Focal Segmental Glomerulosclerosis (FSGS)
|
|
|
- Douglas Parsons
- 6 years ago
- Views:
Transcription
1 Nov 20th, 2:15-3:15 pm. ASFA Regional Meeting, Seattle, 2015 Focal Segmental Glomerulosclerosis (FSGS) David M. Ward, MD, FRCP, HP(ASCP) Professor of Medicine, Division of Nephrology, University of California San Diego. From the Therapeutic Apheresis Program, U. C. San Diego Medical Center, San Diego, California 92103
2 DISCLOSURES: The speaker has the following potential conflicts TerumoBCT, Inc. Honoraria, Consulting Therakos, Inc. Honoraria Alexion Pharmaceuticals Advisory Board Aethlon Medical Inc. Consulting Institutional support in the form of unrestricted educational grants from TerumoBCT, Alexion, Fresenius-Kabi (formerly Fenwal), Therakos.
3 Therapeutic Plasmapheresis Aminco Celltrifuge, Glasgow, circa 1973 IBM 2997 centrifuge, UCSD, 1982 Membrane plasmafiltration, UCSD, 1984
4 UC San Diego Therapeutic Apheresis Program Plasma exchange (TPE/PLEX) RBC exchange (RBCX-A) WBC / platelet depletion Research IBM 2997 Membrane TPE (mtpe/mplex) started 1983
5 UC San Diego Therapeutic Apheresis Program Plasma exchange (TPE/PLEX) ongoing started 2008 RBC exchange (RBCX-A) WBC / platelet depletion 0 0 started 2014 Research IBM 2997 Cobe Spectra Terumo Optia Stem cell harvest (HPC-A) Membrane TPE (mtpe/mplex) started 1989 started 2012 Photopheresis (ECP) LDL-apheresis (LDL-A) started 2003 Therakos XTS started 2011 Therakos CellEx started 2012 Kaneka Liposorber
6 UC San Diego Therapeutic Apheresis Program Number of procedures per year by modality Plasmapheresis (TPE) - outpatient Plasmapheresis (TPE) - inpatient* Stem cell harvest (HPC-A) Photopheresis (ECP) Cytapheresis (WBC, Plt., RBCX) LDL-apheresis (since March 2012) Research (Academic years run from July 1 st to June 30th)
7 SAVE THE DATE March 3-5, y day conference. Co-directors: David M. Ward MD Amber P. Sanchez MD Isagani I. Marquez, Jr, BSN RN cme.ucsd.edu/apheresis APC Apheresis Physicians College at UCSD 5-day immersion in the Apheresis Unit, with mentorship by experts. Round on 70+ procedures; one-on-one discussions; lectures and workshops. Limited to 3-4 participants. Offered 4 times per year. Contact
8 APC Apheresis Physicians College at UCSD 5-day immersion in the Apheresis Unit, with mentorship by experts. Round on 70+ procedures; one-on-one discussions; lectures and workshops. Limited to 3-4 participants. Offered 4 times per year. Contact Faculty: David M. Ward, MD Amber P. Sanchez, MD Nadine Benador, MD Isagani I. Marquez, Jr., RN, BSN ( Jhun ) (Instructor is David except where shown otherwise) 8:30-9:30 9:45-11:15 11:15-12:15 Monday 14 th Tuesday 15 th Wednesday 16 th Thursday 17 th Friday 18 th Badges (Teri), Introductions & Orientation. Pre-test Patient rounds TPE, ECP Classroom Apheresis methods. Dosing and prescribing TPE. Classroom Photopheresis (ECP); Case discussions Patient rounds TPE, ECP, LDL Classroom Diseases treated by TPE. Machine design Classroom Medical Director duties & qualifications. Program management and QA. Patient rounds TPE, ECP, LDL Round on 2 inpatients with anti-nmda-r encephalitis. Discussion of Acute CNS indications & management Classroom Pediatric apheresis (Nadine) Patient rounds TPE, ECP, LDL, RBCX Classroom Non-standard referrals. Insurance authorization. Classroom Case discussion session. Remaining issues. Patient rounds (Amber) - TPE, ECP, RBCX Classroom Post-test & discussion. Award of certificates. 12:15 Lunch break Lunch break Lunch break Lunch break Weekly Apheresis Patient Care Meeting 1:00-2:00 2:00-3:30 3:45-4:45 Classroom Anticoagulation, WBC-depletion, RBC-exchange. Patient rounds TPE, ECP Classroom Case analysis. Case discussion Classroom Adverse events (Amber) Patient rounds (Amber) TPE, ECP Machine hands-on and Q&A (Jhun) Classroom LDL-apheresis (Amber) Patient rounds TPE, ECP, RBCX RBCX-apheresis hands-on demonstration (Jhun) Classroom Case analysis. Case discussion session Patient rounds TPE, ECP, citrate ECP Classroom Stem cell harvest for BMT and research 1:00: Lunch break. 1:30: Doc Talk weekly case review with faculty and fellows. 2:30: Patient rounds TPE, ECP, citrate ECP Wrap-up discussion. Adjourn.
9 FSGS (Focal Segmental Glomerulosclerosis) OUTLINE: 1. Seminal cases. 2. Glomerular anatomy and pathology. 3. FSGS is a group of diseases with different etiologies. 4. The molecular machinery that regulates podocyte morphology. 5. Candidate glomerular permeability factors that may cause the recurrent type of FSGS. 6. Indications for TPE treatment for FSGS. 7. Use of Immunoadsorption, DFPP, etc. 8. Use of dextran-sulfate plasma adsorption (LDLapheresis).
10 FSGS (Focal Segmental Glomerulosclerosis) Case reports (3) published 1972: Hoyer JR, et al. Lancet. ii: , 1972
11 FSGS (Focal Segmental Glomerulosclerosis) Case report published 2012: 27 year old man, ESRD due to primary FSGS. Kidney transplant from sister. Day 2: recurrence of nephrotic syndrome (heavy proteinuria). Day 6: Biopsy - recurrence of FSGS (podocyte foot-process fusion). Rapid loss of renal function, severe depletion of serum albumin. Day 14: Kidney removed and re-transplanted into a 66 year old man with ESRD (diabetic nephropathy). Immediate graft function with rapid reduction of proteinuria. Biopsies at day 8 & day 25 after re-transplantation - glomerular lesions returning to normal. Gallon L, et al. Resolution of recurrent focal segmental glomerulosclerosis after retransplantation. N Engl J Med 366: , 2012.
12 Kidney Nephron Glomerulus Efferent arteriole Afferent arteriole Tubule
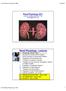
13 Normal Glomeruli FSGS Focal = some glomeruli not affected Segmental = some parts not affected
14 FSGS (Focal Segmental Glomerulosclerosis) Plasma exchange (TPE) for recurrent FSGS: Post-transplant recurrence of FSGS known for >40 years (1). Recurs post-transplant in ~ 23% of adults with primary FSGS (3). Recurrence rates higher in children. Recurrence rates higher if previous transplant loss to recurrence. Successful treatment of recurrence by TPE is well established (4-11). Opinion is in favor of TPE pre-transplant for severe cases. (1) Hoyer, JR, et al. Lancet. ii: , reprinted with commentary in (2) Hoyer, JR et al: Am Soc Nephrol 12: , 2001 (3) Meyrier A: Nephrol Dial Transplant 19: , 2004 (4) Valdivia P, et al. Transplant Proc 37: , 2005 (5) Schachter ME, et al: Clin Nephrol 74: , 2010 (6) Ponticelli C, Glassock RJ: Clin J Am Soc Nephrol 5: , 2010 (7) Zimmerman SW: Nephron 40: , 1985 (8) Gungor O, et al. Transplant Proc 43: , 2011 (9) Tsagalis G, et al. Artif Organs 35: , 2011 (10) Moroni G, et al. Transpl Int 23: , 2010 (11) Gonzalez E, et al. Pediatr Transplant 15: , 2011
15 FSGS (Focal Segmental Glomerulosclerosis) Clinical features: Proteinuria, microscopic hematuria, hypertension. Nephrotic syndrome in 30 50%. Progressive renal failure: 70% reach end stage in 10 years. Treatment: 20-40% of nephrotic cases may be helped by corticosteroids. Data also support use of cyclosporine, mycophenolate, cyclophosphamide, etc. Use ACE-inhibitors or ARB s (non-specific treatment for heavy proteinuria and/or progressive glomerular impairment).
16 FSGS (Focal Segmental Glomerulosclerosis) FSGS is a group of diseases: Actually FSGS is a pattern of response to injury that has multiple etiologies. How to distinguish the recurrent type before transplant is done? Estimates of post-transplant recurrence rates vary because of this denominator problem. Conflicting classifications of the different types of FSGS. Recent strides in defining different types based on pathogenesis. Attempts at standardization of classification beginning to gain acceptance.
17 Etiology/ mechanism FSGS is a group of diseases Primary FSGS Secondary FSGS Familial FSGS Collapsing form of FSGS FSGS due to scarring from other GN Circulating factors toxic to podocyte integrity. Adaptive injury (hyperfiltration damage). Genetic defects of podocyte and slitpore proteins. Toxins & viruses (HIV, parvo B19, pamidronate, etc.) Non-specific scarring after inflammatory type of glomerulonephritis. These 4 have in common: Primary damage to the podocyte foot-processes of the visceral epithelial cells of the glomerulus. When podocyte injury progresses to podocyte cell death, there is consequent sclerosis of the glomerular capillary tuft.
18 Normal Glomerulus - Diagram Parietal epithelium Bowman s capsule Bowman s space (urinary space) Proximal tubule epithelium Visceral epithelial (podocyte) cell body Glomerular basement membrane (GBM) Capillary lumen Endothelial cell body Mesangium Efferent arteriole Mesangial cell body Afferent arteriole David M Ward, 2014
19 Normal Glomerulus Parietal epithelium Bowman s capsule Bowman s space (urinary space) Visceral epithelial (podocyte) cell body Glomerular basement membrane (GBM) Capillary lumen Endothelial cell body Mesangium Mesangial cell body david m ward, 2003
20 Normal Glomerulus Parietal epithelium Bowman s capsule Bowman s space (urinary space) Visceral epithelial (podocyte) cell body Glomerular basement membrane (GBM) Capillary lumen Endothelial cell body Mesangium Mesangial cell body david m ward, 2003
21 Electron Microscopy - Normal Glomerular Capillary Loop
22 Micrograph The McGraw-Hill Companies Inc, 2011 Scanning Electron Microscopy Glomerular Capillary Loop Outside = epithelium ( podocyte ) Inside = endothelium Podocyte foot-processes Capillary lumen Endothelial fenestrae
23 Scanning Electron Microscopy Podocyte Foot Processes
24 Micrograph The McGraw-Hill Companies Inc, 2011 Scanning Electron Microscopy Glomerular Capillary Loop Outside = epithelium ( podocyte ) Inside = endothelium Podocyte foot-processes Capillary lumen Endothelial fenestrae
25 Normal Glomerular Capillary Loop tall short tall short tall short light dark light dark dark light Capillary lumen Part of Epithelial Cell (Podocyte) Mesangial Matrix Mesangial Cell David M Ward, 2012 Glomerular Basement Membrane
26 Normal Glomerular Capillary Loop Part of Epithelial Cell (Podocyte) Capillary lumen Mesangial Matrix Mesangial Cell David M Ward, 2012 Glomerular Basement Membrane
27 Normal Glomerular Capillary Loop Podocyte Foot Processes Slit diaphragms span between podocyte foot processes Outside = Epithelium (Podocytes) Formation of glomerular filtrate Mesangial Matrix Mesangial Cell David M Ward, 2012 Glomerular Basement Membrane
28 Podocyte Foot Process Architecture Slit diaphragms span between podocyte foot processes Illustration from Sever S et al, J Clin Invest 117:2095, 2007
29 Podocyte Foot Process Architecture Slit diaphragms span between podocyte foot processes Illustrations from Sever S et al, J Clin Invest 117:2095, 2007 and Ronco P, (editorial) J CIin Invest 117:2081, 2007
30 Podocyte Foot Process Architecture Healthy: Illustrations from Sever S et al, J Clin Invest 117:2095, 2007 and Ronco P, (editorial) J CIin Invest 117:2081, 2007
31 Podocyte Foot Process Architecture Healthy: Collapsed / effaced : Illustrations from Sever S et al, J Clin Invest 117:2095, 2007 and Ronco P, (editorial) J CIin Invest 117:2081, 2007
32 FSGS is a group of diseases Etiology/ mechanism Histological hallmarks Distinguishing clinical features Primary FSGS Circulating factors toxic to podocyte integrity. Effacement of podocyte foot processes is diffuse (universal). Nephrotic syndrome. Recurrence after kidney transplantation. Secondary FSGS Adaptive injury (hyperfiltration damage). Foot process effacement is focal and segmental. Glom & tubular hypertrophy. Sub-nephrotic, rarely major hypoalbuminemia. Exacerbated by APOL1 gene variants. Familial FSGS Genetic defects of podocyte and slitpore proteins. Variable depending on affected gene. Various patterns; some systemic syndromes. Collapsing form of FSGS Toxins & viruses (HIV, parvo B19, pamidronate, etc.) Segmental collapse of glom basement membranes, with occlusion of capillaries. Poor response to treatment. Increased rate of progression to end-stage renal failure. FSGS due to scarring from other GN Non-specific scarring after inflammatory type of glomerulonephritis. Segmental or global sclerosis where glomerular tuft disrupted. Where not, features of underlying GN. Features variable, depending on the primary process.
33 FSGS (Focal Segmental Glomerulosclerosis) Increasing incidence; greater if African genetic background. Prominent cause of ESRD. (1) The incidence is increasing. (1) Most common cause of non-diabetic nephrotic syndrome in USA. Global incidence estimated at 8 cases per million per year. (2) Lifetime risk in USA is: ~0.2% for European Americans ~0.7% for African Americans. (3) (1) Kitiyakara C, Eggers P, Kopp JB: Am J Kidney Dis 44: , 2004 (2) McGrogan A, Franssen CF, de Vries CS: Nephro Dial Transplant 26: , 2011 (3) Kitiyakara C, Kopp JB, Eggers P: Semin Nephrol 23: , 2003
34 FSGS (Focal Segmental Glomerulosclerosis) FSGS is more common in African Americans. African-American ancestry confers high risk for FSGS and hypertension-attributed ESRD (end-stage renal disease); (also of HIV-nephropathy and diabetes-associated ESRD). Early hypotheses included speculation regarding a one-time selection event for salt-conserving genes. Then genome-wide analysis (GWAS) showed association with a locus on chromosome 22, in or near the gene for MYH9 (myosin heavy chain 9). (1) However, causal mutations in MYH9 could not be found. (2) Linkage disequilibrium with a nearby site was suspected; mutations in the APOL1 gene were found. (3) (1) Kao WH et al., Nat Genet 40:1185, 2008; Kopp JB et al. Nat Genet 40:1175, 2008 (2) Freedman BI et al., Kidney Int 75:736, 2009 (3) Genovese G, et al. Science 329: , 2010
35
36 FSGS (Focal Segmental Glomerulosclerosis) FSGS is more common in African Americans. Good gene, bad gene. The same gene variants that promote destruction of the kidney s filtration units (above) also combat Trypanosoma brucei rhodesiense parasites. Leslie M. Science 329:263, 2010 (Editorial)
37 FSGS (Focal Segmental Glomerulosclerosis) FSGS is more common in African Americans. In African-Americans, FSGS and hypertension-attributed ESRD are associated with two independent sequence variants in the APOL1 gene on chromosome 22. FSGS odds ratio = 10.5 (95% confidence interval ); H-ESRD odds ratio = 7.3 (95% confidence interval ). The two APOL1 variants are common in West African chromosomes but absent in chromosomes of other origin. Both reside within haplotypes that harbor signatures of positive selection. ApoL1 (apolipoprotein L-1) is a serum factor that lyses trypanosomes. In vitro assays revealed that only the kidney disease-associated ApoL1 variants lysed Trypanosoma brucei rhodesiense. Genovese G, Friedman DJ, Ross MD, Lecordier L, Uzureau P, Freedman BI, Bowden DW, Langefield CD, Oleksyk TK, Knob AU, Bernhardy AJ, Hicks PK, Nelson GW, Vanhollebecke, B, Winkler CA, Kopp JB, Pays E, Pollak MR. Association of trypanolytic ApoL1 variants with kidney disease in African Americans. Science 329: , 2010
38 FSGS is a group of diseases Etiology/ mechanism Histological hallmarks Distinguishing clinical features Primary FSGS Circulating factors toxic to podocyte integrity. Effacement of podocyte foot processes is diffuse (universal). Nephrotic syndrome. Recurrence after kidney transplantation. Secondary FSGS Adaptive injury (hyperfiltration damage). Foot process effacement is focal and segmental. Glom & tubular hypertrophy. Sub-nephrotic, rarely major hypoalbuminemia. Exacerbated by APOL1 gene variants. Familial FSGS Genetic defects of podocyte and slitpore proteins. Variable depending on affected gene. Various patterns; some systemic syndromes. Collapsing form of FSGS Toxins & viruses (HIV, parvo B19, pamidronate, etc.) Segmental collapse of glom basement membranes, with occlusion of capillaries. Poor response to treatment. Increased rate of progression to end-stage renal failure. FSGS due to scarring from other GN Non-specific scarring after inflammatory type of glomerulonephritis. Segmental or global sclerosis where glomerular tuft disrupted. Where not, features of underlying GN. Features variable, depending on the primary process.
39 Hereditary Podocytopathies Genetic abnormalities of podocyte proteins cause FSGS-type lesions DISEASE Finnish type NPHS2 mutation Familial FSGS 1 Familial FSGS 2 Gene/Protein Nephrin Podocin α actinin 4 TRP C6 Tryggvason K, Patrakka J, Wartiovaara J. Mechanisms of Disease: Hereditary Proteinuria Syndromes and Mechanisms of Proteinuria N Engl J Med 354: , 2006 Illustration from Ronco P, (editorial) J CIin Invest 117:2081, 2007
40 Other genetic pathways in production of glomerular sclerosis Mitochondrial gene abnormalities can cause podocyte damage. Primary coenzyme Q10 deficiency secondary to genetic defects in the COQ2 gene COQ2 nephropathy. (1) Multiple others. (2) (1) Diomedi-Camassei F, et al. COQ2 nephropathy: a newly described inherited mitochondriopathy with primary renal involvement. J Am Soc Nephrol. 18:2773, 2007 (2) Rahman S, Hall AM. Mitochondrial disease an important cause of end stage renal failure. Pediatric Nephrol 28: , 2013
41 Hereditary podocytopathies DISEASE LOCUS GENE PROTEIN CLINICAL Congenital nephrotic syndrome (Finnish type) Steroid-resistant nephrotic syndrome 19q13.1 NPHS1 Nephrin AR, in utero 1q25-32 NPHS2 Podocin AR, young adult Pierson s type nephrosis Laminin beta 2 AR, post birth Nail-Patella syndrome LMX1B AD, children Denys-Drash syndrome WT1 AD, ESRD by 3 Familial FSGS type 1 19q13 ACTN4 alpha Actinin 4 AD, adolescents Familial FSGS type 2 TRP C6 AD, adolescents Tryggvason K, Patrakka J, Wartiovaara J. Mechanisms of Disease: Hereditary Proteinuria Syndromes and Mechanisms of Proteinuria N Engl J Med 2006; 354:
42 FSGS is a group of diseases Etiology/ mechanism Histological hallmarks Distinguishing clinical features Primary FSGS Circulating factors toxic to podocyte integrity. Effacement of podocyte foot processes is diffuse (universal). Nephrotic syndrome. Recurrence after kidney transplantation. Secondary FSGS Adaptive injury (hyperfiltration damage). Foot process effacement is focal and segmental. Glom & tubular hypertrophy. Sub-nephrotic, rarely major hypoalbuminemia. Exacerbated by APOL1 gene variants. Familial FSGS Genetic defects of podocyte and slitpore proteins. Variable depending on affected gene. Various patterns; some systemic syndromes. Collapsing form of FSGS Toxins & viruses (HIV, parvo B19, pamidronate, etc.) Segmental collapse of glom basement membranes, with occlusion of capillaries. Poor response to treatment. Increased rate of progression to end-stage renal failure. FSGS due to scarring from other GN Non-specific scarring after inflammatory type of glomerulonephritis. Segmental or global sclerosis where glomerular tuft disrupted. Where not, features of underlying GN. Features variable, depending on the primary process.
43 FSGS is a group of diseases Primary FSGS Secondary FSGS Familial FSGS Collapsing form of FSGS FSGS due to scarring from other GN Etiology/ mechanism Circulating factors toxic to podocyte integrity. Adaptive injury (hyperfiltration damage). Genetic defects of podocyte and slitpore proteins. Toxins & viruses (HIV, parvo B19, pamidronate, etc.) Non-specific scarring after inflammatory type of glomerulonephritis. Predict recurrence in transplant response to TPE Predict no recurrence in transplant no response to TPE
44 FSGS (Focal Segmental Glomerulosclerosis) Predicting post-transplant recurrence: genetic markers Study patients: 83 children with primary FSGS who received at least one renal allograft. (mean age 6.7 years at diagnosis; 13 years at first transplantation). 53 of these were analyzed for NPHS2 mutations (gene for Podocin). Results: FSGS recurred in 30 patients (36%) (median 13 days; range 1.5 to 152 days). 23 patients received a second kidney transplant, and FSGS recurred in 11 (48%) (median 16 days; range 2.7 to 66 days). Recurrence of FSGS: 0% (0 of 11) in patients with homozygous or compound heterozygous NPHS2 mutations versus 45% in patients without mutations. Conclusion: Genetic testing for pathogenic mutations may be important for prognosis and treatment of FSGS both before and after transplantation. Jungraithmayr TC et al. Screening for NPHS2 mutations may help predict FSGS recurrence after transplantation. J Am Soc Nephrol 22: , 2011.
45 Foot Process Effacement (FPE) by glomerular permeability factors At what anatomic sites could glomerular permeability factors act to cause reversible damage to the podocyte cytoskeleton? Illustration from editorial by Ronco P, J CIin Invest 117:2081, 2007
46 Foot Process Effacement (FPE): role of Dynamin and Cathepsin L Critical elements in maintaining podocyte foot-process integrity Dynamin Cathepsin L Actin Illustration from editorial by Ronco P, J CIin Invest 117:2081, 2007
47 Foot Process Effacement (FPE): role of Dynamin and Cathepsin L Evidence from a murine model Dynamin maintains FP structure Dynamin by regulating Actin. Critical elements in Cathepsin L (Cat L) induces proteinuria by switching off maintaining podocyte Cathepsin L the active, GTP-bound form of Dynamin. Is increased in foot-process integrity Hu proteinuric diseases. Is increased Actin in a murine model. Cat L-deficient mice resist foot process effacement (FPE) Gene delivery into normal mice: of a mutant Dynamin (that does not bind GTP) g induces FPE and proteinuria. of the Cat L-cleaved product of Dynamin g induces FPE and proteinuria. Gene delivery into proteinuric mice: of 2 different Cat L-resistant Dynamin mutants g reverses proteinuria and FPE. Sever S, et al. Proteolytic processing of dynamin by cytoplasmic cathepsin L is a mechanism for proteinuric kidney disease. J Clin Invest 117: , 2007
48 Foot Process Effacement (FPE): role of Dynamin and Cathepsin L Evidence from a murine model Sever S, et al. Proteolytic processing of dynamin by cytoplasmic cathepsin L is a mechanism for proteinuric kidney disease. J Clin Invest 117: , 2007
49 Further Recent Insights into the Machinery of Podocyte Integrity Puromycin Aminonucleoside Nephropathy (PAN) is a standard model of podocytopathy in animals. Neph1 protein has an intracellular domain (Neph1CD) that is involved in podocyte response to injury. Transduction of TAT-Neph1CD, which inhibits phosphorylation of Neph1 by PAN, was shown to protect cultured human podocytes from PAN-induced damage. Hayek SS et al. Slit diaphragm protein Neph1 and its signaling: a novel therapeutic target for protection of podocytes against glomerular injury. J Biol Chem 289: , 2014
50 Further Recent Insights into the Machinery of Podocyte Integrity Control: Neph1 on cell membranes with intact actin cytoskeleton PAN induces Neph1 loss from cell membranes and disrupts actin cytoskeleton Transduced TAT-Neph1 on cell membranes with intact actin cytoskeleton Transduced TAT-Neph1 resists PAN-induced damage to Neph1 & actin cytoskeleton Hayek SS, et al. Slit diaphragm protein Neph1 and its signaling: a novel therapeutic target for protection of podocytes against glomerular injury. J Biol Chem 289: , 2014
51 Further Recent Insights into the Machinery of Podocyte Integrity Control of actin cytoskeleton: Neph1 Synaptospondin Nephrin signalling endosome Cathepsin L / Dynamin interaction etc. Collapse of actin cytoskeleton Illustration from Sever S et al, J Clin Invest 117:2095, 2007
52 Effect of Glomerular Permeability Factors on foot-process morphology Plasma from cases of recurrent FSGS has a similar effect Effect of permeability factor(s) Proteinuria in experimental animals given FSGS plasma.(1) Shrinking of cultured glomeruli in vitro if FSGS plasma added.(2) This Glomerular Volume Variation (GVV) test has been standardized as a semi-quantitative research assay of permeability factor activity.(3) (1) Savin VJ, McCarthy ET, Sharma M. Semin Nephrol 23:147-60, 2003 (2) Savin VJ, et al. N Engl J Med 334: , 1996 (3) Godfrin Y, et al. Kidney Int 50: , 1996
53 Glomerular Permeability Factors in Recurrent FSGS Candidate molecules: Small, highly glycosylated, hydrophobic protein(s)/peptide(s) 30 to 50 kda, poorly characterized. (1) Permeability activity is decreased by plasmapheresis. (2) Normal plasma contains substances that block or inactivate the FSGS permeability factor. In vitro, blocking by cyclosporine, indomethacin, etc. Proteinuric effect inhibited by galactose. (3) Clinical benefit in FSGS patients given oral galactose (4, 5) now disproven. (1) (2) (3) (4) (5) Savin VJ, et al. Circulating factor associated with increased glomerular permeability to albumin in recurrent focal segmental glomerulosclerosis. N Engl J Med 334: , 1996 Savin VJ, McCarthy ET, Sharma M. Permeability factors in focal segmental glomerulosclerosis. Semin Nephrol 23:147-60, 2003 Savin V, et al. Transl Res 151: , 2008 De Smet E, et al. Nephrol Dial Transplant 24: , 2009 Kopac M, et al. Ther Apher Dial 15: , 2011
54 Glomerular Permeability Candidate - CLC1 Candidate molecule: CLC1 (Cardiotrophin-like cytokine 1) CLC1 is a member of the interleukin-6 family (approx. 220 AA, 24kDa). Decreases nephrin expression in cultured podocytes. CLC1 inhibitors reverse the permeability effect of plasma from FSGS patients. Data are preliminary. McCarthy ET, Sharma M, Savin VJ. Circulating permeability factors in idiopathic nephrotic syndrome and focal segmental glomerulosclerosis. Clin J Am Soc Nephrol 5: , 2010
55 Glomerular Permeability Candidate - supar Candidate molecule: supar (= soluble urokinase-type Plasminogen Activator Receptor) In 2011, research implicated supar, the soluble form of the urokinase receptor present on podocytes: supar levels (22 to 45 kda fragments) are elevated in 70% of patients with FSGS, but not in other glomerular diseases. In animal models, supar causes podocyte injury by activation of β3 integrin. In kidney biopsies, β3 integrin is found on podocytes in patients with FSGS (but not other diseases). Wei C, et al. Circulating urokinase receptor as a cause of focal segmental glomerulosclerosis. Nat Med 17: , 2011
56 Glomerular Permeability Candidate - supar supar removal by plasmapheresis in recurrent FSGS (posttransplant) Initial studies of plasmapheresis (TPE): clinical remission if supar levels <2,000 pg/ml. serum no longer induces podocyte β3 integrin. In 2 patients: TPE failed to reduce supar levels <2,000 pg/ml. did not achieve clinical remission. serum still strongly activated β3 integrin. Wei C, et al. Circulating urokinase receptor as a cause of focal segmental glomerulosclerosis. Nat Med 17: , 2011
57 Glomerular Permeability Candidate - supar Further evidence of pathogengic role of supar Study patients: Two cohorts with biopsy-proven primary FSGS: 70 patients from the North America based FSGS clinical trial (CT). 94 patients from European PodoNet study of steroid-resistant nephrotic syndrome. Results: Elevated supar in 84.3% (CT) and 55.3% (PodoNet), versus 6% of controls (P=0.0001); inflammation did not account for this difference. Reduction of supar correlates with treatment and with reduction of proteinuria, with higher odds for complete remission (P=0.04). Conclusions: supar levels elevated in geographically and ethnically diverse patients with FSGS. Reductions in supar levels correlate with different therapeutic regimens and with remission; this supports the role of supar in pathogenesis. Unexpected finding: In the PodoNet cohort, patients with an NPHS2 mutation had higher supar levels than those without a mutation. (NPHS2 codes for Podocin.) Wei C et al. Circulating supar in two cohorts of primary FSGS. J Am Soc Nephrol 23: , 2012
58 Glomerular Permeability Candidate - supar Contradictatory evidence for a pathogenic role of supar in FSGS Bock ME et al. Serum soluble urokinase-type receptor levels do not distinguish focal segmental glomerulosclerosis from other causes of nephrotic syndrome in children. Clin J Am Soc Nephrol 8: , Franco-Palacios CR, et al. Urine but not serum soluble urokinase receptor(supar) may identify cases of recurrent FSGS in kidney transplant candidates. Transplantation 96: , 2013 Meijers B et al. The soluble urokinase receptor is not a clinical marker for focal segmental glomerulosclerosis. Kidney Int 85: , 2014 Wada T, et al. A multicenter cross-sectional analysis study of circulating soluble urokinase receptor in Japanese patients with glomerular disease. Kidney Int 85: , 2014 Cathelin D, et al. Administration of recombinant soluble urokinase receptor per se is not sufficient to induce podocyte alterations and proteinuria in mice. JASN 25: , 2014 Harita Y, et al. Decreased glomerular filtration as the primary factor of elevated circulating supar levels in FSGS. Pediatr Nephrol 29: , 2014
59 Glomerular Permeability Candidate - supar 241 patients from the NEPTUNE observational study After adjusting for baseline supar concentration, age, gender, proteinuria, and time, the change in supar from baseline was associated with egfr, but this association was not different for patients with FSGS as compared with other diagnoses. Thus these results do not support a pathological role for supar in FSGS. Spinale JM et al. A reassessment of soluble urokinase-type plasminogen activator receptor in glomerular disease. Kidney Int 87: , 2015
60 Glomerular Permeability Candidate - supar Data from 3683 patients Hayek SS et al. Soluble Urokinase Receptor and Chronic Kidney Disease. NEJM 373: , 2015
61 Other candidate systems for intervention in FSGS Corticotrophin and Melanocortin receptors ACTH (corticotrophin) is cleaved to α-msh (melanocyte stimulating hormone) which binds to the receptor MC1R on the podocyte. (1) Thus ACTH gel (Acthar) may work by stimulating corticosteroids or directly by the above mechanism (1) Bomback AS, et al. Treatment of resistant glomerular diseases with adrenocorticotropic hormone gel: a prospective trial. Am J Nephrol 36:58-67, 2012
62 Other candidate systems for intervention in FSGS Angiotensin System receptors Angiotensin II regulates and enhances the expression of transient receptor potential cation channel 6 (TRPC6) on podocytes. (1) Antibodies to angiotensin (AT1) receptors on podocytes can cause proteinuria. (2) Therefore ACE-inhibitors and ARBs perhaps not just non-specific treatments for nephrotic diseases. (1) Nijenhuis T, et al. Angiotensin II contributes to podocyte injury by increasing TRPC6 expression via an NFAT-mediated positive feedback signaling pathway. Am J Pathol 179: , (2) Alachkar N, Gupta G, Montgomery RA. Angiotensin antibodies and focal glomerulosclerosis. N Eng J Med 368: , 2013
63 Indications for plasmapheresis for FSGS TPE for post-transplant recurrence of FSGS TPE for peri-transplant prophylaxis of FSGS TPE for primary FSGS in native kidneys
64 Indications for plasmapheresis for FSGS TPE for post-transplant recurrence (slide 1 of 2): TPE is established first-line therapy (plus immunosuppression with mycophenolate, cyclophosphamide or rituximab). ASFA (2013) recommends initial regimen of TPE daily for 3 days, then at least 3 times per week for the next 2 weeks. Thereafter, TPE can be continued 2-3/week until remission occurs, as judged by serial quantitation of urine protein and serum creatinine, which can take weeks to months. (1, 2) One series performed 17 TPE treatments in each of 7 adults, all of whom had functioning grafts 10 months later. (3) Other series claim remission rates up to 80%in adults (4), and 88% in children. (5) (1) Schwartz J, Winters JL, Padmanabhan A, et al. J Clin Apher 28: , 2013 (2) Sanchez AP and Ward DM, Semin Dialysis 25: , 2012 (3) Valdivia P, et al. Transplant Proc 37: , 2005 (4) Moroni G, et al. Transpl Int 23: , 2010 (5) Gonzalez E, et al. Pediatr Transplant 15: , 2011
65 Indications for plasmapheresis for FSGS TPE for post-transplant recurrence (slide 2 of 2): One large retrospective series concluded that: Modern post-transplant immunosuppressive drug regimens do not reduce the recurrence rate of FSGS in adults. However, TPE achieved remission in 75% of cases. (1) Patients receiving treatment for recurrent FSGS or preemptively (for high-risk profile): Of the different treatment approaches, TPE combined with rituximab (anti-cd20) was most associated with prolonged remission of proteinuria. (2) (1) Schachter ME, et al. Recurrent focal segmental glomerulosclerosis in the renal allograft: single center experience in the era of modern immunosuppression. Clin Nephrol 74: , 2010 (2) Hickson LTH, et al. Kidney transplantation for primary focal segmental glomerulosclerosis: outcomes and response to therapy for recurrence. Transplantation 87: , 2009
66 Indications for plasmapheresis for FSGS TPE for peri-transplant prophylaxis: 10 patients at high risk because of rapid progression (4) or prior recurrence in a transplant (6) received 8 TPE treatments in the peri-operative period. 3 had recurrence within 3 months (all had prior graft loss to recurrence); 2 developed ESRD, 3 rd with significant renal dysfunction. 7 (including 3 with prior graft loss to recurrence) were free of recurrence at follow-up ( days), mean creatinine 1.53 mg/dl. (1) More recently, in 34 pediatric transplant cases, prophylactic TPE posttransplant appeared not to confer any outcome benefit compared with treatment of actual recurrence. (2) (1) Gohh RY, et al. Preemptive plasmapheresis and recurrence of FSGS in highrisk renal transplant recipients. Am J Transplantation 5: , 2005 (2) Gonzalez E, et al. Preemptive plasmapheresis and recurrence of focal segmental glomerulosclerosis in pediatric renal transplantation. Pediatr Transplant 15: , 2011
67 Indications for plasmapheresis for FSGS TPE for primary FSGS (in native kidneys): TPE (averaging 17 treatments) plus corticosteroids and cyclophosphamide achieved sustained remissions in 8 of 11 previously unresponsive adults. (1) TPE (six treatments) without consistent immunosuppressive drugs reduced proteinuria in only 2 of 8 patients. (2) Expert opinion based on very limited experience (3): Consider TPE for Severe disease manifestations despite an adequate trial of initial immunosuppressive therapy, in which very high levels of circulating permeability factor have been demonstrated. Continued massive proteinuria and hypoalbuminemia despite exposure to an adequate course of prednisone, cyclosporine, and mycophenolate. (1) Mitwalli AH. Adding plasmapheresis to corticosteroids and alkylating agents: does it benefit patients with focal segmental glomerulosclerosis? Nephrol Dial Transplant 13: , 1998 (2) Feld SM, et al. Plasmapheresis in the treatment of steroid resistant focal segmental glomerulosclerosis in native kidneys. Am J Kidney Dis 32: , 1998 (3) Appel GB and Cattran DC. Treatment of primary FSGS. In UpToDate online.
68 Type of plasmapheresis for FSGS Conventional plasma exchange (plasma removal and replacement): Established first-line treatment for recurrent FSGS (1-9) Removes macromolecules of all sizes: IgG (140 kda) supar (22 to 45 kda) Ill-defined permeability factors (30 to 50 kda) CLC1 (24 kda), etc., etc. (1) Zimmerman SW: Nephron 40: , 1985 (2) Valdivia P, et al. Transplant Proc 37: , 2005 (3) Schachter ME, et al: Clin Nephrol 74: , 2010 (4) Ponticelli C, Glassock RJ: Clin J Am Soc Nephrol 5: , 2010 (5) Moroni G, et al. Transpl Int 23: , 2010 (6) Gungor O, et al. Transplant Proc 43: , 2011 (7) Tsagalis G, et al. Artif Organs 35: , 2011 (8) Gonzalez E, et al. Pediatr Transplant 15: , 2011 (9) Wei C, et al. Nature Medicine 17: , 2011
69 (a) blood return Albumin fraction (b) blood return blood return Purified plasma Purified plasma Globulin fraction #1 #2 #1 #2 from patient Effluent from patient from patient Whole plasma Whole plasma Whole plasma Fig. 3. Circuit diagrams of (a) primary membrane plasma separation plus secondary plasma fractionation, and (b) primary centrifugal plasma separation plus secondary plasma perfusion column. In the left panel (a), the primary separation of plasma from blood (#1) is in a hollow-fiber membrane plasma filter with a pore size of 0.3 microns and a molecular weight cut-off in excess of 1,000 kda. The secondary processing of plasma (#2) is in a hollow-fiber membrane plasma fractionator with a pore size of microns and a molecular weight cut-off of approximately 100 kda. Albumin (67 kda) passes through the secondary membrane and can be used as replacement fluid for the patient. Immunoglobulins, including IgG (146 kda), stay within the hollow-fiber lumen which drains to the effluent bag, thus removing most of the autoantibody present in the plasma. Membrane specifications are those of Asahi products (Asahi Kasei Kuraray Medical Co., Tokyo 101-8,101, Japan). In the right panel (b), the primary separation of plasma from blood (#1) is by a continuous-flow centrifuge, and the secondary processing of plasma (#2) is in a perfusion column that can contain an immuno-adsorbent or chemical adsorbent (see text). The pathogenic molecule binds to the column, which is replaced when exhausted. Other systems employ pairs of columns that can be regenerated by washing out the bound pathogenic molecule; one column is in active use while the other is being washed clean, and they switch periodically during the procedure. Either type of primary separation (#1) can in principal be coupled to any type of secondary plasma purification (#2). Many secondary devices in use in Europe and Japan, and some primary/secondary combination systems, are not FDA- Approved in the USA. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] Ward DM, Conventional apheresis therapies: a review. J Clin Apheresis, 26: , 2011
70 Immunoadsorption (IA) plasmapheresis: Protein A columns Type of plasmapheresis for FSGS Reported as effective for recurrent FSGS (1) Removes IgG, but probably not small proteins like supar, etc. Anti-IgG columns Reported as effective for recurrent FSGS (2, 3) Removes IgG, but probably not small proteins like supar, etc. (1) Dantal J, Bigot E, Bogers W, et al. Effect of plasma protein adsorption on protein excretion in kidney-transplant recipients with recurrent nephrotic syndrome. N Engl J Med 330:7 14, 1994 (2) Haas M, et al. Plasma immunadsorption treatment in patients with primary focal and segmental glomerulosclerosis. Nephrol Dial Transplant 13: , 1998 (3) Dantal J, Godfrin Y, Koll R, et al: Antihuman immunoglobulin affinity immunoadsorption strongly decreases proteinuria in patients with relapsing nephrotic syndrome. J Am Soc Nephrol 9: , 1998
71 Type of plasmapheresis for FSGS Double-filtration (cascade) plasmapheresis: Returns albumin (67 kda) and all smaller molecules to the patient. blood return Albumin fraction #1: Plasma-filter Pore size: large Cut-off: >1000 kd Membrane specifications are those of Asahi products (Asahi Kasei Kuraray Medical Co., Tokyo 101-8,101, Japan) Diagram from Ward DM, J Clin Apheresis 26: , 2011 from patient #1 Whole plasma #2 Globulin fraction Effluent #2: Plasma-fractionator Pore size: medium Cut-off: ~ 100 kd IgM ~ 970 kda IgG ~ 140 kda Albumin ~ 67 kda supar ~22-45 kda
72 Type of plasmapheresis for FSGS Tryptophan adsorption column: Effective for steroid resistant FSGS. (1) (1) Beige J, et al. Immunoadsorption with tryptophan adsorbers for successful treatment of late steroid-refractory focal glomerulosclerosis. Am J Transplant 3:1459, 2003
73 Type of plasmapheresis for FSGS Update on immunoglobulin-binding IA columns: IgG-binding columns are specifically designed to extract only immunoglobulins. Example Globaffin columns use peptide ligand PGAM146 (Fresenius, Germany). (1) However, there is evidence from one case report that Immunoadsorption (IA) using Globaffin reduced supar also. The authors speculate that supar may bind to immunoglobulin molecules. (2) (1) Sanchez AP, Cunard R, Ward DM. The selective therapeutic apheresis procedures. J Clin Apheresis 28: 20-29, 2013 (2) Morath C, et al. Management of severe recurrent focal segmental glomerulosclerosis through circulating soluble urokinase receptor modification. Am J Therapeutics 20: , 2013
74 Plasma exchange vs. Immunadsorption (anti-igg column) TPE IA IA IA TPE IA IA IA TPE = conventional plasmapheresis replacing with FFP and 5% albumin (1 to 1.5 x PV). IA = immunoadsorption plasmapheresis with Globaffin columns (2 to 2.5 x PV) Morath C, et al. Am J Therapeutics 20: , 2013
75 Plasma exchange vs. Immunadsorption (anti-igg column) TPE IA IA IA TPE IA IA IA * * Podocyte AP5 activity = bioassay for podocyte β3 integrin activation by AP5 staining quantitated by mean fluorescence intensity (MFI) Morath C, et al. Am J Therapeutics 20: , 2013
76 Dextran Sulfate Adsorption (LDL-Apheresis) for FSGS Use of LDL-apheresis (dextran sulfate columns): FDA approval for pediatric FSGS in October Humanitarian Use Device application for Kaneka Liposorber. Pediatric FSGS indication: children with nephrotic syndrome, proteinuria >3.5g/day, hypoalbuminemia, hyperlipidemia, and progressive renal decline.
77 LDL removal from separated plasma 1. Adsorption Liposorber (Dextran sulfate adsorption) * TheraSorb LDL (Anti-ApoB immunoadsorption) 2. Precipitation H.E.L.P. (Heparin-induced precipitation) * 3. Filtration LDL Apheresis - systems available worldwide Double Filtration Plasmapheresis (DFPP) Direct LDL adsorption from whole blood Liposorber D (Dextran sulfate adsorption) * = FDA-approved Direct Adsorption of Lipoprotein (DALI) (Polyacrylate adsorption) Sanchez AP, Cunard R, Ward DM. The selective therapeutic apheresis procedures. J Clin Apheresis 28:20-29, 2013
78 Dextran Sulfate Adsorption (LDL-Apheresis) Hattori et al. Am J Kidney Dis 42: , pediatric patients with biopsy proven FSGS, all steroid resistant after 8 weeks (and prior treatment with cyclosporin-a). LDL apheresis on Kaneka Liposorber 2x per week for 3 weeks, then 1x per week for 6 weeks. 7 of 11 had marked reduction in proteinuria or achieved remission. Appeared to improve response to steroids.
79 Role of Lipids in Glomerulosclerosis Stenvinkel P, et al. Eur J Clin Invest 30: , adults (age 34-62) with hypercholesterolemia due to nephrotic syndrome from diseases other than FSGS (4 Membranous GN, 2 MPGN and 1 IgA GN) Treated with LDL-apheresis using Kaneka dextran sulfate columns. All benefitted with regard to reduction of LDL and Lp(a). Serum albumin increased (p=0.01) and proteinuria tended to decrease (NS) during this time. Confounding factors include immunosuppressive drugs. Hyperlipidemia contributing to glomerular damage: Grone H, et al. Induction of glomerulosclerosis by dietary lipids. Lab Invest 60: , 1989 Keane WF, et al. Injurious effects of LDL on human mesangial cell. Kidney Int. 37:509, 1990 Diamond JR, Karnovsky MJ. A putative role of hypercholesterolemia in progressive glomerular injury. Annu Rev Med 43:83-92, 1992
80 The POLARIS Trial Dextran Sulfate Adsorption (LDL-Apheresis) (Prospective Observational Survey on the Long-Term Effects of LDL Apheresis on Drug-Resistant Nephrotic Syndrome) 64 courses in 58 patients with steroid +/- cyclosporine resistant nephrotic syndrome, ages (17 courses excluded for insufficient data). All treated on Kaneka Liposorber system (dextran sulfate adsorption). Average 9.6 LDL-A procedures per course. 3.5 L. (av.) plasma processed per procedure. 55% of courses were in patients with FSGS. Proteinuria fell similarly in FSGS cases (from to 3.26 g ) and in non- FSGS cases ( to ). Muso E, et al. Immediate therapeutic efficacy of LDL-apheresis for drug-resistant nephrotic syndrome: evidence from the short term results from the POLARIS study. Clin Exp Nephrol 19: , 2015
81 Type of plasmapheresis for FSGS Therapeutic results that illuminate pathogenesis: There is secure evidence that whole plasma removal (TPE) is of major clinical benefit in FSGS (post-transplant recurrent type). Rituximab, corticosteroids and other immunosuppressants can also be effective what is the role of the immune system? Are immunoadsorption (IAPP) or double-filtration (DFPP) truly effective? Do they have mechanisms of action other than removal of glomerular permeability factors? Research needs first to validate claims for their clinical effectiveness. Until there is clarification, conventional plasma exchange (TPE) has been recommended as the preferred apheresis modality (1). The efficacy of dextran-sulfate plasma adsorption (LDL-apheresis) needs to be confirmed, and its mode of action elucidated. (1) Sanchez AS and Ward DM. Therapeutic Apheresis for Renal Disorders. Seminars in Dialysis 25:19-131, 2012
82 SUMMARY: FSGS (Focal Segmental Glomerulosclerosis) 1. Recurrence of FSGS after kidney transplant: evidence for endogenous circulating permeability factors. 2. FSGS is a group of diseases. 3. West African genes promote FSGS-like glomerular lesions. 4. Genetic abnormalities of podocyte proteins compromise podocyte foot-process architecture and lead to FSGS-like lesions. 5. FSGS of the type that recurs post-transplant is less common than other types. 6. Circulating permeability factors can cause podocyte foot-process damage. 7. Candidate molecules: kda factors, CLC1, supar, others. 8. TPE for FSGS recurring post-transplant is established and effective treatment. 9. Use of TPE for native-kidney FSGS and peri-transplant prophylaxis is less clear. 10. Immunoadsorption, DFPP, etc. may not be equivalent to TPE. 11. Dextran-sulfate plasma adsorption (LDL-apheresis) appears effective.
83 Thank you for your attention PDF of these slides from or
Glomerular Pathology- 1 Nephrotic Syndrome. Dr. Nisreen Abu Shahin
 Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Columns and Combined Circuits
 Wednesday, March 7 th, 2018. 11:00 am 12:30 pm Workshop F06: Principles, Applications and Practical Issues of Plasma Exchange 11:45 am 12:00 Columns and Combined Circuits David M. Ward, MD, FRCP, HP(ASCP)
Wednesday, March 7 th, 2018. 11:00 am 12:30 pm Workshop F06: Principles, Applications and Practical Issues of Plasma Exchange 11:45 am 12:00 Columns and Combined Circuits David M. Ward, MD, FRCP, HP(ASCP)
Practical Issues in Plasmapheresis: Set-up and Troubleshooting, Combined CRRT and Apheresis
 Workshop G14 Wednesday, 10:15 11:45 a.m. Practical Issues in Plasmapheresis: Set-up and Troubleshooting, Combined CRRT and Apheresis 1. David M. Ward, MD, FRCP Use of Hybrid Apheresis/CRRT circuits 2.
Workshop G14 Wednesday, 10:15 11:45 a.m. Practical Issues in Plasmapheresis: Set-up and Troubleshooting, Combined CRRT and Apheresis 1. David M. Ward, MD, FRCP Use of Hybrid Apheresis/CRRT circuits 2.
Genetics of Steroid Resistant Nephrotic syndrome. Velibor Tasic University Children s Hospital Skopje, Macedonia
 Genetics of Steroid Resistant Nephrotic syndrome Velibor Tasic University Children s Hospital Skopje, Macedonia Nephrotic syndrome - definition Oedema Massive proteinuria (> 50mg/kg/d or> 40mg/m2/h Hypoalbuminemia
Genetics of Steroid Resistant Nephrotic syndrome Velibor Tasic University Children s Hospital Skopje, Macedonia Nephrotic syndrome - definition Oedema Massive proteinuria (> 50mg/kg/d or> 40mg/m2/h Hypoalbuminemia
Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS
 Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS Proteinuria is a major healthcare problem that affects several hundred million people worldwide. Proteinuria is a cardinal
Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS Proteinuria is a major healthcare problem that affects several hundred million people worldwide. Proteinuria is a cardinal
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
C1q nephropathy the Diverse Disease
 C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
The evolution of the classification of nephrotic syndrome Laura Barisoni, MD
 The evolution of the classification of nephrotic syndrome Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University Old classification schemes: Proteinuria and
The evolution of the classification of nephrotic syndrome Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University Old classification schemes: Proteinuria and
Beneficial effect of LDL-apheresis in refractory nephrotic syndrome
 Clin Exp Nephrol (2014) 18:286 290 DOI 10.1007/s10157-013-0930-5 REVIEW ARTICLE WCN 2013 Satellite Symposium Kidney and Lipids Beneficial effect of LDL-apheresis in refractory nephrotic syndrome Eri Muso
Clin Exp Nephrol (2014) 18:286 290 DOI 10.1007/s10157-013-0930-5 REVIEW ARTICLE WCN 2013 Satellite Symposium Kidney and Lipids Beneficial effect of LDL-apheresis in refractory nephrotic syndrome Eri Muso
3. PODOCYTE INJURY IN GLOMERULAR DISEASES
 How to Cite this article: Podocyte Injury in Glomerular Diseases - ejifcc 20/01 2009 http://www.ifcc.org 3. PODOCYTE INJURY IN GLOMERULAR DISEASES Mirjana Sabljar Matovinović Podocytes are injured in diabetic
How to Cite this article: Podocyte Injury in Glomerular Diseases - ejifcc 20/01 2009 http://www.ifcc.org 3. PODOCYTE INJURY IN GLOMERULAR DISEASES Mirjana Sabljar Matovinović Podocytes are injured in diabetic
CHAPTER 2. Primary Glomerulonephritis
 2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Familial DDD associated with a gain-of-function mutation in complement C3.
 Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s. Part 1: Clinical
 Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s Part 1: Clinical Pa#ent DM 18 year old McMaster student Back pain, severe fa#gue Oct 2006 Leg swelling to ER Nov
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s Part 1: Clinical Pa#ent DM 18 year old McMaster student Back pain, severe fa#gue Oct 2006 Leg swelling to ER Nov
Case # 2 3/27/2017. Disclosure of Relevant Financial Relationships. Clinical history. Clinical history. Laboratory findings
 Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Glomerular diseases mostly presenting with Nephritic syndrome
 Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Hasan Fattah 3/19/2013
 Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
RENAL EVENING SPECIALTY CONFERENCE
 RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
Chapter 6: Idiopathic focal segmental glomerulosclerosis in adults Kidney International Supplements (2012) 2, ; doi: /kisup.2012.
 http://www.kidney-international.org chapter 6 & 2012 KDIGO Chapter 6: Idiopathic focal segmental glomerulosclerosis in adults Kidney International Supplements (2012) 2, 181 185; doi:10.1038/kisup.2012.19
http://www.kidney-international.org chapter 6 & 2012 KDIGO Chapter 6: Idiopathic focal segmental glomerulosclerosis in adults Kidney International Supplements (2012) 2, 181 185; doi:10.1038/kisup.2012.19
The evolution of the classification of nephrotic syndrome and the new taxonomy for the podocytopathies Laura Barisoni, MD
 The evolution of the classification of nephrotic syndrome and the new taxonomy for the podocytopathies Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University
The evolution of the classification of nephrotic syndrome and the new taxonomy for the podocytopathies Laura Barisoni, MD Department of Pathology and Medicine, Division of Nephrology New York University
Genetic Testing of Children with Steroid Resistant Nephrotic Syndrome
 The 5 th Global Congress For Consensus in Pediatrics & Child Health Genetic Testing of Children with Steroid Resistant Nephrotic Syndrome Fang Wang Peking University First Hospital Nephrotic Syndrome (NS)
The 5 th Global Congress For Consensus in Pediatrics & Child Health Genetic Testing of Children with Steroid Resistant Nephrotic Syndrome Fang Wang Peking University First Hospital Nephrotic Syndrome (NS)
Nephritic vs. Nephrotic Syndrome
 Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Glomerular pathology-2 Nephritic syndrome. Dr. Nisreen Abu Shahin
 Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Lupus Related Kidney Diseases. Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017
 Lupus Related Kidney Diseases Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017 Financial Disclosures MedImmune Lupus Nephritis Kidney Biopsy Biomarkers
Lupus Related Kidney Diseases Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017 Financial Disclosures MedImmune Lupus Nephritis Kidney Biopsy Biomarkers
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s
 Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s The basic facts about proteinuria and FSGS A primer on proteinuria Endothelium and glycocalyx Podocytes Pathology
Focal Segmental Glomerulosclerosis and the Nephro6c Syndrome Dr. A. Gangji Dr. P. Marge>s The basic facts about proteinuria and FSGS A primer on proteinuria Endothelium and glycocalyx Podocytes Pathology
CHAPTER 2 PRIMARY GLOMERULONEPHRITIS
 CHAPTER 2 Sunita Bavanandan Lim Soo Kun 19 5th Report of the 2.1: Introduction This chapter covers the main primary glomerulonephritis that were reported to the MRRB from the years 2005-2012. Minimal change
CHAPTER 2 Sunita Bavanandan Lim Soo Kun 19 5th Report of the 2.1: Introduction This chapter covers the main primary glomerulonephritis that were reported to the MRRB from the years 2005-2012. Minimal change
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephrotic syndrome minimal change disease vs. IgA nephropathy. Hadar Meringer Internal medicine B Sheba
 Nephrotic syndrome minimal change disease vs. IgA nephropathy Hadar Meringer Internal medicine B Sheba The Case 29 year old man diagnosed with nephrotic syndrome 2 weeks ago and complaining now about Lt.flank
Nephrotic syndrome minimal change disease vs. IgA nephropathy Hadar Meringer Internal medicine B Sheba The Case 29 year old man diagnosed with nephrotic syndrome 2 weeks ago and complaining now about Lt.flank
Nephrotic Syndrome NS
 Nephrotic Syndrome NS By : Dr. Iman.M. Mudawi Pediatric Nephrology Unit Gaafar Ibn Auf Hospital Definitions: In children NS is applied to any condition with a triad of: Heavy proteinuria (UACR ratio >200
Nephrotic Syndrome NS By : Dr. Iman.M. Mudawi Pediatric Nephrology Unit Gaafar Ibn Auf Hospital Definitions: In children NS is applied to any condition with a triad of: Heavy proteinuria (UACR ratio >200
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Renal Pathology 1: Glomerulus. With many thanks to Elizabeth Angus PhD for EM photographs
 Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Anna Vinnikova, MD APOL1
 Anna Vinnikova, MD APOL1 I have no relevant financial relationships with commercial interests But I have a passionate interest in the following problem: National decline in Nephrology Fellowship applications
Anna Vinnikova, MD APOL1 I have no relevant financial relationships with commercial interests But I have a passionate interest in the following problem: National decline in Nephrology Fellowship applications
Renal Physiology - Lectures
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
THE KIDNEY AND SLE LUPUS NEPHRITIS
 THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
Case 3. ACCME/Disclosure. Laboratory results. Clinical history 4/13/2016
 Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
21 st Budapest Nephrology School
 Genetics of non-diabetic kidney disease 21 st Budapest Nephrology School Barry I. Freedman, MD, FACP John H. Felts III Professor (Internal Medicine) Chief, Section on Nephrology Podocyte disorders β3 integrin
Genetics of non-diabetic kidney disease 21 st Budapest Nephrology School Barry I. Freedman, MD, FACP John H. Felts III Professor (Internal Medicine) Chief, Section on Nephrology Podocyte disorders β3 integrin
RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT. J. H. Helderman,MD,FACP,FAST
 RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT J. H. Helderman,MD,FACP,FAST Vanderbilt University Medical Center Professor of Medicine, Pathology and Immunology Medical Director, Vanderbilt Transplant
RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT J. H. Helderman,MD,FACP,FAST Vanderbilt University Medical Center Professor of Medicine, Pathology and Immunology Medical Director, Vanderbilt Transplant
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Urinary CD80 as a Replacement for Renal Biopsy for Diagnosis of Pediatric Minimal Change Disease
 KIDNEY DISEASES Urinary CD80 as a Replacement for Renal Biopsy for Diagnosis of Pediatric Minimal Change Disease Heba Mostafa Ahmed, 1 Dina Ahmed Ezzat, 1 Noha A Doudar, 2 Mai Adel 1 1 Departement of Pediatrics,
KIDNEY DISEASES Urinary CD80 as a Replacement for Renal Biopsy for Diagnosis of Pediatric Minimal Change Disease Heba Mostafa Ahmed, 1 Dina Ahmed Ezzat, 1 Noha A Doudar, 2 Mai Adel 1 1 Departement of Pediatrics,
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Atypical IgA Nephropathy
 Atypical IgA Nephropathy Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA XXXIII Chilean Congress of Nephrology, Hypertension and Transplantation Puerto Varas, Chile October 6, 2016 IgA
Atypical IgA Nephropathy Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA XXXIII Chilean Congress of Nephrology, Hypertension and Transplantation Puerto Varas, Chile October 6, 2016 IgA
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Dr P Sigwadi Paediatric Nephrology
 Dr P Sigwadi Paediatric Nephrology Prevalence - 5-15 % on a single urine sample After a series of 4 tests only 0.1% of children had persistent positive proteinuria Persistent proteinuria indicates the
Dr P Sigwadi Paediatric Nephrology Prevalence - 5-15 % on a single urine sample After a series of 4 tests only 0.1% of children had persistent positive proteinuria Persistent proteinuria indicates the
Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab
 TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
Tuesday Conference 7/23/2013. Hasan Fattah
 Tuesday Conference 7/23/2013 Hasan Fattah 48 AA male, PMH: HTN, proteinuria since 2009, sent from primary clinic for high Cr evaluation (7.1), last known of 1.1 in 2010 associated with sub-nephrotic range
Tuesday Conference 7/23/2013 Hasan Fattah 48 AA male, PMH: HTN, proteinuria since 2009, sent from primary clinic for high Cr evaluation (7.1), last known of 1.1 in 2010 associated with sub-nephrotic range
Surgical Pathology Report
 Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Pathology of Complement Mediated Renal Disease
 Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis
 GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
Nephrology Grand Rounds. Mansi Mehta November 24, 2015
 Nephrology Grand Rounds Mansi Mehta November 24, 2015 Case 51yo F with PMH significant for Hypertension referred to renal clinic for evaluation of elevated Cr. no known history of CKD; baseline creatinine
Nephrology Grand Rounds Mansi Mehta November 24, 2015 Case 51yo F with PMH significant for Hypertension referred to renal clinic for evaluation of elevated Cr. no known history of CKD; baseline creatinine
Steroid Resistant Nephrotic Syndrome. Sanjeev Gulati, Debashish Sengupta, Raj K. Sharma, Ajay Sharma, Ramesh K. Gupta*, Uttam Singh** and Amit Gupta
 Steroid Resistant Nephrotic Syndrome Sanjeev Gulati, Debashish Sengupta, Raj K. Sharma, Ajay Sharma, Ramesh K. Gupta*, Uttam Singh** and Amit Gupta From the Departments of Nephrology, Pathology* and Biostatistics**,
Steroid Resistant Nephrotic Syndrome Sanjeev Gulati, Debashish Sengupta, Raj K. Sharma, Ajay Sharma, Ramesh K. Gupta*, Uttam Singh** and Amit Gupta From the Departments of Nephrology, Pathology* and Biostatistics**,
Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, ; doi: /kisup.2012.
 http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
STEROID-RESISTANT NEPHROTIC SYNDROME (SRNS)
 MARIO NEGRI INSTITUTE FOR PHARMACOLOGICAL RESEARCH CLINICAL RESEARCH CENTRE FOR RARE DISEASES ALDO E CELE DACCO' Villa Camozzi - 24020 Ranica (Bergamo) Italy Telephone 39-35-4535304 fax 39-35-4535373 STEROID-RESISTANT
MARIO NEGRI INSTITUTE FOR PHARMACOLOGICAL RESEARCH CLINICAL RESEARCH CENTRE FOR RARE DISEASES ALDO E CELE DACCO' Villa Camozzi - 24020 Ranica (Bergamo) Italy Telephone 39-35-4535304 fax 39-35-4535373 STEROID-RESISTANT
Membranous nephropathy. By Mohammed Kamal Nassar, MD Lecturer of Nephrology Mansoura University
 Membranous nephropathy By Mohammed Kamal Nassar, MD Lecturer of Nephrology Mansoura University Membranous nephropathy Definition: Immune complex glomerular disease in which immune deposits of IgG and complement
Membranous nephropathy By Mohammed Kamal Nassar, MD Lecturer of Nephrology Mansoura University Membranous nephropathy Definition: Immune complex glomerular disease in which immune deposits of IgG and complement
Proteinuria Nephrotic syndrome
 Proteinuria Nephrotic syndrome Pathophysiology & management Miriam Davidovits, MD Institute of Nephrology Schneider Children s Medical Center of Israel 1 Abnormal excretion of protein into the urine is
Proteinuria Nephrotic syndrome Pathophysiology & management Miriam Davidovits, MD Institute of Nephrology Schneider Children s Medical Center of Israel 1 Abnormal excretion of protein into the urine is
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Proteinuria Nephrotic syndrome
 Proteinuria Nephrotic syndrome Pathophysiology & management Miriam Davidovits, MD Institute of Nephrology Schneider Children s Medical Center of Israel 1 Abnormal excretion of protein into the urine is
Proteinuria Nephrotic syndrome Pathophysiology & management Miriam Davidovits, MD Institute of Nephrology Schneider Children s Medical Center of Israel 1 Abnormal excretion of protein into the urine is
The topic of normal vascular and glomerular anatomy is introduced
 Normal Vascular and Glomerular Anatomy Arthur H. Cohen Richard J. Glassock The topic of normal vascular and glomerular anatomy is introduced here to serve as a reference point for later illustrations of
Normal Vascular and Glomerular Anatomy Arthur H. Cohen Richard J. Glassock The topic of normal vascular and glomerular anatomy is introduced here to serve as a reference point for later illustrations of
Nephrotic syndrome in children. Bashir Admani KPA Nephrology Precongress 24/4/2018
 Nephrotic syndrome in children Bashir Admani KPA Nephrology Precongress 24/4/2018 What is Nephrotic syndrome?? Nephrotic syndrome is caused by renal diseases that increase the permeability across the glomerular
Nephrotic syndrome in children Bashir Admani KPA Nephrology Precongress 24/4/2018 What is Nephrotic syndrome?? Nephrotic syndrome is caused by renal diseases that increase the permeability across the glomerular
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Pathogenesis of IgA Nephropathy. Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS
 Pathogenesis of IgA Nephropathy Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS History Immunoglobin A nephropathy was first described by Berger and Hinglais in 1968 in Paris
Pathogenesis of IgA Nephropathy Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS History Immunoglobin A nephropathy was first described by Berger and Hinglais in 1968 in Paris
Paediatrics Dr. Bakr Lecture 3 Nephrotic Syndrome
 P a g e 1 DEFINITION Paediatrics Dr. Bakr Lecture 3 Nephrotic Syndrome Definition: nephrotic syndrome is a disorder characterized by heavy proteinuria with hypoprpteinimia,hyper lipidemia and edema. It
P a g e 1 DEFINITION Paediatrics Dr. Bakr Lecture 3 Nephrotic Syndrome Definition: nephrotic syndrome is a disorder characterized by heavy proteinuria with hypoprpteinimia,hyper lipidemia and edema. It
General introduction. General introduction
 General introduction 1 Chapter 1 Proteinuria is the excretion of proteins into the urine. Presence of abnormal proteinuria, the urinary excretion of abnormal amounts of serum proteins (briefly called proteinuria),
General introduction 1 Chapter 1 Proteinuria is the excretion of proteins into the urine. Presence of abnormal proteinuria, the urinary excretion of abnormal amounts of serum proteins (briefly called proteinuria),
Enterprise Interest Nothing to declare
 Enterprise Interest Nothing to declare Minimal change disease (MCD) related new electron microscopy findings in a patient on Levothyroxine sodium (LT) for hypothyroidism: A case report Dr. Ali Al-Omari
Enterprise Interest Nothing to declare Minimal change disease (MCD) related new electron microscopy findings in a patient on Levothyroxine sodium (LT) for hypothyroidism: A case report Dr. Ali Al-Omari
Renal Disease and PK/PD. Anjay Rastogi MD PhD Division of Nephrology
 Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS
 FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
Ανάπτυξη Βιοτράπεζας για την Ανίχνευση Πρώιμων Βιοδεικτών σε Ασθενείς με Χρόνια Νεφρική Νόσο
 Ανάπτυξη Βιοτράπεζας για την Ανίχνευση Πρώιμων Βιοδεικτών σε Ασθενείς με Χρόνια Νεφρική Νόσο ΔΗΜΗΤΡΙΟΣ Σ. ΓΟΥΜΕΝΟΣ Νεφρολογικό και Μεταμοσχευτικό Κέντρο Πανεπιστημιακό Νοσοκομείο Πατρών Causes of chronic
Ανάπτυξη Βιοτράπεζας για την Ανίχνευση Πρώιμων Βιοδεικτών σε Ασθενείς με Χρόνια Νεφρική Νόσο ΔΗΜΗΤΡΙΟΣ Σ. ΓΟΥΜΕΝΟΣ Νεφρολογικό και Μεταμοσχευτικό Κέντρο Πανεπιστημιακό Νοσοκομείο Πατρών Causes of chronic
Acthar Gel. H. P. Acthar Gel (corticotropin; ACTH) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 7 Last Review Date: November 30, 2018 Acthar Gel Description H.
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 7 Last Review Date: November 30, 2018 Acthar Gel Description H.
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
Blood Group Incompatible Renal Transplantation and Apheresis. Liz Wright Clinical Nurse Specialist Great Ormond Street Hospital NHS FT
 Blood Group Incompatible Renal Transplantation and Apheresis Liz Wright Clinical Nurse Specialist Great Ormond Street Hospital NHS FT Background There is growing interest in transplantation across the
Blood Group Incompatible Renal Transplantation and Apheresis Liz Wright Clinical Nurse Specialist Great Ormond Street Hospital NHS FT Background There is growing interest in transplantation across the
Diabetic Nephropathy
 Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
Glomerular tip adhesions predict the progression of IgA nephropathy
 Maeda et al. BMC Nephrology 2013, 14:272 RESEARCH ARTICLE Open Access Glomerular tip adhesions predict the progression of IgA nephropathy Kunihiro Maeda 1, Shogo Kikuchi 2, Naoto Miura 1, Keisuke Suzuki
Maeda et al. BMC Nephrology 2013, 14:272 RESEARCH ARTICLE Open Access Glomerular tip adhesions predict the progression of IgA nephropathy Kunihiro Maeda 1, Shogo Kikuchi 2, Naoto Miura 1, Keisuke Suzuki
C3 Glomerulopathy. Jun-Ki Park
 C3 Glomerulopathy Jun-Ki Park 03.08.11 For the last 30 years classification MPGN is based on glomerular findings by light microscopy with further specification on EM and staining for Ig and complement
C3 Glomerulopathy Jun-Ki Park 03.08.11 For the last 30 years classification MPGN is based on glomerular findings by light microscopy with further specification on EM and staining for Ig and complement
Use of mycophenolate mofetil in steroid-dependent and -resistant nephrotic syndrome
 Pediatr Nephrol (2003) 18:833 837 DOI 10.1007/s00467-003-1175-4 BRIEF REPORT Gina-Marie Barletta William E. Smoyer Timothy E. Bunchman Joseph T. Flynn David B. Kershaw Use of mycophenolate mofetil in steroid-dependent
Pediatr Nephrol (2003) 18:833 837 DOI 10.1007/s00467-003-1175-4 BRIEF REPORT Gina-Marie Barletta William E. Smoyer Timothy E. Bunchman Joseph T. Flynn David B. Kershaw Use of mycophenolate mofetil in steroid-dependent
ACCME/Disclosure. Case #1. Case History. Dr. Bracamonte has nothing to disclose
 Case #1 ACCME/Disclosure Dr. Erika Bracamonte Associate Professor of Pathology University of Arizona, College of Medicine Banner University Medical Center, Tucson Dr. Bracamonte has nothing to disclose
Case #1 ACCME/Disclosure Dr. Erika Bracamonte Associate Professor of Pathology University of Arizona, College of Medicine Banner University Medical Center, Tucson Dr. Bracamonte has nothing to disclose
H.Jalanko has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve.
 H.Jalanko has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. Management dilemmas in infants with congenital nephrotic syndrome (CNS) Hannu Jalanko
H.Jalanko has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. Management dilemmas in infants with congenital nephrotic syndrome (CNS) Hannu Jalanko
IgA Nephropathy - «Maladie de Berger»
 IgA Nephropathy - «Maladie de Berger» B. Vogt, Division de Néphrologie/Consultation d Hypertension CHUV, Lausanne 2011 Montreux CME SGN-SSN IgA Nephropathy 1. Introduction 2. Etiology and Pathogenesis
IgA Nephropathy - «Maladie de Berger» B. Vogt, Division de Néphrologie/Consultation d Hypertension CHUV, Lausanne 2011 Montreux CME SGN-SSN IgA Nephropathy 1. Introduction 2. Etiology and Pathogenesis
An unusual association between focal segmental sclerosis and lupus nephritis: a distinct concept from lupus podocytopathy?
 CEN Case Rep (2015) 4:70 75 DOI 10.1007/s13730-014-0142-1 CASE REPORT An unusual association between focal segmental sclerosis and lupus nephritis: a distinct concept from lupus podocytopathy? Hironari
CEN Case Rep (2015) 4:70 75 DOI 10.1007/s13730-014-0142-1 CASE REPORT An unusual association between focal segmental sclerosis and lupus nephritis: a distinct concept from lupus podocytopathy? Hironari
Idiopathic focal segmental glomerulosclerosis: a favourable prognosis in untreated patients?
 O R I G N A L A R T I C L E Idiopathic focal segmental glomerulosclerosis: a favourable prognosis in untreated patients? J.K.J. Deegens 1* K.J.M. Assmann 2, E.J. Steenbergen 2, L.B. Hilbrands 1, P.G.G.
O R I G N A L A R T I C L E Idiopathic focal segmental glomerulosclerosis: a favourable prognosis in untreated patients? J.K.J. Deegens 1* K.J.M. Assmann 2, E.J. Steenbergen 2, L.B. Hilbrands 1, P.G.G.
Glomerulonephritis. Dr Rodney Itaki Anatomical Pathology Discipline.
 Glomerulonephritis Dr Rodney Itaki Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Gross anatomy Ref: Goggle Images Microanatomy
Glomerulonephritis Dr Rodney Itaki Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Gross anatomy Ref: Goggle Images Microanatomy
Minimal change disease and idiopathic FSGS: manifestations of the same disease
 PERSPECTIVES OPINION Minimal change disease and idiopathic FSGS: manifestations of the same disease Rutger J. Maas 1, Jeroen K. Deegens 1, Bart Smeets 2, Marcus J. Moeller 3 and Jack F. Wetzels 1 Abstract
PERSPECTIVES OPINION Minimal change disease and idiopathic FSGS: manifestations of the same disease Rutger J. Maas 1, Jeroen K. Deegens 1, Bart Smeets 2, Marcus J. Moeller 3 and Jack F. Wetzels 1 Abstract
The soluble urokinase receptor is not a clinical marker for focal segmental glomerulosclerosis
 http://www.kidney-international.org & 214 International Society of Nephrology see commentary on page 499 The soluble urokinase receptor is not a clinical marker for focal segmental glomerulosclerosis Björn
http://www.kidney-international.org & 214 International Society of Nephrology see commentary on page 499 The soluble urokinase receptor is not a clinical marker for focal segmental glomerulosclerosis Björn
Types Pathophysiology Clinical manifestations D.Dx. Investigations. Treatment. Complications.
 Types Pathophysiology Clinical manifestations D.Dx. Investigations. Treatment. Complications. Nephrotic syndrome affects 1-3 per 100,000 children
Types Pathophysiology Clinical manifestations D.Dx. Investigations. Treatment. Complications. Nephrotic syndrome affects 1-3 per 100,000 children
Resistant Nephrotic Syndrome: Review of Trials Using ACTH and a Case Series of Six Patients Treated with ACTHar
 British Journal of Medicine & Medical Research 5(11): 1453-1457, 2015, Article no.bjmmr.2015.164 ISSN: 2231-0614 SCIENCEDOMAIN international www.sciencedomain.org Resistant Nephrotic Syndrome: Review of
British Journal of Medicine & Medical Research 5(11): 1453-1457, 2015, Article no.bjmmr.2015.164 ISSN: 2231-0614 SCIENCEDOMAIN international www.sciencedomain.org Resistant Nephrotic Syndrome: Review of
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Nephrotic Syndrome. Sara Alsharhan PharmD candidate, KSU 2014
 Nephrotic Syndrome Sara Alsharhan PharmD candidate, KSU 2014 Outline Introduction Nephrotic syndrome classifications Signs and symptoms Diagnoses Management Complications Monitoring Case presentation Introduction
Nephrotic Syndrome Sara Alsharhan PharmD candidate, KSU 2014 Outline Introduction Nephrotic syndrome classifications Signs and symptoms Diagnoses Management Complications Monitoring Case presentation Introduction
29th Annual Meeting of the Glomerular Disease Collaborative Network
 29th Annual Meeting of the Glomerular Disease Collaborative Network Updates on the Pathogenesis IgA Nephropathy and IgA Vasculitis (HSP) J. Charles Jennette, M.D. Brinkhous Distinguished Professor and
29th Annual Meeting of the Glomerular Disease Collaborative Network Updates on the Pathogenesis IgA Nephropathy and IgA Vasculitis (HSP) J. Charles Jennette, M.D. Brinkhous Distinguished Professor and
INTRODUCTION TO GLOMERULAR DISEASES
 INTRODUCTION TO GLOMERULAR DISEASES Goal: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
INTRODUCTION TO GLOMERULAR DISEASES Goal: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Evaluation and Management of Proteinuria. Negiin Pourafshar, MD University of Virginia Division of Nephrology
 Evaluation and Management of Proteinuria Negiin Pourafshar, MD University of Virginia Division of Nephrology Case A 30-year-old man, is turned down for life insurance because of the presence of an unspecified
Evaluation and Management of Proteinuria Negiin Pourafshar, MD University of Virginia Division of Nephrology Case A 30-year-old man, is turned down for life insurance because of the presence of an unspecified
Acthar Gel. H. P. Acthar Gel (corticotropin; ACTH) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 6 Last Review Date: December 8, 2017 Acthar Gel Description H. P.
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.10 Subject: Acthar Gel Page: 1 of 6 Last Review Date: December 8, 2017 Acthar Gel Description H. P.
The spectrum of primary nephrotic syndrome includes a
 In-Depth Review A Proposed Taxonomy for the Podocytopathies: A Reassessment of the Primary Nephrotic Diseases Laura Barisoni,* H. William Schnaper, and Jeffrey B. Kopp *Department of Pathology, New York
In-Depth Review A Proposed Taxonomy for the Podocytopathies: A Reassessment of the Primary Nephrotic Diseases Laura Barisoni,* H. William Schnaper, and Jeffrey B. Kopp *Department of Pathology, New York
Diabetes, Obesity and Heavy Proteinuria
 Diabetes, Obesity and Heavy Proteinuria Clinical Case 41 yo Black woman with heavy proteinuria History 2014: noted to have proteinuria on routine lab testing (1.1g/g). 1+ edema. Blood pressure has been
Diabetes, Obesity and Heavy Proteinuria Clinical Case 41 yo Black woman with heavy proteinuria History 2014: noted to have proteinuria on routine lab testing (1.1g/g). 1+ edema. Blood pressure has been
Index. electron microscopy, 81 immunofluorescence microscopy, 80 light microscopy, 80 Amyloidosis clinical setting, 185 etiology/pathogenesis,
 A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
Low-Density Lipoprotein Apheresis Therapy for Steroid- and Cyclosporine-Resistant Idiopathic Membranous Nephropathy
 CASE REPORT Low-Density Lipoprotein Apheresis Therapy for Steroid- and Cyclosporine-Resistant Idiopathic Membranous Nephropathy Yoshinori Sato,3, Shinichiro Tsunoda 2,3, Tsuyoshi Nozue 3,QinyaPan 3, Harue
CASE REPORT Low-Density Lipoprotein Apheresis Therapy for Steroid- and Cyclosporine-Resistant Idiopathic Membranous Nephropathy Yoshinori Sato,3, Shinichiro Tsunoda 2,3, Tsuyoshi Nozue 3,QinyaPan 3, Harue
Nephrotic syndrome Dr.Basma Adel FIFTH GRADE
 Nephrotic syndrome Dr.Basma Adel FIFTH GRADE 2017-2018 At the end of this lecture you should know: Types Pathophysiology Clinical manifestations D.Dx. Investigations. Treatment. Complications. 12/3/2017
Nephrotic syndrome Dr.Basma Adel FIFTH GRADE 2017-2018 At the end of this lecture you should know: Types Pathophysiology Clinical manifestations D.Dx. Investigations. Treatment. Complications. 12/3/2017
Dr Michael Rayment Chelsea and Westminster Hospital, London
 17 TH ANNUAL CONFERENCE OF THE BRITISH HIV ASSOCIATION (BHIVA) Dr Michael Rayment Chelsea and Westminster Hospital, London 6-8 April 2011, Bournemouth International Centre A decade of renal biopsies in
17 TH ANNUAL CONFERENCE OF THE BRITISH HIV ASSOCIATION (BHIVA) Dr Michael Rayment Chelsea and Westminster Hospital, London 6-8 April 2011, Bournemouth International Centre A decade of renal biopsies in
The CARI Guidelines Caring for Australasians with Renal Impairment. Idiopathic membranous nephropathy: use of other therapies GUIDELINES
 Idiopathic membranous nephropathy: use of other therapies Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES No recommendations possible based on Level I or II evidence
Idiopathic membranous nephropathy: use of other therapies Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES No recommendations possible based on Level I or II evidence
Secondary IgA Nephropathy & HSP
 Secondary IgA Nephropathy & HSP Anjali Gupta, MD 1/11/11 AKI sec to Hematuria? 65 cases of ARF after an episode of macroscopic hematuria have been reported in the literature in patients with GN. The main
Secondary IgA Nephropathy & HSP Anjali Gupta, MD 1/11/11 AKI sec to Hematuria? 65 cases of ARF after an episode of macroscopic hematuria have been reported in the literature in patients with GN. The main
