Ucer, C; Wright, S; Scher E; West, N; Retzepi, M; Simpson, S; Slade, K; Donos, N
|
|
|
- Daniel Baker
- 6 years ago
- Views:
Transcription
1 ADI GUIDELINES On Peri-implant Monitoring and Maintenance Ucer, C; Wright, S; Scher E; West, N; Retzepi, M; Simpson, S; Slade, K; Donos, N Scope of the Problem: During the last two decades implant treatment has become a part of mainstream dentistry as a predictable modality for replacing missing teeth. Nevertheless, most of the evidence supporting this predictability is based on survival statistics, which use presence or absence of implants as an end-point outcome measure. The survival rates, unfortunately, do not account for the slowly progressing, on-going biological problems such as peri-implant diseases. Long-term biological complications arising from peri-implant infection and inflammation result in progressive crestal bone loss (CBL), which places the implant at risk of being lost. Although the technical and mechanical complications have been reduced up to a certain extent due to advances in implant technology and design, there is still no clarity on how to manage biological complications around implants. History of periodontal disease, satisfactory plaque control, patient susceptibility, smoking, compliance and availability of adequate professional supportive therapies are important issues affecting implant patients. Monitoring and maintaining implants in function satisfactorily is therefore one of the biggest challenges that the implant team faces. The whole implant team; the implant surgeon, restoring dentist, the general dental practitioner, the hygienist/therapist, as well as the patient (by being compliant) all have individual responsibilities and duty of care in this respect. These guidelines are produced as a summary of ADI s Expert Panel Consensus meeting, held on 19th November 2012 in London, on the management of peri-implant diseases. The guidelines are not prescriptive protocols but good practice recommendations based on expert opinion informed by best available current evidence on the subject. Nevertheless, clinicians are strongly advised to seek up-to-date information and opinion from different sources when managing patients. Introduction: A cause-effect relationship has been demonstrated between dental plaque and peri-implant diseases (Mombelli et al, 2007). Reversible inflammation affecting the peri-implant soft tissues without any bony involvement is known as peri-implant mucositis. When this leads to crestal bone loss it is referred to as peri-implantitis, which is irreversible. Both conditions have similarities, respectively, to gingivitis and periodontitis in pathogenesis (Okayasu and Wang, 2011) but the disease progression might be faster around implants due to physiological differences in connective tissue morphology (Lang and Berglund, 2011). 1
2 It has been demonstrated that high level of implant success requires meticulous peri-implant maintenance and plaque control to keep the supporting tissues healthy (Wenstrom et al. 2005). This normally involves more than a customary visit every three months for a scale and polish. A professional periodontal and peri-implant maintenance programme should be instigated meticulously, with periodic documentation of clinical parameters and treatment end-points such as bleeding (BOP) and peri-implant pocketing (PPD) and stability of crestal bone levels (CBL). The supportive maintenance therapy should be individualised according to each patient s clinical requirements with full recording of all clinical parameters to facilitate a clear risk management strategy. Table 1: Aetiology of Peri-implant Diseases (PID): Host Susceptibility History of periodontal/peri-implant disease (strong evidence) Genetic susceptibility (insufficient evidence) Systemic disease/medical co-morbidities (e.g. uncontrolled diabetes, immunosuppression, radiotherapy) (insufficient evidence) Prosthetic Design Impassive fit (insufficient evidence) Poor access for plaque control (good evidence) Occlusal trauma or adverse loading conditions (inconclusive evidence) Implant Design Surface and/or geometry (inconclusive evidence) Excessive stress concentration at Bone Implant Interface (mostly preclinical evidence) Increased risk of plaque adhesion or retention (e.g. exposed endosteal implant surface) Type of abutment connection (inconclusive evidence) Patient Factors Poor plaque control (strong evidence) Smoking (strong evidence) Bone quality and quantity (mostly preclinical evidence) Iatrogenic Factors (dentist/surgeon related) Surgical trauma (mechanical damage) Implant malpositioning Extrusion of excess luting cement* This table summarises the biological and mechanical causative and predisposing factors that have been implicated in PID (see references ) (Adapted from Heitz-Mayfield et al 2008). * Cementitis is caused by extrusion of luting cement acting as plaque retention between the abutment and implant shoulder leading to peri-implant inflammation, fistula formation, discharge or bleeding. If untreated, this could also progress into deep seated infection with crestal bone loss. The use of radiopaque luting cements and satisfactory removal of all excess material after cementation is essential to eliminate cementitis. 2
3 Monitoring: Following the completion of treatment, the patient should be instructed on adequate home care and plaque control measures focusing on inter-dental cleaning with inter-proximal brushes. The patient should also be enrolled in an individually designed supportive periodontal therapy (SPT) and infection control program according to their specific risk assessment profile (Donos et al 2012). The objective is to prevent development or recurrence of infection around the natural dentition and the implants. The following regime of SPT is recommended: Periodic Examination: A routine examination (3, 6 or 12 monthly intervals) is recommended depending on severity of the case and presence of risk factors for disease development or progression (Donos et al 2012). The purpose of the peri-implant examination should be: a) To determine the health of peri-implant tissues and to identify any potential problems early. The following periodontal indices should be evaluated: bleeding on probing (BOP), probing depths (PD), and presence of plaque, suppuration or mobility. b) To check crestal bone levels in relation to a known reference point (e.g. implant shoulder). A baseline radiograph serves as a reference and is repeated as and when indicated by clinical circumstances and parameters including patient susceptibility. c) To reassess and reinforce plaque control/smoking cessation d) To check the stability of underlying medical conditions (e.g. diabetes) e) To check occlusal integration and harmony, identify occlusal trauma and associated wear and tear f) To check removable prostheses and need for relining g) To check and reinforce patient s oral hygiene technique and home-care Professional plaque control measures including oral hygiene reinforcement and subgingival/mucosal instrumentation should be performed as indicated every 3-6 months with ultrasonic and hand instruments specially modified for titanium surfaces. Clinical and Radiological Diagnostic Parameters: 1) Radiographs: A baseline radiograph is recommended at the time of implant loading to determine alveolar bone levels after the completion of the initial adaptive bone remodelling phase (Lang and Berglundh, 2011). The panoramic radiograph is not generally suitable to visualise peri-implant bone levels consistently. The baseline periapical radiograph is to serve as the reference from which future bone changes and progression of peri-implant disease could be determined. The radiograph should be repeated after the first year in function to check the stability of peri-implant bone support or when clinical parameters indicate disease. The frequency of subsequent radiological investigations should be dictated by individual clinical parameters. Presence of high (BoP) scores and PD 5mm are indications for further radiographic examination for bone margin evaluation and determination of further treatment needs (Donos et al, 2012). 2) Probing: Studies have shown no harm in routine peri-implant probing. Therefore, probing is recommended as a subjective index of monitoring the condition of the peri-implant soft tissues (Lang et al 2002 and 2004). Presence of exudate, bleeding (BOP) or swelling should be noted together with peri-implant pocket depth (PPD) measurements. The key parameter for diagnosis of peri-implant mucositis is BOP with gentle probing (<0.25N) (Lang and Berglundh, 2011), using ideally a calibrated metal or a plastic probe. Contrary to earlier concerns, this will not damage the tissues or the implant surface if carried out with light digital pressure. 3
4 The following periodontal indices to assess the presence or absence of peri-implant diseases (e.g. mucositis or peri-implantitis), should be evaluated periodically: 1. Plaque index (PI) 2. Bleeding on probing (BOP) (e.g. spontaneous : on probing or 30s after probing ) 3. The peri-implant probing depth (when possible using 6-point charting) 4. Presence of discharge, exudate, sinus or a fistula Table 2: Limitations of Probing: Probing is essential for diagnosis of peri-implant disease. However, probing may be limited by: Contour of prostheses Depth of the implant shoulder Design of implant shoulder/abutments 3) Mobility: Implant mobility should be checked for all free-standing implant restorations whenever possible as radiographs are not always diagnostic of a deterioration in osseointegration. A percussion test is often all that is needed to detect absence of mobility. However, it is inadvisable to disconnect a fixed prosthesis to check on individual implant mobility unless clinical signs and symptoms strongly suggest loss of osseointegration. Removal of abutments/restorations could disturb the equilibrium within the implant-abutment-soft tissue junction. Use of resonance frequency analysis (RFA), although a poor indicator of implant failure, has been shown to be a reliable test of implant stability and therefore could be used to document initial implant stability and integration. However, routine removal of restorations to document implant stability is not recommended. Table 3: Peri-implant Mucositis: Disease outcome: reversible Signs and symptoms (S&S) Bleeding on probing Increased PD Swelling Discharge or suppuration Pain or tenderness and/or fistula Diagnostic criteria: no radiological sign of CBL Table 4: Peri-implantitis: Disease outcome: irreversible Signs and symptoms (S&S) Bleeding on probing Increased PD Swelling Fistula Discharge or suppuration Diagnostic criteria: radiological sign of CBL Pain or tenderness 4
5 Table 5: Diagnosis of Peri-implant Diseases (PID): To clinically diagnose the presence of peri-implant diseases the following should be evaluated: Probing (using a light force <0.25N): Increase in PPD (from a fixed reference point) indicates loss of attachment. Enables a clinical diagnosis of peri-implantitis. BOP: Indicates inflammation. Diagnostic of peri-implant mucositis Periapical radiography: Crestal bone loss confirms the diagnosis of peri-implantitis. Continual CBL indicates Implant at Risk (IaR) Other S&S: Exudate; swelling and pain Interpretation of Results: a) Radiographs: the presence of peri-implant radiolucency or crestal bone loss is checked using the implant shoulder as a reference point. Distance between implant threads could be used to calculate the magnification factor when estimating bone loss. Baseline radiographs are used as a reference to compare stability of crestal bone support. b) Probing: (a calibrated periodontal probe) (<0.25N) is recommended. Probe using 6-point pocket charting when possible with a fixed reference point (e.g. crown margin). Record presence or absence of bleeding (BOP or 30s delayed), plaque accumulation, peri-implant pocket depth (mm) (PPD) and any suppuration. BPE score of teeth/ implants should be noted at each recall visit. Full mouth periodontal charting once a year or as clinically deemed necessary (e.g especially when BPE >3 or 4). Deeper pockets harbour pathogenic bacteria, therefore pocket reduction and improved plaque control should be an initial objective of peri-implant maintenance. c) Bleeding on probing: diagnostic of peri-implant mucositis. However false positives are possible if more than gentle pressure is exerted which could force the tip of the probe to penetrate circularly oriented weak fibres. d) Other S&S: Hyperplasia/fistula/exudate/pain. 5
6 Management and Individualised Supportive Therapy: Duty of Care and Patient/Clinician Responsibilities: Long-term success of implant treatment is multifactorial and primarily depends on satisfactory maintenance of health of peri-implant tissues. However, certain predisposition to peri-implant disease should be recognised and addressed during long-term maintenance of patients particularly with higher susceptibility. In this respect the dental team including the practitioner and the hygienist/therapist who are responsible for routine maintenance of the implant patient should be fully aware of their duty of care, not only in documenting the baseline clinical parameters of the health of peri-implant tissues but also in continuing to monitor these periodically during maintenance. Moreover, the implant patient should be fully educated on the effect of dental plaque on the long-term success of implants. Patients who present with higher risk or susceptibility (diabetes, smokers, history of periodontal disease) should be fully made aware of the implications of the risks and their need for systematic professional maintenance. Patients should be educated on their own responsibilities regarding the correct oral hygiene and home-care techniques. Clinicians are also required to screen their implant cases by periodic auditing of outcomes based on their implant log books. Routine Maintenance: The overall objectives of routine implant maintenance are similar to that of periodontal maintenance: establish presence of health or disease and offer supportive maintenance to improve plaque removal and oral hygiene. Implants should be cleaned subgingivally with gentle pressure using (preferably) titanium scalers. The use of plastic instruments are not recommended as these have been shown to be less efficient in removing subgingival plaque off implant surfaces. Table 6: Professional Cleaning Instruments and Devices: Different levels of evidence none considered state of the art. Titanium hand scalers Air abrasive device Lasers Consider recommending an antiseptic mouthwash such as Corsodyl, Delmopinol or essential oil mouthwash to control bacterial invasion. (Chlorhexidine must not be used at the same time as toothpaste, it should be used about 30 minutes afterwards otherwise there are interactions and decreased activity). Review to evaluate improvement in plaque control and to ensure full resolution. If untreated, peri-implant mucositis could lead to deeper pocketing and loss of peri-implant crestal bone. Table 7: Recommended Home Cleaning Devices Different levels of evidence none considered state of the art. Dental floss Interdental brushes Chlorhexidine, essential oils, or Delmopinol (weak evidence) See next page: 6
7 Maintenance Algorithm: Maintenance Fit of Prosthesis Baseline Periapical Radiograph Baseline PPD Oral hygiene Recall Every 6 months: PPD BOP / Exudate Mobility OH Prosthesis stability / Occlusion Peri-implant Tissue Tone, texture, colour At 1 Yr and Biannually: PA radiograph Mobility or Continued CBL after treatment for severe Peri-implantitis Yes Rule out loose prosthetic structure Explantation Healthy implant Mucositis / Poor OH Peri-implantitis Peri-implantitis PPD < 3mm PPD < 3mm PPD > 3mm PPD > 3mm No BOP BOP + ve/plaque + ve BOP + ve/plaque + ve BOP + ve/plaque + ve No Radiographical CBL No Radiographical CBL CBL < 2mm (cw BL) CBL > 2mm (cw BL) Aesthetic Assessment Recession will occur; is this acceptable? Warning: Non-surgical treatment may have reduced success in disease resolution when compared to surgical treatment No No Yes Risk Assessment Is surgery safe? Yes Maintenance Algorithm Non-surgical Algorithm* Surgical Algorithm* * Please refer to the ADI Guidelines on the Management of Peri-implant Diseases for these algorithms. 7
8 Long-term Monitoring and Outcome Measures: Studies have identified certain risk factors and co-morbidities that may affect the pathogenesis and progression of peri-implant diseases. These include radiotherapy, uncontrolled diabetes, susceptibility to periodontal disease, bruxism and smoking. Although for some of these conditions the evidence is insufficient or inconclusive, these risk factors should be carefully monitored and managed in patients with dental implants. Diabetic control should be checked using HB1Ac tests at least annually and patients should be counselled to discontinue smoking. Meticulous plaque control and control of occlusal harmony becomes more critical in patients who are susceptible to PID. Documentation of Long-term Monitoring of Implants: Records of individualised supportive therapy plan and recall attendance Periodontal indices Baseline and serial radiographs Restorative parameters and function Technical problems Mechanical problems with abutments/screws etc Crestal bone support and maintenance of osseointegration General patient satisfaction including aesthetics Success and Survival Criteria: In absence of an objective test, implant success should be documented using surrogate outcome measures or treatment end-points such as pain, BOP, PD and crestal bone loss (CBL). Survival statistics simply report on the presence or absence of an implant at the time of evaluation and do not take into consideration the health of the peri-implant tissues, thus a failing implant with gross bone loss could be reported as surviving. It is mandatory for the clinicians in charge of implant patient s maintenance to monitor and document implant outcome periodically and meticulously using the abovementioned parameters in order to manage emerging problems in a timely fashion. We suggest the following classification of implant success or failure: Table 8: Definition of Implant Success and Failure: Success Stable marginal bone levels after an initial crestal bone loss of < 1.5mm No BOP PD < 4 mm No mobility Good plaque control (FMPI < 20%) At Risk Initial bone loss of < 4mm but bone loss has been stabilised PD < 5mm No BOP immediate or delayed PI less than ideal Failing < 50% progressive bone loss which has not stabilised Deep pocketing BOP Less than ideal PC Pain Exudates/discharge Failed Deep pocketing Discharge BOP Mobility Lost or about to be lost 8
9 References: 1 Albrektsson T Branemark PI, Hannsson HA Lindstrom J Osseointegrated titanium implants. Requirements for ensuring a long-lasting direct bone-to-implant anchorage in man Acta Orthop Scand 1981; 52; Adell R, Lekholm U, Rockler B, Branemark PI A 15 year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg 1981;10: Berglundh T, Persson L, Klinge B. A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. J Clin Periodontol 2002;29: Zitzmann NU, Berglundh T Definition and prevelance of peri-implant diseases J Clin Periodontol 2008; 35: Matthoes N, Collier S, Walmsley AD Specialists management decisions and attitudes towards mucositiss and peri-implantitis BDJ 2012;212:E1 6 Lang NP, Berglundh T Proceedings of the Seventh European Workshop on Periodontology J of Clin Periodontol 2011; 38:s Thomas GW The Positive Relationship between Excess Cement and Peri-implant Disease J Periodontol Sep;80(9): Lindhe J, Meyle J; Group D of European Workshop on Periodontology. Peri-implant diseases: Consensus Report of the Sixth European Workshop on Periodontology. J Clin Periodontol Sep;35(8 Suppl): doi: /j X x. 9 Savi GE, Aglietta M, Eick S, Sculean A, Lang NP, Ramseier CA Reversibility of experimental peri-implant mucositis compared to experimental gingivitis in man. Clin Oral Implant Research in press. 10 Zitzmann N, Berglundh T. Definition and prevalence of peri-implant diseases J Clin Periodontol : Iacono VJ Dental Implants in Periodontal Therapy J Periodontol 71: Silverstien 2003 no to probing?? Silverstein L, Garg A, Callan D, Shatz P: The key to success: Maintaining the long-term health of implants. Dentistry Today 1998;17(2): Silverstein L, Kurtzman GM. Dental implants: oral hygiene and maintenance. Implant Dentistry Today : Lang NP, Wetzel AC, Stich H, Caffesse RG.Histologic probe penetration in healthy and inflamed peri implant tissues. Clin Oral Implants Res Dec; 5(4): Heitz-Mayfield LJ. Peri-implant diseases: diagnosis and risk indicators J Clin Periodontol : Lindhe J, Meyle J; Group D of European Workshop on Periodontology. Peri-implant diseases: Consensus Report of the Sixth European Workshop on Periodontology. J Clin Periodontol : Sison S Implant maintenance and the dental hygienist. Access 2003 supp Pontoriero R, Tonelli MP, Carnevale G, Mombelli A, Nyman SR, Lang NP.Peri-implant probing (with a color-coded plastic probe) around a symptomatic implant shows a... Eur J Oral Sci 1998;106: e Espostio M, Hirsch JM, Lekholm U, Thomsen P Differential diagnosis and treatment of the strategies for biological complications and failing oral implants Int J Maxillofac Implants : Pye AD, Lockhart DEA, Dawson MP, Murray CA, Smith AJ A review of dental implants and infection Journal of Hospital Infection 72; Augthun M, Tinschert J, Huber A. In Vitro studies on the effect of cleaning methods on different implant surfaces. J Periodontol 1998;69(8): Fox SC, Moriarty JD, Kusy RP The effects of scaling a titanium implant surface with metal and plastic instruments J Periodontol : Mann M, Parmar D, Walmsley A D, Lea S C Effect of plastic-covered ultrasonic scalers. Clin Oral Impl Res : Kawashima H, Sato S, Kishida M, Yagi H, Matsumoto K, Ito K Treatment of Titanium Dental Implants With Three Piezoelectric Ultrasonic Scalers: An In Vivo Study J Periodontol : Mengel R, Buns CE, Mengel C, Flores-de-Jacoby L. An In Vitro study of the treatment with different instrument. Int J Oral Maxillofac Implants :91 26 Brookshire FV, Nagy W, Dhuru V B, Ziebert G, Chada S. The qualitative effects of various types of hygiene insruments on commercially pure titanium. J Prosthet Dent : Sison S Implant maintenance and the dental hygienist. Access 2003 supp Strietzel FP, Reichart PA, Kale A, Kulkarni M, Kuchler I (2007) Smoking interferes with prognosis of dental treatment; a systematic review and meta-analysis J Clin Periodontol 34: Bain C (2003) Implant installation in the smoking patient Periodontology : Galindo-Moreno P, Fauri M, Avila-Ortiz G, Fernandez J, Cabrera-Leon A, Sanchez-Fernandez E (2004) Influence of alcohol and tobacco habits on peri-implant marginal bone loss: a prospective study Clin Oral Impl Res 16: Kumar A, Jaffin RA, Berman C (2002) The effect of smoking on achieving osseointegration of surface modified implants: a clinical report. Int J Oral & Maxillofacial implants 17: Lobbezzo F, Van der Zaag J, Naeije M (2006) Bruxism: Its multiple cause and its effect on dental implants J Oral Rehabil :
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Maintenance in the Periodontally Compromised Patient. Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club
 Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
The Endodontic / Implant Controversy
 The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
Primary prevention of periimplantitis: peri-implant mucositis S152
 J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Peri-implant marginal bone loss: What is the current concensus? an academic controversy or a clinical challenge?
 Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester
 Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
14/09/15. Assessment of Periodontal Disease. Outline. Why is Periodontal assessment needed? The Basics of Periodontal assessment
 Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Auditing in periodontal treatment and disease.
 .. Auditing in periodontal treatment and disease. Background. Undiagnosed and untreated periodontal disease is one of the fastest growing areas of litigation and complaints in dentistry. People are living
.. Auditing in periodontal treatment and disease. Background. Undiagnosed and untreated periodontal disease is one of the fastest growing areas of litigation and complaints in dentistry. People are living
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
There are three referral categories used in the dental referral system:
 Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
History Why we need to classify?
 Aiming to Cover: MSc ADVANCED GENERAL DENTAL PRACTICE Classification & Recognition of Periodontal Disease Classification of periodontal disease Recognition of Disease DR MIKE MILWARD BDS (Birmingham),
Aiming to Cover: MSc ADVANCED GENERAL DENTAL PRACTICE Classification & Recognition of Periodontal Disease Classification of periodontal disease Recognition of Disease DR MIKE MILWARD BDS (Birmingham),
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Clinical Management of an Unusual Case of Gingival Enlargement
 Clinical Management of an Unusual Case of Gingival Enlargement Abstract Aim: The purpose of this article is to report a case of conditioned gingival enlargement managed by nonsurgical periodontal therapy.
Clinical Management of an Unusual Case of Gingival Enlargement Abstract Aim: The purpose of this article is to report a case of conditioned gingival enlargement managed by nonsurgical periodontal therapy.
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners
 Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and
Appendix 1 - Restorative Dentistry Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and
An Introduction to Dental Implants
 An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
The International Journal of Periodontics & Restorative Dentistry
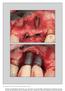 The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES
 Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Screenings, Indices Their influence on the treatment plan (Berne concept)
 Screenings, Indices Their influence on the treatment plan (Berne concept) 1. 2. 3. 4. Garguilo AW, Wentz FM, Orban B. Dimensions and relations of thedentogingival junction in humans. J Periodontol 1961;
Screenings, Indices Their influence on the treatment plan (Berne concept) 1. 2. 3. 4. Garguilo AW, Wentz FM, Orban B. Dimensions and relations of thedentogingival junction in humans. J Periodontol 1961;
Implantology without Periodontology is like Yin without Yang.
 Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
Periodontal Maintenance
 Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Dental Radiography Series
 Dental Radiography Series Guidelines for prescribing dental radiographs. Background Radiological s are used to discover and define the type and extent of disease in many clinical situations. However, public
Dental Radiography Series Guidelines for prescribing dental radiographs. Background Radiological s are used to discover and define the type and extent of disease in many clinical situations. However, public
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr.
 Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
 ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Periodontal (Gum) Disease
 Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Gum Disease (Periodontitis) THE FACTS. and Specialist Treatments available THE DENTAL IMPLANT CLINIC. centre of excellence
 Gum Disease (Periodontitis) THE FACTS and Specialist Treatments available THE DENTAL IMPLANT CLINIC centre of excellence Our specialist service The Dental Implant Clinic offers specialist services in
Gum Disease (Periodontitis) THE FACTS and Specialist Treatments available THE DENTAL IMPLANT CLINIC centre of excellence Our specialist service The Dental Implant Clinic offers specialist services in
Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients
 Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients Taha Y. Hamad, B.D.S., H.D.D., M.Sc. (1) Background: Excessive crestal bone loss after dental implant occurs
Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients Taha Y. Hamad, B.D.S., H.D.D., M.Sc. (1) Background: Excessive crestal bone loss after dental implant occurs
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
EVERYONE I M P L A N T C O M P A N Y
 A SMILE FOR EVERYONE I M P L A N T C O M P A N Y WHAT IS AN IMPLANT? A dental implant is an effective alternative to the root of a tooth. It consists of a titanium screw only a few millimetres in size.
A SMILE FOR EVERYONE I M P L A N T C O M P A N Y WHAT IS AN IMPLANT? A dental implant is an effective alternative to the root of a tooth. It consists of a titanium screw only a few millimetres in size.
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Assessment of Knowledge of Oral Hygiene Aids among Dentists
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 10, Issue 5 (Sep.- Oct. 2013), PP 60-64 Assessment of Knowledge of Oral Hygiene Aids among Dentists
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 10, Issue 5 (Sep.- Oct. 2013), PP 60-64 Assessment of Knowledge of Oral Hygiene Aids among Dentists
Risk management in clinical practice. Part 10. Periodontology
 Risk management in clinical practice. Part 10. Periodontology P. Baker 1 and I. Needleman 2 in brief Failure to diagnose or treat periodontal disease is the fastest growing area of litigation in dentistry.
Risk management in clinical practice. Part 10. Periodontology P. Baker 1 and I. Needleman 2 in brief Failure to diagnose or treat periodontal disease is the fastest growing area of litigation in dentistry.
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y
 Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Electronic Dental Records
 Electronic Dental Records Dr. Douglas K Benn, Professor of Maxillofacial Radiology & Director of Oral Diagnostic Systems, University of Florida and Health Conundrums LLC 8/2/2008 Dr Benn, University of
Electronic Dental Records Dr. Douglas K Benn, Professor of Maxillofacial Radiology & Director of Oral Diagnostic Systems, University of Florida and Health Conundrums LLC 8/2/2008 Dr Benn, University of
Delta Dental of Virginia Clinical Policy # 402
 Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Diagnosis. overt Examination. Definitive Examination. History. atient interview. Personal History. Clinical Examination.
 Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
THE AMERICAN ACADEMY OF PERIODONTOLOGY
 THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
Overcoming and Preventing Dental Implant Complications: Abutment Fracture Case Report
 CASE REPORT J Korean Dent Sci. 2013;6(1):27-33 http://dx.doi.org/10.5856/jkds.2013.6.1.27 ISSN 2005-4742 Overcoming and Preventing Dental Implant Complications: Abutment Fracture Case Report Se Hoon Kahm
CASE REPORT J Korean Dent Sci. 2013;6(1):27-33 http://dx.doi.org/10.5856/jkds.2013.6.1.27 ISSN 2005-4742 Overcoming and Preventing Dental Implant Complications: Abutment Fracture Case Report Se Hoon Kahm
The notable success of dental implants. Relationship Between Smoking and Bleeding on Probing RESEARCH
 RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
Core build-up using post systems
 Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Contents Graduate Diploma of Dental Implantology
 Graduate Diploma of Dental Implantology Information Brochure Contents Graduate Diploma of Dental Implantology DOH 551 Introduction to Dental Implants and Basic Restorative Implantology Module 1 Fundamentals
Graduate Diploma of Dental Implantology Information Brochure Contents Graduate Diploma of Dental Implantology DOH 551 Introduction to Dental Implants and Basic Restorative Implantology Module 1 Fundamentals
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014
 Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014 Tooth Replacement treatment options and benefits Identify Existing Patients
Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014 Tooth Replacement treatment options and benefits Identify Existing Patients
Periodontal Case Report
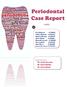 Periodontal Case Report By Dan AlAhmed 431200041 Saleha AlZahrani 431200123 Raghad AlSaawy 431200297 Afnan AlAssiri 431200687 Mawadh Demyati 431200824 Hend Jaddoh 431201247 Alaa AlDoss 431201808 Rawan
Periodontal Case Report By Dan AlAhmed 431200041 Saleha AlZahrani 431200123 Raghad AlSaawy 431200297 Afnan AlAssiri 431200687 Mawadh Demyati 431200824 Hend Jaddoh 431201247 Alaa AlDoss 431201808 Rawan
SIGNIFICANCE OF FAILING DENTITION AND IMPACT ON ORAL HEALTH BSDHT CONFERENCE
 SIGNIFICANCE OF FAILING DENTITION AND IMPACT ON ORAL HEALTH BSDHT CONFERENCE PREVENTION IS BETTER THAN CURE The aim of our treatment should be to create a situation of stability, predictability and longevity
SIGNIFICANCE OF FAILING DENTITION AND IMPACT ON ORAL HEALTH BSDHT CONFERENCE PREVENTION IS BETTER THAN CURE The aim of our treatment should be to create a situation of stability, predictability and longevity
Dentistry at Willow Mill Veterinary Hospital. Importance of Good Oral Hygiene. Steps for a Healthy Mouth
 Willow Mill Veterinary Hospital 11 Willow Mill Park Road Mechanicsburg, PA 17050 www.willowmillvet.com Phone: (717)766-7981 Fax: (717) 766-6727 Email:willowmillvethosp@gmail.com Mon-Fri: 8AM-7PM, Sat:
Willow Mill Veterinary Hospital 11 Willow Mill Park Road Mechanicsburg, PA 17050 www.willowmillvet.com Phone: (717)766-7981 Fax: (717) 766-6727 Email:willowmillvethosp@gmail.com Mon-Fri: 8AM-7PM, Sat:
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report
 Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
European Federation of Periodontology
 The 1999 classification system was the first to recognise the need to classify gingival diseases and conditions, but there were many flaws in its approach. It did not define health and the description
The 1999 classification system was the first to recognise the need to classify gingival diseases and conditions, but there were many flaws in its approach. It did not define health and the description
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review
 The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
Managing the failing dentition
 C L I N I C A L Managing the failing dentition Kamal Suri 1 Increasingly, the numbers of patients walking through the doors of our practices are those whose dentition is slowly in decline. I am presented
C L I N I C A L Managing the failing dentition Kamal Suri 1 Increasingly, the numbers of patients walking through the doors of our practices are those whose dentition is slowly in decline. I am presented
Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus
 Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus Doina Lucia Ghergic, Claudia Florina Andreescu, Catalina Grigore Constanta, Romania Summary Diabetes
Assessment of periodontal status and oral hygiene habits in a group of adults with type I diabetes mellitus Doina Lucia Ghergic, Claudia Florina Andreescu, Catalina Grigore Constanta, Romania Summary Diabetes
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Regaining Your Gum Tissue. Soft-Tissue Regeneration With Geistlich Mucograft
 Regaining Your Gum Tissue Soft-Tissue Regeneration With Geistlich Mucograft Why is Healthy Gum Tissue So Important? Gum tissue can recede due to grinding of the teeth, thin insufficient gum tissue, as
Regaining Your Gum Tissue Soft-Tissue Regeneration With Geistlich Mucograft Why is Healthy Gum Tissue So Important? Gum tissue can recede due to grinding of the teeth, thin insufficient gum tissue, as
IMPLANTS. Guideline Number: DCG Effective Date: January 1, 2018
 IMPLANTS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG007.04 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1 COVERAGE RATIONALE...1
IMPLANTS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG007.04 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1 COVERAGE RATIONALE...1
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Interrelationship between Periodontitis and Peri-Implantitis: Myth or Reality?
 REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93.
 Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Limited To Endodontics Newsletter. Limited To Endodontics A Practice Of Endodontic Specialists July Volume 2
 Limited To Endodontics Newsletter LTE Limited To Endodontics A Practice Of Endodontic Specialists July 1 2009 Volume 2 Endodontic Treatment For The Compromised Tooth The goal of endodontic therapy is to
Limited To Endodontics Newsletter LTE Limited To Endodontics A Practice Of Endodontic Specialists July 1 2009 Volume 2 Endodontic Treatment For The Compromised Tooth The goal of endodontic therapy is to
Informed Consent. (Initials )
 Informed Consent 1. EXAMINATIONS AND X-RAYS I understand that the initial visit may require radiographs in order to complete the examination, diagnosis and treatment plan. I understand I am to have work
Informed Consent 1. EXAMINATIONS AND X-RAYS I understand that the initial visit may require radiographs in order to complete the examination, diagnosis and treatment plan. I understand I am to have work
The London Centre for Implant and Aesthetic Dentistry. Information sheet : Gum disease (Gingivitis and Periodontitis)
 Information sheet : Gum disease (Gingivitis and Periodontitis) (2016a. This information sheet contains general information and must be read in conjunction with your personalised treatment plan for specific
Information sheet : Gum disease (Gingivitis and Periodontitis) (2016a. This information sheet contains general information and must be read in conjunction with your personalised treatment plan for specific
Implant failures, peri-implant bone loss and other complications
 Surgical Risk Factors in Implant Dentistry: Influence on Failures and Bone Loss Murray Arlin, DDS, Dip. Perio, FRCD(C) Implant failures, peri-implant bone loss and other complications do occur, so it is
Surgical Risk Factors in Implant Dentistry: Influence on Failures and Bone Loss Murray Arlin, DDS, Dip. Perio, FRCD(C) Implant failures, peri-implant bone loss and other complications do occur, so it is
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature
 The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space
 Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
BASIC Level 1 Practitioner Certification
 Chapter 5 Place the Prosthesis Because dental implants are now an important and distinct part of prosthodontic dentistry, general dentists must be well versed in all aspects of the treatment option. The
Chapter 5 Place the Prosthesis Because dental implants are now an important and distinct part of prosthodontic dentistry, general dentists must be well versed in all aspects of the treatment option. The
Safety and esthetics with
 Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
DENTAL IMPLANTS Overview
 DENTAL IMPLANTS Overview NAME: DATE: DENTIST: RECORD GATHERING: RADIOGRAPHS: PRE- TREATMENT: PRE-OP SCALE & CLEAN: SURGERY (temp/no temp/healer cap): POST-OP REVIEW: FINAL RESTORATIVE APPOINTMENTS: OTHER
DENTAL IMPLANTS Overview NAME: DATE: DENTIST: RECORD GATHERING: RADIOGRAPHS: PRE- TREATMENT: PRE-OP SCALE & CLEAN: SURGERY (temp/no temp/healer cap): POST-OP REVIEW: FINAL RESTORATIVE APPOINTMENTS: OTHER
Treatment Concepts for PERI-IMPLANTITIS
 Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Patient information on the treatment of gum disease. More than 2 million patients treated. Saving teeth for more than 20 years Straumann Emdogain
 Patient information on the treatment of gum disease More than 2 million patients treated Saving teeth for more than 20 years Straumann Emdogain What do you know about gum disease? Gum disease is the most
Patient information on the treatment of gum disease More than 2 million patients treated Saving teeth for more than 20 years Straumann Emdogain What do you know about gum disease? Gum disease is the most
Evaluation of fixed partial denture in relation to gingival recession and other factors
 Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
Evaluation of fixed partial denture in relation to gingival recession and other factors Faiza M. Abdul Ameer,B.D.S., M. Sc. (1) Zainab M. Abdul Ameer,B.D.S., M. Sc (2) ABSTRACT Background: Gingival recession
When Teeth Go Bad How nurse advice can help reduce recurrences of dental disease. Callum Blair BVMS MRCVS
 When Teeth Go Bad How nurse advice can help reduce recurrences of dental disease Callum Blair BVMS MRCVS Dental disease is a common condition affecting cats and dogs. An often quoted statistic is that
When Teeth Go Bad How nurse advice can help reduce recurrences of dental disease Callum Blair BVMS MRCVS Dental disease is a common condition affecting cats and dogs. An often quoted statistic is that
SPECIAL SUPPLEMENT. Inside this issue: 2014 No. 3. Peri-implant disease Implant surface: An evolution Summaries of select scientific publications
 www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
WHAT IS THE PURPOSE OF WHAT WE DO? TEAM PERIODONTICS: WORKING TOGETHER TO IMPROVE PATIENT CARE YOU ARE THE PERIODONTISTS IN YOUR PRACTICE!
 Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Appendix. CPT only copyright 2007 American Medical Association. All rights reserved. NTHSteps Dental Guidelines
 Appendix NTHSteps Dental Guidelines N N.1 American Academy of Pediatric Dentistry Periodicity Guidelines.................. N-2 N.2 American Dental Association Guidelines for Prescribing Dental Radiographs.........
Appendix NTHSteps Dental Guidelines N N.1 American Academy of Pediatric Dentistry Periodicity Guidelines.................. N-2 N.2 American Dental Association Guidelines for Prescribing Dental Radiographs.........
Clinpro Glycine Prophy Powder
 Clinpro Glycine Prophy Powder 3M 2016. All Rights Reserved VIDEO 3M 2016. All Rights Reserved 2 Presentation Overview Air Polishing Procedure With Clinpro Glyciene Prophy Powder Use and Efficiency for
Clinpro Glycine Prophy Powder 3M 2016. All Rights Reserved VIDEO 3M 2016. All Rights Reserved 2 Presentation Overview Air Polishing Procedure With Clinpro Glyciene Prophy Powder Use and Efficiency for
Referral of Patients. to the. Community Dental Referral Service. Hillingdon
 Referral of Patients to the Community Dental Referral Service In Hillingdon June 2012 1 Contents Page Background 3 Best use of Resources 3 Process for Referral 3-4 Acceptance Criteria for Specialist Treatment
Referral of Patients to the Community Dental Referral Service In Hillingdon June 2012 1 Contents Page Background 3 Best use of Resources 3 Process for Referral 3-4 Acceptance Criteria for Specialist Treatment
Building a Strong Team for the Dental Implant Practice
 Building a Strong Team for the Dental Implant Practice Samuel M. Strong, DDS Stephanie Strong, RDH, BS Course Synopsis This course deals with the organization and training to successfully complete restorative
Building a Strong Team for the Dental Implant Practice Samuel M. Strong, DDS Stephanie Strong, RDH, BS Course Synopsis This course deals with the organization and training to successfully complete restorative
