ENOUS AND HOMOLOGOUS
|
|
|
- Timothy Cummings
- 5 years ago
- Views:
Transcription
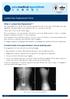
1 USE OF FROZEN CRANIAL BONE FLAPS FOR AUTOG- ENOUS AND HOMOLOGOUS GRAFTS IN CRANIOPLASTY AND SPINAL INTERBODY FUSION K E N N E T H H. ABBOTT, M.D. Department of Neurosurgery, The Ohio State University, Columbus, Ohio (Received for publication January ~7, 1953) CCASIONALLY the neurosurgeon finds it necessary in the course of a craniotomy for various conditions to leave a wide decompression, and therefore must sacrifice all or a part of a cranial bone flap. Under such circumstances he must either discard the bone or find a suitable method of preserving it. If suitably preserved it m a y be replaced at a later date, thus avoiding the use of artificial materials or other autogenous or homologous bone to fill in the cranial defect. It is the purpose of this paper to report m y experience with freezing of such cranial bone flaps and later replacing t h e m and following their course for a period of years. Attention will also be called to the value of preserving cranial bone in this manner for use in homologous cranioplasty in depressed skull fractures, after removal of tumors of the skull, and in other situations where tantalum, plastics, autogenous or homologous bone might be used for cranioplasty. Although little has been recorded concerning the use of cranial bone preserved by freezing, it has become apparent from conversation with many O FIG. 1. Case 1. Left lateral view of autogenous cranial graft ~6 months after operation. 380
2 USE OF FROZEN CRANIAL BONE FLAPS FOR GRAFTS 381 neurosurgeons that such autogenous and homologous grafts are being used not infrequently. It therefore seems advisable to record these experiences. The writer's experience began in January 1950, as a matter of necessity for decompressive purposes after the removal of a left frontal parasagittal meningioma when acute edema developed in the left frontal lobe. Rather than preserve the bone flap in alcohol, merthiolate, or other antiseptics, freezing was chosen as the method of preservation. The bone flap was wrapped in sterile towels, put in a sterile pan, and again wrapped in sterile towels. A few hours later it was placed in a "deep freeze" at the writer's home. The bone lay in the deep freeze at -10~ (-~3.3~ for 16 days. Three hours after removing the bone flap from the freezer it was aseptically inspected at the operating table and found to be in the same'condition as when it was removed from the skull. It was then replaced to its former site as an autogenous graft. The wound healed per primam with x-ray evidence of a normal take of this frozen preserved autogenous graft. Roentgenograms have been made of this graft at frequent intervals and now after e years the graft shows no evidence of serious shrinkage or loss of calcium content (Fig. 1). (X-rays of the graft at 3~ months appear the same as in Fig. 1.) Since this first experience with freezing a bone flap, the writer has used this same procedure in a total of 5 similar cases.* In addition there are on hand several bone flaps that have not been replaced. Thus there has developed a cranial bone bank which is proving useful for homologous grafts. Because experience in these cases has been so favorable, a brief review of the use of frozen cranial bone for homologous bone grafts for cranial defects will be detailed as well as their use in a modification of the Cloward type of spinal interbody fusion after removal of a protruded intervertebral disc. REPORTS OF CASES GROUP A. AUTOGENOUS CRANIAL GRAFTS Case 1. Female, aged 43 years. On Jan. 34, 1950, a left frontotemporoparietal craniotomy was performed for the removal of a parasagittal meningioma, angiomatous in type, weighing 300 gm. The bone flap was removed this same date because of severe cerebral edema. The flap was placed in the deep freezer chamber and on Feb. 9, 1950, was replaced. Postoperative roentgenograms taken at 13 months and 36 months (Fig. 1) show an excellent take of the graft. Case 2. Female, aged 43 years. On Mar. 8, 1950, a left parietofrontal craniotomy was performed for the removal of a meningioma. On March 18 subdural and epidural hemorrhages were evacuated. On March 19 the patient was again returned to surgery because of progressive severe cerebral edema with coincident symptoms of severe increased intracranial pressure. On April 10 osteomyelitis of the bone flap * Since this was submitted for publication 4 more such grafts have proven successful (~ autogenous and ~ homologous).
3 KENNETH H. ABBOTT Fro. ~. Case 2. (A) X-ray taken ~ months after replacement of autoclaved and frozen (5 months) bone flap, showing beginning absorption of the bone. (B) Showing severe absorption of graft ~6 months after replacement. was disclosed. The bone flap was removed, autoclaved, suitably wrapped, and placed in the deep freezer chamber. On Sept. 7, 1950, the autoclaved bone flap was replaced. Postoperative roentgenograms in November 1950 (Fig. ~A) disclosed early absorptive changes in the graft, while those made in November 195~ (Fig. ~B) show very severe absorption of the bone flap. FIG. 8. Case 3. Left lateral view showing frozen (~4 days) autogenous graft 16 months after operation.
4 USE OF FROZEN CRANIAL BONE FLAPS FOR GRAFTS 383 Comment. This is the only infected and subsequently autoclaved and frozen cranial bone flap I have a t t e m p t e d to replace. I t is also the only cranial graft t h a t has shown severe absorption. There are p r o b a b l y several reasons w h y such bone absorbs rather than maintains its normal structure and calcium content. I t seems probable t h a t the infection, plus the heat of autoclaving, m a y have so altered its structure as to prevent revascu]arization and remineralization. Case 3. Male, aged 48 years. On Aug. ~0, 1950 a left temporofroutal craniotomy was performed for evacuation of a chronic subdural hematoma. On Aug. ~, 1950, a postoperative subdural and epidural blood clot was removed. Because of acute cerebral edema the bone flap was removed and placed in the deep freezer chamber. On Aug. 30, 1950, the patient was again returned to surgery. There was a small amount of blood clot with a large accumulation of cerebrospinal fluid in the epidural and subdural spaces. He recovered with moderate neurologic residuals. Hence, the bone flap was not replaced until Sept. 14, The postoperative x-rays taken on Jan. ~3, 195~ (Fig. 3), 16 months after replacement of the bone flap, show the autogenous graft has taken well without demineralization. Case 4. Male, aged 68 years. On Sept. ~3, 1950 a right temporofrontoparietal craniotomy was carried out for the evacuation of a massive chronic subdural hematoma. On Sept. ~4, 1950 the patient was returned to surgery for evacuation of postoperative hemorrhage. On Sept. ~6, 1950, because of severe cerebral edema, FIo. 4. Case 5. Lateral view showing frozen (~3 days) autogenous cranial bone graft 9 months after replacement.
5 884 KENNETH H. ABBOTT the bone flap was removed and placed in the deep freezer chamber. He made an uneventful recovery. On Nov. 9, 1950, the bone flap was replaced. No postoperative x-rays were taken. The patient expired consequent to a coronary occlusion on Jan. 31,1951. Autopsy revealed a perfect take of the autogenous skull graft without local complications. There was no evidence of loss of calcium content or absorption of the graft. Unfortunately, no postoperative roentgenograms were available in this case. Case 5. Male, aged 8 years. On Feb. 19, 1953, a right frontotemporoparietal craniotomy was performed for a probable frontal lobe tumor, but none was found. The brain was under considerable increased tension, the pulse was slow, and the blood pressure was moderately elevated; hence it became apparent that decompression was mandatory. The dura mater was not closed, the brain being protected by a thin film of polyethylene sutured loosely in place. The bone flap was removed and placed in the deep freezer chamber. Subsequent studies of the tissue removed for biopsy revealed an "eosinophilic encephalitis." [This has been studied by several neuropathologists and no further diagnosis could be made.] By Mar. 14, 1953, the edema had subsided and the bone flap was replaced. Postoperative x-ray films made in December 1953 (Fig. 4) gave evidence of a satisfactory take of the frozen autogcnous graft. GROUP ~B. HOMOLOGOUS CRANIAL GRAFTS (to cranium) Case 6. Male, aged 45 years. On Sept. 1, 1951 a frontal osteoma was removed. A frozen homologous cranial bone was used as a graft carefully fitted to fill in the area and correct the disfigurement. The bone used had been frozen approximately 389 months and came from a patient who had succumbed following operative removal of a glioblastoma multiforme that necessitated a decompression. Postoperative roentgenograms 8 months later show an excellent take of the graft (Fig. 5). Case 7. Female, aged 39 years. On Apr. 18, 1953 an osteoid-osteoma was removed from the temporofrontal area. A frozen homologous cranial bone graft was used to fill in the area of defect. A successful take of the graft is shown by roentgenograms taken 8 months later (Fig. 6). Case 8. Male, aged 9 years. On Mar. 38, 1953 an old small depressed frontal skull fracture was elevated. Although some of the fragments were used to close the defect, more material was needed to fill in the remaining small defect; hence a small piece of frozen cranial bone was chosen. The wound healed satisfactorily. Roentgenograms taken in November 1953 (7 months later) revealed an excellent take of the graft (Fig. 7) and there was a very good cosmetic result. Case 9. Male, aged 16 years. One year previously, an eosinophilic granuloma had been removed (by another neurosurgeon), leaving a pulsating defect in the right frontotemporal area. This had worried the patient and he came in for a plastic procedure. On Aug. 11, 1953 a frozen homologous cranial bone graft was wired into the area, followed by primary union of the wound.
6 USE OF FROZEN CRANIAL BONE FLAPS FOR GRAFTS 385 FIG. 5. Case 6. Lateral view of frozen homologous cranial graft 8 months after operation. Fro. 6. Case 7. Lateral view of frozen homologous cranial graft 8 months after operation.
7 386 KENNETH H. ABBOTT FIG. 7 (left). Case 8. X-ray of homologous cranial graft 7 months after operation. Fro. 8 (right). Case 9. X-ray of homologous cranial graft 4 months after operation. Postoperative x-rays made in December 195~ (Fig. 8) revealed a good take of the graft, and inspection of the wound disclosed complete disappearance of the defect, leaving a satisfactory cosmetic result. GROUP C. HOMOLOGOUS CRANIAL GRAFTS (Spinal fusion--modified Cloward interbody fusion) The writer has now used multiple discs of frozen homologous cranial bone for fusion of the lumbar vertebral bodies (interbody fusion) after removal of the major portion of the intervertebral disc. The technique employed is a modification of Cloward's I operation for the fusion of the vertebral bodies: A guarded auger drill with pre-set depth stop is used to make the proper size "hole" in the intervertebral area, thus freshening the contiguous edges of the bodies of the vertebrae. Discs of cranial bone are carefully made with a hole saw of the same diameter as the auger drill. These are carefully placed in the intervertebral hole made by the auger. The Cloward vertebral spreader is released and the discs can be seen to seat themselves into the bodies of the vertebrae. Excellent stabilization of the bodies of the vertebrae can be demonstrated immediately. X-ray evidence of fusion of the vertebral bodies with preservation of the disc space has been demonstrated at a 6-month postoperative period. The technique for "pre-fit dowels" was first carried out by Wiltberger using autogenous bone dowels from the ilium. The writer has chosen to use the harder bone in the hope of maintaining the disc space.* * More recently a "pre-fit dowel" of iliac cancellous bone has been inserted between two cranial bone discs. This is done to facilitate earlier interbody fusion.
8 USE OF FROZEN CRANIAL BONE FLAPS FOR GRAFTS 387 However, the time interval (10 months) is not long enough to evaluate the method. These discs of skull bone can be seen in place at the lumbosacral level in the roentgenogram shown in Fig. 9. DISCUSSION While it is true that freezing has long been a satisfactory method of preserving bone by orthopedic surgeons, and freezing of soft tissues (nerves, arteries, tendons, fascia, etc.) has been used for other grafting purposes, to our knowledge this is the first report wherein the freezing of cranial bone has been described for autogenous and/or homologous Fro. 9. Lateral view of lumbosacral area showing g buttons of homologous cranial bone for interbody fusion in situ 6 months after operation. grafting on the skull itself. While it has proven successful in the writer's hands, he is cognizant of the problems peculiar to this and other methods of preserving bone. Attempts to maintain sterility of the skull bone have been done by the following means. First, the bone is immediately wrapped in several sterile towels and as quickly as possible is placed in a freezing chamber where it is "quick-frozen" and then it is not touched again until ready for use. In recent cases the bone has been dipped in or sprinkled with an aqueous solution of penicillin and streptomycin. It is hoped that this will further protect the graft from contamination. Furthermore, it has been the policy to place variable amounts of penicillin and streptomycin solution in the cranial bone-grafted wound just before the closure is completed. The patient is placed on heavy antibiotic therapy for ~ days before and for 5 days after the bone-graft operation. Whether or not other measures to prevent infection should be tried remains to be seen. So far the precautions as outlined have been sufficient to prevent infection of the graft. Some have suggested that each patient should be placed on heavy antibiotic therapy before each cranial operation. Then if a cranial bone graft is removed it will contain sufficient antibiotic to prevent growth of contaminating organisms. This may be possible but it seems doubtful. The desirability of having a separate small "deep freeze" type of unit to be used for this bone is immediately apparent. When one has to use a small corner of a large freezer unit used for other purposes, all too frequently various "accidents" will happen to the preciously preserved bone flap. In preparing "skull bone discs" for a modification of the Cloward I type of fusion of the bodies of the vertebrae (interbody fusion) I have chosen to use a "hole saw" and prepare these all at one time from a section of skull
9 388 KENNETH H. ABBOTT bone. They are packaged in groups of four discs and kept in the freezer unit at -10~ (-s176 This procedure has saved a great deal of time and has avoided further trauma and pain to the patient necessitated in the usual procedures. The writer has not as yet studied the important factors of changes in structure of the cranial bone caused by freezing. The degree of shrinkage of the graft has not been fully ascertained. It has been established that most homologous bone grafts shrink by at least ten per cent. Some of the cranial bone grafts herein studied may have shrunk a little, but it has not been of sufficient degree to be of clinical significance. Studies concerning this matter are under way and will be the subject of a future report. The course of one autogenous graft (Case ~, Group A) is of special interest for it was an infected bone flap which was autoclaved and then preserved by freezing for 5 months. This is the only graft that has shown serious severe absorption. It would therefore seem inadvisable to preserve and use such a graft. A similar disappointing experience was demonstrated with merthiolate-preserved cranial bone used for a homologous cranial graft. SUMMARY A method of preserving cranial bone flaps by rapid freezing for use either as autogenous or homologous grafts in the skull is described. Its successful use in 5 cases of autogenous cranial grafts and 4 of homologous cranial grafts is detailed. Incidental use of homologous grafts of frozen skull bone in the form of small discs for interbody fusions in a modification of the Cloward and Wiltberger type of spinal fusion is recorded. The matters of sterility, contamination, and bone shrinkage are discussed. It is concluded that the freezing of cranial bone when available is a safe, satisfactory, and desirable method. This method allows the use of a normal body tissue for grafting in the skull or spine, rather than using metal and plastic substances. REFERENCE 1. CLOWARD, R.B. The treatment of ruptured lumbar intervertebral discs by vertebral body fusion. I. Indications, operative technique, after care. J. Neurosurg., 1958, 10:
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
OPERATIVE TECHNIQUE. CONSTRUX Mini PTC. Mini PTC Spacer System
 OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
Surgical management of diastatic linear skull fractures in infants
 Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Aesculap CranioFix absorbable
 Aesculap CranioFix absorbable Aesculap Neurosurgery Instructions for use/technical description CranioFix absorbable Gebrauchsanweisung/Technische Beschreibung CranioFix resorbierbar 2 1 3 5 6 9 4 9 7
Aesculap CranioFix absorbable Aesculap Neurosurgery Instructions for use/technical description CranioFix absorbable Gebrauchsanweisung/Technische Beschreibung CranioFix resorbierbar 2 1 3 5 6 9 4 9 7
TABLE OF CONTENTS. ShurFit Anterior Cervical Interbody Fusion (ACIF) System Overview 2. Implant Specifications 3. Instrument Features 4
 Surgical Technique TABLE OF CONTENTS ShurFit Anterior Cervical Interbody Fusion (ACIF) System Overview 2 Product Highlights 2 Indications 2 Implant Specifications 3 Instrument Features 4 Surgical Technique
Surgical Technique TABLE OF CONTENTS ShurFit Anterior Cervical Interbody Fusion (ACIF) System Overview 2 Product Highlights 2 Indications 2 Implant Specifications 3 Instrument Features 4 Surgical Technique
SpineFAQs. Cervical Disc Replacement
 SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
Get back to: my life. Non-fusion treatment for lumbar spinal stenosis
 Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Aesculap CeSpace TM PEEK and CeSpace TM XP Spinal Implant System Instructions for Use
 Aesculap CeSpace TM PEEK and CeSpace TM XP Spinal Implant System Instructions for Use Page 1 of 5 Indications for use: When used as a Vertebral Body Replacement Device: The CeSpace PEEK and CeSpace XP
Aesculap CeSpace TM PEEK and CeSpace TM XP Spinal Implant System Instructions for Use Page 1 of 5 Indications for use: When used as a Vertebral Body Replacement Device: The CeSpace PEEK and CeSpace XP
PRIVILEGE APPLICATION FORM - [Mercy Medical Center]
![PRIVILEGE APPLICATION FORM - [Mercy Medical Center] PRIVILEGE APPLICATION FORM - [Mercy Medical Center]](/thumbs/89/98821167.jpg) Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
nva Anterior Lumbar Interbody Fusion System
 nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
Customized Cranial and Craniofacial Implants. Instructions For Use. 7000revD_Instructions_For_Use. Page 1 of 8
 Customized Cranial and Craniofacial Implants Instructions For Use Page 1 of 8 Table of Contents INDICATIONS... 3 DESCRIPTION OF DEVICE... 3 CONDITIONS OF USE... 3 CONTRAINDICATIONS... 3 KELYNIAM GLOBAL
Customized Cranial and Craniofacial Implants Instructions For Use Page 1 of 8 Table of Contents INDICATIONS... 3 DESCRIPTION OF DEVICE... 3 CONDITIONS OF USE... 3 CONTRAINDICATIONS... 3 KELYNIAM GLOBAL
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY
 Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
C-THRU Anterior Spinal System
 C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
SYNTHECEL Dura Repair. Assurance and Versatility for Dura Reconstruction.
 SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
Pathologies, Procedures and Room Set-Up
 Pathologies, Procedures and Room Set-Up Degenerative diseases - arthritis, osteoperosis Most common cause for neck pain and back pain Herniated disks or bulging disk Commonly occur at L4-5, L5-S1 Spinal
Pathologies, Procedures and Room Set-Up Degenerative diseases - arthritis, osteoperosis Most common cause for neck pain and back pain Herniated disks or bulging disk Commonly occur at L4-5, L5-S1 Spinal
A Patient s Guide to Lumbar Discectomy. PHYSIO.coza
 A Patient s Guide to Lumbar Discectomy SANDTON MEDICLINIC 011 706 7495 FAIRWAYS LIFE HOSPITAL 011 875 1827 ST STITHIANS 082 378 9642 JEPPE BOYS HIGH SCHOOL 084 816 5457 JOHANNESBURG, SANDTON@PHYSIO.CO.ZA
A Patient s Guide to Lumbar Discectomy SANDTON MEDICLINIC 011 706 7495 FAIRWAYS LIFE HOSPITAL 011 875 1827 ST STITHIANS 082 378 9642 JEPPE BOYS HIGH SCHOOL 084 816 5457 JOHANNESBURG, SANDTON@PHYSIO.CO.ZA
Neurosurgery (Orthopaedic PGY-1) Goals. Objectives
 Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Zimmer Anterior Buttress Plate System. Surgical Technique
 Zimmer Anterior Buttress Plate System Surgical Technique 2 Zimmer Anterior Buttress Plate System Surgical Technique Zimmer Anterior Buttress Plate System Surgical Technique Description, Indications & Contraindications...
Zimmer Anterior Buttress Plate System Surgical Technique 2 Zimmer Anterior Buttress Plate System Surgical Technique Zimmer Anterior Buttress Plate System Surgical Technique Description, Indications & Contraindications...
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
Primary Repair of Compound Skull Fractures by Replacement of Bone Fragments*
 1. Neurosurg. / Volume 30 / lune, 1969 Primary Repair of Compound Skull Fractures by Replacement of Bone Fragments* FRED C. KRISS, M.D., JAMES A. TAKEN, M.D., AND EDGAR A. KAHN, M.D. Department o] Surgery,
1. Neurosurg. / Volume 30 / lune, 1969 Primary Repair of Compound Skull Fractures by Replacement of Bone Fragments* FRED C. KRISS, M.D., JAMES A. TAKEN, M.D., AND EDGAR A. KAHN, M.D. Department o] Surgery,
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
Lumbar drains. Information for patients Neurosurgery
 Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
T HE continuity of the dura mater is a prime necessity. Various processes
 THE USE OF ORLON FOR DURAL REPLACEMENT JORGE HUERTAS, M.D. Department of Neurology, Georgetown University Hospital, Washington, D.C. (Received for publication April 11, 1955) T HE continuity of the dura
THE USE OF ORLON FOR DURAL REPLACEMENT JORGE HUERTAS, M.D. Department of Neurology, Georgetown University Hospital, Washington, D.C. (Received for publication April 11, 1955) T HE continuity of the dura
F OR several years we have used a linear. Limited exposure in cerebral surgery. Technical note. trephine aid drill. Technique
 Technical note DONALD H. WILSON, M.D. Section o/ Neurosurgery, Dartmouth-Hitchcock Medical Center, Hanover, New Hampshire ~' A limited exposure is possible, and perhaps preferable, for most cerebral surgery.
Technical note DONALD H. WILSON, M.D. Section o/ Neurosurgery, Dartmouth-Hitchcock Medical Center, Hanover, New Hampshire ~' A limited exposure is possible, and perhaps preferable, for most cerebral surgery.
1105 two (2) vertebrae... 1, add on per additional vertebra
 SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
nvt Transforaminal Lumbar Interbody Fusion System
 nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvp Posterior Lumbar Interbody Fusion System
 nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Apache Cervical Interbody Fusion Device. Surgical Technique. Page of 13. LC-005 Rev F
 LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Facharzt fiir Unfallchirurgie Arbeitsunfallkrankenhaus, Linz, Austria
 THE USE OF DEEP-FROZEN CRANIAL-BONE HOMOGRAFTS IN THE REPAIR OF DEFECTS OF THE SKULL By R. STRELI, M.D. Facharzt fiir Unfallchirurgie Arbeitsunfallkrankenhaus, Linz, Austria IN orthopaedic and traumatic
THE USE OF DEEP-FROZEN CRANIAL-BONE HOMOGRAFTS IN THE REPAIR OF DEFECTS OF THE SKULL By R. STRELI, M.D. Facharzt fiir Unfallchirurgie Arbeitsunfallkrankenhaus, Linz, Austria IN orthopaedic and traumatic
Fusion Device. Surgical Technique. Cervical Interbody Fusion with Trabecular Metal Technology
 TM-S Fusion Device Surgical Technique Cervical Interbody Fusion with Trabecular Metal Technology 2 TM-S Fusion Device Surgical Technique Disclaimer This surgical technique is not intended for use in the
TM-S Fusion Device Surgical Technique Cervical Interbody Fusion with Trabecular Metal Technology 2 TM-S Fusion Device Surgical Technique Disclaimer This surgical technique is not intended for use in the
SURGICAL TECHNIQUE MANUAL. InterFuse T
 1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
SAMPLE. Neurosurgery/ Neurology. A comprehensive illustrated guide to coding and reimbursement ICD-10. Coding Companion
 Coding Companion www.optumcoding.com Neurosurgery/ Neurology A comprehensive illustrated guide to coding and reimbursement 2017 a ICD-10 A full suite of resources including the latest code set, mapping
Coding Companion www.optumcoding.com Neurosurgery/ Neurology A comprehensive illustrated guide to coding and reimbursement 2017 a ICD-10 A full suite of resources including the latest code set, mapping
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE
 CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
Osteosynthesis involving a joint Thomas P Rüedi
 Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
DISCLAIMER OF WARRANTY AND LIMITATION OF REMEDY
 0086 Instructions for Use ShurFit Anterior Cervical Interbody Fusion System Caution: Federal (USA) law restricts this device to sale by or on the order of a physician DISCLAIMER OF WARRANTY AND LIMITATION
0086 Instructions for Use ShurFit Anterior Cervical Interbody Fusion System Caution: Federal (USA) law restricts this device to sale by or on the order of a physician DISCLAIMER OF WARRANTY AND LIMITATION
Solitaire Anterior Spinal System
 Surgical Technique Solitaire Anterior Spinal System Independent Stabilization for the Anterior Column Available in Titanium and Contents Introduction... Page 1 Design Features... Page 2 Instruments...
Surgical Technique Solitaire Anterior Spinal System Independent Stabilization for the Anterior Column Available in Titanium and Contents Introduction... Page 1 Design Features... Page 2 Instruments...
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Surgical Technique. Apache Anterior Lumbar Interbody Fusion
 Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Advantage ALIF. Keith Shevlin Managing Director
 Advantage ALIF Unit 10, 9-11 Myrtle Street, Crows Nest NSW 2065 Keith Shevlin Managing Director keithshevlin@precisionsurgical.com.au Advantage ALIF Introduction & Indications for Use 1 Surgical Technique
Advantage ALIF Unit 10, 9-11 Myrtle Street, Crows Nest NSW 2065 Keith Shevlin Managing Director keithshevlin@precisionsurgical.com.au Advantage ALIF Introduction & Indications for Use 1 Surgical Technique
PART III IN HOSPITAL ON CALL ANESTHESIA COVERAGE
 Anesthesia g) A consultation may not be claimed where the patient is referred to the anesthetist for the sole purpose of providing post-operative Patient Controlled Analgesia. h) Tariff 8406 may not be
Anesthesia g) A consultation may not be claimed where the patient is referred to the anesthetist for the sole purpose of providing post-operative Patient Controlled Analgesia. h) Tariff 8406 may not be
Anterior Cervical Discectomy
 Anterior Cervical Discectomy Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with having a cervical disc
Anterior Cervical Discectomy Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with having a cervical disc
Quality of Life. Quality of Motion. A Patient s Guide to. Artificial Lumbar Disc Replacement
 Quality of Life. Quality of Motion. A Patient s Guide to Artificial Lumbar Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Lumbar Disc Degeneration, a lower spine condition
Quality of Life. Quality of Motion. A Patient s Guide to Artificial Lumbar Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Lumbar Disc Degeneration, a lower spine condition
Complex Limb Injury. Exceptional healthcare, personally delivered
 Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature
 Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
I N individuals who have sustained antenor polar brain injury, the differentiation
 VOL. 122, No. 3 FRONTAL EPIDURAL HEMATOMA* THE ANGIOGRAPHIC DIAGNOSIS WITH A NEW FINDING By DAVID DEE, JR., M.D.,f MERLIN E. WOESNER, M.D., and ISAAC SANDERS, M.D. LOS ANGELES, CALIFORNIA I N individuals
VOL. 122, No. 3 FRONTAL EPIDURAL HEMATOMA* THE ANGIOGRAPHIC DIAGNOSIS WITH A NEW FINDING By DAVID DEE, JR., M.D.,f MERLIN E. WOESNER, M.D., and ISAAC SANDERS, M.D. LOS ANGELES, CALIFORNIA I N individuals
VTI INTERFUSE S SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK.
 VTI INTERFUSE S SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK. CONTENTS InterFuse S Product Description Indications for Use X-Ray Marker Locations and Product Specifications Instrument Set 3 4 5-7 STEP
VTI INTERFUSE S SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK. CONTENTS InterFuse S Product Description Indications for Use X-Ray Marker Locations and Product Specifications Instrument Set 3 4 5-7 STEP
Posterior Cervical Decompression
 Posterior Cervical Decompression Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a narrowing of your
Posterior Cervical Decompression Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a narrowing of your
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
THE RECOVERY PROCESS
 THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
Surgical technique. SynCage-C short
 Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
QIN4432TRICREV01. IMPORTANT PRODUCT INFORMATION FOR TRITANIUM C Cervical Cage. Version 1 1 STERILE PRODUCT
 IMPORTANT PRODUCT INFORMATION FOR TRITANIUM C Cervical Cage STERILE PRODUCT DESCRIPTION The Stryker Spine Tritanium C Anterior Cervical Cage is a hollow, ring shaped titanium alloy (Ti-6Al- 4V) interbody
IMPORTANT PRODUCT INFORMATION FOR TRITANIUM C Cervical Cage STERILE PRODUCT DESCRIPTION The Stryker Spine Tritanium C Anterior Cervical Cage is a hollow, ring shaped titanium alloy (Ti-6Al- 4V) interbody
PRO-DENSE BONE GRAFT SUBSTITUTE
 PRO-DENSE BONE GRAFT SUBSTITUTE 152917-0 The following languages are included in this packet: For additional languages, visit our website www.wright.com. Then click on the option. For additional information
PRO-DENSE BONE GRAFT SUBSTITUTE 152917-0 The following languages are included in this packet: For additional languages, visit our website www.wright.com. Then click on the option. For additional information
Adult - Cerebrovascular. Adult - Cranio-Cervical Junction. Adult - Epilepsy. Adult - Hydrocephalus
 list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
Alamo T Transforaminal Lumbar Interbody System Surgical Technique
 Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
A Patient s Guide to Artificial Joint Replacement of the Ankle
 A Patient s Guide to Artificial Joint Replacement of the Ankle Introduction Surgery to replace the ankle joint with an artificial joint (called ankle arthroplasty) is becoming more common. This surgery
A Patient s Guide to Artificial Joint Replacement of the Ankle Introduction Surgery to replace the ankle joint with an artificial joint (called ankle arthroplasty) is becoming more common. This surgery
100 Interpace Parkway Parsippany, NJ
 100 Interpace Parkway Parsippany, NJ 07054 www.biometspine.com 800-526-2579 All trademarks are the property of Biomet, Inc. or one of its subsidiaries, unless otherwise indicated. Rx Only. 2009 EBI, LLC.
100 Interpace Parkway Parsippany, NJ 07054 www.biometspine.com 800-526-2579 All trademarks are the property of Biomet, Inc. or one of its subsidiaries, unless otherwise indicated. Rx Only. 2009 EBI, LLC.
Posterior. Lumbar Fusion. Disclaimer. Integrated web marketing. Multimedia Health Education
 Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries. Goes to 6N
 Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Flexible Fragment Fixation. Surgical Technique
 Flexible Fragment Fixation Surgical Technique 2 F 3 Flexible Fragment Fixation The F 3 Fragment Plating System offers low profile, yet strong fixation in a locked plating construct that can be contoured
Flexible Fragment Fixation Surgical Technique 2 F 3 Flexible Fragment Fixation The F 3 Fragment Plating System offers low profile, yet strong fixation in a locked plating construct that can be contoured
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW
 MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
LBL-014. Rev
 Package Insert Z- CLAMP ISP System Device Description: The Z-CLAMP ISP System is supplemental fixation device consisting of a variety of shapes and sizes of one-level lumbar and sacral plates and screws.
Package Insert Z- CLAMP ISP System Device Description: The Z-CLAMP ISP System is supplemental fixation device consisting of a variety of shapes and sizes of one-level lumbar and sacral plates and screws.
Anterior Cervical Discectomy and Fusion (ACDF)
 Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Developments in bone grafting in veterinary orthopaedics part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Doxpal. Self-retaining Retractor
 Doxpal Self-retaining Retractor Doxpal Easy to use and reposition Doxpal retractors are easy to use and easy to reposition due to the elastic properties of the plastic. There are no locking devices to
Doxpal Self-retaining Retractor Doxpal Easy to use and reposition Doxpal retractors are easy to use and easy to reposition due to the elastic properties of the plastic. There are no locking devices to
PRO-DENSE Bone Graft Substitute The following languages are included in this packet:
 EN PRO-DENSE Bone Graft Substitute 133486-11 The following languages are included in this packet: English (en) For additional languages, visit our website www.wmt.com Then click on the Prescribing Information
EN PRO-DENSE Bone Graft Substitute 133486-11 The following languages are included in this packet: English (en) For additional languages, visit our website www.wmt.com Then click on the Prescribing Information
Restoration not just repair
 DURAGEN ENGLISH Restoration not just repair r e g e n e r at i v e t e c h n o l o g y PRODUCTS FOR SALE IN EUROPE, MIDDLE-EAST and AFRICA ONLY. More than a graft DuraGen is a matrix for repair of the
DURAGEN ENGLISH Restoration not just repair r e g e n e r at i v e t e c h n o l o g y PRODUCTS FOR SALE IN EUROPE, MIDDLE-EAST and AFRICA ONLY. More than a graft DuraGen is a matrix for repair of the
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
TABLE OF CONTENTS. Vault C Anterior Cervical Discectomy 2 and Fusion (ACDF) System Overview. Implants 3. Instruments 5. Surgical Technique 10
 Surgical Technique TABLE OF CONTENTS Vault C Anterior Cervical Discectomy 2 and Fusion (ACDF) System Overview Indications 2 Implants 3 Instruments 5 Surgical Technique 10 1. Preoperative planning 10 2.
Surgical Technique TABLE OF CONTENTS Vault C Anterior Cervical Discectomy 2 and Fusion (ACDF) System Overview Indications 2 Implants 3 Instruments 5 Surgical Technique 10 1. Preoperative planning 10 2.
INTELLIGENT SPINAL SYSTEM
 INTELLIGENT SPINAL SYSTEM I. Introduction II. Product Specification III. Surgical Technique IV. Ordering Information V. IFU for Lospa IS SPINAL SYSTEM The LOSPA IS spinal system consists of
INTELLIGENT SPINAL SYSTEM I. Introduction II. Product Specification III. Surgical Technique IV. Ordering Information V. IFU for Lospa IS SPINAL SYSTEM The LOSPA IS spinal system consists of
ACP. Anterior Cervical Plate System SURGICAL TECHNIQUE
 ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
Surgical Technique Manual
 InterFuse S Interbody Fusion System Surgical Technique Manual VERTEBRAL TECHNOLOGIES MS 4043-02 Rev. O Product Overview Introduction The VTI InterFuse S implant is an interbody fusion device that combines
InterFuse S Interbody Fusion System Surgical Technique Manual VERTEBRAL TECHNOLOGIES MS 4043-02 Rev. O Product Overview Introduction The VTI InterFuse S implant is an interbody fusion device that combines
Transforaminal Lumbar Interbody Fusion
 Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
Yasargil Permanent Aneurysm Clips
 Yasargil Permanent Aneurysm Clips Yasargil aneurysm clips Figure captions 1 Yasargil Phynox aneurysm clip, example of a straight clip 2 Yasargil titanium aneurysm clip, example of a straight clip 3 Yasargil
Yasargil Permanent Aneurysm Clips Yasargil aneurysm clips Figure captions 1 Yasargil Phynox aneurysm clip, example of a straight clip 2 Yasargil titanium aneurysm clip, example of a straight clip 3 Yasargil
product overview Implant heights range from 8mm-20mm in 2mm increments, with two lordocic angle options of 6 and 12.
 ETHOS A-Spacer PEEK System Surgical Technique Guide Synchronizing Medical Innovation with Global Markets product overview The SyncMedical Ethos PEEK IBF System is an intervertebral body fusion device for
ETHOS A-Spacer PEEK System Surgical Technique Guide Synchronizing Medical Innovation with Global Markets product overview The SyncMedical Ethos PEEK IBF System is an intervertebral body fusion device for
AN INTRODUCTION TO REGENERATIVE MEDICINE
 AN INTRODUCTION TO REGENERATIVE MEDICINE You ve undoubtedly come across some discussion of stem cells, likely with regard to stem cell research. But stem cells have a wide variety of uses in the medical
AN INTRODUCTION TO REGENERATIVE MEDICINE You ve undoubtedly come across some discussion of stem cells, likely with regard to stem cell research. But stem cells have a wide variety of uses in the medical
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Lumbar Disc Replacement FAQs
 ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS. By B. GRUNDT, M.D. Oslo, Norway
 SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
