Hepatic Progenitor Cells Activation, Fibrosis, and Adipokines Production in Pediatric Nonalcoholic Fatty Liver Disease
|
|
|
- Jemima Higgins
- 5 years ago
- Views:
Transcription
1 STEATOHEPATITIS/METABOLIC LIVER DISEASE Hepatic Progenitor Cells Activation, Fibrosis, and Adipokines Production in Pediatric Nonalcoholic Fatty Liver Disease Valerio Nobili, 1 * Guido Carpino, 2 * Anna Alisi, 1 Antonio Franchitto, 3,4 Gianfranco Alpini, 5 Rita De Vito, 6 Paolo Onori, 7 Domenico Alvaro, 4,8 and Eugenio Gaudio 3 Hepatic progenitor cells (HPCs) play a major role in liver repair and regeneration. We evaluated HPC involvement in pediatric nonalcoholic fatty liver disease (pnafld). Thirty biopsies of consecutive children and adolescents with untreated NAFLD (19 with nonalcoholic steatohepatitis [NASH] and 11 without NASH) were studied using immunohistochemistry and immunofluorescence. HPCs and HPC-expressing adipokines (e.g., adiponectin, resistin, and glucagon-like peptide 1 [GLP-1]) were counted and correlated with steatosis, inflammation, hepatocyte ballooning, fibrosis, and NAFLD activity score (NAS). The HPC compartment was expanded in pnafld, especially in children with NASH, and was independently associated with degree of fibrosis (r ; P ). NASH livers were also characterized by increased hepatocyte apoptosis, cell-cycle arrest, and an expanded pool of intermediate hepatocytes. Adiponectin expression in HPCs of pnafld patients was down-regulated with respect to the healthy liver, and this expression was inversely correlated with NAS score (r ; P < 0.001) and steatosis (r ; P < 0.001). Resistin expression in HPCs increased in pnafld and was related to degree of fibrosis (r ; P < 0.05). GLP-1 was overexpressed in HPCs of pnafld patients, and GLP-1 expression was related to degree of steatosis (r ; P < 0.05) and NAS (r ; P < 0.01). Conclusions: HPC activation is involved in the response of the liver to oxidative stress in pnafld and is correlated with fibrosis and the progression toward NASH. HPCs express adiponectin, resistin, and GLP-1, which become available to resident liver cells and are strongly associated with the severity of NAFLD. These results may have important pathophysiological implications in the modulation of hepatic insulin resistance and the progression of liver injury. (HEPATOLOGY 2012;56: ) See Editorial on Page 2013 Nonalcoholic fatty liver disease (NAFLD) is one of the most important causes of liverrelated 1 morbidity and mortality in children. 2 Its general prevalence is currently estimated at 3%- 10% in children in westernized countries, but because of its close association with the epidemic of pediatric obesity, this estimate rises to 50%-70% in obese subjects. 3 NAFLD includes a spectrum of diseases ranging from simple fatty liver to nonalcoholic steatohepatitis Abbreviations: Abs, antibodies; ALT, alanine transaminase; AST, aspartate transaminase; BMI, body mass index; CK-7, cytokeratin-7; CRN, NAFLD/NASH Clinical Research Network; DR, ductular reaction; ECs, endothelial cells; GGT, gamma-glutamyl aminotransferase; GLP-1, glucagon-like peptide-1; HOMA-IR, homeostatic model assessment of insulin resistance; HPC, hepatic progenitor cell; HPF, high-power field; HSCs, hepatic stellate cells; IF, immunofluorescence; IHs, intermediate hepatocytes; IHC, immunohistochemistry; IR, insulin resistance; ISI, insulin sensitivity index; Mcp-1, monocyte chemotactic protein-1; NAFLD, nonalcoholic fatty liver disease; NAS: NAFLD activity score; NASH, nonalcoholic steatohepatitis; OGGT, oral glucose tolerance test; pnafld, pediatric nonalcoholic fatty liver disease; RT, room temperature; SEM, standard error of the mean; SH, steatohepatitis; Tg, triglycerides. From the 1 Unit of Liver Research, Bambino Gesù Children s Hospital, Instituto di Ricovero e Cura a Carattere Scientifico (IRCCS), Rome, Italy; 2 Department of Health Sciences, University of Rome Foro Italico, Rome, Italy; 3 Department of Anatomical, Histological, Forensic Medicine, and Orthopedic Sciences, Sapienza University of Rome, Rome, Italy; 4 Eleonora Lorillard Spencer-Cenci Foundation, Rome, Italy; 5 Division of Research, Central Texas Veterans Health Care System, Department of Medicine, Scott & White Digestive Disease Research Center, Scott & White and Texas A&M Health Science Center College of Medicine, Temple, TX; 6 Unit of Pathology, Bambino Gesù Children s Hospital, IRCCS, Rome, Italy; 7 Department of Experimental Medicine, University of L Aquila, L Aquila, Italy; and 8 Department of Sciences and Medical and Surgical Biotechnologies, Sapienza University of Rome, Rome, Italy. Received November 22, 2011; accepted March 19, E.G. was supported by a research project grant from the University Sapienza of Rome (Rome, Italy) (Fondo per gli Investimenti della Ricerca di Base [FIRB] grant no. RBAP10Z7FS_001 and by Research Program for the Development of Research of National Interest [PRIN] grant no. 2009X84L84_001). D.A. was supported by FIRB grant no. RBAP10Z7FS_004 and by PRIN grant no. 2009X84L84_002). *These authors contributed equally to this work. 2142
2 HEPATOLOGY, Vol. 56, No. 6, 2012 NOBILI ET AL (NASH) and may progress to cirrhosis and hepatocellular carcinoma, 1 although this outcome is rare in children. 4 NASH development is characterized by intricate interactions between resident and recruited cells that enable liver-damage progression. The increasing general agreement is that the cross-talk between hepatocytes, hepatic stellate cells (HSCs), and macrophages in NAFLD has a main role in the derangement of lipid homeostasis, insulin resistance (IR), danger recognition, immune-tolerance response, and fibrogenesis. 5 However, much remains unknown about the intraand intercellular mechanisms underlying the progression toward NASH. In NAFLD, hepatic stem/progenitor cells (HPCs) are activated when oxidative stress inhibits the regenerative capacity of mature hepatocytes, supporting the hypothesis that HPC expansion is a component of the adaptive response of the liver to oxidative stress. 6 HPC activation and proliferation determines the appearance of a ductular reaction (DR) that is characterized by tortuous structures with no discernable lumen (i.e., reactive ductules), composed of progenitor cells with highly variable marker profiles. 7-9 Several studies have suggested that DR drives hepatic fibrogenesis during liver injury. 10 In NASH, DR is independently correlated with progressive portal fibrosis, raising the possibility of a second (i.e., periportal) pathway for fibrogenesis that is independent of the deposition of zone 3 subsinusoidal collagen by HSCs. 11 In pediatric NASH, portal fibrosis may represent the predominant form of fibrosis. 12,13 A class of circulating factors named adipokines are involved in the development of NAFLD and its progression to fibrosis. 14 The liver is a source of various adipokines, although the cell types responsible for their production 15,16 and their involvement in NAFLD progression remain to be elucidated. This study aimed to evaluate the activation of the HPC compartment and the expression of adiponectin, resistin, and glucagon-like peptide-1 (GLP-1) by HPCs in patients with pediatric NAFLD (pnafld) and to determine how these parameters correlate with the histological aspects of liver damage. Patients and Methods Patients and Clinical Data. This retrospective study included 30 consecutive untreated children and adolescents (boys, 13; girls, 17; median age, 10.9 years; range, 8-14) with biopsy-proven NAFLD, who were referred to Bambino Gesù Children s Hospital during January 2010-January Secondary causes of steatosis were excluded, including alcohol abuse (140 g/week), total parenteral nutrition, and drugs. Using standard clinical, laboratory, and histological evaluations, hepatitis A, B, and C, cytomegalovirus, Epstein-Barr virus infections, autoimmune liver disease, metabolic liver diseases, Wilson s disease, and alpha-1-antitrypsin deficiency were ruled out. The children included in our analyses showed clinical and pathological features resembling those observed in our general pediatric population with NAFLD. 17 These patients were diagnosed with NAFLD through liver biopsy recommended because of persistently (i.e., 6 months) elevated alanine aminotransferase (ALT) levels and the presence of an echogenic texture of the liver on ultrasonography. Furthermore, the patients received no dietary or other therapeutic treatment regimens before diagnosis. The study protocol conformed to the ethical guidelines of the 1975 Declaration of Helsinki and the recommendations of the local ethics committee. Informed consent was obtained. Weight, height, and body mass index (BMI) were measured. 17 ALT, aspartate aminotransferase (AST), gamma-glutamyl transpeptidase (GGT), total triglycerides (Tg), and total cholesterol were evaluated using standard laboratory methods. Insulin was measured using a radioimmunoassay (Myria Technogenetics, Milan, Italy). Glucose and insulin were measured at 0, 30, 60, 90, and 120 minutes of an oral glucose tolerance test (OGTT) performed with 1.75 g of glucose/ kg of body weight (up to 75 g). Degree of IR and sensitivity was determined by the homeostatic model assessment of insulin resistance (HOMA-IR), and the insulin sensitivity index (ISI) was derived from an OGGT, respectively. 17 Liver Biopsy and Histopathological Analysis. The clinical indication for biopsy was either to assess the presence of NASH and the degree of fibrosis or to Address reprint requests to: Eugenio Gaudio, M.D., Department of Human Anatomy, Histology, Forensic Medicine, and Orthopedics, Sapienza University of Rome, Via Borelli 50, Rome, Italy. eugenio.gaudio@uniroma1.it; fax: þ Copyright VC 2012 by the American Association for the Study of Liver Diseases. View this article online at wileyonlinelibrary.com. DOI /hep Potential conflict of interest: Nothing to report. Additional Supporting Information may be found in the online version of this article.
3 2144 NOBILI ET AL. HEPATOLOGY, December 2012 diagnose other likely independent or competing liver diseases. Liver biopsy was performed after an overnight fast by using an automatic core biopsy 18-gauge needle under general anesthesia and ultrasound guidance. Two biopsy passes within different liver segments were performed for each subject. Liver biopsy specimens were fixed in buffered formalin and embedded in paraffin. Standard histological stains were performed. Steatosis, inflammation, hepatocyte ballooning, and fibrosis were scored using the NAFLD Clinical Research Network (CRN) criteria. 12 Features of steatosis, lobular inflammation, and hepatocyte ballooning were combined to obtain the NAFLD activity score (NAS). As recommended by a recent NASH CRN article, 18 a microscopic diagnosis, based on overall injury pattern (i.e., steatosis, hepatocyte ballooning, and inflammation), as well as the presence of additional lesions (e.g., zonality of lesions, portal inflammation, and fibrosis), has been assigned to each case. 19 Accordingly, biopsies were subdivided into not steatohepatitis (not-sh) and definite steatohepatitis (definite-sh) subcategories. 18 Additional details are described in the Supporting Materials and Methods. Liver specimens from 6 lean, nondiabetic children (boys, 4; girls, 2; median age, 13 years; range, 12-16) without liver disease were used as controls. Control liver fragments were obtained from patients who underwent laparotomy or laparoscopic procedures (for cholecystectomy), from liver donors (orthotopic liver transplantation), or incidental normal liver biopsies (i.e., children exhibiting persistent or intermittent elevations of liver enzymes for >6 months). Histological analysis was performed by a single pathologist blinded to clinical and laboratory data. Immunohistochemistry and Immunofluorescence. For immunohistochemistry (IHC), sections were incubated overnight at 4 C with primary antibodies (Abs) against cytokeratin-7 (CK-7), adiponectin, resistin, GLP-1, p21 waf1, and cleaved caspase-3. A complete list of primary Abs is included in the Supporting Materials and Methods. Samples were then incubated for 20 minutes at room temperature (RT) with secondary biotinylated Ab and, successively, with streptavidin/horseradish peroxidase (LSABþ; code K0690; Dako Cytomation, Glostrup, Denmark). Diaminobenzidine (code K3468, Dako) was used as the substrate, and the sections were counterstained with hematoxylin. For double immunofluorescence (IF) staining, nonspecific protein binding was blocked with 5% normal goat serum. To perform double immunostaining with two mouse primary Abs (CK-7/adiponectin, CK-7/ resistin, and CK-7/GLP-1), we followed a three-step protocol: Sections were incubated with anti-ck-7, an antimouse secondary fluorescent Ab (Alexa Fluor 488; Invitrogen Ltd., Paisley, UK) was applied, and the second primary Ab was prelabeled with a fluorophore by using an APEX-594 labeling Kit (Invitrogen) and was applied to the section. All Abs were diluted (1:50) and incubated at RT for 1 hour. Slides were counterstained with 4,6-diamidino-2-phenylindole. Negative controls (the primary Ab was replaced with preimmune serum) were included for all immunoreactions. Sections were examined with a Leica Microsystems (DM 4500 B; Weltzlar, Germany) microscope equipped with a JenOptik Prog Res C10 Plus Videocam (JenOptik AG, Jena, Germany). Observations were processed with an image analysis system (IAS, Delta Sistemi, Rome, Italy) and were independently performed by two pathologists in a blinded fashion. Only biopsies containing at least five portal spaces were considered. The HPC compartment was evaluated by counting the number of CK-7-positive cells within the bile/reactive ductules by using a previously reported procedure. 7,20 Solitary CK-7-positive HPCs or those in small clumps that were localized in the parenchyma or at the portal interface were included in these counts because they should be considered as a histological sectioning of bile/reactive ductules through a transverse plane without any unique IHC markers to distinguish them from cells within bile/reactive ductules. 8 Cholangiocytes lining the interlobular bile ducts were excluded from the counts. The number of HPCs within the ductular reaction was counted within the entire section and expressed as the number of CK-7- positive cells per high-power field (HPF; at 20). 7 Intermediate hepatocytes (IHs) were defined as cells with sizes between those of hepatocytes and HPCs (<40 but >6 lm in diameter), with faint CK-7 immunoreactivity in the cytoplasm and reinforcement at the plasma membrane. 8 The presence of IHs was scored as reported elsewhere: 0 ¼ no IH; 1 ¼ single occasional IHs; and 2 ¼ clusters of IHs. 20 Apoptosis and cell-cycle arrest were assessed by counting the number of hepatocytes that stained strongly positive for cleaved caspase-3 (at the cytoplasm level) and p21 waf1 (at the nuclear level). The apoptotic and p21 indices were calculated by dividing the average number of positive cells by the average number of hepatocytes and expressing the quotient as a percentage for each section. At least 30 lobular fields at 40 magnification were analyzed (1,000 hepatocytes) for each section. Adiponectin, resistin, and GLP-1 expression by CK- 7-positive HPCs was evaluated in serial sections and
4 HEPATOLOGY, Vol. 56, No. 6, 2012 NOBILI ET AL confirmed with IF. Data were expressed both as number of positive cells per HPF and as a percentage of positive cells. Adipokine expression by hepatocytes was semiquantitatively evaluated and expressed as a percentage of positive cells. Statistical Analysis. Data are indicated as mean 6 standard error of the mean (SEM). The Student s t test or Mann-Whitney s U test was used to determine differences between groups for normally or not normally distributed data, respectively. Similarly, Pearson s correlation coefficient or Spearman s nonparametric correlation was used. The association of independent factors with the degree of fibrosis was evaluated using stepwise multivariate logistic or linear regression analysis. A P value of <0.05 was considered statistically significant. Statistical analyses were performed using SPSS statistical software (SPSS, Inc., Chicago, IL). Results Histological and Clinical Data. The diagnosis of NAFLD was confirmed histopathologically. Eleven subjects (37%) had simple steatosis (i.e., isolated fat deposition in hepatocytes), whereas 19 subjects (63%) exhibited varying degrees of fibrosis and inflammation. NAS scores ranged from 0 to 8. According to the NASH CNR criteria, 12,18 patients were divided into two distinct groups: not-sh (N ¼ 11) and definite- SH or NASH (N ¼ 19). Fibrosis of some degree was observed in 25 biopsy samples (83%): stage 1c in 11 samples (37%), stage 2 in 11 (37%), and stage 3 in 3 (10%). Five biopsy samples (17%) showed no fibrosis. Control biopsy samples had healthy liver histological features. Anthropometric and laboratory data are described in Table 1. These parameters were similar for the two groups. HPCs in pnafld Biopsy Samples. Overall, pnafld biopsy samples showed an expanded HPC population ( CK-7-positive cells per HPF), compared to those of healthy livers ( ; P < 0.01), and were characterized by CK-7-positive reactive ductules at the portal-parenchymal interface (Fig. 1; Table 2). Definite-SH biopsies showed a more extensive expansion of the HPC population ( ), compared to not-sh biopsies ( ; P < 0.05). Values in the latter, however, were higher than those in healthy livers (P < 0.05). In pnafld, HPC number was correlated with steatosis (r ¼ 0.417; P < 0.05) and NAS scores (r ¼ 0.403; P < 0.05), but not with hepatocyte ballooning or lobular inflammation. Table 1. Anthropometric and Laboratory Parameters of the Study Population pnafld pnafld pnafld Mann-Whitney s Whole Sample Not-SH Definite-SH U Test Parameters (N ¼ 30) (N ¼ 11) (N ¼ 19) (P Value) Sex, male/female 13/17 7/4 12/7 Age, years Weight, kg Height, cm BMI, kg/m WC, cm Cholesterol, mg/dl Tg, mg/dl ALT, U/L AST, U/L GGT, U/L Glucose, mg/dl Insulin, lu/ml HOMA-IR ISI Data are reported as median value. Abbreviation: WC, waist circumference. Taking in account the degree of fibrosis (Table 2), we found no difference in the number of HPCs between pnafld biopsies without fibrosis ( ) and healthy livers (P ¼ 0.087). pnafld biopsies with fibrosis displayed a significant HPC compartment expansion ( ), compared to biopsies from healthy controls (P < 0.01) and pnafld biopsies without fibrosis (P < 0.01). In pnafld patients, HPC number was correlated with degree of fibrosis (r ¼ 0.582; P < 0.05; Fig. 2A). The number of HPCs in pnafld showed no significant correlation with insulin serum levels, HOMA- IR, or ISI. Logistic regression analysis revealed that the number of HPCs in pnafld was significantly associated (t ¼ 2.320; P ¼ 0.033) with degree of fibrosis, but not inflammation or NAS scores. No intermediate hepatocytes were found in not-sh biopsies. In contrast, single occasional or clusters of intermediate hepatocytes were present in definite-sh biopsies (Fig. 1C,D). The presence of intermediate hepatocytes in pnafld was correlated with the number of HPCs (r ¼ 0.685; P < 0.001), hepatocyte ballooning (r ¼ 0.534; P < 0.01), and NAS scores (r ¼ 0.428; P < 0.05), but not with fibrosis, steatosis, or inflammation. Evaluation of Hepatocyte Cell-Cycle Arrest and Apoptosis in pnafld Biopsies. The p21 waf1 and apoptotic indices in hepatocytes (Fig. 3) were higher in definite-sh biopsies ( and , respectively) than in not-sh biopsies ( and , respectively; P < 0.05 for both).
5 2146 NOBILI ET AL. HEPATOLOGY, December 2012 Fig. 1. IHC results for CK-7 in liver biopsies of pnafld patients. (A) pnafld biopsies in patients categorized as not-sh display minimal involvement of the HPC compartment (arrows). (B) In biopsies of patients with definite-sh (i.e., NASH), the expansion of the HPC pool is prominent and is characterized by the appearance of reactive ductules at the periphery of portal spaces (arrows). (C and D) Clusters of intermediate hepatocytes were present in definite-sh biopsies (arrows). Original magnification 20 (A-C) and 40 (D). Moreover, the p21 waf1 and apoptotic indices in hepatocytes were correlated with HPC number (r ¼ 0.698, P < 0.01; and r ¼ 0.758, P < 0.01, respectively) and NAS score (r ¼ 0.476, P < 0.05; and r ¼ 0.470, P < 0.05, respectively), but not with other variables. Adiponectin, Resistin, and GLP-1 Expression in pnafld Biopsies. The percentages of adiponectin-, resistin-, and GLP-1-positive HPCs have been evaluated in serial sections using CK-7 as a progenitor cell marker 11 ; the data were further confirmed through double IF. CK-7 immunostaining clearly and specifically recognized HPCs in reactive ductules, cholangiocytes of interlobular bile ducts, and intermediate hepatocytes, but was consistently negative in mature hepatocytes and stromal and endothelial cells (ECs). In healthy livers and pnafld biopsies, adiponectin, resistin, and GLP-1 were significantly expressed by hepatocytes, cholangiocytes, and HPCs, as observed both in serial sections and through double IF (Figs. 4-6). Stromal cells were negative for adiponectin, resistin, and GLP-1, whereas ECs of portal vessels and sinusoids were negative for resistin and GLP-1, but positive for adiponectin (Supporting Fig. 1), as described elsewhere. 16 The separate channels of IF are shown in Table 2. Number of HPCs in pnafld and Absolute Number and Percentage of Adipokine-Positive HPCs Controls pnafld (All Patients) pnafld No Fibrosis pnafld Fibrosis pnafld Not-SH pnafld Definite-SH (N ¼ 6) (N ¼ 30) (N ¼ 5) (N ¼ 25) (N ¼ 11) (N ¼ 19) HPCs (cells per HPF) * * Adiponectin % positive HPCs No. of positive HPCs * Resistin % positive HPCs No. of positive HPCs * GLP1 % positive HPCs * * No. of positive HPCs * * Data are expressed as mean 6 SEM. *P < 0.05 versus healthy livers. P < 0.01 versus healthy livers and pnafld with no fibrosis. P < 0.05 versus healthy livers and pnafld with not-sh. P < 0.01 versus pnafld with not-sh.
6 HEPATOLOGY, Vol. 56, No. 6, 2012 NOBILI ET AL Fig. 2. Bivariate correlation of the HPC number with fibrosis and adipokine expression. (A) Number of HPCs per HPF is significantly correlated with fibrosis score. (B) Percentage of adiponectin-positive HPCs is inversely correlated with the NAS. (C) Number of resistin-positive HPCs per HPF is significantly correlated with fibrosis score. (D) Number of GLP-1-positive HPCs per HPF is significantly correlated with NAS score. Supporting Figs. 2-4, showing the specific expression of adipokines by HPCs within reactive ductules. Evaluation of adiponectin expression showed that the percentage of HPCs expressing adiponectin and the absolute number of adiponectin-positive HPCs per HPF did not differ between healthy liver biopsies and pnafld biopsies (Table 2). Taking the diagnostic category into account (Table 2; Fig. 4), we found that the percentage of adiponectin-positive HPCs in definite-sh biopsies ( ) was significantly lower than that in not-sh biopsies ( ; P < 0.01) and healthy controls ( ; P < 0.05). In addition, in pnafld patients, the percentage of adiponectin-positive HPCs per HPF was inversely correlated with NAS score (r ¼ 0.792; P < 0.001; Fig. 2B), steatosis (r ¼ 0.769; P < 0.001), hepatocyte ballooning (r ¼ 0.408; P < 0.05), and lobular inflammation (r ¼ 0.487; P < 0.01), but not with fibrosis. Adiponectin expression in the HPCs of NASH patients appeared to be down-regulated in relation to the NAS score and steatosis, but not fibrosis. Evaluation of resistin expression (Fig. 5) revealed that the percentage of HPCs expressing resistin was similar between healthy biopsies ( ) and pnafld biopsies ( ) and between definite-sh biopsies ( ) and not-sh biopsies ( ). However, the absolute number of resistin-positive HPCs per HPF in children with NAFLD ( ) was significantly higher than in healthy livers ( ; P < 0.05). Moreover, biopsies of livers with fibrosis displayed a higher number of positive cells ( ) than those of livers without fibrosis ( ; P < 0.05) and healthy controls (P < 0.05). In definite- SH biopsies, the number of resistin-positive HPCs per HPF ( ) was higher than that in not-sh biopsies ( ; P < 0.05) and controls (P < 0.05; Table 2). In pnafld patients, the absolute number of resistin-positive HPCs was directly correlated with fibrosis score (r ¼ 0.432; P < 0.05; Fig. 2C), but not with other histological parameters. The more expanded the HPC pool, the greater was the resistin expression, which correlated with the degree of fibrosis.
7 2148 NOBILI ET AL. HEPATOLOGY, December 2012 Fig. 3. IHC for p21 waf1 and cleaved caspase-3 in liver biopsies of pnafld patients. (A) Nuclear p21 waf1 expression by hepatocytes (arrows) was significantly increased in patients with definite-sh, compared to that in not-sh biopsies. Positive control (human colon) appears in the right image: Positive cells were located at the surface epithelium (arrows), whereas negative cells were found at the bottom of intestinal crypts (arrowheads). (B) Cytoplasmic cleaved caspase-3 expression by hepatocytes (arrows) was significantly higher in definite-sh biopsies than in not-sh biopsies. Positive control (human colon) is provided in the right image: Positive cells were located at the surface epithelium (arrows), whereas negative cells were found at the bottom of intestinal crypts (arrowheads). Original magnification: 40. The percentage of resistin-positive hepatocytes (Fig. 5C) in pnafld ( ) was higher than that in controls ( ; P < 0.05) and was correlated with the number of HPCs (r ¼ 0.617; P < 0.05), steatosis (r ¼ 0.591; P < 0.05), and NAS scores (r ¼ 0.546; P < 0.05). No correlations were observed with other histological parameters, such as ballooning, inflammation, or fibrosis. The percentage of GLP-1-positive HPCs (Fig. 6) in pnafld biopsies ( ) was higher than that in controls ( ; P < 0.05). The absolute number of GLP-1-positive HPCs per HPF was significantly (P < 0.05) higher in pnafld biopsies than in healthy livers, in definite-sh biopsies than in not-sh biopsies, and in biopsies with fibrosis than in biopsies without fibrosis (Table 2). Furthermore, GLP-1-positive HPCs correlated with steatosis (r ¼ 0.577; P < 0.01), hepatocyte ballooning (r ¼ 0.496; P < 0.05), and NAS score (r ¼ 0.594; P < 0.01; Fig. 2D), but not with inflammation or fibrosis. HPC expansion in NAFLD patients was associated with enhanced GLP-1 expression, which correlated with steatosis, but not with lobular inflammation or fibrosis. The percentage of GLP-1-positive hepatocytes (Fig. 6C) in pnafld biopsies ( ) was higher than that in healthy livers ( ; P < 0.05) and was correlated with the number of HPCs (r ¼ 0.704; P < 0.05). The percentage of GLP-1-positive hepatocytes was higher in definite-sh biopsies ( ) than in not-sh biopsies ( ; P < 0.05) and was correlated with ballooning (r ¼ 0.549; P < 0.05) and NAS scores (r ¼ 0.506; P < 0.05), but not with steatosis, fibrosis, or inflammation. Intermediate hepatocytes were positive (approximately 10%) for adiponectin, resistin, and GLP-1 (data not shown). Discussion The main findings of our study indicate the following: (1) The HPC compartment is markedly expanded in pnafld, especially in children with definite-sh
8 HEPATOLOGY, Vol. 56, No. 6, 2012 NOBILI ET AL Fig. 4. Adiponectin expression in pnafld patients. (A) Double IF for CK-7 (green) and adiponectin (red) in not-sh biopsies. Nuclei are shown in blue. Numerous CK-7-positive progenitor cells coexpress adiponectin (yellow cells: yellow arrows). (B) IHC for CK-7 (left) and adiponectin (right) in serial sections of not-sh biopsies. CK-7-positive HPCs highly express adiponectin (arrows); adiponectin is also expressed by hepatocytes and cholangiocytes of interlobular bile ducts and in hepatic artery branches. (C) Double IF for CK-7 (green) and adiponectin (red) in definite-sh (NASH) biopsies. Nuclei are shown in blue. In definite-sh (NASH), CK-7-positive HPCs are mostly adiponectin negative (green cells: green arrows). (D) IHC for CK-7 (left) and adiponectin (right) in serial sections of definite-sh (i.e., NASH). In NASH, adiponectin is still expressed by hepatocytes; in contrast, CK-7-positive reactive ductules composed of HPCs are adiponectin negative (arrows), confirming the findings obtained through double IF. Original magnification: 40. (i.e., NASH), and this expansion is associated with degree of fibrosis and indices of hepatocyte damage (i.e., apoptotic and p21 indices), and NASH livers are also characterized by the expansion of the intermediate hepatocyte pool; (2) HPCs and hepatocytes express adiponectin, resistin, and GLP-1; (3) adiponectin expression in the HPCs of NAFLD patients appears to be lower than that in healthy livers and this expression is inversely correlated with NAS and steatosis; (4) resistin expression increases in the HPCs of pnafld patients and is correlated with degree of fibrosis; and (5) GLP-1 expression in HPCs is enhanced in pnafld in relation to steatosis, hepatocyte ballooning, and NAS. In healthy conditions, HPCs are mostly quiescent cells that take no or minimal part in liver parenchyma renewal, because the replacement of necrotic and apoptotic hepatocytes occurs through the replication of adjacent hepatocytes within the lobules. 7-9,21 In chronic liver diseases, however, this primary pathway is impaired by various insults, thereby activating a secondary proliferative pathway of HPCs and the appearance of DR, which represents the morphological expression of HPC activation. 7,22 In NAFLD, oxidative stress plays a major role in the impairment of hepatocyte replication through the direct induction of p21 by hydrogen peroxide or by the triggering of the apoptotic cascade. 11 Our previous studies on pediatric NAFLD have shown that oxidative stress-marker levels are increased in patients with NASH and correlate with the severity of SH. 23 In the present study, we showed that massive HPC expansion, especially in children with NASH, is associated with degree of liver injury, hepatocyte apoptosis, and cell-cycle arrest. A population of intermediate hepatocytes was observed in NASH liver biopsies, but not in biopsies of not-sh patients. The number of intermediate hepatocytes in pnafld biopsies was correlated with both the
9 2150 NOBILI ET AL. HEPATOLOGY, December 2012 Fig. 5. Resistin expression in pnafld patients. (A) Double IF for CK-7 (green) and resistin (red) showed that in pnafld, numerous CK-7-positive HPCs coexpress resistin (in yellow: yellow arrows). Magnification of the area in the white box is provided in the right image. As indicated by white arrows, the cells (i.e., fibroblasts) around reactive ductules are clearly negative for both antigens, confirming that the positivity is specifically restricted to HPCs in reactive ductules. Nuclei are shown in blue. (B) IHC in serial sections of pnafld biopsies for CK-7 and resistin confirmed that numerous CK-7-positive HPCs express resistin (arrows). Notably, resistin is also expressed in hepatocytes and interlobular bile ducts. (C) In pnafld, resistin is also expressed by hepatocytes; in particular, in biopsies with definite-sh, steatotic hepatocytes are diffusely positive for resistin (right image). Original magnification: 40. number of HPCs and hepatocyte damage (i.e., ballooning), suggesting that the activation of the progenitor cell compartment and its hepatocyte differentiation are the result of the combination of impaired hepatocyte regeneration and increased hepatocyte injury caused by long-standing oxidative stress. The resident stem/progenitor cell pool participates in the repair of liver damage either through the replacement of dead cells or by driving fundamental repair processes, including fibrosis and angiogenesis. 9,24,25 In this context, our results in pediatric subjects seem to confirm data from adult patients, in which DR is independently correlated with progressive portal fibrosis. 11 In our study, HPC compartment expansion was independently correlated through multivariate logistic regression analysis with degree of fibrosis, indicating that in pediatric NASH, DR is also a main driver of fibrosis. DR might modulate hepatic fibrogenesis during liver injury through two possible mechanisms: (1) DR cells produce agents that are chemotactic for inflammatory cells and may activate HSCs, 10 and (2) DR cells undergo epithelial-mesenchymal transition, contributing to the portal myofibroblast pool. 10,26 In this study, we found no correlation between the HPC number and IR markers. This finding agrees with those of previous studies, in which these markers (e.g., insulin, HOMA-IR, and ISI) were not associated with liver fibrosis in pediatric populations. 13,27,28 Controversy persists in the literature, however, because (1) hyperinsulinemia is a common feature of pnafld, and some evidence exists that it may be an independent predictor of liver fibrosis, 27 and (2) even if ISI is a better marker of insulin sensitivity than fasting insulin and HOMA-IR, it had no practical application for the prediction of liver fibrosis. 27 We have previously shown how the activated and expanded HPC compartment expresses many neuroendocrine features. 24,25 Resistin, GLP-1, and adiponectin expression in HPCs adds new insights into this
10 HEPATOLOGY, Vol. 56, No. 6, 2012 NOBILI ET AL Fig. 6. GLP-1 expression in pnafld patients. (A) Double IF for CK-7 (green) and GLP-1 (red) showed that in pnafld, numerous CK-7-positive HPCs coexpress GLP-1 (in yellow: yellow arrows). Magnification of the area in the white box is provided in the right image. As indicated by white arrows, the cells (i.e., fibroblasts) around reactive ductules are clearly negative for both antigens, confirming that the positivity is specifically restricted to HPCs in reactive ductules. Nuclei are shown in blue. (B) IHC in serial sections of pnafld biopsies for CK-7 and GLP-1 confirmed that numerous CK-7-positive HPCs express GLP-1 (arrows). Notably, GLP-1 is also expressed in hepatocytes and interlobular bile ducts (arrowhead). (C) In pnafld, GLP-1 is also expressed by hepatocytes; in particular, in definite-sh biopsies (right), steatotic hepatocytes are diffusely positive for GLP-1, compared to those in not-sh biopsies (left), in which GLP-1-positive hepatocytes are less numerous. Original magnification: 40. scenario. The specificity of the immunostaining of these adipokines in HPCs was confirmed using double IF for CK-7 and by the negative reactivity of stromal cells. Although adipokine expression is prominent in adipose tissue, it has also been shown to occur within the liver. Leptin, for example, is expressed by activated HSCs and correlates with fibrogenesis, 29 adiponectin expression has been shown in liver tissue and is decreased in patients with NASH, 16 and resistin is expressed in the human liver, where it influences IR and the development of liver inflammation and fibrosis. 15 In pediatric livers, we showed that adiponectin, resistin, and GLP-1 were significantly expressed by HPCs and hepatocytes and showed marked changes throughout the course of pnafld. Parallel with their expansion, HPCs down-regulated their expression of adiponectin and up-regulated that of resistin and GLP-1. The inverse correlation we found between adiponectin and steatosis and NAS agrees with the current understanding 16 that this adipokine (1) is inversely correlated with fat mass and down-regulated in obesity and type 2 diabetes, (2) suppresses hepatic glucose production, improves insulin signaling, and exerts insulin-sensitizing effects in the liver, skeletal muscle, and adipose tissue, (3) is down-regulated in steatotic liver disease through various mechanisms, including fetuin-a hepatic secretion, and (4) ameliorates necroinflammation and steatosis when administered in experimental NASH. Several lines of evidence link the biology of resistin with hepatic inflammation. In rats, resistin administration significantly worsens inflammation after lipopolysaccharide injection, 30 and activated human HSCs respond to resistin with increased expression of proinflammatory chemokines and nuclear factor-kappa B activation. 15,31 Hepatic resistin expression increases in alcoholic SH and NASH and is correlated with inflammatory cell infiltration. 15 Resistin has been particularly associated with macrophage recruitment within the liver; this relationship could be related to the release of monocyte chemotactic protein-1 (Mcp-
11 2152 NOBILI ET AL. HEPATOLOGY, December ), which contributes to macrophage infiltration. Treatment with human resistin can induce Mcp-1 in ECs and HSCs in vitro. 14,15 Resistin could play a role in modulating the response of heterogenic macrophages in NAFLD. 32 NAFLD is classically associated with an increase in M1 proinflammatory cytokines (e.g., tumor necrosis factor-alpha and interlukin-12) 32 ; however, the M2 macrophages could play a role in hepatic fibrosis because they typically express higher levels of transforming growth factor-beta, which tends to promote collagen expression by HSCs. 33 The capability of resistin to induce alternatively activated M2 macrophages, rather than the classically activated M1 macrophages, could represent an interesting topic for future investigation. The correlation between resistin in HPCs and degree of fibrosis in pnafld is consistent with the current understanding of resistin expression. GLP-1 has insulin-independent effects on glucose disposal in extrapancreatic tissues, including the liver. 34 In hepatocytes, GLP-1 activates glycogen synthesis and has been implicated in the regulation of glucose homeostasis and IR in animal models of NAFLD. 35,36 A role for GLP-1 in the pathophysiology of cholangiocytes has also been shown. In particular, GLP-1 can sustain the growth of cholangiocytes in a biliary damage model, in which it is synthesized and locally released by proliferating cholangiocytes to sustain their proliferation in an autocrine/paracrine manner. 37 Herein, we showed that GLP-1 was also produced by proliferating hepatic stem/ progenitor cells. Its expression was correlated with HPC expansion and was higher in definite-sh biopsies than in not-sh biopsies, suggesting that GLP-1 plays a role in sustaining HPC proliferation in an autocrine/paracrine manner during NAFLD progression. Our findings open new perspectives on the pathophysiology of NAFLD and suggest several hypotheses to be tested. First, adipokines and, especially, GLP-1 and resistin may play a major role in promoting the resistance of HPCs to oxidative stress, favoring their differentiation during the course of NASH. 37 A second hypothesis is that these adipokines could be secreted into the peribiliary plexus, and easily reach hepatocytes, in which they may participate in modulating hepatic IR. Third, these adipokines may represent a new tool in the cross-talk between HPCs and HSCs, a mechanism considered to be the basis of periportal fibrosis. References 1. Brunt EM. Pathology of nonalcoholic fatty liver disease. Nat Rev Gastroenterol Hepatol 2010;7: Alisi A, Manco M, Vania A, Nobili V. Pediatric nonalcoholic fatty liver disease in J Pediatr 2009;155: Dunn W, Schwimmer JB. The obesity epidemic and nonalcoholic fatty liver disease in children. Curr Gastroenterol Rep 2008;10: Starley BQ, Calcagno CJ, Harrison SA. Nonalcoholic fatty liver disease and hepatocellular carcinoma: a weighty connection. HEPATOLOGY 2010;51: Tilg H, Moschen AR. Evolution of inflammation in nonalcoholic fatty liver disease: the multiple parallel hits hypothesis. HEPATOLOGY 2010; 52: Roskams T, Yang SQ, Koteish A, Durnez A, DeVos R, Huang X, et al. Oxidative stress and oval cell accumulation in mice and humans with alcoholic and nonalcoholic fatty liver disease. Am J Pathol 2003;163: Spee B, Carpino G, Schotanus BA, Katoonizadeh A, Vander Borght S, Gaudio E, et al. Characterisation of the liver progenitor cell niche in liver diseases: potential involvement of Wnt and Notch signalling. Gut 2010;59: Roskams TA, Theise ND, Balabaud C, Bhagat G, Bhathal PS, Bioulac- Sage P, et al. Nomenclature of the finer branches of the biliary tree: canals, ductules, and ductular reactions in human livers. HEPATOLOGY 2004;39: Gaudio E, Carpino G, Cardinale V, Franchitto A, Onori P, Alvaro D. New insights into liver stem cells. Dig Liver Dis 2009;41: Theise ND, Kuwahara R. The tissue biology of ductular reactions in human chronic liver disease. Gastroenterology 2007;133: Richardson MM, Jonsson JR, Powell EE, Brunt EM, Neuschwander- Tetri BA, Bhathal PS, et al. Progressive fibrosis in nonalcoholic steatohepatitis: association with altered regeneration and a ductular reaction. Gastroenterology 2007;133: Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. HEPATOLOGY 2005;41: Nobili V, Marcellini M, Devito R, Ciampalini P, Piemonte F, Comparcola D, et al. NAFLD in children: a prospective clinical-pathological study and effect of lifestyle advice. HEPATOLOGY 2006;44: Marra F, Bertolani C. Adipokines in liver diseases. HEPATOLOGY 2009; 50: Bertolani C, Sancho-Bru P, Failli P, Bataller R, Aleffi S, DeFranco R, et al. Resistin as an intrahepatic cytokine: overexpression during chronic injury and induction of proinflammatory actions in hepatic stellate cells. Am J Pathol 2006;169: Kaser S, Moschen A, Cayon A, Kaser A, Crespo J, Pons-Romero F, et al. Adiponectin and its receptors in non-alcoholic steatohepatitis. Gut 2005;54: Nobili V, Manco M, Devito R, Di Ciommo V, Comparcola D, Sartorelli MR, et al. Lifestyle intervention and antioxidant therapy in children with nonalcoholic fatty liver disease: a randomized, controlled trial. HEPATOLOGY 2008;48: Brunt EM, Kleiner DE, Wilson LA, Belt P, Neuschwander-Tetri BA. Nonalcoholic fatty liver disease (NAFLD) activity score and the histopathologic diagnosis in NAFLD: distinct clinicopathologic meanings. HEPATOLOGY 2011;53: Brunt EM. Nonalcoholic steatohepatitis: definition and pathology. Semin Liver Dis 2001;21: Katoonizadeh A, Nevens F, Verslype C, Pirenne J, Roskams T. Liver regeneration in acute severe liver impairment: a clinicopathological correlation study. Liver Int 2006;26: Fausto N. Liver regeneration and repair: hepatocytes, progenitor cells, and stem cells. HEPATOLOGY 2004;39: Turanyi E, Dezso K, Csomor J, Schaff Z, Paku S, Nagy P. Immunohistochemical classification of ductular reactions in human liver. Histopathology 2010;57: Nobili V, Parola M, Alisi A, Marra F, Piemonte F, Mombello C, et al. Oxidative stress parameters in paediatric non-alcoholic fatty liver disease. Int J Mol Med 2011;26: Alvaro D, Mancino MG, Glaser S, Gaudio E, Marzioni M, Francis H, et al. Proliferating cholangiocytes: a neuroendocrine compartment in the diseased liver. Gastroenterology 2007;132:
12 HEPATOLOGY, Vol. 56, No. 6, 2012 NOBILI ET AL Glaser SS, Gaudio E, Miller T, Alvaro D, Alpini G. Cholangiocyte proliferation and liver fibrosis. Expert Rev Mol Med 2009;11:e Omenetti A, Porrello A, Jung Y, Yang L, Popov Y, Choi SS, et al. Hedgehog signaling regulates epithelial-mesenchymal transition during biliary fibrosis in rodents and humans. J Clin Invest 2008;118: Nobili V, Alisi A, Vania A, Tiribelli C, Pietrobattista A, Bedogni G. The pediatric NAFLD fibrosis index: a predictor of liver fibrosis in children with non-alcoholic fatty liver disease. BMC Med 2009;7: Nobili V, Parkes J, Bottazzo G, Marcellini M, Cross R, Newman D, et al. Performance of ELF serum markers in predicting fibrosis stage in pediatric non-alcoholic fatty liver disease. Gastroenterology 2009;136: Saxena NK, Ikeda K, Rockey DC, Friedman SL, Anania FA. Leptin in hepatic fibrosis: evidence for increased collagen production in stellate cells and lean littermates of ob/ob mice. HEPATOLOGY 2002;35: Beier JI, Guo L, von Montfort C, Kaiser JP, Joshi-Barve S, Arteel GE. New role of resistin in lipopolysaccharide-induced liver damage in mice. J Pharmacol Exp Ther 2008;325: She H, Xiong S, Hazra S, Tsukamoto H. Adipogenic transcriptional regulation of hepatic stellate cells. J Biol Chem 2005;280: Lumeng CN, Saltiel AR. Inflammatory links between obesity and metabolic disease. J Clin Invest 2011;121: Spencer M, Yao-Borengasser A, Unal R, Rasouli N, Gurley CM, Zhu B, et al. Adipose tissue macrophages in insulin-resistant subjects are associated with collagen VI and fibrosis and demonstrate alternative activation. Am J Physiol Endocrinol Metab 2010;299:E1016-E Holst JJ. The physiology of glucagon-like peptide 1. Physiol Rev 2007; 87: Ayala JE, Bracy DP, James FD, Burmeister MA, Wasserman DH, Drucker DJ. Glucagon-like peptide-1 receptor knockout mice are protected from high-fat diet-induced insulin resistance. Endocrinology 2010;151: Lee YS, Shin S, Shigihara T, Hahm E, Liu MJ, Han J, et al. Glucagon-like peptide-1 gene therapy in obese diabetic mice results in longterm cure of diabetes by improving insulin sensitivity and reducing hepatic gluconeogenesis. Diabetes 2007;56: Marzioni M, Alpini G, Saccomanno S, Candelaresi C, Venter J, Rychlicki C, et al. Glucagon-like peptide-1 and its receptor agonist exendin-4 modulate cholangiocyte adaptive response to cholestasis. Gastroenterology 2007;133:
Expression of vascular endothelial growth factors and their receptors by hepatic progenitor cells in human liver diseases
 Original Article Expression of vascular endothelial growth factors and their receptors by hepatic progenitor cells in human liver diseases Antonio Franchitto 1,2, Paolo Onori 3, Anastasia Renzi 1, Guido
Original Article Expression of vascular endothelial growth factors and their receptors by hepatic progenitor cells in human liver diseases Antonio Franchitto 1,2, Paolo Onori 3, Anastasia Renzi 1, Guido
Challenges in the Diagnosis of Steatohepatitis
 The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
NASH Bench to Bedside
 NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup
 REVIEW REVIEW Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup Puneet Puri, M.B.B.S., M.D. and Arun J. Sanyal, M.B.B.S., M.D. Nonalcoholic fatty liver disease (NAFLD) is defined
REVIEW REVIEW Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup Puneet Puri, M.B.B.S., M.D. and Arun J. Sanyal, M.B.B.S., M.D. Nonalcoholic fatty liver disease (NAFLD) is defined
Steatotic liver disease
 Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
Non alcoholic fatty liver and Non alcoholic Steatohepatitis. By Dr. Seham Seif
 Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health
 CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
New insights into fatty liver disease. Rob Goldin Centre for Pathology, Imperial College
 New insights into fatty liver disease Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Prevalence of NASH Global prevalence of NAFLD is 25% with highest prevalence in the Middle
New insights into fatty liver disease Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Prevalence of NASH Global prevalence of NAFLD is 25% with highest prevalence in the Middle
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and
 Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical
 Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016.
 Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche,
 Supplemental Methods Analytical determinations ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche, Basel, Switzerland). Glucose, triglyceride, total
Supplemental Methods Analytical determinations ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche, Basel, Switzerland). Glucose, triglyceride, total
Liver Pathology in the 0bese
 Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy
 Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
The effect of aerobic exercise on serum level of liver enzymes and liver echogenicity in patients with non-alcoholic fatty liver disease
 Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE The effect of aerobic exercise on serum level of liver enzymes
Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE The effect of aerobic exercise on serum level of liver enzymes
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology
 Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need?
 Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk Fatty liver disease Is there fatty
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk Fatty liver disease Is there fatty
Hyaluronic acid predicts hepatic fibrosis in children with nonalcoholic fatty liver disease
 ORIGINAL ARTICLES Hyaluronic acid predicts hepatic fibrosis in children with nonalcoholic fatty liver disease VALERIO NOBILI, ANNA ALISI, GIULIANO TORRE, RITA DE VITO, ANDREA PIETROBATTISTA, GIUSEPPE MORINO,
ORIGINAL ARTICLES Hyaluronic acid predicts hepatic fibrosis in children with nonalcoholic fatty liver disease VALERIO NOBILI, ANNA ALISI, GIULIANO TORRE, RITA DE VITO, ANDREA PIETROBATTISTA, GIUSEPPE MORINO,
British Liver Transplant Group Pathology meeting September Leeds cases
 British Liver Transplant Group Pathology meeting September 2014 Leeds cases Leeds Case 1 Male 61 years Liver transplant for HCV cirrhosis with HCC in January 2014. Now raised ALT and bilirubin,? acute
British Liver Transplant Group Pathology meeting September 2014 Leeds cases Leeds Case 1 Male 61 years Liver transplant for HCV cirrhosis with HCC in January 2014. Now raised ALT and bilirubin,? acute
(C) Fig 5.1 Classical non alcoholic steatohepatitis (NASH). (A) Steatosis, hepatocyte ballooning, and inflammation (the trio of changes
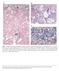 (A) (B) (C) Fig 5.1 Classical non alcoholic steatohepatitis (NASH). (A) Steatosis, hepatocyte ballooning, and inflammation (the trio of changes representing the minimal histological criteria of steatohepatitis)
(A) (B) (C) Fig 5.1 Classical non alcoholic steatohepatitis (NASH). (A) Steatosis, hepatocyte ballooning, and inflammation (the trio of changes representing the minimal histological criteria of steatohepatitis)
Hepatitis C wi w t i h Ju J dy y W y W a y t a t t
 Hepatitis C with Judy Wyatt Hepatitis C and the histopathologist Pre-2006 biopsy based treatment of moderate-severe chronic hepatitis Now biopsy for: Watchful waiting, to confirm mild disease? Cirrhosis
Hepatitis C with Judy Wyatt Hepatitis C and the histopathologist Pre-2006 biopsy based treatment of moderate-severe chronic hepatitis Now biopsy for: Watchful waiting, to confirm mild disease? Cirrhosis
Improving Access to Quality Medical Care Webinar Series
 Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES
 NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
AAIM: GI Workshop Follow Up to Case Studies. Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease
 AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need?
 Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk @robdgol FATTY LIVER DISEASE Brunt
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk @robdgol FATTY LIVER DISEASE Brunt
PITFALLS IN THE DIAGNOSIS OF MEDICAL LIVER DISEASE WITH TWO CONCURRENT ETIOLOGIES I HAVE NOTHING TO DISCLOSE CURRENT ISSUES IN ANATOMIC PATHOLOGY 2017
 CURRENT ISSUES IN ANATOMIC PATHOLOGY 2017 I HAVE NOTHING TO DISCLOSE Linda Ferrell PITFALLS IN THE DIAGNOSIS OF MEDICAL LIVER DISEASE WITH TWO CONCURRENT ETIOLOGIES Linda Ferrell, MD, UCSF THE PROBLEM
CURRENT ISSUES IN ANATOMIC PATHOLOGY 2017 I HAVE NOTHING TO DISCLOSE Linda Ferrell PITFALLS IN THE DIAGNOSIS OF MEDICAL LIVER DISEASE WITH TWO CONCURRENT ETIOLOGIES Linda Ferrell, MD, UCSF THE PROBLEM
Laboratory analysis of the obese child recommendations and discussion. MacKenzi Hillard May 4, 2011
 Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
NAFLD AND TYPE 2 DIABETES
 NAFLD AND TYPE 2 DIABETES Sonia Caprio, MD STOPNASH Symposium on the Origin and Pathways of Nonalcoholic Steatohepatitis Washington 7, 215 Global Projection of Diabetes Hossain P et al. N Engl J Med 27;356:213
NAFLD AND TYPE 2 DIABETES Sonia Caprio, MD STOPNASH Symposium on the Origin and Pathways of Nonalcoholic Steatohepatitis Washington 7, 215 Global Projection of Diabetes Hossain P et al. N Engl J Med 27;356:213
NONALCOHOLIC FATTY LIVER DISEASE. Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD. April 13, 2012
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
The classical metabolic work-up, approved by the Ethics Committee of the Antwerp
 SUPPLEMENTARY MATERIALS METHODS Metabolic work-up The classical metabolic work-up, approved by the Ethics Committee of the Antwerp University Hospital and requiring written informed consent, included a
SUPPLEMENTARY MATERIALS METHODS Metabolic work-up The classical metabolic work-up, approved by the Ethics Committee of the Antwerp University Hospital and requiring written informed consent, included a
IS LIVER BIOPSY NECESSARY IN PATIENTS WITH NONALCOHOLIC FATTY LIVER DISEASE?
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2016 vol. 120, no. 3 INTERNAL MEDICINE - PEDIATRICS UPDATES IS LIVER BIOPSY NECESSARY IN PATIENTS WITH NONALCOHOLIC FATTY LIVER DISEASE? R. S. Gavril 1, Laura Mihalache
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2016 vol. 120, no. 3 INTERNAL MEDICINE - PEDIATRICS UPDATES IS LIVER BIOPSY NECESSARY IN PATIENTS WITH NONALCOHOLIC FATTY LIVER DISEASE? R. S. Gavril 1, Laura Mihalache
Internal and Emergency Medicine Official Journal of the Italian Society of Internal Medicine. ISSN Volume 8 Number 3
 Hepatic Steatosis Index and Lipid Accumulation Product as middle-term predictors of incident metabolic syndrome in a large population sample: data from the Brisighella Heart Study Arrigo F. G. Cicero,
Hepatic Steatosis Index and Lipid Accumulation Product as middle-term predictors of incident metabolic syndrome in a large population sample: data from the Brisighella Heart Study Arrigo F. G. Cicero,
LIVER PATHOLOGY. Thursday 28 th November 2013
 LIVER PATHOLOGY Thursday 28 th November 2013 Liver biopsy assessment of steatosis Amar Paul Dhillon Royal Free Hospital RIBA, London Thursday 28th November 2013 NAFLD didn t exist before 2001 and liver
LIVER PATHOLOGY Thursday 28 th November 2013 Liver biopsy assessment of steatosis Amar Paul Dhillon Royal Free Hospital RIBA, London Thursday 28th November 2013 NAFLD didn t exist before 2001 and liver
WHAT THE EXPERIMENTAL MODELS CAN TEACH US IN NAFLD/NASH? Claudio Tiribelli, MD PhD Scientific Director FIF
 WHAT THE EXPERIMENTAL MODELS CAN TEACH US IN NAFLD/NASH? Claudio Tiribelli, MD PhD Scientific Director FIF ctliver@fegato.it Worldwide estimated prevalence of NAFLD distribution of PNPLA3 genotypes 2017-Younussi
WHAT THE EXPERIMENTAL MODELS CAN TEACH US IN NAFLD/NASH? Claudio Tiribelli, MD PhD Scientific Director FIF ctliver@fegato.it Worldwide estimated prevalence of NAFLD distribution of PNPLA3 genotypes 2017-Younussi
Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease
 ORIGINAL ARTICLE Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease Hisamitsu Miyaaki 1, Tatsuki Ichikawa 1,NaotaTaura 1, Satoshi Miuma
ORIGINAL ARTICLE Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease Hisamitsu Miyaaki 1, Tatsuki Ichikawa 1,NaotaTaura 1, Satoshi Miuma
Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis
 Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis Naoki Tanaka 1, Akira Horiuchi 2, Takahide Yokoyama 3, Shigeyuki Kawa 1, and Kendo Kiyosawa 1 1 Department of Gastroenterology,
Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis Naoki Tanaka 1, Akira Horiuchi 2, Takahide Yokoyama 3, Shigeyuki Kawa 1, and Kendo Kiyosawa 1 1 Department of Gastroenterology,
Nonalcoholic fatty liver disease (NAFLD) is rapidly
 Lifestyle Intervention and Antioxidant Therapy in Children with Nonalcoholic Fatty Liver Disease: A Randomized, Controlled Trial Valerio Nobili, 1 Melania Manco, 1 Rita Devito, 2 Vincenzo Di Ciommo, 3
Lifestyle Intervention and Antioxidant Therapy in Children with Nonalcoholic Fatty Liver Disease: A Randomized, Controlled Trial Valerio Nobili, 1 Melania Manco, 1 Rita Devito, 2 Vincenzo Di Ciommo, 3
Steatosi epatica ed HCV
 Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
Slide 7 demonstrates acute pericholangitisis with neutrophils around proliferating bile ducts.
 Many of the histologic images and the tables are from MacSween s Pathology of the Liver (5 th Edition). Other images were used from an online source called PathPedia.com. A few images from other sources
Many of the histologic images and the tables are from MacSween s Pathology of the Liver (5 th Edition). Other images were used from an online source called PathPedia.com. A few images from other sources
IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA
 UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H.
![3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H. 3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H.](/thumbs/82/84935173.jpg) U.S. Adults: 1988 Nineteen states with 10-14% 14% Prevalence of Obesity (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Metabolic John P. Cello, MD Professor of Medicine and Surgery, University of California,
U.S. Adults: 1988 Nineteen states with 10-14% 14% Prevalence of Obesity (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Metabolic John P. Cello, MD Professor of Medicine and Surgery, University of California,
Update on Non-Alcoholic Fatty Liver Disease. Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI
 Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
NONALCOHOLIC FATTY LIVER DISEASE
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
Non-Alcoholic Fatty Liver Disease
 Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
With the rise in obesity, nonalcoholic fatty. Hedgehog Pathway and Pediatric Nonalcoholic Fatty Liver Disease
 Hedgehog Pathway and Pediatric Nonalcoholic Fatty Liver Disease Marzena Swiderska-Syn, 1 Ayako Suzuki, 1 Cynthia D. Guy, 2 Jeffrey B. Schwimmer, 3 Manal F. Abdelmalek, 1 Joel E. Lavine, 4 and Anna Mae
Hedgehog Pathway and Pediatric Nonalcoholic Fatty Liver Disease Marzena Swiderska-Syn, 1 Ayako Suzuki, 1 Cynthia D. Guy, 2 Jeffrey B. Schwimmer, 3 Manal F. Abdelmalek, 1 Joel E. Lavine, 4 and Anna Mae
Mass Histology Service
 Mass Histology Service A complete anatomical pathology laboratory www.masshistology.com Telephone: (877) 286-6004 Report on Pathology A Time Course Study of the Local Effects of Intramuscular XXXXXXX Injection
Mass Histology Service A complete anatomical pathology laboratory www.masshistology.com Telephone: (877) 286-6004 Report on Pathology A Time Course Study of the Local Effects of Intramuscular XXXXXXX Injection
Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar
 Original Research Article Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar Naresh Kumar 1, Jyoti Kumar Dinkar 2*, Chandrakishore
Original Research Article Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar Naresh Kumar 1, Jyoti Kumar Dinkar 2*, Chandrakishore
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE
 PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
Nonalcoholic fatty liver disease (NAFLD) is the most common
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1249 1254 Cytokeratin 18 Fragment Levels as a Noninvasive Biomarker for Nonalcoholic Steatohepatitis in Bariatric Surgery Patients DIMA L. DIAB,* LISA YERIAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1249 1254 Cytokeratin 18 Fragment Levels as a Noninvasive Biomarker for Nonalcoholic Steatohepatitis in Bariatric Surgery Patients DIMA L. DIAB,* LISA YERIAN,
In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease
 REVIEW In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease Ting-Ting Chan, M.R.C.P., and Vincent Wai-Sun Wong, M.D. Nonalcoholic fatty liver disease (NAFLD) affects 15% to 40% of the general
REVIEW In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease Ting-Ting Chan, M.R.C.P., and Vincent Wai-Sun Wong, M.D. Nonalcoholic fatty liver disease (NAFLD) affects 15% to 40% of the general
Improving the Lives of Patients with Liver Diseases
 Improving the Lives of Patients with Liver Diseases Corporate Presentation March 2019 Safe Harbor Statement This presentation contains "forward-looking" statements that involve risks, uncertainties and
Improving the Lives of Patients with Liver Diseases Corporate Presentation March 2019 Safe Harbor Statement This presentation contains "forward-looking" statements that involve risks, uncertainties and
An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications
 REVIEW An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications Naim Alkhouri, M.D.,*, and Andrea Scott, B.S.* Nonalcoholic fatty liver disease (NAFLD)
REVIEW An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications Naim Alkhouri, M.D.,*, and Andrea Scott, B.S.* Nonalcoholic fatty liver disease (NAFLD)
The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis
 The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis Objectives: Liver biopsy is the gold standard for diagnosing the extent of fibrosis in NAFLD/NASH;
The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis Objectives: Liver biopsy is the gold standard for diagnosing the extent of fibrosis in NAFLD/NASH;
Primary biliary cirrhosis (PBC) is a chronic cholestatic
 RAPID COMMUNICATION Bile Ductules and Stromal Cells Express Hedgehog Ligands and/or Hedgehog Target Genes in Primary Biliary Cirrhosis Youngmi Jung, 1 Shannon J. McCall, 2 Yin-Xiong Li, 1 and Anna Mae
RAPID COMMUNICATION Bile Ductules and Stromal Cells Express Hedgehog Ligands and/or Hedgehog Target Genes in Primary Biliary Cirrhosis Youngmi Jung, 1 Shannon J. McCall, 2 Yin-Xiong Li, 1 and Anna Mae
METABOLIC SYNDROME AND HCV: FROM HCV
 METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
Pitfalls in the diagnosis of well-differentiated hepatocellular lesions
 2013 Colorado Society of Pathology Pitfalls in the diagnosis of well-differentiated hepatocellular lesions Sanjay Kakar, MD University of California, San Francisco Outline Hepatocellular adenoma: new WHO
2013 Colorado Society of Pathology Pitfalls in the diagnosis of well-differentiated hepatocellular lesions Sanjay Kakar, MD University of California, San Francisco Outline Hepatocellular adenoma: new WHO
EVALUATION OF ABNORMAL LIVER TESTS
 EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
AMR in Liver Transplantation: Incidence
 AMR in Liver Transplantation: Incidence Primary AMR 1/3 to 1/2 of ABO-incompatible transplants Uncommon with ABO-compatible transplant Secondary AMR Unknown incidence: rarely tested Why is AMR uncommon
AMR in Liver Transplantation: Incidence Primary AMR 1/3 to 1/2 of ABO-incompatible transplants Uncommon with ABO-compatible transplant Secondary AMR Unknown incidence: rarely tested Why is AMR uncommon
HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO
 HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO The identification of abnormal liver enzymes usually indicates liver damage but rarely
HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO The identification of abnormal liver enzymes usually indicates liver damage but rarely
Fibrosis & Structural Decline of Liver Allografts: what and how to measure & potential underlying causes. Carla Venturi Monteagudo MD, PhD
 Fibrosis & Structural Decline of Liver Allografts: what and how to measure & potential underlying causes Carla Venturi Monteagudo MD, PhD THE NORMAL LIVER ARCHITECTURE Parenchymal Cells -Hepatocytes -Cholangiocytes
Fibrosis & Structural Decline of Liver Allografts: what and how to measure & potential underlying causes Carla Venturi Monteagudo MD, PhD THE NORMAL LIVER ARCHITECTURE Parenchymal Cells -Hepatocytes -Cholangiocytes
Future of stem cell therapy in liver disease Domenico ALVARO, MD Sapienza, University of Rome, Italy
 Future of stem cell therapy in liver disease Domenico ALVARO, MD Sapienza, University of Rome, Italy AISF, 17 th Pre Meeting Future Scenarios in Hepatology, 18-02-2015. CELL THERAPY and LIVER DISEASES
Future of stem cell therapy in liver disease Domenico ALVARO, MD Sapienza, University of Rome, Italy AISF, 17 th Pre Meeting Future Scenarios in Hepatology, 18-02-2015. CELL THERAPY and LIVER DISEASES
UMHS-PUHSC JOINT INSTITUTE
 Role of Visceral Adiposity in the Pathogenesis of Non-Alcoholic Fatty Liver Disease in Lean versus Obese Patients: A Comparative Study between Patients at UMHS versus PUHSC Lai WEI and Anna LOK W Zhang,
Role of Visceral Adiposity in the Pathogenesis of Non-Alcoholic Fatty Liver Disease in Lean versus Obese Patients: A Comparative Study between Patients at UMHS versus PUHSC Lai WEI and Anna LOK W Zhang,
Digestive system L 4. Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section
 Digestive system L 4 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the structure of liver. 2-Define liver lobule, and identify its zones. 3-Define portal
Digestive system L 4 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the structure of liver. 2-Define liver lobule, and identify its zones. 3-Define portal
Do Histological Features Inform DILI mechanisms?
 Do Histological Features Inform DILI mechanisms? Drug-Induced Liver Injury (DILI) Conference XVII June, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Disclosures No financial or other conflicts
Do Histological Features Inform DILI mechanisms? Drug-Induced Liver Injury (DILI) Conference XVII June, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Disclosures No financial or other conflicts
Interface hepatitis in PBC: Prognostic marker and therapeutic target
 Interface hepatitis in PBC: Prognostic marker and therapeutic target Raoul Poupon Service d Hépatologie, Hôpital Saint-Antoine, Paris Faculté de Médecine Pierre & Marie Curie, Paris Key features of
Interface hepatitis in PBC: Prognostic marker and therapeutic target Raoul Poupon Service d Hépatologie, Hôpital Saint-Antoine, Paris Faculté de Médecine Pierre & Marie Curie, Paris Key features of
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse
 Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
Nottingham Patterns of liver fibrosis and their clinical significance
 Nottingham 2006 Patterns of liver fibrosis and their clinical significance Alastair D Burt Professor of Pathology and Dean of Clinical Medicine University of Newcastle upon Tyne Collapse of reticulin
Nottingham 2006 Patterns of liver fibrosis and their clinical significance Alastair D Burt Professor of Pathology and Dean of Clinical Medicine University of Newcastle upon Tyne Collapse of reticulin
M30 Apoptosense ELISA. A biomarker assay for detection and screening of NASH
 M30 Apoptosense ELISA A biomarker assay for detection and screening of NASH NASH A Global Disease In the Western countries, Non-Alcoholic Fatty Liver Disease (NAFLD) is the most common liver disease, strongly
M30 Apoptosense ELISA A biomarker assay for detection and screening of NASH NASH A Global Disease In the Western countries, Non-Alcoholic Fatty Liver Disease (NAFLD) is the most common liver disease, strongly
Evercore ISI Presentation- Madrigal
 Evercore ISI Presentation- Madrigal Forward-Looking Statements Any statements, other than statements of historical facts, made in this presentation regarding our clinical studies and our research and development
Evercore ISI Presentation- Madrigal Forward-Looking Statements Any statements, other than statements of historical facts, made in this presentation regarding our clinical studies and our research and development
Pathogenesis of Cholangiolocellular Carcinoma: Possibility of an Interlobular Duct Origin
 REVIEW ARTICLE Pathogenesis of Cholangiolocellular Carcinoma: Possibility of an Interlobular Duct Origin Fukuo Kondo 1,2 and Toshio Fukusato 2 Abstract Cholangiolocellular carcinoma (CoCC) is categorized
REVIEW ARTICLE Pathogenesis of Cholangiolocellular Carcinoma: Possibility of an Interlobular Duct Origin Fukuo Kondo 1,2 and Toshio Fukusato 2 Abstract Cholangiolocellular carcinoma (CoCC) is categorized
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NAFLD/NASH. Definitions. Pathology NASH. Vicki Shah PA-C, MMS Rush University Hepatology
 NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
Case #1. Digital Slides 11/6/ year old woman presented with abnormal liver function tests. Liver Biopsy to r/o autoimmune hepatitis
 45 year old woman presented with abnormal liver function tests Liver Biopsy to r/o autoimmune hepatitis Further down. ANA 1: 160; ASMA 1:80 ANA 1: 160; ASMA 1:80 IgG = 14.5 g/l (upper normal range: 16)
45 year old woman presented with abnormal liver function tests Liver Biopsy to r/o autoimmune hepatitis Further down. ANA 1: 160; ASMA 1:80 ANA 1: 160; ASMA 1:80 IgG = 14.5 g/l (upper normal range: 16)
Interpretation of the liver hypertrophy in the toxicological evaluation of veterinary medicinal products
 Provisional translation The Food Safety Commission Final decision on September 7, 2017 This English version of the Commission Decision is intended to be reference material to provide convenience for users.
Provisional translation The Food Safety Commission Final decision on September 7, 2017 This English version of the Commission Decision is intended to be reference material to provide convenience for users.
Acute Hepatitis in a Patient with NASH and Elevation of CMV-IgM
 Acute Hepatitis in a Patient with NASH and Elevation of CMV-IgM Uta Drebber, MD Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the
Acute Hepatitis in a Patient with NASH and Elevation of CMV-IgM Uta Drebber, MD Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the
Disclosure. Objectives. Smash the Nash: A practical approach to fatty liver disease
 Smash the Nash: A practical approach to fatty liver disease Bruce D. Askey, MS, ANP-BC Associate Lecturer North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology Guthrie Clinic
Smash the Nash: A practical approach to fatty liver disease Bruce D. Askey, MS, ANP-BC Associate Lecturer North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology Guthrie Clinic
Original Article. Significance of Hepatic Steatosis in Chronic Hepatitis B Infection INTRODUCTION
 Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Chapter 18 Liver and Gallbladder
 Chapter 18 Liver and Gallbladder 解剖學科徐淑媛 本堂重點 1. Liver : functions & histology 2. Gallbladder Physiology Liver Produce circulating plasma proteins Vitamin Iron Degradation Metabolism Bile manufacture (exocrine)
Chapter 18 Liver and Gallbladder 解剖學科徐淑媛 本堂重點 1. Liver : functions & histology 2. Gallbladder Physiology Liver Produce circulating plasma proteins Vitamin Iron Degradation Metabolism Bile manufacture (exocrine)
NIH Public Access Author Manuscript Am J Med Sci. Author manuscript; available in PMC 2015 January 01.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Med Sci. 2014 January ; 347(1):. doi:10.1097/maj.0b013e31828b25a5. Association Between Metabolic Syndrome and Its Individual
NIH Public Access Author Manuscript Published in final edited form as: Am J Med Sci. 2014 January ; 347(1):. doi:10.1097/maj.0b013e31828b25a5. Association Between Metabolic Syndrome and Its Individual
Crosstalk between Adiponectin and IGF-IR in breast cancer. Prof. Young Jin Suh Department of Surgery The Catholic University of Korea
 Crosstalk between Adiponectin and IGF-IR in breast cancer Prof. Young Jin Suh Department of Surgery The Catholic University of Korea Obesity Chronic, multifactorial disorder Hypertrophy and hyperplasia
Crosstalk between Adiponectin and IGF-IR in breast cancer Prof. Young Jin Suh Department of Surgery The Catholic University of Korea Obesity Chronic, multifactorial disorder Hypertrophy and hyperplasia
A Combination of the Pediatric NAFLD Fibrosis Index and Enhanced Liver Fibrosis Test Identifies Children With Fibrosis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:150 155 A Combination of the Pediatric NAFLD Fibrosis Index and Enhanced Liver Fibrosis Test Identifies Children With Fibrosis NAIM ALKHOURI,* CHRISTINE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:150 155 A Combination of the Pediatric NAFLD Fibrosis Index and Enhanced Liver Fibrosis Test Identifies Children With Fibrosis NAIM ALKHOURI,* CHRISTINE
How to Approach a Medical Liver Biopsy. 9 th Bryan Warren School of Pathology Pancreatic and Liver Pathology. Sarajevo, 6 th -7 th November 2015
 1 A Brief Introduction to the Liver Sessions 9 th Bryan Warren School of Pathology Pancreatic and Liver Pathology Sarajevo, 6 th -7 th November 2015 Stefan Hübscher, Institute of Immunology & Immunotherapy,
1 A Brief Introduction to the Liver Sessions 9 th Bryan Warren School of Pathology Pancreatic and Liver Pathology Sarajevo, 6 th -7 th November 2015 Stefan Hübscher, Institute of Immunology & Immunotherapy,
902 Biomed Environ Sci, 2014; 27(11):
 902 Biomed Environ Sci, 2014; 27(11): 902-906 Letter to the Editor Curcuminoids Target Decreasing Serum Adipocyte-fatty Acid Binding Protein Levels in Their Glucose-lowering Effect in Patients with Type
902 Biomed Environ Sci, 2014; 27(11): 902-906 Letter to the Editor Curcuminoids Target Decreasing Serum Adipocyte-fatty Acid Binding Protein Levels in Their Glucose-lowering Effect in Patients with Type
Serum Levels of CK18 M30 and Leptin Are Useful Predictors of Steatohepatitis and Fibrosis in Paediatric NAFLD
 ORIGINAL ARTICLE: HEPATOLOGY AND NUTRITION Serum Levels of CK18 M30 and Leptin Are Useful Predictors of Steatohepatitis and Fibrosis in Paediatric NAFLD Emer Fitzpatrick, y Ragai R. Mitry, y Alberto Quaglia,
ORIGINAL ARTICLE: HEPATOLOGY AND NUTRITION Serum Levels of CK18 M30 and Leptin Are Useful Predictors of Steatohepatitis and Fibrosis in Paediatric NAFLD Emer Fitzpatrick, y Ragai R. Mitry, y Alberto Quaglia,
NAFLD & NASH: Russian perspective
 NAFLD & NASH: Russian perspective Vasily Isakov, MD, PhD Professor, Chief, Department Gastroenterology & Hepatology, Federal Research Center of nutrition, biotechnology and food safety Disclosures Received
NAFLD & NASH: Russian perspective Vasily Isakov, MD, PhD Professor, Chief, Department Gastroenterology & Hepatology, Federal Research Center of nutrition, biotechnology and food safety Disclosures Received
«STEATOSI EPATICA ED EPATOPATIE METABOLICHE» Ester Vanni Division of Gastroenterology University of Turin
 «STEATOSI EPATICA ED EPATOPATIE METABOLICHE» Ester Vanni Division of Gastroenterology University of Turin OUTLINE NAFLD overview NAFLD and menarche NAFLD and pregnancy NAFLD and menopause Other metabolic
«STEATOSI EPATICA ED EPATOPATIE METABOLICHE» Ester Vanni Division of Gastroenterology University of Turin OUTLINE NAFLD overview NAFLD and menarche NAFLD and pregnancy NAFLD and menopause Other metabolic
Journal of. Gastroenterology and Hepatology Research. Human Hepatic Progenitor Cell Expansion in Liver Fibrosis of Elderly Cadavers INTRODUCTION
 Journal of Gastroenterology and Hepatology Research Online Submissions: http://www.ghrnet.org/index./joghr/ doi: 10.17554/j.issn.2224-3992.2018.07.776 Journal of GHR 2018 August 21; 7(4): 2632-2643 ISSN
Journal of Gastroenterology and Hepatology Research Online Submissions: http://www.ghrnet.org/index./joghr/ doi: 10.17554/j.issn.2224-3992.2018.07.776 Journal of GHR 2018 August 21; 7(4): 2632-2643 ISSN
2 nd International Workshop on NASH Biomarkers, Washington DC, May 5-6, 2017
 Hepatic Proton Density Fat Fraction Correlates With Histologic Measures of Steatosis and Is Responsive to Changes in Those Measures in a Multi-center Nonalcoholic Steatohepatitis Clinical Trial Michael
Hepatic Proton Density Fat Fraction Correlates With Histologic Measures of Steatosis and Is Responsive to Changes in Those Measures in a Multi-center Nonalcoholic Steatohepatitis Clinical Trial Michael
Although lobular stellate cell activation and zone 3
 GASTROENTEROLOGY 2007;133:80 90 Progressive Fibrosis in Nonalcoholic Steatohepatitis: Association With Altered Regeneration and a Ductular Reaction MICHELLE M. RICHARDSON,* JULIE R. JONSSON,* ELIZABETH
GASTROENTEROLOGY 2007;133:80 90 Progressive Fibrosis in Nonalcoholic Steatohepatitis: Association With Altered Regeneration and a Ductular Reaction MICHELLE M. RICHARDSON,* JULIE R. JONSSON,* ELIZABETH
Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease
 ORIGINAL ARTICLE Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease Takashi Wada and Mikio Zeniya Abstract Objective We investigated the distribution and characteristics of the
ORIGINAL ARTICLE Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease Takashi Wada and Mikio Zeniya Abstract Objective We investigated the distribution and characteristics of the
Yun-Jung Choi, Jiangao Song, Jeff D. Johnson, Charles McWherter. NASH-TAG Conference Park City, Utah January 4, 2019
 Combination Therapy of Seladelpar and Liraglutide Attenuates Obesity, Hepatic Steatosis and Fibrosis in a Diet-induced and Biopsy-confirmed Mouse Model of NASH Yun-Jung Choi, Jiangao Song, Jeff D. Johnson,
Combination Therapy of Seladelpar and Liraglutide Attenuates Obesity, Hepatic Steatosis and Fibrosis in a Diet-induced and Biopsy-confirmed Mouse Model of NASH Yun-Jung Choi, Jiangao Song, Jeff D. Johnson,
Downloaded from zjrms.ir at 3: on Monday February 25th 2019 NAFLD BMI. Kg/m2 NAFLD
 logistic regression Student s t-test P< BMI BMI P< ALT AST P< Email:mkhoshbaten@yahoo.com Kg/m2 NASH RUQ B C II Case-Control II Logistic Regression Chi-Square T-test P< Grade Model 1- A diffuse hyper echoic
logistic regression Student s t-test P< BMI BMI P< ALT AST P< Email:mkhoshbaten@yahoo.com Kg/m2 NASH RUQ B C II Case-Control II Logistic Regression Chi-Square T-test P< Grade Model 1- A diffuse hyper echoic
Update on Nonalcoholic Fatty Liver Disease. Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic
 Update on Nonalcoholic Fatty Liver Disease Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic Outline Defining the phenotypes of nonalcoholic fatty liver disease NAFLD Diagnostics
Update on Nonalcoholic Fatty Liver Disease Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic Outline Defining the phenotypes of nonalcoholic fatty liver disease NAFLD Diagnostics
The association between white blood cell subtypes and prevalence and incidence of nonalcoholic fatty liver disease
 834477EJI0010.1177/2058739219834477European Journal of InflammationZhang et al. letter2019 Letter to the Editor The association between white blood cell subtypes and prevalence and incidence of nonalcoholic
834477EJI0010.1177/2058739219834477European Journal of InflammationZhang et al. letter2019 Letter to the Editor The association between white blood cell subtypes and prevalence and incidence of nonalcoholic
Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis
 The Turkish Journal of Pediatrics 2015; 57: 492-497 Original Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis Aysel Ünlüsoy-Aksu 1,
The Turkish Journal of Pediatrics 2015; 57: 492-497 Original Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis Aysel Ünlüsoy-Aksu 1,
Non-Alcoholic Fatty Liver Disease An Update
 Non-Alcoholic Fatty Liver Disease An Update Stefan Hübscher, School of Cancer Sciences, University of Birmingham Dept of Cellular Pathology, Queen Elizabeth Hospital, Birmingham First described in 1980
Non-Alcoholic Fatty Liver Disease An Update Stefan Hübscher, School of Cancer Sciences, University of Birmingham Dept of Cellular Pathology, Queen Elizabeth Hospital, Birmingham First described in 1980
Supplementary Figure S1. Effect of Glucose on Energy Balance in WT and KHK A/C KO
 Supplementary Figure S1. Effect of Glucose on Energy Balance in WT and KHK A/C KO Mice. WT mice and KHK-A/C KO mice were provided drinking water containing 10% glucose or tap water with normal chow ad
Supplementary Figure S1. Effect of Glucose on Energy Balance in WT and KHK A/C KO Mice. WT mice and KHK-A/C KO mice were provided drinking water containing 10% glucose or tap water with normal chow ad
Role of APN and TNF-α in type 2 diabetes mellitus complicated by nonalcoholic fatty liver disease
 Role of APN and TNF-α in type 2 diabetes mellitus complicated by nonalcoholic fatty liver disease X. Lin 1,2, Z. Zhang 2, J.M. Chen 2, Y.Y. Xu 2, H.R. Ye 2, J. Cui 2, Y. Fang 2, Y. Jin 2, D.R. Zhu 2 and
Role of APN and TNF-α in type 2 diabetes mellitus complicated by nonalcoholic fatty liver disease X. Lin 1,2, Z. Zhang 2, J.M. Chen 2, Y.Y. Xu 2, H.R. Ye 2, J. Cui 2, Y. Fang 2, Y. Jin 2, D.R. Zhu 2 and
