LRI Children s Hospital
|
|
|
- Corey Ross
- 5 years ago
- Views:
Transcription
1 LRI Children s Hospital Hypoglycaemia in Infants & Children (not for use in the NNU or for Children diagnosed with diabetes) Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: June 2018 Version: V 2 Revision due: June 2021 Written by: Z.Mohamed, J Greening, J Forster Trust Ref: C19/ Introduction & Scope Clinical hypoglycaemia has been defined as a plasma glucose concentration low enough to cause symptoms and/or signs of impaired brain function [1].This glucose concentration varies from one patient to another, depending on the availability of alternative fuels and previous blood glucose concentrations. Moreover, in neonates, a decrease in blood glucose is expected after delivery and is physiologically normal. Hypoglycaemia is, therefore, a spectrum and the blood glucose concentration should be interpreted together with the clinical history and concentrations of counter-regulatory hormones and intermediate metabolites [1]. Biochemical hypoglycaemia refers to the inadequacy of circulating levels of blood glucose (BG) and is accepted as laboratory blood glucose measurement of < 2.6mmol/l in a neonate. After 72 hours of age in a term baby, normal blood glucose levels are Readings persistently below this level beyond 72 hours of age are abnormal [2, 6, 7]. Brain glucose utilisation becomes limited at approximate plasma glucose values of 3 to 3.6mmol/l, below which neuroglycopenic symptoms are triggered [1]. Therefore beyond neonatal period and in older children a value of BG 3mmol/l is recommended as lower limit for hypoglycaemia [1]. Hypoglycaemia may be associated with clinical symptoms and signs or be asymptomatic. This guideline is for the use of Medical and Nursing staff managing and preventing hypoglycaemia in infants and children within the Children s Hospital. For guidance in the treatment of hypoglycaemia in children with diabetes, please refer to UHL Hypoglycaemia in Children and Young People with Diabetes C95/2016. Related documents: UHL Consent to Examination or Treatment Policy A16/2002 Title: Hypoglycaemia in Infants & Children Page 1 of 15
2 UHL Intravenous Medication & Fluids Policy B25/2010 UHL Venous Access Policy B13/2010 UHL Aseptic Non Touch Technique (ANTT) Guideline B20/2013 UHL Infection Prevention Policy B4/2005 Measuring Capillary Blood Glucose C57/2005 UHL Prevention & Management of Hypoglycaemia in Neonates C22/ Hypoglycaemia Management. For infants < 6 months who are at risk of hypoglycaemia we consider the value for BG at which intervention is warranted to be 2.6 mmol/l. for children > 6 month consider intervention at BG value 3mmol/l In the absence of blood ketones (<0.1 mmol/l) a higher limit of BG 3.5 mmol/l must be used This is because there is an increased risk of neuroglypenia and brain insult in the absence of alternative brain fuel such as lactate and ketones that may be driven by hyperinsulinaemic state [4]. PLEASE REFER TO THE ALGORITHM: QUICK GUIDE FLOW CHART FOR EMERGENCY MANAGEMENT AND INVESTIGATION OF HYPOGLYCAEMIA (PAGE 3). [IF IN DOUBT, CONTACT THE ON-CALL PAEDIATRIC ENCORINOLOGY AND METABOLIC CONSULTANTS VIA SWITCH BOARD AVAILABLE 24 HRS- [see page 7] Background: Extrauterine adaptation of glucose homeostasis occurs after birth by gluconeogenesis. Following the clamping of the umbilical cord, blood glucose concentration decreases rapidly followed by a gradual stabilisation over the next 6-12 hours. Studies have demonstrated a wide range of glucose concentrations during the first 72 hours, with values ranging from mmol/l in healthy breast fed infants [2, 6]. Low plasma glucose activates a number of counterregulatory pathways resulting in increased systemic lipolysis with ketone utilisation by the brain [6]. Other alternative fuels such as pyruvate and lactate are also utilised by the brain and, as a result of these, the healthy newborn infant is probably not at risk of hypoglycaemia associated neuronal injury over the first few days. In contrast, preterm infants and those with altered homeostasis due to hyperinsulinemic states or intrauterine growth restriction may not produce alternative metabolites and are, therefore, at higher risk [2, 10, 11]. In majority of healthy neonates, the frequently observed low blood glucose concentrations are not related to any significant problem and merely reflect normal processes of metabolic adaptation to extra-uterine life [2]. However, when low blood glucose levels are prolonged or recurrent, they may result in acute systemic effects and cause long-term neurological damage or death [8, 11]. In addition, in a small number of infants, who may have maladaptation of glucose homeostasis, blood glucose monitoring with proactive recognition and treatment is essential [15]. Title: Hypoglycaemia in Infants & Children Page 2 of 15
3 Algorithm Flow Chart towards Emergency Management and Investigation of Hypoglycaemia *For contact details of the endocrine and metabolic teams please see page 7 Child age <6month Management of A B C Child age >6month BG < 2.6mmol/L mmol/l No acidosis/ ketones > 0.5mmol/l Fast acting carbohydrate -Oral glucose tablets -Oral glucose gel 1 tube = 10g - 150ml fruit juice DO NOT DELAY CORRECTION OF HYPOGLYCAEMIA WHILST AWAITING CONFIRMATION OF LAB GLUCOSE Tolerating feeds Check blood gas for acidosis and check Blood Ketones (bedside) Acidosis+ or ketones mmol/l Insert cannula Hypo screen (6ml blood)/next urine passed -See HYPO PACK list Fast acting carbohydrate -Oral glucose tablets -Oral glucose gel 1 tube = 10g - 150ml fruit juice BG < 3 mmol/l ketones <0.1 with +/- acidosis Insert cannula Hypo screen (6ml blood) see HYPOPACK list Send lab glucose to confirm Put urine bag on to collect next urine passed IV Access? Safe Caution At risk Colour codes Recheck in mins Aim BG >3mmol/L Sugary fluids / milk feeds if tolerated. Monitor for 4-6 hours Recurrent hypoglycaemia <3mmol/l >6m <2.6mmol/l <6m No Likely Ketotic hypoglycaemia Advice polycal if <2yrs age or fruit juice at the time of reduced fluid intake *GIR- glucose infusion rate Yes Correction of hypoglycaemia with IV dextrose Titrate IV / oral *Contact consultant metabolic/endocrine team early (via switch), for advice before discharge Not tolerating feeds IV dextrose bolus 2ml/kg followed by 10% dextrose/ 0.9% saline* infusion at a rate ml/kg/hr Aim BG > 3.5mmol/l at all times Calculate *GIR see below Drowsy/ unresponsive F/U with Immediate Insert IV / IO access If unwell/recurrent or persistent hypos, commence an IV glucose infusion using 10% dextrose/0.45% saline* at a rate of ml/kg/hr or increase concentration of dextrose to 12.5% until central access is established. Recheck BG at 5 min interval until blood sugar stable >3.5 mmol If unable to maintain BG >3.5 mmol despite IV dextrose may need glucagon infusion 5mcg/kg/hr. *Contact paediatric endocrinologist for advice via switch BG>2.6mmol/l % dextrose solution x ml/hr Weight (kg) X 6 Continue maintenance fluids, if commenced Gradually reintroduce feeds IF BG falls to less than 3 mmol/l within 60 mins of a feed use continuous feeds Check pre-feed blood sugar If continuing IVI monitor U&E s regularly (see IV fluid guidelines) Yes No Give IM glucagon < 8y (or <25 Kg) 0.5mg >8y (or > 25 Kg) - 1mg BG < 2.6mmol/l Check cannula patent Blue cannula prefered repeat 2ml/kg bolus 10% dextrose Increase rate up to 6ml/kg/hr 10%dextrose 0.45%saline Increase percentage dextrose in infusion -Central venous access if >12.5% dextrose. *Seek expert opinion if metabolic cause suspected. If adrenal insufficiency suspected give Hydrocortisone 4mg/kg max. 100mg iv and inform endocrine consultant on call Monitor U&E s regularly HYPO PACK Investigations for Hypoglycaemia: Labels can be printed from ICE. Title: Hypoglycaemia in Infants & Children Page 3 of 15
4 Symptoms: The following are typical symptoms and signs of hypoglycaemia but please be aware that this list is not exhaustive and a blood sugar should be checked in any unwell child. Neonate Pallor Sweating Tachypnoea Jitteriness Apnoea Hypotonia Feeding difficulties Irritability Abnormal cry Convulsions Infant and older child Anxiety Tremor Palpitations Weakness Nausea & Vomiting Hunger Abdominal pain Headache Confusion Coma Visual Disturbance Convulsions Initial assessment History Age Feeding History Birth history and weight Neonatal jaundice Tolerance to fasting/illness Drug ingestion Family history and parental consanguinity Signs Features of sepsis Hepatomegaly Encephalopathy Optic atrophy/cataracts Genitalia appearance Skin pigmentation Title: Hypoglycaemia in Infants & Children Page 4 of 15
5 Investigative work up for Hypoglycaemia: HYPO PACK Investigation Labels can either be printed from ICE (Hypoglycaemia tab under Path Order Sets ). The relevant bottles are stocked and found in the Yellow hypoglycaemia boxes available as a package in the Emergency Department and Paediatric wards. Take at least 6mls of blood during cannulation Priority tests are Glucose, acylcarnitine, Insulin, C-peptide and Cortisol, FFA, Beta hydroxybutyrate Get 2 ice packs ready. Please note that a separate form is required for specimens 1, 2 and 3 (i.e. 3 separate request forms) Please contact a porter to run the samples to the lab on ice immediately. A total of 6ml in 6 blood specimen bottles required (3 orange, 2 yellow, 1 white) ** RED- Time critical samples must be collected at the time of hypoglycaemia Lab Investigation Specimen type* Volume** Blood taken Time taken BLOOD Bedside Blood glucose stix 1 drop Bedside Blood gas (capillary /venous) 0.5 ml Fast-track 1 *Glucose and Lactate Fluoride oxalate (YELLOW top) 0.5 ml Fast-track 1 Ammonia On ice Lithium Heparin (ORANGE top) 0.5 ml Fast-track 1 U&E s, *Cortisol and GH White (WHITE top) 1.0 ml Specials 2 *Insulin and C- peptide On ice Lithium Heparin (ORANGE top) 1.5 ml Specials 2 *FFA and 3β-OHbutyrate Fluoride oxalate (YELLOW top) 1.0 ml Specials 2 *Acylcarnitine, Gal-1- Put and amino acids Lithium Heparin (ORANGE top)+ (drop-guthrie card) 1.0 ml URINE Bedside Urine dip ketones Specials 3 Urine organic acids Reducing substances Urine sample (universal pot) 5 ml Miscellaneous Testing: Alcohol Salicylates Blood Cultures LFT U&E Title: Hypoglycaemia in Infants & Children Page 5 of 15
6 Emergency management of hypoglycaemia: If child is conscious and not vomiting, Give oral glucose dextrogel ½ tube (5g) for infants < 6 months and 1 tube if > 6 months. In an older child give oral glucose g. 2 scoops of polycal in 30 ml milk or water, 200 ml milk or 2 teaspoons sugar, followed by a snack of starchy carbohydrates or a milk feed in infants In patients with altered consciousness give 2 ml/kg 10% glucose as intravenous bolus followed by infusion containing 10% glucose If no IV access available give stat glucagon IM: 0.5mg for patients < 8 yrs age or <25 kg, 1 mg for patients > 8 yrs age or >25 kg. Please note, this MUST be immediately followed by IV or IO access with infusion of Dextrose to maintain normal glycaemic state (BG>3.5mmol/L). Monitor BG at least 1hrly until stable. GLUCAGON IS RARELY EFFECTIVE IN METABOLIC PATIENTS PLEASE REFER TO SPECIFIC METABOLIC GUIDELINES IN Specific management for differing types of hypoglycaemia (Follow algorithm pg. 3) 1) Non-Ketotic hypoglycaemia If blood ketones < 0.1 mmol/l and glucose requirement is >8 mg/kg/min in an infant consider the diagnosis of hyperinsulinism. To calculate glucose requirement use the formula below. Glucose Infusion Calculator Glucose infusion rate (GIR) in mg / kg / min = % dextrose solution x ml/hr Weight x 6 Please see appendix 2 protocol to manage an infant with hyperinsulinism (if suspected, MUST CONSULT PAEDIATRIC ENDOCRINOLOGIST ON-CALL VIA SWITCH). If inborn error of metabolism is suspected, contact paediatric metabolic consultant on-call or (Sheffield- out of hours) see BIMDG emergency management guidelines ( for specific disorder and seek advice from metabolic consultant via switch. 2) Ketotic hypoglycaemia (KH) KH is the most common cause of hypoglycaemia in young nondiabetic children with or without metabolic disorder, chronic conditions such as gastrointestinal, endocrine or heart disease, Problems are usually precipitated by an intercurrent illness associated with anorexia or vomiting. A range of metabolic disorders can cause hypoglycaemia with ketosis. For any patient presenting with ketotic hypoglycaemia as the very first presentation, please refer to the flow chart for management (Algorithm 1, page 2). Title: Hypoglycaemia in Infants & Children Page 6 of 15
7 If this patient is known to have underlying metabolic condition and presents with ketotic hypoglycaemia, please refer to ( for specific guidelines on management. BIMDG have outlined specific emergency guidelines to treat and prevent high catabolic state, speak to metabolic team early, patient will usually have an emergency protocol and open access to emergency department and must be seen without delay. The fasting tolerance is shorter during infections in many IEMs depending on the metabolic condition [3]. As well as increasing the tendency to hypoglycaemia, catabolism often leads to the accumulation of toxic metabolites. It is, therefore, important to minimise catabolism, primarily by maintaining a high glucose intake with additional measures in specific disorders ( Please ensure you contact the Metabolic team consultant (via switch) for advice in such instance. It is recommended to prevent ketotic hypoglycaemia with additional support of emergency regimen of drinks containing soluble glucose polymer to provide large amounts of carbohydrate and calories at the time of reduced intake/losses. See Appendix 3. If children are unable to tolerate the oral emergency regimen, they need admission and intravenous glucose. Patients should receive this treatment even if their blood glucose is normal as its primary purpose is to reduce catabolism and prevent problems [3, 14]. Patients with fatty acid oxidation defects, for example, can develop arrhythmias or encephalopathy without hypoglycaemia, presumably due to accumulation of toxic metabolites. If it occurs, hypoglycaemia is a relatively late feature [16]. Fasting Provocation Test for hypoglycaemia (MUST be only done after discussion with endocrine/metabolic consultant) A fasting provocation test is occasionally indicated to help establish a diagnosis. This should never be completed without consulting a Paediatric endocrinologist/ metabolic consultant and a separate protocol is available for this. Contact details of Metabolic team : [ hr service provided 5/7 a week] Consultants : Dr J Forster Dr M Sharrard Clinical nurse specialist Metabolic Team: Siobhan Felix: OOH service via hospital switch board or Sheffield Switch board over weekends Contact details of Endocrine team : [ hr service provided 5/7 a week] Dr J Greening / Dr Vaya Tziaferi / Dr S Shenoy / Clinical Nurse Specialist Endocrine Team: Pauline Jones: OOH service via hospital switch board ask for the East Midland Paediatric Endocrine Consultant oncall service Title: Hypoglycaemia in Infants & Children Page 7 of 15
8 Interpreting the Results of the Hypoglycaemia Screen [3,9] Low Ketones (<0.5mmol/L) Raised Insulin (Insulin > 3mu/L When BG < 2.6mmol/L) Hyperammonia Metabolic acidosis Deranged LFT's Low cortisol Low sodium + High Potassium GH deficiency Raised lactate Urine Fatty acid oxidation defects or defects in ketogenesis Hyperinsulinism of infancy Hyperinsulinism of infancy Beckwith- Weidman syndrome Pancreatic islet cell adenoma Insulin poisoning Maternal diabetes Fatty acid oxidation defects Some organic acidaemia Urea cycle disorders Liver dysfunction Hyperinsulinism Fatty acid oxidation defects MCAD, LCAD Defects in ketogenesis Sepsis Glycogen storage disorders Organic acid disorders Most metabolic conditions in extremes Sepsis Liver disease Glycogen storage disease Galactosaemia Fat oxidation defects Hereditary fructose intolerance Adrenal insufficiency Congenital adrenal hyperplasia ACTH deficiency/ Hypopituitarism Adrenal disorders Panhypopituitarism Isolated GH deficiency Metabolic liver disease Prolonged convulsion Fructose 1,6-bisphosphatase Glycogen storage disorders(gsd 1) Sepsis Specific amino or organic acid disorders Title: Hypoglycaemia in Infants & Children Page 8 of 15
9 3. Education and Training Training of junior medical staff and nursing: at induction and adhoc ward training of how to follow the pathway. Education: presentation of abnormal results at in-house endocrine/metabolic meetings + children s hospital grand round. 4. Monitoring and Audit Criteria Key Performance Indicator 100 % compliance of hypo screens with full panel obtained >95% complication of contact with speciality team if hypopack blood taken Method of Assessment Frequency Lead Reporting arrangements Audit / Chem path Yearly JEG Local clinical practice team Monitor via monthly Biochemistry meeting/ audit Monthly JEG Local clinical practice team 5. Supporting Documents and Key References 1. Thornton PS, Stanley CA, De Leon DD, et al. Recommendations from the Pediatric Endocrine Society for Evaluation and Management of Persistent Hypoglycemia in Neonates, Infants, and Children. J Pediatr 2015;167: Stanley CA, Rozance PJ, Thornton PS, et al. Re-evaluating transitional neonatal hypoglycemia : mechanism and implications for management. J Pediatr 2015;166: e1. 3. Morris AAM; Thekekara A; Wilks Z; Clayton PT; Leonard JV; Aynsley-Green A; Evaluation of fasts for investigating hypoglycaemia or suspected metabolic disease. Archives of Disease in Childhood. 1996;75(2): Cornblath M, Hawdon JM, Williams AF, et al. Controversies regarding definition of neonatal hypoglycemia: suggested operational thresholds. Pediatrics 2000;105: Güemes M, Rahman SA, Hussain K. What is a normal blood glucose? Arch Dis Child Sep doi: /archdischild Hay, W.W., Jr., et al., Knowledge gaps and research needs for understanding and treating neonatal hypoglycemia: workshop report from Eunice Kennedy Shriver National Institute of Child Health and Human Development. J Pediatr, (5): p Lucas, A., R. Morley, and T.J. Cole, Adverse neurodevelopmental outcome of moderate neonatal hypoglycaemia. BMJ, (6659): p McKinlay, C.J., et al., Neonatal Glycemia and Neurodevelopmental Outcomes at 2 Years. N Engl J Med, (16): p Saudubray JM, De Lonlay P, Touati G, et al. Genetic hypoglycaemia in infancy and childhood: pathophysiology and diagnosis. J Inherit Metab Dis 2000;23: Sprague JE, Arbelaez AM. Glucose counterregulatory responses to hypoglycemia. Pediatr Endocrinol Rev 2011;9:463 73; quiz Title: Hypoglycaemia in Infants & Children Page 9 of 15
10 11. Cryer PE. Hypoglycemia, functional brain failure, and brain death. J Clin Invest 2007;117: National Metabolic Biochemistry Network. Best Practice Guidelines for the Investigation of Hypoglycaemia in Children metbioguidelines. 13. Wong CP; Forsyth RJ; Kelly TP; Eyre JA: Incidence, aetiology and outcome of nontraumatic coma: a population based study. Archives of Disease of Childhood. 2001;84(3): Bonham JR. Investigation of hypoglycaemia in childhood. Ann Clin Biochem 1993;30: Aynsley-Green A. Glucose, the brain and the paediatric endocrinologist. Hormone Res 1996;46: Glycaemic emergencies. BNF June Hypoglycaemia of the newborn. Review of the literature. WHO Huidekoper H, Duran M, Turkenburg M, et al. Fasting adaptation in idiopathic ketotic hypoglycemia: a mismatch between glucose production and demand. Eur J Pediatr 2008;167: Lang TF, Hussain K. Chapter six Pediatric hypoglycemia. In: Gregory SM, ed. Advances in clinical chemistry. Elsevier, 2014: Bodamer OA, Hussein K, Morris AA, et al. Glucose and leucine kinetics in idiopathic ketotic hypoglycaemia. Arch Dis Child 2006; 91: Key Words Hypoglycaemia, Glucose, Ketotic Guideline Lead (Name and Title) J Greening - Cons Paediatrician CONTACT AND REVIEW DETAILS Executive Lead Ruth Radcliffe Details of Changes made during review: Page 3 Flow chart Added ref to contact details of specialist teams on page 3 above flow chart Changed preparations of oral glucose sources Added age range to weight range when assessing for IM glucagon Added preference to use blue cannula for access Added age range to weight range for IV glucose/im glucagon page 6 Appendix 2: advice change - point 3 (0.5 mg in <8 yrs or <25 Kg; and 1 mg in >8 yrs or >25 Kg) point 5 (e.g. chlorothiazide 7-10 mg/kg/day, divided into 12-hourly doses) Appendix 1: Algorithm and causes of hypoglycaemia in childhood. Table 1: Causes of hypoglycaemia. Table 2: Dextrose solutions: Conversion from ml/kg/day to mg/kg/min of dextrose Table 3: Making up dextrose solutions of higher concentrations Appendix 2: Protocol for management of hyperinsulinaemic Hypoglycaemia in Neonates Appendix 3: Emergency glucose polymer regimen for metabolic disorders in childhood. Title: Hypoglycaemia in Infants & Children Page 10 of 15
11 Appendix 1. Algorithm and causes of hypoglycaemia in childhood. Blood Ketones +>0.5mmol/L Ketones (-ve) <0.5mmol/L Title: Hypoglycaemia in Infants & Children Page 11 of 15
12 TABLE 1: CAUSES OF HYPOGLYCAEMIA. Hyperinsulinism Transient: Infant of diabetic mother, perinatal asphyxia, rhesus disease, intra-uterine growth retardation, Beckwith-Wiedemann syndrome, idiopathic. Congenital Hyperinsulinism due to gene mutations. Carbohydrate deficient glycoprotein syndrome (CDG). Defects in the metabolism of fatty acids (SCHAD). Hormonal deficiency Cortisol, growth hormone, ACTH, glucagon, adrenaline rarely hyothyroidism. Defects in hepatic glycogen release/storage Glycogen storage diseases: Glucose-6-phosphatase, Amylo-1,6-glucosidase deficiency, Liver phosphorylase deficiency. Hepatic glycogen synthase deficiency. Defects in gluconeogenesis Fructose-1,6-bisphosphatase deficiency, phosphoenolpyruvate carboxykinase (PEPCK) deficiency. Defects of fatty acid oxidation Medium Chain Acyl-CoA Dehydrogenase Deficiency. Long Chain Acyl-CoA Dehydrogenase Deficiency (+ VLCAD). Short Chain Acyl-CoA Dehydrogenase Deficiency. Multiple Acyl CoA Dehydrogenase deficiency (MADD) Carnitine deficiency (primary and secondary). Carnitine palmitoyl transferase deficiency (CPT 1 and 2). Defects in ketone body synthesis or utilization HMG CoA synthase deficiency, HMG CoA lyase deficiency, beta-ketothilase defeciency Metabolic conditions (relatively common ones) Organic acidaemias (Propionic, Methylmalonic). Maple syrup urine disease, galactosaemia, fructosaemia, tyrosinaemia. Glutaric aciduria type 2. Defects in glucose transport Defects of transporters GLUT2 Drug induced Sulphonylurea, Insulin, Beta-blocker, Salicylates. Miscellaneous causes (mechanism not clear) Ketotic hypoglycaemia (the commonest cause of hypoglycaemia). Infections (sepsis, malaria), congenital heart disease. Title: Hypoglycaemia in Infants & Children Page 12 of 15
13 Appendix 2: Protocol for management of hyperinsulinaemic hypoglycaemia in neonates MANAGEMENT IN THIS GROUP OF PATIENTS MUST BE DISCUSSED WITH THE ON- CALL ENDOCRINE CONSULTANT VIA SWITCHBOARD. Blood samples are taken at the time of hypoglycaemia (blood glucose < 2.6 mmol/l). Perform the hypoglycaemia screen as suggested in the protocol for the Investigation of hypoglycaemia. Management 1. Give 2 ml/kg of 10% glucose as a slow IV injection, and then continue with a 10% glucose infusion at a rate of 6 to 8 mg/kg/minute (i.e. 3.6 ml/kg/hour of 10% glucose). NB: A large bolus of glucose should not be given, as this will cause unnecessary hyperglycaemia and may provoke further (i.e. reactive) hypoglycaemia. 2. Monitor blood glucose with regular BG stix, initially frequently to establish a plateau and then at 1 2-hourly intervals, aiming to maintain the blood glucose level at 3 4 mmol/l. 3. If venous access is difficult, glucagon (0.5 mg in <8 yrs or <25 Kg; and 1 mg in >8 yrs or >25 Kg) by intramuscular injection can be given. An exaggerated hyperglycaemic response is consistent with a diagnosis of hyperinsulinism. The effect is usually transient. 4. If blood glucose concentrations drop to < 3.5 mmol/l, then the glucose infusion rate should be increased (often mg/kg/minute). If the glucose requirement is > 12 mg/kg/minute, consider starting a glucagon infusion (to discuss with the on-call paediatric endocrine consultant) 5. Consider starting therapy with diazoxide 5 20 mg/kg/day (start at the low end of the range), covered with a diuretic (e.g. chlorothiazide 7-10 mg/kg/day, divided into 12-hourly doses), if hyperinsulinism is confirmed. Chlorothiazide therapy is used to cover any fluid retention that may occur with diazoxide, and also because there is a synergistic effect between diazoxide and chlorothiazide. 6. Monitor U&Es carefully, and start potassium replacement as necessary. 7. Stop bolus feeding as it is a stimulus to insulin secretion and will exacerbate the hypoglycaemia. 8. If the patient requires high glucose infusion rates to maintain normoglycaemia, the diazoxide dose should be increased to 15 mg/kg/day with maximum doses of thiazide diuretic. Alternatively, the patient may be given octreotide 10 micrograms/kg/day and glucagon 5 microgram/kg/hour as a continuous infusion. (to discuss with the on-call paediatric endocrine consultant). 9. Venous access may become a problem, and insertion of a long line should be considered at an early stage. 10. If the child shows no signs of improvement, and is requiring maximal therapy, then the child needs to be referred to NORCHI centre at Manchester/ HI service at Great Ormond street London for further management. Title: Hypoglycaemia in Infants & Children Page 13 of 15
14 11. May need fast provocation test, adequate blood glucose monitoring training for family and emergency hypoglycaemia correction kit/ open access letter prior to discharge. Contact endocrine team early for advise at least hours prior to planned fast provocation test. 12. Summary of drug dosage used in hyperinsulinism: Drug Diazoxide Chlorothiazide Octreotide Lanreotide Sirolimus Glucagon infusion Dose Total daily dose up to 5-15 mg/kg/day in 3 divided doses, in combination with a thiazide diuretic. ( start at 5mg/kg/day) Total daily dose up to 7-10 mg/kg/day in 2 divided doses. 10 micrograms/kg/day as a continuous iv or s/c infusion. Or s/c QDS dose Dosage in discussion with endocrinologist in conjunction with GOSH or Manchester NORCHI service Dosage in discussion with endocrinologist in conjunction with GOSH or Manchester NORCHI service 5 microgram/kg/hour to max 10mcg/kg/hr by iv infusion. TABLE 2: Dextrose solutions: Conversion from ml/kg/day (dextrose solutions of different concentrations) to mg/kg/minute of dextrose Daily fluid intake (ml/kg/d) 10% Dextrose 12.5% Dextrose 15% Dextrose 17.5% Dextrose 20% Dextrose 22.5% Dextrose 25% Dextrose mg/kg/min mg/kg/min mg/kg/min mg/kg/min mg/kg/min mg/kg/min mg/kg/min TABLE 3: Making up dextrose solutions of different concentrations Final dextrose concentration required Volume of 50% Dextrose Volume of 10% Dextrose Total volume of final solution 12.5% ml ml 500 ml 15% 62.5 ml ml 500 ml 17.5% ml ml 500 ml 20% 125 ml 375 ml 500 ml 22.5% ml ml 500 ml 25% ml ml 500 ml Title: Hypoglycaemia in Infants & Children Page 14 of 15
15 Appendix 3: Emergency feed regimen Age up to 1 year; Regimen recipes 10% CHO solution; Provides 40kcals/100ml Age upto 2 year, Regimen recipes 15% CHO solution ; Provides 60kcals/100ml Title: Hypoglycaemia in Infants & Children Page 15 of 15
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
Staff at the Nottingham Children s Hospital. Guidelines process; paediatric endocrinology team
 Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
CARE OF THE NEWBORN HYPOGLYCAEMIA
 CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
Neonatal Hypoglycaemia
 Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359
 Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
Learning Objectives. At the conclusion of this module, participants should be better able to:
 Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number:
 This is an official Northern Trust policy and should not be edited in any way Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number: NHSCT/10/293 Target audience: Midwifery,
This is an official Northern Trust policy and should not be edited in any way Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number: NHSCT/10/293 Target audience: Midwifery,
Guidelines for the Prevention and Management of Hypoglycaemia
 ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
Neonatal Hypoglycaemia Guidelines
 N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
Neonatal Hypoglycemia
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Hyperglycaemia. Clinical presentation. Definition of hyperglycaemia. Approach to the problem
 Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Deb Cobie Judy Evans Professionally Approved By Dr Saravanan Consultant Lead for Risk Management June 2009
 TREATMENT OF NEONATAL HYPOGLYCAEMIA Developed in response to: Contributes to CQC Standards No CLINICAL GUIDELINES Register No: 04219 Status: Public Intrapartum NICE Guidelines RCOG guideline C5a Consulted
TREATMENT OF NEONATAL HYPOGLYCAEMIA Developed in response to: Contributes to CQC Standards No CLINICAL GUIDELINES Register No: 04219 Status: Public Intrapartum NICE Guidelines RCOG guideline C5a Consulted
Clinical Director for Women s and Children s Directorate
 TREATMENT OF NEONATAL HYPOGLYCAEMIA IN THE HIGH RISK INFANT CLINICAL GUIDELINES Register No: 12025 Status: Public Developed in response to: Intrapartum NICE Guidelines RCOG guideline Contributes to CQC
TREATMENT OF NEONATAL HYPOGLYCAEMIA IN THE HIGH RISK INFANT CLINICAL GUIDELINES Register No: 12025 Status: Public Developed in response to: Intrapartum NICE Guidelines RCOG guideline Contributes to CQC
Hypoglycemia in congenital hyperinsulinism
 How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA
 NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
Nottingham Neonatal Service Guideline
 Title: Screening and Management of Neonatal Hypoglycaemia Version: 10 Ratification Date: Review Date: Jan 2023 Approval: Nottingham Neonatal Service Clinical Guideline Meeting Author: Shalini Ojha 1, Lara
Title: Screening and Management of Neonatal Hypoglycaemia Version: 10 Ratification Date: Review Date: Jan 2023 Approval: Nottingham Neonatal Service Clinical Guideline Meeting Author: Shalini Ojha 1, Lara
Controversies in Neonatal Hypoglycemia PAC / LAC CONFERENCE, JUNE 1 ST 2017
 Controversies in Neonatal Hypoglycemia PRIYA JEGATHEESAN, MD PAC / LAC CONFERENCE, JUNE 1 ST 2017 Disclosure I have no conflicts of interest to disclose Objectives Review Recommendations from different
Controversies in Neonatal Hypoglycemia PRIYA JEGATHEESAN, MD PAC / LAC CONFERENCE, JUNE 1 ST 2017 Disclosure I have no conflicts of interest to disclose Objectives Review Recommendations from different
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری
 بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
Prevention and Management of Hypoglycaemia
 Prevention and Management of Hypoglycaemia Use for ALL babies on the Labour Ward, Postnatal Ward & Transitional Care. This guideline is based on the BAPM Hypoglycaemia Guideline 2017. This guideline should
Prevention and Management of Hypoglycaemia Use for ALL babies on the Labour Ward, Postnatal Ward & Transitional Care. This guideline is based on the BAPM Hypoglycaemia Guideline 2017. This guideline should
PRACTICE GUIDELINES WOMEN S HEALTH PROGRAM
 C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
Hypoglycaemia (low blood sugar) & ketotic hypoglycaemia
 Information for parents and carers Hypoglycaemia (low blood sugar) & ketotic hypoglycaemia What is hypoglycaemia? Hypoglycemia is having a blood glucose (also known as blood sugar) level that is too low
Information for parents and carers Hypoglycaemia (low blood sugar) & ketotic hypoglycaemia What is hypoglycaemia? Hypoglycemia is having a blood glucose (also known as blood sugar) level that is too low
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE 1.0 PURPOSE AND INTENT Title: Approval Date: March 2016 Approved by: Neonatal Patient Care Teams, HSC & SBH Women s Health Maternal Newborn Committee Child Health Standards
NEONATAL CLINICAL PRACTICE GUIDELINE 1.0 PURPOSE AND INTENT Title: Approval Date: March 2016 Approved by: Neonatal Patient Care Teams, HSC & SBH Women s Health Maternal Newborn Committee Child Health Standards
W1A- Cases I Learned From
 W1A- Cases I Learned From David H Adamkin, MD Professor of Pediatrics Director, Division of Neonatology Director of Nutritional Research Rounsavall Chair of Neonatal Medicine Co-Director of Neonatal Fellowship
W1A- Cases I Learned From David H Adamkin, MD Professor of Pediatrics Director, Division of Neonatology Director of Nutritional Research Rounsavall Chair of Neonatal Medicine Co-Director of Neonatal Fellowship
Overview. o Limitations o Normal regulation of blood glucose o Definition o Symptoms o Clinical forms o Pathophysiology o Treatment.
 Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
HYPOGLYCAEMIA OF THE NEWBORN ON BIRTHING SUITE AND POSTNATAL WARD
 HYPOGLYCAEMIA OF THE NEWBORN ON BIRTHING SUITE AND POSTNATAL WARD INTRODUCTION Healthy term infants are able to mobilise energy stores through a process known as counter regulation and are unlikely to
HYPOGLYCAEMIA OF THE NEWBORN ON BIRTHING SUITE AND POSTNATAL WARD INTRODUCTION Healthy term infants are able to mobilise energy stores through a process known as counter regulation and are unlikely to
Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules)
 Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules) SETTING FOR STAFF PATIENTS Medical and nursing staff Children and young
Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules) SETTING FOR STAFF PATIENTS Medical and nursing staff Children and young
Diabetes Emergency Caesarean section or other unplanned surgery (GL822)
 Diabetes Emergency Caesarean section or other unplanned surgery (GL822) i.e. insulin dependent diabetic having unplanned surgery e.g. a diabetic woman with pre-labour SROM prior to elective Caesarean section.
Diabetes Emergency Caesarean section or other unplanned surgery (GL822) i.e. insulin dependent diabetic having unplanned surgery e.g. a diabetic woman with pre-labour SROM prior to elective Caesarean section.
Paediatric Hypoglycaemia and the Laboratory. AACB Webinar, 8 th April 2015 Tina Yen
 Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Newborn Hypoglycemia
 Newborn Hypoglycemia Self Learning Module Developed by the Interprofessional Education and Research Committee of the Champlain Maternal Newborn Regional Program (CMNRP) 2013 TABLE OF CONTENTS Definition....3
Newborn Hypoglycemia Self Learning Module Developed by the Interprofessional Education and Research Committee of the Champlain Maternal Newborn Regional Program (CMNRP) 2013 TABLE OF CONTENTS Definition....3
Pathway for Adult Patients with Diabetes attending the Emergency Department (ED) with Hypoglycaemia
 Leicestershirediabetes Guidelines Pathway for Adult Patients with Diabetes attending the Emergency Department (ED) with Hypoglycaemia Patient attends ED Support available from Diabetes Specialist Nurses
Leicestershirediabetes Guidelines Pathway for Adult Patients with Diabetes attending the Emergency Department (ED) with Hypoglycaemia Patient attends ED Support available from Diabetes Specialist Nurses
Diabetes Labour guideline (GL820)
 Diabetes Labour guideline (GL820) Approval Approval Group Job Title, Chair of Committee Date Maternity & Childrens Services Mr Mark Selinger, Consultant 6 th June 2014 Clinical Governance Committee Obstetrician
Diabetes Labour guideline (GL820) Approval Approval Group Job Title, Chair of Committee Date Maternity & Childrens Services Mr Mark Selinger, Consultant 6 th June 2014 Clinical Governance Committee Obstetrician
Clinical Guideline. SPEG MCN Protocols Sub Group SPEG Steering Group
 Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
INTRAVENOUS FLUID THERAPY
 INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
Objectives. Why is blood glucose important? Hypoglycaemia. Hyperglycaemia. Acute Diabetes Emergencies (DKA,HONK)
 Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow June 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood Glucose
Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow June 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood Glucose
Neonatal Hypoglycemia. Presented By : Kamlah Olaimat 25\7\2010
 Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Objectives. Why is blood glucose important? Hypoglycaemia. Hyperglycaemia. Acute Diabetes Emergencies (DKA,HONK)
 Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow September 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood
Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow September 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Management of Glucose in the Preterm Infant. Charles A. Stanley, MD Division of Endocrinology Children s Hospital of Philadelphia
 Management of Glucose in the Preterm Infant Charles A. Stanley, MD Division of Endocrinology Children s Hospital of Philadelphia Disclosures Charles Stanley, MD I have no relevant financial relationships
Management of Glucose in the Preterm Infant Charles A. Stanley, MD Division of Endocrinology Children s Hospital of Philadelphia Disclosures Charles Stanley, MD I have no relevant financial relationships
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Staff at the Nottingham Children s Hospital. Guidelines process.
 Diabetes and Surgery Title of Guideline Contact Name and Job Title (author) Guideline for the management of children and young people with diabetes aged 18 or under requiring surgery Dr Priyha Santhanam,
Diabetes and Surgery Title of Guideline Contact Name and Job Title (author) Guideline for the management of children and young people with diabetes aged 18 or under requiring surgery Dr Priyha Santhanam,
INTRAVENOUS FLUIDS PRINCIPLES
 INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
All Wales Paediatric Steroid Replacement Therapy Card
 All Wales Paediatric Steroid Replacement Therapy Card All Wales Paediatric Steroid Replacement Therapy Card 1.0 BACKGROUND Patients that require long-term steroid replacement therapy for adrenal suppression
All Wales Paediatric Steroid Replacement Therapy Card All Wales Paediatric Steroid Replacement Therapy Card 1.0 BACKGROUND Patients that require long-term steroid replacement therapy for adrenal suppression
LRI Children s Hospital
 LRI Children s Hospital Management of Children on Ketogenic Diet for Epilepsy Staff relevant to: Health professionals caring for children with epilepsy being managed on a ketogenic diet. Team approval
LRI Children s Hospital Management of Children on Ketogenic Diet for Epilepsy Staff relevant to: Health professionals caring for children with epilepsy being managed on a ketogenic diet. Team approval
7/11/2018. Oral Dextrose Gel Treatment for Newborns with Hypoglycemia Reduces NICU Admissions DISCLOSURE. Objectives
 Gaps in Knowledge, Competence, Performance, or Patient Outcomes DISCLOSURE The content of this presentation does not relate to any product of a commercial entity; therefore, I have no relationships to
Gaps in Knowledge, Competence, Performance, or Patient Outcomes DISCLOSURE The content of this presentation does not relate to any product of a commercial entity; therefore, I have no relationships to
Not Your Typical Case of Ketotic Hypoglycemia
 Not Your Typical Case of Ketotic Hypoglycemia Linda Steinkrauss, RN, MSN, CPNP Objectives By the end of this session, attendees should be able to: 1. Discuss the difference between idiopathic ketotic hypoglycemia
Not Your Typical Case of Ketotic Hypoglycemia Linda Steinkrauss, RN, MSN, CPNP Objectives By the end of this session, attendees should be able to: 1. Discuss the difference between idiopathic ketotic hypoglycemia
GUIDELINE FOR THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS WITH DIABETES MELLITUS
 GUIDELINE FOR THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS WITH DIABETES MELLITUS Guideline author Accountable Executive Lead Approving body Policy reference Diabetes Specialist Nurse Consultant Diabetologist
GUIDELINE FOR THE MANAGEMENT OF HYPOGLYCAEMIA IN ADULTS WITH DIABETES MELLITUS Guideline author Accountable Executive Lead Approving body Policy reference Diabetes Specialist Nurse Consultant Diabetologist
HYPOGLYCAEMIA OF THE NEWBORN
 HYPOGLYCAEMIA OF THE NEWBORN INTRODUCTION Healthy term infants are able to mobilise energy stores through a process known as counter regulation and are unlikely to suffer any ill effects if fed on demand
HYPOGLYCAEMIA OF THE NEWBORN INTRODUCTION Healthy term infants are able to mobilise energy stores through a process known as counter regulation and are unlikely to suffer any ill effects if fed on demand
Lynda Astbury Lead Diabetes Specialist Nurse
 Lynda Astbury Lead Diabetes Specialist Nurse WARNING SIGNS AND SYMPTOMS Is patient Feeling unwell? Blood glucose level above 13mmol/L Or higher than the patients day to day readings (even if not eating)
Lynda Astbury Lead Diabetes Specialist Nurse WARNING SIGNS AND SYMPTOMS Is patient Feeling unwell? Blood glucose level above 13mmol/L Or higher than the patients day to day readings (even if not eating)
Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick Neonatal Pharmacist
 CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Hypoglycaemia. Parent Information Leaflet
 Hypoglycaemia Parent Information Leaflet July 2017 Definition Hypoglycaemia (hypo) in children with diabetes is a blood glucose of less than 4.0mmol/L. The first time your child has a hypo will be an anxious
Hypoglycaemia Parent Information Leaflet July 2017 Definition Hypoglycaemia (hypo) in children with diabetes is a blood glucose of less than 4.0mmol/L. The first time your child has a hypo will be an anxious
Four is the Floor Symptoms can be felt at higher levels if control is poor Worth confirmation using BG meter if at all possible
 Sandra Coats Diabetes Specialist Nurse 1 Hypoglycaemia Hyperglycaemia Diabetes and Illness sick day Diabetic Ketoacidosis HONK/HHS 2 What is Hypoglycaemia BG levels below 4mmol/l. Four is the Floor Floor
Sandra Coats Diabetes Specialist Nurse 1 Hypoglycaemia Hyperglycaemia Diabetes and Illness sick day Diabetic Ketoacidosis HONK/HHS 2 What is Hypoglycaemia BG levels below 4mmol/l. Four is the Floor Floor
Hypoglyceamia and Exercise
 Hypoglyceamia and Exercise Noreen Barker Diabetes Specialist Nurse May 2016 Hypoglyceamia What is a hypo? Why are we concerned? Signs and symptoms Treatments Causes Hypo unawareness Managing diabetes and
Hypoglyceamia and Exercise Noreen Barker Diabetes Specialist Nurse May 2016 Hypoglyceamia What is a hypo? Why are we concerned? Signs and symptoms Treatments Causes Hypo unawareness Managing diabetes and
PHARMACOLOGY AND PHARMACOKINETICS
 DRUG GUIDELINE Insulin, human neutral (Actrapid ) Intravenous Infusion for SCOPE (Area): FOR USE IN: Critical Care Unit, Emergency Department and Operating Suite EXCLUSIONS: Paediatrics (seek Paediatrician
DRUG GUIDELINE Insulin, human neutral (Actrapid ) Intravenous Infusion for SCOPE (Area): FOR USE IN: Critical Care Unit, Emergency Department and Operating Suite EXCLUSIONS: Paediatrics (seek Paediatrician
Neurodevelopmental Risk?
 Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Hypoglycaemic disorders
 Hypoglycaemic disorders 1. Hypoglycaemia in patients with diabetes mellitus 2. Hypoglycaemia in non-diabetic patients 3. Clinical, laboratory and imaging diagnosis 4. Case report 5. GLP-1 receptor scintigraphy
Hypoglycaemic disorders 1. Hypoglycaemia in patients with diabetes mellitus 2. Hypoglycaemia in non-diabetic patients 3. Clinical, laboratory and imaging diagnosis 4. Case report 5. GLP-1 receptor scintigraphy
Information for health professionals
 Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
4/23/2015. Linda Steinkrauss, MSN, PNP. No conflicts of interest
 Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
Title Hypoglycaemia Management and Prevention in Neonates Guideline. Author s job title Senior Neonatal Staff Nurse and Educator Directorate Medical
 Document Control Title in Neonates Guideline Author Author s job title Senior Neonatal Staff Nurse and Educator Directorate Medical Department SCU Version Date Issued Status Comment / Changes / Approval
Document Control Title in Neonates Guideline Author Author s job title Senior Neonatal Staff Nurse and Educator Directorate Medical Department SCU Version Date Issued Status Comment / Changes / Approval
PES Recommendations for Evaluation and Management of Hypoglycemia in Neonates, Infants, and Children Paul S. Thornton On behalf of the Team
 Cook Children s 1 PES Recommendations for Evaluation and Management of Hypoglycemia in Neonates, Infants, and Children Paul S. Thornton On behalf of the Team Cook Children s 2 Co-Chair: Charles Stanley
Cook Children s 1 PES Recommendations for Evaluation and Management of Hypoglycemia in Neonates, Infants, and Children Paul S. Thornton On behalf of the Team Cook Children s 2 Co-Chair: Charles Stanley
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Patient Demographics 5/12/2016
 Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
Joint Trust Guideline for 72 hour fast for investigation of spontaneous hypoglycaemia in adults For use in:
 For use in: Cringleford & Langley Wards & Clinical Investigation Unit By: Registered nurses and medical staff on Cringleford & Langley Wards For: Adult patients suspected of having spontaneous hypoglycaemia
For use in: Cringleford & Langley Wards & Clinical Investigation Unit By: Registered nurses and medical staff on Cringleford & Langley Wards For: Adult patients suspected of having spontaneous hypoglycaemia
Hypoglycemia. When recognized early, hypoglycemia can be treated successfully.
 Hypoglycemia Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized early, hypoglycemia
Hypoglycemia Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized early, hypoglycemia
Use this version only
 Integrated Care Pathway PAEDIATRIC DIABETIC KETOACIDOSIS (DKA) Use this version only Patient Label Details Ward: Consultant: Named Nurse: Date of Admission: Date of Discharge/Transfer: ALL STAFF TO WRITE
Integrated Care Pathway PAEDIATRIC DIABETIC KETOACIDOSIS (DKA) Use this version only Patient Label Details Ward: Consultant: Named Nurse: Date of Admission: Date of Discharge/Transfer: ALL STAFF TO WRITE
ASY-805.1: Insulin Tolerance Test. ASY-805.2: Associated Documents. ASY-805.3: Distribution of Documents. ASY-805.4: Review of Document: a b
 ASY-805.1: Insulin Tolerance Test ASY-805.2: Associated Documents a b Handbook page task print-out ASY-805.3: Distribution of Documents Copy No Number Location 1 Quality Centre 2 3.1 W232 3 3.20 W232 Laminated
ASY-805.1: Insulin Tolerance Test ASY-805.2: Associated Documents a b Handbook page task print-out ASY-805.3: Distribution of Documents Copy No Number Location 1 Quality Centre 2 3.1 W232 3 3.20 W232 Laminated
In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus
 In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus This procedural document supersedes any previous guidelines in relation to this subject: PAT/T 49 v.2 In Hospital Management of
In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus This procedural document supersedes any previous guidelines in relation to this subject: PAT/T 49 v.2 In Hospital Management of
Insulin Tolerance Test Protocol - RNS Endocrinology
 Page 1 of 7 - RNS Endocrinology Test name Insulin tolerance test. Alternate test names. Related Tests. Indication(s) Investigation of the hypothalamic pituitary axis (HPA) with regard to the release of
Page 1 of 7 - RNS Endocrinology Test name Insulin tolerance test. Alternate test names. Related Tests. Indication(s) Investigation of the hypothalamic pituitary axis (HPA) with regard to the release of
Managing Hyperglycaemia in Acute (Adult) Inpatients Requiring Enteral Feeding Guidelines
 Document Control Title Managing Hyperglycaemia in Acute (Adult) Inpatients Requiring Author Author s job title Specialist Nurse Consultant Physician Department Directorate Unscheduled Care Version Date
Document Control Title Managing Hyperglycaemia in Acute (Adult) Inpatients Requiring Author Author s job title Specialist Nurse Consultant Physician Department Directorate Unscheduled Care Version Date
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
MSUD Dietetic Management Pathway
 MSUD Dietetic Management Pathway Presumptive positive screen for MSUD (symptomatic infant) Refer to Clinical Management Guidelines and Initial Clinical Referral Guidelines and Standards (www.bimdg.org)
MSUD Dietetic Management Pathway Presumptive positive screen for MSUD (symptomatic infant) Refer to Clinical Management Guidelines and Initial Clinical Referral Guidelines and Standards (www.bimdg.org)
Glutaric aciduria type 1 (GA1) Dietetic Management Pathway
 Glutaric aciduria type 1 (GA1) Dietetic Management Pathway Presumptive positive screen for GA1 See Clinical Management Guidelines and Clinical Referral Guidelines and Standards (www.bimdg.org) Unwell baby:
Glutaric aciduria type 1 (GA1) Dietetic Management Pathway Presumptive positive screen for GA1 See Clinical Management Guidelines and Clinical Referral Guidelines and Standards (www.bimdg.org) Unwell baby:
Clinical Guidance. Management of hypoglycaemia in paediatric diabetes
 Clinical Guidance Management of hypoglycaemia in paediatric diabetes Summary This guidance is for the use of nurses and doctors management of children with diabetes suffering an episode of hypoglycaemia
Clinical Guidance Management of hypoglycaemia in paediatric diabetes Summary This guidance is for the use of nurses and doctors management of children with diabetes suffering an episode of hypoglycaemia
Case 1. Managing Neonatal Hypoglycemia: Can formula supplementation be avoided? Faculty Financial Disclosures 3/8/2018
 Managing Neonatal Hypoglycemia: Can formula supplementation be avoided? Shawnte R. James, MD, FAAP Assistant Professor Newborn Medicine Hospitalist Emory University School of Medicine Department of Pediatrics
Managing Neonatal Hypoglycemia: Can formula supplementation be avoided? Shawnte R. James, MD, FAAP Assistant Professor Newborn Medicine Hospitalist Emory University School of Medicine Department of Pediatrics
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Blood Glucose Monitoring
 Blood Glucose Monitoring What is Glucose? A simple sugar that enters the diet as part of sucrose, lactose, or maltose Part of a polysaccharide called dietary starch Most of the body s energy comes from
Blood Glucose Monitoring What is Glucose? A simple sugar that enters the diet as part of sucrose, lactose, or maltose Part of a polysaccharide called dietary starch Most of the body s energy comes from
Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI)
 Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI) Dr Pratik Shah Clinical Research fellow in Hyperinsulinism Clinical Molecular Genetics Unit Institute of Child
Use of Lanreotide (long acting Somatostatin analogue) in Congenital Hyperinsulinism (CHI) Dr Pratik Shah Clinical Research fellow in Hyperinsulinism Clinical Molecular Genetics Unit Institute of Child
Please inform the Diabetes Nurse Specialist that this patient has been admitted within 24hrs of admission.
 Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation
 CHILDREN S SERVICES Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation Background Surgery places stress on the body and will alter glucose control and insulin
CHILDREN S SERVICES Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation Background Surgery places stress on the body and will alter glucose control and insulin
Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery
 Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery Background Surgery places physical and emotional stress on the body. This, alongside new surroundings, parental anxiety and
Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery Background Surgery places physical and emotional stress on the body. This, alongside new surroundings, parental anxiety and
THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals
 Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
MCADD. MEDIUM CHAIN ACYL CoA DEHYDROGENASE DEFICIENCY. Dietary management guidelines for dietitians
 MCADD MEDIUM CHAIN ACYL CoA DEHYDROGENASE DEFICIENCY Dietary management guidelines for dietitians AUTHOR Marjorie Dixon Principal Paediatric Dietitian, Great Ormond Street Hospital for Children, NHS Trust,
MCADD MEDIUM CHAIN ACYL CoA DEHYDROGENASE DEFICIENCY Dietary management guidelines for dietitians AUTHOR Marjorie Dixon Principal Paediatric Dietitian, Great Ormond Street Hospital for Children, NHS Trust,
Linda Boyajian, RN, MSN, CRNP Congenital Hyperinsulinism Center Children s Hospital of Philadelphia
 Linda Boyajian, RN, MSN, CRNP Congenital Hyperinsulinism Center Children s Hospital of Philadelphia Congenital Hyperinsulinism refers to a variety of congenital disorders in which hypoglycemia is caused
Linda Boyajian, RN, MSN, CRNP Congenital Hyperinsulinism Center Children s Hospital of Philadelphia Congenital Hyperinsulinism refers to a variety of congenital disorders in which hypoglycemia is caused
Paediatric Directorate
 Paediatric Directorate Dehydration Guidelines Primary cause of dehydration diarrhoea +/- vomiting. Approximately 10%Children < 5yrs present with gastroenteritis each year Diagnosis History - sudden change
Paediatric Directorate Dehydration Guidelines Primary cause of dehydration diarrhoea +/- vomiting. Approximately 10%Children < 5yrs present with gastroenteritis each year Diagnosis History - sudden change
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
Positive Newborn Screens: What do you do next?
 Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Inborn Errors of Metabolism (IEM)
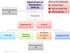 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
For The Management Of. Hypoglycemia
 Guidelines For The Management Of Hypoglycemia By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council For
Guidelines For The Management Of Hypoglycemia By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council For
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE 1.0 PURPOSE AND INTENT Title: Approval Date: March 2016, Last Revised July 2018 Approved by: Neonatal Patient Care Teams, HSC & SBH Women s Health Maternal Newborn
NEONATAL CLINICAL PRACTICE GUIDELINE 1.0 PURPOSE AND INTENT Title: Approval Date: March 2016, Last Revised July 2018 Approved by: Neonatal Patient Care Teams, HSC & SBH Women s Health Maternal Newborn
