Canadian Diabetes Association 2008 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada
|
|
|
- Magdalene Jones
- 5 years ago
- Views:
Transcription
1 Canadian Diabetes Association 2008 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada Kathleen Gibson, RD CDE SLICK Dietitian September
2 Outline Facts about Diabetes What are Clinical Practice Guidelines? What are the key areas for community practice? What is diabetes? Putting it into Practice How does SLICK fit in? 2
3 Facts: Diabetes in the 21 st century One of the most challenging health problems facing the world 246 million people worldwide diagnosed in th leading cause of death in developed countries Complications heart attacks, stroke, kidney failure, amputations and blindness 380 million people worldwide projected to be diagnosed by 2025
4 Facts: Diabetes in Canada 2.4 million Canadians living with diabetes 1.9 million formally diagnosed in ,000 Canadians have undiagnosed type 2 diabetes More than 150,000 Albertans living with diabetes 6 million Canadians with pre-diabetes or at high risk of type 2 diabetes Fastest growing population segments at highest risk! Aboriginal Asian, Southeast Asian, Latin American and African Boomers
5 Facts: Economic Burden Worldwide Over $1,500 billion est. cost USA $174 billion est. direct and indirect cost Canada $17.4 billion est. economic cost
6 Facts: Direct Acute Care Costs Canada $5.6 billion est. direct costs in 2005 Estimated at $8.14 billion in in 10 hospital admissions 10% of 2,803,300 admissions in 2006 were for diabetes or diabetes-related complications This represents 10% of the annual cost of Canada s entire health care system. Includes things like: hospitalization for surgery or emergency, in-hospital medications, devices and supplies, physician and specialist visits Does not include: rehab after major surgery or amputation, personal costs to the individual or family A key finding shows that the rate of complications related to diabetes has not changed, despite increased information about the importance of management.
7 What is to be done?
8
9 What are Clinical Practice Guidelines? Comprehensive, evidence-based recommendations for health care professionals to consider in the management of their clients living with diabetes. First presented in 1998, and again in 2003 and 2008 Every update includes the latest evidence related to the prevention and management of diabetes A reference tool to help translate the best available evidence into practice. Comprehensive means all-inclusive. There are 44 chapters under the following headings. Definition/Classification/Diagnoses, Screening for Type 1 and Type 2 Diabetes, Prevention of Diabetes, Management, Macrovascular and Microvascular Complications, Diabetees in Children, Diabetes in Special Populations and Appendices. The majority of the chapters fall under Management and Complications Evidence-based means based on peer-reviewed research Developed by a team of 76 expert volunteers including specialists, family physicians, nurses, dietitians, pharmacists and other health care professionals.
10 What are Clinical Practice Guidelines? Meant to help in the decision-making process But the actual treatment decisions are supposed to be individualized Client values and preferences need to be part of the decision-making process Hope that the use of these guidelines leads to better lives for people living with diabetes in Canada
11 Key Areas for our Practice Definition, Classification and Diagnosis of Diabetes (S10) Screening for Diabetes (S14) Prevention of Diabetes (S17) Management Self Management (S25) Targets (S29) Lifestyle (Physical Activity, Nutrition Therapy) (S37, S40) Pharmacological Treatments (S46, S53) Hypoglycemia (S62) Complementary and Alternative Medicine (S91) The S numbers refer to the pages in the Clinical Practice Guidelines.
12 Key Areas for our Practice - continued Complications Heart Disease (S95, S99, S102, S119, S123) Cholesterol (S107) High Blood Pressure (S115) Kidney Disease (S126) Retinopathy (or eye damage) (S134) Neuropathy (or nerve damage) (S140) Foot Care (S143) Sexual Health (S147)
13 Key Areas for our Practice - continued Diabetes in Children Type 1 (S150) Type 2 (S162) Diabetes in Special Populations Diabetes and Pregnancy (S168) Diabetes in the Elderly (S181) Type 2 Diabetes in Aboriginal People (S187) There is plenty of other information in the CPG. The CDA has developed a powerpoint that goes through each section of the guidelines and it is 261 slides long. That would be a four+ hour presentation! We are going to try to focus on the key points. Other information includes in-hospital management of diabetes, physchological aspects of diabetes, pancreas and islet transplant
14 Basic Diabetes Information When someone has diabetes, it means their body has difficulty making insulin, or has trouble using the insulin their body makes. Insulin is required to get the glucose from our blood into the body to be burned as fuel. The glucose in our blood comes from the food we eat. If the glucose stays in the blood and gets too high it can cause immediate problems. Slightly higher blood glucose levels over the long term can cause damage to the body (eyes, heart, kidneys, limbs)
15 Four terms related to diabetes (S10): Prediabetes Type 1 diabetes Type 2 diabetes Gestational diabetes Prediabetes is a new term and refers to two specific conditions that place a person at increased risk of developing full-blown diabetes. The first is call Impaired Fasting Glucose which means your blood glucose first thing in the morning is higher than it should be, but not high enough to give you diabetes. The second is called Impaired Glucose Tolerance which means that after you eat food, your body is not able to get all the glucose out of your blood and your blood glucose stays higher than it should. But again, not high enough to be called diabetes. Not everyone with prediabetes will go on to get diabetes. With some lifestyle changes it is possible to stop or reverse the pathway. Type 1 diabetes refers to people who make virtually no insulin of their own. For an unknown reason, the pancreas is unable to produce insulin and the blood glucose rises very quickly and dangerously. Type 1 represents only 5-10% of the people with diabetes. Type 2 diabetes may range from your body not being able to use the insulin you produce (insulin resistance) to your body not being able to make enough insulin. Insulin is the key in both type 1 and type 2. The difference is the pathway that happens in the body, and the speed with which it happens. Gestational diabetes refers to diabetes that happens only during pregnancy and often disappears immediately after the birth of the child. It is a form of insulin resistance, and often insulin is needed to help control blood glucose.
16 Diagnosis of diabetes (S10) FPG 7.0 mmol/l OR Casual PG 11.1 mmo/l + symptoms of diabetes OR 2hPG in a 75-g OGTT 11.1 mmol/l Fasting means no caloric intake for at least 8 hours Casual means any time of day without regard to the interval since the last meal Classic symptoms of diabetes: poydipsia (increased thirst), polyuria (increased peeing) and unexplained weight loss Oral Glucose Tolerance Test: a client is given a known amount of glucose (75 g) to eat and/or drink and their blood glucose is measured 2 hours later. Note: A confirmatory lab glucose test must be done in all cases on another day in the absence of unequivocal hyperglycemia accompanied by acute metabolic decompensation.
17 Risk factors for Type 2 Diabetes (S14) Older than 40 years old Family History Member of a high-risk population Female Gestational diabetes History of delivery of baby 9 lbs We are going to focus mostly on Type 2 diabetes, but will touch on prediabetes and gestational. This first set are things we have no control over (unless we lie about our age!). Family History refers to first degree relatives: parents, brothers, sisters and children. Does not include grandparents, cousins, aunties and uncles Gestational diabetes increases a women s risk of developing diabetes, and uncontrolled gestational increases the child s risk of getting diabetes. By 2011, 50% of Canadians will be over 40 years of age and at risk for type 2 diabetes.
18 Preventable Risk Factors (S14) Prediabetes High blood pressure High cholesterol Overweight Carrying your weight on your stomach Low physical activity levels Unhealthy eating habits These are things we have some control over. Recall that prediabetes can be controlled and perhaps reversed. And the other factors are things we can change and improve.
19 Screening for Diabetes (S14, S187) For adults with 1 additional risk factor: A FPG every 1-2 years For children 10 years old with 1 additional risk factor: A FPG every 2 years For very obese children (BMI 99.5 %ile): An OGTT every year We are going to refer to Aboriginal Clients for the rest of the presentation. Some of the targets are different for this population since it is a high-risk population. The prevalence of diabetes in Alberta is 5.3%. The prevalence of diabetes in Aboriginal people in Alberta is 11.9%. This 2006 data is from the Alberta Diabetes Surveillance System. In addition to screening, routine medical care should include identification of the preventable risk factors (overweight/obesity, elevated waist circumference/bmi, lack of physical activity, unhealthy eating habits, prediabetes) to identify higher-risk people who would benefit from diabetes prevention and individualized counselling. Individuals with normal results but with risk factor (besides Aboriginal heritage) should receive post-test counselling on promotion of healthy lifestyles to prevent diabetes. People with diagnosed prediabetes and/or polycystic ovary syndrome (PCOS) should be encouraged to have an annual OGTT. These recommendations are all at a level D, which means a consensus by the panel evaluating this information.
20 Prevention of Diabetes (S17, S188) Programs need to be culturally appropriate Focus on: Increasing awareness of diabetes Increasing physical activity Improving eating habits Achieving healthy body weights (loss of 5% of initial body weight) Creating an environment supportive of a healthy lifestyle People with prediabetes may benefit from medication to help prevent type 2 diabetes. This would be part of a community-based Diabetes Program. Prediabetes medication could include Metformin or an alpha-glucosidase inhibitor (Acarbose). So someone on metformin may not have diabetes, but is on the medication to prevent getting diabetes.
21 Management of Diabetes Diabetes care depends on the daily commitment of the person with diabetes to self-management practices (S20) This daily commitment is supported by a multidisciplinary Diabetes Healthcare Team Can include any or all of the following: Family physician, specialist, nurse, dietitian, CHR, pharmacist, social worker, SLICK team This idea of self-management is key to diabetes care. This section of the CPGs refers to Organization of Diabetes Care Involves the client, and the health care workers who help the person with diabetes and their support people manage their care. Family support is helpful to the person with diabetes. The Team should facilitate the transfer of information among all members of the team as appropriate to ensure continuity of care.
22 Self management Education (S25) Increase the client s involvement in, confidence with and motivation for control of their diabetes. A key part is self-monitoring of blood glucose, SMBG (using a glucometer, and knowing what the numbers mean) Healthy self-management behaviours include: Healthy Eating Checking blood glucose Using medications Physical Activity Smoking Cessation People with diabetes should be offered timely diabetes education that is tailored to encourage and enhance self-care practices and behaviours Places to get this education for clients: Aboriginal diabetes Wellness Program, Diabetes Education Centres as part of a hospital, Community health care workers, Empowerment is a key idea. Clients need to play an active role in their diabetes care for the best health outcomes. Places to get additional information about diabetes: Canadian Diabetes Association, Aboriginal Diabetes Wellness Program, PRIADE
23 Targets for Control (S29) Good control of blood glucose is key to managing diabetes. Good control of blood glucose can reduce the risks of complications such as heart disease. Both fasting and post-meal glucose levels can play a role in complications. When setting treatment goals, individual risk factors need to be considered: age, presence of complications, awareness of low blood glucose There have been many clinical trials related to diabetes control and its role with complications. Fasting refers to at least 8 hours without caloric intake. Post-meal refers to 2 hours after a meal. Fasting gives an indication of how your body is doing without the influence of food. Post-meal allows the Diabetes Team to know how well the body is handling food.
24 Targets for Control - continued A1C Before Meals After Meals After Meals if A1C target not met 7.0 % mmol/l mmol/l mmol/l A1C is the glycated hemoglobin and is it is a measure of how well the blood glucose has been controlled in the previous 3 months. It is related to both the fasting and the post-meal blood glucose levels. A level of < 7.0% is related to reduced complications in all people with diabetes. A1C can be measured at a lab, or by the SLICK team Before meals includes first thing in the morning (fasting). After meals is 2 hours after a meal. If you ate supper at 6pm, you would check at 8pm. Blood glucose can be measured in the lab, or with a glucometer by the client or a health care provider. But recall, these are guidelines. Individual client targets are made with the diabetes healthcare team and take into consideration the needs of the client.
25 Monitoring Blood Glucose Control (S32) A1C Every 3 months if targets are not met, and when treatment is being changed. Every 6 months if targets are regularly met and treatment is stable SMBG Needs to be individual and depends on medications used We ve talked about what to measure and what number we are looking for. Now we need to talk about when to measure. Recall that A1C is a measure of how the blood glucose has been over the previous 3 months (how long a red blood cell lives). Meeting the target helps reduce the risk of complications for all people with diabetes. Insulin alone: at least 3 times per day and include before meal and after meal measurements Diabetes pills or lifestyle alone: individualized and should include both before and after meal measurements Insulin and diabetes pills: at least once per day, at different times of the day
26 Physical Activity (S37) 1. At least 150 minutes of moderate aerobic physical activity each week. Spread over at least 3 days per week, with no more than 2 consecutive days without exercise. 2. All people with diabetes, including the elderly, should perform resistance exercise 3 times per week. 3. An exercise ECG stress test should be considered for activity more vigorous than brisk walking. One of the cornerstones of diabetes management. Moderate activity means: biking, brisk walking, continuous swimming, dancing, raking leaves, water aerobics Vigorous activity means: brisk walking up a hill, jogging, aerobics, hockey, basketball, fast swimming, fast dancing The activity should happen for at least 10 minutes at a time. Resistance exercise means activities that use muscle strength to move a weight or work against a resistant load. Often refers to weight lifting or using resistance bands. This area requires initial instruction and periodic supervision from someone with expert skills. This could be an exercise specialist, physiotherapist, occupational therapist. The stress test is important in people who were previously sedentary (didn t move much) and who are at high-risk for heart disease. If the plan is for walking, a stress test is not required.
27 Nutrition Therapy (S40) Nutrition counselling by a registered dietitian, in either small group or one-on-one setting. Follow Eating Well with Canada s Food Guide. Maintain regular timing and spacing of meals. Consistency with starchy foods is helpful Choose foods with a low glycemic index. Caution is needed when taking insulin and using alcohol. Another cornerstone of diabetes management. Following a healthy eating plan can drop A1C by 1-2%. Eating Well with Canada s Food Guide is the key piece for health eating for all Canadians, including those with diabetes. There is no diabetes diet. Low glycemic foods tend to be higher in fibre. Teaching about glycemic index depends on the individual s interest and ability.
28 Medications in type 2 diabetes (S53) If targets are not met using lifestyle within 2-3 months, medication should be started. If the A1C >9.0% at diagnosis, medication(s) should be started along with lifestyle changes. Often more than one medication is needed to reach target A1C. This target should be achieved in 6 to 12 months. Metformin is often the first medication started. Basal insulin can be used along with oral medications. The earlier targets can be met, the better it is for the long term success of the client. Recall that nutrition can decrease an A1C by 1-2% The medications drop the A1C at different rates. Metformin can also drop A1C by 1-2%. Any client using insulin or insulin secretagogues should be informed about hypoglycemia.
29 Hypoglycemia (S62) Means a blood glucose < 4.0 mmol/l Can be caused by medications for clients with type 2 diabetes Treat a low blood glucose with 15g of carbohydrate (3 glucose tabs, 4 dextrose tabs, 3 tsp of sugar mixed with water, 175 ml regular pop), wait 15 minutes and check blood glucose again. Retreat if necessary. If the next meal is > 1 hr away, a snack can prevent a repeat low blood sugar. Important not to over treat a low blood sugar. Prevents a rebound swing to a blood glucose that is too high. The symptoms can include trembling, sweating, anxiety, hunger, nausea, confusion, weakness, vision changes, difficulty speaking, headaches, sizziness
30 Influenza and Pneumococcal Immunization (S86) People with diabetes should receive an annual influenza vaccine. People with diabetes should be considered for vaccination against penumococcus. People with diabetes, especially with kidney or heart complications are at high risk for complications from influenza and pneumococcal disease. The vaccination can reduce hospitalizations by up to 40%.
31 Complementary and Alternative Medicine (S91) Up to 30% of people with diabetes use complementary and alternative medicine for various issues. Potentially serious problems Not enough evidence regarding safety and efficacy. Clients with diabetes should be routinely asked if they are using complementary and alternative medications. Includes herbal medications, dietary supplements, minerals, vitamins and other micronutrients Issues with potential side effects with physician prescribed medications. Possible harm from some herbal remedies. Studies on complementary and alternative medicines are often small, and of short duration. If a client chooses complementary medicine over Western medicine, it is important to still check all the targets for diabetes management to know if it is working and not harming the client. Remember that diabetes management is focused on the client, and the client has the right to choose. It is our job to make sure they have all the information to make the best choice.
32 Heart Disease Complications of Diabetes Kidney Disease Eye Disease Amputations These are the main complications of diabetes. Because Type 2 diabetes can be slow progressing, people may already have some complications when they are diagnosed. First Nations people in Canada have both high rates of diabetes and its complications.
33 Complications Prevention (S102) Step 1. Vascular protection Step 2. Treat high blood pressure Step 3. Protect the kidneys Protect the heart is the top priority. Can protect against both macrovascular and microvascular events. Macrovascular refers to large blood vessels and an event would be cardiovascular disease, heart attack, stroke Microvascular refers to small blood vessels and is related to kidney disease, eye disease and issues with the feet.
34 Heart Disease People with diabetes develop heart disease years earlier than someone without diabetes. The following individuals should be considered high risk: Men 45 years and Women 50 years Men < 45 years and Women < 50 years with more than 1 of: Exisiting heart disease, kidney disease, eye disease, family hx, extreme single risk factor, diabetes > 15 years with age >30 years Assessment for heart disease risk should include: Smoking, physical activity, nutrition, duration of diabetes, sexual function history, waist circumference, lipid profile, blood pressure, glycemic control, kidney function, periodic ECGs E.g., LDL > 5.0 mmol/l, SBP > 180 mm Hg
35 Heart Disease - continued Baseline resting ECG should be performed in: All people > 40 years All people with duration > 15 years All people with high blood pressure, kidney disease and/or reduced pulse A repeat resting ECG should be done every 2 years in people considered at high risk for heart disease.
36 Heart Disease - continued Vascular protection (S102) for all people with diabetes: Lifestyle modification (healthy body weight, healthy diet, physical activity, smoking cessation) Optimize blood pressure control (< 130/<80) Optimize blood glucose control (A1C 7.0%) For people at high risk: ACE inhibitor or ARB therapy Low dose aspirin Lipid-lowering medication (LDL <2.0 mmol/l, TC:HDL < 4.0) Primary target for blood pressure for people with diabetes is <130/80 Blood Glucose targets A1C <= 7% Dylipidemia targets: LDL-C <2.0 mmol/l, secondary target of TC:HDL ratio < 4.0 Can only determine LDL if person is fasting for at least 9 hours. Smoking and gum chewing is not fasting. Only sips of water can be taken.
37 Heart Disease - continued Lipid (S107) Fasting lipid levels should be measured at diagnosis and then every 1-3 years. More frequent testing is needed if someone is on medication for lipids (at least once per year). Blood Pressure (S115) People with diabetes and high BP should be aggressively treated to reach the target of <130/80 mm Hg. This may require more than one medication.
38 Kidney Disease Chronic kidney disease is one of the most common and devastating complication of diabetes. Fifty percent (50%) of people with diabetes have kidney disease. Kidney disease from diabetes is one of the leading causes of kidney failure in Canada. Screening for kidney disease: at diagnosis of diabetes and once a year afterwards.
39 Kidney Disease - continued What is screening? Urine dipstick for protein: screens for other kidney disease Random Albumin to Creatinine Ratio (ACR): screens for the presence of very small proteins in the urine. Men < 2.0 mmol/l Women <2.8 mmol/l Estimated Glomerular Filtration Rate (egfr): serum creatinine, age, gender If the ACR is elevated beyond the targets, 2 repeat ACRs need to happen within the next three months. ACR can be elevated by other things: recent major exercise, fever, urinary tract infection, congestive heart failure, menstruation, severe high blood pressure, extremely high blood glucose. People with diabetes and chronic kidney disease should have an ACR done every 6 months.
40 Kidney Disease - continued To prevent the onset, and delay the progression: 1. Best possible control of blood glucose 2. Best possible control of blood pressure Using an ACE inhibitor or ARB, has been shown to protect the kidneys. Targets are the same for all people with diabetes! A1C < 7.0%, BP<130/80 mm Hg Even without evidence of elevated blood pressure! You may have a client on an ACE or an ARB who does not have high blood pressure, but may show signs of kidney disease.
41 Eye Disease (S134) Diabetic retinopathy is the most common cause of new cases of legal blindness in people of working age. An estimated 2 million people in Canada have some form of diabetic retinopathy (just about everyone with diabetes!). Vision loss is associated with a 4-fold increase in early death.
42 Eye Disease Screening (S134) When: At diagnosis for all people with type 2 diabetes. If retinopathy is not present, rescreen annually. How: Gold standard is 7-field stereoscopic colour fundus photography with interpretation by a specialist. Direct ophthalmoscopy through dilated pupil Because the burden of diabetes is higher in Aboriginal peoples, it is recommended that the screening happen annually. Gold standard means the best! Direct observation can happen with an ophthalmologist or an optometrist. A few optometrists now have cameras in their offices, but most are not trained to the gold standard method.
43 Eye Disease Prevention (S135) 1. Best possible control of blood glucose 2. Best possible control of blood pressure 3. Best possible control of lipids Seems familiar! In people with Type 1, good control meant a 76% reduction in the onset of eye disease. For people with Type 2, high blood glucose is an independent risk factor in the onset and progressions of retinopathy. Treatment of Retinopathy includes: Laser therapy surgery
44 Nerve Damage (S140) Detectable nerve damage will develop within 10 years of diagnosis in 40 to 50% of people with diabetes. Risk factors for nerve damage and pain are exposure to: high blood glucose high triglycerides overweight/obese, Smoking high blood pressure Under-diagnosis is a fundamental problem in the primary care of people with diabetes.
45 Nerve Damage Screening (S140) At diagnosis and then annually. Done using a 10-g Semmes-Weinstein monofilament or a 128-Hz tuning fork. (S199) Assessing the loss of sensation on the top and bottom of the foot. May include reflexes and assessment of pedal pulses Decreased sensation can lead to foot damage, ulceration, infection and eventual amputation Best measure of prevention? Best possible control of blood glucose!
46 Foot Care (S143) Foot problems are a major cause of illness and death in people with diabetes. Foot problems contribute to increased healthcare costs. Foot examinations should be done by the individual daily and healthcare providers at least annually. Range of motion, callus pattern, bony deformities, skin temperature and sensation testing. People at high risk for foot ulceration and amputation should receive foot care education, professionally fitted footwear, smoking cessation strategies and early referrals to specialized care. Any infection must be treated aggressively.
47 Sexual Health (S147) Erectile dysfunction affects 34 to 45% of men with diabetes. Risk factors: Increasing age Duration of diabetes Poor control of blood glucose Smoking High blood pressure Poor control of lipids Cardiovascular disease ED can negatively affect quality of life for those affected, regardless of age. Men should be regularly screened. There are validated questionnaires that are sensitive and specific are listed in the CPGs. Women are affected by increased urinary tract infections, yeast infections, vaginal dryness. Best first step: best possible control of blood glucose.
48 Type 2 in Children and Adolescents (S162) Increasing in frequency over the past 20 years, especially in high risk populations. Risk factors: Family history Overweight Impaired glucose tolerance Polycystic ovary syndrome, acanthosis nigricans Exposure to diabetes in utero High blood pressure High blood lipids Family history is a first degree or second-degree relative: mother, father, sister, brother; grandparents, aunts, uncles Impaired glucose tolerance how your body handles the meal Mother had gestational diabetes Recall screening is for age>10 years, FPG every 2 years.
49 Type 2 in children Management: Healthy eating Physical activity Attain a healthy body weight Family counselling Medications (metformin or insulin) Screening targets and frequency are the same as for adults with type 2 diabetes At diagnosis and annually thereafter
50 Diabetes and Pregnancy (S168) Pre-existing diabetes Best possible control of blood glucose before conception Pre-pregnancy: A1C: 7.0% During pregnancy A1C: 6.0% Fasting and before meals: mmol/l 1 hour after a meal: mmol/l 2 hours after a meal: mmol/l Targets are much stricter to prevent harm to the fetus.
51 Gestational Diabetes Onset happens during pregnancy. Screening between 24 and 28 weeks gestation. Initial screen is with a 50-g glucose load and blood glucose check 1 hour later. If positive (between 7.8 and 10.2 mmol/l), then a 75-g OGTT is done. If >10.3 mmol/l, then gestation diabetes
52 Gestational Diabetes - continued Gestational diabetes is diagnosed if 2 of the following values are found on the OGTT. If only one is met, then Impaired Glucose Tolerance of pregnancy is diagnosed. Fasting blood glucose 5.3 mmol/l 1 hour blood glucose 10.6 mmol/l 2 hour blood glucose 8.9 mmol/l Once diagnosed, the targets are the same as for women with pre-pregnancy diabetes.
53 Gestational Diabetes- continued During pregnancy A1C: 6.0% Fasting and before meals: mmol/l 1 hour after a meal: mmol/l 2 hours after a meal: mmol/l Test blood glucose at both before and after meals (4 times a day) If targets are not met within 2 weeks using nutrition alone, then insulin should be started. Targets are much stricter to prevent harm to the fetus.
54 Postpartum All mothers should be encouraged to breastfeed. Gestation Diabetes OGTT 6 weeks and 6 months postpartum. Follow screening for diabetes guidelines. Get screened for diabetes when planning next pregnancy.
55 How can SLICK fit in? Complications Screening Team (mobile and communitybased) Screen for: Blood Glucose Control (A1C, blood glucose) Cardiovascular (blood pressure, lipids, lifestyle counselling) Kidneys (urine dipstick, ACR) Eyes (visual acuity, gold standard photographs) Nerves (sensation testing) We do not screen for diabetes! Our clients are to have a diagnosis of diabetes. We can be a component of a community diabetes program, but we are not THE program. The mobile teams are attempting to visit each community twice a year. But the A1C should be measured q 3 months. So clients need to be followed by their doctors or nurse practitioner or primary care network.
56 Questions? Discussion?
Diabetes. What you need to know
 Diabetes What you need to know Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2016 University Health Network. All rights reserved. This information
Diabetes What you need to know Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2016 University Health Network. All rights reserved. This information
Clinical Practice Guidelines for Diabetes Management
 Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Prediabetes 101. What is it and what can I do about it? Intermountainhealthcare.org/diabetes
 Prediabetes 101 What is it and what can I do about it? Patient Education Intermountainhealthcare.org/diabetes What do you already know about prediabetes? Fact or Fiction? There are often no symptoms of
Prediabetes 101 What is it and what can I do about it? Patient Education Intermountainhealthcare.org/diabetes What do you already know about prediabetes? Fact or Fiction? There are often no symptoms of
Monthly WellPATH Spotlight November 2016: Diabetes
 Monthly WellPATH Spotlight November 2016: Diabetes DIABETES RISK FACTORS & SELF CARE TIPS Diabetes is a condition in which the body does not produce enough insulin or does not use the insulin produced
Monthly WellPATH Spotlight November 2016: Diabetes DIABETES RISK FACTORS & SELF CARE TIPS Diabetes is a condition in which the body does not produce enough insulin or does not use the insulin produced
Living Well with Diabetes
 Living Well with Diabetes What is diabetes? Diabetes Overview Diabetes is a disorder of the way the body uses food for growth and energy. Most of the food people eat is broken down into glucose, the form
Living Well with Diabetes What is diabetes? Diabetes Overview Diabetes is a disorder of the way the body uses food for growth and energy. Most of the food people eat is broken down into glucose, the form
Each Home Instead Senior Care franchise office is independently owned and operated Home Instead, Inc.
 Each Home Instead Senior Care franchise office is independently owned and operated. 2010 Home Instead, Inc. Diabetes is a group of diseases characterized by high blood glucose levels. Our bodies break
Each Home Instead Senior Care franchise office is independently owned and operated. 2010 Home Instead, Inc. Diabetes is a group of diseases characterized by high blood glucose levels. Our bodies break
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES
 RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
Personal Diabetes Passport
 Personal Diabetes Passport Contact information: Name: Physician: Diabetes Education Centre: Dietitian: Ophthalmologist: Chiropodist: Type of Diabetes: Type 1 (T1DM) Increased risk for diabetes Type 2(T2DM)
Personal Diabetes Passport Contact information: Name: Physician: Diabetes Education Centre: Dietitian: Ophthalmologist: Chiropodist: Type of Diabetes: Type 1 (T1DM) Increased risk for diabetes Type 2(T2DM)
Diabetes: Assessing your risk
 Diabetes: Assessing your risk What is diabetes? There are 2 types of diabetes. Type 1 diabetes occurs when the body does not make a hormone called insulin. Insulin helps the body use sugar (also called
Diabetes: Assessing your risk What is diabetes? There are 2 types of diabetes. Type 1 diabetes occurs when the body does not make a hormone called insulin. Insulin helps the body use sugar (also called
Objectives 10/11/2013. Diabetes- The Real Cost of Sugar. Diabetes 101: What is Diabetes. By Ruth Nekonchuk RD CDE LMNT
 Diabetes- The Real Cost of Sugar By Ruth Nekonchuk RD CDE LMNT Objectives To explain diabetes To explain the risks of diabetes To enumerate the cost of diabetes to our country To enumerate the cost of
Diabetes- The Real Cost of Sugar By Ruth Nekonchuk RD CDE LMNT Objectives To explain diabetes To explain the risks of diabetes To enumerate the cost of diabetes to our country To enumerate the cost of
Am I at Risk for Type 2 Diabetes?
 Am I at Risk for Type Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes On this page: What is type diabetes? Can type diabetes be prevented? What are the signs and symptoms of type diabetes?
Am I at Risk for Type Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes On this page: What is type diabetes? Can type diabetes be prevented? What are the signs and symptoms of type diabetes?
DIABETES AND CHRONIC KIDNEY DISEASE
 DIABETES AND CHRONIC KIDNEY DISEASE Stages 1 4 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
DIABETES AND CHRONIC KIDNEY DISEASE Stages 1 4 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
Type 2 Diabetes. What is diabetes? What is type 2 diabetes? What is type 1 diabetes? Understanding blood glucose and insulin
 Page 1 of 7 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The first-line treatment is diet, weight control and physical activity. If the blood sugar (glucose) level remains high
Page 1 of 7 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The first-line treatment is diet, weight control and physical activity. If the blood sugar (glucose) level remains high
Diabetes Mellitus Type 2
 Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Diabetes. Ref HSCW 024
 Diabetes Ref HSCW 024 Why is it important? Diabetes is an increasingly common, life-long, progressive but largely preventable health condition affecting children and adults, causing a heavy burden on health
Diabetes Ref HSCW 024 Why is it important? Diabetes is an increasingly common, life-long, progressive but largely preventable health condition affecting children and adults, causing a heavy burden on health
Am I at Risk for Type 2 Diabetes?
 NATIONAL DIABETES INFORMATION CLEARINGHOUSE Am I at Risk for Type 2 Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes U.S. Department of Health and Human Services National Institutes of Health
NATIONAL DIABETES INFORMATION CLEARINGHOUSE Am I at Risk for Type 2 Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes U.S. Department of Health and Human Services National Institutes of Health
Date of Birth. Black/African American. What is your occupation? Retired? Yes No
 Health Risk Assessment Today s Date: Name Date of Birth GENERAL INFORMATION What is your race? American Indian or Alaskan Native Native Hawaiian or Other Pacific Islander Asian, Chinese, Japanese, Korean
Health Risk Assessment Today s Date: Name Date of Birth GENERAL INFORMATION What is your race? American Indian or Alaskan Native Native Hawaiian or Other Pacific Islander Asian, Chinese, Japanese, Korean
Guiding Principles. for Diabetes Care: For Health Care. Providers
 Guiding Principles N A T I O N A L for Diabetes Care: D I A B E T E S For Health Care E D U C A T I O N Providers P R O G R A M The National Diabetes Education Program (NDEP) has developed these Guiding
Guiding Principles N A T I O N A L for Diabetes Care: D I A B E T E S For Health Care E D U C A T I O N Providers P R O G R A M The National Diabetes Education Program (NDEP) has developed these Guiding
Diabetes: Everything You Want to Know. LCDR Bernadine John, RN, BSN, CDE
 Diabetes: Everything You Want to Know LCDR Bernadine John, RN, BSN, CDE I have no financial affiliation to disclose as a conflict of interest regarding this presentation. DM Standards of Care The IHS Division
Diabetes: Everything You Want to Know LCDR Bernadine John, RN, BSN, CDE I have no financial affiliation to disclose as a conflict of interest regarding this presentation. DM Standards of Care The IHS Division
Why do we care? 20.8 million people. 70% of people with diabetes will die of cardiovascular disease. What is Diabetes?
 What is Diabetes? Diabetes 101 Ginny Burns RN MEd CDE Diabetes mellitus is a group of diseases characterized by high levels of blood glucose resulting from defects in insulin production, insulin action
What is Diabetes? Diabetes 101 Ginny Burns RN MEd CDE Diabetes mellitus is a group of diseases characterized by high levels of blood glucose resulting from defects in insulin production, insulin action
American Diabetes Association: Standards of Medical Care in Diabetes 2015
 American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
DIABETES MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
MY PERSONAL ROADMAP WORKBOOK
 FINALLY. Celebrate your successes, even the small ones! Learn from your efforts that don t turn out as you hoped or expected. If you do this, you can t fail! Set yourself up to succeed. Remember.. Most
FINALLY. Celebrate your successes, even the small ones! Learn from your efforts that don t turn out as you hoped or expected. If you do this, you can t fail! Set yourself up to succeed. Remember.. Most
Standards of Medical Care in Diabetes 2016
 Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Clinical Practice Guideline Key Points
 Clinical Practice Guideline Key Points Clinical Practice Guideline 2008 Key Points Diabetes Mellitus Provided by: Highmark Endocrinology Clinical Quality Improvement Committee In accordance with Highmark
Clinical Practice Guideline Key Points Clinical Practice Guideline 2008 Key Points Diabetes Mellitus Provided by: Highmark Endocrinology Clinical Quality Improvement Committee In accordance with Highmark
Physical Activity/Exercise Prescription with Diabetes
 Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
DIABETES AND CHRONIC KIDNEY DISEASE
 DIABETES AND CHRONIC KIDNEY DISEASE Stage 5 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
DIABETES AND CHRONIC KIDNEY DISEASE Stage 5 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
V. N. Karazin Kharkiv National University Department of internal medicine Golubkina E.O., ass. of prof., Shanina I. V., ass. of prof.
 V. N. Karazin Kharkiv National University Department of internal medicine Golubkina E.O., ass. of prof., Shanina I. V., ass. of prof., Macharinskaya O.S., ass. of prof; Supervisor: prof. Yabluchanskiy
V. N. Karazin Kharkiv National University Department of internal medicine Golubkina E.O., ass. of prof., Shanina I. V., ass. of prof., Macharinskaya O.S., ass. of prof; Supervisor: prof. Yabluchanskiy
Hypoglycemia, Sick Days/DKA and Hospitalization
 Hypoglycemia, Sick Days/DKA and Hospitalization General survival skills for your client with diabetes at home and in Hospital Diabetes Canada guidelines for your client with diabetes while they are in
Hypoglycemia, Sick Days/DKA and Hospitalization General survival skills for your client with diabetes at home and in Hospital Diabetes Canada guidelines for your client with diabetes while they are in
Diabetes 101: A Brief Overview of Diabetes and the American Diabetes Association
 Diabetes 101: A Brief Overview of Diabetes and the American Diabetes Association What Happens When We Eat? After eating, most food is turned into glucose, the body s main source of energy. Normal Blood
Diabetes 101: A Brief Overview of Diabetes and the American Diabetes Association What Happens When We Eat? After eating, most food is turned into glucose, the body s main source of energy. Normal Blood
Diabetes for CNAs. This course has been awarded two (2.0) contact hours. This course expires on August 31, 2017.
 Diabetes for CNAs This course has been awarded two (2.0) contact hours. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction and distribution of these materials
Diabetes for CNAs This course has been awarded two (2.0) contact hours. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction and distribution of these materials
Manage Diabetes with Small Changes
 In This Issue: } Manage with Small Changes } The Role of Your Educator } Prediabetes: A Call to Action } Insulin and : Your Questions Answered Manage with Small Changes One man learns simple ways to keep
In This Issue: } Manage with Small Changes } The Role of Your Educator } Prediabetes: A Call to Action } Insulin and : Your Questions Answered Manage with Small Changes One man learns simple ways to keep
DIABETES AWARENESS TYPES, RISKS AND CONTROL
 Spotlight on Health 2017 DIABETES AWARENESS TYPES, RISKS AND CONTROL Currently it is estimated that 1 in 11 adults (415 million people) have diabetes, although approximately 46% of people with diabetes
Spotlight on Health 2017 DIABETES AWARENESS TYPES, RISKS AND CONTROL Currently it is estimated that 1 in 11 adults (415 million people) have diabetes, although approximately 46% of people with diabetes
Page 0 of 20. Health Profiles. Diabetes Montgomery County, OH. Public Health - Dayton & Montgomery County Epidemiology Section
 Page 0 of 20 Health Profiles Diabetes Montgomery County, OH Public Health - Dayton & Montgomery County Epidemiology Section January 2014 Page 1 of 20 Prepared by: Epidemiology Section of Public Health
Page 0 of 20 Health Profiles Diabetes Montgomery County, OH Public Health - Dayton & Montgomery County Epidemiology Section January 2014 Page 1 of 20 Prepared by: Epidemiology Section of Public Health
ADDRESSING CHRONIC DISEASES
 ADDRESSING CHRONIC DISEASES Health-Management Strategies for Use with Behavioral Health Clients Mary Brunette, MD Delia Cimpean Hendrick, MD SCOPE AND SEQUENCE For more information about this program,
ADDRESSING CHRONIC DISEASES Health-Management Strategies for Use with Behavioral Health Clients Mary Brunette, MD Delia Cimpean Hendrick, MD SCOPE AND SEQUENCE For more information about this program,
Clinical Care Performance. Financial Year 2012 to 2018
 Clinical Care Performance Financial Year 2012 to 2018 SHP Clinical Care Performance Diabetes Mellitus Hyperlipidemia Hypertension Diabetes Mellitus Find out how our patients are doing for: HbA1C HbA1c
Clinical Care Performance Financial Year 2012 to 2018 SHP Clinical Care Performance Diabetes Mellitus Hyperlipidemia Hypertension Diabetes Mellitus Find out how our patients are doing for: HbA1C HbA1c
5/21/2013. Welcome. Today. Facts about Diabetes. Living Well with Diabetes Including: Physical Activity. Learn about diabetes and how to manage it
 Welcome Living Well with Diabetes Including: Physical Activity Today. Learn about diabetes and how to manage it If you or your client have medical questions about diabetes, talk with their doctor, healthcare
Welcome Living Well with Diabetes Including: Physical Activity Today. Learn about diabetes and how to manage it If you or your client have medical questions about diabetes, talk with their doctor, healthcare
Diabetes Mellitus: Evaluation and Care Management
 Diabetes Mellitus: Evaluation and Care Management Michael King, MD Assistant Professor Residency Program Director University of Kentucky Dept. of Family & Community Medicine Learning Objectives 1. Review
Diabetes Mellitus: Evaluation and Care Management Michael King, MD Assistant Professor Residency Program Director University of Kentucky Dept. of Family & Community Medicine Learning Objectives 1. Review
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES
 Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
PRESS RELEASE. November is Diabetes Awareness Month Severity/Epidemic and Risk Factors of Diabetes
 November 7, 2012- (Part 1 in a series of 5) November is Diabetes Awareness Month Severity/Epidemic and Risk Factors of Diabetes Data released from the American Diabetes Association have found almost 26
November 7, 2012- (Part 1 in a series of 5) November is Diabetes Awareness Month Severity/Epidemic and Risk Factors of Diabetes Data released from the American Diabetes Association have found almost 26
Diabetes. Diabetes in Balance
 Diabetes Introduction to Diabetes If you are living with type 2 diabetes, it is important that your lifestyle has the right balance between the appropriate treatment, regular exercise and a healthy diet.
Diabetes Introduction to Diabetes If you are living with type 2 diabetes, it is important that your lifestyle has the right balance between the appropriate treatment, regular exercise and a healthy diet.
Diabetes and Kidney Disease: Time to Act. Your Guide to Diabetes and Kidney Disease
 Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
Diabetes - The Facts
 Diabetes - The Facts What is Diabetes? In people with diabetes, blood glucose levels are higher than normal because the body either does not produce enough insulin or cannot use insulin properly. The body
Diabetes - The Facts What is Diabetes? In people with diabetes, blood glucose levels are higher than normal because the body either does not produce enough insulin or cannot use insulin properly. The body
Health Risk Assessment
 Health Risk Assessment Today s Date: Name Date of Birth GENERAL INFORMATION What is your race? American Indian or Alaskan Native Native Hawaiian or Other Pacific Islander Asian, Chinese, Black/African
Health Risk Assessment Today s Date: Name Date of Birth GENERAL INFORMATION What is your race? American Indian or Alaskan Native Native Hawaiian or Other Pacific Islander Asian, Chinese, Black/African
Living a Healthier Life
 For People With Diabetes Living a Healthier Life This health information is being provided for general educational purposes only. Your health care provider is the single best source of information regarding
For People With Diabetes Living a Healthier Life This health information is being provided for general educational purposes only. Your health care provider is the single best source of information regarding
Chronic Kidney Disease due to Diabetes (Diabetic Nephropathy)
 Chronic Kidney Disease due to Diabetes (Diabetic Nephropathy) Patient information Oxford Kidney Unit If you have been told you have chronic kidney disease (CKD) due to diabetic nephropathy this leaflet
Chronic Kidney Disease due to Diabetes (Diabetic Nephropathy) Patient information Oxford Kidney Unit If you have been told you have chronic kidney disease (CKD) due to diabetic nephropathy this leaflet
Standards of Medical Care in Diabetes 2018
 Standards of Medical Care in Diabetes 2018 Eric L. Johnson, M.D. Associate Professor University of North Dakota School of Medicine and Health Sciences Assistant Medical Director Altru Diabetes Center Grand
Standards of Medical Care in Diabetes 2018 Eric L. Johnson, M.D. Associate Professor University of North Dakota School of Medicine and Health Sciences Assistant Medical Director Altru Diabetes Center Grand
Understanding Common Medical Issues Session 5
 1 Housekeeping items Washrooms Refreshment breaks Introductions 2 Learning Objectives To identify how the body produces insulin, how it is used and causes that reduce the efficiency of insulin production.
1 Housekeeping items Washrooms Refreshment breaks Introductions 2 Learning Objectives To identify how the body produces insulin, how it is used and causes that reduce the efficiency of insulin production.
ARE YOU AT INCREASED RISK FOR CHRONIC KIDNEY DISEASE?
 ARE YOU AT INCREASED RISK FOR CHRONIC KIDNEY DISEASE? www.kidney.org National Kidney Foundation s Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation s Kidney Disease
ARE YOU AT INCREASED RISK FOR CHRONIC KIDNEY DISEASE? www.kidney.org National Kidney Foundation s Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation s Kidney Disease
Diabetes AN OVERVIEW. Diabetes is a disease in which the body is no longer
 AN OVERVIEW Diabetes As you prepare to leave our center, we want to be sure you have the knowledge and skills to monitor and manage your own health conditions. You are the most important person on your
AN OVERVIEW Diabetes As you prepare to leave our center, we want to be sure you have the knowledge and skills to monitor and manage your own health conditions. You are the most important person on your
Type 2 Diabetes. Care for your body today for a healthier tomorrow
 Type 2 Diabetes Care for your body today for a healthier tomorrow Understanding diabetes You may already know that having diabetes means you have too much sugar in your blood. Why do you have high blood
Type 2 Diabetes Care for your body today for a healthier tomorrow Understanding diabetes You may already know that having diabetes means you have too much sugar in your blood. Why do you have high blood
Rick Fox M.A Health and Wellness Specialist
 Metabolic Diseases Rick Fox M.A Health and Wellness Specialist Metabolic Diseases Metabolism is the process your body uses to get or make energy from the food you eat. Food is made up of proteins, carbohydrates
Metabolic Diseases Rick Fox M.A Health and Wellness Specialist Metabolic Diseases Metabolism is the process your body uses to get or make energy from the food you eat. Food is made up of proteins, carbohydrates
Diabetes Self-Care Information and Record Booklet
 Diabetes Self-Care Information and Record Booklet Your personal guide... what you do each day really matters. This document is available online at www.wisconsindiabetesinfo.org What is Diabetes? Diabetes
Diabetes Self-Care Information and Record Booklet Your personal guide... what you do each day really matters. This document is available online at www.wisconsindiabetesinfo.org What is Diabetes? Diabetes
National Aboriginal Diabetes Association. Gestational Diabetes (developed by Sarah Smith, 4 th yr Nursing, University of Manitoba)
 National Aboriginal Diabetes Association Gestational Diabetes (developed by Sarah Smith, 4 th yr Nursing, University of Manitoba) Who we are NADA is a not-for-profit members-led organization established
National Aboriginal Diabetes Association Gestational Diabetes (developed by Sarah Smith, 4 th yr Nursing, University of Manitoba) Who we are NADA is a not-for-profit members-led organization established
Understanding gestational diabetes
 Understanding gestational diabetes Gestational diabetes is a form of diabetes that occurs in women during pregnancy. About 12 14% of pregnant women will develop gestational diabetes, usually around the
Understanding gestational diabetes Gestational diabetes is a form of diabetes that occurs in women during pregnancy. About 12 14% of pregnant women will develop gestational diabetes, usually around the
Diabetes. What is it and how can we prevent it? - Brigette Pereira and Natalie Wowk- Slukynsky, First Nations and Inuit Health Branch
 Diabetes What is it and how can we prevent it? - Brigette Pereira and Natalie Wowk- Slukynsky, First Nations and Inuit Health Branch What is Diabetes? Diabetes is a disease where your body is not able
Diabetes What is it and how can we prevent it? - Brigette Pereira and Natalie Wowk- Slukynsky, First Nations and Inuit Health Branch What is Diabetes? Diabetes is a disease where your body is not able
Diabetes. What is diabetes?
 Diabetes 966 860 258 www.medcarespain.com doctors@medcarespain.com The incidence of diabetes has reached epidemic proportions. About 350 million people worldwide have diabetes, and according to the World
Diabetes 966 860 258 www.medcarespain.com doctors@medcarespain.com The incidence of diabetes has reached epidemic proportions. About 350 million people worldwide have diabetes, and according to the World
STANDARDS OF MEDICAL CARE IN DIABETES 2014
 STANDARDS OF MEDICAL CARE IN DIABETES 2014 I. CLASSIFICATION AND DIAGNOSIS Classification of Diabetes Type 1 diabetes β-cell destruction Type 2 diabetes Progressive insulin secretory defect Other specific
STANDARDS OF MEDICAL CARE IN DIABETES 2014 I. CLASSIFICATION AND DIAGNOSIS Classification of Diabetes Type 1 diabetes β-cell destruction Type 2 diabetes Progressive insulin secretory defect Other specific
Standards of Medical Care In Diabetes
 Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
Diabetes Overview. How Food is Digested
 Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Diabetes Mellitus Aeromedical Considerations. Aviation Medicine Seminar Bucharest, Romania. 11 th to 15 th November 2013
 Diabetes Mellitus Aeromedical Considerations Aviation Medicine Seminar Bucharest, Romania. 11 th to 15 th November 2013 Metabolic, Nutritional or Endocrine disorders Applicants with metabolic, nutritional
Diabetes Mellitus Aeromedical Considerations Aviation Medicine Seminar Bucharest, Romania. 11 th to 15 th November 2013 Metabolic, Nutritional or Endocrine disorders Applicants with metabolic, nutritional
Common Diabetes-related Terms
 Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
ABOUT TYPE 2 DIABETES
 ABOUT TYPE 2 DIABETES Because the more you know, the better you ll feel. What You ll Find Attitudes and Beliefs Type 2 Diabetes What Is It? Where You ll Find It Page 4-5 This booklet is designed to help
ABOUT TYPE 2 DIABETES Because the more you know, the better you ll feel. What You ll Find Attitudes and Beliefs Type 2 Diabetes What Is It? Where You ll Find It Page 4-5 This booklet is designed to help
Modified version focused on CCNC Quality Measures and Feedback Processes
 Executive Summary: Standards of Medical Care in Diabetes 2010 Modified version focused on CCNC Quality Measures and Feedback Processes See http://care.diabetesjournals.org/content/33/supplement_1/s11.full
Executive Summary: Standards of Medical Care in Diabetes 2010 Modified version focused on CCNC Quality Measures and Feedback Processes See http://care.diabetesjournals.org/content/33/supplement_1/s11.full
Indian Pharmaceutical Association Indian Pharmaceutical Association
 55 th National Pharmacy Week November 20 th to 26 th 2016 Theme Pharmacists for a Healthy India: Role in Prevention and Management of Diabetes Indian Pharmaceutical Association www.ipapharma.org Indian
55 th National Pharmacy Week November 20 th to 26 th 2016 Theme Pharmacists for a Healthy India: Role in Prevention and Management of Diabetes Indian Pharmaceutical Association www.ipapharma.org Indian
A Summary Report: 2003
 D iabetes in Idaho A Summary Report: 2003 Idaho Department of Health and Welfare Division of Health Bureau of Community and Environmental Health This publication was supported by Grant No. U32/CCU022691-02
D iabetes in Idaho A Summary Report: 2003 Idaho Department of Health and Welfare Division of Health Bureau of Community and Environmental Health This publication was supported by Grant No. U32/CCU022691-02
Rev. date Kaiser Foundation Health Plan of Washington
 PE3620000-01-17 Rev. date 2014013 2017 Kaiser Foundation Health Plan of Washington Gestational diabetes Information to help you stay healthy during your pregnancy What is gestational diabetes? How gestational
PE3620000-01-17 Rev. date 2014013 2017 Kaiser Foundation Health Plan of Washington Gestational diabetes Information to help you stay healthy during your pregnancy What is gestational diabetes? How gestational
Diabetes. HED\ED:NS-BL 037-3rd
 Diabetes HED\ED:NS-BL 037-3rd Diabetes Diabetes mellitus is an epidemic disease and based on a recent study published on 2011, the estimated number of affected people is 366 million worldwide and the number
Diabetes HED\ED:NS-BL 037-3rd Diabetes Diabetes mellitus is an epidemic disease and based on a recent study published on 2011, the estimated number of affected people is 366 million worldwide and the number
Diabetes Mellitus. Disclaimer. Multimedia Health Education
 Disclaimer This movie is an educational resource only and should not be used to manage Diabetes or blood sugar control.all decisions about management of diabetes must be made in conjunction with your Physician
Disclaimer This movie is an educational resource only and should not be used to manage Diabetes or blood sugar control.all decisions about management of diabetes must be made in conjunction with your Physician
Diabetes 101: A Brief Overview of Diabetes and the American Diabetes Association
 Diabetes 101: A Brief Overview of Diabetes and the American Diabetes Association What Happens When We Eat? After eating, most food is turned into glucose, the body s main source of energy. Normal Blood
Diabetes 101: A Brief Overview of Diabetes and the American Diabetes Association What Happens When We Eat? After eating, most food is turned into glucose, the body s main source of energy. Normal Blood
Am I at Risk for Type 2 Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes
 Nat i o N a l Diabetes inf o r m a t i o N Cle a r i N g h o u s e Am I at Risk for Type 2 Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes U.S. Department of Health and Human Services NATIONAL
Nat i o N a l Diabetes inf o r m a t i o N Cle a r i N g h o u s e Am I at Risk for Type 2 Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes U.S. Department of Health and Human Services NATIONAL
Diabetes Overview. Basics of Diabetes
 Diabetes Overview Basics of Diabetes Objectives Review the prevalence of diabetes, how it develops and the risk of developing diabetes Review diabetes diagnosis Identify the key areas of medically managing
Diabetes Overview Basics of Diabetes Objectives Review the prevalence of diabetes, how it develops and the risk of developing diabetes Review diabetes diagnosis Identify the key areas of medically managing
Adult Diabetes Clinician Guide NOVEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
An Overview of Diabetes
 An Overview of Diabetes What is Diabetes? Diabetes is a disease in which the body is unable to properly use and store glucose (a form of sugar). Glucose backs up in the bloodstream causing a person s blood
An Overview of Diabetes What is Diabetes? Diabetes is a disease in which the body is unable to properly use and store glucose (a form of sugar). Glucose backs up in the bloodstream causing a person s blood
Preventing Diabetes. prevent or delay type 2 diabetes from
 Preventing Diabetes Introduction Diabetes is a common condition. If not controlled, diabetes can lead to serious complications such as blindness, amputations, and even death. Before people develop diabetes,
Preventing Diabetes Introduction Diabetes is a common condition. If not controlled, diabetes can lead to serious complications such as blindness, amputations, and even death. Before people develop diabetes,
Torbay Children s Diabetes Service
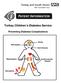 Torbay Children s Diabetes Service Preventing Diabetes Complications Retinopathy Stroke Gum Disease Nephropathy Cardiovascular disease Neuropathy Diabetes Complications Thinking and talking about the possibility
Torbay Children s Diabetes Service Preventing Diabetes Complications Retinopathy Stroke Gum Disease Nephropathy Cardiovascular disease Neuropathy Diabetes Complications Thinking and talking about the possibility
Outcomes of diabetes care in England and Wales. A summary of findings from the National Diabetes Audit : Complications and Mortality reports
 Outcomes of diabetes care in England and Wales A summary of findings from the National Diabetes Audit 2015 16: Complications and Mortality reports About this report This report is for people with diabetes
Outcomes of diabetes care in England and Wales A summary of findings from the National Diabetes Audit 2015 16: Complications and Mortality reports About this report This report is for people with diabetes
Active living with diabetes: Practical guidelines to Exercise
 Active living with diabetes: Practical guidelines to Exercise Dr. Agnes Coutinho Registered Kinesiologist April 2018 AGENDA 1.Brief overview of diabetes 2.How does exercise/physical activity impact diabetes
Active living with diabetes: Practical guidelines to Exercise Dr. Agnes Coutinho Registered Kinesiologist April 2018 AGENDA 1.Brief overview of diabetes 2.How does exercise/physical activity impact diabetes
UNDERSTANDING TYPE 2 DIABETES
 1 UNDERSTANDING TYPE 2 DIABETES PUTTING IT INTO REMISSION WITH A LOW-CARB HIGH-FAT DIET Jacqueline A. Eberstein, R.N. Director of Protocol, HEALcare The Scope of the Challenge 2 The People The Scope of
1 UNDERSTANDING TYPE 2 DIABETES PUTTING IT INTO REMISSION WITH A LOW-CARB HIGH-FAT DIET Jacqueline A. Eberstein, R.N. Director of Protocol, HEALcare The Scope of the Challenge 2 The People The Scope of
Blood pressure and kidney disease
 Blood pressure and High blood pressure is the second most common cause of. Your heart pumps your blood through tubes (blood vessels) called arteries and veins. When your blood moves through the blood vessels,
Blood pressure and High blood pressure is the second most common cause of. Your heart pumps your blood through tubes (blood vessels) called arteries and veins. When your blood moves through the blood vessels,
Quick Reference Guide
 2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
What s new in diabetes care? Connect and Learn April 13, 2018 Tess Montada-Atin NP-Adult, CDE
 What s new in diabetes care? Connect and Learn April 13, 2018 Tess Montada-Atin NP-Adult, CDE (IDF, 2017) https://www.diabetes.ca News flash: 5 types of diabetes? 5 clusters based on: patient characteristics
What s new in diabetes care? Connect and Learn April 13, 2018 Tess Montada-Atin NP-Adult, CDE (IDF, 2017) https://www.diabetes.ca News flash: 5 types of diabetes? 5 clusters based on: patient characteristics
Starting KAZANO gave me MORE POWER than metformin alone, with 2 medicines in 1 tablet
 For many adults with type 2 diabetes Starting KAZANO gave me MORE POWER than metformin alone, with 2 medicines in 1 tablet Individual results may vary. Not actual patient. KAZANO is a prescription medicine
For many adults with type 2 diabetes Starting KAZANO gave me MORE POWER than metformin alone, with 2 medicines in 1 tablet Individual results may vary. Not actual patient. KAZANO is a prescription medicine
The recommended protocol is for all patients suffering from diabetes to have yearly foot checks. This was checking the foot pulses and doing
 Foot disease is a common long-term complication of diabetes. There are different types of foot disease caused by diabetes, but they all stem from a similar process. Raised blood sugar for a prolonged amount
Foot disease is a common long-term complication of diabetes. There are different types of foot disease caused by diabetes, but they all stem from a similar process. Raised blood sugar for a prolonged amount
Stanford Youth Diabetes Coaches Program Instructor Guide Class #1: What is Diabetes? What is a Diabetes Coach? Sample
 Note to Instructors: YOU SHOULD HAVE ENOUGH COPIES OF THE QUIZ AND THE HOMEWORK TO PASS OUT TO EACH STUDENT. Be sure to use the NOTES view in Powerpoint for what to cover during class. It is important
Note to Instructors: YOU SHOULD HAVE ENOUGH COPIES OF THE QUIZ AND THE HOMEWORK TO PASS OUT TO EACH STUDENT. Be sure to use the NOTES view in Powerpoint for what to cover during class. It is important
Patient Information. First Name Middle Last Preferred Name. Street Address City State Postal Code
 Ms. Patient Information First Name Middle Last Preferred Name Street Address City State Postal Code Work Phone ( ) Home Phone ( ) Cell Phone ( ) Email Preferred Contact Email Cell Home Work Emergency Contact
Ms. Patient Information First Name Middle Last Preferred Name Street Address City State Postal Code Work Phone ( ) Home Phone ( ) Cell Phone ( ) Email Preferred Contact Email Cell Home Work Emergency Contact
STATE OF THE STATE: TYPE II DIABETES
 STATE OF THE STATE: TYPE II DIABETES HENRY DRISCOLL, MD, CHIEF of ENDOCRINOLOGY MARSHALL U, CHERTOW DIABETES CENTER, HUNTINGTON VAMC HEATHER VENOY, RD, LD, CDE DIETITIAN, DIABETES EDUCATOR, CHERTOW DIABETES
STATE OF THE STATE: TYPE II DIABETES HENRY DRISCOLL, MD, CHIEF of ENDOCRINOLOGY MARSHALL U, CHERTOW DIABETES CENTER, HUNTINGTON VAMC HEATHER VENOY, RD, LD, CDE DIETITIAN, DIABETES EDUCATOR, CHERTOW DIABETES
Health Risk Reduction. Printable Materials
 Health Risk Reduction Printable Materials Activity C: Activity Cards Activity Card #1 High Cholesterol About High Cholesterol High cholesterol is one of the major risk factors for heart disease. Decreasing
Health Risk Reduction Printable Materials Activity C: Activity Cards Activity Card #1 High Cholesterol About High Cholesterol High cholesterol is one of the major risk factors for heart disease. Decreasing
How to Fight Diabetes and Win. Diabetes. the Basics NUTURNA. Advance Diabetic Support
 How to Fight Diabetes and Win Diabetes the Basics NUTURNA TM Advance Diabetic Support Diabetes: the Basics Diabetes affects over 29 million people in the United States and nearly one-third of these people
How to Fight Diabetes and Win Diabetes the Basics NUTURNA TM Advance Diabetic Support Diabetes: the Basics Diabetes affects over 29 million people in the United States and nearly one-third of these people
PLEASE REMEMBER TO BRING TO EACH APPOINTMENT
 PLEASE REMEMBER TO BRING TO EACH APPOINTMENT Conversion table for HbA1c% to mmol/mol Old DCCT aligned HbA1c(%) New IFCC HbA1c (mmol/mol) 4.0 20 5.0 31 6.0 42 6.5 48 7.0 53 7.5 59 8.0 64 9.0 75 10.0 86
PLEASE REMEMBER TO BRING TO EACH APPOINTMENT Conversion table for HbA1c% to mmol/mol Old DCCT aligned HbA1c(%) New IFCC HbA1c (mmol/mol) 4.0 20 5.0 31 6.0 42 6.5 48 7.0 53 7.5 59 8.0 64 9.0 75 10.0 86
Medication Guide SEGLUROMET (seg-lur-oh-met) (ertugliflozin and metformin hydrochloride) tablets, for oral use
 Medication Guide SEGLUROMET (seg-lur-oh-met) (ertugliflozin and metformin hydrochloride) tablets, for oral use Read this Medication Guide carefully before you start taking SEGLUROMET and each time you
Medication Guide SEGLUROMET (seg-lur-oh-met) (ertugliflozin and metformin hydrochloride) tablets, for oral use Read this Medication Guide carefully before you start taking SEGLUROMET and each time you
Application of the Diabetes Algorithm to a Patient
 Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Diabetes Mellitus Type 2
 Diabetes Mellitus Type 2 Definition Type 2 diabetes, once known as adult-onset or noninsulin-dependent diabetes, is a chronic condition that affects the way your body metabolizes sugar (glucose), your
Diabetes Mellitus Type 2 Definition Type 2 diabetes, once known as adult-onset or noninsulin-dependent diabetes, is a chronic condition that affects the way your body metabolizes sugar (glucose), your
Type 1 Diabetes - Pediatrics
 Type 1 Diabetes - Pediatrics Introduction Type 1 diabetes prevents the body from removing sugar from the blood stream normally. Diabetes can lead to serious health problems if it is not treated. Currently
Type 1 Diabetes - Pediatrics Introduction Type 1 diabetes prevents the body from removing sugar from the blood stream normally. Diabetes can lead to serious health problems if it is not treated. Currently
Training Your Caregiver: Diabetes
 Diabetes, often referred to by doctors as diabetes mellitus, describes a group of metabolic diseases in which the person has high blood glucose (blood sugar), either because insulin production is inadequate,
Diabetes, often referred to by doctors as diabetes mellitus, describes a group of metabolic diseases in which the person has high blood glucose (blood sugar), either because insulin production is inadequate,
Diabetes-Facing it Head On! Going for the 3 Increases: Increase in Health, Increase in Happiness & Increase in Energy
 Diabetes-Facing it Head On! Going for the 3 Increases: Increase in Health, Increase in Happiness & Increase in Energy Strategies for Success in Health Management By: James J. Messina, Ph.D. What is Type
Diabetes-Facing it Head On! Going for the 3 Increases: Increase in Health, Increase in Happiness & Increase in Energy Strategies for Success in Health Management By: James J. Messina, Ph.D. What is Type
Follow-Up Patient Self-Assessment (Version 2)
 Follow-Up Patient Self-Assessment (Version 2) Demographics: Name: Address: E-mail: Phone Number: Date of Birth: What is your height? What is your current weight? feet inches lbs Have there been any change(s)
Follow-Up Patient Self-Assessment (Version 2) Demographics: Name: Address: E-mail: Phone Number: Date of Birth: What is your height? What is your current weight? feet inches lbs Have there been any change(s)
Diabetes Summary of Medical Guidelines
 Diabetes Summary of Medical Guidelines Key concepts in setting glycemic controls: goals should be individualized; certain populations (children, pregnant women, and elderly) require special considerations;
Diabetes Summary of Medical Guidelines Key concepts in setting glycemic controls: goals should be individualized; certain populations (children, pregnant women, and elderly) require special considerations;
Diabetes Refresher Head to Toe
 Diabetes Refresher Head to Toe Clinical Health Education 7/1/2014 Chronic Conditions Management Department What contributes to diabetes complications? What are you doing now to prevent these complications?
Diabetes Refresher Head to Toe Clinical Health Education 7/1/2014 Chronic Conditions Management Department What contributes to diabetes complications? What are you doing now to prevent these complications?
Diabetes and stroke. What is diabetes? What are the symptoms of diabetes? Stroke Helpline: Website: stroke.org.uk
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Diabetes is a condition caused by too much sugar in your blood. There are over three million people in the UK who have diabetes. If it s not controlled
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Diabetes is a condition caused by too much sugar in your blood. There are over three million people in the UK who have diabetes. If it s not controlled
