Supporting Information Table SI. Individual rfixfc Pharmacokinetic Parameters Determined Using Compartmental Analysis (Major Surgeries)
|
|
|
- Collin Benjamin Banks
- 5 years ago
- Views:
Transcription
1 Supporting Information Table SI. Individual rfixfc Pharmacokinetic Parameters Determined Using Compartmental Analysis (Major Surgeries) Subject ID Study arm * Actual dose (iu/kg) Terminal half-life (h) Clearance (ml/h/kg) Incremental recovery (iu/dl per iu/kg) Time to 1% (d) rfixfc, recombinant factor IX Fc fusion protein; FIX, factor IX. * Subjects requiring major surgery who did not transfer from Arms 1 3 underwent a 120-hour washout period (of their pre-study FIX therapy), 4 weeks before the scheduled surgery, followed by a pharmacokinetic assessment with 50 iu/kg of rfixfc. Blood samples were collected up to 168 hours after the infusion to determine the individual pharmacokinetic profile. Subjects who intended to continue study participation in another treatment arm following surgery underwent initial pharmacokinetic testing as described for that arm. The arithmetic mean terminal half-life observed in the pharmacokinetics subgroup (n=22) of the B-LONG study was hours ( The average terminal half-life observed in the major surgery cohort (n=12) was shorter because the sampling duration for the majority of subjects was shorter than the 240 hours used in the pharmacokinetics subgroup of B-LONG. 1
2 Table SII. Individual Subjects rfixfc Surgical Dosing Regimens * Subject ID Presurgery dose 0 Day Subsequent dose ND 61 7 ND 44 8 ND 44 8 ND 44 8 ND 44 8 ND ND ND ND ND 66 0 ND ND 66 0 ND ND ND ND 68 3 ND ND ND ND 39.8 ND ND ND ND ND ND ND ND ND ND 50 4 ND 50 4 ND 50 4 ND 50 4 ND ND ND 63 2 ND 63 2 ND 63 2 ND ND ND 95 3 ND 95 3 ND 95 3 ND ND ND 47 6 ND ND ND ND ND ND ND ND ; ; ; ; 16 9; 42 4; ND ND ND 51 3 ND ND 53 6 ND ND ND ND ND ND ND 58 3 ND 58 3 ND ND ND 58 3 ND ND ND ND ND 58 3 ND ; 49 4 ** ND ND 49 4 ND 45 5 ND 45 5 ND ND ND ND ND 43 9 rfixfc, recombinant factor IX Fc fusion protein; ND, no dose. * Actual dosing of rfixfc, with doses given in units of iu/kg. 2
3 Subject received an infusion of iu/kg rfixfc the day before surgery. Two of the infusions on Day 3 were administered to treat a bleeding episode. Subject underwent 2 surgical procedures, with the second surgery occurring 3 days after the first surgery. Dosing on the day of the first surgery until the second surgery is shown in the first row; dosing beginning on the day of the second surgery and during the subsequent 14 days is shown in the second row. Dose urgently self-administered by the subject to treat bleeding from trauma site. ** Dose administered immediately prior to surgery. Unauthorised dose administered by the surgeon. Dose administered in accordance with the investigator s instructions, which were given before the investigator became aware of the unauthorised dose administered the previous evening. 3
4 Additional surgery narratives Subject 4 Subject 4, a 34-year-old male, underwent total left knee replacement. Four-hundred six days (~14 months) prior to surgery, the subject enrolled in the nonsequential pharmacokinetic subgroup of Arm 1. Medical history of note included decreased motion in both elbows, both knees, and both ankles; arthropathy of the knees, ankles, and elbows; and muscle wasting of the left arm and both upper legs. Surgical history included on-study dental extraction 151 days (~5 months) prior to surgery without incident (minor surgery subject 4 in Table IV). Prior to surgery, the subject received an initial prophylaxis regimen of ~50 iu/kg once weekly. Following 2 spontaneous bleeding episodes, the subject s prophylaxis dose was adjusted to ~60 iu/kg once weekly starting from ~2 months prior to surgery. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was <100 ml, and postoperative blood loss was approximately 75 ml. The dosing regimen consisted of a presurgery dose of iu/kg, iu/kg 4 hours later, and iu/kg on postoperative Days 1 and 2. The subject received iu/kg every other day on Days 4 6 postsurgery. The subject received 39 7 iu/kg on postoperative Day 7, 61 0 iu/kg on Day 8, 62 5 iu/kg every day on Days 9 13, and 63 6 iu/kg on postoperative Day 14. The subject did not receive treatment with recombinant factor IX Fc fusion protein (rfixfc) on Days 3 and 5 postsurgery. No serious adverse events were reported during the postoperative period. Subject 5 Subject 5, a 30-year-old male, underwent total right knee arthroplasty. One-hundred three days (~3 months) prior to surgery, the subject enrolled in Arm 4. Medical history of note included 4
5 hepatitis C, broken back, epilepsy with tonic clonic seizures, and a recent staphylococcus infection. Surgical history included bilateral release of right knee, complete hip replacement, left knee arthroscopic surgery, and spinal fusion. Prior to surgery, the subject received an initial prophylaxis regimen of ~70 iu/kg once weekly. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 250 ml, and postoperative blood loss was 0 ml. The dosing regimen consisted of a presurgery dose of iu/kg and 67 8 iu/kg every day for Days 1 3 postsurgery. The subject received 61 0 iu/kg daily on postoperative Days 4 7 and 59 6 iu/kg on postoperative Day 8. On Day 3, the subject received 3 total units of red blood cells (RBCs) due to low haemoglobin levels, as stated by the attending physician. No serious adverse events were reported during the postoperative period. Subject 6 Subject 6, a 35-year-old male, underwent right knee arthroscopy. One-hundred two days (~3 months) prior to surgery, the subject enrolled in the sequential pharmacokinetic subgroup of Arm 1. Medical history of note included human immunodeficiency virus (HIV), hypertension, diabetes mellitus, haemophilic arthropathy, right knee medial/lateral meniscal tear, acute subdural haematoma of the left frontoparietal region, grand mal seizure secondary to subdural haematoma, and a recent upper respiratory tract infection. Surgical history included appendectomy, synovectomy, chondroplasty of the right knee, and left frontal craniotomy for the evacuation of subdural haematoma. Prior to surgery, the subject received an initial prophylaxis regimen of iu/kg once weekly. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 10 ml, and postoperative blood loss data were not provided. The dosing regimen consisted of a presurgery dose of
6 iu/kg, 64 8 iu/kg 5 hours later, and 50 4 iu/kg on postoperative Days 1 and 2. The subject received 50 4 iu/kg every other day on postoperative Days 3 13 and on Day 14. The subject did not receive treatment with rfixfc on Days 4, 6, 8, 10, and 12 postsurgery. No serious adverse events were reported during the postoperative period. Subject 7 Subject 7, a 50-year-old male, underwent arthroscopic subtalar fusion of the right ankle. Twohundred forty-three days (~8 months) prior to surgery, the subject enrolled in Arm 3. Medical history of note included seizure disorder and haemophilic arthropathy. Surgical history included left ankle fusion, left elbow replacement, open reduction and internal fixation for left femur spiral fracture, right ankle fusion, total left knee arthroplasty, and total left knee arthroplasty revision. Prior to surgery, the subject received episodic treatment of iu/kg for bleeding episodes as they occurred. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was <5 ml, and postoperative blood loss was 0 ml. The dosing regimen consisted of a presurgery dose of iu/kg, 79 5 iu/kg 8 hours later, and 79 5 iu/kg every day for Days 1 3 postsurgery. The subject received 60 4 iu/kg on postoperative Day 5 and 63 2 iu/kg every other day on postoperative Days The subject did not receive treatment with rfixfc on Days 4, 7, 9, 11, 13, and 14 postsurgery. No serious adverse events were reported during the postoperative period. Subject 8 Subject 8, a 17-year-old male, underwent external fixation of the right knee. Ninety-eight days (~3 months) prior to surgery, the subject enrolled in Arm 4. Medical history of note included 6
7 severe arthropathy of the right knee, muscle atrophy of the right leg with flexion of the right knee, and asthma. Prior to surgery, the subject received an initial prophylaxis regimen of ~50 iu/kg once weekly. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 100 ml, and postoperative blood loss was 0 ml. The dosing regimen consisted of a presurgery dose of iu/kg, 95 3 iu/kg 12 hours later, and 95 3 iu/kg on Day 1 postsurgery. The subject received 95 3 iu/kg every other day on postoperative Days 2 8 and 47 6 iu/kg on postoperative Days 12 and 14. The subject did not receive treatment with rfixfc on Days 3, 5, 7, 9, 10, 11, and 13 postsurgery. No serious adverse events were reported during the postoperative period. Subject 9 Subject 9, a 54-year-old male, underwent right arm tendon transfer. One-hundred sixty-three days (~5 months) prior to surgery, the subject enrolled in the nonsequential pharmacokinetic subgroup of Arm 1. Medical history of note included hepatitis C, left and right elbow arthropathy, left ankle prosthesis, fixed subtalar joint right ankle, and haemophilic arthropathy. Surgical history included arthroscopic menisectomy on the right knee, extraction of subcutaneous pins, surgical fixation of the right foot, and a triple arthrodesis of the left ankle. Prior to surgery, the subject received an initial prophylaxis regimen of ~50 iu/kg once weekly. When baseline pharmacokinetic results became available, the dose was changed to ~20 iu/kg weekly. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 130 ml, and postoperative blood loss was approximately 40 ml. The dosing regimen consisted of a presurgery dose of 82 1 iu/kg, 60 7 iu/kg 6 hours later, and 41 1 iu/kg on Days 1 and 2 postsurgery. The subject received 21 2 iu/kg every day on 7
8 postoperative Days 3 7 and 42 3 iu/kg on postoperative Day 14. The subject did not receive treatment with rfixfc on Days 8 13 postsurgery. No serious adverse events were reported during the postoperative period. Subject 10 Subject 10, a 43-year-old male, underwent large intestine fistula closure. Sixty-seven days (~2 months) prior to surgery, the subject enrolled in Arm 4. Medical history of note included abdominal haematoma (evacuated 3 times), rectal/colon fistula, hepatitis B, previous surgery scars on the abdomen, right and left knee joint deformity, left knee joint ankylosis, right ankle joint limitation of motion, atrophy of the muscle of the right thigh, haematoma at left leg muscle, and infection at the left thigh fracture site. Surgical history included surgery on the abdomen (middle and lumbar area) due to fistula, plate fixation on left thigh fracture site, and right knee arthroscopic synovectomy. Prior to surgery, the subject received an initial prophylaxis regimen of ~26 iu/kg every 5 days. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 300 ml, and postoperative blood loss was approximately 500 ml. The postoperative bleeding was primarily due to diffuse oozing from the surgical wound; the incision was midline from sternum to the pubic bone and approximately the lower one-third of the wound was left open with the drain inserted, to heal by secondary intention. The subject received 7 total units of fresh frozen plasma and RBCs (2 units intraoperatively and an additional 5 units within 2 weeks of surgery). The dosing regimen consisted of iu/kg the day before surgery, a presurgery dose of 59 3 iu/kg, 50 8 iu/kg 9 hours later, 50 8 iu/kg 12 hours later, and 25 4 iu/kg on Day 2 postsurgery. The subject received 3 doses of 50 8 iu/kg each on postoperative Day 3 (2 of these were administered to treat a 8
9 bleeding episode), 2 doses of 50 8 iu/kg and 33 9 iu/kg on postoperative Day 4, and 2 doses of 42 4 iu/kg each every day on postoperative Days 5 7. On Days 8 and 9, the subject received 42 4 iu/kg. On Day 10, the subject received 2 doses of 42 4 iu/kg each and 1 dose of 16 9 iu/kg. On Days 11 13, the subject received 50 8 iu/kg twice daily. On Day 14, the subject received 1 dose of 50 8 iu/kg and a second dose of 25 4 iu/kg. The subject did not receive treatment with rfixfc on Day 1 postsurgery. No serious adverse events were reported during the postoperative period. During the postoperative period, the subject received the study-prohibited medication prothrombin complex concentrate, and was subsequently withdrawn due to noncompliance with the study protocol. As with all major surgery subjects in the study, this subject also tested negative for inhibitor development. Subject 11 Subject 11, a 24-year-old male, underwent 2 surgical procedures (incision and drainage of an abscessed pilonidal cyst; incision and drainage of a dental abscess) on 2 separate dates. Twohundred sixteen days (~7 months) prior to surgery, the subject enrolled in the nonsequential pharmacokinetic subgroup of Arm 1. Medical history of note included right elbow and right knee arthropathy and right thigh pseudo-tumour. Prior to surgery, the subject received an initial prophylaxis regimen of ~54 iu/kg (actual dose) once weekly. The first surgical procedure was incision and drainage of an abscessed pilonidal cyst. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 0 ml, and postoperative blood loss was 0 ml. The dosing regimen consisted of a presurgery dose of 51 3 iu/kg and 51 3 iu/kg on postoperative Days 2 and 4. The subject received 53 6 iu/kg on postoperative Days 7 and 14. The subject did not receive treatment with rfixfc on Days 1, 3, 5, 9
10 6, and 8 13 postsurgery. By definition, pilonidal cyst, the event which led to the surgery, was considered a serious adverse event that occurred during the initial portion of the surgical period. This event was assessed by the investigator as unrelated to the study drug. No serious adverse events were reported during the postoperative period. The subject underwent a second surgical procedure (incision and drainage of a dental abscess, with multiple dental extractions) 29 days after the first surgery. The surgery was uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 0 ml, and postoperative blood loss was 0 ml. The dosing regimen consisted of a presurgery dose of 58 3 iu/kg and 58 3 iu/kg on postoperative Days 1, 3, 7, and 13. The subject did not receive treatment with rfixfc on Days 2, 4 6, 8 12, and 14 postsurgery. He received antifibrinolytic treatment as systematic adjuvant therapy. By definition, dental abscess, the event which led to the surgery, was considered a serious adverse event that occurred during the initial portion of the surgical period. This event was assessed by the investigator as unrelated to the study drug. No serious adverse events were reported during the postoperative period. Subject 12 Subject 12, a 22-year-old male, underwent 2 surgical procedures (debridement, fracture dislocation, partial amputation; amputation of left middle finger) on 2 separate dates. Threehundred sixty-four days (~12 months) prior to surgery, the subject enrolled in the nonsequential pharmacokinetic subgroup of Arm 1. Medical history of note included bee sting allergy and haemophilic arthropathy. Prior to surgery, the subject received an initial prophylaxis regimen of ~54 iu/kg (actual dose) once weekly. On Day 0 (day of first surgery), the subject underwent 10
11 emergency surgery following a work-related accident of crushing injury to his finger. Surgery included debridement and fracture dislocation, and partial amputation. During the first surgery on the left middle finger, it became apparent that amputation of this finger was necessary, but consent had not been obtained for this procedure. A second major surgery, amputation of the left middle finger through proximal interphalangeal joint, was performed 3 days after the first surgery. Both surgeries were uneventful, and haemostatic response was evaluated as excellent. Estimated intraoperative blood loss was 0 ml, and postoperative blood loss was 0 ml for both surgeries. Immediately after the accidental injury on the day of the first surgery, the subject urgently self-administered iu/kg of rfixfc for bleeding from the trauma site at 15:00 hours. At 19:00 hours on the same day, the subject received an additional dose of 49 4 iu/kg immediately prior to surgery, as indicated by the subject s FIX levels and per investigator s instructions. At 21:50 hours, an unauthorised dose of 98 7 iu/kg was given by the surgeon, which was not discussed with the haematologist/investigator. At 09:15 hours on Day 1 postsurgery, the subject was dosed with 49 3 iu/kg in accordance with the investigator s instructions, as the investigator was not yet aware of the unauthorised dose given the previous evening. The dosing regimen on the subsequent days consisted of 49 3 iu/kg on postoperative Day 2, 56 3 iu/kg on Day 3, 49 4 iu/kg on Day 4, and 41 9 iu/kg on Day 5 postsurgery. The subject received 49 4 iu/kg on postoperative Day 7 and 45 5 iu/kg on Days 9 and 11 postsurgery. On Day 17 (14 days after the second surgery), the subject received 43 9 iu/kg. The subject did not receive treatment with rfixfc on Days 6, 8, 10 and postsurgery. By definition, limbcrushing injury, the event which led to the surgery, was considered a serious adverse event that occurred during the initial portion of the surgical period. This event was assessed by the 11
12 investigator as unrelated to the study drug. No serious adverse events were reported during the postoperative period. 12
Haemophilia and Orthopaedic Surgery. Brett Halliday Orthopaedic Surgeon Holy Spirit Northside and Royal Brisbane Hospitals
 Haemophilia and Orthopaedic Surgery Brett Halliday Orthopaedic Surgeon Holy Spirit Northside and Royal Brisbane Hospitals Disclaimer Director of Education OTC South Pacific No funds or company support
Haemophilia and Orthopaedic Surgery Brett Halliday Orthopaedic Surgeon Holy Spirit Northside and Royal Brisbane Hospitals Disclaimer Director of Education OTC South Pacific No funds or company support
SCHEDULE OF BENEFITS GAI
 SCHEDULE OF BENEFITS The Schedule of Benefits provides a brief outline of the coverage and benefits including the maximum benefit amount, benefit periods, and any limitations applicable to benefits provided
SCHEDULE OF BENEFITS The Schedule of Benefits provides a brief outline of the coverage and benefits including the maximum benefit amount, benefit periods, and any limitations applicable to benefits provided
CASE REPORT. Antegrade tibia lengthening with the PRECICE Limb Lengthening technology
 CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Policy/ Purpose: Definitions: (Definitions of acronyms or specialized terminology) Instructions:
 Title: Surgical Procedure Scheduling After 2200 Hours by Central Processing Document #: 5962 Version: 1 Facility: St. Charles Bend Page 1 of 5 Owner: Roberts, Andrew,Manager Central Processing Effective
Title: Surgical Procedure Scheduling After 2200 Hours by Central Processing Document #: 5962 Version: 1 Facility: St. Charles Bend Page 1 of 5 Owner: Roberts, Andrew,Manager Central Processing Effective
Post test for O&P 2 Hrs CE. The Exam
 Post test for O&P 2 Hrs CE The Exam This examination is taken in "open book" format. That means you are free to answer the questions after research or discussion with your fellow workers. We feel this
Post test for O&P 2 Hrs CE The Exam This examination is taken in "open book" format. That means you are free to answer the questions after research or discussion with your fellow workers. We feel this
Power to Transform Outcomes
 CASE STUDIES CASE STUDY Courtesy of Dr Parihar Consultant Orthopaedic Surgeon, Center for Limb Lengthening & Reconstruction, Mangal Anand Hospital, Mumbai, India Clinical particulars 42-year-old female
CASE STUDIES CASE STUDY Courtesy of Dr Parihar Consultant Orthopaedic Surgeon, Center for Limb Lengthening & Reconstruction, Mangal Anand Hospital, Mumbai, India Clinical particulars 42-year-old female
Institute for Bone, Joint Replacement, Orthopaedics Spine and Sports Medicine
 24-Hour Helpline: 011-30403040 BLK Super Speciality Hospital Pusa Road, New Delhi - 110005 (India). www.blkhospital.com Institute for Bone, Joint Replacement, Orthopaedics Spine and Sports Medicine Introduction
24-Hour Helpline: 011-30403040 BLK Super Speciality Hospital Pusa Road, New Delhi - 110005 (India). www.blkhospital.com Institute for Bone, Joint Replacement, Orthopaedics Spine and Sports Medicine Introduction
Chapter 12 Worksheet Code It
 Class: Date: Chapter 12 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. The type of fracture corresponds to the type of treatment. 2. An open fracture is always treated
Class: Date: Chapter 12 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. The type of fracture corresponds to the type of treatment. 2. An open fracture is always treated
Case Study: David. Conditions Treated Femoral Neck Fracture with Avascular Necrosis of the Hip. Age Range During Treatment 16 Years
 Case Study: David Conditions Treated Femoral Neck Fracture with Avascular Necrosis of the Hip Age Range During Treatment 16 Years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of
Case Study: David Conditions Treated Femoral Neck Fracture with Avascular Necrosis of the Hip Age Range During Treatment 16 Years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of
Complications of Treatment: Nonsurgical and Surgical
 Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
2013 MCT CPC-H Quiz #8 Chapters 13 and 14
 2013 MCT CPC-H Quiz #8 Chapters 13 and 14 Name: Date: Instructor: Score: 1. A female patient presents to the outpatient clinic for excision of a 4.8 cm malignant melanoma of the left inner thigh. A 6 cm
2013 MCT CPC-H Quiz #8 Chapters 13 and 14 Name: Date: Instructor: Score: 1. A female patient presents to the outpatient clinic for excision of a 4.8 cm malignant melanoma of the left inner thigh. A 6 cm
Musculoskeletal System
 Musculoskeletal System CPT CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the
Musculoskeletal System CPT CPT copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the
The Orthopaedic Coding Coach 2010 Orthopaedic Coding Tips By Karen Zupko & Associates
 The Orthopaedic Coding Coach 2010 Orthopaedic Coding Tips By Karen Zupko & Associates Use of Modifiers October 14, 2010 I was recently told that when applying more than one modifier, they should be listed
The Orthopaedic Coding Coach 2010 Orthopaedic Coding Tips By Karen Zupko & Associates Use of Modifiers October 14, 2010 I was recently told that when applying more than one modifier, they should be listed
The Practical Use of LIGASANO white in Plastic Surgery
 Practical experience 3 The Practical Use of LIGASANO white in Plastic Surgery Emergency Hospital of Mureş County, Romania Reports of practical experience from the burn center and plastic surgery department
Practical experience 3 The Practical Use of LIGASANO white in Plastic Surgery Emergency Hospital of Mureş County, Romania Reports of practical experience from the burn center and plastic surgery department
Osteoarthrosis, unspecified whether generalized or localized, lower leg. Osteoarthrosis, localized, not specified whether primary or secondary, pelvic
 Page 1 Appendix TABLE E-1 Codes (and Definitions) in Humana Database Used for Study Inclusion and Exclusion of Patients Who Underwent,, or 1 to 2-Level Inclusion ICD-9-P-8154 Total knee replacement ICD-9-D-71596
Page 1 Appendix TABLE E-1 Codes (and Definitions) in Humana Database Used for Study Inclusion and Exclusion of Patients Who Underwent,, or 1 to 2-Level Inclusion ICD-9-P-8154 Total knee replacement ICD-9-D-71596
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatric Surgery. Procedure List. As Of.
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Ankle Replacement Surgery
 Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
CASE NO: 1 PATIENT DETAILS : Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO :
 CASE NO: 1 PATIENT DETAILS : Name : XXXX Age : 53yr Sex : Female Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO : 201518441 CHIEF COMPLAINTS : - Pain in the right knee since
CASE NO: 1 PATIENT DETAILS : Name : XXXX Age : 53yr Sex : Female Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO : 201518441 CHIEF COMPLAINTS : - Pain in the right knee since
Prophylaxis & Arthropathy
 Prophylaxis & Arthropathy On-Demand and Prophylaxis Treatment Coagulation factor replacement may be given when a bleed occurs (on-demand therapy) or before bleeding occurs, to prevent bleeds (prophylactic
Prophylaxis & Arthropathy On-Demand and Prophylaxis Treatment Coagulation factor replacement may be given when a bleed occurs (on-demand therapy) or before bleeding occurs, to prevent bleeds (prophylactic
injury poisoning and certain other (s00-t98)
 1 of 13 1 injury poisoning and certain other consequences of external causes (s00-t98) ICD S T P10-P15 ( ) O70-O71 ( ) S T injuries to the head (s00-s09) injuries to the neck (s10-s19) injuries to the
1 of 13 1 injury poisoning and certain other consequences of external causes (s00-t98) ICD S T P10-P15 ( ) O70-O71 ( ) S T injuries to the head (s00-s09) injuries to the neck (s10-s19) injuries to the
A Patient s Guide to Adult Forearm Fractures
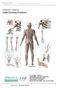 A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Issue Number: 0157 Date: 10/01/219
 Bulletin Changes to CCSD Schedule of Procedures Issue Number: 0157 Date: 10/01/219 The CCSD has reviewed requests to the CCSD Procedure Schedule for the months of December/January and has agreed on the
Bulletin Changes to CCSD Schedule of Procedures Issue Number: 0157 Date: 10/01/219 The CCSD has reviewed requests to the CCSD Procedure Schedule for the months of December/January and has agreed on the
Hemofílie. MUDr.Ivan Vonke, MBA OKH, Nemocnice České Budějovice, a.s.
 Hemofílie e MUDr.Ivan Vonke, MBA OKH, Nemocnice České Budějovice, a.s. Hemophilia Incidence: Hemopilia A (deficiency of factor VIII): 1-2 of 10 000 male newborns in all ethnic groups Hemophilia B (deficiency
Hemofílie e MUDr.Ivan Vonke, MBA OKH, Nemocnice České Budějovice, a.s. Hemophilia Incidence: Hemopilia A (deficiency of factor VIII): 1-2 of 10 000 male newborns in all ethnic groups Hemophilia B (deficiency
ACCIDENT CLAIM DOCTOR S STATEMENT
 ACCIDENT CLAIM DOCTOR S STATEMENT For Official Use _ G E L S Name of Life Assured: NRIC/ Passport No.: 1. of Accident: of first consultation for this current condition: (s) of subsequent consultation(s):
ACCIDENT CLAIM DOCTOR S STATEMENT For Official Use _ G E L S Name of Life Assured: NRIC/ Passport No.: 1. of Accident: of first consultation for this current condition: (s) of subsequent consultation(s):
Table showing JSB guidelines (10 th Edition) for the assessment of general damages in personal injury cases
 Table showing JSB guidelines (10 th Edition) for the assessment of general damages in personal injury cases All personal injury damages will depend on all or some of the following factors: The severity
Table showing JSB guidelines (10 th Edition) for the assessment of general damages in personal injury cases All personal injury damages will depend on all or some of the following factors: The severity
Hong Kong College of Emergency Medicine OSCE July 2010
 Case 1 A 70 year old gentleman was taking warfarin for his past history of right leg deep vein thrombosis. He slipped and fell and suffered from head injury. He was sent to A&E and his GCS was 9/15 on
Case 1 A 70 year old gentleman was taking warfarin for his past history of right leg deep vein thrombosis. He slipped and fell and suffered from head injury. He was sent to A&E and his GCS was 9/15 on
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Page 1 of 6. Appendix 1
 Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
ASPEN MEDICAL SURGERY REGINA
 It is hereby certified that ASPEN MEDICAL SURGERY REGINA Has successfully completed an inspection as is required under the College s Bylaw 26.1 and is therefore approved as a Non Hospital Treatment Facility
It is hereby certified that ASPEN MEDICAL SURGERY REGINA Has successfully completed an inspection as is required under the College s Bylaw 26.1 and is therefore approved as a Non Hospital Treatment Facility
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 5 Basic Surgical Procedures Key Points 2 5.1 Wound Management Many important procedures can be performed under local anesthesia and do not require a surgical specialist
Surgical Care at the District Hospital 1 5 Basic Surgical Procedures Key Points 2 5.1 Wound Management Many important procedures can be performed under local anesthesia and do not require a surgical specialist
ICD-10 Service Line Overview Musculoskeletal
 ICD-10 Service Line Overview Musculoskeletal ICD-10 incorporates much greater clinical detail and specificity as well as updated terminology to be consistent with current clinical practices. ICD-10-CM
ICD-10 Service Line Overview Musculoskeletal ICD-10 incorporates much greater clinical detail and specificity as well as updated terminology to be consistent with current clinical practices. ICD-10-CM
Table of Compensation for Injury 1/2015
 Table of Compensation for 1/2015 Valid from 01.04.2015 1. CRANIAL INJURIES 1.1 Cranial bone fractures: a) fracture of cranial dome 10 b) fracture of cranial base 15 c) fracture of cranial dome and base
Table of Compensation for 1/2015 Valid from 01.04.2015 1. CRANIAL INJURIES 1.1 Cranial bone fractures: a) fracture of cranial dome 10 b) fracture of cranial base 15 c) fracture of cranial dome and base
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
Arteriovenostomy for renal dialysis 39.27, 39.42
 Surgery categories NHSN Surgery codes (Reference: NHSN Operative Procedure Category Mappings to ICD-9-CM Codes, October 2010 www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf) Operative aortic aneurysm
Surgery categories NHSN Surgery codes (Reference: NHSN Operative Procedure Category Mappings to ICD-9-CM Codes, October 2010 www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf) Operative aortic aneurysm
Surgical Privileges Form Orthopedic Surgery CLINICAL PRIVILEGES REQUEST Applicant s Name:. Scope of Practice:... License No. (If Any):... Facility:..
 Name of applicant Surgical Privileges Form Orthopedic Surgery CLINICAL PRIVILEGES REQUEST Applicant s Name:. Scope of Practice:... License No. (If Any):..... Facility:.. Requested Recommended Not Privileges
Name of applicant Surgical Privileges Form Orthopedic Surgery CLINICAL PRIVILEGES REQUEST Applicant s Name:. Scope of Practice:... License No. (If Any):..... Facility:.. Requested Recommended Not Privileges
Urgent Cases and Foreign Bodies
 Urgent Cases and Foreign Bodies Catherine J. Brandon, MD, MS University of Michigan Ann Arbor, MI, USA Introduction: Patients added on to the schedule from the emergency department or as urgent add-on
Urgent Cases and Foreign Bodies Catherine J. Brandon, MD, MS University of Michigan Ann Arbor, MI, USA Introduction: Patients added on to the schedule from the emergency department or as urgent add-on
Appendix C Podiatriac Services
 Appendix C Podiatriac Services CPT/ HCPCS Codes Description Auth required Y or N Mod Service Limits Age Limits Notes 10021-10022 Fine Needle Aspiration w/ or w/o imaging guidance 10060-10061 10120-10121
Appendix C Podiatriac Services CPT/ HCPCS Codes Description Auth required Y or N Mod Service Limits Age Limits Notes 10021-10022 Fine Needle Aspiration w/ or w/o imaging guidance 10060-10061 10120-10121
Tibial Shaft Fractures
 Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
MICROCURRENT TREATMENT OF SCARS
 MICROCURRENT TREATMENT OF SCARS ALLEN BERGER, DC CONFLUENCE WELLNESS CENTER PC 1776 S JACKSON ST. STE 418 DENVER CO 80210 303-394-4204 ALLEN.R.BERGER@GMAIL.COM WWW.CONFLUENCEWELLNESS.COM PATIENT ONE 64
MICROCURRENT TREATMENT OF SCARS ALLEN BERGER, DC CONFLUENCE WELLNESS CENTER PC 1776 S JACKSON ST. STE 418 DENVER CO 80210 303-394-4204 ALLEN.R.BERGER@GMAIL.COM WWW.CONFLUENCEWELLNESS.COM PATIENT ONE 64
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
The First rfviii WITH A PROLONGED HALF-LIFE
 Visit ELOCTATEpro.com for more information The First rfviii WITH A PROLONGED HALF-LIFE Indications ELOCTATE [Antihemophilic Factor (Recombinant), Fc Fusion Protein] is a recombinant DNA derived, antihemophilic
Visit ELOCTATEpro.com for more information The First rfviii WITH A PROLONGED HALF-LIFE Indications ELOCTATE [Antihemophilic Factor (Recombinant), Fc Fusion Protein] is a recombinant DNA derived, antihemophilic
ผศ.นพ.ธรา ธรรมโรจน ภาควชาออรโธปดกส คณะแพทยศาสตร, มหาวทยาล!ยขอนแก#น
 1972 ผศ.นพ.ธรา ธรรมโรจน ภาควชาออรโธปดกส คณะแพทยศาสตร, มหาวทยาล!ยขอนแก#น Common Fracture in lower Extremity Common Fracture in Adult(Traumatic Associated Fracture) Fracture of Tibia and Fibular Fracture
1972 ผศ.นพ.ธรา ธรรมโรจน ภาควชาออรโธปดกส คณะแพทยศาสตร, มหาวทยาล!ยขอนแก#น Common Fracture in lower Extremity Common Fracture in Adult(Traumatic Associated Fracture) Fracture of Tibia and Fibular Fracture
Emergency Medicine Scope of Practice
 Emergency Medicine Scope of Practice All Physician Assistants working in Emergency Medicine will encounter a wide variety of non acute, urgent and emergent patient complaints and conditions. Given the
Emergency Medicine Scope of Practice All Physician Assistants working in Emergency Medicine will encounter a wide variety of non acute, urgent and emergent patient complaints and conditions. Given the
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
PAIN POINT CHECKLIST THE ULTIMATE TO MAXIMISE COMPENSATION FROM YOUR CLAIM
 THE ULTIMATE PAIN POINT CHECKLIST TO MAXIMISE COMPENSATION FROM YOUR CLAIM A visual checklist for personal injury claimants that allows users to comprehensively list and discuss their injuries with their
THE ULTIMATE PAIN POINT CHECKLIST TO MAXIMISE COMPENSATION FROM YOUR CLAIM A visual checklist for personal injury claimants that allows users to comprehensively list and discuss their injuries with their
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
bilateral, both before below elbow twice a day below knee bedrest
 Abbreviations Student Name: A approximately assessment assist active active assist abdominal aortic aneurysm active assistive range of motion abduction/adduction acromioclavicular joint anterior cruciate
Abbreviations Student Name: A approximately assessment assist active active assist abdominal aortic aneurysm active assistive range of motion abduction/adduction acromioclavicular joint anterior cruciate
Average Gross Charges ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W CC ,254 ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W MCC - 280
 ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W CC - 281 15,254 ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W MCC - 280 24,827 ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W/O CC/MCC - 282 11,575 AFTERCARE,
ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W CC - 281 15,254 ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W MCC - 280 24,827 ACUTE MYOCARDIAL INFARCTION, DISCHARGED ALIVE W/O CC/MCC - 282 11,575 AFTERCARE,
Cluster - 26 ORTHOPEDICS. X Ray of Affected Limb, MIR of Shoulder
 Sr.No Package no 1708 26.1 Orthopeidc 1709 26.2 Orthopeidc Sub speciality Procedure name Pre-Operative Investigation AC joint reconstruction/ Stabilization/ Acromionplasty (Nonoperative management is recommended
Sr.No Package no 1708 26.1 Orthopeidc 1709 26.2 Orthopeidc Sub speciality Procedure name Pre-Operative Investigation AC joint reconstruction/ Stabilization/ Acromionplasty (Nonoperative management is recommended
Ankle Arthritis PATIENT INFORMATION. The ankle joint. What is ankle arthritis?
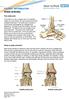 PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
Early Results of Total Knee Replacements:
 Early Results of Total Knee Replacements: "A Clinical and Radiological Evaluation" K.S. Dhillon, FRCS* Jamal, MS* S. Bhupinderjeet, MBBS** * Dept. of Orthopaedic Surgery University of Malaya, Kuala Lumpur
Early Results of Total Knee Replacements: "A Clinical and Radiological Evaluation" K.S. Dhillon, FRCS* Jamal, MS* S. Bhupinderjeet, MBBS** * Dept. of Orthopaedic Surgery University of Malaya, Kuala Lumpur
OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries. Differentiate when an orthopedic injury is a medical emergency
 1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma >
 Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma > Version 5 December 2013 1 Version control Version number Date Amendments
Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma > Version 5 December 2013 1 Version control Version number Date Amendments
ABOS/CORD Surgical Skills Assessment Program
 American Board of Orthopaedic Surgery Establishing Education & Performance Standards for Orthopaedic Surgeons ABOS/CORD Surgical Skills Assessment Program ABOS Essential Knowledge, Skills, and Behaviors
American Board of Orthopaedic Surgery Establishing Education & Performance Standards for Orthopaedic Surgeons ABOS/CORD Surgical Skills Assessment Program ABOS Essential Knowledge, Skills, and Behaviors
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Williams CM, Maher CG, Latimer J, et al. Efficacy
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Williams CM, Maher CG, Latimer J, et al. Efficacy
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation
 Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
Femoral Fractures in Adolescents: A Comparison of Four Methods of Fixation By Leonhard E. Ramseier, MD, Joseph A. Janicki, MD, Shannon Weir, BSc, and Unni G. Narayanan, MBBS, MSc, FRCSC Investigation performed
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
Ultrasound ICD-10-CM
 Ultrasound ICD-10-CM Clinical Documentation Guides Brought to you by www.codingstrategies.com The Resource for Physician and Outpatient Coding, Compliance & ICD-10-CM OTHER CLINICAL DOCUMENTATION GUIDES
Ultrasound ICD-10-CM Clinical Documentation Guides Brought to you by www.codingstrategies.com The Resource for Physician and Outpatient Coding, Compliance & ICD-10-CM OTHER CLINICAL DOCUMENTATION GUIDES
Columbia/NYOH Department of Orthopaedics Shoulder, Elbow, and Sports Medicine Service Competency Requirements
 Updated 2/8/10 Columbia/NYOH Department of Orthopaedics Shoulder, Elbow, and Sports Medicine Service Competency Requirements Patient Care Faculty will evaluate the resident s ability to obtain History,
Updated 2/8/10 Columbia/NYOH Department of Orthopaedics Shoulder, Elbow, and Sports Medicine Service Competency Requirements Patient Care Faculty will evaluate the resident s ability to obtain History,
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
ICD-10-PCS Coding Guidelines
 ICD-10-PCS Coding Guidelines Table of Contents A. Conventions....1 B. Medical and Surgical Section Guidelines......4 2. Body System...4 3. Root Operation....5 4. Body Part...9 5. Approach..12 6. Device...13
ICD-10-PCS Coding Guidelines Table of Contents A. Conventions....1 B. Medical and Surgical Section Guidelines......4 2. Body System...4 3. Root Operation....5 4. Body Part...9 5. Approach..12 6. Device...13
CEU Final Exam for Code It! Sixth Edition
 CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
Multiple joint reconstructions in one patient: computer-assisted simultaneous procedures
 Case Report Page 1 of 5 Multiple joint reconstructions in one patient: computer-assisted simultaneous procedures Mahmoud Hafez, Hosamuddin Hamza, Raid Aumran Essa The Orthopaedic Department, October 6
Case Report Page 1 of 5 Multiple joint reconstructions in one patient: computer-assisted simultaneous procedures Mahmoud Hafez, Hosamuddin Hamza, Raid Aumran Essa The Orthopaedic Department, October 6
A TIBIAL VALGUS OSTEOTOMY
 PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO A TIBIAL VALGUS OSTEOTOMY and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office YOU HAVE INCIPIENT INTERNAL OSTEOARTHRITIS OF THE
PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO A TIBIAL VALGUS OSTEOTOMY and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office YOU HAVE INCIPIENT INTERNAL OSTEOARTHRITIS OF THE
23 rd Annual LLRS Meeting
 23 rd Annual LLRS Meeting Daniel Schlatterer, DO Vice Chair, Dept. of Ortho Surgery Director, Ortho Trauma Atlanta Medical Center Atlanta, Georgia Use of Integra and Split Thickness Skin Graft for Coverage
23 rd Annual LLRS Meeting Daniel Schlatterer, DO Vice Chair, Dept. of Ortho Surgery Director, Ortho Trauma Atlanta Medical Center Atlanta, Georgia Use of Integra and Split Thickness Skin Graft for Coverage
Haemophilia. Management of Haemophiliac Arthropathy Orthopaedic Point of View. Epidemiology of Haemophilic joint disease
 Haemophilia Management of Haemophiliac Arthropathy Orthopaedic Point of View Dr. Alexander Chan Department of Orthopaedics & Traumatology Prince of Wales Hospital Deficiency of clotting factor VIII, and
Haemophilia Management of Haemophiliac Arthropathy Orthopaedic Point of View Dr. Alexander Chan Department of Orthopaedics & Traumatology Prince of Wales Hospital Deficiency of clotting factor VIII, and
Icd 10 left ankle arthroscopy
 P ford residence southampton, ny Icd 10 left ankle arthroscopy 07/21/2017 Laser sight for taurus pt111 g2 07/21/2017 News anchors leg shots 07/23/2017-Keflex and sulfa allergy-scorpio woman pisces man
P ford residence southampton, ny Icd 10 left ankle arthroscopy 07/21/2017 Laser sight for taurus pt111 g2 07/21/2017 News anchors leg shots 07/23/2017-Keflex and sulfa allergy-scorpio woman pisces man
ACTIVE IMMUNIZING AGENTS
 Therapeutic Injections and Immunizations Immunizations Immunizations are an excluded service for purposes of travel, employment and emigration, and may only be claimed if the injection is for a publicly
Therapeutic Injections and Immunizations Immunizations Immunizations are an excluded service for purposes of travel, employment and emigration, and may only be claimed if the injection is for a publicly
Posterior. Lumbar Fusion. Disclaimer. Integrated web marketing. Multimedia Health Education
 Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Pre-participation Physical Evaluation
 Pre-participation Physical Evaluation HISTORY FORM Date of Exam: Name Sex Age Date of Birth Grade School Sport(s) Address Phone Personal Physician In case of emergency, contact: Relationship Phone (H)
Pre-participation Physical Evaluation HISTORY FORM Date of Exam: Name Sex Age Date of Birth Grade School Sport(s) Address Phone Personal Physician In case of emergency, contact: Relationship Phone (H)
Differentialdianosis to CRPS Departmentdoctor Bo Biering-Sørensen, Pain Clinic, Neurological Department
 Differentialdianosis to CRPS Departmentdoctor Bo Biering-Sørensen, Pain Clinic, Neurological Department Dato (Sidehoved/fod) Case 1 36 year old man other ethnically background than Danish 2006 Left foot
Differentialdianosis to CRPS Departmentdoctor Bo Biering-Sørensen, Pain Clinic, Neurological Department Dato (Sidehoved/fod) Case 1 36 year old man other ethnically background than Danish 2006 Left foot
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION INTRODUCTION The anterior cruciate ligament (ACL) is one of the major stabilising ligaments in the knee. It is a strong rope like structure located in the centre
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION INTRODUCTION The anterior cruciate ligament (ACL) is one of the major stabilising ligaments in the knee. It is a strong rope like structure located in the centre
Orthopaedic & Rheumatologic Institute Outcomes
 Orthopaedic & Rheumatologic Institute 213 Outcomes Measuring Outcomes Promotes Quality Improvement Measuring and understanding outcomes of medical treatments promotes quality improvement. Cleveland Clinic
Orthopaedic & Rheumatologic Institute 213 Outcomes Measuring Outcomes Promotes Quality Improvement Measuring and understanding outcomes of medical treatments promotes quality improvement. Cleveland Clinic
Shoulder Arthroscopy
 Disclaimer This movie is an educational resource only and should not be used to make a decision on Shoulder Arthroscopy. All decisions about Arthroscopy must be made in conjunction with your surgeon or
Disclaimer This movie is an educational resource only and should not be used to make a decision on Shoulder Arthroscopy. All decisions about Arthroscopy must be made in conjunction with your surgeon or
Skilled Orthopaedic Team Improving Outcomes for Northern Michigan. MunsonHealthcare.org
 Skilled Orthopaedic Team Improving Outcomes for Northern Michigan A2 Surgeons Save Leg Munson Trauma team includes three orthopaedic traumatologists A3 Arm and Hand Trauma Hand surgeons collaborate with
Skilled Orthopaedic Team Improving Outcomes for Northern Michigan A2 Surgeons Save Leg Munson Trauma team includes three orthopaedic traumatologists A3 Arm and Hand Trauma Hand surgeons collaborate with
These are guidelines only and can be deviated from if it is thought to be in the patient s best interest.
 Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics Venous thromboembolism (VTE) is a recognised complication associated with inactivity and surgical procedures. Therefore, all
Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics Venous thromboembolism (VTE) is a recognised complication associated with inactivity and surgical procedures. Therefore, all
TOTAL KNEE ARTHROPLASTY (Total Knee Replacement) The Knee Joint
 (Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
(Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES
 ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
Hand injuries. The metacarpal bones may fracture through the base, shaft or the neck.
 Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Operations included in the National Joint Registry (NJR)
 Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma > Version 8 June 2018 1 Version control Version number Date Amendments 1
Operations included in the National Joint Registry (NJR) Quick links, go to: Hips > Knees > Ankles > Elbows > Shoulders > Trauma > Version 8 June 2018 1 Version control Version number Date Amendments 1
Shellie Sulzberger, LPN, CPC, ICDCT-CM. Tracy Bird, FACMPE, CPC, CPMA, CEMC
 Shellie Sulzberger, LPN, CPC, ICDCT-CM Tracy Bird, FACMPE, CPC, CPMA, CEMC Reasonable efforts have been made to provide the most accurate and current information on coding and documentation changes. However
Shellie Sulzberger, LPN, CPC, ICDCT-CM Tracy Bird, FACMPE, CPC, CPMA, CEMC Reasonable efforts have been made to provide the most accurate and current information on coding and documentation changes. However
Regions Hospital Delineation of Privileges Orthopaedic Surgery
 Regions Hospital Delineation of Orthopaedic Surgery Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Regions Hospital Delineation of Orthopaedic Surgery Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
TURNINGPOINT CLINICAL POLICY
 1 P a g e NOTE: For services provided on December 3, 2018 and after, Horizon Blue Cross Blue Shield of New Jersey ( Horizon BCBSNJ ) has contracted with TurningPoint Healthcare Solutions, LLC to conduct
1 P a g e NOTE: For services provided on December 3, 2018 and after, Horizon Blue Cross Blue Shield of New Jersey ( Horizon BCBSNJ ) has contracted with TurningPoint Healthcare Solutions, LLC to conduct
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
MUSCULOSKELETAL INJURIES
 WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
Orthopedic Surgery Clinical Privilege List
 Description of Service Alberta Health Services (AHS) Medical Staff who are specialists in Orthopedic Surgery (or its associated subspecialties) and have privileges in the Section of Orthopedic Surgery
Description of Service Alberta Health Services (AHS) Medical Staff who are specialists in Orthopedic Surgery (or its associated subspecialties) and have privileges in the Section of Orthopedic Surgery
JRI Thompson Hemiarthroplasty
 JRI ORTHOPAEDICS LTD 18 Churchill Way, 35A Business Park, Chapeltown, Sheffield, S35 2PY, UK Instructions for Use JRI Thompson Hemiarthroplasty Page 1 of 6 English 3 Page 2 of 6 Important Information Please
JRI ORTHOPAEDICS LTD 18 Churchill Way, 35A Business Park, Chapeltown, Sheffield, S35 2PY, UK Instructions for Use JRI Thompson Hemiarthroplasty Page 1 of 6 English 3 Page 2 of 6 Important Information Please
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Idelvion. (coagulation factor IX [recombinant], albumin fusion protein) New Product Slideshow
![Idelvion. (coagulation factor IX [recombinant], albumin fusion protein) New Product Slideshow Idelvion. (coagulation factor IX [recombinant], albumin fusion protein) New Product Slideshow](/thumbs/95/122489856.jpg) Idelvion (coagulation factor IX [recombinant], albumin fusion protein) New Product Slideshow Introduction Brand name: Idelvion Generic name: Coagulation factor IX (recombinant), albumin fusion protein
Idelvion (coagulation factor IX [recombinant], albumin fusion protein) New Product Slideshow Introduction Brand name: Idelvion Generic name: Coagulation factor IX (recombinant), albumin fusion protein
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Phase II Health Sciences as Applied to Coaching.
 Phase II Health Sciences as Applied to Coaching www.topform.us Overview What is going to be covered today is.. Skeletal System Muscular System Most common injuries to know about in your sport Part One:
Phase II Health Sciences as Applied to Coaching www.topform.us Overview What is going to be covered today is.. Skeletal System Muscular System Most common injuries to know about in your sport Part One:
Chapter 24. Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty. Introduction. Operative Technique. Patient Preparation and Positioning
 Chapter 24 Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty Introduction Osteoarthritis in the thumb carpometacarpal (CMC) joint is a common condition, especially in women over 60 years of
Chapter 24 Arthroscopic Thumb Carpometacarpal Interposition Arthroplasty Introduction Osteoarthritis in the thumb carpometacarpal (CMC) joint is a common condition, especially in women over 60 years of
Hip Surgery and Mobility
 Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
