Evaluation of bone healing using rhbmp-2 soaked hydroxyapatite in ridge augmentation: a prospective observational study
|
|
|
- Briana Hunt
- 5 years ago
- Views:
Transcription
1 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:40 DOI /s Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Evaluation of bone healing using rhbmp-2 soaked hydroxyapatite in ridge augmentation: a prospective observational study Hyun-Suk Kim 1*, Ju-Cheol Park 2,3, Pil-Young Yun 1 and Young-Kyun Kim 1,3* Abstract Background: The goal of this study is to evaluate complication and effectiveness of alveolar ridge augmentations using a hydroxyapatite-based alloplastic bony substitute with rhbmp-2. Methods: A total of 10 patients (4 males, 6 females; 58.5 ± 8.6 years) participated in this clinical research. Alveolar ridge augmentations were performed in edentulous (4 maxillary posterior, 5 mandibular posterior, and 1 mandibular anterior) regions. Anorganic bovine bone (ABB; Bio-Oss, Geistlich Pharma AG, Wolhusen, Switzerland) was used as the bone graft material in the control group (n = 5)) while hydroxyapatite-based alloplastic bony substitute with rhbmp-2(ha+rhbmp-2; NOVOSIS -Dent, CGBio Inc., Seongnam, Korea) was used in the experimental group (n = 5). In order to evaluate relative changes in bone volume and resorption rate of the bone graft material, CBCT radiographs were taken immediately and at 4 months after the bone graft in all subjects. Among the 10 patients, 8 received dental implants in Seoul National University Bundang Hospital, while the others received in local clinics. Bone specimens for further histomorphometric examinations were gained from these 8 patients using trephine burs during the implant placements. Clinical, radiographic, and histomorphometric evaluations were focused because of the small sample size. Results: When CBCT radiographs were compared between immediately and at 4.07 ± 0.13 months after the bone graft, both alveolar bone widths (ABB 2.52 ± 0.18 mm, HA+rhBMP ± 0.85 mm) and heights (ABB 1.68 ± 0.17 mm, HA+rhBMP ± 0.28 mm) increased in the two groups. Resorption rates of transplanted bone graft material in the alveolar bone widths and heights were (ABB 29.7 ± 8.8%, HA+rhBMP ± 7.4%) and (ABB 39.2 ± 21.8%, HA+rhBMP ± 6.5%), respectively. Histomorphometrically, ABB group showed bone formation via osteoconduction and HA+rhBMP-2 group via osteoinduction. HA+rhBMP-2 group showed more bone formation around the bone graft materials than the ABB group. Postoperative complications were not found in all subjects. Conclusions: Our study had following conclusions: (1) Ridge augmentations using HA+rhBMP-2 could be clinically useful to supplement implant placements in edentulous regions. (2) Serious postoperative complications related to the graft material did not occur. Keywords: Alveolar ridge augmentation, Bone morphogenetic protein 2, Bone regeneration, Hydroxyapatite * Correspondence: 54211@snubh.org; kyk0505@snubh.org 1 Department of Oral and Maxillofacial Surgery, Section of Dentistry, Seoul National University Bundang Hospital, 300 Gumi-dong, Bundang-gu, Seongnam, Gyunggi-do, South Korea Full list of author information is available at the end of the article The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
2 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:40 Page 2 of 6 Background Adequate bone volume is one of the important factors to obtain osseointegration in dental implants. In 1986, Lekholm et al. reported that for the implant success, a minimum of 1 mm or more of the buccal and lingual bone was necessary surrounding the implant surface. Clinicians often encounter patients with deficient vertical or horizontal alveolar bones. Reasons may vary from trauma, periodontal disease, tooth extraction, and to tumor. Under such circumstances, the implant surface may not be entirely covered by the bone, and this could increase the risk of infection, gingival recession, non-esthetic appearance, poor oral hygiene maintenance, and peri-implantitis [1]. The ideal bone graft material should have no immune response and include growth factors that facilitate rapid bone formation and re-vascularization. It should also be able to maintain space for new bone infiltration and readily available in clinics. Autografts are known to be the ideal material for the reconstruction of bone defects. Autografts have osteogenesis, osteoconduction, and osteoinduction abilities that enable rapid bone healing without inducting immune responses. They are, however, difficult to obtain in sufficient quantities without causing complications in the donor site and a large amount of the transplanted grafts often get absorbed. To overcome the problems, other bone substitutes such as allografts, xenografts, and alloplasts have been developed and used. However, allografts and xenografts could be problematic due to the risk of infection and high price. The alloplasts are cheap and have no risk of infection, but they lack osteogenesis and osteoinduction abilities to form viable bone tissue [2]. Bone morphogenetic protein (BMP), the leading osteoinductive growth factor, has been studied since 1995 and extensively in the 2000s. Animal studies focused on discovering roles of BMP in guided bone regeneration (GBR) when delivered with drug carriers [3, 4]. In general, osteoinductive capabilities should be given to osteoconductive bone graft materials for bone graft material development. Various proteins, such as BMP-2, 4, 7, and 14, have been reported to have osteoinductive abilities in animal experiments. In particular, BMP-2 act as a growth and differentiation factor in the body and promotes the new bone formation by acting extensively at the entire stage of osteogenesis ranging from mesenchymal stem cellsosteoprogenitor-preosteoblast-osteoblast-osteocytic osteoblast-osteocyte [5]. BMP-2 also showed potential for bone regeneration through various studies including sinus augmentation [6, 7], alveolar bone preservation [8], bone augmentation [9], and periodontal recovery [10]. Ike and Urist reported that BMP-2 contained in dentin exhibited osteoinductive abilities important for osteogenesis [11]. Jung et al. showed that GBR with combination of the xenograft (Bio-Oss) with rhbmp-2 can enhance the maturation process of bone regeneration [12]. Similar to other growth factors, BMP-2 requires a carrier system that could provide optimal cellular and vascular growth, cellular attachment, and release kinetics [13, 14]. Highly soluble, BMP-2 requires robust scaffolds over long periods that act as drug carrier at the implant site to exert osteoinductive effects [15, 16]. Ideal scaffolds should control-release growth factors and prevent degradations. Various materials have been proposed, and absorbable collagen sponge (ACS) has been the most documented carrier for rhbmp-2 because of its high binding and retention capacities for the rhbmp-2. According to a study by Hwang, the use of rhbmp-2 with ACS could result in accelerated bone formation compared to conventional bone grafting in postoperative bone defects [17]. However, collagen lacks osteoconductivity as well as structural integrity in transplanted sites. Therefore, calcium phosphates, such as hydroxyapatite (HA) and β-tricalcium phosphate (β-tcp), have been considered as suitable candidates for rhbmp-2 delivery system because of their space-providing properties [18]. The goal of this study is to evaluate effectiveness and complication of alveolar ridge augmentations using a hydroxyapatite-based alloplastic bony substitute with rhbmp-2. Methods Patients A total of 10 patients (4 males, 6 females; 58.5 ± 8.6 years) participated in this clinical research. Alveolar ridge augmentations were performed in edentulous (4 maxillary posterior, 5 mandibular posterior, and 1 mandibular anterior) regions. Surgical procedure All patients received alveolar bone augmentation in the deficient ridge areas. Under local anesthesia using 1% lidocaine with 1:100,000 epinephrine (Huons, Hwasung, Korea), vertical and horizontal incisions were made in the mucoperiosteum of the labial or buccal sides of edentulous regions. A periosteal flap was elevated with a periosteal elevator, and a selection of bone graft materials was placed underneath the highly cross-linked resorbable collagen membrane (Ossix Plus, Datum Dental Ltd., Telrad, Israel). Anorganic bovine bone (ABB; Bio-Oss, Geistlich Pharma AG, Wolhusen, Switzerland) was used as the bone graft material in the control group (n = 5) while hydroxyapatite-based alloplastic bony substitute with rhbmp-2(ha+rhbmp-2; NOVOSIS -Dent, CGBio Inc., Seongnam, Korea) was used in the experimental group (n = 5). NOVOSIS -DENT uses synthetic
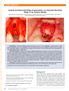
3 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:40 grafting bone (hydroxyapatite) as multi-pore ceramic supporter to convey BMP-2 to the human body. Graft materials were prepared according to manufacturer s instructions. The mucoperiosteal flaps were then closed with 4 0 Vicryl (polyglactin; Ethicon Inc., Sommerville, NJ) using a simple interrupted suture technique. Patients who underwent surgery took antibiotics (amoxicillin/clavulanate; Augmentin, Ilsung Pharmaceuticals Co., Seoul, Korea) and a non-steroidal anti-inflammatory drug (talniflumate; Somalgen, Kunwha Pharmaceutical Co., Seoul, Korea) for 5 days postoperatively. A 100 ml of 0.1% chlorhexidine mouth gargling (Hexamedine, Bukwang Pharm, Ansan, Korea) was prescribed for oral hygiene maintenance. Sutures were stitched out between 1 and 2 weeks after the surgery. Case A 60-year-old female came to our department for restoration of left mandibular premolar and molar areas. On deficient alveolar ridge, ABB with resorbable collagen membrane was grafted. To radiographically evaluate the bone resorption and formation, as well as to provide support for graft materials, tenting screws were installed around the bone grafts (Fig. 1). Measurement of alveolar bone volume change To evaluate relative changes in bone volume and resorption rate of the bone graft material, three dimensional measurements were obtained by cone-beam computed tomography (CBCT) immediately and at 4 months after the bone graft in all subjects (Fig. 2). The changes in bone width and height between the two groups were calculated, and Mann-Whitney U test (SPSS Inc., Chicago, IL, USA) was used to evaluate statistical significance. P values less than 0.05 were considered to be statistically significant. Among 10 patients, 8 received dental implants in Seoul National University Bundang Hospital, while the others received in local clinics. Page 3 of 6 Histomorphometric assessment Bone specimens for further histomorphometric examinations were gained from the 8 patients who received implants in Seoul National University Bundang Hospital (control n = 4, experimental n = 4) using trephine burs during the implant placements. The acquired specimens were decalcified using 10% formic acid for 3 weeks, embedded in paraffin, and sagittal sections were obtained and then stained with hematoxylin and eosin (H&E) for histologic examinations. Because of a small sample size, histologic, radiographic, and clinical evaluations were focused. To determine the relative amount of bone formation, the new bone formation ratio was measured using the analysis LS starter program. The new bone formation was observed around the material in each of the 4 patient samples of each selected group, and the mean values of the areas were calculated. Statistical difference between bone formation of the two groups were calculated using Mann-Whitney U test. This study was approved by the Institutional Review Board of Seoul National University Bundang Hospital (E ). Results Postoperative complications were not found in all subjects. Augmented bone volumes and resorption rates When CBCT radiographs were compared between immediately and at 4.07 ± 0.13 months after the bone graft, both alveolar bone widths (ABB 2.52 ± 0.18 mm, HA+rhBMP ± 0.85 mm) and heights (ABB 1.68 ± 0.17 mm, HA +rhbmp ± 0.28 mm) increased in the two test groups. Resorption rates of transplanted bone graft material in the alveolar bone widths and heights were (ABB 29.7 ± 8.8%, HA+rhBMP ± 7.4%) and (ABB 39.2 ± 21.8%, HA+rhBMP ± 6.5%), respectively (Table 1). Significant differences were not found in bone width and Fig. 1 Intraoral photographs of ridge augmentation using bone graft material and resorbable collagen membrane. a Deficient alveolar ridge. b Mucoperiosteal flap elevation. c Tenting screws installed around the bone grafts. d Bone graft placed. e Resorbable collagen membrane applied
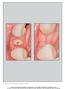
4 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:40 Page 4 of 6 Fig. 2 CBCT, postoperative view. a Immediately after the bone graft. b Four months after the graft height resorptions between ABB and HA+rhBMP-2 groups (width p = 0.841, height p =0.548). Histomorphometric findings of new bone formation Bone formations were observed in both groups, but the appearance was different. Histomorphometrically, HA +rhbmp-2 group showed more bone formation around the bone graft materials than the ABB group (Fig. 3). Osteoconduction was observed around the material in the ABB group. In other words, ABB served as a bridge to bone formation as a scaffold. In the HA+rhBMP-2 group, osteoinduction occurred around the material and bone formation was observed. HA+rhBMP-2 group (35.2 ± 19.7%) showed more relative bone formation compared to the ABB group (28.9 ± 10.3%), but significant difference was not found (p = 0.886) (Fig. 4). Discussion Despite possessing good biocompatibility and osteoconductive potential, most of commercially available graft materials lack osteoinductive potential. Much research thus has been focused on graft materials mixed with additives that could promote osteogenic potentials such as bone morphogenetic protein (BMP). Kim et al. studies showed that demineralized dentin matrix (DDM) could act as an effective rhbmp-2 carrier [4, 13]. Kim also had reported that HA or DDM scaffolds could be combined with rhbmp-2 and promote bone formation [19]. A study from Kim et al. showed that low-dose Escherichia coli derived rhbmp-2 with HA is as effective as anorganic bovine bone xenografts in early stages for enhanced bone formation after maxillary sinus floor augmentation without any major intraoperative or postoperative complications [7]. The soft tissue and residual graft areas showed no significant differences between the groups and rhbmp-2 antibody in the serum after BMP-2/H grafting did not increase significantly. A study by Burkus et al. showed that formation of anti-bmp-2 antibodies are low and transient in patients treated with rhbmp-2 [20]. Moreover, small formation of antibodies did not affect fusion success and had no visible affect clinical sequelae. Many studies support that BMP-2 is an effective osteoinducer, and there is no evidence that administration of rhbmp-2 at the time of surgery links with an increased risk of cancer [21, 22]. However, rhbmp-2 could induce adverse clinical effects, including ectopic bone formation and tissue inflammation when used in high concentrations [23, 24]. NOVOSIS -Dent is a graft material used in combination with rhbmp-2 and HA carrier in alveolar bone defect areas. In order for rhbmp-2 to exert its effects, it must act locally at the site where new bone formation is required, and for this reason, it is commonly used with carriers capable of releasing from local sites. The carrier of NOVOSIS -Dent is HA, a material that occupies 65% of the bone and 98% of the dental enamel, and it provides osteoconduction by providing a porous structure Table 1 Amount of bone augmentation Group Width Height T 1 (mm) T 4 (mm) Bone resorption (%) T 1 (mm) T 4 (mm) Bone resorption (%) ABB 3.7 ± ± ± ± ± ± 21.8 HA+rhBMP ± ± ± ± ± ± 6.5 P value Abbreviations: ABB anorganic bovine bone, HA hydroxyapatite, rhbmp-2 recombinant human bone morphogenetic protein-2, T 1 immediately postoperative augmented bone, T 4 augmented bone after 4 months after the graft
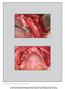
5 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:40 Page 5 of 6 Fig. 3 Histologic findings after 4 months of bone healing. a ABB. b HA+rhBMP-2. New bone formations (arrows) are observed between the graft materials (stars) and adjacent bones (83% porosity, 300 μm pore size). NOVOSIS -Dent provides osteoconduction by using HA as a carrier and osteoinduction capability by utilizing BMP-2 to form a new bone at the bone defect site. In this study, HA+rhBMP-2 showed relatively good bone formation compared with ABB. Although HA+rhBMP-2 had less volume of bone augmentation (widths ABB 2.52 ± 0.18 mm, HA+rhBMP ± 0.85 mm; heights ABB 1.68 ± 0.17 mm, HA+rhBMP ± 0.28 mm) and more resorptions over 4-month periods (widths ABB 29.7 ± 8.8%, HA+rhBMP ± 7.4%, p = and heights ABB 39.2 ± 21.8%, HA+rhBMP ± 6.5%, p = 0.548), it showed relatively more bone formation in histomorphometric assessments (ABB 28.9 ± 10.3%, HA+rhBMP ± 19.7%; p = 0.886). This suggests that HA+rhBMP-2 group may provide new bone formation through osteoinductive abilities provided by the osteogenic protein. This characteristic observation might be consistent with the in vivo and in vitro studies that the delivered rhbmp-2-activated dentin resorption that was associated with giant cells, ultimately promoting the bone formation and remodeling capacity in later stage [13, 25]. However, even though the average bone formation was higher in HA+rhBMP-2 group, the statistical difference was marginal because of the limited number of the cases. Therefore, the result needs to be confirmed by themorenumberofthecasesinthefuturestudy. Conclusions Bone graft material including rhbmp-2 showed good bone formation and remodeling capabilities. Within its limitation, this study suggested that ridge augmentations using rhbmp- 2 soaked HA could be clinically useful to supplement implant placements in edentulous regions. Additionally, serious postoperative complications related to the graft material did not occur. Additional file Additional file 1: Case form and result of data. (XLSX 37 kb) Acknowledgements Not applicable Funding There was no funding in support of this study. Availability of data and materials The dataset supporting the conclusions of this article is included within the article and Additional file 1. Authors contributions KHS participated in data collection and writing the manuscript. YPY participated in the study design and performed the statistical analysis. KYK participated in the study design and coordination and helped to draft the manuscript. PJC participated in histomophometric analysis of specimens. All authors read and approved the final manuscript. Authors information All of the authors have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in this manuscript. This manuscript represents original works and is not being considered for publication elsewhere. Ethics approval and consent to participate This study was approved by the Institutional Review Board of Seoul National University Bundang Hospital (E ). Fig. 4 Relative bone formation. HA+rhBMP-2 group showed more bone formation around the bone graft materials than the ABB group histologically, however, without statistical significance (p = 0.886) Consent for publication Consent for publication was obtained. Competing interests The authors declare that they have no competing interests.
6 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:40 Page 6 of 6 Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Oral and Maxillofacial Surgery, Section of Dentistry, Seoul National University Bundang Hospital, 300 Gumi-dong, Bundang-gu, Seongnam, Gyunggi-do, South Korea. 2 Department of Oral Histology, School of Dentistry, Seoul National University, Daehak-ro 101, Jongno-gu, Seoul 03080, South Korea. 3 Department of Dentistry and Dental Research Institute, School of Dentistry, Seoul National University, Daehak-ro 101, Jongno-gu, Seoul 03080, South Korea. Received: 7 August 2017 Accepted: 20 November 2017 References 1. Park SJ, Seon HG, Koh SW, Chee YD (2012) Retrospective clinical study on marginal bone loss of implants with guided bone regeneration. Maxillofac Plast Reconstr Surg 34(6): Kim YK, Lee J, Um IW, Kim KW, Murata M, Akazawa T, Mitsugi M (2013) Tooth-derived bone graft. J Korean Assoc Oral Maxillofac Surg 39(3): doi: /jkaoms Hwang ST, Han IH, Huh JB, Kang JK, Ryu JJ (2011) Review of the developmental trend of implant surface modification using organic biomaterials. J Adv Prosthodont 49(3): Um IW, Hwang SH, Kim YK, Kim MY, Jun SH, Ryu JJ, Jang HS (2016) Demineralized dentin matrix combined with recombinant human bone morphogenetic protein-2 in rabbit calvarial defects. J Korean Assoc Oral Maxillofac Surg 42(2): Cheng H, Jiang W, Phillips FM, Haydon RC, Peng Y, Zhou L, Szatkowski JP (2003) Osteogenic activity of the fourteen types of human bone morphogenetic proteins (BMPs). J Bone Joint Surg Am 85(8): Boyne PJ, Marx RE, Nevins M, Triplett G, Lazaro E, Lilly LC, Nummikoski P (1997) A feasibility study evaluating rhbmp-2/absorbable collagen sponge for maxillary sinus floor augmentation. Int J Periodontics Restorative Dent 17(1): Kim HJ, Chung JH, Shin SY, Shin SI, Kye SB, Kim NK, Kook MS (2015) Efficacy of rhbmp-2/hydroxyapatite on sinus floor augmentation: a multicenter, randomized controlled clinical trial. J Dent Res 94(suppl):158S 165S 8. Hanisch O, Tatakis DN, Boskovic MM, Rohrer MD, Wikesjö UM (1997) Bone formation and re-osseointegration in peri-implantitis defects following surgical implantation of rhbmp-2. Int J Oral Maxillofac Implants 12(5): Howell TH, Fiorellini J, Jones A, Alder M, Nummikoski P, Lazaro M, Cochran D (1997) A feasibility study evaluating rhbmp-2/absorbable collagen sponge device for local alveolar ridge preservation or augmentation. Int J Periodontics Restorative Dent 17(2): Sigurdsson TJ, Nygaard L, Tatakis DN, Fu E, Turek TJ, Jin L, Wikesjö UM (1996) Periodontal repair in dogs: evaluation of rhbmp-2 carriers. Int J Periodontics Restorative Dent 16(6): Ike M, Urist MR (1998) Recycled dentin root matrix for a carrier of recombinant human bone morphogenetic protein. J Oral Implantol 24(3): Jung RE, Glauser R, Schärer P, Hämmerle CH, Sailer HF, Weber FE (2003) Effect of rhbmp-2 on guided bone regeneration in humans. Clin Oral Implants Res 14(5): Kim YK, Um IW, An HJ, Kim KW, Hong KS, Murata M (2014) Effects of demineralized dentin matrix used as an rhbmp-2 carrier for bone regeneration. J Hard Tissue Biol 23(4): Asahina I (2014) Bone morphogenetic proteins: their history and characteristics. J Hard Tissue Biol 23(3): Bessho K, Tagawa T, Murata M (1989) Purification of bone morphogenetic protein derived from bovine bone matrix. Biochem Biophys Res Commun 165(2): Sato K, Urist MR (1985) Induced regeneration of calvaria by bone morphogenetic protein (BMP) in dogs. Clin Orthop Relat Res 197: Hwang DY, On SW, Song SI (2016) Bone regenerative effect of recombinant human bone morphogenetic protein-2 after cyst enucleation. Maxillofac Plast Reconstr Surg 38(1): Geiger M, Li RH, Friess W (2003) Collagen sponges for bone regeneration with rhbmp-2. Adv Drug Deliv Rev 55(12): Kim YK (2014) Bone graft using two types of scaffolds and recombinant human bone morphogenetic protein-2: case series study. Oral Biology Research 38(2): Burkus JK, Gornet MF, Glassman SD, Slosar PJ, Rosner MK, Deckey JE, Hatcher BM (2011) Blood serum antibody analysis and long-term follow-up of patients treated with recombinant human bone morphogenetic protein- 2 in the lumbar spine. Spine 36(25): Mines D, Gu Y, Kou TD, Cooper GS (2011) Recombinant human bone morphogenetic protein-2 and pancreatic cancer: a retrospective cohort study. Pharmacoepidemiol Drug Saf 20(2): Cooper GS, Kou TD (2013) Risk of cancer after lumbar fusion surgery with recombinant human bone morphogenic protein-2 (rh-bmp-2). Spine 38(21): Zara JN, Siu RK, Zhang X, Shen J, Ngo R, Lee M, Wu BM (2011) High doses of bone morphogenetic protein 2 induce structurally abnormal bone and inflammation in vivo. Tissue Eng Part A 17(9 10): Wong DA, Kumar A, Jatana S, Ghiselli G, Wong K (2008) Neurologic impairment from ectopic bone in the lumbar canal: a potential complication of off-label PLIF/TLIF use of bone morphogenetic protein-2 (BMP-2). Spine J 8(6): Murata M, Um IW (2014) Advances in oral tissue engineering. Quintessence, Illinois
Minimal invasive horizontal ridge augmentation using subperiosteal tunneling technique
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:41 DOI 10.1186/s40902-016-0087-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Minimal invasive horizontal
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:41 DOI 10.1186/s40902-016-0087-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Minimal invasive horizontal
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Long-term results of new deproteinized bovine bone material in a maxillary sinus graft procedure
 Long-term results of new deproteinized bovine bone material in a maxillary sinus graft procedure pissn 2093-2278 eissn 2093-2286 Seung-Yun Shin 1, You-Jeong Hwang 2, Jung-Hoon Kim 3,4, Yang-Jo Seol 3,
Long-term results of new deproteinized bovine bone material in a maxillary sinus graft procedure pissn 2093-2278 eissn 2093-2286 Seung-Yun Shin 1, You-Jeong Hwang 2, Jung-Hoon Kim 3,4, Yang-Jo Seol 3,
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
Applications of Moldable Autogenous Tooth Bone Graft (M-AutoBT) Mixed with Hydroxypropylmethyl Cellulose for Sinus Lifting
 Clinical Report Young-Kyun Kim et al.:moldable Autogenous Tooth Bone Graft for Sinus Lifting Journal of Hard Tissue Biology 24[4] (2015) 391-396 2015 The Hard Tissue Biology Network Association Printed
Clinical Report Young-Kyun Kim et al.:moldable Autogenous Tooth Bone Graft for Sinus Lifting Journal of Hard Tissue Biology 24[4] (2015) 391-396 2015 The Hard Tissue Biology Network Association Printed
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Socket preservation using deproteinized horsederived
 Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26
 P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
Familial tooth bone graft for ridge and sinus augmentation: a report of two cases
 CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.37 pissn 2234-7550 eissn 2234-5930 Familial tooth bone graft for ridge and sinus augmentation: a report of two cases Young-Kyun Kim 1, Su-Gwan Kim
CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.37 pissn 2234-7550 eissn 2234-5930 Familial tooth bone graft for ridge and sinus augmentation: a report of two cases Young-Kyun Kim 1, Su-Gwan Kim
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Effectiveness of guided bone regeneration and protein collagen sponge on socket preservation post tooth-extraction.
 Biomedical Research 2017; 28 (12): 5402-5407 ISSN 0970-938X www.biomedres.info Effectiveness of guided bone regeneration and protein collagen sponge on socket preservation post tooth-extraction. Tao Wang
Biomedical Research 2017; 28 (12): 5402-5407 ISSN 0970-938X www.biomedres.info Effectiveness of guided bone regeneration and protein collagen sponge on socket preservation post tooth-extraction. Tao Wang
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Reconstruction of large oroantral defects using a pedicled buccal fat pad
 Yang et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:7 https://doi.org/10.1186/s40902-018-0144-6 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Reconstruction
Yang et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:7 https://doi.org/10.1186/s40902-018-0144-6 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Reconstruction
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Sinus Augmentation Studies Methods and Definition
 FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
Space maintenance in autogenous fresh demineralized tooth blocks with platelet rich plasma for maxillary sinus bone formation: a prospective study
 DOI 10.1186/s40064-016-1886-1 RESEARCH Open Access Space maintenance in autogenous fresh demineralized tooth blocks with platelet rich plasma for maxillary sinus bone formation: a prospective study Eun
DOI 10.1186/s40064-016-1886-1 RESEARCH Open Access Space maintenance in autogenous fresh demineralized tooth blocks with platelet rich plasma for maxillary sinus bone formation: a prospective study Eun
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Pattern of bone resorption after extraction
 Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
Continuing Education 2
 Posterior Tooth Replacement with Dental Implants in Sites Augmented with rhbmp-2 at Time of Extraction A Case Series Barry P. Levin, DMD; and Peter Tawil, DDS Learning Objectives discuss the augmentation
Posterior Tooth Replacement with Dental Implants in Sites Augmented with rhbmp-2 at Time of Extraction A Case Series Barry P. Levin, DMD; and Peter Tawil, DDS Learning Objectives discuss the augmentation
Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report
 Case report J Korean Acad Periodontol 2009;39:287-291 Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report Ki-Tae Koo, Jang-Yeol Park, Jun-Seok Park, Tae-Il
Case report J Korean Acad Periodontol 2009;39:287-291 Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report Ki-Tae Koo, Jang-Yeol Park, Jun-Seok Park, Tae-Il
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Soft-Tissue Success with the. Clinical Success. Proven Matrix. with the Proven. Geistlich Mucograft Geistlich Mucograft Seal
 Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Alloplastic Grafts - Beta-tricalcium phosphate
 Alloplastic Grafts - Beta-tricalcium phosphate Presentation of clinical cases Mario Ernesto García-Briseño DDS and Professor in Periodontics - Autonomous University of Guadalajara (UAG), Mexico This case
Alloplastic Grafts - Beta-tricalcium phosphate Presentation of clinical cases Mario Ernesto García-Briseño DDS and Professor in Periodontics - Autonomous University of Guadalajara (UAG), Mexico This case
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
Versatile grafting Solutions
 Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
A New Technique for Minimally Invasive Maxillary Lateral Sinus Augmentation: a Case Report
 A New Technique for Minimally Invasive Maxillary Lateral Sinus Augmentation: a Case Report Xiu Lian HU 1, Xian ZHOU 1, Jian Hui LI 1, Ye LIN 1 Numerous techniques are described for lateral sinus augmentation,
A New Technique for Minimally Invasive Maxillary Lateral Sinus Augmentation: a Case Report Xiu Lian HU 1, Xian ZHOU 1, Jian Hui LI 1, Ye LIN 1 Numerous techniques are described for lateral sinus augmentation,
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
Bone graft material using teeth
 REVIEW ARTICLE http://dx.doi.org/10.5125/jkaoms.2012.38.3.134 pissn 2234-7550 eissn 2234-5930 Bone graft material using teeth Young-Kyun Kim Department of Oral and Maxillofacial Surgery, Section of Dentistry,
REVIEW ARTICLE http://dx.doi.org/10.5125/jkaoms.2012.38.3.134 pissn 2234-7550 eissn 2234-5930 Bone graft material using teeth Young-Kyun Kim Department of Oral and Maxillofacial Surgery, Section of Dentistry,
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
The body wants to heal
 58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
BioVin Collagen Membrane
 BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
We want to keep you smiling. Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Tooth out what's next?
 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Extraction socket preservation using β tricalcium phosphate bone graft plug and platelet rich fibrin membrane A case series
 2014; 1(1): 39-43 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2014; 1(1): 39-43 2014 IJADS www.oraljournal.com Received: 02-01-2015 Accepted: 07-02-2015 Shantipriya Reddy Prof and Head, department
2014; 1(1): 39-43 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2014; 1(1): 39-43 2014 IJADS www.oraljournal.com Received: 02-01-2015 Accepted: 07-02-2015 Shantipriya Reddy Prof and Head, department
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Strong bone for beautiful teeth. Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Complications of postoperative swelling of the maxillary sinus membrane after sinus floor augmentation
 Complications of postoperative swelling of the maxillary sinus membrane after sinus floor augmentation Abstract Objective The aim of this article was to investigate postoperative swelling of the maxillary
Complications of postoperative swelling of the maxillary sinus membrane after sinus floor augmentation Abstract Objective The aim of this article was to investigate postoperative swelling of the maxillary
ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report
 ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report Yaqian Chen, Qingqing Wu, Yi Man State Key Laboratory of Oral Diseases, West China
ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report Yaqian Chen, Qingqing Wu, Yi Man State Key Laboratory of Oral Diseases, West China
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Clinical Success. with the Proven. Clinical Success. with the Proven Bone Substitute Products
 Clinical Success with the Proven Bone Substitute Products Clinical Success with the Proven Bone Geistlich Bio-Oss Substitute Geistlich Bio-Oss Collagen Geistlich Bio-Oss Pen Documented More than 1,000
Clinical Success with the Proven Bone Substitute Products Clinical Success with the Proven Bone Geistlich Bio-Oss Substitute Geistlich Bio-Oss Collagen Geistlich Bio-Oss Pen Documented More than 1,000
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Clinical UM Guideline
 Clinical UM Guideline Subject: Bone Grafts for Dental and Oral Surgical Services Guideline #: 04-201 Current Effective Date: 03/24/2017 Status: Revised Last Review Date: 02/08/2017 Description This document
Clinical UM Guideline Subject: Bone Grafts for Dental and Oral Surgical Services Guideline #: 04-201 Current Effective Date: 03/24/2017 Status: Revised Last Review Date: 02/08/2017 Description This document
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
Extraction socket sealing using palatal gingival grafts and resorbable collagen membranes
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:39 DOI 10.1186/s40902-017-0137-x Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Extraction socket sealing using
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:39 DOI 10.1186/s40902-017-0137-x Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Extraction socket sealing using
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic. Review
 Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Chemicals in Surgical Periodontal Therapy
 Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
Assessment of the autogenous bone graft for sinus elevation
 ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2013.39.6.274 pissn 2234-7550 eissn 2234-5930 Assessment of the autogenous bone graft for sinus elevation Wang Peng, Il-Kyu Kim, Hyun-Young Cho, Sang-Pill
ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2013.39.6.274 pissn 2234-7550 eissn 2234-5930 Assessment of the autogenous bone graft for sinus elevation Wang Peng, Il-Kyu Kim, Hyun-Young Cho, Sang-Pill
Ridge Augmentation. Selection of Applicable Abstracts and Posters. Using Titanium-Reinforced PTFE Membranes
 Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
Socket Treatment. Procedure Guide
 Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Product Catalog. Dental Bone & Tissue Regeneration
 Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region
 CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
