Department of Dental Surgery, University of Calabar Teaching Hospital, Calabar, Nigeria
|
|
|
- Gavin Small
- 5 years ago
- Views:
Transcription
1 Original Article Use of Oral Mucoperiosteal and Pterygo Masseteric Muscle Flaps as Interposition Material in Surgery of Temporomandibular Joint Ankylosis: A Comparative Study Anyanechi CE, Osunde OD, Bassey GO Department of Dental Surgery, University of Calabar Teaching Hospital, Calabar, Nigeria Address for correspondence: Dr. Otasowie Daniel Osunde, Department of Dental Surgery, Maxillofacial Unit, University of Calabar Teaching Hospital, Calabar, Nigeria. E mail: otdany@yahoo.co.uk Abstract Background: The most common complication of surgery for the release of temporomandibular joint (TMJ) ankylosis is relapse of the ankylosis. To prevent re ankylosis, a variety of interpositional materials have been used. Aim: The aim was to compare the surgical outcome of oral mucoperiosteal flap, not hitherto used as interpositional material, with pterygo masseteric muscles flap after surgical release of TMJ ankylosis. Subjects and Methods: This was a prospective randomized study of all consecutive patients treated for the release of complete TMJ bony ankylosis, from January 2003 to December 2012, at the Oral and Maxillofacial unit of our institution. The patients were randomized into two groups: The pterygo masseteric group comprises 22 patients while the oral mucoperiosteal group had 23 patients. Information on demographics, clinical characteristics, and postoperative complications over a 5 year follow up period were obtained, and analyzed using the statistical package for social sciences (Statistical Package for the Social Sciences version 13, Chicago, IL, USA). A P < 0.05 was considered significant. Results: The age of the patients ranged from 15 to 28 mean 20.3 (3.35) years while the duration of ankylosis ranged from 2 to 16 mean 5.1 (3.4) years. The baseline demographic (gender; P = 0.92; side; P = 0.58) and clinical characteristics in terms of etiology (P = 0.60) and age (P = 0.52) were comparable in both treatment groups. All the patients presented with complete bony TMJ ankylosis with a preoperative inter incisal distance of <0.5 cm. The intraoperative mouth opening achieved ranged from 4 cm to 5 cm, mean 4.6 (0.27) cm and this was not different for either group (P = 0.51). The patients were followed up postoperatively for a period ranging from 3 to 5 years, mean 3.4 (0.62) years. The mouth opening decreased, over the period of postoperative review, from the initial range of 4 5 cm to cm, and this was not different in both groups (P = 0.18). Conclusion: This study suggests that oral mucoperiosteal flap could be an option in the choice of interpositional materials in surgery of TMJ ankylosis. Keywords: Ankylosis, Interpositional materials, Temporomandibular joint Introduction Ankylosis of the temporomandibular joint (TMJ) involves fusion of the mandibular condyle to the glenoid fossa in the Quick Response Code: Access this article online Website: DOI: ***** base of the skull, which causes distressing conditions such as impaired speech, difficulty in chewing, poor oral hygiene, facial disfigurement, compromise of the airway, and psychological stress. [1 4] Surgical treatment are aimed at improving esthetics, functional, and psychological well being of the affected individuals as well as preventing re ankylosis. [1 5] The most frequently reported complications after treatment of ankylosis are limited mouth opening, and re ankylosis which occurs within 6 months postoperatively. [5] This re ankylosis can be prevented by aggressive resectioning of the bony or fibrous tissues, especially in the medial aspect of the condyle, and by placement of interpositional materials. [6] 30 Annals of Medical and Health Sciences Research Jan-Feb 2015 Vol 5 Issue 1
2 Many materials have been used for insertion at the ostectomy gap after resection of a bony segment: Alloplastic materials [7] (acrylic, Proplast Teflon, Silastic), and autogenous tissues (temporalis muscle flaps, masseter medial pterygoid muscles slings, dermis, costochondral grafts, and cartilage). [8,9] The several suggested materials only show that there is yet no ideal interpositional materials devoid of undesirable effects. Alloplasts as interpositional material may predispose the recipient site to infections or foreign body reactions. [5] In addition, there may be extrusion which may necessitate secondary procedures to retrieve the material. Long term results of silicone sheet as an interpositional material revealed that 16.7% of the patients required second surgeries to remove the implants after an average interval of 5.6 years. [10] Other commonly used autogenous materials such as dermis, fascia lata and costochondra grafts, and cartilages are not vascularized in addition to the disadvantage of donor site morbidity. The temporalis muscle and fascia flap have been widely used for the reconstruction of the TMJ. In spite of its numerous advantages which include its autogenous nature, resilience, adequate blood supply, and proximity to the joint, it is not feasible in the intraoral TMJ arthroplasty. The pterygo masseteric muscle flap as an interpositional material was first described by Eschmarc in the second half of the 19 th century. [11] The advantages include anatomical proximity, vascularity and ease of suturing across the created joint. Although temporalis muscle and fascia flap is fast becoming the material of choice, pterygo masseteric flap still plays a role as an interpositional material, especially when ramus or angle ostectomy is carried out. Oral mucoperiosteal flaps may also serve as an interpositional material because its qualities are comparable to that of pterygo masseteric flap in terms of the vascularity, anatomical proximity, and the ease of suturing across the ostectomized segment. To the authors knowledge, the use of oral mucoperiosteum as interpositional material has not been previously described as revealed by a literature search. The aim of this study was to compare treatment outcome using oral mucoperiosteal flap and pterygo masseteric muscular flap as interpositional materials in surgery of TMJ ankylosis. Subjects and Methods This was a prospective randomized study of all consecutive patients treated for the release of complete TMJ bony ankylosis, from January 2003 to December 2012, at the Oral and Maxillofacial Unit, Department of Dental Surgery, of the University of Calabar Teaching Hospital. The criteria used for the diagnosis of complete bony TMJ ankylosis were: (1) Restricted mouth opening with maximal interdental distance of <0.5 cm; (2) absence of palpable movement at one or both condylar head, and (3) presence of bony consolidation in the region of the TMJ, on posterio anterior, lateral oblique mandible, and TMJ radiographic views (Transcranial). Although computed tomography Scan has become the gold standard in radiologic diagnosis of TMJ ankylosis, poverty among our patients precludes its routine use for diagnosis of TMJ ankylosis in our center. All selected patients underwent the interpositional gap arthroplasty with interpositional material varying between muscles and oral mucoperiosteum. The study protocol was approved by the Ethics Committee of our institution. A written consent was obtained from all the selected participants after adequate explanation of the study protocol. Randomization All consecutive patients who presented to the Oral and Maxillofacial unit of our institution with complete bony ankylosis (<0.5 cm) of the TMJ were consecutively randomized into two treatment groups as they present. In the first group, pterygo masseteric muscles flap was placed as interpositional material (control group) and in the second group oral mucoperiosteal flap was interposed in the ostectomized segments (experimental group). Surgical technique All procedures were carried out using intraoral approach by the same surgeon and assistant in the same operating theatre. To facilitate intubation, all patients required elective tracheostomy under local anesthesia because of lack of fiber optic laryngoscope in our institution. Under general anesthesia, the lateral surface of the angle ramus region of the mandible was accessed through a gingival marginal incision starting from the disto buccal angle of the 2 nd molar continues posterio laterally along the anterior border of the ramus and external oblique ridge and continues superiorly to the occlusal plane of the mandibular and maxillary teeth. A mucoperiosteal flap was then raised to expose the molar angle ramus region up to the sigmoid notch. With adequate soft tissue retraction and placement of protective flat metal instrument (periosteal elevator about 2.5 cm wide) beneath the mandible, osteotomies were carried out above the lingula in all the cases [Figure 1], using a mallet and an osteotome in combination with bone rongeur where necessary to create a gap of about cm. In all the cases, the initial bone cut was carried out in steps rather than through and through and then completed with a bone rongeur. This was necessary in order to prevent injury to any adjoining neurovascular bundle. Mouth opening was achieved by osteotomy/ostectomy in combination with coronoidectomy when the initial mouth opening achieved was <3 cm. This inter incisal distance was further improved using mouth crank, which also enhanced the surgical access. When adequate mouth opening has been achieved, the surgical site was thoroughly irrigated; interpositional materials were placed depending on the treatment group. In the experimental group, the mucoperiosteum related to the created gap was raised, rotated, and sutured medio laterally across the gap as an interpositional material [Figure 2a]. Pterygo masseteric muscle flap was sutured across the gaps as interpositional Annals of Medical and Health Sciences Research Jan-Feb 2015 Vol 5 Issue 1 31
3 Figure 1: Point of ostectomy. Note this level is above the lingula material in the control group [Figure 2b]. After adequate toileting and achievement of hemostasis, the reflected mucoperiosteal flaps in the control group, and the remainder in the experimental group were opposed using 3/0 black silk sutures. Using this protocol, an inter incisal distance of 4 5 cm was achieved intraoperatively in all the cases. Both groups were placed on the same antibiotics and analgesics except for the choice of interpositional material as described. Parenteral ampiclox 500 mg 6 h, metronidazole 500 mg 8 h and pentazocine 30 mg 6 h were given for the first 48 h, and continued with oral clindamycin 150 mg 12 h and oral naproxen sodium 550 mg 12 h for 10 days. After completion of the above regimen, patients were advised to continue with Paracetamol 1000 mg 8 h when necessary. Postoperative jaw exercises and follow up Jaw exercises began 48 h postoperatively and were vigorously carried out to the limit of patients tolerance. Our protocol involved use of stacks of wooden spatulas to open the mouth 6 8 times a day with each session lasting a minimum of 30 min. In between each active session patients were encouraged to continue the mouth opening exercises by chewing sugar free gums. Patients were reviewed daily for the first 7 10 days and then discharged to continue follow up on out patient basis. Post discharge follow ups continued biweekly for the 1 st month and then monthly up to the 1 st year. Thereafter patients were reviewed every 3 months for the first 2 years and then 6 monthly up to 5 years postsurgery. Patients who did not attain a minimum of 3 years postoperative follow up were excluded from the study. At each postoperative review section, the mouth opening was measured to determine the maximal interincisal distance. Using the criterion defined by Ansari et al., [12] re ankylosis was diagnosed when the mouth opening was <1.9 cm. Other evaluated parameters included occlusal anomaly which in this context, referred to malocclusion on both static, vertical, and on lateral excursion as well as deviation of the chin on opening or a Figure 2: (a) Oral mucoperiosteal flap raised, rotated, and sutured bucco lingually across the created bony gap, (b) Pterygomasseteric muscle flap as interposition material closing the mouth. The maximum inter incisal distance and the lateral excursion were assessed clinically with ruler that was calibrated in millimeter. The measurements were carried out by the same examiner three times during each postoperative visit and the average taken to eliminate intra observer error or discrepancies. Injury to the facial nerve, especially the buccal and the marginal mandibular branches were assessed by asking the patient to blow their cheek, purse the lip, and to smile. Inability to blow the cheek, purse the lip, or deviation of the lower lip indicated damage to these branches of the facial nerve. Loss or altered lower labial sensation indicated inferior alveolar nerve damage. In addition, serial plane radiographs were done at 1 month postsurgery; and then, at 6 monthly intervals up to 5 years postoperatively. Statistical analysis The data were analyzed using the statistical package for social sciences (Statistical Package for the Social Sciences version 13, Chicago, IL, USA). Categorical variables were presented as frequencies and percentages while continuous variables were presented as mean and standard deviations. Inferential statistics were done using Chi square and independent t tests as appropriate. A P < 0.05 was considered significant. Results A total of 48 patients with TMJ ankylosis was seen within the period of study. Three patients were excluded from the analysis because the duration of their postoperative follow up was <3 years. Of the 45 patients who met the inclusion criteria, 23 had oral mucoperiosteal flap as interpositional material while the remaining 22 were done with pterygo masseteric muscle flap. The age of the patients ranged from 15 to 28 mean 20.3 (3.35) years while the duration of ankylosis ranged from 2 to 16 mean 5.1 (3.4) years. The baseline demographic and clinical characteristics of both groups were comparable [Table 1]. Trauma (40/45 [88.9%]) and middle ear b 32 Annals of Medical and Health Sciences Research Jan-Feb 2015 Vol 5 Issue 1
4 Table 1: Demographic and clinical characteristics of study groups Variables Mucoperiosteum (n=23) Muscles (n=22) Gender Female Male Aetiology Trauma Infection 2 3 Side Left Right 7 10 Bilateral 4 3 Contralateral coronoidectomy Yes No Mean (SD) T Age (years) 20.6 (3.4) 19.9 (3.3) Follow-up (years) 3.5 (0.6) 3.2 (0.6) All data in frequency except where otherwise stated. SD: Standard deviation χ 2 P Figure 3: Mouth opening 3.4 cm, at 3 years postoperative review for a case treated for bilateral bony temporomandibular joint ankylosis infections (5/45 [11.1%]) were the observed etiologic factor for the development of TMJ ankylosis in this study. All the patients presented with complete bony TMJ ankylosis with a preoperative inter incisal distance of <0.5 cm. The immediate or intraoperative mouth opening achieved ranged from 4 to 5 mean 4.6 (0.27) cm and this was not different for either group (t = 0.66, df = 43, P = 0.51). There were no intra operative complications observed during the study. The patients were followed up postoperatively for a period ranging from 3 to 5 years, mean 3.4 (0.62) years. There was a decrease in the intraoperative mouth opening, over the period of postoperative review, from the initial range of 4 5 cm to cm [Figure 3]. This reduction in mouth opening was observed throughout the study period, and it occurred uniformly across both treatment groups. Presurgery lateral excursion was 0 cm for both groups. The occlusion, at 1 month postoperatively, was stable without the derangement in both groups [Figure 4]. At 3 years, the mean lateral excursions was not different for both treatment groups and these were estimated at 0.7 (0.15) cm bilaterally postsurgery in both unilateral and bilateral ankylosis. Furthermore, at 3 years postoperative review, the mouth opening were essentially the same in both the oral mucoperiosteum (3.0 cm) and the pterygo masseteric muscle groups (2.9 cm) [Figure 5]. However, there were anterior open bite and Angle class 2 division 1 malocclusion in bilateral ankylosis [Figure 6], while unilateral cases presented with premature occlusion on the ipsilateral side and a cross bite on the contralateral side. At 5 year postoperative radiographic evaluation of a left unilateral case, the ostectomized segment was still intact, and the margins have been corticalized [Figure 7]. There was no injury to either the facial or the inferior alveolar nerves. Due to Figure 4: Postoperative occlusion at 1 month review period for bilateral temporomandibular joint ankylosis Figure 5: Mouth opening at 3 years postoperative review. Note the similarity between the mucoperiosteal and muscle groups financial constraints nothing was done to correct the occlusal anomalies and facial deformity. Annals of Medical and Health Sciences Research Jan-Feb 2015 Vol 5 Issue 1 33
5 Figure 6: Postoperative occlusal and skeletal changes for the patient in Figure 4, at 3 years review period. Note the anterior open bite and class 2 malocclusion Discussion The most common complication of surgery for the release of TMJ ankylosis is relapse of the ankylosis. To prevent re ankylosis, a variety of interpositional materials have been used which include temporalis muscle and fascia, the dermis, auricular cartilage, fascia lata, fat, lyo dura, silastic, silicone, and various metals. [13 17] While majority of the autogenous materials are associated with donor site morbidity, the alloplastic materials have been linked with infections at the recipient site, foreign body reactions and extrusions. [5] In the present study, we proposed the use of oral mucoperiosteal flap as an interpositional material and compared the results with pterygo masseteric muscle flap which is one of the earliest documented material used in interpositional gap arthroplasty. The results of the mouth opening achieved and occlusal derangement when the treatment techniques were compared at the end of the postoperative review period were similar. The reduction in mouth opening occurred uniformly across both study population over time. This reduction in mouth opening may be explained in terms of healing contractures as documented in several studies. [6,11,18] Apart from healing contractures reduction in mouth opening may also be due to fibrous or bony re ankylosis. [5,6] The dimension of the initial passive mouth opening achieved at surgery without application of undue force, aggressive resection of the ankylotic mass as well as consistent postoperative mouth opening exercises have been reported as the main determinant factors for the prevention of re ankylosis. [6,9,18] In this series, no case of re ankylosis was recorded over the period of follow up, both clinically and radiographically, probably due to the initial mouth opening achieved at surgery, estimated at 4 5 cm as well as the presence of interpositional material at the created bony gaps. Absence of re ankylosis may also have been due to the high level of patients compliance with the postoperative jaw exercises which led to corticalization of the ostectomized Figure 7: Postoperative radiograph at 5 year review period, for a patient treated for left unilateral temporomandibular joint ankylosis. Note the corticalization of the ostectomized segment segments. [19] The other reason may not be unconnected with the ages of the subjects, with the youngest being 15 years. Older patients may obviously tolerate the postoperative mouth opening exercises more than children due to differences in the level of pain threshold. The malocclusion recorded in the two treatment groups and in unilateral, and bilateral ankylosis are consistent with previous reports. [5,20] As previously reported, this malocclusion including the reduced lateral mandibular excursion is due to healing contractures, reankylosis, retrusion of the mandible following ostectomy and it is synonymous with techniques that results in shortening of ramus of the mandible. [2,3,5] However the anterior open bite or ipsilateral premature contact with contralateral cross bite as it occurs in bilateral and unilateral TMJ ankylosis respectively, is less with techniques that restores the anatomical height of the ramus using either autogenous or alloplastic material. [5,12,18] Unfortunately, due to financial constraints on the part of these patients, the abnormalities including facial disfigurement were not corrected during the follow up period. The subjects have decided to come to terms with their deformities. Oral mucoperiosteal flaps like other previously reported flaps used in interpositional arthroplasty have the advantages of being vascularized, ease of suturing across the created false joint, and in addition its anatomical proximity to the surgical site. There may not be additional morbidity to the donor site since the interposed segment is part of the mucoperiosteal flap raised to expose the mandibular body angle ramus regions. Our choice of intraoral approach in the treatment of TMJ ankylosis in this study confers additional advantages compared to the conventional extraoral surgical approach. Ko et al. [21] previously reported on the release of TMJ ankylosis through intraoral approach and the results were excellent with no re ankylosis. Intraoral endoscopic approach to the TMJ has also been described by Sembronio et al. [8] In this 34 Annals of Medical and Health Sciences Research Jan-Feb 2015 Vol 5 Issue 1
6 technique, the ankylotic bone excision was performed through the pre auricular access and the resection was completed intraorally, with endoscopic assistance, using a piezoelectric osteotome. Our technique differed slightly in that the site of the ostectomy in the present study was lower without excision of the ankylotic mass. The advantages of intraoral arthroplasty are absence of facial scar, reduced risk of injury to the facial and the auriculotemporal nerves, absence of sialocoele, reduced hemorrhage as well as the possibility of carrying out coronoidectomy or coronoidotomy through the same surgical access. [9,22] The reduced hemorrhage may partly be due to reflection of soft tissues away from the medial surface of the ramus above the lingula and thus protecting the maxillary artery from the surgical field. [21] Additional blood loss may arise from transection of subcutaneous and other vessels related to the extraoral lines of incision. The main draw back of intraoral arthroplasty is the limited field of surgery and the high level of dexterity required by both the operator and assistant. [22] Conclusion This study has demonstrated the use of oral muccoperiosteal flap as an interpositional material. Because of the relatively small sample size of our study population, we suggest further studies with lager sample sizes and over a longer follow up period to validate the findings of the present study. References 1. Posnick JC, Goldstein JA. Surgical management of temporomandibular joint ankylosis in the pediatric population. Plast Reconstr Surg 1993;91: López EN, Dogliotti PL. Treatment of temporomandibular joint ankylosis in children: Is it necessary to perform mandibular distraction simultaneously? J Craniofac Surg 2004;15: Chidzonga MM. Temporomandibular joint ankylosis: Review of thirty two cases. Br J Oral Maxillofac Surg 1999;37: Qudah MA, Qudeimat MA, Al Maaita J. Treatment of TMJ ankylosis in Jordanian children A comparison of two surgical techniques. J Craniomaxillofac Surg 2005;33: Kaban LB, Perrott DH, Fisher K. A protocol for management of temporomandibular joint ankylosis. J Oral Maxillofac Surg 1990;48: Su Gwan K. Treatment of temporomandibular joint ankylosis with temporalis muscle and fascia flap. Int J Oral Maxillofac Surg 2001;30: Bello SA, Aluko Olokun B, Olaitan AA, Ajike SO. Aetiology and presentation of ankylosis of the temporomandibular joint: Report of 23 cases from Abuja, Nigeria. Br J Oral Maxillofac Surg 2012;50: Sembronio S, Albiero AM, Polini F, Robiony M, Politi M. Intraoral endoscopically assisted treatment of temporomandibular joint ankylosis: Preliminary report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007;104:e Kaban LB, Bouchard C, Troulis MJ. A protocol for management of temporomandibular joint ankylosis in children. J Oral Maxillofac Surg 2009;67: Schliephake H, Schmelzeisen R, Maschek H, Haese M. Long term results of the use of silicone sheets after diskectomy in the temporomandibular joint: Clinical, radiographic and histopathologic findings. Int J Oral Maxillofac Surg 1999;28: Huang IY, Lai ST, Shen YH, Worthington P. Interpositional arthroplasty using autogenous costal cartilage graft for temporomandibular joint ankylosis in adults. Int J Oral Maxillofac Surg 2007;36: Ansari SR, Iqbal S, Aslam S. Surgical correction of TMJ ankylosis A study on the incidence and evaluation of success rates of various surgical procedures. Pak Oral Dent J 2003;23: Chossegros C, Guyot L, Cheynet F, Blanc JL, Gola R, Bourezak Z, et al. Comparison of different materials for interposition arthroplasty in treatment of temporomandibular joint ankylosis surgery: Long term follow up in 25 cases. Br J Oral Maxillofac Surg 1997;35: Chossegros C, Guyot L, Cheynet F, Blanc JL, Cannoni P. Full thickness skin graft interposition after temporomandibular joint ankylosis surgery. A study of 31 cases. Int J Oral Maxillofac Surg 1999;28: Karaca C, Barutcu A, Menderes A. Inverted, T shaped silicone implant for the treatment of temporomandibular joint ankylosis. J Craniofac Surg 1998;9: Matukas VJ, Lachner J. The use of autologous auricular cartilage for temporomandibular joint disc replacement: A preliminary report. J Oral Maxillofac Surg 1990;48: Paterson AW, Shepherd JP. Fascia lata interpositional arthroplasty in the treatment of temporomandibular joint ankylosis caused by psoriatic arthritis. Int J Oral Maxillofac Surg 1992;21: Sadakah AA, Elgazzar RF, Abdelhady AI. Intraoral distraction osteogenesis for the correction of facial deformities following temporomandibular joint ankylosis: A modified technique. Int J Oral Maxillofac Surg 2006;35: Adekeye EO. Ankylosis of the mandible: Analysis of 76 cases. J Oral Maxillofac Surg 1983;41: Matsuura H, Miyamoto H, Ogi N, Kurita K, Goss AN. The effect of gap arthroplasty on temporomandibular joint ankylosis: An experimental study. Int J Oral Maxillofac Surg 2001;30: Ko EC, Chen MY, Hsu M, Huang E, Lai S. Intraoral approach for arthroplasty for correction of TMJ ankylosis. Int J Oral Maxillofac Surg 2009;38: Khadka A, Hu J. Autogenous grafts for condylar reconstruction in treatment of TMJ ankylosis: Current concepts and considerations for the future. Int J Oral Maxillofac Surg 2012;41: How to cite this article:???? Source of Support: Study was self funded. Conflict of Interest: None declared. Annals of Medical and Health Sciences Research Jan-Feb 2015 Vol 5 Issue 1 35
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty
 Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Simultaneous gap arthroplasty and intraoral distraction and secondary contouring surgery for unilateral temporomandibular joint ankylosis
 Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
Modified T-Plate Interpositional Arthroplasty for Temporomandibular Joint Ankylosis: A New and Versatile Option
 Original rticle Modified T-Plate Interpositional rthroplasty for Temporomandibular Joint nkylosis: New and Versatile Option Imran hmad, Mohd ltaf Mir, Lalit Mohan ariar Department of Plastic and Reconstructive
Original rticle Modified T-Plate Interpositional rthroplasty for Temporomandibular Joint nkylosis: New and Versatile Option Imran hmad, Mohd ltaf Mir, Lalit Mohan ariar Department of Plastic and Reconstructive
Scholars Journal of Medical Case Reports
 DOI: 10.21276/sjmcr.2016.4.11.17 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2016; 4(11):863-868 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher
DOI: 10.21276/sjmcr.2016.4.11.17 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2016; 4(11):863-868 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher
Original Article OUTCOME OF TEMPOROMANDIBULAR JOINT ARTHROPLASTY WITH TEMPORALIS FSCIA INTERPOSITION
 Original Article OUTCOME OF TEMPOROMANDIBULAR JOINT ARTHROPLASTY WITH TEMPORALIS FSCIA INTERPOSITION Sajjad Ahmed *, Riaz Ahmed Warriach **, Muhaad Arshad Badar ***, Arslan wahid ****, Hanan Shafique *****
Original Article OUTCOME OF TEMPOROMANDIBULAR JOINT ARTHROPLASTY WITH TEMPORALIS FSCIA INTERPOSITION Sajjad Ahmed *, Riaz Ahmed Warriach **, Muhaad Arshad Badar ***, Arslan wahid ****, Hanan Shafique *****
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS. FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy
 MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
Reconstruction of temporomandibular joint ankylosis with temporalis myofascial flap in a cat: a case report
 Reconstruction of temporomandibular joint ankylosis with temporalis myofascial flap in a cat: a case report S.Y. Heo, H.B. Lee K.C Lee, N.S. Kim College of Veterinary Medicine, Chonbuk National University,
Reconstruction of temporomandibular joint ankylosis with temporalis myofascial flap in a cat: a case report S.Y. Heo, H.B. Lee K.C Lee, N.S. Kim College of Veterinary Medicine, Chonbuk National University,
Intraoral mandibular distraction osteogenesis in facial asymmetry patients with unilateral temporomandibular joint bony ankylosis
 Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Journal of Cranio-Maxillo-Facial Surgery
 Journal of Cranio-Maxillo-Facial Surgery 45 (2017) 441e448 Contents lists available at ScienceDirect Journal of Cranio-Maxillo-Facial Surgery journal homepage: www.jcmfs.com Surgical management of ankyloses
Journal of Cranio-Maxillo-Facial Surgery 45 (2017) 441e448 Contents lists available at ScienceDirect Journal of Cranio-Maxillo-Facial Surgery journal homepage: www.jcmfs.com Surgical management of ankyloses
Temporomandibular Joint. Dr Noman ullah wazir
 Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study
 Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
Regeneration, Reconstruction & Restoration Reconstruction Functional Outcomes of Temporomandibular Joint Ankylosis Treatments: A 10-year cohort study Mohammad Taghi Kiani a*, Mohammad Bayat b, Maryam Ajami
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
3. The Jaw and Related Structures
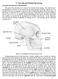 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
King's College Hospital Dental School, London, S.E. 5.
 OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Review Article Role of coronoid process in reconstruction of temporomandibular joint Gopalakrishnan V 1, Sahoo NK 2
 Review Article Role of coronoid process in reconstruction of temporomandibular joint Gopalakrishnan V 1, Sahoo NK 2 1 Maj V Gopalakrishnan BDS, MDS Graded specialist, No 1 Airforce dental centre, Palam,
Review Article Role of coronoid process in reconstruction of temporomandibular joint Gopalakrishnan V 1, Sahoo NK 2 1 Maj V Gopalakrishnan BDS, MDS Graded specialist, No 1 Airforce dental centre, Palam,
Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy
 1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Temporomandibular Joint Ankylosis:Evaluation of surgical outcomes
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 8 Ver. I (Aug. 2014), PP 60-66 Temporomandibular Joint Ankylosis:Evaluation of surgical outcomes
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 8 Ver. I (Aug. 2014), PP 60-66 Temporomandibular Joint Ankylosis:Evaluation of surgical outcomes
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Radiographic assessment of lower third molar prior to surgery: A report of four cases
 Radiographic assessment of lower third molar prior to surgery: A report of four cases V Sreenivas Prasad Department of Oral and Maxillofacial Surgery, College of Dentistry, Gulf Medical University, Ajman,
Radiographic assessment of lower third molar prior to surgery: A report of four cases V Sreenivas Prasad Department of Oral and Maxillofacial Surgery, College of Dentistry, Gulf Medical University, Ajman,
Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note
 Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Navigation-Guided Lateral Gap Arthroplasty as the Treatment of Temporomandibular Joint Ankylosis
 CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY Navigation-Guided Lateral Gap Arthroplasty as the Treatment of Temporomandibular Joint Ankylosis Haijun Gui, MD, DDS,* Jinyang Wu, DDS,y Steve G. F. Shen,
CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY Navigation-Guided Lateral Gap Arthroplasty as the Treatment of Temporomandibular Joint Ankylosis Haijun Gui, MD, DDS,* Jinyang Wu, DDS,y Steve G. F. Shen,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting
 44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
Correction of Dentofacial Deformities (Orthognathic Surgery)
 Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
TMJ ANKYLOSIS: A MULTI PROBLEMATIC DISORDER OF TEMPOROMANDIBULAR JOINT
 wjpmr, 2017,3(1), 324-330. SJIF Impact Factor: 3.535 Review Article WORLD JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH ISSN 2455-3301 www.wjpmr.com WJPMR TMJ ANKYLOSIS: A MULTI PROBLEMATIC DISORDER OF
wjpmr, 2017,3(1), 324-330. SJIF Impact Factor: 3.535 Review Article WORLD JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH ISSN 2455-3301 www.wjpmr.com WJPMR TMJ ANKYLOSIS: A MULTI PROBLEMATIC DISORDER OF
The Melbourne Temporomandibular Total Joint Replacement System
 The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
Article Management of temporomandibular joint ankylosis in Yemeni children by metatarsal bone grafts.
 Article Management of temporomandibular joint ankylosis in Yemeni children by metatarsal bone grafts. Ali Al-Hudaid, 1 Abdullwahab Aldialami, 1 Jameel Helmi, 1 Mohammed Al-Wesabi 1 & Ahmed Madfa. 2,3 Affiliations:
Article Management of temporomandibular joint ankylosis in Yemeni children by metatarsal bone grafts. Ali Al-Hudaid, 1 Abdullwahab Aldialami, 1 Jameel Helmi, 1 Mohammed Al-Wesabi 1 & Ahmed Madfa. 2,3 Affiliations:
LOGIC SURGICAL TECHNIQUE GUIDE. In d i c at i o n s. Co n t r a i n d i c at i o n s. Mandibular Distraction System
 TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Interesting Case Series. Virtual Surgical Planning in Orthognathic Surgery
 Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
TMJ Joint Replacement System
 TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
Oral & Maxillofacial Surgery
 Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: orthodontics_for_pediatric_patients 2/2014 10/2017 10/2018 10/2017 Description of Procedure or Service Children
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: orthodontics_for_pediatric_patients 2/2014 10/2017 10/2018 10/2017 Description of Procedure or Service Children
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Original Article. Indications and Outcome of Mandibular Condylar and Ramus Surgeries. Patients and Methods. Introduction
 Original Article Indications and Outcome of Mandibular Condylar and Ramus Surgeries Babatunde O Akinbami, Oladimeji A Akadiri Department of Oral and Maxillofacial Surgery, University of Port Harcourt Teaching
Original Article Indications and Outcome of Mandibular Condylar and Ramus Surgeries Babatunde O Akinbami, Oladimeji A Akadiri Department of Oral and Maxillofacial Surgery, University of Port Harcourt Teaching
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
A New Method of Treatment of Temporomandibular Joint Ankylosis with Osteodistraction Using the Sh-Device: A Case Report
 Case Report A New Method of Treatment of Temporomandibular Joint Ankylosis with Osteodistraction Using the Sh-Device: A Case Report Gholamreza Shirani 1, Mahnaz Arshad 2, Xaniar Mahmoudi 3 1 Assistant
Case Report A New Method of Treatment of Temporomandibular Joint Ankylosis with Osteodistraction Using the Sh-Device: A Case Report Gholamreza Shirani 1, Mahnaz Arshad 2, Xaniar Mahmoudi 3 1 Assistant
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Fibrous Ankylosis of the Temporomandibular Joint in a Young Child ABSTRACT
 JDC CASE REPORT Fibrous Ankylosis of the Temporomandibular Joint in a Young Child Nigel R. Figueiredo, BDS, MDS 1 Manoj Meena, BDS, MDS 2 Ajit D. Dinkar, BDS, MDS 3 Manisha M. Khorate, BDS, MDS 4 ABSTRACT
JDC CASE REPORT Fibrous Ankylosis of the Temporomandibular Joint in a Young Child Nigel R. Figueiredo, BDS, MDS 1 Manoj Meena, BDS, MDS 2 Ajit D. Dinkar, BDS, MDS 3 Manisha M. Khorate, BDS, MDS 4 ABSTRACT
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
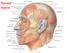 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Temporomandibular Joint
 6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
J. 0. AKINOSI, B.D.s., F.D.S.R.C.S.
 British Journal of Oral Surgery 15 (1977-78) 83-87 A NEW APPROACH TO THE MANDIBULAR NERVE BLOCK J. 0. AKINOSI, B.D.s., F.D.S.R.C.S. Department of Oral Surgery and Pathology, College of Medicine, Lagos
British Journal of Oral Surgery 15 (1977-78) 83-87 A NEW APPROACH TO THE MANDIBULAR NERVE BLOCK J. 0. AKINOSI, B.D.s., F.D.S.R.C.S. Department of Oral Surgery and Pathology, College of Medicine, Lagos
DR.SHERIN.A.KHALAM,MSc(PSY),MDS,FICOI Associate Professor, PMS College of Dental Science & Research, Kerala University of Health Sciences; Consultant
 DR.SHERIN.A.KHALAM,MSc(PSY),MDS,FICOI Associate Professor, PMS College of Dental Science & Research, Kerala University of Health Sciences; Consultant Maxillofacial Surgeon & Surgical Head, SUT Royal Hospitals,
DR.SHERIN.A.KHALAM,MSc(PSY),MDS,FICOI Associate Professor, PMS College of Dental Science & Research, Kerala University of Health Sciences; Consultant Maxillofacial Surgeon & Surgical Head, SUT Royal Hospitals,
Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor
 Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Postnatal Growth. The study of growth in growing children is for two reasons : -For health and nutrition assessment
 Growth of The Soft Tissues Postnatal Growth Postnatal growth is defined as the first 20 years of growth after birth krogman 1972 The study of growth in growing children is for two reasons : -For health
Growth of The Soft Tissues Postnatal Growth Postnatal growth is defined as the first 20 years of growth after birth krogman 1972 The study of growth in growing children is for two reasons : -For health
Mesial Step Class I or Class III Dependent upon extent of step seen clinically and patient s growth pattern Refer for early evaluation (by 8 years)
 Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2017
 NC Dental Reimbursement s Refer to the NC and Health Choice Clinical Coverage Policies on the DMA website. D0120 Periodic oral evaluation 24.51 D0140 Limited oral evaluation - problem focused 34.94 D0145
NC Dental Reimbursement s Refer to the NC and Health Choice Clinical Coverage Policies on the DMA website. D0120 Periodic oral evaluation 24.51 D0140 Limited oral evaluation - problem focused 34.94 D0145
Anatomy and physiology of Temporomandibular Joint
 Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Postoperative malocclusion after maxillofacial fracture management: a retrospective case study
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:27 https://doi.org/10.1186/s40902-018-0167-z Maxillofacial Plastic and Reconstructive Surgery REVIEW Open Access Postoperative malocclusion
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:27 https://doi.org/10.1186/s40902-018-0167-z Maxillofacial Plastic and Reconstructive Surgery REVIEW Open Access Postoperative malocclusion
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
SURGICAL DENTAL PROCEDURES. FOR GENERAL DENTISTS Services listed with no corresponding fees will require prior
 FOR GENERAL DENTISTS Services listed with no corresponding fees will require prior EXTRACTION OF ERUPTED TEETH (See Appendix A) 84040 Removal of erupted tooth, uncomplicated procedure 43.55 46.68 84042
FOR GENERAL DENTISTS Services listed with no corresponding fees will require prior EXTRACTION OF ERUPTED TEETH (See Appendix A) 84040 Removal of erupted tooth, uncomplicated procedure 43.55 46.68 84042
Author(s) Fujimura, Kazuma; Bessho, Kazuhisa.
 Title Rigid fixation of intraoral mandibular prognathism. vertico Author(s) Fujimura, Kazuma; Bessho, Kazuhisa Citation Journal of oral and maxillofacial s 1173 Issue Date 2012-05 URL http://hdl.handle.net/2433/155855
Title Rigid fixation of intraoral mandibular prognathism. vertico Author(s) Fujimura, Kazuma; Bessho, Kazuhisa Citation Journal of oral and maxillofacial s 1173 Issue Date 2012-05 URL http://hdl.handle.net/2433/155855
SURGICAL'MANAGEMENT'OF' PLEXIFORM'AMELOBLASTOMA:'A' CASE'REPORT'
 HARSH,Ashutosh* PUROHIT,Pragya* PUROHIT,NC** ADLAKHA,Twisha*** SURGICALMANAGEMENTOF PLEXIFORMAMELOBLASTOMA:A CASEREPORT ABSTRACT Ameloblastoma is a benign but locally invasive neoplasm of odontogenicepithelium.patientsusuallypresentlateafterthetumor
HARSH,Ashutosh* PUROHIT,Pragya* PUROHIT,NC** ADLAKHA,Twisha*** SURGICALMANAGEMENTOF PLEXIFORMAMELOBLASTOMA:A CASEREPORT ABSTRACT Ameloblastoma is a benign but locally invasive neoplasm of odontogenicepithelium.patientsusuallypresentlateafterthetumor
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL
 What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
TMJ Parametro Classico
 TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
EVALUATION OF THE PLEURAL DISRUPTION FOLLOWING COSTOCHONDRAL GRAFT HARVESTING FROM FOURTH TO SEVENTH RIBS OF ADULT MALE CADAVERS
 EVALUATION OF THE PLEURAL DISRUPTION FOLLOWING COSTOCHONDRAL GRAFT HARVESTING FROM FOURTH TO SEVENTH RIBS OF ADULT MALE CADAVERS M. E. Daneshvar *1 A. Ghafoori 2 and P. Namiranian 1 1) Department of Oral
EVALUATION OF THE PLEURAL DISRUPTION FOLLOWING COSTOCHONDRAL GRAFT HARVESTING FROM FOURTH TO SEVENTH RIBS OF ADULT MALE CADAVERS M. E. Daneshvar *1 A. Ghafoori 2 and P. Namiranian 1 1) Department of Oral
Osteochondroma of the mandibular condyle cured by conservative resection
 Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
Lec [8]: Mandibular nerve:
![Lec [8]: Mandibular nerve: Lec [8]: Mandibular nerve:](/thumbs/94/121295776.jpg) Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
Figure (2-6): Labial frenum and labial notch.
 The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient with facial asymmetry
 CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
CASE REPORT http://dx.doi.org/10.5125/jkaoms.2014.40.1.32 pissn 2234-7550 eissn 2234-5930 Unilateral intraoral vertical ramus osteotomy based on preoperative three-dimensional simulation surgery in a patient
International J. of Healthcare and Biomedical Research, Volume: 03, Issue: 01, October 2014, Pages
 Original article: Distraction osteogenesis following gap arthroplasty to correct facial asymmetry - a defined protocol in treatment of patients with temporomandibular joint ankylosis. 1Dr. Babu S. Parmar,
Original article: Distraction osteogenesis following gap arthroplasty to correct facial asymmetry - a defined protocol in treatment of patients with temporomandibular joint ankylosis. 1Dr. Babu S. Parmar,
For many years, patients with
 Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Dr. Robert Lowe is one of the great teachers in dentistry. Recently, he received the Gordon J. Christensen Award from the Chicago Dental Society in recognition of his excellence in teaching. Some of my
Horizontal jaw relations: The relationship of mandible to maxilla in a
 Horizontal relations Horizontal jaw relations: The relationship of mandible to maxilla in a horizontal plane (in anteroposterior and side to side direction). a- Protruded or forward relation. b-lateral
Horizontal relations Horizontal jaw relations: The relationship of mandible to maxilla in a horizontal plane (in anteroposterior and side to side direction). a- Protruded or forward relation. b-lateral
2018 Dental Code Set For dates of service from 1/1/ /31/2018
 D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
2018 Dental Code Set
 D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
DISTRACTION PRODUCT OVERVIEW. For a wide variety of facial applications
 DISTRACTION PRODUCT OVERVIEW For a wide variety of facial applications DISTRACTION PRODUCT OVERVIEW. STRONG, MODULAR, VERSATILE CRANIOFACIAL DISTRACTION External Midface Distractor Distraction of the maxilla,
DISTRACTION PRODUCT OVERVIEW For a wide variety of facial applications DISTRACTION PRODUCT OVERVIEW. STRONG, MODULAR, VERSATILE CRANIOFACIAL DISTRACTION External Midface Distractor Distraction of the maxilla,
IMPACTED CANINES. Unfortunately, this important tooth is the second most common tooth to be impacted after third molars
 IMPACTED CANINES After we talked about impacted third molars, today we ll discuss about maxillary impacted canines in upper dental arch, how to manage these cases as a dental surgeon. You will study about
IMPACTED CANINES After we talked about impacted third molars, today we ll discuss about maxillary impacted canines in upper dental arch, how to manage these cases as a dental surgeon. You will study about
Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital,
 Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
Dr. Ellen Wen-Ching Ko, DDS, MS Professor, Department of Craniofacial Orthodontics, Chang Gung Memorial Hospital, Taipei, Taiwan Professor, Graduate Institute of Craniofacial and Dental Science, Chang
REFERENCES for PLATELET RICH PLASMA (PRP)
 REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
Complex Occlusal Rehabilitation: A Case Report
 Complex Occlusal Rehabilitation: A Case Report DR. ALI TUNKIWALA INTRODUCTION The most difficult problems in clinical practice are those where there is interaction of various pathogenic factors with consequent
Complex Occlusal Rehabilitation: A Case Report DR. ALI TUNKIWALA INTRODUCTION The most difficult problems in clinical practice are those where there is interaction of various pathogenic factors with consequent
06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]
![06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.] 06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]](/thumbs/84/91182117.jpg) Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
SURGICAL DENTAL PROCEDURES. FOR GENERAL DENTISTS Services listed with no corresponding fees will require prior approval
 Code Dentist Oral Surg. 84000 New Patient Exam 62.56 75.05 Exam (Subsequent) 39.37 49.48 FOR GENERAL DENTISTS Services listed with no corresponding fees will require prior approval EXTRACTION OF ERUPTED
Code Dentist Oral Surg. 84000 New Patient Exam 62.56 75.05 Exam (Subsequent) 39.37 49.48 FOR GENERAL DENTISTS Services listed with no corresponding fees will require prior approval EXTRACTION OF ERUPTED
Monday Morning Pearls of Practice by Bobby Baig
 Dec 19, 2016 Monday Morning Pearls of Practice by Bobby Baig baig@buildyoursmile.com Prosthodontic Associates 2300 Yonge St, suite 905 Toronto, M4P1E4 www.buildyoursmile.com CBCT and Implant Dentistry:
Dec 19, 2016 Monday Morning Pearls of Practice by Bobby Baig baig@buildyoursmile.com Prosthodontic Associates 2300 Yonge St, suite 905 Toronto, M4P1E4 www.buildyoursmile.com CBCT and Implant Dentistry:
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
PRE-OP and POST-OP SURGICAL CONSIDERATIONS
 PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2014
 NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2014 The inclusion of a rate on this table does not guarantee
NC Medicaid Dental Reimbursement Rates General Dentist, Oral Surgeon, Pediatric Dentist, Periodontist, & Orthodontist Effective Date: January 1, 2014 The inclusion of a rate on this table does not guarantee
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
