process and the vessels of the periodontal ligament. 28 The peri-implant mucosa has also shown to exhibit an inflammatory response, similar to gingival tissues, characterized by increased proportions of T- and B-cells in the inner connective tissue. However, the host response is less pronounced than in gingival tissues BIOLOGICAL WIDTH/SEAL Animal and human studies have shown that an adequate biological width/seal can only be achieved if there is a supracrestal smooth titanium surface of at least 3 mm long in the apico-coronal direction. 1,21,32-35 The junctional epithelium occupies approximately 2 mm of this surface, while the rest of it is occupied by the connective tissue. Berglundh and Lindhe observed that the values for two-part implants were 2.0 mm for JE, and 1.3 to 1.8 mm for CT. 23 Cochran et al. observed the values for a biological width/seal around one-part implants before and after loading period of 12 months. Mean values for 3-month unloaded implants were 0.49 mm for sulcus depth (SD), 1.16 mm for the junctional epithelium attachment (JE), and 1.36 mm for the connective tissue attachment (CT). These dimensions differed from the 3-month loaded implants that showed 0.50 mm for SD, 1.44 mm for JE, and 1.01 mm for CT. After the 12-month loading period, these values were 0.16 mm for SD, 1.88 mm for JE, and 1.05 mm for CT. 1 It can be speculated that the biological width/seal increases approximately 1 mm after implant loading, possibly due to crestal bone resorption. THE INFLUENCE OF IMPLANT DESIGN Since a biological seal is formed by epithelial and connective tissue attachments to the implant surface, the length of titanium surface interfaced with the peri-implant mucosa may influence the location of the biological seal. One-part implants seem to provide a more predictable surface for soft tissue attachment, since the length of the smooth titanium surface is stable, and the implant/abutment connection is positioned more coronally. 36 Soft tissue attachment in two-part implants are dependent on the location of the restorative margin that must respect the dimensions necessary for the formation of a biological seal/width. 154
5 If the required dimensions are not respected, an apical migration of the biological seal/width can be expected with subsequent exposure of the rough implant surface to the implant/mucosal interface. In two-part implant, the microgap present at the implant/abutment interface may result in an inflammatory infiltrate due to presence of microorganisms that can populate the implant/abutment junction. 22 The inflammatory infiltrate is a protective host defense mechanism that limits microbial invasion, preventing further deterioration of implant supporting tissues. Ericsson et al. showed that an apical migration of the junctional epithelium occurs after abutment connection in two-part implant, allowing a biological seal to be formed. 34 Weber et al. compared the formation of the biological seal around one- and two-part implants and demonstrated that a biological seal is formed irrespective of the implant design. However, two-part implants resulted in a longer junctional epithelium attachment, which was located more apically. The distance from the crestal bone was also shorter in comparison to one-part implants. No differences were found in the length of connective tissue attachment. 37 Similar findings was also reported by Hermann et al. 38 KERATINIZED VS. NON-KERATINIZED PERI-IMPLANT MUCOSA The need of the keratinized mucosa surrounding dental implants in order to maintain peri-implant mucosal health is controversial, since healthy tissues can be noted not only on the presence but also on the absence of keratinized peri-implant mucosa. Becker et al. speculated that keratinized peri-implant mucosa is not a necessary prerequisite for peri-implant health and that movable mucosa around the trans-epithelial extension of an endosseous implant is not necessarily a vulnerable situation. 39 However, Warrer et al. used an animal model and demonstrated that implants surrounded by non-keratinized mucosa may exhibit more crestal bone loss and mucosal recession, when compared to implants surrounded by a keratinized mucosa, under similar levels of plaque accumulation. 40 Similar observation was also demonstrated by Strub et al. 41 Adell et al. reported based on 15-year results of 2,768 implants placed in 371 subjects, that even when a movable mucosa was found surrounding implants, a clinically healthy mucosa was noted. 42 Wennstrom and Lindhe evaluated the prospective and retrospective studies of Branemark to associate implant failure with nonkeratinized peri-implant mucosa. An overall 90% success rate in terms of fixture survival and in which the marginal tissue was keratinized gingiva in only 67% and 51% of the facial and lingual surfaces respectively demonstrated that the absence of a keratinized peri-implant mucosa does not predispose implant failure. 3,43 On the other hand, Kirsch and Ackermann published 10-year clinical results of 2,284 implants, with a failure rate of 2.2%. The study suggested that the main cause of failure was insufficient width of keratinized peri-implant mucosa. 44 The difference in the two studies may be attributed to the difference that the retrospective and prospective studies of Branemark were in fully edentulous cases, while the majority of the implants in Kirsch's study were in partially edentulous mouths. Although the absence of a keratinized mucosa does not seem to predispose implant failure, keratinized tissue may facilitate personal home care and maintenance procedures. Connective tissue grafts, free gingival grafts, and other techniques, have been described and have achieved predictable results for 155
6 augmentation of keratinized mucosa around dental implants ASSESSMENT OF SOFT TISSUE HEALTH Experimental evidence during the last decade supported the concept of a host-parasite imbalance being the major responsible reason for implant failures after loading 53,54. As in the case of teeth, the imbalance in the host-parasite equilibrium can manifest itself in a series of inflammatory changes, which lead to two distinct clinical syndromes: 1) Mucositis is a reversible inflammatory lesion confined to the superficial peri-implant mucosal tissues, and 2) Peri-implantitis is a lesion involving the peri-implant soft tissues as well as the marginal portion of the bone-implant interface. As is true for gingivitis and periodontitis, the relationship between peri-implant mucositis and peri-implantitis is not known with respect to the natural history, evolution and progression. 55 dental implants rarely fail beyond the first year after restoration. 56,57 Endosseous However, it has been suggested that conventional periodontal therapy should be instituted if inflammation develops around an implant. 58,59 Problems limited to the peri-implant mucosa and not involving the supporting bone have been defined as "ailing implants" and, more recently, as biological complications. 36,54 Probing studies in dental implants are dependent on the emergence profile of the final restoration. Assessment of probing depth around overcontoured crowns is largely irrelevant unless the superstructure is removed, allowing probing parallel to the long axis of the fixture. Peri-implant probing depth, mucosal recession, bleeding upon probing, and peri-implant exudation have been suggested as useful diagnostic tools for biological complications Probing studies in dental implants are also dependent on the presence or absence of inflammation since it has been shown that a probe is able to penetrate into the connective tissue and reaching close proximity to the alveolar bone even in presence of mild to moderate mucositis. 63 Successful implants usually allow approximately 3 mm of probe penetration, while deeper probing depths are often associated with a marked difference in the composition of the peri-implant 1, 62 microflora. While the overall prevalence of peri-implantitis ranges from 5-10%, the prevalence of peri-implant mucositis seems to be higher. Smedberg et al. reported that radiological diagnosed marginal bone defects in 6% of implants after 2 years in function; 28% of the patients were diagnosed as having peri-implant mucositis. 64 However, the classic study of Adell and coworkers reported that the mean values of peri-implant mucositis and plaque were 7.6 and 13.7% respectively. 42 The microbiological findings related to healthy and failing implants are similar as those for healthy and periodontally compromised teeth. 60,62 Increased levels of subgingival Porphyromonas gingivalis, Prevotella intermedia, and Fusobacterium nucleatum may lead dental implants to fail. On the other hand, failing implants with a traumatic etiology may have a microflora comprised predominantly of streptococci which is consistent with periodontal health. 65 The microbiota present in the oral cavity can influence bacterial colonization around implants since implants placed in partially edentulous periodontal patients had the same microflora found in their periodontal pockets. 66,67 Salcetti et al. found increased levels of 156
7 PGE 2, IL-1ß, and PDGF in failing implant sites demonstrating that not only the microbiota but also the host response is similar to those of periodontally diseased teeth. 68 Sbordone et al. evaluated implants placed in partially edentulous patients with previous history of moderate to severe chronic periodontitis. They found that the treated periodontal sites were stable at 3 years, with nearly 90% of the sites demonstrating CAL<1 mm. Despite the similarity of the microbiota of the samples from implant and natural tooth sites, no evidence of recurrent periodontal attachment loss or implant failure was noted. 69 These findings support the recommendation that patients with implants should be evaluated at regular visits for periodontal maintenance procedures, and any clinical signs and symptoms of peri-implant mucositis or peri-implantitis should be recorded and treated. CONCLUSIONS The use of dental implants in the treatment of partially or fully edentulous patients has become an important addition in oral/dental rehabilitation. The literature to date concurs that coated, non-coated, or plasma-sprayed implants all have the capacity to achieve osseointegration, if appropriate surgical techniques are involved. The fact that implants penetrate the oral mucosa and the mucosa is able to seal around the implant, leads to the assumption that the peri-implant mucosa fulfills the function of acting as a barrier to protect the anchorage to the alveolar bone. The biological seal has shown to be present irrespective of the implant design, but a smooth titanium surface is preferable for soft tissue attachment. Research has shown that insufficient plaque removal may lead to peri-implant disease with or without bone loss. However, it is unclear how important this cause is as a cause of implant failure, compared with other factors, such as inadequate bone healing, unfavorable quantity and quality of bone, or (bio) mechanical and functional problems. It is also not understood if the presence or absence of keratinized peri-implant mucosa is needed to slow down or prevent tissue breakdown. The current knowledge has shown that the keratinized mucosa maybe desirable, but not necessary. Future studies in these areas are necessary and will certainly provide a better understanding in this field. ACKNOWLEDGMENT This work was partially supported by the University of Michigan Periodontal Graduate Student Research Fund. REFERENCES 1. Cochran DL, Hermann JS, Schenk RK, Higginbottom FL, Buser D. Biologic width around titanium implants. A histometric analysis of the implanto-gingival junction around unloaded and loaded nonsubmerged implants in the canine mandible. J Periodontol 1997; 68: Listgarten MA. Soft and hard tissue response to endosseous dental implants. Anat Rec 1996; 245: Lindhe J, Berglundh T. The interface between the mucosa and the implant. Periodontol ; 17:
8 4. Donley TG, Gillette WB. Titanium endosseous implant-soft tissue interface: a literature review. J Periodontol 1991; 62: Meffert R. The soft tissue interface in dental implantology. Implantologist 1986; 5: Gould TR, Brunette DM, Westbury L. The attachment mechanism of epithelial cells to titanium in vitro. J Periodontal Res 1981; 16: Hansson HA, Albrektsson T, Branemark PI. Structural aspects of the interface between tissue and titanium implants. J Prosthet Dent 1983; 50: McKinney RV Jr., Steflik DE, Koth DL.. Evidence for a junctional epithelial attachment to ceramic dental implants. A transmission electron microscopic study. J Periodontol 1985; 56: Kawahara H, Kawahara D, Mimura Y, Takashima Y, Ong JL. Morphologic studies on the biologic seal of titanium dental implants. Report II. In vivo study on the defending mechanism of epithelial adhesions/attachment against invasive factors. Int J Oral Maxillofac Implants 1998; 13: Kawahara H, Kawahara D, Hashimoto K, Takashima Y, Ong JL. Morphologic studies on the biologic seal of titanium dental implants. Report I. In vitro study on the epithelialization mechanism around the dental implant. Int J Oral Maxillofac Implants 1998; 13: Adell R, Lekholm U, Rockler B, et al. Marginal tissue reactions at osseointegrated titanium fixtures (I). A 3-year longitudinal prospective study. Int J Oral Maxillofac Surg 1986; 15: Lekholm U, Adell R, Lindhe J, et al. Marginal tissue reactions at osseointegrated titanium fixtures. (II) A cross-sectional retrospective study. Int J Oral Maxillofac Surg 1986; 15: Fitton JH, Dalton BA, Beumer G, Johnson G, Griesser HJ, Steele JG. Surface topography can interfere with epithelial tissue migration. J Biomed Mater Res 1998; 42: Cochran D, Buser D. Attachment and growth of periodontal cells on smooth and rough titanium. Int J Oral Maxillofac Implants 1994; 9: Schroeder A, van der Zypen E, Stich H, Sutter F. The reactions of bone, connective tissue, and epithelium to endosteal implants with titanium-sprayed surfaces. J Maxillofac Surg 1981; 9: Wennstrom J, Lindhe J. Plaque-induced gingival inflammation in the absence of attached gingiva in dogs. J Clin Periodontol 1983; 10: Jansen JA, de Wijn JR, Wolters-Lutgerhorst JM, van Mullem PJ. Ultrastructural study of epithelial cell attachment to implant materials. J Dent Res 1985; 64: Lauer G, Wiedmann-Al-Ahmad M, Otten JE, Hubner U, Schmelzeisen R, Schilli W. The titanium surface texture effects adherence and growth of human gingival keratinocytes and human maxillar osteoblast-like cells in vitro. Biomaterials 2001; 22: Liljenberg B, Gualini F, Berglundh T, Tonetti M, Lindhe J. Some characteristics of the ridge mucosa before and after implant installation. A prospective study in humans. J Clin Periodontol 1996; 23: Liljenberg B, Gualini F, Berglundh T, Tonetti M, Lindhe J. Composition of plaque-associated lesions in the gingiva and the peri-implant mucosa in partially edentulous subjects. J Clin Periodontol 1997; 24: Ericsson I, Lindhe J. Probing depth at implants and teeth. An experimental study in the dog. J Clin Periodontol 1993; 20: Ericsson I, Persson LG, Berglundh T, Marinello CP, Lindhe J, Klinge B. Different types of inflammatory reactions in peri-implant soft tissues. J Clin Periodontol 1995; 22: Berglundh T, Lindhe J. Dimension of the periimplant mucosa. Biological width revisited. J Clin Periodontol 1996; 23: Buser D, Warrer K, Karring T, Stich H. Titanium implants with a true periodontal ligament: an alternative to osseointegrated implants? Int J Oral Maxillofac Implants 1990; 5: Chavrier CA, Couble ML. Ultrastructural immunohistochemical study of interstitial collagenous components of the healthy human keratinized mucosa surrounding implants. Int J Oral Maxillofac Implants 1999; 14:
9 26. Comut AA, Weber HP, Shortkroff S, Cui FZ, Spector M. Connective tissue orientation around dental implants in a canine model. Clin Oral Implants Res 2001; 12: Chavrier C, Couble ML, Hartmann DJ. Qualitative study of collagenous and noncollagenous glycoproteins of the human healthy keratinized mucosa surrounding implants. Clin Oral Implants Res 1994; 5(3): Berglundh T, Lindhe J, Jonsson K, Ericsson I. The topography of the vascular systems in the periodontal and peri-implant tissues in the dog. J Clin Periodontol 1994; 21: Zitzmann NU, Berglundh T, Marinello CP, Lindhe J. Experimental peri-implant mucositis in man. J Clin Periodontol 2001; 28: Tonetti MS, Imboden M, Gerber L, Lang NP. Compartmentalization of inflammatory cell phenotypes in normal gingiva and peri-implant keratinized mucosa. J Clin Periodontol 1995; 22: Marchetti C, Farina A, Cornaglia AI. Microscopic, immunocytochemical, and ultrastructural properties of peri-implant mucosa in humans. J Periodontol 2002; 73: Abrahamsson I, Berglundh T, Wennstrom J, Lindhe J. The peri-implant hard and soft tissues at different implant systems. A comparative study in the dog. Clin Oral Implants Res 1996; 7: Abrahamsson I, Berglundh T, Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol 1997; 24: Ericsson I, Nilner K, Klinge B, Glantz PO. Radiographical and histological characteristics of submerged and nonsubmerged titanium implants. An experimental study in the Labrador dog. Clin Oral Implants Res 1996; 7: Berglundh T, Lindhe J. Healing around implants placed in bone defects treated with Bio-Oss. An experimental study in the dog. Clin Oral Implants Res 1997; 8: Cochran D. Implant therapy I. Ann Periodontol 1996; 1: Weber HP, Buser D, Donath K, et al. Comparison of healed tissues adjacent to submerged and non-submerged unloaded titanium dental implants. A histometric study in beagle dogs. Clin Oral Implants Res 1996; 7: Hermann JS, Buser D, Schenk RK, Schoolfield JD, Cochran DL. Biologic Width around one- and two-piece titanium implants. Clin Oral Implants Res 2001; 12: Becker W, Becker BE, Newman MG, Nyman S. Clinical and microbiologic findings that may contribute to dental implant failure. Int J Oral Maxillofac Implants 1990; 5: Warrer K, Buser D, Lang NP, Karring T. Plaque-induced peri-implantitis in the presence or absence of keratinized mucosa. An experimental study in monkeys. Clin Oral Implants Res 1995; 6: Strub JR, Gaberthuel TW, Grunder U. The role of attached gingiva in the health of peri-implant tissue in dogs. 1. Clinical findings. Int J Periodontics Restorative Dent 1991; 11: Adell R, Lekholm U, Rockler B, Branemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg 1981; 10: Wennstrom JL, Bengazi F, Lekholm U. The influence of the masticatory mucosa on the peri-implant soft tissue condition. Clin Oral Implants Res 1994; 5: Kirsch A, Ackermann KL. The IMZ osteointegrated implant system. Dent Clin North Am 1989; 33: Silverstein LH, Lefkove MD, Garnick JJ. The use of free gingival soft tissue to improve the implant/soft-tissue interface. J Oral Implantol 1994; 20: Silverstein LH, Lefkove MD. The use of the subepithelial connective tissue graft to enhance both the aesthetics and periodontal contours surrounding dental implants. J Oral Implantol 1994; 20: Silverstein LH, Kurtzman D, Garnick JJ, Trager PS, Waters PK. Connective tissue grafting for improved implant esthetics: clinical technique. Implant Dent 1994; 3: Sclar AG. Use of the epithelialized palatal graft with dental implants. Atlas Oral Maxillofac Surg Clin North Am 1999; 7: Sclar A. Cosmetic soft-tissue enhancement for dental implants. Alpha Omegan 2000; 93: The acellular dermal matrix: soft-tissue development for dental implants. Dent Implantol Update 2001; 12:
10 51. Becker W. Esthetic soft-tissue augmentation adjacent to dental implants. Compend Contin Educ Dent 2001; 22: 250-2, 54, 56 passim. 52. El-Askary AS. Use of connective tissue grafts to enhance the esthetic outcome of implant treatment: a clinical report of 2 patients. J Prosthet Dent 2002; 87: Esposito M, Thomsen P, Ericson LE, Lekholm U. Histopathologic observations on early oral implant failures. Int J Oral Maxillofac Implants 1999; 14: Esposito M, Hirsch J, Lekholm U, Thomsen P. Differential diagnosis and treatment strategies for biologic complications and failing oral implants: a review of the literature. Int J Oral Maxillofac Implants 1999; 14: Mombelli A. Prevention and therapy of peri-implant infections. Proceedings of the 3rd European Workshop on Periodontology. Implant Dent 1999; 1: Albrektsson T, Dahl E, Enbom L, et al. Osseointegrated oral implants. A Swedish multicenter study of 8139 consecutively inserted Nobelpharma implants. J Periodontol 1988; 59: Buser D, Mericske-Stern R, Bernard JP, et al. Long-term evaluation of non-submerged ITI implants. Part 1: 8-year life table analysis of a prospective multi-center study with 2359 implants. Clin Oral Implants Res 1997; 8: Sbordone L, Ramaglia L, Barone A, Ciaglia RN, Tenore A, Iacono VJ. Periodontal status and selected cultivable anaerobic microflora of insulin-dependent juvenile diabetics. J Periodontol 1995; 66: Sbordone L, Barone A, Ramaglia L, Ciaglia RN, Iacono VJ. Antimicrobial susceptibility of periodontopathic bacteria associated with failing implants. J Periodontol 1995; 66: Mombelli A, Buser D, Lang NP. Colonization of osseointegrated titanium implants in edentulous patients. Early results. Oral Microbiol Immunol 1988; 3: Mombelli A, Lang NP. The diagnosis and treatment of peri-implantitis. Periodontol ; 17: Mombelli A. Microbiology and antimicrobial therapy of peri-implantitis. Periodontol ; 28: Schou S, Holmstrup P, Stoltze K, Hjorting-Hansen E, Fiehn NE, Skovgaard LT. Probing around implants and teeth with healthy or inflamed peri-implant mucosa/gingiva. A histologic comparison in cynomolgus monkeys (Macaca fascicularis). Clin Oral Implants Res 2002; 13: Smedberg JI, Lothigius E, Bodin I, Frykholm A, Nilner K. A clinical and radiological two-year follow-up study of maxillary overdentures on osseointegrated implants. Clin Oral Implants Res 1993; 4: Mombelli A, van Oosten MA, Schurch E Jr., Land NP. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol 1987; 2: Lee KH, Tanner AC, Maiden MF, Weber HP. Pre- and post-implantation microbiota of the tongue, teeth, and newly placed implants. J Clin Periodontol 1999; 26: Lee KH, Maiden MF, Tanner AC, Weber HP. Microbiota of successful osseointegrated dental implants. J Periodontol 1999; 70: Salcetti JM, Moriarty JD, Cooper LF, et al. The clinical, microbial, and host response characteristics of the failing implant. Int J Oral Maxillofac Implants 1997; 12: Sbordone L, Barone A, Ciaglia RN, Ramaglia L, Iacono VJ. Longitudinal study of dental implants in a periodontally compromised population. J Periodontol 1999; 70: Garguilo A. Dimensions and relationships of the dentogingival junction in humans. J Periodontol 1961; 32:
11 Reprint request to: Dr. Hom-Lay Wang Graduate Periodontics, University of Michigan School of Dentistry 1011 N, University Avenue, Ann Arbor, Michigan , USA FAX: Received on November 18, Revised on December 12, Accepted on December 21, Copyright 2002 by the Editorial Council of the International Chinese Journal of Dentistry. 161
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The 2B-3D rule for implant planning, placement and restoration
 IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Tae-Hyung Kim. The Graduate School. Yonsei University. Department of Dental Science
 Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The peri-implant mucosa has
 Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
Soft tissue responses to differential shapes of the implant abutment
 대한치주과학회지 : Vol. 36, No. 1, 2006 Soft tissue responses to differential shapes of the implant abutment Soo-Yong Ahn 1, Chong-Hyun Han 2, Seong-Joo Heo 3, Tae-Il Kim 1, Yang-Jo Seol 1, Yong-Moo Lee 1, Young
대한치주과학회지 : Vol. 36, No. 1, 2006 Soft tissue responses to differential shapes of the implant abutment Soo-Yong Ahn 1, Chong-Hyun Han 2, Seong-Joo Heo 3, Tae-Il Kim 1, Yang-Jo Seol 1, Yong-Moo Lee 1, Young
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
A Panoramic View of Junctional Epithelium And Biologic Width Around Teeth And Implant
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. IX (September. 2017), PP 61-70 www.iosrjournals.org A Panoramic View of Junctional Epithelium
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. IX (September. 2017), PP 61-70 www.iosrjournals.org A Panoramic View of Junctional Epithelium
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs
 Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Immediate Implant Placement:
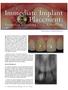 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Review. The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang*
 The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang* The success of dental implants is highly dependent on integration between the implant
The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang* The success of dental implants is highly dependent on integration between the implant
Detection of predominant subgingival periopathogens around submerged and non submerged hydroxy apatite implants
 [Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
[Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Importance of existence of keratinized gingival on the health of tissue around over dentures supporting implants: a case report
 Importance of existence of keratinized gingival on the health of tissue around over dentures supporting implants: a case report Maliheh Hamedi Jahroumi 1, Majid Vatankhah 2, Maryam Voosooghi shashkolati
Importance of existence of keratinized gingival on the health of tissue around over dentures supporting implants: a case report Maliheh Hamedi Jahroumi 1, Majid Vatankhah 2, Maryam Voosooghi shashkolati
Over the past few decades, an improved
 RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
5 Professor and Chair, Department of Periodontics, Dental
 Biologic Width Around Different Implant-Abutment Interface Configurations. A Radiographic Evaluation of the Effect of Horizontal Offset and Concave Abutment Profile in the Canine Mandible Santiago J. Caram,
Biologic Width Around Different Implant-Abutment Interface Configurations. A Radiographic Evaluation of the Effect of Horizontal Offset and Concave Abutment Profile in the Canine Mandible Santiago J. Caram,
Alveolar ridge preservation techniques
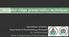 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Michael P. Hänggi,* Daniel C. Hänggi, John D. Schoolfield, Jürg Meyer,* David L. Cochran, and Joachim S. Hermann
 J Periodontol May 2005 Crestal Bone Changes Around Titanium Implants. Part I: A Retrospective Radiographic Evaluation in Humans Comparing Two Non-Submerged Implant Designs With Different Machined Collar
J Periodontol May 2005 Crestal Bone Changes Around Titanium Implants. Part I: A Retrospective Radiographic Evaluation in Humans Comparing Two Non-Submerged Implant Designs With Different Machined Collar
The Significance of Keratinized Mucosa on Implant Health: A Systematic Review
 Review The Significance of Keratinized Mucosa on Implant Health: A Systematic Review Guo-Hao Lin,* Hsun-Liang Chan, and Hom-Lay Wang Background: Whether a minimal width of keratinized mucosa (KM) is required
Review The Significance of Keratinized Mucosa on Implant Health: A Systematic Review Guo-Hao Lin,* Hsun-Liang Chan, and Hom-Lay Wang Background: Whether a minimal width of keratinized mucosa (KM) is required
Vertical and/or horizontal alveolar
 CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report of two cases
 Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Evaluation of fixed partial denture in relation to gingival recession and other factors
 Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Themucosalbarrieratimplant abutments of different materials
 Maria Welander Ingemar Abrahamsson Tord Berglundh Themucosalbarrieratimplant abutments of different materials Authors affiliation: Maria Welander, Ingemar Abrahamsson, Tord Berglundh, Department of Periodontology,
Maria Welander Ingemar Abrahamsson Tord Berglundh Themucosalbarrieratimplant abutments of different materials Authors affiliation: Maria Welander, Ingemar Abrahamsson, Tord Berglundh, Department of Periodontology,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
EFFECT OF DISTANCE BETWEEN ONE PIECE IMPLANTS ON CRESTAL BONE RESORPTION
 EUROPEAN JOURNAL OF INFLAMMATION Vol. 9, no. 2 (S), 0-0 (2011) EFFECT OF DISTANCE BETWEEN ONE PIECE IMPLANTS ON CRESTAL BONE RESORPTION S. FANALI 1, F. CARINCI 2, I. ZOLLINO 2, G. BRUNELLI 3, R. MONGUZZI
EUROPEAN JOURNAL OF INFLAMMATION Vol. 9, no. 2 (S), 0-0 (2011) EFFECT OF DISTANCE BETWEEN ONE PIECE IMPLANTS ON CRESTAL BONE RESORPTION S. FANALI 1, F. CARINCI 2, I. ZOLLINO 2, G. BRUNELLI 3, R. MONGUZZI
Tooth Retained Implant: No More an Oxymoron
 بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
=0.73; P=.503). Conclusions. It can be concluded that initial tissue thickness can influence crestal bone changes around implants.
 SCIENTIFIC ARTICLES Stomatologija, Baltic Dental and Maxillofacial Journal, 11: 83-91, 2009 Reaction of crestal bone around implants depending on mucosal tissue thickness. A 1-year prospective clinical
SCIENTIFIC ARTICLES Stomatologija, Baltic Dental and Maxillofacial Journal, 11: 83-91, 2009 Reaction of crestal bone around implants depending on mucosal tissue thickness. A 1-year prospective clinical
Alfredo Montes Imeri, D.D.S.
 Proximal bone levels of plateau-designed, press fit implants adjacent to a natural teeth and implants A THESIS SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY: Alfredo
Proximal bone levels of plateau-designed, press fit implants adjacent to a natural teeth and implants A THESIS SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY: Alfredo
The Socket Shield Technique A case Report
 The Socket Shield Technique A case Report Haseeb H. Al-Dary Private Practice, Amman Jordan dary_haseeb@yahoo.com ABSTRACT In the aim of achieving an optimal esthetic result, implant dentistry has become
The Socket Shield Technique A case Report Haseeb H. Al-Dary Private Practice, Amman Jordan dary_haseeb@yahoo.com ABSTRACT In the aim of achieving an optimal esthetic result, implant dentistry has become
As the number of dental
 Volume 77 Number 8 Significance of Keratinized Mucosa in Maintenance of Dental Implants With Different Surfaces Dyeus M. Chung,* Tae-Ju Oh,* Jeffrey L. Shotwell, Carl E. Misch,* and Hom-Lay Wang* Background:
Volume 77 Number 8 Significance of Keratinized Mucosa in Maintenance of Dental Implants With Different Surfaces Dyeus M. Chung,* Tae-Ju Oh,* Jeffrey L. Shotwell, Carl E. Misch,* and Hom-Lay Wang* Background:
Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique
 e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Peri-implant Inflammation Defined by the Implant-Abutment Interface
 RESEARCH REPORTS Clinical N. Broggini 1,5, L.M. McManus 1,2, J.S. Hermann 1,3, R. Medina 4, R.K. Schenk 5, D. Buser 5, and D.L. Cochran 1 * Departments of 1 Periodontics and 2 Pathology, University of
RESEARCH REPORTS Clinical N. Broggini 1,5, L.M. McManus 1,2, J.S. Hermann 1,3, R. Medina 4, R.K. Schenk 5, D. Buser 5, and D.L. Cochran 1 * Departments of 1 Periodontics and 2 Pathology, University of
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Biologic width: Understanding and its preservation Malathi K 1, Singh A 2
 Biologic width: Understanding and its preservation Malathi K 1, Singh A 2 Review Article 1 Dr K Malathi Professor & Head, Periodontics Government Dental college and Hospital Tamil Nadu, India 2 Dr Arjun
Biologic width: Understanding and its preservation Malathi K 1, Singh A 2 Review Article 1 Dr K Malathi Professor & Head, Periodontics Government Dental college and Hospital Tamil Nadu, India 2 Dr Arjun
The treatment of destructive periodontal disease, due to specific periodontopathic
 1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
SPECIAL SUPPLEMENT. Inside this issue: 2014 No. 3. Peri-implant disease Implant surface: An evolution Summaries of select scientific publications
 www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Original Article Revisiting peri-implant soft tissue histopathological study of the peri-implant soft tissue
 Int J Clin Exp Pathol 2014;7(2):611-618 www.ijcep.com /ISSN:1936-2625/IJCEP1312023 Original Article Revisiting peri-implant soft tissue histopathological study of the peri-implant soft tissue Eduarda Silva
Int J Clin Exp Pathol 2014;7(2):611-618 www.ijcep.com /ISSN:1936-2625/IJCEP1312023 Original Article Revisiting peri-implant soft tissue histopathological study of the peri-implant soft tissue Eduarda Silva
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Dent Clin N Am 49 (2005) Peri-implantitis
 Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Dr. Jyoti Bansal, Dr. Abhishek Bansal, Dr. Suresh D.K., Dr. Anish Manocha
 Case Report 1 2 3 4 Dr. Jyoti Bansal, Dr. Abhishek Bansal, Dr. Suresh D.K., Dr. Anish Manocha Bansal J, Bansal A, DK Suresh, Manocha A. Immediate loading of single stage implants with minimally invasive
Case Report 1 2 3 4 Dr. Jyoti Bansal, Dr. Abhishek Bansal, Dr. Suresh D.K., Dr. Anish Manocha Bansal J, Bansal A, DK Suresh, Manocha A. Immediate loading of single stage implants with minimally invasive
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Replacement of missing teeth by means of
 Peri-Implant Bone Level Around Implants with Platform-Switched Abutments Stefan Fickl, Dr Med Dent 1 /Otto Zuhr, Dr Med Dent 2 /Jamal M. Stein, Dr Med Dent 3 / Markus B. Hürzeler, Prof Dr Med Dent 2,4
Peri-Implant Bone Level Around Implants with Platform-Switched Abutments Stefan Fickl, Dr Med Dent 1 /Otto Zuhr, Dr Med Dent 2 /Jamal M. Stein, Dr Med Dent 3 / Markus B. Hürzeler, Prof Dr Med Dent 2,4
The following resources related to this article are available online at jada.ada.org ( this information is current as of July 11, 2011):
 Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery
 A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery Seung-Mi Jeong, DDS, PhD, a Byung-Ho Choi, DDS, PhD, b Jihun
A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery Seung-Mi Jeong, DDS, PhD, a Byung-Ho Choi, DDS, PhD, b Jihun
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study
 Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study Nicola Ursula Zitzmann, Dr Med Dent 1 /Peter Schärer, Prof Dr Med Dent, MS 2 / Carlo Paolo Marinello, Prof
Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study Nicola Ursula Zitzmann, Dr Med Dent 1 /Peter Schärer, Prof Dr Med Dent, MS 2 / Carlo Paolo Marinello, Prof
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Initially, implant dentistry was focused on
 CASE LETTER Correction of Esthetic Complications of a Malpositioned Implant: A Case Letter Sergio Alexandre Gehrke, PhD INTRODUCTION Initially, implant dentistry was focused on successful osseointegration
CASE LETTER Correction of Esthetic Complications of a Malpositioned Implant: A Case Letter Sergio Alexandre Gehrke, PhD INTRODUCTION Initially, implant dentistry was focused on successful osseointegration
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Nicholas Caplanis DMD MS 6/13/2012
 Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
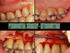 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Biological width following immediate implant placement in the dog: flap vs. flapless surgery
 Juan Blanco Célia Coutinho Alves Vanesa Nuñez Luis Aracil Fernando Muñoz Isabel Ramos Biological width following immediate implant placement in the dog: flap vs. flapless surgery Authors affiliations:
Juan Blanco Célia Coutinho Alves Vanesa Nuñez Luis Aracil Fernando Muñoz Isabel Ramos Biological width following immediate implant placement in the dog: flap vs. flapless surgery Authors affiliations:
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
BOUCHLARIOTOU, Ioana, et al. Abstract
 Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation
 The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study
 A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
The clinical use of endosseous implants has
 A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
The Bulletin Spring 2000
 The Bulletin Spring 2000 Spring Meeting - Friday March 31, 2000 Joint Symposium: Northeastern Society of Periodontists and Northeastern Gnathological Society New York Marriott Marquis Hotel 1535 Broadway
The Bulletin Spring 2000 Spring Meeting - Friday March 31, 2000 Joint Symposium: Northeastern Society of Periodontists and Northeastern Gnathological Society New York Marriott Marquis Hotel 1535 Broadway
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Simultaneous placement of an interpositional free gingival graft with nonsubmerged implant placement
 Simultaneous placement of an interpositional free gingival graft with nonsubmerged implant placement Joo-Yeon Sohn 1, Jung-Chul Park 1, Kyoo-Sung Cho 1, Chang-Sung Kim 2, * 1 Department of Periodontology,
Simultaneous placement of an interpositional free gingival graft with nonsubmerged implant placement Joo-Yeon Sohn 1, Jung-Chul Park 1, Kyoo-Sung Cho 1, Chang-Sung Kim 2, * 1 Department of Periodontology,
The International Journal of Periodontics & Restorative Dentistry
 The nternational Journal of Periodontics & Restorative Dentistry 2009 BY QUNTESSENCE PUBLSHNG CO, NC. PRNTNG OF THS DOCUMENT S RESTRCTED TO PERSONAL USE ONLY. NO PART OF THS ARTCLE 549 Time Sequence of
The nternational Journal of Periodontics & Restorative Dentistry 2009 BY QUNTESSENCE PUBLSHNG CO, NC. PRNTNG OF THS DOCUMENT S RESTRCTED TO PERSONAL USE ONLY. NO PART OF THS ARTCLE 549 Time Sequence of
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
