(12) United States Patent
|
|
|
- Stephanie Byrd
- 5 years ago
- Views:
Transcription
1 (12) United States Patent USOO B2 (10) Patent No.: US 8,623,055 B2 Abdou (45) Date of Patent: Jan. 7, 2014 (54) SPINOUS PROCESS FUSION AND (56) References Cited ORTHOPEDICMPLANTS AND METHODS U.S. PATENT DOCUMENTS (71) Applicant: Samy Abdou, San Diego, CA (US) A 1 1/1985 Kapp et al. 6, B1 1 1/2001 Asfora (72) Inventor: Samy Abdou, San Diego, CA (US) 7,048,736 B2 5, 2006 Robinson et al. 7,727,233 B2 6, 2010 Blackwell et al. (*) Notice: Subject to any disclaimer, the term of this 7,846,186 B2 * 12/2010 Taylor ,249 patent is extended or adjusted under 35 SES E: $38: EM, al. aoe U.S.C. 154(b) by 0 days. 2003/ A1 2/2003 Mitchell et al. 2007/ A1* 11/2007 Peckham /61 (21) Appl. No.: 13/669, , O A1* 6, 2009 St. Clair et al ,279 (22) Filed: Nov. 5, 2012 * cited by examiner (65) Prior Publication Data US 2013/OO6O284A1 Mar. 7, 2013 Primary Examiner Eduardo C Robert ar. f. Assistant Examiner Steven Cotroneo Related U.S. Application Data (74) Attorney, Agent, or Firm GaZdzinski & Associates, PC (63) Continuation of application No. 12/727,641, filed on Mar. 19, 2010, now Pat. No. 8,303,629. (60) Provisional application No. 61/210,581, filed on Mar. (57) ABSTRACT 19, A spinal implant device immobilizes an attached vertebrae through 9. a minimallv y invasive surgical 9. approachwhile p provid (51) Int. Cl. ing a compartment within the implant for the placement of A6B 7/70 ( ) bone 9. graft or bone 9. graft substitute. The bone 9. graft material (52) U.S. Cl. fuses the spinous processes and/or lamina portion of bone of USPC /248 (58) Field of Classification Search USPC / ; 623/ See application file for complete search history. the vertebral bone to which the device is attached. 25 Claims, 21 Drawing Sheets
2 U.S. Patent Jan. 7, 2014 Sheet 1 of 21 US 8,623,055 B2
3
4 U.S. Patent Jan. 7, 2014 Sheet 3 of 21
5 U.S. Patent Jan. 7, 2014 Sheet 4 of 21 US 8,623,055 B2 s d) S -
6 U.S. Patent Jan. 7, 2014 Sheet 5 of 21 US 8,623,055 B2 s s
7 U.S. Patent Jan. 7, 2014 Sheet 6 of 21 US 8,623,055 B2 60 Z60
8 U.S. Patent Jan. 7, 2014 Sheet 7 of 21
9 U.S. Patent Jan. 7, 2014 Sheet 8 of 21 US 8,623,055 B2 & AA Filii Ei Illiili III lity AIEEE f E. E. OO.9) L s
10 U.S. Patent Jan. 7, 2014 Sheet 9 of 21 US 8,623,055 B2 S. A Y\
11 U.S. Patent Jan. 7, 2014 Sheet 10 of 21 US 8,623,055 B2 /* A has us V \. a1 (5) \ N
12 U.S. Patent Jan. 7, 2014 Sheet 11 of 21 US 8,623,055 B2
13 U.S. Patent Jan. 7, 2014 Sheet 12 of 21 US 8,623,055 B2
14 U.S. Patent Jan. 7, 2014 Sheet 13 of 21 US 8,623,055 B2
15 U.S. Patent Jan. 7, 2014 Sheet 14 of 21 US 8,623,055 B2
16 U.S. Patent Jan. 7, 2014 Sheet 15 of 21 US 8,623,055 B2
17 U.S. Patent Jan. 7, 2014 Sheet 16 of 21 US 8,623,055 B2
18 U.S. Patent Jan. 7, 2014 Sheet 17 of 21 US 8,623,055 B2 g/l (61-)
19 U.S. Patent Jan. 7, 2014 Sheet 18 of 21 US 8,623,055 B2 S wome D (S u O CD CD >
20 U.S. Patent Jan. 7, 2014 Sheet 19 of 21 US 8,623,055 B2 ºd u) ggolyg
21 U.S. Patent Jan. 7, 2014 Sheet 20 of 21 US 8,623,055 B2
22 U.S. Patent Jan. 7, 2014 Sheet 21 of 21 US 8,623,055 B2
23 1. SPINOUS PROCESSFUSION AND ORTHOPEDIC MPLANTS AND METHODS REFERENCE TO PRIORITY DOCUMENT This application is a continuation of and claims priority to U.S. patent application Ser. No. 12/727,641, issuing as U.S. Pat. No ,629 on Nov. 6, 2012, which is hereby incor porated by reference in its entirety, and which claims priority of U.S. Provisional Patent Application Ser. No. 61/210,581 filed Mar. 19, Priority of the aforementioned filing date is hereby claimed and the disclosure of the Provisional Patent Application is hereby incorporated by reference it its entirety. BACKGROUND The present disclosure relates to devices and methods that permit fixation and stabilization of the bony elements of the skeleton of a patient. The devices permit adjustment and maintenance of the spatial relationship(s) between neighbor ing bones. Depending on the specifics of the embodiment design, the motion between adjacent skeletal segments may be limited or completely eliminated. Spinal degeneration is an unavoidable consequence of aging and the disability produced by the aging spine has emerged as a major health problem in the industrialized world. Alterations in the anatomical alignment and physi ologic motion that normally exists between adjacent spinal Vertebrae can cause significant pain, deformity, weakness, and catastrophic neurological dysfunction. Surgical decompression of the neural tissues and immobi lization of the vertebral bones is a common option for the treatment of spinal disease. Currently, vertebral fixation is most frequently accomplished by anchoring bone screws into the pedicle portion of each vertebral body and then connect ing the various screw fasteners with an interconnecting rod. Subsequent rigid immobilization of the screw/rod construct produces rigid fixation of the attached bones. A shortcoming of the traditional rod/screw implant is the large Surgical dissection required to provide adequate expo Sure for instrumentation placement. The size of the dissection site produces unintended damage to the muscle layers and otherwise healthy tissues that Surround the diseased spine. A less invasive spinal fixation implant would advantageously minimize the damage produced by the Surgical exposure of the spine. In U.S. Pat. No. 7,048,736, Robinson etal teach the use of interspinous process plate to fixate adjacent vertebrae. As disclosed, the device is used to Supplement orthopedic implant and for bone graft material placed into the interver tebral disc between the attached vertebra. Thus the device functions to immobilize the vertebrae until bone fusion occurs but, in itself, does not provide a compartment for bone graft placement within the posterior aspect of the spine. Since bone graft material must be placed in order to achieve verte bral fusion, the device must be used in conjunction with bone graft material that is placed at a secondary site of the attached Vertebra bones, such as within the disc space, between adja cent transverse processes, and the like. This is a significant disadvantage and prevents use of the Robinson device by itself to both immobilize and fuse the vertebral bones. The growing experience with spinal fusion has shed light on the long-term consequences of vertebral immobilization. It is now accepted that fusion of a specific spinal level will increase the load on, and the rate of degeneration of the spinal segments immediately above and below the fused level. As the number of spinal fusion operations have increased, so US 8,623,055 B have the number of patients who require extension of their fusion to the adjacent, degenerating levels. The rigidity of the spinal fixation method has been shown to correlate with the rate of the degenerative progression of the adjacent segments. In specific, implantation of Stiffer instrumentation, Such as rod/screw implants, produced a more rapid progression of the degeneration disease at the adjacent segment than use of a less stiff fixation implant. SUMMARY This application discloses several exemplary devices that attach onto the spinous processes of adjacent vertebrae and address the limitation and shortcomings of prior devices and methods. In one embodiment, a device comprises an implant immobilizes the attached vertebrae through a minimally inva sive Surgical approach while providing a compartment within the implant for the placement of bone graft or bone graft substitute. The bone graft material then fuses the spinous processes and/or lamina portion of bone of the vertebral bone to which the device is attached. In another embodiment, the implant permits movement of the attached bone within a defined range of motion. The device is capable of preventing aberrant anterior and/or posterior spondylolisthesis as well as limiting the extent of flexion, extension, lateral flexion and rotation of the attached vertebral. Spinous process fixation provides good segmental immobilization through a mini mally invasive Surgical approach. In other exemplary embodiments, the implant is anchored to the pedicle portion of at least one vertebral bone to provide Superior bone fixation. In another embodiment, a bone anchor is placed through the pedicle of the inferior vertebra, across the disc space above the inferior vertebra, and into the lower boney surface of the upper vertebral bone. The implant employs a fastener that can be placed as free-standing device, or it can then be anchored to or interconnected with a fixation device that is anchored onto at least one spinous process. Further, a fastener may be used in this way through each of the two pedicles that are located on each side of the vertebral midline. In another embodiment, an implant or orthopedic device is adapted to fixate the spinous processes of vertebral bones. The implant includes at least one bone engagement or abut ment member located on each side of a spinous process of a first vertebra and a second vertebra, wherein the abutment members are adapted to forcibly abut the side of each spinous process. The implant has a locking mechanism that is adapted to rigidly immobilize at least a first abutment member on one side of the spinous process with at least a second abutment member on the other side of the spinous process (i.e., across the vertebral midline in the mid-sagittal plane from the first abutment member) using an interconnecting member (Such as, for example, a rod, plate, etc) that crosses the vertebral midline. The locking mechanism is capable of reversibly transitioning between a first state, wherein the orientation between at least one abutment member and the interconnect ing member is changeable in at least one plane and a second state, wherein the orientation between at least one abutment member and the interconnecting member is rigidly affixed. The implant further includes a compartment within at least one abutment member that is adapted to contain bone graft material, which can be bone graft, bone graft Substitute, or a combination thereof. In an aspect, there is disclosed an orthopedic implant for the fusion of adjacent bony segment. The implant comprises a first member and a second member opposed to the first member, wherein the first and second member define a space
24 3 therebetween sized to receive a bone. The first and second members have opposed surfaces each surface having at least one spiked protrusion for capturing a bone therebetween. At least one of the members defines an internal compartment adapted to contain a bone graft material, the compartment communicating with at least one bore hole in the at least one member for communicating the bone graft material with the captured bone. The bone graft material in the compartment extends from a first side of the first captured bone to a first side of a second captured bone, wherein the first side of the first and second capturedbones are also the sides penetrated by the spike protrusions. In another aspect, an orthopedic device configured to attach onto a spinous process of a first vertebral bone is disclosed. In one embodiment, the device comprises a first body comprising (i) a bone abutment Surface configured to abut an ipsilateral side of the spinous process, and a second Surface configured to oppose the bone abutment Surface, (ii) a second body comprising a bone abutment Surface configured to substantially face the bone abutment surface of the first body, and to abut a contralateral side of the spinous process, and a second Surface configured to oppose the bone abutment Surface, (iii) an interconnecting member configured to mov ably couple the first body and the second body, and (iv) a locking feature comprising an unlocked State and a locked state, the locked State configured to limit movement between the interconnecting member and at least one of the first body and the second body. At least one aperture is configured to extend from an opening of the bone abutment Surface of the first body to an opening of the second surface of the first body, the aperture being sized to permit bony fusion between the ipsilateral side of the spinous process and a bone forming material positioned within a cavity configured to abut the second surface of the first body. The cavity is configured to permit placement of at least a portion of the bone forming material after attachment of the orthopedic device onto the spinous process of the first vertebral bone. In yet another aspect, a method for stabilization of a first vertebral bone and a second vertebral bone is disclosed. In one embodiment, the method comprises: (i) positioning a first fixation member relative an ipsilateral side of a spinous pro cess of the first vertebral bone and an ipsilateral side of a spinous process of the second vertebral bone, (ii) positioning a second fixation member relative a contralateral side of the spinous process of the first vertebral bone and a contralateral side of the spinous process of the second vertebral bone, (iii) advancing at least one of the first and second fixation mem bers towards the other, (iv) capturing the spinous process of the first vertebral bone and the spinous process of the second vertebral bone between the first and second fixation members, (v) preventing separation of the first and second fixation members after the advancement, and (vi) advancing a bone screw through a pedicle portion of one the first and second Vertebral bones, the bone screw traversing a disc space between the first and second vertebral bones, and comprising a distal segment positioned within the body of another one of the first and second vertebral bones. In a further embodiment, the method comprises: (i) posi tioning a first fixation member such that the first fixation member extends from an ipsilateral side of a spinous process of each of the first and second vertebral bones, (ii) positioning a second fixation member Such that the second fixation mem ber extends from a contralateral side of the spinous processes of each of the first and second vertebral bones, (iii) advancing at least one of the first and second fixation members towards the other thereby capturing the spinous processes of the first and second vertebral bones there between, (iv) preventing US 8,623,055 B separation of the first and second fixation members after the advancement, (v) advancing a fastener through a pedicle por tion of one of the first and second vertebral bones, (vi) seating at least a segment of the interconnecting member within a receptacle of the fastener, and (vii) coupling the receptacle of the fastener to the interconnecting member. Multiple additional embodiments are described herein. Other features and advantages should be apparent from the following description of various embodiments, which illus trate, by way of example, the principles of the disclosed devices and methods. BRIEF DESCRIPTION OF THE DRAWINGS FIG. 1 illustrates perspective and orthogonal views of a pair of vertebral bones. FIG. 2 shows a perspective view of a bone implant system in a completely assembled State FIG. 3 shows the system with an interconnecting rod detached. FIG. 4 shows the system in an exploded state FIG. 5 shows various orthogonal views of an exemplary body member of the system. FIGS. 6A and 6B show plan views of the body member. FIG.7 shows perspective views of a locking member of the system. FIG. 8 show orthogonal views of the locking member. FIGS. 9A and 9B shows an embodiment of the system including a rod with spherical ends. FIG. 10 shows a method of implanting and using the sys tem 105. FIG. 11 shows the system in an implanted state. FIG. 12A shows an embodiment of an assembled bone screw assembly. FIG. 12B shows the bone screw assembly in an exploded State. FIGS. 13A, 13B, 14, and 15 show a method and device for using the bone implant system with one or more bone screw assemblies. FIG. 16 shows use of the system wherein one vertebral bone does not have a spinous process that will permit device fixation. FIGS. 17A and 17B show an additional embodiment of the system 105 that may be used with a bone screw. FIG. 18 illustrates an embodiment wherein a fastener is positioned through the pedicle of the inferior vertebra V1, across the disc space between the two vertebrae and into the inferior aspect of the upper vertebra. FIGS. 19A-19C show an exemplary embodiment of the fastener of FIG. 18. FIG. 20 shows the fastener in an implanted state. FIG. 21 shows the fastener and the system in an implanted State. DETAILED DESCRIPTION In order to promote an understanding of the principals of the disclosure, reference is made to the drawings and the embodiments illustrated therein. Nevertheless, it will be understood that the drawings are illustrative and no limitation of the scope of the invention is thereby intended, Any such alterations and further modifications in the illustrated embodiments, and any such further applications of the prin ciples of the invention as illustrated herein are contemplated as would normally occur to one of ordinary skill in the art. FIG. 1 illustrates perspective and orthogonal views of a pair of vertebral bones. The vertebrae are represented sche
25 5 matically and those skilled in the art will appreciate that actual vertebral bones may contain features that are not depicted in FIG. 1. FIG. 2 shows a perspective view of a bone implant system 105 in an assembled state. The system 105 includes several components, including at least two body members 110 and an elongated interconnecting member, Such as a rod 112 or plate, that interconnects the body members 110 in a spaced rela tionship with the space between the body members 110 sized and shaped to receive a portion of a vertebral body, Such as a spinous process. (The system 105 is described herein in the exemplary context of being used with a rod 112 but it should be appreciated that a plate or other interconnecting member may be used in place of the rod 112.) Each body member 110 has a corresponding locking mem ber 122 that couples to the respective body member 110 as described below. In addition, each locking member 122 has a corresponding locking nut 123 that can be threaded onto the locking member 122 and used to apply a downward locking force onto the respective member 110 and the rod 112 to immobilize the member 110, rod 112, and locking member 122 relative to one another, as described more fully below. FIG.3 shows the system 105 with the interconnecting rod 112 detached. FIG. 4 shows the system 105 in an exploded state. It should be appreciated that the use of terms herein such as upward, downward, front and back are with refer ence to the orientation shown in drawings and are not intended to be limiting. An exemplary embodiment of the body member 110 is now described with reference to FIG.5 and FIGS. 6A and 6B. FIG. 5 shows various orthogonal views of the body member 110 while FIGS. 6A and 6B show plan views of the body member 110. FIG. 6A shows the body member 110 with internal lines and FIG. 6B shows the body member 110 without internal lines. The illustrated embodiment of the system 105 includes a pair of body members 110, each of which is a mirror image of the other. With reference to FIGS. 5, 6A, and 6B, each body member 110 is an elongated body having outer walls that define a cavity that is at least partially enclosed by the outer walls. The body members are sized and shaped to be positioned next to and abut a spinous process of a vertebral body. In particular, each body member 110 includes a first side wall 1102, a second side wall 1104 opposed to the first side wall, a front wall 1106 and a back wall 1108 opposed to the front wall The walls 1102, 1104, 1106, and 1108 define an inner cavity The upper and lower boundaries of the inner cavity 1109 may be at least partially open, as depicted, or completely closed by additional walls. The cavity 1109 is adapted to open onto the space outside of member 110 through at least one aperture of the walls 1102, 1104, 1106, and/or 1108 and/or through the upper and lower boundaries of the cavity 109. That is, in an embodiment, the cavity 1109 is not a completely closed cavity. Thus, the walls 1102, 1104, 1106, and/or 1108 may include one or more holes, apertures, or openings that provide communication between the cavity 109 and a location outside of the body member 110. The cavity 1109 is adapted to receive and contain a bone graft material (which can be bone graft, bone graft Substitute, or a combination thereof) so that, when the system is implanted in the spine, the contained bone graft material can contact at least one vertebral bony surface through the afore mentioned aperture of the walls or through the upper lower boundaries of the cavity 109 that surround cavity The bone graft material may then form a fusion mass with that bony Surface. US 8,623,055 B With reference to FIG.5 and FIG. 6B, the side wall 1102 of each body member 110 includes a channel that is sized and shaped to accept a corresponding locking member 122. The other side wall 1102 also includes a complementary channel The locking member 122 is sized and shaped so that it can be inserted onto a respective body member 110 over the channels and as shown in FIG. 2. With reference still to FIGS. 5, 6A, and 6B, the wall 1102 includes one or more cut outs or seats sized and shaped to accept an instrument that can compress each of the two body members 110 toward and into the side bony aspect of a vertebral spinous process once the system 105 is coupled to a vertebral body. The seat does not necessarily extend through the full thickness of wall The wall 1104 of each body member 110 includes one or more protrusions that are adapted to forcibly penetrate and fixate onto a bony surface of a vertebral bone onto which member 110 is forcibly applied. The protrusions have a shape. Such as a pointed shape, that is configured to facilitate penetration into and fixation with the bony surface. One or more full thickness bore holes may extend through the wall 1104 of each body member 110 so that bone graft mate rial contained in cavity 1109 can pass through the hole(s) and contact at least a portion of the vertebral bony surface that is in contact with the wall 1104 and thereby form a fusion mass with the vertebral bone. As mentioned, the upper and lower boundaries of the cavity 1109 may be at least partially open (as shown in FIG. 5). The open upper and lower boundaries provide access to the cavity 109 to facilitate the placement of the bone graft material into cavity The open upper and lower boundaries may also serve as means through which bone graft material contained in cavity 1109 may come into contact with the adjacent ver tebral bone. Further, in an embodiment, either the upper and/ or lower boundaries of the cavity 1109 may contain a closed portion that encloses the upper or lower boundary. For example, the body member 110 may include a lower wall (FIG. 6B) that entirely or at least partially encloses the lower boundary of the cavity 1109 so as to limit contact between the graft material contained in cavity 1109 and struc tures that are preferably protected from bone graft contact. Such structures may include the dural surface of the spinal nerve column or spinal nerve. The lower wall may serve other functions, as discussed more fully bellow. An exemplary embodiment of a locking member 122 is now described with reference to FIGS. 7 and 8. Each locking member has a pair of opposed, upwardly extending side walls 1222 that form a space therebetween. The space between the side walls is sized and shaped to complement the shape of the channels and on the body member 110. In this manner, the locking member 122 can be slid or otherwise coupled onto a corresponding body member 110 in the region of the channels and The region of the locking member 122 below the side walls 1222 includes a protrusion 1226 that is contoured or shaped to form a seat that is sized and shaped to receive the rod 112, as described more fully below. The seat has a rounded surface that may complement the shape of the rod 112 so that the rod 112 can be firmly seated onto the seat. In addition, the lower region of the side walls 1222 form ledges that overhang the seat. The ledges and protrusion 1226 collectively form a space/ seat in which the interconnecting rod can be captured and/or immobilized relative to the locking member The pro trusion 1226 may include one more features adapted to accept a spherical portion of the interconnecting rod. For example, an indentation may be positioned on the protrusion for receiving a spherical portion of the interconnecting rod. The
26 7 indentation may be sized and shaped to receive any of a variety of shaped portions of the rod not limited to a spherical portion. With reference to FIG. 7, the interior surface of the side walls 1222 may have threads 1224 that threadingly mate with a corresponding locking nut 123. This permits the locking nut 123 to be threaded downward into the space between the side walls The assembled system 105 is now further described with reference to FIG. 2. The two body members 122 are posi tioned in a spaced apart relationship and coupled to one another via the rod 112. That is, the rod 112 is seated onto the seats formed by the protrusions 1226 on the lower portion of the locking members 122. Each of the locking members 122 is positioned on a respective body member 110 such as over the channels and (FIG. 5). Thus, the locking members 122 are attached to the body members while the rod 112 is seated on the locking members 122 such that a space is defined between the body members 110 to collectively form the system 105. The body members 110, locking members 122, and rod 112 can all be locked and immobilized relative to one another using the locking nuts 123. In particular, each locking nut is advanced downward into a locking member 122 such that the locking nut provides a downward force onto the body mem ber 110, at least a portion of which is positioned between the locking nut 123 and rod 112. With downward advancement of nut 123, a lower or an inferior surface of the locking nut 123 is moved toward, and forced against, the upper edge(s) of the respective body member 110. The upper edge(s) may include each of the first side wall 1102 and/or the second side wall The locking member 122 is thus forced upward relative to member 110 and the interconnecting rod 112 is forcibly con strained between ledge 1226 of the locking member 122 and the surface of the lower wall (FIG. 6A, 6B) of the cavity In this way, each of the body members 110 is immobilized relative to the interconnecting rod. While rod 112 is depicted as having a spherical portion 1122 in FIGS. 2-3, a rod having a spherical end (as shown in FIGS.9A-9B) may be alternatively used. Further, a straight or curvilinear rod without a spherical protrusion, a plate, or an interconnecting member of any applicable geometric con figuration may be alternatively used to interconnect the body members 110. As can be seen in FIGS. 2 and 9A-9B, the spherical portion of rod 112 interacts with the indentation in the seat of locking member 122 and also with the lower Surface of the wall of the member 110. This interaction allows the interconnecting rod 112 to be oriented and fixed in any one of a variety of positions (including non-orthogonal positions) relative to the body member 110 to which it is attached. FIG. 10 shows a method of implanting and using the sys tem 105. In use, the system is positioned posterior to the spinous processes, SP1 and SP2, of the vertebral bones to be immobilized. (Note that in FIG. 10, the system 105 is posi tioned above the posterior aspect of the vertebral bones. Thus, the system 105 is actually shown in a position that is anatomi cally posterior to the vertebral spinous processes, SP1 and SP2.) At this point in the implantation of the system 105, each of the locking nuts 123 is sufficiently loose so that each body member 110 can move relative to the interconnecting mem ber 112. The system 105 is then moved so that each body member 110 rests adjacent to a side of each of the spinous processes SP1 and SP2 of the two vertebral bones to be immobilized. That is, the body members will be positioned on either side of at least one spinous process such that a spinous process is positioned between a pair of body members 110. US 8,623,055 B Each body member 110 is then forced towards (that is, medial) the spinous processes positioned between the body members so that the protrusions of each second side wall 1104 of each body member 110 is forced into the side of the spinous process that is adjacent to it. In other words, the body members 110 are forced toward one another and also toward the spinous processes positioned between the body members 110 such that the protrusions penetrate the sides of the spinous processes. The body members 110 are forced towards one another by the action of at least one driver instrument (in an embodiment, the driver instrument may be shaped like pliers) that is pref erably adapted to interact with and compress each body mem ber 110 toward one another. The driver instrument may inter act with at, at least, one of indentations/cutouts of side wall 1102 of each body member 110. While at least one driver instrument maintains compression across the opposing body members 110 (and maintain a force that pushes the body members 110 toward one another), each of the locking nuts 123 is advanced downward toward the body members, as described above. The locking nuts 123 are advanced until all members (body member 110, locking member 122, and rod 112) of the system 105 are immobilized relative to one another. The driver instrument(s) is removed and each cavity 1109 (of the body members 110) is packed with bone graft material. Note that the bone graft material is then be placed in contact with the lateral wall of the spinous process, or forced out the lower surface of cavity 1109 and placed into contact with the posterior aspect of the vertebral lamina (VL), or both. (In the implanted State, the vertebral lamina are situated ana tomically anterior to the implant.) The implanted system is shown in FIG. 11. There is now described an additional embodiment wherein a bone screw assembly may be anchored into the pedicle portion of the vertebral bone and used as an additional point of device fixation. FIG. 12A shows an embodiment of an assembled bone screw assembly. FIG. 12B shows the bone screw assembly in an exploded state. The illustrated screw assembly is for example and those of ordinary skill in the art will appreciate that a large number of bone screws that are presently known, and/or yet to be known, may be alternative used in this application. With reference to FIGS. 12A and 12B, the exemplary embodiment of the bone screw assembly includes a bone screw having a head and a shank. The head of the bone screw can be seated in a receiver assembly of the bone screw assem bly. The receiver assembly includes an outer housing and an inner housing that collectively form a seat for the head of the bone screw. The bone screw assembly further includes a locking nut assembly that includes an upper member that is positioned above the head of the bone screw, a washer mem ber and a locking nut. The upper member has a pair of out wardly extending arms that fit between upwardly extending prongs of the inner and outer housings of the housing assem bly. In use, with reference to FIG. 13A and FIG. 13B, at lease one bone screw assembly is placed into a pedicle portion of the vertebral bone. A screw assembly may be placed into the pedicle portion of each of the two pedicles of the lower (i.e., inferior) vertebral bone of the pair of vertebrae to be immo bilized. In use, each bone screw may be positioned into the pedicle portion of the vertebral bones using any trajectory that permits proper screw placement. In a preferred embodiment, at least one bone screw is placed into the pedicle portion of the lower vertebral bone through a bone entry point that rests immediately inferior to the inferior articulating process of the
27 upper (i.e., superior) vertebral bone of the pair of vertebrae to be immobilized. In this way, the inferior articulating process of the upper vertebral bone abuts the superior surface of the bone screw and prevents further extension of the upper ver tebra relative to the lower vertebra. (Note that a facet joint is anatomically comprised of the articulation between the infe rior articulating process (IAP) of an upper (Superior) verte bral bone and the superior articulating process (SAP) of a lower (inferior) bone. These definitions of anatomical struc tures are known to those of ordinary skill in the art. They are described in more detail in Atlas of Human Anatomy, by Frank Netter, third edition, Icon Learning Systems, Teter boro, N.J. The text is hereby incorporated by reference in its entirety.) An elongated interconnecting rod is used to interconnect the screw assemblies. A system 105 is placed with body members 110 on each side of the spinous process (as described above) and coupled onto the rod as described above. (Alternatively, the interconnecting rod can be implanted with system 105 assembled and then lowered onto the screw assemblies.) After the placement of all instrumen tation, the locking nuts 123 and the locking nut assembly 52 (shown in FIG. 12) of the bone screws assemblies are then locked and all members of the system 105 and bone screw assembly are immobilized. FIGS. 13 and 14 shown an assembled construct. This provides a significant increase in the immobilization power of the system 105. In another embodiment, multi-level fixation can be per formed with serial implantation of multiple systems 105. The stepped configuration of each system 105 permits the place ment of more than one system 105 on a single spinous pro cess. FIG. 15 shows the fixation of three adjacent vertebral bones using two systems 105. While the systems 105 are shown attached to bone screws as in the embodiment of FIGS. 13 and 14, the systems 105 may be alternatively used without a bone screw anchor, as in the embodiment of FIG. 11. FIG.16 shows use of the system 105 wherein one vertebral bone does not have a spinous process that will permit device fixation. This situation can occur when, for example, the system 105 is used to immobilize the L5 and S1 vertebral bones. In that application, the S1 spinous process is often too Small to accommodate the fixation of a portion of body mem ber 110. In an additional embodiment, the situation can also arise when one of the vertebral bones had undergone a prior laminectomy. In either situation, the system 105 placed such that the body members 110 are affixed to the spinous process of a first vertebra and the pedicle portion of a second vertebra, wherein the attachment to the pedicles is preferably per formed through the use of pedicle bone screws. That is, the system 105 is attached to pedicle screws via the rod 112. By way of illustration, FIG. 16 shows that the lamina and spinous process of the inferior vertebra bone V1 have been removed. The lamina 207 and spinous process 209 of the upper vertebra V2 remains intact. While the protrusions of each body member 110 over the inferior vertebra bone V1 are shown as not contacting one another, in actual application the protrusions from each body member 110 over the removed lamina may abut at least a portion of the wall 1104 of the other member 110. FIGS. 17A and 17B show an additional embodiment of the system 105 that may be used with a bone screw. In this embodiment, the bone screw 214 transverse the pedicle por tion of a first vertebral bone, crosses the disc space between the first and second vertebral bones and enters the inferior surface of the second vertebral bone. While the bone screw is shown being detached from the system 105, it may be alter US 8,623,055 B natively comprised of a bone screw assembly that can fixate onto the interconnecting rod (similar to the embodiments of FIGS. 13 and 14). As shown in FIGS. 17A and 17B, a bone screw is used to cross the disc space and fixate the two vertebral bones. This fixation compliments the posterior fixation provided by the system 105 and thus provides fixation of the two vertebral bones that is both anterior and posterior to the spinal canal. In an alternative embodiment, a fastenerorbone screw may be similarly positioned into the pedicle of the inferior verte bra. The fastener then transverses the pedicle, crosses the disc space between the two vertebrae and enters the inferior aspect of the upper vertebra. The fastener may be further adapted to move the top vertebral bone relative to the lower vertebral bone. After re-positioning of the two vertebral bones, a sys tem 105 may be then applied to the posterior aspect of the two vertebrae. These devices and methods of use are particularly useful to re-align, at least partially, Vertebral bones that may be mal-aligned. FIG. 18 illustrates an embodiment whereina bone screw or fastener 310 is positioned through the pedicle of the inferior vertebra V1, across the disc space between the two vertebrae and into the inferior aspect of the upper vertebra. FIG. 19A shows an exemplary embodiment of the fastener 310. The fastener includes a first threaded elongated segment 3102 and a second threaded elongated segment 3104 that are attached to one another in an assembled state. FIG. 19B shows an assembled fastener wherein the two device segments 3102 and 3104 are attached with at least one link member The link members 3106 are elongated members that attach at opposite ends to the device segments 3102 and 3104 in a pivoting manner. The fastener 310 is implanted while in the configuration depicted in FIG. 19B. In this configuration, the link members 3106 are pivoted outward such that the seg ments 3102 and 3104 are moved further away from one another. After placement, the fastener is transitioned into the configuration shown in FIG. 19C wherein the link members 3106 are pivoted inward such that the segments 3102 and 3104 are moved toward away one another. The instrumenta tion needed to place the fastener into bone is not shown, but may be a simple driver that engages head While not shown, the mechanism and/or instrumentation needed to tran sition the fastener from the configuration of FIG. 19B into the configuration of FIG. 19C may include any of the mecha nism/instruments known in the art movement of a member 3104 relative to a member For example, it is contem plated that a small internal threaded screw is positioned within proximal member The engagable head of the small internal screw rests within head 3101 and the internal screw has a trajectory within the interior of the screw 310 that is eccentrically positioned along the long axis of member The trajectory of the small internal screw is schemati cally shown by A in FIG. 19C. To transition the screw 310 from the embodiment of FIG. 19B to the embodiment of FIG. 19C, the Small screw is engaged and threadedly advanced so as to forcibly abut the member 3106 within the interior of screw 310 at or about point X (FIG. 19C). With advancement of the small internal screw, member 3106 is forcibly rotated about a fixation pin FIG. 20 illustrates how, with transition to the configuration of FIG. 19C, the fastener310 can produce the posterior move ment of the upper vertebra V2, as well as an increase in the distance between the vertebra across the disc space. The fastener can also produce an increase in segmental lordosis, wherein the lordotic curvature of the lumbar spine is reformed, with a change to the configuration of FIG. 19C.
28 11 While the link members 3106 are shown as being substan tially equal in length, they may alternatively be non-equalso at produce desired movement of the bones (such as additional lordosis) with configuration change of the fastener. After reducing the bones as shown in FIG. 20, the system 105 may be attached to the spinous processes of the vertebral bones in order to immobilize the vertebrae in this position. This is shown in FIG. 21. While bone screw 310 is illustrated as a singular bone screw with the movable feature discussed above, it may alternatively containa proximal housing assem bly that is adapted to accept an interconnecting rod. A example of a screw assembly is shown in FIG. 12. The illus trated Screw assembly is for example and those of ordinary skill in the art will appreciate that a large number of bone screws that are presently known, and/or yet to be known, may be alternative used in this application. The disclosed devices or any of their components can be made of any biologically adaptable or compatible materials. Materials considered acceptable for biological implantation are well known and include, but are not limited to, stainless steel, titanium, tantalum, shape memory alloys, combination metallic alloys, various plastics, resins, ceramics, biologi cally absorbable materials and the like. Any components may be also coated/made with osteo-conductive (such as deminer ized bone matrix, hydroxyapatite, and the like) and/or osteo inductive (such as Transforming Growth Factor TGF-B. Platelet-Derived Growth Factor PDGF, Bone-Morpho genic Protein BMP and the like) bio-active materials that promote bone formation. Further, any surface may be made with a porous ingrowth Surface (such as titanium wire mesh, plasma-sprayed titanium, tantalum, porous CoCr, and the like), provided with a bioactive coating, made using tantalum, and/or helical rosette carbon nanotubes (or other carbon nanotube-based coating) in order to promote bone in-growth or establish a mineralized connection between the bone and the implant, and reduce the likelihood of implant loosening. Lastly, the system or any of its components can also be entirely or partially made of a shape memory material or other deformable material. While this specification contains many specifics, these should not be construed as limitations on the scope of an invention that is claimed or of what may be claimed, but rather as descriptions of features specific to particular embodi ments. Certain features that are described in this specification in the context of separate embodiments can also be imple mented in combination in a single embodiment. Conversely, various features that are described in the context of a single embodiment can also be implemented in multiple embodi ments separately or in any Suitable Sub-combination. More over, although features may be described above as acting in certain combinations and even initially claimed as such, one or more features from a claimed combination can in some cases be excised from the combination, and the claimed com bination may be directed to a Sub-combination or a variation of a sub-combination. Similarly, while operations are depicted in the drawings in a particular order, this should not be understood as requiring that such operations be performed in the particular order shown or in sequential order, or that all illustrated operations be performed, to achieve desirable results. Although embodiments of various methods and devices are described herein in detail with reference to certain versions, it should be appreciated that other versions, embodiments, methods of use, and combinations thereof are also possible. Therefore the spirit and scope of the appended claims should not be limited to the description of the embodiments con tained herein. US 8,623,055 B The invention claimed is: 1. A method for stabilization of a first vertebral bone and a second vertebral bone, said method comprising: positioning a bone abutment Surface of a first fixation member to abutan ipsilateral side of a spinous process of said first vertebral bone and an ipsilateral side of a spinous process of said second vertebral bone, said first fixation member comprising a second Surface opposite at least a segment of said bone abutment Surface and having at least one aperture configured to extend between said bone abutment Surface and said second Surface, said aperture being sized to permit formation of a bony fusion there through; positioning a second fixation member relative to a con tralateral side of said spinous process of said first verte bral bone and a contralateral side of said spinous process of said second vertebral bone; advancing at least one of said first and second fixation members towards the other; capturing said spinous process of said first vertebral bone and said spinous process of said second vertebral bone between said first and second fixation members; preventing separation of said first and second fixation members after said advancement; advancing a bone screw through a pedicle portion of one said first and second vertebral bones, said bone screw traversing a disc space between said first and second Vertebral bones, and comprising a distal segment posi tioned within said body of an other one of said first and second vertebral bones; and positioning a bone forming material adjacent to said sec ond surface of said first fixation member; wherein said first fixation member is configured to permit placement of at least a portion of said bone forming material after said advancement of said at least one of said first and second fixation members towards the other. 2. The method of claim 1, wherein preventing separation of said first and second fixation members after said advancement comprises using a locking feature of an interconnecting mem ber. 3. The method of claim 1, further comprising penetrating at least one of said spinous process said first vertebral bone and said spinous process of said second vertebral bone via a protrusion on a bone abutment Surface of said first fixation member. 4. The method of claim 1, further comprising penetrating at least one of said spinous process said first vertebral bone and said spinous process of said second vertebral bone via a protrusion on a bone abutment Surface of said second fixation member. 5. The method of claim 1, wherein said act of preventing separation of said first and second fixation members com prises positioning a locking feature at an intersection of said first fixation member and an interconnecting member config ured to couple said first fixation member to said second fixa tion member. 6. The method of claim 5, further comprising coupling said bone screw to said interconnecting member. 7. The method of claim 1, wherein said act of preventing separation of said first and second fixation members com prises positioning a locking feature at an intersection of said second fixation member and an interconnecting member con figured to couple said first fixation member to said second fixation member. 8. The method of claim 1, further comprising placing a bone forming material within a cavity of said second fixation member, said bone forming material causing formation of a
29 13 bony fusion with said contralateral side of said spinous pro cess of said first vertebral bone. 9. The method of claim 8, wherein said act of placing said bone forming material within said cavity of said second fixa tion member occurs after said advancement of said at least one of said first and second fixation members towards the other. 10. A method for stabilization of a first vertebral bone and a second vertebral bone, comprising: positioning a first fixation member to extend from an ipsi lateral side of a spinous process of said first vertebral bone to an ipsilateral side of a spinous process of said second vertebral bone, said first fixation member com prising a bone abutment Surface and a second Surface opposite at least a segment of said bone abutment Sur face, at least one aperture of said first fixation member being configured to extend between said bone abutment Surface and said second Surface, said aperture sized to permit formation of a bone fusion there through; positioning a second fixation member to extend from a contralateral side of said spinous processes of said first Vertebral bone to a contralateral side of a spinous process of said second vertebral bone; advancing at least one of said first and second fixation members towards the other, thereby capturing said spinous processes of said first and second vertebral bones there between; preventing separation of said first and second fixation members after said advancement; advancing a fastener through a pedicle portion of one of said first and second vertebral bones; seating at least a segment of an interconnecting member within a receptacle of said fastener, said interconnecting member being configured to couple said first and second fixation members; and positioning a bone forming material adjacent to said sec ond surface of said first fixation member; wherein said first fixation member is configured to permit placement of at least a portion of said bone forming material after said advancement of said at least one of said first and second fixation members towards the other. 11. The method of claim 10, wherein: said fastener comprises a bone screw; and said preventing separation comprises use of at least a lock ing feature. 12. The method of claim 11, wherein said act of using a locking feature to prevent said separation further comprises positioning said locking feature at an intersection of said interconnecting member and said first fixation member. 13. The method of claim 11, wherein said act of using a locking feature to prevent said separation further comprises: positioning said locking feature at an intersection of said interconnecting member and said second fixation mem ber; and transitioning said locking feature from an unlocked to a locked configuration. 14. The method of claim 10, further comprising causing at least one protrusion of said bone abutment surface of said first fixation member to penetrate one of said spinous processes of said first and second vertebral bones. 15. The method of claim 10, further comprising causing at least one protrusion of a bone abutment Surface of said second fixation member to penetrate one of said spinous processes of said first and second vertebral bones. 16. The method of claim 10, further comprising placing a bone forming material within a cavity of said second fixation member, said bone forming material causing formation of a US 8,623,055 B bony fusion with said contralateral side of said spinous pro cess of said first vertebral bone. 17. A method for stabilization of a first vertebral bone and a second vertebral bone, said method comprising: causing a bone abutment Surface of a first fixation member to abutan ipsilateral side of a spinous process of said first Vertebral bone and an ipsilateral side of a spinous pro cess of said second vertebral bone, said first fixation member comprising a second Surface opposite at least a segment of said bone abutment Surface and having at least one aperture configured to extend between said bone abutment Surface and said second surface, said aperture being sized to permit formation of a bony fusion therethrough; causing a second fixation member to be positioned relative to a contralateral side of said spinous process of said first Vertebral bone and a contralateral side of said spinous process of said second vertebral bone; advancing said first and second fixation members towards one another, capturing said spinous process of said first vertebral bone and said spinous process of said second vertebral bone between said first and second fixation members; preventing separation of said first and second fixation members; advancing a bone screw through a pedicle portion of one said first and second vertebral bones, said bone screw configured to traverse a disc space between said first and second vertebral bones, and comprising a distal segment positioned within said body of an other one of said first and second vertebral bones; and positioning a bone forming material adjacent to said sec ond surface of said first fixation member, said first fixa tion member being configured to permit positioning of at least a portion of said bone forming material after said advancement of said at least one of said first and second fixation members towards the other. 18. The method of claim 17, wherein preventing separation of said first and second fixation members after said advance ment comprises using a locking feature of an interconnecting member. 19. The method of claim 17, further comprising penetrat ing at least one of said spinous process said first vertebral bone and said spinous process of said second vertebral bone via a protrusion on a bone abutment Surface of said first fixation member. 20. The method of claim 17, further comprising penetrat ing at least one of said spinous process said first vertebral bone and said spinous process of said second vertebral bone via a protrusion on a bone abutment Surface of said second fixation member. 21. The method of claim 17, wherein said act of preventing separation of said first and second fixation members com prises positioning a locking feature at an intersection of said first fixation member and an interconnecting member config ured to couple said first fixation member to said second fixa tion member. 22. The method of claim 21, further comprising coupling said bone screw to said interconnecting member 23. The method of claim 17, wherein said act of preventing separation of said first and second fixation members com prises positioning a locking feature at an intersection of said second fixation member and an interconnecting member con figured to couple said first fixation member to said second fixation member. 24. The method of claim 17, further comprising placing a bone forming material within a cavity of said second fixation
Berry (43) Pub. Date: May 6, (76) Inventor: Bret Berry, Cordova, TN (US) (57) ABSTRACT
 US 20040O88054A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2004/0088054A1 Berry (43) Pub. Date: (54) LATERALLY EXPANDABLE CAGE (52) U.S. Cl.... 623/17.11 (76) Inventor: Bret
US 20040O88054A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2004/0088054A1 Berry (43) Pub. Date: (54) LATERALLY EXPANDABLE CAGE (52) U.S. Cl.... 623/17.11 (76) Inventor: Bret
(12) United States Patent (10) Patent No.: US 8,906,092 B2
 USOO8906092B2 (12) United States Patent (10) Patent No.: US 8,906,092 B2 Abdou (45) Date of Patent: Dec. 9, 2014 (54) SPINOUS PROCESS FIXATION DEVICES 2010/0234889 A1* 9, 2010 Hess... 606,249 AND METHODS
USOO8906092B2 (12) United States Patent (10) Patent No.: US 8,906,092 B2 Abdou (45) Date of Patent: Dec. 9, 2014 (54) SPINOUS PROCESS FIXATION DEVICES 2010/0234889 A1* 9, 2010 Hess... 606,249 AND METHODS
( 12 ) United States Patent
 ( 12 ) United States Patent Ingwer et al. US009907655B2 ( 10 ) Patent No. : US 9, 907, 655 B2 ( 45 ) Date of Patent : Mar. 6, 2018 ( 54 ) COMPONENTS FOR ARTIFICIAL JOINTS ( 56 ) References Cited U. S.
( 12 ) United States Patent Ingwer et al. US009907655B2 ( 10 ) Patent No. : US 9, 907, 655 B2 ( 45 ) Date of Patent : Mar. 6, 2018 ( 54 ) COMPONENTS FOR ARTIFICIAL JOINTS ( 56 ) References Cited U. S.
(12) United States Patent
 US009 198767B2 (12) United States Patent Abdou (10) Patent No.: (45) Date of Patent: US 9,198,767 B2 Dec. 1, 2015 (54) (71) (72) (*) (21) (22) (65) (60) (51) (52) (58) DEVICES AND METHODS FOR SPINAL STABILIZATION
US009 198767B2 (12) United States Patent Abdou (10) Patent No.: (45) Date of Patent: US 9,198,767 B2 Dec. 1, 2015 (54) (71) (72) (*) (21) (22) (65) (60) (51) (52) (58) DEVICES AND METHODS FOR SPINAL STABILIZATION
US 9,107,705 B2. Aug. 18, (45) Date of Patent: (10) Patent No.: Abdou ( ); A61F 2002/30471 ( ); A61F. (12) United States Patent (54)
 US009 107705B2 (12) United States Patent Abdou (10) Patent No.: (45) Date of Patent: US 9,107,705 B2 Aug. 18, 2015 (54) (76) (*) (21) (22) (65) (51) (52) (58) (56) DYNAMIC SPINAL STABILIZATION SYSTEMIS
US009 107705B2 (12) United States Patent Abdou (10) Patent No.: (45) Date of Patent: US 9,107,705 B2 Aug. 18, 2015 (54) (76) (*) (21) (22) (65) (51) (52) (58) (56) DYNAMIC SPINAL STABILIZATION SYSTEMIS
(12) United States Patent (10) Patent No.: US 8,137,401 B2
 USOO8137401B2 (12) United States Patent (10) Patent No.: US 8,137,401 B2 Stad et al. (45) Date of Patent: Mar. 20, 2012 (54) INTERVERTEBRAL DEVICE HAVING (56) References Cited EXPANDABLE ENDPLATES U.S.
USOO8137401B2 (12) United States Patent (10) Patent No.: US 8,137,401 B2 Stad et al. (45) Date of Patent: Mar. 20, 2012 (54) INTERVERTEBRAL DEVICE HAVING (56) References Cited EXPANDABLE ENDPLATES U.S.
(12) Patent Application Publication (10) Pub. No.: US 2004/ A1
 (19) United States US 2004O230191A1 (12) Patent Application Publication (10) Pub. No.: US 2004/0230191 A1 Frey et al. (43) Pub. Date: Nov. 18, 2004 (54) DISTRACTION AND RETRACTION SYSTEM FOR SPINAL SURGERY
(19) United States US 2004O230191A1 (12) Patent Application Publication (10) Pub. No.: US 2004/0230191 A1 Frey et al. (43) Pub. Date: Nov. 18, 2004 (54) DISTRACTION AND RETRACTION SYSTEM FOR SPINAL SURGERY
(12) Patent Application Publication (10) Pub. No.: US 2016/ A1
 US 20160135857A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2016/0135857 A1 Marrero, SR. (43) Pub. Date: May 19, 2016 (54) CURVEDTIBIOTALARFUSION NAIL AND Publication Classification
US 20160135857A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2016/0135857 A1 Marrero, SR. (43) Pub. Date: May 19, 2016 (54) CURVEDTIBIOTALARFUSION NAIL AND Publication Classification
(12) Patent Application Publication (10) Pub. No.: US 2007/ A1
 US 2007 O185493A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2007/0185493 A1 Feibel et al. (43) Pub. Date: Aug. 9, 2007 (54) CLAVICULAR BONE PLATE (30) Foreign Application
US 2007 O185493A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2007/0185493 A1 Feibel et al. (43) Pub. Date: Aug. 9, 2007 (54) CLAVICULAR BONE PLATE (30) Foreign Application
(12) Patent Application Publication (10) Pub. No.: US 2010/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2010/0094345 A1 Saidha et al. US 2010.009.4345A1 (43) Pub. Date: Apr. 15, 2010 (54) TRANSCONNECTOR (76) (21) (22) (86) Inventors:
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2010/0094345 A1 Saidha et al. US 2010.009.4345A1 (43) Pub. Date: Apr. 15, 2010 (54) TRANSCONNECTOR (76) (21) (22) (86) Inventors:
(12) United States Patent
 US008556757B2 (12) United States Patent Kilshaw (10) Patent No.: (45) Date of Patent: Oct. 15, 2013 (54) BICYCLE GEAR MECHANISM (76) Inventor: Richard J. Kilshaw, Lake Oswego, OR (US) *) Notice: Subject
US008556757B2 (12) United States Patent Kilshaw (10) Patent No.: (45) Date of Patent: Oct. 15, 2013 (54) BICYCLE GEAR MECHANISM (76) Inventor: Richard J. Kilshaw, Lake Oswego, OR (US) *) Notice: Subject
(12) Patent Application Publication (10) Pub. No.: US 2017/ A1
 (19) United States US 20170181774A1 (12) Patent Application Publication (10) Pub. No.: US 2017/0181774 A1 CAHILL (43) Pub. Date: Jun. 29, 2017 (54) MULTI-MODE TORQUE DRIVERS (52) U.S. Cl. EMPLOYING ANTI-BACKDRIVE
(19) United States US 20170181774A1 (12) Patent Application Publication (10) Pub. No.: US 2017/0181774 A1 CAHILL (43) Pub. Date: Jun. 29, 2017 (54) MULTI-MODE TORQUE DRIVERS (52) U.S. Cl. EMPLOYING ANTI-BACKDRIVE
I lllll llllllll Ill lllll lllll lllll lllll lllll
 (12) United States Patent Masini I lllll llllllll Ill lllll lllll lllll lllll lllll 111111111111111111111111111111111 US006558426Bl (10) Patent No.: US 6,558,426 Bl (45) Date of Patent: May 6, 2003 (54)
(12) United States Patent Masini I lllll llllllll Ill lllll lllll lllll lllll lllll 111111111111111111111111111111111 US006558426Bl (10) Patent No.: US 6,558,426 Bl (45) Date of Patent: May 6, 2003 (54)
IIII. United States Patent (19) Nolan et al. 11 Patent Number: 5,776,150 45) Date of Patent: Jul. 7, 1998
 United States Patent (19) Nolan et al. 54) SUTURE ASSIST DEVICE 75) Inventors: Leo J. Nolan; John P. Measamer, both of Cincinnati; James D. Staley, Jr., Loveland; Robert F. Welch, Maineville, all of Ohio
United States Patent (19) Nolan et al. 54) SUTURE ASSIST DEVICE 75) Inventors: Leo J. Nolan; John P. Measamer, both of Cincinnati; James D. Staley, Jr., Loveland; Robert F. Welch, Maineville, all of Ohio
SE CE. E. E. C. alignment.
 USOO6478799B1 (12) United States Patent (10) Patent No.: US 6,478,799 B1 Williamson (45) Date of Patent: Nov. 12, 2002 (54) INSTRUMENTS AND METHODS FOR USE FOREIGN PATENT DOCUMENTS N PERFORMING KNEE SURGERY
USOO6478799B1 (12) United States Patent (10) Patent No.: US 6,478,799 B1 Williamson (45) Date of Patent: Nov. 12, 2002 (54) INSTRUMENTS AND METHODS FOR USE FOREIGN PATENT DOCUMENTS N PERFORMING KNEE SURGERY
(12) Patent Application Publication (10) Pub. No.: US 2009/ A1
 (19) United States US 20090305855A1 (12) Patent Application Publication (10) Pub. No.: US 2009/0305855A1 Terre (43) Pub. Date: Dec. 10, 2009 (54) ABDOMINAL EXERCISE MACHINE (57) ABSTRACT An abdominal exercise
(19) United States US 20090305855A1 (12) Patent Application Publication (10) Pub. No.: US 2009/0305855A1 Terre (43) Pub. Date: Dec. 10, 2009 (54) ABDOMINAL EXERCISE MACHINE (57) ABSTRACT An abdominal exercise
(12) Patent Application Publication (10) Pub. No.: US 2012/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2012/0265315 A1 Kusogullariet al. US 20120265315A1 (43) Pub. Date: Oct. 18, 2012 (54) SHOULDER PROSTHESIS (75) Inventors: Levent
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2012/0265315 A1 Kusogullariet al. US 20120265315A1 (43) Pub. Date: Oct. 18, 2012 (54) SHOULDER PROSTHESIS (75) Inventors: Levent
(12) Patent Application Publication (10) Pub. No.: US 2009/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2009/0039210 A1 Yates et al. US 20090039210A1 (43) Pub. Date: Feb. 12, 2009 (54) (76) (21) (22) (60) CPAP HOSE SUPPORT SYSTEM Inventors:
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2009/0039210 A1 Yates et al. US 20090039210A1 (43) Pub. Date: Feb. 12, 2009 (54) (76) (21) (22) (60) CPAP HOSE SUPPORT SYSTEM Inventors:
(12) United States Patent (10) Patent No.: US 6,837,905 B1
 USOO6837905B1 (12) United States Patent (10) Patent No.: US 6,837,905 B1 Lieberman (45) Date of Patent: Jan. 4, 2005 (54) SPINAL VERTEBRAL FUSION IMPLANT 6,106,557 A * 8/2000 Robioneck et al.... 623/17.15
USOO6837905B1 (12) United States Patent (10) Patent No.: US 6,837,905 B1 Lieberman (45) Date of Patent: Jan. 4, 2005 (54) SPINAL VERTEBRAL FUSION IMPLANT 6,106,557 A * 8/2000 Robioneck et al.... 623/17.15
(12) United States Patent
 USOO9381093B1 (12) United States Patent Morris et al. (10) Patent No.: (45) Date of Patent: *Jul. 5, 2016 (54) (71) (72) (73) (*) (21) (22) (63) (51) (52) (58) LOCKING DEVICE FOR FXATION MECHANISM OF MEDICAL
USOO9381093B1 (12) United States Patent Morris et al. (10) Patent No.: (45) Date of Patent: *Jul. 5, 2016 (54) (71) (72) (73) (*) (21) (22) (63) (51) (52) (58) LOCKING DEVICE FOR FXATION MECHANISM OF MEDICAL
(12) United States Patent (10) Patent No.: US 7,744,043 B2
 USOO774.4043B2 (12) United States Patent () Patent No.: Otinger (45) Date of Patent: Jun. 29, 20 (54) CPAP HOSETENDER 6,854,694 B1* 2/2005 Van Etten... 248,75 7,040,581 B2 * 5/2006 Noelke et al.... 248,75
USOO774.4043B2 (12) United States Patent () Patent No.: Otinger (45) Date of Patent: Jun. 29, 20 (54) CPAP HOSETENDER 6,854,694 B1* 2/2005 Van Etten... 248,75 7,040,581 B2 * 5/2006 Noelke et al.... 248,75
(12) United States Patent (10) Patent No.: US 7,108,510 B2
 US00710851 OB2 (12) United States Patent (10) Patent No.: US 7,108,510 B2 Niznick (45) Date of Patent: Sep. 19, 2006 (54) ENDOSSEOUS DENTAL IMPLANT 6,733,291 B1* 5/2004 Hurson... 433,173 20O2/O110784 A1*
US00710851 OB2 (12) United States Patent (10) Patent No.: US 7,108,510 B2 Niznick (45) Date of Patent: Sep. 19, 2006 (54) ENDOSSEOUS DENTAL IMPLANT 6,733,291 B1* 5/2004 Hurson... 433,173 20O2/O110784 A1*
(12) Patent Application Publication (10) Pub. No.: US 2011/ A1
 (19) United States US 2011 0160728A1 (12) Patent Application Publication (10) Pub. No.: US 2011/0160728A1 Blitz et al. (43) Pub. Date: Jun. 30, 2011 (54) INTRAMEDULLARY COMPRESSION NAIL AND RELATED METHOD
(19) United States US 2011 0160728A1 (12) Patent Application Publication (10) Pub. No.: US 2011/0160728A1 Blitz et al. (43) Pub. Date: Jun. 30, 2011 (54) INTRAMEDULLARY COMPRESSION NAIL AND RELATED METHOD
(12) United States Patent
 (12) United States Patent Globerman et al. USOO6402777B1 (10) Patent No.: (45) Date of Patent: US 6,402.777 B1 Jun. 11, 2002 (54) RADIOPAQUE STENT MARKERS (75) Inventors: Oren Globerman, Holon; Mordechay
(12) United States Patent Globerman et al. USOO6402777B1 (10) Patent No.: (45) Date of Patent: US 6,402.777 B1 Jun. 11, 2002 (54) RADIOPAQUE STENT MARKERS (75) Inventors: Oren Globerman, Holon; Mordechay
(12) Patent Application Publication (10) Pub. No.: US 2017/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2017/0143905 A1 Goyal et al. US 20170143905A1 (43) Pub. Date: May 25, 2017 (54) (71) (72) (21) (22) (60) NEEDLE-FREE INUECTION GUIDE
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2017/0143905 A1 Goyal et al. US 20170143905A1 (43) Pub. Date: May 25, 2017 (54) (71) (72) (21) (22) (60) NEEDLE-FREE INUECTION GUIDE
(12) United States Patent
 (12) United States Patent US00880 1757B2 (10) Patent No.: US 8,801,757 B2 Abdou (45) Date of Patent: Aug. 12, 2014 (54) SPINAL STABILIZATION SYSTEMS AND (56) References Cited METHODS OF USE U.S. PATENT
(12) United States Patent US00880 1757B2 (10) Patent No.: US 8,801,757 B2 Abdou (45) Date of Patent: Aug. 12, 2014 (54) SPINAL STABILIZATION SYSTEMS AND (56) References Cited METHODS OF USE U.S. PATENT
EP A2 (19) (11) EP A2 (12) EUROPEAN PATENT APPLICATION. (43) Date of publication: Bulletin 2012/28
 (19) (12) EUROPEAN PATENT APPLICATION (11) EP 2 474 278 A2 (43) Date of publication: 11.07.2012 Bulletin 2012/28 (1) Int Cl.: A61B 17/80 (2006.01) (21) Application number: 1210644.8 (22) Date of filing:.01.2012
(19) (12) EUROPEAN PATENT APPLICATION (11) EP 2 474 278 A2 (43) Date of publication: 11.07.2012 Bulletin 2012/28 (1) Int Cl.: A61B 17/80 (2006.01) (21) Application number: 1210644.8 (22) Date of filing:.01.2012
TECHNICAL BROCHURE. Capture Facet Fixation System
 TECHNICAL BROCHURE Capture Facet Fixation System Table of Contents Product Overview...2 Instruments...4 Capture Facet Screw Surgical Technique Patient Preparation and Positioning...6 Guide Pin Placement...7
TECHNICAL BROCHURE Capture Facet Fixation System Table of Contents Product Overview...2 Instruments...4 Capture Facet Screw Surgical Technique Patient Preparation and Positioning...6 Guide Pin Placement...7
(12) Patent Application Publication (10) Pub. No.: US 2008/ A1
 US 20080082047A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2008/0082047 A1 Harmon (43) Pub. Date: Apr. 3, 2008 (54) VEIN HOLDER (52) U.S. Cl.... 604/115 (76) Inventor: Stoney
US 20080082047A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2008/0082047 A1 Harmon (43) Pub. Date: Apr. 3, 2008 (54) VEIN HOLDER (52) U.S. Cl.... 604/115 (76) Inventor: Stoney
Threshold Pedicular Fixation System Surgical Technique
 Threshold Pedicular Fixation System Surgical Technique Table of Contents Patient Preparation and Positioning... 2 Determining Incision Location... 3 Assembling the Cannulated Awl... 4 Guide Wire Placement...
Threshold Pedicular Fixation System Surgical Technique Table of Contents Patient Preparation and Positioning... 2 Determining Incision Location... 3 Assembling the Cannulated Awl... 4 Guide Wire Placement...
(12) United States Patent
 USOO8584.853B2 (12) United States Patent Knight et al. (10) Patent No.: (45) Date of Patent: US 8,584.853 B2 Nov. 19, 2013 (54) METHOD AND APPARATUS FORAN ORTHOPEDCFXATION SYSTEM (75) Inventors: Adam T.
USOO8584.853B2 (12) United States Patent Knight et al. (10) Patent No.: (45) Date of Patent: US 8,584.853 B2 Nov. 19, 2013 (54) METHOD AND APPARATUS FORAN ORTHOPEDCFXATION SYSTEM (75) Inventors: Adam T.
(12) United States Patent (10) Patent No.: US 6,224,174 B1
 USOO6224174B1 (12) United States Patent (10) Patent No.: US 6,224,174 B1 Mu (45) Date of Patent: *May 1, 2001 (54) POSTER DISPLAY APPARATUS 3.817,393 6/1974 Neilsen... 211/50 4,164,309 8/1979 Staats...
USOO6224174B1 (12) United States Patent (10) Patent No.: US 6,224,174 B1 Mu (45) Date of Patent: *May 1, 2001 (54) POSTER DISPLAY APPARATUS 3.817,393 6/1974 Neilsen... 211/50 4,164,309 8/1979 Staats...
(12) Patent Application Publication (10) Pub. No.: US 2007/ A1
 (19) United States US 2007025.0167A1 (12) Patent Application Publication (10) Pub. No.: US 2007/0250167 A1 Bray et al. (43) Pub. Date: Oct. 25, 2007 (54) (75) (73) (21) (22) (60) SPINE IMPLANTS Inventors:
(19) United States US 2007025.0167A1 (12) Patent Application Publication (10) Pub. No.: US 2007/0250167 A1 Bray et al. (43) Pub. Date: Oct. 25, 2007 (54) (75) (73) (21) (22) (60) SPINE IMPLANTS Inventors:
(12) Patent Application Publication (10) Pub. No.: US 2004/ A1
 US 20040121286A1 (19) United States (12) Patent Application Publication (10) Pub No: US 2004/0121286 A1 Aravena et al (43) Pub Date: (54) ORGANIC SHAPED INTERFACE FOR Related US Application Data DENTAL
US 20040121286A1 (19) United States (12) Patent Application Publication (10) Pub No: US 2004/0121286 A1 Aravena et al (43) Pub Date: (54) ORGANIC SHAPED INTERFACE FOR Related US Application Data DENTAL
(12) United States Patent (10) Patent No.: US 6,413,232 B1
 USOO6413232B1 (12) United States Patent (10) Patent No.: US 6,413,232 B1 Townsend et al. (45) Date of Patent: Jul. 2, 2002 (54) ORTHOPEDIC KNEE BRACE HAVING AN 5,807,294. A 9/1998 Cawley et al. ADJUSTABLE
USOO6413232B1 (12) United States Patent (10) Patent No.: US 6,413,232 B1 Townsend et al. (45) Date of Patent: Jul. 2, 2002 (54) ORTHOPEDIC KNEE BRACE HAVING AN 5,807,294. A 9/1998 Cawley et al. ADJUSTABLE
(12) Patent Application Publication (10) Pub. No.: US 2017/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2017/0196770 A1 Klintenstedt et al. US 201701.96770A1 (43) Pub. Date: Jul. 13, 2017 (54) (71) (72) (21) (22) (63) (60) (30) CNTAINER
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2017/0196770 A1 Klintenstedt et al. US 201701.96770A1 (43) Pub. Date: Jul. 13, 2017 (54) (71) (72) (21) (22) (63) (60) (30) CNTAINER
TM TM Surgical Technique
 TM TM Surgical Technique TABLE OF CONTENTS Reli SP Spinous Plating System Overview Device Description Implant Features Indications Instruments Access Instruments Preparation Instruments Insertion Instruments
TM TM Surgical Technique TABLE OF CONTENTS Reli SP Spinous Plating System Overview Device Description Implant Features Indications Instruments Access Instruments Preparation Instruments Insertion Instruments
A U X I L I A R Y C O N N E C T O R S Surgical Technique
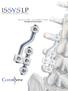 A U X I L I A R Y C O N N E C T O R S Surgical Technique AUXILIARY CONNECTORS ISSYS LP Auxiliary Connectors The ISSYS LP auxiliary connectors were designed to provide medial-lateral variability for the
A U X I L I A R Y C O N N E C T O R S Surgical Technique AUXILIARY CONNECTORS ISSYS LP Auxiliary Connectors The ISSYS LP auxiliary connectors were designed to provide medial-lateral variability for the
(12) Patent Application Publication (10) Pub. No.: US 2003/ A1. Giannelli (43) Pub. Date: Sep. 4, 2003
 US 20030166439A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2003/0166439 A1 Giannelli (43) Pub. Date: Sep. 4, 2003 (54) ROWING MACHINE Publication Classification (76) Inventor:
US 20030166439A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2003/0166439 A1 Giannelli (43) Pub. Date: Sep. 4, 2003 (54) ROWING MACHINE Publication Classification (76) Inventor:
(12) United States Patent (10) Patent No.: US 6,358,254 B1
 USOO6358254B1 (12) United States Patent (10) Patent No.: US 6,358,254 B1 Anderson (45) Date of Patent: Mar. 19, 2002 (54) METHOD AND IMPLANT FOR EXPANDING 5,722.977 A * 3/1998 Wilhelmy... 606/61 A SPINAL
USOO6358254B1 (12) United States Patent (10) Patent No.: US 6,358,254 B1 Anderson (45) Date of Patent: Mar. 19, 2002 (54) METHOD AND IMPLANT FOR EXPANDING 5,722.977 A * 3/1998 Wilhelmy... 606/61 A SPINAL
L8 Spine System SURGICAL TECHNIQUE. Add: No.1-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China
 Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
(12) United States Patent (10) Patent No.: US 7,128,575 B1. Sohn (45) Date of Patent: Oct. 31, 2006
 US007128575B1 (12) United States Patent (10) Patent No.: US 7,128,575 B1 Sohn (45) Date of Patent: Oct. 31, 2006 (54) TOOTHELEVATOR 1,762,888 A 6/1930 Roberts... 433/159 2,030,798 A 2/1936 Krajeski......
US007128575B1 (12) United States Patent (10) Patent No.: US 7,128,575 B1 Sohn (45) Date of Patent: Oct. 31, 2006 (54) TOOTHELEVATOR 1,762,888 A 6/1930 Roberts... 433/159 2,030,798 A 2/1936 Krajeski......
(12) Patent Application Publication (10) Pub. No.: US 2012/ A1
 (19) United States US 20120083881A1 (12) Patent Application Publication (10) Pub. No.: US 2012/0083881 A1 Claybrooks (43) Pub. Date: Apr. 5, 2012 (54) STAND-ALONE ANTERIOR FUSION DEVICE (52) U.S. Cl....
(19) United States US 20120083881A1 (12) Patent Application Publication (10) Pub. No.: US 2012/0083881 A1 Claybrooks (43) Pub. Date: Apr. 5, 2012 (54) STAND-ALONE ANTERIOR FUSION DEVICE (52) U.S. Cl....
(12) United States Patent
 US007094007B2 (12) United States Patent Satran et al. (10) Patent No.: (45) Date of Patent: Aug. 22, 2006 (54) TANGENTIAL CUTTING INSERT AND MILLING CUTTER (75) Inventors: Amir Satran, Kfar Vradim (IL);
US007094007B2 (12) United States Patent Satran et al. (10) Patent No.: (45) Date of Patent: Aug. 22, 2006 (54) TANGENTIAL CUTTING INSERT AND MILLING CUTTER (75) Inventors: Amir Satran, Kfar Vradim (IL);
Spinal Terminology Basics
 Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
(12) United States Patent (10) Patent No.: US 7.690,305 B2
 US0076903 05B2 (12) United States Patent (10) Patent No.: US 7.690,305 B2 Harjula et al. (45) Date of Patent: Apr. 6, 2010 (54) INCREMENT CHARGE FOR 4,408,534 A * 10, 1983 Araki et al.... 102.288 FIN-STABILIZED
US0076903 05B2 (12) United States Patent (10) Patent No.: US 7.690,305 B2 Harjula et al. (45) Date of Patent: Apr. 6, 2010 (54) INCREMENT CHARGE FOR 4,408,534 A * 10, 1983 Araki et al.... 102.288 FIN-STABILIZED
nva Anterior Lumbar Interbody Fusion System
 nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
United States Patent (19) Groesch et al.
 United States Patent (19) Groesch et al. 54 DUMMY FOR CAR CRASH TESTING 75) Inventors: Lothar Groesch; Gabriel Netzer, both of Stuttgart; Lothar Kassing, Nufringen, all of Fed. Rep. of Germany 73) Assignee:
United States Patent (19) Groesch et al. 54 DUMMY FOR CAR CRASH TESTING 75) Inventors: Lothar Groesch; Gabriel Netzer, both of Stuttgart; Lothar Kassing, Nufringen, all of Fed. Rep. of Germany 73) Assignee:
(12) Patent Application Publication (10) Pub. No.: US 2003/ A1
 US 2003O130096A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2003/0130096 A1 LaCroce (43) Pub. Date: Jul. 10, 2003 (54) BARBELL WITH PLURAL HAND GRIPPING Publication Classification
US 2003O130096A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2003/0130096 A1 LaCroce (43) Pub. Date: Jul. 10, 2003 (54) BARBELL WITH PLURAL HAND GRIPPING Publication Classification
(12) Patent Application Publication (10) Pub. No.: US 2009/ A1
 US 20090287233A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2009/0287233 A1 Huculak (43) Pub. Date: Nov. 19, 2009 (54) SMALL GAUGE MECHANICAL TISSUE Publication Classification
US 20090287233A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2009/0287233 A1 Huculak (43) Pub. Date: Nov. 19, 2009 (54) SMALL GAUGE MECHANICAL TISSUE Publication Classification
(12) Patent Application Publication (10) Pub. No.: US 2016/ A1
 (19) United States US 20160213850A1 (12) Patent Application Publication (10) Pub. No.: US 2016/0213850 A1 LOOF et al. (43) Pub. Date: Jul. 28, 2016 (54) MEDICAMENT DELIVERY DEVICE Publication Classification
(19) United States US 20160213850A1 (12) Patent Application Publication (10) Pub. No.: US 2016/0213850 A1 LOOF et al. (43) Pub. Date: Jul. 28, 2016 (54) MEDICAMENT DELIVERY DEVICE Publication Classification
(12) Patent Application Publication (10) Pub. No.: US 2005/ A1
 (19) United States US 2005O130094A1 (12) Patent Application Publication (10) Pub. No.: US 2005/0130094A1 Graham (43) Pub. Date: Jun. 16, 2005 (54) ORTHODONTIC ACCESSORY ARCH BAR (52) U.S. Cl.... 433/20
(19) United States US 2005O130094A1 (12) Patent Application Publication (10) Pub. No.: US 2005/0130094A1 Graham (43) Pub. Date: Jun. 16, 2005 (54) ORTHODONTIC ACCESSORY ARCH BAR (52) U.S. Cl.... 433/20
TSLP Thoracolumbar Spine Locking Plate
 Anterior thoracolumbar spine locking plate TSLP Thoracolumbar Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
Anterior thoracolumbar spine locking plate TSLP Thoracolumbar Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
4.5 System. Surgical Technique. This publication is not intended for distribution in the USA.
 4.5 System Surgical Technique This publication is not intended for distribution in the USA. Contents EXPEDIUM 4.5 Spine System 2 Features and Benefits 3 Surgical Technique Extended Tandem Connector 4 Placement
4.5 System Surgical Technique This publication is not intended for distribution in the USA. Contents EXPEDIUM 4.5 Spine System 2 Features and Benefits 3 Surgical Technique Extended Tandem Connector 4 Placement
Y o u r Id e a s En g i n e e r e d t o Li f e
 ISSYS LP Spinal Fixation System Surgical Guide Y o u r Id e a s En g i n e e r e d t o Li f e In t r o d u c t i o n ISSYS LP Sp i n a l Fixation System The foundation of the ISSYS LP Spinal Fixation System
ISSYS LP Spinal Fixation System Surgical Guide Y o u r Id e a s En g i n e e r e d t o Li f e In t r o d u c t i o n ISSYS LP Sp i n a l Fixation System The foundation of the ISSYS LP Spinal Fixation System
(12) United States Patent (10) Patent No.: US 6,210,432 B1
 USOO6210432B1 (12) United States Patent (10) Patent No.: US 6,210,432 B1 Solem et al. (45) Date of Patent: Apr. 3, 2001 (54) DEVICE AND METHOD FOR TREATMENT 5,980,552 * 11/1999 Pinchasik et al.... 623/1.16
USOO6210432B1 (12) United States Patent (10) Patent No.: US 6,210,432 B1 Solem et al. (45) Date of Patent: Apr. 3, 2001 (54) DEVICE AND METHOD FOR TREATMENT 5,980,552 * 11/1999 Pinchasik et al.... 623/1.16
(12) United States Patent
 (12) United States Patent USOO888265OB2 (10) Patent No.: US 8,882,650 B2 Finger (45) Date of Patent: Nov. 11, 2014 (54) EYELID PLAQUE (58) Field of Classification Search USPC... 600/1-8, 235, 236, 184,
(12) United States Patent USOO888265OB2 (10) Patent No.: US 8,882,650 B2 Finger (45) Date of Patent: Nov. 11, 2014 (54) EYELID PLAQUE (58) Field of Classification Search USPC... 600/1-8, 235, 236, 184,
(12) United States Patent (10) Patent No.: US 7, B2
 US007052479B2 (12) United States Patent (10) Patent No.: US 7,052.479 B2 Drennan (45) Date of Patent: May 30, 2006 (54) TRACTION DEVICE 3,762.405 A * 10/1973 De George... 602/23 3,771,519 A * 11/1973 Haake......
US007052479B2 (12) United States Patent (10) Patent No.: US 7,052.479 B2 Drennan (45) Date of Patent: May 30, 2006 (54) TRACTION DEVICE 3,762.405 A * 10/1973 De George... 602/23 3,771,519 A * 11/1973 Haake......
(12) Patent Application Publication (10) Pub. No.: US 2016/ A1
 US 2016O1 OO694A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2016/0100694 A1 PELLETER (43) Pub. Date: Apr. 14, 2016 (54) KNEE PILLOW Publication Classification (71) Applicant:
US 2016O1 OO694A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2016/0100694 A1 PELLETER (43) Pub. Date: Apr. 14, 2016 (54) KNEE PILLOW Publication Classification (71) Applicant:
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
NewBridge. Laminoplasty Fixation INTERNATIONAL EDITION
 NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
nvt Transforaminal Lumbar Interbody Fusion System
 nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvp Posterior Lumbar Interbody Fusion System
 nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
(12) United States Patent (10) Patent No.: US 8,715,321 B2
 US008715321 B2 (12) United States Patent (10) Patent No.: US 8,715,321 B2 Butler et al. (45) Date of Patent: May 6, 2014 (54) SPINAL FACET FASTENER D374,482 S 10/1996 Goble et al.... D24f145 5,643,321
US008715321 B2 (12) United States Patent (10) Patent No.: US 8,715,321 B2 Butler et al. (45) Date of Patent: May 6, 2014 (54) SPINAL FACET FASTENER D374,482 S 10/1996 Goble et al.... D24f145 5,643,321
X-spine Surgical Technique
 X-spine Surgical Technique The X90 Pedicle Screw System Revolutionary Design and Function This document is intended exclusively for experts in the field, particularly physicians, and is not intended for
X-spine Surgical Technique The X90 Pedicle Screw System Revolutionary Design and Function This document is intended exclusively for experts in the field, particularly physicians, and is not intended for
United States Patent (19)
 United States Patent (19) Kesling 54) ORTHODONTIC HOOKASSEMBLY AND APPLIANCE 75 Inventor: Christopher K. Kesling, LaPorte, Ind. 73 Assignee: TP Orthodontics, Inc., LaPorte, Ind. 21 Appl. No.: 852,046 22
United States Patent (19) Kesling 54) ORTHODONTIC HOOKASSEMBLY AND APPLIANCE 75 Inventor: Christopher K. Kesling, LaPorte, Ind. 73 Assignee: TP Orthodontics, Inc., LaPorte, Ind. 21 Appl. No.: 852,046 22
(12) Patent Application Publication (10) Pub. No.: US 2014/ A1
 (19) United States US 2014001 1160A1 (12) Patent Application Publication (10) Pub. No.: US 2014/0011160 A1 JOrneus et al. (43) Pub. Date: Jan. 9, 2014 (54) (71) (72) (73) (21) (22) (30) ABUTMENT SYSTEMAND
(19) United States US 2014001 1160A1 (12) Patent Application Publication (10) Pub. No.: US 2014/0011160 A1 JOrneus et al. (43) Pub. Date: Jan. 9, 2014 (54) (71) (72) (73) (21) (22) (30) ABUTMENT SYSTEMAND
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
Piersch (45) Date of Patent: Jun. 29, 1993
 United States Patent (19) 11) USOO5222902A Patent Number: 5,222,902 Piersch (45) Date of Patent: Jun. 29, 1993 54 INTERLOCKING BLOCKS 3,890,738 6/1975 Bassani... 44.6/1 3,900,985 8/1975 Yoen... 44.6/124
United States Patent (19) 11) USOO5222902A Patent Number: 5,222,902 Piersch (45) Date of Patent: Jun. 29, 1993 54 INTERLOCKING BLOCKS 3,890,738 6/1975 Bassani... 44.6/1 3,900,985 8/1975 Yoen... 44.6/124
US A United States Patent (19) 11 Patent Number: 5,474,555 Puno et al. 45 Date of Patent: Dec. 12, 1995
 I III US005474555A United States Patent (19) 11 Patent Number: Puno et al. 45 Date of Patent: Dec. 12, 1995 (54) SPINAL IMPLANT SYSTEM 4,771,767 9/1988 Steffee. 4,805,602 2/1989 Puno et al.... 606/73 75
I III US005474555A United States Patent (19) 11 Patent Number: Puno et al. 45 Date of Patent: Dec. 12, 1995 (54) SPINAL IMPLANT SYSTEM 4,771,767 9/1988 Steffee. 4,805,602 2/1989 Puno et al.... 606/73 75
M.I.S. MAKE IT SMART IN ONE SYSTEM. Surgical Technique. Hip Knee Spine Navigation
 M.I.S. MAKE IT SMART IN ONE SYSTEM Surgical Technique Hip Knee Spine Navigation M.U.S.T. Mini Open Surgical Technique Hip Knee Spine Navigation 2 C O N T E N T S 1 INTRODUCTION 4 2 SURGICAL TECHNIQUE 5
M.I.S. MAKE IT SMART IN ONE SYSTEM Surgical Technique Hip Knee Spine Navigation M.U.S.T. Mini Open Surgical Technique Hip Knee Spine Navigation 2 C O N T E N T S 1 INTRODUCTION 4 2 SURGICAL TECHNIQUE 5
(12) Patent Application Publication (10) Pub. No.: US 2011/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2011/0144694 A1 Laeng et al. US 20110144694A1 (43) Pub. Date: (54) (76) (21) (22) (60) BONE FXATIONASSEMBLY Inventors: Appl. No.:
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2011/0144694 A1 Laeng et al. US 20110144694A1 (43) Pub. Date: (54) (76) (21) (22) (60) BONE FXATIONASSEMBLY Inventors: Appl. No.:
(12) Patent Application Publication (10) Pub. No.: US 2014/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2014/0287886 A1 Patti US 20140287886A1 (43) Pub. Date: Sep. 25, 2014 (54) (71) (72) (21) (22) (60) PROTECTOR FOR EXERCISE BAR Applicant:
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2014/0287886 A1 Patti US 20140287886A1 (43) Pub. Date: Sep. 25, 2014 (54) (71) (72) (21) (22) (60) PROTECTOR FOR EXERCISE BAR Applicant:
(12) United States Patent (10) Patent No.: US 8,623,090 B2. Butler (45) Date of Patent: Jan. 7, 2014
 USOO8623090B2 (12) United States Patent (10) Patent No.: US 8,623,090 B2 Butler (45) Date of Patent: Jan. 7, 2014 (54) SPINAL DISC PROSTHESES 2005/0039836 A1 2/2005 Dugan et al. 2005/005.5099 A1 3, 2005
USOO8623090B2 (12) United States Patent (10) Patent No.: US 8,623,090 B2 Butler (45) Date of Patent: Jan. 7, 2014 (54) SPINAL DISC PROSTHESES 2005/0039836 A1 2/2005 Dugan et al. 2005/005.5099 A1 3, 2005
VECTRA-T SURGICAL TECHNIQUE. The Translational Anterior Cervical Palate System. This publication is not intended for distribution in the USA.
 VECTRA-T The Translational Anterior Cervical Palate System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description alone does not provide
VECTRA-T The Translational Anterior Cervical Palate System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description alone does not provide
Valencia Pedicle Screw Surgical Technique
 Valencia Pedicle Screw Surgical Technique VALENCIA CIRCUIT TABLE OF CONTENTS Design Rationale Indications for Use Surgical Technique 1. Pedicle Preparation 2. Screw Insertion 3. Rod Placement 4. Locking
Valencia Pedicle Screw Surgical Technique VALENCIA CIRCUIT TABLE OF CONTENTS Design Rationale Indications for Use Surgical Technique 1. Pedicle Preparation 2. Screw Insertion 3. Rod Placement 4. Locking
(12) United States Patent
 (12) United States Patent Kimber et al. USOO6565529B1 (10) Patent No.: US 6,565,529 B1 (45) Date of Patent: May 20, 2003 (54) TAMPEREVIDENT SYRINGE DESIGN (75) Inventors: Michael Browning Kimber, New South
(12) United States Patent Kimber et al. USOO6565529B1 (10) Patent No.: US 6,565,529 B1 (45) Date of Patent: May 20, 2003 (54) TAMPEREVIDENT SYRINGE DESIGN (75) Inventors: Michael Browning Kimber, New South
SURGICAL TECHNIQUE MANUAL. InterFuse T
 1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
HydraLok. Operative Technique. Polyaxial Pedicle Screw System
 HydraLok Operative Technique Polyaxial Pedicle Screw System Table of Contents Introduction...1 OPERATIVE TECHNIQUE OVERVIEW...2 DETAILED OPERATIVE TECHNIQUE...4 LOCATE AND PREPARE THE PEDICLE...4 PROBE
HydraLok Operative Technique Polyaxial Pedicle Screw System Table of Contents Introduction...1 OPERATIVE TECHNIQUE OVERVIEW...2 DETAILED OPERATIVE TECHNIQUE...4 LOCATE AND PREPARE THE PEDICLE...4 PROBE
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
(12) United States Patent
 USOO8707549B2 (12) United States Patent Burns et al. () Patent No.: (45) Date of Patent: Apr. 29, 2014 (54) (75) (73) (*) (21) (22) (65) (51) (52) (58) ERGONOMIC GRIPASSEMBLES AND HANDLES FORULTRASOUND
USOO8707549B2 (12) United States Patent Burns et al. () Patent No.: (45) Date of Patent: Apr. 29, 2014 (54) (75) (73) (*) (21) (22) (65) (51) (52) (58) ERGONOMIC GRIPASSEMBLES AND HANDLES FORULTRASOUND
(12) United States Patent
 (12) United States Patent Brown et al. USOO6494.914B2 (10) Patent No.: (45) Date of Patent: US 6,494.914 B2 Dec. 17, 2002 (54) UNICONDYLAR FEMORAL PROSTHESIS AND INSTRUMENTS (75) Inventors: David Ray Brown,
(12) United States Patent Brown et al. USOO6494.914B2 (10) Patent No.: (45) Date of Patent: US 6,494.914 B2 Dec. 17, 2002 (54) UNICONDYLAR FEMORAL PROSTHESIS AND INSTRUMENTS (75) Inventors: David Ray Brown,
United States Patent (19) Annoni
 United States Patent (19) Annoni (54. TOOTH TRANSILLUMINATING LIGHT HOLDER 76) Inventor: Jerry D. Annoni, 450 Maple Ave., Vallejo, Calif. 94591 (21) Appl. No.: 427,850 22 Filed: Sep. 29, 1982 51) Int.
United States Patent (19) Annoni (54. TOOTH TRANSILLUMINATING LIGHT HOLDER 76) Inventor: Jerry D. Annoni, 450 Maple Ave., Vallejo, Calif. 94591 (21) Appl. No.: 427,850 22 Filed: Sep. 29, 1982 51) Int.
ASFORA ANTERIOR CERVICAL PLATE SYSTEM (AACP) SURGICAL PROCEDURE MANUAL
 ASFORA ANTERIOR CERVICAL PLATE SYSTEM (AACP) SURGICAL PROCEDURE MANUAL Contents: Introduction Indications Contraindications Warnings Precautions Implant Overview Instruments Overview Surgical Technique
ASFORA ANTERIOR CERVICAL PLATE SYSTEM (AACP) SURGICAL PROCEDURE MANUAL Contents: Introduction Indications Contraindications Warnings Precautions Implant Overview Instruments Overview Surgical Technique
Table of Contents.
 surgical technique The Ambassador TM Anterior Cervical Plate System is a versatile system of implants and instruments with a variety of sizes to provide optimal anatomic compatibility. The integrated cam
surgical technique The Ambassador TM Anterior Cervical Plate System is a versatile system of implants and instruments with a variety of sizes to provide optimal anatomic compatibility. The integrated cam
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
United States Patent (19)
 USOO5437669A United States Patent (19) 11 Patent Number: Yuan et al. Date of Patent: Aug. 1, 1995 54). SPINAL FEXATION SYSTEMS WITH 5,246,442 9/1993 Ashman et al... 606/61 BFURCATED CONNECTORS 5,257,993
USOO5437669A United States Patent (19) 11 Patent Number: Yuan et al. Date of Patent: Aug. 1, 1995 54). SPINAL FEXATION SYSTEMS WITH 5,246,442 9/1993 Ashman et al... 606/61 BFURCATED CONNECTORS 5,257,993
United States Patent (19) 11 Patent Number: 4,821,355 Burkhardt (45) Date of Patent: Apr. 18, 1989
 United States Patent (19) 11 Patent Number: 4,821,5 Burkhardt () Date of Patent: Apr. 18, 1989 (54) SELF-ADJUSTING ORTHOPEDIC 4,447,922 5/1984 Brochu... 5/434 CERVICAL PLLOW 4,528,705 7/1985 Greenawalt...
United States Patent (19) 11 Patent Number: 4,821,5 Burkhardt () Date of Patent: Apr. 18, 1989 (54) SELF-ADJUSTING ORTHOPEDIC 4,447,922 5/1984 Brochu... 5/434 CERVICAL PLLOW 4,528,705 7/1985 Greenawalt...
(12) Patent Application Publication (10) Pub. No.: US 2012/ A1
 (19) United States US 2012.0089051A1 (12) Patent Application Publication (10) Pub. No.: US 2012/0089051A1 Draudt et al. (43) Pub. Date: Apr. 12, 2012 (54) BLOOD GLUCOSE METER HAVING INTEGRAL LANCET DEVICE
(19) United States US 2012.0089051A1 (12) Patent Application Publication (10) Pub. No.: US 2012/0089051A1 Draudt et al. (43) Pub. Date: Apr. 12, 2012 (54) BLOOD GLUCOSE METER HAVING INTEGRAL LANCET DEVICE
Handling instructions. USS Low Profile. Thoracolumbar posterior fixation system.
 Handling instructions USS Low Profile. Thoracolumbar posterior fixation system. U Table of contents Introduction Indications and contraindications 3 USS Low Profile implants 4 Handling implants with stick
Handling instructions USS Low Profile. Thoracolumbar posterior fixation system. U Table of contents Introduction Indications and contraindications 3 USS Low Profile implants 4 Handling implants with stick
US A 11 Patent Number: 5,577,984 Bare, II 45) Date of Patent: Nov. 26, ) FRAME FOR AWARIABLE IMPACT /1988 U.S.S.R..
 United States Patent (19) III IIHIII US005577984A 11 Patent Number: Bare, II 45) Date of Patent: Nov. 26, 1996 54) FRAME FOR AWARIABLE IMPACT 1416140 8/1988 U.S.S.R.. THERAPY SYSTEM 1556691 4/1990 U.S.S.R.
United States Patent (19) III IIHIII US005577984A 11 Patent Number: Bare, II 45) Date of Patent: Nov. 26, 1996 54) FRAME FOR AWARIABLE IMPACT 1416140 8/1988 U.S.S.R.. THERAPY SYSTEM 1556691 4/1990 U.S.S.R.
(12) United States Patent (10) Patent No.: US 6,234,797 B1
 USOO6234797B1 (12) United States Patent (10) Patent No.: Ura (45) Date of Patent: *May 22, 2001 (54) DENTAL IMPLANT AND METHOD FOR 5,322,443 6/1994 Beaty. INSTALLING THE SAME 5,336,225 8/1994 Zang. 5,338,197
USOO6234797B1 (12) United States Patent (10) Patent No.: Ura (45) Date of Patent: *May 22, 2001 (54) DENTAL IMPLANT AND METHOD FOR 5,322,443 6/1994 Beaty. INSTALLING THE SAME 5,336,225 8/1994 Zang. 5,338,197
The Most Reliable Spinal Solution
 MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
mild Devices Kit - Instructions for Use
 INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
Transforaminal Lumbar Interbody Fusion Cage (TLIF)
 Transforaminal Lumbar Interbody Fusion age (TLIF) 990100010 DOULE ENGINE MEDIL MTERIL O., LTD. No. 218 Houxiang Road, Haicang District, Xiamen 361022, P.R.hina Tel: +86 592 6087101 Fax: +86 592 6587078
Transforaminal Lumbar Interbody Fusion age (TLIF) 990100010 DOULE ENGINE MEDIL MTERIL O., LTD. No. 218 Houxiang Road, Haicang District, Xiamen 361022, P.R.hina Tel: +86 592 6087101 Fax: +86 592 6587078
Surgical Technique Manual
 InterFuse S Interbody Fusion System Surgical Technique Manual VERTEBRAL TECHNOLOGIES MS 4043-02 Rev. O Product Overview Introduction The VTI InterFuse S implant is an interbody fusion device that combines
InterFuse S Interbody Fusion System Surgical Technique Manual VERTEBRAL TECHNOLOGIES MS 4043-02 Rev. O Product Overview Introduction The VTI InterFuse S implant is an interbody fusion device that combines
(12) Patent Application Publication (10) Pub. No.: US 2005/ A1
 US 2005.0020415A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2005/0020415 A1 Reno (43) Pub. Date: (54) ISOMETRIC EXERCISE EQUIPMENT WITH Publication Classification PORTABLE
US 2005.0020415A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2005/0020415 A1 Reno (43) Pub. Date: (54) ISOMETRIC EXERCISE EQUIPMENT WITH Publication Classification PORTABLE
