Clin Transplant 2005 DOI: /j x Copyright r Blackwell Munksgaard 2005 Clinical Transplantation
|
|
|
- Shavonne Morrison
- 5 years ago
- Views:
Transcription
1 Clin Transplant 2005 DOI: /j x Copyright r Blackwell Munksgaard 2005 Clinical Transplantation The low-dose (1 mg) adrenocorticotropin stimulation test in kidney and kidney pancreas transplant patients: a potential guideline for steroid withdrawal Baz-Hecht M, Osher E, Yachnin T, Nakache R, Nakache G, Tordjman K, Stern N. The low-dose (1 mg) adrenocorticotropin stimulation test in kidney and kidney pancreas transplant patients: a potential guideline for steroid withdrawal. Clin Transplant 2005 DOI: /j x r Blackwell Munksgaard, 2005 Abstract: Chronic steroid treatment is known to impair the hypothalamic pituitary adrenal axis (HPA) but the need to assess HPA function prior to withdrawal of steroid therapy in post-transplant patients has not been uniformly accepted. We evaluated the status of the HPA axis in 48 kidney or kidney pancreas transplant patients who were considered for possible discontinuation of glucocorticoid therapy using a recently validated dynamic test of HPA integrity, the low-dose (1 mg) adrenocorticotropin (ACTH) test. HPA suppression was detected in 29 (60%) of the patients, four of which had severe hypoadrenalism prohibitive of steroid withdrawal. Neither the duration of steroid treatment nor 8:00 AM serum cortisol was a useful marker of hypoadrenalism. 8:00 AM cortisol in subjects with normal HPA reserve and subjects with partial hypoadrenalism overlapped considerably but levels o5 mg/dl were indicative of severe hypoadrenalism. Pre-withdrawal diagnosis of partial hypoadrenalism allowed the identification of subjects requiring no further steroid replacement under regular daily circumstances. However glucocorticoid supplementation was prescribed in the event of stress such as infection, exceptional effort, trauma or surgery. Individuals with partial HPA impairment, but not patients with severe HPA suppression, improved upon retesting 3 months later. Patients exhibiting normal response to 1 mcg ACTH enjoyed an uneventful course following steroid withdrawal. Since hypoadrenalism is extremely common in post-transplant patients, we recommend the use of the low-dose ACTH test as a convenient method to identify patients with various degrees of hypoadrenalism prior to steroid withdrawal. MBaz-Hecht a, E Osher a, T Yachnin b, R Nakache b, GNakache b,ktordjman a and NStern a a Institute of Endocrinology, Metabolism and Hypertension and b The Unit of Organ Transplantation, Sackler Faculty of Medicine, Tel Aviv Sourasky Medical Center, Tel Aviv University,TelAviv,Israel Key words: adrenocorticotropin test kidney/ kidney pancreas transplantation steroid withdrawal Corresonding author: Merav Baz Hecht MD, 15 Winthrop Rd, Brookline, MA, 02445, USA. Tel.: ; fax: ; meravbh@comcast.net Accepted for publication 29 July 2005 Long-term treatment with corticosteroids may suppress normal pituitary adrenal axis function and expose the patient to risk if corticosteroids are withdrawn, especially under stressful conditions such as surgery or severe infection. Corticosteroids have been a part of anti-rejection treatment since the beginning of solid organ transplantation. To minimize unfavorable metabolic side effects with long-term treatment, multiple protocols have been proposed for the withdrawal of corticosteroids at various intervals after transplantation (1 7). The adrenocorticotropin (ACTH) test is used to assess hypothalamic pituitary adrenal (HPA) reserve. Traditionally, this test was based on the use of a high dose of ACTH (250 mg). Following the intravenous administration of this dose, circulating ACTH levels increase much above the concentrations of endogenous ACTH observed under 72
2 Low-dose ACTH test in kidney transplant patients stressful conditions or in response to the gold standard test of assessing the integrity of the HPA axis, i.e., insulin induced hypoglycemia (8). As the traditional high dose ACTH test provides a supraphysiologic stimulus to the adrenal cortex it could overcome partial impairment in the HPA reserve and elicit a falsely normal response. Indeed, there is substantial evidence that, despite its simplicity and worldwide acceptance, the traditional high dose ACTH test misses up to 30 50% of patients with well- documented secondary hypoadrenalism (9,10), most of whom are afflicted with partial impairment but some with severe, occasionally life threatening cortisol deficiency. Based on these considerations, the use of the low-dose of ACTH (mostly 1 mg) has been introduced into clinical endocrine testing in recent years (11 15). Further, several studies have demonstrated that this test detects impairment in the function of the HPA axis in patients subjected to various forms of glucocorticoid therapy (14 16). Previous studies have tested the pituitary adrenal axis in kidney-transplant patients using the 250 mg ACTH test. These reports have focused on kidneytransplant patients returning to hemodyalysis (17 19), or after a stressful event (20). One study addressed the elective process of steroid withdrawal in stable post-transplant patients employing the 1 mg ACTH test to assess adrenal response (21). Our study assessed the prevalence of adrenal suppression in stable kidney transplant patients and the usefulness of the 1 mg ACTH test as guidance before steroid withdrawal, and suggests a cutoff point predictive of expected consequences of steroid withdrawal. Patients and methods Kidney and kidney pancreas transplant patients were selected from January 2001 to December 2002 as candidates for steroid withdrawal using the following criteria: no evidence of acute rejection 3 6 months after transplantation; stable serum creatinine for at least 6 months; triple drug immunosuppression prior to steroid withdrawal. At that point all patients were already on a lowdose of prednisone (5 mg/d) combined with a calcineurine inhibitor (cyclosporine or tacrolimus) and an antimetabolic drug (azathioprine or mycophenolate mofetil). We measured 8:00 AM serum cortisol level in all patients before taking their daily prednisone tablets. In patients in whom cortisol level was 15 mg/dl we proceeded with withdrawal of prednisone. If 8:00 AM cortisol level was o15 mg/ dl patients were scheduled to undergo the low-dose ACTH test. During the test, 1 mg of synacten (synthetic 1 34 ACTH) was injected intravenously. Serum cortisol level was measured just before and as well as 20, 30 and 40 min after the administration of synacten. Based on the results of the test patients were classified into three groups: (i) Normal responders, in whom peak stimulated cortisol level was 18 mg/dl (12,13); (ii) Borderline responders, whose peak stimulated cortisol level was o18 mg/ dl, but whose 8:00 AM cortisol level was 45 mg/dl; (iii) Abnormal responders in whom 8:00 AM cortisol level was o5 mg/dl and stimulated cortisol level was o18 mg/dl. Patients exhibiting a normal response were taken off steroid therapy. In patients with borderline test prednisone treatment was also withdrawn. However, these subjects were closely monitored for symptoms of steroid deficiency. Patients with an abnormal test continued to receive a maintenance dose of prednisone (5 7.5 mg/d). Patients underwent physical examination, blood tests and 24 urine collections for creatinine clearance before as well as 3 months after steroid withdrawal. Serum creatinine level was measured every 1 2 wk during the first month after steroid withdrawal and at monthly intervals thereafter. In patients with borderline response the ACTH test was repeated 3 months after steroid withdrawal. Statistical analysis We used Paired t-test and the Wilcoxon non-parametric test to compare various parameters after 3 months of steroid withdrawal with baseline levels. Analysis of variance was performed to examine the association between length of steroid treatment and the results of the 1 mg ACTH test. Statistical significance level was set to The SPSS software (version 10.0, SPSS Inc., Chicago, IL, USA) was used for the analysis. Results HPA assessment with the 1 mg ACTH test was performed in 48 kidney and kidney pancreas transplant patients included in our study. In the process of evaluation, 17 patients were deemed inappropriate for steroid withdrawal for reasons unrelated to the results of this test but were included in the overall analysis. There were 20 females and 28 males, 37 with kidney transplant and 11 with kidney pancreas transplant. From these, the cohort organs were harvested from 29 cadaver donors and 19 livingrelated donors. In 40 of the patients included in this series this was the first transplantation whereas for eight patients the present procedure was the second transplantation. The patients age at the time of transplantation was yr (range, yr). The primary causes of end stage kidney disease 73
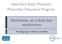
3 Baz-Hecht et al. were diabetes mellitus (type 1 diabetes 11 patients; type 2 diabetes two patients), polycystic kidneys (seven patients), chronic glomerulonephritis (eight patients), and hypertension (four patients). Less common underlying diseases were chronic pyelonephritis (two patients), interstitial nephritis (three patients), Alport s disease (two patients), nephrolithiasis (two patients) and reflux, oxaluria, and cystinuria (one patient each). In 4 patients the cause of kidney failure remained unknown. The mean duration of steroid treatment prior to performing the ACTH test was wk. The results of the 1 mg ACTH test were normal in 19 patients, borderline in 25 patients and abnormal in four patients (Figs 1 3). There was no correlation between the duration of steroid treatment and the results of the test. Four patients had a grossly abnormal cortisol response profile, with 8:00 AM cortisol levels ranging at mg/dl and peak ACTH stimulated cortisol levels of mg/dl (Fig. 3). These individuals who fulfilled standard criteria for overt hypoadrenalism, were the only patients in the present series whose 8:00 AM cortisol levels were o5 mg/dl. All patients but one from whom steroids were withdrawn, did not experience any Fig. 3. Peak vs. 8:00 AM cortisol levels according to 1 mg synacten test result. symptoms of steroid withdrawal. One patient with a borderline results (8:00 AM cortisol of 7 mg/dl and peak stimulated cortisol of 10.4 mg/dl) developed severe weakness upon prednisone withdrawal necessitating the re-administration of a maintenance dose. In three patients steroid treatment was renewed because of a rise in creatinine level: in one patient 1 week following the withdrawal of prednisone; in the two other patients 10 and 12 months after the discontinuation of glucocorticoid therapy. When the 1 mg ACTH test was repeated 3 months after steroid withdrawal (n 5 13), the cortisol response improved, though it did not necessarily normalize, in all patients with borderline results (data not shown) except for the patient who developed severe weakness following the attempted withdrawal of steroids. Normalization was observed in 5/9 subjects with initial borderline results, but not in Table 1. Clinical and laboratory parameters of the study cohort before and 3 months after steroid withdrawal. Values are mean 7 SEM Fig. 1. 8:00 AM cortisol levels (mean 7 SEM). Fig. 2. Peak cortisol levels according to 1 mg synacten test results (results are shown as mean 7 SEM). Parameter Before After Mean % change p-value Weight (kg) NS BMI (kg/m 2 ) NS Systolic BP (mmhg) Diastolic BP (mmhg) NS Glucose (mg/dl) NS HbA1c (%) a NS Total cholesterol (mg/dl) Triglycerides (mg/dl) NS HDL (mg/dl) NS LDL (mg/dl) a NS Creatinine (mg/dl) NS Creatinine clearance a NS (ml/min) Na (meq/l) NS K(meq/L) NS a HbA1c was available only in 12 patients, LDL-cholesterol only in 15 patients and creatinine clearance only in 13 of 25 patients. 74
4 Low-dose ACTH test in kidney transplant patients Table 2. The changes in body mass index (BMI) according to prewithdrawal BMI BMI Number of patients Change (%) BMI r obmi o BMI any of the four patients with severe depression of the pituitary-adrenal axis upon the initial testing. Table 1 depicts several anthropometric, clinical and biochemical parameters recorded before as well as 3 months after steroid withdrawal. As shown, significant reductions were noted in systolic blood pressure and total cholesterol but not in any of the other parameters listed. Because of an unexpected trend for body mass index (BMI) elevation after the withdrawal of steroids, we reanalyzed the change in BMI according to pre-withdrawal BMI. Patients were divided into standard weights, normal weight (BMI r25), overweight (25o BMI o30), and obese (BMI 30). As shown in Table 2, the main increase in BMI was seen in the group of normal weight patients and not in the obese patients. Discussion The 1 mg ACTH test was used in this study to evaluate its use for the detection of HPA dysfunction in kidney and kidney pancreas transplant patients in whom steroid withdrawal is being considered in light of an apparent favorable status of the transplant itself. Several findings in the present analysis could apply well to the daily care of such patients. In this series of consecutive and unselected 48 transplant patients subjected to glucocorticoid therapy for a rather variable duration, only 40% (19 patients) had an entirely normal test, whereas 60% responded abnormally: 25 (52%) had partial impairment of the HPA axis and 4 (8%) had severe depression of HPA. The distinction between borderline and abnormal results is clearly arbitrary as best exemplified by the patient with a borderline response who required resumption of prednisone therapy shortly after withdrawal. Indeed, current criteria for the diagnosis of HPA suppression do not address the distinction between partial and complete hypoadrenalism but rather between normal and subnormal results. Hence, while the precise definition of borderline or partial impairment of the HPA axis following glucocorticoid therapy awaits further refinement, the protocol followed by us proved fairly useful, as withdrawal from steroids based on the results of the 1 mg ACTH test was without symptoms of cortisol deficiency in all subjects but one. Overall, the high rate of diagnosed hypoadrenalism in our study is in agreement with four previous reports in which HPA suppression, diagnosed by the more traditional 250 mg ACTH test, was observed in 44% to 66% of kidney transplant patients (17 20). Based on the reported higher sensitivity of the 1 mg ACTH test, one might have expected that it would yield a higher rate of abnormal results than the 250 mg test. One possible explanation for the apparent lack of such difference between our study and previous reports utilizing the high dose test may be the longer duration of steroid therapy in the other studies. Particularly in the article reporting the highest rate of HPA axis impairment, where subnormal response to ACTH was detected in 66% of patients, nine of 21 patients received steroids for periods exceeding 302 wk (18), which was the longest period of steroid treatment in our study (applied only in one of 48 patients). While no correlation between the length of treatment and the appearance of hyoadrenalism was found in our patients, it is plausible that this applies to short to medium treatment periods only, whereas following extremely long steroid therapy, such as reported by Rodger et al. (18), suppression of the HPA axis may be more common. A recently reported study (21), used a more stringent cutoff level of 20 mg/dl instead of 18 mg/dl and yet 69% of their patients had normal ACTH test results, which is about double of ours, and double the results of other studies (17 20) that used the much higher ACTH dose (250 mg/dl). Moreover, the mean duration of steroid treatment in that study was about double (36 months) of ours, inviting more and not less adrenal axis impairment. Separately, that study s 8:00 AM cortisol levels unexpectedly decreased after steroid withdrawal, all which may suggest some difference in methods. The 8:00 AM serum cortisol per se is clearly insufficient to correctly identify glucocorticoid treated transplant patients with HPA axis impairment. As shown in Figs 1 3, only subjects with severe HPA suppression can be singled out based on 8:00 AM cortisol levels. In contrast, baseline serum cortisol levels 45 mg/dl provide no specific information as concentrations in normal subjects and in patients with partial secondary hypoadrenalism overlap considerably. Based on the first 3 months of follow-up, all subjects considered normal by the cortisol response to 1 mg ACTH, indeed enjoyed an uneventful course in terms of their adrenal reserve. Resumption of steroid treatment, when indicated, was dictated by the status of the transplant (i.e. a rising serum creatinine), not by the HPA status. 75
5 Baz-Hecht et al. The identification of a borderline cortisol response to 1 mg ACTH may be a good predictor of further improvement upon repeat testing within 3 months, whereas a grossly abnormal response appears to be associated with protracted hypoadrenalism within the same time frame. This would suggest that repeat ACTH testing in transplant patients with grossly suppressed adrenal function due to steroid treatment should be considered only after time intervals exceeding 3 months. A reasonable practice, (though presently not supported by specific evidence) would be to defer repeat testing in these patients until the 8:00 AM serum cortisol rises above 5 mg/dl. The significant reduction in systolic blood pressure and total cholesterol 3 months after steroid withdrawal suggests that even at low maintenance doses may have deleterious metabolic effects. Similarly, Hricik et al. (4) observed significant reduction in blood pressure, cholesterol level, and glycohemoglobin following steroid withdrawal. Fabrega et al. (2) reported favorable effect of steroid withdrawal on glucose homeostasis, body weight and hypertension in post-kidney-transplant diabetic patients. In contrast, Sivaraman et al. (6) reported that metabolic benefits were noted when prednisone was tapered down from 10 mg/d to 10 mg every other day, with no further improvement upon discontinuation of steroid treatment. Further, as our patients were closely followed and aggressively treated for hypertension, diabetes, hyperlipidemia and other cardiovascular risk factors before and as well as during the 3 months of follow-up, this type of intervention could have obscured even larger benefits that might have resulted from steroid withdrawal per se. In conclusion our work shows that a significant percentage of kidney/kidney pancreas transplant patients have depressed adrenal reserve that cannot be predicted by either the length of prior steroid treatment or by 8:00 AM serum cortisol. The 1 mg ACTH test is easy to perform and provides useful information, which facilitates rational treatment of these complex patients. We recommended its routine use before the elective process of steroid withdrawal. References 1. HRICIK DE, WHALEN CC, LAUTMAN J et al. Withdrawal of steroids after renal transplantation clinical predictors of outcome. Transplantation 1992: 53: FABREGA AJ, COHAN J, MESLAR P, POLLAK R. Effect of steroid withdrawal on long-term renal allograft recipients with posttransplantation diabetes mellitus. Surgery 1994: 116: RATCLIFFE PJ, DUDLEY CR, HIGGINS RM, FIRTH JD, SMITH B, MORRIS PJ. Randomized controlled trial of steroid withdrawal in renal transplant recipients receiving triple immunosuppression. Lancet 1996: 348: HRICIK DE, SCHULAK JA. Metabolic effects of steroid withdrawal in adult renal transplant recipients. Kidney Int Suppl 1993: 43: S GOMEZ E, LAURES A, POBES A, BALTAR J, PORTAL CG, NAVASCUES R. Steroid withdrawal in renal transplantation treated with cyclosporine A: long term evaluation. Transplant Proc 2001: 33: SIVARAMAN P, NUSSBAUMER G, LANDSBERG D. Lack of longterm benefit of steroid withdrawal in renal transplant recipients. Am J Kidney Dis 2001: 37: PASCUAL J, QUEREDA C, ZAMORA J, HERNANDEZ D, Spanish Group for Evidence-Based Medicine in Renal Transplantation. Steroid withdrawal in renal transplant patients on triple therapy with a calcineurin inhibitor and mycophenolate mofetil: a meta-analysis of randomized, controlled trials. Transplantation 2004: 78: DARMON P, DADOUN F, FRACHEBOIS C et al. On the meaning of low-dose ACTH(1 24) tests to assess functionality of the hypothalamic pituitary adrenal axis. Eur J Endocrinol 1999: 140: LINDHOLM J, KEHLET H. Re-evaluation of the clinical value of the 30 min ACTH test in assessing the hypothalamic pituitary adrenocortical function. Clin Endocrinol 1987: 26: HUREL SJ, THOMPSON CJ, WATSON MJ, HARRIS MM, BAYLIS PH, KENDALL-TAYLOR P. The short term synacthen and insulin stress tests in the assessment of the hypothalamic pituitary adrenal axis. Clin Endocrinol 1996: 44: DICKSTEIN G, SHECHNER C, NICHOLSON WE et al. Adrenocorticotropin stimulation test: effects of basal cortisol level, time of day, and suggested new sensitive low dose test. J Clin Endocrinol Metab 1991: 72: TORDJMAN K, JAFFE A, GRAZAS N, APTER C, STERN N. The role of the low dose (1 microgram) adrenocorticotropin test in the evaluation of patients with pituitary diseases. J Clin Endocrinol Metab 1995: 80: TORDJMAN K, JAFFE A, TROSTANETSKY Y, GREENMAN Y, LIMOR R, STERN N. Low-dose (1 microgram) adrenocorticotropin (ACTH) stimulation as a screening test for impaired hypothalamo pituitary adrenal axis function: sensitivity, specificity and accuracy in comparison with the high-dose (250 microgram) test. Clin Endocrinol 2000: 52: BROIDE J, SOFERMAN R, KIVITY S et al. Low-dose adrenocorticotropin test reveals impaired adrenal function in patients taking inhaled corticosteroids. J Clin Endocrinol Metab 1995: 80: KANNISTO S, KORPPI M, REMES K, VOUTILAINEN R. Serum dehydroepiandrosterone sulfate concentration as an indicator of adrenocortical suppression in asthmatic children treated with inhaled steroids. J Clin Endocrinol Metab 2001: 86: HENZEN C, SUTER A, LERCH E, URBINELLI R, SCHORNO XH, BRINER VA. Suppression and recovery of adrenal response after short-term, high-dose glucocorticoid treatment. Lancet 2000: 355: CANAFAX DM, MANN HJ, SUTHERLAND DER, SIMMONS RL, NAJARIAN JS. The use of a cosyntropin stimulation test to predict adrenal suppression in renal transplant patients being withdrawn from prednisone. Transplantation 1983: 36: RODGER RS, WATSON MJ, SELLARS L, WILKINSON R, WARD MK, KERR DN. Hypothalamic pituitary adrenocortical 76
6 Low-dose ACTH test in kidney transplant patients suppression and recovery in renal transplant patients returning to maintenance dialysis. Q J Med 1986: 61: SHAPIRO R, CARROLL PB, TZAKIS AG, CEMAJ S, LOPATIN WB, NAKAZATO P. Adrenal reserve in renal transplant recipients with cyclosporine, azathioprine, and prednisone immunsupression. Transplantation 1990: 49: BROMBERG SJ, ALFREY EJ, BARKER CF et al. Adrenal suppression and steroid withdrawal in renal transplant recipients. Transplantation 1991: 51: MIOZZARI M, AMBUHL PM. Steroid withdrawal after longterm medication for immunosuppressive therapy in renal transplant patients: adrenal response and clinical implications. Nephrol Dial Transplant 2004: 19:
Steroid withdrawal after long-term medication for immunosuppressive therapy in renal transplant patients: adrenal response and clinical implications
 Nephrol Dial Transplant (2004) 19: 2615 2621 doi:10.1093/ndt/gfh421 Advance Access publication 27 July 2004 Original Article Steroid withdrawal after long-term medication for immunosuppressive therapy
Nephrol Dial Transplant (2004) 19: 2615 2621 doi:10.1093/ndt/gfh421 Advance Access publication 27 July 2004 Original Article Steroid withdrawal after long-term medication for immunosuppressive therapy
REACH Risk Evaluation to Achieve Cardiovascular Health
 Dyslipidemia and transplantation History: An 8-year-old boy presented with generalized edema and hypertension. A renal biopsy confirmed a diagnosis of focal segmental glomerulosclerosis (FSGS). After his
Dyslipidemia and transplantation History: An 8-year-old boy presented with generalized edema and hypertension. A renal biopsy confirmed a diagnosis of focal segmental glomerulosclerosis (FSGS). After his
CHAPTER 5 RENAL TRANSPLANTATION. Editor: Dr Goh Bak Leong
 CHAPTER 5 RENAL TRANSPLANTATION Editor: Dr Goh Bak Leong Expert Panel: Dr Goh Bak Leong (Chair) Dato Dr (Mr) Rohan Malek Dr Wong Hin Seng Dr Fan Kin Sing Dr Rosnawati Yahya Dr S Prasad Menon Dr Tan Si
CHAPTER 5 RENAL TRANSPLANTATION Editor: Dr Goh Bak Leong Expert Panel: Dr Goh Bak Leong (Chair) Dato Dr (Mr) Rohan Malek Dr Wong Hin Seng Dr Fan Kin Sing Dr Rosnawati Yahya Dr S Prasad Menon Dr Tan Si
The one microgram adrenocorticotropin test in the assessment of hypothalamic pituitary adrenal function
 European Journal of Endocrinology (1998) 139 575 579 ISSN 0804-4643 The one microgram adrenocorticotropin test in the assessment of hypothalamic pituitary adrenal function Bruno Ambrosi, Laura Barbetta,
European Journal of Endocrinology (1998) 139 575 579 ISSN 0804-4643 The one microgram adrenocorticotropin test in the assessment of hypothalamic pituitary adrenal function Bruno Ambrosi, Laura Barbetta,
Organ rejection is one of the serious
 Original Article Outcomes of Late Corticosteroid Withdrawal after Renal Transplantation in Patients Exposed to Tacrolimus and/or Mycophenolate Mofetil: Meta-Analysis of Randomized Controlled Trials A.
Original Article Outcomes of Late Corticosteroid Withdrawal after Renal Transplantation in Patients Exposed to Tacrolimus and/or Mycophenolate Mofetil: Meta-Analysis of Randomized Controlled Trials A.
CHAPTER 5 RENAL TRANSPLANTATION
 CHAPTER 5 RENAL TRANSPLANTATION Editor: Dr. Goh Bak Leong Expert Panel: Dato Dr. Zaki Morad b Mohd Zaher (Chair) Dr. Goh Bak Leong (Co-Chair) Dr. Fan Kin Sing Dr. Lily Mushahar Mr. Rohan Malek Dr. S. Prasad
CHAPTER 5 RENAL TRANSPLANTATION Editor: Dr. Goh Bak Leong Expert Panel: Dato Dr. Zaki Morad b Mohd Zaher (Chair) Dr. Goh Bak Leong (Co-Chair) Dr. Fan Kin Sing Dr. Lily Mushahar Mr. Rohan Malek Dr. S. Prasad
CHAPTER 14. Renal Transplantation
 15th Report of the Malaysian RENAL TRANSPLANTATION CHAPTER 14 Renal Transplantation Editor: Dr. Goh Bak Leong Expert Panel: : Dato Dr. Dato Zaki Dr. Morad Zaik Morad Mohd (Chair) Zaher (Chair) Dr. Goh
15th Report of the Malaysian RENAL TRANSPLANTATION CHAPTER 14 Renal Transplantation Editor: Dr. Goh Bak Leong Expert Panel: : Dato Dr. Dato Zaki Dr. Morad Zaik Morad Mohd (Chair) Zaher (Chair) Dr. Goh
CHAPTER 5 RENAL TRANSPLANTATION. Editor: Dr Goh Bak Leong
 CHAPTER 5 RENAL TRANSPLANTATION Editor: Dr Goh Bak Leong Expert Panel: Dr Goh Bak Leong (Chair) Dato Dr Zaki Morad Mohd Zaher Dato Dr (Mr) Rohan Malek Dr Fan Kin Sing Dr Lily Mushahar Dr Lim Soo Kun Dr
CHAPTER 5 RENAL TRANSPLANTATION Editor: Dr Goh Bak Leong Expert Panel: Dr Goh Bak Leong (Chair) Dato Dr Zaki Morad Mohd Zaher Dato Dr (Mr) Rohan Malek Dr Fan Kin Sing Dr Lily Mushahar Dr Lim Soo Kun Dr
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Ahmed Al Nahari Pediatric Endocrinology Fellow March 11,2016
 Ahmed Al Nahari Pediatric Endocrinology Fellow March 11,2016 Scholar: Review the literature in an evidenced based manner to determine the difference in our clinical setting. Advocate: Develop a better
Ahmed Al Nahari Pediatric Endocrinology Fellow March 11,2016 Scholar: Review the literature in an evidenced based manner to determine the difference in our clinical setting. Advocate: Develop a better
Objectives. Kidney Complications With Diabetes. Case 10/21/2015
 Objectives Kidney Complications With Diabetes Brian Boerner, MD Diabetes, Endocrinology, and Metabolism University of Nebraska Medical Center Review screening for, and management of, albuminuria Review
Objectives Kidney Complications With Diabetes Brian Boerner, MD Diabetes, Endocrinology, and Metabolism University of Nebraska Medical Center Review screening for, and management of, albuminuria Review
CHAPTER 5 RENAL TRANSPLANTATION. Editor: Rosnawati Yahya. Expert Panels: Hooi Lai Seong Ng Kok Peng Suryati Binti Yakaob Wong Hin Seng.
 CHAPTER 5 Editor: Roswati Yahya Expert Panels: Hooi Lai Seong Ng Kok Peng Suryati Binti Yakaob Wong Hin Seng Contents 5. Stock and Flow of Rel Transplantation Stock and Flow Transplant Rates 5.2 Recipients
CHAPTER 5 Editor: Roswati Yahya Expert Panels: Hooi Lai Seong Ng Kok Peng Suryati Binti Yakaob Wong Hin Seng Contents 5. Stock and Flow of Rel Transplantation Stock and Flow Transplant Rates 5.2 Recipients
CHAPTER 5 RENAL TRANSPLANTATION. Editor: Dr Rosnawati Yahya
 CHAPTER 5 Editor: Dr Rosnawati Yahya Expert Panels: Dr Rosnawati Yahya Dr Ng Kok Peng Dr Suryati Binti Yakaob Dr Mohd Zaimi Abd Wahab Dr Yee Seow Ying Dr Wong Hin Seng Contents 5. Stock and Flow of Renal
CHAPTER 5 Editor: Dr Rosnawati Yahya Expert Panels: Dr Rosnawati Yahya Dr Ng Kok Peng Dr Suryati Binti Yakaob Dr Mohd Zaimi Abd Wahab Dr Yee Seow Ying Dr Wong Hin Seng Contents 5. Stock and Flow of Renal
Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study
 NDT Plus (2010) 3 [Suppl 2]: ii32 ii36 doi: 10.1093/ndtplus/sfq064 Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study Miguel Gonzalez-Molina 1, Miguel Angel
NDT Plus (2010) 3 [Suppl 2]: ii32 ii36 doi: 10.1093/ndtplus/sfq064 Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study Miguel Gonzalez-Molina 1, Miguel Angel
OUT OF DATE. Choice of calcineurin inhibitors in adult renal transplantation: Effects on transplant outcomes
 nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
STUDY. Prevalence of Adrenal Insufficiency Following Systemic Glucocorticoid Therapy in Infants With Hemangiomas
 STUDY Prevalence of Adrenal Insufficiency Following Systemic Glucocorticoid Therapy in Infants With Hemangiomas Jefferson P. Lomenick, MD; Kent L. Reifschneider, MD; Anne W. Lucky, MD; Denise Adams, MD;
STUDY Prevalence of Adrenal Insufficiency Following Systemic Glucocorticoid Therapy in Infants With Hemangiomas Jefferson P. Lomenick, MD; Kent L. Reifschneider, MD; Anne W. Lucky, MD; Denise Adams, MD;
Endocrine Topic Review. Sethanant Sethakarun, MD
 Endocrine Topic Review Sethanant Sethakarun, MD Definition Cushing's syndrome comprises a large group of signs and symptoms that reflect prolonged and in appropriately high exposure of tissue to glucocorticoids
Endocrine Topic Review Sethanant Sethakarun, MD Definition Cushing's syndrome comprises a large group of signs and symptoms that reflect prolonged and in appropriately high exposure of tissue to glucocorticoids
CHISCG1: Short Synacthen Test for the Investigation of Adrenal Insufficiency
 Pathology at the Royal Derby Hospital Short Synacthen Test Standard Clinical Guidelines Chemical Pathology Department Valid Until 31 st August 2011 Document Code: CHISCG1 Short Synacthen Test for the Investigation
Pathology at the Royal Derby Hospital Short Synacthen Test Standard Clinical Guidelines Chemical Pathology Department Valid Until 31 st August 2011 Document Code: CHISCG1 Short Synacthen Test for the Investigation
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Acthar Gel. H. P. Acthar Gel (corticotropin; ACTH) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 7 Last Review Date: November 30, 2018 Acthar Gel Description H.
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 7 Last Review Date: November 30, 2018 Acthar Gel Description H.
Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation
 IJMS Vol 34, No 2, June 2009 Original Article Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation Reza Hekmat, Hamid Eshraghi Abstract Background:
IJMS Vol 34, No 2, June 2009 Original Article Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation Reza Hekmat, Hamid Eshraghi Abstract Background:
Prediction of Adrenocortical Insufficiency After Pituitary Adenoma Surgery Using Postoperative Basal Cortisol Levels
 Physiol. Res. 64: 531-536, 2015 Prediction of Adrenocortical Insufficiency After Pituitary Adenoma Surgery Using Postoperative Basal Cortisol Levels V. HÁNA Jr. 1, J. JEŽKOVÁ 1, M. KOSÁK 1, M. KRŠEK 1,
Physiol. Res. 64: 531-536, 2015 Prediction of Adrenocortical Insufficiency After Pituitary Adenoma Surgery Using Postoperative Basal Cortisol Levels V. HÁNA Jr. 1, J. JEŽKOVÁ 1, M. KOSÁK 1, M. KRŠEK 1,
The Journal of Bioscience and Medicine 3, 1 (2013) Article
 The Journal of Bioscience and Medicine 3, 1 (2013) Article Early postoperative serum cortisol measurements guide management in a steroid-sparing protocol and predict need for long-term steroid replacement
The Journal of Bioscience and Medicine 3, 1 (2013) Article Early postoperative serum cortisol measurements guide management in a steroid-sparing protocol and predict need for long-term steroid replacement
Considering the early proactive switch from a CNI to an mtor-inhibitor (Case: Male, age 34) Josep M. Campistol
 Considering the early proactive switch from a CNI to an mtor-inhibitor (Case: Male, age 34) Josep M. Campistol Patient details Name DOB ESRD Other history Mr. B.I.B. 12 January 1975 (34yo) Membranous GN
Considering the early proactive switch from a CNI to an mtor-inhibitor (Case: Male, age 34) Josep M. Campistol Patient details Name DOB ESRD Other history Mr. B.I.B. 12 January 1975 (34yo) Membranous GN
Date: 23 June Context and policy issues:
 Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy
 ISPUB.COM The Internet Journal of Urology Volume 9 Number 1 Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy S Bontha, N Sanalkumar, M Istarabadi, G Lepsien,
ISPUB.COM The Internet Journal of Urology Volume 9 Number 1 Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy S Bontha, N Sanalkumar, M Istarabadi, G Lepsien,
Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study. Arab Medical University. Benghazi, Libya
 Original Article Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study Alshkri MM 1, Elmehdawi RR 2 1 Benghazi Diabetes Center. 2 Medical Department, Faculty of Medicine,
Original Article Metabolic Syndrome among Type-2 Diabetic Patients in Benghazi- Libya: A pilot study Alshkri MM 1, Elmehdawi RR 2 1 Benghazi Diabetes Center. 2 Medical Department, Faculty of Medicine,
Recommendations differ slightly in defining a suppressed patient, but general guidelines are below (Table 1):
 PJ Nicholoff Steroid Protocol Background/Assessment Normal basal secretion of cortisol from the adrenal gland is approximately 5-7 mg/m2/day or 8-10 mg/day for adults. This amount increases during minor
PJ Nicholoff Steroid Protocol Background/Assessment Normal basal secretion of cortisol from the adrenal gland is approximately 5-7 mg/m2/day or 8-10 mg/day for adults. This amount increases during minor
cortisol level: a reliable and costeffective
 Original Article Singapore Med J 2007; 48 (6) : 519 Sixty -minute post-synacthen serum cortisol level: a reliable and costeffective screening test for excluding adrenal insufficiency compared to the conventional
Original Article Singapore Med J 2007; 48 (6) : 519 Sixty -minute post-synacthen serum cortisol level: a reliable and costeffective screening test for excluding adrenal insufficiency compared to the conventional
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
Impact of Physical Activity on Metabolic Change in Type 2 Diabetes Mellitus Patients
 2012 International Conference on Life Science and Engineering IPCBEE vol.45 (2012) (2012) IACSIT Press, Singapore DOI: 10.7763/IPCBEE. 2012. V45. 14 Impact of Physical Activity on Metabolic Change in Type
2012 International Conference on Life Science and Engineering IPCBEE vol.45 (2012) (2012) IACSIT Press, Singapore DOI: 10.7763/IPCBEE. 2012. V45. 14 Impact of Physical Activity on Metabolic Change in Type
UNUSUAL CAUSE OF ADRENAL INSUFFICIENCY. Dr.Khushboo Dr.S.Balasubramanian s unit
 UNUSUAL CAUSE OF ADRENAL INSUFFICIENCY Dr.Khushboo Dr.S.Balasubramanian s unit BRIEF HISTORY 7 year old male child presented with Fever : 3 days Vomiting : 3 days h/0 Acute encephalopathy with fever O/E
UNUSUAL CAUSE OF ADRENAL INSUFFICIENCY Dr.Khushboo Dr.S.Balasubramanian s unit BRIEF HISTORY 7 year old male child presented with Fever : 3 days Vomiting : 3 days h/0 Acute encephalopathy with fever O/E
Cedars Sinai Diabetes. Michael A. Weber
 Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
ASTHMA TREATMENT AND THE HPA AXIS
 ASTHMA TREATMENT AND THE HPA AXIS Paul A. Greenberger, M.D. 7/12/2010 10:30-10:50 10:50 Objectives To review HPA axis suppression and its clinical significance in adults and children To describe methods
ASTHMA TREATMENT AND THE HPA AXIS Paul A. Greenberger, M.D. 7/12/2010 10:30-10:50 10:50 Objectives To review HPA axis suppression and its clinical significance in adults and children To describe methods
Long-term prognosis of BK virus-associated nephropathy in kidney transplant recipients
 Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
THE KIDNEY AND SLE LUPUS NEPHRITIS
 THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
Is the plasma ACTH concentration a reliable parameter in the insulin tolerance test?
 European Journal of Endocrinology (2003) 149 535 541 ISSN 0804-4643 CLINICAL STUDY Is the plasma ACTH concentration a reliable parameter in the insulin tolerance test? K Borm, M Slawik, L Seiler, F Flohr,
European Journal of Endocrinology (2003) 149 535 541 ISSN 0804-4643 CLINICAL STUDY Is the plasma ACTH concentration a reliable parameter in the insulin tolerance test? K Borm, M Slawik, L Seiler, F Flohr,
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
Intruduction PSI MODE OF ACTION AND PHARMACOKINETICS
 Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Subclinical Problems in the ICU:
 Subclinical Problems in the ICU: Corticosteroid Insufficiency C. S. Cutillar, M.D., FPCP, FPSEM Associate Professor Cebu Institute of Medicine H-P-A Axis during Critical Illness CRH ACTH H-P-A Axis during
Subclinical Problems in the ICU: Corticosteroid Insufficiency C. S. Cutillar, M.D., FPCP, FPSEM Associate Professor Cebu Institute of Medicine H-P-A Axis during Critical Illness CRH ACTH H-P-A Axis during
Solid Organ Transplantation 1. Chapter 55. Solid Organ Transplant, Self-Assessment Questions
 Solid Organ Transplantation 1 Chapter 55. Solid Organ Transplant, Self-Assessment Questions Questions 1 to 9 are related to the following case: A 38-year-old white man is scheduled to receive a living-unrelated
Solid Organ Transplantation 1 Chapter 55. Solid Organ Transplant, Self-Assessment Questions Questions 1 to 9 are related to the following case: A 38-year-old white man is scheduled to receive a living-unrelated
The endocrine system is complex and sometimes poorly understood.
 1 CE Credit Testing the Endocrine System for Adrenal Disorders and Diabetes Mellitus: It Is All About Signaling Hormones! David Liss, BA, RVT, VTS (ECC) Platt College Alhambra, California For more information,
1 CE Credit Testing the Endocrine System for Adrenal Disorders and Diabetes Mellitus: It Is All About Signaling Hormones! David Liss, BA, RVT, VTS (ECC) Platt College Alhambra, California For more information,
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Endocrine part one. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
ULTIMATE BEAUTY OF BIOCHEMISTRY. Dr. Veena Bhaskar S Gowda Dept of Biochemistry 30 th Nov 2017
 ULTIMATE BEAUTY OF BIOCHEMISTRY Dr. Veena Bhaskar S Gowda Dept of Biochemistry 30 th Nov 2017 SUSPECTED CASE OF CUSHING S SYNDROME Clinical features Moon face Obesity Hypertension Hunch back Abdominal
ULTIMATE BEAUTY OF BIOCHEMISTRY Dr. Veena Bhaskar S Gowda Dept of Biochemistry 30 th Nov 2017 SUSPECTED CASE OF CUSHING S SYNDROME Clinical features Moon face Obesity Hypertension Hunch back Abdominal
Management of Post-transplant hyperlipidemia
 Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Management of Post-transplant hyperlipidemia B. Gisella Carranza Leon, MD Assistant Professor of Medicine Lipid Clinic - Vanderbilt Heart and Vascular Institute Division of Diabetes, Endocrinology and
Audit of Adrenal Function Tests. Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK
 Audit of Adrenal Function Tests Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK Introduction Audit Overview of adrenal function tests Education Audit why? Explore
Audit of Adrenal Function Tests Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK Introduction Audit Overview of adrenal function tests Education Audit why? Explore
Joslin Diabetes Center Joslin Diabetes Forum 2013: The Impact of Comorbidities on Glucose Control Scenario 2: Reduced Renal Function
 Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use
 Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Αναγκαιότητα και τρόπος ρύθμισης του διαβήτη στους νοσηλευόμενους ασθενείς
 Αναγκαιότητα και τρόπος ρύθμισης του διαβήτη στους νοσηλευόμενους ασθενείς Αναστασία Θανοπούλου Επίκουρη Καθηγήτρια Β Παθολογικής Κλινικής Πανεπιστημίου Αθηνών Διαβητολογικό Κέντρο, Ιπποκράτειο Νοσοκομείο
Αναγκαιότητα και τρόπος ρύθμισης του διαβήτη στους νοσηλευόμενους ασθενείς Αναστασία Θανοπούλου Επίκουρη Καθηγήτρια Β Παθολογικής Κλινικής Πανεπιστημίου Αθηνών Διαβητολογικό Κέντρο, Ιπποκράτειο Νοσοκομείο
Adrenal insufficiency 25/09/57
 Adrenal insufficiency นายแพทย อ ดมศ กด เล ศส ทธ พร โรงพยาบาลมหาราชนครราชส มา 25/09/57 Adrenal insufficiency Cause Primary VS secondary Acute VS Chronic Diagnosis Critically ill VS non-critically ill Treatment
Adrenal insufficiency นายแพทย อ ดมศ กด เล ศส ทธ พร โรงพยาบาลมหาราชนครราชส มา 25/09/57 Adrenal insufficiency Cause Primary VS secondary Acute VS Chronic Diagnosis Critically ill VS non-critically ill Treatment
Kidney Allograft Stone after Kidney Transplantation and its Association with Graft Survival
 Original Article Kidney Allograft Stone after Kidney Transplantation and its Association with Graft Survival M. S. Rezaee-Zavareh 1,2, R. Ajudani 1, M. Ramezani Binabaj 1, F. Heydari 2, B. Einollahi 2
Original Article Kidney Allograft Stone after Kidney Transplantation and its Association with Graft Survival M. S. Rezaee-Zavareh 1,2, R. Ajudani 1, M. Ramezani Binabaj 1, F. Heydari 2, B. Einollahi 2
Plasma Cortisol Level during Hemodialysis with Kolff's Artificial Kidney
 Tohoku J. exp. Med., 1970, 100, 23-29 Plasma Cortisol Level during Hemodialysis with Kolff's Artificial Kidney Seigi Tsuchida and Hiroatsu Sugawara Department of Urology (Prof. S. Shishito), Tohoku University
Tohoku J. exp. Med., 1970, 100, 23-29 Plasma Cortisol Level during Hemodialysis with Kolff's Artificial Kidney Seigi Tsuchida and Hiroatsu Sugawara Department of Urology (Prof. S. Shishito), Tohoku University
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
The CARI Guidelines Caring for Australasians with Renal Impairment. Membranous nephropathy role of steroids GUIDELINES
 Membranous nephropathy role of steroids Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES There is currently no data to support the use of short-term courses of
Membranous nephropathy role of steroids Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES There is currently no data to support the use of short-term courses of
Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting glucose: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Is Knowing Half the Battle? Behavioral Responses to Risk Information from the National Health Screening Program in Korea
 Is Knowing Half the Battle? Behavioral Responses to Risk Information from the National Health Screening Program in Korea Hyuncheol Bryant Kim 1, Suejin A. Lee 1, and Wilfredo Lim 2 1 Cornell University
Is Knowing Half the Battle? Behavioral Responses to Risk Information from the National Health Screening Program in Korea Hyuncheol Bryant Kim 1, Suejin A. Lee 1, and Wilfredo Lim 2 1 Cornell University
Metabolic Syndrome. Shon Meek MD, PhD Mayo Clinic Florida Endocrinology
 Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
CARE PATHWAYS. Allyson Ashley
 CARE PATHWAYS Allyson Ashley WHAT IS A CARE PATHWAY? An explicit statement of the goals and key elements of care based on evidence, best practice, and patient s expectations and their characteristics The
CARE PATHWAYS Allyson Ashley WHAT IS A CARE PATHWAY? An explicit statement of the goals and key elements of care based on evidence, best practice, and patient s expectations and their characteristics The
Serum Cholesterol Changes in Long-Term Survivors of Liver Transplantation: A Comparison Between Cyclosporine and Tacrolimus Therapy
 Serum Cholesterol Changes in Long-Term Survivors of Liver Transplantation: A Comparison Between Cyclosporine and Tacrolimus Therapy Ramón Charco,* Carme Cantarell, Victor Vargas,* Luis Capdevila, Jose
Serum Cholesterol Changes in Long-Term Survivors of Liver Transplantation: A Comparison Between Cyclosporine and Tacrolimus Therapy Ramón Charco,* Carme Cantarell, Victor Vargas,* Luis Capdevila, Jose
Relationship between Post-kidney Transplantation Antithymocyte Globulin Therapy and Wound Healing Complications
 Original Article Relationship between Post-kidney Transplantation Antithymocyte Globulin Therapy and Wound Healing Complications G. R. Pourmand 1, S. Dehghani 1*, A. Saraji 1, S. Khaki 1,2, S. H. Mortazavi
Original Article Relationship between Post-kidney Transplantation Antithymocyte Globulin Therapy and Wound Healing Complications G. R. Pourmand 1, S. Dehghani 1*, A. Saraji 1, S. Khaki 1,2, S. H. Mortazavi
New York State Medicaid Prescriber Education Program
 New York State Medicaid Prescriber Education Program Metformin as a first-line medication Treating type 2 diabetes mellitus Key messages 1) Metformin should be used as a first-line medication in almost
New York State Medicaid Prescriber Education Program Metformin as a first-line medication Treating type 2 diabetes mellitus Key messages 1) Metformin should be used as a first-line medication in almost
Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, ; doi: /kisup.2012.
 http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
Objectives. Pathophysiology of Steroids. Question 1. Pathophysiology 3/1/2010. Steroids in Septic Shock: An Update
 Objectives : An Update Michael W. Perry PharmD, BCPS PGY2 Critical Care Resident Palmetto Health Richland Hospital Review the history of steroids in sepsis Summarize the current guidelines for steroids
Objectives : An Update Michael W. Perry PharmD, BCPS PGY2 Critical Care Resident Palmetto Health Richland Hospital Review the history of steroids in sepsis Summarize the current guidelines for steroids
Adrenal Insufficiency in Patients with Liver Cirrhosis and Severe Sepsis: Effect on Survival after Treatment with Hydrocortisone ABSTRACT
 20 Original Article Adrenal Insufficiency in Patients with Liver Cirrhosis and Severe Sepsis: Effect on Survival after Treatment with Hydrocortisone Pattanasirigool C Prasongsuksan C Settasin S Letrochawalit
20 Original Article Adrenal Insufficiency in Patients with Liver Cirrhosis and Severe Sepsis: Effect on Survival after Treatment with Hydrocortisone Pattanasirigool C Prasongsuksan C Settasin S Letrochawalit
Post Transplant Immunosuppression: Consideration for Primary Care. Sameh Abul-Ezz, M.D., Dr.P.H.
 Post Transplant Immunosuppression: Consideration for Primary Care Sameh Abul-Ezz, M.D., Dr.P.H. Objectives Discuss the commonly used immunosuppressive medications and what you need to know to care for
Post Transplant Immunosuppression: Consideration for Primary Care Sameh Abul-Ezz, M.D., Dr.P.H. Objectives Discuss the commonly used immunosuppressive medications and what you need to know to care for
Ron Shapiro, MD, Abdul S. Rao, MD, D. Phil., Paulo Fontes, MD, Adrianna Zeevi, Ph.D., Mark Jordan, MD, Velma P. Scantlebury, MD,
 Kidney IBone Marrow Transplantation Ron Shapiro, MD, Abdul S. Rao, MD, D. Phil., Paulo Fontes, MD, Adrianna Zeevi, Ph.D., Mark Jordan, MD, Velma P. Scantlebury, MD, Carlos Vivas, MD, H. Albin Gritsch,
Kidney IBone Marrow Transplantation Ron Shapiro, MD, Abdul S. Rao, MD, D. Phil., Paulo Fontes, MD, Adrianna Zeevi, Ph.D., Mark Jordan, MD, Velma P. Scantlebury, MD, Carlos Vivas, MD, H. Albin Gritsch,
Additional file 2: Details of cohort studies and randomised trials
 Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
C h a p t e r 3 8 Cushing s Syndrome : Current Concepts in Diagnosis and Management
 C h a p t e r 3 8 Cushing s Syndrome : Current Concepts in Diagnosis and Management Padma S Menon Professor of Endocrinology, Seth G S Medical College & KEM Hospital, Mumbai A clinical syndrome resulting
C h a p t e r 3 8 Cushing s Syndrome : Current Concepts in Diagnosis and Management Padma S Menon Professor of Endocrinology, Seth G S Medical College & KEM Hospital, Mumbai A clinical syndrome resulting
Prediction of adrenocortical insufficiency after pituitary adenoma surgery using postoperative basal cortisol levels
 Prediction of adrenocortical insufficiency after pituitary adenoma surgery using postoperative basal cortisol levels Václav Hána jr. 1, Jana Ježková 1, Mikuláš Kosák 1, Michal Kršek 1, Josef Marek 1, David
Prediction of adrenocortical insufficiency after pituitary adenoma surgery using postoperative basal cortisol levels Václav Hána jr. 1, Jana Ježková 1, Mikuláš Kosák 1, Michal Kršek 1, Josef Marek 1, David
The role of glycated hemoglobin in the screening and diagnosis of renal posttransplantation diabetes
 Federal University of Rio Grande do Sul Graduate Program in Endocrinology Brazil The role of glycated hemoglobin in the screening and diagnosis of renal posttransplantation diabetes Ana Laura Pimentel
Federal University of Rio Grande do Sul Graduate Program in Endocrinology Brazil The role of glycated hemoglobin in the screening and diagnosis of renal posttransplantation diabetes Ana Laura Pimentel
Case Report Beneficial Effect of Conversion to Belatacept in Kidney-Transplant Patients with a Low Glomerular-Filtration Rate
 Case Reports in Transplantation, Article ID 190516, 4 pages http://dx.doi.org/10.1155/2014/190516 Case Report Beneficial Effect of Conversion to Belatacept in Kidney-Transplant Patients with a Low Glomerular-Filtration
Case Reports in Transplantation, Article ID 190516, 4 pages http://dx.doi.org/10.1155/2014/190516 Case Report Beneficial Effect of Conversion to Belatacept in Kidney-Transplant Patients with a Low Glomerular-Filtration
ASSESSMENT OF THE PAEDIATRIC NEEDS IMMUNOLOGY DISCLAIMER
 European Medicines Agency Evaluation of Medicines for Human Use London, September 2006 Doc. Ref.: EMEA/381922/2006 ASSESSMENT OF THE PAEDIATRIC NEEDS IMMUNOLOGY DISCLAIMER The Paediatric Working Party
European Medicines Agency Evaluation of Medicines for Human Use London, September 2006 Doc. Ref.: EMEA/381922/2006 ASSESSMENT OF THE PAEDIATRIC NEEDS IMMUNOLOGY DISCLAIMER The Paediatric Working Party
Drug Class Monograph
 Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
Steroid Minimization: Great Idea or Silly Move?
 Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Diltiazem use in tacrolimus-treated renal transplant recipients Kothari J, Nash M, Zaltzman J, Prasad G V R
 Diltiazem use in tacrolimus-treated renal transplant recipients Kothari J, Nash M, Zaltzman J, Prasad G V R Record Status This is a critical abstract of an economic evaluation that meets the criteria for
Diltiazem use in tacrolimus-treated renal transplant recipients Kothari J, Nash M, Zaltzman J, Prasad G V R Record Status This is a critical abstract of an economic evaluation that meets the criteria for
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care
 Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Assessing Adrenal Function in Ill, Hospitalized Patients. Bruce Redmon, MD Division of Endocrinology, Diabetes and Metabolism
 Assessing Adrenal Function in Ill, Hospitalized Patients Bruce Redmon, MD Division of Endocrinology, Diabetes and Metabolism Disclosures Very surprised when I received an email two weeks ago disclosing
Assessing Adrenal Function in Ill, Hospitalized Patients Bruce Redmon, MD Division of Endocrinology, Diabetes and Metabolism Disclosures Very surprised when I received an email two weeks ago disclosing
The endocrine system is made up of a complex group of glands that secrete hormones.
 1 10. Endocrinology I MEDCHEM 535 Diagnostic Medicinal Chemistry Endocrinology The endocrine system is made up of a complex group of glands that secrete hormones. These hormones control reproduction, metabolism,
1 10. Endocrinology I MEDCHEM 535 Diagnostic Medicinal Chemistry Endocrinology The endocrine system is made up of a complex group of glands that secrete hormones. These hormones control reproduction, metabolism,
9.3 Stress Response and Blood Sugar
 9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
Downloaded from ismj.bpums.ac.ir at 20: on Friday March 22nd 2019
 - ( ) - -. :. ( ) :.. :... :. : // : -// : Email :Kazem_an@modares.ac.ir /..().(). ) (HLA.(). ( ) ( ). ) () ( ) ( () () () ( ). ().().().().().() (). / / / /..().. / / : (LDL). SPSS) SPSS STATA. (Inc,
- ( ) - -. :. ( ) :.. :... :. : // : -// : Email :Kazem_an@modares.ac.ir /..().(). ) (HLA.(). ( ) ( ). ) () ( ) ( () () () ( ). ().().().().().() (). / / / /..().. / / : (LDL). SPSS) SPSS STATA. (Inc,
Dexamethasone suppression test predicts later development of an impaired adrenal function after a 14-day course of prednisone in healthy volunteers
 European Journal of Endocrinology (21) 162 943 949 ISSN 84-4643 CLINICAL STUDY Dexamethasone suppression test predicts later development of an impaired adrenal function after a 14-day course of prednisone
European Journal of Endocrinology (21) 162 943 949 ISSN 84-4643 CLINICAL STUDY Dexamethasone suppression test predicts later development of an impaired adrenal function after a 14-day course of prednisone
Five years of living donor kidney transplantation at University clinical center Tuzla, Bosnia and Herzegovina, from 1999 through 2004
 Clinical Science Five years of living donor kidney transplantation at University clinical center Tuzla, Bosnia and Herzegovina, from 1999 through 2004 Senaid Trnačević 1, Goran Imamović 2, Mustafa Bazardžanović
Clinical Science Five years of living donor kidney transplantation at University clinical center Tuzla, Bosnia and Herzegovina, from 1999 through 2004 Senaid Trnačević 1, Goran Imamović 2, Mustafa Bazardžanović
Targeted Adverse Event (ADV)
 North American Pediatric Renal Trials Collaborative Studies Production Release 14.0 [$sitecode] User: Adverse Event: Adverse Event Date: Targeted Adverse Event (ADV) Web Version: 1.0; 2.0; 06-20-13 1.
North American Pediatric Renal Trials Collaborative Studies Production Release 14.0 [$sitecode] User: Adverse Event: Adverse Event Date: Targeted Adverse Event (ADV) Web Version: 1.0; 2.0; 06-20-13 1.
European Risk Management Plan. Measures impairment. Retreatment after Discontinuation
 European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
The role of physical activity in the prevention and management of hypertension and obesity
 The 1 st World Congress on Controversies in Obesity, Diabetes and Hypertension (CODHy) Berlin, October 26-29 2005 The role of physical activity in the prevention and management of hypertension and obesity
The 1 st World Congress on Controversies in Obesity, Diabetes and Hypertension (CODHy) Berlin, October 26-29 2005 The role of physical activity in the prevention and management of hypertension and obesity
Nephrology Dialysis Transplantation
 Nephrol Dial Transplant (1999) 14: 394 399 Original Article Nephrology Dialysis Transplantation Reduced kidney transplant rejection rate and pharmacoeconomic advantage of mycophenolate mofetil Rudolf P.
Nephrol Dial Transplant (1999) 14: 394 399 Original Article Nephrology Dialysis Transplantation Reduced kidney transplant rejection rate and pharmacoeconomic advantage of mycophenolate mofetil Rudolf P.
Welcome and Introduction
 Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Patient Education. Transplant Services. Benefits and. Of a kidney/pancreas transplant
 Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES
 RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
Controversies in Renal Transplantation. The Controversial Questions. Patrick M. Klem, PharmD, BCPS University of Colorado Hospital
 Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
62-year-old woman with severe headache. Celeste Thomas November 1, 2012
 62-year-old woman with severe headache Celeste Thomas November 1, 2012 History of Present Illness History of hypertension and hyperlipidemia Presented to outside hospital after awakening from sleep with
62-year-old woman with severe headache Celeste Thomas November 1, 2012 History of Present Illness History of hypertension and hyperlipidemia Presented to outside hospital after awakening from sleep with
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation
 Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Acthar Gel. H. P. Acthar Gel (corticotropin; ACTH) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 6 Last Review Date: December 8, 2017 Acthar Gel Description H. P.
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 6 Last Review Date: December 8, 2017 Acthar Gel Description H. P.
Validation of diagnostic utility of fasting plasma glucose and HbA1c in stable renal transplant recipients one year after transplantation
 Ussif et al. BMC Nephrology (2019) 20:12 https://doi.org/10.1186/s12882-018-1171-3 RESEARCH ARTICLE Open Access Validation of diagnostic utility of fasting plasma glucose and HbA1c in stable renal transplant
Ussif et al. BMC Nephrology (2019) 20:12 https://doi.org/10.1186/s12882-018-1171-3 RESEARCH ARTICLE Open Access Validation of diagnostic utility of fasting plasma glucose and HbA1c in stable renal transplant
Chronic Kidney Disease (CKD) Stages. CHRONIC KIDNEY DISEASE Treatment Options. Incident counts & adjusted rates, by primary diagnosis Figure 2.
 Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Chapter 1: CKD in the General Population
 Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
